Given the complexity of pain, several workshop participants highlighted the need for a greater understanding of the underlying mechanisms of pain. Throughout the workshop, individual participants explored the known cellular and molecular mediators of pain and considered opportunities in the preclinical space that might advance therapeutic development.
NEURAL CIRCUITS, CELLS, AND MOLECULAR MEDIATORS OF PAIN
There have been great advances in understanding pain from a systems and circuitry perspective, as well as the physiology and cell biology of central and peripheral systems mediating pain sensation and behavior, said Tony Yaksh. This understanding now includes the recognition that pain processing involves complex circuitry as well as the involvement of neuronal and non-neuronal cells, synapses, sodium channels, and inflammatory mediators (Woller et al., 2017). Moreover, there is a commonality in some of the neural circuits involved in pain and addiction, as well as in depression, said Nora Volkow. Indeed, patients with substance use disorders are at much greater risk of suffering from chronic pain, and patients with chronic pain are at greater risk of suffering from depression, she added. What that means is that targeting this shared neurocircuitry may have wider benefits than would be had simply by targeting the μ-opioid or the type 3 dopamine receptor, said Volkow.
Although neuron transmission in acute pain is relatively well understood, the molecular physiology of chronic pain remains less clear, said Luda Diatchenko, professor and Canada Excellence Research Chair in Human Pain Genetics at McGill University. Only recently have scientists begun to understand the genetics of pain, she said. From studies of very rare monogenic pain disorders, the first gene linked to pain—the gene for the neurotrophin nerve growth factor (NGF)—was identified about 20 years
ago (Indo et al., 1996). Diatchenko said that understanding the mechanisms by which NGF enhances pain led to the identification of two major drug targets, NGF itself and its cognate receptor—the tropomyosin-related kinase A receptor (TrkA) (Mantyh et al., 2011). More recently, mutations in the sodium channel gene SCN9A were found to be responsible for more than half of all cases of congenital insensitivity to pain (Drenth and Waxman, 2007). Diatchenko said that more than six pharmaceutical companies have compounds targeting the sodium channel in development.
Today, thanks to genetic linkage analysis and association studies, dozens of genes have been associated with various pain conditions (Zorina-Lichtenwalter et al., 2016) (see Figure 3-1).
More genome-wide analysis studies (GWASs) are coming, said Diatchenko. Her lab has put together a searchable database called the Human Pain Genes Database (HPGDB) to summarize information about each single positive association result as a tool to be used for drug development.
William Maixner, suggested that genetic studies are enabling what he called “reverse translation,” in which identification of genes linked to disease lead to the identification of targets. Using molecular signatures identified in a series of cohort studies, he and his colleagues have identified three novel targets: epidermal growth factor receptor (EGFR) (Martin et al., 2017), β-adrenergic receptor (Martin et al., 2015), and the six trans-membrane helix isoform of the μ-opioid receptor (6TM-mOR) (Shabalina et al., 2009). There are now chemical entities in development, ready to move from preclinical to clinical studies, he said.
PRECLINICAL EFFORTS TO IDENTIFY PAIN TARGETS AND TREAT PAIN
To gain a better understanding of what is needed for the development of safe, effective, and non-addictive pain treatments, many workshop participants discussed novel methods for identifying targets for pain and considered what might be done to improve target validation.
