9
Visionary Statements on Potential Priorities to Address the Convergence
The final portion of the workshop in session four featured visionary statements on the potential priorities to break down silos and address the convergence of infectious diseases and noncommunicable diseases (NCDs). Speakers were asked to share insights on potential top priorities that would have a significant effect on the convergence, untapped opportunities that can be leveraged, and thoughts on how these efforts could synergize with existing global health initiatives, such as universal health coverage. This portion of the session was moderated by Mosa Moshabela, dean and head of the School of Nursing and Public Health at the University of KwaZulu-Natal, South Africa. Presentations on visionary statements were given by Jay Varma, senior advisor at the Africa Centres for Disease Control and Prevention; K. Srinath Reddy, president of the Public Health Foundation of India; and Patricia García, professor at the Cayetano Heredia University School of Public Health, Peru. The visionary statements were followed by a final synthesis discussion with the audience. The workshop concluded with closing remarks from Peter Daszak, president of EcoHealth Alliance.
ADAPTING PUBLIC HEALTH PRACTICE IN AFRICA TO A NEW UNDERSTANDING OF MICROBES AND HEALTH
Jay Varma, senior advisor at the Africa Centres for Disease Control and Prevention, presented a visionary statement that focused on integrated approaches and building the needed infrastructure to adapt a public health approach in Africa to address infectious diseases and NCDs. Varma
explained that the Africa Centres for Disease Control and Prevention—the new public health agency of the African Union, an intergovernmental agency that represents all 55 countries on the African continent—is dedicated to a vision of a fully integrated and prosperous Africa. The Africa Centres for Disease Control and Prevention was created in response to the health and disease transmission implications of the recently ratified continental free-trade agreement that ensures the free movement of goods, people, and services.
Varma stated that discussions of diseases or health challenges with policy makers should be linked to the concepts of universal health care and health security. The classical divide pins universal health care to NCDs and health security to infectious diseases, he noted, but it is possible to demonstrate how both types of diseases apply to both concepts. The concept of integration is a core component of the vision of the African Union, said Varma. It all extends from the colonial independence movement and the concept of Pan-Africanism to the need for a unified African voice, he added. This could mean a continental free-trade agreement, a single African passport (eventually), and a single air transport market. A component of this integration is the creation of institutions, including the Africa Centres for Disease Control and Prevention and the creation of a new African Medicines Agency that will be analogous to the U.S. Food and Drug Administration, Varma explained. The African Union is also committed to the creation of a National Public Health Institute in all 55 member states. Varma also highlighted the importance of infrastructure. Some areas in Africa have some of the fastest growing economies in the world, but infrastructure will need to be developed that permeates across countries in a way that promotes development across the continent, not just within individual countries, he noted.
Public Health Impact Pyramid
Varma presented an illustration of the public health impact pyramid (see Figure 9-1), as well as the ratio of population impact to individual effort at each level of the pyramid. He explained that the size of the population impact of interventions is greatest at the bottom of the pyramid and lowest at the top, while the individual effort needed to implement the intervention falls along an opposite gradient. For example, interventions that target socioeconomic factors through developmental, environmental, and structural changes may have the broadest population health impact while requiring the least amount of individual effort. At the next highest level are interventions to change the context to make individuals’ default decisions healthier. Such interventions include taxation or banning certain products, like trans fats. Long-lasting protective interventions delivered to individuals—such as vaccines—require more individual effort, both on the health system side as
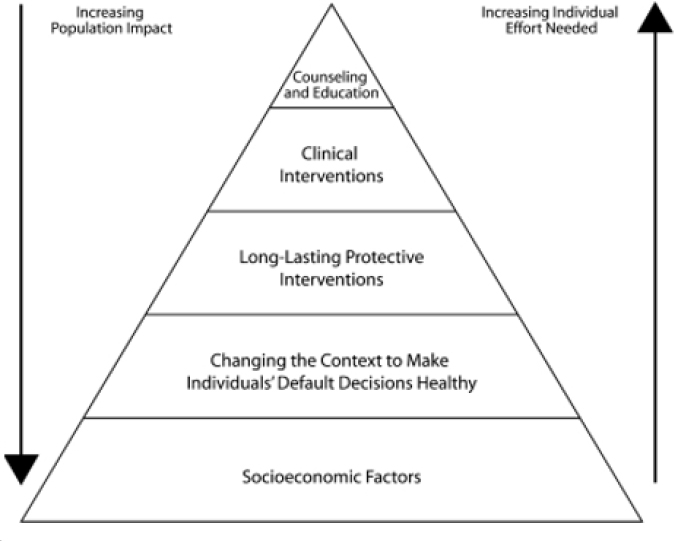
SOURCES: Varma presentation, June 12, 2019; Frieden, 2010.
