4
Outsourcing Options and Marketplace Tools
This chapter covers four presentations on outsourced options for facilities management and marketplace tools that could aid in the workforce modeling process for the Veterans Health Administration (VHA). The speakers represented three private-sector companies in facilities management—CBRE, JLL, Plan4 Healthcare—and the RSMeans costing tool.
WORKFORCE PLANNING
This workshop session described work undertaken by CBRE Group, Inc. (CBRE), to bring consistency and best practices to health care clients across the United States. For this workshop session, the committee had asked the speaker to address the following questions, which he touched on throughout the course of his presentation:
How does your approach calculate workload requirements for different jobs? Does the approach consider as-is and desired productivity levels? Can the approach adjust staffing requirements to account for location-specific conditions? How does the approach account for anticipated changes in skill and workload requirements? And, are individual jobs largely considered interchangeable or are they ever staffed at the team level?
John Poulos (senior managing director, CBRE) began by explaining that part of his role as vice chairman of CBRE’s health care sector involves an attempt to bring consistency and best practices to all of CBRE’s health care accounts nationwide. He then described a number of factors that are key to accomplishing this goal.
To calculate workload requirements and assess productivity, Poulos emphasized the importance of the implementation and effective management of an appropriate work order system. He noted that there are many work order systems in existence, most of which can track the metrics necessary for effective workforce planning if properly managed. The work order system should encompass all of an organization’s facilities and assets, and it should contain accurate preventive maintenance schedules and estimated completion times for both preventive maintenance and regular work orders. He noted that work orders can be tagged with “service levels” that are tied to the appropriate response time, depending on the urgency of the task. This tagging also provides those who place work orders with an idea of when the work will be completed. Poulos noted that customer satisfaction surveys can be used to assess the effectiveness of a work order system and that many of CBRE’s accounts average 99 percent customer satisfaction.
Appropriate use of a work order system allows the tracking of various metrics, Poulos noted, with such tools as Tableau1 providing easy access to that information. Important metrics to monitor include execution of preventive maintenance to assure 100 percent completion each month, overtime, and the utilization rate for technicians’ time. In terms of tech utilization, Poulos went on to explain that tech utilization data can be used to determine whether employees are over- or underworked and can also be applied to identify and upscale efficient employees. Those effective individuals can be trained to perform tasks currently performed by vendors, ultimately decreasing vendor costs. However, Poulos acknowledged, the usefulness of a work order system to track these metrics ultimately requires that employees enter information accurately and consistently.
To address the issue of adjusting staffing requirements to account for location-specific conditions, Poulos said that gearing ratios—such as 41,000 square feet per full-time-equivalent staff person (FTE) for hospitals or 100,000 square feet per FTE for outpatient centers—are good guidelines, but in order to staff appropriately, each facility has to be examined individually to determine the function of the facility and the services it provides. The age of the facility is also a factor affecting the gearing ratio. Poulos stressed that there is no simple formula for adjusting staffing between locations: “You do need to look at the function of the facility, the service that it provides and, again, considering the safety of the patient as being primary, you staff accordingly.”
Throughout his presentation, Poulos touched on other factors relevant to effective workforce planning. He noted that, in his experience, centralization was a consistent theme. Poulos used the example of the Cleveland Clinic, in which CBRE was involved, to illustrate this point. Originally, every medical center in the Cleveland Clinic had its own administrator and its own maintenance crew, and signed its own leases. Procedures differed from location to location. CBRE brought everything under a single management group, with a director of operations and regional directors of engineering. To make the sweeping changes required for centralization, Poulos emphasized the importance of communication at all levels, clear alignment of individual goals with the overall goals of the organization, and building of a “caretaker mentality” among the entire workforce.
Following Poulos’s presentation, the first questions and discussion focused on centralization. Kim O’Keefe (committee member) asked about the procedure CBRE uses for centralization. Poulos explained that CBRE first works with an organization to establish buy-in at the local level, so that each facility agrees to turn over control. CBRE brings in the leadership, technology, and best practices, and the current workforce is hired and reorganized to place workers in appropriate positions. Employee satisfaction surveys are implemented to assess employee reaction to the process. In response to a question from a participant, Poulos stated that voluntary employee loss in the first year following centralization trends around 10–14 percent.
