SOCIOECONOMIC IMPACTS OF DEPLOYMENT ON SERVICE MEMBERS AND SPOUSES
![]()
This chapter examines the social and economic impacts of deployment to Operation Enduring Freedom (OEF), Operation Iraqi Freedom (OIF), and Operation New Dawn (OND) on individual service members and their spouses. It also assesses estimates of the long-term costs associated with deployment and the signature wounds of the conflicts, posttraumatic stress disorder (PTSD), traumatic brain injury (TBI), and depression. Costs of those and other injuries can be borne by many individuals beyond the afflicted service member. The chapter presents those assessments based on the current state of knowledge in these areas, which continues to evolve rapidly. The chapter’s main findings are the following:
• Veterans of the post-9/11 period suffer higher rates of unemployment than nonveterans, but veterans who are employed appear to earn higher wages than their nonveteran counterparts, after adjusting for demographic characteristics.
• Long deployments, PTSD, and disability are associated with unemployment.
• Activated reservists may have lower earnings when they return from active duty if they have PTSD.
• Studies of veterans from earlier periods suggest that negative impacts of deployment to OEF, OIF, and OND and combat exposure may be revealed later in the life cycles of today’s veterans and service members. Surveillance systems should be in place.
• The budgetary costs of providing care for injured veterans are significant and will rise over time. The uncompensated socioeconomic costs of war injuries may be large. Planning for the funding and provision of care should take a long-term perspective.
• Spouses of service members face an array of challenges that are often made more acute by deployment, and their socioeconomic well-being can suffer. Spouses of veterans face similar issues and impacts, about which less is known.
To examine socioeconomic impacts, the committee sought to measure the impact of deployment to OEF, OIF, and OND on several outcomes: veterans’ civilian employment if separated from the military; service members’ earnings and other income both during and following service; their household wealth and finances; their acquired education and access to further education; the incidence of homelessness among separated veterans; the incidence of criminal behavior; and spousal employment, earnings, and education. The committee first reviewed extant studies of deployment-related outcomes along these dimensions. Because there are relatively few population-based studies of socioeconomic well-being among veterans of
OEF, OIF, and OND, the committee also examined other studies whose findings seemed likely to generalize to OEF, OIF, and OND population.
The committee also reviewed recent studies of the short- and long-term budgetary and socioeconomic costs of war-related injuries and trauma. Budgetary costs include the costs of health care treatments and disability benefits paid by the Department of Veterans Affairs (VA), which reflect the direct cost of caring for injured veterans. The socioeconomic costs of injuries consist of all other negative impacts stemming from injuries that could have been avoided had the injury not occurred. There is agreement in the literature that short-run budgetary costs of caring for wounded veterans are large but affordable. If past trends continue, the long-run budgetary costs are likely to be much larger, although specific predictions of long-term costs associated with PTSD, and especially TBI, are highly uncertain. The socioeconomic costs of injury are controversial but deserving of more study given the nature of psychological wounds and their prevalence in the recent conflicts.
In the following sections, the committee first presents its assessments of the social and economic impacts of deployment on individual service members. Second, the committee discusses socioeconomic impacts of deployment on military spouses and speculates about the impacts on spouses of veterans. Third, the committee discusses estimates of short- and long-term costs associated with war injuries. Fourth and finally, the committee highlights gaps in knowledge and articulates a research plan for increasing understanding of the impacts and costs of deployment.
SOCIOECONOMIC IMPACTS OF DEPLOYMENT ON SERVICE MEMBERS
This section presents what is known about how deployment to OEF, OIF, and/or OND has affected the socioeconomic well-being of service members and veterans. There are a number of reasons why deployment might have affected outcomes, and, in particular, the earnings and employment status of veterans, their level of education, and their wealth and risk of homelessness (see Chapter 7). Military service of any kind represents a break in civilian labor force participation, which may carry an earnings penalty if military experience is less rewarded in the labor market than civilian experience. For enlistees, time spent in the military could postpone or preclude further schooling. The psychological and physical wounds associated with deployment to a combat or war zone might directly reduce human capital, impair veterans’ ability to work, and generate psychosocial impediments to functioning in civilian society. Unreimbursed medical expenses associated with mental or physical injuries may absorb wealth, and household finances might be strained by long and frequent absences of deployed service members. It also is possible that military service could positively affect socioeconomic outcomes. Deployment to a war zone raises military compensation, and Congress has also authorized generous education subsidies for certain cohorts, including post-9/11 veterans. The net effect of deployment on socioeconomic outcomes could therefore be either positive or negative, and it could change over the life cycles of surviving veterans.
Readjusting to civilian life is the first challenge faced by separated service members, and several conditions associated with combat or deployment-related stress may impact their socioeconomic well-being in the near term. Sayer et al. present a snapshot of readjustment problems faced by a sample of OEF and OIF combat veterans who had sought and received VA medical care (Sayer et al., 2010). Respondents were home from their most recent deployment for
a median of 42 months, and 22% reported more than one deployment to Iraq or Afghanistan. About one-quarter (27%) reported a formal PTSD diagnosis, while 7% had a substance use disorder diagnosis, but a screening tool used in the survey estimated higher incidences of PTSD (41%) and substance abuse (38%). More than one-third (40%) reported at least some difficulty readjusting to civilian life within the last 30 days, and many reported at least some difficulty getting along with a spouse or partner (42%), or with relatives (34%), or with finding meaning in life (42%). Roughly a third reported at least some productivity problems, including difficulty keeping a job and problems completing the tasks needed for home, work, or school.
Perhaps the most visible indicator of socioeconomic well-being among recent veterans is their employment status, which is measured and reported monthly in the Current Population Survey (CPS) of the Bureau of Labor Statistics (BLS). The CPS does not ask about deployment, so little can be said about the specific impacts of deployment to OEF, OIF, and OND based on these data, but the available literature has produced some useful insights. Others studies using different data have also evaluated the effect of military service and deployment on earnings. For those on active duty, earnings rise mechanically with deployment through the combat zone tax exclusion and the additions of imminent danger pay or hostile fire pay. For National Guard and reserves, deployment could raise or lower earnings depending on how military pay compares to the civilian pay that is foregone during deployment. For all service members, deployment-related injuries may reduce future earnings ability, although the VA disability system is designed to replace such losses. The committee found little research that had explicitly examined the impact of deployment to these recent wars on educational attainment, wealth, homelessness, or crime, but this chapter presents some related findings that are related and plausibly relevant. For example, earlier research has suggested that veterans may obtain education that is less valuable than that obtained by nonveterans. Patterns of homelessness among all US veterans suggest that younger veterans are relatively more at risk, which suggests that veterans who deployed to OEF, OIF, and OND might be at greater risk of being homeless (see Chapter 7).
Employment
When recent veterans or recently separated reserve component soldiers return to their communities, in addition to readjusting to family life and personal relationships, they also must readjust to the civilian workforce. Recently separated veterans, who probably enlisted at a young age, may be entering the civilian workforce for the first time following separation. Of those returning, 20% or more have psychiatric symptoms, and nearly as many (18%) have problems with steady employment (Tanielian and Jaycox, 2008). The Uniformed Services Employment and Reemployment Rights Act (USERRA) requires that employers accept recently separated reserve component service members back into their previously held positions, but that does not necessarily guarantee seamless readjustment.
As described in the committee’s Phase 1 report, reserve service members who have been activated are more likely to be unemployed after they have returned from their deployments, a relationship that appears to strengthen as the term of deployment lengthens (Loughran and Klerman, 2008). Other researchers have shown that job loss was associated with PTSD and poorer mental health among National Guard troops who had deployed in 2005–2007 (Riviere et al., 2011). To what extent that relationship represents a causal effect of deployment-related trauma on employment status or reverse causality of poor mental health by job loss is technically unclear. But it seems likely that deployed veterans have difficulties finding and keeping jobs
because they suffer combat-related disabilities. Adler et al. showed that disabled OEF and OIF veterans have difficulties with work-related tasks, for example (Adler et al., 2011).
Burnett-Zeigler et al. looked at employment status among 585 recently separated (45–60 days) National Guard service members (Burnett-Zeigler et al., 2011). Less than half (41%) of the participants were employed at the time of the survey. Service members below age 30 were much less likely to be employed (29%) than those aged 31 or older (57%). Those that reported recent combat exposure were more likely to be employed (46%) compared to those that did not (36%). Surprisingly, physical- and mental-health status, PTSD, depression, alcohol use, and anxiety were not significantly associated with employment status, although those with either better mental health or poorer physical health were more likely to be employed full rather than part time. As those authors noted, negative effects of mental health status, alcohol use, recent combat exposure, and PTSD might require more time before they measurably affect employment, because many of those characteristics are themselves unobservable to employers and probably affect maintaining employment more than obtaining it.
