
1
Introduction
Human beings encounter microorganisms every day. In modern societies, most of these interactions occur inside the buildings where humans live and work. Data collected by the National Human Activity Pattern Survey (NHAPS), for example, revealed that Americans spent an average of nearly 69 percent of a 24-hour day in a residence, 5.4 percent in an office or factory, and nearly 13 percent in other indoor locations (Klepeis et al., 2001). Patterns were similar for Americans and Canadians, and the study found that spending significant time indoors had remained the case across several decades. Despite the age of the NHAPS data, it is unlikely that people are now spending less time inside. Thus, improving understanding of what humans encounter in their indoor environments, how these exposures affect them, and how their environments can be modified to affect these exposures has the potential to contribute to future health and well-being.
The microbial communities that surround humans are diverse and dynamic—consisting of ever-changing combinations of bacteria, viruses, and microbial eukaryotes (microorganisms whose cells have nuclei, such as fungi). They include microbes that may be actively persisting or proliferating; those that are inactive, dormant, or dying; and microbial molecules.1
___________________
1 This Consensus Study Report considers built environment microbiomes as including a variety of microorganisms, including bacteria, viruses, and microbial eukaryotes (such as fungi, microscopic algae, and protozoa), and encompassing not only intact microorganisms but also microbial components and chemical products of microbial metabolism (such as mycotoxins and volatile organic compounds). The relevant microbial communities are found not only in the occupied spaces of built environments but also in indoor infrastructure, such as premise plumbing and ventilation ductwork, as well as in “unconditioned” indoor spaces, such as crawl spaces.
Microorganisms that live and die in built environments can have effects on human occupants. Prior to the advent of genomics and other molecular tools, studies of indoor microorganisms relied primarily on culture and microscopy to explore these microbial communities. Recent studies have taken advantage of the development of novel tools to quantify and sequence the DNA of communities of microbes and study their functions, revealing their abundance and complexity and leaving still more questions than answers about what these communities are doing and what functions they serve in people’s indoor environments. Despite the wealth of research thus far, then, much remains unknown about the direct and indirect connections between humans and microorganisms in their built environments.
STUDY CHARGE
As more knowledge emerges about the communities of indoor microbes, the question arises as to whether this knowledge might be used to inform building design and operation to create and maintain more healthful indoor environments. This Consensus Study Report addresses this complex question. Because far more currently is unknown than known, the report does not provide a simple answer to this question. In accordance with the committee’s statement of task (see Box 1-1), the report (1) summarizes the state of knowledge on microbiomes of the built environment and their relationships to human health, as well as their other potential impacts; (2) identifies knowledge gaps; and (3) outlines a research agenda for filling these gaps and moving the field forward.
STUDY FOCUS AND SCOPE
Microorganisms can impact the built environment and its occupants in a variety of ways. One of the key motivators for studying microbial communities of the built environment is to learn more about how microorganisms and their products affect human health. Such effects may arise from an infection causing a disease, as a result of allergic and other physiologic responses leading to symptoms, or by other means. For example, a number of studies have explored the transmission of pathogens, such as influenza virus or Legionella bacteria in indoor settings, as well as adverse associations among interior dampness, fungi, and respiratory health. Other potential effects are being explored as well, including whether exposure to environmental microorganisms affects the human microbiome. Alongside the consideration of indoor microbes as a potential source of risk, studies have suggested potential benefits from not living in too sterile an environment and from particular types of early-life exposures to microorganisms. The effects of exposures in the built environment likely have personal
dimensions, influenced by such factors as age, genetics, and health status. Similar exposures to similar microorganisms may have beneficial, adverse, or neutral effects in different people, factors that will need to be considered in developing future guidance. In addition to effects on health, microorganisms affect building materials and building systems, including through degradation, corrosion, and fouling as a result of biofilm formation. These effects can have economic and sustainability costs, and the varied effects and trade-offs involved will influence the assessment of potential interventions to modify indoor microbiomes.
Both microbial communities and the built environments they inhabit are highly diverse. Myriad types of buildings and building uses exist in myriad climates, so clearly there is no “typical” building. Moreover, the built environment contains more than buildings. Used broadly, the term encompasses roads and transit systems, transportation vehicles such as ships
and airplanes, space vehicles and space stations, manufacturing facilities, water supply systems and sources, wastewater treatment plants, and other components of the urban environments in which a majority of people in developed countries live.
