3
Cross-Sector Collaboration
Research has shown that the foundations of health are built in the earliest years, said session moderator Debbie Chang of Nemours. Young children are particularly sensitive to the social determinants of health. Those social determinants exist in multiple sectors, including housing, early care and education, school-age education, business, and health care, among others. In this session, the panelists discussed collaboration among the various sectors at the intersection of early care and education and health. George Askew, the deputy commissioner of the Division of Family and Child Health in the New York City Department of Health and Mental Hygiene (DOHMH), provided examples of cross-sector initiatives concerning early care and education and health across the agency. Kimberly Shinn-Brown, the program director of the Ozarks Area Community Action Corporation (OACAC) Head Start program in Springfield, Missouri, shared examples of how Head Start can improve population health and health equity for children. Krista Scott, the senior director of Health Policy at Child Care Aware, described how state child care agencies are working to make care settings healthier through professional development, settings standards, and investing in quality. Michelle Suarez, an early childhood developer with Prosper Lincoln at Nebraska Children and Families Foundation, described the development of a cross-sector community agenda to improve the health and prosperity of Lincoln, targeting early childhood for health, wellness, and prevention interventions.
Following the presentations and discussion, participants moved to the adjacent gallery to reflect on the panel discussion with other attendees
and to consider specific questions that were posed on posters around the gallery. Upon reconvening in plenary session, Larry Pasti of the Forum for Youth Investing and a senior director at Big Picture Approach Consulting moderated a discussion of individual participants’ responses to the questions. (Session highlights are presented in Box 3-1.)
NEW YORK CITY DEPARTMENT OF HEALTH AND MENTAL HYGIENE1
The New York City DOHMH serves a diverse population of about 8.5 million people, Askew said. For perspective, he noted that the second most populous city in the United States is Los Angeles, with 3.9 million residents, and if New York City were a state, it would be the 12th-largest state in the country.
Division of Family and Child Health
Upon joining the DOHMH in 2014, Askew said, he set out to bring together under one umbrella all of the pieces of the health department that were engaged with children or families. The Division of Family and Child Health was established to improve the health of children, women, and families in New York City, with an emphasis on reducing health disparities and advancing equity. The division’s goal is that all of the children, women, and families in New York City recognize their power and are given the opportunity to reach their full health and development potential. The Division of Family and Child Health portfolio includes
- Bureau of Maternal, Infant, and Reproductive Health, overseeing around 120,000 births in New York City every year;
- Bureau of Early Intervention, which spends about $500 million per year on early intervention services and serves about 30,000 to 40,000 children in New York City;
- Office of School Health, which serves about 1.2 million school-age children; and
- Early Childhood Health and Development Unit, which is working to change the culture and the way in which the health department understands, supports, and nurtures babies, infants, and toddlers in New York City.
___________________
1 This section is the rapporteur’s synopsis of the presentation by George Askew, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
Cross-Division Collaboration on Social-Emotional Learning
The Division of Family and Child Health and the Division of Mental Hygiene, both within the DOHMH, are involved in a cross-sector collaboration to integrate mental health consulting on social-emotional learning (SEL) into early care and education classroom sites throughout the city.
Social-emotional development, Askew explained, involves developing the capacity of the child (birth to 5 years of age) to form close and secure adult and peer relationships; to experience, manage, and express a full range of emotions; to explore the environment; and to learn, all in
the context of family, community, and culture. SEL is the process through which children and adults acquire the knowledge and skills to recognize and manage emotions, show caring and concern for others, establish positive relationships, make responsible decisions, and handle challenging situations constructively. (He noted that these definitions were adapted from materials developed by Zero to Three.)
The SEL initiative is part of ThriveNYC, which was launched by the First Lady of New York City, Chirlane McCray, as a comprehensive plan to approach mental health and substance misuse in the city.2 ThriveNYC uses a public health approach to change the way people think about mental health and also the way that the city government and its many partners provide care. The SEL project, Askew said, is based on the “Act early” guiding principle of ThriveNYC, which is to give New Yorkers more tools to weather challenges and to capitalize on opportunities by investing in prevention and early intervention. As a component of ThriveNYC, the SEL project is a cross-system collaboration among the Department of Education (DOE, which oversees the universal pre-K program); the Administration for Children’s Services (the city’s child welfare system, which handles EarlyLearn, an early childhood/early care and education system that includes the Head Start program); and the DOHMH.
