2
Global Health Transitions
The workshop opened with a keynote presentation by Tim Evans from the World Bank Group. Evans described major transitions in global health, focusing on the interactions with demographic and economic transitions and their potential implications for policy and service design. After his presentation, Evans moderated a panel discussion on multilateral programmatic transitions occurring in global health. Adding to the health, demographic, economic, and multilateral programmatic transitions described by Evans and the first panel, a second panel followed with representatives from bilateral funding agencies sharing their agencies’ approaches to transitions. A final session on transitions focused on effects at the country level. This chapter summarizes Evans’s presentation, the three panels following, and the related discussions with the workshop participants.
DEMOGRAPHIC AND HEALTH TRANSITIONS
To start his presentation Evans described the relationship between development, demography, and transitions in health. The premise of this relationship is that as societies develop, they transition from high fertility to low fertility and from high mortality to low mortality. Demographic transitions significantly affect health systems and are unfolding rapidly in some countries. For example, China will have more than 100 million people over the age of 80 by 2050 (World Bank, 2018b). These population transitions, he said, can be cataclysmic in their effect on a country’s ability to provide
social protection and health services. However, the anticipated effects of demographic change are often overlooked since population statistics are generally based on 10-year censuses. Linking these demographic transitions to health, Evans quoted a “theory of the epidemiology of population change” created by Abdel R. Omran at the turn of this century (Omran, 1971). Omran’s theory focuses on the interface between demography and epidemiology (see Figure 2-1). This perspective is fundamental, Evans asserted, to designing health systems aligned with a population’s needs.
Turning to a different type of transition, Evans noted a major programmatic transition occurring in global health—the end of the GPEI. As the world inches closer to universal certificated polio eradication, the GPEI is winding down, and as it comes to a close, Evans emphasized the importance of retaining the skills, knowledge, and human resources developed and supported through the initiative’s 30-year history (the GPEI transition is described in detail later in this chapter).
While GPEI programming and support depend on disease burden and eventual eradication, the programming and support from other large global health funding initiatives are based on a country’s level of development (see Box 2-1). The growing economies of formerly poor countries
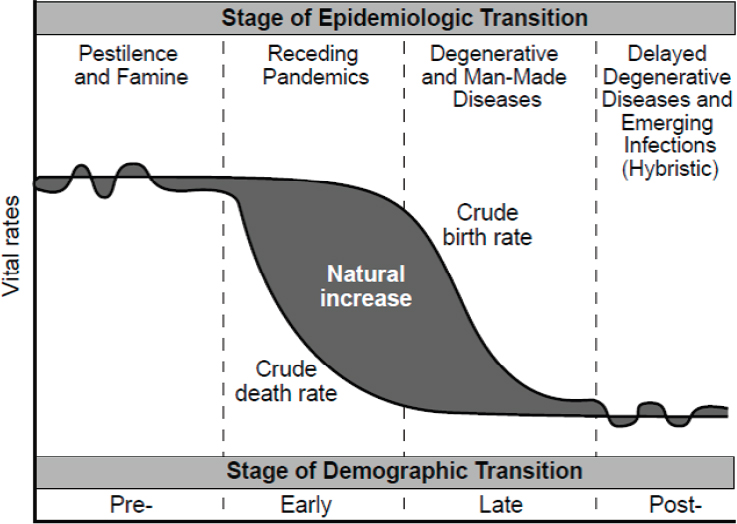
SOURCES: As presented by Tim Evans on June 13, 2018. From Rockett, 1999. Used with permission.
raise questions about the eligibility of these countries to continue receiving concessional financing by the World Bank and other development assistance agencies. The World Bank, Evans explained, has developed the Country Policy Institutional Assessment (CPIA) that is used to determine a country’s eligibility for concessional financing (see Figure 2-2). The CPIA draws on a number of variables rather than a single wealth threshold, such as income per capita. Other health financing institutions, such as Gavi and the Global Fund to Fight AIDS, Tuberculosis and Malaria (Global Fund), have different eligibility criteria that determine transitions in the levels and types of support (see Box 2-1).
Before closing, Evans acknowledged a priority on the global health agenda that is gaining momentum while these transitions are occurring: the global goal of universal health coverage (UHC) at the national level. This goal, he said, embodies the aspirations of people everywhere in the 21st century and is driving policy makers to provide comprehensive health care. Two globally accepted targets for UHC are set for 2030: (1) at least 80 percent of the poorest 40 percent of the population must have access to essential health services; and (2) financial risk protection for all. However, Evans admitted that meeting these targets will be challenging. Most LMICs’ health systems are financed mainly on an out-of-pocket basis, creating an obstacle to UHC. Globally, he said, about half a trillion dollars are spent out of pocket on health annually. Devising innovative ways of prepaying and pooling these expenditures will be critical to achieving greater efficiency and equity in health expenditure and accelerating progress toward UHC. Beyond financing, Evans also noted the challenge of improving health delivery systems and services to ensure an appropriate level of quality. Before closing, Evans mentioned two recently created initiatives to help solve health financing challenges for investments in maternal, newborn, and child health (the Global Financing Facility) and for health funding during emergencies (the Pandemic Emergency Financing Facility).
In ending his presentation, Evans quoted a childhood ice hockey hero, Wayne Gretzky (a fellow Canadian), who had some advice pertinent to transitions: “Skate to where the puck is going, not where it is.” Anticipating where the next challenge is will increase the likelihood of successful transitions.
MULTILATERAL PROGRAM ELIGIBILITY AND TRANSITION POLICIES IN PRACTICE
Following his presentation on the demographic and economic transitions in global health, Evans moderated a panel and discussion on the transition policies and approaches of three major multilateral organiza-
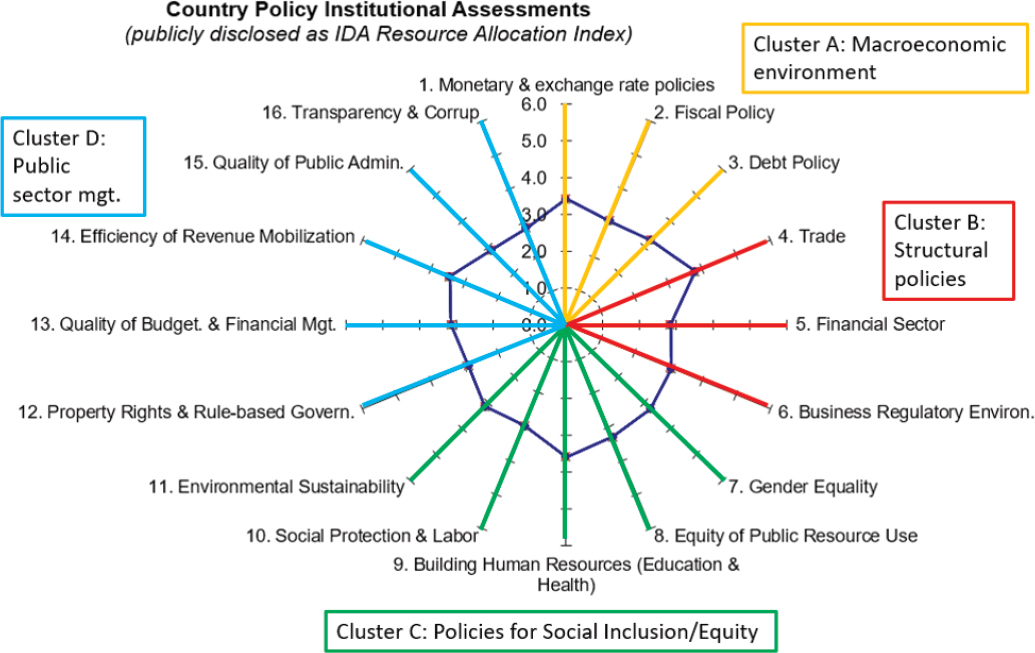
NOTE: IDA = International Development Association.
