9
Interventions
Varied approaches have been used to mitigate the negative health impacts of social isolation and loneliness. This chapter first describes a number of large-scale efforts to review the effectiveness of interventions for social isolation or loneliness, with a focus on several approaches that are specific to health care settings. Next, the role of technology is considered, both as an intervention tool and a factor that exacerbates or contributes to social isolation and loneliness. Then, ethical issues pertaining to interventions are discussed and potential sources of funding for interventions are explored. The committee notes that educational approaches and awareness campaigns may be considered a type of intervention; however, these topics are covered in Chapter 8. Finally, the committee suggests ways to reframe interventions using a public health approach. Given the complexity of the terminology used in relation to social isolation and loneliness, a reminder of key definitions is provided in Box 9-1.
LARGE-SCALE REVIEWS OF INTERVENTIONS
Several studies and projects have examined interventions intended to ameliorate social isolation or loneliness specifically, or their associated health impacts; these interventions have generally not been limited to health care providers or settings (see Table 9-1). An extensive review of all interventions for social isolation and loneliness outside of the health care setting (e.g., efforts to create intergenerational communities) is beyond the scope of this report. However, the committee discusses these large-scale reviews here
for two reasons: first, most of these large-scale reviews do not separate interventions by setting and therefore the committee wanted to capture as much evidence on the effectiveness of interventions as possible; second, health care professionals and others will likely need to be aware of efforts in the community for possible referral.
Most of these large-scale reviews note the poor quality of the evidence concerning the effectiveness of such interventions. In particular, the authors of these reviews note several weaknesses in the study designs, including a lack of long-term follow-up, a limited range of ages included among “older adults,” variability in the definitions of social isolation and loneliness, variability in the measurement tools and outcome measures used, and small sample sizes. Several studies reported that successful interventions tended to have certain key features, including the active participation of older adults, having an educational focus, and using a group-based approach.
In addition to reviews in the published literature, there have been other efforts to assess interventions for social isolation and loneliness among older adults (again, not limited to health care settings). The committee summarizes several of these efforts other than the studies listed in Table 9-1 in the following sections.
TABLE 9-1 Published Reviews of Interventions for Social Isolation and Loneliness
| Author | Focus | Number of Studies | Key Findings | Recommendations |
|---|---|---|---|---|
| Findlay (2003) | Social isolation in older adults | 17 |
|
|
| Cattan et al. (2005) | Social isolation and loneliness in older adults | 30 |
|
|
| Dickens et al. (2011) | Social isolation in older adults | 32 |
|
|
| Masi et al. (2011) | Loneliness in all ages | 50 |
|
|
| Author | Focus | Number of Studies | Key Findings | Recommendations |
|---|---|---|---|---|
| Centre for Policy on Ageing (2014) | Loneliness in all ages | 72 |
|
— |
| Cohen-Mansfield and Perach (2015) | Loneliness in older adults | 34 |
|
— |
| Gardiner et al. (2018) | Social isolation and loneliness in older adults | 38 |
|
|
AARP Foundation Catalog Project
The AARP Foundation commissioned Jessica Retrum of Metropolitan State University of Denver to do research toward the ultimate goal of creating “an interactive tool designed to serve as a resource catalog for evidence-based or promising practices to address loneliness and social isolation in older adults.”1 In her analysis, Retrum examined both published and unpublished interventions. Unpublished interventions were collected by outreach to groups that had previously contacted the AARP Foundation. Tables 9-2 through 9-5 describe the interventions evaluated in this review, categorized by target population, intervention level, intervention type, and the rigor of the evaluation in order to give a sense of the breadth of these interventions.
Retrum found that the most effective interventions included
- Specific targeting of socially isolated individuals;
- A multi-systemic approach;
- Active participation of the older adults; and
- Having a sound theoretical basis.2
Furthermore, Retrum noted3 the following persistent challenges to the evaluation of interventions for social isolation and loneliness:
- A limited number of studies quantifying the impact of interventions;
- A shortage of randomized controlled trials (RCTs) and quasi-experimental studies;
- Variability in the concepts being measured;
- A targeting of either the general community or individuals who are “easy to find”; and
- Difficulty in recruiting those who are extremely isolated or lonely.
The committee noted that many of these studies, both published and unpublished, did not indicate that they had used a validated tool (as described in Chapter 6). Rather, many of these interventions assessed impact through qualitative interviews, surveys, and internally designed measurement tools.
___________________
1 Presentation by Jessica Retrum to the committee on February 27, 2019.
2 Retrum, J. 2017. PowerPoint presentation—A review of interventions: Addressing social isolation in older adults. In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
3 Retrum, J. 2017. PowerPoint presentation—A review of interventions: Addressing social isolation in older adults. In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
TABLE 9-2 Target Population
| Catalog | Totals | General Older Population | Health-Related Issue/Condition | Vulnerable Group | Residents in a Setting |
|---|---|---|---|---|---|
| Literature Review Interventions | 92 | 37 | 7 | 31 | 17 |
| Unpublished Interventions | 48 | 13 | 10 | 22 | 3 |
SOURCES: Retrum, 2017; American Public Health Association (APHA) data (used with permission from APHA). In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
TABLE 9-3 Intervention Level
| Catalog | Totals | One-on-One | Group | Community |
|---|---|---|---|---|
| Literature Review Interventions | 92 | 27 | 41 | 24 |
| Unpublished Interventions | 48 | 31 | 13 | 3 |
SOURCES: Retrum, 2017; American Public Health Association (APHA) data (used with permission from APHA). In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
TABLE 9-4 Intervention Type
| Catalog | Totals | Intentionally Addresses | General Social Activity/Engagement | Environment Change/New Resource (e.g., transportation, neighborhood safety) |
|---|---|---|---|---|
| Literature Review Interventions | 92 | 41 | 55 | 39 |
| Unpublished Interventions | 48 | 27 | 21 | 12 |
SOURCES: Retrum, 2017; American Public Health Association (APHA) data (used with permission from APHA). In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
TABLE 9-5 Rigor of Evaluation
| Catalog | Totals | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|---|
| Literature Review Interventions | 92 | 0 | 18 | 22 | 31 | 21 |
| Unpublished Interventions | 48 | 10 | 4 | 30 | 4 | 0 |
NOTE: On a scale of 1 to 5, 1 = lowest, 5 = highest.
SOURCES: Retrum, 2017; American Public Health Association (APHA) data (used with permission from APHA). In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
Agency for Healthcare Research and Quality Rapid Review
In 2019 the Agency for Healthcare Research and Quality (AHRQ) conducted a review to “rapidly evaluate the effect of interventions targeting social isolation/loneliness in community-dwelling older adults (60 years and older) on outcomes of social isolation/loneliness, health, and health care utilization” (Veazie et al., 2019, p. ii). The researchers focused on 16 individual studies, but only half of these studies were deemed to be of good or fair quality. Ultimately, the researchers found limited evidence that the interventions significantly affected health outcomes. Two studies related to health services access interventions were found to be of poor quality. The researchers noted several challenges overall with the evidence base, including differences in constructs and measures, the overall poor quality of the studies (based on their quality assessments of study design), short follow-up periods, a lack of measurement of health care utilization or potential harms, and a failure to control for confounders. The researchers also noted that most studies were conducted outside of the United States. The report includes several recommendations for improving the quality of the evidence base, including
- “Collaborate with health systems, payers, and patient advocacy groups to agree upon standardized definitions and measures for social isolation and loneliness. As mentioned previously, social isolation is currently measured with myriad constructs and measures, which complicates the ability to draw conclusions between social isolation and health outcomes” (Veazie et al., 2019, p. 14).
- “Recruit and report results for a diverse population . . . to determine important population differences” (Veazie et al., 2019, p. 15).
Campaign to End Loneliness
The United Kingdom’s Campaign to End Loneliness (see more in Chapter 8) noted that “in recent years there have been a number of attempts to bring together what is known about the effectiveness of loneliness interventions, however the conclusions drawn have been partial, and often contradictory” (Jopling, 2015, p. 7). As a result, the campaign assembled an expert panel to hear about promising loneliness interventions happening in communities that may not have been captured in the published literature. While conceding that they found “a lack of high-quality evidence to demonstrate the impact of different interventions on loneliness,” the members of the expert panel suggested that “evidence exists on a spectrum, and even where the evidence is of a lower quality it can be an important step in the development of a firmer understanding of what works” (p. 8). The expert panel identified a variety of approaches that held the most promise, grouping them into four types of interventions: foundation services, direct interventions,
gateway services, and structural enablers. However, most of these approaches have little evidence to support their effectiveness.
Foundation Services
The campaign describes foundation services as the first steps “coming before and providing a way into the more commonly recognized loneliness interventions” (Jopling, 2015, p. 9) and focus on three main challenges surrounding the uptake and effectiveness of interventions. First, reaching individuals includes using data to identify individuals at high risk; training individuals in a community to recognize signs of loneliness, make referrals, and provide support; and linking interventions to health care. (See Chapter 7 for more on the role of the health care system.) Second, understanding the nature of an individual’s loneliness and developing a personalized response includes guided discussions in which the individual’s circumstances, needs, and wishes are identified. One key factor is the individual’s trust in the person asking questions. Finally, supporting lonely individuals to access appropriate services includes providing links to a “trusted buddy or mentor” (Jopling, 2015). The expert panel felt the most effective approaches were framed as “holistic and person-centred services, aimed at promoting healthy and active ageing, building resilience and supporting independence” that could be tailored to address loneliness (Jopling, 2015, p. 12). The expert panel recognized the lack of a robust evidence base for the effectiveness of these approaches and suggested that these approaches warranted further study.
Direct Interventions
While the expert panel preferred more “holistic approaches,” they also considered interventions that seek to address loneliness directly. These include “supporting individuals to reconnect with and/or maintain existing relationships, fostering and enabling new connections, and helping people to change their thinking about their social connections” (Jopling, 2015, p. 25). The report notes,
It is clear the vast majority of loneliness interventions currently available seek to reduce loneliness by increasing the quantity and quality of relationships, and most do this by supporting individuals to develop new relationships. Most experts believed that these kinds of interventions were effective in tackling loneliness, but few held up specific examples as showing significant promise over others. Instead they argued that any and all such interventions could be helpful if they were chosen by the older person and well-suited to their needs (hence the importance of the foundation services). Many experts talked about the need for communities to offer a menu of such approaches. (Jopling, 2015, p. 10)
Experts varied in their opinions about whether group interventions or one-on-one approaches were more effective. The experts agreed that the most effective
direct group-based interventions target a specific group, focus on a shared interest (or on education), and include the older individuals in the planning process. They also felt that some people had significant barriers to making connections, and so, in spite of the lack of evidence, they recognized the importance of one-on-one approaches such as “befriending.”
Gateway Services
Gateway services are services such as transportation and technology that can affect social connection. In particular, the lack of access to such services could also impede the effectiveness of broader interventions. (See section later in this chapter on access to technology.)
Structural Enablers
Structural enablers are defined by the campaign as approaches that consider the environmental factors needed within communities to help reduce loneliness. These approaches are often used in conjunction with other interventions and include working with an asset-based community development approach (wherein the intervention identifies and takes advantages of community assets instead of identifying community needs), promoting volunteerism, and using age-friendly approaches (see more on age-friendly health systems later in this chapter).
TYPES OF INTERVENTIONS RELEVANT TO THE HEALTH CARE SYSTEM
Although the terms “treatment” and “intervention” are often used synonymously, they actually refer to different things. An individual suffering from an illness or disease receives treatment from a health care provider to mitigate the disease and its symptoms. Interventions, on the other hand, are designed to improve health status or encourage behavior change and are applied in the larger community by public health authorities (WHO, 2019b). While only a few treatments have been suggested to mitigate social isolation or loneliness, a variety of interventions targeting isolation and loneliness have been proposed.
Direct interventions are those that explicitly target social isolation, loneliness, or related social concepts. Direct interventions can fall into one of several categories: changing cognition, social skills training and psychoeducation, supported socialization, and wider community groups that create a broader sense of social integration (Mann et al., 2017). Outside of the health care system, these types of interventions often include one-on-one befriending approaches in which volunteers reach out through phone calls to individuals identified as being socially isolated or lonely. Within the health care system, this may include reaching out to individuals identified as being at risk for social isolation or loneliness in order to
connect them to needed services. Alternatively, interventions may include convening groups of at-risk individuals, in part to provide opportunities for social interaction. However, these types of approaches do not necessarily help individuals develop high-quality relationships, and lonely people in particular may withdraw, for example, due to an unconscious predisposition or hypervigilance to social threat (Caciopppo et al., 2015a,b).
