7
Disaster Preparedness
The day before September 11, 2001, the cover story of U.S. News and World Report described an emergency care system in critical condition as a result of demand far in excess of its capacity (Shute and Marcus, 2001; see Figure 7-1). While the article focused on the day-to-day problems of diversion and boarding, the events of the following day brought home a frightening realization to many. If we cannot take care of our emergency patients on a normal day, how will we manage a large-scale disaster? Federal, state, and local government entities have since realized the importance of hospitals, particularly emergency departments (EDs), in planning for such events, and significant progress has been made on integrating inpatient resources into planning for disasters (Schur, 2004). More than 4 years after September 11, however, Hurricane Katrina revealed how far we have to go in this regard. While Katrina was unusual in its size and scope, the capacity of the emergency care system to respond effectively even to smaller disasters is still in question (GAO, 2003a).
Disaster response involves many different community resources—from police and fire to medical providers, structural and environmental engineers, and transportation and housing experts. The hospital plays a small but crucial role in this larger picture. It is the epicenter of medical care delivered to those who are injured. Running a hospital is an enormously complex task under the best of circumstances; preparing a hospital for a disaster is infinitely more complicated. Planning for disasters involves a range of difficult questions: For what types of disaster events should hospitals prepare? Should every hospital prepare for disasters, or should medical response be regionalized? When does “busy” rise to the level of disaster, who makes that

FIGURE 7-1 U.S. News and World Report, cover story on September 10, 2001.
SOURCE: Reprinted from Shute and Marcus, 2001, with permission.
decision, and how does a large, complex organization shift from routine to disaster mode? How does a hospital protect itself and its staff from chemical or biological agents when patients are contaminated?
This chapter examines these and other questions, and considers the current level of hospital disaster preparedness. It also explores the special problems associated with rural hospitals, and presents the committee’s recommendations for enhancing hospital preparedness.
DEFINING DISASTER
The term “disaster” denotes a low-probability but high-impact event that causes a large number of individuals to become ill or injured. The In-
ternational Federation of Red Cross and Red Crescent Societies defines a disaster as an event that causes more than 10 deaths, affects more than 100 people, or leads to an appeal for assistance by those affected (Bravata et al., 2004b). This report expands that definition in the context of hospital-based emergency and trauma care to include any event that creates a significant, short-term spike in the demand for emergency care services that requires extraordinary measures to address adequately.
Disasters can range from large multiple-vehicle crashes to massive events such as the North Ridge earthquake, Hurricane Katrina, and the terrorist attacks of September 11. Disasters can be natural, such as earthquakes, floods, and disease outbreaks; or they can be man-made, such as transportation incidents, terrorist bombings, and biological or chemical attacks. The federal government has grouped terrorist threats into five categories—chemical, biological, radiological, nuclear, and explosive (CBRNE)—which are also useful for classifying general threats (see Box 7-1).
Each type of threat presents different challenges to hospitals, which must able to respond to each in some capacity. Given finite resources, however, hospitals must attempt to focus their resources on the most likely and potentially serious scenarios. Bombings are the most common form of terrorist attack (Frykberg, 2004). They often result in the worst forms of both blunt and penetrating trauma in addition to burns, as shown by recent experience; examples include the train and subway attacks in Madrid (Gutierrez de Ceballos et al., 2004) and London, Oklahoma City bombing (Teague, 2004), and the Atlanta Centennial Olympics bombing (Feliciano et al., 1998). Worldwide, there were more than 500 terrorist bombings between 2001 and 2003, resulting in 4,600 deaths (U.S. Department of State, 2005a,b,c). Over the past 25 years, few acts of global terrorism have involved the use of chemical or biological agents. In contrast, explosives and/or firearms have been used to commit countless acts of terrorism in Israel, Egypt, Kenya, Argentina, Colombia, Bali, Yemen, Russia, the United Kingdom, Germany, France, Italy, and many other countries. The possibility of bioterrorism or a nuclear attack is also real, however, and the impact of such incidents on public health would be catastrophic.
To some degree, each region must prioritize its response preparedness according to the likelihood of the different types of events it could face. Thus New York City should probably spend more resources than Topeka, Kansas, on preparation for biological or nuclear attack; Topeka, on the other hand, should focus more of its preparedness efforts on tornados. The scope of various types of disasters is illustrated by selected recent events, which are summarized in Table 7-1.
The federal government has promoted the idea of preparing for “all hazards.” But federal disaster planning has paid much more attention to biological and chemical threats than to explosive attacks by terrorists or,
|
BOX 7-1 Classification of Terrorist Threats The federal government groups terrorist threats into five categories— chemical, biological, radiological, nuclear, and explosive—commonly referred to as CBRNE. Each type of threat has unique characteristics and medical impacts:
|
until Hurricane Katrina, to natural disasters (Arkin, 2005). Of the 15 National Planning Scenarios introduced by the Department of Homeland Security (DHS) to guide disaster preparation efforts, only two involve natural disasters and only one an attack using explosives (see Box 7-2). Following Hurricane Katrina, however, DHS altered the selection process for its Urban Area Security Initiatives grants to ensure that the program would place as much weight on cities under threat from natural disasters as those likely to be terrorism targets (Jordan, 2006).
Because of the unpredictability of demand for emergency services, hospitals face fluctuations in utilization on an hourly, daily, and weekly basis. With many hospitals already operating at or near full capacity (as detailed in Chapter 2), temporary surges can exacerbate chronic ED crowding, boarding, and ambulance diversion. While these surges in demand can severely stretch the resources of a hospital’s staff and diminish the quality and safety of patient care, hospitals generally maintain their normal standard of care through these surges. In a disaster situation, however, hospitals may need to shift to a sufficiency-of-care mode, in which the focus is on saving as many lives as possible rather than ensuring that each patient receives the usual standard of care (AHRQ, 2005). In the most extreme cases—for example, a full-blown influenza pandemic such as that experienced worldwide in 1918—this could mean assigning the most severely ill or injured patients to “expectant care,” a strategy that withholds treatment for those who have
TABLE 7-1 Recent Disaster Events (United States and Worldwide)
|
Type |
Examples |
Locations |
No. of Deaths |
|
Natural |
Hurricane (Katrina) |
New Orleans/Louisiana/ Mississippi/Alabama (2005) |
1,326 |
|
Avian influenza |
6 countries (2005–2006) |
118 (as of October 20, 2005) |
|
|
Earthquake |
Kashmir (2005) |
73,000 (69,000 injured) |
|
|
Tsunami |
12 countries (2004) |
212,611 |
|
|
SARS |
25 countries (2002–2003) |
774 |
|
|
Earthquake |
Northridge, California (1994) |
57 (5,000+ injured) |
|
|
Man-made |
Subway bombing |
London (2005) Madrid (2004) |
52 (700 injured) 191 (2,000 injured) |
|
Nightclub fire |
Rhode Island (2003) |
100 (200+ injured) |
|
|
Nightclub bombing |
Bali (2002) |
202 |
|
|
Anthrax |
Washington, D.C. (2001) |
5 (13 injured) |
|
|
Terrorist attacks of September 11 |
New York and Washington, D.C. (2001) |
2,752 |
|
|
Embassy bombings |
Nairobi and Tanzania (1998) |
224 (4,000+ injured) |
|
|
Release of sarin gas |
Tokyo, Japan (1995) |
12 (5,000 injured) |
|
|
SOURCES (in order listed): Associated Press, 2006a; BBC News, 2006b; Times Foundation, 2005; CNN.com, 2005a; IOM, 2004; Insurance Information Network of California, 2006; CNN.com, 2005b; Gutierrez de Ceballos et al., 2004; Associated Press, 2006b; BBC News, 2006a; CNN.com, 2002; Hirschkorn, 2003; Rand Corporation, 2004; Accountability Review Boards on the Embassy Bombings in Nairobi and Dar es Salaam, 1999; BBC News, 2005. |
|||
|
BOX 7-2 Department of Homeland Security’s 15 National Planning Scenarios
SOURCE: DHS, 2005b. |
very little chance of survival to focus resources on saving the largest possible number of lives.
A hospital’s decision to switch from routine to disaster mode has enormous implications. When to make that decision and what actions to take as a result are complex. A number of initiatives are exploring these questions. For example, within the Department of Health and Human Services (DHHS), the Centers for Disease Control and Prevention’s (CDC) National Center for Injury Prevention and Control, Division of Injury Response, is developing a consensus report describing the detailed actions to be taken by hospital and trauma center departments and personnel in the event of an explosive mass casualty event (CDC National Center for Injury Control and Prevention, 2006). The Agency for Healthcare Research and Quality (AHRQ) has sponsored research, convened expert panels, and published guidance for hospitals and communities on preparing for biological and other terrorist events. The Health Resources and Services Administration’s (HRSA) Bioterrorism Hospital Preparedness Program specifically targets hospital preparedness, with a focus on the development and implementa-
tion of regional plans to improve the capacity of hospitals to respond to bioterrorist attacks.