SOURCES: As presented by Tim Evans on June 13, 2018. Created by P. Geli, World Bank Group, 2018.
tions: Gavi, GPEI, and the Global Fund. The panel included presentations with representatives from each organization covering their approaches to country eligibility and transition processes, and current and anticipated effects on countries at different stages of transition. Panelists also shared how the programs are approaching engagement with the private sector in the transition process.
Gavi, the Vaccine Alliance
Santiago Cornejo of Gavi spoke about the organization’s policies and experiences with transitioning countries out of Gavi financing. To frame his remarks, Cornejo described some common programmatic and financing challenges Gavi countries face in supporting their immunization efforts. He emphasized the importance of both financing and programmatic sustainability to support a country’s immunization program to allow for effective planning, budgeting, and prioritizing. Low-income countries often have weak foundations for their health and immunization systems, which are coupled with acute fiscal constraints. As countries progress to higher levels of development, their systems are relatively stronger but with institutional capacity gaps in key areas. They also frequently have growing domestic resources but inadequate processes for allocative efficiency and prioritization. As countries continue to develop, there is often correlative progress on immunization programs and financing. However, these gains are vulnerable to risks, and there are sometimes missed opportunities for broader impact and efficiencies. As these stages of development come to light, Cornejo emphasized how countries’ needs evolve with their development transitions, triggering a need for evolution in the types of engagement and support offered by Gavi (see Figure 2-3).
Gavi’s policy for eligibility, cofinancing, and sustainability reflects these evolving needs and guides the alliance’s institutional framework for country transitions (see Figure 2-4). The policy, Cornejo noted, serves as a key mechanism for domestic resource mobilization and financial sustainability (Gavi, 2018b). Gavi’s sustainability approach for country transitions recognizes the following:
- Domestic financing is key but is not enough.
- Programmatic sustainability requires critical national capacities.
- Getting the sequencing of interventions right and addressing systemic bottlenecks early on is key.
- Support should be adapted to needs and reflect a country’s transition status.
- Existing systems should be leveraged where possible.
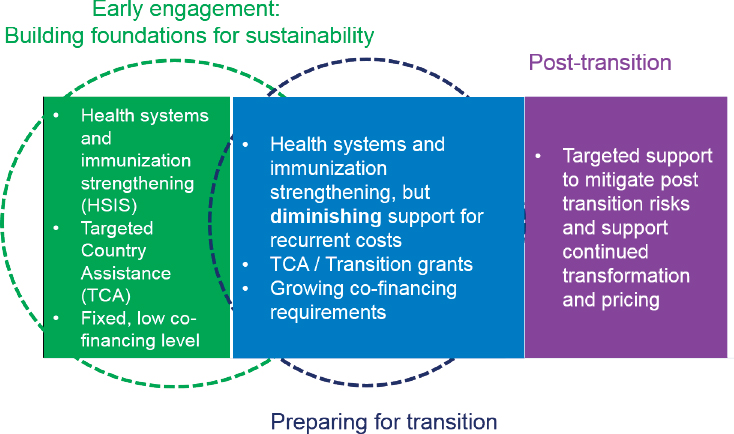
SOURCE: As presented by Santiago Cornejo on June 13, 2018.
To date, 16 countries have transitioned out of Gavi support, and 9 additional countries are in transition. Cornejo admitted the results from Gavi’s transitions have been uneven. Some posttransition countries have maintained high vaccine coverage rates, but others have much lower rates. The poor performers are mostly postconflict countries, but even some high-coverage countries are deficient in regulatory matters, procurement, the supply chain, and data systems. In addition to challenges with adjusting to loss of financing, some posttransition countries have struggled with the loss of Gavi’s technical support as well as the political status that an alliance such as Gavi confers. Cornejo shared several findings and lessons from Gavi’s experiences to date with country transitions (see Box 2-2).
Cornejo provided an example of how Gavi is adapting its policies for transitions based on the lessons it is learning. The Gavi board recently decided to continue Gavi’s engagement in posttransition countries. Through their continued engagement, these transitioned countries can benefit from Gavi’s supportive environment to mitigate critical risks and gaps.
Cornejo stated that private-sector engagement is core to Gavi’s operating model. On one level, Gavi partners with the private sector for financing. On another level, it partners with the private sector to leverage specific technical experience. This second level is particularly relevant in
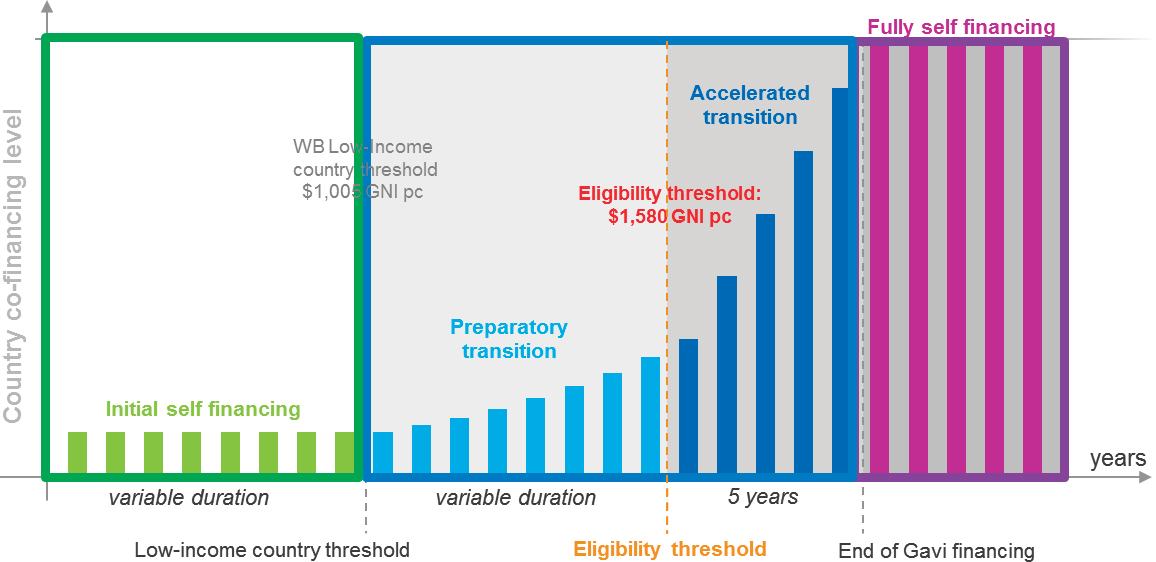
NOTE: GNI = gross national income; pc = per capita.