Originally, SEL focused on mental health treatment and referrals, Askew said, but it later changed into a provider of mental health consulting services. This focus on consulting enables the program to build capacity in adults working with children and also to build supports focused on prevention (rather than treatment). This focus changed as a result of the community response—specifically, when it was found that mental health consultation was in higher demand than treatment. The program continues to learn from the needs and responsiveness of the children, and more children will now be served in their early care and education classrooms, where mental health supports are less threatening and more accessible, given the life situations of many of the targeted families. Most of the 30 mental health consultants hold master’s degrees in social work or a mental health–related degree (e.g., art therapy). Askew said that this program represents about 50 percent of their workload, with the other 50 percent related to treatment.
The framework for the public health approach to early childhood mental health was adapted from the Georgetown University Framework for Early Childhood Mental Health Consultation, Askew said. The New York City model is intended to build capacity (see Figure 3-1), and the first step is to build supportive environments as well as nurturing and
___________________
2 For a brief overview of ThriveNYC, see https://www1.nyc.gov/assets/operations/downloads/pdf/pmmr2017/thrivenyc.pdf (accessed October 30, 2017).
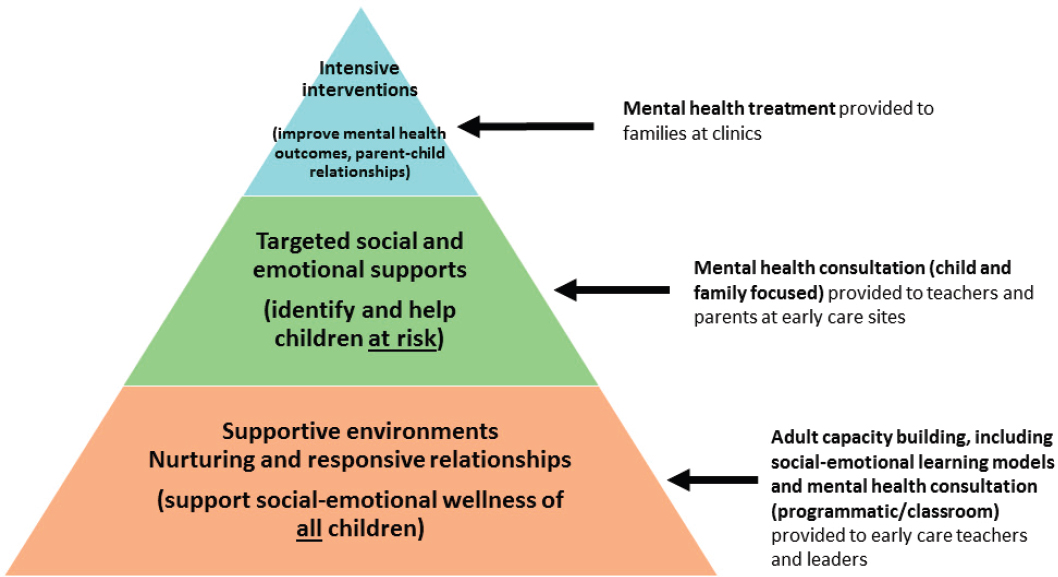
SOURCES: Askew presentation, September 14, 2017; Bureau of Children, Youth, and Families, New York City Department of Health and Mental Hygiene, 2017.
responsive relationships that will support the social-emotional wellness of all children. This is done through building the capacity of teaching and program staff to foster positive learning and development, to promote each child’s social and emotional well-being, and to build relationships with children and communication with parents. The second step is to offer targeted social and emotional supports and to identify those children who need help or are at risk. This is done through specific mental health case consultation. Each mental health consultant carries a case load of about five sites, with a maximum of three classrooms per consultant per site. The number of case-specific consultations will then vary depending upon the needs identified at each site. The New York City model asks that consultants spend one day per week at each early care and education site. The third step is to provide mental health treatment for those children who need it. This is an intensive intervention to alleviate distress and return children to healthy development.
Mental Health Consultation: Accelerators, Challenges, and Community Impact
ThriveNYC has been a program accelerator for the SEL program, Askew said, as all mental health consultants are funded through ThriveNYC. Sustainability has been a challenge, as mental health consultants are not covered through Medicaid. Askew mentioned the possibility of using Medicaid coverage through the First 1,000 Days on Medicaid initiative in New York.3 Dosage is also an issue. For this approach to be effective, Askew said, the dosage has to be fairly high in order to build the kinds of relationships needed in these environments. Spending only one day per week at each site limits the case load that the mental health consultants can carry. Another challenge is reach. Currently the workforce is reaching about 75 out of 400 sites. The workload of teachers and other adults who are serving children in early learning situations is heavy, and it becomes an obstacle to teachers’ full involvement and to their ability to benefit from the intervention of the mental health consultant.
