3
Addressing Biothreats through Successful
Engagement
KEY MESSAGES
- Working effectively in host countries depends on the ability to communicate with local leadership, and to coordinate with multiple actors–both domestic and international. This, in turn, depends on diplomatic skills and the ability to develop, deepen, and sustain personal relationships of trust with counterparts in the host country.
- Biological Threat Reduction Program (BTRP) initiatives rely on partner country interest, perception of need, and governance structures, which can be achieved best when the diplomatic skills needed to work closely and respectfully with country partners are well developed.
- Biosecurity is not only directly affected by critical scientific disciplines, but also by interdisciplinary perspectives, and indirectly by social, economic, and cultural concerns that may be unique to the BTRP partner country.
BENEFITS OF SCIENTIFIC ENGAGEMENT TO BIOTHREAT REDUCTION
Engagement of scientists has been a cornerstone of biological threat reduction programs since their formal inception in the 1990s. The U.S. Department of Defense (DOD) promoted peaceful use of scientific knowledge and skills in the former Soviet Union with scientific partnerships. During the past decade, these engagements have provided opportunities to broach the concepts of biosafety and biosecurity with scientists in countries that never supported offensive bioweapons research and development, and to enhance biosurveillance capabilities in partner
countries using safer technologies, such as next-generation sequencing. More generally, scientist engagement ensures that activities are appropriate for the local research and public health, policy, threat and risk, and socio-cultural contexts. Furthermore, partnerships among physicians, veterinarians, public health practitioners, and scientists help to build local One Health (interlinked human, animal, plant, and environmental health) capabilities, enabling countries to prevent, detect, and respond to health security threats. Engagement also provides opportunities for scientists to become part of international research and health networks, which enables sharing of norms, awareness-raising of emerging threats and threat mitigation strategies, access to training programs and funding opportunities, and expert consultation. Long-term partnerships promote the realization of the benefits to scientists and the international community.
What Principles Guide Successful Biosecurity and Health Security Programs?
Biosecurity investments focus on natural, accidental, and intentional biological threats. More broadly, DOD investments in global health security help to prevent the spread of human and animal infectious diseases and reduce the risk of biothreats to deployed U.S. military forces, American citizens living or traveling abroad, and as a consequence to local populations as well. “At the core of global health security is a strong health system with the resources and personnel necessary to identify infectious disease threats and respond quickly before regional or global transmission” (White House, 2019, p. 7). Successful biosecurity and health security assistance programs are guided by particular principles of engagement, listed here from strategic to practical.
- All biological threats—natural, accidental, and intentional—are most effectively treated as a single challenge with many dimensions.
- To maximize biosecurity and global health security, all countries need to address naturally occurring, accidentally caused, or intentionally introduced threats and risks although the specifics of those threats and risks and associated activities will differ in different countries.
- The overall biosecurity mission encompasses anticipation, deterrence, prevention, detection, response, mitigation, and recovery. Action or intervention is possible at every stage.
- Biosecurity investments focusing on prevention and preparedness are far more cost-effective than those focusing on response.
- Successful and sustainable engagements need to be tailored to the needs of a particular country and formulated with an understanding of the overall context, which encompasses political, military, social, economic, and cultural dynamics.
- Those tailored engagements may include, if appropriate, the collaborative, multisectoral, and transdisciplinary approach known as One Health, which recognizes the interconnections among people, animals, plants, and the environment.
- Host governments need to take ownership of and support programs for such programs to be effective and sustainable.
- Biosecurity investments need to be flexible and timely while trying to anticipate future threats–both the what and the where, even if the when cannot be estimated.
Successful programs match people, and the most effective engagements involve collaborative partnerships and strong relationships among trusted, credible, and knowledgeable interlocutors built over time; through trust in such relationships, contentious issues can more readily be resolved and trust between nations can be enhanced. Establishing such trusted relationships is challenging, however. Each country has its own professional culture, bureaucratic tendencies, systems of incentives and disincentives, traditions and practices, policies and procedures associated with even minor tasks, not to mention schedules of holidays, celebrations, observances, and vacations. Navigating these complexities is not easy and requires a deftness of professional engagement that is as difficult to cultivate as it is essential to success.
- The most effective programmatic investments build on existing infrastructure and complement other related or overlapping programs.
- Strengthening biosafety and biosecurity systems requires interdisciplinary, whole-of-government collaboration, to include foreign, defense, finance, health, agriculture, environment, law enforcement, education, and other departments/ministries.
- Strengthening of such systems requires facilities to identify, secure, safely monitor, and store dangerous pathogens, including clinical and environmental samples that may contain viable dangerous pathogens.
- Promoting a culture of biosafety, biosecurity, and responsible conduct in the life sciences and identifying and responding effectively to biosafety and biosecurity emergencies is also essential.
- Programs need clear lines of authority, accountability and responsibility; transparent data and information systems; and a robust monitoring and evaluation framework.
- The impact of biosecurity and biosafety engagement will be maximized by fostering linkages, synergies, and partnership among experts in regional and global networks; we are better off working together than separately.