How employers might perceive veterans in the hiring pool is the subject of research by Kleykamp (2009). The author examined how prior military experience might influence a potential employer’s interest in an employee candidate in New York City. Fabricated resumes were faxed in response to classified job listings in an effort to record callback rates for veteran vs nonveteran applicants, where military experience was classified as either combat or administrative. Resumes were matched on education, work experience, race (based on name), sex, and approximate age and were submitted in matched pairs. The researchers measured differences between veterans and their nonveteran peers in call backs or emails from the potential employers. There was no significant difference in callback rates among white, black, or Hispanic applicants with clerical (noncombat) experience in veterans vs nonveterans. Among combat veterans, there was no significant difference in callback rates for white and Hispanic applicants. However, 13 black civilian applicants (10%) received callbacks while black combat veterans did not receive any callbacks, a statistically significant difference that may represent biased perceptions. Combat-related trauma such as PTSD appears to affect employability and/or productivity, and some research suggests there may have been differential effects of combat exposure by race in the Vietnam era (Rohlfs, 2010). If employers in fact perceive recent veterans as more likely to suffer from invisible war wounds, they might discriminate in hiring.
Resnick and Rosenheck (2008) looked at the relationship between PTSD and employment among veterans in Veterans Health Administration Compensated Work Therapy, a vocational rehabilitation program. They found that veterans with PTSD were 19% less likely to be employed upon completion of the program compared to veterans without a PTSD diagnosis. Smith et al. (2005) examined the effect of PTSD symptom severity on employment outcomes among 325 Vietnam veterans. For every 10-point rise in Clinician-Administered PTSD Scale (CAPS) score, which is considered a meaningful increase in PTSD symptoms, the likelihood of no work increased 5.9 percentage points, the probability of part-time work decreased 2.1 percentage points, and the probability of full-time work decreased 3.8 percentage points. Interestingly, CAPS scores had no significant association with earnings once hired.
Although PTSD diagnosis among OEF, OIF, and OND veterans hovers around 10–20% (Hoge et al., 2004), there is little to no direct evidence of latent effects of deployment on employment. In an unpublished working paper, Edwards (2012) examines patterns of socioeconomic well-being among 753 veterans of the post-9/11 period surveyed in the 2010
National Survey of Veterans (NSV). The 2010 NSV sampled a nationally representative cross section of all living veterans between late 2009 and early 2010. Among the 453 veterans who self-reported being deployed in support of OEF and/or OIF, rates of employment and unemployment were both about 1 percentage point higher than among post-9/11 veterans who had not deployed, but the differences were statistically indistinguishable. Correcting for different underlying propensities of deployment across demographic groups revealed some limited evidence of greater employment rates among the deployed. Adjusting for differences in demographic characteristics switched the sign of the association but left the result statistically insignificant.
There are clear gaps in research concerning how deployment and physical or mental trauma may affect later employment. One key shortcoming is that there are few studies examining how prevention or treatment programs early in the postdeployment period may differentially affect later employment. Tanielian and Jaycox (2008) and related studies by the RAND Corporation have addressed employment and health dynamics over a 2-year window, but further research is needed. A second issue concerns questions of preexisting robustness or predisposition among service members prior to deployment. Military service might attract resilient individuals, or it might reflect difficulties maintaining civilian employment, or both might be true for different service members. Analysis of pre-service screening information linked to post-service outcomes, to disentangle causes and effects, should be a top research priority.
Employment patterns among veterans relative to nonveterans or to all civilians are reported in the monthly CPS of the BLS and in the annual August supplement to the CPS, which asks detailed questions about disability ratings and membership in the National Guard or reserve. Those data reveal the challenges that are broadly faced by veterans of the post-9/11 era and particularly by young veterans. In 2011, the unemployment rate among all post-9/11 veterans aged 18 and over was one-third higher than among equivalent nonveterans, 12.1% compared to 8.7%. Among young veterans aged 18–24, the rate was almost twice as high, 30.2% compared to 16.1% (BLS, 2012a). Monthly statistics on veterans’ employment are reported without seasonal adjustment and tend to fluctuate.
Part of the observed differences in employment rates may be driven by basic demographic differences between veterans and nonveterans beyond age and sex, such as educational attainment and race or ethnicity. After controlling for all demographic differences and other compositional factors in the CPS data, Kleykamp (2012) reveals that male veterans of the post-9/11 era between the ages of 18 and 40 faced a 2.6 percentage point disadvantage in unemployment rates, 10.6% compared to 8% for comparable nonveterans, over the period 2005– 2010. For female veterans in the same age group, the difference was even more stark: 11.5% compared to 7%, a difference of 4.5 percentage points.
A recent RAND study examines the effects on employment of the 2007 expansion of the Work Opportunity Tax Credit (WOTC) (Heaton, 2012). The expansion provided a maximum credit of $4,800 toward the hiring of any veteran drawing VA disability benefits who had been discharged within the previous 12 months or unemployed for 6 or more of those months. In contrast with standard employment tax credits targeting disadvantaged workers whose effectiveness at raising employment has often been empirically ambiguous (Heaton, 2012; Katz, 1998; Neumark, 2011), the 2007 WOTC expansion appears to have raised employment by some 2 percentage points, on average, among disabled veterans above what it would have been, with
robustness across specifications. Impacts on veterans younger than 40 or on female veterans were not statistically significant. The effects of a 2009 extension of the WOTC to cover unemployed veterans more broadly and a related extension and expansion under the Vow to Hire Heroes Act of 2011 remain unclear and await future research efforts.
Earnings
Researchers at RAND have found that reserve service members benefited in the short and long runs from being activated, but they also suffered lower earnings in the year immediately after returning from active duty during the OEF and OIF era. As described in the Phase 1 report, those researchers have demonstrated that reserve service members likely earned more after they were activated in the OEF or OIF era than they did before. The researchers have begun more recently to assess how the earnings of activated reservists change over time when they return to civilian life (Loughran and Klerman, 2010). According to that research, reservists earn less in the first year after they return from active duty than do reservists who were not activated. Over time, however, they earn more. Taken together, these findings suggest that deployment negatively affects earnings only in the year immediately after the end of active duty.
RAND researchers have also explored how the earnings of activated reservists are affected by PTSD symptoms, suggesting that deployed reservists have lower earnings after deployment if they have those mental health symptoms (Heaton and Loughran, 2010). The researchers combine information derived from the postdeployment health assessment reports with administrative data on earnings for approximately 300,000 reservists who served between 2003 and 2006. They compare results from cross-sectional analyses with those from regressions that employ fixed effects and instrumental variables methods to take account of nonrandom selection. According to that research, reservists with PTSD had slightly lower earnings than those who did not have the disorder in the year immediately after they returned from active duty. In subsequent years, they were more likely to leave the armed forces, and thus also experienced a drop in their military earnings, which meant that they earned less overall (Heaton and Loughran, 2010).
The 2010 NSV asked about household income but not earnings per se. Edwards (2012) found that household income was lower among veterans who deployed to OEF and/or OIF, but that the penalty was due to demographic differences associated with deployment, such as age and sex. Household income would also include any lost earnings replaced by disability benefits, making it difficult to tell what might have happened to earnings as a result of deployment-related mental or physical trauma. But the 2010 NSV data indicates lower VA disability among post-9/11 veterans who deployed to OEF and/or OIF, or essentially a healthy warrior effect.
A more recent RAND study (Heaton et al., 2012) used a causal estimation approach to analyze whether veteran’s disability compensation was sufficient to cover lost productivity among returning service members with combat-related injuries, measured as life-altering or lifethreatening combat injuries on the Post-Deployment Health Assessment. The analysis found that while lost earnings due to combat-related injuries were substantial, disability payments more than replaced lost earnings for the average wounded veteran. But disability payments did not quite replace household earnings losses among those with less severe injuries, although lost earnings were also lower for those with less severe injuries. The RAND study did not isolate the effects for veterans with PTSD or other mental health disabilities. However, a 2007 Center for
Naval Analysis study (Christensen et al., 2007) found that disability compensation for veterans classified with a primary physical disability adequately replaced expected lifetime earnings, while disability compensation for veterans with a primary mental disability compensated for only about 80–90% of expected lifetime earnings.
In CPS data, male and female veterans of the post-9/11 era had higher wages than observationally equivalent nonveterans, 6% in the case of males and 5% for females, during 2005–2010 (Kleykamp, 2012). This result is notable in light of reduced employment among the same veterans during the same period, and it could represent the effects of heterogeneity among veterans, with employers selecting healthy veterans with transferrable skills.
Loughran et al. (2011) present a new look at the causal effect of military service on the earnings and education of individuals who applied for active-component enlistment between 1989 and 2003. They compare subsequent outcomes among enlistees with outcomes among applicants who chose not to enlist, an extension of the method proposed by Angrist (1998), and they reveal sustained increases in earnings associated with military service that are concentrated among enlistees who are still serving in the military and among enlistees with lower AFQT scores. Those effects could represent a compensating wage differential paid for military service, the value added of skills imparted during military service, or a combination of both.
The rise in the use of private contractors by the US government to provide security and other services during recent overseas engagements may be important for veterans’ earnings, but the committee is unaware of any systematic study of this issue. Earnings may be high for such occupations, but presumably so are the risks. To the extent they include such individuals, labor market surveys may be providing measures of average earnings that present a skewed picture of the typical experience among separated veterans.
