Key Messages Identified by Individual Speakers and Participants
- Educators have only a certain amount of time to deliver a curriculum that provides students with the knowledge and experience they need to become competent, practicing providers. The focus should not be solely on designing a balanced work–life curriculum, but rather on finding the most effective pedagogy that maximizes opportunities and available technology. (Talbott and Valachovic)
- Task shifting/sharing or task-specific role training represents a departure from traditional delivery models that depend on specialist workers. Such shifts in responsibilities could also expand access of services—from preventive and wellness interventions to health care treatments—to more individuals and communities in response to a changing world with changing societal needs. (Wise)
- Processes and programs that best serve the target population or person, keeping in mind safety and quality, would build a less fragmented system through a team-based or collaborative approach. (Goldblatt and Tagliareni)
- Health literacy is one mechanism for rebalancing the power structures between health and wellness professionals, health systems, and society and is the currency for identifying solutions to society’s problems. (Cabe, Coleman, Pleasant)
ENVISIONING THE NEW WORKFORCE:
FRAMING ISSUES THROUGH DEBATE
Continuing on the theme of partnerships, Christopher Olsen from the Association of American Veterinary Medical Colleges (AAVMC) and the University of Wisconsin–Madison remarked about the wide variety of disciplines that have come together to discuss and debate issues of great importance to educators across the health professions. His intention in planning the agenda was to select crosscutting themes that resonated with all health professional educators in a transdisciplinary manner. In addition, Olsen wanted the material to be presented in a format that would engage the audience and demonstrate potentially useful pedagogy. Keeping with his intentions, two issues of mutual concern were identified by the workshop planning committee and illuminated using a debate structure.
The First Debate
The first debate was moderated by Deborah Trautman from the American Association of Colleges of Nursing (AACN) and pitted Richard Valachovic from the American Dental Education Association (ADEA) against the formidable challenger Richard Talbott representing the Association of Schools of the Allied Health Professions. They each argued one side of the debate proposition that read: “Health professional schools should adjust their curriculum and training to provide greater work–life balance for their learners.” Talbott argued for while Valachovic argued against the proposition.
Trautman set the stage for the debate by acknowledging that living and learning environments have become increasingly complex with many more interconnections. The health professions, as with others in higher education, are committed to creating an academic environment that is conducive to learning and attractive to students who will become the backbone of a future health workforce. Because of certain generalized personality traits exhibited in employees, employers and educational institutions that offer greater work–life balance may be particularly luring to the younger generation, known as millennials. However, whether this produces the strongest health workforce remains an issue of considerable controversy.
Some of the dispute is believed to be caused by generational differences that exist between millennials (people born between the years 1982 and 2005, also known as Generation Y) and their older teachers, mentors, and employers. According to Eckleberry-Hunt and Tucciarone (2011), millennials have certain distinguishing characteristics that set them apart from previous generations and create challenges as well as opportunities. This group is entrenched in technology. They are consummate multitaskers and
bore easily because they understand how to maximize and leverage new technology platforms. Many of them came of age during or were born after the September 11, 2001, attacks in the United States. Their era is marked by globalization, teamwork, and free expression through social media. They share a strong commitment for a balanced lifestyle and equality on the job, which has led some to describe them as lazy, unmotivated, selfish, and at times unprofessional with their inappropriate use of technology.
Box 3-1 lays out the arguments proposed by the two debaters that, according to them, do not necessarily reflect their true opinions.
BOX 3-1
Arguments For (Talbott) and
Against (Valachovic) the Debate Proposition:
Health Professional Schools Should Adjust
Their Curriculum and Training to Provide
Greater Work–Life Balance for Their Learners
Arguments For
- The value of a work–life balance
- “Decrease in work–life balance has been linked to higher unwanted turnover, lower physical and psychological well-being, lower productivity, greater stress-related ailments, and the like. The waste is immeasurable” (Rao and Indla, 2010, abstract).
- There is evidence on the negative public health impact of a poor work–life balance (Lunau et al., 2014).
- “People with higher education were more often found to have a strong work–life conflict (time and strain based).... A negative relationship between work-life conflict and health satisfaction over time was found. People reporting strong work–life conflict at every wave reported lower health satisfaction than people with consistently weak work–life conflict” (Knecht et al., 2011, abstract).
- Work–life imbalance worsens stress and anxiety. This begins in school and cuts across all health professions and across national borders.
- Examples of health professional students’ stresses and impacts
- Social work: A survey of 68 undergraduate and graduate social work students showed that about 34 percent of students indicated high levels of depressive symptoms and were at high risk of clinical depression, 6 percent met criteria for posttraumatic stress disorder, and 3 percent were highly likely to have a dissociative disorder (Horton et al., 2009).
- Nursing: Nursing students are particularly vulnerable to stress citing clinical practice as one of the most anxiety producing components in nursing programs. Stressors include lack of experience, fear of making mistakes, having difficult patients, discomfort at being evaluated, and concern over possibly harming a patient by giving them wrong information or medication
-
-
(Sharif and Masoumi, 2005). One study showed that one-third of nursing students experience stress that is severe enough to induce such mental health problems as anxiety and depression (Pryjmachuk, 2004).
- Medicine: “According to a 2006 Mayo Clinic study, students enter medical school with mental health profiles similar to their peers from college. But they begin to show higher rates of mental distress as they progressed through medical school. The same study found that the most depressed students often are the least likely to reach out for help because of stigma related to mental illness” (AAMC, 2013).
- Test anxiety affects all students and educational anxiety and depression cuts across borders. High rates of anxiety and depression related to academic performance has been recorded in Beirut, Europe, Greece, India, Malaysia, Pakistan, the United Kingdom, and the United States. In China there is tremendous anxiety around the risk of failure for all students (Saravanan and Wilks, 2014).
- How are students coping with stress? Studies have shown significant changes in health habits of students in response to the stresses and time constraints of high-intensity education. This includes increases in alcohol consumption and decreases in exercise and socialization. “The changes in health habits were predictive of both emotional and academic adjustment, with students who decreased in positive health habits, particularly socialization, being more depressed at finals” (Ball and Bax, 2002, abstract).
-
- What are the risks of a work–life curriculum imbalance and the potential benefits of work–life curriculum balance?
- Burnout, due to the rigors of school combined with any or all other personal commitments, has been shown to start in school (Dyrbye et al., 2006).
- Providing a greater work–life balance will prevent education-initiated professional burnout.