SOURCES: As presented by Santiago Cornejo on June 13, 2018. Figure available at https://www.gavi.org/about/programmepolicies/eligibility-and-transition (accessed October 23, 2018).
the context of addressing the institutional capacity issues common for transitioning countries. An example is Gavi’s partnership with United Parcel Service (UPS) and Freight in Time (FIT) for supply chain management. Cornejo also emphasized the importance of partnering with the local private sector as part of a sustainability strategy in transitioning countries.
Cornejo closed his remarks by noting that there is no silver bullet for successful country transitions. Rather, he suggested the focus during transitions should be on getting the basics right: there is no substitute for appropriate regular planning, budgeting, disbursement, and execution. He also underlined the importance of including a wide range of stakeholders in the process.
The Global Polio Eradication Initiative
Rebecca Martin of the U.S. Centers for Disease Control and Prevention (CDC) began her presentation on GPEI by acknowledging that the program’s biggest legacy will be a polio-free world. Thanks to GPEI, only three polio endemic countries remain: Afghanistan, Nigeria, and Pakistan. As this large-scale public–private partnership (PPP) inches closer to its end goal, it is focusing on its ramp-down strategy and, importantly, how to best use the assets it supported over the past three decades.
Before discussing the upcoming transition, Martin described the current status of GPEI. With so few endemic countries, GPEI’s donors, Martin said, have asked why the initiative still requires a $1 billion annual budget. The answer is that no one in the world is safe from polio until the disease is completely eradicated. Until then, the infrastructure built up by GPEI, including surveillance systems, laboratories, and human resources, is needed to detect the polio virus wherever it might emerge as well as support the capacity for outbreak response. Currently, more than 60 countries receive funding from GPEI, with more than 95 percent allocated to 16 resource-poor countries. Potential for risks and fragility at the country level determine resource allocation decisions.
The achievement of full universal polio eradication will trigger the end of GPEI, and transition planning is now under way to plan for its eventual ramp down. GPEI maintains a transition management group, and a Transition Independent Monitoring Board (TIMB) is advising the process. Transition strategy and planning focus on three core objectives: sustaining polio eradication, managing GPEI’s legacy assets, and supporting countries in their transition out of GPEI support and funding.
After the world is certified to be polio free, sustaining eradication will require a postcertification system, Martin explained. The priorities for this system will include the following:
- Keeping the virus under containment conditions that meet sound biosafety and biosecurity requirements, preventing escape from a laboratory or virus manufacturing facility
- Withdrawing the oral live attenuated polio vaccine (OPV) from use and protecting populations through immunization with inactivated polio vaccine (IPV) over the 10 years after the certification of eradication of the poliovirus
- Continuing surveillance to detect reemergence of the poliovirus and, should an outbreak occur, mounting a rapid response to prevent transmission of the virus
A second core objective of the GPEI transition is transferring its assets and lessons learned to other health programs. Martin emphasized the extensive assets developed through GPEI and noted how they can be used by programs battling other diseases. Examples that she quoted include an extensive infrastructure of global disease surveillance systems, vaccine supply and logistics networks, a worldwide network of more than 140 polio laboratories, thousands of skilled staff members, and millions of community-based health workers who can reach the most remote populations. GPEI, she pointed out, already is supporting a wide range of disease programs, such as routine measles immunization cam-
paigns, maternal and child health programs, and sanitation and hygiene programs (GPEI, 2018).
A third objective focuses on supporting countries in the current ramping down of GPEI support and funding. This includes mainstreaming polio essential functions into existing health programs, creating national action plans to map existing assets, and absorbing necessary health system functions into national budgets. As part of the process, national plans are being developed to map existing GPEI assets. No risk assessment on the effects of GPEI transitioning out of countries has been performed.
Martin gave several examples of how the polio program supports health activities for other diseases at the country level. In India, polio immunization staff joined a nationwide campaign to vaccinate all unvaccinated and partially vaccinated children in India against seven vaccine-preventable diseases. In Nigeria, a polio emergency operation center was set up to use its surveillance and contact tracing capabilities during the 2014 Ebola outbreak in West Africa. In Nepal, the polio surveillance system for immunization campaigns not only against polio but also against tuberculosis (TB), diphtheria, tetanus, pertussis, and measles. While these promising examples demonstrate how GPEI assets are supporting other health priorities, Martin pointed with caution to South Sudan; the country’s immunization program is entirely funded by GPEI. Without careful planning, the effects of GPEI’s withdrawal on the country’s immunization program and broader health system could be immense.
Martin closed by sharing that GPEI is discussing how to use its assets for other global health initiatives, including for Gavi and the Joint External Evaluation process for the Global Health Security Agenda.
The Global Fund to Fight AIDS, Tuberculosis and Malaria
Matthew MacGregor of the Global Fund described the organization’s approach to transitions from external financing and supporting countries in the process. He started his remarks by acknowledging the overlap in several of the Global Fund’s observations and priorities when approaching transitions with the programs presented earlier in the panel. It is hoped, he said, that this overlap reveals useful shared lessons that can inform transition approaches for the global health community.
MacGregor described the Global Fund’s Sustainability, Transition, and Co-financing (STC) policy, the guiding policy for the organization’s approach to transitions from external financing and supporting countries in the process (Global Fund, 2016). The STC policy focuses on three related and inter-connected pieces: the process of transitions, the over-
arching goal of sustainability and sustained impact, and the use of cofinancing as one of the tools to help achieve both. Introduced in 2016, the policy is a response to several factors:
- The changing nature of global health financing
- The need to increasingly focus Global Fund resources and investments on those countries with greatest disease burdens and least ability to pay
- Lessons learned from previous Global Fund transitions (particularly challenges related to interventions and services for key and vulnerable populations)
- Recognition that successful transitions are hard and require resources
- A commitment of the Global Fund to partner with countries to more proactively support countries to prepare for transition in order to sustain gains and continue to scale even beyond Global Fund financing
A number of overarching pillars guide the implementation of the policy:
- A need to embed sustainability across the portfolio, regardless of where a country is on the development continuum, ensuring early attention to potential long-term transition and sustainability challenges
- Enhanced focus on domestic financing (overall increases in funding) and co-financing of Global Fund financed interventions
- Accelerating efforts to prepare for transition as a country moves to higher income status and/or lower disease burden, especially for all upper-middle-income countries and lower-middle-income countries with disease components that have lower disease burdens
- Recognition that efforts to address sustainability and transition need to be flexible, given the varied financial and epidemiological contexts of countries across the development continuum
- Systematic efforts to work with partners (including technical agencies, bilateral partners, development banks, and civil society partners) to leverage capacity, collaborate on joint priorities, and accelerate STC efforts
The STC policy formalized the concept of transition funding for disease components with existing Global Fund grants that have become newly ineligible in order to address bottlenecks in the transition process
and to allow for a more gradual transition. The policy also changed the Global Fund’s approach to co-financing by requiring countries to demonstrate progressive government spending on health and co-financing of Global Fund–supported programs and by differentiating co-financing requirements for countries at different stages of development. Lower-income countries have the flexibility to focus additional co-financing commitments on health systems. As countries progress in their development, the size of co-financing commitments increases, and more requirements are placed on where co-financing commitments need to be targeted, including a progressive focus on disease programs, systemic transition and sustainability bottlenecks (often related to health systems), and programs targeting key and vulnerable populations. The inclusion of transition funding, the requirements on how Global Fund funds can be used by higher-income countries, and the thematic areas where co-financing commitments must be made reflect the Global Fund’s lessons learned from previous transitions. Figure 2-5 illustrates the application of the STC policy across the spectrum of countries at different stages of development.
