5
Mediators and Moderators
The Statement of Task charged the committee to consider “factors that moderate and mediate the links between social isolation/loneliness and health outcomes.” By identifying the moderators and mediators of the effects of social isolation and loneliness, one can explore the mechanisms underlying those effects as well as why the effects may differ from one population to another and under which conditions an effect may be stronger or weaker (MacKinnon and Luecken, 2008). Mediators (i.e., mechanisms or pathways) are the factors that help explain how social isolation or loneliness affects health outcomes, while moderators are the factors that can influence the magnitude or direction of the effect of social isolation or loneliness on health. Identifying mediators helps explain the mechanisms, or plausible pathways, by which social isolation and loneliness influence health outcomes, while identifying moderator variables helps to determine whether the health effects of social isolation or loneliness are stronger for some groups than for others.
This chapter represents the portion of the committee’s guiding framework related to the mediators and the moderators (largely at the individual level) of the associations between social connections and health outcomes (see Figure 5-1). (See Chapter 1 for more on moderators at the level of the community and society.) Current evidence suggests that there are multiple mediators that each may influence health (see Figure 5-2). This report does not provide an exhaustive review of all known mechanisms. Rather, the following sections summarize the current evidence concerning a few key mechanisms that exert critical roles in explaining the association between social connections and health outcomes. Then the chapter identifies and summarizes the evidence for several variables that have been identified as potential plausible moderators.
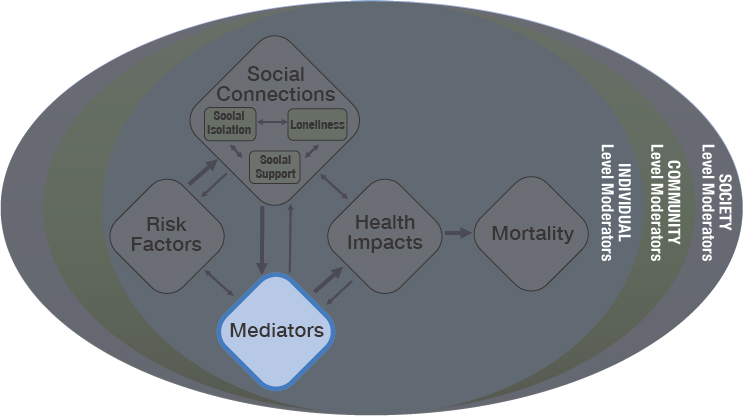
As noted in earlier chapters, this chapter uses the term “social connection” as an umbrella term that includes aspects of social isolation, loneliness, and social supports. Social isolation and loneliness are referred to specifically in line with available evidence. Given the complexity of the terminology used in relation to social isolation and loneliness, a reminder of key definitions is provided in Box 5-1.
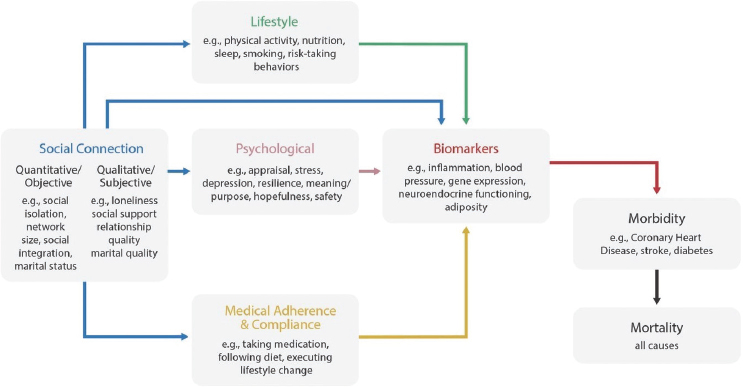
SOURCE: Holt-Lunstad and Smith, 2016.