- These students are tomorrow’s workforce. They are needed to take care of today’s aging population.
- An unengaged health provider (and trainee) can be dangerous.
- Provide lifelong coping mechanisms.
- This generation learns through demonstration. Providing students with greater work–life balance speaks volumes regarding its importance for their physical and mental well-being.
- Create the next generation of faculty and role models.
- Being trained in a balanced environment will provide a positive introduction to the health professions.
- Burnout, due to the rigors of school combined with any or all other personal commitments, has been shown to start in school (Dyrbye et al., 2006).
- Globally, as of 2010 approximately 273 million (4.5 percent of the population) had an anxiety disorder (Vos et al., 2012).
- Providing the next generation with curricula and training that includes greater work–life balance for their learners will ensure a physically and mentally strong health workforce to provide care and to demonstrate to the next generation how to cope with the stress and rigors of education and future work.
Arguments Against
- Generation Y is just one cohort passing through history. Generations before them did not necessarily share their perspectives on life. Educators tend to view Generation Y as lazy, unmotivated, and selfish, and this view is shared in the business world. Generation Y counters that they simply want work–life balance. In other words, work does not come first. Millennials do not look at an organization to see how they will fit into it; rather, they look at how that organization will fit into their lives. These are relatively selfish, almost narcissistic, views for people professing to devote their careers to the care of others.
- The acceleration in knowledge has never been greater than it is today, and there is no reason that we should not expect it to accelerate even more over the next 40 years of Generation Y’s professional lives. Previous generations of health professionals were able to develop a command of knowledge about their field during their entry-level education and postgraduate training and continuing education that served them and their patients well over their careers. The current explosion of knowledge means that this will no longer be the case. This leads us to require our current students and residents to be able to develop competencies in contemporary health sciences, and to prepare themselves as critical thinkers and lifelong learners. If anything, this will mean more time and effort devoted to learning during their education and training.
- Graduating student debt in the health professions has never been higher. Adding more time to the curriculum for work–life balance would only increase the level of debt and diminish total earnings over the professional lives of these students.
- Limiting the time devoted to patient care by students and residents affects the safety of current and future patients. There are no rigorous studies that show that restricting student and resident work hours increases patient safety. In fact, there are studies that show that limiting the time that learners devote to patient care reduces their ability to follow a hospital patient over the length of his or her stay.
Debaters’ Comments
Valachovic said he believes that educators have only a certain amount of time to deliver a curriculum that provides students with the knowledge and experience they need to become competent, practicing providers. The focus, he said, should not be solely on designing a balanced work–life curriculum, but rather on finding the most effective pedagogy that maximizes opportunities and available technology. Talbott agreed and added that numerous structural changes to how students learn were mentioned previously by speakers (i.e., greater community engagement). These changes could be part of the solution for bridging the generational workforce gap.
United States–Nigeria Comparison
Following the debate, Emilia Iwu, a U.S.-based Nigerian nurse working on her doctoral degree in nursing at Rutgers University, provided her perspective that compared and contrasted work–life balance in Nigeria versus North America. The culture and context are different, she said. In Nigeria, students work very hard with the understanding that they will be able to relax in the future. Delayed gratification is a well-accepted way of life in Nigeria. In Nigeria, younger students tend to enroll full-time while pursing college education, while students in North America often work while attending school. She could understand the need for a work–life curriculum for older adult professional students who combine employment and university education, and how they would benefit from such strategies. She also acknowledged the dilemma between the need to acquire the necessary knowledge and skills to deliver upon graduation and the risk of overloading the curriculum.
Another difference Iwu identified is the limited access Nigerian students and professors have to technological resources. In North America, access to stable Internet and e-learning platforms are readily available. In Nigeria, most of the teaching is done face to face and is paper based, and students’ technological capabilities are not fully tapped. One cross-cultural challenge Iwu has observed is the pressure of an overburdened curriculum.
Perspective of a Chinese Physician and Educator
Xuejun Zeng, a medical doctor and educator at Peking Union Medical College, provided her views of the work–life balance in China from a provider’s and educator’s perspective. Learning how to balance life and work are major challenges for Chinese physicians, often times resulting in a lack of balance between work and life.
Some students are opting not to go into medicine because of the over-
whelming pressure associated with the profession. Many Chinese health care workers have joined teams as a way of overcoming some of the work-related stresses. Regardless of the coping mechanisms, Zeng was clear that certain pressures are inherent in medicine and must be expected. She believes that students understand this when opting to go into medicine. In some ways, students enjoy the hard work that goes along with their studies and experience inner growth when taking care of patients, she said. Often times, young physicians are guided by attending doctors as they learn how to manage time, find their role on a team, and communicate with patients and their families.
Zeng believes that obtaining these competencies improves students’ ability to better balance their life with their work. She added that role modeling plays an important part of their personal development. But she is also aware of a lack of social and emotional support from peers and the stress this can create, particularly for junior physicians. And while it makes sense to her that she and her colleagues should pay attention to mental health issues among their colleagues and students, it is hard to adjust the traditional attitude of working hard in her profession. Diligence is still greatly valued in China.
Zeng has started a train-the-trainer program for junior attending physicians on how to educate and better support students and residents during their clinical work, the time of greatest stress and the least opportunity for balance.
The Second Debate
Holly Wise from the American Council of Academic Physical Therapy moderated the second debate that addressed whether or not new task-specific roles should be the strategy for health professionals to meet individual and community health needs. Wise explained the debate issue in terms of tasks.
There are task-specific roles and there is task shifting that began as a cost-effective way to address chronic workforce shortages. Task shifting involves scaling up the health workforce through the rational redistribution of tasks among health teams, said Wise. Specific tasks are moved where appropriate from health workers with more in-depth training to health workers with less training or possibly to community members or others who receive training in one specific area in which they are needed to work.
In the end, the purpose of task shifting is to make more efficient use of the available human resources. It should not be associated with second-rate services. On the contrary, task shifting could be a means of improving the overall quality of health by moving the bulk of culturally appropriate human resources closer to the communities they serve, as is the case with
community health workers. Task shifting, that some term task sharing, could also save money if less expensive health professionals are used for routine care while the more expensive health professionals focus on issues they are uniquely qualified to address. In 2006, the World Health Organization (WHO) launched a task-shifting plan that involved retraining health workers for specific roles in response to the HIV/AIDS crisis and the workforce shortages in areas around the world. There have been other instances where people with chronic conditions such as asthma or diabetes have been trained to manage their own care; then, with additional training, the same people become peer navigators offering valuable services to health teams.