FINDING 1.4: Natural, accidental, and internationally caused outbreaks can have similar consequences for health, the economy, and national security. Despite the initial cause of the outbreak, they also have similar requirements related to common prevention, detection, response, and recovery initiatives. There are advantages to addressing these events as different manifestations of the same family of challenges. An integrated view of biological threats prevents bureaucratic boundaries from interfering with partnerships and progress. Natural, accidental, and intentional outbreaks may have ambiguous origins but the capabilities needed to address them overlap. Ultimately, needs of force protection and national health and safety may be similar in most cases, especially those with the broadest potential national security impact.
The Importance of Coordination and Communication to Engage Successfully
No U.S. government program currently has or should be expected to have the authority or the capability to act on every aspect of biosecurity; but today, organizational divisions and boundaries in the United States and globally can interfere with realizing improvements in efficiency and cost-effectiveness. To address that problem, BTRP needs to be part of a regular interagency coordination mechanism focused on mission problems and opportunities rather than on agencies and jurisdictions. Similarly, there should be regular intergovernmental discussions to connect and coordinate U.S. government and international community efforts to anticipate problems and develop interventions throughout the biological threat lifecycle.
BTRP would benefit from engaging more deeply with experts across the U.S. government and with a variety of scientists from numerous institutions that hold meetings at various public scientific forums on the
broad spectrum of natural, accidental, and intentional biological threats (e.g., the International Conference on Emerging Infectious Diseases, American Society for Microbiology, Infectious Diseases Society of America, Association of Healthcare Emergency Preparedness Professionals, and American Biological Safety Association).
BTRP endorses interdisciplinary coordination in approaching complex problems, such as preparing for naturally occurring emerging infectious disease threats through One Health approaches. However, BTRP is insufficiently engaged with agricultural institutions and One Health programs. With interest in working with international partners for better global health, and in particular, infectious diseases, increased communication with these organizations to better coordinate funds and avoid unnecessary duplication of efforts in regions would be beneficial. This would increase the effectiveness of the funding on all three sides—the U.S. government, the U.S. or other nongovernmental organizations, and the country partner.
Deeper understanding and engagement with agricultural institutions and agricultural businesses is important for improved biosecurity, as many new and emerging pathogenic threats are projected to be zoonotic (Mark et al., 2016). Several other organizations have related efforts with which BTRP should more thoroughly engage: U.S. Department of Agriculture, including the Agricultural Research Service, the Animal and Plant Health Inspection Service, the Food Safety and Inspection Service, and the new National Bio and Agro-Defense Facility under construction in Manhattan, Kansas; U.S. Agency for International Development efforts to strengthen global capacity for detection and discovery of zoonotic viruses with pandemic potential, and the Infectious Disease Detection and Surveillance project improving the quality of real-time surveillance of antimicrobial resistance and zoonotic diseases; the World Organisation for Animal Health (OIE); the Food and Agriculture Organization of the United Nations (FAO); and veterinary and agricultural colleges.
ONE HEALTH
The One Health approach is increasingly endorsed by many professional, governmental, and international organizations as the best approach for addressing complex problems such as emerging infectious diseases, food security, and antimicrobial resistance (See Box 3-1 for the example of the Bat One Health Research Network). As the U.S. Centers
for Disease Control and Prevention (CDC) notes, “One Health is not a new concept, but it has become more important in recent years. This is because many factors have changed interactions between people, animals, and our environment. These changes have led to the emergence and reemergence of many diseases” (CDC, 2018).
One Health promotes an integrated approach to infectious disease, linking efforts toward promoting human, animal, plant, and environmental health. Involvement of FAO in the Global Health Security Agenda
(GHSA) suggests that opportunities to more effectively include plant pathogens in the discussions, through the agriculture and food system, may be developing as a critical and currently unmet need of global health security initiatives (See Box 3-2). The danger of emerging plant pathogens and the potentially devastating effects of a pandemic affecting critical food crops is much enhanced by the widespread practice, especially in large-scale agriculture, of monocropping (McDonald and Stukenbrock, 2016).
One deficit in many One Health training and implementation programs is the common tendency to neglect the food–animal production industry (Gray and Mazet, 2019). Within these industries, many new pathogenic threats are emerging or being amplified, threatening both livestock and, directly and indirectly, humans as well. This situation is caused, in part, by the increasing scale of modern industries, providing large, dynamic populations of animals that can be decimated completely if exposed to a pathogen that cannot be controlled by current veterinary and biosecurity practices. Outbreaks in these larger animal populations may also affect animals on smaller farms. The now-endemic pathogen could become susceptible to continued pressures to evolve and possibly become more virulent to humans and/or animals (Gray and Merchant,
2018). Examples include antimicrobial-resistant pathogens in poultry and swine, which have been linked to human morbidity (Marshall and Levy, 2011), and the many types of influenza A virus, which now freely circulate in swine (Borkenhagen et al., 2019) and could have pandemic potential in humans.
A decade ago there were anticipations of global spread of African Swine Fever (ASF) and measures to prepare to prevent or respond to a pandemic outbreak were not systematically implemented prior to the current rapidly spreading multi-country outbreak of ASF in Asia (Costard et al., 2009). Box 3-3 highlights an example of a BTRP engagement that builds on these One Health concepts.
