5
Assessment and Implementation Strategies for Improving the Health of Rural Populations
The fourth session of the workshop focused on the assessment and implementation of strategies for improving the health of rural populations, including the community health needs assessment (CHNA) tool, the Minnesota Integrating Behavioral Health project, rural development hubs, and strategies to catalyze innovation in sustainability and financing of rural population health. The session was moderated by Allen Smart from PhilanthropywoRx.
COMMUNITY HEALTH NEEDS ASSESSMENT
Darrold Bertsch from Sakakawea Medical Center (SMC) and Coal Country Community Health Center (CCCHC) discussed how the CHNA tool can be used to support population health efforts. He described the CHNA process and how it has been applied to inform organizational planning and collaborative assessment activities. CHNA is a tool that health care entities use to define their service area, identify the specific needs in that area, and facilitate planning to meet the health care needs within that area. Through a systematic process that draws on community input and support, the CHNA tool can identify health needs and health systems issues through data and information gathering and analysis. Bertsch added that CHNAs are conducted to identify and prioritize health needs within a community, which can provide justification for the allocation of resources based on the needs that are identified during the assessment process.
CHNAs are routinely conducted by a variety of entities and organizations, said Bertsch. For example, critical access hospitals (CAHs) must conduct CHNAs every 3 years, as mandated by the Patient Protection and Affordable Care Act, in order to identify community needs and move toward addressing them. Public health entities are required to conduct CHNAs for accreditation purposes and, more importantly, to inform the development of community health improvement plans that enable public health units to address community-specific needs. The Health Resources and Services Administration (HRSA) requires community health centers to use CHNAs—both for grant applications and for subsequent reporting from grant applications—to identify community needs and how those needs are being met in the scope of services provided by that health center. Bertsch noted that CHNAs are sometimes conducted independently without necessarily linking together to identify needs and work collaboratively to address them. However, the communities and organizations that tend to be most successful in using CHNAs are those where the needs assessments are conducted collaboratively and followed by collaborative planning.
Community Health Needs Assessment Process
Bertsch provided an overview of the CHNA process (see Box 5-1).1 The process begins with reflecting and strategizing about the overarching goals to be accomplished through the needs assessment. The next step is to identify and engage with a variety of stakeholders who will be providing input and participating in the CHNA process (e.g., health care providers, local clergy, government agencies). Then, the community is defined based on the service area of the organization or multiple organizations participating in the assessment. Next, data are collected to identify needs using various types of strategies, including individual surveys, individual interviews, focus groups, or information available online, such as county health rankings. The data are then analyzed to prioritize community health issues through a series of meetings with smaller groups, followed by larger group meetings. The results of the entire scope of the assessment are then documented and communicated to stakeholders. This process yields a package of documents that serves as the guide for the remainder of the CHNA cycle; the success of the CHNA process is dependent on stakeholders making use of these documents. Next, the implementation phase begins. Using the results from the CHNA, stakeholders develop and begin to execute implementation strategies. The final
___________________
1 More information about the community health needs assessment process is available at https://www.healthycommunities.org/resources/community-health-assessment-toolkit (accessed September 8, 2020).
phase is ongoing monitoring and evaluating of progress toward the goals that have been identified through the CHNA process. Bertsch added that if health priorities change as strategies are being implemented, implementation strategies need to be adjusted accordingly to meet the community’s current health care needs.
Use of Community Health Needs Assessment Findings for Strategic Planning
Bertsch described how CHNA findings can be used for strategic planning and implementation. CHNA findings are used for strategic planning both for individual organizations and for collective planning within service areas. It tends to be more effective when health care entities in a community work collectively to develop strategic plans and then hold each other accountable to facilitate, implement, and monitor the initiatives developed during the strategic planning process. CHNA findings can also be used to collaborate with local public health units to develop and implement community health improvement plans. Through subsequent monitoring and regular meetings to review progress, local population health committees can use the CHNA findings to adjust strategic plans as needed. Bertsch emphasized that coordinated and collaborative assessment and planning are critical for ensuring that the CHNA process produces the greatest possible community benefit. He added that in some states, CHNA results are aggregated for use in statewide planning efforts. For instance, the Center for Rural Health in North Dakota aggregates CHNA data from individual providers to provide statewide data
on health needs. This allows stakeholders to compare their communities’ health needs and priorities with state averages and with the needs and priorities of other communities.