MEDIATORS: BEHAVORIAL, PSYCHOLOGICAL, AND BIOLOGICAL MECHANISMS
The mechanisms by which social connection—or the lack thereof—affects the development and course of disease have been elucidated by a robust and growing evidence base. Much of this evidence emerged in the context of examining the protective effects of social relationships and social support; however, this work relates specifically to both social isolation and loneliness. Relevant to social isolation are the experimental studies that randomly assign participants to either a social or an alone condition. In animals, this meant studying some animals housed in isolation versus others housed socially. In humans, many experimental studies examined physiological responses in an individual performing a task (typically stressful) in either the presence of or receiving support from someone (e.g., stranger) and contrasted that with a control condition (e.g., being alone). Later, more nuanced approaches were used to systematically examine aspects of social connection. Examples include testing in the presence of a stranger versus a friend (or other relationship types, such as spouses), having a wide social network versus a small network (even if not present), and observing the effects of perceived availability of social support. Evidence about biological mediators also comes from non-experimental studies. For example, it may not be possible to use random assignments to examine biological responses in everyday life or to study
clinical populations. Thus, field studies are often employed in which biomarkers are collected.
Several reviews and meta-analyses link social support to changes in cardiovascular, neuroendocrine, and immune function (Uchino, 2006). Figure 5-2 illustrates different theoretical perspectives of the mechanisms that mediate the relationship between social connection and morbidity and mortality (Berkman et al., 2000; Cohen, 1988; Thoits, 1995; Umberson, 1987). The committee highlights some of these pathways in the following sections.
Health-Related Behaviors (Lifestyle)
As discussed in Chapter 3, heath-related behaviors can mediate the relationship between social isolation or loneliness and health outcomes. Social isolation and loneliness or the characteristics of one’s social networks may affect health-related behaviors (e.g., smoking, physical inactivity), which in turn can affect health, either positively or negatively. One study of nearly 8,600 older adults found that “physical inactivity, daily smoking, and poor sleep mediated the association between loneliness and adverse health conditions” (Christiansen et al., 2016, p. 80). As with other factors, health-related behaviors may have a bi-directional relationship with social isolation and loneliness in that health-related behaviors can also exacerbate or reduce social isolation and loneliness. For example, household-based physical activity is associated with reduced social isolation (Robins et al., 2018). In one study with older adults, participation in the SilverSneakers® group exercise program directly decreased social isolation through membership in the program; that is, the greatest impact came from the membership itself in that members were less likely to be socially isolated than nonmembers (Brady et al., 2020). Furthermore, SilverSneakers® members had decreased feelings of loneliness associated with their improved overall health. The practice of tai chi has been associated with reductions in loneliness (Chan et al., 2017; Park and Park, 2010). (See Chapter 9 for more on exercise as an intervention.) Participation in an exercise program for health may lead to reductions in social isolation or loneliness due to the social nature of the program rather than the exercise itself. However, there is some evidence that exercise can help to improve sleep patterns and reduce inflammation (Asian Scientist Newsroom, 2014; Kline, 2014; Park and Park, 2010; Woods et al., 2012).
Sleep
While much of the research on health-enhancing behaviors focuses on smoking, nutrition, and physical activity, a growing body of research points to sleep as vitally important to health. Sleep influences a variety of physical health conditions, including cardiovascular disease, weight gain and obesity, diabetes, and metabolic syndrome, and poor sleep has been associated with an increased mortality risk. Multiple studies have demonstrated a robust association between social
support and favorable sleep outcomes, and a lack of social and emotional support significantly predicts insufficient sleep (Kent de Grey et al., 2018; Williams et al., 2016). Social isolation and loneliness have been identified as key factors that alter the quantity and quality of sleep, which in turn influences health and safety at work (Magnavita and Garbarino, 2017). Loneliness has been linked to increased sleep fragmentation and sleep quality, leading to negative effects on metabolic, neural, and hormonal regulations (Cacioppo et al., 2002; Davidson and Rossall, 2015; Hawkley et al., 2010a; Jacobs et al., 2006; Kurina et al., 2011; Valtorta et al., 2016a). Thus, social isolation and loneliness may influence health via poorer sleep, while greater social support may lead to better health via more favorable sleep.
