LIVED EXPERIENCE AND PROVIDER PERSPECTIVES
To ensure that patient and provider experiences were central to the workshop discussions, the workshop opened with perspectives from a person living with chronic pain and a family physician. According to Christin Veasley, director of the Chronic Pain Research Alliance, chronic pain is the leading cause of disability worldwide and a major contributor to the rising number of suicides (Petrosky et al., 2018). Yet both Veasley and Daniel Cherkin noted that a substantial gap exists between the scientific and clinical understanding of pain and the decisions people make about how to manage their pain. This gap, said Veasley, arises from multiple factors: an insufficient workforce to address chronic pain; the paucity of team-based medical homes; the classification of pain disorders by symptoms rather than mechanisms; the lack of objective measures of pain; insufficient high-quality evidence about the efficacy of both pharmacological (e.g., opioids) and nonpharmacological (e.g., massage) treatments for pain; and insufficient data on risks, benefits, and cost-effectiveness of the various treatment alternatives.
Patients living with chronic pain face several decisional dilemmas, said Veasley. These include (1) how to evaluate which nonpharmacological treatment options may work when, for some approaches, little evidence exists to inform this decision; (2) how to choose the optimal combination of safe and effective treatments; and (3) how to choose the optimal modality, type, or technique within each selected treatment (e.g., the type of massage that would be most likely to provide pain relief). Veasley suggested that by developing research questions based on the decisional dilemmas faced by patients, the field could generate an evidence base, improve reimbursement, improve outcomes, and reduce uncertainty.
One reason for the low level of evidence available for nonpharmacological approaches to pain management is the variability in frequency, duration, and type among studies, said Veasley. Another problem is that in order to systematically and quantitatively review data from studies, outcomes must be assessed in a comparable manner, which is complicated by the fact that chronic pain may vary substantially from day to day and week to week and by limitations of the scales used for assessing pain. The frequent presence of comorbidities adds further complications given that patients may be receiving many different therapies for pain and nonpain conditions. All of this variability makes it hard to know exactly what is or is not working.
Moreover, she said, the experience and management of pain varies according to the underlying conditions that are contributing to a person’s pain. For example, managing pain in a person with new-onset osteoarthritis is going to be very different from managing the pain of a person with diabetic neuropathy who also has obesity and a sleep disorder.
Mark Ryan, a family physician at Virginia Commonwealth University, added that providers face other challenges when trying to manage patients’ pain. The national conversation on pain management did not begin to shift until the early 2000s, shortly after Ryan began his residency. The Joint Commission established standards for assessing and treating pain in 2001 (Baker, 2017; Phillips, 2000), but Ryan said it was challenging to assess pain using the scale that asks a patient to rate their pain on a scale of 0 to 10, rather than using metrics that assess global function, quality of life, or other relevant aspects of the pain experience. Practitioners, like patients, face a significant gap in measuring and understanding pain, and in assessing the effectiveness and potential harms of treatments. Moreover, treatment in the early 2000s was almost completely focused on medication, he said. The idea of integrative and comprehensive care that includes behavioral health and physical therapy was not included as part of physician training.
When Ryan moved to a rural practice in 2003, other challenges became evident, including the lack of local resources for pain management and limited access to pain management specialists. Now in his current position in Richmond, Virginia, he faces different challenges—for example, 40 percent of new adult patients in his practice lack insurance, are covered by the system’s indigent care plan, and have limited access to nonpharmacological therapies. Although he can make referrals for physical therapy or other services, patients face practical barriers that limit access to those services, such as transportation challenges and concerns about taking time off work to go to appointments on a consistent basis. Outside of the health system, even insured patients face significant challenges. Examples include pain management programs that limit the type of insurance they accept, specialists who focus primarily on procedures such as nerve blocks or epidural injections, and the lack of an integrated pain service.
Concerns about opioid use have exacerbated the difficulties providers experience in caring for patients with pain, said Ryan. Taken together, these challenges have led to dissatisfied and unhappy patients with significant concerns, and dissatisfied, unhappy providers who lack the tools they need to manage their patients’ pain appropriately. There are also pressures
at the health system level to manage chronic pain in an expeditious manner while also caring for patients’ other primary care needs.