This report does not address all of these built environments; it focuses primarily on single-family residential buildings (homes) and multioccupancy commercial and mixed-use buildings, including apartments, offices, and schools. These spaces represent environments in which humans spend large amounts of time. The report does not delve in detail into farm environments, factories, gathering spaces such as retail malls or amphitheaters, or transit systems, although it draws several comparisons with studies conducted in specialized living and working environments, such as hospitals and the International Space Station. The report also focuses on built environments found in temperate regions of the world and does not draw detailed comparisons among microbiomes and their impacts in nations with more widely varying climates and levels of economic development.
Even with these constraints, the building types considered in the report vary significantly in design, construction, operation, and occupant population. Residential buildings generally are designed so that occupants have control over environmental conditions such as temperature, humidity, and connection to the outdoor environment via operable doors and windows. However, the level of engagement of occupants in exercising such controls varies widely, with some being actively engaged in operating and maintaining the various building systems and others dealing with these systems only when the systems have become nonfunctional. The occupants of residential buildings generally are stable over time, and even transitory occupants tend to be related biologically to primary occupants. Occupants may span a range of ages, physical conditions, and overall health status, and occupant densities and occupancy characteristics can change over time. As the field moves closer to practice and to developing guidance on how indoor microorganisms affect health and how building factors affect these indoor microbiomes, it will also be important to consider challenges facing residents living in poor housing stock and of lower socioeconomic status, who may have less control over environmental conditions, may not be able to improve their residences, or may need information and resources to address indoor microbiome–built environment issues.
Commercial buildings, on the other hand, are necessarily transitory spaces. Most office buildings accept visitors every day, and the occupants are normally not related to one another. Commercial buildings generally are managed more intentionally relative to residences, typically with dedicated staff who operate and maintain the various building systems. Occupants usually have little to no control over their indoor environment. Even when individual occupants can control the temperature and lighting of their
indoor environment or have operable windows, they still are subject to central management of many other aspects of that environment, and public spaces (e.g., lobbies and meeting rooms) are much less likely to allow for occupant control. Occupants in commercial buildings are also subject to the actions of other occupants and, as a result, may be exposed to temperatures, lighting, noise, cleaning products, or other conditions they would not necessarily choose for themselves.
EMERGING TOOLS THAT FACILITATE ANALYSIS
Although the percentage of microorganisms that can be cultured from an environmental sample varies, estimates as low as 1 percent have been reported (Amann et al., 1995; Kallmeyer et al., 2012; Quince et al., 2008). Thus, a reliance on culture-based surveys significantly limits understanding of microbial populations, including those present in buildings. New approaches for analyzing genetic material in environmental samples have revolutionized microbiology, and the tools available for detecting microbial DNA and RNA, along with associated bioinformatics approaches for connecting those sequences to microbial identification, have improved over the past decade. Simultaneously, databases containing reference microbial genomes have grown. Although these genomics technologies have brought new understanding of the composition and diversity of microbial communities in buildings, they also have limitations—for example, sequencing approaches do not distinguish between living and dead microorganisms—and having information on viability thus remains important. Additional high-throughput “omics” approaches with which to study microbial proteins and metabolic products provide valuable information not only on which species are present indoors but also on what these microorganisms are doing. These culture-independent techniques will need to be combined with culture-dependent methods, computer modeling, building characterization tools, and epidemiology to increase knowledge about the environments in which people live and work and how these building and microbial conditions are affecting them.