Educational and Vocational Needs
Veterans who served during the OEF and OIF period might have greater educational attainment than they might otherwise because of the educational benefits that are available to veterans under the different forms of the GI Bill. Until September 2009, such veterans could draw on funding from the Montgomery GI Bill. After that, they have had access to the more generous funding available through the Post-9/11 GI Bill era. Yet apparently no research has systematically examined how these benefits may have affected veterans’ education. A recent story published in the Chronicle of Higher Education suggests that approximately 270,000 students used benefits from the Post-9/11 GI Bill in 2009–2010. The same article reports that among the top 15 institutions receiving GI Bill benefits, 7 were for-profit organizations and 5 were community colleges (Sewall, 2010). According to focus groups conducted by RAND, veterans credit the more generous benefits of the Post-9/11 GI Bill with inspiring them to obtain higher education (Steele et al., 2011). One congressional study, however, points out that veterans have disproportionately used the funding to obtain education from private for-profit educational institutions, which have significantly lower retention rates than do nonprofit institutions (Senate Health Education Labor and Pension Committee, 2011). Recently, President Obama issued an Executive Order (April 27, 2012) intended to provide mechanisms for “oversight, enforcement and accountability” of the GI Bill and other training and education benefits. Such mechanisms should provide meaningful information about the cost and quality of educational programs.
We know of relatively little research that explicitly examines the effects of serving or being deployed during the OEF and OIF period on educational attainment. One study has, however, assessed the effects of service in a sample that includes veterans who served during the first years of the OEF and OIF period and suggests that the effects might be negative. Among comparable military applicants between 1989 and 2003, those who ultimately enlisted were more likely to get associate’s degrees, and less likely to get bachelor’s degrees following military service than those who did not enlist. Enlistees also finished their education at older ages than did nonenlistees (Loughran et al., 2011). Similarly, Wang et al. (2012) found that military service appears to increase attainment of associate’s degrees. Furthermore, Elman and O’Rand (2004) have demonstrated that people benefit less from earning associate’s degrees than they do from earning bachelor’s degrees. They have also shown that people who earn degrees when they are older also do not benefit as much from their education as do people who earn their degrees when they are younger. Thus, more recent veterans may suffer in general from two features of their education: the type of degree and the age at which they receive it.
The 2010 NSV asked about educational attainment and use of VA educational benefits, including among deployed and nondeployed veterans of the post-9/11 era. Edwards (2012) reports that veterans who deployed had fewer years of education than the nondeployed, but that the difference vanishes after controlling for demographic differences. Veterans who deployed were more likely to report using VA educational benefits and more likely to report having completed VA-subsidized education or training programs.
According to CPS data from 2005–2010, post-9/11 veterans were more likely to be enrolled in college than their civilian counterparts after controlling for other observable differences (Kleykamp, 2012). Male veterans between ages 18 and 40 were more likely (31.4% vs 22.8%) to be enrolled in college as were nonveterans, and there were similar findings for female veterans (39.2% vs 27.7%), although the latter differences were statistically insignificant, possibly because of a stronger effect of marital status or other covariates.
Veterans have access to vocational training through the VA and through a variety of individual veterans service organizations, although the efficacy of these programs is unclear. The Veterans Opportunity to Work (VOW) to Hire Heroes Act (2011) included provisions for additional training assistance to long-term unemployed veterans between the ages 35 and 60 who may not be eligible for the GI Bill, through the Veterans Retraining Assistance Program. This program was only recently implemented, and no evaluation of its efficacy is available. Veterans with at least a 10% service-connected disability rating may be eligible for the Vocational Rehabilitation and Employment (VR&E, also called VetSuccess) program. The program connects veterans with counselors to develop a plan under one of five tracks (self-employment, reemployment, rapid access to employment, independent living, and employment through longterm services) and to identify and coordinate services to achieve success in that track. The committee is not aware of any research that systematically identifies the vocational training needs of OEF, OIF, and OND veterans and their families, or of research evaluating the efficacy of such education and training programs. However, the GAO has raised concerns that the VR&E program has emphasized training programs over actual employment. In particular, veterans in training programs received subsistence payments while in training and for 2 months during an employment search, while those seeking direct employment did not receive any subsistence payments. Unsurprisingly, given these incentives, 80% of VR&E enrollees were in training programs, while only 7% were in the rapid access to employment program (GAO, 2009).
Further, the GAO highlighted the opacity of VR&E performance measures and a recent change in how rehabilitation outcomes were measured, with the new measures increasing the rate of rehabilitation (GAO, 2009).
Legislation passed in 2008 (Veterans’ Benefits Improvement Act of 2008 in October of 2008, section 334) mandated a 20-year longitudinal study of three cohorts of participants in the VA vocational rehabilitation programs. A baseline report on a cohort of vocational rehabilitation participants in 2010 found that approximately 75% of the 10,793 participants served from the Gulf War era (1990) onward but did not report on OEF and OIF veterans separately. Of the 10,793 participants, 42 were between ages 17 and 21 (0.4%), 1,501 were between ages 22 and 29 (14.4%), and 2,719 were between ages 30 and 39 (26.0%), suggesting that many veterans in the VA vocation rehabilitation program may have served in OEF and/or OIF. The report does not report statistics for OEF or OIF or deployment and does not identify the vocational needs or outcomes of the population of interest in that report.
In the fall of 2012, the military announced a revamping of the transition assistance program (TAP) planned for November that was to focus on enhancing flexibility and guidance for service members in planning their post-service careers (Sheftick, 2012). The reconfiguration is meant to help establish a new model of the military life cycle in which service members start planning earlier in their military careers for separation and post-service employment or entrepreneurship. The committee believes this is a wise endeavor and calls on the DOD to conduct cost-effectiveness studies of the new TAP. Providing earlier advising regarding educational and occupational goals could be a relatively inexpensive way to improve postseparation employment and earnings outcomes.
Household Wealth and Finances
As reported in the committee’s Phase 1 report, the challenges posed by overseas deployment for the finances of military families can be significant. Although deployment typically raises military compensation, the absence of a key family member alone can create liquidity problems for families. To combat predatory lending practices targeting military families short on liquidity, the National Defense Authorization Act for Fiscal Year 2007 implemented new regulations on payday loans made to active duty service members and their families.
The committee is aware of few subsequent studies of the financial well-being of military families or of veterans who deployed to OEF, OIF, and/or OND. Elbogen et al. (2012) examine how positive screenings for major depression, PTSD, and TBI were associated with self-reported measures of financial well-being or stress among 1,388 veterans of the post-9/11 era who responded to the 2009 National Post-Deployment Adjustment Survey. While it remains unclear how veterans with mental health trauma may compare with nonveterans, this study shows they suffer significantly reduced financial well-being compared to other post-9/11 veterans, possibly because of impeded decision-making capabilities. The study also showed that veterans without financial stresses were less likely to report readjustment difficulties like criminal arrest or homelessness.
The 2010 NSV asked veterans of all periods about a few limited aspects of financial wellbeing, including homeownership, the presence of capital income (i.e., interest or dividends), and Internet access at home. As discussed by Edwards (2012), none of those indicators varied
significantly across deployment status. That is consistent with the negligible association between deployment and household income among post-9/11 veterans in those data.
Crime
The committee found no studies reviewing veteran status and criminal behavior among OEF and OIF veterans. However, homelessness, poverty, mental illness, and substance abuse are all predisposing factors for criminal behavior. While the committee is not aware of any studies associating OEF and/or OIF combat exposure with criminal behavior, Egendorf et al. (1981) found that among a sample of noninstitutionalized Vietnam veterans over age 23, 24% of those with heavy combat exposure were arrested after service compared to 10% of those with light or no combat exposure and 14% of comparable nonveterans. Only about 10% of arrests among veterans led to a conviction, but this is likely an underestimate because incarcerated veterans were not included in the study.
Despite the link between combat exposure and subsequent criminal behavior found in some veteran subpopulations (Rohlfs, 2010), veterans as a group are less likely to be incarcerated than nonveterans. The Bureau of Justice Statistics reports that, in 2004, the age-adjusted incarceration rate for veterans was about 10% lower than that for nonveterans (1,253 per 100,000 vs 1,390 per 100,000 respectively) (Noonan and Mumola, 2007). According to that same study, veterans were also somewhat more likely than nonveterans to be serving sentences for violent or sexual crimes, and veterans were more likely than other violent offenders to have victimized women or minors.
The only statistic concerning crime among veterans of OEF and OIF that the committee found was also reported by Noonan and Mumola (2007) and was based on incarceration data for 2004. Given that the conflicts extended well into the following decade, those patterns are unlikely to be broadly informative of criminal behavior among the OEF, OIF, and OND cohort. The study revealed that in 2004, 4% of the veteran population in state and federal prison were veterans of OEF and OIF. Data from the 2004 American Community Survey (Ruggles et al., 2010) indicated that about 8% of all US veterans or resident military in 2004 had served in the post-9/11 era. Although far from a perfect comparison, because one should at a minimum adjust for age-related differences between these subpopulations, this quick look suggests that by 2004, criminal behavior was not disproportionately prevalent among veterans of OEF or OIF.