CRITICAL HOSPITAL ROLES IN DISASTERS
Evaluations of ED disaster preparedness consistently yield the same finding: EDs are better prepared than they used to be, but still fall short of where they should be (Schur et al., 2004). A survey conducted by CDC in 2003 gives a comprehensive picture of hospital preparedness in the years following September 11 (Niska and Burt, 2005). Hospitals vary widely in the degree to which they have prepared for the range of possible threats. At the time of the survey, almost all hospitals (97.3 percent) had plans for responding to natural disasters because holding natural disaster drills is a requirement for accreditation by the Joint Commission for Accreditation of Healthcare Organizations (JCAHO). More than 80 percent of hospitals had plans for chemical (85.5 percent) and biological (84.8 percent) threats, and more than 70 percent had plans for nuclear and radiological (77.2 percent) and explosive (76.9 percent) threats.
The remainder of this section reviews the current status of and recommended actions for enhancing hospital preparedness across five critical hospital roles during disasters: maintaining surge capacity, carrying out planning and coordination with the wider health and public safety communities, conducting training and disaster drills, protecting the hospital and its staff, and performing surveillance.
Surge Capacity
Hospitals in most large population centers are operating at or near full capacity. In many cities, hospitals and trauma centers have problems dealing with a multiple-car highway crash, much less the volume of patients likely to result from a large-scale disaster. During emergencies, hospitals can do a number of things to free up capacity and extend their resources, but there are serious physical limitations on this expansion of their capabilities. Surveys indicate that the numbers of available beds, ventilators, isolation rooms, and pharmaceuticals may be insufficient to care for victims of a large-scale disaster (Kaji and Lewis, 2004). The Rhode Island nightclub fire (discussed further below) demonstrated that even medium-sized incidents can overwhelm local hospital capacities (Hick et al., 2004). The frequent ambulance diversions and ED boarding discussed earlier in this report also signal limitations on hospital surge capacity.
The issue of capacity is an immediate problem because many hospitals and their EDs are already maximizing their existing capacity after years of capacity shedding designed to reduce costs. According to the American
Hospital Association (AHA), 60 percent of hospitals were operating at or over capacity in 2001 (The Lewin Group, 2002). Many hospitals have already opened up additional beds in an effort to alleviate overcrowding, but continue to face nursing shortages and staffing issues in supporting the existing beds (Derlet and Richards, 2000; Asplin and Knopp, 2001).
The limiting factor in the ability to respond to a disaster will vary by hospital and by type of disaster. An important limiting factor is the availability of specialists who can treat the types of cases resulting from a disaster event. For an event involving a rare biological or chemical agent, there may be limited expertise in the community. For more common types of events, such as blast injuries, the limitation will likely be an inadequate supply of surgical specialists (including neurosurgeons, orthopedic surgeons, and burn surgeons) to treat the volume of cases requiring their specialized services. While other staff, such as emergency physicians, critical care specialists, and nurses, are important, they are less likely to represent a major constraint on the ability to treat additional patients. One way in which hospitals can alleviate staff shortages is to use emergency medical services (EMS) personnel as physician extenders. In many disaster scenarios, the prehospital component is over in 1–2 hours, making a large number of EMS personnel available just as hospital activity is peaking.
Physical space is an important consideration, but probably not the most critical factor. Hospitals can add to available capacity on short notice by halting elective admissions and discharging noncritical patients. In addition, they can sometimes use ED hallways, inpatient hallways, and nonclinical areas to house victims in an emergency. According to the CDC survey, however, only 61 percent of hospitals had developed plans for the use of nonclinical space in such cases (Niska and Burt, 2005). In some instances, particularly a more circumscribed disaster, hospitals can make room for patients by transferring existing inpatients to more distant facilities. But the CDC study revealed that only 46 percent of hospitals had agreements with other hospitals to accept patients in the case of a disaster (Niska and Burt, 2005).
Intensive care unit (ICU) beds are much more difficult to empty on short notice than other beds and are probably the key limiting factor in terms of physical capacity, as they often are in day-to-day crowding (GAO, 2003a). Another physical limitation is the number of negative pressure rooms needed to prevent the spread of airborne pathogens. Limitations in available equipment, such as mechanical ventilators and decontamination showers, are also important. The committee concludes that the lack of adequate hospital surge capacity is a serious and neglected element of current disaster preparedness efforts.
Planning and Coordination
When a disaster occurs, the normal operating assumptions about patients, responses, and treatments often must be jettisoned. Depending on the type of event, some of the nonroutine things that can happen include the following (Ackermann et al., 1998; Auf der Heide, 2006):
-
Victims who are less injured and mobile (the so-called “walking wounded”) will often self-transport to the nearest hospitals, quickly overwhelming those facilities.
-
Casualties are likely to bypass on-site triage, first aid, and decontamination stations.
-
EMS responders will often self-dispatch. Providers from other jurisdictions may appear at the scene and transport patients, sometimes without coordination or communication with local officials.
-
In some cases, local facilities are not aware of the event until or just before patients start arriving. Hospitals may receive no advance notice of the extent of the event or the numbers and types of patients they can expect.
-
There may be little or no communication among regional hospitals, incident commanders, public safety, and EMS responders to coordinate the response regionwide.
Consider the regional response needed after the Rhode Island nightclub fire in February 2003. During a concert, a fire broke out on the stage in the small venue and quickly spread throughout the nightclub before many patrons could escape. The fire consumed the building in 3 minutes, and 96 people were killed. It took 160 firefighters from 15 communities to put out the flames; 65 ambulances also responded (Gutman et al., 2003; Ginaitt, 2005).
The first patients began to arrive at local hospitals minutes after the fire broke out. Most hospitals received notification from EMS before patients began to arrive, but several others said they received no notification, or there was limited or incorrect information regarding the number of patients to expect. A total of 273 victims sought care at hospitals. The closest hospital to the nightclub (3 miles away), Rhode Island’s second largest, is a 359-bed acute care hospital that handles 58,000 ED visits per year. It received 82 patients, 25 percent of whom were admitted and 25 percent of whom were transferred to other hospitals. A level I trauma center located 12 miles away from the nightclub received 68 patients; approximately 63 percent were admitted (Gutman et al., 2003). A number of other Rhode Island hospitals, as well as Massachusetts General, University of Massachusetts Medical Center, and Shriners Hospital for Children, also received patients. It was only the second time that Shriners had opened its doors to adult patients (Ginaitt, 2005).
However, there was limited communication between hospitals and no means for hospital coordination and prioritization of helicopter transfers of patients to burn centers. As a result, 10 transfers by helicopter occurred from four different hospitals within the first few hours. All air medical resources available in New England were used that evening (Gutman et al., 2003). The amount of regional resources needed to respond to this medium-sized emergency incident is striking. It demonstrates the need for hospitals to coordinate planning with each other as well as other responders, including prehospital providers and air medical personnel. This often means working and planning with groups across state lines to decide on and implement the surge capacity, workforce training, protective equipment, and surveillance and communications systems appropriate for the region.
Coordination among Local, Regional, State, and Federal Entities
The underlying philosophy of disaster management is that every event is handled at the lowest possible geographic, organizational, and jurisdictional level (DHS, 2004). When a disaster event becomes larger than can be handled adequately by local response capabilities, the state usually gets involved, enabling the allocation of statewide resources to the affected area. The state government has ultimate responsibility for the health and wellbeing of its citizens, and can allocate funding and statewide emergency resources, utilize National Guard troops, and draw on state supplies of drugs and vaccines. When an event becomes too big to be handled at the state and local levels, it may be declared an “incident of national significance.” In this case, the command structure shifts to the federal response outlined by the National Incident Management System (NIMS) through DHS, opening the way for federal resources, including federal stockpiles, disaster management assistance teams (DMATs), and federal dollars, to be deployed to support operations.
Most agree that for disaster response to be effective, incident control must be clear, communications good, and providers at the local level involved in the process. In the event of a disaster, local emergency providers must respond as additional resources are mobilized at state or federal levels. The medical care component of most disasters is usually over after a few hours, so even if these additional resources can be assembled, they may arrive too late to be of much help (Waeckerle, 1991). Further, only regional and local planning can adequately anticipate and address local utilization patterns that will impact the execution of disaster plans. Therefore, all hospitals must be prepared to receive patients suffering from any type of illness, injury, or exposure.
To respond effectively, hospitals must interface with incident command at multiple levels and be prepared to deal with transitions between levels, for
example, when incident command shifts from the local to the state or federal level. Each hospital should be familiar with the local office of emergency preparedness and know how hospitals are represented at the emergency operations center during an event, whether through the hospital association, the health department, the EMS system, or some other mechanism. Using an existing program, such as the Hospital Emergency Incident Command System (HEICS), can aid hospitals in internal preparedness and coordination with the rest of the system. HEICS is a standardized approach to disaster management—essentially an internal hospital application of NIMS—that was developed and has been used nationwide for a decade.
