7
Achieving Acceptance of COVID-19 Vaccine
Approval, allocation, and distribution of one or more safe and effective coronavirus disease 2019 (COVID-19) vaccines will be a remarkable achievement. However, as has been pointed out repeatedly since the earliest days of the COVID-19 pandemic, readying a vaccine is just the starting point of what will be a challenging journey to achieving widespread public acceptance of COVID-19 vaccines. Strong demand for and acceptance of COVID-19 vaccines will be critical for protecting vulnerable populations and for regaining our pre-pandemic social and economic lives, but ensuring demand and promoting acceptance will be challenging.
Recent survey data from several sources suggest that willingness to be vaccinated with a novel COVID-19 vaccine is hovering at around 60–70 percent of the general population (Fisher et al., 2020; Kamisar and Holzberg, 2020; Mullen O’Keefe, 2020; Resnick, 2020; Thigpen and Funk, 2020). It is lower—in some cases, much lower—in specific sociodemographic groups: Black or Hispanic communities; those with lower educational attainment; and those who live in rural areas, among other groups (Callaghan et al., 2020; Fisher et al., 2020; Kamisar and Holzberg, 2020; Reich, 2020; Resnick, 2020). The reasons given for COVID-19 vaccine hesitancy are many. Some people have concerns about the safety of the vaccine, particularly given the unprecedented speed with which COVID-19 vaccines have moved through the development pipeline (Silverman, 2020). Distrust in the government, in the medical research community, and in pharmaceutical companies is also common (Fisher et al., 2020). Some people may feel they do not need the vaccine, either because they have already had (or believe they have had) COVID-19, they do not believe COVID-19
is a serious threat to their health, or they simply do not believe in vaccination (Fisher et al., 2020).
In surveys that capture a “not sure” or “maybe” response to questions about accepting a COVID-19 vaccine, this hesitant group is often larger than the “no” or plan to decline group (Fisher et al., 2020; Kamisar and Holzberg, 2020). Hesitant or unsure respondents may be waiting for more information about vaccine trial outcomes (safety and efficacy) or the vaccine approval process; they may also want to wait and see how those in their social networks behave. If the “wait and see” group sits out the early months of widespread vaccine rollout, achieving high population coverage will be delayed. Among the majority of U.S. residents reporting that they do plan to take the vaccine, ensuring that they actually receive the vaccine is also challenging. As has been observed frequently with seasonal influenza vaccination, even individuals with strong intentions to receive an influenza vaccine will often procrastinate, forget, or balk at seemingly small logistic or financial barriers (Harris et al., 2009, 2011; Schmid et al., 2017).
In this chapter, the committee reviews the complex and dynamic landscape of vaccine hesitancy, discusses its specific application and relevance to COVID-19 vaccination, and highlights the World Health Organization’s (WHO’s) Measuring Behavioral and Social Drivers of Vaccination (BeSD) Increasing Vaccination Model as an organizing framework for recommendations to address COVID-19 vaccine hesitancy and ensure robust demand for an approved vaccine.
THE LANDSCAPE OF VACCINE HESITANCY
Many intersecting social, cultural, legal, and historical factors shape the landscape into which a COVID-19 vaccine will be launched. The committee highlights several of the most relevant in the following sections.
Vaccine Hesitancy Is Common and on the Rise
Over the past 20 years, U.S. residents—and in particular, parents of young children—have reported increasing concerns about vaccine safety, the number of vaccines included in the routine childhood immunization schedule, and purported links (repeatedly proved incorrect) between vaccination and neurocognitive or biomedical conditions (Maglione et al., 2014). Potential consequences of vaccine hesitancy—which the committee views as an attitude, preference, or motivational state—are the behaviors of vaccine refusal or delay (Brewer et al., 2017). A cohort study by Glanz and colleagues (2013) found that in eight managed care organizations across the United States more than 10 percent of parents reported delaying or refusing vaccinations for their children. Another behavioral manifestation
of increased hesitancy is rising rates of personal belief and other nonmedical exemptions from school and day care entry vaccine mandates. From 2005–2006 through 2012–2013, the national rate of nonmedical exemptions almost doubled, and from 2011–2012 to 2017–2018, the median total nonmedical exemption rate increased by nearly 67 percent (Bednarczyk et al., 2019; Wang et al., 2014). Vaccine refusal and exemptions are high enough in some focused geographic regions to sustain outbreaks of vaccine-preventable diseases. According to one 2018 study, a select group of metropolitan “hot spots” in the United States are responsible for a large number of nonmedical exemptions, and overall, there is an inverse relationship between nonmedical exemption rates and measles, mumps, and rubella vaccine coverage in states with hot spots (Olive et al., 2018). Recent outbreaks of infectious diseases, including measles and mumps, may be attributed to current trends in childhood vaccine hesitancy and refusal among parents (Saint-Victor and Omer, 2013; Zipprich et al., 2015). Beyond routine childhood immunizations, many U.S. residents decline the seasonal influenza vaccine, and coverage rates for many teen and adult vaccines are well below what is needed to achieve adequate population health protection (Williams et al., 2017). Globally, vaccine hesitancy was listed among WHO’s list of Ten Threats to Global Health in 2019 (WHO, 2019).