MacGregor reflected on the progress toward self-sufficiency of countries approaching transition. Both before and since the development of the STC policy, significant progress has been made to strengthen the sustainability of national programs and to support transitions. Countries approaching transition are assuming a significant amount of the overall disease response and many now fund and manage most national programs. In addition, the focus on sustainability and preparing for transition in the day-to-day “business” of the Global Fund has also increased. However, as detailed in Box 2-3, he acknowledged there are ongoing challenges.
MacGregor touched on the essential role of partners in supporting countries preparing to transition. Many transition challenges go beyond specific Global Fund investments or competencies and require greater engagement with a variety of in-country stakeholders, for example, Ministries of Finance and Planning and the private sector. The Global Fund works with partners to coordinate technical assistance by seeking ways of increasing countries’ domestic financing, assisting in overcoming bottlenecks in the transition process, and improving the efficiency of investments. MacGregor also noted a challenge unique to the Global Fund: it is often active in places where other multilateral and bilateral donors have already transitioned. This circumstance limits the number of traditional partners on the ground and strengthens the case for identifying new, less traditional partners. As a final comment, MacGregor affirmed that successful transitions will be essential for ending epidemics. “They embody what we want and what we aspire to in country ownership.”

NOTES: Specific focus areas for any individual country or disease components will depend on and vary based on country context. COE = challenging operating environment; LIC = low-income country; LMIC = low- and middle-income country; RAI = Regional Artemisinin-resistance Initiative; STC = Sustainability, Transition, and Co-financing policy; UMIC = upper-middle-income country.
SOURCES: As presented by Matthew MacGregor on June 13, 2018. Figure created by the Global Fund.
Discussion
Simon Bland of UNAIDS opened the discussion by asking Evans about his views on human capital spending and the use of the World Bank’s leverage to boost countries’ domestic investments in sectors such as health. Evans assured him that he considers human capital an important prerequisite to achieving successful transitions. Investments in education and health are clearly linked to economic growth, he said (Suri et al., 2011). The World Bank has developed a human capital index to rank countries by how well they perform and the degree to which they invest in health and education. In Evans’s experience, this ranking helps stratify countries in terms of their likely domestic resource mobilization. Many people, he said, view health and education as luxury items, and even the World Bank, in its early days, considered education and health “social overhead.” Even today, many finance ministers do not altogether appreciate the real value of health and education, he observed. Evans shared that the World Bank categorizes capital in three areas: physical, natural/environment, and human. The expectation is for the World Bank’s financing to move toward an equal one-third distribution across these areas of capital.
Ikuo Takizawa of the Japan International Cooperation Agency (JICA) expressed concern that the polio surveillance systems would be challenging for other disease programs to use given the robust level of funding polio has received versus others. In reply, Martin pointed out that other
programs have adapted and are using the polio surveillance systems not only for detection of acute flaccid paralysis but also for environmental surveillance. The funding needed for continuous use of these systems is certainly a critical issue, she conceded. Carel IJsselmuiden of the Council on Health Research for Development (COHRED) asked Martin what proportion of funds will be taken from the budgets of the 16 poorest countries currently funded by the GPEI. Martin pointed out that all 16 countries are supported by technical advisory groups, interagency coordination committees, and Gavi, which is a member of the GPEI’s Transition Management Group.
Concurring with Matthew MacGregor’s remark in his presentation that governments are not readily persuaded to support key and vulnerable populations or civil society organizations, Takizawa wanted to know how successful the Global Fund has been in dealing with governments on this issue. MacGregor replied that one cannot take for granted that a government will fund services for key and vulnerable populations, but there are examples that contradict that statement. An incentive for the government, he suggested, might be the way in which the Global Fund manages its cofinancing policies. The Global Fund increasingly passes its funding through government systems. As a result, the funds are on the government’s budget, so that when the funding of the Global Fund diminishes, the government provides the funds needed to pay for services to the key and vulnerable populations. As for the civil society organizations, MacGregor emphasized the important advocacy role they play. They are also essential, he added, in protecting the human rights of vulnerable populations, but governments are reluctant to fund these functions. Other potential partners, he said, are required to step in and provide the needed support.
Nduku Kilonzo from Kenya’s National AIDS Coordinating Council prompted MacGregor to define the term country ownership. MacGregor declined, acknowledging it is a challenging term with natural tensions between internal and external financing considerations. When it comes to transitions, decisions about when programs transition are made by the external funding organizations, which creates this tension. MacGregor suggested that what is important from the Global Fund’s perspective in this regard is being clear and upfront about what its policy is. A second question from Kilonzo addressed country financing flows, which involve a series of well-oiled mechanisms, such as planning, approving, negotiating, and managing financial envelopes. Kilonzo asked where transitions fit into this in-country financing routine. MacGregor replied that managing a transition was a donor- and organization-driven procedure.
Evans closed the session with a few reflections on the past 20 years of health development financing and implications for transitions now and in
the future. Twenty years ago, no one would have predicted health development financing would grow to an annual sum of half a dozen billion dollars. When the billion-dollar era in global health financing occurred, Evans suggested there was an inebriated sense that with billions, everything could be accomplished. From his observations, only within the last 5 years has the realization of the global trillion-dollar health sector come. The question now is how development finance can become catalytic in contributing to the trillion-dollar challenge. Evans pointed to the 2015 Addis Ababa Financing for Development conference as the moment when the global health community came together to respond to this question.1 He acknowledged the challenge with mobilizing domestic resources for health while providing development assistance. Proposals to shift development assistance away from grant financing and toward global public goods are being made; however, Evans emphasized that this shift will only be successful if coupled with effective domestic resource use and mobilization.
Evans suggested that the growing body of work on projections of financing for health can help to stratify countries based on likely trajectories for domestic resource mobilization.2 These projections illuminate a small but significant minority of countries with a 40- to 50-year trajectory for developing a strong engine of national financing. Accordingly, the development community needs to orient expectations for different types of development assistance based on the likely trajectories of country needs, Evans said. Stratification of countries based on development trajectories can help structure the policy discourse toward a future with realistic horizons for different countries, increasing the likelihood of successful transitions.
BILATERAL APPROACHES AND POLICIES FOR TRANSITIONS PRESENTED AT THE WORKSHOP
The panel discussion on multilateral approaches to transitions was followed by panel presentations from bilateral funders on their approaches to supporting countries in transition. First, Ambassador
___________________
1 See Addis Ababa Action Agenda, 2015. Available at http://www.un.org/esa/ffd/wpcontent/uploads/2015/08/AAAA_Outcome.pdf (accessed October 23, 2018).