Medical Adherence
One way in which social relationships influence health is through their influence on adherence to medical advice. Adherence, or cooperation with medical treatment recommendations, can have a significant impact on medical outcomes; however, 25–40 percent of individuals are non-compliant, which leads to poorer health outcomes (DiMatteo, 2004; DiMatteo et al., 2000). Support from significant relationships can encourage greater responsiveness to recommendations. A systematic meta-analysis, including 122 empirical studies, examined the effects of structural and functional aspects of social connection on medical adherence (DiMatteo, 2004). The study found that most measures of social connection were significantly related to medical adherence; however, functional measures (e.g., social support) were stronger predictors of adherence than structural measures (e.g., marital status, living alone). When examining social support specifically, practical support more strongly predicted adherence than did emotional support. Thus, being socially isolated and lacking social support significantly reduces medical adherence, which may partially explain poorer health outcomes.
Psychological Pathways
As noted in Figure 5-2 there are several potential psychological pathways by which social connections influence morbidity and mortality. The following sections provide the evidence for stress and depression being examples of these pathways.
Stress
Relationships can help individuals cope with stress through the presence of other people who can provide advice on how to handle a problem (i.e., informational support), provide assistance or resources to handle the actual situation (e.g., tangible support such as a ride, loan, or meal), help the individual feel better
(i.e., emotional support), or communicate that one is loved or cared for (i.e., belonging support). The stress-buffering model argues that this social support in turn buffers the pathogenic influence of stress (Cohen and Wills, 1985). A number of studies show that social support attenuates the physiological stress response (Che et al., 2018). Many reviews have looked at the mechanisms by which the stress-buffering effect operates (Brown et al., 2018; Ditzen and Heinrichs, 2014; Hostinar, 2015; Hostinar and Gunnar, 2015; Robles and Kiecolt-Glaser, 2003).
Conversely, not having relationships that one can rely on (i.e., social isolation) in times of need can be expected to result in poorer physiological stress responses. In a systematic review of 11 studies on loneliness, higher levels of loneliness were associated with heightened blood pressure and inflammatory reactivity to stress (Brown et al., 2018). Stress reactivity may be one potential way in which social isolation, loneliness, and social support influences biomarkers of health. It is important to note that the behavioral and psychological mechanisms are not independent and may influence the other. For example, stress can negatively influence health behaviors (e.g., Ng and Jeffery, 2003) while health behaviors (e.g., exercise) can reduce perceptions of stress (e.g., Rejeski et al., 1992).
Anxiety and Depression
Additional research points to other psychological pathways, including anxiety and depression. Several studies have linked social support to lower rates of depression and greater subjective well-being. For example, one study found that that depression increased as in-person social contact decreased and that individuals with lower rates of in-person social contact had “a significantly higher probability of clinically significant depressive symptoms 2 years later” (Teo et al., 2015, p. 2). Furthermore, in older adults both social isolation and loneliness have been shown to independently affect the probability of suffering from depression or anxiety (Domènech-Abella et al., 2019), providing evidence of the bi-directionality of anxiety and depression with social isolation and loneliness. Thus, social isolation, loneliness, and social support may influence health via the impact on these psychological factors, which in turn influence biomarkers of health.
Biological Mechanisms (Biomarkers)
While social connection may influence biological mechanisms via behavioral and psychological pathways, there is also evidence of a direct influence (as noted in Figure 5-2). Indeed, much of the evidence establishing the overall effect of social connection came from studies that adjusted for relevant lifestyle (e.g., smoking, alcohol, physical activity) and psychological (e.g., depression) factors, indicating that social connection influences mortality independently of such factors. Further evidence documents the direct influence that social connection may have on health-relevant physiological pathways.