An evaluation is currently being conducted to explore the community impact of the SEL program in the different demographics being served, Askew said. The evaluation is also attempting to look at value in improving teacher well-being as a result of the support and consultations being brought to the environment.
___________________
3 See https://www.health.ny.gov/health_care/medicaid/redesign/first_1000.htm (accessed October 30, 2017).
Other Early Care and Education Initiatives at the DOHMH
Askew concluded by briefly describing several other early care and education initiatives at the DOHMH. The Early Intervention program worked with the DOE and the Child Care Bureau to amend the Health Code to ensure that therapists were able to deliver services to children with delays and disabilities in early care and education settings. Askew explained that there had been some issues with care providers not allowing the therapists to enter the early care and education settings. He suggested that states consider what steps might be needed to better facilitate access to children in their natural environments and their least restrictive environments. In response to a question, Askew acknowledged that there is always the question of the ability to enforce the elements of the health code. For any amendments to the health code, he said, there must be some ability to track that it actually gets done.
The DOHMH is also focused on oral health, and it is integrating oral health messaging into its partner newsletters. The results of a Child Dental Survey, which assessed risk and prevention behaviors for tooth decay among children, led the DOHMH to launch an early childhood dental caries campaign. The department has also developed, Askew said, a policy proposal to amend the child care regulations and the health code to mandate tooth brushing at all child care centers in New York City.
The DOHMH’s Division of Prevention and Primary Care has a variety of programs focused on nutrition, healthy eating, physical activity, and active design, Askew said. For example, the Eat Well, Play Hard program is a nutrition education program led by registered dieticians in group child care centers. The program reaches approximately 100 centers in the city and targets children ages 3 and 4 years old as well as caregivers and child care staff. The Farm to Preschool program provides opportunities for parents and staff to purchase a box of local produce at child care centers, offers nutrition education and cooking demonstrations for adults, and provides teachers with a curriculum to engage children in gardening.
Finally, the Active Design in Early Child Care Settings program provides active design mini-grants to early child care centers located in low-income neighborhoods throughout the five boroughs. The goal of these mini-grants, Askew said, is for sites to purchase low-cost enhancements that increase active play in the outdoor spaces at their centers (e.g., gardens, circulation routes, loose toys). These are just some of the ways the New York City DOHMH is working to integrate health into the early care and education setting, he concluded.
HEAD START AS A LEVER TO IMPROVE POPULATION HEALTH
Head Start is a federally funded program serving pregnant women and children, from birth to kindergarten entry, who are at or below the federal poverty guideline, Shinn-Brown said. Federal requirements for the program are intended to support the whole child, and Head Start is meant to be a comprehensive child and family development program.
Health is a critical factor in early childhood education and school readiness. Children who come to school with, for example, teeth that hurt, runny noses and earaches, or trauma in their lives and behavioral dysfunction in their families do not learn as well as children who come to school without those challenges, Shinn-Brown said. Head Start is focused on primary prevention and health promotion, and the program gathers data to inform its practice and ensure that it is supporting children’s health. Head Start is federally mandated to provide screening, referral, follow-up, integrated health education, and ongoing observation and assessment, she said. Head Start programs are able, through specific processes, to use Medicaid funds and private insurance funds to offset the costs of providing these services; Head Start itself is the payer of last resort.
Supporting Health Equity
Head Start supports health equity. It is more cost effective for families to have good health care than it is for them to suffer the ill effects of poor health care, Shinn-Brown said. She raised concerns about cost containment measures within state systems that tend to force families out of care, instead of bringing them into care.
One approach to fostering equity is addressing family health literacy. Shinn-Brown referred participants to the work of Ariella Herman of the University of California, Los Angeles, Health Care Institute.4 The Health Care Institute’s approach to health literacy education is used by Head Start programs. Shinn-Brown said that Herman’s groundbreaking work has demonstrated the importance of health literacy in helping parents be good consumers of health care, in reducing lost time for illness and absenteeism both for parents and their children, and in reducing emergency department visits and increasing connections with medical and dental homes.