In essence, task shifting or task-specific role training represents a departure from traditional delivery models that depend on specialist workers. Such shifts in responsibilities could expand access of services—from preventive and wellness interventions to health care treatments—to more individuals and communities in response to a changing world with changing societal needs.
With the explosion of information technologies and the growing access to personal health data against a backdrop of low health literacy levels, there is great potential for new configurations of health workers. For example, information technology (IT) workers could be hired to obtain online medical histories and perform other basic tasks involving virtual communication with patients or clients. Such task shifting and role-specific training could be proposed as an efficient approach to scaling up the health workforce that could reduce costs in certain circumstances, although it would require new resources and infrastructure. It would require a system of checks and balances involving credentialing, regulation, and legislation, just to name a few of the challenges. Quality assurance mechanisms need to be put in place to protect the people receiving the care as well as the health workers themselves, said Wise. Key elements must be in place to ensure that this strategy is safe, efficient, effective, equitable, and sustainable.
These comments provided the context in which the debate arguments were made. As seen in Box 3-2, Liza Goldblatt, representing the Academic Consortium for Complementary and Alternative Health Care, spoke in favor of creating new task-specific roles while Elaine Tagliareni from the National League for Nursing spoke in opposition of the proposition.
Debaters’ Comments
Goldblatt believed the best strategy would be to expand the reach of health providers into communities by including local workers into the health care team. The precise mix of team members would be situation dependent and would vary with the environment. Processes and programs that best serve the target population or person, keeping in mind safety and
BOX 3-2
Arguments For (Goldblatt) and
Against (Tagliareni) the Debate Proposition:
The Creation of New Task-Specific Roles Should Be the
Strategy for Health Professionals to Meet Individual and
Community Health Needs
Arguments For
- This is already happening in Brazil under Francisco Campos and in New Mexico as noted by Arthur Kaufman, so there are models to draw from throughout the world.
- Better use of health workers with defined skills will maximize the limited time of health professionals and improve the financial resource allocation so expensive professionals perform interventions they are uniquely qualified to do, as well as being part of a health care team approach. The health workers would serve as liaisons between the individual and the team to help relieve some of the burden of the health professionals.
- Health workers would be drawn from the communities they serve and thus would ensure culturally sensitive care is provided. In the United States, with more than 75 percent of the health care dollars being spent on people with largely preventable, chronic conditions (Gerteis et al., 2014), more health coaches and other local community members who specifically focus on lifestyle issues are imperative for ensuring compliance through frequent follow-up. A collaborative, team-based person/patient-centered approach would include these workers.
- Greater employment of community workers would improve the local economy.
- More efficient care through the targeted use of technology for communication.
Arguments Against
- Case study: Health Affairs, March 2015 (Aronson, 2015)
- Story of Eva: Fragmented care, no coordination of services, limited effectiveness of clinical practice by task-oriented health care professional.
- One year later: Three caregivers managing her care with only one specialist. What made the difference? Integration of services, ability of key staff to manage comprehensive care.
- Conclusion: Comprehensive realignment of the current workforce and modification of traditional roles for both providers and patients.
- Why? Changing role of consumer and health care workforce.
- Rise of consumerism and more use of Internet and patient assuming the role of authority for treatment alternatives.
- Evolving role of health care workforce with emergence of informatics and collaborative practice: Health care is now an information-intense activity; this role belongs to all health care workers.
- Challenge: There is a flux in the current roles of both patients and providers as they both increase the scope of health-related information.
- International and national models of retraining existing workforce to accelerate the process.
- WHO—Scaling up HIV services: “Treat, Train, and Retain” Plan to strengthen and expand the scope of current workforce.
- Helping Babies Breathe Global Development Alliance in Tanzania: training existing midwife workforce specifically on facilitating breathing and decreasing maternal hemorrhage. There has been a 47 percent decrease in neonatal mortality since 2009 due to this specific intervention (Msemo et al., 2013).
- Banner Health in Arizona: Retraining medical assistant, already in the system, to free up physicians and nurse practitioners from traditional roles (i.e., inform about normal labs results); shifting tasks across teams.
- Raising the visibility of solutions.
- At a time when the world is facing a shortage of health workers, the focus needs to be on policy and programs to bolster the global health workforce. Think globally and act locally to build clinical practice that retrains and re-delegates functions within the system.
quality, would build a less fragmented system through a team-based and collaborative patient/person-centered approach. Goldblatt strongly feels that this approach should promote health and well-being in addition to improving the treatment of diseases and conditions and should draw on resources that uniquely benefit the local community.
Tagliareni agreed that it is a hybrid, but when she thinks about the solution, she feels collaborative practice is where the focus needs to be; instead of emphasizing sharing tasks, the focus should be on the competency a person or patient requires from the team. In this way, roles will shift as modes of practice take precedence over single tasks. That means health practitioners have to understand they do not “own” their role but that it is defined by the context and function of the team and the work ahead of them.
Perspective of a Nurse from Nigeria
Emilia Iwu again provided her perspective on the debate topic—this time as a nurse practitioner working in Nigeria. She began her remarks by telling the participants that Nigeria is among the sub-Saharan African countries that adopted task shifting as a model of care provision. Task shifting is
currently referred to as task sharing because of misconceptions that created a threatening environment as health care workers feared they would lose their traditional responsibilities entirely. Some role recipients were afraid of task dumping. Therefore, task sharing is a more representative term that describes the team work involved.
Task sharing is not a new concept, said Iwu. It has been in use since the precolonial and colonial era, when lay workers were trained to perform task-specific roles as dispensaries and health posts. However, the term task sharing is fairly new and has many advantages. As a result of task sharing in Nigeria, nurses, midwives, and community health workers have improved access to antiretroviral treatment. With appropriate training, peer educators and community volunteers assist with HIV treatment support. These roles motivate and empower new cadres of workers and encourage their participation in health service delivery, especially in communities. They often work in hard to reach areas, thereby improving access to services, bringing care closer to clients’ homes, and significantly reducing travel time for many consumers. Task shifting has saved many lives. It could involve training and use of new health workers or retraining and expanding the roles of existing workers. Examples include Life Saving Skills1 and Helping Babies Breathe,2 described by Tagliareni in maternal child health services. In these situations, nurses and midwives received training on evidence-based interventions that ultimately decreased neonatal mortality. In Nigeria, similar programs in addition to prevention of HIV transmission from infected mothers to their infants involve expanded roles for nurses and midwives. According to Iwu, when collaboration and teamwork truly exist, task sharing that engages a multidisciplinary team of health workers is a perfect mix. It is cost-effective both in the short term and the midterm.