James Smith (committee cochair) asked whether pushback was experienced from center executives in response to the centralization of Northwestern Medicine (also a CBRE project). Poulos replied: “They were all for it. They didn’t want to deal with it.” Smith further asked how much time it took to show that the centralization method was more cost-effective and responsive. Poulos replied more expansively: “It took about 18 months. It takes time. A lot of people look for results immediately. They think that an outsource agreement is a magic wand, and it really isn’t. It takes time. We needed people to engage with each employee and help them understand what it is we were trying to accomplish. And we needed to put our systems in place. Tagging assets alone is monumental. So, with all these things in place, we are seeing the successes and recording them, but it takes at least 18 months, in some cases 24, if the portfolio is very dispersed.”
Several questions focused on methods of staffing specific trades and on the way variations between different facilities in an organization affect their staffing methodologies. Smith asked, “As you look at the individual facilities, how do you take into account and how do you resource based on the age of buildings and the number of buildings at a facility?” Poulos replied that the process takes time because even if the age and number of buildings is known, the maintenance status of the equipment within those buildings is often unknown at the outset. As this information is acquired, the appropriate staffing can be performed to align with the need. Poulos explained that staffing for specific trades is often based on historical workload rather than algorithms because new buildings need different trades than older buildings.
___________________
1 Tableau is a data visualization tool created by Tableau Software. The company creates interactive data visualization products focused on business intelligence.
David Alvarez (VHA) asked Poulos to delineate some of the factors that should be considered when staffing facilities of different ages. For a quick determination of whether current staffing is appropriate, Poulos suggested that basic gearing ratios be used while also looking into the function of each facility to account for such factors as procedure rooms that would alter the gearing ratio. When these numbers are compared with actual staffing numbers, an assessment of over- or understaffing can be made. Furthermore, he said, if a work order system is in place and the information is reliable, staffing assessments can be further refined on the basis of the number and type of work orders. He noted that the condition of buildings should also be factored in. However, he noted, although facility condition assessments are very useful for understanding the day-to-day maintenance and staffing needs of specific facilities, these assessments are often not performed due to high cost.
Robert Anselmi (committee member) asked Poulos to describe the scope of the services CBRE provides for clients. Poulos explained that, as a global real estate company, CBRE can do everything from full facilities management, in which it is responsible for every piece of infrastructure (as at the Cleveland Clinic), to project management tasks, such as expanding an office or building out a suite. Additional functions undertaken by CBRE include administration of leases; compliance with applicable state and federal laws; market studies to verify that rents are appropriate; energy management; real estate tax management; quality control management of vendor contracts, such as cleaning services; and building infrastructure replacement plans, based on facility condition assessments and risk. In summary, Poulos said: “So it really is full service. Anything that has anything to do with a facility is within our ability to perform. But each organization wants something different, and we customize the solution to meet that need.”
FACILITY BENCHMARKING
For this workshop session on procedures and best practices for facilities management functions in the health care industry, the committee had asked the speaker to address the following questions, which he touched on throughout the course of his presentation:
What are the most critical factors to include in a staffing model? How do you determine when a heuristic model is good enough? Can you have several models with different structures, even bases, for different groups of staff? And, how well have your models covered the diversity of elements of an organization?
Ed Ricard (JLL) described JLL as a global organization that performs real estate and facility management, with approximately 7 years of involvement in the health care industry. JLL has 90,000 employees and manages over 5 billion square feet of facilities worldwide. It currently partners with approximately 230 hospitals and has also performed consulting for more than 600 additional hospitals, using a team of industry professionals who help those hospitals look for opportunities to improve in the areas of finance, risk, and patient satisfaction.
Ricard explained that an integrated facilities management function, in which the facilities team works in concert with the clinical team to improve the patient experience, is an important goal for every health care organization. He described several interdependent initiatives that can be implemented to achieve an integrated facilities management function. One such initiative is a “center of excellence,” consisting of a team of experts in health care, emergency management, sourcing, energy, and sustainability, that creates standards and processes to help facility directors and engineers improve their performance. Another initiative involves implementing an integrated facilities model to begin to standardize operational compliance among independent medical facilities. Another initiative that could be implemented to achieve integration is the application of a standardized computerized maintenance management system to improve employee productivity and responsiveness. Using technology for such a system, said Ricard, ultimately influences the environment of care in a facility. Employee development is yet another initiative that can be undertaken, he explained, because training is the key to the effective utilization of technology.
