Summary
Hospital-based emergency and trauma care is critically important to the health and well-being of Americans. In 2003, nearly 114 million visits were made to hospital emergency departments (EDs)—more than one for every three people in the United States. About one-quarter of those visits were due to unintentional injuries, the leading cause of death for people aged 1 through 44. While most Americans encounter the ED only rarely, they count on it to be there when they need it.
Over the last several decades, the role of hospital-based emergency and trauma care has evolved. EDs continue to focus on their traditional mission of providing urgent and lifesaving care, but have taken on additional responsibilities to meet the needs of communities, providers, and patients. Today, their complex role also encompasses safety net care for uninsured patients, public health surveillance, disaster preparedness, and serving as an adjunct to community physician practices. In some rural communities, the hospital ED may be the main source of health care for a widely dispersed population. While the demands on emergency and trauma care have grown dramatically, however, the capacity of the system has not kept pace. Balancing these roles in the face of increasing patient volume and limited resources has become increasingly challenging. The situation is creating a widening gap between the quality of emergency care Americans expect and the quality they actually receive.
STUDY CHARGE
The Institute of Medicine’s (IOM) Committee on the Future of Emergency Care in the United States Health System was formed in September
2003 to examine the emergency care system in the United States; explore its strengths, limitations, and future challenges; describe a desired vision of the system; and recommend strategies for achieving that vision. The committee was also tasked with taking a focused look at the state of pediatric emergency care, prehospital emergency care, and hospital-based emergency and trauma care. This is the third of three reports presenting the committee’s findings and recommendations in these three areas. Summarized below are the committee’s findings and recommendations for meeting the challenge of high demand for emergency care and achieving the vision of a 21st-century emergency care system.
THE CHALLENGE OF HIGH DEMAND AND INADEQUATE SYSTEM CAPACITY
Between 1993 and 2003, the population of the United States grew by 12 percent, hospital admissions increased by 13 percent, and ED visits rose by more than 2 million per year from 90.3 to 113.9 million—a 26 percent increase (see Figure ES-1). Not only is ED volume increasing, but patients coming to the ED are older and sicker and require more complex and time-consuming workups and treatments. Moreover, during this same period, the United States experienced a net loss of 703 hospitals, 198,000 hospital beds, and 425 hospital EDs, mainly in response to cost-cutting measures
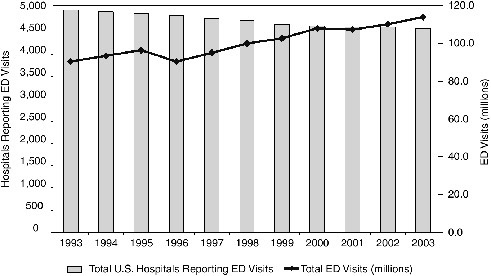
FIGURE ES-1 Hospital emergency departments versus numbers of visits.
SOURCE: AHA, 2005b; McCaig and Burt, 2005.
and lower reimbursements by managed care, Medicare, and other payers. By 2001, 60 percent of hospitals were operating at or over capacity.
The high demand for hospital-based emergency and trauma care reflects several trends. First, EDs have become one of the nation’s principal sources of care for patients with limited access to other providers, including the 45 million uninsured Americans. Indeed, the Emergency Medical Treatment and Active Labor Act of 1986 prevents hospitals from restricting access for uninsured patients by requiring hospitals to provide a medical screening examination to all patients and to stabilize or transfer patients as needed. With limited access to community-based primary and specialty care, many turn to the emergency system when in medical need, often for conditions that have worsened because of a lack of regular primary care.
Medicaid beneficiaries also turn to the ED. In fact, Medicaid enrollees visit the ED at a higher rate than any other category of patient (81 visits per 100 enrollees)—double the rate of the uninsured population and nearly four times that of privately insured patients. Although Medicaid enrollees are insured, the low rates of provider reimbursement in many states limit the number of office-based practitioners who are willing to accept them as patients.