Despite the potentially positive impacts, said Iwu, there are some drawbacks. Regulatory issues and service structure often lag behind role creation and transition. This underscores the importance of advocacy for appropriate and timely regulatory changes from the onset. Lack of commensurate compensation for new roles, nonabsorption of the nontraditional, and new cadres of service providers often complicate implementation of task sharing if not tackled proactively. Unrealistic professional restrictions that limit the scope of practice and training for some health workers prevents maximum participation in patient care. Restrictions on maximal training limits their capacity to prevent health emergencies in the presence of obstacles for timely referral or patient access to the next level of care. Adequate training
________________
1 For more information about Life Saving Skills, visit http://www.midwife.org/Life-Saving-Skills-LSS (accessed August 20, 2015).
2 For more information about Helping Babies Breathe, visit http://www.helpingbabiesbreathe.org (accessed July 6, 2015).
and access to mentoring providers are crucial elements. Another challenge, Iwu said, is sustainability; creating roles for health workers through parallel structures that are not integrated into existing health systems halts services when external funding is no longer available.
In general, incorporating new cadres of workers into existing civil service structures could be a difficult task. Policy makers need to be engaged at the initial planning stages, said Iwu. Collaboration with the appropriate leadership and stakeholders ensures support and facilitates policy changes. These provide the enabling environment for effective task-sharing implementation and scope-of-practice modifications.
Iwu was reluctant to commit to a debate side, but she did provide the global context in which these issues could be further considered.
GLOBALIZATION AND CHALLENGES TO HPE
Andrew Pleasant is the senior director for Health Literacy and Research at Canyon Ranch Institute (CRI) in Tucson, Arizona. He moderated the session that focused on health literacy which, according to CRI, “allows the public and personnel working in all health-related contexts to find, understand, evaluate, communicate, and use information to make informed decisions about health” (The Centre for Literacy, n.d.; CRI, 2011). This is what CRI board president Richard Carmona described as the currency for his success as the 17th surgeon general of the United States. Carmona (2003) states that health literacy could save lives and money, as well as improve health and well-being. Pleasant framed his remarks around health literacy as the “currency of a globalized health professional education.”
In his introductory remarks, Pleasant began by describing how health and literacy come together to create health literacy. He described health as not just the absence of disease but as a resource for life. He labeled literacy as reading, writing, speaking, listening, and numeracy as well as being able to apply those skills. The power of literacy begins to be revealed, he said, when people (usually but not always at a younger age) transition from learning how to read to reading to learn. That is an important transition during which people begin to use skills to not only inform themselves but also to change the world.
Pleasant referred to some of the origins of health literacy that began within a traditional health and medical context. An example used was a medication instruction to take one pill three times daily. One problem with this medication instruction is the lack of specificity so that instead of spreading out the dose, all three pills might be taken in the morning hours—leading to potentially dangerous situations. Another example highlighted the use of technical terms such as sodium, trans fats, and radiography that are unknown or unfamiliar to most people, especially those at the lowest
literacy levels. Providing practical information in more common terms like salt, fat, and X-rays would be a universal precautionary approach to health literacy.
According to Pleasant, health literacy is one mechanism for rebalancing the power structures between health care systems and society. He explained his remark by highlighting the complexity of health insurance language, forms, and bureaucratic structures and requirements that he feels could be easily simplified to lower barriers to the public’s understanding of health and health care navigation. Chronic disease prevention and treatment are other areas where people could grasp concepts and use information to make informed choices more easily if instructions were expressed in terms that are more readily understood. Pleasant noted the link between low health literacy and poorer health outcomes, and said that the cause for this is not necessarily the fault of the individuals but rather a result of complex systems and judgments made in those systems about people with low health literacy. For example, he said, people with lower health literacy have been shown to be less likely to receive referrals for kidney transplants given the same medical condition as those with higher health literacy (Grubbs et al., 2009). And people with low health literacy are also more expensive to health systems, he said, because they present later and in worse health conditions than their more health literate counterparts (IOM, 2004). In this regard, Pleasant concluded that health literacy is the strongest social determinant of health.
According to data in the report by Kutner et al. (2006), 53 percent of adults in the United States have intermediate health literacy, 36 percent have basic or below basic health literacy, and only 12 percent were considered proficient. While Pleasant reiterated the correlation between low health literacy and poor health, he also highlighted that there are outliers on either side—those who have low health literacy but excellent health and vice versa—who are just now beginning to be studied. A similar pattern to the United States is seen in Europe. The European Health Literacy Survey (HLS-EU) (2012) found that roughly 47 percent of respondents had inadequate or problematic health literacy scores, and the roughly half remaining were either intermediate (36 percent) or proficient (17 percent). Pleasant also pointed out that while the bulk of health literacy studies have focused on the deficit model (lower health literacy producing poorer health outcomes), a paucity of studies have examined the area of how higher health literacy actually produces better health outcomes.
Pleasant then shared his “roadmap for behavior change” that builds a logic model based on a foundational awareness of:
- Fundamental literacy: If your language fails, you fail.
- Scientific literacy: If you remove the science, you fail.
- Cultural literacy: If you ignore culture, you fail.
- Civic literacy: If you do not engage and empower people, you fail (Zarcadoolas et al., 2006).
When all of these elements are addressed, it is then feasible and fruitful to help people find, understand, evaluate, communicate, and then use information. Pleasant described this as his logic model of health literacy that is used at CRI for applying their theory of behavior change. The first step in his model is the ability for people to find information. The next step, he said, involves assisting and supporting people in understanding that information and then evaluating the practicality of that information based on one’s personal life situation and lived environment. Pleasant believes that health literacy extends further to helping people communicate to others in their lives what they have understood and evaluated. He remarked that from his experience, this communication begins to build social support for the informed decisions and potential future changes in behavior. Finally, he said, people can use their health literacy to inform decisions about their health in order to make and sustain behavior changes. Pleasant pointed to numerous examples of programs around the world that have started to put health literacy into their training programs (IOM, 2013). Some of the examples were presented at the workshop by Clifford Coleman and Jennifer Cabe.
Integrating Health Literacy into Health Professional Education
Clifford Coleman, M.D., M.P.H.