Organized, Well-Funded, and Influential Anti-Vaccine Groups
Anti-vaccine sentiment is as old as vaccination itself. Today, groups dedicated to anti-vaccination advocacy are active across the United States (Ball, 2020; Cohen and Vigue, 2020; Johnson et al., 2020; Reich, 2020), and have spurred disease outbreaks including measles outbreaks in the Somali community in Minneapolis, Minnesota (2017), and the Orthodox Jewish community in New York (2019). Recently, online social networks have become a leading source of deliberate misinformation on vaccines, driven by both anti-vaccination advocates and by bots and trolls hoping to amplify debates and drive skepticism. A 2018 study on vaccination activity on Twitter found that bots, trolls, and so-called “content polluters” covered the topic more extensively than did average users, with polluters in particular driving anti-vaccine content (Broniatowski et al., 2018). A 2020 analysis of nearly 100 million people expressing views regarding vaccination on Facebook showed significant growth in anti-vaccination clusters, compared to pro-vaccination clusters, with anti-vaccination clusters being more likely to engage with undecided individuals; the authors predicted that based on current trends, anti-vaccination views will dominate in the next 10 years (Johnson et al., 2020). They also noted that, unlike the singularly focused messaging of pro-vaccination advocates, anti-vaccination messages typically draw on a combination of issues, including safety concerns, con-
spiracy theories, and distrust of government and scientists. Examination of vaccine advertisements on Facebook showed that the median number of ads per buyer was higher for anti-vaccine ads than for pro-vaccine ads and were paid for by a small set of anti-vaccine advertisement buyers (Jamison et al., 2020).
Evidence suggests that members of the anti-vaccination movement are already mobilizing to discourage individuals from receiving a COVID-19 vaccine (Ball, 2020). Deliberately false information about COVID-19 vaccinations (e.g., they are a mechanism to implant microchips into people) is already being widely disseminated. Some members of the anti-vaccination movement have been opposed to other measures to deal with the COVID-19 pandemic, including stay-at-home orders, mask wearing, and contact tracing (Bogel-Burroughs, 2020). A better understanding of both the anti-vaccination movement and approaches that could be successful to counter their actions is needed.
Medical Exploitation and Distrust
Beyond a history of a system that has not always been trustworthy for many populations, a painful legacy of health care discrimination, medical research exploitation, and unconsented experimentation on Black, Latinx, American Indian, Alaska Native, and other marginalized communities has contributed to justified distrust of government-sponsored medical research (Frakt, 2020; Gamble, 1997). Examples include the infamous Tuskegee study—in which hundreds of Black men in Alabama were lied to about being treated for syphilis while the disease was allowed to run its course; the Edmonston-Zagreb vaccine trial, during which parents of immunized infants (mostly Black and Latinx) were not informed that the vaccine used was an unapproved experimental vaccine; and less well known but equally abhorrent instances of unconsented sterilization of Latinx and American Indian and Alaska Native women (Carpio, 2004; Gamble, 1997; University of Wisconsin, 2018). This legacy leaves many communities of color wary of participation in medical research, suspicious of initiatives to engage them in health promotion or surveillance efforts, and, in many cases, reluctant to become vaccinated (Hoffman, 2020). For example, in a study of influenza vaccine uptake among Medicare Fee-for-Service beneficiaries, vaccine receipt was higher among White (49.4 percent) and Asian (47.6 percent) beneficiaries compared to Black (32.6 percent) and Hispanic (29.1 percent) beneficiaries (Hall et al., 2020). Multiple surveys have shown Black and Latinx respondents to be less likely to report intentions to get vaccinated when a COVID-19 vaccine is available (Callaghan et al., 2020; Cohen and Vigue, 2020; Fisher et al., 2020; Kamisar and Holzberg, 2020; Resnick, 2020), and there is widespread concern about the ability of COVID-19
vaccine Phase III trials to enroll individuals from Black, Latinx, Indigenous, and other marginalized communities (Chastain et al., 2020; Feuerstein et al., 2020). Culturally tailored outreach and promotion campaigns that acknowledge this history and actively seek to rebuild trust among marginalized communities will be needed to ensure that the benefits of vaccination are available to all, and to help mitigate disparities that already exist.
