Summary
Childbirth services play a critical role in the provision of U.S. health care. The current U.S. maternity care system, however, is fraught with inequities in access and quality and high costs, and there is growing recognition of the mismatch between the collective expectations of the care and support women1 deserve and what they actually receive. Moreover, the United States has among the highest rates of maternal and neonatal mortality and morbidity of any high-resource country, particularly among Black and Native American women. It is clear, then, that the systems supporting childbirth in the United States are in need of improvement. This report focuses on opportunities for improvement in one crucial component of U.S. maternity care: the settings in which childbirth occurs. While the vast majority of U.S. women experience childbirth in hospital settings, there is wide variation in the geographic availability of maternity hospitals and in hospital capabilities, types of maternity care providers available, and access to minimal-intervention birth options. In addition, a small (but growing) percentage of women give birth in birth centers or at home (0.52% and 0.99%, respectively). Yet not all women are able to access these options should they desire them, nor is it easy to transfer to a higher level of care when a transfer is indicated. In this context, and given the current state
___________________
1 For the purposes of this report, the term “pregnant women” is used to describe pregnant individuals. The committee recognizes that intersex people and people of various gender identities, including transgender, nonbinary, and cisgender individuals, give birth and receive maternity care. Because we understand the term “woman” may be isolating and not reflective of how some individuals choose to identify, we periodically use the terms “pregnant people” or “pregnant individuals” in place of “pregnant women.” See Box 1-1 in this report.
of U.S. maternity care, two urgent questions for women, families, policy makers, and researchers arise: How can an evidence-informed maternity care system be designed that allows multiple safe and supportive options for childbearing families? How can birth outcomes be improved across and within all birth settings?
To address these questions, congressional representatives asked the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) to task the National Academies of Sciences, Engineering, and Medicine with convening an ad hoc committee of experts to provide an evidence-based analysis of the complex findings in the research on birth settings, focusing particularly on health outcomes experienced by subpopulations of women.
CONCEPTUAL MODEL
In conducting this study, the committee developed a conceptual model (see Figure S-1) identifying key opportunities that can be leveraged to improve policy and practice across birth settings. The triangle at the center indicates three elements that contribute to the ultimate goal of positive outcomes in maternity care: access to care, quality of care, and informed choice and risk assessment. The pregnant person and infant are at the center of this triad, surrounded by the maternity care team; the systems and settings in which care takes place; and collaboration and integration among providers and systems. The physical setting in which a birth takes place is one part of this overall picture, but it is nested among other elements that are relevant regardless of setting and that can be optimized for positive outcomes across and within different birth settings. All of these elements are embedded within the complex sociocultural environment that shapes health outcomes at the individual level and can affect whether these elements are optimally achieved. The components of this environment—the social, clinical, financial, and structural factors that contribute to access, informed choice, quality of care, and outcomes—represent opportunities for interventions to improve individual and population health, well-being, and health equity.
UNDERSTANDING BIRTH SETTINGS
As noted above, women in the United States give birth at home, in birth centers, and in hospitals. Across and even within these categories, the resources and services available differ significantly.2 Women also are cared for
___________________
2 For the purposes of this report, the committee defines a birth center as a freestanding health facility not attached to a hospital. Home births are those that occur at a woman’s residence and can be either planned or unplanned.
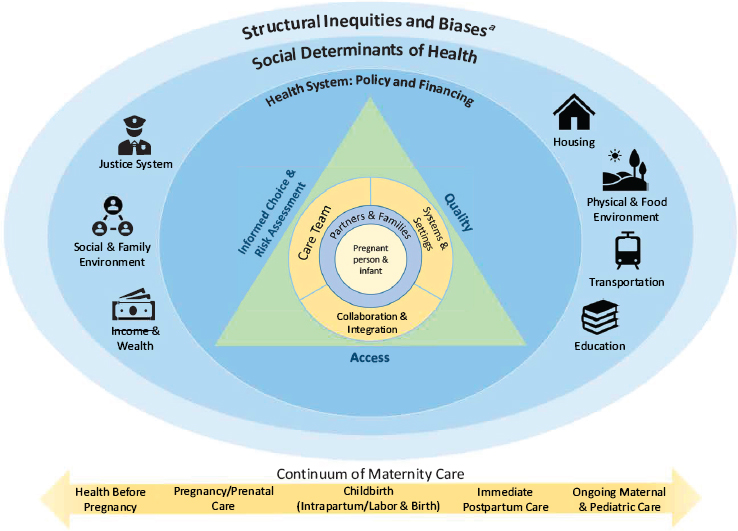
aStructural inequities and biases include systemic and institutional racism. Interpersonal racism and implicit and explicit bias underlie the social determinants of health for women of color.
