2
The Changing Biothreat Landscape
KEY MESSAGES
- The National Security Strategy, National Biodefense Strategy, and Global Health Security Strategy include the following within the scope of biological threats: naturally occurring, accidental, and intentional biological incidents; and One Health.
- The nature of the biothreat is evolving, including the effects of global changes in the biotechnology on Biological Threat Reduction Program (BTRP) initiatives; what actions might BTRP take now to keep pace with these changes?
- Because the international landscape for addressing biological threats involves many nongovernmental, governmental, and intergovernmental actors, effective coordination and communication are critical to ensuring success of biological threat reduction programs.
In recent years, the concept of biothreat has continued to evolve to include natural, accidental, and intentional threats and their social, economic, political, and security consequences; exploitation of biotechnologies for malicious and/or military use; and unauthorized access to biological data. This evolution reflects the significant changes that have been observed in human and animal health, the biotechnology landscape, the bio-based economy, and international sample and data-sharing policies. These changes have been enabled by globalization of the biological and biotechnological sciences, Internet-connected facilities and information systems, an influx of new funders and practitioners, and increased investments in biodiversity and environmental scanning.
The U.S. government policy landscape for biodefense and health security focuses on factors and technologies that either enable or prepare strategic plans to respond to natural, accidental, or intentional biothreats. In 2019, the National Security Strategy, National Defense Strategy,
National Biodefense Strategy, Global Health Security Strategy, and U.S. government involvement in the Global Health Security Agenda (GHSA) and associated human and animal health agreements all contributed to the overarching context within which BTRP now finds itself operating. This relatively recent governing framework is built on a nonproliferation foundation, which is promoted by the Biological and Toxin Weapons Convention, United Nations Security Council Resolution 1540, and the legislation and policies governing Cooperative Threat Reduction Programs (CTR). Within this complex policy context, BTRP’s efforts to prevent biothreats is further complicated by the influence of threats emanating from cyber-attacks of facilities and information systems, and policies preventing open, transparent sharing of samples and scientific data.
This chapter provides a high-level outlook on the evolving nature of the biothreat, specifically focusing on how global changes in the biotechnology landscape may affect BTRP initiatives and what actions BTRP can take now to keep pace with these changes.
FINDING 2.1: The development of threat-specific prevention and detection approaches can be improved through anticipation of current and future threats presented by natural, accidental, and intentional incidents involving high-consequence pathogens and toxins and by misuse of advances in scientific research, development, and application.
FINDING 6.1: Preparing for and responding to existing and potential biosecurity threats requires an agile ability to consider traditional biological threats and the contributions of new research strategies and tools to understand the pathogenesis and epidemic potential of emerging pathogens.
GLOBAL HEALTH SECURITY
The mailing of anthrax-laced letters just 1 month after the terrorist attacks on September 11, 2001, in the United States (FBI), highlighted several inadequacies in U.S. and international preparedness and response to biological threats. Since that time, the international community has recognized the importance of addressing biological threats whether naturally occurring, accidental, or intentionally-released.
This broader definition of biothreats had developed in the late 1990s with the 1997 emergence of H5N1 influenza virus in humans (Neumann et al., 2010). Several subsequent outbreaks highlighted the need to stengthen capabilities for addressing biological events that could result in significant harm to human, animal, and plant health, economies, and society: the emergence of West Nile virus in the United States in 1999 (Roehrig, 2013); the Amerithrax incidents in 2001; the 2003 outbreak of Severe Acute Respiratory Syndrome coronavirus (SARS-CoV) (Denison, 2004); and the 2012 outbreak of Middle East Respiratory Syndrome coronavirus (MERS-CoV) (Coleman and Frieman, 2013).
Indeed, as this report was being finalized in January 2020, an outbreak of a novel coronavirus originating in Wuhan, China, was reported (Wang et al., 2020). Within 1 month of its recognition it had caused more confirmed infections than SARS-CoV over the entire course of that outbreak. The novel coronavirus has resulted in the quarantine of major cities in China with the cessation of air, train, and road traffic, as well as closure of international borders and the implementation of passenger screening at airports around the world for fever or clinical symptoms, and has already been declared by the World Health Organization (WHO) to be a Public Health Emergency of International Concern. With increasingly rapid modern transportation and globalization of commerce, unintentional threats to national security include pathogens that can spread rapidly, spillover from animals to humans, cause severe disease in humans and/or animals, devastate agricultural systems, cause fear and loss of trade and/or tourism, impact the security of the food supply chain, and impose economic harms (Jones et al., 2013).
Investments in biodiversity (i.e., sequencing organisms in different environments), detection of microbial species from different sources, and better diagnostic technologies have revealed the large number and diversity of emerging and re-emerging pathogens that infect humans, animals, and plants. In addition, the intentional contamination of livestock or crops (preharvest or postharvest) has long been considered a potential national security threat, and examples, while relatively few, are quite relevant (Caudle III, 2001; Hugh-Jones and Brown, 2006; Keremidis et al., 2013). These agriculture and food system vulnerabilities were recognized in Homeland Security Presidential Directive/HSPD-9 (White House, 2004b), through which the Departments of Agriculture (USDA) and Health and Human Services (HHS), and the Environmental Protection Agency were directed to work together in conducting disease surveillance and developing response programs to prioritize and mitigate such “disease,
pest, or poisonous agents” threats (White House, 2004b). Furthermore, the rapid and modern distribution of animal and plant products underscores the scale and broader impact of international incidents on the security of nations, such as the accidental contamination by a pathogen or a toxin in complex food products.
Consistent with the broader definition of biothreats, the International Health Regulations (IHR) (2005) and GHSA incorporated a systems-based approach for proactively, rather than reactively, addressing these types of natural, accidental, and intentional biological threats.