FINDING 5.2: The inextricable links among human, animal, plant, and environmental health highlight the risk of natural or human-made pathogens in the food system, along trade and travel routes, and through changes in the environment. Each of these factors can either severely affect production of major plant food crops and meat products, or promote the appearance and spread of new potentially zoonotic infectious disease threats to humans in addition to their impacts on the affected animal populations. These risks could result in significant health, social, political, and economic consequences leading directly to political and civil unrest–especially in countries with pre-existing marginal or unstable governmental systems and weak infrastructure.
FINDING 5.3: Inadequate provision of fundamental needs, such as food and clean water, enables transmission of environmental pathogens into the human population and increases opportunities for conflict, which present a different type of security risk.
TRUSTED RELATIONSHIPS ARE CRITICAL TO SUCCESS
As stated earlier in this report, the success of an international engagement program typically is not achieved solely because of the program, the training, the research, the introduction of a new technology, or even the money (Carmeli et al., 2012). While formal institutional relationships are, of course, critical, highly successful and sustainable engagements are often the result of two or more individuals who may come from widely diverse backgrounds in their respective home countries but who see a common need, generally agree regarding how to address that need, and are able to work together in an environment of openness and trust. It is not unusual for the most effective relationships to be formed between individuals of similar stature in their respective communities (Brown and Franz, 2016).
This is not the first time that the importance of human relationships in Cooperative Threat Reduction (CTR) programs has been underscored. One of the recommendations in the 2009 National Academy of Sciences report called for the recognition, “that personal relationships and professional networks that are developed through U.S. government CTR
programs contribute directly to our national security and that new metrics should be developed to reflect this” (NAS, 2009, p. 13).
It is easier to measure activities than to measure the impact of relationships. Seeking success and program efficiency, the DOD CTR Program has spent hundreds of thousands of (engagement) dollars asking domestic academics and nongovernmental organizations (NGOs) to design systems of metrics with which to evaluate the effectiveness of engagements. There is little evidence that these costly and often very complex schemes have been useful or even used. In 2016, some senior staff members from BTRP and their collaborators authored a paper titled, Scientific Collaborations: How Do We Measure the Return on Relationships? (Fair et al., 2016). This paper, particularly coming from within BTRP, is an important recognition of the principle and the consistent identification of relationships of trust as a critical factor underlying successful collaborations.
This study committee underscores the notion that human relationships of trust not only contribute to the effectiveness of engagement programs but are critical to success, sustainability, and the positive security effects that must be generated. When these relationships are established between serious and professionally compatible individuals, confidence, trust, openness, and truly effective communication often results. The BTRP publication describes the value of visualizing and quantifying scientific social networks that develop from a specific event–such as a training workshop–to estimate the impact of collaborations on a field or mission, such as reducing the threat of infectious diseases. This depends on support of investigators to “communicate and coordinate their research, training, and educational activities across disciplinary, organizational, geographic, and international boundaries,” and the use of alternative metrics to generate real-time evidence of research influence (Fair et al., 2016, p. 6). This may be through social media as a means of assessing how the work is being discussed and shared, and by whom, including researchers as well as the public. The committee also recognizes that this return on relationships (sometimes referred to as “ROR”) concept (Fair et al., 2016, p. 2) is a hard lesson for U.S. engagement programs and implementers to absorb and operationalize, and that it will require considerable discussion and development of tools tied to assessing the impact of CTR programs for the concept to be fully adopted.
FINDING 3.1: Successful programs match people from the two partner countries who have the necessary technical and
diplomatic skills, and the willingness to develop relationships of trust through working together toward common goals. These interpersonal relationships form the resilient core of the larger institutional relationships.
There are a number of prior examples of U.S. government-led and -supported global programs that have succeeded and improved response to infectious disease threats, and provide insights for BTRP to consider.
LEARNING FROM DISPARATE EXPERIENCE
An Example of Success Fighting against a Deadly Infectious Disease Pandemic Threatening Stability and Security: The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR)
HIV/AIDS, a threat of zoonotic origin, has been an ongoing pandemic for nearly four decades. While there has been enormous progress to control and treat HIV, the virus still defies global efforts to halt transmission. In the early to mid-1990s, before highly active antiretroviral therapy became affordable for large numbers of people, the pandemic grew dramatically. Many believed it not only threatened the stability of the hardest-hit countries, but also represented a security threat for countries like the United States.
For the first time in history, the United Nations Security Council discussed a health issue as a threat to international peace and security. Vice President Al Gore presided over the meeting on January 10, 2000 (UN, 2000b) as United Nations (UN) Secretary-General Kofi Annan explained the security implications of the pandemic:
The impact of AIDS in [southern and eastern Africa] is no less destructive than that of warfare itself. Indeed, by some measures it is far worse. Last year, AIDS killed about ten times more people in Africa than did armed conflict.
By overwhelming the continent’s health services, by creating millions of orphans and by decimating health workers and teachers, AIDS is causing social and economic crises which in turn threaten political stability. It also threatens good governance, through high death rates among the elites, both public and private.
