8
Transferability of Models and Lessons Learned
Key Messages
To be able to convince those to participate and to pay, you need to have real added value.
—Monique Dolfing-Vogelenzang
If we are talking about women’s empowerment while focusing on midwives and nurses, we should also look at other types of health workers that commit to empower women, like community health workers, for future support.
—Akiko Maeda
There should be a commitment at the provider level to the AAAQ framework around Availability, Accessibility, Acceptability, and Quality of services. There has to be a coherent financing mechanism that really drives population health management as opposed to quantity of services provided.
—Krishna Udayakumar
I think we have real issues about scaling and replication, but we could definitely learn lessons from abroad and internally.
—Deborah Bae
On the afternoon of the second day, participants rotated through three different breakout groups to explore with more granularity issues of financing and training of nursing and midwifery enterprise. They also explored how elements of empowerment and health systems strengthening might be intentionally incorporated into new financing and training models that could be transferred to the United States. The intentionality of women’s empowerment was highlighted as an area of particular interest for the small groups to consider. In each group, participants discussed potential transferability of models to new settings and lessons learned relating to context, needs, and culture. They also identified challenges and opportunities, promising models, and potential strategies for success. Participants reconvened in a large group to provide individual insights based on the small group discussions. The following is a summary of the small group discussions presented by the group leaders, and they should not be viewed as consensus.
CHALLENGES AND OPPORTUNITIES: FINANCING NURSING AND MIDWIFERY ENTERPRISES THAT EMPOWER WOMEN AND STRENGTHEN HEALTH SYSTEMS1
Group leader Monique Dolfing-Vogelenzang raised the issue of nurse franchising for developing countries that could also have implications for the United States. The franchise would include a toolbox with a set of standards, guidelines, and services that would be made available to all of the clinics, and tailored in primary health care services to specific patient groups. One main focus would be the marketing around a strong branding identity with pricing, quality elements, back-office operations, group purchasing power, referral system, and information and communications technology (ICT) tools.
Because the franchisees would be part of a strong network, they would also be able to leverage collective power for negotiation and discussion around regulation. One major stakeholder would be schools that train nurses, midwives, doctors, and/or community health workers. And in addition to donor funds at the start, Dolfing-Vogelenzang noted that the early inclusion of investors would yield greater sustainability.
The model could commence with one or two facilities that serve as central hubs where processes and infrastructure would be vetted. Additional franchises could then be added in replication. Franchise owners would receive training, the toolkit, and access to financing as part of the membership fee. Clients would pay for services, whether out of pocket or by insurance
________________
1 This section summarizes information presented by Monique Dolfing-Vogelenzang, Medical Credit Fund (MCF).
card, and process and costs would be continually evaluated to ensure affordability and sustainability.
One consideration raised by Dolfing-Vogelenzang involves convincing consumers and providers to participate and to pay. This could possibly be addressed by offering health financing through the government, or by giving schools an important though not necessarily leadership-oriented role. Standards and guidelines would also add value by providing a universal level of quality within a country. A flexible model would allow franchisees a certain degree of freedom to remain competitive with other facilities in the area.
A number of challenges implicit in this model were also articulated by individual members of the group:
- The lack of and need for business and startup expertise,
- The economics of patient capacity to pay,
- Patient mix (including ability to pay, illness, and severity of illness),
- Restrictive regulation,
- Access to capital, both short and long term,
- Quality standards and support,
- Knowledge around best practices, and
- Lack of trust, including brand trust.
A model such as this, said Dolfing-Vogelenzang, could provide a number of opportunities to address these challenges, such as engaging patients and communities, meeting the needs of the population, developing different models of financing, involving different types of providers, and involving schools.
STRATEGIES AND SUPPORT: START-UP, SCALE-UP, SUSTAINABILITY, AND TRANSFERABILITY OF ACTUAL AND THEORETICAL MODELS GLOBALLY AND TO THE UNITED STATES2
Small group leader Akiko Maeda suggested that gaps in existing services and care models might actually be opportunities to create or adopt new models that would build on the comparative strength of nurses and midwives in the United States and around the world. She also noted that, in thinking about women’s empowerment, some consideration could be given to other health workers who commit to empowering women. While a number of potential areas of need exist, one particular space is long-term care management, particularly community-based care coordination.
________________
2 This section summarizes information presented by Akiko Maeda, The World Bank.
Maeda offered a few thoughts on how to explore this area, as discussed in her breakout group:
- Examine the landscape for opportunities without focusing too narrowly or broadly.
- Be aware of the acceptability of a strategy, and how to mainstream such models from the perspective of consumers, other professionals, and the market.
- Provide nurses and health workers additional support in business management.
- Understand the additional value that nursing and midwifery bring to coordination and management leadership.
- Provide long-term in-service training and support mentorship.