In addition, the ED often serves as primary care provider, a role for which it is not optimally designed. Rather, the ED is designed for rapid, high-intensity responses to acute injuries and illnesses. Physicians in the ED face constant interruptions and distractions, and typically lack access to the patient’s full medical records. Because nonemergency patients are usually low triage priorities, they often experience extremely long wait times as they are passed over for more urgent cases.
Costs are another concern. When an ED is not busy, the cost of treating an additional nonemergency patient is probably quite low. But while the literature on this issue is mixed, a number of studies suggest that nonemergency care in the ED is more costly than that in alternative settings. Indeed, ED charges for minor problems have been estimated to be two to five times higher than those of a typical office visit. When the ED is at full capacity, treating additional patients who could be cared for in a different environment means fewer resources—physicians, nurses, ancillary personnel, equipment, and time and space—available to respond to emergency cases.
By law, the front door of the ED is always open. When a hospital’s inpatient beds are full, as is frequently the case, ED providers cannot transfer the most severely ill and injured patients to an inpatient unit. As a result, ED patients who require hospitalization begin to back up in the ED. The aggregate result of this imbalance between public demand and hospital capacity is an epidemic of overcrowded EDs, frequent “boarding” of patients waiting for inpatient beds, and ambulance diversion:
-
Overcrowding—ED overcrowding is a nationwide phenomenon, affecting rural and urban areas alike. In one study, 91 percent of EDs responding to a national survey reported overcrowding as a problem; almost 40 percent reported that overcrowding occurred daily. Overcrowding induces stress in providers and patients, and can lead to errors and impaired overall quality of care.
-
Boarding—A consequence of crowded EDs is the practice of boarding—holding a patient who needs to be admitted in the ED until an inpatient bed becomes available. It is not unusual for patients in a busy hospital ED to be boarded for 48 hours or more. In a nationwide survey of nearly 90 EDs across the country, conducted on a typical Monday evening, 73 percent of hospitals reported boarding two or more patients. Boarding not only compromises the patient’s hospital experience, but also adds to an already stressful work environment for physicians and nurses and enhances the potential for errors, delays in treatment, and diminished quality of care.
-
Ambulance diversion—Another consequence of crowding is ambulance diversion—when EDs become saturated to the point that patient safety is compromised, ambulances are diverted to alternative hospitals. Once a safety valve to be used in extreme situations, this has now become a commonplace event. A recent study reported that 501,000 ambulances were diverted in 2003, an average of 1 per minute. According to the American Hospital Association, nearly half of all hospitals, and close to 70 percent of urban hospitals, reported time on diversion in 2004. Ambulance diversion can lead to catastrophic delays in treatment for seriously ill or injured patients. It also frequently leads to treatment in facilities with inadequate expertise and resources appropriate to the patient’s severity of illness, placing the patient at significant risk.
FINDINGS AND RECOMMENDATIONS
This section presents the committee’s key findings and recommendations for meeting the challenge of increased demand and inadequate capacity and improving the quality of hospital-based emergency and trauma care. These findings and recommendations address the need to enhance operational efficiency, the use of information technology, the burden of uncompensated care, inadequate disaster preparedness, the emergency care workforce, and the need for research in emergency care.
Enhanced Operational Efficiency
Hospital EDs and trauma centers have little control over external forces that contribute to crowding, such as increasing numbers of uninsured or the growing severity of patients’ conditions. There is, however, a great deal
they can do to manage the impact of these forces. Innovations in industrial engineering that have swept through other sectors of the economy, from banking to air travel to manufacturing, have failed to take hold in health care delivery—a sector of the economy that now consumes 16 percent of the nation’s gross domestic product and is growing at twice the rate of inflation.