Indirect interventions are those that do not specifically aim to mitigate isolation or loneliness but may nonetheless have significant effects on an individual’s perceived or objective isolation (Mann et al., 2017). For example, a physician may recommend hearing aids to assist an individual with impaired hearing; as a result, the individual may find it easier to interact in social environments and make connections with others, thereby reducing social isolation and loneliness. Similarly, participation in an exercise program for health may lead to reductions in social isolation or loneliness due to the social nature of the program rather than the exercise itself.
The following sections describe several types of interventions that aim to address social isolation or loneliness that are particularly relevant for the health care system.
Social Prescribing
No agreed-upon definition of social prescribing currently exists, though it is widely accepted that social prescribing helps patients access non-clinical sources of support, which are often provided by the community sector (Moffatt et al., 2017). Social prescribing has been defined as a “non-medical referral, or linking service, to help people identify their social needs and develop ‘well-being’ action plans to promote, establish, or re-establish integration and support in their communities, with the aim of improving personal well-being” (Carnes et al., 2017, p. 2). While community-based organizations have traditionally employed social prescribing as a way to help support individuals in their communities, social prescribing has been suggested as a way for health care practitioners to respond to isolation and loneliness in their patients. In her comments to this committee in 2018, Helen Stokes-Lampard, the chair of the Royal College of General Practitioners in the United Kingdom, described social prescribing as “a fancy name for what good doctors have always done, which is navigate our patients towards other resources outside of the health care sector that can help them.”4 Community-based organizations have long used this approach. For the purposes of this report, social prescribing will refer to the steps that health care providers can take to link patients with existing social services programs.
___________________
4 Video presentation by Helen Stokes-Lampard to the committee. In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
Connecting people with volunteer organizations and community groups has the potential to affect health and well-being both directly (e.g., lowering stress) and indirectly (e.g., improving access to social services) and may be seen as a way of extending primary care (South et al., 2008). Social prescribing attempts to prevent worsening health by commissioning secondary services that can help alleviate social concerns that affect health (e.g., food or housing insecurity), thereby reducing the costly interventions provided in specialist or inpatient settings (Dayson and Bashir, 2014).
Various interventions to mitigate the negative effects of isolation and loneliness fall within the realm of the community sector. Community-based groups such as social welfare systems, community organizations, religious groups, and government groups may be natural partners for the health care system when it comes to addressing social isolation and loneliness. Because social prescribing is tailored to existing voluntary and community-sector-led programs, it is believed to result in better social and clinical outcomes for people with chronic conditions and their caretakers, a more cost-efficient way to use health and social care5 resources, and a wider and more diverse and responsive local provider base (Dayson and Bashir, 2014). However, despite the promising nature of many community-based programs, this type of support often remains underused due to the weak or nonexistent link between health care practitioners and community-based services (South et al., 2008).
Different models of social prescribing interventions are presented in Box 9-2. Little evidence exists concerning the results of social prescribing interventions on social isolation and loneliness, and what evidence does exist is mixed (Moffatt et al., 2017). However, social prescribing interventions do have a number of promising features, including that they are long-term in nature, they address the existence of mental and physical comorbidities and social isolation simultaneously, they target specific groups (e.g., women, caretakers, or people with diabetes), they involve affected individuals in the intervention design process, and they address related socioeconomic issues (Centre for Policy on Ageing, 2014; Moffatt et al., 2017; Polley et al., 2016; see Figure 9-1).
One social prescribing tool tested in the United Kingdom, the Patient-Led Assessment for Network Support (PLANS), attempted to consolidate up-to-date information about health-relevant local resources into one website for people living with chronic health conditions (Blickem et al., 2013). The conceptual basis of PLANS was the notion that the needs of people with chronic health conditions cannot be adequately met through small targeted interventions that are not integrated into everyday life. The website included a self-assessment questionnaire, the results of which provided users with a tailored set of social and health resources available in the community. The resources were grouped into the areas of providing relevant health information, well-being (time spent doing meaningful and enjoyable things),
___________________
5 Social care refers to “services that address health-related social risk factors and social needs” (NASEM, 2019, p. 1).
practical support (help with every day, independent living), and services related to diet and exercise (Blickem et al., 2013).
Another example of a social prescribing system was piloted in Rotherham, United Kingdom, from 2012 to 2014, with the aim of increasing the capacity of general practitioners to meet the non-clinical needs of patients with long-term conditions. The pilot employed a team of voluntary and community sector advisors who received referrals from general practitioners, completed an assessment of referred individuals to identify their needs, and then linked
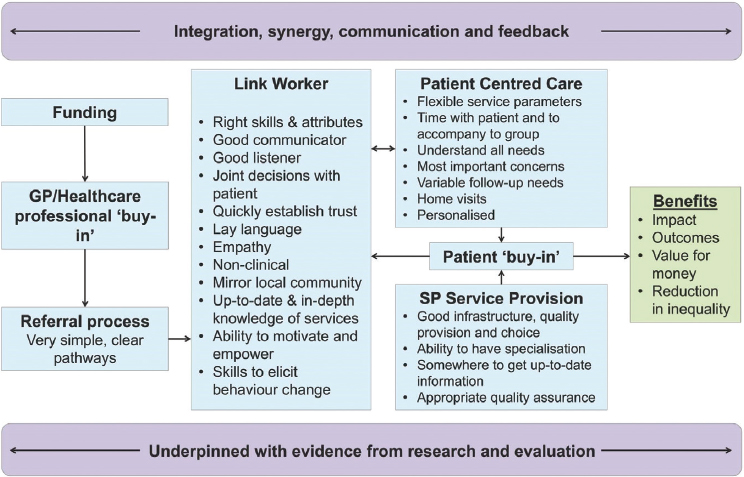
NOTE: GP = general practitioner; SP = social prescribing.
SOURCE: Polley et al., 2016.
individuals with appropriate social services. Referrals were made to a variety of social service providers, and the services addressing isolation or loneliness included befriending services, group activity programs, home visits, and group therapy sessions. An analysis of the pilot found that among the patients who received social prescribing services, inpatient admissions were reduced as much as 21 percent and accident and emergency attendance were reduced by as much as 20 percent (Dayson and Bashir, 2014). However, the sample size and length of the pilot were both small, so these results were not statistically significant.
Support Groups and Group Membership
In general, peer support groups, such as those for individuals with a common illness or condition, have proved to be of value. For social isolation and loneliness, group interventions may be aimed directly at those who are socially isolated or lonely. One approach is to provide guidance for improving social skills (Masi et al., 2011). For example, a “friendship enrichment program” in the Netherlands (that included training in skills relevant to friendship), which was aimed at women aged 55 and older, resulted in 63 percent of the participants reporting having made new friends through social and education activities (compared to 33 percent among women who did not participate in the program, but were interested in improving their friendships) (Martina and Stevens, 2007). However, the execution of social skills may be complicated by issues of performance anxiety
(Knowles et al., 2015). Support groups may also be directed at people who share common underlying causes of social isolation and loneliness, such as bereavement or widowhood (Chow et al., 2018; Stewart et al., 2001).
On the other hand, the reduction of social isolation or loneliness may result from an individual’s participation in group activities aimed at other purposes, such as education, volunteerism, or health promotion activities. For example, a study of SilverSneakers®,6 a fitness program for older adults, found that “membership directly increased physical activity and self-rated health, directly decreased social isolation, and indirectly decreased loneliness” (Brady et al., 2020, p. 301). A study of the “hidden elderly” in Hong Kong (defined as “older adults who are socially isolated and refuse social participation”) found that participation in a tai chi qigong program resulted in improvement in loneliness (as measured by the de Jong Gierveld Loneliness Scale).7 Key elements of the program included the training of community elders to act as “health ambassadors” of the project; these individuals lived near the hidden elderly and helped to create a sense of neighborhood and peer-to-peer relationships. A clinical trial, Leveraging Exercise to Age in Place (LEAP),8 is now under way to evaluate the impact of a participation in a community exercise program on social isolation. The LEAP study plans to evaluate changes in the Duke Social Support Index at 26 weeks after enrollment. However, a recent AHRQ rapid review (discussed earlier in this chapter) states
Physical activity interventions to reduce social isolation showed the most promise at improving the health of older adults; however, effects were inconsistent and short-term. (Veazie et al., 2019, p. ii)
Cognitive Behavioral Therapy and Mindfulness
The ways in which humans think and perceive involve both conscious and unconscious mechanisms. As a result, loneliness can generate a vicious cycle in which lonely people withdraw further because they perceive social interactions as negative or unfriendly. Hawkley et al. (2007) found that lonely individuals perceive greater negativity in social interactions than do non-lonely individuals and that lonely individuals perform more poorly on tests of executive functioning than non-lonely individuals (Cacioppo and Hawkley, 2009). Loneliness is also associated with hypervigilance for social threat9 (Cacioppo et al., 2015b). Taken together, biased
___________________
6 For more information on SilverSneakers®, see www.silversneakers.com (accessed November 14, 2019).
7 See https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5221552 (accessed November 14, 2019).
8 See https://clinicaltrials.gov/ct2/show/NCT03624049 (accessed November 14, 2019).
9 Hypervigilance to social threats is “an assumption in line with the evolutionary model of loneliness that indicates feeling socially isolated (or on the social perimeter) leads to increased attention and surveillance of the social world and an unwitting focus on self-preservation” (Cacioppo et al., 2016, p. 138).
perceptions and hypervigilance toward negativity may cause lonely individuals to unconsciously withdraw from social connections, even though they may consciously desire to connect with others. This reaction creates problems in particular when lonely individuals attempt to connect with others but perceive the interactions negatively and become discouraged, leading to a vicious cycle of loneliness and withdrawal.
Cognitive Behavioral Therapy
Cognitive behavioral therapy (CBT) is a type of psychotherapy that is used to help patients deal with a variety of issues ranging from more serious mental health disorders such as depression and posttraumatic stress disorder to day-today stressors and anxieties (Mayo Clinic, 2019). The goal of CBT is to teach individuals to identify their own faulty perceptions and irrational beliefs in order to approach and respond to challenging or stressful situations in a more clearheaded and effective way (McWhirter, 1990). By challenging automatic and negative thought patterns, CBT may be useful in helping lonely individuals reframe the way they think about their relationships, their assumptions about others’ views, or their expectations of success at overcoming loneliness (Mann et al., 2017). CBT has been found effective in addressing social anxiety disorder, insomnia, and unipolar depression (Butler et al., 2006; Edinger et al., 2001; Gress et al., 2008; Heimberg, 2002; Koszycki et al., 2007).
Few CBT-based interventions for loneliness or isolation have been tested in RCTs, and those that have been tested through RCTs have found mixed results. Mann and colleagues (2017) identified 10 published RCTs on cognitive approaches to improving loneliness or related concepts (e.g., social support, social network, social isolation) in people with mental health problems. Of the interventions considered, most therapies showed no effect on loneliness; however, two online CBT interventions for individuals suffering from depression were found to be successful at decreasing depressed mood and loneliness at 12-month follow-up (Saulsberry et al., 2013). While there is limited evidence of the effectiveness of CBT in mitigating social isolation and loneliness, many consider CBT to be a promising path forward (Mann et al., 2017).
Interpersonal Psychotherapy
CBT and interpersonal psychotherapy are both recognized as being “empirically-based psychotherapeutic interventions for mood disorders,” and “both are diagnosis-targeted, time-limited, present-focused treatments that encourage the patient to regain control of mood and functioning” (Markowitz and Weissman, 2004, p. 136). Interpersonal psychotherapy was originally developed as a treatment for depression (Cuijpers et al., 2011; De Mello et al., 2005). Interpersonal psychotherapy differs from CBT in that its focus is on maladaptive thinking specifically related to interpersonal relationships.
Interpersonal psychotherapy for depression focuses on two principles: viewing depression as a medical illness (not the fault of the patient) and making the connection between mood and triggering life events, such as bereavement (Markowitz and Weissman, 2004). While interpersonal therapy has not been extensively studied as an intervention specifically for social isolation or loneliness, its focus on maladaptive thinking and interpersonal relationships could be an approach to explore.
