Corneal Topography and Contact Lenses
Stephen D. Klyce
The cornea is a unique part of the ocular tunic, serving both as a tough coat to resist trauma and as a highly refractive, transparent optical element in the visual pathway. It is in essence an armored window, the port of entry for light to the eye and the visual system. But while the individual collagen fibers that give strength to the cornea are stronger than steel—collectively enmeshed as they are in a viscous extracellular matrix of sugar-protein macromolecules —they can be rearranged by abnormal forces such that the shape of the cornea can be altered.
Since the corneal surface is the major refracting element in the eye, even small changes in its shape can alter visual acuity. Visual acuity of 20/20 or better is required for air-to-air combat as well as for any other mission relying on direct visual sighting such as marksmanship. A major consideration is the fact that, while people can be fit with contact lenses to provide this acuity in the refracting lane of the clinic, contact lenses can and do produce both acute and chronic changes in visual acuity. With every blink of the eye (and the blink rate is increased with contact lens wear), the lenses are compressed and decentered to varying degrees. This causes a postblink defocusing that can last a second or more. When the lenses dry, lose their mobility, or center improperly, a series of blinks is required before proper acuity is achieved.
CHRONIC EFFECTS
The chronic effects of contact lens wear on acuity are well known. Contact lenses can alter the shape of the cornea, and this fact was exploited vigorously for a time when practitioners sought to predictably change the shape of the cornea with contact lenses. However, this effort, called
orthokeratology, was largely abandoned following negative results of a carefully controlled clinical trial by Polse et al. (1983). Unintentional or spontaneous changes in corneal shape are also a fairly common problem—changes that cause a loss of a line or more of visual acuity on the Snellen Chart—and these changes are not often reported because they occur so slowly that patients are unaware of the change until some loss of function is detected, such as having trouble reading highway signs. This problem is exacerbated by emotional ties to the contact lens modality to achieve adequate visual acuity.
At Louisiana State University (LSU) Eye Center in New Orleans, we have been interested in the problem of contact-lens-induced corneal warpage for several years now, since we were not able to address this problem adequately with the routine clinical tools available in the past such as the keratometer and the photokeratoscope. However, we have developed methods over this period that finally allow accurate assessment of the corneal topographic alterations that can be produced by contact lenses, and I will briefly review this technology and present a few case reports.
Clinical keratometers measure the power of the corneal surface from four points about 3 millimeters apart and it is assumed that the cornea is purely spherical or ellipsoidal, despite the fact that Mandell (1970) clearly showed over 30 years ago that corneas, even for a normal population, clearly deviated from spherical or ellipsoidal models. Many subsequent research papers attempted to reconstruct true corneal shape by computer analysis of photokeratoscopic images.
LSU STUDIES
At LSU we were first concerned with accurate corneal surface reconstruction from photokeratoscopic images for which there is, unfortunately, no exact solution (Klyce, 1984). However, better approximations of true shape are nearly complete at LSU (cf. Wang et al., 1989). The more difficult task was to design graphical presentation schemes that could portray corneal distortions in a fashion permitting rapid interpretation by the clinician. Stereo-pair wire models of corneal surface distortion failed for the majority of the clinical audience. However, when color-coded contour maps of corneal surface powers were presented, clinicians could easily interpret their meaning and use them for diagnosis, for evaluation of refractive surgery, and for guidance in the correction of astigmatism following corneal transplantation and cataract procedures (Maguire et al., 1987). We have transferred these concepts to the corneal modeling system (CMS), a state-of-the-art automatic corneal topography analyzer manufactured by Computed Anatomy, Inc. in New York (Gormley et al., 1988). With this device it is now possible to evaluate in detail the effects of contact lens wear on corneal shape. The standard CMS graphic display is a color-coded contour map of corneal
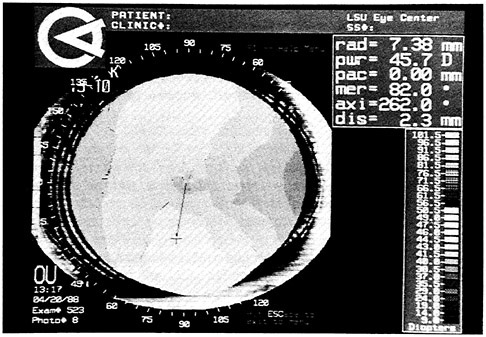
FIGURE 1 Gray scale contour map of suspected keratoconus in a right eye, typically an inferior region of the cornea with higher than normal power. The cross-hair lies at the apex of the putative cone, and the score box in the upper right-hand corner reads 45.7D at this point. The key in the lower right indicates that over the near-normal range of corneal powers (1.5D intervals) lower powers are represented by dark shades, higher powers by lighter shades. If there were powers below 34D, they would be represented by an intensity-graded series of cross-hatching at 5D intervals; if there were powers above 51.5D, they would be represented by an intensity-graded series of meshing. SOURCE: S.E. Wilson, and S.D. Klyce, LSU Eye Center, unpublished data.
surface powers. For this report a gray scale version of the display was used. In each of the cases of contact-lens-induced corneal warpage presented below, only one eye is shown, but both eyes were similarly affected. Details of this study can be found in Wilson et al. (1990a, 1990b).