2 See the World Health Report: Health Systems Financing, 2010. Available at http://apps.who.int/iris/bitstream/handle/10665/44371/9789241564021_eng.pdf;jsessionid=D67F8C6B1CD77D63E0F295662C3D8B0E?sequence=1 (accessed October 23, 2018). Also, see Trends in future health financing and coverage: Future health spending and universal health coverage in 188 countries, 2016–40, 2018. Available at http://www.healthdata.org/researcharticle/trends-future-health-financing-and-coverage-future-health-spending-and-universal (accessed October 23, 2018).
Deborah Birx described The U.S. President’s Emergency Plan for AIDS Relief’s (PEPFAR’s) experiences with country transitions. Kerry Pelzman of the U.S. Agency for International Development (USAID) and Ikuo Takizawa of JICA followed, and each described how their governments are supporting countries experiencing transitions through their development agencies (see Box 2-4). Ambassador John Lange from the UN Foundation moderated the panel.
The President’s Emergency Plan for AIDS Relief
Birx began her remarks by commenting on country ownership and leadership. To achieve progress, Birx emphasized that countries must own their epidemics and have the political will to address their unique HIV epidemic. She added that community engagement plays a critical role in fostering country ownership (see Box 2-5 on the Research Fairness Initiative for an example of supporting country ownership presented at the workshop).
Turning to PEPFAR’s approach to transitions, she explained that PEPFAR’s country eligibility criteria are based on the burden of HIV rather than a specific country’s income level. The program does not begin to approach transition until the disease has reached a steady state of epidemic control—where the epidemic is no longer expanding. PEPFAR defines epidemic control as the point in which the annual number of new infections falls below the total number of deaths of HIV-positive patients. She added that controlling the HIV pandemic, and any pandemic, is key to a country’s long-term fiscal capacity.
PEPFAR’s approach to program and partner management is guided by three pillars: accountability, transparency, and impact (see Figure 2-6). These three pillars prompted PEPFAR to start working intentionally with the Global Fund to align budgets, data, and resources. PEPFAR spearheaded an effort to align PEPFAR, Global Fund, and host country HIV/AIDS budgets. They completed a resource mapping exercise to provide data that are more comprehensive and that clearly define the program elements for which each entity is responsible. These data, Birx said, will strengthen joint planning, avoid duplication, and inform future programming decisions. Over the past 4 years, both PEPFAR and the Global Fund were able to double their results in a flat budget, Birx stated, demonstrating what is possible when there is political will at the government level and intentionality at the multilateral and bilateral levels.
Progress in controlling the epidemic has also been remarkably successful in several African countries, notably in Malawi, Swaziland, and Zimbabwe, Birx explained. The success, she said, stems largely from governments that have adopted the policy quickly and that worked together with their communities. Interestingly, some countries that were least suc-
SOURCES: As presented by Ambassador Deborah Birx on June 13, 2018. Available at https://www.pepfar.gov/documents/organization/267809.pdf (accessed October 23, 2018).
cessful in controlling the epidemic were those that received the most funds from the Global Fund and PEPFAR, demonstrating that success is not solely a resource issue but is dependent on how those resources are used and on policies that ensure those resources have maximum impact. Other successes include a positive outcome to control a major AIDS epidemic under way in northern Namibia. The rural nature and the different languages of those affected by the epidemic complicated control efforts, but challenges were overcome with a combination of government innovation and listening and responding to the community. Despite these difficulties, almost 70 percent of community members were taking their medication, and the communities were able to attain a 68 percent viral load suppression rate, which kept them healthy and prevented them from transmitting the virus.
Returning to PEPFAR’s approach to country funding based on burden of disease rather than income level, Birx contrasted the progress between a low-income and a middle-income country—Malawi and South Africa. In Malawi, both the number of new infections by an absolute number and the number of deaths by an absolute number have continued to dramatically decline despite a youth bulge and increasing population (see Figure 2-7). In South Africa, progress has been much slower (see Figure 2-8). South Africa is now investing billions in their epidemic, but they are still struggling to
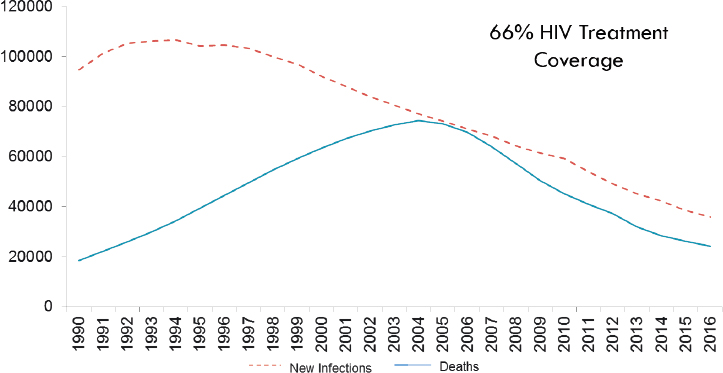
SOURCE: As presented by Ambassador Deborah Birx on June 13, 2018. Available at https://www.pepfar.gov/documents/organization/267809.pdf (accessed October 23, 2018).
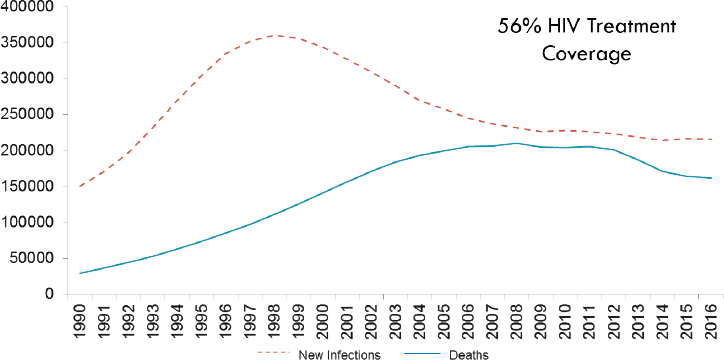
SOURCE: As presented by Ambassador Deborah Birx on June 13, 2018.
control the epidemic due to the depth and breadth of the pandemic that expanded during a time of less government engagement and recognition of the disease. Birx shared that 4 years ago, there was talk about transitioning South Africa, but the country still needs additional resources to address the core barriers to controlling their epidemic.
As PEPFAR continues to make programming decisions, Birx said, it relies heavily on site-level data to maximize the efficiencies of its resources. It is this level of data that enables PEPFAR to define exactly what is needed for specific populations. Barriers to epidemic control occur in pockets, and Birx feels it is PEPFAR’s job to work with communities and governments to respond in specific ways that target resources for maximum results.
U.S. Agency for International Development
In opening her remarks, Pelzman noted the convergence between the workshop’s focus and USAID’s current priorities under Administrator Mark Green: country transitions to self-reliance and private-sector engagement. Pelzman first addressed the priority of country transitions and then turned to private-sector engagement, describing private-sector engagement as a means to achieving USAID’s objectives.