International Health Regulations (IHR 2005)
For more than three decades, infectious disease specialists have documented the emergence and re-emergence of pathogens throughout the world. Before 2005, IHR required member states of WHO to report single cases of cholera, plague, or yellow fever; described measures for decontaminating transportation vehicles; and created requirements for health documents for individuals traveling from infected to unaffected areas that confirmed prior vaccination against yellow fever virus (WHO, 1983). In May 2005, the World Health Assembly adopted the revised IHR, an international legal instrument known as IHR (2005), to update the global framework to detect, report, and respond to any infectious diseases, chemical, and radiological incidents causing public health effects of international concern, not just cholera, plague, and yellow fever. The emergence and rapid global spread of SARS-CoV in 2003 emphasized the need for global action and served as an important driver for the approval of the revised IHR (2005) to prevent, protect against, control and respond to the international spread of disease while avoiding unnecessary interference with international traffic and trade. IHR (2005) is also designed to reduce the risk that diseases might spread to other countries via international airports, ports, and ground crossings (WHO, 2009 and 2016a). These threats can include natural and human-made biological, chemical, and radiological incidents. IHR (2005) establishes a set of rules to support the Global Outbreak Alert and Response Network, and requires countries to improve international surveillance and reporting mechanisms for public health events, and strengthen their national surveillance and response capacities.
IHR (2005) officially entered into force in June 2007 and now is binding in 196 countries across the globe, including all WHO member states (WHO, 2016a). Every government was obligated to develop,
strengthen, and maintain the capacity to detect, assess, notify, and report events, and to respond to public health threats and emergencies of international concern within 5 years of coming into force, with the possibility of two 2-year extensions (WHO, 2016a, p. 11). However, fewer than 20 percent of countries had achieved full compliance with IHR (2005) by the 2012 deadline (Hamblion et al., 2014). To assist countries in implementing IHR (2005), WHO released a monitoring framework for countries to assess and improve or develop core capacities for preventing, preparing for, and controlling public health emergencies of international concern (WHO, 2018). The core capabilities cover laboratory capacity (which includes biosafety and biosecurity) and disease surveillance (Refaey, 2011), both of which fall within BTRP’s current initiatives. Unfortunately, resources available to WHO and within individual countries to upgrade national capacity are limited, preventing many countries from fully achieving the IHR (2005) core capabilities.
FINDING 4.1: The International Health Regulations (2005) require all countries to achieve minimum core competency to detect, assess, report, and respond to public health, plant, and animal health risks and emergencies of national and international concern. Not all countries have met these requirements, in significant part because of inadequate resources to implement assessment and capacity strengthening support at the country level.
The Global Health Security Agenda
The challenges that many countries faced in implementing IHR (2005) led the United States, WHO, the United Nations (UN) Food and Agriculture Organization (FAO), World Organisation for Animal Health (OIE), and 18 countries to launch GHSA in February 2014 (CDC, 2014). GHSA was intended to provide financial and technical resources to countries to address gaps in their public health systems that prevent achievement of the IHR (2005) core competencies. Sixty-seven countries are members of GHSA today (GHSA, 2019), and the number continues to grow. Unlike IHR (2005), GHSA focuses only on public health threats caused by infectious diseases. The initial set of action packages focused on antimicrobial resistance, zoonotic disease, biosafety and biosecurity, immunization, national laboratory system, real-time disease surveillance, reporting, workforce development, emergency operations centers, linking of public health with law and multisectoral rapid response, and medical
countermeasures and personnel deployment (GHSA, 2018a). BTRP-funded activities overlap with and could contribute to GHSA action packages on biosafety and biosecurity, national laboratory systems, real-time disease surveillance, emergency operations centers, and linking of public health with law and multisectoral rapid response (See Figure 2-1).
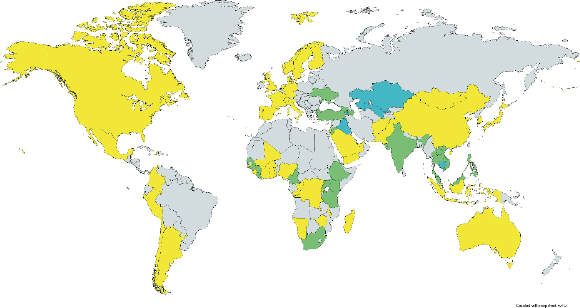
SOURCES: Brooks and Newman, 2018; GHSA, 2019; U.S. DOD, 2020a. Created using mapchart.net.
At the 2017 GHSA Ministerial Meeting in Uganda, member states agreed to extend the GHSA another 5 years. The GHSA 2024 Framework, which was released in 2018 (2018b), affirmed GHSA’s mission, vision, core principles, and strategic initiatives; established a secretariat function to support communication among GHSA members; and created task forces on advocacy and communication, stakeholder engagement, accountability and results, and action package coordination to aid in achieving the GHSA strategic initiatives. In addition, GHSA established a new action package on sustainable financing to promote national-level investment in preparedness for new and emerging infectious disease outbreaks. BTRP’s recent efforts in promoting multilateral cooperation to address biological threats and sustainability by enhancing partner country capabilities to detect, monitor, and prevent biological threats aligns with the original and 2024 objectives of GHSA. BTRP’s continued inclusion of experts from human and animal health, security, and scientific sectors in
its activities could support GHSA objectives. Consistent with the vision articulated in Chapters 5 and 6 of this report, BTRP could also engage government funders and philanthropic organizations to promote long-term support for continuing capability-building in biosafety, biosecurity, pathogen surveillance, training and workforce development, and other relevant areas. Furthermore, BTRP could engage the GHSA leadership on metrics and evaluation, building on its commissioned report on Measuring Cooperative BioEngagement Program Performance (Young et al., 2014).
WHO also developed the Joint External Evaluations (JEE) tool (WHO, 2016b), which is a voluntary external assessment process that identifies gaps in capacity, determines a country’s level of health security capacity; and measures progress toward a country’s ability to prevent, detect, and respond to infectious diseases threats. Progress has been achieved with the support of GHSA, member countries, and the Alliance for Health Security Cooperation, which currently has 73 members and focuses on developing multisectoral capability-building towards achieving the IHR (2005) core capacities (AHSCa). The country assessment process involves four phases: (1) self-assessment; (2) external evaluation; (3) country planning; and (4) capacity building. As of July 2019, 100 JEEs have been conducted since the first JEE was conducted in February 2016 (AHSCb; WHO, 2019f), 92 of which are available on the WHO website (WHO, 2019a). Box 2-1 highlights selected examples of recommendations of priority actions identified through the JEEs (WHO, 2017a, b, c). Forty-eight countries have completed National Action Plans for Health Security (NAPHS) to address gaps identified through the JEEs, and 12 countries have initiated development of their NAPHS (WHO, 2019c).