Genetic Approaches for Target Identification and Translation
The discovery of genetic variants that are associated with any medical condition provides novel biological insight and potential therapeutic targets and biomarkers, which can be used to advance the development of new treatments, including personalized medicine, said Diatchenko. Translating
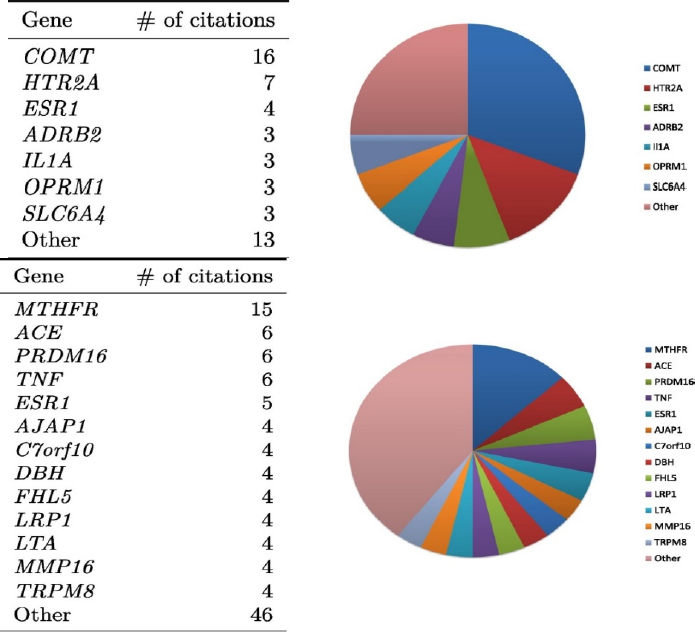
NOTE: ACE = angiotensin I converting enzyme; ADRB2 = beta-2 adrenergic receptor; AJAP1 = adherens junctions-associated protein 1; C7orf10 = succinylCoA:glutarate-CoA transferase; COMT = catechol-O-methyl transferase; DBH = dopamine beta-hydroxylase; ESR1 = estrogen receptor 1; FHL5 = four-and-a-half LIM domains 5; GCH1 = GTP cyclohydrolase; HTR2A = 5-hydroxytryptamine (serotonin) receptor 2A; IL1A = interleukin 1A; LRP1 = low density lipoprotein receptor-related protein 1; LTA = lymphotoxin alpha; MMP16 = matrix metalloproteinase 16; MTHFR = methelynetetrahydrofolate reductase; OPRM1 = mu-1 opioid receptor; PRDM16 = PR domain-containing 16; SLC6A4 = solute carrier family 6 (serotonin transporter); TNF = tumor necrosis factor; TRPM8 = transient receptor potential cation channel, subfamily M, member 8 (menthol and cold receptor).
SOURCES: Presented by Luda Diatchenko, October 12, 2017; Zorina-Lichtenwalter et al., 2016.
those discoveries into new drugs involves several steps, moving from association studies, to understanding the molecular genetic mechanisms of functional variants, to animal studies demonstrating how the genetic variant contributes to pain in vivo, and finally to clinical trials. Diatchenko
used the metaphor of a “translational clock” to illustrate how her team “ticked” through these steps on the way to developing a treatment for facial pain. They first showed that variants of the gene encoding catecholamine-O-methyltransferase (COMT) were associated with pain sensitivity and the risk of developing facial pain (Diatchenko et al., 2005). Next, they identified the molecular mechanism via the alternation of the secondary structure of RNA responsible for this phenomenon (Nackley et al., 2006). Following this, they showed in animal models that pain sensitivity is increased by inhibiting COMT via the activation of beta adrenergic receptors (Nackley et al., 2007); and finally they conducted a clinical trial, which showed that propranolol, a non-selective beta-blocker, was effective in treating facial pain in the manner dependent of COMT genotype (Tchivileva et al., 2010). Using a similar approach, they have demonstrated that inhibition of EGFR with compounds already on the market blocks pain in mice (Martin et al., 2017). Diatchenko noted that both of these approaches use repurposed drugs, and that neither of these classes of drugs have a potential for abuse.
Genetics has also shown that there may be multiple molecular pathways leading to a single pain syndrome such as migraine (Freilinger et al., 2012), said Diatchenko. What that means, she said, is that even in a population subgroup there may be heterogeneity in response to a certain treatment. Moreover, genetic variants and pathways that contribute to chronic pain are not necessarily organ specific, but may be involved in many different types of pain, she added. Instead of planning treatment regimens based on the type or site of pain, it may be more effective to use molecular profiling of individuals to identify therapeutic targets (see Figure 3-2). This will require a lot more GWASs, she said, and can only be done through the collaboration of geneticists working across different pain fields.
Disease Modeling in Human Cells, Tissue, and Organoids
Clifford Woolf proposed using stem cell–derived neurons for the following purposes: investigating known targets, conducting target-based drug screens, disease modeling to identify mechanistic drivers of pain, identifying individuals at risk of transitioning from acute to chronic pain, conducting phenotypic drug screens, aiding in personalized treatment selection, and conducting in vitro clinical trials. This is possible, he said, by
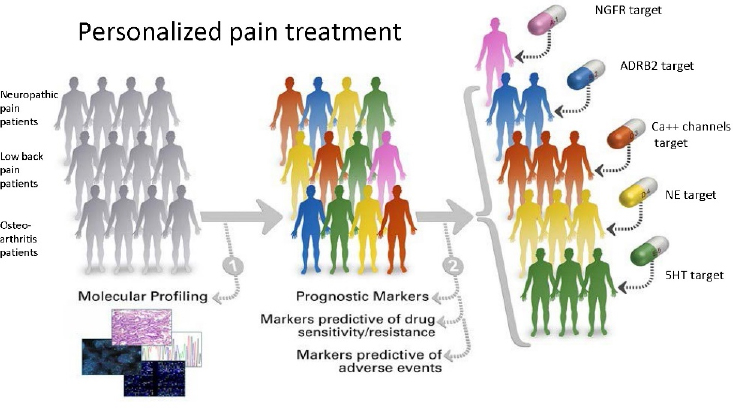
NOTE: 5-HT = serotonin; ADRB2 = beta-2 adrenergic receptor; Ca++ = calcium; NE = norepinephrine; NGFR = nerve growth factor receptor.