STUDYING THE INTERSECTION OF MICROBIAL COMMUNITIES, BUILT ENVIRONMENTS, AND HUMAN OCCUPANTS
Microorganisms within buildings are found in air, on surfaces, and in water systems. They are carried on and arise from living creatures that inhabit the environment, including human occupants, pets, plants, and pests, each of which has its own associated microbial communities. A simplified representation of the ecosystem built around these interactions among humans, the indoor environment, and indoor microorganisms is depicted
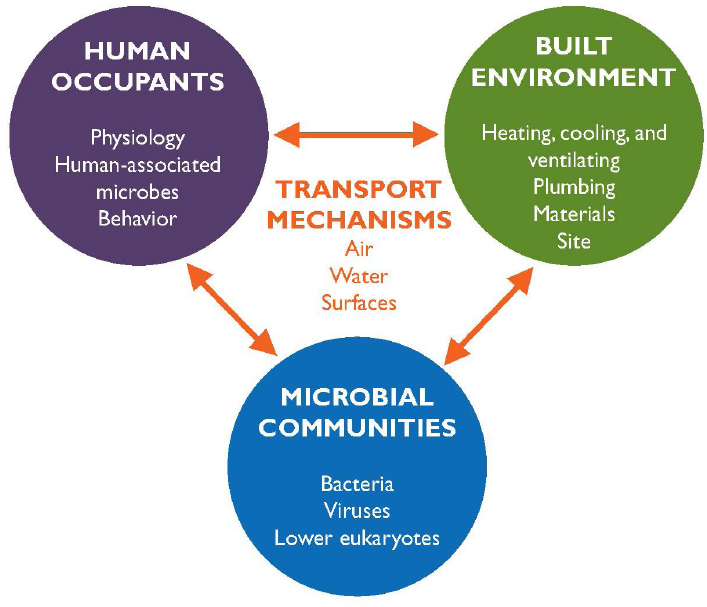
in Figure 1-1. Examples of factors that affect community interactions are included in each circle, and the primary reservoirs of microbes and mechanisms of their transport are shown in the triangle connecting the circles. Not every factor is captured in this representation. For example, indoor building structures other than heating, ventilation, and air conditioning (HVAC) and plumbing systems and the outdoor environment beyond a building site may affect indoor microbiomes, as may building operation and maintenance practices that affect indoor building and building system conditions. The report’s subsequent chapters explore these dimensions and their linkages in greater detail.
Ecosystems can be characterized in a number of ways, and an initial grounding in basic principles of ecological theory can aid in understanding how changes to one component of the system may affect other components. Some simple ecological relationships are briefly introduced below. The report turns to the idea of system models in more detail in Chapter 5, which explores the use of models in addressing specific questions, testing
hypotheses, and assessing the impacts of different types of interventions on built environments, their associated microbiomes, and their human occupants.
The Built Environment as an Ecosystem: Fundamental Ecological Principles
A single building can be thought of as akin to an island that emerges from the ocean. It is a habitat patch that can be colonized by groups of microorganisms, all of which have the potential to proliferate further and interact. The resident community of microbes in a building will be amplified by colonization, modulated by in situ population dynamics, and depleted by extinction or depletion to below detectable levels.2
A mass balance (or material balance) equation is a technical way of describing the flows of a material into and out of a system. By identifying and accounting for what enters and leaves, this approach helps in understanding the properties and functions of a system and has widespread application across science and engineering. This concept is a useful way of describing the abundance (N) of a representative microbial population in an environment. The number of organisms grows through births (B) and immigration (I) into the habitat being studied, and decreases through deaths (D) and emigration (E). Expressing this mathematically, change in the species’ abundance over time (dN/dt) is
![]()
In a real environment, each of the terms of this simple equation encompasses a number of complex relationships—for example, accounting for multiple “immigration” sources of a particular microorganism in the built environment or accounting for multiple types of microorganisms, each with a different abundance. Examples of microbial inflows and outflows in a highly simplified built environment are depicted in Figure 1-2. As this simplified figure shows, microorganisms can enter a built environment from the outside through
- ventilation, such as through open doors and windows or through HVAC systems;
- through building water supply and premise plumbing systems through evaporation or aerosolization;
- infiltration, which includes moisture seepage or air leakage; and
___________________
2 These dynamics generally refer to the processes that affect the composition, persistence, and proliferation of microbial communities.