Ricard expanded on the center of excellence concept, explaining that its goal is to provide best practices, and these must be evidence based. Ricard noted that JLL shares its best practices not only across life sciences and health care, but across all business units so that information about effective practices is available to all, to aid in continuous development and to define the business process. One critical best practice provided by the
center of excellence involves standardization. For example, Ricard explained, every location should use the same general ledger codes, and pieces of equipment should have standardized barcoding and definitions. This type of standardization not only helps with understanding where the money is being spent, but also helps to drive maintenance strategy, and it allows for comparisons between facilities. He said that the data obtained through standardization of facilities maintenance procedures and equipment may eventually enable a comparison with clinical outcomes.
Ricard noted that hospitals share enough similarities with other types of properties, such as class A office buildings and hotels, that it is possible to run hospitals similarly to such other properties. He stated that JLL aims to help the facilities management and clinical functions of hospitals work together, as they do in the hotel industry, for example, “so that everybody knows and understands that the ultimate goal is the patient experience.” In order for integration to occur, Ricard stressed, close collaboration between the facilities management team and the clinical team is needed so that the facilities staff can fully understand the needs of the clinicians. Both the clinical staff and the facilities staff must understand that the physical environment of the health care facility is a priority, because the clinical needs of the organization cannot be met if the physical environment fails.
Ricard asked the workshop participants to imagine an ideal facilities management function: mechanical equipment that runs as designed and provides reliable outcomes, standardized engineering practices that are widely established, data-driven decisions to drive improvements, and drawings that reflect the actual conditions of the building. He explained that this vision can be achieved by partnering with a team responsive in building requests and service work, working collaboratively with the clinical side, maintaining all systems, and training employees appropriately. Ricard stated his belief that development and training are critical components of success in building an ideal facilities team, as it is in furthering the careers of individuals, but he acknowledged that many hospitals spend their training dollars on clinicians, not on facilities staff. He noted that JLL has developed certifications for a number of technical specialties, 20 percent of which are very specific to the health care environment. Skills assessments are done for new employees, and programs are designed to help them learn skills, become more efficient, and understand the importance of their role in the organization.
Ricard stressed that JLL understands the importance of data, and he detailed various forms of data collected by JLL and how they are used. For example, data on financials, employee productivity, uptime, and response times can be used to create key performance indicators that can help an organization improve in those areas of facilities management. Customer satisfaction surveys can provide data that will ultimately improve the experience of doctors, nurses, and patients. JLL also gathers data from all of its hospital partners, ranging from the size and location of each facility to the number of open work orders that are work-safety related, in order to monitor facilities, set priorities, and make business decisions.
The majority of the questions and discussion in the session focused on various aspects of JLL’s facilities management function. Anselmi asked Ricard several questions related to this process. First, he asked Ricard to elaborate on the kinds of staff JLL uses to perform successful facilities management. Ricard explained that in areas where JLL has multiple hospital clients, each hospital will have a generalist on-site, but the hospital clients will share specialists, such as HVAC [heating, ventilation, and air conditioning] specialists, that are employed by JLL. Ricard noted that JLL also has an engineering group consisting of seven full-time individuals dedicated to compliance, operational excellence, and assistance with issues in facilities. A group of performance managers collect and analyze data, using those data to help facility directors understand their priorities. Ricard noted that JLL also has staff dedicated to finance, sourcing, energy, and sustainability.
Anselmi next asked how work orders are created in JLL’s system. Ricard replied that this can happen in a variety of ways, depending on the client. He noted that JLL has a maintenance call center, completely dedicated to health care, that operates around the clock. He also explained that JLL’s goal is for 80 percent of work orders to be proactive, generated directly by the facilities department. The circulating generalist in each hospital should also have a relationship with the clinical staff, particularly the nurses, so that any work that needs to be done can be directly relayed to that generalist, who will then either do the work immediately or put in a work order.
Anselmi’s third question about facilities management processes was whether JLL performs capital asset management or oversight of construction projects. Ricard replied “yes”: last year, JLL did $1.1 billion worth of project management in hospitals alone, ranging from building entire hospitals to small projects. He explained
that for most of the company’s clients, JLL is responsible for all nonstrategic capital. Anselmi then asked about the staff JLL has on-site during construction projects, and Ricard responded by stressing that facilities functions and projects must always be coordinated so that projects do not disrupt hospital operations. Some clients will be assigned a full-time project manager who works collaboratively with the facilities team. Also, JLL has project management teams in 85 offices across the United States, and these staff can be brought into hospitals to assist with large projects.