Under GHSA, efforts have been undertaken to improve data sharing through the implementation of the JEEs. Although nearly all JEE Mission Reports are available online, questions remain about how the assessment information should be used and who should have access to it (WHO, 2019a). Some experts have argued for a coordination center with ties to WHO to compile and coordinate this information, and others call for a more coordinated and streamlined JEE process. The JEEs serve as a guide to inform country capability needs for biosafety and biosecurity, biosurveillance, and other IHR (2005)-related capacities. In addition, the JEEs provide opportunities for multisectoral coordination to address country needs. JEEs, NAPHS, and other analyses can complement BTRP’s assessments of a partner country’s capabilities, identifying gaps that are prioritized by partner countries, and developing evaluation metrics for BTRP activities in priority countries.
U.S. efforts under GHSA generally involve strengthening existing programming toward global health security that is aligned with GHSA goals. Although GHSA is a multisectoral effort, the National Security Council is the responsible body for overall strategy and coordination for the U.S. government’s global health security program. Key implementing agencies include the Department of Defense (DOD), U.S. Agency for International Development (USAID), HHS, and Department of State (White House, 2019). Coordination across relevant U.S. departments and agencies will need to improve in order to implement a whole-of-government approach to global health security. In 2019, the U.S. government issued the Global Health Security Strategy (GHSS), which provides the United States’ overarching approach to prevention, detection, and response to biological threats internationally and documents roles and responsibilities of each department. A critical component of GHSS is continuous communication and coordination among U.S. government agencies involved in implementing the strategy.
OIE has developed the Performance of Veterinary Services (PVS) Pathway, the OIE’s flagship capacity-building platform for the sustainable improvement of national veterinary services. “Cyclical in nature, the PVS Pathway provides a robust mechanism for the continuous improvement of national veterinary services, through a staged approach using a set of proven tools and methods to evaluate, plan, cost, and support the strengthening of national veterinary services” (OIE, 2020a). The initial “PVS Evaluations comprise a 2- to 6-week mission, (which) delivers a thorough, qualitative assessment of the performance of a country’s veterinary services and their compliance with OIE international standards. It is an external evaluation conducted by a group of OIE trained and certified experts, who collect and analyse baseline information and evidence collated during the mission, including an extensive field component. The mission uses the proven OIE PVS tool, (through which) 45 critical competencies are systematically evaluated via documentation reviews, interviews, and physical observations against five qualitative graded levels of advancement, each with detailed descriptions or indicators to transparently guide the process” (OIE, 2020b). So far 37 missions have been completed (as of August 2019); 30 reports are available on the OIE website.
INTERNATIONAL HEALTH SECURITY PARTNERS
In addition to governments, intergovernmental and multilateral organizations, nongovernmental organizations, academic institutions, and the private sector play major roles in preventing, detecting, and responding to emerging, reemerging, and intentionally introduced pathogens. These entities generally fall into four major but overlapping categories: (1) international health; (2) development; (3) security; and (4) science. Although detailed descriptions of all efforts and entities involved in each of these categories is beyond the scope of this report, the diversity of actors is relevant to understanding the system in which BTRP is working to address biological threats.
Several intergovernmental efforts and entities exist to address infectious diseases affecting humans, animals, and/or plants, including the IHR (2005) (WHO, 2019e), GHSA, and OIE. In addition to the country members of GHSA (GHSA, 2020), two nongovernmental entities (the Private Sector Roundtable and GHSA Consortium) serve as members of the GHSA Steering Group and task forces, and several additional academic, nonprofit, and private-industry organizations contribute to GHSA Action Package implementation. OIE, which was established in 1924 to address animal diseases globally, has 182 member countries and is affiliated with more than 70 intergovernmental and regional organizations (GHSA, 2020; OIE, 2020c; USAHA, 2019). FAO, which is a specialized UN agency aimed at combatting hunger, has 194 member countries, works in more than 130 countries, and provides emergency response to outbreaks of transboundary animal diseases (e.g., highly pathogenic avian influenza, foot-and-mouth disease, peste des petits
ruminants [sheep and goat plague], and Rift Valley fever, and plant pathogens (FAO, 2019c, 2019e; Jungcurt, 2017)). FAO also hosts the International Plant Protection Convention (FAO, 2020b).
International organizations, universities, nonprofit organizations, private industry, and philanthropic organizations play significant roles in preventing and responding to health threats and risks. The Coalition for Epidemic Preparedness Innovations is an example of an international public–private partnership established in 2017 by the Wellcome Trust and the governments of Norway and India to help fund and coordinate the development of new vaccines against WHO priority pathogens (CEPI, 2019). Other examples include Gavi, the Vaccine Alliance, which was created in 2000 to promote equal access to vaccines for children in poor countries through public–private partnerships (Gavi, 2019), and the International AIDS Vaccine Initiative, which is a nonprofit organization focused on addressing challenges of human immunodeficiency virus and tuberculosis (IAVI, 2019).
Nonprofit, academic, and government organizations build country capabilities to detect and report pathogen outbreaks, train scientists and clinicians on biosafety and biosecurity concepts, and respond to public health emergencies and transboundary disease threats. Scientists in university, private-sector, and government laboratories help to characterize infectious diseases and outbreak strains; develop and test vaccines, medicines, diagnostic tools, and new technologies for biosurveillance; and educate future generations of scientists. All of these entities can support the promotion and adoption of norms of behavior with respect to biosecurity of pathogens and biosamples, an initiative best conducted through personal networks of trust. Experts from academia and think tanks conduct a variety of activities (e.g., advocacy, global governance, and evaluation and metrics) to monitor and support progress toward achieving global health, health security, and security objectives. For example, NTI, a Washington, DC-based nonprofit organization “recognizes that threat reduction is a shared responsibility between governments and the private sector. (They) raise awareness, advocate for solutions, facilitate implementation of solutions, and foster new thinking about these challenges” (NTI, 2020b).
Because key information about many of these programs and activities are shared among practitioners at conferences, by establishing a presence at these key meetings BTRP could identify experts to engage, be better informed about emerging advances, and identify biosecurity-related issues to address. Support and encouragement for BTRP participation at such
meetings and conferences would benefit its efforts to better engage with international partner countries and with organizations that have a similar mission. The landscape is complex, overlapping, and sometimes competitive, and the optimal way to understand what is going on is to participate.