Tools derived from engineering and operations research have been directed successfully at the problem of hospital efficiency in general and ED crowding in particular. A wide range of tools have been developed and tested for addressing patient flow—defined as the movement of patients through the hospital system—generally with good success. Efficient patient flow can increase the volume of patients treated and discharged and minimize delays at each point in the delivery process while improving the quality of care. For example, while controlled studies have yet to be conducted, a growing body of experience suggests that using queuing theory to smooth the peaks and valleys of patient admissions can eliminate bottlenecks, reduce crowding, improve patient care, and reduce costs. The committee recommends that hospital chief executive officers adopt enterprisewide operations management and related strategies to improve the quality and efficiency of emergency care (4.2).1
A particularly promising technique for managing patient flow is the use of clinical decision units (CDUs), also known as observation units. The technique was developed as a means of monitoring patients with chest pain who had a low to intermediate probability of acute myocardial infarction (AMI). By observing patients for up to 23 hours, ED staff were able to rule out many patients at risk of AMI while using fewer resources than would have been consumed if these same patients had been admitted to the intensive care unit (ICU) or an inpatient telemetry unit. Today, the Centers for Medicare and Medicaid Services (CMS) reimburses CDU stays for only three conditions: chest pain, asthma, and congestive heart failure. Because of the demonstrated success of CDUs, the committee recommends that the Centers for Medicare and Medicaid Services remove current restrictions on the medical conditions that are eligible for separate clinical decision unit payment (4.1).
Incentives to Reduce Crowding and Boarding
While hospitals can use many approaches to reduce crowding and boarding, there are limited financial incentives for them to do so. Hospitals
|
1 |
The committee’s recommendations are numbered according to the chapter of the main report in which they appear. Thus, for example, recommendation 2.1 is the first recommendation in Chapter 2. |
are not reimbursed for differences in costs that are often associated with admissions from the ED. Further, hospitals do not face significant negative financial consequences for operating crowded EDs. In 2004, following a July 2002 alert that tied treatment delays to more than 50 hospital deaths, the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) instituted new guidelines that would have required accredited hospitals to take serious steps to reduce crowding, boarding, and diversion. Under industry pressure, however, these requirements were withdrawn and replaced with a weaker standard. The committee recommends that the Joint Commission on Accreditation of Healthcare Organizations reinstate strong standards designed to sharply reduce and ultimately eliminate emergency department crowding, boarding, and diversion (4.4). Furthermore, because the practices of boarding and diversion are so antithetical to quality medical care, the strongest possible measures should be taken to eliminate them. The committee recommends that hospitals end the practices of boarding patients in the emergency department and ambulance diversion, except in the most extreme cases, such as a community mass casualty event. The Centers for Medicare and Medicaid Services should convene a working group that includes experts in emergency care, inpatient critical care, hospital operations management, nursing, and other relevant disciplines to develop boarding and diversion standards, as well as guidelines, measures, and incentives for implementation, monitoring, and enforcement of these standards (4.5).
Leadership in Improving Hospital Efficiency
Beyond the use of incentives, the committee looks to hospital executives, including both chief executive officers (CEOs) and midlevel managers, to provide visionary leadership in promoting the use of patient flow and operations management approaches to improve hospital efficiency. Hospital leaders should be open to learning from the experiences of industries outside of health care, and should be bold and creative in applying these and other new ideas. To foster the development of hospital leadership in improving hospital efficiency, the committee recommends that training in operations management and related approaches be promoted by professional associations; accrediting organizations, such as the Joint Commission on Accreditation of Healthcare Organizations and the National Committee for Quality Assurance; and educational institutions that provide training in clinical, health care management, and public health disciplines (4.3).
Use of Information Technology
Opportunities to improve patient flow, operational efficiency, and quality of care can be enhanced by appropriate information technologies.
Hospitals, however, lag behind other industries in the use of information technologies, particularly those used to support process management.