Regionalization
Current federal preparedness funding has been geared toward preparing all hospitals to respond at some level to all hazards. Because the range of possible threats is so broad, the feasibility of meaningfully preparing all hospitals is unrealistic. Regionalization of certain aspects of preparedness may facilitate a more timely and effective response (Bravata et al., 2004a). The benefits of regionalizing disaster response include consolidation of inventories of drugs and vaccines; surveillance to identify outbreaks of disease; efficiency of concentrating certain types of medical response at fewer hospitals; and improved communications, command, and control associated with regionwide events (GAO, 2003a). Regionalization is also likely to benefit triage, medical care, outbreak investigations, security management, emergency management, and training.
Regional trauma systems are critical to planning for the care of severely injured patients during a disaster. While 47 states have developed or are developing a statewide trauma system plan and 38 states now designate trauma systems, there is wide variation across states in the level of development of these systems and in the degree of coordination with disaster planning. In one example of a regional approach to disaster planning, Connecticut developed a statewide system for hospital preparedness for bioterrorism that was built on the trauma system (Jacobs et al., 2003). The Connecticut Department of Public Health contracted with two level I trauma centers, which were designated as regional centers of excellence for bioterrorism preparedness. The existing trauma system and communications network provide the basic infrastructure for the system, which links to the Metropolitan Medical Response System centered in Hartford. The two centers of excellence serve to coordinate all aspects of medical disaster response activities within their regions, including surveillance, training, planning, facilities, equipment, and supplies. This model is based on the realization that resources are too scarce for a haphazard approach—disaster funding should be targeted to those regions and hospitals where it will do the most good for the community
in the event of a disaster. Ideally, all assets required for a community or a state to mount an effective response should be developed within the regional context described in Chapter 3.
Federal funding for the development of such approaches is currently limited. The establishment of the Division of Trauma and EMS within DHHS in 1990 helped jump start the development of trauma systems through state grants. But this program was eliminated in 1995, leaving a gap in federal leadership until the creation of the Trauma/EMS Systems program within HRSA’s Division of Healthcare Preparedness in 2001. This program was also recently defunded. While the program operated on a relative shoestring—approximately $3.5 million in fiscal years 2002 to 2005—it provided critical national leadership for planning, infrastructure development, standards development, and coordination with other federal agencies.
Communications
Good communications among the many community services involved in disaster response are essential to an effective response—to ensuring that patients will be directed to the most appropriate facilities, that hospitals will not be overwhelmed with patients, that hospitals will be alerted sufficiently in advance of the arrival of patients to be able to mount the appropriate response, and that resources will be allocated effectively throughout the community. Unfortunately, communication is a significant weakness of the current system, reflecting the existing fragmentation of emergency care. According to the 2003 CDC survey, surprisingly few hospitals had provisions in their bioterrorism response plans for contacting outside entities such as EMS (72 percent), fire departments (66 percent), or other hospitals (51 percent). Hospital collaboration in mass casualty drills with outside organizations followed a similar pattern—only 71 percent collaborated with EMS, 67 percent with fire departments, and 46 percent with other hospitals (Niska and Burt, 2005).
In addition to coordinated communications, investments should be made in enhanced communications equipment. Hospitals should have reliable and redundant digital and voice communications with the regional and state public safety, emergency management, and public health agencies. The loss of hospital communications capabilities during Hurricane Katrina turned out to be a major obstacle to coordinating the evacuation and care of victims. Hospitals should have some satellite telecommunications capability in preparation for a catastrophic event.
Veterans Health Administration
With hospitals, nursing homes, ambulatory care clinics, and counseling clinics in many communities across the country, the Veterans Health Administration (VHA) is well positioned to enhance regional response, particularly since its hospitals are required by law to maintain excess capacity. The VHA currently deploys personnel to all presidentially declared disasters, including Hurricane Andrew, the Northridge earthquake, and the September 11 terrorist attacks. VHA staff also support such events as the Super Bowl, presidential inaugurations, and papal visits. An Emergency Management Academy is being developed to train and equip VHA staff with emergency management skills. In addition, the VHA procures, stores, and maintains pharmaceutical stockpiles for incidents involving weapons of mass destruction (WMD) (Emergency Management Strategic Healthcare Group et al., 2005). The committee recognizes the importance of the VHA in emergency planning and response, and recommends that the Department of Homeland Security, the Department of Health and Human Services, the Department of Transportation, and the states collaborate with the Veterans Health Administration (VHA) to integrate the VHA into civilian disaster planning and management (7.1).
Training and Disaster Drills
The unique aspects of disaster response require specialized training, both in the clinical management of disaster victims and in institutional procedures that may be quite different from those under normal operating conditions (HRSA, 2002; Treat et al., 2001; GAO, 2003a,b; Rivera and Char, 2004). There are strong indications that training is inadequate in both areas.
Hospital Training and Drills
Results of the 2003 CDC survey indicate that progress has been made since September 11 in training hospital staff to deal with emergencies, but deficiencies remain. Training in response to terrorism-related threats varied widely among staff: 92 percent of hospitals trained their nursing staffs in at least one type of threat, while residents and interns received training at only 49 percent of hospitals (Niska and Burt, 2005) (see Figure 7-2). This nevertheless represents an improvement over training prior to September 11. Treat and colleagues (2001), for example, found that fewer than 25 percent of hospitals in and around Washington, D.C., had staff trained in WMD before September 11 (Treat et al., 2001). The CDC survey revealed that staff at most hospitals (89 percent) had received training since September 11 in the
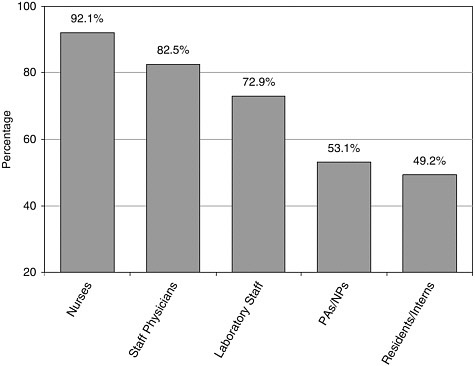
FIGURE 7-2 Percentage of hospitals with staff trained in disaster response.
NOTE: NP = nurse practitioner; PA = physician assistant.
SOURCE: Niska and Burt, 2005.
diagnosis and treatment of exposure to biological agents—most frequently smallpox and anthrax. And three-quarters of hospitals had trained staff in implementing an incident command system.
According to the CDC survey, nearly 90 percent of hospitals (88.4 percent) had conducted a mass casualty drill. The most common scenario was a general disaster response, with far fewer hospitals addressing other types of threats—chemical (44.7 percent), biological (37.5 percent), explosive or incendiary (21.3 percent), nuclear or radiological (15.4 percent), and severe epidemic (7.1 percent).
JCAHO requires hospitals to have an emergency management plan and to evaluate the plan by conducting practice drills, but this effort focuses mainly on logistical aspects rather than personnel training. Some hospitals have developed their own curriculum or training guides for staff (Zavotsky, 2000; Phillips and Lavin, 2004). Researchers have aided these efforts by outlining key recommendations for training components (Waeckerle et al., 2001; Greenberg et al., 2003), developing ideas for future
training approaches (Terndrup et al., 2005), and suggesting best practices based on provider feedback (Alexander et al., 2005). States can overcome the lack of standardized disaster training guidelines and other barriers by expanding and supporting continuing education and facility preparedness requirements.
Introducing on-the-job training for ED personnel is difficult for a number of reasons, however. Many hospitals report inadequate funding to cover the attendance costs (e.g., time off, tuition, travel) of training (ACEP Nuclear, Biological and Chemical Task Force, 2001). At the University of Pittsburgh Medical Center, a disaster drill in the ED costs $3,000 per hour in staff salaries alone (AHRQ, 2004). Also, the ED may experience personnel shortages during training unless coverage is provided for the staff being trained. Additionally, the failure of hospital administrators or ED personnel to recognize the importance of training can result in a lack of support (ACEP Nuclear, Biological and Chemical Task Force, 2001).
HRSA’s National Bioterrorism Hospital Preparedness Program (HRSA, 2006) (discussed in more detail below) provides grants to states to improve hospital preparedness. Guidance to grantees in the initial year of the program (HRSA, 2002) made training a secondary priority, and in the following year it was made optional. However, all grantees noted that they were providing training for bioterrorism and other public health emergencies. The most frequently addressed subject was worker safety, followed by psychosocial issues for both patients and providers. Other topics addressed included responding to CBRNE events, incident command, risk communication, and treatment of special populations (AHRQ, 2004). The grantees used a variety of different methods for training, including face-to-face training, distance learning, field exercises and drills, and distribution of written materials.