Mindfulness
Mindfulness, a way of being in which an individual maintains openness, patience, and acceptance while focusing on life situations in a non-judgmental way, has also been suggested as a way to mitigate the negative effects of isolation and loneliness (Gilmartin et al., 2017). Lindsay and colleagues (2019) conducted an RCT in which smartphone-based training was used to train participants in mindfulness techniques of awareness and acceptance for 2 weeks. The study found that individuals who received mindfulness training reported a 22 percent reduction in daily loneliness compared with the control group; thus, mindfulness training may be a promising way to mitigate the subjective risk factors associated with loneliness.
Pharmaceutical Interventions
Currently, nearly all interventions that have been proposed to treat isolation and loneliness are behavioral or psychological in nature. However, the interventions that focus solely on increasing the time spent socializing or increasing the number of social contacts may be greatly hindered by lonely individuals’ negatively biased perceptions and tendency toward interacting defensively with others. To boost the possible success of behavioral interventions, adjunctive treatments or therapies that target the biological underpinnings of biased cognition have been suggested as a potential tool. Adjunctive therapy is a form of treatment used in tandem with a primary treatment with the goal of assisting the primary therapy (NCI, 2011). In theory, pharmaceuticals could be used to minimize some of the negative behavioral effects of social isolation and loneliness (e.g., anxiety, fear), allowing individuals to maximize the satisfaction gained from their social interactions and building relationships with others, which in turn may increase the success of behavioral therapies (e.g., CBT). However, consideration is needed for whether decreasing symptoms of loneliness, for example, might mitigate motivation to increase human connection, and thereby lead to increased isolation.
Research in animal models suggests that behavioral or psychological interventions for isolation and loneliness may benefit from adjunctive biological treatments that target the underlying neurobiology. This includes the potential use of selective serotonin reuptake inhibitors (e.g., fluoxetine), neurosteroids (e.g., allopregnenolone), or oxytocin (Cacioppo et al., 2015b). Fluoxetine has been
associated with improving behaviors related to anxiety and fear (Cacioppo et al., 2015b; Mayo-Wilson et al., 2014; Pinna, 2010). In animal models, isolation of the animals has been associated with a decrease in the concentration in the brain of pregnenolone (Serra et al., 2000), a hormone that has been associated with memory enhancement (Vallée et al., 2001). In humans pregnenolone has been shown to improve depressive symptoms in individuals with bipolar disorder (Brown et al., 2014), though evidence of its effects on memory is contradictory (Vallée et al., 2001). The use of pregnenolone for loneliness is currently in a phase II clinical trial (NIH, 2016). Oxytocin is associated with social affiliation, and its use in animal models suggests it could mitigate the harmful effects of social isolation (Carter et al., 2008; Grippo et al., 2009, 2012; Young et al., 2014). The use of oxytocin in humans has been suggested to promote positive social behaviors, but the evidence for its use is mixed, and more research is needed about which individuals might benefit the most (Bartz et al., 2011; Cacioppo et al., 2015b).
Interventions That Target Social Determinants of Health Broadly
Social determinants of health are often interconnected, and therefore social isolation and loneliness may be addressed through efforts to address the social determinants of health more holistically. For example, many Medicaid programs are moving toward screening for social determinants of health and connecting individuals to needed supports (Manatt Health, 2019). An example of a program targeting the social determinants of health broadly is AIRnyc. This community-based organization uses community health workers to link patients to services in order to address social determinants related to diabetes prevention and management, asthma, hypertension, aging in place, behavioral health, maternal health, and substance use disorder at the individual and household levels.10 (See Chapter 7 for more on the role of the health care system in addressing the social determinants of health. See later in this chapter for more on financing interventions for social isolation and loneliness through existing programs directed at the social determinants of health.)
Centene, one of the nation’s largest Medicaid managed care organizations, serves more than 14.5 million managed care members across 32 states. The organization has committed itself to providing “access to high-quality health care, innovative programs, and a wide range of health solutions that help families and individuals get well, stay well, and be well” (Centene, 2019). Centene is in the process of developing new strategies to address the social determinants of health broadly, which could include social isolation and loneliness, through efforts to address factors known to be at the core of the health and well-being of individuals. Centene envisions these long-term efforts as a way to create sustainable funding for programs that will address issues such as linguistic and cultural differences between the social sector (e.g., community benefit organizations) and the health
___________________
10 For more information, see https://www.air-nyc.org (accessed August 3, 2019).
sector (e.g., hospitals and payers organizations). Centene envisions a scalable program with broad impact that is guided by a standard set of protocols, procedures, and analytics that can be individualized to different markets. There has not yet been a formal evaluation of this program.
Interventions That Target Social Isolation and Loneliness in the Health Care System
A handful of trial interventions specifically targeting social isolation or loneliness within the health care system have been developed, though few of these have been empirically proven to work. CareMore Health is an integrated health plan and care delivery system for Medicare and Medicaid patients. In 2017 it created the Togetherness Program, which is composed of three inter-related approaches for helping people found to be isolated: Phone Pal, a phone-based interaction; a home-based visiting program; and leveraging existing care centers as social hubs with a community health worker embedded in the space. Individuals can opt into the Togetherness Program during their initial HealthyStart visit or can be referred to the program by physicians in the CareMore system.11 Early results suggest that the Togetherness Program has decreased emergency room use among enrolled patients by 3.3 percent compared to baseline; additionally, hospital admissions per thousand members are 20.8 percent lower among program participants than in the control group (Business Wire, 2018). CareMore appointed a chief togetherness officer who manages the program and fosters internal and external partnerships related to the topic (Jain and Samitt, 2018).
UnitedHealthcare, a large health insurance company, launched the Navigate4Me program in fall 2017 for individuals enrolled in its Medicare Advantage plans who live with complex health issues such as diabetes, congestive heart failure, or multiple chronic conditions (UnitedHealth Group, 2018). The program offers health navigators who support and guide individuals through the complicated health care system, providing both clinical and administrative assistance (such as answering health questions and resolving billing issues) in addition to addressing the social determinants of health (e.g., by connecting individuals with reliable transportation or housing assistance). UnitedHealth Group reports early positive results, with a 14 percent reduction in hospitalizations and a 9 percent reduction in emergency room visits for people with congestive heart failure (UnitedHealth Group, 2018). In 2018, eligibility for the program was expanded and specifically made available to individuals at risk for social isolation.
Kaiser Permanente, an integrated managed care consortium, launched Thrive Local in 2019. This program created a new social health network in Oregon and southwest Washington State with the aim of creating connections between health care providers and social services agencies. To best address the social needs of its members, Thrive Local will be built locally in partnership with nonprofit and
___________________
11 Presentation by Dr. Sachin Jain to the committee on April 25, 2019.
government agencies, with the goal of including other health systems and health centers (Kaiser Permanente, 2019). Thrive Local will be integrated into Kaiser’s electronic health record as a way of tracking social needs and referrals to social providers (Johnson, 2019).
Other health insurance companies are beginning to identify social isolation and loneliness as problems that need to be addressed in their broader health campaigns. Humana’s Bold Goal12 is a population health strategy that specifically addresses the social determinants of health, including loneliness and social isolation, in order to improve health status. As part of this, Humana created a Loneliness Toolkit (Humana, 2018) for consumers that addresses such issues as health care needs, staying engaged, and supporting loved ones who may be isolated or lonely. Humana also developed a one-page guide (Humana, 2019) for physicians, which focuses on defining social isolation and loneliness, highlighting their major health impacts, presenting the three-item UCLA Loneliness Scale, and advising physicians on potential referrals and resources. Other health insurance companies are leveraging existing health promotion programs to combat isolation and loneliness. In May 2018, Cigna released the results from a survey assessing the impact of loneliness in the United States; the president and chief executive officer, David Cordani, said of the data: “[W]e’re seeing a lack of human connection, which ultimately leads to a lack of vitality” (Cigna, 2018). Cigna is using existing programs, such as its Health Advisor Program, Health Information Line, and Employee Assistance Program, in order to address loneliness in the company’s employee and patient populations (Cigna, 2018).
Interventions That Target Specific Risk Factors
Another approach to addressing social isolation and loneliness in the health care system is to identify specific underlying risk factors (particularly health-related risk factors) and to address those issues as appropriate within the health care system. Interventions that fail to target the underlying causes of isolation and loneliness are likely to be less successful.
For example, as mentioned in Chapter 4, untreated hearing loss is associated with social isolation and loneliness (Chen, 1994; Mick et al., 2014, 2018; Pronk et al., 2013; Sung et al., 2016; Weinstein and Ventry, 1982). Several studies suggest that treating hearing loss with hearing aids or cochlear implants may mitigate the effects of hearing loss on loneliness (Contrera et al., 2017; Weinstein et al., 2016).
Other interventions that target specific risk factors focus on enhancing cognition (Winningham and Pike, 2007); enhancing physical mobility or exercise (Brady et al., 2020; Ollonqvist et al., 2012; Tse et al., 2014; Wallace et al., 2014; Zijlstra et al., 2009); and dealing with bereavement or widowhood (Chow et al., 2018; Stewart et al., 2001). (See Chapter 7 for more on the role of the health care system in identifying and addressing the underlying causes of social isolation and loneliness.)
___________________
12 For more information, see https://populationhealth.humana.com (accessed August 5, 2019).
COALITIONS AND PARTNERSHIPS TO ADDRESS SOCIAL ISOLATION AND LONELINESS
The 2019 National Academies consensus study report Integrating Social Care into the Delivery of Health Care identified assistance, alignment, and advocacy as key activities to facilitate the integration of health care and social care (NASEM, 2019). Assistance activities “reduce social risk by providing assistance in connecting patients with relevant social care resources” (p. 44). Alignment activities are “undertaken by health care systems to understand existing social care assets in the community, organize them in such a way as to encourage synergy among the various activities, and invest in and deploy them to prevent emerging social needs and improve health outcomes” (p. 46). Advocacy activities involve health care organizations partnering with social care organizations “to promote policies that facilitate the creation and redeployment of assets or resources in order to improve health outcomes and prevent emergence of unmet social needs” (p. 47). Furthermore, the National Academies committee that produced the report noted that in such activities, “health care organizations leverage their political, social, and economic capital within a community or local environment to encourage and enable health care and social care organizations to partner and pool resources, such as services and information, to achieve greater net benefit” (p. 47). Cross-sector coalitions and partnerships are two strategies for increasing assistance, alignment, and advocacy. For the purposes of this current report, the committee identified the formation of coalitions and partnerships to share best practices as among the key strategies (or even interventions themselves) underlying the identification and implementation of effective interventions for social isolation and loneliness in older adults. Several coalitions and partnerships have been formed specifically in response to the growing public recognition of the health impacts of social isolation and loneliness. The sections below highlight a few examples.
Oregon Healthy Aging Summit
The Oregon Healthy Aging Summit was a collaborative effort “to develop a road-map and accelerate action to promote the healthy aging of older adults in Oregon”13 by bringing together policy makers, providers, patients, and researchers to address issues related to social isolation. The summit sought to represent many diverse groups who may have specialized needs such as people of different races or sexual orientation or individuals living in less populous or rural locales. The summit was structured around the AHRQ rapid evidence review (described earlier in this chapter), with the review acting as a framework for summit presentations and discussions.
___________________
13 Guise, J. M. 2018. PowerPoint presentation to committee—Addressing social isolation to improve the health of older adults: A rapid review and summit. In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
Several different programs targeting social isolation were discussed, including those related to physical activities, social support, arts and recreation, and access to health services. Some of the major priorities outlined by summit participants were:
- The development of an information system to connect health systems and community resources.
- The co-creation of measures and implementation strategies and the evaluation of programs using the same definitions and measures.
- The development and maintenance of a person-centered approach that promotes equity.
Post-summit activities included setting up a shared email (healthaging@ohsu.edu), establishing and expanding connections, collecting and distributing information on resources, and planning subsequent meetings with health system leaders to discuss sharing data and social services locator services.