Support for the broad spectrum of global health security efforts is provided by an equally diverse group of funders, including private donors, philanthropic organizations, and government funding agencies. Funders of global health, national security, development, and scientific research support global health security activities. Private funders include the Open Philanthropy Project, Skoll Global Threats Fund, Bill & Melinda Gates Foundation; multinational organizations such as the Asian Development Bank and the World Bank Group; and philanthropic arms of private industry, such as the Pfizer Foundation. Government funders include a variety of organizations, such as the U.S. CTR programs (e.g., DOD BTRP and the Department of State Biosecurity Engagement Program), the Global Partnership Against the Spread of Weapons of Mass Destruction (GPWMD, 2017), the European Commission Horizon 2020 (European Commission, 2019), USAID, and the development agencies of other countries (e.g., U.K. Department for International Development (U.K. Government, 2019)), the U.S. Centers for Disease Control and Prevention, European Centre for Disease Prevention and Control, and other similar organizations.1
FINDING 5.4: Navigating the diverse landscape of international experts, implementing organizations, coordinating organizations, and funders can be difficult given the sheer number of entities involved. To be most effective, any actor engaging in these efforts–including BTRP–must leverage existing capabilities, cooperate with other funders regardless of any difference in mission, and promote deconfliction of activities in countries where human and financial resources are limited. To obtain the most information and understand the necessary response, these actors also need to coordinate with one another and to communicate and share information for the immediate public health needs and for generating research data for the future.
___________________
1 See Appendix C for a more detailed list of organizations and descriptions involved in global health security.
DATA SHARING RELEVANT TO GLOBAL HEALTH SECURITY
Developing better analytical and data-sharing capabilities within and between countries is essential for biological threat reduction efforts to succeed. For example, a more detailed understanding of human and animal migration pathways is needed to more effectively assess disease threats. However, the issue of sample and data sharing has presented significant challenges, especially since 2006, when H5N1 avian influenza was a significant public health concern (Fidler, 2008).2 Numerous countries have passed laws regulating sample and data sharing within the biodiversity and access and benefit-sharing context (CBD, 2019). Some countries, including Indonesia, have now strengthened their policies to require material transfer agreements and approval for sharing of samples and data with foreign scientists, and the penalty for noncompliance now includes fines and prison time (Rochmyaningsih, 2019). Achieving the goals of biological threat reduction requires the capacity to safeguard samples that contain virulent strains of a pathogen. Without such assurances, transport of samples out of a country could be labeled biopiracy. To be able to transfer samples, BTRP could negotiate material transfer agreements with partner countries, perhaps using a common template agreement that is tailored to different countries to ensure consistency in sample and data sharing.
FINDING 4.2: Sample and data-sharing are critical to early detection of transboundary outbreaks, but access to this information may be limited because of strict sample and data-sharing policies in partner countries. Delays in data access could delay reporting to international health organizations, alerting neighboring countries to the potential threat, and initiating emergency response activities in a timely manner, including development of field ready diagnostic tests, and planning of clinical trials of countermeasures, including therapeutics and vaccines.
___________________
2 There was an objection to isolates from samples being used for seasonal vaccine development because a company stood to profit from the use of the sample, but none of the profit would be allocated to the country that provided the sample. Moreover, the country of origin would have to buy the vaccine at unaffordable prices.
SECURITY AND DEFENSE OF AGRICULTURE AND FOOD SUPPLIES
As the world population continues to grow, agriculture also is changing to meet food production needs. In 2017, FAO identified five key trends: (1) increased human population growth with concomitant increases in agriculture production; (2) increased complexity of food production systems and consolidation of small producers resulting in larger, more complex industries; (3) increased susceptibility of agriculture to the changing climate and natural and human-made disasters; (4) greater impact of agriculture industries on the environment; and (5) increased competition between industries for natural resources to continue food production (FAO, 2017). The report states that changes in agriculture must be made to avoid some of the observed trends threatening longer-term food security. In 2018, food insecurity was said to impact an estimated 820 million people in the world and potentially disrupt political infrastructure in affected countries (Deaton and Lipka, 2015; FAO, 2019d), suggesting threats to agriculture could represent significant risk to national and regional security (FAO, 2019b). In addition, high food insecurity results in malnutrition, which impedes the immune response to infection and increases morbidity and mortality. It also drives people to move into environments that represent an enhanced threat of infection.
Expanding BTRP’s current efforts in biosurveillance of animal and plant pathogens would promote early warning of and response to transboundary zoonotic diseases and potentially destabilizing effects on governments and populations (See Table 2-1 for a list of select diseases at the human-animal-environment interface and the potential health and financial burdens they may cause). Foreign animal diseases that do not directly affect humans, such as foot and mouth disease (FMD) or African swine fever (ASF), and diseases that only sporadically cause human disease such as highly pathogenic avian influenza (HPAI), can destroy large populations of food production animals, which, in turn, could initiate economic and subsistence disasters. For instance, USDA estimates that an outbreak of FMD in the United States could cost anywhere from $15 to $100 billion (USDA, 2017). The 2014-2015 incursions of H5N2 HPAI among U.S. poultry led to the culling of an estimated 50 million birds at a cost in excess of $2 billion (FAO, 2019a; USDA, 2017).
The recent explosive spread of ASF in Asia is an example of how these animal and food security threats can rapidly create hardship. From initial detection in China in August 2018 through October 2019, ASF has spread
rapidly to Cambodia, the Democratic People’s Republic of Korea, Laos, Mongolia, Myanmar, the Republic of Korea, and Vietnam (FAO, 2019a). This outbreak has become a major swine industry disruptor that is rapidly changing the economics of pork in China and Vietnam, resulting in a 30 to 40 percent increase in the cost of pork (Economist, 2019), and a 63 percent increase in orders to import pork products into mainland China (Gu and Singh, 2019). Such long-term economic distress and food security problems can destabilize nations, even when direct transmission of infection to humans is unlikely without genetic modification of the agents that permit it to breach species barriers and spillover to humans.