well as the human side. At the second highest level of the pyramid are clinical interventions through effective models of care. However, the dilemma is that clinical interventions impact less of the population and require much more individual effort, he noted. At the top of the pyramid are individual-level interventions such as counseling and education. Varma said that in the public health field, efforts are directed toward working from the bottom to the top of the pyramid, prioritizing interventions that can have an impact across the broadest population level while requiring the least amount of effort at the individual level.
Applying the Public Health Pyramid to Integrating Infectious and Noncommunicable Disease Interventions
Varma used the public health pyramid to suggest ways to integrate interventions against both infectious diseases and NCDs. At the level of clinical intervention, chronic disease screening and control could be introduced into vertical infectious disease programs, like those for HIV and tuberculosis (TB). He noted that HIV programs are more likely to be well funded and have
the existing infrastructure to provide comprehensive clinical services to an individual. The challenge is that this strategy will impact a smaller proportion of the population relative to the tremendous amount of individual effort required at both the patient and the provider levels, he added.
At the level of long-lasting protective interventions, Varma suggested deploying vaccines that prevent cancer. He noted that one of the greatest strides at the intersection of chronic diseases and infectious diseases was the discovery that infectious diseases cause cancer. Today, however, the hepatitis B virus vaccine and human papillomavirus (HPV) vaccine are both severely underused, he said. For the hepatitis B virus vaccine, immunization at birth is important to effectively prevent perinatal transmission (Mele et al., 2001; Hepatitis B Foundation, 2019). Barriers to administration of the HPV vaccine include the age requirement as well as enduring stigma around sexual health and the prevention of sexually transmitted infections (Holman et al., 2014).
Next steps, he stated, are to consider the role of seasonal influenza vaccination, the prevention of cardiovascular morbidity, and the prevention of diabetic ketoacidosis. A further step is to consider medical products that can be used to prevent cancer. Varma also noted that hepatitis C can now be treated more easily than TB, which is an instructive example of how some diseases (e.g., hepatitis C and HIV) are prioritized over others. Significantly reducing liver cancer deaths will require closing the gap that persists between HIV and hepatitis C in the infectious disease world, he added. Varma said this is a clear, easy win to reduce deaths from liver cancer. Helicobacter pylori administration could also be used to treat and prevent gastric cancer at this level of the pyramid.
At the level of changing the context to make individuals’ default decisions healthy ones, Varma said that a primary aim is to ensure that universal health care is also high-quality care. This begins with patient safety as a subset of quality; a subset of patient safety is infection prevention (Varma, 2019). Efforts to create robust changes related to infection prevention are ongoing through advocacy for public health laws related to the standards and regulation of safety in health care facilities. Beyond the clear benefit for health security, this can also contribute to the longer-term benefit of infrastructure development. If it is possible to prevent infections and build an antimicrobial stewardship program, he said, then it should also be possible to build a patient safety program along the continuum of providing quality care. This is an organic way to create durable change in a health system that better manages both infectious and noninfectious diseases, he added.
Opportunities for Public Health Surveillance
Varma described strategies to improve public health through surveillance. Cancer registries are low-hanging fruit among surveillance opportunities in
many areas of Africa. Currently, cancer registries are underused across the continent, and the registries that do exist have low coverage, he explained. Furthermore, there is limited connection between the data being collected and national-level public health policies related to screening for malignancies, prevention of malignancies, and access to oncology treatments. Developing cancer registries can inform the assessment of the burden of disease, which can be used to build a case for the prevention of cancer through vaccines that target pathogens, he explained. This can also provide an entry point to the control and treatment of NCDs, he added.
Varma’s next suggestion to improve surveillance involves genomic intelligence. The Africa Centres for Disease Control and Prevention is working to build a continent-wide infrastructure for pathogen genomic intelligence, said Varma. This has the potential to inform clinical decision making, outbreak control, and vaccine design. This could also contribute to the architecture needed to integrate human genomics into medicine and inform the development of precision medicine. He added that this effort will require new human resources, including bioinformatics-informed epidemiologists and microbiologists.
