1
Introduction
The workplace is where 156 million working adults in the United States spend many waking hours, and it has a profound influence on health and well-being. Work-related injuries and illnesses can impact quality of life (BLS, 2017a). Although some occupations and work-related activities are more hazardous than others and face higher rates of injuries, illness, disease, and fatalities, workers in all occupations face some form of work-related safety and health concerns (e.g., musculoskeletal disorders arising from repetitive motions, work-related stress, pulmonary symptoms or diseases caused by airborne exposures, and injuries resulting from falls or unstable work areas). Not only are such hazards a threat to worker wellbeing and hence to the nation’s health, but one study estimated the annual cost of occupational injuries, illnesses, and deaths in the United States at $250 billion, which is more than the $219 billion for all cancer and approaching the $431.8 billion for all cardiovascular disease (Leigh, 2011). Reducing that health burden is the goal of occupational safety and health (OSH) surveillance.
OSH surveillance provides the data and analyses needed to improve worker safety and health and to understand the relationships between work and injuries and illnesses. Today, OSH surveillance efforts are fragmented across multiple federal and state agencies that collect, store, analyze, and interpret data to meet their specific agency needs. Agency resources dedicated specifically to work-related safety and health surveillance are limited, partly because the responsibility for occupational health and safety issues is divided between labor and public health and there has never been core public health funding allocated specifically for OSH surveillance. Many
factors point to a need to rethink and improve OSH surveillance in the United States including changes in the nature of work, the workforce, and employer-worker relationships that have occurred over the past 40 years along with ever evolving methods and technologies for identifying, reducing, and eliminating work-related health and safety risks.
A more cohesive and “smarter” OSH surveillance system is needed to address the demands and concerns of the current and future workforce. It needs to be “smarter” in the sense that the system needs to be one that demonstrates efficiencies, integrates strategies across multiple data sources, coordinates efforts across key surveillance agencies, and applies domain knowledge effectively to interpret data and to deliver insights to key stakeholders. Furthermore, there is an opportunity to think creatively about envisioning how that “smarter” system might build upon the current system and regulatory climate in the United States and take full advantage of new information technologies. Additionally, effective and comprehensive OSH surveillance models from other countries can be explored. This report aims to put forth a vision and pragmatic framework for a national OSH surveillance system in the United States with the goal of improving worker safety and health.
BACKGROUND
The topic of occupational safety and health surveillance across the United States was last examined comprehensively in a 1987 National Research Council (NRC) report Counting Injuries and Illnesses in the Workplace: Proposals for a Better System (NRC, 1987). In a more recent series of eight reports by the NRC and the Institute of Medicine that evaluated the National Institute for Occupational Safety and Health’s (NIOSH’s) research programs, all of the reports identified the need for improved OSH surveillance and for additional surveillance research (IOM and NRC, 2009). The Council of State and Territorial Epidemiologists has also issued calls for improvements to address surveillance gaps (Boulton et al., 2003; CSTE, 2010, 2014). There is recognition that surveillance could be conducted more innovatively and collaboratively; for instance, by leveraging activities and resources regardless of whether they are drawn directly from various sectors of the workforce or other public health domains, or borrowed from unrelated fields. There is also the recognition that enhanced coordination of surveillance activities could enable individual state and federal agency responsibilities to better protect workers. New data sources and information technologies, such as those supporting health care reform (the Affordable Care Act), could also be used to support occupational safety and health needs.