In already unstable societies, this cocktail of disasters is a sure recipe for more conflict. And conflict, in turn, provides fertile ground for further infections. The breakdown of health and education services, the obstruction of humanitarian assistance, the displacement of whole populations and a high infection rate among soldiers—as in other groups which move back and forth across the continent—all these ensure that the epidemic spreads ever further and faster. (UN, 2000a)
During his State of the Union address in January 2003, President George W. Bush announced what has come to be known as the President’s Emergency Plan for AIDS Relief (PEPFAR), which received strong bipartisan support from Congress.
PEPFAR is the largest commitment by any nation in the world to address a single disease and is generally viewed as one of the most significant and successful global health initiatives ever undertaken. It is a prime example of the U.S. government generating trust and respect from citizens and governments. Initially authorized at a level of $15 billion over 5 years, the PEPFAR appropriation for FY 2018 totaled more than $6.5 billion, with 79 percent for bilateral HIV programs and 21 percent allocated to the Global Fund to Fight AIDS, Tuberculosis and Malaria (KFF, 2019b).
The program has saved millions of lives over the years. In FY 2018, through PEPFAR support, nearly 14.8 million people received antiretroviral therapy and nearly 6.4 million were supported through orphans and vulnerable children programs (PEPFAR, 2019b). As of September 2018, PEPFAR has “supported testing services for nearly 95 million people; prevented more than 2.4 million babies from being born with HIV, who would have otherwise been infected; provided care for more than 6.8 million orphans and vulnerable children; supported training for more than 270,000 new healthcare workers; and, supported antiretroviral treatment for more than 14.6 million people” (PEPFAR 2018).
In recognition of the security implications of the HIV/AIDS pandemic, particularly when the partner country military is itself significantly infected by the virus, DOD has been an important provider of PEPFAR assistance.
DOD implements portions of the PEPFAR programs by supporting HIV/AIDS prevention, treatment, and care; providing strategic information; supporting human capacity development; and facilitating
“program and policy development in host militaries and civilian communities of 73 countries around the world. These activities are accomplished through direct military-to-military assistance, support to NGOs and universities, and collaboration with other U.S. government agencies in-country. Members of the defense forces in 13 PEPFAR focus countries have been the recipients of DOD military-specific HIV/AIDS prevention programs designed to address their unique risk factors, in addition to treatment and care programs for their personnel. In these 13 countries alone, military programs have the potential to make an impact on more than 1.2 million people, including active-duty troops, their dependents, employees, and surrounding civilian communities. DOD supports a broad spectrum of military-specific HIV-prevention programs, infrastructure development and support (including laboratory, clinic and hospital facility renovation, equipment, and training), and treatment and care activities” (PEPFAR, 2019c).
PEPFAR’s focus on prevention, care, and treatment of HIV/AIDS requires a very high level of collaboration within the U.S. government, with civil society and the private sector, with a multitude of bilateral and multilateral institutions, and with many other stakeholders. Cooperation with the host government and its military forces is fundamental to the success of the program.
An essential element of PEPFAR’s success, and one worth emulating, has been its use of a coordinating mechanism known as Country Operational Plans. PEPFAR emphasizes that it “is committed to continually strengthening its partnership with host-country governments to ensure alignment between PEPFAR contributions and national priorities and investments. Collaborative planning between PEPFAR and host-country governments is critical to ensuring that prioritized interventions are scaled, geographic priorities are shared, and that all available resources for HIV/AIDS in the country are utilized optimally” (PEPFAR, 2019a, p. 109).
In a presentation at a 2018 National Academies of Sciences, Engineering, and Medicine workshop in Amsterdam focused on assisting infectious disease laboratories in low-resource countries, Jonathan Towner of CDC said that it is often easier to add on to an existing laboratory than to build a new laboratory. In that respect, the many HIV diagnostic laboratories established by PEPFAR across Africa have become a great resource for combating other infectious diseases when additional capacities were needed. Towner provided examples: CDC converted the HIV diagnostic laboratory in Luanda, Angola, and built on the HIV
laboratory in Gulu, Uganda, for diagnostic work on viral hemorrhagic fevers. This study committee notes that these established laboratories are more than buildings and equipment. They are useful because they are institutions, with trained people, practices, organization, relationships, and established supply chains. Utilization of these investments is a model of how to leverage engagements (NASEM, 2019).
An Example of the Spread of a Deadly, Previously Unknown Pathogen that Was Stopped through Effective Governmental Action: The SARS Outbreak (2003)
One particularly dramatic example of an emerging infectious disease outbreak is the 2003 Severe Acute Respiratory Syndrome (SARS) outbreak, a contemporary example of the sudden appearance of a previously unknown pathogen that spread around the world as infected individuals rapidly traveled to distant countries via air routes. It eventually infected at least 8,096 persons with proven or probable SARS, resulting in 774 deaths (CDC, 2016).