A MULTIFACETED UNDERSTANDING OF THE CONVERGENCE
K. Srinath Reddy, president of the Public Health Foundation of India, opened his visionary statement by explaining that he is a cardiologist and an epidemiologist by training, but a public health advocate by passion. The Public Health Foundation of India aims to address the diversity of public health challenges that India faces across the spectrum of infectious diseases and NCDs—thus, convergence is a lived reality for Reddy. He reflected on how the message about the need for convergence could be communicated to the world at large. A first step is to convey that there is already compelling evidence of convergence, both across countries and within countries—not just convergence of infectious diseases and NCDs occurring in the same populations. There is a reversal in the social gradient to the extent that the poorest people, both across and within countries, are disproportionately affected. Thus, there is also a convergence in the domain of equity, he added.
Convergence and the Health Transition
Convergence is under way within communities, families, and individuals and across the life course, said Reddy. This makes the case for the long-neglected concept of life-course epidemiology and exposes how epidemiology has been studied in a segmented and fragmented fashion. It is now recognized that communicable diseases and NCDs can coexist in an individual, either at different points in time or at the same point in time
across the life course. The advent of microbiome research implores us to rethink the artificial distinction between microbes and humans. “What evolution has brought together, let no siloed science tear asunder,” he said. The health transition is shaping the manner and timing in which this convergence is manifesting, Reddy said, although the pace and progress may vary across continents. For instance, if Rwanda does not now have many of the traditional NCDs that pervade high-income and even middle-income countries, it is because Rwanda is at an earlier phase of health transition. He anticipated that the health transition will propel countries like Rwanda into the next phase, which calls for preemptive action against commercial, social, and other determinants to prevent some of those populations from acquiring and manifesting that risk. At the same time, it is necessary to deal with the reality of convergence as the health transition evolves.
In different populations across the world—and in rural and urban settings within the same countries—the health transition is happening at different paces, but the direction of transition is fairly clear, remarked Reddy. He quoted Rudolph Virchow’s question about the epidemic of typhus in Upper Silesia, “Do we not always find the diseases of the populous traceable to defects in society?” If diseases are the expression of individual life under unfavorable circumstances, he explained, then epidemics must be indicative of the masses. In Virchow’s time, typhus was related to poverty. Today, it is tobacco that is related to poverty, noted Reddy. Multimorbidities demonstrate that the convergence is manifesting in multiple ways—from clustered clinical presentations of people with diabetes and urinary tract infections, to clustered presentations of diabetes, HIV/AIDS, and TB. It is also clear that there are cross-linked pathogenic pathways, even when there is no direct assault of microbes that are causing NCDs, he added. These pathogenic pathways can trigger inflammation, which itself can become a systemic phenomenon that causes vascular damage, among other consequences. Reddy suggested that it is no longer tenable to use Koch’s postulates as the necessary criteria for linking a microbial assault with vascular damage and other noncommunicable conditions, given the discovery, for example, of common pathways of inflammation in thrombogenesis that are triggered by microbial infections.
Embracing the Complexity of Convergence
Reddy explained that as the scientific understanding of convergence progresses, it will become evident that the spectrum of science is reductionist in content, but holistic in context. Biology is influenced by beliefs and behaviors, which, in turn, are influenced by a multitude of social, economic, and environmental determinants. He quoted the naturalist John Muir’s observa-
tion that “When we try to pick out anything by itself, we find it hitched to everything else in the Universe.” Complexity is the reality of the world and of nature, he added. It is now recognized that in people with multiple coexistent conditions, multiple risk factors operate in concert.
All of the environmental exposures that occur during the course of an individual’s lifetime and the body’s own responses to those exposures constitute the exposome. It is the genome in the exposome that ultimately interacts to produce the disease. All of these factors need to be investigated and, where possible, acted upon, said Reddy. Fortunately, powerful tools are now available to integrate data from social sciences, environmental sciences, life sciences, and clinical registries. This provides an opportunity to integrate and identify all of the connections and the key action points at which some effect can be achieved early on.