by a number of different providers during their pregnancy and when giving birth, and these providers differ in how they are educated, trained, licensed, and credentialed. Moreover, women pay for maternity care through a variety of mechanisms, including private insurance (both individually purchased and employer-sponsored), Medicaid, Medicare, and self-pay; and the payment mechanism can affect what services, providers, and settings are available. State policies and regulations, too, can influence a woman’s birth experience, through laws as to which providers can practice, their scope of practice, and the legal status of birth settings. Contextual factors (e.g., the social determinants of health, structural inequities and biases, medical risk factors) also influence where care is delivered and the content of care.
CLINICAL RISK AND SYSTEMIC INFLUENCES ON OUTCOMES IN PREGNANCY AND CHILDBIRTH
Although pregnancy and birth unfold without complication in most cases, neither is devoid of risk, and some groups of women enter pregnancy and birth with more risk than others. Risk during pregnancy—which the
committee defines as the increased likelihood of an adverse maternal, fetal, or neonatal outcome—is conferred by four main sources: individual medical and obstetrical factors; health system–related factors, such as policy and financing decisions; the social determinants of health; and structural inequities and biases in the health system and in society at large. At a population level, these risk factors reflect the pattern of inequities in maternity care observed along racial/ethnic, geographic, and economic lines. For an individual woman, these sources of risk can interact and intersect, in some cases amplifying each other. For example, women with substance use disorders, a medical risk factor, are also less likely to receive adequate prenatal care and more likely to experience intimate partner violence than are pregnant women without substance use disorders, thereby increasing their risk in pregnancy and childbirth. Moreover, these risk factors affect both the pregnant individual’s and the health care provider’s decision making, shaping which birth settings have the capacity to offer safe, risk-appropriate care.
Women, however, may conceive of, tolerate, or understand risk differently from their health care providers, or may simply have competing priorities and values (e.g., control, respect, faith) that they prioritize over and above medical risks. There is broad consensus that women capable of doing so have the right to make informed decisions about their care, including decisions about their choice of care provider and place of birth (American College of Nurse-Midwives, 2017b; American College of Obstetricians and Gynecologists, 2017a). Informed choice, however, requires a set of real options, accurate and accessible information about the risks and benefits of those options, appropriate and ongoing medical/obstetrical risk assessment, respect for women’s informed decisions (including informed refusals), and recognition that those choices may change over the course of care.
Such choice is often constrained by systemic factors that limit access. In its conceptual model, for example, the committee recognizes that structural inequities and biases are historically rooted and deeply embedded in policies, laws, governance, and culture such that power and resources are distributed differentially across characteristics of identity (race, ethnicity, gender, class, sexual orientation, and others), all of which influence health outcomes. For example, any discussion of risk assessment, choice, and equity in birth settings and birth outcomes must encompass the historical problem of disparate outcomes influenced by structural racism. Racism and discrimination—both in the health care system and in everyday life—have a well-documented impact on the health of marginalized communities. The adverse impacts of racism can be manifested in lower-quality health care; residential segregation and lack of affordable housing; or the accumulation of daily stressors resulting from micro- and macro-level aggressions, unconscious and conscious bias, and discrimination. They can thereby influence
the health outcomes of pregnant people and their infants, causing considerable racial/ethnic disparities in pregnancy-related outcomes.
Moreover, birthing facilities and maternity care providers are unevenly distributed across the United States, leaving many women without access to prenatal, birthing, and postpartum care and choices among options near home. Women living in rural communities and underserved urban areas also have greater risks of such poor outcomes as preterm birth and maternal and infant mortality, in part because of a lack of access to maternity and prenatal care in their local area. In addition, some areas may lack access to midwifery care because certain types of midwives are not licensed in some states and do not have admitting privileges in some medical facilities, a factor that varies across the country. Indeed, the wide variation in regulation, certification, and licensing of maternity care professionals across the United States is an impediment to access across all birth settings. Moreover, access to all types of birth settings and providers is limited because of the lack of universal coverage of the cost of care for all women, for all types of providers, and at all levels. Taken together, system-level factors and social determinants of health such as structural racism, lack of financial resources, availability of transportation, housing instability, lack of social support, stress, limited availability of healthy and nutritious foods, lower level of education, and lack of access to health care (including mental health care) are correlated with higher risk for poor pregnancy outcomes and inequity in care and outcomes.