The sequence of events is now well known. The initial indication of a new outbreak reached public attention via a report in ProMED-mail (Program for Monitoring Emerging Diseases) on February 10, 2003, followed by a report on February 11 that the Chinese Ministry of Health was aware of 300 cases of an atypical pneumonia syndrome in Guangdong province in southern China (ISID, 2003a, b). One month later, cases were also identified in Hong Kong and Vietnam, and the World Health Organization (WHO) and CDC issued health alert notifications (WHO, 2003). Laboratory analysis at CDC, the Bernard Nocht Institute for Tropical Medicine in Hamburg, Germany, and Queen Mary Hospital, University of Hong Kong, indicated the cause to be a previously unknown coronavirus, soon to be named SARS (Drosten et al., 2003; Ksiazek et al., 2003; Peiris et al., 2003). Over the next 4 months, as the outbreak affected Canada and the United States, CDC assigned more than 800 staff to the response, both domestically and internationally. CDC issued infection control guidance for patients with suspected SARS, interim laboratory biosafety guidelines for handling and processing specimens from these patients, and guidelines for management of exposures to SARS in healthcare and other institutional settings. CDC also provided travel alerts and advisories for U.S. citizens regarding travel to high-risk destinations. CDC contributed the equivalent of 46,714 days of work to the SARS response, met nearly 12,000 flights, and distributed more than 2.7 million
health alert notices to passengers arriving directly and indirectly from affected areas. When ill passengers were reported on a flight arriving in the United States, they were met by members of the CDC quarantine staff to evaluate the affected passenger for possible SARS, provide referrals to a healthcare provider, collect locating information from other passengers, and coordinate with federal, state, and local public health authorities (IOM, 2004).
By the end of the outbreak there were 438 probable and suspect cases of SARS in Canada, primarily in Toronto, including 44 deaths and 25,000 Toronto residents placed in quarantine (Health Canada, 2003). By contrast in the United States there were just eight proven, 19 probable, and 137 suspected SARS infections reported, with no fatalities (CDC, 2003). Had the United States not taken sufficient action to prevent the spread of SARS into the country, the SARS outbreak undoubtedly would have resulted in many U.S. fatalities and huge expenditures. By operating as it was designed and should do, including quick action, a prepared public health system, and a vigorous response prevented a larger outbreak with serious outcomes.
SARS heightened awareness among the international public health and political communities that every country faced biothreats, ranging from newly emerging diseases to bioterrorism, that might not be foreseeable, and it spurred completion of the revised International Health Regulations (IHR) (2005). The outbreak also demonstrated the importance of disease surveillance of transborder diseases through networks and underscored the nexus between animal health and human health, with concerns ranging from small wet markets to large-scale agricultural operations. Rapidly moving pathogens of pandemic concern are at the human–animal intersection. And it is noteworthy that the second wave of SARS, in Toronto in May 2003, is believed to have come from relaxed use of infection-control precautions–thereby emphasizing the critical role of strict biosecurity and biosafety procedures. The U.S. government’s response to SARS carries lessons for the many government agencies working to reduce biological threats, including the Defense Threat Reduction Agency and BTRP, to improve disease surveillance and biosecurity aspects of the response to prevent, mitigate, and control outbreaks in partner countries. Through effective engagement, BTRP can contribute to establishing the means by which emerging diseases can be detected early and response can be initiated safely, securely, and rapidly.
An analysis done at the U.S. Air Force Counterproliferation Center explains the direct relevance to military commanders to outbreaks such as SARS:
Several key points for military commanders should be highlighted from the international lessons learned regarding quarantine and SARS. First and foremost is the understanding that the most severe biologic event a commander may encounter is a previously unknown disease with human-to-human transmission, primarily involving the respiratory route. A new disease like SARS, or a genetically altered agent that may be used by a bioterrorist, requires additional planning for this worst-case scenario. Quarantine needs to be part of the strategy, as was shown with SARS. Second, delay in implementing quarantine can have devastating effects that result in loss of situational control as occurred in China. Decisive actions must be taken and coordinated up the chain of command prior to a commander having sufficient information to make a decision. Third, healthcare workers are at highest risk of becoming exposed or infected prior to identification of the outbreak, which may result in the need for quarantine of entire medical facilities. Fourth, cooperation between support agencies is critical to educate the community, encourage medical identification and treatment, increase patient compliance, enforce requirements when needed, and obtain overall buy-in from the public. Fifth, broad legal and policy challenges exist in responding to an infectious disease outbreak, and guidance is needed to orchestrate a prompt and effective response. This should be addressed prior to a crisis. Sixth, the quarantine implementation plan chosen by leadership should provide the best opportunity to contain the disease without enforcing excessive or unrealistic restrictions on a community as occurred in China and Taiwan. Finally, each disease is unique, requiring an understanding of its epidemiology to ultimately develop a definitive treatment strategy; however the initial response prior to identification of the infectious agent should be nonspecific and cover a worst-case scenario. (Miller, 2005)
An Example of a Previously Known Pathogen Unexpectedly Appearing in a New Location and the Response to a Sudden Transboundary Biological Threat: Ebola in West Africa (2014-2016) and in the Democratic Republic of the Congo (2018-Present)
The Ebola virus outbreak in West Africa in 2014-2016 was an eyeopener and a wake-up call to the continuing critical deficiencies in the national, regional, and global mechanisms for detecting, reporting, and responding to an epidemic as envisioned under IHR (2005), and the potential global threat from infectious disease outbreaks. The best reconstruction of the West Africa outbreak tracks to the death of one young infant in the Forestière region of Guinea at the end of December 2013. The outbreak grew dramatically and spread over the following months, and the strain was identified in mid-March 2014 as Ebola Zaire. By the end of March 2014, the coordinator of the Médecins Sans Frontières project in Conakry, Guinea, cautioned, “We are facing an epidemic of a magnitude never before seen in terms of the distribution of cases in the country” (Samb, 2014).