Reddy maintained that in the move toward person-centered health care, community-centered public health, and people-centered public policy, convergence is not a matter of choice—it is an imperative—and complexity should not be a deterrent. He highlighted a stepwise approach to solutions, despite the barriers to transdisciplinarity that range from siloed funding streams to lack of credit for multidisciplinary authorship. Developing enlightened policy requires scientific credibility, financial feasibility, operational stability, and political viability, said Reddy. He explained that each of those aims requires different streams of research. Scientific credibility is based on biomedical, epidemiological, and clinical research; financial feasibility requires health economics to assist in evaluating cost-effectiveness and affordability, he said. Health systems research is needed to achieve operational stability, scalability, and sustainability. Political viability is founded on social science research to bring together policy makers, health professionals, the community, and the industry to support new policy. This effort requires a changing of mindsets that will be challenging to achieve, said Reddy.
It is easy to talk about transdisciplinary research, he noted, but to operationalize, it will require change in health education for all health professionals to produce individuals shaped by a transdisciplinary understanding. Health professionals will need keen cultural understanding and the ability to collaborate, Reddy said, even when they are developing depth in one area of research in which their expertise will qualify them as leaders. He mentioned the potential effect of dedicated funding streams that could be established by national or international funding agencies to bring together postdoctoral students from different disciplines to jointly address multidisciplinary research challenges and find solutions. Inculcating the culture of transdisciplinary research from an early stage will build researchers who believe in the concept, said Reddy.
Multidisciplinary and Systemic Convergent Action
With respect to health systems, Reddy observed that the United Nations’ Sustainable Development Goals and the push for universal health coverage provide a unifying platform to integrate health and prevention into primary health care and across the overall health system. But there is health beyond health care, he said, which will require multisectoral action in the areas of tobacco control and food systems in agriculture, for example. Empowering frontline health workers and engaging communities provide opportunities for improving health literacy at the primary care and community levels. Educating people about tobacco and appropriate nutrition, for example, can generate grassroots demand for a multisectoral policy response that politicians will have to heed, he noted.
Primary health care should not be considered merely to be a service channel, he said, but as a platform for actively engaging communities in the demand for policy change. Reddy added that addressing convergence will require bringing to the table multiple players who are already engaged in environmental and community work. This includes the message that these cross-sectoral partners are natural allies and that there are clear mutual benefits. A shift in mindset away from exclusively vertical programs has already occurred among funders, he noted. Large international funding agencies are now focusing on capacity building, health systems, and primary health care.
Potential Priorities for Convergent Action
In summary, Reddy outlined his five priorities for spurring continuous change and convergent actions:
- Strengthening primary health care
- Achieving universal health coverage
- Fostering community engagement
- Catalyzing demand for policy response
- Supporting multisectoral and transdisciplinary research
All of those priorities require forging wide-ranging partnerships across multiple stakeholders to build collaborations, he said. The arena of research extends from molecules to markets. The arenas of advocacy and action extend from risk factors to human rights. To that end, he redefined the concept of public–private partnership as “partnership for public purpose.” After defining the public purpose, the deliverables, and the accountability mechanisms, Reddy asserted that the public interest should ultimately set the agenda or it will create a laissez-faire system. Multiple partnerships could
be mobilized under this new definition of partnership for public purpose. Potential partnerships include partnerships between two individuals, partnerships between two private-sector entities, and partnerships between the government, private-sector entities, and nongovernmental organizations.
While local action should be emphasized, Reddy said, global efforts are also needed. In the past century, a sense of shared vulnerability to bioterrorism, pandemics, and other threats provided the impetus for global health. During this century, global health will need to gain momentum from shared values, equity, universal health coverage, and ensuring planetary health for our shared common future, he noted. To date, he stated:
Research has only been sampling limited sections of the global human family, primarily in high-income [settings]. Sampling the entire human family and exploring the vast diversity of gene–environmental interactions is an example of the huge potential benefits of going global.
Going global also presents the opportunity to share lessons from other health systems, other cultures, and other social organization models in order to advance efforts to contain both infectious diseases and NCDs. Many of the determinants of those diseases are transnational, he said, such as pandemics of emerging infectious diseases, tobacco use, environmental change, and commercial determinants of health. He concluded by emphasizing that while equity matters, local capacity building is also crucial. In the words of Miguel Torga, the Portuguese writer, “Universal is local without the walls.” Reddy concluded with a call for breaking down those walls through convergent action.