Application of Community Health Needs Assessment in North Dakota
Bertsch described the practical application of a collaborative CHNA and planning process that was conducted in North Dakota, and he explained how that process benefited SMC in Hazen, North Dakota, and CCCHC in Beulah, North Dakota. SMC and CCCHC are both 501(c)(3) not-for-profit corporations that serve a 4,000-square-mile rural service area in West Central North Dakota with a population of 15,000. Energy is the major industry in this service area. CCCHC was designated as a federally qualified health center in 2003; it comprises four service delivery sites and offers medical, behavioral health, and visiting nurse services. SMC is a 13-bed critical access hospital that offers hospital, hospice, palliative care, and basic care services.
The SMC and CCCHC collaborative CHNA and planning process began in 2011, said Bertsch. The process benefited from integrated leadership and governance for the two facilities, which ensured that both the health center and the hospital remain aligned in terms of vision and strategic initiatives. Multiple community partners were involved in the initial needs assessment. In addition to core partners including SMC, CCCHC, the public health unit, a skilled nursing facility, and emergency medical services providers, additional participants included state and local governments, businesses and industry representatives, school administrations, and other community representatives.
Bertsch outlined several benefits of the collaborative CHNA and planning process in North Dakota. The process benefited from both individual and collective efforts to identify community needs and move forward with developing and implementing the strategic planning process through a collaborative and coordinated community health improvement plan. The population health committee plays a valuable role in monitoring progress and adjusting the implementation plan based on changes in the service area’s health needs, which benefits from a collaborative process that aligns efforts across partner entities. Bertsch remarked that the CHNA process was instrumental in creating a “patient-centered medical neighborhood of care” among organizations involved in the process. This has improved financial performance, clinical outcomes, and quality metrics, and it has enhanced collaborative care, care coordination, and transitions of care. Care coordinators at each organization are able to work together across initiatives because the organizations are collectively involved in the needs
identification and planning processes. This collaborative process has also established a foundation for additional initiatives, Bertsch noted. For instance, SMC and CCCHC have jointly implemented a new electronic medical record system.
Partner organizations in the service area are also participating in value-based care for Medicare and commercial models. This has provided a framework for a patient–family advisory council that includes representatives from each entity in the service area, as well as a group of patients who have used hospital, clinic, long-term care, and emergency medical services. Such initiatives would not have been possible without the collaborative approach to the CHNA process from the outset, he noted, and such an approach will likely serve the community well in addressing future needs. Bertsch added that the framework for collaborative planning and collaboration established by the CHNA process has been helpful in addressing local needs and facilitating responsiveness during the coronavirus disease 2019 (COVID-19) pandemic.
MINNESOTA INTEGRATED BEHAVIORAL HEALTH PROGRAM TO SUPPORT POPULATION HEALTH
Rhonda Barcus from the National Rural Health Resource Center2 discussed the development of the Minnesota Integrated Behavioral Health (IBH) program to support population health. The Minnesota IBH program was funded by the Minnesota Department of Health’s Office of Rural Health and Primary Care as part of a Minnesota Flex Program grant focused on population health. The Department of Health analyzed 59 CHNA findings from Minnesota communities and found that one of the most frequently cited needs was for behavioral health. Specifically, these CHNAs demonstrated a statewide need to build community partnerships and integrate behavioral health and outreach. This was consistent with aggregated local public health department findings, which identified access to behavioral health services as the greatest need statewide. Thus, the Department of Health decided to systematically coordinate behavioral health with general care, said Barcus, because integrating mental health, substance abuse, and primary care services produces the best outcomes and has been shown to be the most effective approach to caring for people with multiple health care needs.