Professional Training Curricula
Training currently provided to physicians in medical school and continuing education programs does not uniformly address the threat of disasters, types of WMD agents, and procedures for handling mass casualty incidents and events. WMD-related training is only a small component of emergency medicine residency programs, but, as mentioned earlier, approximately 38 percent of practicing emergency physicians are neither residency trained nor board certified in emergency medicine and are therefore not exposed to that curriculum. Barriers to training include an already full medical school and residency curriculum and a lack of instructor expertise, equipment, and advocates to lobby for the inclusion of disaster preparedness training (Waeckerle et al., 2001; ACEP Nuclear, Biological and Chemical Task Force, 2001). But opportunities for training in CBRNE agents exist at various levels; medical schools can incorporate instruction on these agents into cur-
rent coursework (e.g., toxicology, epidemiology) and clerkships, residency programs can dedicate time to these agents in both the ED and planned educational experiences, and states can require a certain amount of continuing education on these agents for relicensure (Waeckerle et al., 2001).
Disaster training is also currently not a core component of the nursing curriculum. WMD topics and agents have been added to the Emergency Nurses Association (ENA) Emergency Nurses Core Curriculum; however, only a small percentage of ED nurses receive this training. Additionally, disaster response is not included on the emergency nursing certification exam. Opportunities exist for integrating WMD agents and disaster response techniques into the nursing curriculum. Additional steps might include incorporating articles on disaster response and associated topics in professional nursing journals and introducing related questions into the certified emergency nurse (CEN) board exam (Waeckerle et al., 2001).
The lack of standardized training for ED workers is recognized, and there have been several efforts to improve their competencies. For example, the American Medical Association (AMA) developed courses for physicians and other health professionals in disaster preparedness, including courses in basic disaster life support (BDLS) and advanced disaster life support (ADLS) (AMA, 2003). Additionally, the federal Office of Emergency Preparedness (formerly in DHHS, now in DHS) contracted with the American College of Emergency Physicians (ACEP) to identify the core content of a national program for training prehospital emergency personnel and emergency physicians and nurses to detect and respond to nuclear, biological, and chemical agents. Phase 2 of the contract, which has not yet been funded, would assist with the implementation of that curriculum (ACEP, 2005).
Serious clinical and operational deficiencies, fragmentation, and lack of standardization exist across a broad spectrum of key professional personnel (nurses, physicians, ancillary care providers, administrators, and public health officials) in both individual training and coordination of a team response. The committee believes a concerted effort to integrate disaster preparedness and education into established professional curricula, continuing education, and certification programs is the most reasonable solution to these shortcomings at this point in time. Therefore, to address the need for competency in disaster medicine across disciplines, the committee recommends that all institutions responsible for the training, continuing education, and credentialing and certification of professionals involved in emergency care (including medicine, nursing, emergency medical services, allied health, public health, and hospital administration) incorporate disaster preparedness training into their curricula and competency criteria (7.2).
Protecting the Hospital and Staff
Protecting the Hospital
The hospital represents a critical asset in the event of a disaster, but it is also a vulnerable one. Hospitals can fall victim to the disaster event itself, as occurred in the cases of Katrina and other recent hurricanes. Obviously, each hospital must have procedures in place to maintain essential services when necessary and transport patients to alternative facilities. In addition, when a hospital shuts down, its staff, vehicles, equipment, and supplies may still be useful. Regional disaster planning should include plans to distribute these assets as needed by the community.
Hospitals can be targeted by terrorism directly or indirectly, and there has been little preparation for or even discussion of that possibility. Hospitals should plan for direct attacks and establish plans for limiting access, securing perimeters, protecting water and power supplies, and sheltering staff. A particular vulnerability, because of the information intensity of the hospital environment, is the hospital’s exposure to cyber attack. Such an attack could have a profound impact on clinical operations, communications, telemetry, records, and many other critical functions.
Hospitals are also vulnerable to an influx of disaster victims. Large numbers of victims descending on a hospital can be overwhelming and diminish its effectiveness in dealing with casualties. Patients suspected of exposure to chemical or biological agents can completely shut down a facility if they are not decontaminated properly before entering (the same applies to vehicles as well). Every hospital must have adequate decontamination showers and procedures for dealing with contaminated patients because experience has taught that many victims “self-evacuate” from the scene of a disaster, bypassing on-scene triage and decontamination (Auf der Heide, 2006). In extreme cases, the hospital must be prepared to lock down to prevent the entry of contaminated patients who would otherwise disable the facility—an action antithetical to the open way in which hospitals typically operate.
Protecting Staff
The risk of chemical or biological exposure of hospital staff occurs when exposed patients are not properly decontaminated before arriving at the ED or as ED personnel are in the process of decontaminating victims. The risk of secondary contamination is present if the substance is toxic and likely to be carried on a victim’s clothing, skin, or hair in sufficient quantities to threaten rescuers or health care providers (Horton et al., 2005). There may also be a risk if victims of chemical contamination exhale the fumes they have inhaled in breathing space shared with others.
The sarin attacks in Tokyo and the severe acute respiratory syndrome (SARS) epidemic in China and Toronto are examples of exposure of emergency care providers. The SARS epidemic (see Box 7-3) demonstrated the difficulties associated with containing even a small outbreak—particularly when health professionals themselves are inadequately protected and become both victims and spreaders of disease (Donovan, 2003; Augustine et al., 2004). One of the most important tools in such an event is the availability of negative pressure rooms that prevent the spread of airborne pathogens throughout the ED or inpatient ward. The potential for a major outbreak of avian influenza further highlights the need for this capacity. Unfortunately, the number of such rooms is minimal and is often restricted to a handful of tertiary hospitals in major population centers. The committee believes the lack of an adequate supply of negative pressure rooms is a critical vulnerability of the current system and that the existing capacity of this resource could be quickly overwhelmed by either a terrorist event or a major outbreak of avian influenza or some or other airborne disease, posing an extreme danger to hospital workers and patients. It may be hoped that future ED and hospital bed construction will include designs that allow any patient room to be converted to a negative pressure room.
While an adequate number of negative pressure rooms is essential for control of airborne infections, it is only part of the solution. There must also be substantial training in disease recognition and in decontamination and containment procedures. In addition, it is necessary to learn from SARS and similar experiences and to develop techniques and approaches that add to our understanding of the management of disease outbreaks. One possible containment strategy is to use cohort staffing techniques similar to those employed in neonatal intensive care. In this approach, groups of providers are linked with groups of patients for the episode of care to prevent spread to other patients and providers.
During the sarin event in Tokyo, the failure of hospital providers to wear personal protective equipment (see the discussion below), coupled with a decision to contain the still-clothed contaminated patients in a poorly ventilated hospital chapel, contributed to hospital workers’ secondary sarin exposure (Hick et al., 2004; see Box 7-4). This incident raises an important issue with regard to disasters involving exposures, alluded to above: most ambulatory patients are unlikely to wait for hazardous materials teams to deploy and set up decontamination equipment; instead, victims self-refer to the nearest emergency room (Hick et al., 2004; Horton et al., 2005).
Personal Protective Equipment
The use of personal protective equipment by hospital workers is complicated by the fact that different types of such equipment are needed for
|
BOX 7-3 The SARS Outbreak and Its Implications The 2003 outbreak of severe acute respiratory syndrome (SARS) speaks volumes about the global health care community’s deficiencies in recognizing, controlling, and communicating information about potential infectious diseases. The rapid spread of SARS in early 2003 caught the world off guard and challenged the global public health infrastructure. A clinical syndrome characterized by fever, lower respiratory symptoms, and radiographic evidence of pneumonia (CDC, 2005), SARS is caused by a coronavirus originally transmitted from an animal source. Case control studies suggest that China’s Guangdong Province was the initial focus of infection and transmission (IOM, 2004). Between November 16, 2002, and February 10, 2003, the disease quietly spread throughout provinces in China, as well as neighboring countries, before being officially recognized. Striking mainly adults aged 18–64, the disease was quickly spread by infected travelers and “superspreaders”—people who may infect many others because they have high levels of contact, go undiagnosed for a long period, and may have secondary conditions that aid the spread of disease. Nosocomial transmission made health care providers, patients, and family members of both groups especially susceptible. Deficiencies in both global and local public health infrastructures were apparent at every stage of the epidemic. The virus went unreported from China for 3 months, and later warnings and alerts were slow to be released. Most warnings about symptoms were unrecognized, and guidelines for the use of isolation or personal protective equipment were ignored (Donovan, 2003). The SARS outbreak in Toronto was triggered in part by a patient who sought care in a Toronto ED for fever and a cough. He spent the night in a crowded ED awaiting admission for what was thought at the time to be community-acquired pneumonia. Over the course of the night, he infected 2 nearby patients and several hospital staff members with SARS. Both this index case and the 2 patients he infected subsequently died from the disease, and a total of 31 patients and staff fell ill. Ironically, the same hospital where this incident occurred continues to board admitted patients in its ED (Cass, 2005). But health care workers clearly suffered the most. The aggressive respiratory care provided actually helped spread SARS, while insufficient availability of isolation rooms and personal protective equipment helped boost the case fatality rate for the disease to 10–15 percent (Augustine et al., 2004). Based on data as of December 2003, there were 8,094 total suspected SARS cases, 774 of whom died (WHO, 2005). |
|
BOX 7-4 The Tokyo Subway Attack At approximately 7:45 AM on March 20, 1995, five men, all members of a religious cult, boarded five separate subway trains in Tokyo. Witnesses reported that one of the men boarded a train wearing a sanitary mask and after taking a seat, opened his briefcase and removed a box wrapped in newspaper. The man put the box at his feet and leisurely read the newspaper until the next stop, when he exited the train, leaving the package behind. This man and the four others each released one or more containers of sarin, a lethal, colorless gas. Riders on the subway were immediately affected. Subway stations evacuated all passengers, many choking, vomiting, and blinded by the chemical. More than 4,000 victims of the attack sought treatment at hospitals; most were self-transported. Lacking initial knowledge of the sarin attack and proper personal protective equipment, hospital workers became victims when they were exposed to the nerve agent on the clothing of patients. Twenty-three percent of the hospital house staff (100 health care workers) showed signs of sarin poisoning (Pangi, 2002). |
various types of exposures. Biological and chemical agents require different types of respiratory and dermal protection (Arnold and Lavonas, 2004). Proper selection of personal protective equipment is particularly challenging when the identity of the contaminating agent is unknown. Additionally, such equipment is often restrictive and cumbersome, making triage and patient care more difficult (Suner et al., 2004; Horton et al., 2005).