Information technologies have broad application to hospitals and health systems, but their use involves unique needs and approaches in emergency care. Information is critically important for rapid decision making in emergency and trauma care. But emergency physicians are all too often deprived of critical patient information; indeed, it has been said that EDs operate on information “fumes.” The following information technologies could significantly enhance emergency care: (1) dashboard systems that track and coordinate patient flow, (2) communications systems that enable ED physicians to link to patients’ records or providers, (3) clinical decision-support programs that improve decision making, (4) documentation systems for collecting and storing patient data, (5) computerized training and information retrieval, and (6) systems to facilitate public health surveillance. Given their demonstrated effectiveness in the emergency care setting, the committee recommends that hospitals adopt robust information and communications systems to improve the safety and quality of emergency care and enhance hospital efficiency (5.1). The committee recognizes that the appropriate prioritization of and investment in these approaches will vary based on each institution’s resources and needs.
The Burden of Uncompensated Care
In most hospitals, if reimbursements fail to cover ED and trauma costs, these costs are subsidized by admissions that originate in the ED. But uncompensated care can be an extreme burden at hospitals that have large numbers of uninsured patients. Many hospital ED and trauma center closures are attributed to financial losses associated with emergency and trauma care. Public hospitals and tertiary medical centers bear a large share of this burden, as surrounding community hospitals often transfer their most complex, high-risk patients to the large safety net hospitals for specialized care. Often, the condition of these patients has deteriorated considerably since their arrival at the referring hospital. Hospitals receive Disproportionate Share Hospital (DSH) payments from both Medicare and Medicaid to compensate for these losses, but these payments are inadequate for hospitals with large safety net populations. As a result, the emergency and trauma care safety net system is at risk in many regions. To ensure the continued viability of a critical public safety function, the committee recommends that Congress establish dedicated funding, separate from Disproportionate Share Hospital payments, to reimburse hospitals that provide significant amounts of uncompensated emergency and trauma care for the financial losses incurred by providing those services (2.1).
The committee believes that accurate determination of the optimal
amount of funding to allocate for this purpose, which could run into the hundreds of millions of dollars, is beyond its expertise, but that the government must begin to address this issue immediately. The committee therefore recommends that Congress initially appropriate $50 million for the purpose, to be administered by the Centers for Medicare and Medicaid Services (2.1a). The Centers for Medicare and Medicaid Services should establish a working group to determine the allocation of these funds, which should be targeted to providers and localities at greatest risk; the working group should then determine funding needs for subsequent years (2.1b).
Inadequate Disaster Preparedness
On September 10, 2001, the cover story of U.S. News and World Report described an emergency care system in critical condition as a result of demands far in excess of its capacity. While the article focused on the day-to-day problems of diversion and boarding, the events of the following day brought home a frightening realization to many: If we cannot take care of our emergency patients on a normal day, how will we manage a large-scale disaster? More than 4 years after the terrorist attacks of 2001, Hurricane Katrina revealed how far we have is to go in this regard. While Katrina was unusual in its size and scope, the capacity of the emergency care system to respond effectively even to smaller disasters is very much in question.
Surge Capacity
Hospitals in many large cities are operating at or near full capacity. A multiple-car highway crash can create havoc in an ED. Few hospitals have the capacity to handle a major mass casualty event. One reason for this lack of capacity is the small amount of funding for bioterrorism and other emergency threats that has gone directly to hospitals. For example, hospital grants from the Health Resources and Services Administration’s Bioterrorism Hospital Preparedness Program in 2002 were typically between $5,000 and $10,000—insufficient to equip even one critical care room.
Training
Training for ED workers in disaster preparedness is also deficient. In 2003, hospital training varied widely among staff: 92 percent of hospitals trained their nursing staff in responding to at least one type of threat, but residents and interns received any such training at only 49 percent of hospitals (although this represented an improvement over the situation prior to the terrorist attacks of 2001).