___________________
2 The National Rural Health Resource Center is a nonprofit organization dedicated to sustaining and improving health care in rural communities. As the nation’s leading technical assistance and knowledge center in rural health, the center focuses on five core areas: transition to value and population health, collaboration and partnership, performance improvement, health information technology, and workforce.
The program was developed in collaboration with the hospitals that would be participating in the program, which were focused on tightening and improving care coordination practices for people in the community with behavioral health issues. From the hospital’s perspective, the intention was to provide sufficiently high-quality supportive care to individuals with behavioral health issues that they are less likely to experience a crisis requiring them to seek care in a hospital’s emergency department (ED). Although many communities were already offering a range of behavioral health services, those services were often siloed with minimal collaboration among providers. Barcus added that the development of the IBH brought together a range of different organizations focused on behavioral health and mitigating the potentially negative effects of social determinants of health (SDOH)—including competing organizations, in some cases—to determine how to best serve the people in the community.
Minnesota Integrated Behavioral Health Program Tool Kit
One of the results of the collaborative IBH project was the development of the IBH tool kit.3 Barcus explained that the tool kit was designed both to provide detailed information for entities seeking to address behavioral health in their communities and to serve as a generic process for addressing other population health issues, such as diabetes or heart disease. The tool kit provides details about the IBH project process, including information about the readiness assessment, selection process, technical assistance, evaluation of project outcomes, and lessons learned. The IBH project worked with three cohorts of hospitals across the state—rolling out one cohort each year.
Technical Assistance to Hospital Cohorts
Barcus described the technical assistance provided to participating hospitals throughout the IBH process, which is detailed in the tool kit. For each cohort, a kickoff workshop brought together representatives of the participating hospitals. Next, each hospital in the cohort received an onsite visit to conduct community strategic planning. Quarterly peer calls allowed all of the hospitals in the cohort to share accomplishments, identify barriers and challenges, and brainstorm collaboratively about ways to address those issues. Hospitals also benefited from the provision
___________________
3 The IBH project ran from 2015 to 2019, with cohort 1 in 2015, cohort 2 in 2016, cohort 3 in 2017, and a stigma project in 2018. More information about the IBH tool kit is available at https://www.ruralcenter.org/rhi/mn-ibh (accessed July 21, 2020).
of technical assistance as needed, as well as from educational webinars and workshops focused on sustainability and support for data collection.
Evaluation of Project Outcomes
Barcus described how the IBH project evaluated outcomes. The project used an outcome evaluation process developed by the National Rural Health Resource Center called recommendation adoption progress (RAP) reports. This process seeks to “tell the whole story” by including measurable outcomes as well as other concerns. As part of this process, the hospitals conduct regular interviews with project leaders throughout implementation and demonstrate ways in which the project has become embedded in their hospital culture. The IBH project teams conducted interviews with hospital teams to gain a holistic picture of how projects were being implemented and embedded in the hospital’s culture. To help keep teams focused and motivated, RAP interviews are held quarterly. This holistic picture can be used to inform future projects in other hospitals, noted Barcus. Additionally, this evaluation process can be used to help maintain hospitals’ momentum and promote accountability in realizing progress. For instance, if a hospital has not made the planned progress between quarterly evaluation calls, then the call can be used to help the hospital establish steps to achieve their goals.