Changes in the Nature of Work and the Workforce and Implications for Occupational Safety and Health
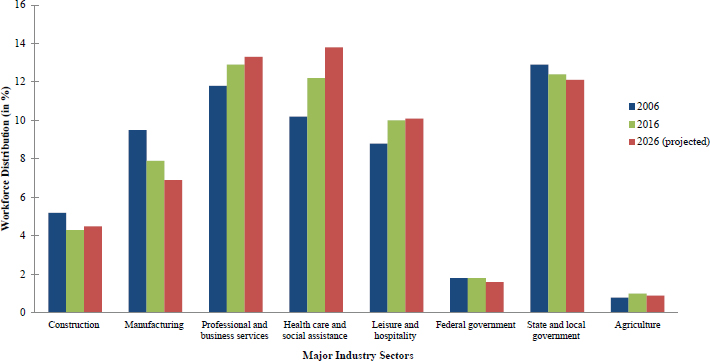
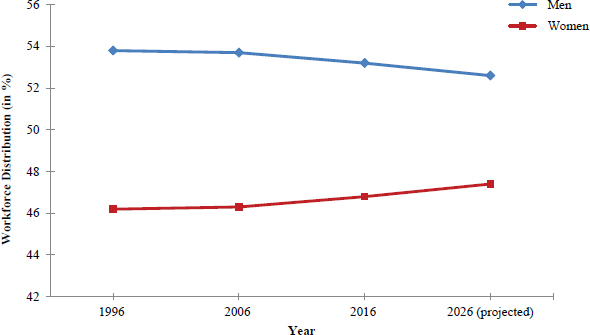
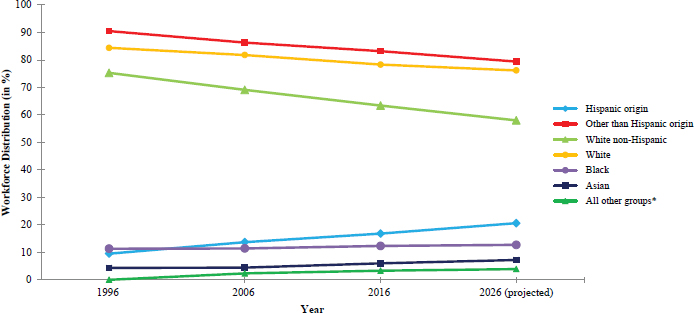
Since the 1987 report, there have been major changes in the nature of work, including employee-employment arrangements, the distribution of employment among industry sectors, and the demographics of the workforce (see Figure 1-1; BLS, 2017a). Employment in manufacturing has declined, while significant growth in employment has occurred in the service sector, including health care. Individuals are likely to be working more than one job over their working life, and may hold multiple jobs at the same time. Growth has occurred in nonstandard work arrangements, such as the use of independent contractors and the outsourcing of functions to other entities, and the development of “on-demand” or “gig” work, where employment is characterized by short-term contracts or freelance work (e.g., drivers who contract with ride-share companies) (Katz and Krueger, 2016). Furthermore, the workforce is more diverse and includes more women (Figure 1-2), racial and ethnic minorities (Figure 1-3), and immigrants (Myers et al., 2013; BLS, 2017b). With these shifts in work and the workforce, employment is more precarious and many workers lack the protections and rights afforded by laws and regulations that make them more vulnerable and subject to abuse.
Approaches to occupational safety and health surveillance have yet to evolve to address effectively the changing nature of work. For example, some current data-collection approaches that use “establishments” as the basic employer unit typically rely on single employers and worksites, which
are insufficient because those approaches are unable to capture gaps and emerging concerns created by the evolution of employment (Weil, 2014). Furthermore, data on hazards, protective safety, and health-management practices in individual work settings have not routinely been collected in a systematic way.
The ability to carry out rigorous workforce safety and health surveillance has other challenges as well. For example, in certain industry sectors (such as agriculture) or demographic groups (such as day laborers or teenagers), the total number of workers in an industry is necessarily a rough estimate due to temporal fluctuations or the nature of the work. The limitations of such denominator data make it difficult to determine baseline rates for injuries or illnesses in order to measure risks, track trends, and evaluate the effectiveness of efforts to reduce injury and disease.
A major change has been in the evolution, effectiveness, and relative ubiquity of information and communications technology (both methods and tools) since the 1987 report. Major advances in data collection and storage, analytic methods, sensors, and mobile devices allow information to be gathered and connected with central collection resources. Although the revolution of Internet search methods has made it easier to search for information, the quality of such large amounts of data obtained is uneven depending on factors such as source and age. Social media have also become sources of insight regarding societal trends and offer one of many methods for information dissemination that new technologies can provide. Occupational safety and health surveillance efforts will need to leverage newer technologies and tools for identifying, organizing, analyzing, and interpreting data in more innovative, powerful, and cost-effective ways. Doing so could reveal problems, trends, and emerging issues within and across sectors, groups, and geographic regions of workers. Also, these technologies offer opportunities to improve the dissemination of information to those that can use surveillance data to take preventive action, thereby improving worker safety and health and reducing associated human and economic costs of work-related injuries and illnesses.