SOURCE: Presented by Luda Diatchenko, October 12, 2017.
combining stem cell technology with CRISPR1 engineering technology, which allows investigators to generate induced pluripotent stem cells (iPSCs) from the fibroblasts of patients with a certain phenotype, characterize neurons grown in culture from those iPSCs, replicate mutations identified in the patient material, and engineer mice to have those same mutations.
For example, his lab has used this approach to interrogate nociceptor or nociceptor-like cells that have high expression of the voltage-gated sodium channel Nav 1.7. Nociceptors are peripheral neurons that detect noxious thermal, mechanical, or chemical stimuli (Basbaum et al., 2009). Woolf and colleagues created cell types with different mutations and were then able to grow clones of these cells and characterize the phenotypes associated with each mutation, including key phenotypes such as temperature sensitivity, which replicates what patients experience.
___________________
1 Clustered Regularly Interspaced Short Palindromic Repeats (CRISPR) is a new, cheap, quick, and easy-to-use gene-editing technique that allows investigators to alter the DNA of nearly any cell or organism.
Woolf said they can also interrogate biophysical properties of sodium channels to determine why certain mutations produce particular phenotypes. Beyond disease modeling, they are also able to use these cells for high-throughput, target-based drug discovery, he said. For instance, they have created panels of cells that express different voltage-gated sodium channels, and used these panels to screen for subtype-specific sodium channel blockers. This is important, he said, because different sodium channels are expressed in different tissues, and it could be dangerous to block a channel that is expressed in cardiac muscle, for example.
According to Woolf, another potentially attractive strategy using the iPSC-CRISPR approach would be to move away from subtype-specific blockers and focus instead on blocking particular cell types or disease states in cells. The advantage of this phenotypic approach is that each cell type has a unique molecular signature in terms of the ion channels expressed. Relatively “dirty” drugs that act on multiple channels with different efficiencies may, in fact, offer advantages for certain disease conditions, he said. Conducting a screen of several thousand compounds annotated to act predominantly on one or several targets could reveal a pattern or signature of compounds that affect a particular phenotype, providing remarkable insight into which pathways are up- or down-regulated in that phenotype, said Woolf. The crucial feature of this approach, he said, is to find a phenotype that is a true surrogate of the human disease state.
Woolf said he thinks it is likely that by using human neurons, it will be possible to develop cell-type and disease-type selective blockers that can provide personalized therapeutics for individual patients, and detect novel agents that act on different cells and different diseases. Stem cells may also be useful to conduct phenotypic screens and screens based on the risk of developing a disease, he said. For example, this approach could allow clinicians to identify in advance patients who are at risk of developing peripheral neuropathy when treated with certain chemotherapeutic agents, and then tailor chemotherapy to the patient. He added that iPSCs could also be used to explore the mechanisms that lead to chemotherapy-induced peripheral neuropathy or to other clinical pain syndromes and identify novel agents that protect against those effects. To accomplish this would require analyzing multiple iPSC lines from deeply phenotyped and genotyped patients, stated Woolf.
Monitoring and Modulating Circuit Activity in Pain
Robert Gereau, professor of anesthesiology at Washington University, proposed an in vivo approach to assessing neural activity at a cellular-level resolution using tools developed as part of the BRAIN Initiative,2 a public–private partnership launched in 2013 to accelerate development of new technologies for mapping brain cells and circuits in order to better understand brain diseases. His lab has been developing optogenetic tools that enable manipulation of neuronal activity in vivo by engineering specific neurons to express light-sensitive proteins, and then using light to entrain action potential firing and manipulate cell function (Copits et al., 2016; Deisseroth, 2011). Gereau said optogenetics provides finer control over the nervous system than was previously possible. By enabling manipulation of subsets of neurons, cell-type specific control is possible, he said.