While there is a renewed emphasis on country transitions at USAID, Pelzman emphasized that approaching transitions is not new for USAID’s Bureau for Global Health. Since 2000, the Bureau for Global Health has engaged in strategic and deliberate processes to assess transition readiness in many of the countries where it works, establishing a precedent within the agency for how such processes should occur. A key transition began in 2006 with the graduation of countries from family planning assistance, Pelzman said. USAID implemented a carefully planned, data-informed approach to transitioning a number of Latin American countries from USAID family planning assistance. Decisions for transition included the total fertility rate and prevalence rates for modern contraceptives. USAID conducted consultative assessments to determine remaining weaknesses and gaps in the family planning programs and set timelines for program graduation. Objective and quantitative data were used in a collaborative process with host country governments and other stakeholders. The overall programmatic goal of the process was to achieve access, quality, and sustainability. The family planning graduation process normally lasted on average 4 to 6 years, with some exceptions. Pelzman shared several key lessons learned from USAID’s family planning assistance transitions, noting the overlap with many of the lessons shared from the previous speakers’ presentations on their organizational approaches to transitions (see Box 2-6).
For USAID, the term transitions does not necessarily mean USAID is ending engagement or funding in a specific country. Transitions often refer to a process of evolving a relationship between USAID and a host country to a new model of partnerships, Pelzman said. In most countries where USAID graduated programs from family planning assistance,
valued partnerships between USAID technical staff and local partners had been established. As part of the transition process, mechanisms were developed to continue these relationships, often evolving into communities of practice or facilitating south-to-south learning. Transition also does not necessarily equate to USAID discontinuing its investment in the health priorities of a partner country. Continued investments may include facilitating partnerships to locate new funding from other stakeholders, such as the private sector, to meet priority goals for USAID and the partner country. One innovative example is USAID’s involvement in the Global Financing Facility in support of the Every Woman, Every Child Initiative.
Pelzman turned to USAID’s priority focus on private-sector engagement, particularly in the context of supporting country transitions and new forms of partnerships between USAID and partner countries. Successful private-sector engagement in global health can increase impact, use USAID resources strategically, and build sustainability in programs to support countries as they transition from donor assistance, Pelzman said. Increasing private-sector engagement is a means to an end often in support of the three types of outcomes Pelzman described. To facilitate successful partnerships with the private sector, USAID recently developed a global private-sector engagement strategy. With this strategy, Pelzman said USAID seeks to best leverage private-sector resources and incentivize engagement to support countries in their path to self-reliance (see Figure 2-9).
Pelzman closed her remarks by emphasizing that each country’s health journey is unique. Countries take different paths during the course
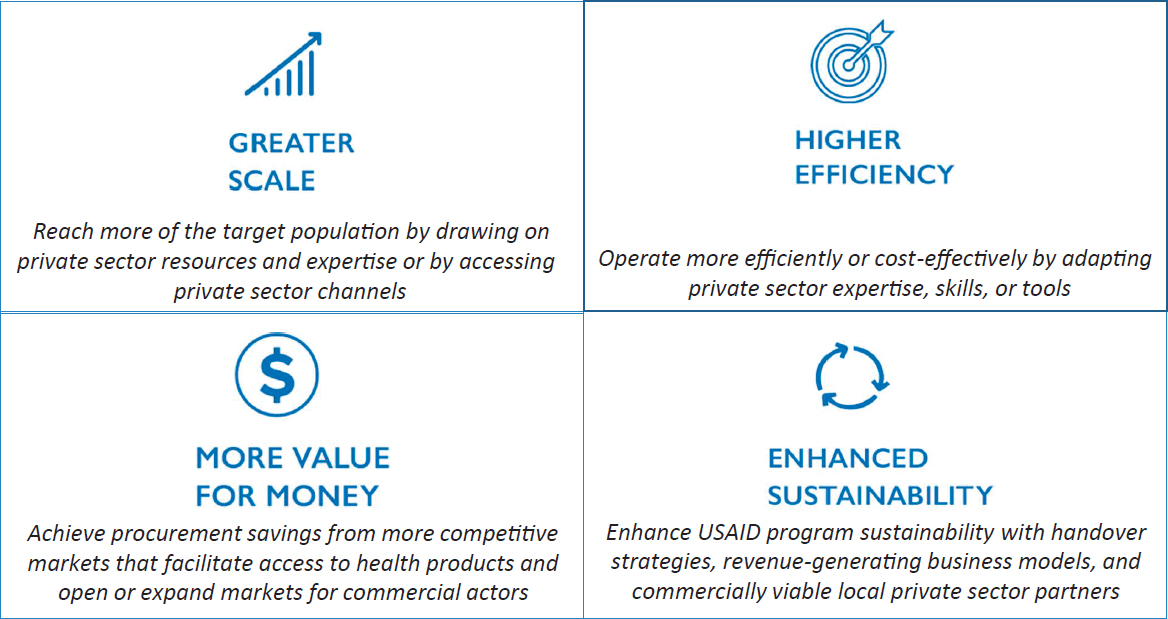
SOURCES: As presented by Kerry Pelzman on June 13, 2018. Figure created by USAID’s Center for Innovation and Impact.
of their journey; factors including political prioritization, stability, and unforeseen natural or human-made disasters can change or interrupt a country’s journey to self-reliance. USAID continues to monitor risks and threats to its investments in countries and progress on the self-reliance journey. As a closing example, Pelzman recounted when Zika emerged in Latin America and the Caribbean in 2016. Many of these countries had transitioned out of USAID’s family assistance programs. However, USAID had maintained relationships with them and those relationships provided a crucial entry in mobilizing an emergency response.
Japan International Cooperation Agency
Providing a perspective from another bilateral global health-funding agency, Takizawa described JICA’s policies and approaches to country transitions. As a baseline for determining a country’s eligibility for assistance, JICA follows the Development Assistance Committee (DAC) list of countries eligible for official development assistance. This list is based on income thresholds, and the approximately 140 countries currently on the list are eligible for JICA assistance. JICA’s country allocation is based on the request coming from the countries and the thematic priorities defined by the Japanese government. The government’s current priority for health centers on UHC and, in support of this central priority, includes strengthening, resiliency, and bolstering the health security of health systems. JICA also supports infectious disease control and maternal and newborn health. Recognizing the shifts in the burden of disease, particularly in the South Pacific Island and South Asian regions where JICA invests, JICA has begun to direct some of its resources to noncommunicable diseases. While the country requests and disease-specific and thematic priorities coupled with thresholds set for the DAC list dictate how and where JICA allocates its resources, Takizawa acknowledged that diplomatic considerations also influence the distribution of its investments. To illuminate this point, he noted that JICA provides some form of assistance in nearly all countries on the list; however, more than 60 percent of JICA’s assistance for health is concentrated in approximately 20 countries.
JICA recognizes that many countries where it invests are experiencing economic transitions. To support the countries during these transitions, JICA mobilizes different modalities, Takizawa said. One of the strengths of this approach is the ability to construct the mix of this modality of assistance to suit the country’s demands and needs as it transitions. These modalities range from concessional loans, grant aid, and technical assistance. In general, as countries grow in income level, they shift away from grant aid and toward concessional loans. Takizawa pointed out that JICA’s terms for its loans to health-sector investments in LMICs are com-
parable to the loans through the World Bank and are more concessional in some income groups. JICA applies preferential terms specifically for the health sector.