The dearth of research on saving behavior and finances among service members, recent veterans, and their spouses is noteworthy given the well-known connection between financial planning earlier in life and later-life outcomes. While the short-run financial stresses faced by military families are relatively unique and important, a comprehensive evaluation of their financial planning and well-being is essential for understanding whether differences in later-life well-being may be linked to military service and deployment.
Summary
The existing literature has identified a few impacts of deployment on average socioeconomic outcomes among service members and veterans, but in general the committee finds limited evidence of impacts on outcomes among deployed post-9/11 veterans at this stage of their life cycles. Based on findings in the committee’s Phase 1 report, there are reasons to suspect the true effects may remain latent for some time. In it, the committee showed how the
numbers of war veterans receiving disability benefits has tended to rise strongly with age among all previous war cohorts. Part of that could be attributable to any trend toward more generous disability rating, but the pattern also suggests latent need that unfolds during the course of aging. In the analysis of the 2010 NSV, Edwards (2012) also examines combat exposure and outcomes among post-9/11 veterans and older veterans. The author shows that deployment to OEF and/or OIF is a strong predictor of combat exposure and that combat exposure strongly predicts poorer self-reported health, although not household income, among post-9/11 veterans. Among older veterans of previous conflicts, combat exposure strongly predicts poorer self-reported health, disability, and poorer marital outcomes, although the impact on household income remains insignificant. Altogether, the limited evidence from the 2010 NSV suggests that overseas deployment increases combat exposure, which has had lifelong impacts on socioeconomic wellbeing among older cohorts of war veterans. Whether and how today’s war veterans might differ from earlier cohorts in their resilience are important questions that may be unanswerable until later in their life cycles. The evidence motivates continued vigilance and development of effective surveillance systems.
SOCIOECONOMIC IMPACTS OF DEPLOYMENT ON SPOUSES
As the committee reported in Phase 1, 55–60% of military service members are married (IOM, 2010), and about 60% of post-9/11 veterans in the 2010 NSV were married (Edwards, 2012). Spouses of active-duty service members face frequent relocations and deployment-related absences, and they may be affected by combat-related trauma if it alters the service member’s roles or relationships in the household. Spouses of veterans may face heightened caregiving responsibilities, earnings requirements, or both, if the veteran is wounded or unemployed. Those multiple effects of deployments can impact the employment, earnings, and educational attainment of spouses. There are likely to be similar consequences for other family members, such as parents or siblings.
There are few studies to date that have assessed the specific impacts of deployment to OEF, OIF, and OND on those spousal outcomes. The 2010 NSV included separate questionnaires sent to spouses of active duty service members, veterans, and deceased veterans, but as of 2012 none of the spouse data are publicly available. The Defense Manpower Data Center (DMDC) has conducted several waves of Active Duty Spouse Surveys (ADSS) that might be informative, but there is controversy regarding sampling and weighting techniques in those data and thus the quality of statistical inference (Al Nassir et al., 2012; Losinger, 2010).
Deployments have been cited by military spouses as key factors affecting their employment. Based on a survey of over 1,000 military spouses, Harrell et al. (2004) report that spouses perceive deployments as likely causing interruptions in work, because time must be reallocated to household matters during the absence of the service member. Furthermore, military spouses in the survey believed potential employers were wary of hiring them because of the probability of absences. That could partially explain why military spouses are less likely to be employed than observationally equivalent civilian counterparts (Hosek et al., 2002). They also earn less, possibly because more frequent relocations reduce job search time and the inability to move nearer to a higher wage job. Accelerated and lengthened deployments to OEF, OIF, and OND might thus have reduced employment among military spouses but seem less likely to have affected their earnings. Concerning spousal education, deployments are likely to have impeded
outcomes to the extent they force a reallocation of time away from studies and toward the household (Harrell et al., 2004). Relocations are probably a larger threat to spousal education because of the difficulties inherent in transferring course credit and variation in curricula across educational institutions.
What we know about spousal socioeconomic outcomes specifically associated with deployment to OEF, OIF, and/or OND is limited to observational inference from self-reports in recent waves of the ADSS. The 2009 Quadrennial Quality of Life Review (DOD, 2009) summarizes the characteristics of military spouses in these surveys and provides some perspectives on the effects of accelerated overseas deployments to OEF, OIF, and/or OND. Data from the 2006 ADSS revealed that 19% of all spouses had lost their jobs during their spouse’s most recent deployment, while among spouses of lowest rank enlisted service members, the share was 27%. More than half (55%) said the deployment had an effect on their jobs, and 31% reported a reduction in earnings due to deployment. The causal effects of deployment on those outcomes may be substantially different.
THE COSTS OF WAR-RELATED INJURIES
PAID BY GOVERNMENTS AND INDIVIDUALS
Like medical treatment costs associated with war-related injuries, socioeconomic impacts of injuries or deployment such as those considered in this chapter can also be conceptualized as costs. If deployment causes mental or physical trauma that reduces the ability to work, for example, the lost earnings are a cost borne by the afflicted service member. The system of VA disability benefits is designed to replace those lost earnings. Provided that disabled veterans are reimbursed, such costs will be measured as a traditionally recognized cost of war-related injury: federally provided VA disability benefits. In addition, any Veterans Health Administration (VHA) treatment costs associated with that injury and with other ailments treated by the VA will be measured as federally provided VA benefits. Death and survivor benefits are also budgetary costs of war-related fatalities that are measured in government statistics.
But there are other types of costs of war-related injuries that will not be captured in the VA budget but that are arguably still relevant for policy and well-being. Health economists believe that optimal medical decisions should take into account the complete range of costs associated with ailments regardless of who pays and that a good measure of the cost of an injury is the willingness to pay to avoid it. According to this framework, the cost of a statistical injury, like a lost limb, for example, is the willingness to pay to avoid the risk of losing a limb. The willingness to pay will include the present value of lost earnings attributable to losing a limb, but it will also include the present value of any lost enjoyment associated with losing a limb, such as the inability to type with both hands, or any residual pain and suffering that treatment cannot reverse. In principle, the willingness to pay is the maximum amount an individual would pay for a medical procedure that could completely reverse the ailment. When choosing among a set of treatments that vary in terms of unit price and effectiveness, patients and care providers seeking to maximize the net benefits to the patient should measure the costs of ailments according to this broader definition. The extra cost associated with an injury above and beyond the present value of lost earnings and treatments, which are typically paid by the VA, can be termed the “socioeconomic cost.”
Those distinctions are important for understanding fundamental differences in scope across cost estimates in the literature. Broadly speaking, most studies either measure just the direct treatment costs that are paid by the VA or, less frequently, treatment costs borne by other payers. Fewer studies attempt to measure the indirect costs associated with injury such as lost productivity, emotional costs, family hardship, and other related factors. Measuring the indirect costs is typically more difficult and thus also more controversial, but it provides answers to an important question. Tallying the direct treatment cost reveals how much the government should set aside to care for wounded veterans. Measuring the full costs helps inform optimal treatment strategies for wounded veterans.
In this section, the committee first reviews the literature on total budgetary costs, or the spending by the VA on disability benefits and health care for injured veterans of OEF, OIF, and OND. Then it explores the broader literature on costs of treatment before examining studies of the full costs of injuries and the cost effectiveness of various treatment interventions.
Budgetary Costs of VHA Treatments
Several studies published since the committee’s Phase 1 report have assessed the budgetary costs of caring for service members injured in OEF, OIF, and/or OND, with special emphasis on the cost of medical care provided through VHA. In late 2010, the Congressional Budget Office (CBO, 2010) provided a 10-year projection of VHA spending associated with OEF, OIF, and/or OND deployments based on current policies. In two scenarios that differed by the assumed rate of medical price inflation and force drawdowns, 10-year cumulative costs were $40 billion and $54 billion. Those forecasts assumed the number of treated veterans was 382,000 in 2010 and that treatments that year cost $5,170 per veteran and would rise either at the rate of Medicare price inflation or 30% faster.
By comparison, Stiglitz and Bilmes (2008) had predicted annual medical costs per treated veteran of OEF, OIF, and/or OND of either $3,500 or $5,765 starting in 2007. In a contemporaneous CBO estimate, the average cost was $2,740 that year (CBO, 2007), which had since been revised upward to $3,176 (CBO, 2010), after adjusting for inflation. Today, the estimates of Stiglitz and Bilmes and CBO are broadly consistent because the average cost per enrolled veteran rose at an average annual rate of 16% between 2007 and 2010 according to the CBO statistics. That was much faster than the 6% rate of medical price inflation assumed by Stiglitz and Bilmes and also faster than the 5.5% rate in the current CBO forecast. Short-term aggregate VHA cost forecasts by CBO and Stiglitz and Bilmes are thus now broadly in agreement. Stiglitz and Bilmes also predicted the present value of total lifetime VHA costs associated with OEF and OIF at between $121 billion and $285 billion. The CBO does not produce detailed long-term forecasts of this type, but the rough agreement between current levels and their predicted rates of growth suggests they would not diverge were they produced.