Early optogenetics studies used implantable fiber optic lasers, said Gereau. More recently he and his colleagues have developed fully implantable, wirelessly powered micro light-emitting diodes (LEDs) (Park et al., 2015), and near-field communication-powered devices implanted in the brain or peripheral structures to provide precise control of neural circuits while at the same time assessing behavioral measures commonly used in animal models. Moving from wired to wireless technologies allows investigators to study responses under more natural conditions, said Gereau. To achieve cellular and subcellular resolution, optogenetic techniques are also used in combination with two-photon microscopy and a virtual-reality behavioral apparatus that allows the animal to be unrestrained, said Gereau.
This technology and others that have been advanced by the BRAIN Initiative are developing rapidly, said Gereau, enabling the identification of cells and circuits that change in association with the development of chronic pain. Steven Hyman, director of the Stanley Center for Psychiatric Research at the Broad Institute, questioned the translatability of this approach to human diseases because they are not working with human cells. Volkow added that integrating all the complex factors relevant for the human condition into these models presents huge barriers. Gereau agreed that many hurdles must be overcome before it will be possible to manipulate circuitry in humans, but to dismiss this as an impossibility ignores the innovation and advances that have been made. He added that neuromodulation and neurostimulation therapies—which are less precise technologies in comparison to optogenetics—are already being used in humans. The
___________________
2 For more information, go to https://www.braininitiative.nih.gov (accessed January 2, 2018).
promise of being able to get cell-type specificity into these neuromodulatory therapies holds immense promise, he said.
Animal Models of Pain
A number of animal models have been developed to recapitulate the elements of pain from stimulus to behavior, and from acute to chronic, said Yaksh. In these animal models, pain may be induced by thermal, chemical, or mechanical injury; may be acute or persistent; and may evoke multiple different physiological (e.g., swelling and erythema) and behavioral (e.g., guarding of the paw, limb movement, vocalization) responses.
These various models have been used successfully in preclinical development of many different classes of drugs to treat different types of pain, said Yaksh. For example, he noted that antagonists, and more recently antibodies against the calcitonin gene-related peptide (CGRP) receptor, have been developed for the treatment of migraine based on preclinical studies demonstrating their efficacy (Durham and Vause, 2010; Tso and Goadsby, 2017). However, there have also been a number of drugs that appeared safe and efficacious in preclinical studies, but failed to show clinical efficacy or caused serious side effects in clinical trials, he said. Yaksh noted that while the number of pain drug candidates that move from preclinical to Phase I studies, and then advance to Phase II studies, is only about 11 percent; this figure compares favorably with other disease areas. Some of these compounds are not advanced for strategic or other reasons not reflecting a failure of the preclinical model, said Yaksh. Nonetheless, new approaches are needed to address shortcomings in existing models and to enable longer-term studies, he said. For example, longer-term studies are needed that model chronic inflammatory conditions such as arthritis; that more closely recapitulate the human phenotype; that address spontaneous versus evoked behaviors, thus precluding the need for ongoing handling by investigators; and that enable assessment of reinforcing effects of pain relief, said Yaksh. Volkow added that even when a signal is seen in an animal model, it may not be replicated in a clinical study because humans develop tolerance to the medication. For this reason, she said, preclinical animal models should be evaluated within time windows relevant for the human condition.
Selecting or developing the best model first requires that investigators determine what they are trying to model, such as whether it is evoked or spontaneous, whether it is associated with tissue or nerve injury or inflammation, and whether it is acute or chronic, said Yaksh. To illustrate the
challenges, he used the example of fibromyalgia, a condition that affects an estimated 2 to 8 percent of Americans, predominantly women (Clauz, 2014). Fibromyalgia is a clinical diagnosis with no confirmatory clinical or laboratory endpoint (Fitzcharles et al., 2013), said Yaksh. Diagnosis is based on the presence of multiple non-specific symptoms with no clear etiology. Symptoms include widespread musculoskeletal pain (including temporomandibular joint pain), fatigue, anxiety, affective disorders, dysautonomia, and sleep disorders (Sluka and Clauw, 2016). Of the preclinical models used for fibromyalgia (e.g., intramuscular hypertonic saline, reserpine-induced myalgia, and cold stress), none have any particular mechanistic relevance to the pain states as it relates to drug development, said Yaksh.