- Support a model in which the workforce is connected with the community, so that both can be empowered.
- Bridge secondary school graduates and postsecondary graduate programs with remedial education and rural pipelines, to provide a career pathway for disenfranchised or marginalized populations.
- Ensure fair, market-comparable wages while still maintaining affordability.
- Shift the paradigm away from immutable groups of professionals with specific skills toward a matching of health care needs and skillsets that creates value.
PROMISING APPROACHES: BRINGING TOGETHER THE KEY ELEMENTS OF NURSING/ MIDWIFERY PRACTICE AND EDUCATION/TRAINING AND SOCIAL ENTERPRISE/SOCIAL FINANCE3
Group leader Krishna Udayakumar explained that the discussion in his group explored the pathway from the inputs of education, training, and practice of nurses and midwives and social investment and enterprise to the outputs of health systems strengthening and women’s empowerment. He presented one potential framework to illuminate that pathway, which could be applied to multiple models of health care delivery in the United States and abroad (see Figure 8-1). In the middle of Figure 8-1 is the strengthening of organizations that deliver health and health-related services, especially those focused on community and primary care, as well as maternal and child health. These organizations include business models, traditional provider models, and, eventually, new provider models. Adequate educa-
________________
3 This section summarizes information presented by Krishna Udayakumar, International Partnership for Innovative Healthcare Delivery (IPIHD).
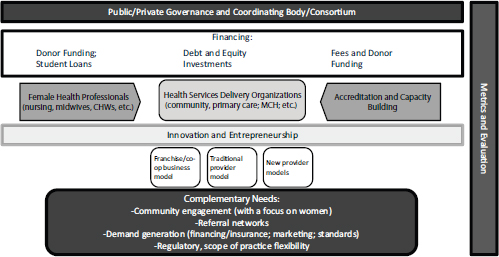
FIGURE 8-1 A framework for strengthening health systems and empowering women through nursing and midwifery and social enterprise: The long-term vision.
NOTE: CHWs = community health workers; MCH = maternal and child health.
SOURCE: Udayakumar, 2014.
tion and training of female health care professionals (including nurses, midwives, community health workers, physicians, etc.) can strengthen these organizations, as can accreditation and capacity building functions. Feeding into this is a culture of entrepreneurship that not only builds from known models but also continues to innovate.
Each of the pieces are financed by different mechanisms: education and training could be funded by a combination of donor and government sources as well as student loans; provider organizations could be supported through debt and equity investments; and accreditation organizations could be funded by fees from the providers as well as some donor and government organizations.
Additional complementary needs to enhance the framework include community engagement, referral networks, demand generation, and flexibility in both regulatory and scope of practice issues. Udayakumar remarked that it is unlikely any single actor could create such an ecosystem, and that a consortium governance model might be most effective.
While this is a long-term vision, individual participants emphasized that team-based professional education and clinical training models—particularly focused on community primary care and leadership development—could be important elements for the short term. Udayakumar also stressed the transformative potential of using established best practices, building models, and providing a defined core basket of services to horizontally integrate
across disciplines. He suggested that provider organizations could make a commitment to women’s empowerment by adding related metrics into their evaluations.
FINANCING REVERSE INNOVATION4
Following the group leader presentations, Deborah Bae remarked that a number of the issues raised in lower- and middle-income countries have direct and indirect application to the United States, where there are pockets of poverty and high variability in access to services. She cautioned that rather than thinking about two systems, one for OECD-member (Organisation for Economic Co-operation and Development) countries and the other for developing countries, there could be convergence around a single system, because a number of themes and issues are relevant across the globe.
She also highlighted the importance of integrating consumer engagement into health systems; quality metrics could resonate with the people whose health is being improved, particularly patient-reported outcomes. In fact, one good indicator of empowering patients is to provide them the tools to measure their own health, rather than always having to go to the clinic or doctor’s office.
From a funding perspective, she emphasized the value in learning from successful existing models then adapting and improving those models rather than continuously funding new pilots. She proposed a few ideas, such as social exchange labs and aggregators, where independent evidence can identify universal core elements of successful programs. But one frustration she voiced is that for more than four decades, programs and innovations have been funded without seeing big changes in health services provision in the United States. She cautioned that donor funding can be a double-edged sword; funding can and should support many innovative and even basic initiatives like scholarships, but they are not sustainable. She closed by noting that partnership and collaboration hold the keys to moving toward sustainability, and models from multiple countries could produce benefits in the United States.
REFERENCE
Udayakumar, K. 2014. Promising approaches and models: Report. Presented at the IOM workshop: Empowering women and strengthening health systems and services through investing in nursing and midwifery enterprise: Lessons from lower-income countries. Bellagio, Italy, September 10.
________________
4 This section summarizes information presented by Deborah Bae, Robert Wood Johnson Foundation (RWJF).