Unique Challenges to COVID-19 Vaccine Acceptance
Even among persons typically supportive of vaccination, concerns have been raised about COVID-19 vaccines given the unique circumstances of its development and testing. In one study, 15 percent of persons who said they were at least somewhat supportive of vaccines said they would not get a COVID-19 vaccine (Murphy, 2020). The unprecedented speed with which COVID-19 vaccines have been developed is an important component of safety concerns. If a COVID-19 vaccine is approved or authorized (e.g., through Emergency Use Authorization) by the U.S. Food and Drug Administration (FDA) in the coming months, the vaccine development and approval process will have occurred far more quickly than for any previous vaccine.
Concerns have also been raised that the vaccine development process is being rushed for political ends and are reflected in recent polling as well (Silverman, 2020). To counter these concerns, FDA has developed recommendations for the performance of any approved COVID-19 vaccine (e.g., it will be at least 50 percent effective) and has committed to the use of an independent advisory committee to decide about licensure of candidate vaccines (Burton, 2020). Nine leading pharmaceutical companies involved in COVID-19 vaccine development have also signed a public pledge that no shortcuts will be taken during the approval process (Facher, 2020). Despite these reassurances, the recent emergency use authorization of convalescent plasma (a COVID-19 therapy) based on what many considered insufficient data to support efficacy has reinforced concerns about the politicization of the FDA process (Mahase, 2020; NIH, 2020). It is also important to note that potential mistrust in public health authorities and a COVID-19 vaccine are not emerging on a “blank canvas.” More broadly, other systemic failures to contain or mitigate COVID-19, including personal protective equipment shortages, inconsistent and frequently changing guidelines regarding the use of masks and diagnostic testing, and inadequate testing and contact tracing programs, have further eroded the public’s trust in government response. In light of these events and the other circumstances previously described, ensuring confidence in COVID-19 vaccines in tandem with other preventive measures will be an important challenge, and one that will likely require greater attention than for a typical new vaccine.
WHO BESD INCREASING VACCINATION MODEL
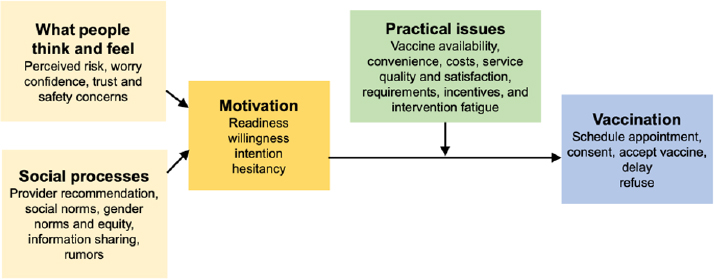
In 2018, WHO convened an expert working group called BeSD to advance the development of tools to track and address under-vaccination; BeSD also published a theoretical Increasing Vaccination Model. This model, based on earlier work by Brewer and colleagues (2017), provides a useful organizing framework for important demand-side considerations related to addressing vaccine hesitancy and successfully promoting the novel coronavirus vaccine (WHO, 2020) (see Figure 7-1).
Motivation
At the heart of WHO’s BeSD Increasing Vaccination Model is motivation to be vaccinated. Motivation can be captured by concepts like readiness, willingness, hesitancy, or intention. Motivation is what is measured in survey questions such as, “How likely is it that you will get a COVID-19 vaccine when it is available?” In the Increasing Vaccination Model, motivation is shaped both by what people think and feel about vaccination, and also by social processes that play out in their environment. What people believe about the severity of COVID-19 and the effectiveness and safety of a vaccine, their trust in public health or medical authorities, their tolerance for risk, and how they feel about needles are all examples of “think and feel” elements that precede motivation.