CASE REPORTS
Case 1
Figure 1 presents data for a patient who complained of red and irritated eyes. With contact lenses she was seeing only 20/50. Her best corrected refraction was 20/25 in each eye. Both lenses were mobile, but both were riding low. With the CMS her power distribution was suggestive of early keratoconus in both eyes. To test the possibility of contact-lens-induced

FIGURE 2 Same cornea as in Figure 1 1 month after discontinuance of contact lens wear. The corneal power distribution now shows a regular corneal cylinder. Apparently the lenses in both eyes were riding low, flattening the cornea superiorly, which led to the keratoconic pattern seen at the patient's first visit. SOURCE: S.E. Wilson and S.D. Klyce, LSU Eye Center, unpublished data.
warpage, she was instructed to leave her lenses out for 1 month. On her return, corneal topography analysis was repeated, and her corneas now (Figure 2) exhibited regular corneal cylinder. Evidently the lenses had sphericized the superior corneal cylinder, leaving the lower cylinder intact. She was refitted with rigid gas-permeable lenses, achieving 20/20 acuity in each eye.
Case 2
Another patient presented with pain and glare sensitivity in both eyes. She was wearing Hydrocurve soft contact lenses with a base curve of 9.5 millimeters. The lenses were mobile, but keratometry and keratoscopy showed irregular mires and central distortion (Figure 3). She was instructed to discontinue contact lens wear for 3 weeks. On her return, she was asymptomatic and the corneal distortion seen on her first visit was absent (Figure 4). She was fitted with SoftMate contact lenses with a steeper base of 9.0 millimeters and is doing well with them.
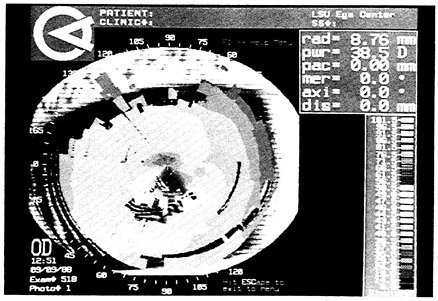
FIGURE 3 Central corneal distortion with irregular keratoscope mires in the right eye of a patient fitted contact lenses with perhaps too flat a base curve. SOURCE: S.E. Wilson and S.D. Klyce, LSU Eye Center, unpublished data.
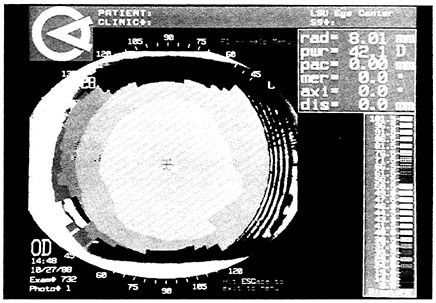
FIGURE 4 The cornea of Figure 3 was completely normal 3 weeks after discontinuing contact lens wear. The concentric rings of power shown here are typical for a cornea deemed “spherical” with keratometry. The lower power in the corneal periphery is normal and can partly correct for spherical aberration in the eye. SOURCE: S.E. Wilson and S.D. Klyce, LSU Eye Center, unpublished data.
SUMMARY
In summary, I have presented several concerns regarding the use of contact lenses for military personnel. Acute or chronic fluctuations in visual acuity can degrade performance, leading to loss of functionality, but the impact of this in terms of overall military performance is unknown. Advances in technology have made it possible to evaluate contact lens effects on corneal shape. This technology should be used in prospective studies to determine the risk factors associated with contact lens wear in adverse conditions.
ACKNOWLEDGMENT
This work was supported by USPNS research grants EY 03311 and EY 02377. Computed Anatomy, Inc., generously supplied the corneal modeling system used in this study.
REFERENCES
Gormley, D.J., M. Gersten, R.S. Koplin, and V. Lubkin 1988 Corneal modeling. Cornea 7:30–35.
Klyce, S.D. 1984 Computer-assisted corneal topography: high resolution graphical presentation and analysis of keratoscopy. Investigative Ophthalmology and Visual Science 25:1426–1435.
Maguire, L.J., D.E. Singer, and S.D. Klyce 1987 Graphic presentation of computer-analyzed keratoscope photgraphs Archives of Ophthalmology 105:223–230.
Mandell, R. 1970 System of Ophthalmology. Vol V., Ophthalmic Optics and Refraction. S. Duke-Elder and D. Abrams, eds. St. Louis: C. V. Mosby
Polse, K.A., R.J. Brand, J.S. Schwalbe, D.W. Vastine, and R.J. Keener 1983 The Berkeley orthokeratology study, part II: efficacy and duration American Journal of Optometry and Physiological Optics 60:187–198.
Wang, J., D.A. Rice, and S.D. Klyce 1989 A new reconstruction algorithm for improvement of corneal topographical analysis. Refractive and Corneal Surgery 5:379–387.
Wilson, S.E., D.T.C. Lin, S.D. Klyce, J.J. Reidy, and M.S. Insler 1990a Topographic changes in contact lens-induced corneal warpage. Ophthalmology 97:734–744. 1990b Rigid contact lens decentration—a risk factor. CLAO J 16:177–182.