RETHINKING AND REFRAMING EFFORTS TO ADDRESS THE CONVERGENCE
Patricia García, professor at the Cayetano Heredia University School of Public Health, Peru, presented her visionary statement by highlighting five priorities to address the convergence:
- Research support
- Systems thinking
- Advanced methods and tools
- Public communication and health literacy
- Policy changes
García opened her presentation by reflecting on two influential people in her life. One was her professor in medical school, who encouraged her to
specialize in infectious diseases based on the presumption that eventually it would become clear that most health conditions were related in some way to viral or bacterial infections. The second was her grandmother, who lived to the age of 100 years and was adamant about taking care of one’s intestinal flora—a precursor to the current understanding of the microbiome.
Before presenting her five top priorities, García summarized her solution in a single sentence: “We need to undo all the things that we have been doing for years.” The process should start with training, she said, because the current system of medical education has created professional silos and overspecialization. She suggested rethinking the education system for health professionals to create a system that is more comprehensive and person centered. Similarly, the mindset of funders will need to shift from a focus on diseases to a focus on people. Broader efforts should focus on strengthening health services, rather than creating parallel systems—separate models should not be created for lower- and middle-income countries and for middle- and high-income countries, she noted. García emphasized prevention and strengthening both day-to-day and specialized services at all levels of care, from the community to specialized hospitals.
Research Support for the Study of Convergence
García’s first priority is to continue supporting research on the convergence of infectious disease and NCDs that takes into consideration life course, gender, ethnicity, and diverse environments. This includes a research focus on the influence of the maternal microbiota on infants (Dominguez-Bello, 2019). Gut bacteria cross-communicate with the neuroendocrine and immune systems to effect change in a wide range of social and affective behavior (Francis and Dominguez-Bello, 2019). The maternal microbiota is a determinant of the offspring’s cognitive development, behavior, and health (Francis and Dominguez-Bello, 2019). Perturbations in the maternal microbiota can alter maternal–infant bonding (Francis and Dominguez-Bello, 2019). In the early-life microbiota of an infant, antibiotics can induce changes that have long-lasting metabolic consequences in body fat distribution and weight gain (Gibson et al., 2015; Francis and Dominguez-Bello, 2019). Research is also emerging about the relationship between microbial biota and cancer (Vivarelli et al., 2019).
She noted that microbiotas vary among people living in different environments, which warrants further study in areas of the world that have not yet been sampled. Microbiota are not composed of bacteria, she added. For example, parasites can be part of the microbiota. She highlighted the emergence of associations between parasitic infections and chronic diseases (Blitz et al., 2018) and the known link between people with human T cell leukemia virus type 1 and parasitic diseases (Gonçalves et al., 2010). There
are also diseases in which parasites likely cause some type of dysregulation of mucosal immunity, she said. A study of women living in the Peruvian Amazon found that they have high rates of parasites, and those infected with HPV more rapidly develop cancer and have a worse response to treatment (Gravitt et al., 2016). She cited this as an example of the type of research into diverse environments that needs to be supported.
Systems Thinking in Research, Study Design, and Analysis
García’s second priority is to encourage more systems thinking in research and analysis to test the practical implementation of interventions. While basic science and academic research are necessary, the ultimate goal is to drive evidence-based policy actions. A shift in thinking will be needed to bring research into policies for prevention, surveillance and detection, control, and treatment. Funders tend to prefer randomized controlled trials, which are beneficial, but she said qualitative research and descriptive epidemiology within prespecified conceptual models warrant prioritization as well. She added that confining research will not help researchers understand all the complexities at hand.
Studying systems requires understanding the community context and all of the actors involved. She said because randomized trial research is carried out in sterile, controlled settings, the research output usually fails to become policy because reality is more much complex than the research environment. Systems-based research can be used to leverage cross-sectoral collaborations and break down silos among various stakeholders from research to practice, she continued. Actors in other sectors are not looking for randomized trial research. Policy makers, for example, are looking for cost-effectiveness analyses and community-based research about their constituents, she said.
Cutting-Edge Tools to Explore Links Between Infectious and Noncommunicable Diseases
García discussed the importance of developing cutting-edge methods and tools to explore links between infectious diseases and NCDs. She listed point-of-care diagnostics and user-initiated interventions to engage communities as part of the solution through self-testing, self-collection, and self-sampling. Better health information systems need to be developed, as well as better methods for analyzing big data, she added.