PURPOSE OF THIS STUDY
The National Academies of Sciences, Engineering, and Medicine formed an ad hoc committee to undertake the current study requested and sponsored by three key federal agencies involved with occupational safety and health: NIOSH, the Bureau of Labor Statistics (BLS), and the Occupational Safety and Health Administration (OSHA). The committee was tasked with developing a vision for “smarter” occupational safety and health surveillance in the United States (see Statement of Task, Box 1-1). To address the task statement, the collective expertise and experience of
the committee includes individuals with expertise in occupational epidemiology, occupational medicine, occupational safety and health, hazard/exposure surveillance, public health, statistics, survey methods, biomedical informatics, data mining and analytics, economics, cost-benefit analysis, and workplace organization and management (see Appendix B). The committee held information-gathering meetings with invited experts to help it address its task, and members of the public were invited to attend and provide comments at these meetings (see Appendix C).
The committee intends the report to be useful to the study sponsors and to other federal and state agencies that have an interest in occupational safety and health. The report may also be of interest broadly to employers, labor unions and other worker advocacy organizations, the workers’ compensation insurance industry, as well as state epidemiologists, academic researchers, and the broader public health community. The study was undertaken over an 18-month period during which there were major changes in the U.S. political scene and in government priorities. Because of uncertainties regarding those evolving priorities and resource availability, the committee has offered observations and recommendations that are intended to suggest useful efforts for both the short and long term. The report’s short-term recommendations in most cases do not require new resources except in cases where new work is recommended, new resources may be required (e.g., see Recommendation D in Chapter 6). The recommendations are lettered alphabetically in the order that they appear in the report and do not correlate with their order of priority; however, actions to carry out the recommendations along with the timing and methods for addressing them will be dependent on the creation of the coordinating entity recommended in the meta-recommendation (Recommendation Q; see Appendix A for the full recommendations). The committee views the report as serving as a reference that will serve the long-term planning needs of the OSH community and other stakeholders, independent of the availability of new OSH resources or opportunities for organizational change in the short term.
KEY TERMS AND DEFINITIONS
Occupational Safety and Health Surveillance
Surveillance is not unique to occupational safety and health. The Centers for Disease Control and Prevention (CDC) identified surveillance as the first of the 10 core public health functions: “[To] monitor environmental and health status to identify and solve community environmental health problems” (CDC, 2011). Surveillance is defined by CDC as “the ongoing, systematic collection, analysis, and interpretation of health data, essential to the planning, implementation and evaluation of public health practice,
closely integrated with the dissemination of these data to those who need to know” (Thacker et al., 2012). Many argue that surveillance is the cornerstone of public health practice, because successful prevention programs inevitably build on an effective system for monitoring and responding to what happens in the community. Quality public health surveillance efforts rely on consistent and systematic application of methods over time. Gathering data is of little value if those data are not analyzed and interpreted to produce information and understanding that is promptly disseminated to those in a position to take action.
There is a useful distinction between case- and population-based surveillance. In case-based approaches, the focus is on early identification of individual cases that require follow-up or immediate action by those who are typically legally mandated to do so (for example, the efforts of public health workers who identify and rapidly isolate or treat those with communicable diseases and of public health scientists who control or isolate an identified hazardous exposure). In population-based surveillance the focus is on a wider group and on collecting data to assess the extent of a health-related event and to monitor trends within a defined population over time and locale. Case- and population-based surveillance activities are complementary approaches. A specific circumstance may require immediate attention or intervention, even while the information about that case contributes to the ongoing collection of data about a population of similar individuals.
OSH surveillance is a subset of the broader public health surveillance field. In OSH surveillance, data are collected on work-related health outcomes (e.g., injuries, diseases, or fatalities) and on the presence of health and safety hazards (e.g., hazardous exposures or conditions). To date, the major focus has been on gathering data about health outcomes and analyzing these data to identify both sentinel cases and trends to inform the targeting and evaluation of efforts to control hazards and prevent occupational injuries and illnesses. The information produced by surveillance has also been used to inform policy development, to guide educational and regulatory activities, to develop safer technologies, and to enable research. The issue of hazard surveillance has not been emphasized in the U.S. approach to OSH surveillance, although it is a topic that may be addressed internally by some larger employers and is an area of ongoing investigation.