At the same time, it is well known that humans are very socially motivated (Reid et al., 2011). It is generally important to people that they fit in and garner social approval; and people commonly take their behavioral cues from those around them. This means that a strong recommendation from a health care provider or a clergy member can increase motivation to vaccinate, whereas hearing from friends, family members, or social net-
SOURCE: WHO, 2020.
work contacts who choose not to become vaccinated can decrease motivation. The importance of both thoughts and feelings and social processes in shaping motivation makes it very evident how influential, disruptive, and “sticky” misinformation can be. Myths about vaccine risks, misinterpretations of data about the severity of the disease being prevented, or intentional distortions or misreporting of scientific evidence can all shape what people think and feel; the impact of misinformation on motivation increases as it is propagated and amplified through social networks.
Practical Issues
The motivation to be vaccinated results in actual vaccination only if practicalities of availability, accessibility, cost, convenience, service quality, and incentives are all addressed. As previously noted, researchers know from seasonal influenza vaccination (and other screening and prevention behaviors, such as colonoscopies and the proper use of sunscreen) that the motivation–behavior gap can be large. While many of these practical issues were addressed in Chapter 5, it is worth highlighting the aspects of vaccination that can impact demand through behavioral mechanisms. These include:
- Vaccine availability: Is the vaccine available in my neighborhood? Do I have to go to a doctor’s office, or can I get vaccinated at my pharmacy, my job, or my gym?
- Cost: Do I have to pay for the vaccine? Is there an administration fee? What’s my co-pay? Even small fees and cost sharing can introduce friction and reduce demand.
- Convenience: Can I get the vaccine after hours? Do they have a drive-through? Is there a long wait? How easy is it to make an appointment and sign-in?
- Service quality: Do I feel welcome at the vaccine location? Am I treated well? Is there an opportunity to ask questions or follow up with concerns?
STRATEGIES FOR VACCINE PROMOTION AND ADDRESSING VACCINE HESITANCY
A 2015 systematic review of strategies to address vaccine hesitancy stated that “given the complexity of vaccine hesitancy and the limited evidence available on how it can be addressed, identified strategies should be carefully tailored according to the target population, their reasons for hesitancy, and the specific context” (Jarrett et al., 2015). This lesson will be critically important for addressing hesitancy around COVID-19 vaccination
in the United States and elsewhere, especially as unique concerns around the development and safety of COVID-19 vaccines continue to evolve. There is no “one-size-fit-all” solution to vaccine hesitancy, and nuanced approaches are key to ensuring that existing health inequities are addressed and to ensuring that those who are hesitant do not turn to outright vaccine refusal. By addressing vaccine hesitancy in order to gain and build public trust, it is critical to consider the needs and input of specific populations, a position endorsed by WHO’s tailoring immunization programmes guidance (WHO, 2020). Multiple literature reviews have noted that single-component interventions to address vaccine hesitancy and promote vaccine uptake are not as effective as those that include multiple components, though the ideal combination of intervention strategies requires further investigation (Brewer et al., 2017; Dubé et al., 2015; Jarrett et al., 2015). Furthermore, the strength of the relationship between stated intentions to vaccinate and actual vaccination behavior requires further investigation (Brewer et al., 2017). Interventions that target direct behavior change, as opposed to those that aim to modify thoughts and feelings about vaccination or the social norms around them, have also been found to be more effective (Brewer et al., 2017). Strategies categorized as behavior focused include incentives, sanctions, and requirements—including, for example, vaccination requirements for school entry. A shared theme among these strategies is that many attempt to shift the framing of vaccination such that it is viewed as a routine, expected behavior—such that vaccination is viewed as the accepted norm (Brewer et al., 2017). This approach is already popular for many routine childhood immunizations in the United States.
Among the strategies discussed by WHO to address vaccine hesitancy are the engagement of community leaders, social mobilization tactics, mass media campaigns, the use of reminder and follow-up systems, training and education of health care professionals, nonfinancial incentives, vaccine mandates, efforts to make vaccination more convenient, and efforts to increase general knowledge and awareness about vaccines and vaccination (Jarrett et al., 2015; WHO, 2020). Ultimately, using a combination of these elements and others, evidence suggests that efforts to counter vaccine hesitancy and promote the vaccine should emphasize putting “people at the center” of efforts, as stated by a 2020 report produced by the Johns Hopkins Center for Health Security focused on the role of the public in COVID-19 vaccination (a report that strongly emphasized the importance of community-informed social and behavioral research and interventions in preparing for mass COVID-19 vaccination) (Schoch-Spana et al., 2020). In particular, dialogue-based interventions—which include social mobilization, engagement with community leaders and trusted community representatives (as discussed in Chapters 5 and 6), and other communication across scales—have been highlighted as potentially effective, and they rein-
force the importance of community involvement in creating, adjusting, and implementing these solutions to ensure adequate buy-in and trust (Dubé et al., 2015; Jarrett et al., 2015). The immunization of thought leaders and celebrities could also play a role in compelling members of the public to vaccinate (Freed et al., 2011; Hoffman et al., 2017; Najera, 2019), and overall, vaccine promotion messengers should be trusted, credible, and consistent (Tumpey et al., 2018). Structurally, a COVID-19 vaccine promotion campaign with its expected large scale and impact could look to mimic the success of an example such as the “Truth campaign” against tobacco use in the United States (Farrelly et al., 2009), and could draw on the experience of existing government investment in this area through CDC (including the Vaccinate with Confidence approach) and the National Vaccine Program (CDC, 2019; NVPO and Emory University, 2017).