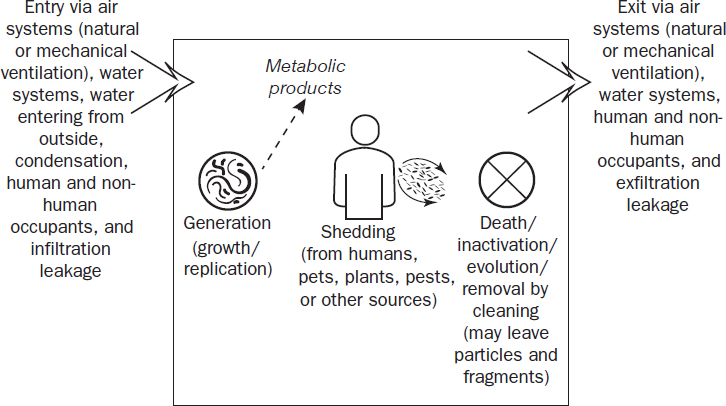
- transport on humans and other occupants, including pets and pests, and the microbes associated with soil and particulate matter these occupants track indoors.
Within the built environment, microorganisms can increase as a result of
- growth and replication if the environment has the right nutrients, water, and conditions for reproduction; and
- shedding from humans and other living occupants, each of which has its own associated microbiomes.
Microorganisms can leave the built environment through
- microbial death, although nonliving and dormant microbes and microbial fragments may remain;
- water via premise plumbing systems;
- air exfiltration and moisture seepage;
- outward transport by natural or mechanical ventilation;
- outward transport on humans and other occupants; and
- removal by cleaning, such as mopping, dusting, and vacuuming.
Permissive and Restrictive Environments
The habitat in an indoor environment also varies in terms of its “quality,” in the sense of how well or poorly it suits an organism’s life cycle. In the built environment, a permissive environment is one that has suitable conditions such that microorganisms can grow or persist. These conditions include such aspects as humidity/moisture, nutrients, temperature, pH, and lack of inhibitory compounds. Conversely, a restrictive environment is one in which suitable conditions are lacking and/or inhibitory substances are present such that microbial growth is limited by these substances and persistence is reduced, although persistence via dormancy may continue.
Making Use of Population Dynamics Equations
Equation 1-1 above, which can be used to assess the abundance of one microbial population, can also be utilized in different scenarios. These scenarios may include, for example, the microorganisms being inactive (in which case birth rate is zero), conditions in which immigration and emigration are equal, or a steady state in which there is no change in a species’ abundance over time. Solving the equation for these and other conditions demonstrates that a relationship will exist between internal abundance (within the built environment) and concentration in the external “source” landscape. This relationship has two implications. First, it is important to note that microbial communities encompass not only viable microbes but also dormant microorganisms, as well as microbial fragments, which may play a role in impacting human health. The density of a microorganism in the built environment habitat will generally be affected by the density of microbes in the source landscape (e.g., in outdoor air), although indoor bacterial concentrations, for instance, can be higher than those outdoors as a result of indoor sources. Second, simple models such as this can also make predictions about transient dynamics and how long a system needs to settle into a new state following a perturbation. Box 1-2 provides additional examples of how mathematical representations help frame questions to enable better understanding of key system parameters and yield implications for studying population interactions in the built environment. Although these concepts may appear to be simplified and abstract, understanding the variables and processes behind how microbial communities develop, grow, and fail can guide models and predictions of how these communities will respond to features within the built environment (e.g., mechanical versus natural ventilation), as well as to perturbations (e.g., the occurrence of
flooding) or interventions (e.g., the inclusion of high-efficiency particulate air [HEPA] filters in a building’s HVAC system).
The ability to apply such ecological analyses and modeling effectively remains preliminary in the indoor environment: many variables are still being characterized, while a number of additional factors (such as exposure to nonviable components and metabolites) may be relevant to understanding microbial impacts. As the field moves forward and research continues to resolve, or at least further clarify, these complexities, this modeling and prediction capability will contribute greatly to moving the field from basic research to application.