Improved Communication and Health Literacy
Better public and mass communication is García’s fourth priority. She said information about the convergence needs to be communicated—
through positive messages—to health professionals and the general public to disseminate current knowledge about the known and suspected associations between micro-organisms and chronic diseases and conditions. She added that health literacy efforts need to go further in clearly explaining to the public that microbes can cause chronic diseases, that the microbiota can be shaped by diet, and that there are trade-offs associated with using antibiotics.
Potential Priority Policy Changes
García’s final priority is to promote policy changes directed toward the integration of public health activities and health services for infectious diseases and NCDs as part of universal health coverage. The phrase associated burden is more apt than dual burden, she said, and the disease approach should be replaced with a person-centered approach supported by comprehensive health strategies. Convergent, comprehensive strategies for prevention, surveillance, and disease control should take into account overlapping high-risk populations that are in need of enhanced simultaneous surveillance for infectious diseases and NCDs, she said. This simultaneous surveillance will contribute to monitoring and measuring impact, she added.
These strategies could offer targeted, coordinated care delivered in innovative ways. She suggested investing in capacity building and promoting efficiencies in systems, while also managing expectations about potential cost savings. Providers need to be engaged in these policy changes to facilitate task sharing and task shifting when new activities arise, García stated; community engagement and empowerment are also needed. She suggested that the fight against corruption can begin at the community level, but progress should be measured to strengthen anticorruption efforts going forward.
FINAL SYNTHESIS DISCUSSION
Mosa Moshabela, dean and head of the School of Nursing and Public Health at the University of KwaZulu-Natal, South Africa, opened the floor for a final discussion. The topics of discussion focused on the role of establishing causality, communication and messaging strategies for relevant stakeholders, and furthering research on the microbiome and the exposome.
The Role of Establishing Causality
Moshabela asked García to comment about the need to establish evidence-based causality, given that real-world research is often criticized for not being robust in terms of establishing causality. García responded that she is challenging that notion and suggesting that research should be brought into the field, whether it is under the guise of implementation
research, integration science, or program science. Funders need to understand that a research ethos focused only on showing causality does not work in the real world, she said, because all of the other components of the systems have not yet been analyzed. To operationalize funding in the most cost-effective way and in a way that translates research into policy, she said, both quantitative and qualitative research are needed.
It is helpful to understand what people are thinking and why they behave the way they do, she added. Humans are so complex that successfully introducing any element into a human-based system is dependent on understanding and taking into account that complexity, she said.
Reddy remarked that causality is challenging because it cannot always be analyzed in a linear way. For NCDs, there are Bradford Hill criteria for causation, but construct validation can be used for more complex issues. If there is reasonable evidence of the ecological association of intake of external agents—such as secondhand tobacco smoke or sugar-sweetened beverages—with adverse health effects, then a precautionary principle can be applied and the evidence of the intervention can follow, he added.
Communication and Engagement with Policy Makers and Relevant Stakeholders
Peter Daszak, president of EcoHealth Alliance, asked the panelists how to simplify complex messages such that policy makers will understand and support this agenda. Varma replied that throughout his career, he has struggled to communicate not with the public, but with their representatives and decision makers at various levels. Even though there are ways to use science to communicate the direct linkages between the factor that is sought to be altered and the desired intervention or beneficial outcome, it is difficult to do so effectively without explicating the direct causal link and discussing correlation. In many settings, he said interventions to control sugar-sweetened beverages, for example, can come across as nanny state policy. In his experience, it is more effective to frame the intervention in terms of targeting a specific factor as an “enemy” that needs to be fought against. A challenge for the African Union, he added, is that it is an established deliberative body, but it does not yet have full institutional functioning capacity. It is relatively easy to pass declarations, but he noted the execution is not commensurate because supposedly binding commitments do not have tangible effects.
Reddy commented that the message communicated to policy makers could be that we do not have the luxury of dealing with infectious disease and NCD issues sequentially, particularly in a country like India. They need to be addressed simultaneously because both of them cause mortality, morbidity, and economic damage. Systems must be built to competently deal with both issues and their consequences, he noted. Reddy also commented
on the issue of choice versus policies perceived to be nanny state. Industry may push the importance of individual choice, but choices are often made on the basis of the information presented, he said—hence the importance of health literacy, so that choices are not shaped by aggressive marketing and peer pressure. Interventions to control the tobacco or alcohol industries could help to address this. He added that healthy choices, such as eating adequate fruits and vegetables, are also constrained by socioeconomic circumstances for many people. If the healthier choice is not made easier and affordable, he said, then the purported choice is actually a euphemism.