Approaches such as social marketing and human-centered design can also support vaccine promotion strategies that are community centered and nuanced, such that those most hesitant to be vaccinated or those most vulnerable to severe outcomes from COVID-19 are targeted appropriately (Nowak et al., 2015; Schoch-Spana et al., 2020). Social marketing, which has been used previously to improve coverage and understanding of human papillomavirus vaccination, among other examples, does this through “tactical segmentation” and consideration of both shared demographic and behavioral characteristics and the reasoning behind these characteristics (Nowak et al., 2015). Given that social marketing is end-user driven, the use of such tactics will be critical for reaching potentially skeptical populations, such as communities of color, workers in essential industries, and even health care professionals, who also have been shown to play a critical role in driving vaccination trust and coverage through their own recommendations and communications with patients (Brewer et al., 2017; Dubé et al., 2015; Jarrett et al., 2015; Schoch-Spana et al., 2020). Strategies derived from the fields of behavioral economics and choice architecture could play a role as well.
CONCLUDING REMARKS
Operation Warp Speed has been granted a nearly $10 billion budget to develop one or more safe and effective COVID-19 vaccines, and additional funds will be spent to distribute and deliver a vaccine (HHS, 2020). Ensuring public acceptance of a vaccine is a crucial “last mile” challenge; failing to address vaccine hesitancy or rebuild trust puts the entire investment at risk. Bridging this last mile will require additional resources and significant effort at the national and community levels to ensure that equitable allocation of a COVID-19 vaccine becomes a reality. Operation Warp Speed has been an unprecedented effort to rapidly bring to market a safe and effective
vaccine, and a similarly urgent initiative is needed to speed innovations in social, behavioral, and communication science in order to promote acceptance of that same vaccine.
REFERENCES
Ball, P. 2020. Anti-vaccine movement could undermine efforts to end coronavirus pandemic, researchers warn. Nature. https://www.nature.com/articles/d41586-020-01423-4#ref-CR1 (accessed September 22, 2020).
Bednarczyk, R. A., A. R. King, A. Lahijani, and S. B. Omer. 2019. Current landscape of nonmedical vaccination exemptions in the United States: Impact of policy changes. Expert Review of Vaccines 18(2):175–190. doi: 10.1080/14760584.2019.1562344.
Bogel-Burroughs, N. 2020. Antivaccination activists are growing force at virus protests. The New York Times. https://www.nytimes.com/2020/05/02/us/anti-vaxxers-coronavirus-protests.html (accessed September 22, 2020).
Brewer, N. T., G. B. Chapman, A. J. Rothman, J. Leask, and A. Kempe. 2017. Increasing vaccination: Putting psychological science into action. Psychological Science in the Public Interest 18(3):149–207. doi: 10.1177/1529100618760521.
Broniatowski, D. A., A. M. Jamison, S. Qi, L. AlKulaib, T. Chen, A. Benton, S. C. Quinn, and M. Dredze. 2018. Weaponized health communication: Twitter bots and Russian trolls amplify the vaccine debate. American Journal of Public Health 108(10):1378–1384. doi: 10.2105/AJPH.2018.304567.
Burton, T. M. 2020. FDA to require proof virus vaccine is effective before approving its use. https://www.wsj.com/articles/fda-to-issue-guidance-on-covid-19-vaccine-approval-11593516090?mod=hp_lead_pos3 (accessed September 22, 2020).
Callaghan, T., A. Moghtaderi, J. Lueck, P. Hotez, U. Strych, A. Dor, E. Fowler, and M. Motta. 2020. Correlates and disparities of COVID-19 vaccine hesitancy. SSRN Electronic Journal. doi: 10.2139/ssrn.3667971.