Shinn-Brown said that Head Start also supports health equity through family advocates who work individually with families to help them set
___________________
4 For information, see http://www.anderson.ucla.edu/centers/price-center-forentrepreneurship-and-innovation/for-professionals/health-care-institute (accessed October 30, 2017).
goals that support positive health outcomes. The family advocates emphasize health promotion and disease prevention, and they work with families to help them maintain their insurance coverage, overcome barriers to access (especially in rural areas), and keep appointments.
Developing Relationships with the Community and the Health System
Every Head Start program must conduct a community assessment of the factors that affect the health of the population it serves, Shinn-Brown said. Each Head Start program also convenes a health services advisory committee, which is a multidisciplinary group of professionals, including parents, who help the program make decisions about services, referrals, resources, and policies and procedures.
Head Start partners with many different types of providers to supplement Head Start funding with community resources. These providers include federally qualified health centers; hospital systems; mental health providers; community health departments; the Supplemental Nutrition Program for Women, Infants, and Children (WIC); and others. Shinn-Brown said that Head Start struggles to provide mental health services in her state, and she emphasized the importance of mental health services for young children who experience trauma and of trauma-informed practices to support young children and their families.
Providing the Required Health Screenings
Head Start programs are required to provide a range of health screenings, using valid and reliable tools. Vision is tested using an instrument-based screening approach and symbol sets. As an example of how valuable these screening practices can be, Shinn-Brown said that OACAC Head Start serves just under 1,000 children in its 10-county service area in Missouri, and last year 156 children were referred for a vision concern. Head Start does not offer diagnoses, but instead it screens and refers families to their primary care provider for follow-up. Of the 156 children referred, 136 received glasses. This means, she said, that more than 10 percent of the children in OACAC Head Start—children who had a medical home—had not been identified as having a significant vision concern early in their childhood experience. Other screenings include hearing, dental, developmental, sensory, behavioral and mental health, nutrition status, and injury prevention. OACAC Head Start partners with Parents as Teachers, a home visit–based curriculum model for child development, to provide developmental screens. Shinn-Brown noted that sensory screening can be a challenge when a child has a sensory processing dis-
order, for example, or autism spectrum issues. As mentioned, Head Start programs may use Medicaid and private insurance as a reimbursement stream and may use Medicaid reimbursement to offset the cost of these types of screenings. OACAC Head Start contracts with a local physician, who writes standing orders for all of the required screenings so that they are billable. Shinn-Brown said that Medicaid reimbursement also allows her Head Start program to fund three full-time counselors on staff as well as a full-time nurse and a part-time nurse. She said that the state is continuing to work through the transition from a Medicaid fee-for-service model to a managed care system and is lagging behind in terms of best practices.
Challenges
Shinn-Brown highlighted several challenges Head Start faces. Many states, including Missouri, lack coordinated, state-wide early childhood systems, she said. For example, there are barriers to Head Start and WIC providers sharing information about children who are nutritionally at risk (above the 95th percentile or below the 5th percentile). There are now ongoing efforts to find ways to share information instead of duplicating efforts, she said.
Another challenge is that, especially in rural areas, there is an over-reliance on the parent report in the health system to meet the Medicaid Early and Periodic Screening, Diagnostic, and Treatment requirements, Shinn-Brown said. She observed that there is often a “wait and see” attitude among pediatricians in the more rural areas when it comes to developmental issues. This results in children not being referred for services when they could have been eligible for Missouri’s First Steps early intervention services for children ages birth to 3 years (under Part C of the Individuals with Disabilities Education and Improvement Act), she added.
Access to appropriate behavioral health supports for very young children, including to mental health professionals trained in a trauma-informed care approach, is also lacking, Shinn-Brown said. Health equity and access affect suspensions and expulsions in young children, particularly young children of color. Until there is a more effective way of supporting young children with a trauma-informed care approach, she said, young children will continue to be expelled from classrooms and then bounce from program to program until they land at Head Start’s door. This is a complicated and difficult situation, she said, and she emphasized the need to support all child care providers so that they in turn are able to support all children.
HEALTH, ACCESS, AND AFFORDABILITY IN CHILD CARE
Child Care Aware of America is a national nonprofit membership organization for local child care resource and referral agencies.5 In many states, Scott said, these agencies are responsible for consumer education and for connecting parents and families with child care in their area, which involves getting to know families and what they need. Resource and referral agencies also conduct much of the training and professional development done within states to help improve the child care workforce, and they are also involved in policy development and advocacy.