Some primarily animal pathogens also can infect humans with varying degrees of efficiency. Since 2013, HPAI H7N9 strains in China have infected millions of domestic poultry birds and more than 1,500 humans with a reported case-fatality rate of 39 percent (Wang, G.-L. et al., 2019), although this may reflect only symptomatic cases, as it does not incorporate information on mild or asymptomatic infections. Some pathogen threats to humans are found naturally in domestic animals, but cause the animals little or no harm, and as a result are designated reservoir species. For example, the MERS-CoV, which circulated with little evidence of disease in camels, has infected more than 2,500 people in 27 countries with a reported mortality rate of 35 percent (WHO, 2019b). Controlling both types of pathogens (those affecting animals only and those affecting humans but not their animal hosts) requires collaboration between the human and animal health sectors, their institutions, and their professional staff in a One Health approach. Examples include the recent control of HPAI H7N9 infections in humans through vaccination of poultry (Wang, G.-L. et al., 2019), and the reductions in human infections with MERS-CoV through multiple public health interventions including steps to prevent human exposure through camels, camel waste, and camel milk (WHO, 2019g). Such interdisciplinary collaborations have value for controlling many zoonotic and environmental pathogens (e.g., those found in water or soil).
These outbreaks exemplify the rapid spread of agricultural pathogens within countries and to neighboring countries and trade partners, emphasizing the importance of having disease surveillance systems in place for pathogens currently circulating in the food systems of affected countries, but not yet epidemic or pandemic (FAO, 2019a; Huang et al., 2013; Huong Giang et al., 2016; Tong-Qing et al., 2010; Zhou et al., 2019).
FINDING 5.1: Outbreaks of animal and plant pathogens that adversely affect the agricultural system and food
industry can directly or indirectly impact human health and have the potential to lead to destabilization of societies and economies, and/or national and regional conflicts.
TRAVEL AND TRADE
Globalized trade and modern transportation are increasing the movement of infectious disease threats (Saker et al., 2004). Similarly, introduction of a novel disease to a geographic region might lead to continued autochthonous spread of the disease far beyond the initial cases, for example, West Nile virus introduction, or dengue virus in several countries, including the United States. A 2006 report identified three main threat consequences from modern transportation network expansion: (1) infectious disease pandemics; (2) vector invasion events; and (3) importation of vector-borne pathogens (Tatem et al., 2006). The increasing volume and speed of travel allows people to move from one point on the Earth to virtually any other place well within the incubation period of many infectious disease pathogens. Dissemination of infection across the globe can occur within 24 hours. These factors continue to determine the spread of pathogens, witnessed today by the incredibly rapid movement of influenza A(H1N1)pdm09 virus (Colizza et al., 2007), the changes in the geographical spread of Aedes aegypti and Aedes albopictus mosquitos (Els et al., 2018), and the rapid geographical expansion of arboviral pathogens transmitted by these mosquitos, such as dengue, Zika, and chikungunya viruses (Solimini et al., 2018). Although some of these pathogen expansion trends can be attributed to environmental factors favoring the pathogen or vector (e.g. climate, including temperature, humidity, and precipitation) and human factors other than travel (e.g. human population density, increasing incursions of larger numbers of humans into pristine forest and other ecosystems, and environmental destruction that increases vector breeding), it is the rapid and expanding global movement of people, animals, and international trade in agricultural products that is the primary contributor to the spread of infectious diseases that threaten national and regional security (Findlater and Bogoch, 2018). Several examples reflect the silent movement of pathogens via people, reservoir species such as bats and birds that fly long distances, and insect vectors that are trapped and transported on airplanes and find large numbers of susceptible hosts and local vectors capable of amplifying infection rates. Some of these examples include: (1) the recent appearance of Nipah virus in Kerala in
the southwest of India, which is thousands of miles from its endemic location in Bengal (Paul, 2018); (2) the spread of Ebola virus in urban centers of West Africa in 2014 and in the northeast of the Democratic Republic of the Congo in 2018; (3) the introduction and spread of West Nile virus into the United States in 1999 (Roehrig, 2013); (4) the first local transmission of chikungunya virus in the Americas, as identified in Caribbean countries and territories in 2013; and (5) the emergence and pandemic spread of Zika virus in Brazil in 2016 (Proenca-Modena et al., 2018).
FINDING 1.1: The emergence and dissemination of pathogens as reservoir and vector hosts spread into new geographic areas, as well as through movement of humans, international travel, and trade in potentially infected animals, plants, and animal and plant products can cause disease outbreaks in geographically distinct regions and countries with no prior knowledge of or experience with the agent, exposing susceptible humans, animals, or plants, providing opportunities for health risks, economic disruption, and destabilization, and increasing the risk of local outbreaks.
TABLE 2-1 Disease Impacts at the Human–Animal–Environment Interface
| Disease | Situation | Financial Cost | Health Burden | Human–Animal– Environment Interface | Source |
|---|---|---|---|---|---|
| Highly pathogenic avian influenza | January 2004-January 2009, Asia; human and animal health service costs, compensation, production and revenue losses to the livestock sector; losses primarily to smallholder producers in East Asia affecting livelihoods, trade opportunities, food and nutrition security and safety | $20 billion | 486 human cases with 282 deaths | Wild birds mixing with backyard poultry; agricultural intensification without sufficient biosecurity; food security challenges | FAO, 2004; WHO, 2015 |
| Antimicrobial resistance | Estimated cumulative impacts by 2050 | $100 trillion (up to $6.1 trillion/year in high-impact scenario) | 10 million human deaths annually | Agriculture/aquaculture contribute to direct transmission of resistant strains and antimicrobial dispersion; reduced efficacy threatens both health and food production | Jonas et al., 2017; Review on Antimicrobial Resistance, 2014 |
| Severe Acute Respiratory Disease (SARS) | November 2002-July 2003; trade and travel disrupted in China; spread to 29 countries | $41.5 billion | 8,500 cases, 813 deaths | Bat-human contact facilitated disease emergence; live markets may have had an amplification role | World Bank, 2012 |
| East Coast fever | Annually for Kenya, Malawi, Tanzania, and Zambia, from endemic disease; death or reduced growth and productivity | More than $200 million | Tick-borne agricultural disease (cattle, sheep, and goats); threat to livelihood, food and nutrition security | DFID and GalvMED, 2010; Minjauw and Mcleod, 2003 | |
| Schistosomiasis (zoonotic) | Based on estimated 14 percent total schistosomiasis (zoonotic and non-zoonotic) burden; heavily impacting parts of Southeast Asia, some Africa | 10 million DALYs annually | Ecological changes from anthropogenic activity (damming and irrigation) create favorable habitat for vector; non-zoonotic forms can also reduce livestock productivity | Torgerson and Macpherson, 2011 | |
| Top 13 neglected zoonotic diseases of importance to low-income livestock keepers | Zoonotic gastrointestinal disease; leptospirosis; cysticercosis; zoonotic tuberculosis; rabies; leishmaniasis; brucellosis; echinococcosis; toxoplasmosis; Q fever; zoonotic trypanosomosis, hepatitis E; and anthrax | 2.4 billion cases and 2.2 million deaths annually | Various environmental determinants and agricultural exposures | Grace et al., 2012 |
NOTE: DALY, disability-adjusted life year
SOURCE: All figures from Table 2-1 in Berthe et al., 2018, p. 30.
