3
Health Impacts of Social Isolation and Loneliness on Morbidity and Quality of Life
Feelings of social connection as well as feelings of disconnection have enormous influences on our bodies, as well as on our behaviors.
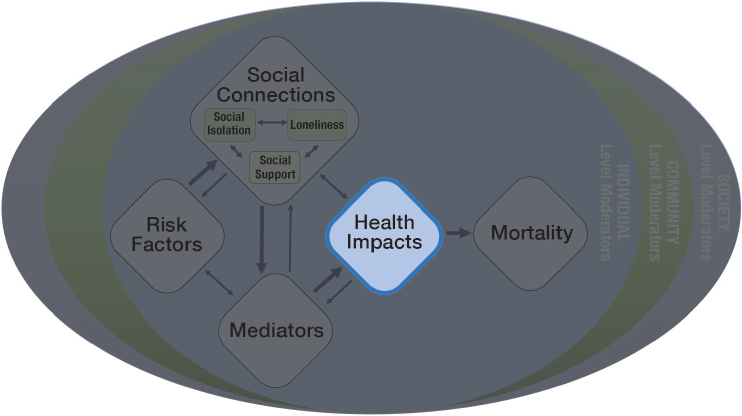
As described in Chapter 2, studies of all-cause mortality provide compelling evidence of the health impacts of social isolation, and several aspects of social connection have been associated with specific causes of death (e.g., cardiovascular disease, cancer). But the health effects of social isolation and loneliness extend beyond mortality. Social isolation, loneliness, and other aspects of social connection can also significantly affect the risk of developing certain health conditions as well as the course of these health conditions and various measures of the quality of life. While most of the studies in this area evaluate social isolation and loneliness as risk factors and the health conditions as outcomes, the relationship between social isolation or loneliness and health is often bi-directional. (See Chapter 4 for more on health conditions as risk factors for social isolation and loneliness.) This chapter focuses on the evidence base for the impact of social isolation and loneliness on a wide range of physical, cognitive, and mental health conditions as well as on self-reported health and quality of life among adults aged 50 and older. The material presented in this chapter provides a summary of the relevant published literature. It is not intended to serve as a comprehensive review of every study published on these topics. This chapter represents the portion of the committee’s guiding framework related to health impacts (see Figure 3-1). Given the complexity of the terminology used in relation to social isolation and loneliness, a reminder of key definitions is provided in Box 3-1.
IMPACT ON HEALTH OUTCOMES
In addition to the robust evidence linking social isolation and loneliness with mortality (see Chapter 2), other research has established that social isolation and loneliness are linked with specific health conditions. As described in previous chapters, the scientific literature concerning social isolation and loneliness draws on a variety of conceptual and measurement approaches that collectively characterize related aspects of social relationships. In the following sections, the committee presents evidence of the effects of different aspects of social connection on health, using the terminology and definitions as described by the individual authors of the cited studies.
Cardiovascular Disease and Stroke
Cardiovascular disorders and morbidities have been studied extensively as outcomes of social isolation and loneliness. A meta-analysis of 23 studies using 16 longitudinal datasets found that poor social relationships (e.g., social isolation, loneliness) increased the risk of developing coronary heart disease and stroke, independent of traditional cardiovascular disease risk factors (Valtorta et al., 2016a). Despite variability in the measurement of social isolation and loneliness across studies, poor social relationships were found to be associated with a 29 percent increase in risk of incident coronary heart disease and a 32 percent increase in the risk of stroke, and this was consistent across genders (Valtorta et al., 2016a). Other studies support these findings. For example, studies of patients after myocardial infarction have consistently found low social support to be a marker of poor prognosis and to be associated with increased mortality, readmission, and re-infarction rates (Barth et al., 2010; Glozier et al., 2013). An earlier review found both low social integration and loneliness to be associated with an increased risk for hypertension (Cuffee et al., 2014). A longitudinal study of nearly 5,400 adults over the age of 50 found loneliness to be associated with an increased risk for cardiovascular disease (defined by coronary heart disease and stroke), but not social isolation (Valtorta et al., 2018a). Data from the United Kingdom Biobank found that isolated and lonely persons were at increased risk of acute myocardial infarction and stroke (Hakulinen et al., 2018). One study of heart failure patients who self-reported high “perceived social isolation” (i.e., loneliness) found a 68 percent increased risk of hospitalization, a 57 percent increased risk of emergency department visits, and a 26 percent increased risk of outpatient visits compared with patients reporting low perceived social isolation (Manemann et al., 2018). (See Chapter 9 for more on the impacts of social isolation and loneliness on health care use.)