Los Angeles Social Isolation and Loneliness Impact Coalition
The Los Angeles Social Isolation and Loneliness Impact Coalition was created through a collaborative arrangement between the Motion Picture and Television Fund (MPTF) and the AARP Foundation with the goal of addressing the health and financial impacts of social isolation and loneliness in older adults. The coalition seeks to build on and promote existing community-wide efforts focused on addressing social isolation and loneliness and creating partnerships and sustainable social interventions that can be expanded nationally. MPTF initiated a volunteer-operated call center called A Daily Call Sheet that facilitates communication with very isolated or low-income individuals, many of whom have chronic illnesses. In describing the work of the coalition to the committee, Maureen Feldman, the director of Social Isolation Impact Project in Los Angeles and the director and the founding chair of the Los Angeles Social Isolation and Loneliness Impact Coalition explained that to date, [roughly] 10,000 social calls have been made through this program to active industry members, retirees, and relatives of industry members. While the coalition is not specifically focused on the role of the health care system, coalition member and collaborative efforts have been broad and include
- annual summits on social isolation and loneliness with participation from for-profit and not-for-profit businesses, academic institutions, and faith-based organizations;
- the creation of a call program toolkit to help establish new social outreach programs and to train volunteers;
- the initiation of ongoing data collection and analysis protocols;
- the implementation of new friendly call programs;
- the training of local police on social isolation issues and resources for homeless individuals;
- connecting people in need with key resources; and
- providing access to economical graduate education to older adults.
According to Feldman, a survey of coalition members in 2018 revealed that the top reasons for joining the coalition included developing partnerships (87 percent), sharing of best practices (80 percent), and learning about the latest research (70 percent). In describing the work of the coalition, Feldman explained, “Together we will find ways to effectively collaborate and create meaningful change.”
AARP Foundation Connect2Affect
As noted in Chapter 8, the AARP Foundation has partnered with the Gerontological Society of America, Give an Hour, n4a, and UnitedHealthcare to share information about successful interventions and the latest academic research on social isolation (AARP Foundation, 2019). The Connect2Affect website includes an option for individuals to share resources related to new research or best practices. Like the Campaign to End Loneliness’ Learning Network (see Chapter 8), this repository largely represents an effort to share resources and does not primarily conduct evidence-based assessments of interventions on their own.
TECHNOLOGICAL INTERVENTIONS
Information technology (IT) can provide a platform for the delivery of targeted individual or group interventions. A variety of technologies have been tested as ways to reduce social isolation and loneliness in older adults (Chipps et al., 2017; Khosravi et al., 2016). Table 9-6 provides an overview of potential IT solutions with different functionalities, the types of technologies used, and specific examples of their use to address social isolation and loneliness. (This chapter will focus on the use of technology for interventions. See Chapters 6 and 7 for a discussion on the use of technology for assessment.)
With the growth of artificial intelligence (AI), social robots and conversational agents are often viewed as effective tools for social engagement in gerontology. Virtual reality is another platform that is expected to help older adults with social engagement. More traditional and widely available tools, such as social media groups and video conferencing, are frequently integrated into behavioral or supportive interventions for isolated older adults. With any of these technological approaches, challenges related to user friendliness remain.
Internet Use
The potential of the Internet to connect older adults has been examined since the early days of online communities. While new tools are being introduced to
TABLE 9-6 Types of Information Technology Tools to Address Older Adults’ Social Isolation and Loneliness
| Function | Technology | Example(s) |
|---|---|---|
| Assessment (mining data to identify or predict patterns of social isolation and loneliness) | Passive home-based monitoring sensors | Motion sensors and door/window sensors capture time spent inside versus outside the home, the number of visitors, the amount of time spent in the presence of others |
| Tracking of usage patterns of online and phone tools | Tracking time spent interacting on social media platforms, time spent on the phone, number of phone calls and video calls initiated and received | |
| Wearable sensors | Activity and sleep tracking facilitated by a wrist-worn watch provides data for one’s life-space (as a series of concentric areas radiating from the room where one sleeps and extending to the residential setting, neighborhood, community, and beyond) | |
| Intervention | Social media “virtual communities” | Engagement in peer-support groups (for example, Facebook “secret groups” to exchange information and seek emotional support) |
| Virtual reality | Virtual reality (VR) systems including hardware (a VR headset) and software (with virtual reality content specifically designed for older adults with the goal of providing reminiscence therapy elements with familiar experiences or engagement with new stimulations) | |
| Social robots/conversational agents | Use of conversational agents with artificial intelligence functions to engage users in dialogue either for general companionship or for meeting specific goals (reminders, health or safety assessment) | |
| Video-mediated “friendly visits” | Use of video conferencing software such as Skype or FaceTime or commercially available software for volunteers or other staff to conduct regular “friendly visits” | |
increase social engagement, the inability of older adults to use them may exacerbate their isolation. Older adults who are not familiar with new media platforms seem more likely to become isolated from groups or cohorts that use emerging technologies for communication (Melenhorst et al., 2001). White et al. (2002) facilitated Internet access for 100 older adult volunteers from four congregate housing sites and two nursing facilities over a 5-month period. The volunteers were randomly assigned to receive Internet training or to a waitlist control group. Results showed a trend toward lower loneliness and depression among those who received training, but this was not statistically significant.
Cotten and colleagues (2013) examined the usage of information technologies among older adults in assisted and independent living communities in Alabama and found that Internet use was associated with lower levels of loneliness. Similar findings were reported by Russell et al. (2008) in a study surveying older Australian Internet users: Internet use facilitated access to bonding capital (maintaining close ties) and also bridging capital (connections across social networks). Also in Australia, in a later online survey study of older adults, greater use of the Internet as a communication tool was associated with a lower level of social loneliness; however, greater use of the Internet to find new people was associated with a higher level of emotional loneliness (Sum et al., 2008).
In 2010 Hogeboom and colleagues used the Health and Retirement Survey (HRS) to examine associations between Internet use and social networks among 2,284 adults over 50 years of age. Frequency of contact with friends, frequency of contact with family, and attendance at organizational meetings (not including religious services) were found to have a significant positive association with Internet use. These survey findings suggested that Internet use can strengthen social networks for older adults.
Internet use has also been found to be beneficial in the context of social isolation and loneliness for homebound older adults. The CHIPS (Computers for Homebound and Isolated Persons) Program sought to create an online community for individuals who were homebound and to connect seniors with others in similar circumstances (Bradley and Poppen, 2003). A 1-year follow-up showed that the participants’ level of satisfaction in the amount of contact with others increased significantly.
Tsai and Tsai (2011) used video conferencing software to connect nursing home residents with remote family members during a 3-month intervention deployed in 16 nursing homes in Taiwan. The program had a long-term effect in alleviating depressive symptoms and loneliness for nursing home residents, and it also improved long-term emotional social support and short-term appraisal support.
Czaja and colleagues (2018) noted the importance for older adults of having “meaningful access” (p. 476) to the Internet and computer-mediated strategies for social support. They reported that access to the Personal Reminder Information and Social Management (PRISM) computer system yielded lower levels of social isolation and less perceived loneliness in older adults after 6 months. Although the differences between the PRISM group and the control group were not maintained after 12 months, the PRISM group still showed improvements in social isolation and loneliness compared to baseline. The investigators noted that technological interventions such as PRISM would not supplant human interaction, but might supplement other strategies.
Social Media Use
The Pew Research Center (2018) estimates that older adults are the fastest-growing group of individuals to adopt and use social media sites. Social media
use can be differentiated into active and passive use. Active use refers to “activities that facilitate direct exchanges with others,” whereas passive use pertains to the “monitoring of other people’s lives without engaging in direct exchanges with others” (Verduyn et al., 2017, p. 281). However, different segments of the older adult population may be using social media in different ways or have different levels of comfort with its use. For example, older adults seem to use Facebook less actively than younger adults (Hayes et al., 2015).
A 2012 Pew Report identified three factors that contribute to social media use among older adults: receiving social support, reconnecting with peers in their age groups, and bridging generational gaps (Zickuhr and Madden, 2012). Jung et al. (2017) conducted in-depth interviews to identify why older adults use or avoid Facebook. Six main motivators were identified: the desire to keep in touch, sharing photos, social surveillance, responding to family member requests, convenience in communication, and curiosity. The main reasons given for avoiding Facebook included privacy considerations, technology limitations, the triviality of the communication, time commitment, and frustration with the platform features.
Ang and Chen (2018) found that online social participation has the potential to alleviate the negative effects of pain on mental well-being, indicating that online social participation could supplement attempts to facilitate social engagement in later life, in particular for those whose social activities may be affected by the pain they experience. Grieve and colleagues (2013) concluded that offline social connectedness and Facebook connectedness were separate constructs. Furthermore, by studying 274 older adult Facebook users, they found that using Facebook could provide the opportunities for developing and maintaining social connectedness in the online environment and showed that lower depression and anxiety and greater life satisfaction were associated with Facebook connectedness. A simple association between social network site usage and loneliness may not, however, be automatically assumed among community-dwelling older adults. Aarts et al. (2015) surveyed 626 adults aged 60 years or older in the Netherlands to investigate the relationship between social sites usage and loneliness and found that, in general, social network sites usage appeared unrelated to loneliness.
Social Robots and Conversational Agents
A social robot is defined as an artificial agent (often embodied with anthropomorphic or zoomorphic features) that interacts with humans by following the social norms and behaviors attached to its role (Broekens et al., 2009; Taipale et al., 2015). Social robots have been developed and tested for their potential to meet the mental health needs of older adults through interactions involving information exchange (Broadbent et al., 2014). Pu and colleagues (2019), in their meta-analysis of RCTs examining the effectiveness of social robots for older adults, reported that social robot interactions have the potential to “improve engagement, interaction, and stress indicators, as well as reduce loneliness and the use of medications
among older adults” (p. e37). One of the most common and frequently examined social robots is PARO, a robotic baby harp seal, which has been tested in various settings with older adults with and without cognitive limitations (Jøranson et al., 2016; Liang et al., 2017; Robinson et al., 2013). Other examples include a robotic dog named AIBO (Banks et al., 2008), a humanoid communication robot called NAO (Soler et al., 2015), a humanoid robot designed to communicate and behave like a 3-year-old boy (Tanaka et al., 2012), and health care robots IrobiQ and Cafero (Broadbent et al., 2014).
Broader in concept than social robots, conversational agents are “systems that mimic human conversation using text or spoken language” (Laranjo et al., 2018, p. 1248). Conversational technologies involve the use of intuitive, natural language on the part of both the user and the system. This is in contrast to systems that require input that is formulated to be interpreted by a computer system (e.g., computer terminals) or technologies that require selection and interactions through the manipulation of graphical elements (e.g., point and click via mouse). Conversational technologies are envisioned to be more intuitive to use, easier to learn, and more resistant to communication breakdowns than non-conversational technologies (Cassell et al., 1999). Voice-based personal assistants such as the Amazon Alexa and Google Home are commercial examples of technologies that attempt to make use of conversational interaction.
Agents and agent-based systems refer to technologies that are capable of autonomous action. These systems can act without the direct involvement of humans, can initiate action in response to a certain set of conditions in their environment, and can interact with other agents and humans (Jennings and Wooldridge, 1998). A classic example of an agent is an automated online travel assistant that supports users in locating, selecting, and booking travel plans (e.g., Schiaffino and Amandi, 2009).
Embodied conversational agents (ECAs) leverage the use of parts of the body, such as hands, the face, or a tonal shift via vocal cords, to regulate conversation and contribute content (Cassell et al., 1999). For example, an ECA might express confusion through facial features in order to prompt a user to repeat or rephrase a sentence or clap to show enthusiasm or appreciation of a point. ECAs range in appearance from cartoonlike to highly realistic and possess the ability to engage in verbal and non-verbal conversation in a human-like manner (Cassell, 2001). The three key components of a typical ECA are (1) an interface through which information is collected from users, (2) a visual representation or interface through which the agent communicates with users, and (3) an algorithm or software that allows it to reason like a human (Cassell, 2001; Provoost et al., 2017).