Barcus explained that hospitals participating in the IBH project were also asked to develop their own measures—based on the specific populations that each hospital serves—in four general categories: (1) hospital-specific use of services measure, (2) hospital-specific cost-of-services measure, (3) hospital-specific health outcomes measure, and (4) hospital-specific individual measure. For example, a hospital-specific use of services measure might be specified as a measure of how many people with a certain type of behavioral health diagnosis are reporting to the hospital’s ED each quarter. That hospital might then choose a cost-of-services measure that tracks the cost of services for each individual with that diagnosis who reported to the ED that quarter. These hospital-specific measures are discussed during quarterly evaluation calls. Barcus presented a practical example from one of the participating hospitals, which created a roving therapist position after finding that inmates in the local jail with depression and anxiety were presenting at the ED for treatment during crisis. The roving therapist began visiting the jail to counsel inmates with depression and anxiety to help prevent them from reaching a crisis point by providing them with longer-term supportive care. Over the subsequent year, the number of patients brought to the ED from the jail decreased and there were no inpatient psychiatric transfers among inmates in the jail who were seen by the roving therapist.
Integrating Behavioral Health: Measurable Outcomes and Promising Practices
Barcus outlined measurable outcomes used by hospitals that participated in the Minnesota IBH project to assess whether behavioral health was successfully integrated:4
- Increased access to behavioral health services,
- Increased discharge to home,5
- Decreased transfers to inpatient settings,
- Decreased cost of transferring ED patients as well as cost of ED visits,
- Decreased ED visits and admissions,
- Decreased mental health holds,
- Decreased Patient Health Questionnaire (PHQ-9) scores at 6-month follow-up, and
- Decreased jail psychiatric transfers.
Barcus also described examples of promising practices that participating hospitals identified as driving meaningful changes within hospitals. One of the most effective practices identified was stakeholder collaboration, which is the practice of identifying and engaging with stakeholders in the planning of projects. Resource directories were effective in allowing providers and consumers to identify available opportunities to access services. She noted that hospitals often began the IBH process presuming that more behavioral health resources were needed. However, establishing a resource directory can demonstrate that there are actually sufficient resources in place that consumers and providers are unaware of due to siloing and lack of collaboration. To help simplify the release process, some participating hospitals created a universal release of information that includes a list of potential agencies that will support a client’s care release.6 The use of community navigators can provide support and help ensure that clients are following their treatment plans and/or taking their medications. Another promising practice was the use of mobile crisis teams that report directly to clients’ homes to assess and deescalate situations. For hospitals that rely on the police to transport patients to an
___________________
4 More information about the Minnesota IBH project is available at https://www.ruralcenter.org/rhi/mn-ibh (accessed July 21, 2020).
5 This outcome measures how often patients can be sent home instead of being discharged. Hospitals consider it a success when patients can be sent home instead of being discharged to inpatient care; these cases are referred to as “discharge to home.”
6 A sample universal release of information form can be found at https://www.ruralcenter.org/sites/default/files/Luverne%20Consent%20ROI.pdf (accessed July 21, 2020).
inpatient medical facility—often at great cost to the community—decommissioned police vehicles that have been purchased or donated can be used in lieu of an ambulance.
Barcus noted that implementing the Make It OK campaign is a promising practice for fighting stigma.7 Across all three hospital cohorts in the IBH project, stigma around mental illness, behavioral health, and substance abuse was identified as one of the biggest barriers to good community care coordination. The Make It OK campaign has been used within and beyond hospitals to promote awareness and destigmatize mental illness and substance abuse.8 In addition to using this campaign, other strategies for mitigating stigma include the formation of a committee of community partners to address stigma, engaging local institutions, and offering education and training on stigma reduction. Community collaboration is a key aspect of successful approaches to stigma reduction used by participating hospitals, Barcus added. In addition to strategies such as partnering with schools, churches, and businesses, some hospitals collaborated with music, art, and theater communities to create productions that would bring people together to help address the stigma of mental illness and substance abuse.
ROLE OF RURAL DEVELOPMENT HUBS AND POLICY IN CONNECTING RURAL DEVELOPMENT, HEALTH, AND OPPORTUNITY
Katharine Ferguson from The Aspen Institute Community Strategies Group discussed the role of rural development hubs and rural policy in connecting development, health, and opportunity in rural communities. She also suggested strategies to modernize federal rural policy and develop a stronger rural development ecosystem.