Protection of Hospitals and Staff
Protecting hospitals and their staff from biological or chemical events poses extraordinary challenges. The outbreak of severe acute respiratory syndrome (SARS) in Toronto in 2003 revealed the difficulties associated with containing even a small outbreak—particularly when health professionals themselves become both victims and spreaders of disease. One of the most important tools in such an event is negative pressure rooms that prevent the spread of airborne pathogens. Unfortunately, the number of such rooms is limited, and they are generally restricted to a handful of tertiary hospitals in each major population center. The committee believes that this lack of adequate negative pressure suites is a critical vulnerability of the current system, and that the existing capacity could be quickly overwhelmed by either a terrorist event or a major outbreak of avian influenza or some other airborne disease, posing an extreme danger to hospital workers and patients.
Staff must also be protected through appropriate personal protective equipment. Current training and equipment in this regard are inadequate. In 2005, the Occupational Safety and Health Administration developed guidelines for use of personal protective equipment, but more needs to be done.
Approaches to Improve Disaster Preparedness
To address the above concerns about surge capacity, training, and protection of hospitals and staff, the committee recommends that Congress significantly increase total preparedness funding in fiscal year 2007 for hospital emergency preparedness in the following areas: strengthening and sustaining trauma care systems; enhancing emergency department, trauma center, and inpatient surge capacity; improving emergency medical services’ response to explosives; designing evidence-based training programs; enhancing the availability of decontamination showers, standby intensive care unit capacity, negative pressure rooms, and appropriate personal protective equipment; and conducting international collaborative research on the civilian consequences of conventional weapons terrorism (7.3).
In addition, to further address the need for competency in disaster medicine across disciplines, the committee recommends that all institutions responsible for the training, continuing education, and credentialing and certification of professionals involved in emergency care (including medicine, nursing, emergency medical services, allied health, public health, and hospital administration) incorporate disaster preparedness training into their curricula and competency criteria (7.2).
The Emergency Care Workforce
Emergency care is delivered in an inherently challenging environment, often requiring providers to make life-and-death decisions with little time and information. Emergency care providers wage battles on many fronts, including scheduling diagnostic tests; obtaining timely laboratory results and drugs; getting patients admitted to the hospital; finding specialists willing to come in during the middle of the night; and finding psychiatric centers, skilled nursing facilities, or specialists who are willing to accept referrals. ED staff often confront violence and deal with an array of social problems that confound their attempts to heal their patients. As a result, providers on the front lines of emergency care are increasingly exhausted, stressed out, and frustrated by the deteriorating state of emergency care and the safety net it supports.
On-Call Specialists
One of the most troubling trends is the increasing difficulty of finding specialists to take emergency call. Providing emergency call has become unattractive to many specialists in critical fields such as neurosurgery and orthopedics. Specialists have difficulty collecting payment for on-call services, in part because many emergency and trauma patients are uninsured; nearly 80 percent of specialists in one survey had difficulty obtaining payment for such services. Liability concerns also discourage many specialists from taking emergency call. Procedures performed on emergency patients are inherently risky and expose specialists to an increased likelihood of litigation. Patients are often sicker, and emergency procedures are frequently performed in the middle of the night or on weekends, when the hospital’s staffing and capabilities are not at their peak. A national survey of neurosurgeons found that 36 percent had been sued by patients seen through the ED. These factors drive premiums for physicians who take emergency call well above those for physicians who do not. The problem has been exacerbated by recently revised guidelines under the Emergency Medical Treatment and Active Labor Act that make it easier for on-call physicians to limit their emergency practices.
Hospitals are using a number of different strategies to stabilize the services of on-call physicians. One promising approach is to regionalize the services of certain on-call specialties so that every hospital need not maintain on-call services for every specialty. Such regionalization would rationalize the limited supply of specialists by ensuring coverage at key tertiary and secondary locations based on actual need, replacing the current haphazard approach that is based on many factors other than need. For example, one county is developing a communitywide cooperative that will contract collec-
tively for the services of certain specialists. The committee recommends that hospitals, physician organizations, and public health agencies collaborate to regionalize critical specialty care on-call services (6.1).