Early in 2012, the CBO released results from a new study of longitudinal data obtained from the VHA on the treatment of PTSD and TBI among OEF, OIF, and OND service members (CBO, 2012). To preserve confidentiality, the data were coded in a way that scrambled effects associated with calendar year, such as medical price inflation or changing eligibility, with effects associated with time in treatment. As a result, it is difficult to be certain about the sources of change in average costs or enrollment through time or during treatment. For example, the average cost of treating TBI rose strongly during the 4 years of treatment in the study, but the CBO argued that was primarily a data artifact reflecting an expansion of the definition of TBI to include milder cases following the shift toward comprehensive screening in 2007.
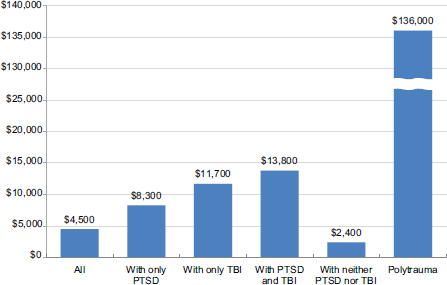
FIGURE 8.1 Average cost per OEF/OIF/OND veteran treated in VHA, 2007.
SOURCE: CBO, 2012.
CBO argued that was primarily a data artifact reflecting an expansion of the definition of TBI to include milder cases following the shift toward comprehensive screening in 2007.
Cost and prevalence estimates are, therefore, rough measures, but the results of this study are illuminating (see Figure 8.1). The CBO reported average costs and number of treated OEF, OIF, and OND veterans in the first year of treatment by condition. The implicit average cost for the 497,300 treated veterans was roughly $4,500 in the year 2007, slightly higher than previous CBO estimates. The difference likely reflects the data construction, in which statistics were averaged across several years. Average costs in the first year for the 103,500 veterans with only PTSD were $8,300; for the 8,700 with only TBI was $11,700; and for the 26,600 with both PTSD and TBI, $13,800. Average costs for the 358,000 veterans with neither PTSD nor TBI were $2,400. For the 500 veterans with polytrauma, costs were $136,000 (CBO, 2012).
The CBO study also offers a glimpse into the dynamics of these illnesses over time. Among veterans without PTSD or TBI, only about 40% remained in treatment after 4 years, with almost the entire reduction coming after the first year. Continuation of treatment was highest among patients with PTSD and TBI, more than 90% of whom remained in treatment for all 4 years. Roughly 80% of patients with only PTSD remained in treatment all 4 years, while about 70% of patients with only TBI remained. Although imperfect, those utilization statistics suggest a relatively long right tail of medical expenditures for veterans with psychological ailments and especially among those with multiple diagnoses (CBO, 2012). That could represent lingering trauma, the structure of health and disability benefits, or some combination of these.
Trends in average treatment costs offered no clear evidence about the intensity of treatments. When measured over the entire veteran cohort, which includes those who remain in treatment and those who leave treatment, average treatment costs typically fell over time because patients left treatment, lowering the numerator (costs). When measured over the veterans who remained in treatment, average costs showed no clear trend.
The committee also reviewed literature in the medical sciences that explored costs of war-related injuries, most of which focused on treatment costs. Topic areas covered in these articles included mental health trauma such as PTSD and depression; loss of limb; suicide; TBI; and a variety of miscellaneous topics such as cost measurement techniques, costs relative to length of deployment, and overall health care utilization among returning veterans.
Relatively few studies report actual cost estimates rather than offering commentary or discussing costs in a general sense. Among those that estimate costs, most typically consider treatment costs only and do not assess effects of injuries or treatments on quality of life, productivity, or other secondary outcomes. Most studies also focus on annual costs in the short run, rather than long-term or lifetime costs. Given knowledge about lifetime impacts of combat exposure, such a singular focus seems misplaced.
Studies that make longer-term projections tend to focus on the impacts of physical injuries. Blough et al. (2010) estimate the lifetime costs of prosthetics and assistive devices for amputees. Their per-person lifetime estimates range from $0.8 million to $3 million, depending on the type of amputation. Those are likely to be lower bounds because they do not incorporate the cost of repairs or the costs of new technological developments that might improve the quality of prosthetics but also increase their cost. Another key limitation is that Blough et al. do not explore effects on quality of life or work productivity.
Masini et al. (2009) estimate inpatient costs and disability benefits for injured service members, both overall and by type of injury. For the 31,708 injured patients as of May 2008, they found that total inpatient costs for initial hospitalization were $718 million and projected disability benefits were $1.9 billion. Their estimates might be too low because they do not account for inflation or cost-of-living adjustments, nor do they consider outpatient visits, rehabilitation, and prosthetics. In their study, the majority of costs accrue to patients with extremity injuries such as loss of limb, as opposed to injuries to the head and neck, thorax, and abdomen.
Studies that estimate treatment costs are also limited because they typically only consider VHA care. In some and perhaps many cases, patients who use the VA for health care might be only partially reliant on the VA. They might receive health insurance coverage through an employer or through the employer of a spouse or other family member. Care delivered outside the VA is relevant in assessing the total costs of injury, and the case could be made that it is more relevant than VHA care in understanding the burden on veterans and their families. However, it is more difficult to measure care received outside of the VHA, since federal agencies do not routinely track veteran’s provider visits if they are paid for by private sources.
Another notable limitation of existing studies is that they often do not consider the association between deployment to OEF, OIF, and OND and costs, perhaps because they cannot measure deployment. For example, Leslie et al. (2011) estimate total health care utilization costs for a sample of veterans after their first year back from OEF and OIF. They found that average costs were $2,185 for men and $1,847 for women. But it is impossible to attribute these costs to deployment to OEF, OIF, and OND without knowing what veterans’ health care costs would have been in the absence of deployment. Furthermore, those are estimates for all returning veterans, regardless of their health status. In a separate study, Chan et al. (2009) estimated that
annual average VHA costs are $5,860 for veterans with depression and $7,300 for veterans with depression and PTSD symptoms. Both of those statistics are broadly consistent with the results of the recent CBO study of VHA data (CBO, 2012), but Chan et al. did not limit their study to OEF, OIF, and OND veterans. The average age of their sample is 55, suggesting that it contains a mix of Vietnam, OEF, OIF, and OND, and other veterans.
One way in which existing studies are helpful is that they highlight the importance of ancillary costs of well-known deployment-related conditions, above and beyond the direct treatment costs associated with the conditions themselves. Although the literature often does not actually measure these ancillary costs, at least it itemizes them. Examples include consequences of TBI, such as personality changes and aggression; infections stemming from TBI; and increased general medical use among those with PTSD. Formulating long-term policy responses to war injuries requires a better understanding of their ancillary impacts.
Costs of Treating or Not Treating Mental-Health Disorders
Some of the more successful omnibus studies of the full costs of mental-health trauma associated with deployment and cost-effective treatment interventions include the ongoing Invisible Wounds research project developed by the RAND Corporation (Tanielian and Jaycox, 2008). To estimate the costs of PTSD and major depression among service members deployed to OEF, OIF, and OND, RAND conducted its own telephone-based survey of prevalence in the population and then modeled a broad array of outcomes over a 2-year period based on other research regarding probabilities of remission and relapse and intervention cost and effectiveness. RAND then published a followup study with some updated statistics (Kilmer et al., 2011). The contributions of the RAND studies are manifold. They measure the total costs over 2 years of mental health trauma associated with PTSD and major depression, including treatment costs, lost earnings, reductions in quality of life, and the value of lives lost to potential suicides. By estimating changes in the total costs across changes in treatment regimen, these studies also inform the optimal choice of treatments.
As reported by Kilmer et al. (2011), estimates suggest that more than 20% of service members returning from OEF, OIF, and OND would experience major depression or PTSD within 2 years, or more than 58,000 out of a deployed cohort of 261,827. They project aggregated 2-year costs of major depression or PTSD totaling $923 million in their baseline forecast, or about $16,000 per case. The cost of suicide is considerable at about $5,000 or 32% of the total, but the largest element is lost productivity, at about $10,200 per case or 64% of the total. Treatment costs over 2 years accounted for only 4–5% of the total. If the afflicted service member successfully obtained a VA disability rating that covered lost earnings, the government rather than the service member would bear that cost. In the case of suicide, although there are military and VA death gratuities, the contribution to total cost is large in those estimates because they are based on a large estimate of the private value of a statistical life, $7 million per life lost. Although that estimate is commonly used in the health economics literature and by government agencies, it is an order of magnitude larger than official death gratuities. Thus, the cost of suicides primarily represents a privately borne cost, which may be viewed as controversial.