ECAs have been investigated primarily in the areas of gaming and health care. In health care, ECAs have been used in patient education (e.g., nurse agents to explain medical documents to patients), clinician training (e.g., training mental health professionals), and the delivery of behavioral interventions (e.g., interventions targeting behavior change), including serious games and
physical activity (Bickmore et al., 2009, 2010; Carpenter et al., 2012; Johnson et al., 2016; Kanaoka and Mutlu, 2015; Lisetti et al., 2013). Some work has examined the use of conversational agents specifically for older adults. Bickmore et al. (2013) demonstrated that ECAs were effective in significantly increasing physical activity levels in older adults when compared to a group of pedometer users. Vardoulakis et al. (2012) conducted a study with an agent (using the so-called “Wizard of Oz” methodology for which the older adult interacts with a computer controlled by another human) and found that older adults obtained a sense of companionship and support from the agent and were interested in discussing a wide range of topics. Yaghoubzadeh et al. (2013) used participatory design to create and demonstrate the feasibility of a virtual agent to assist with daily activities of older adults. Their study showed that older adults were able to engage and interact successfully with the agent (Yaghoubzadeh et al., 2013). In addition, ECAs have also been shown to be beneficial for health management. For example, Looije et al. (2010) showed that a virtual assistant was rated more highly than real persons, particularly for conveying empathy. The ability to express empathy is a social behavior that can significantly aid in persuasive efforts to facilitate healthy behaviors (Looije et al., 2010). Some ECAs have been developed for individuals with conditions that increase in prevelance with aging, such as dementia (Sakai et al., 2012). The conversational agents in these studies have taken on various appearances, from human-like (Bickmore et al., 2013) to animal characters (Looije et al., 2010).
ETHICAL AND PRACTICAL CONSIDERATIONS FOR INTERVENTION
When interventions for social isolation and loneliness are designed, various ethical and practical consideration arise, including (but not limited to) how levels of social isolation and loneliness are assessed (see Chapter 6), who implements the intervention, which settings are appropriate for an intervention, and what the intervention entails or how it functions. While many interventions considered in this chapter are relatively low-tech, technology-based interventions have been gaining in popularity. Various ethical considerations related to using technology with older adults have been studied, particularly around robotic care (Sharkey and Sharkey, 2012; Sorell and Draper, 2014), smart home technologies (Chung et al., 2016), and telehealth (Demiris et al., 2006, 2009). While newly introduced technologies can have a positive impact on health of older adults, potential harms also need to be considered, particularly in the areas of privacy, informed consent, and autonomy (Chung et al., 2016; Demiris et al., 2009). A recent review of the literature found that 67 percent of the current intelligent assistive technologies (IATs) in dementia care (e.g., handheld devices, mobility aids, smart home sensors, robots) were designed without considering their ethical implications (Ienca et al., 2018). Moreover, among those IATs developed with attention to ethics at the design level, there was great variation in the kinds of ethical considerations that
had been addressed. For example, privacy considerations had been addressed in only 5 percent of the examined technologies.
In evaluating the potential of any intervention to prevent or mitigate social isolation and loneliness, either as a single intervention or in combination with other interventions, questions of accessibility, acceptability, cost, and the feasibility need to be addressed. This section explores potential ethical and practical concerns related to both technological and non-technological interventions.
Accessibility
Accessibility refers to ensuring that services and technologies are usable by people with disabilities, either by design or by the addition of adaptive software or hardware. Given that visual, motor, and hearing changes are common with aging, making technology accessible to older adults may include such things as making digital displays accessible to people with vision loss (e.g., providing options to increase font size) and accounting for motor changes such as tremors (Hanson, 2001; Kaeberlein and Martin, 2015; Saxon et al., 2015). However, ECAs and social robots as well as other new technologies (e.g., voice based personal assistants such as Amazon’s Alexa) are adopting voice as an interaction mechanism. The use of one’s voice may be a more accessible interface for people who have low vision, but, on the other hand, it may present issues for people who are deaf or hard of hearing. Adjusting the volume of audio output of technology is a way that people often compensate for age-related hearing loss (Pacala and Yueh, 2012), but the conversational aspect of these new technologies means that new dynamics need to be investigated in regard to accessibility (e.g., turn-taking in conversation when one party has hearing loss). Cognitive accessibility also needs to be considered in regard to voice-based interactions with ECAs or robots because of the normal cognitive changes that occur with aging as well as the increased incidence of dementia.
Research on technology for aging has expanded to encompass factors affecting other types of accessibility, including structural, financial, and personal barriers (Chung et al., 2016; Demiris et al., 2006, 2009). Although technology adoption by older adults is increasing (Pew Research Center, 2017), a large proportion of older adults remain without access to technology, such as the Internet and hardware (e.g., tablets), that are needed for use of these ECAs. In addition, disparities due to differences in socioeconomic status affect older adults’ technology use and access to technology (Smith et al., 2015). Financial accessibility will likely be an issue because the ECA services that are emerging for older adults—particularly those that involve a “human in the loop”—often involve recurring monthly payments.
Another potential factor affecting accessibility is literacy. Preliminary studies show that many ECAs can be used by individuals with lower literacy levels (Bickmore et al., 2009, 2010). These studies show that ECAs are not bound by
time constraints like providers, and they are able to convey information clearly and multiple times, making them easy to comprehend by patients (Bickmore et al., 2009, 2010).
Privacy and Data Protection
With the rise of consumer-facing technologies, discussions of privacy and confidentiality are evolving. Existing norms and legislation related to health information are being reconsidered and extended to include new devices oriented toward patients. Specific issues related to ECAs or social robots include the protection, storage, and transmission of audio and video data (Demiris et al., 2006). ECAs that interface with health care providers need to meet the standards set by the Health Insurance Portability and Accountability Act.14 Consumers usually use passwords to protect information and accounts. Passwords that require the memorization of a string of characters may not be the ideal solution for many people, particularly for older adults with cognitive impairment, or in cases when multiple people, including caregivers, may interface with the technology. In this scenario, privacy issues intersect with accessibility concerns. Given that ECAs in the home use audio and sometimes video data, they pose privacy risks not only to people using them, but to others who enter the space where they are deployed. Another potential privacy risk relates to the transmission of data by social robots and ECAs to family members or health care providers concerning the health conditions and activities of older adults, who may not want that information shared.
Autonomy
Autonomy represents the freedom of an individual to make decisions regarding their own life in accordance with their own goals, values, and preferences. Autonomy is an essential guiding principle for interventions and a key ethical issue in the care of older adults. However, respecting the autonomy of older adults may present challenges when the older person does not have full decision-making capacity, or when other family members are involved in the older adult’s care.15 A 2019 study by AARP found that “76 percent of Americans age 50 and older say they prefer to remain in their current residence and 77 percent would like to live in their community as long as possible.”16 Many new technologies, including ECAs, are designed to support older adults in living independently. Regardless,
___________________
14 Health Insurance Portability and Accountability Act, Public Law 191. 104th Congress. August 21, 1996.
15 See https://journalofethics.ama-assn.org/article/autonomy-and-quality-life-elderly-patients/2008-06 (accessed November 4, 2019).
16 See https://www.aarp.org/research/topics/community/info-2018/2018-home-communitypreference.html (accessed November 4, 2019).
concerns may arise for the use of these types of technologies, leading to lost autonomy and personal liberty (Bickmore, 2005; Garner et al., 2016). However, the loss of independence and autonomy may not be the most important ethical factor to consider when it comes to particular populations, such as frail older adults (Zwijsen et al., 2011). Though the majority of published literature has not yet addressed the ethical implications of social robots or ECAs, there are some articles that have begun to outline some of the potential considerations (Bickmore, 2005; Bickmore et al., 2005). For example, Bickmore et al. (2005) discussed issues concerning an agent deceiving users into thinking it is a person, agents reducing expressivity, and the autonomy of users. Garner and colleagues (2016) conducted group discussions with various stakeholders to understand the concerns and reservations related to using a virtual carer system for older adults.
Informed Consent
For all types of interventions, informed consent is perhaps the ethical issue that has received the most attention in research. However, technological approaches confer unique challenges for the informed consent process. Some approaches stress the importance of ongoing consent and the ability to rescind consent (Neill, 2003). These approaches, however, assume that an individual is continuously able to assess risk and what is in his or her own best interests.
For technological interventions, researchers are beginning to argue that conventional ways of obtaining informed consent are not sufficient for research (Vitak et al., 2017). Some of these concerns arise because of the persistence and vastness of data created, stored, and transmitted by new technologies, which can lead to possible future uses that were unspecified at the time of consent (Vitak et al., 2017). Data collected by ECAs might be seen as valuable for researchers who study aging, and there is a need to understand how informed consent can best be obtained for older adults with these new technologies. Furthermore, in the case of ECAs, social relationships may be built over time. Users may develop trust in virtual agents that may affect their ability to assess risks. Trust—and misplaced trust—are informed consent–related issues found in many settings involving research or interventions (de Melo-Martín and Ho, 2008), but they become particularly complicated when trust is developed between participants and the system that is deployed. Trust developing between an individual and a device could mean that an older adult reveals more personal information than would otherwise be the case because of the perceived lower interpersonal risk of sharing and a failure to realize that in some cases this information may become accessible to third parties or other stakeholder groups.
Additional informed consent concerns that are specific to social robots or ECAs include the high level of digital literacy needed to understand the mechanisms of the technology. Moreover, users may need to understand AI, networks, and data transmision in order to fully apprehend the risks associated with ECAs.
Data literacy in this case becomes a great challenge because users need to understand how their data are collected, who can access them, and what the potential risks may be. Informed consent with ECAs, as with other technologies, is further complicated when individuals are experiencing cognitive impairment and dementia—conditions that increase in prevalence as people age. Ideally, an individual’s capacity to consent is determined on a case-by-case basis with attention paid to the magnitude of the potential harm of the research or intervention and to the participant’s understanding of the risks (Appelbaum, 2007); however, both of these factors are difficult to assess with the new technologies.
Finally, consideration may be needed regarding informed consent for the use of IT beyond research, such as a new technology introduced for patient care in the home (e.g., video cameras).
Exacerbating Rather Than Reducing Isolation
For older adults, particular attention will need to be paid to the impact of interventions that substitute for human contact. For example, attachment to companion animals has been shown to be associated with changes in psychological health (Raina et al., 1999). A key concern for technological interventions is that the same tools intended to address isolation and loneliness could lead to further isolation by ultimately substituting for human contact (Chung et al., 2016; Sharkey and Sharkey, 2012; Sparrow and Sparrow, 2006). This issue may be a particular concern with social robots and ECAs, given that these technologies rely on social interactions and building relationships. Pilot studies with ECAs have demonstrated that older adults can engage and interact with ECAs and thus may potentially develop relationships with these devices (Bickmore et al., 2005; Tsiourti et al., 2014). Methods that have been suggested to reduce isolation and dependence include periodically checking on a person’s dependence and having time limits for the usage of the system (Garner et al., 2016). This approach becomes difficult to implement, however, when the effectiveness of the ECA may rely on a continuous connection and relationship built over time. As IT tools become formally integrated into traditional health services in order to reduce cost and human resources, it will be important to assess whether virtual or AI-based interactions meant to replace human observers or interaction partners lead to a lower quality of engagement and an increased sense of loneliness, at least for some older adults. Another challenge is attachment. ECAs and other technologies developed for older adults may have high costs, sometimes with services attached that require continuous payment, and the participants may have to stop using devices because of such constraints as the research study period, financial resources, and travel.
Additionally, as mentioned in Chapter 7, there may be stigma associated with being labelled as socially isolated or lonely. Such stigma might risk causing the individuals to be blamed for being isolated or feeling lonely instead of viewing
these problems as being due to a variety of factors at the level of the individual, community, and society. As a result, individuals suffering from social isolation or loneliness may not want to identify as such for the purposes of receiving an intervention, thereby exacerbating their isolation or loneliness.
Perceptions of Safety and Functionality
Although interventions such as new technologies are often developed to support safety for older adults, unintended consequences may arise. For example, a power cord attached to a technology could pose a falling risk. ECAs, however, may be more likely to be on mobile platforms and therefore pose less of a hazard. Perceptions of functionality also might lead to potential safety issues (Yusif et al., 2016). Given the social element of the devices, people might expect devices to be able to fill social safety roles, such as alerting others in case of emergencies—even when this is beyond the technical capabilities of the device or not implemented for fear of adverse events and litigation. Additionally, individuals might come to depend on functionalities such as medication reminders, and if a device malfunctioned or a company shut down, it could leave older adults without the support they had come to rely on (Hensel et al., 2006).
Infantilization of Older Adults
The introduction of social robots or ECAs for older adults in some cases introduces concerns for the infantilization of these individuals (i.e., creating a behavioral pattern in which the older adult is treated in a child-like manner). This may be especially true when there is a perception that “toys” or “robotic pets” are ways to engage and entertain isolated or lonely older adults (Birks et al., 2016; Salari and Rich, 2001). Infantilization needs to be acknowledged and addressed by system designers both in the design and selection of features for the hardware and software systems and in the integration of existing knowledge bases for AI solutions. Because knowledge bases are informed by existing data and assumptions, ageism and other biases may be reflected in the way a system is designed to interact with an older adult.