García remarked that messages need to be tailored for specific policy makers. Data can be helpful when they are presented in a simple way, especially in discussions about associations or correlations. Some policy makers will only be interested in potential cost savings, so working with an economist to create a cost-effectiveness analysis can bolster the communication strategy. She added that Peru is rolling out the process of labeling processed foods, which was achieved through using appropriate, consistent language about the cost savings created by consequent reductions in chronic disease. She said that human testimonies or stories can be powerful in gaining buy-in from policy makers, as well. Her final consideration was that the communication strategies be collaborative and engage with other partners. She illustrated that when she worked with mothers in communities on the benefits of HPV vaccination, it led to a grassroots campaign that filtered up and engaged female policy makers in government.
Varma commented on the power of generating public outrage in driving change. He suggested framing chronic diseases as a product of genetic fatalism or being “born that way,” or “being stuck in lifestyle choices.” If people believe that having a chronic condition is beyond their own control, as infectious diseases are, then he suggested they are more likely to demand that the government take action to protect them. García agreed and noted that people perceive infectious diseases as something that can be actively helped with medications. The association between infectious diseases and NCDs could be leveraged to promote preventive vaccines and technologies and garner public support, which will influence their policy makers to act. She reiterated that communication needs to be tailored for the audience, be it health providers, the general public, specific communities, or policy makers. There is also a role for international organizations and global health entities to support policy makers in shaping new policies or adjusting existing ones.
Reddy suggested identifying “prime movers” who need to be supported in terms of research, academia, and funding. Academia needs to articulate the need, he suggested, so that the funders who are entrenched in existing siloed funding streams will change their behaviors. Policy makers can bring about changes in the health system, but health system managers, planners, and patient groups also need to be actively engaged by health professionals.
Specifically, he said that health system managers will be the prime movers in the transition toward convergence at the service-delivery level. While the media can be a useful channel for communication, he said academics and civil society also have a role in correcting falsehoods (e.g., myths around vaccine safety) to ensure that they are not disseminated widely, while also holding the media accountable.
Microbiome and Exposome Research: Motivations and Implications
The need to expand the scope of surveillance beyond only diseases, for example, by using existing tools to carry out surveillance that capture information on socioeconomic contexts, was raised by Tolullah Oni, clinical senior research associate in the MRC Epidemiology Unit at the University of Cambridge. She asked why it seems easier to think about the microbiome than the exposome, and suggested thinking innovatively about surveillance approaches that incorporate both disease and the exposome. Additionally, she noted that rather than focusing on precision medicine, a push for precision public health may be more appropriate to support population health efforts.
García commented that some efforts are being made to measure exposomes in the form of social determinants of health. She suggested that measuring microbiomes may be more enticing because technology and interventions seem more marketable. Discussion of exposomes and social determinants of health involves complex societal issues that are beyond the capacity of many governments to address, especially in systems plagued by corruption and resource constraints, said García. Although microbiomes seem complicated, they are less complex to address than changing entrenched social determinants, such as poverty. The level of funding channeled toward infectious diseases, she added, could yield more benefits if it were used to fund interventions against poverty.
Daszak reflected that people are fundamentally drawn to a technological quick fix for problems, such as vaccines or antibiotics. Microbiome research is exciting because it is so complicated and so little understood, yet it holds such promise. He added that even the word exposome is more enticing than social determinants of health. Reddy noted the word exposome was coined in 2005 by Christopher Wild to include not only social determinants but also environmental determinants, toxic exposures, the body’s response, and epigenetics. He said that this calls for reconsidering previous assumptions about genetic determinism, given the number of potentially modifiable factors in the exposome.
Moshabela recalled four points from Knight’s plenary presentation: work on the microbiome requires a complex combination of food or diet, immunology, microbiology, and antibiotics. However, the overarching
focus is on how to manipulate the microbiome. Although a person can be empowered to manipulate the microbiome through dietary changes, it takes 6 to 12 months. It is feasible to empower people to manage their microbiomes autonomously, but it would be easier to manipulate the microbiome through some kind of technological intervention. Moshabela said that a tension lies in how to move from understanding the microbiome to developing medicalized interventions to manipulate it, while also developing interventions that can empower people to manipulate their own microbiomes. There is a need to carefully think about the quest for easy solutions compared to challenging solutions that may be more sustainable, he added.