MATERNAL AND NEWBORN OUTCOMES BY BIRTH SETTING
Data and methodological limitations make the study of outcomes by birth setting challenging. Both vital statistics and birth registry data have limitations for evaluating birth outcomes by setting, provider type, and intentionality. In addition to these data deficiencies, the literature on birth settings compares a wide array of beneficial and nonbeneficial outcomes across and within settings. Studies often use differing definitions and terminology and report differing outcomes, making it difficult to conduct assessments or draw useful conclusions. In addition, the overall small number of women giving birth in home and birth center settings in the United States leads to unstable estimates with wide confidence intervals for outcomes of such rare events as maternal and fetal death. Furthermore, the literature on health outcomes by birth setting largely does not address difference by race/ethnicity or other subpopulations.
With these caveats in mind, the committee reviewed the available evidence and concluded that each birth setting—home, birth center, and hospital—has both risks and benefits for either the pregnant woman or the newborn. “Too little, too late” (TLTL) and “too much, too soon” (TMTS)
patterns in the provision of maternity care contribute to excess morbidity and mortality, and in the context of inequality, these extremes often coexist within a single health care system. While the evidence suggests that no setting can fully eliminate risk from birth, many risks are modifiable at the level of systems, policies, processes, and providers.
Based on its review of the evidence, the committee found the following regarding outcomes comparing birth settings:
- Statistically significant increases in the relative risk of neonatal death in the home compared with the hospital setting have been reported in most U.S. studies of low-risk births using vital statistics data. However, the precise magnitude of the difference is difficult to assess given flaws in the underlying data. Regarding serious neonatal morbidity, studies report a wide range of risk for low-risk home versus hospital birth and by provider type. Given the importance of understanding these severe morbidities, the differing results among studies are of concern and require further study.
- Vital statistics studies of low-risk births in freestanding birth centers show an increased risk of poor neonatal outcomes, while studies conducted in the United States using models indicating intended place of birth have demonstrated that low-risk births in birth centers and hospitals have similar to slightly elevated rates of neonatal mortality. Findings of studies of the comparative risk of neonatal morbidity between low-risk birth center and hospital births are mixed, with variation across studies by outcome and provider type.
- In the United States, low-risk women choosing home or birth center birth compared with women choosing hospital birth have lower rates of intervention, including cesarean birth, operative vaginal delivery, induction of labor, augmentation of labor, and episiotomy, and lower rates of intervention-related maternal morbidity, such as infection, postpartum hemorrhage, and genital tract tearing. These findings are consistent across studies. The fact that women choosing home and birth center births tend to select these settings because of their desire for fewer interventions contributes to these lower rates.
- Some women experience a gap between the care they expect and want and the care they receive. Women want safety, freedom of choice in birth setting and provider, choice among care practices, and respectful treatment. Individual expectations, the amount of support received from caregivers, the quality of the caregiver–patient relationship, and involvement in decision making appear to be the greatest influences on women’s satisfaction with the experience of childbirth.
- International studies suggest that home and birth center births may be as safe as hospital births for low-risk women and infants when (1) they are part of an integrated, regulated system; (2) multiple provider options across the continuum of care are covered; (3) providers are well-qualified and have the knowledge and training to manage first-line complications; (4) transfer is seamless across settings; and (5) appropriate risk assessment and risk selection occur across settings and throughout pregnancy. Such systems are currently not widespread in the United States.
- A lack of data and the relatively small number of home and birth center births prevent exploration of the relationship between birth settings and maternal mortality and severe maternal morbidity.
In summary, given both the acute and downstream risks of unnecessary interventions and the risks associated with potentially delayed access to lifesaving obstetric and neonatal interventions, there is no risk-free option for giving birth.
FRAMEWORK FOR IMPROVING BIRTH OUTCOMES ACROSS BIRTH SETTINGS
The system-level factors that influence outcomes across birth settings are responsive to intervention, yet these interventions are largely outside the scope of the health care system. Housing instability, limited transportation, and intimate partner violence (i.e., social determinants of health) fall into this category. Given the committee’s charge, we focus on factors that can be influenced within the health care system, through changes to either service delivery or the services themselves. Of course, the committee acknowledges that while many disparities in outcomes accrue within the health care system, drivers of inequities in these outcomes begin outside the health care system. This reality undergirds our framework for maternal and newborn care in the United States—recognizing the need to build a culture of health equity; ensuring that pregnant people and infants receive the right amount of care at the right time; and delivering care in a respectful way, regardless of circumstance—but there is a critical need for more research on how these factors affect birth outcomes.