LABORATORY SYNTHESIS OF PATHOGENS
Advances in genetic engineering technologies, including DNA and RNA sequencing and synthesis, and precise editing of genes have lowered the barriers to obtaining pathogens without the need for samples from nature. Use of these, and other advances in molecular biology, to create a pathogen in the laboratory for the purpose of economic gain or to deliberately infect populations for malicious political or military advantage is conceivable and may occur at any time. Examples of advances that enable acquisition or manipulation of pathogens are described here.
Researchers in the United States described the first-ever chemical synthesis of a pathogen (poliovirus) by stitching together short pieces of DNA complementary to the poliovirus genome that were purchased from a commercial service provider, and demonstrated that the synthesized copy of the genome could be used to produce virus that replicated in tissue culture cells (Cello et al., 2002).
Since then, several viruses have been produced from sequence alone through a similar chemical synthesis approach. In 2017, a Canadian research group published the recreation of the extinct horsepox virus, which is a close relative of vaccinia virus (the historical vaccine strain for smallpox), from published sequence information (Noyce et al., 2018). This experiment involved close collaboration between the researchers and the DNA synthesis provider to create the 30 kilobase fragments of the horsepox virus, which presented its own challenges; the required use of DNA structures (specifically, hairpin sequences) taken from the vaccinia virus; and production of the live virus using a helper virus replicating system in tissue culture cells (Gryphon Scientic, 2019).
Although U.S. and Canadian regulators were diligent in analyzing the potential direct risks associated with this work and its publication, this research led many security experts to be concerned about the implications of adversaries replicating similar experiments in order to recreate smallpox itself (Greenfeildboyce, 2018; Koblentz, 2018; Kupferschmidt, 2018; Kushner, 2019). Although the technical know-how and resources needed, and legal restrictions on access to smallpox virus genetic sequences, suggest that these concerns may apply to a very small number of adversaries, the United States’ current select-agent-list-based policies for biosecurity and biodefense work may limit the ability to counter harmful exploitation of the knowledge, skills, and methodologies involved in this and similar work. Despite the difficulty in translating the methods from
horsepox to smallpox (DiEuliis et al., 2017), the implications of this research on acquisition of pathogens highlights the need to monitor science and technology advances beyond a specified list of pathogens and the potential for malicious exploitation. For example, reverse genetics is an established approach to synthesizing virus from sequence alone, which was the method used to resurrect the 1918 influenza virus in 2005 from sequences obtained from cadavers frozen in permafrost (Tumpey et al., 2005), and to create the Ebola virus strain from the 2018-2019 outbreak in the Democratic Republic of the Congo for the purpose of strain characterization (McMullan et al., 2019).
In 2010 and 2016, the J. Craig Venter Institute reported it had created a synthetic bacterial cell and minimal viable bacterial cell, respectively (Hutchison, 2016; IOM, 2011; JCVI, 2008, 2010, 2016). Although the researchers were able to create synthetic bacterial cells at a cost of $40 million (Hotz, 2010), they experienced hurdles in generating live, replicating bacteria from those genomes, including the need for complementarity of genome sequence and cellular parts. In early 2019, U.S. researchers described the creation of live bacteria using chemical synthesis of a rewritten bacterial genome (Venetz et al., 2019), indicating the increasing sophistication of synthetic genomics methods.
In addition to synthesizing viruses and bacteria, the emergence of CRISPR-based genome editing tools has elicited concern about their potential use to create harmful pathogens. In 2016, genome editing was classified as a weapon of mass destruction in a report by the U.S. Office of the Director of National Intelligence (Regalado, 2016; U.S. DNI, 2016). This classification shifted gene editing to an emerging technology to monitor in the 2017 version of the report (U.S. DNI, 2017), and has been discussed at the Meeting of Experts of the Biological and Toxin Weapons Convention (Australian Government, 2018; Mackby, 2018; UN, 2018). Despite these concerns, genome editing tools have been used by researchers for beneficial purposes such as to examine the function of genomic and extra-genomic sequences (Ford et al., 2019; Rousset et al., 2018; Wang et al., 2018) and develop new approaches for treating infections (Bakhrebah et al., 2018; Hamers, 2018; Shabbir et al., 2019).
FINDING 4.3: Methods for engineering and synthesizing viruses and bacteria are being democratized, enabling easier access to pathogens created or modified from gene sequence data. Although the skills, knowledge, and human and financial resources needed to create or modify live pathogens from chemical synthesis, reverse genetics, or genome editing
are specialized and high, their use may be possible by scientists from nation states and well-resourced non-state actors intent on using microbial pathogens for malicious purposes.
FINDING 2.2: New scientific advances, including multi-use technologies, methods, and information highlight the need for more robust approaches for analyzing the anticipated and unanticipated consequences of scientific efforts, including misuse, reducing potential risks, and reaping the scientific benefits for prevention and detection of biological risks.
EMERGING BIOTECHNOLOGY
Several significant changes and advances in biotechnology have occurred during the past decade, which have significant implications for the biological threat landscape and for medical progress. Although these changes do not encompass all advances in biotechnology, they do illustrate the need to account for different individuals, organizations, countries, and fields that could enable or limit threat reduction investments or enhance vulnerabilities and risk in partner countries.