Influence of Community and Economic Development Efforts on Health
Ferguson highlighted the need to consider factors beyond clinical settings and health behaviors in advancing health, equity, and opportunity—this, in essence, is the thesis of population health. She noted that the underlying framework on which county-level health rankings and road
___________________
7 See https://www.youtube.com/watch?v=KCL5YgNJTdw&feature=youtu.be (accessed September 21, 2021) and https://www.youtube.com/watch?v=2EiIwksKqQo&feature=youtu.be (accessed April 9, 2021).
8 More information about the Make It OK campaign is available at https://makeitok.org (accessed July 21, 2020).
maps are based indicates that about 50 percent of health outcomes are related to social and economic factors (around 40 percent) and physical environment (about 10 percent),9 and she emphasized the need to consider what it takes to create a healthy place where people feel they belong and can thrive, in addition to the more common focus on healthy people and individual opportunity.10 Social and economic factors that span people and place include education, employment, income, family and social support, and community safety. Factors in the physical environment that are decidedly place focused include air and water quality as well as housing and transit.
Ferguson said that the concept of SDOH has been crucial in creating a structure and vocabulary for thinking beyond health care to health, well-being, and opportunity, but that the social determinants framework must continue to evolve to better reflect the full range of actors who are essential to creating an equitable, healthy, thriving, and sustainable place. Taking a broader lens means that actors, factors, and activities essential to health include community and economic development professionals, civic participation, tax and fiscal policy, structural racism, community building, place making and community planning decisions and the built environment, employers and workforce, and entrepreneurship and small business development in addition to the more commonly known actors and factors such as community health workers, schools and educators, day care providers, social service providers, safety and security providers, food assistance providers, and housing accessibility and affordability. In short, when a place—rather than a people—lens is applied to health, a wide range of systemic and structural factors ranging from racial justice to community planning and tax policy become essential to health.
Awareness is growing beyond public health and academic circles that place—where people live—is an important component of health and equity in the United States, with a critical intersection between race, class, and place. Some areas may have excellent schools, employers, transportation service, mental health services, and recreational opportunities, while others have subpar services or lack of services. Disparities have always existed, she noted, and the COVID-19 pandemic is making them more evident. The University of Michigan’s Poverty Solutions Lab has developed a Multidimensional Index of Deep Disadvantage that measures
___________________
9 More information about the County Health Rankings and Road Maps model is available at https://www.countyhealthrankings.org/explore-health-rankings/measures-data-sources/county-health-rankings-model?componentType=health-factor&componentId=25 (accessed July 22, 2020).
10 Within this framework, about 30 percent of health outcomes are related to health behaviors (e.g., tobacco use, diet and exercise, alcohol and drug use, sexual activity) and 20 percent are related to clinical care, including access to care and quality of care.
five health status factors to assess what it is like to live in a particular place in the United States.11 This index demonstrates that place matters and that great disparities exist across the country. For example, poverty is endemic and opportunity is limited in the Black Belt, in Appalachia, and in the colonias on the southwest U.S. border,12 an area that is largely Indian country. Ferguson said that these areas should be evaluated with a broad lens in order to determine how structures and systems make it difficult to create healthy places and for individuals to realize opportunities in these regions:
The cultural, historical, economic, and geographic context of place is essential and often points to regions where overcoming barriers to opportunity requires taking a much broader lens and think through how [to] look at the structures and the systems that are making it hard to realize opportunity.
Ferguson highlighted a set of rural and regional intermediary organizations that tend to be less visible as important developmental actors in communities and rural regions. These include community development financial institutions and credit unions created specifically to serve underserved regions, as well as community foundations, community colleges, community action agencies, regionally focused nonprofit organizations, value-chain coordinators, statewide rural organizations, social enterprise collaboratives and cooperatives, and regional councils of governments, among others. Ferguson noted that these organizations may not have an obvious place in the SDOH framework, but they are critical partners for making progress in population health by addressing root causes and effecting systemic change. A subset of those rural and regional intermediary organizations could be considered rural development hubs, she suggested.