Because the committee recognizes that no birth setting is risk free and supports a woman’s right to choose where and with whom she gives birth, we focus on opportunities for addressing the question of how each setting can improve outcomes and make birth safer. With the goal of building respect for pregnant people, their infants, their partners, and their families regardless of their circumstances (race, ethnic origin or immigration status,
gender identity, sexual orientation, marital status, family composition, religion, income, or education) or birth or health choices, the committee suggests opportunities for practice, policy, and systems change that reduce barriers to the exercise of those choices.
Hospital Settings
The committee recognizes that many interventions are overused in U.S. hospital settings today. There are promising strategies and approaches for lowering the rates of nonmedically indicated and morbidity-related interventions, such as the primary cesarean rate in hospital settings. Evidence from promising models in the United States points to performance measurement, support for continuous quality improvement (QI), and mechanisms for accountability as key strategies for improving outcomes for pregnant women and infants while potentially yielding high-value care through cost savings as well. Emerging literature points to four core components of successful QI initiatives: engagement of multiple disciplines and partner organizations, mobilization of low-burden and rapid-cycle data, provision of up-to-date guidance for implementation using safety bundles and toolkits, and availability of coaching and peer learning. While many QI initiatives have shown promising results, many current QI initiatives are underfunded. To build on these promising findings and effectively implement QI at all levels of health care, QI initiatives will need to receive sufficient and sustainable financing from both government and private entities.
CONCLUSION 7-1: Quality improvement initiatives—such as the Alliance on Innovation in Maternal Health and the National Network of Perinatal Quality Collaboratives—and adoption of national standards and guidelines—such as the Maternal Levels of Care of the American College of Obstetricians and Gynecologists and Society for Maternal-Fetal Medicine; the American Academy of Pediatrics’ Neonatal Levels of Care; and guidelines for care in hospital settings developed by the Association of Women’s Health, Obstetric, and Neonatal Nurses, the Society for Obstetric Anesthesia and Perinatology, and the American College of Nurse-Midwives—have been shown to improve outcomes for pregnant people and newborns in hospital settings.
Women’s ability to exercise choice with regard to birth setting is also limited by a lack of access-to-care options in hospital settings.
CONCLUSION 7-2: Providing currently underutilized nonsurgical maternity care services that some women have difficulty obtaining, including vaginal birth after cesarean, external cephalic version, planned
vaginal breech, and planned vaginal twin birth, according to the best evidence available, can help hospitals and hospital systems ensure that all pregnant people receive care that is respectful, appropriate for their condition, timely, and responsive to individual choices. Developing in-hospital low-risk midwifery-led units or adopting these practices within existing maternity units, enabling greater collaboration among maternity care providers (including midwives, physicians, and nurses), and ensuring cultivation of skills in obstetric residency and maternal-fetal medicine fellowship programs can help support such care.
High-value payment models with measures, performance targets, and value-based payment are also mechanisms for accountability. While maternity care costs have risen, performance has routinely fallen short and is worsening for some indicators. Payment tied to value, whether or not optimal care occurred or an optimal outcome was achieved, can incentivize quality, create conditions for innovative systems, improve care and outcomes, and reduce costs, among other favorable improvements.
CONCLUSION 7-3: Efforts are needed to pilot and evaluate high-value payment models in maternity care and identify and develop effective strategies for value-based care.
Home and Birth Center Settings
Examples from international experience demonstrate that positive outcomes for pregnant women and infants can be achieved across birth settings in the context of a system that promotes coverage for all women and types of providers, collaboration, seamless transfer, and coordination among providers and settings. Moreover, a recent U.S. study suggests that greater integration of midwifery professionals within a state’s maternal care system may be related to improved maternal and newborn health outcomes. This evidence indicates that key components of integration and collaboration include shared care and access to safe and timely consultation, seamless transfer across settings, appropriate risk assessment and risk selection across settings and throughout the episode of care, well-qualified maternity care providers with the knowledge and training to manage first-line complications, collaborative QI initiatives, and the use of multidisciplinary model guidelines for transfer between settings.