Exposure of Emergency Providers to Medical Malpractice Claims
As noted above, physicians providing emergency and trauma care face extraordinary exposure to medical malpractice claims—far greater than those not providing such care. Safety net providers are especially affected by the liability problem: as on-call panels diminish at community hospitals, these hospitals increasingly export their sickest patients to the large safety net hospitals, which have no choice but to accept them. The result is even higher concentrations of uninsured, high-risk patients. Protections must be instituted so that emergency providers and EDs do not become the dumping ground for the liability crisis. Although the public is largely unaware of the situation, this crisis has already seriously eroded the capacity of emergency and trauma care across many cities. Therefore, the committee recommends that Congress appoint a commission to examine the impact of medical malpractice lawsuits on the declining availability of providers in high-risk emergency and trauma care specialties, and to recommend appropriate state and federal actions to mitigate the adverse impact of these lawsuits and ensure quality of care (6.2).
The Rural Workforce
Rural EDs face persistent shortages of emergency and trauma physicians, as well as on-call specialists. With such shortages likely to continue, it is important to find alternative ways of enhancing emergency services in rural areas. One approach is to increase collaboration between rural hospitals and regional academic health centers to foster training, resource sharing, and coordination of care. The committee recommends that states link rural hospitals with academic health centers to enhance opportunities for professional consultation, telemedicine, patient referral and transport, and continuing professional education (6.6).
Need for Emergency Care Research
Although emergency medicine and trauma surgery are relatively young specialties, researchers have made important contributions to both basic science and clinical practice that have dramatically improved emergency care and have resulted in significant advances in general medicine. Examples are assessment and management of cardiac arrest, including the development and refinement of guidelines for cardiopulmonary resuscitation (CPR), the
pharmacology of resuscitation, understanding and treatment of hemorrhagic shock, and electrocardiogram (EKG) analysis of ventricular fibrillation. Because emergency care and trauma care are young fields, however, they are not strongly represented in the political infrastructure of the National Institutes of Health (NIH), its various institutes, and its study sections. As a result, scant resources are allocated to advance the science of such care, and few training grants are offered to develop researchers who want to focus on emergency care. For example, only .05 percent of NIH training grants awarded to medical schools goes to departments of emergency medicine—an average of only $51.66 per graduating resident. In contrast, internal medicine receives approximately $5,000.00 per graduating resident.
The current uncoordinated approach to organizing and funding emergency and trauma care has been inadequate. There are well-defined emergency and trauma care research questions that would benefit from a coordinated and well-funded research strategy. Therefore, the committee recommends that the Secretary of the Department of Health and Human Services conduct a study to examine the gaps and opportunities in emergency and trauma care research, and recommend a strategy for the optimal organization and funding of the research effort (8.2).
This study should include consideration of training of new investigators, development of multicenter research networks, funding of General Clinical Research Centers that specifically include an emergency and trauma care component, involvement of emergency and trauma care researchers in the grant review and research advisory processes, and improved research coordination through a dedicated center or institute (8.2a).
Congress and federal agencies involved in emergency and trauma care research (including the Department of Transportation, the Department of Health and Human Services, the Department of Homeland Security, and the Department of Defense) should implement the study’s recommendations (8.2b).
ACHIEVING THE VISION OF A 21ST-CENTURY EMERGENCY CARE SYSTEM
Hospital-based emergency and trauma care is part of an interdependent system of emergency services; thus optimizing such care requires improvements in both hospital-based care and the larger system. To that end, the committee developed a vision for the future of emergency care that centers around three goals: coordination, regionalization, and accountability. Many elements of this vision have been advocated previously; however, progress toward achieving these elements has been derailed by deeply entrenched
parochial interests and cultural attitudes, as well as funding cutbacks and practical impediments to change. Concerted, cooperative efforts at all levels of government—federal, state, regional, local—and the private sector are necessary to finally break through and achieve this vision.