Research on OSH surveillance is valuable, both for deriving new insights and recommending new interventions (i.e., research “using” data collected through surveillance) and for addressing the needs of the surveillance community to develop new approaches or technologies to address shortcomings in current surveillance practices (i.e., research “in support of” surveillance processes and methods). Both surveillance activities and surveillance research are driven by the actual practice of occupational safety and health. In that applied context, information produced by the
analysis and interpretation of data collected through surveillance is used to address a problem in a specific workplace, industry, or region, often working with employers, workers’ organizations, and health care providers. In understanding OSH surveillance, it is useful to consider three key elements: processes that constitute a surveillance system, components that enable these processes, and methods that are applied to accomplish surveillance processes. Chapter 6 of this report focuses on the processes, and Chapter 7 identifies and discusses enabling components and associated methods (see Box 1-2 for definitions).
Issues of data completeness and data quality underlie all OSH surveillance. Throughout this report attention is directed to overcoming some of the known limitations in collecting data on the wide range of working populations. For example, one limitation in the Bureau of Labor Statistics annual Survey of Occupational Injuries and Illnesses (SOII) is that it does not include self-employed individuals, contract workers, or those in on-demand jobs.
As a core public health function, surveillance provides timely information to control or prevent exposure to hazards with the goal of reducing morbidity and mortality and improving population health. Thus, surveillance is generally viewed in a positive light and as a public good. Surveillance activities need to be sensitive to the privacy rights of individuals, and transparency is needed to ensure that all relevant stakeholders are informed about the steps that are taken to appropriately protect data collected about individual workers and the workplace. Thus, in public health and occupational health settings, the term surveillance is generally free of the negative connotations associated with government intrusion into the private lives of individuals. Concerns about privacy and confidentiality in occupational health surveillance are perhaps most pertinent if the information about an employee’s health could be used by an employer against the employee. Ensuring that an ethical framework continues to undergird OSH surveillance is critical to providing necessary information to protecting workers and achieving safer and healthier workplaces.
Employers can find OSH surveillance requirements challenging. Employers understand that they have the primary responsibility for safety in their workplaces—as part of their ethical duty to their employees, as mandated by statute, and to maintain a sustainable workforce in today’s economy. While employers often seek useful and timely information to improve safety in their workplaces, they may become concerned if they feel that their time and efforts are spent primarily for the sake of regulatory compliance. The OSH surveillance community is well aware of potential tensions and the need to ensure that complying with reporting requirements provide results that are valued by employers and workers.
Workplace Hazard and Exposure Surveillance
In the United States, OSH surveillance has focused primarily on health outcomes (lagging indicators) while hazard surveillance (a leading indicator) has received less attention. Hazard refers to the potential of a substance or condition to cause harm, while risk considers the probability that the hazard will cause harm. Thus, the health risk of a working condition is a function of both the presence of a hazard associated with the health condition and the extent of the exposure of an individual or population to that hazard.1 In the context of surveillance, a hazard surveillance system (e.g., a chemical use inventory or registry) identifies potential workplace hazards and can provide information on the distribution and location of a hazard where there is potential for exposure. An exposure surveillance system, monitors actual contact that workers have with the substance or condition (potentially including data on who the workers are who were exposed, the duration of the exposure, and the level or intensity of the exposure).
Although the discussion above is most easily understood in terms of airborne chemical hazards or physical agents, it is equally relevant to acute injury risks. For instance, work at height may be considered a hazard, whereas the exposure would be the proximity of the work to an unguarded leading edge. Similarly, moving heavy objects to an elevated position may constitute a hazard, the exposure would be related to the weight, the frequency and the biomechanical load determined by the lifting task, and presence of mechanical lifting aids.
The relationships among hazard, exposure, and the “work-relatedness” of an illness or injury can be highly complex and subject to interpretation (Oppliger and Seixas, 2017). An injury or illness is work related if it was sustained in the workplace. However, only a small proportion of illnesses where work is a component in the mix of causes are currently ascribed to work exposures. For example, an individual’s lung disease (e.g., chronic obstructive pulmonary disease or asthma) or chronic back strain can be due to work-related exposures along with other factors in the worker’s life or genetic makeup (see Chapter 4). Oppliger and Seixas (2017) note that “Even ascribing acute injury to work is not as obvious as identifying the location at which the injury occurs; an injury at work may be partially due to non-work-related stressors (e.g., personal stressors affecting attention or vigilance) while injuries off the job may commonly have work-related contributions (e.g., neurologic toxins, long hours, shift work, or other stressors causing fatigue, etc.)”. Thus, for both acute and chronic injuries and illnesses, agreed-upon surveillance case definitions are necessary to
___________________
1 Risk=f(Hazard, Exposure). Where risk is the probability of an adverse outcome in a defined population; hazard is the inherent damaging potential of agent or condition; and exposure is the probability, frequency, and intensity of the agent interacting with an individual.
manage the uncertainty of the contribution of work to a wide range of health conditions.