PRIOR EFFORTS ON WHICH THIS REPORT BUILDS
Research into the microbial populations associated with different built environments and the health effects of exposure to these microorganisms extends back for decades. In the public health community, many investigations have focused on how pathogens infect occupants within a building. Since the early 20th century, for example, research has explored the release of droplets into air through coughing and sneezing and the contributions of these aerosol and contact factors to the development of colds and flu (Dick et al., 1987; Lindsley et al., 2010; Marr, 2016; Stephens, 2016; Wells et al., 1939). Similarly, the proliferation and transmission of waterborne pathogens through municipal water systems and indoor plumbing have been studied for many years, drawing attention to the effects of such conditions as pipe degradation and water stagnation times in storage facilities and premise piping (NRC, 2006; Rhoads et al., 2015, 2016). For example, Legionella can colonize as biofilms in showers and be expelled in aerosols (Schoen and Ashbolt, 2011), and mycobacterium avium complex and Pseudomonas may colonize and persist in a similar manner (Falkinham et al., 2015). The recent water crisis in Flint, Michigan, provides one illustration of the importance of water quality, in this case impacting a subsequent outbreak of Legionnaires’ disease (Schwake et al., 2016).
The positive and negative health consequences associated with the built environment also have been studied in the context of the relationship between indoor air quality and asthma. A report of the National Academies of Sciences, Engineering, and Medicine states that “major sources of indoor allergens in the United States are house dust mites, fungi and other microorganisms, domestic pets (cats and dogs), and cockroaches” (IOM, 1993, p. 2) that can be found in the buildings in which humans now spend more than 90 percent of their time (Klepeis et al., 2001). Increases in and exacerbation of asthma and allergies have been correlated with exposures to specific sources of indoor allergens (IOM, 1993, 2000). A 2004 Institute of Medicine report also “found evidence of an association between expo-
sure to damp indoor environments and some respiratory health outcomes” (IOM, 2004, p. 10) (see also Mendell et al., 2011; WHO, 2009).
Other studies have addressed less-defined impacts of building conditions on human occupants. In the 1970s, for example, a number of environmental health investigations were prompted by symptoms associated with “sick building syndrome,” in which people reported headaches, mucous-membrane irritation, and difficulty concentrating linked to arriving at and departing from a particular building without a clearly identified exposure or cause (Cox-Ganser et al., 2010, 2011; Hinkle and Murray, 1981; Hodgson and Kreiss, 1986; Kreiss, 1989; Levin, 1989; Melius et al., 1984; NRC, 1981; WHO, 1983). Around the same time, environmental awareness and concerns about energy efficiency led to changes in ventilation in public buildings, which in some cases included inoperable windows or HVAC systems that were undersized for the spaces they served or that operated contrary to their design intent. These changes sometimes resulted in decreased outdoor air ventilation rates and, at other times, in increased indoor dampness. The relative contributions of indoor microbes, their components, or their metabolic products to the development of symptoms of sick building syndrome are not well understood. Nevertheless, research into these symptoms has helped focus some members of the design, engineering, and construction fields on ways to promote occupant comfort and health.
The air quality of specialized environments, such as airplanes, also has received scrutiny, with one report recommending an increase in the number of cabin air changes per hour to “meet general comfort conditions, and dilute or otherwise reduce normally occurring odors, heat, and contaminants” (NRC, 2002, p. 4). In some circumstances, greater ventilation leads to more desirable outcomes. Similarly, studies on human exposure to particulate matter (PM) have noted that “levels of indoor PM have the potential to exceed outdoor PM levels,” thus making indoor environments as critical to health as outdoor air, despite the fact that “the majority of studies have focused on outdoor PM levels and their impacts” (NASEM, 2016, p. 2). Concern about the health effects of indoor PM and lack of clarity regarding its components have led to renewed interest in understanding these indoor and outdoor sources, including microbial components. While increased ventilation with filtration of outdoor air can reduce the concentration of indoor PM (although not necessarily of gaseous pollutants), potential trade-offs, which could include economic and energy impacts, have yet to be fully studied.
In-depth studies to explore the connections among microbial communities, different environmental conditions in built environments, and such outcomes as health or illness need to integrate expertise from microbial ecology, building and building system design and operation, epidemiology and human health, materials science, and a number of other fields. During
the past decade, the Alfred P. Sloan Foundation Microbiomes of the Built Environment (MoBE) program has catalyzed a number of complementary research collaborations at the intersection of microbial ecology and building science3 to begin to tackle these challenges, foster greater cross-disciplinary collaboration, and bring attention to the idea of studying built environments as one would other types of ecosystems. The present report builds on the results of a number of studies supported by foundations, agencies, and societies, including the Sloan program, EPA, NIH, NSF, NASA, the American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE), and others.