As senior director for health policy at Child Care Aware, Scott said, she is focused on how to make child care settings as healthy as possible. She listed some of the current state-level early care and education priorities that the member agencies are working on. In Minnesota, for example, one of the priority issues is addressing a shortage of licensed care providers. In Maryland, the current priority is increasing the Child Care Subsidy Program budget to help the lowest-income families access child care.
Another priority area for the agencies is the implementation of the reauthorized Child Care Development Block Grant, in light of the many new requirements for such grants. Scott highlighted three key aspects of the reauthorized block grant: it authorizes the Child Care and Development Fund, which provides federal funds for states to disburse child care subsidies for low-income families; it establishes baseline standards for child care systems that states must meet in order to receive this funding; and the receipt of funding obligates states to invest in improving the quality of child care. Scott noted that only one in every ten children who are eligible for federal child care subsidies actually receive them.
Establishing Standards
Prior to the reauthorization of the block grant, Scott said, states varied widely with regard to basic health and safety standards, and she referred participants to two Child Care Aware reports, We Can Do Better and Leaving Children to Chance, which chronicle state policies on health and safety requirements for child care.6 At the time of the reports (2013 and 2012, respectively), most states had requirements for basic health and safety, but only 16 states met all of the 10 health and 10 safety practices recommended by pediatric experts. Scott also mentioned the Child Care Licensing Database, which compares state licensing regulations to the recommended
___________________
5 See http://childcareaware.org (accessed October 30, 2017).
6 These reports and other advocacy and policy resources are available at http://usa.childcareaware.org/advocacy-public-policy/child-care-and-development-block-grant-ccdbg (accessed October 30, 2017).
standards outlined by the Administration for Children and Families in the report Caring for Our Children Basics.7
Investing in Quality
As noted, the reauthorized block grant requires states to invest in activities that improve the quality of child care. The amount of funds that must be spent on quality improvement increases over the course of implementation of the reauthorized block grant, Scott said, and by 2021 states will be required to set aside a total of 12 percent of their block grant funds for quality-improvement activities (9 percent, plus an additional 3 percent specifically for infant/toddler quality-improvement activities). Under the program requirements there are many different quality-improvement activities that states can spend block grant funding on. Scott mentioned several examples, including basic health and safety training for all child care providers (including health, nutrition, physical activity, and obesity prevention); consumer education, including websites with information on quality, best practices, and support services (e.g., WIC, Medicaid); and the incorporation of healthy active living into quality rating and improvement systems.
Healthy Child Care, Healthy Communities
Scott described the Healthy Child Care, Health Communities Project as an example of how Child Care Aware partners with state systems to help them include health in their state child care plans. Child Care Aware has developed recommended language for states to use in drafting their state plans. She noted that Alabama used this language to make public comment recommendations on its initial state plan. In addition, a toolkit was created to help states develop messaging that resonates with child care providers and the public to increase acceptance of change. Focus groups on staff health and wellness were held in order to understand the ways in which the new policies being enacted were affecting the behaviors of the child care providers themselves. Scott noted, for example, that providers are modeling healthy behavior in front of the children (e.g., not drinking soda), which is good for them as well as for the children.
Geographic information system mapping is done to examine the current use of existing resources from an equity perspective. These data
___________________
7 The Child Care Aware of America Child Care State Licensing Database is available at http://licensingdatabase.usa.childcareaware.org. The Administration for Children and Families report Caring for Our Children Basics is available at https://www.acf.hhs.gov/sites/default/files/ecd/caring_for_our_children_basics.pdf (accessed October 30, 2017).
are then used to drive project investments and engage stakeholders to develop cross-sector solutions. The Alabama Farm to Early Care and Education program, for example, is exploring the relationship between family child care providers and proximity to farmers, with regard to opportunities for the procurement of fresh local foods. In New York, breastfeeding-friendly communities are being mapped. In Indiana, mapping is being done of where there is access to safe spaces to play in community revitalization neighborhood grantees, to identify where investments are needed, and to encourage care providers to use those spaces for active play.
In closing, Scott described her theory of change (see Figure 3-2). It is not enough to have healthy spaces, she said. Affordable and accessible child care, elements of healthy child care, and equity-rooted change levers must come together to achieve high-quality child care and healthy communities, which in turn affect the social determinants of health.