According to Cole and colleagues (2007), “a large body of epidemiological research has linked characteristics of the social environment to human physical health, but the genomic mechanisms of these effects remain largely unexplored” (p. R189.2). Research is emerging on how social conditions influence gene expression. While most studies of gene expression differences in lonely and socially isolated individuals versus socially connected individuals are not focused on older adults, many studies provide insight as to the role of gene expression in mediating the relationship between social connection and health, and the potential to identify biomarkers as targets for intervention (Cole et al., 2007, 2011, 2015a,b; Murray et al., 2019; Slavich and Cole, 2013). Intersecting with gene expression, activity of the central nervous system may also have a role in mediating the effects of social isolation and loneliness on health (Cacioppo et al., 2014; Canli et al., 2018). The following sections summarize the evidence for several biological pathways, including cardiovascular, neuroendocrine, and immune or inflammatory pathways.
Cardiovascular
Given the strong links that social isolation and loneliness have with risks for cardiovascular disease (see Chapter 3), it is critically important to understand how social relationships influence the underlying molecular processes. Recurring interpersonal experiences and their physiological effects may be an important pathway linking social relationships and coronary heart disease. Loneliness and social stress have been associated with the activation of the hypothalamic–pituitary–adrenocortical (HPA) axis and the sympathetic nervous system, and “repeated and chronic social stress leads to glucocorticoid resistance, enhanced myelopoiesis, upregulated proinflammatory gene expression, and oxidative stress” (Xia and Li, 2018, p. 837), although how loneliness-associated cardiovascular disease may develop as a result of these mechanisms is unclear. Researchers have linked social isolation and loneliness to elevated vascular resistance and heightened blood pressure (Hawkley et al., 2006, 2010b) and to higher rates of metabolic syndrome (Blanquet et al., 2016; Whisman, 2010). Meta-analyses indicate that loneliness is associated with atypical physiological reactivity to acute stress, including exaggerated blood pressure and inflammatory reactivity (Brown et al., 2018). Social isolation is associated with a higher resting heart rate, higher systolic blood pressure, and larger total/high-density lipoprotein cholesterol ratio response to stress (Grant et al., 2009; McCrory et al., 2016).
Strong evidence also links greater degrees of social support to cardiovascular functioning that confers lower risk for disease (Uchino, 2006). This evidence comes from laboratory-based studies that experimentally manipulate social situations, from field studies that monitor cardiovascular function in daily life, and from longitudinal studies that examine the long-term effects of social conditions. Lab-based paradigms examine conceptual links between social isolation, loneliness, or social support and the reactivity hypothesis of disease (Lepore, 1998)—that is,
that high levels of cardiovascular reactivity (e.g., blood pressure or heart rate) are related to a higher risk for the development and exacerbation of cardiovascular disease (e.g., Brindle et al., 2018; Chumaeva et al., 2010; Gianaros et al., 2002; Heponiemi et al., 2007; Smith and Jordan, 2015; Uchino et al., 1996). Several studies have also found that particularly for older adults, social support is associated with lower resting blood pressure (Ong and Allaire, 2005; Uchino et al., 1995, 1999). Social support has also been linked to lower ambulatory blood pressure in everyday life (Gump et al., 2001; Linden et al., 1993; Spitzer et al., 1992; Steptoe et al., 2000). Finally, higher cumulative social support has been associated with lower odds of high blood pressure (Hernandez et al., 2014).
Neuroendocrine
The major neuroendocrine systems involved in the stress response are the HPA and the sympathetic adrenomedullary axes. Given that social connections (or the lack thereof) can either blunt or exacerbate stress responses, these may be important pathways to consider. For instance, loneliness is associated with increased HPA activity, specifically an increase in the level of stress-sensitive glucocorticoids (cortisol in humans). Research has linked the HPA axis with trait loneliness (associated with a flattening of the diurnal cortisol curve), daily loneliness (a cortisol awakening response on the following day), and momentary increases in loneliness (momentary cortisol increases in youth who also had high interpersonal stress) (Doane and Adam, 2010). Research in animal models that experimentally manipulate social threat and social isolation has demonstrated that social isolation can have a causal effect on neuroendocrine functioning (Cacioppo et al., 2015a). And loneliness in older adults has been associated with lower cortisol output (Schutter et al., 2017).