Rural Development Hubs
Ferguson’s organization, The Aspen Institute Community Strategies Group, has defined a rural development hub as “a place-rooted organization working hand in glove with people and organizations within
___________________
11 More information about communities of deep disadvantage is available at https://poverty.umich.edu/projects/understanding-communities-of-deep-disadvantage (accessed July 22, 2020).
12 The Texas Office of the Secretary of State defined the colonias as residential areas along the Texas–Mexico border that may lack basic living necessities like potable water, septic or sewer systems, electricity, paved roads, or safe and sanitary housing. More information about the colonias is available at https://mhpsalud.org/inside-texas-border-communities-colonias (accessed July 22, 2020).
and across a region to build inclusive wealth, increase local capacity, and create opportunities for better livelihoods, health, and well-being” in the report Rural Development Hubs: Strengthening America’s Rural Innovation Infrastructure (The Aspen Institute Community Strategies Group, 2019). In developing the report, the group conducted interviews with leaders in 43 rural development hubs across the country that were representative in terms of geography, types of organization, and populations. The leaders were asked how they thought about their work, what challenges they face, and what would help them improve their work. Ferguson noted that a wide range of organizations can be considered rural development hubs, as already outlined. Although their work is critical for rural development, these intermediary organizations are not always easy to identify as potential partners in the current models used by public health organizations because they often work behind the scenes as partners to direct-service organizations and local organizations that public health is more likely to recognize.13
Outcome-Oriented, Wealth-Building Framework for Development
Rural development hubs may be radically different in terms of function and location, Ferguson said. However, a commonality among these organizations is their commitment to an asset-based approach to community and economic development rather than an overreliance on older approaches to economic development that often emphasize business recruitment and resource extraction. Instead, many rural development hubs are aligned with a wealth-building framework for development that is oriented around three outcomes:14 (1) to grow multiple forms of capital, (2) to root ownership in the region, and (3) to improve livelihoods for those living on the margins. Specifically, these organizations tend to have a shared understanding of the need to recognize, invest in, and grow many kinds of capital—including individual, intellectual, social, natural, political, cultural, and financial capital—that are needed to create vibrant thriving communities and sustain economies. These organizations have a common interest in creating locally rooted wealth (not merely jobs), so that people in their regions will profit and experience better economic and health outcomes. Ferguson noted that locally rooted ownership creates more pathways for local-level ownership, control, and influence over economic drivers and for access to the wealth generated by those drivers. To improve the livelihoods of marginalized populations, these types of
___________________
13 The Aspen Institute Community Strategies Group’s report on rural development hubs includes tools that can be used to identify rural development hubs.
14 For more information, see https://www.wealthworks.org (accessed October 28, 2020).
organizations aim to strengthen and improve livelihoods by providing high-quality, living-wage work and careers for all residents. They also focus on equity and inclusivity, aiming to improve the holistic livelihood of communities, added Ferguson.
Expanded Rural Hub Development Toolbox
Ferguson compared the toolbox for economic development, as traditionally construed, with the expanded toolbox that is common among rural development hubs. Traditional economic development tools include marketing a place or region, resource extraction (often timber, coal, or oil), and business recruitment through tax credits or investment-ready development (e.g., industrial parks). All of these tools may be used by rural development hubs, but their expanded toolbox also includes additional tools. These include systems thinking using a regional lens, a broader understanding of capital, community engagement with a focus on equity, and an emphasis on local ownership. More broadly, the expanded toolbox conceptualizes success in a way that focuses on health, resilience, high-quality jobs, and building and retaining local wealth.