PROSPER LINCOLN
Prosper Lincoln is a community initiative that seeks to transform Lincoln, Nebraska, into a thriving community for people to live, work, and play, where there is equitable opportunity for all residents to have the income, education, and resources they need to be successful, Suarez said.8 Lincoln, the capital of Nebraska, is home to about 280,000 people. The unemployment rate is 2.6 percent, the crime rate is low, and there is affordable housing. In 2014 the first Lincoln Vital Signs report was released, examining the statistics and demographics in Lincoln. The report concluded that Lincoln does many things exceptionally well and should be proud of its accomplishments and the quality of life, Suarez said. However, it was also found that a growing proportion of Lincoln’s population faces real need and that Lincoln’s children are particularly vulnerable. Prosper Lincoln was begun as the community’s response to these findings, with the overall goal of addressing youth success, economic prosperity, and quality of life. Eight key sectors have been involved in the development of the community agenda: (1) nonprofit organizations, networks, and cultural centers; (2) businesses; (3) neighborhoods and the general public; (4) the public sector; (5) the faith community; (6) anchor institutions (e.g., universities, hospitals); (7) K–12 education; and (8) philanthropy and donors. Together, these sectors are working to improve the health and prosperity of Lincoln.
Also in 2014, the Community Health Endowment of Lincoln undertook a mapping project to better understand the role of place in the
___________________
8 For more information, see https://www.prosperlincoln.org (accessed October 30, 2017).

SOURCE: Scott presentation, September 14, 2017.
health status and behaviors in the community. The results showed that place matters. Depending on where one lives in Lincoln, Suarez said, life expectancy varies by as much as 20 years or more.
To begin to address these issues of quality of life in Lincoln, funding priorities were identified, and early childhood was targeted for health, wellness, and prevention interventions. High-quality early childhood development and learning affect children in both the short term and long term, Suarez said. The foundation for later learning, behavior, and health is dependent upon the quality of early learning and care. Interventions and support are most effective in the first 3 years of life, but many of the children who need help and support the most are not receiving it. In Lincoln, approximately 65 percent of the most vulnerable children ages 3 to 5 are not enrolled in preschool programs. The percent of children in poverty in Lincoln increased by 78 percent between 2008 and 2015, and more than 12,100 children (1 in 5) are now living in poverty. The program capacity of high-quality early care and education programs is insufficient to meet this demand.
Prosper Lincoln Strategic Plan for Early Childhood
The Prosper Lincoln community agenda was developed around three priorities: early childhood, employment skills, and innovation. Strategic plans were developed over the course of 12 months, through an intensive community engagement process, and the implementation of the plans began in August 2016. The overall desired outcome of the strategic plan for early childhood, Suarez explained, is to reach the Prosper Lincoln goal of nurturing every child on the path to success. The specific goal is for all children to be kindergarten ready. Work is ongoing with the public school system to identify measures of literacy and numeracy and to determine how to measure SEL learning and executive function.
Suarez said that the “kindergarten ready” goal also implies that schools and communities are ready to meet the needs of the children. In this regard, a Community Early Childhood System of Care self-assessment was conducted. Providers and parents were asked about their perspectives on schools, family resources, health, and early childhood mental health. Provider and parent responses were compared to identify gaps and develop priorities for action, which led to the convening of three workgroups focused on the following topics:
- Quality care and education. Data and mapping studies inform the work of this group. More resources are needed, Suarez said, so that children from low-income families have access to high-quality early care and education.
- Comprehensive health, including early childhood mental health. This group is convening public sessions to develop a vision of what Lincoln wants for its children. Specifically, it is asking: What are the essential community elements needed to ensure that children and their families are safe, heathy, and kindergarten ready? What systems of data collection are needed to better track children’s progress from birth to kindergarten and to make sure that stakeholders who support children are all on the same page?
- Communication and messaging. Communication and messaging is a very important part of the strategy, Suarez said. She noted that the mayor of Lincoln met with about 100 business leaders who are coming to the table because they see the potential return on investment in a healthier community.
Programs
Suarez shared an example of a parent education program at a school with a very large immigrant and refugee population. The program was designed so that parents could explore a topic related to children with a focus on early childhood, learn about books they can share with their children, and practice a learning activity they can do at home with their children. Suarez said that because English is not the first language for many of these families, the presentation includes many visual examples. For example, the idea that protective factors help create strong families was likened to the use of insulation in a house. Concepts such as executive function can be difficult to communicate, but graphics can help to get the message across, she said. There are also interpreters available to help translate the presentation. Programs include a book and a play activity and emphasize the importance of pretend play as part of learning. Parents try the activity during the program, and they discuss examples of what they can talk about with their children at home. The activity adds enjoyment and levity to the program as well as providing parents with a play activity they can do at home. There is also interactive discussion of various topics, such as keeping families strong, parental resilience, and concrete support systems, with parents sharing their ideas.