In addition to physical, chemical, and biological agents, musculoskeletal strain is increasingly recognized in many jobs associated with a wide range of both acute and chronic injury and a significant degree of disability. Even so, the assessment of various elements of exposure for musculoskeletal risks—including force, posture, repetition, work pace, work-rest cycles, and sedentary work—continues to present significant challenges.
The assessment of hazardous psychosocial exposures in the workplace is also challenging, with the potential for health impacts related to work organization (e.g., numbers of coworkers, social support, reporting relationships, and supervisory responsibilities), job demands (e.g., hours, shift work, unpredictability, and exposure to demanding customers), job control (e.g., ability to control rate or order of work components), and fair treatment (e.g., perceptions that both the individual and workers in general are being treated fairly by the employer). Health effects generally associated with these include cardiovascular disease, depression and anxiety, suicide, effects related to sleep deprivation including injury risk, and even workplace violence.
Costs, Effectiveness, Efficiency, and Cost Effectiveness
One important goal of a 21st-century OSH surveillance system is to collect the most relevant data at the lowest cost feasible. A surveillance system would meet the definition of being cost effective if it identifies data with the biggest impact on improving worker safety and health while minimizing the cost of collecting those data (Gold et al., 1996; Haddix et al., 1996). A cost-effective surveillance system would also recognize trade-offs between the importance of individual data elements in identifying factors that can be modified to improve worker safety and health and the costs of collecting each of those data elements. As a result, a cost-effective surveillance system might be less comprehensive than an ideal system because the costs of collecting the ideal set of surveillance data might be judged to be prohibitively expensive from a societal perspective. Finally, an efficient system for collecting OSH data may not be effective or cost effective if it targets the collection of data that have only minimal impact on improving worker safety and health outcomes.
A fundamental concept in conducting a cost-effectiveness analysis of any intervention, including an OSH surveillance system, is that costs and benefits are always measured and compared from a societal perspective (Gold et al., 1996; Haddix et al., 1996; Muennig, 2008). A societal perspective is preferred when considering the value of public investments and policy because comparing costs and benefits solely from the perspective of
individual stakeholders can lead to erroneous conclusions and recommendations. Thus, this report adopts a societal perspective of cost effectiveness.
The costs of a surveillance system include not only the costs of data collection, but also the costs associated with the health and productivity consequences of occupational exposures, injuries, illnesses, and mortality on workers, their families, and society. As previously noted, the most recent estimate of the total economic burden of occupational illness, injury, and death is $250 billion annually in the United States (Leigh, 2011). Therefore, an improved OSH data surveillance system can be used by policy makers and stakeholders to prioritize interventions for reducing the economic costs of occupational illness, injury, and death to society. Identifying areas of greatest need for OSH interventions through use of an improved surveillance system and then targeting effective interventions based on previous research and evidence is likely to produce significant and substantial savings to employers, employees, and society (Schulte et al., 2017). The importance of assessing costs and benefits of an improved OSH surveillance system is discussed further in Chapter 7.
ORGANIZATION OF THE REPORT
This report covers the breadth of the committee’s statement of task. Chapter 2 sets forth the guiding principles and objectives developed by the committee and used as a basis for the report’s recommendations. The chapter also provides an overview of the committee’s vision of a future “smarter” surveillance system. In Chapter 3 the committee examines the federal and state agencies and stakeholders engaged in occupational safety and health surveillance in the United States. It also summarizes the major recommendations of the 1987 NRC report and the response to that report’s recommendations. Chapter 4 provides a more detailed summary of the current status of OSH surveillance in the United States. It summarizes the current approaches to surveillance of fatal and nonfatal occupational injuries and of occupational illnesses. The chapter also discusses the current, albeit limited, state of hazard surveillance and addresses the crosscutting issues of state-based surveillance, surveillance research, and data on populations at risk. OSH surveillance activities outside the United States are summarized in Chapter 5, emphasizing activities that may offer lessons for ongoing work in this country. To address the gaps identified in Chapter 4, Chapter 6 then discusses the promising developments, processes, and technologies that can be used to improve OSH surveillance, including electronic reporting initiatives, electronic health records, the mobilization of workers’ compensation systems, and new directions for hazard surveillance. This is followed by a focus in Chapter 7 on key actions essential for moving forward with an improved national OSH surveillance system, emphasizing (1) quantification
of the economic and health burden of occupational illness and injury, (2) coordination of surveillance efforts, (3) use of information technology, and (4) enhanced training and support for surveillance practitioners. The report’s concluding chapter offers a final overarching meta-recommendation and summarizes the report’s conclusions and recommendations for achieving a smarter OSH surveillance system.