Oregon Health & Science University
Cliff Coleman works at a Federally Qualified Health Center (FQHC) clinic at the Oregon Health & Science University. Coleman is a nationally recognized expert in the field of health literacy. His teaching and research activities focus on workforce training to improve the clinical and public health response to low health literacy. He began with a quote from the composer John Powell who said, “Communication works for those who work at it.” According to Coleman, what educators and providers have learned from studying health literacy over the past decade is that health professions schools have not been addressing health literacy in the correct manner. This provides a tremendous opportunity to transform health professions education to dramatically improve care and outcomes.
The Institute of Medicine (IOM) recognized this issue in a 2004 report noting that health professionals lacked adequate education around health literacy and called for better training in this area (IOM, 2004). Although the U.S. educational system has responded slowly to this recommendation,
there has been some movement in recent years. Coleman confirmed this in his 2011 literature review (Coleman, 2011). He also identified a trend in the health literacy curricula of the health professions that fell into three categories. The first is the typical and most common way institutions have approached health literacy training, which is through stand-alone lectures or one-time workshops. The second is somewhat less common, which is to educate using a series of instructional workshops or didactic series. And the third is merely suggested by the literature, which is to integrate a health literacy curriculum for health care professionals. Such a program would infuse health literacy into education through multiple topics in a seamless manner that may not be overtly apparent. This is what Coleman and his colleagues are undertaking at Oregon Health & Science University.
At roughly the same time as the literature review, Coleman and Appy (2012) looked into how U.S. medical schools were addressing health literacy in their curricula. Of the 133 allopathic schools surveyed, 63 responded and 44 of them acknowledged the topic in their required curricula. However, the average amount of time devoted to health literacy education was approximately 3 hours over the course of a 4-year curriculum.
More recently, Coleman studied family medicine residencies in the United States. There was a 31 percent survey response rate (137/444) to his survey, with 58 programs indicating inclusion of health literacy in their required curriculum (Coleman et al., n.d.-b). On average, residents received about 2 to 5 hours of instructional time over the typical 3 years residency program. What was most interesting to Coleman was that almost every one of the residency directors who responded with comments said that better training around health literacy would significantly improve the clinical care their residents could deliver.
After considering the results of his surveys, Coleman then went back to the findings from his earlier literature review. What he uncovered was that health literacy curricula were being held back by a lack of competencies. Health professions educators were unsure what to teach their students and learners about health literacy. To respond to the need, Coleman, Hudson, and Maine (2013) published a consensus report that looked across all health professions and identified 62 health literacy competencies trainees should have before graduation. In addition, 32 best practices were identified out of this study (see Table 3-1).
While this study did identify a broad set of health literacy competencies important to a wide array of health professions, the total number of competencies was too large for practical purposes. His solution was to prioritize the long lists of competencies, which he and colleagues are undertaking in a follow-up study that is not yet published.
Coleman then addressed data on the effectiveness of health literacy educational interventions. It appears that learners do improve their self-
TABLE 3-1 Results: Competencies and Practices Accepted by Delphi Round
| Item Type | Round 1 | Round 2 | Round 3 | Round 4 | Total |
| Knowledge | 19/24 | 5/5 | –/– | –/– | 24/24 |
| Skill | 21/28 | 2/4a | 2/3b | 2/3 | 27/29 |
| Attitude | 11/11 | –/– | –/– | –/– | 11/11 |
| Practice | 27/32 | 4/5 | 1/2c | 0/1 | 32/33 |
| Total | 78/95 | 11/14 | 3/5 | 2/4 | 94/97 |
| (82.1%) | (78.6%) | (60%) | (60%) | (96.9%) | |
a Three skill items were sent out with incorrect wording in Round 2 and were rated again in Round 4.
b One skill item divided into two separate items for Round 3.
c One practice item added in Round 3.
SOURCE: Coleman et al., 2013, as presented by Coleman on April 23, 2015.
perceived knowledge about and intentions to use health literacy best practices (Coleman and Fromer, 2015; Mackert et al., 2011). However, those intentions appear to be short lived based on Coleman’s study of medical students at Oregon Health Sciences (Coleman et al., in press). Looking at more advanced trainees, their knowledge persisted over time, but they reported not implementing what they learned. The same cycle occurred following supplemental health literacy training (Coleman et al., n.d.-a). This led Coleman to assume there is something about the system that is not supporting the adoption of health literacy practices. It led him to radically transform their medical school curriculum that was based on five guiding principles as follows:
- Moving from systems-based to case-based curriculum
- Organized in seven blocks of related systems
- Clinical and science “threads” run longitudinally
- Compressing preclinical curriculum to 18 months
- Competency driven
The main change was to thread health communications longitudinally throughout the curriculum so important issues like health literacy are continuously reinforced. For health literacy, Coleman and his colleagues drew ideas from Kaiser Permanente in developing their own “habits model.” The model tracks four domains during multiple simulated patient encounters taking place during the preclinical curriculum. These include
- Habit 1: Make a positive connection.
- Habit 2: Establish an agreed upon agenda.
- Habit 3: Facilitate understanding.
- Habit 4: Confirm understanding.
To operationalize these habits, students practice with standardized patients every 2 weeks. It is at these encounters where students demonstrate their growing skills and knowledge within these four domains. Habit two involves negotiating a shared agenda at every encounter. Habit three includes providing need-to-know information up front, trying to limit the amount of information provided to the most important, and avoiding medical jargon in conversations with patients. Habit four asks students to elicit questions in a patient-centered manner and then use a teach-back3 technique to be sure the student communicated clearly.
Coleman then gave the floor to Jennifer Cabe to expand the health literacy discussion and revisit integrating health literacy into health professions’ curricula.
Applying Best Practices of Health Literacy
Jennifer Cabe, M.A.
Canyon Ranch Institute
Jennifer Cabe is executive director and a board member for CRI, a nonprofit, public charity focused on advancing health literacy and improving prevention using integrative approaches to health. She is also a member of the faculty at the Ohio State University (Ohio State) College of Nursing. Cabe previously worked in the Office of the Surgeon General, where she was responsible for the development and implementation of health literacy and communication initiatives in partnership with health professionals, advocacy groups, policy makers, community leaders, and the public. In her presentation, Cabe described three programs. The first is the new Bachelor of Science in Health and Wellness Innovation degree at Ohio State; the second is the CRI Life Enhancement Program (CRI LEP); and the third is the CRI Theater for Health program.