Carpio, M. V. 2004. The lost generation: American Indian women and sterilization abuse. Social Justice 31(4)(98):40–53. http://www.jstor.org/stable/29768273 (accessed September 22, 2020).
CDC (Centers for Disease Control and Prevention). 2019. Vaccinate with confidence. https://www.cdc.gov/vaccines/partners/vaccinate-with-confidence.html (accessed September 15, 2020).
Chastain, D. B., S. P. Osae, A. F. Henao-Martínez, C. Franco-Paredes, J. S. Chastain, and H. N. Young. 2020. Racial disproportionality in covid clinical trials. The New England Journal of Medicine 383(9):e59. doi: 10.1056/NEJMp2021971.
Cohen, E., and D. Vigue. 2020. US government slow to act as anti-vaxxers spread lies on social media about coronavirus vaccine. CNN. https://www.cnn.com/2020/08/12/health/anti-vaxxers-covid-19/index.html (accessed September 22, 2020).
Dubé, E., D. Gagnon, and N. E. MacDonald. 2015. Strategies intended to address vaccine hesitancy: Review of published reviews. Vaccine 33(34):4191–4203. doi: 10.1016/j. vaccine.2015.04.041.
Facher, L. 2020. Amid broad mistrust of FDA and Trump administration, drug companies seek to reassure public about COVID-19 vaccine safety. STAT. https://www.statnews.com/2020/09/08/pharma-pledge-reassure-covid-19-safety (accessed September 22, 2020).
Farrelly, M. C., J. Nonnemaker, K. C. Davis, and A. Hussin. 2009. The influence of the national truth® campaign on smoking initiation. American Journal of Preventive Medicine 36(5):379–384. doi: 10.1016/j.amepre.2009.01.019.
Feuerstein, A., D. Garde, and R. Robbins. 2020. COVID-19 clinical trials are failing to enroll diverse populations, despite awareness efforts. STAT. https://www.statnews.com/2020/08/14/covid-19-clinical-trials-are-are-failing-to-enroll-diverse-populations-despite-awareness-efforts (accessed September 22, 2020).
Fisher, K. A., S. J. Bloomstone, J. Walder, S. Crawford, H. Fouayzi, and K. M. Mazor. 2020. Attitudes toward a potential SARS-CoV-2 vaccine: A survey of U.S. Adults. Annals of Internal Medicine. September 4, 2020, online ahead of print. doi: 10.7326/M20-3569.
Frakt, A. 2020. Bad medicine: The harm that comes from racism. The New York Times, July 8, 2020. https://www.nytimes.com/2020/01/13/upshot/bad-medicine-the-harm-that-comes-from-racism.html (accessed September 22, 2020).
Freed, G. L., S. J. Clark, A. T. Butchart, D. C. Singer, and M. M. Davis. 2011. Sources and perceived credibility of vaccine-safety information for parents. Pediatrics 127(Suppl 1):S107–S112. doi: 10.1542/peds.2010-1722P.
Gamble, V. N. 1997. Under the shadow of Tuskegee: African Americans and health care. American Journal of Public Health 87(11):1773–1778. doi: 10.2105/AJPH.87.11.1773.
Glanz, J. M., S. R. Newcomer, K. J. Narwaney, S. J. Hambidge, M. F. Daley, N. M. Wagner, D. L. McClure, S. Xu, A. Rowhani-Rahbar, G. M. Lee, J. C. Nelson, J. G. Donahue, A. L. Naleway, J. D. Nordin, M. M. Lugg, and E. S. Weintraub. 2013. A population-based cohort study of undervaccination in 8 managed care organizations across the United States. JAMA Pediatrics 167(3):274–281. doi: 10.1001/jamapediatrics.2013.502.
Hall, L. L., L. Xu, S. M. Mahmud, G. A. Puckrein, E. W. Thommes, and A. Chit. 2020. A map of racial and ethnic disparities in influenza vaccine uptake in the medicare fee-for-service program. Advances in Therapy 37(5):2224–2235. doi: 10.1007/s12325-020-01324-y.
Harris, K. M., J. Maurer, and N. Lurie. 2009. Do people who intend to get a flu shot actually get one? Journal of General Internal Medicine 24(12):1311–1313. doi: 10.1007/s11606-009-1126-2.