Design and development of biological systems and examination of biological data have expanded well beyond the biomedical and biological sciences to include trained specialists in engineering, computer information and data, and material sciences. In addition, expertise also resides in formally untrained practitioners from the do-it-yourself and amateur biology communities, some of whom may be technically competent but lack the essential ancillary training of the professional workforce, including the ethical norms and legal boundaries about what is permissible science and behavior, and the reinforcement provided by professional peers and formal institutions. These new practitioners simultaneously have enabled new industries, digitalization of biology, and design of new technologies to manipulate biological materials while also challenging current governance and oversight structures within and outside the United States. Fields such as synthetic biology, which is distinguished from genetic engineering by the use of engineering-based problem solving (i.e., the design–build–test–learn cycle), have been a primary means through which both technically and nontechnically trained individuals have engaged in the biological sciences. Information may be
disseminated via various social media platforms and chat groups, rather than through peer-reviewed literature or at high-level academic conferences. These changes have resulted in new international competitions involving high school and college-level students in bioengineering, new applications in industrial chemistry and biology, new platforms for vaccine and therapeutics development, and new design-based approaches for manipulating biological systems and enabling the creation of non-natural materials, synthetic pathogens, and novel organisms.
Advanced biotechnology integrates expertise from teams of scientists and engineers from multiple disciplines, optimizing the speed of development and commercial potential of new technologies, applications, and services in health and the life sciences. This environment has facilitated entrepreneurial efforts, spawning numerous companies that combine computational design, robotics, and bioengineering to create new organisms that produce desired products including chemicals and their precursor molecules, drugs and their precursors, and proteins including biologically active toxins. Further facilitating these efforts is the use of genome editing tools that enable precise genetic changes in an organism’s DNA. Although genome editing tools are more advantageous for modifying plant, animal, and human cells than many bacteria, viruses, and yeast, for which established and robust engineering technologies exist, the growing awareness of the risks of genome editing tools to national and international security has elicited concern among security experts.
Similarly, biology has become significantly more dependent on computation and information science systems. The increasing reliance on software to collect and compile data, digital databases that allow for deposition and recall of scientific data, computational algorithms and cloud-computing environments to analyze data, design software to engineer biological systems, and laboratory control systems has enabled a whole new set of opportunities for scientific advancement and challenges for national security. Real and potential compromise of these software systems has introduced a new set of problems that often do not conform to pathogen-based threat reduction measures but could have significant effects on human and animal health systems, agriculture, industry, and economic stability. In addition, the Fourth Industrial Revolution (World Economic Forum, 2019) in biotechnology (i.e., the coupling of digital and physical systems in the biological sciences) has provided opportunities for countries that have strong talent in computer and data science to become competitors to the United States in these fields. One possible outcome of
this situation is the exploitation of data and these capabilities by adversaries against U.S. entities and interests. Although the United States and its allies likely will continue innovating and advancing biology and biotechnology, they will not be the only voice internationally in setting norms for responsible science, a phenomenon currently being observed through the completed and proposed plans for editing of live, viable human embryos. Differences among countries’ norms for ethical life sciences (including professional and behavioral norms against the development, production, and stockpiling of biological weapons, or the use of biotechnology for destructive purposes) could counteract past and current BTRP efforts.
Enabling advances in these and other fields is the operating mission of existing and new funders. In 2017, Science reported that less than 50 percent of research conducted in the United States is funded by the U.S. government (Mervis, 2017; NSB, 2018). Nongovernmental funders include philanthropic organizations, private companies, venture capital, foreign governments, and even the public through crowdsourcing. This expansion of funders provides opportunities for researchers to secure support for innovative and high-risk/high-reward projects, while simultaneously diluting requirements for oversight of research. For example, the Canadian researchers who synthetized horsepox virus from published genetic sequence data, received funds from a private U.S. company (DiEuliis et al., 2017). In addition, investments in biotechnology are viewed as important to the social and economic well-being of increasing numbers of countries internationally, including some low-income and/or conflict-ridden countries. BRTP’s objectives align well with broader efforts to ensure international norms against the use of scientific knowledge, skills, technologies, and equipment to harm people, animals, and plants.
FINDING 6.2: The biological sciences and biotechnology are advancing at a pace that far exceeds current security assessments. Although the future is always hard to predict, the potential for DOD to anticipate current and future capabilities and uses cannot be based on current scientific and technological activities alone, but rather must be amplified by accessing insights into where that science is going, what is the leading edge, and what are the hot topics and breakthrough achievements. This requires a sufficient and critical mass of well-trained scientists from diverse fields within the agency. The ability of these scientists to contribute
fully will be strengthened by participation in high-level scientific conferences, reading of relevant publications, and networking with academia and leading biotechnology companies. They could also benefit from engagement with a high-level external scientific advisory group composed of experts in diverse scientific disciplines, particularly individuals with relevant international experience.
DATA SECURITY
Several years ago, BTRP began building national and regional capacity to detect emerging pathogens through molecular diagnostics (i.e., next-generation sequencing and bioinformatics analysis), rather than traditional microbiological techniques (i.e., culturing of pathogens in the laboratory), and through regional networks for bat surveillance (Fair, 2017; U.S. DOD, 2015). The data generated through sequencing, shared among partners, analyzed using software, and stored in digital formats may be vulnerable to cyber-attack. Data and software provenance and integrity is extremely important for these biosurveillance efforts to help diagnostic and research scientists accurately identify and characterize pathogens circulating in wildlife and infecting animals and humans. Therefore, breaches of the information systems that generate, transmit, and store data and the software that is used to analyze data can compromise the results, which could alter detection of biological threats and determination of their origins (i.e., naturally occurring, accidental, or intentionally released) (Berger and Schneck, 2019; Murch and DiEuliis, 2019).
FINDING 2.3: Facilities and information systems using cybersecurity and data security approaches are vulnerable to exploitation by malicious actors who could access, monitor, steal, or manipulate data and analytic results remotely and without notice, or disrupt the flow of data to scientific partners. Cyber-related threats now include threats to facilities and information systems, harmful use of genomics and advanced data analytics, and the development of new biological systems.
POLICY FRAMEWORK FOR BTRP PLANNING AND INVESTMENT
Although BTRP is a component of the Defense Threat Reduction Agency, it receives its programmatic determinations through a process led by the Office of the Secretary of Defense for Policy (OSD(P)). This process involves identification of priority countries and overarching initiatives through consultation3 with BTRP leadership in accordance with the National Security and National Defense Strategies. In addition to aligning BTRP efforts with the National Security Strategy and National Defense Strategy objectives, OSD(P) has three criteria it uses to determine with which countries BTRP should partner: (1) countries where biological threats exist; (2) countries that have poor infrastructure to address biological threats and risks; and (3) countries at risk of state and non-state use of biological agents as weapons. OSD(P) works closely with the Department of State and Congress to coordinate efforts and seek approval for country engagement on topics of national security interest. This determination process can be lengthy (at times taking years), in part because requests for new determinations may be deprioritized for other, more pressing requests, and due to the limited capacity of OSD(P) to review multiple requests simultaneously. However, once this process is complete and Congress has given its approval, the determination is made and sent to BTRP for implementation. At this stage, BTRP is responsible for developing its 5-year strategy for threat reduction within the determinations provided. Although the determination process can be long and BTRP plans 5 years in the future, it does have some authority to allocate funds for emerging issues if the need arises, as described further below.