The great utility of the RAND studies is that they help inform optimal treatment policies. In their simulations, Kilmer et al. (2011) found that expanding evidence-based treatments to all afflicted service members, rather than the half they expect will receive them in the baseline,
would significantly reduce the total costs of major depression and PTSD, even though it would raise treatment and thus budgetary costs paid by the VHA. Expanding evidence-based treatments to all, which in this study primarily involves increases in the frequency and intensity of psychotherapy sessions and increases in the frequency of selective serotonin reuptake inhibitors, would more than quadruple treatment costs per case, from $706 to $3,206, but it would actually reduce total costs per case by about 15%, from $16,000 to $13,551. This is because the RAND model suggests that universal evidence-based treatments would reduce average lost productivity and the chance of suicide by about 30% each, reducing those cost components by a total of almost $5,000 per case. The broad-based accounting of the RAND study suggests that expanding evidence-based treatment of major depression and PTSD in this way would be a socially desirable outcome that veterans would themselves choose if they could determine VHA treatment strategies. But VHA treatment costs rise. Still, the net effect of this change in policy could be to reduce total VA spending if disability benefits were reduced by the amount of the gained productivity, $3,320, which exceeds the increase in VHA treatment costs.
Although those studies have been groundbreaking in their discussion of mental-health trauma and the costs and benefits of treatments, the studies have not been able to assess the costs of TBI as thoroughly because the state of knowledge about TBI is not as advanced. In addition, the studies have not been able to fully address all costs that could be attributed to combat-related mental health trauma, such as homelessness, family strain, and the costs of pain and suffering. Going forward, these types of studies, and the basic science describing the dynamics of ailments, are critical focal points for future research efforts and funding.
CONCLUSIONS
Veterans of the post-9/11 period suffer higher rates of unemployment than nonveterans, but veterans who are employed appear to earn higher wages than their nonveteran counterparts. Using nationally representative data, researchers have shown that the average OEF/OIF veteran is more likely to be unemployed than comparable nonveterans (BLS, 2012b; Kleykamp, 2012). But employed veterans also appear to have higher earnings than their nonveteran counterparts after adjusting for observable differences (Kleykamp, 2012). Others have found that reservists earn less at first when they are activated, but over time they appear to earn more than comparable reservists who were not activated (Loughran and Klerman, 2010). A recent study suggests that hiring tax credits may be an effective tool for increasing employment rates of disabled veterans (Heaton et al., 2012), but there is no direct evidence yet that such policies can increase employment among younger veterans of the post-9/11 era.
Long deployments, PTSD, and disability are associated with unemployment, and activated reservists may have lower earnings when they return from active duty if they have PTSD. Some researchers have found that OEF and OIF veterans were more likely to be unemployed if they had PTSD, poor mental health, or if they were deployed for longer time periods than those without those symptoms or who were deployed for shorter time periods (Loughran and Klerman, 2010; Riviere et al., 2011). One study showed that veterans also appeared to earn less if they had PTSD symptoms (Heaton and Loughran, 2010). Another study reported that combat exposure among National Guard members who deployed to OEF and OIF seemed to increase the odds of employment, and that there was no simple association between mental health symptoms and employment (Burnett-Zeigler et al., 2011).
Studies of veterans from earlier periods suggest that negative impacts of deployment to OEF, OIF, and OND and combat exposure may be revealed later in the life cycles of today’s veterans and service members. Surveillance systems should be in place. As the committee noted in its Phase 1 report, the number of veterans from past war cohorts who are observed drawing disability benefits tends to rise over time before ultimately falling as the cohort reaches old age and dies. The pioneering work of Hearst et al. (1986) on the Vietnam draft lottery suggested that elevated mortality due to suicide and motor vehicle accidents was plausibly caused by prior military service. Patterns also suggest that rising disability compensation among Vietnam veterans may reflect the program’s implicit work disincentives (Angrist et al., 2010).
The budgetary costs of providing care for injured veterans are significant and are likely to rise over time. Uncompensated socioeconomic costs of war injuries may be large. Planning for the funding and provision of care should take a long-term perspective. Academic researchers and the nonpartisan Congressional Budget Office now tend to agree on short- and medium-term forecasts of budgetary costs associated with medical treatment. If past trends continue, these costs will continue to rise over the remaining lifetimes of OEF and OIF veterans and present a clear motivation for long-term planning. In the short term, research suggests that spending more now to implement evidence-based treatments of mental health trauma will generate significant cost savings in the future, most significantly by reducing suicides, which impose enormous costs on families (Kilmer et al., 2011; Tanielian and Jaycox, 2008).
Spouses of service members face an array of challenges that are often made more acute by deployment, and their socioeconomic well-being can suffer. Spouses of veterans face similar issues and impacts, about which less is known. Researchers have shown that spouses of service members are less likely to be employed than nonmilitary spouses, and they appear to earn less than their nonmilitary counterparts (Hosek et al., 2002). Spouses of service members deployed to OEF, OIF, and OND have likely faced the same challenges that confront military spouses generally, such as potential job loss, earnings losses, and other costs of household reorganization (DOD, 2009).
STUDIES OF SOCIOECONOMIC OUTCOMES CURRENTLY UNDER WAY
As was made clear in the committee’s Phase 1 report and in the responses of VA and Department of Defense (DOD) to that report, there are several studies currently under way that can address socioeconomic outcomes associated with deployment to OEF, OIF, and OND. But the number of these studies is very small relative to the broader array of inquiries focused on specific health impacts of military deployments.
In particular, the list of currently federally funded studies given in Appendix D of this report contains very few studies that address the social and economic outcomes discussed in this chapter. These studies, highlighted in Appendix D, are being conducted by VA researchers on VA populations and might not be representative of the overall veteran population, many of whom are not enrolled in such services. Veterans of OEF and OIF who do not interface regularly with the VA are unlikely to be the subjects of current funded research, a major shortcoming in the committee’s view.
But as the committee mentioned in its Phase 1 report (p. 156), and as the responses of VA and DOD discussed, two ongoing studies are likely to shed light on the socioeconomic impacts
of deployment: the Millennium Cohort Study (McSally, 2007) and RAND’s Deployment Life Study (DLS). As of this writing, the committee is unaware of research based on those datacollection efforts that specifically addresses socioeconomic outcomes.
The committee remains concerned that socioeconomic outcomes for separated veterans and their families will not be suitably measured by existing studies, which do not explicitly focus on separated military service members and thus may not measure them in large enough numbers. There was no indication in VA’s response to the committee’s Phase 1 report that it has plans to assess socioeconomic well-being among the population of OEF and OIF veterans in any systematic way. The only analysis tool the committee found for such purposes is the 2010 NSV, which offers limited insights (Edwards, 2012).
In addition to the DLS and other concurrent RAND studies, the committee is aware of ongoing inquiries into the effects of military service in the National Longitudinal Study of Adolescent Health (Add Health), which follows a nationally representative sample of individuals born between 1976 and 1984. Data collection is funded by the National Institute of Child Health and Human Development. Cesur et al. (2013) use those data to assess the impact of deployment to combat zones on mental health and medical costs. Wang et al. (2012) use the Add Health to explore military service, preservice social status, and educational attainment. Some of these efforts are being funded by a grant from the Army Research Institute for the Behavioral and Social Sciences. While datasets that sample individuals from the population are sometimes limited in their power to describe military and veteran subsamples, the committee believes these efforts will produce important new insights because the data are more representative of all veterans than studies of individuals who have entered the VA system.
FUTURE RESEARCH DIRECTIONS
The committee’s statement of task requested information about gaps in care and opportunities for research. For many social and economic outcomes, the committee does not know enough to definitively describe the gaps associated with deployment that might exist between deployed and nondeployed service members and veterans and their families. Furthermore, where gaps can be identified, the mechanisms for those gaps, or why those gaps might exist, are often unknown. Measuring gaps and understanding mechanisms are important first steps in recommending changes in policies. As a result, the committee’s recommendations for future research directions on socioeconomic outcomes focus primarily on enhancing data collection and analysis and surveillance efforts. But some readjustment needs associated with deployment are already clear, and the committee begins by discussing their nature and implications.
The committee believes there are several clear policy implications regarding the lifelong costs associated with deployment-related mental health trauma, such as major depression and PTSD, and TBI. Studies suggest that expanding evidence-based treatment regimens for those disorders, which emphasize more frequent use of psychotherapy and pharmacologic interventions, might increase short-term treatment costs but would strongly reduce the broader costs paid by governments and individuals by improving outcomes. These insights have been gleaned from decades of basic research into mental health trauma; the same efforts must now be directed toward understanding TBI and its sequelae to inform policy with a similar degree of certitude.
• Studies on cost-effectiveness focusing on the signature wounds of TBI, PTSD, and major depression should continue to be funded and conducted; the implications of prior cost effectiveness studies, where knowledge is sufficiently developed, guide the evolution of policy inside the VA and elsewhere.
• Because much current evidence is equivocal on the issue of socioeconomic impacts of deployment to OEF, OIF, and OND, the committee believes that more analysis with improved data is needed. Much statistical evidence cannot support rejection of the hypothesis that there is no effect of deployment on the average service member, nor can it strongly support accepting that the precise effect is zero. But given current patterns connecting overseas deployment with combat exposure, and past patterns of need among older cohorts of war veterans, the committee believes that socioeconomic impacts of deployment may reveal themselves later in the life cycles of today’s service members returning from overseas deployments.