Harris, K. M., J. Maurer, L. Uscher-Pines, A. Kellermann, and N. Lurie. 2011. Seasonal flu vaccination: Why don’t more Americans get it? RAND Corporation.
HHS (U.S. Department of Health and Human Services). 2020. Fact sheet: Explaining Operation Warp Speed. https://www.hhs.gov/about/news/2020/06/16/fact-sheet-explainingoperation-warp-speed.html (accessed September 22, 2020).
Hoffman, J. 2020. Mistrust of a coronavirus vaccine could imperil widespread immunity. The New York Times, July 18, 2020. https://www.nytimes.com/2020/07/18/health/coronavirus-anti-vaccine.html (accessed September 22, 2020).
Hoffman, S. J., Y. Mansoor, N. Natt, L. Sritharan, J. Belluz, T. Caulfield, Y. Freedhoff, J. N. Lavis, and A. M. Sharma. 2017. Celebrities’ impact on health-related knowledge, attitudes, behaviors, and status outcomes: Protocol for a systematic review, meta-analysis, and meta-regression analysis. Systematic Reviews 6(1):13. doi: 10.1186/s13643-016-0395-1.
Jamison, A. M., D. A. Broniatowski, M. Dredze, Z. Wood-Doughty, D. Khan, and S. C. Quinn. 2020. Vaccine-related advertising in the Facebook ad archive. Vaccine 38(3):512–520. doi: 10.1016/j.vaccine.2019.10.066.
Jarrett, C., R. Wilson, M. O’Leary, E. Eckersberger, and H. J. Larson. 2015. Strategies for addressing vaccine hesitancy—a systematic review. Vaccine 33(34):4180–4190. doi: 10.1016/j.vaccine.2015.04.040.
Johnson, N. F., N. Velásquez, N. J. Restrepo, R. Leahy, N. Gabriel, S. El Oud, M. Zheng, P. Manrique, S. Wuchty, and Y. Lupu. 2020. The online competition between pro- and anti-vaccination views. Nature 582(7811):230–233. doi: 10.1038/s41586-020-2281-1.
Kamisar, B., and M. Holzberg. 2020. Poll: Less than half of Americans say they’ll get a coronavirus vaccine. NBC News. https://www.nbcnews.com/politics/2020-election/poll-less-half-americans-say-they-ll-get-coronavirus-vaccine-n1236971 (accessed September 22, 2020).
Maglione, M. A., L. Das, L. Raaen, A. Smith, R. Chari, S. Newberry, R. Shanman, T. Perry, M. B. Goetz, and C. Gidengil. 2014. Safety of vaccines used for routine immunization of US children: A systematic review. Pediatrics 134(2):325–337. doi: 10.1542/peds.2014-1079.
Mahase, E. 2020. COVID-19: US FDA fires spokesperson over misleading claims about convalescent plasma. BMJ 370:m3400. doi: 10.1136/bmj.m3400.
Mullen O’Keefe, S. 2020. One in three Americans would not get COVID-19 vaccine. Gallup News. https://news.gallup.com/poll/317018/one-three-americans-not-covid-vaccine.aspx (accessed September 22, 2020).
Murphy, J. 2020. What happens if some Americans refuse the COVID-19 vaccine? MDLinx. https://www.mdlinx.com/article/what-happens-if-some-americans-refuse-the-covid-19vaccine/5Yqy3Q84Wt27BQktRnhGnD (accessed September 22, 2020).
Najera, R. F. 2019. Celebrities have influence on vaccination. https://www.historyofvaccines.org/content/blog/vaccine-celebrities (accessed September 21, 2020).
NIH (National Institutes of Health). 2020. The COVID-19 treatment guidelines panel’s statement on the emergency use authorization of convalescent plasma for the treatment of COVID-19. https://www.covid19treatmentguidelines.nih.gov/statement-on-convalescent-plasma-eua (accessed September 22, 2020).
Nowak, G. J., B. G. Gellin, N. E. MacDonald, and R. Butler. 2015. Addressing vaccine hesitancy: The potential value of commercial and social marketing principles and practices. Vaccine 33(34):4204–4211. doi: 10.1016/j.vaccine.2015.04.039.
NVPO (National Vaccine Program Office) and Emory University. 2017. The vaccine confidence meeting: Collaborating to advance vaccine confidence. Meeting report August 15–16, 2017. NVPO. https://www.hhs.gov/sites/default/files/2017-vaccine-confidence-meeting-report.pdf (accessed September 22, 2020).