Glucocorticoids regulate physiological functions, including immune, metabolic, cardiovascular, and reproductive functioning, as well as neurodegeneration and apoptosis (Cacioppo et al., 2015a; Xia and Li, 2018). This suggests that the association between loneliness and health may be mediated in part by the dysregulation of the neuroendocrine system (Hackett et al., 2012). Conversely, there is a vast literature documenting the buffering effects, or better regulation of the HPA, associated with social bonding and social support. Hostinar and colleagues (2014) provide a review of the psychobiological mechanisms underlying social buffering of the HPA.
Inflammation
Chronic inflammation has been linked to diseases such as heart disease, stroke, some cancers, and autoimmune disorders, so it is possible that there is a common pathway underlying the broad health effects of social connection on multiple disease outcomes. In particular, a meta-analysis of 41 studies (including more than 73,000 participants) established the influence of social connectedness
(specifically, social support and social integration) on inflammation (Uchino et al., 2018), suggesting that social connectedness may be implicated in inflammatory-related disease development and exacerbation. Other research has shown that objective markers of social connection may be just as important as individual perceptions in terms of their effects on these health risks. For example, in one study, ratings of an individual’s social connections as assessed by friends and family were more predictive of fibrinogen levels (a biomarker of inflammation and cardiovascular risk), than that individual’s own ratings (Kim, D. A., et al., 2016). These data suggest that the social connections themselves may have an objective influence on inflammation that is just as important as—if not more important than—the individual’s perceptions.
Conversely, a lack of social connections has been linked to worse inflammation. Another review finds
(1) that exposure to social stressors increases pro-inflammatory activity, (2) that individuals who are more socially isolated (i.e., lonely) show increased proinflammatory activity, and (3) that individuals who are more socially isolated show increased pro-inflammatory activity in response to an inflammatory challenge or social stressor. (Eisenberger et al., 2017, p. 242)
In the Midlife in the United States study, a positive significant relationship was seen between loneliness and three systemic inflammation biomarkers—interleukin-6, fibrinogen, and C-reactive protein—after controlling for covariates (Nersesian et al., 2018). This finding is consistent with research that has linked loneliness to stronger inflammatory responses (Cole et al., 2007, 2011; Hackett et al., 2012; Jaremka et al., 2013a; Steptoe et al., 2004).
As mentioned earlier, studies of gene expression may provide insight regarding opportunities for intervention. For example, a small randomized controlled trial showed that a mindfulness-based stress reduction program downregulated the loneliness-related pro-inflammatory gene expression in older adults (aged 55–85) (Creswell et al., 2012).
Summary of the Evidence for Mediators
Social connection has a dose–response effect on physiological risk markers across age groups. Yang and colleagues (2016) used data from four nationally representative longitudinal samples of the U.S. population to assess
the prospective association of both structural and functional dimensions of social relationships (social integration, social support, and social strain) with objectively measured biomarkers of physical health (C-reactive protein, systolic and diastolic blood pressure, waist circumference, and body mass index) within each life stage, including adolescence plus young, middle, and late adulthood, and compare such associations across life stages. (Yang et al., 2016, p. 578)
They found that “a higher degree of social connection was associated with a lower risk of physiological dysregulation in a dose–response manner in both early and later life” (Yang et al., 2016, p. 578). Conversely, lower social connection (social isolation) was associated with higher risk. This provides strong evidence that social relationships influence health and longevity via these risk markers.