CONCLUSION 7-4: Integrating home and birth center settings into a regulated maternity and newborn care system that provides shared care and access to safe and timely consultation; written plans for discussion, consultation, and referral that ensure seamless transfer across
settings; appropriate risk assessment and risk selection across settings and throughout the episode of care; and well-qualified maternity care providers with the knowledge and training to manage first-line complications may improve maternal and neonatal outcomes in these settings.
Key to this integration is the appropriate education and training of all maternal and newborn care providers, reflecting the setting and the risk level of those they serve. Appropriate education, training, and certification coupled with licensing statutes, generally written with great specificity, can ensure that planned home and birth center births are limited, to the extent feasible, to healthy, low-risk women and that midwives and other providers working in those settings continually assess and monitor risks and complications so they can be properly and promptly addressed. Such risk assessment would need to consider not only medical and obstetric risk, but also social risk and the contextual lives of pregnant people. When assessing medical risk and monitoring for medical and obstetric complications among women of color, it is critically important that membership in a racial/ethnic group not overdetermine the assessment and constrain the birth setting or maternity care provider options made available to a given woman.
Currently, as noted above, certain types of midwives cannot be licensed in some states or obtain admitting privileges to some medical facilities, and this wide variation in regulation, certification, and licensing of maternity care professionals is an impediment not only to integration but also to access to high-quality care across all birth settings. Therefore, the committee endorses efforts to license certified nurse midwives, certified midwives, and certified professional midwives whose education meets International Confederation of Midwives (ICM) Global Standards for midwifery education, who have completed an accredited midwifery education program, and who are nationally certified in all jurisdictions in the United States.
CONCLUSION 7-5: The availability of mechanisms for all freestanding birth centers to access licensure at the state level and requirements for obtaining and maintaining accreditation could improve access to and quality of care in these settings. Additional research is needed to understand variation in outcomes for birth centers that follow accreditation standards and those that do not.
CONCLUSION 7-6: The inability of all certified nurse midwives, certified midwives, and certified professional midwives whose education meets International Confederation of Midwives Global Standards, who have completed an accredited midwifery education program, and who are nationally certified to access licensure and practice to the
full extent of their scope and areas of competence in all jurisdictions in the United States is an impediment to access across all birth settings.
Informed Choice and Risk Selection
Women have the right to informed choice of the birth setting they desire, but to exercise that choice, they must have access to options for birth settings. As discussed above, therefore, informed choice requires a set of real options, accurate information about the risks and benefits of each option, respect for women’s informed decisions, and recognition that choices may change over the course of care. Decision aids have been found to be useful and effective in helping health care consumers access and understand treatment options and their risks and benefits and in facilitating shared decision making. Counseling can also help women make an informed choice of birth setting, and risk assessment is a vital component of determining the optimal approach to providing such counseling.
CONCLUSION 7-7: Ongoing risk assessment to ensure that a pregnant person is an appropriate candidate for home or birth center birth is integral to safety and optimal outcomes. Mechanisms for monitoring adherence to best-practice guidelines for risk assessment and associated birth outcomes by provider type and settings is needed to improve birth outcomes and inform policy.
CONCLUSION 7-8: To foster informed decision making in choice of birth settings, high-quality, evidence-based online decision aids and risk-assessment tools that incorporate medical, obstetrical, and social factors that influence birth outcomes are needed. Effective aids and tools incorporate clinical risk assessment, as well as a culturally appropriate assessment of risk preferences and tolerance, and enable pregnant people, in concert with their providers, to make decisions related to risk, settings, providers, and specific care practices.
Access to Care and Birth Settings
The committee’s review of the current financing mechanisms and costs associated with maternity care in the United States revealed that access to care is often limited by a woman’s ability to pay, as only a limited number of insurance payers offer coverage for care in home or birth center settings or for certain provider types, and some women are unable to access insurance coverage at all. Moreover, many beneficial maternity care services and supports are not covered. For instance, doula support across birth
settings—a model associated with better outcomes for women and infants, as well as cost savings—is covered by Medicaid in only three states.
CONCLUSION 7-9: Access to choice in birth settings is curtailed by a pregnant person’s ability to pay. Models for increasing access to birth settings for low-risk women that have been implemented at the state level include expanding Medicaid, Medicare, and commercial payer coverage to cover care provided at home and birth centers within their accreditation and licensure guidelines; cover care provided by certified nurse midwives, certified midwives, and certified professional midwives whose education meets International Confederation of Midwives Global Standards, who have completed an accredited midwifery education program, and who are nationally certified; and cover care provided by community-based doulas. Additional research, demonstration, and evaluation to determine the potential impact of these state-level models is needed to inform consideration of nationwide expansion, particularly with regard to effects on reduction of racial/ethnic disparities in access, quality, and outcomes of care.