Guinea, Liberia, and Sierra Leone were ill-equipped for such a disaster because chronic poverty and civil war had undermined local health systems, and there was therefore an insufficient number of doctors and nurses. On top of this, years of civil war and violence had left the populations wary of authority and government, and without trust in the urgently needed outside assistance, rumor and conspiracy theories abounded.
BTRP made significant contributions in the early stages of the outbreak. Dr. Carl Newman, chief scientist for BTRP, informed the committee that, beginning in March 2014, BTRP–through “strategic positioning and good old-fashioned serendipity”–supported laboratories running Ebola diagnostics in Sierra Leone and Liberia. BTRP had a preexisting project working at the Kenema Government Hospital in Kenema, Sierra Leone, focused on understanding the seasonal variability of Lassa fever to help improve surveillance. BTRP’s existing contract enabled it to rapidly pivot from the research project on Lassa fever to providing diagnostics for Ebola. The U.S. Ambassador to Liberia then asked BTRP to establish such diagnostic capacity in Liberia (Newman, 2018).
BTRP (then known as the Cooperative Biological Engagement Program [CBEP]) later described the work in its list of annual accomplishments:
CBEP supported the U.S. and international efforts to stem the ongoing Ebola Virus Disease (EVD) outbreak in West Africa and prepare at-risk countries for potential EVD cases. This outbreak underscored the unique and unpredictable nature of the biological threats that CBEP seeks to reduce by enhancing BS&S [biosafety and biosecurity] practices as well as BSV [biosurveillance] systems. Through provision of equipment, training, and transportable laboratory diagnostic capability, CBEP contributed substantively to the EVD outbreak global response…. [This] showcased CBEP’s nimbleness to support activities in the fight to control the EVD outbreak that devastated Guinea, Sierra Leone, and Liberia. In doing so, CBEP positioned itself as a cornerstone and major contributor to activities in the region carried out by the U.S. interagency and members of the international community handling this emerging threat. (U.S. DOD, 2015)
Within WHO, there was some pressure early-on from certain members of its Regional Office for Africa to downplay the problem for political, economic, and trade reasons. It was not until August 8, 2014, that WHO Director-General Margaret Chan declared the outbreak a Public Health Emergency of International Concern (PHEIC). By then, it was the largest Ebola outbreak ever recorded up to that time (WHO, 2014).
The UN, many governments, foundations, NGOs, and the private sector responded. Existing institutional aid relationships fostered provision of assistance from the United Kingdom to Sierra Leone, France to Guinea, and the United States to Liberia. President Barrack Obama directed that this be a national security priority, and on September 16, 2014, he announced that, at the request of the Liberian government, a military command center would be established in Liberia to support civilian efforts across the region (White House, 2014).
The UN Security Council held an emergency meeting and on September 18, 2014, determined that the “unprecedented extent” of the Ebola outbreak in West Africa constituted a threat to international peace and security. The Security Council emphasized that “the outbreak is undermining the stability of the most affected countries concerned and, unless contained, may lead to further instances of civil unrest, social tensions and a deterioration of the political and security climate” (UN, 2014).
The U.S. military responded rapidly, as described in a subsequent DOD study:
While the military dealt with force health protection in the past (e.g., 1918 Spanish flu pandemic), Operation UNITED ASSISTANCE was the first U.S. military operation to support a disease‐driven foreign humanitarian assistance mission. The international community’s lack of preparedness to respond to the scale and severity of the Ebola outbreak and delayed decision making allowed the disease to spread, complicating the subsequent Department of Defense and international response. The unique aspects of the mission, the evolving Department of Defense roles, the lack of understanding of the operational environment, and force projection shortfalls presented challenges in establishing an expeditionary base in an austere environment. (U.S. DOD, 2016)
By the time the PHEIC related to Ebola in West Africa was eventually lifted on March 29, 2016, a total of 28,616 confirmed, probable, and suspected cases were reported in Guinea, Liberia, and Sierra Leone, with 11,310 deaths (a case fatality rate of almost 40 percent) (WHO, 2016c).