Bachelor of Science in Health and Wellness Innovation
This new bachelor’s degree offered by the Ohio State College of Nursing is designed to meet a variety of community needs as well as the interests
________________
3 According to the Agency for Healthcare Research and Quality (AHRQ), the teach-back method verifies that patients understood directions before leaving the provider’s office.
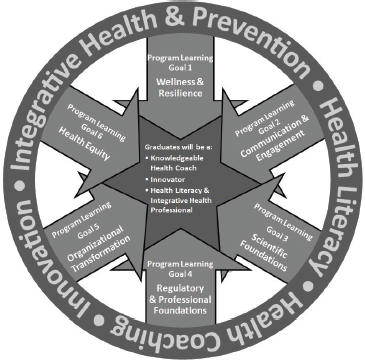
FIGURE 3-1 Bachelor of Science in Health and Wellness Innovation.
SOURCE: Cabe, 2015, courtesy of Canyon Ranch Institute.
of the health care delivery system and those individuals who wish to work in that system but not necessarily in the existing, traditional models. As seen in Figure 3-1, the program is made up of six learning goals that focus on integrative health, prevention, health literacy, and health coaching, all under the rubric of innovation. Cabe believes that part of the popularity of the program is due to students seeing career opportunities in wellness, thanks in part to requirements under the Patient Protection and Affordable Care Act mandating a focus on wellness for large employers and some government entities. This program will build a workforce so organizations can improve their employees’ health outcomes and productivity through wellness activities.4
________________
4 For more information on the CRI partnership with Ohio State, visit http://www.canyonranchinstitute.org/partnerships-a-programs/partnerships/ohio-state-university-college-ofnursing (accessed September 8, 2015).
CRI Life Enhancement Program
Since 2007, CRI has partnered with a variety of U.S. health care delivery organizations in implementing the CRI LEP. The program takes a multidisciplinary, integrative approach to educating partners about how to transfer evidence-based, best practices for preventing, diagnosing, and addressing chronic disease in underserved communities. Their methods are grounded in the best practices of health literacy as described previously by Andrew Pleasant. CRI LEP partners include FQHCs, small rural hospitals, large health and hospital systems, and clinics. All CRI LEP partners serve low-income populations at high risk for chronic disease.
The program focuses on seven core elements:
- Behavior change
- Integrative health
- Nutrition
- Physical activity
- Sense of purpose
- Spirituality
- Social support and follow-up
One week of training takes place in Arizona at Canyon Ranch Health Resort then the CRI LEP Core Team (the Core team), comprised of the partner’s health and wellness professionals, receives on-site training in their community from CRI staff. Local partners and CRI create innovative solutions tailored to the community to address the existing social determinants of health. For example, how might local organizations help their community members with resolving unemployment or underemployment, poor access to fruits and vegetables, and food shortages? The multidisciplinary core team provides at least 40 hours of group sessions and four 1 hour one-on-one consultations for each CRI LEP participant in the areas of integrative health, behavioral health, nutrition, and exercise. To maximize training, each organization must have classrooms and space to engage in fitness activities. CRI collaborates with partners to find funding for, design, and build innovative additions such as teaching kitchens, fitness centers, walking groups, exercise classes, and gardens.
Core team members experience a hands-on, experiential training, including a simulated participant exercise with someone who is trained by CRI to portray a typical participant from the community. This exercise aims to help the team member learn about the participant’s needs and help the participant identify a series of small step behavior changes that can improve his or her health and well-being. A critical component of the simulated participant exercise and of the program itself is what Cabe referred to as
the hand-off. This is when the Core team member recommends a Core team professional (e.g., an integrative health expert, a behavioral health expert, a nutritionist, an exercise specialist, or an expert in spirituality) to the participant. The decision is based on the health professional’s and the participant’s mutual assessment of the participant’s needs. The hand-off also requires each health care professional to provide the team members with an in-depth understanding of each participant’s needs and health status.
Much of the focus here is on building the team. For CRI, team building involves the health professionals understanding and engaging with the work of other professions on the Core team as well as learning how to support the other core team members during challenging times—all with the focus on providing optimal care for their patients and communities. After partners complete the 12-week program and demonstrate their ability to support themselves, the CRI team’s work is complete but not over. The established partnership continues through CRI coaching the core team members via in-person and virtual connections as long as the partner offers the CRI LEP.5
CRI Theater for Health Program
The CRI Theater for Health program started in 2010 as a partnership between CRI and The Clorox Company to advance health literacy and improve household hygiene through the arts in two impoverished communities on the outskirts of Lima, Peru (CRI, 2011; Pleasant et al., 2014). This effort extended the work of Brazilian Augusto Boal (1993), who originated Theatre of the Oppressed—an approach that uses theater to promote social and political change by actively engaging audiences in exploring real situations through the arts (Sullivan et al., 2008). Pleasant and Cabe of CRI and Andre de Quadros of Boston University College of Fine Arts built on the work of Boal to create Theater for Health program in Peru.
In the Lima communities, the overall objective of the program was to decrease the spread of disease from E. coli and Listeria using a series of telenovela-style live performances. The shows were held every weekend in outdoor spaces in the communities for 12 weeks and built stories and plots of romance and intrigue around characters as a way of maintaining the audiences members’ interest in the production. Local actors encouraged community attendance and involvement at the shows by engaging them in developing solutions to real-world health issues in the com-
________________
5 For more information on the CRI LEP, visit http://www.canyonranchinstitute.org/partnerships-a-programs/cri-life-enhancement-program/cri-lep-overview (accessed September 9, 2015).
munity, question-and-answer sessions, and providing rewards for their participation.
This creative process started with formative research with the communities. The research findings were included in an intensive 2-week workshop held in Lima that involved the interdisciplinary team of local actors, directors, and stage personnel; scientific experts from Peru and the United States; and team members from both countries with academic and professional backgrounds in arts, public health, health literacy, and communication. This process educated the artists about the science of household hygiene, and educated the scientists about the process of using the arts in an interactive manner to address health issues. Through this process, the ideal local individual was identified to transform the role of the “Joker,” in Boal’s terms, into a source of valid scientific information for the community members before, during, and after each performance.