Throughout its existence, BTRP has revised its approach several times in response to changing conditions to achieve its goals of (1) facilitating “elimination and safe and secure transport and storage of biological weapons, components, related materials, and delivery vehicles”; (2) preventing “proliferation of biological weapons, components, and related materials, technology, and expertise”; and (3) preventing “proliferation of weapons of mass destruction-related materials, equipment, and technology that could be used for the design, development, production, or use of biological weapons and their means of delivery” (Newman, 2018). Since
___________________
3 Previously, consultation involved an advisory group called the Threat Reduction Advisory Committee, which ended on December 16, 2019 (Federal Register, 2019).
2009, when the National Academy of Sciences (NAS) published its report, Global Security Engagement: A New Model for Cooperative Threat Reduction, BTRP has expanded its investments into at least 27 countries in four continents and has supported projects in three broad categories: (1) building in-country capabilities for detection and surveillance of biological agents; (2) conducting research on pathogens of interest; and (3) enhancing safety and security of laboratories that handle biological agents. For several years, BTRP has been authorized to support programs to prevent and detect incidents involving especially dangerous pathogens, including pathogens on the Biological Select Agents and Toxins list, emerging pathogens, and naturally occurring pathogens that may cause public health emergencies of international concern. These categories also reflect priority actions for IHR (2005) and GHSA. BTRP defines country-specific engagements through the Program Objective Memorandum process in which it charts its 5-year plan for investments in countries and regions of interest, promoting sustainable, goal-oriented planning for its investments. This process does not prevent BTRP from being agile in an outbreak or other emergency situation if its unique capabilities are needed. Throughout this process, BTRP can work with combatant commands to provide support for regional initiatives if they fall within the scope of BTRP guidance and legal authorization. BTRP collaborates with governmental partners in-country to assess and/or identify needs and collect funding proposals that align with the Program Objective Memorandum for the respective country. Finally, BTRP can interact with embassies to promote its initiatives and programs.
Box 2-2 provides the legal framework for BTRP by statute, the National Defense Strategy, the National Security Strategy, the National Biodefense Strategy, the National Strategy for Countering Weapons of Mass Destruction Terrorism, and the Global Health Security Strategy.
FINDING 1.2: BTRP is constrained by both political and geographic requirements that inhibit its ability to respond nimbly to emergent threats. As a result, BTRP is unable to keep pace with the speed at which science and technology are changing the biological risk landscape, reducing its ability to preclude or mitigate potential threats as they emerge.
METRICS AND EVALUATION FOR BIOLOGICAL THREAT REDUCTION PROGRAMS
Metrics and evaluation are an important part of any program, not only to guide continuing improvement, but also as a way to enable funders to assess progress toward achieving their goals and advocate for their budgets. At the request of BTRP, the RAND Corporation published a conceptual framework in 2014 for measuring the performance of bioengagement initiatives (Young et al., 2014). This framework focused on building capacity, capability, and sustainability in partner countries using a combination of quantitative and qualitative metrics. Two years earlier, NAS completed its study on metrics for DOD Cooperative Threat Reduction. This report highlighted key concepts, such as the need to clearly state the program’s objectives and role in addressing biological threats and risks, jointly develop objectives with partner countries to enable buy-in and sustainability, prioritize and refine the metrics over time, and allow for independent evaluation. Furthermore, the NAS committee stressed the importance of tailoring metrics to the scale, scope, and objectives of funded projects and of evaluating achievement toward overall project goals rather than a compilation of measurable activities. In addition to these efforts, the Department of State Biological Engagement Program supported at least two initiatives to develop metrics for its bioengagement program, and other groups have also proposed frameworks for evaluating success of implemented programs (Gryphon Scientic, 2019).
Drawing on these efforts, measuring the success of a project, country portfolio, or a single initiative across several countries involves a two-step process. Together, these steps help to identify the goals or activities that are achieved, factors that promote or enhance successful implementation, and hurdles that need to be overcome before goals are achieved. Although quantitative measures can be identified for specific activities (e.g., the number of individuals trained), achievement of the overall goal of the
effort (e.g., to enhance regional leadership of a partner country in biosafety and biosecurity) likely can only be assessed using qualitative measures. Furthermore, successful achievement of measurable evaluation criteria does not necessarily indicate that the intended goals of the effort have been achieved, a concept that is supported by the 2012 NAS report. Similarly, despite the fact that certain measurable outcomes of a project or activity may indicate failure, achievement of the overall goals may still be achieved. “It is possible to successfully accomplish what is easily measurable and fail in the engagement.” The converse is also true (NAS, 2012, p. 3). As facilitating factors and hurdles are identified throughout project implementation and the evaluation process, they can be incorporated into lessons learned (and, possibly inform the development of best engagement practices) for consideration in future engagements. Another relevant consideration for evaluating country portfolios is the existence of frameworks, such as the JEEs, that countries already may be using to identify gaps, prioritize their own investments and activities, and coordinate with external partners and funders. Developing activity- and goal-based evaluation approaches that can be used to support, complement, and coordinate with the JEE or another process increases the potential for partner country buy-in and sustainability of capabilities.
FINDING 4.4: Measuring threat reduction from engagement programs is difficult. Common quantitative metrics are ineffective. The program needs to continue to develop and try out new approaches, such as the use of a quasi-qualitative rubric for measuring achievement of individual activities and overall goals of projects, country portfolios, and program initiatives. Such non-traditional measurements provide opportunities to course-correct when hurdles are encountered, support conditions and factors that facilitate achievement of goals, and promote partner country buy-in and sustainability of capabilities. This approach to metrics can help to demonstrate accountability, and provide greater awareness of program results and context of engagement, to DOD senior leaders, Congress, and other relevant stakeholders.
This page intentionally left blank.


