A participant asked about the employee loss rate generally seen by clients after they partner with JLL. Ricard replied that JLL hires approximately 94 percent of a client’s employees, and, after 1 year, retention is 92 percent of that initial 94 percent.
Another major topic of discussion concerned the way facilities management is viewed within an organization and the implications of that view. Smith asked Ricard his observations on hospitals where facilities maintenance and engineering are viewed as part of the core mission, in comparison with other hospitals where these functions are viewed only as a cost or support. Ricard said that he can easily tell whether facilities management is considered part of the team simply by observing the way the facilities director is treated by the rest of the hospital staff. In Ricard’s opinion, bridging the gap between the facilities and clinical functions is very important, and the facilities staff bears some of the responsibility for working collaboratively with clinicians to recognize and solve problems.
In response to a related question from Alvarez, Ricard noted that hospital leaders also have to understand that maintaining the environment of a hospital is critical. When hospital leaders do not work collaboratively with facilities management, the hospital environment begins to suffer, which can result in greater infection rates and higher staff turnover. However, in Ricard’s view, as more people with business experience come into hospital management, the environment is beginning to change because these business people are financially trained and can understand how budgets and clinical care outcomes are affected by facilities issues. He explained that when JLL partners with an organization, it gives the facilities group a voice at the executive level. When an older piece of equipment needs to be replaced, for example, JLL works to provide hospital leaders with hard data to make the case for replacement, including the cost of recent repairs, the amount of downtime and the resulting lost revenue, and the energy savings from new equipment, all of which help to illustrate the return on investment.
Several questions revolved around the methods used by JLL to perform staffing modeling and benchmarking. Cheryl Paullin (committee member) asked Ricard which factors JLL considers when creating staffing models for facilities management. Ricard replied that the creation of staffing models is a complex journey that takes about 3 years to complete. Differences in the sizes, ages, and locations of facilities necessitate employees with varying skill sets in each location. Ricard explained that JLL’s first tasks with a partner client are to assess the skills of existing employees and determine the type of equipment in the facility. JLL also uses technology to understand how productive employees are by tracking their hours through work orders. These data, he said, can illuminate opportunities for training in order to improve employee efficiency. Ricard noted that JLL also tries to assess the true need for specialists, for example, by determining how much of an electrician’s time is spent doing electrical work in comparison with work that could be performed by a generalist. In general, Ricard said, the modeling process first involves gaining an understanding of the right skill sets and people needed to staff a facility.
Paullin also asked about JLL’s procedure for benchmarking. Ricard replied that when JLL works with a client, the client is first provided with a data request, asking for information about facilities, finances, and employees. JLL staff also walk the facility to directly observe certain procedures, and they also look at the facility’s computerized maintenance management system. All of the data collected from these activities are formatted to allow comparison with a facility run by JLL, and the client is then provided with a report containing categorized results, opportunities for improvement, and an outline of the steps that could be taken to reach the client’s objectives. Colin Drury (committee cochair) asked whether JLL performs benchmarking across much larger organizations, like the VHA, rather than just single hospitals. Ricard replied that JLL has undertaken large benchmarking studies with several organizations, including Tenet, with 64 hospitals, and Kindred, with 128 hospitals. He noted that the challenge in benchmarking larger organizations is standardizing the data collected among facilities. It is critical, Ricard said, for the benchmarking staff to be trained to look for the same things and gather the same data, and JLL has a site audit tool to help with that data collection.
In concluding, Ricard said that successful change can be challenging, and he cited evidence that 70 percent of change programs fail to achieve their goals, largely due to employee resistance and lack of management support.2 “If we’re going to make change, make sure we’re all buying in, and that we know where we’re going, and that we’re all behind it, and that we have a clear vision and plan of how we’re going to change.”
BUSINESS PLANNING FOR INCREASING OPERATIONAL EFFICIENCY
For this workshop session on the best practices and tools used by Plan4 Healthcare, the committee had asked the speaker to address the following questions, which he touched on throughout his presentation:
How does your approach calculate workload requirements for each job? Does the approach take into account as-is and desired productivity levels of the workforce? Can the approach adjust staffing requirements for location-specific conditions? And who are the key participants in the development process?