Artistic and scientific team members also collaboratively drafted four episodes during that preparatory workshop before the program implementation began, and the other eight episodes were drafted as the program was being implemented. The overall story line was adjusted on a weekly basis to incorporate participating community members’ input and reactions to the previous episodes. After initial drafting, each script was reviewed for language appropriateness, content accuracy, and cultural relevance. In fact, every episode was subject to continual refinement up to the moment of presentation in the community, and input from participating community members was also incorporated on a weekly basis. This input was received during the opportunities for participating community members to interact during each performance and through 20 qualitative interviews conducted with randomly selected audience members after each performance. This created a continuous quality improvement process that incorporated perspectives and information from the interdisciplinary team of scientific experts and artists who trained together, as well as community members. The approach ensured continual engagement of the interdisciplinary team and the community in order to enhance the diffusion and adoption of improved household hygiene behaviors.
According to Cabe, the program was a success for many reasons, including the fact that more than half the families from the Peruvian communities reporting changes in their families’ hygiene behaviors, and a documented decrease in the percentage of positive E. coli and Listeria samples in household food preparation areas.
Understanding and Serving a Globalized Community
Susan Scrimshaw—who was on the IOM committee that produced the 2004 report on health literacy—commended Pleasant on mentioning culture
in his roadmap for behavior change. One issue in developing the culture piece, she said, is that words have different meanings. Even the same word can have a different meaning in different languages. For example, the word stress in the Latin American culture means something very different than the term used in English-speaking nations. And in Brazil where Portuguese is the predominant language, the word trauma relates more to emotional stress versus being physically hit as it is typically referred to in English. To Scrimshaw, the challenge within health literacy is the cultural piece.
Pleasant then asked the group to reflect upon whether health professionals are being prepared to function and serve in a globalized community. In responding, Lemmie McNeilly from the American Speech–Language–Hearing Association stayed with the cultural theme. Given the variety of cultures around the globe, she said, it would be impossible to truly educate anyone to function competently to practice globally and understand all cultures and all languages—yet it is very important that health professionals recognize and celebrate cultural differences. This would involve demonstrating sensitivity to cultural differences, understanding the value of differences, and being educated to use members of the community as interpreters of both the language and the culture, she said. In this way, the provider is able to validate an individual’s values, beliefs, and practices, and is less likely to make assumptions about individuals from other cultures. McNeilly also said it is important not to overgeneralize and assume that a person from a particular culture espouses all of the beliefs and practices associated with that culture.
Michelle Troseth from Elsevier and also representing the National Academies of Practice commented on the importance of cultural competence in preparing health professionals to work in a globalized community that brings the focus back to the individual and the patient. But with the advent of new technologies like the electronic health record, the focus on the person risks being lost. There need to be some common practices across all the professions, she said, to ensure that perspective remains central. One of these practices could involve a shared core competency about health literacy and the teach-back method, which in her opinion would be relatively easy to accomplish.
The teach-back method also resonated with Joanna Cain from the American Board of Obstetrics and Gynecology and the American College of Obstetricians and Gynecologists. She proposed asking the community how they would like their health professionals prepared for work with their community. One possibility would be to have what Cain termed as a “checkout” designed by the communities themselves. The health provider would develop half a page and the checkout person would have the other half to record all the things the health provider missed, misunderstood, or did not cover adequately. It would be akin to a check on how well the provider communicated, and the teach-back method could be the training
tool for all the professions. And while she endorsed this idea, she also questioned its sustainability given present-day pressures to cut costs and shorten providers’ time with patients.
Edward Saltzman representing American Society for Nutrition also commented on the need for students and trainees to obtain foundational skills that are transferrable across different situations and encounters. These skills would be applicable to practice globally and locally, and would create an awareness of the effects of global events on local communities. Many of these skills are components of health literacy as described by Pleasant, Coleman, and Cabe, but competency in cultural sensitivity would be particularly relevant.
Malcolm Cox approached the question slightly differently by expanding the discussion beyond culture. The glue that holds effective education together is work in the community. And while important, health literacy is just one of the ways to enhance community engagement. He challenged the group to think about how a set of constructs might be created that can be used within a community framework to help revolutionize the existing curriculum. This would provide a generic solution that could be taken to deans as the basis for a more specific toolkit for educating health professionals.
Improving Communication in a Globalized World
The next question was addressed using a rapid-fire presentation technique where participants succinctly share ideas in a short amount of time. Table 3-2 is a compilation of the responses generated from the question: How might health literacy be globally integrated into health professional education to improve communication in a globalized world?
As a parting thought, Coleman believed that providing understandable, actionable health information is an ethical imperative that needs to be included in the ethical foundations of training for all the health professions. Access to understandable information is probably the greatest health disparity faced today by all nations. Perhaps by modifying ethical standards that focus on communication it may be possible to approach this disparity on a global scale.
TABLE 3-2 Participant Responses to “How Might Health Literacy Be Globally Integrated into Health Professional Education to Improve Communication in a Globalized World?”
| Person | Affiliation | Response |
| Joanne Schwartzberg | Accreditation Council for Graduate Medical Education | Always ensure that you have understood the patient and use teach-back techniques to ensure that the patient has understood you. |
| Francisco Eduardo de Campos | Former National Secretary of Labor and Education Management in Health of the Ministry of Health, Brazil | Expand the use of community health workers as translators between providers and patients. |
| Brenda Zierler | University of Washington | Do not forget faculty, staff, and preceptor skills development; experiential learning in practice can be used along with training in simulation labs for greater imprinting of experiences. |
| Jan De Maeseneer | Ghent University | Health literacy is not a medical issue but an educational issue; integrate health literacy into all educational tracks, starting from primary school. |
| Warren Newton | American Board of Family Medicine | Provide a breadth of experiences that cut across class and ethnicity, and allow adequate time for students to truly understand differences among people and cultures. |
| Emilia Iwu | Jonas Nursing Scholar | Use real patients who understand their disease process to provide feedback to prelicensure health professional learners about their ability to communicate effectively. |
REFERENCES
AAMC (Association of American Medical Colleges). 2013. Medical schools take active role in reducing students’ stress and anxiety, edited by R. Greenberg. Washington, DC: AAMC.
Aronson, L. 2015. Necessary steps: How health care fails older patients, and how it can be done better. Health Affairs (Millwood) 34(3):528-532.
Ball, S., and A. Bax. 2002. Self-care in medical education: Effectiveness of health-habits interventions for first-year medical students. Academic Medicine 77(9):911-917.
Boal, A. 1993. Theatre of the oppressed. New York: Theatre Communications Group.
Cabe, J. 2015. The power of health literacy in health professional education. Presented at the IOM workshop: Envisioning the Future of Health Professional Education. Washington, DC, April 23.