• Enhanced surveillance efforts and data collection to measure the socioeconomic and other impacts of deployment among aging veterans that may potentially emerge with time should be considered. An expanded set of questions about military service in Census data products such as the American Community Survey or the Current Population Survey of the BLS would be examples of such efforts, as would an expanded and more frequently fielded National Survey of Veterans, or new linkages between VA and military records and existing data collection efforts such as the Health and Retirement Study, Panel Study of Income Dynamics, or the National Longitudinal Study of Adolescent Health.
Isolating causality is a cross-cutting concern for understanding the socioeconomic impacts of military service, overseas deployment, and combat exposure. It is difficult to disentangle the impacts of deployment on outcomes from the effects of other characteristics that may affect deployment and outcomes alike. Military readiness precludes the conducting of randomized control trials, but there are statistical strategies available to deal with nonrandom selection into treatment and control: instrumental variables; limited comparison groups, such as comparing activated to nonactivated reservists; and fixed effects models, in which researchers compare outcomes before and after deployment across different groups or individuals using longitudinal data. All of these would require that enhanced data be made available to researchers.
• Future research and funding efforts seeking to enhance the ability of independent researchers to explore causal relationships between military service and outcomes. One type of approach identifies so-called “instrumental variables” associated with service that are exogenous to an individual’s characteristics but that affect outcomes. Publishing rates of deployment by year or quarter of birth, measurable characteristics that inform without compromising privacy and thus minimizing harm to human subjects, are one such strategy that might prove illuminating, and there might be others. Establishing restricted data centers with longitudinal service records containing detailed characteristics that determine the propensity to deploy would be another strategy.
While there is much successful research on socioeconomic outcomes among older cohorts of veterans, who are measured in publicly available Census data products, there is very little research on the socioeconomic impacts of OEF, OIF, and OND. This is likely because the relevant data are not publicly unavailable.
• To facilitate effective social science research on the impacts of overseas deployment in the near past on outcomes, the VA and DOD should provide new publicly available databases of de-identified data on individuals over time.
Previous research has focused on employment and earnings primarily among reservists, but less is known about employment and earnings among separated veterans.
• The committee suggests that future researchers address the impact of deployment on earnings and employment among all veterans, not just National Guard and reservists. Researchers could link DMDC payroll data on service members to Social Security records to examine earnings and employment. To assess the causal impact of deployment on these outcomes, instrumental variables or other approaches should be used.
• Research on previous generations of veterans identified important gains in educational attainment resulting from military educational benefits like the GI Bill. Little is understood about how or why the new Post-9/11 GI Bill is affecting educational attainment among veterans and among the family members to whom benefits may now be transferred. Future research efforts and funding should explicitly target how overseas deployment to OEF, OIF, and OND might have affected educational attainment among service members or their eligible family members. In particular:
• Research should examine how deployment relates to the use of educational benefits. Are deployed veterans more or less likely to use their educational benefits than are nondeployed veterans? This research should be feasible using existing administrative data, but it should ideally also address issues of causality; veterans may have other characteristics that are associated with both their use of benefits and their deployment.
• Research should examine how deployment relates to overall educational attainment. Do deployed veterans ultimately obtain more or fewer years of schooling than nondeployed veterans? Do they attend different types of institutions, and does that matter for graduation rates? This research likely cannot rely solely on government administrative data, but a partnering with institutions of higher learning could produce data linkages that reveal key patterns.
The committee is unaware of systematic efforts to assess how wealth and household finances are affected by military service or deployment. The committee is also unaware of preexisting datasets that could be used to assess this outcome in large samples; most surveys of finances are either not large to begin with, have small veteran subsamples, or both, which raises acute problems of statistical power.
• Future research and funding efforts should seek to address the impact of deployment on household finances and wealth. Partnering with firms in the private sector, such as USAA or regional banks, might be the easiest way forward short of launching new data collection efforts.
The state of knowledge regarding the tolls of accelerated and lengthened deployment on the socioeconomic status of military spouses is poor, and thus it is difficult to assess needs or recommend policies. Even less is known about the current impacts of past deployments on the spouses of veterans.
• Future studies should attempt to measure the impacts of deployments on spousal well-being in a more systematic way.
Problems of unemployment and underemployment, which are broadly felt by the US civilian population today, appear to be more acute for veterans of the post-9/11 era, particularly young veterans. In 2011, the unemployment rate among all post-9/11 veterans 18 years old and older was more than one-third higher than that among equivalent nonveterans—12.1% compared with 8.7%. Among veterans 18–24 years old, the rate was almost twice as high—30.2% compared with 16.1%. The sources of those disparities remain unclear and could include skills mismatch, impeded ability to maintain or obtain employment because of physical or mental-health trauma, stigma or discrimination, or some combination of those factors or other elements. Successful readjustment depends on reentry into the civilian workforce, and the available evidence suggests that this is an important gap for policy to address. The committee found that the literature assessing the effectiveness of DOD’s and VA’s transition-assistance programs is relatively thin, even though reentry into the labor force is one of the most important readjustment challenges. One study suggests that recent expansions of hiring tax credits might have been effective in raising rates of employment of older veterans who have disabilities. But OEF, OIF, and OND veterans did not appear to benefit from the expansions.
The committee recommends that the Department of Defense and the Department of Veterans Affairs evaluate the effectiveness of transition-assistance programs to ensure that they are effective in reducing unemployment among returning veterans of Operation Enduring Freedom, Operation Iraqi Freedom, and Operation New Dawn.
Evaluation of the effectiveness of transition-assistance programs, with research that examines employment patterns after separation from the military over time, will provide data to ensure that scarce resources can be allocated to effective programs. Further study might focus on whether employment tax credits are a cost-effective means of expanding employment for Operation Enduring Freedom and Operation Iraqi Freedom veterans and whether programs to counsel and prepare service members for long-term postservice careers are effectively implemented.
The Post-9/11 GI Bill is one of the largest expansions of educational subsidies to veterans and their families on record, but its effectiveness is difficult to gauge. The committee is aware of no studies that have explicitly evaluated the effects of deployment to OEF and OIF on the use of the Post-9/11 GI Bill or the effects of the Post-9/11 GI Bill.
The committee recommends a comprehensive evaluation of the effects of the Post-9/11 GI Bill on the educational attainment of veterans and eligible family members.
The committee views the current evidence on the costs of caring for injured veterans as an overwhelming challenge. There is a need to assess the costs of caring for injured veterans systematically and publicly. The Congressional Budget Office publicly assesses short-term and medium-term costs, and, as the VA stated in response to the committee’s Phase 1 report, it already produces some forecasts of health and disability spending. But the committee continues to believe that long-term planning for veterans’ care requires public long-term cost forecasts in
the same way that Social Security and Medicare require them, and these forecasts should take a similar form to be internally and externally useful.
The committee reiterates its call for comprehensive long-term forecasts of the costs of the Veterans Health Administration’s medical care and the Veterans Benefits Administration’s disability benefits associated with combat deployments; these forecasts should be conducted annually and should be released publicly by the Department of Veterans Affairs and confirmed by an independent external authority.
REFERENCES
Adler, D. A., K. Possemato, S. Mavandadi, D. Lerner, H. Chang, J. Klaus, J. D. Tew, D. Barrett, E. Ingram, and D. W. Oslin. 2011. Psychiatric status and work performance of veterans of Operations Enduring Freedom and Iraqi Freedom. Psychiatric Services 62(1):39-46.
Al Nassir, F., R. Lipari, and K. Matos. 2012. Response to notes regarding the 2006 survey of active duty spouses. Armed Forces and Society [Epub].
Angrist, J. D. 1998. Estimating the labor market impact of voluntary military service using Social Security data on military applicants. Econometrica 66(2):39.
Angrist, J. D., S. H. Chen, and B. R. Frandsen. 2010. Did Vietnam veterans get sicker in the 1990s? The complicated effects of military service on self-reported health. Journal of Public Economics 94(11-12):824-837.
Blough, D. K., S. Hubbard, L. V. McFarland, D. G. Smith, J. M. Gambel, and G. E. Reiber. 2010. Prosthetic cost projections for servicemembers with major limb loss from Vietnam and OIF/OEF. Journal of Rehabilitation Research and Development 47(4):387-402.
BLS (Bureau of Labor Statistics). 2012a. BLS Inflation Calculator. http://www.bls.gov/data/inflation_calculator.htm (accessed April 24, 2012).
———. 2012b. Employment Situation of Veterans—2011. Washington, DC: BLS.
Burnett-Zeigler, I., M. Valenstein, M. Ilgen, A. J. Blow, L. A. Gorman, and K. Zivin. 2011. Civilian employment among recently returning Afghanistan and Iraq National Guard veterans. Military Medicine 176(6):639-646.
Cesur, R., J. J. Sabia, and E. Tekin. 2013. The psychological costs of war: Military combat and mental health. Journal of Health Economics 32(1):51-65.