Seth Sinclair (Plan4 Healthcare) explained that Plan4 Healthcare was founded in 2015 with a mission of “enabling smarter planning for better outcomes” for health care facilities, particularly for the VHA. Sinclair noted that he had personally worked in various capacities with approximately 50 hospitals in the VA system. Plan4 Healthcare currently has a team of approximately 20 subject-matter experts, including former directors and chief financial officers of the Veteran’s Integrated Service Network and a health care economist. The team is currently working with 22 VA medical centers (VAMCs), which represent approximately 15 percent of the VA health care system, to assist the VHA with implementing best practices for business planning.
Sinclair outlined the core planning challenge shared by all VAMCs, which involves first determining the goals, objectives, and priorities of the local leadership. Second, each facility has to understand its operational needs and the resources required to meet those needs. Third, each facility has to have a clear picture of its budget and the resources it can afford. He explained that bringing these three factors into balance helps an organization achieve its operational priorities while remaining financially responsible.
Sinclair listed several challenges and variables at play at each VAMC that can interfere with the development of effective core planning. These challenges include, but are not limited to, lack of standardized processes or tools for facility-level planning; differing philosophies on how such planning should be conducted; and leadership turnover, which results in the loss of any progress made in establishing planning processes. Plan4 Healthcare, Sinclair explained, aims to provide solutions to the difficulties posed by these challenges and other variables among VHA facilities in order to aid the organization in business planning and implementation.
Sinclair went on to explain that the concept of Plan4 Healthcare was first tested in 2011 on a single mid-sized VHA facility that was operating with a significant budget deficit. In 1 year, Sinclair’s team was able to use the basic concepts of what eventually became a model to bring the facility back to a balanced budget. That model, SCORE, contains five elements—strategy, collaboration, operations, results, and excellence—that work together systematically to promote data-driven decision making and to foster consistent use of planning tools and practices. He noted that the SCORE model has evolved to support all organizations in planning best practices, not only those organizations in financial distress. These tools and practices allow medical centers to prioritize operations and operate effectively and sustainably within their budgetary constraints. The SCORE model contains a web-based technology platform, called 4Cast, created by Sinclair’s team and tailored for the way VAMCs plan and operate.
To further explain the SCORE model, Sinclair first outlined the process of business planning. Sinclair defined business planning as a bottom-up process in which every department or service in a hospital develops a plan that includes tactical objectives and data-driven resource needs for the coming year. These plans should support the overall goals of the facility. Plans should also be briefed regularly to leaders, with key players from other departments also present, so that the implications of individual plans on other services can be assessed. Sinclair asserted that, if every service in a medical center develops a well-supported business plan, leaders can use these plans to
___________________
2 Ewenstein, B., Smith, W., and Sologar, A. (2015). Changing Change Management. Washington, DC: McKinsey & Company. Available at https://www.mckinsey.com/featured-insights/leadership/changing-change-management.
understand the needs of the entire facility and to prioritize resource requests. Sinclair advocated for this decision-making process even in the face of acknowledged budgetary restraints that make the process difficult: “It’s better than going into the year without having that decision making, without having that transparency, and facilities who don’t do that will get in trouble with their resources as the year progresses.”
Sinclair then provided a practical example of 4Cast in action—a facilities management service business plan created using the 4Cast tool—and explained the various components of the tool that can assist with each stage of the business planning process. As a preliminary step, 4Cast can assist each service with a strength, weakness, opportunity, and challenge analysis, capturing this information so that it can inform the service’s tactical objectives for the year. 4Cast can also capture workload, which is a key component of business planning. Sinclair acknowledged that workload data from VHA facilities are extremely variable, with different metrics used to capture workload, such as the ratio of FTEs per square foot, the numbers of projects, or the number of work orders. He explained that at this phase of the tool’s development, 4Cast allows users to determine their own workload metrics, which the Plan4 Healthcare team eventually plans to aggregate and standardize. Another component of 4Cast that can assist with the business planning process is a make-or-buy analysis tool, which helps organizations determine which services should be done in-house and which should be contracted out. Service-level tactical objectives can also be tracked in 4Cast, and Sinclair asserted that these proposed priorities should be the cornerstone of a service’s business plan. He restated that each objective should support one or more of the facility’s overall priorities in order to keep the service’s business plan grounded and aligned. 4Cast also includes the capability to build action plans in support of each tactical objective.