Role of Rural Development Hubs in Addressing Social Determinants of Health
Ferguson emphasized that rural and regional intermediaries, such as rural development hubs, are essential partners in addressing structural barriers to progress and mitigating the negative consequences of SDOH in rural regions. They consider the whole system and engage a wide array of nontraditional partners among different sectors of the community to achieve positive outcomes in a way that is compatible with the population health. The unique lens and language of rural and regional intermediaries such as rural development hubs makes them an invaluable asset to those working on SDOH and population health. She quoted Patrick Woodie of the North Carolina Rural Center:
Our aim is to create a place at the table for all parts of the community, especially those parts that may look different or have not always been included in the conversation. Inclusion cannot happen on its own. It must be an intentional part of any economic or community development strategy.
Developing a Stronger Rural Development Ecosystem
Ferguson emphasized that strategies are needed to encourage the development of more and stronger rural development hubs and engage
them more broadly in development work. She described 10 routes to a stronger rural development ecosystem, which are organized into three forms of action: shifting mindsets, constructing or revising systems and policies, and building capacity (The Aspen Institute Community Strategies Group, 2019).
Shifting mindsets would benefit from (1) an understanding that addressing equity in the United States requires investments in rural America, (2) an increase in U.S. rural cultural competency, (3) trust in the know-how of rural development hubs, and (4) a reimagining of what impact means in rural contexts.
To construct or revise systems and policies, it would be useful to (5) detect and eradicate government systems and structures that disadvantage rural America, and (6) design policies and programs with rural implementation in mind.
To build capacity, it would be helpful to (7) support analysis and action at the regional level, (8) boost peer learning for hub staff and board leaders, (9) create pipelines and marketplaces that connect investors to America’s rural development, and (10) structure investments and initiatives to strengthen and sustain system-changing organizations. In addition to these 10 routes for building a stronger rural development ecosystem, Ferguson called for the creation of a consensus vision and framework for rural community and economic development.
Strategies to Modernize Federal Rural Policy and Connect Health with Development
Ferguson explained that rural economies were hit hardest by the 2008 recession and have been the slowest to recover. In 2017, average rural employment was still 2 percent lower than it was in 2007.15 Businesses were hit especially hard by the recession; in the first 4 years of recovery, counties with populations under 100,000 lost 17,500 businesses, while economies in counties with populations of 1 million or more gained 99,000 jobs (Ferguson et al., 2020). Existing racial, health, and economic disparities are being exacerbated by the COVID-19 pandemic, and it is critical that these health and economic issues be addressed concurrently. She suggested that events surrounding the COVID-19 pandemic support the claim that health and economic outcomes are integral and need to be addressed simultaneously.
A major challenge in supporting the economic development of rural
___________________
15 More information about rural employment is available at https://www.ers.usda.gov/topics/rural-economy-population/employment-education/rural-employment-andunemployment (accessed July 22, 2020).
communities is that federal rural policy is largely outdated, said Ferguson. While the pressures and opportunities faced by rural economies have radically changed, the existing federal architecture for rural policy is old—largely dating to the 1860s, 1930s, and 1960s—and designed for a different time (Ferguson et al., 2020). She suggested that population health advocates and other health advocates should join in advocating for the modernization of federal rural policy toward a rural policy framework that helps to achieve both economic and health goals. Ferguson presented five principles for reimagining federal policy in the COVID-19 era:
- Support local ownership and strategies.
- Invest in people and institutions.
- Increase flexibility and align federal and state funds to meet local needs.
- Measure and reward outcomes.
- Embrace a regional mindset. (Ferguson et al., 2020)
She suggested that efforts to modernize federal rural policy would benefit from bringing strategy and coherence, expanding financing for domestic development, and elevating the capacity for building and evaluation.
Ferguson concluded by outlining several strategies for connecting health and development. The first was to adopt asset-based and wealth-building approaches, rather than focusing on deficits. The second was to align health and development strategies, including the required comprehensive economic development strategies and CHNAs. The third was to build partnerships and shared frameworks and vocabulary among rural development hub leaders and population health leaders. The fourth was to build momentum for investing in local people, civic institutions, capacity building, and evaluation. Finally, she suggested joining forces to rewrite the rural narratives to reflect the full diversity and potential of rural people and places.