Prosper Lincoln continues to measure the outcomes of its work, Suarez said, and has metrics in place for its early childhood strategies.
DISCUSSION
Moderator Chang observed that discussions of sustainability are often focused on financial sustainability. She suggested that one should consider sustainability in more than just the financial aspects. As discussed
in the examples in both sessions thus far, embedding programs into state systems, establishing training competencies, and collaborating across sectors are non-financial approaches to help sustain programs. Following up on the many examples of collaborations discussed, Chang asked panelists to consider accelerators (i.e., catalysts) that might enable collaboration as well as any barriers to partnerships that might need to be addressed.
Accelerators and Barriers to Partnerships
Askew reiterated that a key accelerator for the SEL initiative has been that it is part of ThriveNYC, which is championed by the First Lady of New York City. Having the backing of the city government can be a great advantage, he said, and political will is a strong driver of activity. Scott agreed with the power of political will. She said that from her experience across 68 partnerships, those partnerships that do not have political will behind them must rely on money and technical assistance to pave their way. Funding brings people to the table and allows them to have conversations they would not typically be able to have. Shinn-Brown agreed with the need for champions in the community. OACAC Head Start looks for children’s champions who will help move an initiative forward. She said that the Mayor’s Commission for Children in Springfield, Missouri, which includes members of the business community, is one such group of champions, and Head Start has leveraged the commission’s talents and connections. The business community is a key accelerator, Suarez agreed, and she said it is important to make sure that community becomes part of the fabric of the work.
One of the basic barriers to collaboration, Askew said, is that it is hard. Breaking down silos and getting people to “leave their egos at the door” and accept a genuine partnership can be difficult, even among colleagues who like each other and who generally work well together. Scott suggested that unintended consequences of policies can be barriers to partnerships. Shinn-Brown observed that there are challenges when an administration is committed but the shared vision has not been firmly and adequately articulated downstream to the staff who are doing the daily work to resolve issues of competing priorities. Suarez suggested that one barrier is that people simply may not fully comprehend the importance of a child’s early years as the foundational time for health and healthy behaviors. A significant, ongoing educational component is needed to ensure that people understand that this is where attention is needed.
Pasti observed that much of the discussion has been centered on external collaboration, and he asked about cross-sector collaboration within a large organization, such as the New York City DOHMH. Askew said that there are often long-standing silos that can be difficult to break
down, but efforts are being made. He cited his efforts to bring together all of the people working on early childhood health and development across multiple areas within the health department to share information and avoid duplication.
Additional Gaps and Opportunities
Carrie Bateman of the New York City DOE pointed to disability as one gap in the intersection between health and education. New York City currently has 270,000 students with disabilities, which is about 21 percent of the total student population, she said, noting that the national rate is about 13 percent.
Dave Kindig of the University of Wisconsin–Madison asked about the degree to which nonprofit hospitals (which are required to do community benefit as a condition of their tax-exempt status) are addressing the early care and education resource gaps. Scott replied that she had heard anecdotally that it is part of the conversation. Chang said that a number of children’s hospitals are focused on this, mentioning in particular Nemours Children’s Health System, Atlanta Children’s Hospital, and Cincinnati Children’s Hospital.
Kindig suggested that one role for those in population health will be finding ways in which the health care system and public health can help the early care and education sector achieve its goals. There is a co-benefit to both sectors. Askew added that it is incumbent upon those in health to partner with those in housing, parks, education, and other sectors in order to address the issues known to be social determinants of health.
GALLERY WALK REFLECTIONS
Following the panel discussion, participants moved to the gallery to consider the following:
- How can cross-sector collaboration in early care and education and health be accelerated? What do organizations need to collaborate more effectively?
- What are the main barriers to collaboration, and what are solutions to overcome them?
- What can be learned from other cross-sector collaborations that could inform early care and education and health interactions?
- What new insights can participants offer?