It is also important that reimbursement levels be adequate to support quality care and allow providers across settings to sustain services. Currently, payment to providers through Medicaid and Medicare may not cover the full cost of care and prevents some providers from accepting more women with Medicaid coverage.
CONCLUSION 7-10: Ensuring that levels of payment for maternity and newborn care across birth settings are adequate to support maternity care options across the nation is critical to improving access.
Access is also limited by the availability of a range of birth settings, including hospital maternity units, in a woman’s locality. Because birthing facilities and maternity care providers are unevenly distributed across the United States, many women cannot access prenatal, birthing, and postpartum care options near their homes. In particular, women living in rural communities and underserved urban areas face greater risks of such poor outcomes as preterm birth and maternal and infant mortality. Rural and urban maternity care deserts present unique challenges to improving maternal and newborn care in the United States, and efforts are urgently needed to resolve disparities in outcomes by geographic location.
CONCLUSION 7-11: Research is needed to study and develop sustainable models for safe, effective, and adequately resourced maternity care in underserved rural and urban areas, including establishment of
sustainably financed demonstration model birth centers and hospital services. Such research could explore options for using a variety of maternity care professionals—including nurse practitioners, certified nurse midwives, certified professional midwives, certified midwives, public health nurses, home visiting nurses, and community health workers—in underserved communities to increase access to maternal and newborn care, including prenatal and postpartum care. These programs would need to be adequately funded for evaluation, particularly with regard to effects on reduction of racial/ethnic and geographic disparities in access, quality, and outcomes of care.
Analyses of the current composition of the maternity and newborn care workforce in the United States show a mismatch between the care needs of the population as a whole and the proportion of providers best equipped to meet those needs. While the system at present relies primarily on a surgical specialty to provide front-line care, most childbearing women are largely healthy and do not need that type of care in first-line providers. The composition of the maternity care workforce in the United States stands in great contrast to that in a number of other countries where the ratio of midwives to obstetricians is much higher. The growing shortage of obstetricians in the United States, due to such factors as early retirement and job dissatisfaction, offers an opportunity to rectify this situation by focusing resources on growing the cadre of providers with nationally recognized credentials who are especially prepared to provide care to healthy low-risk women. As part of these efforts and to address racial/ethnic inequities in outcomes, attention is needed to ensure that the maternity and newborn care workforce resembles the racial/ethnic composition of the population of childbearing women, as well as its linguistic, geographic, and socioeconomic diversity. A large body of literature demonstrates the benefits of a diverse workforce, ranging from providing culturally concordant care to fostering trust in providers and improving outcomes.
CONCLUSION 7-12: To improve access and reduce racial/ethnic disparities in quality of care and treatment, investments are needed to grow the pipeline for the maternity and newborn care workforce—including community health workers, doulas, maternity nurses, nurse practitioners and physicians’ assistants, public health nurses, family medicine physicians, pediatricians, midwives, and obstetricians—with the goal of increasing its diversity, distribution, and size. Greater opportunities for interprofessional education, collaboration, and research across all birth settings are also critical to improving quality of care.
Research, Evaluation, and Data Collection
Despite decades of advancement in medical science and technology, much remains unknown about perinatal health. The scientific challenge is to better understand the science of childbirth—from biology to policy—to improve outcomes for mothers, infants, and families. The committee offers a number of priority areas for future research in this report. In addition, the committee emphasizes that strengthening data collection, in particular, improving the usefulness of birth certificate records for birth settings research, is key to advancing understanding of outcomes across birth settings.
CONCLUSION
The challenges facing the current U.S. maternity care system, while urgent, are not insurmountable, and opportunities for improving the systems that support childbirth exist. To improve maternal and infant outcomes in the United States, it is necessary to provide economic and geographic access to maternity care in all settings, from conception through the first year postpartum; to provide high-quality and respectful treatment; to ensure informed choices about medical interventions when appropriate for risk status in all birth settings; and to facilitate integrated and coordinated care across all maternity care providers and all birth settings. Achieving these objectives will require coordination and collaboration among multiple actors—professional organizations, third-party payers, governments at all levels, educators, and accreditation bodies, among others—to ensure systemwide improvements for the betterment of all women, newborns, and families.