Preclinical Efforts Using Companion Animals
Pathological pain conditions that occur naturally in animals may also provide useful preclinical models. Dorothy Cimino Brown, lead executional scientist for Translational Comparative Medical Research at Elanco, the animal health division of Eli Lilly and Company, runs clinical trials in companion animals, especially dogs. Two types of pain conditions are common in dogs: osteoarthritis and bone cancer. Brown said that of the 72 million owned dogs in the United States, at least 20 percent have clinically significant osteoarthritis, and about 10,000 dogs each year develop bone cancer, usually osteosarcoma. In fact, bone cancer is more common in dogs than in people, she said. The standard of care of canine osteosarcoma is amputation and chemotherapy, but many owners opt for pain management instead of amputation. This choice creates a large population of animals ideally suited for clinical trials of medications in development for bone cancer pain, particularly for novel approaches to pain, said Brown. These trials can support the registration of new treatments for dogs, while at the same time informing human trials, she said. For example, she said that Centrexion Therapeutics is simultaneously developing non-opioid pain therapies for human and canine osteoarthritis that target the TRPV1 (transient receptor potential vanilloid 1) receptor, selectively inactivating local pain fibers that transmit pain signals to the brain.
Supporting the use of companion dogs as models for osteoarthritis treatment studies are the striking parallels between the condition in humans and dogs, said Brown (see Table 3-1). Both experience pain, stiffness, and decreased function due to similar pathogenic mechanisms. Diagnostic and therapeutic approaches are likewise similar. In clinical trials,
TABLE 3-1 Similarities Between Humans and Dogs with Osteoarthritis
| OSTEOARTHRITIS (OA) | ||||
|---|---|---|---|---|
| Humans | Dogs | |||
| Pathology | Cartilage: | Proteoglycan loss, chondrocyte death, erosion | ✔ | ✔ |
| Subchondral Bone: | Increased turnover, thickening, neovascularizatlon | ✔ | ✔ | |
| Joint Margin: | Osteophytes | ✔ | ✔ | |
| Synovlum & Fat Pad: | Inflammation, fibrosis | ✔ | ✔ | |
| Joint Capsule: | Fibrosis, | ✔ | ✔ | |
| Muscle: | Atrophy, fat Infiltration | ✔ | ✔ | |
| Sources of Joint Pain | Direct (contains noclceptors): Subchondral bone remodeling, synovitis,± joint capsule, ± osteophytes | ✔ | ✔ | |
| Indirect (source of inflammatory catabolites, cytokines, chemokines, neuropeptides): cartilage, ligaments | ✔ | ✔ | ||
| Risk Factors | Obesity, age* , trauma* | ✔ | ✔ | |
| Diagnostic Modalities | Radiography, computerized tomography, magnetic resonance imaging, arthroscopy, synovial fluid analysis | ✔ | ✔ | |
| Therapeutic Goals | Control pain and Improve function | ✔ | ✔ | |
| Slow progression | ✔ | ✔ | ||
| Outcome Assessment in Clinical Trial | Pain, mobility, stiffness, and function Indices | ✔ | ✔ | |
| Computerized gait analysis | ✔ | ✔ | ||
| Radiography & advanced Imaging for disease modification | ✔ | ✔ | ||
SOURCE: Presented by Dorothy Brown, October 12, 2017.
similar outcome assessments are used, including gait analysis, functional measures, and pain assessment inventories completed by owners to capture pain and loss of function. Accelerometers have also emerged as potential tools to assess function in a dog’s normal environment. Ablation of TRPV1-positive neurons has also been tested in companion animals with osteosarcoma, Brown said (Brown, 2016). In this use, the drug is delivered centrally as a means of causing cytotoxicity and cell death in TRPV1positive nociceptive neurons. Before advancing to companion animals, the drug was tested in rats, where unilateral injection into the trigeminal ganglia was shown to block sensitivity to corneal application of capsaicin, she said. In dogs with osteosarcoma, efficacy was tested using gait analysis, owner assessment, and activity monitoring. The treatment had no effect on tumor progression, but at least some of the dogs showed evidence of an analgesia effect and functional improvement, said Brown.
The use of companion dogs for clinical trials is “a huge win all the way around,” said Brown, yielding important information about the biology of the disease as well as the efficacy and safety of novel compounds, while at the same time improving treatment for pets. However, there are drawbacks. For example, Yaksh noted that companion animals are associated with inherent greater variability because the investigator must rely on the natural development of the pain state.
To summarize, Yaksh noted that replicating preclinical findings by encouraging detailed reporting of methods and results, incorporating randomization and blinding into preclinical studies, emphasizing effect size and clinical relevance, and routinely including an active control in preclinical modeling could reduce some of the reproducibility issues of preclinical findings and improve the translatability of those findings to the clinical space.