Coordination
One of the most long-standing problems with the emergency care system is that services are fragmented. Prehospital emergency medical services (EMS), hospitals, trauma centers, and public health have traditionally worked in silos. For example, public safety and EMS agencies often lack common radio frequencies and protocols for communicating with each other during emergencies. Similarly, emergency care providers lack access to patient medical histories that could be useful in decision making.
Ensuring that each patient is directed to the most appropriate setting, including a level I trauma center when necessary, requires that many elements within the regional system—community hospitals, trauma centers, and particularly prehospital EMS—coordinate the regional flow of patients effectively. In addition to improving patient care, coordinating the regional flow of patients is a critical tool in reducing overcrowding in EDs.
Unfortunately, only a handful of systems around the country coordinate transport effectively at the regional level. Short of formally instituting diversion, there is typically little information sharing between hospitals and EMS regarding overloaded EDs and trauma centers and the availability of ED beds, operating suites, equipment, trauma surgeons, and critical specialists—information that could be used to balance the load among EDs and trauma centers regionwide. Too often a hospital’s location places it in a logistical situation in which it is overloaded with emergencies and trauma cases while an ED several blocks away may be working at a comfortable 50 percent capacity. There is little incentive for ambulances to drive by a hospital to take patients to a facility that is less crowded.
The benefits to patients of better regional coordination have been demonstrated. The technologies needed to facilitate such coordination exist, and police and fire departments are ahead in this regard. The main impediment appears to be entrenched interests and a lack of vision to motivate change in the current system.
The committee envisions a system in which all patients receive well-planned and coordinated emergency care services. Dispatch, EMS, ED providers, public safety, and public health should be fully interconnected and united in an effort to ensure that each patient receives the most appropriate care, at the optimal location, with the minimum delay. From the standpoint of patients, delivery of emergency care services should be seamless.
Regionalization
Because not all hospitals within a community have the personnel and resources to support the delivery of high-level emergency care, critically ill and injured patients should be directed specifically to those facilities with such capabilities. That is the goal of regionalization. There is substantial evidence that the use of regionalization of services to direct such patients to designated hospitals with greater experience and resources improves outcomes and reduces costs across a range of high-risk conditions and procedures. Thus the committee supports further regionalization of emergency care services. However, use of this approach requires that prehospital providers, as well as patients and caregivers, be clear on which facilities have the necessary resources. Just as trauma centers are categorized according to their capabilities (i.e., level I–level IV/V), a standard national approach to the categorization of EDs that reflects their capabilities is needed so the categories will be clearly understood by providers and the public across all states and regions of the country. To that end, the committee recommends that the Department of Health and Human Services and the National Highway Traffic Safety Administration, in partnership with professional organizations, convene a panel of individuals with multidisciplinary expertise to develop an evidence-based categorization system for emergency medical services, emergency departments, and trauma centers based on adult and pediatric service capabilities (3.1).
This information, in turn, could be used to develop protocols that would guide EMS providers in the transport of patients and improve the regional coordination of patient flow. These protocols should be based on current and emerging evidence about the appropriate models for transport given the patient’s condition and location, and should include protocols that, given appropriate information about the status of facilities, direct patients to less crowded local EDs rather than to the highest-level center. Therefore, the committee also recommends that the National Highway Traffic Safety Administration, in partnership with professional organizations, convene a panel of individuals with multidisciplinary expertise to develop evidence-based model prehospital care protocols for the treatment, triage, and transport of patients (3.2).
Accountability
Without accountability, participants in the emergency care system need not accept responsibility for failures and can avoid making changes to improve the delivery of care. Accountability has failed to take hold in emergency care to date because responsibility is dispersed across many different components of the system, so it is difficult even for policy makers to
determine where system breakdowns occur and how they can subsequently be addressed.