Ryan expressed his hope that the workshop would identify actionable and practical strategies to address pain management in primary care settings, outline evidence-based and effective approaches to chronic pain management that do not rely on opioids or other medications, and encourage research focused on improving chronic pain management in primary care settings. He also advocated for efforts to improve provider–patient communication regarding treatments and goals for managing chronic pain using collaborative and holistic approaches that encourage shared decision making.
Veasley added that a paradigm shift is needed wherein all relevant stakeholders come together at the genesis of a research project and work collaboratively throughout it to bridge the translational divide between basic science and patient care. In addition, research aims that matter to decision makers—including, patients, clinicians, and payers—are needed to ensure successful execution of rigorous science and to promote the adoption of findings into clinical care.
BACKGROUND ON PAIN AND NONPHARMACOLOGICAL PAIN MANAGEMENT
A recent analysis of the burden of disease in the United States found that 5 chronic pain conditions account for more disability than the 12 leading medical conditions (see Figure 2-1), said Kurt Kroenke, chancellor’s professor of medicine at Indiana University and a research scientist at the Regenstrief Institute (Murray et al., 2013). If depression and anxiety are added to the list of pain conditions, which are comorbid in 30 to 50 percent of people with chronic pain, the burden is even greater. Moreover, most people with chronic pain have pain in multiple body sites (Kroenke et al., 2013).
The burden of pain comes not only from the individual perception of pain itself, but from how it affects other aspects of life, including social roles, vocation, and health care seeking, said Steven George. Understanding this complexity is an essential first step in both treating and managing pain.
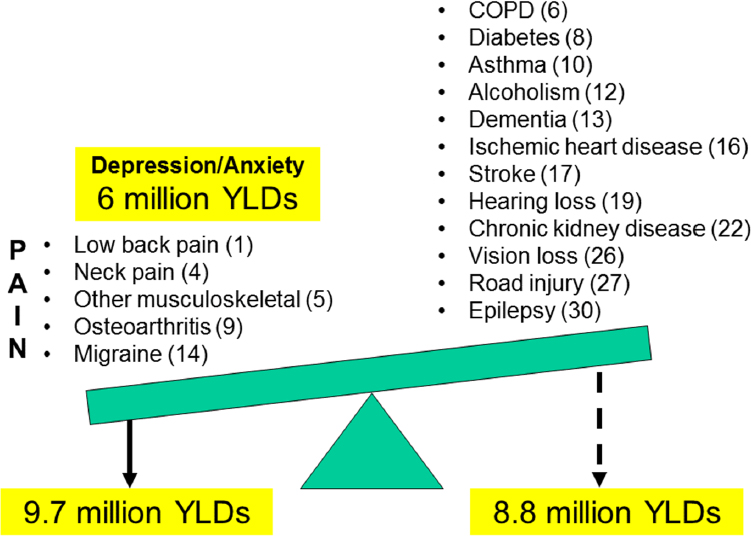
NOTES: In the United States, pain accounts for 9.7 million YLDs in comparison with 8.8 million YLDs for the 12 leading medical conditions. COPD = chronic obstructive pulmonary disease.
SOURCES: Presented by Kurt Kroenke, December 4, 2018; adapted from Murray et al., 2013.
Understanding Pain and Pain Management
George described pain using the analogy of an onion, with the layers being nociception, individual experience, and impact (see Figure 2-2). At the center of the onion is nociception, the nervous system’s response to painful stimuli. Nociception is embedded within other layers of the onion that comprise the individual’s experience of pain such as the beliefs, emotions, and coping strategies that introduce tremendous variability in how pain is experienced. All of these factors contribute to the impact pain has on other aspects of a person’s life. It was no surprise, George added, that when the Institute of Medicine published its report Relieving Pain in America they concluded that pain is a major driver of health care, disability, and reduced quality of life (IOM, 2011b).