Following the West Africa Ebola epidemic, several groups, including the National Academies Commission on a Global Health Risk Framework for the Future, undertook lessons-learned exercises and proposed actions to improve global health preparedness and response for future infectious disease threats. One of the lessons learned from the 2014-2016 outbreak was the confirmation that Ebola can suddenly emerge in a part of Africa in which it was not previously recognized to be a threat. The lack of prior experience with Ebola in West Africa had the effect of skewing diagnostic considerations to other well-described pathogens known to be present in the area, such as cholera and Lassa fever, contributing to the delay in making the correct diagnosis. The belief that the Ebola virus was not circulating in the region was, in fact, a myth, as there already was serosurveillance evidence, albeit limited, that chimpanzees and humans had previously been infected. It is not clear that human virulent Ebola Zaire was present in West Africa long before the outbreak in 2014-2015. These positives could be cross-reactive with other Filoviruses or non-
virulent Ebola viruses not yet characterized. If the data are not entirely convincing, there is some evidence that where there is smoke, there is fire.1
Early identification and counteraction are critically important to a successful response to emerging biological threats. In reality this means that some assets and capabilities need to already be in place for response because: (1) outbreaks can arise in unpredictable locations; (2) disease transmission can be fast; and (3) effective response often requires familiar and trusted relationships.
This work is security work, not just public health work, and this is what DOD does. Although what outbreak will happen at a given time is unpredictable, vulnerabilities to significant outbreaks are observable (See Box 3-4). BTRP was well positioned in West Africa before the 2014 Ebola virus pandemic, which was fortuitous but not accidental. To be effective in the future, biothreat reduction programs will have to anticipate needs and position themselves where those needs are likely to arise.
To their credit, the WHO Member States and Secretariat recognized that WHO leadership and performance during the West Africa Ebola outbreak were not at an optimal level. WHO instituted major institutional reforms, including creation of a Health Emergencies Program and establishment of the Contingency Fund for Emergencies (WHO, 2017d, 2020a). And the World Bank established the Pandemic Emergency Financing Facility to provide surge financing (PEF, 2019).
These new mechanisms came into play in August 2018 in eastern provinces of the Democratic Republic of the Congo (DRC), an area of
___________________
1 In the 1990s, there was an outbreak of Tai Forest Ebola Virus in an Ivory Coast chimpanzee population, and subsequent human infection in a veterinarian. Therefore, if this variant is present, it is certainly possible others – including the bat species of Ebola – are also there (Boisen et al., 2015; Formella and Gatherer, 2016; Keita et al., 2018; O'hearn et al., 2016; Schoepp et al., 2014; Formenty, Boesch, et al., 1999; Formenty, Hatz, et al., 1999).
active armed conflict, extreme poverty, poor healthcare accessibility, and major distrust for authority figures and the government by the population. Given the known presence of the virus elsewhere in DRC and previous outbreaks of Ebola in other nearby countries, such as Uganda, the fact that it had not been identified previously in this part of DRC was not a reassurance that it would not at some time be introduced. The challenges of controlling this continuing outbreak and limiting its spread in a conflict zone are enormous, with more than one million displaced persons, security concerns for health workers attempting to identify cases, immunize, and track and monitor close contacts in areas where cross-border movement of people is common. As of January 2020, more than one year since it first was detected, there were more than 3,400 confirmed and probable cases with a death toll above 2,100, which makes it by far the second-worst epidemic of the virus on record (WHO, 2020b).
Ebola outbreaks have ranged all the way from East Africa to West Africa, and the committee does not underestimate the difficulties in trying to predict where an Ebola outbreak could occur or, given limitations on resources, what could be done in advance to preposition bioengagement programs and surveillance capabilities (particularly in areas of conflict). Nevertheless, one needs to ask if all of this could have been better anticipated. It is difficult not to ask the “what if” questions: What if there had been investments to establish an effective disease surveillance system before the outbreak occurred? What if community engagement and support for improved healthcare systems had been initiated? BTRP was part of the response to Ebola in West Africa in 2014 and needs to be part of forward-looking discussions in the future so that it, too, will be better prepared for the next infectious disease event with national security implications. One means of participating in forward-looking discussions is through professional, scientific networks (See Box 3-5).
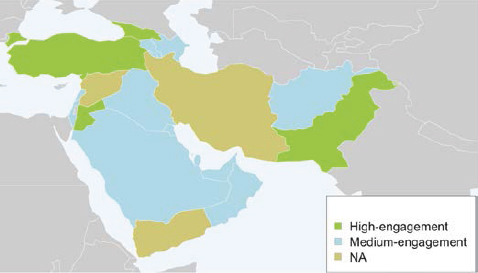
WAB-NET aims to promote bat disease surveillance through capacity building and collaboration, and, to enhance knowledge of the diversity and distribution of native bat species and their associated viral communities.
During the network’s meetings, the members are able to discuss research opportunities that are unique to the region, and outline potential hypotheses that could be tested through an active network of bat researchers studying bat-associated viral associations.
In this regard, the Middle Eastern researchers have opportunities for collaboration through WAB-NET that lead to the improvement of local and regional capacity for zoonotic disease investigations and early detection.
In a region that is politically unstable, WAB-NET could facilitate cross-border research cooperation and continually work to guard against threats posed by zoonotic disease outbreaks. Thus, the network could serve as an instrument for stability and security of the region through early detection of zoonotic disease threats.