Until recently, hospitals had little guidance to follow regarding the specific personal protective equipment that should be available (Hick et al., 2004; OSHA, 2005). JCAHO requires each institution with an ED to have a plan for treating at least one contaminated patient (Arnold and Lavonas, 2004). In January 2005, the Occupational Safety and Health Administration (OSHA) compiled a set of best practices that specifies the personal protective equipment hospitals can use to protect first receivers assisting victims contaminated with unknown substances. This equipment includes a powered air purifying respirator, a chemical-resistant protective garment, head covering if it is not already included in the respirator, double-layer protective gloves, and chemical-protective boots. However, this recommendation assumes that hospitals will make a conscientious effort to limit the secondary exposure of health care workers (e.g., that hospitals will have protocols in place for removing the clothing of and properly decontaminating victims). Additionally, OSHA recommended that hospitals assess specific local hazards and
augment its recommendations accordingly (OSHA, 2005). The committee believes that protection of emergency care and other hospital personnel is a critical deficiency of the current system.
Surveillance
EDs are well positioned to collect and analyze, in collaboration with state and local health departments, data on injury incidence, disease trends, and potential bioterrorism threats in the community (Garrison et al., 1994). The role of EDs in surveillance has been demonstrated by the National Electronic Injury Surveillance System (NEISS), operated by the U.S. Consumer Product Safety Commission. The commission uses data from the NEISS to monitor consumer product–related injuries under its regulatory jurisdiction and recommend changes in policy regarding those products. For example, NEISS helped the commission identify an outbreak of injuries from all-terrain vehicles, which ultimately led to direct intervention by the federal government to restrict access to such vehicles (Garrison et al., 1994). ED surveillance data have played a crucial role in our current understanding of nonfatal injuries, leading to physical safety improvements (better-designed highways) and public safety legislation (changes to speed limits).
To address the threat of bioterrorism and disease outbreaks, hospital EDs can learn to recognize the diagnostic clues that may indicate an unusual infectious disease outbreak so public health authorities can respond quickly (GAO, 2003c). During the SARS outbreak in 2003, hospitals played an important role in identifying infected individuals. ED staff routinely used questionnaires to screen patients for fever, cough, and travel to a country with active SARS. But this screening of patients for SARS symptoms was reactive—EDs were performing it because SARS had become a problem in Toronto, and there was a real possibility of its spreading to cities in the United States. The greater challenge is preparing ED staff and their public health partners to identify an initial outbreak.
Surveillance systems vary considerably from region to region, and according to a recent Government Accountability Office (GAO) report, there are serious gaps in our ability to detect an outbreak. The majority of surveillance systems in existence today are manual ones that rely heavily on ED personnel to communicate information to public health personnel. There are two types of manual surveillance systems: active and passive. With active systems, hospital staff are responsible for reporting incidents and conveying data on illnesses to public health officials, for example, through phone calls or faxes (GAO, 2003c; McHugh et al., 2004). An example of an active system is that operating in Santa Clara County, California. ED nurses make note of every patient who has a chief complaint compatible with one of six syndromes: flu-like symptoms, fever with mental status changes, fever
with skin rash, diarrhea with dehydration, visual or swallowing difficulties/ slurred speech or dry mouth, and acute respiratory distress syndrome. The information is then faxed to the local health department at the end of each nursing shift (Henning, 2003). Because of underreporting by hospitals and the time lag between the diagnosis and the health department’s receipt of information, active systems are not effective in identifying a rapidly spreading outbreak at its earliest stage (GAO, 2003c). Other regions use passive systems, in which information is automatically collected in the course of patient care, and either automatically reported or “mined” by public health workers to solicit information from hospitals (GAO, 2003c; Schur, 2004). Passive systems tend to provide more complete reporting of surveillance data than a system that is fully dependent on voluntary reporting (GAO, 2003c).
In an effort to improve disease surveillance capabilities, some hospitals use electronic surveillance systems to passively collect surveillance data and automatically transfer the data from the ED to health departments. Electronic systems are beneficial in that they allow more timely transmission of data, but are inappropriate for local health departments that do not have adequate resources to manage, analyze, and interpret large influxes of data (Bravata et al., 2004b). CDC funds three ongoing electronic surveillance system networks that collect data from a sample of hospitals. One of these is EMERGency ID NET, which collects data from 11 academically affiliated EDs that cumulatively account for approximately 1 percent of all ED visits (Talan et al., 1998; Barthell et al., 2002). The data are collected during evaluation of patients with specific clinical syndromes; entered into the program’s software within 1 day of a patient visit; and electronically stored, transferred, and analyzed at a central receiving site. With these data, research on emerging infectious disease can be conducted (Talan et al., 1998). But data from systems such as EMERGency ID NET may be limited in that the systems collect data only on certain types of patients, collecting all the data is difficult and time-consuming, distribution to individuals assigned to analyze the data may be delayed, and findings may have little relevance for local efforts (Barthell et al., 2002). This type of system is too slow to trigger rapid response by public health officials.
Some surveillance systems, whether manual or electronic, capture syndromics. Syndromic surveillance is surveillance for disease syndromes (signs and symptoms), rather than for specific clinical or laboratory-defined diseases (Henning, 2003). It is a relatively new concept in public health surveillance. The problem with nonsyndromic systems is that outbreaks of disease may be difficult to diagnose, and delays in diagnosis can result in a larger number of casualties and a more prolonged outbreak. Syndromic surveillance may improve early detection of an outbreak (Henning, 2003). The key is to have systems that can help staff recognize index cases (i.e., the
first one to three patients), as well as clusters of cases presenting to different hospitals in an area.
The most sophisticated of surveillance systems are real-time syndromic surveillance systems. Several large cities (New York, Chicago, Boston, Seattle) began operating such systems, beginning largely in 1999, with special funding from CDC (Henning, 2003). An example is Insight, a computer-based clinical information system at the Washington Hospital Center (WHC) in Washington, D.C., designed to record and track patient data, including geographic and demographic information. The software proved useful during the 2001 anthrax attacks, when it enabled WHC to send complete, real-time data to CDC while other hospitals were sending limited information with a lag of one or more days. The success of Insight attracted considerable grant funding for its expansion; WHC earmarked $7 million for Insight to link it to federal and regional agencies and integrate it with other hospital systems (Kanter and Heskett, 2002).
Although most public health officials are quickly embracing surveillance systems, particularly syndromic systems, more research is needed on their effectiveness. Bravata and colleagues (2004b) recently undertook a review of surveillance systems to evaluate their utility for detecting illnesses and syndromes related to bioterrorism. Researchers reviewed 115 systems (at EDs and other locations), including 9 syndromic surveillance systems. The authors found that few surveillance systems have been comprehensively evaluated; therefore, information is lacking on the ability of such systems to facilitate decision making by clinicians and public health officials (Bravata et al., 2004b).