Growing evidence from both animals and humans suggests that the social environment, particularly social adversity,1 influences the regulation of genes, and it has also been linked to epigenetic changes (Tung and Gilad, 2013). Thus, in addition to the cardiovascular, neuroendocrine, and immune consequences of social relationships, there is now evidence (both correlational and causal) that an individual’s social environment plays a critical role in regulating a large number of genes, many of which are also associated with susceptibility to other external stressors and some diseases (Tung and Gilad, 2013).
MODERATING FACTORS INFLUENCING MORTALITY AND HEALTH OUTCOMES
The effects of social connection on mortality risk are well established (see Chapter 2), as is the evidence of plausible biological mechanisms that explain these effects, which has led to a growing interest in factors that may influence the strength or direction of these effects. Examining such moderators helps determine whether some groups may be more affected by social isolation and loneliness than others. The previous section summarized how social connection influences health, but the data suggest that biological systems are also influenced by early experiences, developmental factors, and genetics, which can moderate this effect (Ditzen and Heinrichs, 2014; Hennessy et al., 2009; Uchino, 2009a,b). While there may be several other potential moderators, this section specifically considers factors relevant to the committee’s Statement of Task, such as age, gender, ethnicity, and socioeconomic status (SES). Furthermore, the evidence concerning relationship quality as a moderator of the association between social connection and health outcomes is described.
Age and Developmental Processes
Naturally, the risk of mortality increases with increasing age. The question arises, however, of whether the effects on mortality of social isolation, loneliness, or social support also increase with age. The meta-analysis by Holt-Lunstad and colleagues (2010) summarized in Chapter 2 synthesized data across
___________________
1 Social adversity includes “acute or chronic exposures which hypothetically would impact on health mainly by directly threatening salient relationships” (Gustafsson et al., 2012, p. 119). Examples include parental loss, mother–infant separation, residential instability, and social isolation (Gustafsson et al., 2012; Tung and Gilad, 2013).
148 prospective studies and found no effect of age, suggesting no difference in the overall effect of various indicators of social connection on mortality risk. However, the majority of these studies used older samples. In a subsequent meta-analysis that focused specifically on the effects of social isolation, loneliness, and living alone on mortality risk, the authors compared the effects among individuals above 65 years old with the effects among younger individuals and found that the mortality risk for those under age 65 was more affected by the social factors than the mortality risk for those over age 65 (Holt-Lunstad et al., 2015). Additional prospective studies have examined the effects of age more directly. For example, a recent study examining social isolation across young, middle-aged, and older adults found a dose–response effect on a variety of health outcomes (Hämmig, 2019). Early life experiences may also influence one’s risk trajectory later in life. For example, several studies now demonstrate that adverse childhood experiences have lasting negative consequences (Caspi et al., 2006; Danese et al., 2009; Lacey et al., 2014). Therefore, while the data in this area are not robust, newer evidence seems to suggest that age may moderate the impact of social isolation and loneliness on mortality risk, with greater risk seen among younger ages.
Demographic Factors
Demographic characteristics including gender, SES, and ethnicity all may influence the relationship between social connections and health outcomes.
Gender
Examining the larger literature via available meta-analytic data indicates that the protective effect of social relationships and the risks associated with social isolation broadly and with loneliness and living alone specifically were similar for men and women (Holt-Lunstad et al., 2010, 2015). Despite prior research suggesting that women have larger social networks than men (Antonuci and Akiyama, 1987; Matud, 2004), gender is not a significant moderator of the relationship between social support and mortality. Similarly, when looking just at loneliness across studies of the risk for all-cause mortality, no significant differences were found by gender, though the strength of the association was slightly higher in men than in women (Rico-Uribe et al., 2018). These data suggest that the effect of relationships on mortality from all causes is consistent for both men and women. These results are consistent with work looking at gender differences in the prevalence of loneliness. A meta-analysis by Maes and colleauges (2019) covering nearly 400,000 individuals synthesized the available evidence on gender differences in loneliness across the lifespan and demonstrated nearly a zero overall effect; furthermore, any effect of age was negligible. Thus, levels of loneliness are similar for males and females across the lifespan.