Consistent with this evidence for social isolation or loneliness as a major risk factor for cardiovascular disease, a review of currently available and widely used cardiovascular risk assessment models concluded that traditional screening for
cardiovascular risk may be improved by taking social relationships into account (Ruwanpathirana et al., 2015).
Dementia and Cognition
Numerous observational studies have examined the associations of high levels of loneliness, low frequency of contact with family and friends, and low levels of participation in community groups with the risk of dementia and cognitive decline in older adults. A 2015 meta-analysis found an increased risk of dementia to be associated with high levels of loneliness, infrequent social contacts, and low-level group participation (Kuiper et al., 2015). Furthermore, this meta-analysis indicated that these social factors increased the risk of dementia by approximately 50 percent, which was comparable to such dementia risk factors as physical inactivity, low education, type 2 diabetes mellitus, and late-life depression (Diniz et al., 2013; Leoutsakos et al., 2015; Norton et al., 2014; Vagelatos and Eslick, 2013).
Similarly, another meta-analysis that included more than 2.3 million participants found that living alone, having a limited social network, having a low frequency of social contact, and having poor social support were all risk factors for dementia (Penninkilampi et al., 2018). The risk ratios for a weak social network and few social contacts were even stronger after adjusting for the presence of depression, indicating that low social connection has discrete effects on dementia risk that are distinct from the effects of depression (Penninkilampi et al., 2018). An elevated risk of dementia was also associated with low social support. Findings for an association between loneliness and risk of dementia in studies were mixed and, being based on a small number of studies, were non-significant overall. Furthermore, a reduced risk of dementia was reported to be associated with high levels of social contacts and social activity, indicating possible protective effects of high social engagement (in addition to the increased risk of dementia at low levels of social engagement) (Penninkilampi et al., 2018).
Social isolation and loneliness have also been examined in multiple cohorts for their association with cognitive decline (Bassuk et al., 1999; Crooks et al., 2008; Ertel et al., 2008; Kelly et al., 2017). The evidence indicates that less frequent social contacts and lower levels of participation in community groups are associated with declines in global cognition, processing speed, executive function, and visuospatial abilities (Braak and Del Tredici, 2012). These associations were found to be independent of many factors, including age, sex, educational attainment, wealth, levels of depression, and physical activity (Saczynski et al., 2006; Shankar et al., 2013). Greater loneliness in older adults has also been associated with worsening performance on measures of global cognition and on specific tests of immediate and delayed recall (Holwerda et al., 2014; Shankar et al., 2013; Tilvis at al., 2004; Wilson et al., 2007).
Notably, social isolation and loneliness have been found to have independent and cumulative effects on cognitive decline and dementia risk in some but not all
studies, suggesting that the structural and functional aspects of social connection may influence cognitive health through both shared and distinct mechanisms (Donovan et al., 2017; Holwerda et al., 2014; Shankar et al., 2013; Wilson et al., 2007). Social interactions are thought to enhance cognitive capacity by activating and maintaining the efficiency of brain networks (Stern, 2012). This effect may point to the existence of a form of neural reserve that supports cognitive function as age-related and pathological brain changes accrue over time (Bennett et al., 2006; Yu et al., 2015). In older adults greater emotional support has been associated with both higher serum levels of brain-derived neurotropic factor and a reduced risk of dementia, suggesting that enriching relationships may also promote neurogenesis and synaptic plasticity (Salinas et al., 2017). In addition, higher loneliness in mid- to late life has been associated with elevated cardiovascular and neuroendocrine markers of stress, impaired sleep, and pro-inflammatory physiological effects, which may accelerate neurodegeneration in the hippocampus and in other brain regions vulnerable to Alzheimer’s disease and vascular cognitive impairment (Cacioppo et al., 2002; Hackett et al., 2012; Hawkley and Cacioppo, 2010; Hawkley et al., 2006; Jaremka et al., 2013a; McHugh and Lawlor, 2013). In cognitively normal older adults, greater loneliness has been associated with higher levels of brain amyloid and regional accumulation of tau protein, linking loneliness with the pathological changes of early Alzheimer’s disease (d’Oleire Uquillas et al., 2018; Donovan et al., 2016). Furthermore, less social engagement with friends, family, and community groups has been associated with a more rapid cognitive decline in these unimpaired older adults with high brain amyloid, indicating an adverse interactive effect of low social connection and early Alzheimer’s pathology on cognitive health (Biddle et al., 2019).