CHALLENGES IN RURAL AREAS
The focus of emergency preparedness has been on urban areas in part because of the perceived increased risk of terrorism in these areas. However, there is a danger associated with neglecting rural areas. Indeed, one might argue that rural areas may be even more vulnerable to a terrorist attack. Many nuclear power facilities, hydroelectric dams, uranium and plutonium storage facilities, and agricultural chemical facilities, as well as all U.S. Air Force missile launch facilities, are located in rural areas and are potential targets for attack. Additionally, if individuals with infectious diseases, such as smallpox, enter the country through Canadian or Mexican borders, rural providers may be the first to identify the threat (ORHP, 2002). Although fewer individuals may be harmed by an incident in a rural area as compared with an urban area, mass disasters are relative, depending on the size of the local population and hospital capacity. The demand for health and hospital care by 200 people could overwhelm a 20-bed facility (AHA, 2001).
The emergency preparedness challenges EDs face are exacerbated in
rural areas because rural hospitals often lack the resources and staff needed to respond swiftly to a catastrophic event (ORHP, 2002). In fact, results of several studies indicate that urban areas are generally further along in bioterrorism preparedness planning than rural areas because they have more experience in dealing with public health emergencies and more resources upon which to draw (Schur et al., 2004). Rural facilities tend to be limited in medical supplies, life-sustaining equipment (such as ventilators), and auxiliary power sources (Gursky, 2004). Additionally, rural hospitals have even more limited surge capacity than hospitals in urban areas; 500 rural hospitals are Critical Access Hospitals, which are limited to 15 beds (ORHP, 2002). Rural hospitals also tend to lack decontamination facilities. In a 2001 study of hospitals in Federal Emergency Management Agency (FEMA) region III, none of the 22 rural hospitals had decontamination stations that could process 10 to 15 patients at a time; 4 of those hospitals had no decontamination plans in place (Treat et al., 2001). Some rural hospitals rely on local EMS personnel to perform decontamination; however, this is concerning because past experience has shown that the vast majority of disaster victims seek care in emergency rooms without accessing EMS (Treat et al., 2001). Moreover, communications systems in rural EDs tend to be unreliable and interrupted by terrain and weather (Gursky, 2004).
Staffing is another crucial problem for rural hospitals. Although the American Hospital Association (AHA) and other groups recommend that rural hospitals develop a reserve staff (retired health workers, persons in training), existing shortages make it difficult to do so. Additionally, some hospital personnel, particularly nurses, work part-time in nearby urban areas and may not be available in the event of a crisis. Training of staff in emergency preparedness is often complicated by the fact that training meetings are frequently held in urban areas that may be quite far away from rural hospitals. One day of training may require 2 or 3 days away from the hospital to accommodate travel time (Schur et al., 2004). Additionally, rural hospitals that rely heavily on contract staff may be reluctant to invest in training opportunities for those individuals since they may not continue working at that hospital in the long term.
Rural hospitals may not have access to the same federal funding for bioterrorism as urban hospitals. This may be particularly problematic because many rural hospitals are older and more isolated, making preparedness measures more expensive (Schur et al., 2004). Rural hospitals have not benefited from Metropolitan Medical Response System (MMRS) funding since that funding is targeted to metropolitan areas. On the other hand, rural hospitals have access to other funding streams not available to urban hospitals; in 2003, DHHS allocated $45 million in federal grants for rural and frontier hospitals (Gursky, 2004).
FEDERAL FUNDING FOR HOSPITAL PREPAREDNESS
Total federal preparedness funding has increased substantially in the 5 years since September 11, 2001. Emergency preparedness funding in DHHS, for example, rose from $237 million in fiscal year 2000 to $9.6 billion in fiscal year 2006 (Broder, 2006). But while the vast majority of terrorist events worldwide have involved conventional explosives and nonbiological agents, federal spending on preparedness has focused heavily on bioterrorism at the expense of other priorities (DePalma et al., 2005). Furthermore, the proportion of these dollars allocated to hospitals for infrastructure, technology, equipment, and training enhancements has been very limited.
Federal preparedness funding has been made available indirectly to hospitals primarily through two programs: MMRS and the Bioterrorism Hospital Preparedness Program. A review of each of these programs indicates that the amount provided to hospitals specifically for improving preparedness efforts has been small (IOM, 2002).
MMRS was created in 1996 to enhance and coordinate local and regional response capabilities for highly populated areas that could be targeted by a terrorist attack using WMD. A total of 124 jurisdictions receive funding under the program. The organizing principles and resources of the program are also applicable to large-scale incidents, such as hazardous material incidents, natural disasters, and disease outbreaks. MMRS was funded at $50 million for both fiscal years 2003 and 2004, and was reduced to $30 million in both fiscal years 2005 and 2006. Each of the 124 jurisdictions will receive $232,030 for fiscal year 2006. Hospitals are aided indirectly through this program by participation in preparedness planning. However, hospitals initially did not participate in the program; it took several years before they were integrated into MMRS planning (DHS, 2005a). MMRS was transferred from DHHS to DHS in 2003 and now resides in the Office of Grants and Training (GAO, 2003b).
The Bioterrorism Hospital Preparedness Program is targeted more specifically to hospital preparedness. The primary focus of the program is on developing and implementing regional plans to improve the capacity of hospitals to respond to bioterrorist attacks. The program made its initial awards in 2002, and the funding is distributed through cooperative agreements with states and selected municipalities, which have considerable flexibility in determining how the funding is allocated across hospitals. The cooperative agreements consist of two phases. In phase I, states are required to develop a needs assessment for a comprehensive bioterrorism preparedness program for hospitals and other health care entities and to begin the initial implementation of the plan. In phase II, states are required to submit more detailed implementation plans, including how they are going to address a series of critical benchmarks outlined by HRSA (GAO, 2003a). Funding for this program grew from $125 million in 2002 to $498 million in fiscal
year 2003 and $515 million in fiscal year 2004 (Gursky, 2004), but fell to $491 million in fiscal year 2005 (HRSA, 2006). The amount going directly to hospitals varied greatly by state, and in many cases hospitals received only a limited amount of the funding. According to one study, the “typical” award to hospitals was approximately $5,000–10,000, though some hospitals received funding in the range of $50,000–100,000 (McHugh et al., 2004). The funding under the program has generally not been sufficient to purchase the equipment needed for one critical care room or to retrofit an airborne infection isolation room in one hospital (Hick et al., 2004).
In addition, CDC funds 52 Centers for Public Health Preparedness (CPHPs). CPHPs are academic institutions that provide a focal point for planning, training, and collaboration between health departments and other community partners in preparing for public health crises.
The allocation of preparedness funding across states has been controversial. The 2005 appropriations bill allocated “hospital preparedness” funding to states on a per hospital bed basis, rather than on the basis of the likelihood of disaster. Critics argue that this apportionment is essentially “pork” rather than an attempt to allocate preparedness dollars rationally according to need. States facing limited risk can receive substantial funding under this approach, while cities such as Washington, D.C., which face a much greater risk, receive a lesser share (ER One, 2005).
Trauma systems also represent a critical component of disaster response. Federal support for the development of these systems and their coordination with other regional disaster planning efforts does not appear to reflect recognition of this fact. Federal funding for state trauma system development and planning has been inconsistent; it was recently dealt a blow with the defunding of the Trauma/EMS Systems program for fiscal year 2006.
States and communities should play an important role in determining how they will prepare for emergencies. To the extent that they are supported in this effort through federal preparedness grants, the critical role and vulnerabilities of hospitals must be more widely acknowledged, and the particular needs of hospitals and hospital personnel must be taken explicitly into account. Therefore, the committee recommends that Congress significantly increase total preparedness funding in fiscal year 2007 for hospital emergency preparedness in the following areas: strengthening and sustaining trauma care systems; enhancing emergency department, trauma center, and inpatient surge capacity; improving emergency medical services’ response to explosives; designing evidence-based training programs; enhancing the availability of decontamination showers, standby intensive care unit capacity, negative pressure rooms, and appropriate personal protective equipment; and conducting international collaborative research on the civilian consequences of conventional weapons terrorism.
SUMMARY OF RECOMMENDATIONS
7.1: The Department of Homeland Security, the Department of Health and Human Services, the Department of Transportation, and the states should collaborate with the Veterans Health Administration (VHA) to integrate the VHA into civilian disaster planning and management.
7.2: All institutions responsible for the training, continuing education, and credentialing and certification of professionals involved in emergency care (including medicine, nursing, emergency medical services, allied health, public health, and hospital administration) should incorporate disaster preparedness training into their curricula and competency criteria.
7.3: Congress should significantly increase total preparedness funding in fiscal year 2007 for hospital emergency preparedness in the following areas: strengthening and sustaining trauma care systems; enhancing emergency department, trauma center, and inpatient surge capacity; improving emergency medical services’ response to explosives; designing evidence-based training programs; enhancing the availability of decontamination showers, standby intensive care unit capacity, negative pressure rooms, and appropriate personal protective equipment; and conducting international collaborative research on the civilian consequences of conventional weapons terrorism.
REFERENCES
Accountability Review Boards on the Embassy Bombings in Nairobi and Dar es Salaam. 1999. Report of the Accountability Review Boards on the Embassy Bombings in Nairobi and Dar es Salaam on August 7, 1998. Washington, DC.