REFERENCES
BLS (Bureau of Labor Statistics). 2017a. Employment by major industry sector. Available online at https://www.bls.gov/emp/ep_table_201.htm (accessed November 21, 2017).
BLS. 2017b. Civilian labor force participation rate, by age, sex, race, and ethnicity. Available online at https://www.bls.gov/emp/ep_table_303.htm (accessed November 21, 2017).
Boulton, M. L., R. A. Malouin, K. Hodge, and L. Robinson. 2003. Assessment of the epidemiologic capacity in state and territorial health departments—United States, 2001. MMWR 52(43):1049-1051.
CDC (Centers for Disease Control and Prevention). 2011. Core functions of public health and how they relate to the 10 essential services. Available online at https://www.cdc.gov/nceh/ehs/ephli/core_ess.htm (accessed April 10, 2017).
CSTE (Council of State and Territorial Epidemiologists). 2010. 2009 National assessment of epidemiology capacity: Findings and recommendations. Available online at http://www.cste2.org/webpdfs/ecabrieffinal2010.pdf (accessed August 22, 2017).
CSTE. 2014. 2013 National assessment of epidemiology capacity: Findings and recommendations. Available online at http://www.cste2.org/2013eca/CSTEEpidemiologyCapacityAssessment2014-final2.pdf (accessed August 22, 2017).
Gold, M. R., J. E. Siegel, L. B. Russell, and M. C. Weinstein. 1996. Cost-Effectiveness in Health and Medicine. New York: Oxford University Press.
Haddix, A. C., S. M. Teutsch, P. A. Shaffer, and D. O. Dunet. 1996. Prevention Effectiveness: A Guide to Decision Analysis and Economic Evaluation. New York: Oxford University Press.
IOM and NRC (Institute of Medicine and National Research Council). 2009. Evaluating Occupational Health and Safety Research Programs: Framework and Next Steps. Washington, DC: The National Academies Press.
Katz, L. F., and A. B. Krueger. 2016. The rise and nature of alternative work arrangements in the United States, 1995-2015. National Bureau of Economic Research: NBER Working Paper No. 22667. Available online at http://www.nber.org/papers/w22667 (accessed November 29, 2017).
Leigh, J. P. 2011. Economic burden of occupational injury and illness in the United States. Milbank Quarterly 89(4):728-772.
Muennig, P. 2008. Cost-Effectiveness Analyses in Health: A Practical Approach, 2nd ed. San Francisco, CA: Jossey-Bass.
Myers, D., S. Levy, and J. Pitkin. 2013. The Contributions of Immigrants and Their Children to the American Workforce and Jobs of the Future. Washington, DC: Center for American Progress. Available online at: https://www.americanprogress.org/issues/immigration/report/2013/06/19/66891/the-contributions-of-immigrants-and-their-children-to-the-american-workforce-and-jobs-of-the-future/ (accessed November 22, 2017).
NRC (National Research Council). 1987. Counting Injuries and Illnesses in the Workplace: Proposals for a Better System. Washington, DC: National Academy Press.
Oppliger, A., and N. Seixas. 2017. What makes a disease ‘occupational’? Annals of Work Exposures and Health 61(2):135-136.
Schulte, P. A., R. Pana-Cryan, T. Schnorr, A. L. Schill, R. Guerin, S. Felknor, and G. R. Wagner. 2017. An approach to assess the burden of work-related injury, disease, and distress. American Journal of Public Health 107(7):1051-1057.
Thacker, S. B., J. R. Qualters, and L. M. Lee. 2012. Public health surveillance in the United States: Evolution and challenges. Morbidity and Mortality Weekly Report 61(3):3-9.
Weil, D. 2014. The Fissured Workplace: Why Work Became So Bad for So Many and What Can Be Done to Improve It. Cambridge, MA: Harvard University Press.
This page intentionally left blank.
