Disparities in Access to Interventions
Older adults may have disparities in their ability to access a variety of interventions. For example, an individual who lives in a rural area may not have any local programs or an individual who has a functional limitation in mobility may be unable to access programs that exist even in their own communities. Limitations in access may be particularly acute when it comes to technological interventions. The concept of a digital divide has been of growing concern as
the use of technology by health care consumers has increased. Questions of equity and “digital inclusion” (Powell and Deetjen, 2019, p. 1) have evolved from issues of simple access to infrastructure and equipment to include access to the knowledge and skills needed to use technology and now to a consideration of who benefits the most and in what ways (Ball et al., 2017; Powell and Deetjen, 2019). The following sections focus on disparities in access to technological interventions.
Differences Between Rural and Urban Environments
Early concerns regarding access to technology were primarily related to the availability of broadband Internet access for people in rural areas and low-income populations in urban areas (van Deursen and van Dijk, 2019). Although broadband is more widely available than in the past and the use of smartphones is now ubiquitous, the question still merits attention, in part because of variations across geographic areas, costs, ease of use, and acceptability to older adults. While access to Web-based and technology-enabled connections has increased and such connections have been described as “a basic utility for social inclusion” (van Deursen and van Dijk, 2019, p. 355), geographic disparities still exist, and issues have surfaced related to knowledge, skills, and costs over time. As of 2018, 39 percent of people living in rural areas in the United States did not have access to broadband in their homes, compared with 4 percent of people in urban areas (Stover, 2018). People living in rural areas often have a limited choice of broadband providers and may experience lower broadband speeds than in urban areas. Wired Internet connectivity is more costly in rural areas because of the lower population density and the need for longer wiring; additionally, wireless technology, particularly on mobile phones, can be costly, and download speeds can vary across carriers (Stover, 2018).
Access to broadband alone does not address access to the necessary hardware, software, peripherals, licenses, and subscription fees (van Deursen and van Dijk, 2019). The resource limitations experienced by some high-risk populations can worsen inequalities in access to technologically mediated supports to address social isolation and loneliness.
Rural residents are increasingly using mobile technologies, such as smartphones, rather than broadband as a means of accessing the Internet (Pew Research Center, 2019b; Stover, 2018). According to a survey conducted by the Pew Research Center in 2019, 71 percent of rural residents owned smartphones, compared with 83 percent of urban residents (Pew Research Center, 2019b). Similarly, 53 percent of older adults owned smartphones compared with 96 percent of young adults aged 18–29 and 79 percent of adults aged 50–64. These findings suggest that older adults living in rural areas do not have the same ubiquitous access to mobile technologies as do those who are younger and living in urban areas.
Age
Age has been specifically identified as a factor in the digital divide (Wu et al., 2015). In a study of adults in the Netherlands, where the Internet saturation is 98 percent, the investigators found that age was negatively related to access to multiple devices and peripherals (e.g., printers, scanners, additional screens, hard drives, docking stations) and also negatively related to total cost of maintenance expenses (van Deursen and van Dijk, 2019). This suggests that even in a technologically advanced society, older adults have fewer devices and peripherals, thereby limiting the types and extent of social connections that are possible using technology.
Pearl (2014) reported on the use of three technologies by members of Kaiser Permanente Northern California: Internet, mobile technologies, and video platforms. He found that 51.2 percent of members over the age of 70 had enrolled in the Kaiser Permanent website, compared with 71.6 percent of members aged 30–70 (Pearl, 2014). This suggests that older adults might be less likely to use technologically mediated strategies than young and middle-aged adults. Although a majority of adults over age 65 are using the Internet (73 percent in 2019), the rate is far lower than in younger age groups (88 percent of adults aged 50–64 and 97 percent of those aged 30–49 years) (Hong and Cho, 2017; Statista, 2020). In an analysis of survey data originally collected at three points in time by the Health Information National Trends Survey of the National Cancer Institute, Hong and Cho (2017) found that older adults were increasingly accessing the Internet. Older adults’ use of Internet resources was primarily for obtaining health information and communicating with their physicians. The study found that education and income were related to Internet use, while rural-versus-urban residence was not. The authors concluded that although the “digital divide” was narrowing, it remained substantial for those who were older, less well educated, and with lower incomes. This suggests that the social determinants of health create barriers to older adults’ access to technologies and that reducing these barriers could be helpful in efforts to reduce social isolation and loneliness. Adults aged 75 and older were less likely than adults aged 65–74 to use the Internet. Hong and Cho stated that “improved access to the Internet may enable older adults’ access to health information, but it may not necessarily lead to the adoption of various aspects of HRIU (health-related Internet use), such as connecting with people online” (Hong and Cho, 2017, pp. 860–861).
Another perspective on the digital divide concerns how and when electronic technologies are used and how different age groups perceive them. Focus groups conducted by Ball et al. (2017) indicated that older adults were offended by the use of electronic technologies when family members or others were physically in their presence, but appreciated their use when apart. Thus, electronic technology use could worsen feelings of social isolation from those in direct contact with older adults but serve as a tool to enhance social connection when at a distance.
Older adults’ use of certain technologies may depend strongly on their comfort and familiarity with the devices. As a result, training older adults in the use of the technology may encourage more seniors to use various devices. For example, Older Adults Technology Services17 trains older adults in community settings in computer skills, including the use of email, the management of medical information, and the building of community networks.
Underserved Populations and the Social Determinants of Health
In a literature review of the impact of sociodemographic factors on the use of eHealth, Reiners et al. (2019) concluded that older adults and individuals with lower incomes were generally less likely to use eHealth. It also appeared that people with less education were less likely to use eHealth. Literacy skills are key to some uses of eHealth. This review suggested that limited access to the appropriate equipment and a lack of the skills needed to use the equipment contributed to older adults’ lower levels of use of eHealth. These authors recommended tailoring eHealth strategies to the needs of individuals, providing education and support for the use of eHealth, and involving caregivers when possible. When older adults live alone, they may be less likely to use electronic strategies because of a lack of support. In a systematic review of studies of eHealth literacy among underserved U.S. populations, Chesser et al. (2015) noted that few of the studies they reviewed were conducted with rural populations.
Mitchell and colleagues (2019) evaluated data from the 2014 HRS and found that older adults from racial and ethnic minorities, including Hispanics and African Americans, used health-related technology less frequently than whites. Although differences were not found across racial and ethnic groups in younger ages, by age 62 differences began to emerge. The authors speculated that language may contribute to the differences seen in older Hispanic adults, and they noted no differences were found in the use of specific technologies, such as “e-mails, text messaging and mobile applications for health” (p. 11), suggesting that targeting the type of technology for its acceptability to the population may be an appropriate strategy.
Older Adults with Disabilities
In a review of the literature, Vázquez et al. (2018) found that the few studies that addressed the use of eHealth by older adults with intellectual disabilities indicated that eHealth was used by this population primarily as support for independent living, telehealth, and communication. The authors recommended using universal design in eHealth to increase the ease of use and also considering
___________________
17 For more information, see https://www.oats.org (accessed October 16, 2019).
the use of strategies such as games and virtual reality. Gell and colleagues (2015) found that older adults with disabilities that led to functional limitations were significantly less likely to use the Internet than those without such limitations. This was particularly true for those individuals who needed help with activities of daily living or mobility outside the home and those with vision or memory impairments. Older adults with other issues, including pain and breathing problems, were more likely to use technology. The investigators noted this may have been because the ease of getting help using technology outweighed the difficulties of trying to do so in other non-technological ways for these specific impairments.
Infrastructure Issues
Pearl (2014) found that reimbursement issues detracted from physicians’ willingness to use technology for virtual visits. Fee-for-service reimbursement systems do not always cover such visits, and issues persist concerning the amount of coverage and managing provider licensure issues across state lines. While newer approaches to care coordination and patient self-management may support using technology to reduce social isolation and loneliness, key infrastructure issues related to reimbursements and regulations may need to be resolved to allow for full adoption.
FINANCING OF INTERVENTIONS
Most of the interventions reviewed earlier in this chapter draw heavily on volunteers and patched together funding from various small grants and donations or are technological innovations that may base their marketing models on the sharing of data by users. While many of these programs had some positive impacts on participants, a volunteer-based model is difficult to grow or maintain on a large scale. Instead, more formal funding mechanisms are needed. The choice of funding source will depend in part on the type of intervention, the cost, and the population being served. However, because there is little scientific evidence to date on the cost and benefits of various interventions addressing social isolation and loneliness in general, and for interventions in health care settings in particular, the committee presents a discussion of funding options in a more general sense, providing a general assessment of possible paths forward.
As noted in Chapter 3, social isolation and loneliness have negative effects on health, but at the same time health limitations (e.g., auditory or mobility problems) result in significantly higher risks of social isolation and loneliness. Given these strong ties, a natural avenue for the implementation and funding of interventions is through the health care and health insurance systems. Furthermore, the 2019 National Academies consensus study report Integrating Social Care into the Delivery of Health Care describes the negative correlation between spending on social care and total health care costs that exists across countries and across states (NASEM, 2019). This correlation suggests that, in addition to improving the lives
of individuals at risk for social isolation and loneliness, investment in this area may prove cost-effective.
Given the committee’s charge to focus its attention on older Americans and the groups most at risk of social isolation and loneliness, this section begins with the potential role of the public Medicare and Medicaid program. Medicare is the primary health insurance provider for those aged 65 or older as well as for those eligible for Social Security Disability Insurance, while those older or disabled individuals with few resources have access to Medicaid. Given their target populations, these programs are well positioned to lead the way in identifying individuals at risk and in providing mechanisms to mitigate the impacts of social isolation and loneliness. Medicare is a federally run program and, as such, changes in this program directed toward social isolation and loneliness can have an impact on a large number of individuals. In 2018 there were approximately 60 million individuals enrolled in Medicare (CMS, 2019a). In contrast, Medicaid programs are run at the state level with funding from both states and the federal government. The state-level administration allows for individual states to tailor coverage to their populations and also allows for the piloting of different programs across states to provide data on numerous interventions at the same time. The total population covered by Medicaid is far larger than that covered by Medicare (approximately 75 million in 2018) (CMS, 2019a), but children make up the largest subset of beneficiaries, so the adult population covered by Medicaid is similar to that covered by Medicare.
The committee suggests three avenues along which the health care system—and particularly Medicare and Medicaid—may address these issues. The first of these avenues is through the use of traditional medical interventions targeting specific underlying health-related causes of social isolation or loneliness. The second is by financing interventions that target social isolation and loneliness, either directly or indirectly. Finally, financing may be considered for public health efforts to increase awareness of the health and medical impacts of social isolation and loneliness, both for reducing the stigma associated with social isolation and loneliness and for helping to identify those at risk. The following sections provide examples of approaches to funding interventions generally. However, the committee recognizes that relatively little is currently invested (particularly by Medicare and Medicaid) into these types of interventions, that many of the programs cited have not been evaluated for their impact specifically on social isolation and loneliness, and significant incentives will likely be needed in order for these approaches to gain traction.
Financing Interventions for Underlying Health-Related Causes
The first mechanism of financing to consider involves using traditional health care interventions that target the underlying cause of social isolation or loneliness. For example, when considering causes of social isolation and loneliness, physical barriers such as hearing or vision impairments or limitations on mobility loom large. Limitations like these make social connections more difficult and have been
demonstrated to increase the likelihood of loneliness or isolation (see Chapter 4). Medicare currently covers some mobility devices when they are medically needed, but it does not cover hearing aids or low vision devices, although these items could potentially be included in an expanded definition of “durable medical equipment.” In some states, Medicaid does cover hearing aids for those who qualify for benefits, but many states do not offer this coverage. Better coverage of hearing aids and other medically needed devices (e.g., wheelchairs, low-vision technologies) could potentially do much to help reduce the prevalence of social isolation and loneliness.18
Financing Interventions Targeting Social Isolation and Loneliness
Social isolation and loneliness might also be targeted by taking advantage of existing programs to assess or address the social determinants of health in general. The recent increase in recognition of the importance of these factors in affecting health outcomes has led to several states beginning to use their Medicaid programs to address such issues as food insecurity, homelessness, and domestic violence. Like social isolation and loneliness, these factors are strongly related to health outcomes, and improving social situations can lead to improvements in health. Although they are outside the typical scope of Medicaid programs and not required by the federal government, these types of outreach activities can be financed through Medicaid waivers that allow for pilot projects or through amendments to state Medicaid programs. While Medicaid programs have begun to address the social determinants of health among children and disabled beneficiaries, the committee has focused primarily on pilot projects that might inform outreach activities targeting older adults at risk of or experiencing social isolation and loneliness. A key component of these pilot projects is evaluation. As such, the research needed to learn about the effectiveness and best practices of these pilots, while still in its infancy, will at least begin to provide some answers in the coming years. However, a recent Government Accountability Office study found serious gaps in many demonstration projects that limited the ability to gauge the effectiveness of these programs (GAO-18-220).