ACEP Nuclear, Biological and Chemical Task Force (American College of Emergency Physicians Nuclear, Biological and Chemical Task Force). 2001. Developing Objectives, Content, and Competencies for the Training of Emergency Medical Technicians, Emergency Physicians, and Emergency Nurses to Care for Casualties Resulting from Nuclear, Biological, or Chemical (NBC) Incidents. Dallas, TX: Department of Health and Human Services, ACEP.
ACEP. 2005. Nuclear, Biological, and Chemical Terrorism. [Online]. Available: http://www.acep.org/webportal/PatientsConsumers/HealthSubjectsByTopic/NuclearBiologicaland-ChemicalTerrorism/default.htm [accessed July 7, 2005].
Ackermann RJ, Kemle KA, Vogel RL, Griffin RC Jr. 1998. Emergency department use by nursing home residents. Annals of Emergency Medicine 31(6):749–757.
AHA (American Hospital Association). 2001. Public Health System’s Capacity to Respond to Bioterrorism. Committee on Government Reform: Subcommittee on Technology and Procurement Policy. Chicago, IL: AHA.
AHRQ (Agency for Healthcare Research and Quality). 2004. Optimizing Surge Capacity: Hospital Assessment and Planning. Bioterrorism and Health System Preparedness (Issue Brief No. 3, AHRQ Publication No. 04-P008). Rockville, MD: AHRQ. [Online]. Available: http://www.ahrq.gov/news/ulp/btbriefs/btbrief3.htm [accessed: May 20, 2006].
AHRQ. 2005. Bioterrorism and Other Public Health Emergencies: Altered Standards of Care in Mass Casualty Events. Rockville, MD: AHRQ.
Alexander AJ, Bandiera GW, Mazurik LA. 2005. A multiple disaster training exercise for emergency medicine residents: Opportunity knocks. Academic Emergency Medicine 12(5):404–409.
AMA (American Medical Association). 2003. AMA Announces New Emergency and Disaster Preparedness Coursework for Physicians and Other Health Care Professionals. [Online]. Available: http://www.ama-assn.org/ama/pub/article/print/1616-7771.html [accessed December 9, 2003].
Arkin WM. 2005. Michael Brown Was Set Up: It’s All in the Numbers. [Online]. Available: http://blogs.washingtonpost.com/earlywarning/2005/09/michael_brown_w.html [accessed November 1, 2005].
Arnold JL, Lavonas E. 2004. CBRNE: Personal Protective Equipment. [Online]. Available: http://www.emedicine.com/emerg/topic894.htm [accessed May 20, 2006].
Asplin BR, Knopp RK. 2001. A room with a view: On-call specialist panels and other health policy challenges in the emergency department. Annals of Emergency Medicine 37(5):500–503.
Associated Press. 2006a. Four Bodies Found Since Dec. 21; Katrina Death Toll Now 1,326. [Online]. Available: http://www.katc.com/global/story.asp?s=4317545&ClientType=Printable [accessed May 1, 2006].
Associated Press. 2006b. Band Ex-Manager Sentenced to Four Years in R.I. Club Fire Case. [Online]. Available: http://www.usatoday.com/news/nation/2006-05-09-fire-hearing_x.htm [accessed May 11, 2006].
Auf der Heide E. 2006. The importance of evidence-based disaster planning. Annals of Emergency Medicine 47(1):34–49.
Augustine J, Kellermann A, Koplan J. 2004. America’s emergency care system and severe acute respiratory syndrome: Are we ready? Annals of Emergency Medicine 43(1):23–26.
Barthell EN, Cordell WH, Moorhead JC, Handler J, Feied C, Smith MS, Cochrane DG, Felton CW, Collins MA. 2002. The frontlines of medicine project: A proposal for the standardized communication of emergency department data for public health uses including syndromic surveillance for biological and chemical terrorism. Annals of Emergency Medicine 39(4):422–429.
BBC News. 2005. Sarin Attack Remembered in Tokyo. [Online]. Available: http://news.bbc. co.uk/2/hi/asia-pacific/4365417.stm [accessed May 1, 2006].
BBC News. 2006a. Bali Death Toll Set at 202. [Online]. Available: http://news.bbc.co.uk/1/hi/in_depth/asia_pacific/2002/bali/default.stm [accessed May 1, 2006].
BBC News. 2006b. Q&A: Bird Flu. [Online]. Available: http://news.bbc.co.uk/2/hi/health/3422839.stm [accessed May 1, 2006].
Bravata DM, McDonald K, Owens DK. 2004a. Regionalization of Bioterrorism Preparedness and Response. Rockville, MD: Agency for Healthcare Research and Quality.
Bravata DM, McDonald KM, Smith WM, Rydzak C, Szeto H, Buckeridge DL, Haberland C, Owens DK. 2004b. Systematic review: Surveillance systems for early detection of bioterrorism-related diseases. Annals of Internal Medicine 140(11):910–922.
Broder DS. 2006, July 16. Unprepared for the attacks: Preparing for flu pandemic. The Washington Post. P. A11.
Cass D. 2005. Once upon a time in the emergency department: A cautionary tale. Annals of Emergency Medicine 46(6):541–543.
CDC (Centers for Disease Control and Prevention) National Center for Injury Control and Prevention. 2006. Presentation at the meeting of the Surge Capacity Expert Meeting. Atlanta, GA: CDC.
CDC. 2005. Severe Acute Respiratory Syndrome (SARS). [Online]. Available: http://www.cdc. gov/ncidod/sars/ [accessed October 15, 2005].
CNN.com. 2002. Anthrax Terror Remains a Mystery. [Online]. Available: http://archives.cnn.com/2002/US/03/26/anthrax.investigation/ [accessed March 14, 2006].
CNN.com. 2005a. Tsunami Deaths Soar Past 212,000. [Online]. Available: http://www.cnn.com/2005/WORLD/asiapcf/01/19/asia.tsunami/ [accessed May 1, 2005].
CNN.com. 2005b. Four Sought in Attempted Attacks: Police Say Man Shot and Killed in Underground Not One of Four. [Online]. Available: http://www.cnn.com/2005/WORLD/europe/07/22/london.tube/index.html [accessed May 1, 2006].
DePalma RG, Burris DG, Champion HR, Hodgson MJ. 2005. Blast injuries. New England Journal of Medicine 352(13):1335–1342.
Derlet RW, Richards JR. 2000. Overcrowding in the nation’s emergency departments: Complex causes and disturbing effects. Annals of Emergency Medicine 35(1):63–68.
DHS (U.S. Department of Homeland Security). 2004. National Response Plan. Washington, DC: DHS.
DHS. 2005a. Metropolitan Medical Response System (MMRS): The First Decade (1995–2005). Washington, DC: DHS.
DHS. 2005b. National Planning Scenarios: Created for Use in National, Federal, State, and Local Homeland Security Preparedness Activities. Washington, DC: DHS.
Donovan K. 2003, April 19. How world let virus spread. Toronto Star. P. A.01.
Emergency Management Strategic Healthcare Group, Veterans Health Administration, Department of Veterans Affairs. 2005. Overview of EMSHG and the 4th Mission. [Online]. Available: http://www1.va.gov/emshg/docs/EMSHGOverview.ppt#256,1,Overview of EMSHG and the 4th Mission [accessed March 1, 2005].
ER One. 2005, December 13. The Washington Post. P. A26.
Feliciano DV, Anderson GV Jr, Rozycki GS, Ingram WL, Ansley JP, Namias N, Salomone JP, Cantwell JD. 1998. Management of casualties from the bombing at the centennial Olympics. American Journal of Surgery 176(6):538–543.
Frykberg ERMF. 2004. Principles of mass casualty management following terrorist disasters. Annals of Surgery 239(3):319–321.
GAO (U.S. Government Accountability Office). 2003a. Hospital Emergency Departments: Crowded Conditions Vary Among Hospitals and Communities. Washington, DC: GAO.
GAO. 2003b. Hospital Preparedness: Most Urban Hospitals Have Emergency Plans but Lack Certain Capacities for Bioterrorism Response. Washington, DC: GAO.
GAO. 2003c. Infectious Diseases: Gaps Remain in Surveillance Capabilities of State and Local Agencies (GAO-03-1176T). Washington, DC: GAO.
Garrison H, Runyan C, Tintinalli J, Barber C, Bordley W, Hargarten S, Pollock D, Weiss H. 1994. Emergency department surveillance: An examination of issues and a proposal for a national strategy. Annals of Emergency Medicine 24(5):849–856.
Geiger J. 2001. Terrorism, biological weapons, and bonanzas: Assessing the real threat to public health. American Journal of Public Health 91(5):708–709.