A small number of observational studies have investigated the possibility of reverse causation (i.e., the possibility that low cognitive function may precede declines in social function). These studies have found inconsistent and, most often, opposing evidence that low cognitive function leads to subsequent social disengagement or loneliness in population-based cohorts; however, other research has demonstrated that older adults with declining cognitive performance experience disruptions in their larger and more diversified social networks (Aartsen et al., 2004; Ayalon et al., 2016; Donovan et al., 2017; Ellwardt et al., 2015; James et al., 2011; Wilson et al., 2007). These and other complementary findings raise the possibility that social function and cognitive abilities are reciprocally related and, in certain aging adults, may decline in tandem (Biddle et al., 2019).
Depression and Anxiety
In cross-sectional studies, social isolation and loneliness have been associated with both depression and anxiety throughout adulthood, including in older adults. In one of the largest studies to date, which included more than 15,000 German adults aged 35–74 years, greater loneliness was related to higher rates of clinically
significant depression, anxiety, and suicidal ideation, independent of age, sex, partnership, and socioeconomic status (Beutel et al., 2017). A systematic review of this topic included eight cross-sectional studies of adults aged 60 and older and found loneliness to have been associated with depression in seven studies and low social engagement to have been associated with depression in one study (Choi et al., 2015). In a cross-sectional study of 314 older U.S. adults living in retirement communities, loneliness was found to be associated with both depression and anxiety, but not with perceived health, medical conditions, or functional status (Bekhet and Zauszniewski, 2012). While loneliness is commonly associated with clinically significant depression, loneliness and depression are recognized as distinct constructs that can also be experienced independently of each other. A study of more than 8,000 older adult participants from the U.S. Health and Retirement Study found that nearly 18 percent of the sample reported frequent feelings of loneliness. Within this lonely group, 53 percent reported levels of depressive symptoms above the threshold for clinically significant depression, and 47 percent reported either no depressive symptoms or depressive symptoms in a subthreshold range (Donovan et al., 2017). A systematic review by Schwarzbach and colleagues (2014) of 25 cross-sectional and 12 longitudinal studies (but not including studies of loneliness) evaluated the relationship between depression and a range of social support and social network measures for older adults. Qualitative aspects of social relations, such as social support, the quality of relations, and a confidant relationship, were most consistently associated with the presence or absence of depression in the cross-sectional studies. However, in the longitudinal studies a lower quantity of social interactions was most often associated with depression over time. Schwarzbach and colleagues (2014) interpreted this to mean that having fewer social interactions or connections may predispose adults to later having inadequate social support when it is needed during stressful events, thereby elevating the risk of incident depression. Correspondingly, close relationships and social support may be experienced as more acutely inadequate in those who are depressed because of the distress and disabilities imposed by these symptoms.
A cross-sectional study of more than 1,400 older U.S. adults also found that the qualitative aspects of social relationships were more strongly related to depression than the quantitative aspects when the depression and social relationships were measured at the same time-point, which was consistent with the pattern observed earlier (Taylor et al., 2018a). Also consistent were findings from a longitudinal study of more than 11,000 older U.S. adults, which quantified the number and types of social contacts as a potential predictor of future depression. A lower frequency of in-person social contacts was related to higher rates of depression over 2 years. Notably, the frequencies of telephone, written, or email contacts were not associated with depression at 2 years, indicating that in-person modes of contact were uniquely protective (Teo et al., 2015).
A growing number of international studies have employed validated instruments for measuring loneliness and have found positive associations of loneliness
with higher depression and anxiety over time. These include analyses from the Irish Longitudinal Study of Ageing, which found both loneliness and low social network to be associated with rates of clinically significant depression and anxiety over 2 years; from the Netherlands Study of Depression in Older Persons, which found that loneliness at baseline predicted a poorer course of depression in persons with late-life depression; and from the Chicago Health, Aging, and Social Relations Study, which found greater loneliness, but not social support or social network, to be associated with higher depression scores over 5 years (Cacioppo et al., 2010; Doménech-Abella et al., 2019; Jeuring et al., 2018). One German study that sought to compare different measurement approaches found that subjective loneliness and network quality best predicted mental health, whereas network size and living alone best predicted physical and cognitive health (Beller and Wagner, 2018b).