Sinclair explained that 4Cast can also assist with the resource side of business planning. The tool contains contracts and fund control points element, which compares historical resource data with projections for the coming year, allowing for justification of any significant differences. Regarding FTE resources, Sinclair underscored the importance of this aspect of an organization’s business plan, explaining that in most VA hospitals, FTEs account for 65–70 percent of the budget. He explained that 4Cast contains a module that allows services to look at FTE needs by position and to project the total cost of FTE resources for the year. This projection involves numerous gain and loss considerations, including historical turnover, retirements, transfers, the timing for filling open positions, and the timing of new hires, to name just a few. Equipment is another resource element traced by 4Cast, and this module can help services to consider all aspects of equipment purchase, including service contracts, additional FTEs required, and space considerations. Sinclair noted that the equipment module pulls data from a system called SEPG [Strategic Equipment Planning Guide], which is used by the VA to manage equipment requests and approvals.
Lastly, Sinclair summarized modules of 4Cast that aid leaders, such as a medical facilities director, in monitoring and analyzing all the data collected by the tool in order to assist with decision making, staffing, and budgeting. Once these decisions are made using the tool, services receive a passed-back budget, detailing, for example, the overall FTE budget, overtime budget, or any other budgets established for that service. Once budgets have been established, 4Cast also has tools that allow service managers to monitor their use of budgeted resources and to project use for the remainder of the year.
Following Sinclair’s presentation, several questions addressed the sources of data used for the SCORE model. Paullin asked how workload data for projected workload requirements were obtained. Sinclair replied that the source depends on the data that are available. He noted that there is a good deal of data available for clinical services, but fewer data are available for administrative services, and Sinclair’s team still relies on the service teams to provide historical workload data. He explained that his team is working diligently to establish a direct connection with all of the back-end data systems in GovCloud.
Brian Norman (Compass Manpower Experts, LLC) asked about the source of data on human capital, and Sinclair explained that the VA has a database called PAID [personnel and accounting integrated data] that lists all current FTEs and their salaries. The PAID database has a mapping system, organized by service, that assigns each FTE a code. He noted that the system can be complicated by several factors, of which the most significant is that each VA medical center has the discretion to create service alignments differently, making comparisons between facilities difficult. However, Sinclair noted, within a single medical center, PAID can be used to capture FTE data in a way that supports the model.
In another data-related question, Steven Broskey (VHA) asked whether Sinclair has seen any correlations between the number of work orders projected and the staffing necessary to complete that work in a timely and thorough manner. Sinclair replied that once enough data have been entered into the 4Cast platform by service chiefs, analytics are used to determine ratios between work orders and staffing requirements. These ratios could then be used for comparing similar facilities. Paullin asked whether tasks related to Joint Commission3 standards have already been populated into the model, since these tasks are required. Sinclair replied that this has not been done, but that these tasks could easily be incorporated as tactical objectives that need to be addressed in a business plan.
Anselmi asked if it has been Sinclair’s experience that the clinical side of VHA facilities takes priority over the facilities management function, resulting in less funding for those support services. Sinclair agreed that the clinical functions are usually first in line for resources, but he also believes that center directors are beginning to understand the ultimate necessity of facilities management in terms of the provision of patient care functions.
To conclude, Sinclair stated his belief that the VHA would benefit from a consistent approach to business planning. In Sinclair’s words, “The return on investment can be 100 times of what it cost in just one year to put that model in place.”
MARKETPLACE TOOLS FOR MODELING
For this workshop session on the RSMeans costing tool, the committee had asked the speaker to address the following questions, which he touched on throughout the course of his presentation:
Are there any reasonable standard models, or model structures, that have seen broad validation and acceptance by customers? How do you know what level of aggregation is “best” for a model: individual departments, groups of departments, or whole organizations? What factors do you consider in the selection of the appropriate tool? How do you weigh these factors, and what kind of trade-offs require more consideration?