ORGANIZATION OF THE REPORT
The subsequent chapters of this report explore aspects of the dynamic interacting systems connecting humans, built environments, and environmental microbial communities.
A critical driver for better understanding these relationships will be the eventual ability to apply insights from microbiome research to the design and operation of buildings for human health and well-being. Chapter 2 emphasizes the human dimension of microbiome–built environment studies. The chapter reviews what is known about how indoor microbial exposures are associated with potential health outcomes and identifies knowledge gaps that need to be filled to advance the field.
Chapter 3 focuses on major components of buildings and reviews the state of knowledge on how buildings and building systems contain, enhance, or diminish microbial communities. It explores the transport of microorganisms into and within buildings associated with air, water, and surfaces and the influence of such factors as occupants and climate, and it concludes by identifying knowledge gaps in these areas.
Chapter 4 reviews tools and methods for studying the nexus of buildings, microbial communities, and human occupants, including tools with which to sample and characterize built environments and the microbial communities within them and approaches for studying health effects. It identifies needs to improve these tools and support further research in the field.
Chapter 5 examines opportunities and challenges for managing the microbiomes of built environments. It considers examples of interventions that could alter building microbiomes and approaches for assessing their potential benefits and trade-offs.
___________________
3 The report uses the term “building science” to refer to the field of knowledge that focuses on understanding physical and operational aspects of buildings and building systems and the impacts on performance; the term “building scientist” is used to refer to a broad range of integrated technical disciplines, including scientists, engineers, and architects who study this area.
Finally, Chapter 6 lays out a vision for the future of buildings as informed by microbial understanding. It provides a research agenda to fill the knowledge gaps identified in the prior report chapters and to make progress toward achieving this vision.
REFERENCES
Amann, R. I., W. Ludwig, and K. H. Schleifer. 1995. Phylogenetic identification and in situ detection of individual microbial cells without cultivation. Microbiological Reviews 59(1):143-169.
Cox-Ganser, J. M., J. H. Park, and K. Kreiss. 2010. Office workers and teachers. In Occupational and environmental lung diseases (Ch. 23), edited by P. Cullinan, S. M. Tarlo, and B. Nemery. Chichester, UK: John Wiley & Sons, Ltd.
Cox-Ganser, J. M., J. H. Park, and R. Kanwal. 2011. Epidemiology and health effects in moisture-damaged damp buildings. In Sick building syndrome and related illness: Prevention and remediation of mold contamination, edited by W. Goldstein. Boca Raton, FL: CRC Press, Taylor & Francis Group. Pp. 11-22.
Dick, E. C., L. C. Jennings, K. A. Mink, C. D. Wartgow, and S. L. Inhorn. 1987. Aerosol transmission of rhinovirus colds. The Journal of Infectious Diseases 156(3):442-448.
Falkinham, J. O., A. Pruden, and M. Edwards. 2015. Opportunistic premise plumbing pathogens: Increasingly important pathogens in drinking water. Pathogens 4(2):373-386.
Gonzalez, A., and R. D. Holt. 2002. The inflationary effects of environmental fluctuations in source–sink systems. Proceedings of the National Academy of Sciences of the United States of America 99(23):14872-14877.
Hinkle, L. E., and S. H. Murray. 1981. The importance of the quality of indoor air. Bulletin of the New York Academy of Medicine 57(10):827-844.
Hodgson, M. J., and K. Kreiss. 1986. Building associated diseases: An update. In Proceedings of IAQ ’86: Managing Indoor Air for Health and Energy Conservation, edited by J. E. Janssen. Atlanta, GA: American Society of Heating, Refrigerating and Air-Conditioning Engineers. Pp. 1-15.
Holt, R. D., M. Barfield, and A. Gonzalez. 2003. Impacts of environmental variability in open populations and communities: “Inflation” in sink environments. Theoretical Population Biology 64(3):315-330.
IOM (Institute of Medicine). 1993. Indoor allergens: Assessing and controlling adverse health effects. Washington, DC: National Academy Press.
IOM. 2000. Clearing the air: Asthma and indoor air exposures. Washington, DC: National Academy Press.
IOM. 2004. Damp indoor spaces and health. Washington, DC: The National Academies Press.