Collectively, these studies establish that social support, social isolation, and loneliness are strongly linked to depression and anxiety. While these associations do not establish causality, the temporal associations suggest that social isolation and loneliness likely cause or worsen depression and anxiety, with in-person contacts and the perceived adequacy of relationships having the largest impacts. The relationships of social isolation and loneliness with depression and anxiety have also been shown to have reciprocal effects over time. (See Chapter 4 for research describing loneliness and social isolation as outcomes of depression and anxiety and for further discussion of loneliness and depression as distinct constructs.)
Chronic Health Conditions and Other Physical Health–Related Factors
In a cross-sectional, population-based sample of 20,007 participants from the Swiss Health Survey, individuals who self-identified as being lonely were found to be 41 percent more likely to be affected by self-reported chronic diseases, 31 percent more likely to have high cholesterol levels, 40 percent more likely to have diabetes, and 94 percent more likely to report self-perceived impaired health (Richard et al., 2017). In a Danish sample, self-reported loneliness was associated with a more than 2.5 times higher risk for poor self-rated health, 91 percent higher risk of limited physical abilities, and a 77 percent higher risk of multiple diagnoses (Jessen et al., 2017). In the United States the relationship between loneliness and functional decline or death was assessed in 1,604 subjects 60 years of age and older, who participated in a longitudinal cohort study between 2002 and 2008; the assessments were conducted every 2 years (Perissinotto et al., 2012). Participants who self-identified as lonely (as measured by the three-item UCLA Loneliness Scale) were more likely to have experienced reductions in the activities of daily living (e.g., bathing, eating), in mobility, and in stair-climbing ability, and they had more difficulty with upper extremity tasks (e.g., pushing or pulling large objects, lifting weights heavier than 10 pounds), ultimately resulting in a 59 percent increased risk of function loss. A longitudinal community-based cohort study of 985 older adults
who reported loneliness and being alone examined the loss of motor function (Buchman et al., 2010). Assessed loneliness at baseline was found to correspond with the rate of motor function decline, with a higher assessed loneliness at baseline resulting in more rapid rates of motor function decline. (See Chapter 4 for information regarding risk factors associated with frailty in older adults.)
Several aspects of the structural and functional characteristics of social connection have been associated with newly and previously diagnosed type 2 diabetes mellitus (T2DM). One study found that individuals with a smaller social network size were more likely to have newly diagnosed and previously diagnosed T2DM; no such relationship was found for pre-diabetes (Brinkhues et al., 2017). On the other hand, pre-diabetes was found to be associated with a lack of social participation, and living alone was associated with a greater likelihood of previously diagnosed T2DM in men, but not in women (Brinkhues et al., 2017).
Loneliness may also have a reciprocal relationship with diabetic outcomes. Diabetes-related complications can limit physical mobility, which may in turn limit an individual’s ability to initiate social interactions or may strain relationships, thus leading to greater loneliness (Jaremka et al., 2013b; Ribu and Wahl, 2004). In a population-based study of adults without diabetes, low satisfaction with one’s social network (perhaps an indirect indication of social isolation and loneliness) was associated with a significantly increased risk of developing T2DM, and the risk for incident T2DM was still significant after controlling for social isolation and living alone (Lukaschek et al., 2017).
Social connections even appear to influence susceptibility to colds. In viral challenge studies, for which all participants are infected with a cold virus, loneliness was associated with greater self-reported cold symptoms (LeRoy et al., 2017). Sociability (assessed using measures of extraversion, agreeableness, and positive relationship style) has been linearly associated with a decreased probability of developing a cold, independent of baseline, demographics, emotional styles, stress hormones, and health practices (Cohen et al., 2003). Having more diverse social networks has been associated with having a greater resistance to upper respiratory illness (Cohen et al., 1997). Furthermore, having a greater number of social roles has been associated with better pulmonary function in older adults (Crittenden et al., 2014).
IMPACT ON HEALTH-RELATED BEHAVIORS
Different aspects of social connection may affect health-related behaviors (e.g., smoking, substance use, exercise, diet, sleep patterns) both positively and negatively. Health-related behaviors have been studied for decades, and early theories held that being married or being a parent helped inhibit risk-taking behaviors such as drinking, smoking, or illicit substance use because these roles afforded a sense of importance or purpose or because having a partner helped to favorably regulate these health behaviors (Gove, 1973; Syme, 1974; Umberson, 1987).