Olive, J. K., P. J. Hotez, A. Damania, and M. S. Nolan. 2018. The state of the antivaccine movement in the United States: A focused examination of nonmedical exemptions in states and counties. PLOS Medicine 15(6):e1002578. doi: 10.1371/journal. pmed.1002578.
Reich, J. 2020. How anti-vaxxers are thinking about a COVID-19 vaccine. Vox. https://www.vox.com/first-person/2020/7/28/21337621/coronavirus-covid-19-vaccine-anti-vaxxer (accessed September 22, 2020).
Reid, A. E., R. B. Cialdini, and L. S. Aiken. 2011. Social norms and health behavior. In Handbook of behavioral medicine: Methods and applications. New York: Springer Science + Business Media. Pp. 263–274.
Resnick, B. 2020. A third of Americans might refuse a COVID-19 vaccine. How screwed are we? Vox. https://www.vox.com/science-and-health/21364099/covid-19-vaccine-hesitancy-research-herd-immunity (accessed September 22, 2020).
Saint-Victor, D. S., and S. B. Omer. 2013. Vaccine refusal and the endgame: Walking the last mile first. Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences 368(1623):20120148.
Schmid, P., D. Rauber, C. Betsch, G. Lidolt, and M.-L. Denker. 2017. Barriers of influenza vaccination intention and behavior—a systematic review of influenza vaccine hesitancy, 2005–2016. PLOS ONE 12(1):e0170550. doi: 10.1371/journal.pone.0170550.
Schoch-Spana, M., E. Brunson, R. Long, S. Ravi, A. Ruth, and M. Trotochaud. 2020. The public’s role in COVID-19 vaccination: Planning recommendations informed by design thinking and the social, behavioral, and communication sciences. Baltimore, MD: Johns Hopkins Bloomberg School of Public Health Center for Health Security.
Silverman, E. 2020. Poll: Most Americans believe the COVID-19 vaccine approval process is driven by politics, not science. STAT News. https://www.statnews.com/pharmalot/2020/08/31/most-americans-believe-the-covid-19-vaccine-approval-process-is-driven-by-politics-not-science (accessed September 22, 2020).
Thigpen, C. L., and C. Funk. 2020. Most Americans expect a COVID-19 vaccine within a year; 72% say they would get vaccinated. Pew Research Center Fact Tank. https://www.pewresearch.org/fact-tank/2020/05/21/most-americans-expect-a-covid-19-vaccine-within-a-year-72-say-they-would-get-vaccinated (accessed September 22, 2020).
Tumpey, A. J., D. Daigle, and G. Nowak. 2018. Communicating during an outbreak or public health investigation. Atlanta, GA: CDC.
University of Wisconsin. 2018. Sterilization of Puerto Rican women: A selected, partially annotated bibliography (Louis de Malave, 1999). https://www.library.wisc.edu/gwslibrarian/bibliographies/sterilization (accessed September 22, 2020).
Wang, E., J. Clymer, C. Davis-Hayes, and A. Buttenheim. 2014. Nonmedical exemptions from school immunization requirements: A systematic review. American Journal of Public Health 104(11):e62–e84. doi: 10.2105/AJPH.2014.302190.
WHO (World Health Organization). 2019. Ten threats to global health in 2019. https://www.who.int/vietnam/news/feature-stories/detail/ten-threats-to-global-health-in-2019 (accessed September 22, 2020).
WHO. 2020. Improving vaccination demand and addressing hesitancy. https://www.who.int/immunization/programmes_systems/vaccine_hesitancy/en/#:~:text=In%20November%202018%2C%20a%20global,be%20finalized%20in%20late%202020 (accessed September 22, 2020).
Williams, W. W., P. J. Lu, A. O’Halloran, D. K. Kim, L. A. Grohskopf, T. Pilishvili, T. H. Skoff, N. P. Nelson, R. Harpaz, L. E. Markowitz, A. Rodriguez-Lainz, and A. P. Fiebelkorn. 2017. Surveillance of vaccination coverage among adult populations—United States, 2015. Morbidity and Mortality Weekly Report Surveillance Summaries 66(11):1–28. doi: 10.15585/mmwr.ss6611a1.
Zipprich, J., K. Winter, J. Hacker, D. Xia, J. Watt, and K. Harriman. 2015. Measles outbreak—California, December 2014–February 2015. Morbidity and Mortality Weekly Report 64(06):153–154.
This page intentionally left blank.
