Medicaid waiver programs (particularly the newest Section 1115 waivers) have been authorized by the Centers for Medicare & Medicaid Services (CMS) to allow Medicaid programs to adapt their services “to best meet their state’s unique needs” such as by expanding coverage to specific groups, providing incentives for healthy behaviors, or improving behavioral health services (NCSL, 2019). As noted by Seema Verma, the CMS administrator,
We know that behaviors and other determinants of health—like where we work, live, learn, and grow—are all factors in our overall health and wellbeing. As we
___________________
18 H.R. 2050, introduced in 2017, called for a demonstration project for the inclusion of low-vision devices.
seek to create a health care system that truly rewards value, we must consider the impact that factors beyond medical care have in driving up health costs. . . . As part of this demonstration, North Carolina will implement a groundbreaking program in select regions to pilot evidence-based interventions addressing issues like housing instability, transportation insecurity, food security, and interpersonal violence and toxic stress. (Verma, 2018)
Interventions of this type typically operate through accountable care organizations and managed care organizations and provide a number of services not normally associated with health insurance organizations. North Carolina has recently launched a pilot enhanced case management system to provide various social support services to Medicaid beneficiaries. The program includes services to help with housing, food security, and domestic violence. Examples include replacing carpet or an air conditioner for an individual with asthma and improving access to healthful food (NCDHHS, 2018). The One Care demonstration project operating through Medicare and Medicaid programs from the Commonwealth Care Alliance in Massachusetts provides a care partner to assist a patient with the social determinants of health as well as with traditional medical services. Loneliness is specifically listed as a targeted social determinant of health but the project is limited to adults younger than 65 (Commonwealth Care Alliance, 2018).
New York also has a broader program addressing the social determinants of health (NYSDOH, 2017, 2019). The New York program includes components that address economic security as well as housing and food security. Notable in the New York plan is that “social and community context” is called out as a key domain. Outreach in these areas can be provided through existing programs such as the Department for the Aging, Department of Health, Office for the Aging, senior centers, virtual senior centers, friendly visitor programs, caregiver support, and social adult day services. Similar pilot programs are operational in other states, and Medicaid managed care plans are similarly exploring ways to improve health outcomes by addressing the social determinants of health.
Medicaid waiver programs can be used as models for interventions specifically addressing social isolation and loneliness among low-income older adults and people with disabilities. An important step in reaching out with interventions along these lines is identifying those most at risk for social isolation and loneliness. Medicaid’s existing coverage of home health care services provide a ready avenue to identify at least some of those at risk for social isolation and loneliness, as do other outreach programs such as Meals on Wheels or other state- and local-run programs.19
___________________
19 Note that the Administration on Aging (AoA) operates in large part by providing funding to states and local communities to support programs addressing the well-being of older adults. A large portion of this funding goes to Meals on Wheels programs, which count on money from AoA for approximately one-third of its budget (Meals on Wheels America, 2017).
For older and disabled individuals who are not eligible for state Medicaid programs, Medicare affords similar opportunities to address social isolation and loneliness. While Medicare itself is a federal rather than state-run program, suggesting that interventions would need to be implemented more broadly, CMS recently finalized its policy to allow Medicare Advantage plans to expand benefits to cover interventions addressing the social determinants of health (CMS, 2019b), and this idea is already gaining traction with numerous private insurers (e.g., Anthem Inc., UnitedHealthcare, Kaiser Permanente) launching programs through their Medicare Advantage plans (Graham, 2019). While many of these programs focus on affordable housing, transportation, and food insecurity, the same models can be used to more aggressively target social isolation and loneliness. The idea behind these pilot projects is that by being more proactive in identifying and intervening for social isolation and loneliness or in reducing the risk, these interventions will act both to reduce total health care costs and increase well-being. Should these projects prove successful, one would imagine that private insurers serving the non-elderly and non-disabled population (i.e., those not covered by Medicare or Medicaid) would begin to consider similar interventions as cost savings mechanisms.
Outside the United States, the National Health Service in the United Kingdom has already created a system of social prescribing to encourage doctors to “prescribe” social activities and engagement. According to a recent evaluation, the most common sorts of interventions were “information and advice, community activity, physical activities, befriending and enabling” (Dayson and Bashir, 2014, p. i). The evaluation found substantial reduction in inpatient admissions, emergency department visits, and outpatient visits. It also found a substantial cost savings on the order of a 50 percent return on investment (see more on social prescribing earlier in this chapter). Similarly, the Australian government provides funding for a program in which volunteers visit low-income older adults (Sutherland Shire Council, 2018).
As described in Chapter 3, social isolation, particularly for an often less-mobile population, can have adverse outcomes on health. Increasing social activities and combating the isolation faced by many people with functional limitations and other disabilities is a key element in encouraging good overall health. The Health Plan of San Mateo found that addressing social isolation is a key to successfully transitioning individuals out of institutional care, particularly as many are leaving a very structured environment (HPSM, 2020). That organization is examining new types of peer supports and other related services to address isolation. The health plan contracts with an organization called Wider Circle,20 which facilitates an activity-based social group led by peers to support individuals with day-today living tasks. Wider Circle also emphasizes physical activity and collects some
___________________
20 For more information, see https://www.widercircle.com (accessed October 15, 2019).
data on health outcomes. The health plan acknowledged that extensive internal review are often required when these services are authorized, but because feedback received from members has been very positive, it will continue to provide these activities (Soper, 2017).
Financing Public Health Campaigns
Finally, financing needs to be considered for efforts at the society-wide level such as public health campaigns to increase awareness, remove stigma, and, more generally, enlist the public’s help in reducing social isolation and loneliness. For example, the National Institutes of Health has promoted public health campaigns about smoking, physical activity, and heart disease (NIH, 2019). (See Chapter 8 for more on public health campaigns.) Publicity campaigns like these could encourage individuals to check in on neighbors or older family members. They could also reduce stigma and thus encourage lonely older adults to reach out for help themselves. By highlighting social isolation and loneliness, public health campaigns could help individuals approaching retirement and old age better plan for meaningful engagement and connections in the future. (See Chapter 10 for more on dissemination and implementation.)
REFRAMING INTERVENTION USING A PUBLIC HEALTH APPROACH
Because of the variety of ways that social isolation and loneliness affect health and well-being, there is no single treatment that can prevent or cure every instance of social isolation or loneliness. Instead, addressing these issues will necessarily involve a variety of different actors and an assortment of interventions focused on different demographics, risk factors, and health impacts. One way to address the problems of isolation and loneliness may be through using a public health framework while designing and implementing different interventions. As defined by the American Public Health Association, “public health promotes and protects the health of people and the communities where they live, learn, work, and play,” which includes promoting wellness by encouraging healthy behaviors and assuring “the conditions in which people can be healthy.” Furthermore, public health includes “spreading the word about ways to stay healthy and giving science-based solutions to problems” (APHA, 2019). A public health framework entails designing interventions to address one of three strategies: primary, secondary, and tertiary prevention.
The aim of primary prevention is to intervene before any health effects occur, such as by changing health behaviors or changing the built environment so that exposures to hazards are decreased (IWH, 2015). Strategies that focus on primary prevention typically include clinical preventive services (e.g., immunization
or post-exposure prophylaxis for individuals exposed to a communicable disease), media campaigns raising public awareness about the link between certain behaviors and health outcomes (e.g., smoking and lung cancer, wearing seatbelts and automobile crash safety), and education aimed at personal health behaviors (e.g., oral and dental hygiene education) (WHO, 2019b). For social isolation and loneliness, primary prevention may include public health awareness campaigns and identifying individuals at high risk. Other approaches, while outside the scope of this committee’s work, might include neighborhood and city planning for housing design and community spaces that would facilitate bringing people together (e.g., common spaces for gathering, sidewalks), facilitate interactions (e.g., opportunities for volunteering, intergenerational housing), and prevent isolation (e.g., more effective public transportation).21
Secondary prevention aims to reduce the impact of a disease or illness that has already occurred by, for example, using screening or assessment to identify the earliest stages of the condition. Some examples of secondary preventions strategies are regimens of daily low-dose aspirin for individuals who have suffered from heart attack or stroke; regular mammogram screening in order to detect early breast cancer; and regimens of antiretroviral medications for individuals who have human immunodeficiency virus. In the case of social connection, secondary prevention strategies are those that attempt to target or influence existing social isolation or loneliness that is felt acutely (in other words, a temporary state of loneliness or social isolation, perhaps due to a sentinel life event). This also includes the assessment for social isolation and loneliness, as discussed in Chapter 7.
Tertiary prevention involves managing a disease post-diagnosis in order to slow or soften the impact of the disease or to stop its progression (CDC, 2017). Examples of tertiary prevention include cardiac or stroke rehabilitation programs, chronic disease management programs for diabetes or depression, and support groups for people with cancer. In the case of social isolation and loneliness, tertiary prevention strategies attempt to address chronically experienced social isolation or loneliness (in other words, “trait” loneliness). Examples include the use of CBT (see earlier in this chapter).
One important consideration in the development of interventions for isolation and loneliness is who (i.e., which actor) is responsible for carrying out these actions. Different actors will be responsible for and involved in different types of interventions. Figure 9-2 suggests levels of responsibility for interventions in loneliness. (Note that these levels of responsibility correspond to the contextual factors of the committee’s framework in Chapter 1.) The figure shows that primary prevention strategies such as public education campaigns and relevant research
___________________
21 Fried, L. 2018. PowerPoint presentation to the committee—Loneliness in older adults: Public health considerations. In Public Access Files for the Committee on the Health and Medical Dimensions of Social Isolation and Loneliness in Older Adults (received December 21, 2018).
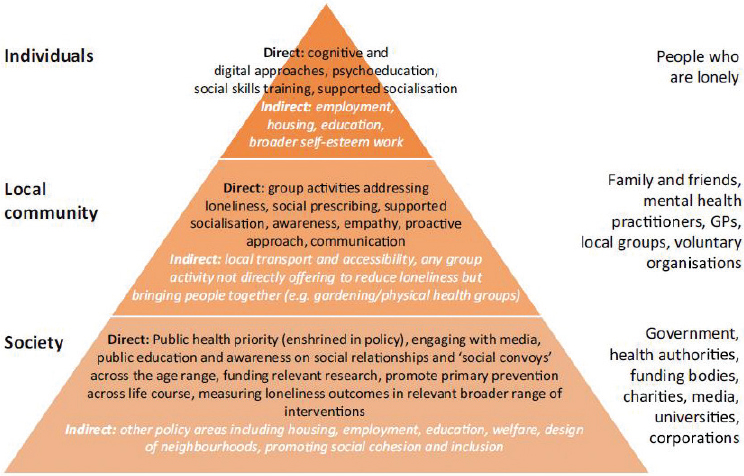
NOTE: GP = general practitioner.
SOURCE: Mann et al., 2017.
funding are the responsibility of government health authorities and nonprofit organizations. Key partners here include organizations such as the U.S. Public Health Service, the Administration for Community Living, and area agencies on aging. Secondary prevention strategies are the responsibility of community actors such as general health care practitioners and local service groups. Those responsible for tertiary prevention strategies include affected individuals and their close associates or care team, including but not limited to family and friends (Mann et al., 2017). However, all of these actors will likely need to work together in concert to address the health and medical impacts of social isolation and loneliness using this public health approach. For example, the Trust for America’s Health “is prioritizing the role of public health to improve the health and well-being of our nation’s growing older adult population” by sharing “models of public health collaborations with the aging sector” (TFAH, 2020). In another example, age-friendly health systems (an initiative of The John A. Hartford Foundation and the Institute for Healthcare Improvement in partnership with the American Hospital Association and the Catholic Health Association of the United States) seek, in part, to “know and align care with each older adult’s specific health outcome goals and care preferences” (IHI, 2020). Collaborations and partnerships such as these around public health and aging could consider their role in addressing social isolation and loneliness among older adults.