Steve Plotner (Gordian) described the RSMeans tool, which provides asset-driven cost data for construction and maintenance functions. He then listed four major areas in which RSMeans could help the VHA with the development of facilities staffing models: (1) RSMeans data could assist with benchmarking of staffing efficiency against industry norms. (2) If facilities staffing is outsourced, RSMeans could serve as a contractual unit price basis or provide independent pricing validation. (3) RSMeans could be used to inform the organization’s programs and budgets, reducing the gap between budgeted and execution costs for facilities maintenance. (4) RSMeans could forecast costs over the entire life cycle of a facility, from planning and design through construction and commissioning, and into the operations phase, when preventive maintenance, repairs, replacements, and asset renewals are needed.
Plotner detailed the history and contents of RSMeans, which evolved from a handwritten book in 1943 to three formats that are available today: printed cost books, the CD-based Costworks software program, and the web-based RSMeans Online. RSMeans now has 20 different cost titles, including electrical, plumbing, mechanical, concrete and masonry, building construction, and facilities maintenance and repair. The RSMeans team has 12 full-time researchers and 10 full-time engineers, and the team spends about 22,000 hours each year researching construction costs.
The RSMeans database is fueled by actively monitored data points in several areas: material pricing, trade wage rates, equipment rental rates, productivity, and location factors. The database contains 55,000 unique material IDs, with material pricing determined by selected materials that serve as material price drivers. These drivers are researched in up to nine regions of the country to develop a national average material price. To obtain data on trade wage rates, the team tracks 35 trades in 314 locations in the United States. They also research up to 638 pieces of construction equipment across the country to come up with average rental costs. Plotner referred to productivity factors as “that secret sauce,” which takes into account how many people are needed to do a job and how long that job takes.
___________________
Plotner provided a detailed explanation of location factors, which help organizations calculate their location-specific cost from the national average cost. A team of four individuals works year-round to develop these factors. They start by shopping a subset of labor rates, materials costs, and equipment rentals in 96 locations across the country. These data are used to create the national average, and each location is then compared with the national average to obtain a ratio, representing the location factor. Algorithms in the database can interpolate between nearby locations using ZIP codes, ultimately resulting in more than 970 specific location factors for different areas of the country.
RSMeans also has cost data specific for facilities maintenance and repair, Plotner explained. These data include three different types of costs: preventative maintenance costs, maintenance and repair costs, and general maintenance costs, which include custodial services. He noted that some of the salient features of the maintenance and repair data include the use of the UNIFORMAT II alphanumeric numbering hierarchy,4 the approximate frequency of maintenance, the types of workers and equipment needed for each task, and labor hours. Preventive maintenance data, which are also based on the UNIFORMAT II numbering system, include specific tasks, labor hours, frequency, and annual/annualized rollups for each piece of equipment. Costs for maintenance tasks, such as landscape and custodial maintenance, can also be calculated with RSMeans, and these costs are calculated per unit of measure, per occurrence. Plotner provided data on lawn renovation as an example of landscape maintenance.
Plotner described a feature of RSMeans Online called the square foot estimator. Using this tool, the cost of an entire construction project can be estimated, based on location, footprint size and perimeter, structural frame, and façade, among other factors. This estimator also feeds into the RSMeans life-cycle cost estimator, which can then provide life-cycle costs for any desired term, illustrating the data in the form of a summary table or charts by the year. Data details include which equipment will need to be replaced and when, as well as costs for preventive maintenance, replacement, and repair over the chosen term.
Plotner provided an example of how RSMeans data can be used in an Excel-based preventive maintenance model (see Figure 4-1). For each facility, maintenance tasks, including quantity and unit of measure, are compiled. Data from RSMeans can be used to determine the annualized labor hours per unit, which will allow a calculation of the number of staff needed to complete the required tasks. RSMeans can also be used to determine both bare materials costs and the in-house costs that include procurement costs and labor-associated costs, including workers’ compensation and payroll taxes. For comparison, subcontractor costs for the same tasks can also be obtained from RSMeans. Plotner concluded by stressing that, as others have noted, data integrity is an essential part of any trustworthy model, and he reminded the workshop participants that models do not stay static but have to be constantly reviewed and improved.