Takizawa highlighted an example of how JICA is innovating in the use of grant and loan assistance modalities. Polio eradication has been one of JICA’s major areas of assistance, and for many years it was funded primarily through grant assistance. In collaboration with the Bill & Melinda Gates Foundation, JICA has transitioned its grant assistance to loans in Pakistan and Nigeria. In this loan conversation, if the country meets agreed to performance indicators, the Gates Foundation repays the principle instead of the recipient government.
JICA is also changing its approach to technical assistance. The traditional model of technical assistance was a knowledge transfer from Japan to the host countries. However, as the host countries develop, JICA is shifting its model to more of a mutual dialogue. For example, JICA recently hosted a delegation from Kenya that included the ministry of health as well as representatives from the ministry of finance, the national parliament, and the counsel of governors for a dialogue on domestic resource mobilization to achieve UHC.
Like USAID, private-sector engagement is a priority for JICA. Takizawa described three ways JICA is approaching private-sector engagement:
- Innovation and technical partnership to mobilize the technical expertise and resources from the Japanese private sector
- Managerial capacity building where the private sector can offer expertise in efficiencies and management practices
- Financial aid; Takizawa shared that since 2008 JICA has issued a bond to mobilize money from the capital market in Japan
As an overarching comment, Takizawa suggested that as all funders approach transitions within the countries where they invest and coordinate with the country and with each other, there are opportunities to better mobilize resources collectively in support of countries.
Discussion
Starting the open discussion with workshop participants, Scott Ratzan of the Anheuser-Busch InBev Foundation asked the panelists about their experiences with developing and measuring the effects of PPPs to support the sustainability of their initiatives. PEPFAR, Birx replied, has worked with many PPPs in the past. From experience, the agency has realized the importance of a clear concept of the kind of partnership needed for a specific goal.
Kate Dodson of the UN Foundation asked Pelzman to elaborate on USAID’s global health strategy for private-sector engagement and share what lessons USAID has learned from past partnerships as well as share its plans for future partnerships. In response, Pelzman explained that USAID seeks out companies with corporate capacity and creative skills to bring into partnerships. An example is the Project Last Mile in South Africa, where USAID is partnering with Coca Cola for technical assistance in logistics management. Adding to Pelzman’s response, Amy Lin, also with USAID, suggested all USAID teams should be briefed on what the private sector is seeking when partnering with health-sector institutions. “They are not just looking to put money on the table. They do want to bring their expertise. And they do want to bring their company people into the global health picture,” she said. On the other hand, Lin noted, USAID itself might usefully give some thought to what its field staff’s expectations are, what their goals are, and how they could become more creative, more strategic, and more proactive in a partnership. Moreover, she suggested that in choosing a partner, USAID should consider not only the large international companies but also in-country, for-profit channels, such as pharmacies and clinics that could facilitate contact with new types of “customers.”
TRANSITIONS AT THE COUNTRY LEVEL
Jo Ivey Boufford of the New York University College of Global Public Health moderated the final panel of the day. Four speakers explored the degree to which developing countries are ready to undergo a transition that will bring to an end or reduce their dependence on donor assistance. The speakers also discussed the role that private-sector partners could play in facilitating the transition process. Muhammad Pate, former minister of health of Nigeria and now chief executive officer with Big Win Philanthropy, a UK-based foundation that invests in children and young people in developing countries to improve their lives, detailed the degree to which Nigeria is prepared to accept transitions. Naresh Goel, deputy director general at the National AIDS Council of the Ministry of Health and Family Welfare in India, outlined the health care problems posed by India’s complex geopolitical governance system and the solutions found to solve them. Siddharth Chatterjee, UN resident coordinator for Kenya and UN Development Programme (UNDP) resident representative for Kenya, showed how a PPP can produce highly desirable health results. John Fitzsimmons, chief of the Revolving Fund for Vaccines of the Pan American Health Organization (PAHO) gave an account of how the 41 countries of the Americas have defeated three infectious diseases.
Nigeria
To frame his remarks on transitions affecting Nigeria, Pate described three relevant characteristics of its political system and economy: a decentralized political system, a large percentage of out-of-pocket health expenditure, and projected upward economic growth. Nigeria operates a fiscally decentralized system of government with autonomous states and limited central accountability mechanisms. Disparities across the different states are significant, Pate shared. Variations in health outcomes, not surprisingly, are also significant. For example, there is greater than a fivefold difference in full immunization coverage between the six geopolitical zones in Nigeria (NBS, 2017). Examining Nigeria and the potential effects of transitions from a national-level context, he suggested, hides vast variations within the country that often exceed the intercountry variations across the African region and even globally.
Health expenditure in Nigeria is heavily weighted toward out-of-pocket expenses, Pate shared. More than two-thirds are private, out-of-pocket expenses, and less than one-third is public—including spending from federal, state, and local governments (WHO, 2018). Less than 10 percent of the total health expenditure in Nigeria comes from external funding sources. The Nigerian economy overall is growing, and Pate noted it is projected to become a significant and economically strong country over the next several years.
After describing these contextual factors, Pate turned to the external programmatic transitions affecting Nigeria. He categorized them as three types. The first type is the transition of external financing instruments, including Gavi and the Global Fund. The second is the World Bank, which takes a more long-term and broader engagement approach than the other external financing instruments and operates at both federal and state levels as well as across sectors. The third type is GPEI and its specific focus on eradicating a single disease. How resources flow from these three types differs. Gavi and the Global Fund sign agreements with governmental and nongovernmental entities. The World Bank signs agreements with both the federal government and states. GPEI provides a significant amount of technical assistance resources through entities such as the World Health Organization (WHO) and the United Nations Children’s Fund (UNICEF).
These programs are all at different stages of transition within Nigeria, and Pate shared a few observations about how they are approaching their transitions. First, he suggested there is an opportunity for greater coordination in-country among them. Secondly, he suggested the in-county stakeholders who are key to the transition process are broader than the ministry of health—the minister that is often the central focus for discus-
sions on transition. The presidency and the parliament play a role in shaping the government’s fiscal priorities over the long term. In terms of sustainability after these transitions occur, Pate suggested that gaps within the institutional systems, as well as policy and regulatory frameworks, need to be addressed. Additionally, there is the issue of human resources and domestic employment through these external programs.
Pate suggested that the support Nigeria needs to sustainably and more effectively manage its health system and services includes technical assistance in public-sector management and planning. In Nigeria, mechanisms to support the development of government efficiencies are lacking even though investments are being made to create efficiencies within externally funded programs. He pointed to the example of supply chain management. There have been initiatives to create efficiencies in the supply chain for externally financed commodities, but these initiatives do not extend into the rest of the health sector even though pharmaceuticals account for a large portion of total health spending in the country.
Before closing, Pate noted a couple of points raised in the earlier panels he believes are important considerations for transitions in Nigeria. First is community engagement. Pate emphasized how vital community engagement is as part of the evolution of donor support over time. Second is the development of new sets of instruments. Nigeria benefited immensely from the Japanese government’s loan buy-down for polio, Pate said. He sees significant potential for innovative financing instruments such as this one to support countries in their transitions. He added a final point of consideration. He has observed an unevenness across external funding programs in the level of negotiation in which they engage with the governments where they are operating. He cautioned about the asymmetries that can result when there are different understandings among partners about the risks associated with agreements.