Social connections and supports have been associated with levels of use (as well as the cessation and relapse) of tobacco and alcohol (Christakis and Fowler, 2008; Havassy et al., 1991; Rosenquist et al., 2010; Seeman and Anderson, 1983). That is, an individual’s levels of alcohol and tobacco use may be affected by the degree of use of his or her social contacts or, in the case of cessation, by the strength of his or her social supports. However, these effects can be positive or negative. For example, studies have shown that smoking cessation among one’s social contacts improves the likelihood that an individual will stop smoking, while living with a smoker or having smokers among one’s social networks decreases the likelihood of smoking cessation (Holahan et al., 2012; Lacey et al., 1993; Moore et al., 2014).
Evidence specifically related to the connection between social isolation and health-related behaviors has shown that older people who are isolated are more likely to have less healthy behaviors such as poor diets, tobacco use, heavy alcohol use, and a lack of physical activity (Choi and DiNitto, 2015; Ho et al., 2018; Kharicha et al., 2007; Kobayashi and Steptoe, 2018; Locher et al., 2005; Schrempft et al., 2019).
While some research has found no relationship specifically between loneliness and certain health-related behaviors (Canham et al., 2016; Hawkley et al., 2009; Kobayashi and Steptoe, 2018; Schrempft et al., 2019), other studies of adults and older adults have found associations of loneliness with low physical activity, being overweight, higher levels of smoking, and greater alcohol consumption (Akerlind and Hornquist, 1992; Barretta et al., 1995; Hawkley et al., 2009; Lauder et al., 2006a; Shankar et al., 2011; Stickley et al., 2013). Also, limited evidence links loneliness with risky sexual behaviors and psychotropic drug use among older adults (Boehlen et al., 2015; Golub et al., 2010). (See Chapter 5 for more on health-related behaviors as a mediator of the relationship between social connection and health.)
Suicidal Ideation and Suicide Attempts
Suicide is a concern for families and communities, and both social isolation and loneliness have been identified as risk factors for suicide for individuals of all ages (Calati et al., 2019; Kochanek et al., 2019). Between 1999 and 2017 suicide rates increased among adults aged 45–74 (from 6.0 to 9.7 per 100,000 adults aged 45–64 and from 4.1 to 6.2 per 100,000 adults aged 65–74), and white males over the age of 85 have been identified as being most at risk for suicide (Hedegaard et al., 2018; Steele et al., 2018). Depression has been found to be the most relevant cause of suicide attempts, but both loneliness and social isolation have also been identified as major contributing factors (Minayo and Cavalcante, 2015).
A number of studies have evaluated the relationship of social isolation with suicide in older adults. In a review of nine studies published between 2010 and 2017 that focused on suicide attempts or suicide ideation in adults 60 years of age and older, the authors found a relationship between both loneliness and social isolation and suicidal thoughts or ideation (Heuser and Howe, 2019).
Similar findings were seen in a systematic review of studies examining suicide risk in nursing homes and other long-term care facilities conducted between 1985 and 2013 (Mezuk et al., 2014). Researchers found that both loneliness and social isolation were correlated with suicidal ideation among residents in these settings.
The majority of studies examine either social isolation or loneliness when evaluating suicide risk. Several recent interview studies found a relationship between suicidal ideation or self-harm in older adults and feelings of loneliness or “aching loneliness” (Huang et al., 2017; van Wijngaarden et al., 2015; Wand et al., 2018). Self-harm in older adults was evaluated in a recent systematic review that included 40 articles published through February 2018. This study, which included a total of 62,755 older adults, found that increased loneliness was among the primary motivations reported for self-harm (Troya et al., 2019). Wiktorsson and colleagues (2010) interviewed 103 suicide attempters aged 70 or older treated at five emergency departments in Western Sweden and compared them with matched community controls. A strong relationship was found between perceived loneliness and attempted suicide, independent of depression. The association between social relationships and suicidal ideation were evaluated in a meta-analysis by Chang et al. (2017), which included findings from 31 studies published between 2000 and November 2016. In that analysis, elderly adults were found to be 57 percent more likely to experience suicide ideation if they had discordant social relationships, and perceived loneliness along with elderly mistreatment and poorly perceived social support were found to be the measures associated with the greatest effect (Chang et al., 2017). Furthermore, death wishes, which may lead to suicidal ideation or future suicide attempts, were found to be significantly associated with loneliness, depression, and poor self-reported health in a study of more than 35,000 people over 65 years of age (Cheung et al., 2017). Bernier et al. (2020) evaluated Seniors Health Survey results from 2,787 French-speaking community dwellers between the ages of 65 and 69 and found that the 5 percent of respondents who wished for death were significantly more isolated than other respondents.
