1
Introduction1
The topic of the resources that are needed to improve health and address the factors that shape health has been a focus of the National Academies of Sciences, Engineering, and Medicine’s Roundtable on Population Health Improvement since its launch. This topic was first addressed in a 2014 workshop that discussed financial mechanisms such as pay-for-success financing and hospital and health system community benefit funding (IOM, 2015). To continue its exploration of the topic of resources, but with a focus on non–health sector models, the roundtable hosted a workshop on October 19, 2016, to explore sustainable financing structures that reflect a recognition of the health and non-health factors that shape the well-being of U.S. communities. The goals of the workshop were to learn from the long-term, sustainable financing strategies used in other sectors, to explore how those approaches could be applied to population health, and to consider structures that work across sectors (e.g., examples where capital flows across sectors).
The uneven distribution of health in the United States has been the result of multiple forces—from a wide variety of sectors—that shape the life experiences of individuals, explained workshop planning committee
___________________
1 The planning committee’s role was limited to planning the workshop, and the Proceedings of a Workshop was prepared by the workshop rapporteur as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants, and are not necessarily endorsed or verified by the National Academies of Sciences, Engineering, and Medicine, and they should not be construed as reflecting any group consensus.
chair Pamela Russo, a senior program officer at the Robert Wood Johnson Foundation. Although health care is a critical factor in health, it is also true that various social, economic, and physical exposures influence who gets sick and who stays healthy, as well as whose lives end prematurely versus whose lives are long and active. Furthermore, there are systematic inequities that affect the health of individuals. However, one will not find alleviating poverty, changing school climates to increase the success of children who have been exposed to multiple adverse events or traumas in their lives, or increasing social cohesion listed as line items on a health sector budget. Establishing long-term, dependable, and adequate funding streams for creating safe, healthy, and equitable conditions in communities has not been a priority for most policy makers, Russo said. Appropriations from federal and state agencies or grants from foundations can catalyze change, but they rarely provide funding for the long term or at scale, which reduces their ability to have a major impact on population health. Thus, the focus of this workshop, Russo said, is to look to other sectors to learn how they have achieved long-term, sustainable funding flows for their agendas.
WORKSHOP OBJECTIVES
As one of its major activities, the Roundtable on Population Health Improvement sponsors workshops for its members, stakeholders, and the public to discuss issues of importance for improving our nation’s health, said George Isham, a senior advisor at HealthPartners, a senior fellow at the HealthPartners Institute for Education and Research, and the co-chair of the Roundtable on Population Health Improvement. The roundtable’s vision is of a strong, healthful, and productive society that cultivates human capital and equal opportunity. This vision rests on the recognition that outcomes such as improved life expectancy, quality of life, and health for all are shaped by interdependent social, economic, environmental, genetic, behavioral, and health care factors and that achieving these outcomes will require robust national and community-based policies and dependable resources. The roundtable has identified six areas in which actions can be taken toward achieving this vision: building dependable relationships; developing effective policies; metrics and measurement; effective communication; research to understand relationships and potential interventions; and resources. The concept of dependable resources lies at the core of this workshop, Isham said.
The agenda for this workshop was developed by an independent planning committee chaired by Russo, which included Carter Blakey, Alex Blandford, Denise Fairchild, Gary Gunderson, Jim Knickman, Bobby Milstein, and Christopher Parker. The Statement of Task given to the
planning committee is provided in Box 1-1. In the context of multi-sector collaboration, with a focus on dependable (not one-time) resources, and with the aim of improving health, wealth, well-being, and health equity, the workshop agenda was developed by the planning committee with the following objectives to:
- Improve the fiscal fluency of decision makers and the public to move toward common purpose at community scale and explore frameworks for funding reinvestment and reallocation.
- Identify existing opportunities and constraints on realigning funding in ways that are conducive to co-benefits (for all sectors involved).
- Discuss the strategies, including the conditions, needed to realign resources (i.e., what it takes to move funding from one arena to another).
- Explore what decision makers, communities, and other stakeholders need in order to speak about realignment with confidence, including the possible opportunities to move funds from one part of the system to another.
In accordance with the policies of the National Academies, the workshop did not attempt to establish any conclusions or recommendations about needs and future directions, but instead focused solely on issues identified by the speakers, discussants, and workshop participants. The planning committee’s role was limited to planning the workshop.
ORGANIZATION OF THE WORKSHOP
This Proceedings of a Workshop summarizes the presentations and discussions that took place at the workshop Building Sustainable Finance Structures for Population Health. In the first session of the workshop, participants considered a historical analysis of four case studies demonstrating how cross-sector policy and financing were applied to address major social determinants of health inequity (see Chapter 2). The next two sessions reviewed current case examples from two non-health sectors, justice and energy. Justice reinvestment (see Chapter 3) uses innovative and preventive methods to reduce detention and incarceration and reinvests the resulting savings in further prevention at the federal, state, and local levels, in both adult and juvenile justice. Clean energy financing (see Chapter 4) interrupts the cycle that drives people out of affordable housing as their energy costs increase, providing multiple savings and co-benefits at the federal, state, and local levels. In describing all of the case examples, speakers discussed strategies to align and accelerate funding streams, the modification of current funding structures, and opportunities and constraints encountered in creating a sustainable, reliable flow of funds. Following the plenary discussions of the case studies, participants broke into three small groups to further consider different types of funding mechanisms and their potential application to population health improvement. Attendees then reconvened in plenary session and group facilitators reported on their groups’ discussions (see Chapter 5). In the final session, roundtable members and participants reflected on the presentations and identified key takeaway messages (see Chapter 6).