To build accountability into the system, the committee recommends that the Department of Health and Human Services convene a panel of individuals with emergency and trauma care expertise to develop evidence-based indicators of emergency and trauma care system performance (3.3). Because of the need for an independent, national process with the broad participation of every component of emergency care, the federal government should play a lead role in promoting and funding the development of these performance indicators. The indicators developed should include structure and process measures, but evolve toward outcome measures over time. These performance measures should be nationally standardized so that statewide and national comparisons can be made. Measures should evaluate the performance of individual providers within the system, as well as that of the system as a whole. Measures should also be sensitive to the interdependence among the components of the system; for example, EMS response times may be related to EDs going on diversion.
Using the measures developed through such a national, evidence-based, multidisciplinary effort, performance data should be collected at regular intervals from all hospitals and EMS agencies in a community. Public dissemination of performance data is crucial to driving the needed changes in the delivery of emergency care services. Dissemination could take various forms, including public report cards, annual reports, and state public health reports. Because of the potential sensitivity of performance data, the data should initially be reported in the aggregate rather than at the level of the individual provider. Individual providers should have full access to their own data so they can understand and improve their performance, as well as contribute to the overall system. Over time, individual provider information should become an important part of the public information on the system. These performance measures should ultimately become the basis for pay-for-performance initiatives as those reimbursement techniques mature.
Achieving the Vision
States and regions face a variety of different situations, including the level of development of trauma systems; the effectiveness of state EMS offices and regional EMS councils; and the degree of coordination among fire departments, EMS, hospitals, trauma centers, and emergency management. Thus no single approach to enhancing emergency care systems will achieve the goals outlined above. A number of different avenues should be explored and evaluated to determine what types of systems are best able to achieve the three goals. The committee therefore recommends that Congress establish a demonstration program, administered by the Health Resources
and Services Administration, to promote coordinated, regionalized, and accountable emergency care systems throughout the country, and appropriate $88 million over 5 years to this program (3.5). Grants should be targeted at states, which could develop projects at the state, regional, or local level; cross-state collaborative proposals would also be encouraged. Over time, and over a number of controlled initiatives, such a process should lead to important insights about what strategies work under different conditions. These insights would provide best-practice models that could be widely adopted to advance the nation toward the committee’s vision for efficient, high-quality emergency and trauma care.
Supporting System Integration
Reducing fragmentation at the state and local levels will require federal leadership and support. Today, however, the federal agencies that support and regulate emergency services mirror the fragmentation of emergency services at the state and local levels. Prehospital EMS, hospital-based emergency care, trauma care, injury prevention and control, and medical disaster preparedness are scattered across numerous agencies within the Department of Health and Human Services, the U.S. Department of Transportation, and the Department of Homeland Security.
Strong federal leadership for emergency and trauma care is at the heart of the committee’s vision for the future, and continued fragmentation of responsibility at the federal level is unacceptable. A lead federal agency could better move the emergency and trauma care system toward improved integration; unify decision making, including funding decisions; and represent all emergency and trauma care patients, providers, and settings, including prehospital EMS (both ground and air), hospital-based emergency and trauma care, pediatric emergency and trauma care, rural emergency and trauma care, and medical disaster preparedness. The committee therefore recommends that Congress establish a lead agency for emergency and trauma care within 2 years of this report. The lead agency should be housed in the Department of Health and Human Services, and should have primary programmatic responsibility for the full continuum of emergency medical services and emergency and trauma care for adults and children, including medical 9-1-1 and emergency medical dispatch, prehospital emergency medical services (both ground and air), hospital-based emergency and trauma care, and medical-related disaster preparedness. Congress should establish a working group to make recommendations regarding the structure, funding, and responsibilities of the new agency, and develop and monitor the transition. The working group should have representation from federal and state agencies and professional disciplines involved in emergency and trauma care (3.6).
