An Example of a Successful DOD Joint Program on Filoviruses and Severe Sepsis: The Joint Mobile Emerging Disease Intervention Clinical Capability, Uganda (Ongoing)
The Makerere University Walter Reed Project (MUWRP) in Uganda was established in 2002, and is one of five international research sites established by DOD through a program centered at the Walter Reed Army Institute of Research. The intention was to establish the capacity to detect outbreaks originating in an unstable region of DRC that cross the border
to Uganda. This project includes an isolation ward, diagnostic laboratory, and clinical research capacity. MUWRP serves as the coordinating entity for the Joint Mobile Emerging Disease Intervention Clinical Capability (JMEDICC) program, as follows:
The Joint Mobile Emerging Disease Intervention Clinical Capability (JMEDICC) program is a collaboration between U.S. and Ugandan researchers. JMEDICC provides a platform for clinical trials in filoviruses during an outbreak setting. The JMEDICC program is establishing a pilot demonstration of the capabilities at Fort Portal Regional Referral Hospital, in Kabarole District. This platform includes establishing an Isolation [Unit], strengthening the hospital laboratories to provide services beyond traditional hospitals in Africa, training staff in advanced supportive care and scientific rigor, conducting clinical research on sepsis and establishing mobile capabilities to conduct clinical research during an outbreak anywhere in the country. This platform will allow for rapid response to test the new therapeutics or medical countermeasures during the next Filovirus outbreak. MUWRP is the coordinating entity in Uganda and works closely with the Infectious Diseases Institute. (MUWRP, 2019)
As a mechanism to provide training through actual research collaborations, JMEDICC initiated the Austere Environment Consortium for Enhanced Sepsis Outcomes (ACESO) study, through the Henry M. Jackson Foundation and the U.S. Naval Medical Research Center. It is aimed at identifying the causes of sepsis in this region of Uganda and improving “survival for patients with sepsis in resource-limited settings through early recognition, diagnosis, and evidence-based clinical management” (MHRP, 2020). Because ACESO was there, local staff were being trained to safely identify and care for patients with Ebola or other emerging infections, track and monitor contacts, and implement studies of natural history and new interventions. It was also available to address the potential arrival of Ebola-infected individuals from the outbreak in DRC. The investment in the JMEDICC program is an example of anticipation. Because it was there at a potentially vulnerable border crossing, Ugandans were prepared and able to react quickly and effectively when a family
incubating Ebola crossed the border from DRC in August 2019, and they effectively prevented further transmission within Uganda.
Examples of Proactive International Engagement: Active Participation in Key International Meetings Focused on Biological Threats
BTRP, the European Union, Canada, and the United Kingdom provided support for and participated in the Second Global Conference on Biological Threat Reduction organized by OIE in 2017. More than 300 participants from 70 countries attended the conference, including delegates from OIE member countries, donors, scientists, and stakeholders from the animal, human, public health, and law enforcement communities.
The conference focused on four topics: (1) developments in nonproliferation instruments and global health security efforts; (2) international discourse on technology applications; (3) systems for promoting collaboration to facilitate preparedness efforts; and (4) biological threat reduction in the future (OIE, 2017). The conference featured side events on “Espionage, epizootics, and economics: safeguarding global animal health”; “Enhancing preparedness through simulated exercises and capability building”; and “Building interagency collaboration at the national and regional levels for biological threat reduction through simulation (table-top) exercises” (OIE, 2017, p. 2). During the conference, OIE identified several overarching themes, including the need to promote collaboration, peaceful use of science and technology advances, international security and health security instruments, and sustainability and self-reliance, all of which are relevant to BTRP’s mission. In its final report, OIE listed several recommendations for addressing these themes and promoting One Health approaches to threat reduction (2017).
By contrast, BTRP senior leadership would have benefited from participation in the November 2018 GHSA Ministerial Meeting in Bali, Indonesia. More than 600 delegates from 49 countries attended, including a large delegation from the U.S. government led by the Deputy Secretary of Health and Human Services and including the Deputy Assistant Secretary of Defense for countering weapons of mass destruction. At the Ministerial Meeting and in several side meetings, GHSA Action Package 3 on Biosafety and Biosecurity was discussed at length. An event on GHSA-relevant Contributions of the Defense and Security Sectors in Support of Civilian Authorities featured speakers from the U.S. Pacific
Command and the African Partner Outbreak Response Alliance as well as the Indonesian surgeon general. A U.S. Deputy Assistant Secretary of Defense stated publically, “We encourage defense sectors to use GHSA’s frameworks to prevent, detect, and respond to threats.” The Bali Ministerial Meeting, and especially the side meetings, resulted in rich and productive discussions involving ministers and senior officials from around the world. They served to advance awareness and collaboration on global health security broadly and on biosafety and biosecurity specifically, while maintaining the important catalytic role of GHSA through the newly approved GHSA 2024 framework. Such engagement and participation of BTRP at these meetings is essential for the program to remain current and scientifically informed, as well as to establish networking connections with key leaders from around the world.
This page intentionally left blank.


