FINDINGS AND CONCLUSIONS
Interventions
- A variety of interventions have been proposed to address social isolation and loneliness. However, there is currently not enough evidence to identify the most effective interventions.
- The evidence base for interventions is limited by sample size and the length of follow-up.
- Few (if any) RCTs have been conducted on these interventions, and many interventions lack a theoretical basis.
- Features of successful interventions may include an educational approach to the intervention, the involvement of the individuals being targeted in the design of the intervention, and a strong theoretical basis for the approach of the intervention.
- Many intervention studies do not use a validated tool (as described in Chapter 6). Rather, these interventions are assessed using qualitative interviews, surveys, and internally designed measurement tools.
- Both direct and indirect interventions hold promise for ameliorating the negative health impacts of social isolation and loneliness. It is important that interventions target the underlying issue causing social isolation or loneliness, if the underlying cause is known (e.g., hearing loss or mobility limitations).
- The preservation of an individual’s autonomy is an essential ethical principle that needs to be respected for all interventions.
- As new evidence develops, a centralized sharing of resources and best practices would benefit all stakeholders.
Technology
- A significant proportion of older adults are using technologies. With education and support, technology provides an important set of opportunities for the toolkit of strategies that can help prevent or mitigate social isolation and loneliness in older adults.
- Technologically mediated interventions might be helpful adjuncts to other interventions intended to prevent or mitigate social isolation and loneliness in older adults.
- Studies of the use of the Internet and, more specifically, social media by older adults introduce mixed findings; several studies show that online tools may increase connection and decrease isolation, while others have shown no links between Internet use and perceived isolation.
- The number of studies examining social robots for social isolation and loneliness has increased significantly in recent years, but there is insufficient evidence of their effectiveness.
- Conversational agents are designed to promote engagement and address loneliness, especially for older adults with mild cognitive impairment; the majority of the evaluations of conversational agents to date have focused on short-term feasibility and acceptability.
- The digital divide, especially the rural–urban digital divide, is a major moderator of the effectiveness of many interventions. Examples of the differences observed in the digital divide include familiarity; access to equipment, software, and fees; acceptability; ease of use with physical or emotional health problems or disabilities; and literacy.
- Special population groups (e.g., different age groups, people with different levels of literacy, people with different levels of income, people with varying functional status, and various racial, ethnic, and cultural groups) need to be considered when designing technological solutions to social isolation and loneliness for older adults.
- Clinician familiarity with technological strategies to improve health, including the prevention or treatment of social isolation and loneliness, is influenced by time, reimbursement strategies, and regulatory issues.
- As with other areas of health care, ethical and legal considerations especially must be explored when the technology is used in interventions for isolation and loneliness.
Financing of Interventions
- Current interventions are largely supported by volunteers, with much of the financial support coming from grants and donations. This is an unsustainable financing model.
- The availability of adequate resources to support and sustain interventions is key to their long-term success.
- Many efforts to develop newer approaches to the funding of interventions (largely for interventions directed at the social determinants of health in general) have not been evaluated for their impact on social isolation and loneliness specifically.
- The committee notes the following findings from the consensus study report Integrating Social Care into the Delivery of Health Care (NASEM, 2019):
- Within existing definitions of health care, state Medicaid programs and their contracted managed care plans and accountable providers are innovating with . . . activities to pay for social care in health care settings using state plan amendment authority and the waiver process (p. 7).
- There remains great variation among states in the level of social care activity; CMS provides only limited guidance about permissible social care activities and benefits (p. 7).
- Medicare’s new supplemental benefits guidance to Medicare Advantage plans . . . has created new opportunities to integrate social care into the health care of Medicare beneficiaries (p. 7).
- Patients enrolled in both Medicaid and Medicare have the highest social needs, but the division of their health care financing between state and federal agencies creates barriers to addressing those needs in a way that integrates social care (p. 9).
- Social service agencies and health care organizations have historically not worked together, and they are funded by different systems (p. 9).
NEXT STEPS AND RECOMMENDATIONS
The committee identified two key areas that need to be addressed related to interventions overall: strengthening community-based networks and resources and improving the overall evidence base.
Strengthening Ties to Community-Based Networks and Resources
Chapters 2 through 4 of this report show that social isolation and loneliness have wide-ranging health and medical impacts and are associated with a vast array of risk factors. Like other social determinants of health, social isolation and loneliness are community-wide problems and require coordinated solutions between the health care system and community-based social service providers. National, state, and local coalitions of public and private health care leaders, including minority-based community organizations, need to work collectively to develop strategies to address social isolation and loneliness in older adults. A report of the Campaign to End Loneliness recommended that service providers make connections with others in order to address the full range of needed supports and services, stating “Providers need to assess what contribution they make to the overall framework of loneliness interventions and build the necessary partnerships to deliver more effectively with other providers” (Jopling, 2015, p. 59).
As noted earlier, cross-sector coalitions and partnerships are two strategies for increasing assistance, alignment, and advocacy activities in order to integrate social care into health care. The committee concludes that such partnerships are similarly needed in order for the health care system to help address social isolation and loneliness in older adults. Therefore, the committee identifies the following goal and recommendations:
GOAL: Strengthen ties between the health care system and community-based networks and resources that address social isolation and loneliness in older adults.
RECOMMENDATION 9-1: Health care providers, organizations, and systems should partner with social service providers, including those serving vulnerable communities, in order to create effective team-based care (which includes services such as transportation and housing support) and
to promote the use of tailored community-based services to address social isolation and loneliness in older adults.
In particular, the committee notes that many health care organizations (e.g., hospitals) are required under federal law to submit community benefit reports. Efforts by such entities to partner with social service providers could be used as an example of their community benefit efforts. As an example of tailored community-based services, the 2019 National Academies consensus study report Integrating Social Care into the Delivery of Health Care cites examples of assistance and alignment as including the provision of transportation vouchers that can be used for ride-sharing services or public transit and the investment in community ride-sharing programs (NASEM, 2019). In the case of social isolation and loneliness, such services would allow individuals to travel to health care appointments and also to overcome individual transportation-related barriers to participation in local community events.
A variety of stakeholders, both within and outside the formal health care system, are testing new approaches to preventing, identifying, and intervening for social isolation or loneliness for older adults. The committee concluded that as new evidence develops, a centralized sharing of resources and best practices would benefit all stakeholders. The committee noted that the U.S. Department of Health and Human Services has funded resource centers aimed primarily at health and social care professionals on a variety of topics that are of wide interest for the care of older adults (HHS, 2019d). Existing centers include the National Falls Prevention Resource Center, the National Clearinghouse for Long-Term Care Information, the National Resource Center on Nutrition and Aging, and the National Resource Center on LGBT (Lesbian, Gay, Bisexual, and Transgender) Aging. These resource centers not only serve as centralized resources for information, but also may provide training and technical assistance (Meyer and Johnston, 2014). Therefore, the committee makes the following recommendation:
RECOMMENDATION 9-2: Given the public health impact of social isolation and loneliness, the U.S. Department of Health and Human Services should establish and fund a national resource center to centralize evidence, resources, training, and best practices on social isolation and loneliness, including those for older adults and for diverse and at-risk populations.
Improving the Evidence Base on Interventions
The committee found that the overall quality of the evidence for specific interventions for social isolation and loneliness in older adults, particularly for interventions related to health care providers, is mixed. Current research uses a variety of definitions, measures, outcomes, and length of follow-up. Furthermore, the population of older people aged 50 and older are heterogeneous in their personal characteristics, their specific needs, and the underlying causes of their social
isolation and loneliness (if present). While there is some evidence for promising approaches, the committee concluded that researchers are only beginning to understand which specific approaches work best for which people and which risk factors. In particular, the committee emphasizes that as social isolation and loneliness are distinct concepts, different intervention approaches may be needed to address each of them.
As discussed in Chapter 7, the health care system has a key role to play in helping to improve the evidence base on effective interventions. To that end, a report from the Campaign to End Loneliness cautions:
As long as there is a shortage of evidence of the impact of loneliness initiatives, there will always be an excuse not to fund this vital work. External evaluations are costly, but all organisations can build into their programmes the opportunity to gather data about their impact. By using recognized and accredited tools, even if only with a sample of service users, we can start to create a reservoir of comparable data, improving the evidence base and building a clearer picture of which initiatives work best and why. (Jopling, 2015, p. 59)
Furthermore, the report notes:
There is a huge shortage of evidence of the impact of loneliness initiatives on minority communities, such as LGBT and BME [black, minority, and ethnic] older people, and older people who live in care homes. This is not necessarily because initiatives do not serve these communities, but because providers have not yet gathered the data that proves that they do, and we do not know enough to be able to work out which approaches work best. Providers need to make sure that the needs of these minority communities are built into service planning, and that efforts are made to evaluate the impact on these groups in particular. (Jopling, 2015, p. 59)
When it comes to specific technological interventions, many gaps in our understanding remain, particularly related to potential unintended harms and ethical concerns. Also, little is known about how current trends, such as the use of social media, will affect social isolation and loneliness in future generations of older adults.
In accordance with the committee’s previously identified goal of developing a more robust evidence base on effective prevention, assessment, and intervention strategies for social isolation and loneliness in older adults, the committee identified three major aspects of the overall evidence base for effective clinical interventions that need to be addressed in order to determine best practices and approaches. First is to improve the breadth and overall quality of the evidence for interventions in clinical settings. The committee notes that along with recommendations for research in Chapters 2 and 3, the development of a more robust evidence base is key to identifying effective interventions that might be scaled rather than investing in random interventions. Second is to increase the overall
funding for such studies. Third is to target research to major gaps in the current evidence base. Within this context, and as noted in Chapter 7, the committee emphasizes that the preservation of an individual’s own decisions regarding his or her life (e.g., living arrangements, community participation) is essential as a guiding principle for all interventions. (See Chapter 10 for more on engaging with the recipients of interventions.)
RECOMMENDATION 9-3: Funders should prioritize research that builds a scientific foundation for clinical and public health interventions that reduce the health and medical impacts of social isolation and loneliness based on standard theoretical frameworks. Researchers and health care providers and systems that study interventions for social isolation or loneliness should consider the following key elements in the design and evaluation of any intervention in order to enhance the ability to compare across studies:
- A theoretical framework that drives particular approaches
- Appropriate choice of measure
- Specific target population
- Scalability
- Sustainability
- Ways to encourage data sharing
For the above recommendation, because of the variability in research designs to date, it is especially important for researchers to describe the theoretical frameworks driving their approaches in order to build a more coherent body of knowledge.
RECOMMENDATION 9-4: Major funders of health research, including the government (e.g., the National Institutes of Health, the Center for Medicare & Medicaid Innovation, and the Patient-Centered Outcomes Research Institute), foundations, and large health plans, should fund research on effective interventions in clinical settings to identify, prevent, and mitigate the effects of social isolation and loneliness in older adults.
RECOMMENDATION 9-5: Those who fund, develop, and operate programs to assess, prevent, and intervene in social isolation and loneliness should prioritize research on the following major gaps in the evidence base:
- Tailored interventions based on a public health framework of primary, secondary, and tertiary prevention. In particular, researchers should examine improved measures to identify individuals who may be at high risk for social isolation or loneliness and primary interventions in order to target such individuals.
- Trends among current younger adults as they age (e.g., use of technology, economic trends) to gain knowledge that informs future approaches to addressing social isolation and loneliness.
- Flexibility in funding to allow for the pilot testing and evaluation of innovative funding mechanisms for interventions.
- Approaches for assessments of and interventions among understudied groups of older adults (e.g., low income, lesbian, gay, bisexual, transgender) and those who face unique barriers to health.
RECOMMENDATION 9-6: System designers as well as those who are developing and deploying technology in interventions should ensure that technological innovations related to social isolation and loneliness are properly assessed and tested so as to understand their full range of benefits and potential adverse consequences in order to prevent harm, and they should work to understand and take into account contextual issues, such as broadband access and having sufficient knowledge and support for using the technology.


















