Bridget Kelly, principal consultant of Burke Kelly Consulting, observed that the reasons for the excitement about the microbiome compared to the exposome may be caused by what “we think is safe and comfortable.” She suggested that while there may be an element of personal discomfort at play in discussion about collecting samples for microbiomes, she noted the profound discomfort and perception of risk to embrace the unknowns and challenges that need to be faced head on.
Varma admitted that the public health sphere often tries to avoid messages that appear overtly political, to the extent possible, but he said, “It is not so much to avoid the discomfort but to find a way to thread the needle a little more.” He explained that his own public health strategy when communicating with policy makers is to avoid talking about the benefits of health interventions and to focus on security from threats, opportunities to make or save money, and justice in alleviating inequities. Rather than avoiding discomfort, he clarified that he tries to frame the issues in ways that appeal to people across the spectrum, from genetic fatalists to those who attribute all outcomes to individual-level decisions.
Reddy said that communicating effectively with a policy maker also depends on the settings and the expectations. For example, policy makers may respond in one way to certain issues when they are acting in an individual capacity or in the context of limited potential for regional or national action. García pointed to conflicts of interest between providers who are delivering services and efforts to allow communities to gain power and autonomy. This is compounded by the history of paternalism toward communities. These tensions need to be resolved, she said, but that is unlikely to happen in a single generation. García said training the upcoming generation differently will help to create a different type of provider who is not uncomfortable in the ways Kelly described.
Building on the point about generational time frames, Oni introduced the concept of the Overton window from political science, describing it as a spectrum used to assess a desired goal on a scale of public acceptance that ranges from unthinkable, to radical, to acceptable, to plausible, to policy. He suggested that when people in public health think about an action, they
typically want to go directly from unthinkable to policy, and when people in public health think about impact, they are trained and conditioned by the funding structure to focus on policy relevance. Oni added that this paradigm could be applied to the microbiome and the exposome. Perhaps the microbiome is currently acceptable and moving toward policy, whereas the exposome is unthinkable or radical, and efforts should focus on moving it up to acceptable. Thinking about time frames can be useful when reflecting about interventions in terms of where they sit in current society in order to determine which interventions are more feasible.
Varma commented that his own experience is the converse of the Overton window—he finds himself advocating for change, but only being consulted when change is not feasible or affordable. He noted that over the past decade or so, the HIV movement has changed the paradigm in public health from the mindset of “only asking for a dollar because I might get a dollar” to demanding a sufficient amount of funding, even if that comes in a piecemeal fashion over time. He emphasized the importance of communication and engaging with communities and civil society to work toward rectifying the low expectations people have with respect to government-provided health services. Varma pointed to this issue as a root cause of infectious disease outbreaks, such as Ebola virus disease. He suggested establishing minimum common standards—for example, high-quality, safe, nutritious food—regardless of whether the motivation concerns the microbiome or standard thermogenesis that results in a healthy body. He concluded by calling for health care professionals and civil society groups to demand better quality of health services from their governments.
CLOSING REMARKS
Daszak provided the workshop’s closing remarks. He highlighted three lessons that he gleaned from discussions over the 1.5 days. Calling back to the blind people and the elephant metaphor from the second session, he suggested that it may not even be an elephant that the blind people are trying to grasp, but something much more difficult to understand—convergence presents a complex, tangled web of information and ideas. He suggested trying to grasp nuggets of value that can be used to simplify the message and communicate more effectively with policy makers. The second lesson is that many people in the infectious disease space and in the NCD space may actually be self-selecting their respective silos, which are reinforced through different belief systems and behaviors, separate journals, distinct funding streams, and disparate research methods. This adds an additional layer of difficulty in trying to break down the silos, he said.
Finally, for Daszak the key lesson is that there is a massive inequity problem, yet convincing policy makers and politicians about investing
in NCDs is enormously challenging. Given that the sense of urgency and concern over pandemics generates huge amounts of attention and money, he suggested finding ways to make NCD-related issues more urgent and more directly applicable to decision makers and funders. This might involve borrowing language from the effective global health security agenda, he noted. For example, the concept of “NCD security” could be used to frame the threats related to political instability and security issues that arise in situations where an entire country or population has a large chronic disease burden that is compounded by poverty and hunger. He concluded by emphasizing the importance of improving public health systems to tackle both infectious diseases and NCDs from the local to national to global levels.


