Kallmeyer, J., R. Pockalny, R. R. Adhikari, D. C. Smith, and S. D’Hondt. 2012. Global distribution of microbial abundance and biomass in subseafloor sediment. Proceedings of the National Academy of Sciences of the United States of America 109(40):16213-16216.
Klepeis, N. E., W. C. Nelson, W. R. Ott, J. P. Robinson, A. M. Tsang, P. Switzer, J. V. Behar, S. C. Hern, and W. H. Engelmann. 2001. The National Human Activity Pattern Survey (NHAPS): A resource for assessing exposure to environmental pollutants. Journal of Exposure Analysis and Environmental Epidemiology 11(3):231-252.
Kreiss, K. 1989. The epidemiology of building-related complaints and illness. Occupational Medicine 4(4):575-592.
Levin, H. 1989. Building epidemiology and investigations—approaches and results (U.S. experience). In Chemical, microbiological, health and comfort aspect of indoor air quality—state of the art in SBS, edited by H. Knöppel and P. Wolkoff. Boston, MA: Kluwer Academic Publishers.
Lindsley, W. G., F. M. Blachere, R. E. Thewlis, A. Vishnu, K. A. Davis, G. Cao, J. E. Palmer, K. E. Clark, M. A. Fisher, R. Khakoo, and D. H. Beezhold. 2010. Measurements of airborne influenza virus in aerosol particles from human coughs. PLOS ONE 5(11):e15100.
Marr, L. 2016. Viruses in the built environment. Presentation to the Committee on Microbiomes of the Built Environment: From Research to Application, October 18, 2017.
Melius, J., K. Wallingford, R. Keenlyside, and J. Carpenter. 1984. Indoor air quality—the NIOSH experience. Annals of the American Conference of Governmental Industrial Hygienists 10:3-7.
Mendell, M. J., A. G. Mirer, K. Cheung, M. Tong, and J. Douwes. 2011. Respiratory and allergic health effects of dampness, mold, and dampness-related agents: A review of the epidemiologic evidence. Environmental Health Perspectives 119(6):748-756.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Health risks of indoor exposure to particulate matter: Workshop summary. Washington, DC: The National Academies Press.
NRC (National Research Council). 1981. Indoor pollutants. Washington, DC: National Academy Press.
NRC. 2002. The airliner cabin environment and the health of passengers and crew. Washington, DC: National Academy Press.
NRC. 2006. Drinking water distribution systems: Assessing and reducing risks. Washington, DC: The National Academies Press.
Quince, C., T. P. Curtis, and W. T. Sloan. 2008. The rational exploration of microbial diversity. The ISME Journal 2(10):997-1006.
Rhoads, W. J., P. Ji, A. Pruden, and M. A. Edwards. 2015. Water heater temperature set point and water use patterns influence Legionella pneumophila and associated microorganisms at the tap. Microbiome 3(1):1-13.
Rhoads, W. J., A. Pruden, and M. A. Edwards. 2016. Convective mixing in distal pipes exacerbates Legionella pneumophila growth in hot water plumbing. Pathogens 5(1):E29.
Schoen, M. E., and N. J. Ashbolt. 2011. An in-premise model for Legionella exposure during showering events. Water Research 45(18):5826-5836.
Schwake, D. O., E. Garner, O. R. Strom, A. Pruden, and M. A. Edwards. 2016. Legionella DNA markers in tap water coincident with a spike in Legionnaires’ disease in Flint, MI. Environmental Science & Technology Letters 3(9):311-315.
Stephens, B. 2016. What have we learned about the microbiomes of indoor environments? mSystems 1(4):e00083-e00116.
Wells, W. F., M. W. Wells, and S. Mudd. 1939. Infection of air: Bacteriologic and epidemiologic factors. American Journal of Public Health and the Nations Health 29(8):863-880.
WHO (World Health Organization). 1983. Indoor air pollutants: Exposure and health effects. EURO Reports and Studies No. 78. Geneva, Switzerland: WHO.
WHO. 2009. WHO guidelines for indoor air quality: Dampness and mold. http://www.euro.who.int/__data/assets/pdf_file/0017/43325/E92645.pdf (accessed April 27, 2017).
