Chan, D., A. D. Cheadle, G. Reiber, J. Unutzer, and E. F. Chaney. 2009. Health care utilization and its costs for depressed veterans with and without comorbid PTSD symptoms. Psychiatric Services 60(12):1612-1617.
Christensen, E., J. McMahon, E. Schaefer, T. Jaditz, and D. Harris. 2007. Final Report for the Veterans’ Disability Benefits Commission: Compensation, Survey Results, and Selected Topics. Alexandria, VA: CNA.
CBO (Congressional Budget Office). 2007. CBO Testimony: Statement of Matthew S. Goldberg, Deputy Assistant Director for National Security, Before the Committee on Veterans Affairs, U.S. House of Representatives, October 17, 2007. Washington, DC: CBO.
———. 2010. Potential Costs of Veterans’ Health. Washington, DC: CBO.
———. 2012. The Veterans Health Administration’s Treatment of PTSD and Traumatic Brain Injury Among Recent Combat Veterans. Washington, DC: CBO.
DOD (Department of Defense). 2009. Report of the 2nd Quadrennial Quality of Life Review. Washington, DC: United States Department of Defense.
Edwards, R. D. 2012. Overseas deployment, combat exposure, and well-being in the 2010 National Survey of Veterans. National Bureau of Economic Research Working Paper Series No. 18227.
Egendorf, A., C. Kadushin, and R. Laufer. 1981. Legacies of Vietnam: Comparative Adjustment of Veterans and Their Peers, Vol 1-5. Washington, DC: Government Printing Office.
Elbogen, E. B., S. C. Johnson, R. H. Wagner, V. M. Newton, and J. C. Beckham. 2012. Financial wellbeing and postdeployment adjustment among Iraq and Afghanistan war veterans. Military Medicine 177(6).
Elman, C., and A. M. O’Rand. 2004. The race is to the swift: Socioeconomic origins, adult education, and wage attainment. American Journal of Sociology 110(1):123-160.
GAO (Government Accountability Office). 2009. VA Vocational Rehabilitation and Employment: Better Incentives, Workforce Planning, and Performance Reporting Could Improve Program. Washington, DC: GAO.
Harrell, M. C., N. Lim, L. Werber Castaneda, and D. Golinelli. 2004. Working Around the Military: Challenges to Military Spouse Employment and Education. Santa Monica, CA: RAND Corporation.
Hearst, N., T. B. Newman, and S. B. Hulley. 1986. Delayed effects of the military draft on mortality. A randomized natural experiment. New England Journal of Medicine 314(10):620-624.
Heaton, P. 2012. The Effects of Hiring Tax Credits on Employment of Disabled Veterans. Santa Monica, CA: RAND Corporation.
Heaton, P., and D. S. Loughran. 2010 (unpublished). Post-Traumatic Stress Disorder and the Earnings of Military Reservists. RAND Corporation.
Heaton, P., A. Miller, and D. S. Loughran. 2012. Compensating Wounded Warriors: An Analysis of Injury, Labor Market Earnings, and Disability Compensation Among Veterans of the Iraq and Afghanistan Wars. Santa Monica, CA: RAND Corporation.
Hoge, C. W., C. A. Castro, S. C. Messer, D. McGurk, D. I. Cotting, and R. L. Koffman. 2004. Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. New England Journal of Medicine 351(1):13-22.
Hosek, J., B. Asch, C. C. Fair, C. Martin, and M. Mattock. 2002. Married to the Military: The Employment and Earnings of Military Wives Compared with Those of Civilian Wives. Santa Monica, CA: RAND Corporation.
IOM (Institute of Medicine). 2010. Returning Home from Iraq and Afghanistan: Preliminary Assessment of Readjustment Needs of Veterans, Service Members, and Their Families. Washington, DC: The National Academies Press.
Katz, L. F. 1998. Wage subsidies for the disadvantaged. In Generating Jobs: How to Increase Demand for Less-Skilled Workers, edited by R. Freeman and P. Gottschalk. New York: Russell Sage Foundation. Pp. 21-53.
Kilmer, B., C. Eibner, J. S. Ringel, and R. L. Pacula. 2011. Invisible wounds, visible savings? Using microsimulation to estimate the costs and savings associated with providing evidence-based treatment for PTSD and depression to veterans of Operation Enduring Freedom and Operation Iraqi Freedom. Psychological Trauma: Theory, Research, Practice, and Policy 3(2):201-211.
Kleykamp, M. 2009. A great place to start?: The effect of prior military service on hiring. Armed Forces and Society 35(2):266-285.
———. 2012. Employment, Earnings and Enrollment Among Post 9/11 Veterans (working paper). College Park, MD: University of Maryland.
Leslie, D. L., J. Goulet, M. Skanderson, K. Mattocks, S. Haskell, and C. Brandt. 2011. VA health care utilization and costs among male and female veterans in the year after service in Afghanistan and Iraq. Military Medicine 176(3):265-269.
Losinger, W. C. 2010. Notes regarding the 2006 survey of active duty spouses. Armed Forces and Society 36(3).
Loughran, D. S., and J. A. Klerman. 2008. Explaining the Increase in Unemployment Compensation for Ex-servicemembers During the Global War on Terror. Santa Monica, CA: RAND Corporation.
———. 2010. The Effect of Activation on the Post-activation Civilian Earnings of Reservists. Santa Monica, CA: RAND Corporation.
Loughran, D. S., P. Martorell, T. Miller, and J. A. Klerman. 2011. The Effect of Military Enlistment on Earnings and Education. Santa Monica, CA: RAND Corporation.
Masini, B. D., S. M. Waterman, J. C. Wenke, B. D. Owens, J. R. Hsu, and J. R. Ficke. 2009. Resource utilization and disability outcome assessment of combat casualties from Operation Iraqi Freedom and Operation Enduring Freedom. Journal of Orthopaedic Trauma 23(4):261-266.
McSally, M. E. 2007. Women in Combat: Is the Current Policy Obsolete? Air War Coll., Maxwell Air Force Base, AL.
Neumark, D. 2011 (unpublished). Spurring Job Creation in Response to Severe Recessions: Reconsidering Hiring Credits. Cambridge, MA: NBER Working Paper.
Noonan, M. E., and C. J. Mumola. 2007. Veterans in State and Federal Prison, 2004. Washington, DC: Bureau of Justice Statistics.
Resnick, S. G., and R. A. Rosenheck. 2008. Posttraumatic stress disorder and employment in veterans participating in Veterans Health Administration Compensated Work Therapy. Journal of Rehabilitation Research and Development 45(3):427-435.
Riviere, L. A., A. Kendall-Robbins, D. McGurk, C. A. Castro, and C. W. Hoge. 2011. Coming home may hurt: Risk factors for mental ill health in US reservists after deployment in Iraq. British Journal of Psychiatry 198:136-142.
Rohlfs, C. 2010. Does combat exposure make you a more violent or criminal person? Evidence from the Vietnam draft. Journal of Human Resources 45(2):271-300.
Ruggles, S., J. T. Alexander, K. Genadek, R. Goeken, M. B. Schroeder, and M. Sobek. 2010. Integrated Public Use Microdata Series: Version 5.0 [machine-readable database]. Minneapolis, MN: University of Minnesota.
Sayer, N. A., S. Noorbaloochi, P. Frazier, K. Carlson, A. Gravely, and M. Murdoch. 2010. Reintegration problems and treatment interests among Iraq and Afghanistan combat veterans receiving VA medical care. Psychiatric Services 61(6):589-597.
Senate Health Education Labor and Pension Committee. 2011. New data on post-9/11 GI Bill Benefits Show Disproportionate Share of Taxpayer Dollars Going to For-profit Colleges with Concerning Outcomes. http://harkin.senate.gov/documents/pdf/4e7b5d0253b75.pdf (accessed July 14, 2012).
Sewall, M. 2010. Bill to expand veterans’ education benefits begins moving through Congress. Chronicle of Higher Education, August 5.
Sheftick, G. W. 2012. New Transition Assistance Program set for November launch. Army News Service. http://www.defense.gov/news/newsarticle.aspx?id=117959 (accessed November 1, 2012).
Smith, M. W., P. P. Schnurr, and R. A. Rosenheck. 2005. Employment outcomes and PTSD symptom severity. Mental Health Services Research 7(2):89-101.
Steele, J. L., N. Salcedo, and J. Coley. 2011. Service Members in School: Military Veterans’ Experiences Using the Post-9/11 GI Bill and Pursuing Postsecondary Education. Santa Monica, CA: RAND Corporation.
Stiglitz, J. E., and L. Bilmes. 2008. The Three Trillion Dollar War. New York: Norton.
Tanielian, T., and L. H. Jaycox. 2008. Invisible Wounds of War: Psychological and Cognitive Injuries, Their Consequences, and Services to Assist Recovery. Santa Monica: RAND Corporation.
Wang, L., J. Glen Elder, and N. J. Spence. 2012. Status configurations, military service, and higher education. Social Forces 91(2):397-422.