Ginaitt PT. 2005. Statewide Emergency Preparedness in Rhode Island: Lessons Learned “The Station” Nightclub Fire. Presentation, Rhode Island Hospital Association. [Online]. Available: http://www.emlrc.org/pdfs/disaster2005presentations/RhodeIslandStationClubFire-LessonsLearned.pdf [accessed May 20, 2006].
Greenberg MI, Hendrickson RG, CIMERC, Drexel University Emergency Department Terrorism Preparedness Consensus, Panel. 2003. Report of the Cimerc/Drexel University Emergency Department Terrorism Preparedness Consensus Panel. Academic Emergency Medicine 10(7):783–788.
Gursky, E. 2004. Hometown Hospitals: The Weakest Link? Bioterrorism Readiness in America’s Rural Hospitals. Washington, DC: National Defense University, Center for Technology and National Security Policy.
Gutierrez de Ceballos JP, Turegano-Fuentes F, Perez-Diaz D, Sanz-Sanchez M, Martin-Llorente C, Guerrero-Sanz JE. 2004. 11 March 2004: The terrorist bomb explosions in Madrid, Spain—an analysis of the logistics, injuries sustained and clinical management of casualties treated at the closest hospital. Critical Care 8.
Gutman D, Biffl WL, Suner S, Cioffi WG. 2003. The station nightclub fire and disaster preparedness in Rhode Island. Medicine and Health, Rhode Island 86(11):344–346.
Henning KJ. 2003. Syndromic Surveillance. Microbial Threats to Health: Emergence, Detection, and Response. Washington, DC: National Academy Press.
Hick JL, Hanfling D, Burstein JL, DeAtley C, Barbisch D, Bogdan GM, Cantrill S. 2004. Health care facility and community strategies for patient care surge capacity. Annals of Emergency Medicine 44(3):253–261.
Hirschkorn P. 2003. New York Reduces 9/11 Death Toll by 40. [Online]. Available: http://www.cnn.com/2003/US/Northeast/10/29/wtc.deaths/ [accessed May 1, 2006].
Horton DK, Burgess P, Rossiter S, Kaye WE. 2005. Secondary contamination of emergency department personnel from o-chlorobenzylidene malononitrile exposure, 2002. Annals of Emergency Medicine 45(6):655–658.
HRSA (Health Resources and Services Administration). A 2002 National Assessment of State Trauma System Development, Emergency Medical Services Resources, and Disaster Readiness for Mass Casualty Events. Rockville, MD: HRSA.
HRSA. 2006. National Bioterrorism Hospital Preparedness Program. [Online]. Available: http://www.hrsa.gov/bioterrorism/ [accessed April 16, 2006].
IOM (Institute of Medicine). 2002. Preparing for Terrorism: Tools for Evaluating the Metropolitan Medical Response System. Washington, DC: The National Academies Press.
IOM. 2004. Learning from SARS: Preparing for the Next Disease Outbreak. Workshop Summary. Washington, DC: The National Academies Press.
Insurance Information Network of California. 2006. Earthquakes. [Online]. Available: http://iinc.org/pdf/EQ%20Kit%20final.updated.pdf [accessed May 1, 2006].
Jacobs LM, Burns KJ, Gross RI. 2003. Terrorism: A public health threat with a trauma system response. The Journal of Trauma, Injury, Infection, and Critical Care 55:1014–1021.
Jordan LJ. 2006, January 2. Homeland security to re-prioritize grants. Washington Dateline.
Kaji AH, Waeckerle JF. 2003. Disaster medicine and the emergency medicine resident. Annals of Emergency Medicine 41(6):865–870.
Kaji AH, Lewis R. 2004. Hospital disaster preparedness in Los Angeles County, California. Annals of Emergency Medicine 44(4).
Kanter RM, Heskett M. 2002. Washington Hospital Center (B): The Power of Insight. Boston, MA: Harvard Business School.
The Lewin Group. 2002. Emergency Department Overload: A Growing Crisis, the Results of the AHA Survey of Emergency Department (ED) and Hospital Capacity. Washington, DC: American Hospital Association.
McHugh M, Staiti AB, Felland LE. 2004. How prepared are Americans for public health emergencies? Twelve communities weigh in. Health Affairs (Millwood, VA) 23(3):201–209.
Niska RW, Burt CW. 2005. Bioterrorism and mass casualty preparedness in hospitals: United States, 2003. Advance Data (364):1–14.
ORHP (Office of Rural Health Policy). 2002. Rural Communities and Emergency Preparedness. Rockville, MD: ORHP.
OSHA (Occupational Safety and Health Administration). 2005. OSHA Best Practices for Hospital-Based First Receivers of Victims from Mass Casualty Incidents Involving the Release of Hazardous Substances. Washington, DC: OSHA.
Pangi R. 2002. Consequence Management in the 1995 Sarin Attacks on the Japanese Subway System (BCSIA Discussion Paper 2002–4, ESDP Discussion Paper ESDP-2002–01).Boston, MA: Harvard University, John F. Kennedy School of Government.
Phillips S, Lavin R. 2004. Readiness and response to public health emergencies: Help needed now from professional nursing associations. Journal of Professional Nursing 20(5):279–280.
Rand Corporation. 2004. RAND Study Shows Compensation for 9/11 Terror Attacks Tops $38 Billion; Businesses Receive Biggest Share. [Online]. Available: http://www.rand.org/news/press.04/11.08b.html [accessed May 1, 2006].
Rivera A, Char D. 2004. Emergency department disaster preparedness: Identifying the barriers. Annals of Emergency Medicine 44(4).
Schur C. 2004. Understanding the Role of the Rural Hospital Emergency Department in Responding to Bioterrorist Attacks and Other Emergencies: A Review of the Literature and Guide to the Issues. Bethesda, MD: NORC Walsh Center for Rural Health Analysis.
Schur CL, Berk ML, Mueller CD. 2004. Perspectives of Rural Hospitals on Bioterrorism Preparedness Planning (W Series, No. 4). Bethesda, MD: NORC Walsh Center for Rural Health Analysis.
Shute N, Marcus MB. 2001. Crisis in the ER. Turning away patients. Long delays. A surefire recipe for disaster. U.S. News & World Report 131(9):54–61.
Suner S, Williams K, Shapiro MM, Kobayashi L, Woolard R, Sullivan F. 2004. Effect of personal protective equipment (PPE) on rapid patient assessment and treatment during a simulated chemical weapons of mass destruction (WMD) attack. Academic Emergency Medicine 11(5):605.
Talan D, Moran G, Mower W, Newdow M, Ong S, Slutsker L, Jarvis W, Conn L, Pinner R. 1998. EMERGEncy ID NET: An emergency department-based emerging infections sentinel network. Annals of Emergency Medicine 32(6):703–711.
Teague DC. 2004. Mass casualties in the Oklahoma City bombing. Clinical Orthopaedics & Related Research (422):77–81.
Terndrup T, Nafziger S, Weissman N, Casebeer L, Pryor E. 2005. Online bioterrorism continuing medical education: Development and preliminary testing. Academic Emergency Medicine 12(1):45–50.
Times Foundation. 2005. Kashmir Earthquake: A Situation Report. India: The Times Group.
Treat KN, Williams JM, Furbee PM, Manley WG, Russell FK, Stamper CD Jr. 2001. Hospital preparedness for weapons of mass destruction incidents: An initial assessment. Annals of Emergency Medicine 38(5):562–565.
U.S. Department of State. 2005a. Patterns of Global Terrorism 2001. [Online]. Available: http://www.state.gov/documents/organization/10319.pdf [accessed November 1, 2005].
U.S. Department of State. 2005b. Patterns of Global Terrorism 2002. [Online]. Available: http://www.state.gov/documents/organization/20177.pdf [accessed November 1, 2005].
U.S. Department of State. 2005c. Patterns of Global Terrorism 2003. [Online]. Available: http://www.state.gov/documents/organization/31912.pdf [accessed November 1, 2005].
Waeckerle JF. 1991. Disaster planning and response. New England Journal of Medicine 324(12):815–821.
Waeckerle JF, Seamans S, Whiteside M, Pons PT, White S, Burstein JL, Murray R, Task Force of Health Care and Emergency Services Professionals on Preparedness for Nuclear BaC Incidents. 2001. Executive summary: Developing objectives, content, and competencies for the training of emergency medical technicians, emergency physicians, and emergency nurses to care for casualties resulting from nuclear, biological, or chemical incidents. Annals of Emergency Medicine 37(6): 587–601.
WHO (World Health Organization). 2005. Summary of Probable SARS Cases with Onset of Illness from 1 November 2002 to 31 July 2003. [Online]. Available: http://www.who.int/csr/sars/country/table2004_04_21/en/index.html [accessed November 10, 2005].
Zavotsky KE. 2000. Developing an ED training program: How to “grow your own” ED nurses. Journal of Emergency Nursing 26(5):504–506.
