Taken together, these results indicate that social isolation and loneliness are related to both suicidal ideation and suicide attempts. None of these studies were designed to determine whether social isolation or loneliness cause suicidality, but they are clearly associated with suicidal thoughts and behaviors, even apart from depression.
IMPACT ON QUALITY-OF-LIFE OUTCOMES
A growing body of research indicates that social isolation and loneliness negatively affect quality of life among older adults, although the empirical literature on these relationships remains relatively limited. The variability in the measures of social isolation and loneliness used in these studies, coupled with the small number of the studies, allows for only a limited scientific understanding of how both phenomena relate to an older adult’s quality of life.
The definitions of quality of life vary across the available research on social isolation and loneliness among older adults. Many of these studies define quality of life as a health-related construct—either as health-related quality of life (HRQL), which offers a broad, multi-dimensional picture of a person’s health and well-being from the individual’s perspective, or as health status, which captures a person’s physical and mental health in narrower terms and represents only one aspect of HRQL (Golden et al., 2009). Other studies employ a more expansive definition of quality of life, including factors such as perceived financial adequacy, satisfaction with life, and “global happiness,” among others (Chappell and Badger, 1989). Holmén et al. (1999) commented that while the common definitions of quality of life at the time focused on health and illness, emerging definitions were generally more expansive in that they allowed for subjective dimensions such as overall life satisfaction.
Current evidence indicates that social isolation negatively affects the quality of life of older adults. Hawton et al. (2011) found that social isolation—defined by a person’s level of contact with others—has a significant, independent, and negative effect on HRQL among older adults, even when accounting for factors such as depression, physical comorbidity, age, gender, living alone, employment status, and accommodation type. In the Hawton et al. (2011) study, older adults who were severely socially isolated were found to have particularly low HRQL scores when compared to peers of similar age in the general population. Other work done in the context of older people’s social networks has found social isolation to be associated with decreased satisfaction with one’s life, hopelessness, increased risk of depressed mood, and decreased happiness (Golden et al., 2009). Additionally, research has illustrated how certain dimensions of social isolation might have a greater effect than others on an older person’s quality of life. Chappell and Badger (1989) interviewed 743 older adults aged 60 years or older to examine 10 indicators of social isolation—whether an older person lives alone, is married, has children, or interacts with confidants or companions, and so on—and they observed that companionship and confidants were more related to an older person’s well-being than the individual’s marital status, living arrangements, or presence of children.
While few studies have documented the impact of loneliness on quality of life among older adults, the research that has been done indicates that both severe and moderate loneliness significantly reduce the physical and mental quality of life among older adults. Being lonely might also lead to reduced satisfaction with one’s life and lower levels of happiness, and one study concluded that older adults who were not lonely showed fewer depressive symptoms (Ekwall et al., 2005; Lim and Kua, 2011; Musich et al., 2015). The combination of loneliness and social isolation might also have an adverse effect on the quality of life among older adults. Golden et al. (2009) discovered that the prevalence of hopelessness—an indicator for a diminished quality of life—was higher among older adults who did not have an integrated social network.
ELDERS AT RISK FOR ABUSE
Elder abuse, which can affect an older adult’s physical health, mental health, and quality of life, is burgeoning globally, and isolated or lonely individuals can be more vulnerable to mistreatment. According to the World Health Organization, approximately one in six adults aged 60 years or older have experienced at least one form of abuse—financial exploitation, physical abuse, psychological (or verbal) abuse, sexual abuse, or outright neglect—during the past year (WHO, 2018). In the United States it has proved difficult to determine the precise extent of elder abuse. Efforts to evaluate the scope of abuse have been hampered by the lack of standardization in how cases of abuse are defined, prosecuted, and reported from one jurisdiction to the next as well as by the large number of abuse cases that go unreported (Acierno et al., 2010; Wang et al., 2015). However, an estimated 5 to 10 percent of older adults in the United States fall victim to some form of abuse (Lachs and Pillemer, 2015; Wang et al., 2015). Based on projections of aging, the number of older victims of abuse could grow from an estimated 2.5 million to 4.9 million in 2016 to as many as 9.8 million by 2060 (ACL, 2018; Ortman et al., 2014).