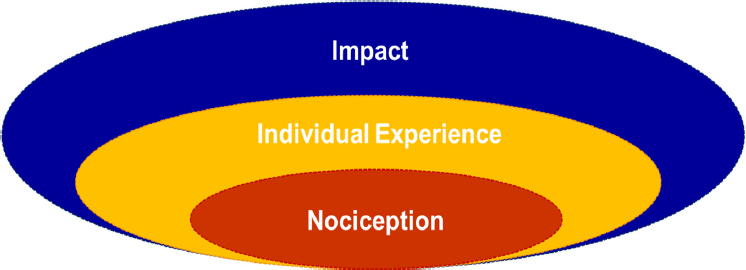
SOURCE: Presented by Steven George, December 4, 2018.
Treating pain is different from managing pain, said George. Individual pain treatments target nociception, while pain management addresses multiple layers. Typically, a patient’s first contact with a health care provider trained in conventional medicine leads to diagnosis and drug treatment, with management of pain through nonpharmacological and other approaches only introduced later. Recent changes in the guidelines for how pain is managed aim to shorten that interlude, moving nonpharmacological care closer to the first contact point through more cohesive and integrated management pathways, said George.
A large therapeutic armamentarium for pain exists, including medications, surgical procedures, physical modalities, and complementary and multidisciplinary approaches, said Dennis Turk, director of the Center for Pain Research on Impact, Measurement, & Effectiveness (C-PRIME) at the University of Washington. The problem, he said, is that for any of these approaches, evidence of effectiveness is modest (Moore, 2013). Kroenke added that the limited effectiveness of pharmacological treatments is true for both opioids and non-opioids (Krebs et al., 2018). While opioids and non-opioids both showed modest benefits in a recent randomized controlled trial for people with moderate to serve chronic pain or hip or knee osteoarthritis, opioids have higher rates of side effects. Moreover, Kroenke noted that in multiple trials for different types of chronic non-neuropathic pain, there is insufficient evidence supporting cannabis as an analgesic (Hill, 2015; Nugent et al., 2017).
Possible explanations for the lack of substantial benefits for pain treatments include an almost exclusive reliance on the biomedical model of pain and a focus on managing pain itself rather than managing the person who has pain, said Turk. The biomedical perspective assumes that pain is
a signal of injury or some structural pathology; that removal of the problem may be possible through some mechanical fix; and that treatment consists of symptomatic relief alone. Turk used the example of fibromyalgia to illustrate the problem of approaching a pain condition with symptomatic treatment. A checklist of 43 symptoms is used to evaluate patients with fibromyalgia, and the average patient endorses 33 of these symptoms. A single treatment would almost certainly be insufficient to deal with the fatigue, pain, cognitive and emotional problems, and many other symptoms reported by patients, he said.
Placebo responses—the perceived improvement in symptoms resulting from an inactive treatment—can also complicate evaluations of the effectiveness of pain treatments. Kroenke said that placebos have been shown to reduce pain by 30 to 50 percent. Placebo responses have biological underpinnings mediated by overlapping pain circuits (Kroenke and Cheville, 2017). Although placebo effects can undermine the ability to demonstrate effectiveness of the investigational treatment in clinical trials, Kroenke said these effects should be maximized in clinical practice.
Other important factors contributing to the modest effectiveness of pain treatments is interindividual variability in pain thresholds, response to various treatments, and psychosocial characteristics that influence the experience of pain and the response to treatments, said Turk. Patients also vary in terms of the relationship between objective evidence of pathology and how intensely they experience pain (e.g., patients with the same extent of tissue pathology respond in widely different ways to the same interventions) (Gerbershagen et al., 2013). Thus, objective pathology alone makes it challenging to predict a person’s pain experience and response to treatment. Furthermore, how much pain a person experiences does not necessarily equate to his or her functional limitations, Turk added.
Assessing an individual’s pain is also fraught with problems, said Turk. Objective information, self-reports, functional performance, and behavioral observations may all be useful, but are poorly correlated with one another and highly variable from person to person. Turk argued that in assessing pain, biological factors are important, but must be considered along with the individual’s history, attitudes, beliefs, emotions, behaviors, and emotional and financial resources. Moreover, to maximize therapeutic effectiveness, clinicians need to determine how best to facilitate, encourage, and motivate patients for self-management when a cure is not possible. In addition, Turk said the field needs to develop and evaluate new treatments and regimens that address pain and comorbidities and prevent
misuse and disability; determine what works for whom; evaluate combination treatments; and investigate strategies to facilitate maintenance and generalization of treatment benefits and relapse prevention.