Audience Participation Activity
The planning committee intended that this workshop be highly interactive, Russo said. As preparation for the forthcoming discussions, an audience participation activity was conducted by Christopher Parker, an associate project director at the Georgia Health Policy Center and a co–principal investigator of Bridging for Health, an initiative sponsored by the Robert Wood Johnson Foundation. Bridging for Health, Parker said, seeks to both identify and to catalyze local multi-sectoral collaborations that are using innovative financing mechanisms that could support population health and health equity.
As an opening exercise, prior to the first session, Parker encouraged participants to affirm the individuals at their table by saying something positive. He encouraged participants to continue to “give each other voice” and ensure that all present had the opportunity to contribute throughout the workshop.
Next, using Poll Everywhere (PollEv.com) to engage both in-person
and webcast attendees, Parker asked three questions and shared the responses in real time. The first poll question prompted participants to enter a word or phrase that best described the state of financing for population health. The theme across the responses, Parker said, was that the state of financing for population health is fragmented, dysfunctional, and generally not what it needs to be, but that there is significant potential for change. The response words and phrases included “fragmented,” “dysfunctional,” “rare,” “lacking,” “constrained,” “stingy,” “uncoordinated,” “nonexistent,” “missing,” “inadequate,” “woefully inadequate,” “not aligned with expectations,” “tricky,” “lopsided,” “in the shadow of the health care financing,” “grant dependent,” “limited,” “seeking direction,” “lacking data,” “not connected enough to innovation,” “new horizon,” “emergent,” “poised to unlock great value,” “potential,” “exciting opportunities for change,” and “full of possibility and potential.”
Parker also asked participants to say what they thought could spark the greatest improvements in financing population health at scale and to describe the extent to which they feel they have enough fiscal fluency to be a champion for population health at scale (see Figures 1-1 and 1-2). Parker then charged participants to listen to the presentations and discussions in a way that increased their own understanding and broadened their own scope and to be actively engaged in the workshop conversations that will help to broaden the scope of others.
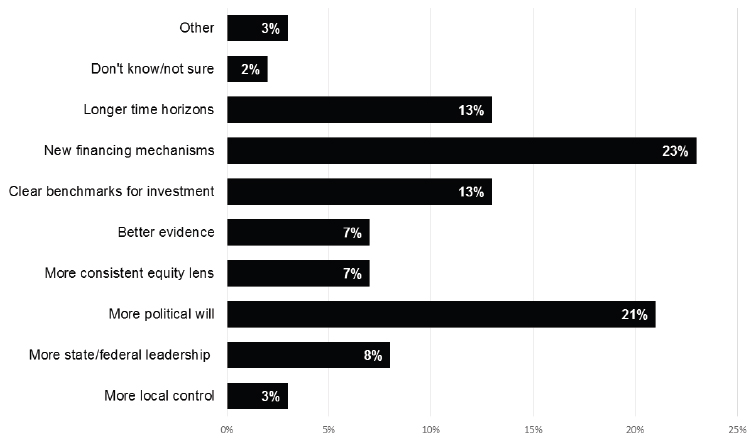
SOURCES: Parker presentation, October 19, 2016 (generated by audience input on PollEverywhere, with poll questions developed by Bobby Milstein and Christopher Parker).
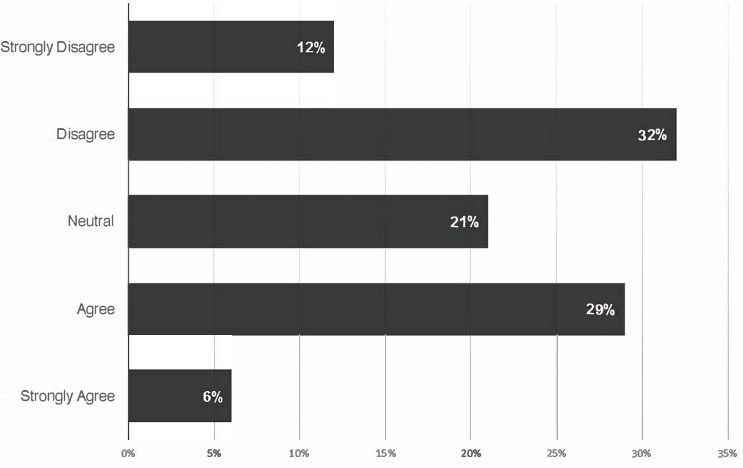
SOURCES: Parker presentation, October 19, 2016 (generated by audience input on PollEverywhere with poll questions developed by Bobby Milstein and Christopher Parker).