Socioeconomic Status
Given the research suggesting that SES may significantly influence health outcomes, many epidemiological studies statistically control for SES, making it difficult to determine whether the impact of social isolation and loneliness on health and mortality may depend on SES. There is some evidence to suggest that the prevalence of loneliness may differ by SES. For example, one study found that among the (economically) poorest people, older adults were less likely to be lonely than those in the younger groups, while among the richest there was no difference in loneliness by age (Domènech-Abella et al., 2017). Cundiff and Smith (2017) found that the collective effect of recurrent and chronic exposures to a variety of stressful interpersonal experiences (e.g., reduced support, work stress, negative stereotypes) may help explain the increased prevalence of chronic psychosocial vulnerabilities among individuals in lower socioeconomic environments, and further link those psychosocial vulnerabilities to the transient physiological mechanisms (i.e., stress responses) that directly affect coronary heart disease. Nonetheless, the evidence base is not robust, and more large-scale research is needed to further elucidate the potential moderating effects of SES.
Race and Ethnicity
The majority of epidemiological studies do not report effect sizes for social isolation, loneliness, social support, or other aspects of social connection that are broken down by race or ethnicity. Therefore, researchers have not been able to adequately examine this factor meta-analytically. Some evidence suggests that the prevalence of loneliness may differ by ethnicity (Jamieson et al., 2018); however, most of these studies did not examine the moderating effect of ethnicity on health or mortality. Nonetheless, some studies provide some illuminating evidence. For example, one study found that, contrary to expectations, social isolation in older black men did not significantly predict metabolic disorders (Das, 2013). In another study both loneliness and social disconnectedness had a significant negative association with physical and mental health among white older adults; however, among African American older adults social disconnectedness was associated with worse physical health and loneliness and associated with worse mental health (Miyawaki, 2015). One of the strongest studies to date was a 10-year U.S. population-based prospective study that examined ethnic and racial variation in social integration2 and its effect on mortality among participants of the U.S. National Health Interview Survey (Barger and Uchino, 2017). This study found no significant effect of received social support on mortality among any of the groups (i.e., white, black, Hispanic), but social integration demonstrated a significant effect on survival among all three groups. Consistent with other research, there was
___________________
2 Low social integration scores are a marker of social isolation.
a dose–response effect among whites, but the gradient was flatter among blacks, and a survival advantage was found only at the highest levels of social integration. Among Hispanics the survival advantage was present at all but the lowest levels. Thus, “extreme group contrasts (i.e., contrasting the highest and lowest social integration categories) also obscures different forms of the mortality gradient for black, white and Hispanic participants” (Barger and Uchino, 2017, p. 4).
Relationship Quality
While the absence of others (i.e., social isolation) is detrimental to health, the presence of others may not necessarily be entirely positive or protective. While social relationships can be characterized by a myriad of positive attributes (e.g., intimacy, companionship, nurturance, joy, and compassion), some relationships are characterized by negative attributes (e.g., conflict, insensitivity, jealousy, burden, rejection, neglect, or even abuse) (Rook and Charles, 2017). These attributes may influence the magnitude and direction of the associations between relationships and health. Multiple studies have demonstrated that negativity in social relationship predicts greater risk for mortality (Birditt and Antonucci, 2008; Friedman et al., 1995; Tanne et al., 2004; Tucker et al., 1996). For example, in a study of breast-cancer patients by Kroenke and colleagues (2013), women with small social networks and low levels of social support and small networks had a significantly higher risk of mortality (Kroenke et al., 2013). Additionally, “larger social networks predicted better prognosis after breast cancer, but associations depended on the quality and burden of family relationships” (Kroenke et al., 2013, p. 261). Similarly, poor-quality relationships and relationship strain were found to more than double the risk of depression 10 years later (Teo et al., 2013b). Thus, in medical settings if relationship quality is ignored it may lead to higher risk rather than lower risk.