India
Significant demographic and economic transitions in India are affecting the health sector and health outcomes in the country. Goel described these transitions, the current health challenges, and the government’s response.
The population of India is increasing, with some estimates predicting that by 2030, it will have the largest population in the world. The economy is also growing rapidly, currently at a rate of 7 percent. If this growth continues, the country’s economy will double within approximately 10 years. Along with this growth, India has recently undergone two major economic reforms, Goel shared. One is demonetization, and the second is the Goods and Services Tax implementation, leading to an
increased use of digital financial transactions and a greater percentage of commerce shifting into the formal economy. Before moving on to the health problems in India, Goel emphasized the vastness of the country. Rather than viewing India as a single country, Goel suggested it should be viewed as a continent of 29 large nations and 7 smaller ones. Within India, some “nations”—states and provinces—are experiencing more development than others.
Urban health, Goel noted, is one serious problem in India. Adequately feeding the population is another: around 40 percent of Indian children are malnourished (NFHS, 2016). Human resources to staff primary health care centers are sorely lacking, he said. Moreover, a large proportion of health care services is provided mainly by private-sector facilities that are paid on an out-of-pocket basis. In Goel’s opinion, India’s problems put the quest for universal health care on the level of a “big dream.” On a more positive note, Goel shared that the government has come up with a new health insurance scheme, the National Health Protection Scheme, funded by the government, that covers 500 million inhabitants living under the poverty threshold.
Switching to his specific tasks as deputy director general with the Indian ministry’s National AIDS Control Organization, Goel emphasized the need to work in a partnership between the public and private sectors to “mount multisectoral responses in order to reach the largest number of people with awareness messages, preventive activities, and care and treatment.” India’s AIDS council has signed a partnership agreement with 16 nonhealth ministries that provide services such as awareness activities, staffing integrated counseling and testing centers, and treating sexually transmitted diseases. Partnerships were also formed with some 200 private-sector firms covering a wide range of activities that bring people into contact with AIDS health facilities.
Kenya
Kenya is a lower-middle-income country that has been proactively tackling its most pressing health challenges through government-led PPPs. Chatterjee shared how these initiatives evolved and are being implemented. Overall, he views the results achieved in Kenya as a lesson that PPPs can be successful even in low-resource settings with significant health challenges.
In 2014, the government of Kenya launched a “free maternal health care policy.” The decision, he explained, was prompted by the reputation that Kenya had acquired as being among the 10 most dangerous countries for a woman giving birth. A study of the country’s maternal death statistics pointed to six counties in Northeastern Kenya that had maternal death rates of more than 3,500 deaths per 100,000 live births.
Chatterjee met with representatives from several private-sector partners: Philips, a Dutch technology firm; GlaxoSmithKline, a pharmaceutical company; Safaricom, a Kenya-based communications company; Huawei, a Chinese company; and the Kenya Healthcare Federation, a Kenyan charity company committed to finding a solution to the alarmingly high maternal death rates. Together they used the study data to identify the areas with the most need. These partners were supported by a strong commitment from the Kenyan government to address maternal health, and in developing their plan of action, the partners consulted with both county governors and national authorities.
Within 30 months, the maternal death rate in these 6 high-mortality counties had fallen to 550 deaths per 100,000 live births. Chatterjee attributed this success to several key aspects of the partnership: capacity development at the county level, engagement of efficient technical staff, and strict financial accountability. Chatterjee noted a convergence of the partnership with two other critical factors for success: political will at the highest level and the right policies being translatable into action as far as the most remote villages. Buoyed by the success of the six-county experience, the Kenyan government has gone a step further in launching a “big four agenda” that covers universal health care, food security, and affordable housing and manufacturing.
Americas Region
Providing a perspective on a regional collaboration to address a specific health issue, Fitzsimmons described some of the transitions the national immunization programs in the Americas experienced since the Expanded Program on Immunization launched 40 years ago.
In 1991, the last case of polio occurred in the region, and in 1994 the region was certified as polio free. Driving this accomplishment, he said, was the commitment of health ministers and a partnership that included USAID, Rotary International, and many others. Next came the elimination of rubella and congenital rubella syndrome declared in 2015, followed by the elimination of measles, declared in 2016. Several partners, Fitzsimmons explained, were instrumental in bringing about these achievements. They implemented many catch-up immunization campaigns and surveillance activities. Fitzsimmons also praised the vaccine suppliers with whom the PAHO teams had a unique relationship. The work of Gavi, he said, in introducing new vaccines from 2000 up to the present, was a vital element. A notable recent transitional event was the agreement signed by the Haitian government to finance its own vaccines.
Generally speaking, three factors were key to the successes of the countries’ immunization programs, Fitzsimmons said. One was the adher-
ence to an annual, multiyear plan and to a regional plan to facilitate technical cooperation between PAHO and its partners in supporting the immunization programs of the region. A second key was drawing up a budget line and legislation to support it. The third key was an effective management structure that underpinned a reliable system for managing countries’ vaccine needs and for negotiating with suppliers for the lowest prices for vaccines and syringes. PAHO’s Revolving Fund was also a key factor in facilitating vaccine payment issues. A recent development, Fitzsimmons noted, is the creation of a capital fund for the 41 countries of the region. It gives each country a credit line enabling it to purchase vaccines regardless of the country’s size. This capital fund holds $200 million currently.
Discussion
The open discussion with the workshop participants started with questions from Simon Bland of UNAIDS to Pate. Bland asked Pate if the Nigerian government is effectively allocating resources for private-sector engagement and what role the private sector could play in aiding decisions on resource allocation. Addressing the first question, Pate said that during his presentation, he spoke of efficiency with regard not only to the amounts being allocated but also to how third-party resources are allocated to support the efficiency of governments. With regard to the role of the private sector, Pate shared that with the support of the Bill & Melinda Gates Foundation, he has garnered a group of private-sector entities to create the Private Sector Health Alliance of Nigeria, a platform for leveraging the innovative health-related capabilities of the private sector. The crucial element, Pate emphasized, is an organized platform to facilitate the mobilization of private-sector resources, ideas, skills and approaches, and expertise for the benefit of the public sector. Picking up on the platform approach, Goel mentioned a Sustainable Development Goals (SDGs) platform that he and his colleagues established in 2017. The platform is co-chaired by the Indian Minister of Health and the UN resident coordinator, and it comprises partners from the private sector, the public sector, and civil society.
Nduku Kilonzo of the National AIDS Coordinating Council in Kenya asked Pate what he sees as the realities of transition and what role the private sector can play within them. In response, Pate noted that transition means many things to many people or sectors. The Global Fund and Gavi, for example, approach transition from the viewpoints of their organizational missions. Other multilateral organizations, such as the World Bank, see transition as a conversation with links to many areas of organizational interest. JICA takes into account the diplomatic consequences
of transition. To answer Kilonzo’s question about the role of the private sector, Pate pointed out that the private sector has the competence, skills, and mindset to do what many governments are unable to do efficiently. The private sector, he said, can help governments to plan, budget, and implement.


