Carmona, R. H. 2003. Health literacy in America: The role of health care professionals. http://www.surgeongeneral.gov/news/speeches/ama061403.html (accessed July 14, 2015).
The Centre for Literacy. n.d. Health literacy—Calgary charter. http://www.centreforliteracy.qc.ca/health_literacy/calgary_charter (accessed September 9, 2015).
Coleman, C. 2011. Teaching health care professionals about health literacy: A review of the literature. Nursing Outlook 59(2):70-78.
Coleman, C. 2015. Curriculum transformation: Integrating health literacy teaching in medical education. Presented at the IOM workshop: Envisioning the Future of Health Professional Education. Washington, DC, April 23.
Coleman, C. A., and S. Appy. 2012. Health literacy teaching in U.S. medical schools, 2010. Family Medicine 44(7):504-507.
Coleman, C. A., and A. Fromer. 2015. A health literacy training intervention for physicians and other health professionals. Family Medicine 47(5):388-392.
Coleman, C. A., S. Hudson, and L. L. Maine. 2013. Health literacy practices and educational competencies for health professionals: A consensus study. Journal of Health Communication 18(Suppl. 1):82-102.
Coleman, C. A., S. Peterson-Perry, and T. Bumsted. In press. Long-term effects of a health literacy curriculum for medical students. Family Medicine.
Coleman, C. A., R. Garvin, B. Sachdeva, A. Kobus, and S. Peterson-Perry. n.d.-a. Health literacy training for family medicine residents: Effects of a longitudinal curriculum.
Coleman, C. A., N. T. Nguyen, R. Garvin, C. Sou, and P. A. Carney. n.d.-b. Health literacy teaching in U.S. family medicine residency programs: A national survey.
CRI (Canyon Ranch Institute). 2011. Health literacy. http://www.canyonranchinstitute.org/about-cri/focus-areas/health-literacy (accessed July 7, 2015).
Dyrbye, L. N., M. R. Thomas, J. L. Huntington, K. L. Lawson, P. J. Novotny, J. A. Sloan, and T. D. Shanafelt. 2006. Personal life events and medical student burnout: A multicenter study. Academic Medicine 81(4):374-384.
Eckleberry-Hunt, J., and J. Tucciarone. 2011. The challenges and opportunities of teaching “Generation Y.” Journal of Graduate Medical Education 3(4):458-461.
Gerteis, J., D. Izrael, D. Deitz, L. LeRoy, R. Ricciardi, T. Miller, and J. Basu. 2014. Multiple chronic conditions chartbook. AHRQ publications No. Q14-0038. Rockville, MD: AHRQ.
Grubbs, V., S. E. Gregorich, E. J. Perez-Stable, and C. Y. Hsu. 2009. Health literacy and access to kidney transplantation. Clinical Journal of the American Society of Nephrologists 4(1):195-200.
HLS-EU (European Health Literacy Survey) Consortium. 2012. Comparative report on health literacy in eight EU member states. The European health literacy Survey HLS-EU. http://www.health-literacy.eu (accessed August 28, 2015).
Horton, G. E., N. Diaz, and D. Green. 2009. Mental health characteristics of social work students: Implications for social work education. Social Work in Mental Health 7(5): 458-475.
IOM (Institute of Medicine). 2004. Health literacy: A prescription to end confusion. Washington, DC: The National Academies Press.
IOM. 2013. Health literacy: Improving health, health systems, and health policy around the world: Workshop summary. Washington, DC: The National Academies Press.
Knecht, M. K., G. F. Bauer, F. Gutzwiller, and O. Hämmig. 2011. Persistent work-life conflict and health satisfaction: A representative longitudinal study in Switzerland. BMC Public Health 11:271.
Kutner, M., E. Greenber, Y. Jin, and C. Paulsen. 2006. The health literacy of America’s adults: Results from the 2003 National Assessment of Adult Literacy (NCES 2006-483). Washington, DC: U.S. Department of Education.
Lunau, T., C. Bambra, T. A. Eikemo, K. A. van der Wel, and N. Dragano. 2014. A balancing act? Work-life balance, health and well-being in European welfare states. European Journal of Public Health 24(3):422-427.
Mackert, M., J. Ball, and N. Lopez. 2011. Health literacy awareness training for healthcare workers: Improving knowledge and intentions to use clear communication techniques. Patient Education and Counseling 85(3):e225-e228.
Msemo, G., A. Massawe, D. Mmbando, N. Rusibamayila, K. Manji, H. L. Kidanto, D. Mwizamuholya, P. Ringia, H. L. Ersdal, and J. Perlman. 2013. Newborn mortality and fresh stillbirth rates in Tanzania after Helping Babies Breathe training. Pediatrics 131(2):e353-e360.
Pleasant, A., A. de Quadros, M. Pereira-León, and J. Cabe. 2014. A qualitative first look at the arts for behavior change program: Theater for health. Arts & Health 7(1):54-64.
Pryjmachuk, S. 2004. Sources of stress, stress and coping in a population of pre-registration nursing and midwifery students (Research Completed). Duration of Project: 1999-2003. Principle Investigator: Steven Pryjmachuk. Manchester, UK: University of Manchester School of Nursing, Midwifery, and Social Work.
Rao, T. S. S., and V. Indla. 2010. Work, family or personal life: Why not all three? Indian Journal of Psychiatry 52(4):295-297.
Saravanan, C., and R. Wilks. 2014. Medical students’ experience of and reaction to stress: The role of depression and anxiety. Scientific World Journal. Article ID 737382.
Sharif, F., and S. Masoumi. 2005. A qualitative study of nursing student experiences of clinical practice. BMC Nursing 4(6):1-7.
Sullivan, J., S. Petronella, E. Brooks, M. Murillo, L. Primeau, and J. Ward. 2008. Theatre of the oppressed and environmental justice communities: A transformational therapy for the body politic. Journal of Health Psychology 13(2):166-179.
Vos, T., et al. 2012. Years lived with disability (YLDS) for 1160 sequelae of 289 diseases and injuries 1990-2010: A systematic analysis for the global burden of disease study 2010. Lancet 380(9859):2163-2196.
Zarcadoolas, C., A. F. Pleasant, and D. S. Greer. 2006. Advancing health literacy: A framework for understanding and action. San Francisco, CA: Jossey-Bass.


