Indeed, a broad literature documents the protective effects of marriage in terms of reducing risk for mortality (Manzoli et al., 2007; Rendall et al., 2011) and loneliness (Cohen-Mansfield et al., 2016); however, not all marriages are high quality, and there is evidence that marital quality is an important moderator. For example, a meta-analytic review of 126 studies found that marital quality was inversely associated with a variety of health outcomes, including mortality risk (Robles et al., 2014). Similarly, distressed marriages have been associated with poorer immune outcomes (Price et al., 2018) and greater morbidity and mortality risk (Choi and Marks, 2011; Kimmel et al., 2000; King and Reis, 2012; Robles and Kiecolt-Glaser, 2003; Robles et al., 2014). Thus, when assessing for social isolation or loneliness practitioners should not assume a lack of risk based on marital status alone.
Studies done in clinical settings offer evidence that relationship quality can significantly influence treatment adherence. A meta-analysis by DiMatteo (2004) found that adherence to medical regimens was lower in patients from families in conflict and higher in patients from cohesive families. Furthermore, the social
conflict that arises as a result of a well-intended efforts to encourage medication adherence (that may be interpreted as nagging or attempts to exert control) has been shown to reduce (rather than increase) medication adherence (Warner et al., 2013). However, another study among people with a chronic illness showed that negative social relations at baseline were associated with decreased risk for mortality (Birditt and Antonucci, 2008), and the authors suggested that this may be due to the buffering effect of social control. Thus, it cannot be assumed that medical adherence will be always be enhanced by increasing family or staff involvement.
There is substantial evidence that the quality of relationships also influences biomarkers of health. For example, studies examining the influences of cardiovascular functioning have found that positivity in social relationships (e.g., support, satisfaction) is associated with protective effects, while negativity (e.g., strain, conflict) and ambivalence in relationships are associated with deleterious cardiovascular functioning (e.g., elevated blood pressure, cardiovascular reactivity) (Birmingham and Holt-Lunstad, 2018; Holt-Lunstad and Uchino, 2019; Robles, 2014). Similarly, poor-quality relationships more than doubled the risk of depression 10 years later (Teo et al., 2013b).
FINDINGS AND CONCLUSIONS
Mediators
- Strong evidence links loneliness, social isolation, and social support to changes in cardiovascular, neuroendocrine, and immune function as well as to the physiological stress response. A lack of social connections has been linked to higher levels of inflammation, which may point to a plausible biological mechanism for the association of social isolation and loneliness with a variety of negative health outcomes.
- Social isolation and loneliness have been linked to decreased quality of sleep, which itself can influence a variety of physical health conditions, including cardiovascular disease, weight gain and obesity, diabetes, metabolic syndrome, and increased risk for mortality.
Moderators
- There is some evidence that demographic factors (e.g., age, gender, ethnicity, SES) moderate the influence of social connection and health. Recent evidence suggests that social isolation and loneliness may carry a higher risk among those under age 65 relative to those over age 65. No reliable gender differences have emerged.
- Both the positive and negative attributes of relationships can significantly influence the magnitude and direction of the association between these relationships and health.
- Higher quality and more numerous relationships is associated with protective health effects and a lower risk of mortality.
- Having poorer quality and fewer relationships is associated with harmful effects on health including higher risk for morbidity and mortality, poorer treatment adherence, and poorer health-relevant biological responses.
- Understanding both the negative and the positive attributes of social relationships is needed to fully understand how these relationships impact health.
- Decreasing social isolation may not reduce risk if attention is not paid to the quality of the relationships; thus, indicators of quality need to be included in assessments.
This page intentionally left blank.
