Anselmi said that in his past experience with RSMeans, he found that the maintenance data did not go to the depth that was needed. He asked whether the RSMeans database currently contains information that addresses maintenance of advanced HVAC systems, medical gas systems, and other systems that are necessary in a health care setting. Plotner replied that the current database “probably will not go into depth in the health care arena. It will cover maybe 80 percent of it, but that missing 20, which is what you really need, we would have to develop in conjunction with you.” He provided the example of the Bureau of Indian Affairs, for which the RSMeans team developed new data, almost doubling the agency’s preventive maintenance database.
Paullin asked Plotner whether RSMeans contains data specific to health care facilities. Plotner replied that one of their 75 models is an outpatient surgery center, and Tony Edwards (Gordian), a colleague of Plotner, said that custom data also exist for other health facilities, including the Cleveland Clinic. Edwards explained: “There is an emergent health care practice where we are actually doing a lot of custom health care data. I think also from a builder standpoint, because of our engagements with many hospitals as well, some of that data exists to support health care.” Plotner concluded the discussion on the availability of health care data in RSMeans by explaining that if the VHA decided to contract with RSMeans, the team would develop new data for the VHA, as the company has done for other federal clients.
___________________
4 UNIFORMAT II is a standard for classifying building specifications, cost estimating, and cost analysis in the United States and Canada, maintained and published by the Construction Specifications Institute and Construction Specifications Canada.
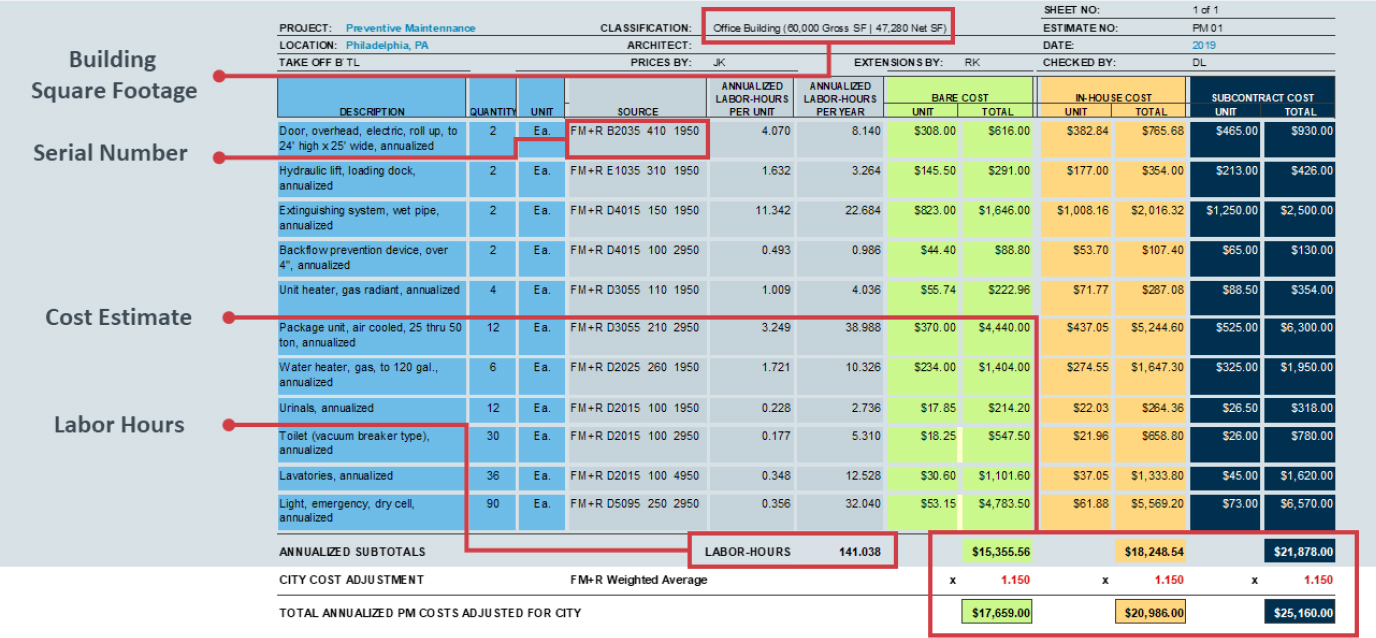
SOURCE: Plotner, S. (2019). Marketplace Tools for Modeling Panel. Presentation for the Workshop on Resourcing, Workforce Modeling, and Staffing (slide #20). Reprinted with permission.