Providing Complementary and Integrative Health Approaches to Different Populations in the United States
David Elton, senior vice president of clinical programs at Optum, presented claims data to describe usage patterns for pharmacological and nonpharmacological pain treatments, noting that claims-based data do not fully reflect usage because they are blind to out-of-pocket expenditures for many nonpharmacological therapies, such as acupuncture, chiropractic services, and massage, and to non-covered services such as yoga, virtual reality, and mindfulness. Claims-based data are also affected by other distortions such as incorrect coding, capitation, and other factors. Nonetheless, and keeping these caveats in mind, Elton said the data from UnitedHealthcare/Optum show that spending on nonpharmacological therapies focused on pain across commercial, Medicare, and Medicaid enrollees totaled about $3.4 billion, or 2.4 percent of all costs in 2017. He noted that Medicare and Medicaid populations encounter increased coverage constraints because most states provide limited to no coverage for acupuncture and chiropractic care.
Using a technique that takes claims data and creates “episodes of care” as a means of understanding spending by diagnostic condition, Elton showed that musculoskeletal complaints are responsible for about 16 percent of costs as well as most prescriptions for opioids and opioid-containing medicines, with back pain being the most frequent complaint.
Elton and colleagues have looked at how a person’s first point of contact after the onset of back pain influences the use of nonpharmacological therapies and opioid use; although, Elton noted that they were not able to adjust for factors that might confound the association between the type of first contact point and opioid use. What they found was that when the first point of contact was a physical therapist, chiropractor, or acupuncturist, the odds of early and long-term exposure to opioids was markedly reduced. He added that while the guidelines suggest that chiropractic manipulation has an important role to play, patients receive this care only if they start with a chiropractor. The same is true for acupuncture, massage, and other nonpharmacological therapies, said Elton, calling this an unacceptable level of variation in care delivery. He added that patients’ decisions
about who will be their first point of contact vary considerably due to individual preferences and how the pain manifests; however, all providers should be aware that these other therapies are indicated and preferred over opioids for most back pain.
Elton added that an economic model on the value of these therapies indicated that if the front-line use of chiropractic or physical therapy could be increased from 30 to 50 percent in 2 years, more than $200 million could be saved per year. He suggested that simple changes in coverage and practice could achieve these savings, adding that he and his colleagues will be testing this idea over the next couple of years.
Reducing Disparities in Pain Management
Managing pain is especially difficult in low-income populations for multiple reasons, said Beverly Thorn, professor emeritus of psychology at the University of Alabama. Although these populations have higher rates of pain, disability, and comorbidities, they lack access to health care resources and consequently get less treatment for pain, she said. Access limitations may also affect other subpopulations, said David Atkins, director of the Department of Veterans Affairs Health Services Research and Development Service. For example, while veterans often have physically demanding jobs that increase the incidence of chronic pain, they may also be unable to take the time off for multiple sessions of acupuncture, chiropractic, or cognitive behavior therapy (CBT).
Thorn noted that low-income populations are often excluded from clinical trials for various reasons, including low literacy. Given that the conclusions drawn from randomized clinical trials with middle-income participants may not generalize to the broader population, Thorn argued for research that focuses on modifying treatments for disadvantaged individuals. For example, she and her colleagues have adapted CBT and self-management treatments by adapting the workbooks and other tools for people with low literacy. In a randomized clinical trial of this literacy-adapted and simplified group CBT approach compared with group pain education or usual care, they showed that after treatment, participants in the modified CBT and group pain education arms had lower pain intensity scores and improved function compared with the usual care arm (Thorn et al., 2018). Interestingly, she said, individuals with the lowest literacy levels and lowest cognitive function received the most benefit from adapted CBT. Anthony Delitto added that modifications of some nonpharmacolog-
ical approaches such as exercise and yoga are also needed for certain subpopulations (e.g., older adults) who may have limited mobility, flexibility, strength, or stamina.