Physical or social isolation can increase a person’s susceptibility to abuse. Socially isolated individuals are both more vulnerable to abuse (Acierno et al., 2010) and more likely to become abusers (Amstadter et al., 2011). In addition to any psychological anguish it may cause, elder abuse can lead to housing displacement or disruption, worse physical health, or, in extreme cases, even death (Wong and Waite, 2017). Perpetrators of elder abuse are most often family members—spouses or adult children—or unrelated caregivers and are often male and financially dependent on the abused adult; substance abuse problems or having a history of mental health issues are common in abusers (Fulmer et al., 2005; Labrum and Solomon, 2015; Lachs and Pillemer, 2015; Sibbald and Holroyd-Leduc, 2012; Wong and Waite, 2017). Many cases of abuse go unreported by both the abused individuals and the perpetrators of abuse because of other factors, such as the possibility of losing housing or a caregiver, or emotional or financial reasons that could be at stake (Wong and Waite, 2017).
FINDINGS AND CONCLUSIONS
- Substantial evidence shows that social isolation and loneliness are strongly associated with a greater incidence of major psychological, cognitive, and physical morbidities and lower perceived well-being or quality of life.
- Strong evidence indicates that social isolation and loneliness have effects on the risk of cardiovascular and cerebrovascular morbidities. A smaller amount of evidence indicates that social connection has effects on the course of other chronic health conditions, such as type 2 diabetes mellitus, or on health characteristics, such as mobility and functioning in the activities of daily living.
- Substantial evidence links social isolation and loneliness with accelerated cognitive decline in older adults and an increased risk of incident dementia.
- Social connection is strongly linked to depression and anxiety. Temporal associations suggest that social isolation and loneliness likely cause or worsen depression and anxiety. Complementary research suggests that depression and anxiety increase the likelihood of low social connection, which is further addressed in Chapter 4.
- While some research shows no relationship specifically between loneliness and certain health-related behaviors, other studies have found associations of loneliness with lower physical activity, being overweight, higher levels of smoking, and greater alcohol consumption.
- Emerging evidence suggests that social isolation and loneliness negatively affect the quality of life of older adults. However, the existing empirical literature on this relationship is relatively small, and interpretations are limited by variability in the measures and definitions of social isolation and loneliness used.
- Reports of elder abuse, including financial exploitation, physical abuse, psychological (or verbal) abuse, sexual abuse, or outright neglect, are disturbingly common. In the United States there is a lack of infrastructure for reliably measuring this problem.
NEXT STEPS AND RECOMMENDATIONS
Substantial evidence supports the association of social isolation, loneliness, and certain other indicators of social connection (e.g., social support) with an increased incidence of major physical, cognitive, and psychological morbidities; poorer health-related behaviors; and lower perceived well-being or HRQL. Existing evidence suggests that certain aspects of social connection may be especially predictive of certain health outcomes and that the relationship between social connection and health is often bi-directional.
As discussed in Chapter 2, the committee identified the increased funding of basic research as a key to achieving the goal of developing a more robust evidence base on effective prevention, assessment, and intervention for social isolation and loneliness. Specifically, the committee concludes that identifying, prioritizing, and developing ways to translate scientific knowledge of the impacts of social isolation and loneliness on health into effective and efficient clinical and public health interventions (see Chapter 9) first requires a better understanding of how social isolation and loneliness impact health, including the risk factors for social isolation and loneliness (see Chapter 4), the mediators (or mechanisms) by which social isolation and loneliness affect health (see Chapter 5), and the moderators that affect the magnitude of those relationships (see Chapter 5). Furthermore, more needs to be determined about whether and when (e.g., at what stage of
the life course, or when the situation is acute or chronic) an intervention will have downstream effects on health outcomes. Therefore, drawing from information in all of these chapters, the committee makes the following recommendation as a strategy to mitigate or eliminate the negative health impacts of social isolation and loneliness:
RECOMMENDATION 3-1: Major funders of health research, including the government (e.g., the National Institutes of Health, the Center for Medicare & Medicaid Innovation, and the Patient-Centered Outcomes Research Institute), foundations, and large health plans should fund research to improve the scientific understanding of the links between social connection and health, including the study of risk factors and mechanisms.