Upon reconvening, Pasti summarized the responses to the questions posed in the gallery and moderated the discussion. He observed that
much of the workshop conversation around collaboration was focused on children from birth to age 3. He emphasized the need to engage those working beyond the birth to age 3 segment in conversations about common terms, programs, and practices in order to better enable support of young people as they grow throughout their life spans. To increase the chances that the efforts are sustainable, collaboration across the age span will be important. Reflecting on the comments that were made in the gallery, Pasti drew out three main themes: trust, infrastructure, and leveraging the existing work.
- Trust. Pasti noted that the issue of trust was raised during the discussions of community engagement. Trust is also essential for collaboration. Some of the comments noted the issue of “turf” as a barrier to collaboration. It was also noted that, when engaging in new collaborations, it is important to pay attention to the history of collaboration in the particular community. Building relationships was highlighted as an important element of collaboration. The element of trust is also critical to family engagement, Pasti observed. Family engagement is not just talking to a family’s members about what their needs are, but it is also having them actively involved in the solutions, interventions, and evaluations, thereby fostering community ownership of the issues and outcomes. One aspect of collaboration that is often overlooked is youth engagement, as the focus is often on the parents. Pasti mentioned an example from one of the communities involved in the 100 Million Healthier Lives initiative. A group of high school students who had learned about a continuous improvement model felt that model was important and wanted to share it, so they started teaching sixth-graders the continuous improvement model. This raises the question of how to tap into youth and engage young people in more meaningful ways, Pasti said. He mentioned the concept of two-generation approaches that address the needs of both parents and children (i.e., the whole family).
- Infrastructure. Several comments posted focused on the infrastructure or the “ingredients” needed to make collaboration work. Governance and the rules of engagement are important, Pasti said. This includes treating one another with respect and making sure that the roles and responsibilities are clear. It is also important to “get down to basics” and establish exactly what it is that the collaboration is for (e.g., money, sharing information, training and professional development, data, evaluation, technical assistance, resources).
- Leveraging the existing work. Comments were made about the need to pay attention to the existing work. As mentioned earlier,
sustainability is not only about money; it can also stem from embedding initiatives into existing programs and systems. An example was posted about leveraging health sector regulations around community health needs assessment and community health improvement plans. How can early care and education and health initiatives be built into those plans to provide sustainability? Can early education and health initiatives be tied into other “cradle to career” programs? There were also comments about the use of common terms. Pasti noted that the same words cannot always be used across programs, as particular terminology might be required by regulation or statute. Conversations are needed to ensure translation and understanding of what is included when a particular term is used.
One participant emphasized that leadership is essential to collaboration. She suggested that there is a knowledge gap among those in leadership positions who make decisions about funding and financing within the state Medicaid offices, within managed care and health insurance companies, and within health agencies concerning issues involving young children. Those in leadership positions do not think about young children, she suggested, perhaps because they are not the primary drivers of cost in their decisions. She mentioned New York’s First 1,000 Days on Medicaid Initiative as a step toward spreading the message about the need to focus on early child development. Pasti agreed and mentioned the need to invite a broad array of stakeholders to the table and to not make assumptions about what they do or do not know. In addition, training is generally attended by those with the same background or responsibilities. There are opportunities to invite others beyond the early child care and health sectors, such as those working in child welfare. Pasti suggested that cross-system professional development can help break down the barriers between disciplines and foster understanding of what is important to each organization. Start small, he suggested, and invite other stakeholders to existing trainings.
Elizabeth Groginsky, the assistant superintendent for early learning in the District of Columbia, referred participants to the program Our Children, Our Community, Our Change and to the Early Development Instrument, a population-based measure of school readiness.9 The program has mapped the city at the neighborhood-cluster level for health, development, and school readiness at the pre-K/age 4 level. Additional data, such as violent crime and assets, were overlaid on the readiness maps. The mapping process brought many partners together, she said,
___________________
9 See http://www.raisedc.org/ourchildren (accessed October 30, 2017).
and the mayor encouraged all of the state district agencies to take a look at it. Such population-based data can help sectors come together and share data that could add to the conversation, she said. There is also a facilitator’s guide that leads people through how to bring cross-sector local community partners together to facilitate conversation and begin to take action on the data. The goal is to change those conditions in communities that are affecting young children entering school so they are ready to learn. Pasti added that these mapping data also help to facilitate conversations about equity. There are some areas, for example, that have high assets but low scores. The data allow for consideration of the deeper issues that affect students.
This page intentionally left blank.






