INNOVATIONS IN SUSTAINING RURAL POPULATION HEALTH
Karen Minyard from the Georgia Health Policy Center discussed insights from the COVID-19 pandemic and explored how to promote financial innovations for sustaining population health. She described a sustainability framework developed by the Georgia Health Policy Center and discussed the mindset required to see the flow of funds in a system and develop financial innovations. Minyard remarked that rural communities are neither monolithic nor completely distinct from one another.
Many subgroups of rural areas share historical, cultural, economic, and geographical commonalities, but they still differ in various ways along the key domains of health care systems, population, environment, infrastructure, and community health status. Infrastructure includes the economy, Internet access, and policy. The health care system includes accessibility, insurance, and the health care workforce. The environment includes climate, housing, exposure, and safety. Population includes culture, demographics, history, and mindsets, she added.
Rural Health Concerns Related to the COVID-19 Pandemic
Minyard explained that at the beginning of the COVID-19 pandemic, the Georgia Health Policy Center asked 200 rural grantees to share concerns regarding rural health. They raised the following key concerns:
- The need for community health workers who could provide social support in the virtual world
- The question of how to deliver effective virtual trainings and conduct effective virtual meetings
- The question of how to handle peer-support services and recovery support related to the opioid epidemic in the pandemic environment
- The need to use telehealth in new ways to meet emerging needs
- The need to adjust approaches to data collection and evaluation during the pandemic
- The need to work with schools to develop strategies to support the community
Minyard described the COVID-19 pandemic as a technological trial by fire, particularly for rural areas. Major challenges that are endemic in rural areas include inconsistent Internet access, lack of cellular service, lack of technology for virtual visits, and discomfort using technology. However, innovation has already emerged from these challenges in rural areas. These include using new telehealth platforms that can function even on low bandwidth Internet connections, the potential integration of COVID-19 measures into electronic health record systems, new strategies to address the health needs in correctional facilities, and the use of school buses to deliver meals. Many of the grantees appreciated having flexibility regarding their HRSA responsibilities in their grants from the Federal Office of Rural Health Policy, because many providers’ states had begun to cut their funding. The grantees suggested that going forward, it will be important for them to remain up to date on changing policies,
information, and regulations as well as maintaining and expanding telehealth capabilities and developing creative strategies for outreach and connections with clients that incorporate the new measures that were implemented during the pandemic.
Innovations in Sustainability and Financing
Minyard described the framework developed by the Georgia Health Policy Center, which emphasizes the importance of positioning for sustainability. The framework holds that sustainability cannot be established in the short term, leading up to a grant application process. Rather, sustainability is a complex process that must be maintained through strategic vision, collaboration, leadership, relevance and practicality, evaluation and return on investment, communication, efficiency and effectiveness, and capacity. She pointed out that the work described by Bertsch and Barcus included many of these components—including relevance, practicality, evaluation, collaboration, and strategic vision—which will likely contribute to the sustainability of their efforts.
Blueprint for Action to Improve Community Health Through Innovations in Financing
Financing is a critical consideration for sustaining rural population health, said Minyard. Funding sources must be identified within health systems, and implementers must develop innovative strategies to achieve their aims using available funds. In this sense, she added, innovation occurs when the flow of funds is influenced to drive improvements in targeted communities. Such innovations typically involve the application, combination, and creation of financing tools and methods. The Georgia Health Policy Center developed a blueprint for action, which shows how to improve community health through innovative financing (see Figure 5-1).
The blueprint underlines the importance of stewardship and strategy as elements that inform the financing process and how they can be used to answer questions related to funding. Financial instruments can only be implemented after ascertaining how much money is needed initially and annually, the expected returns on investment, and how funds will be administered. She added that finding overlooked sources of funding, such as local governments or banks, requires a broad view of how money flows through public health systems. Focusing only on particular financial instruments is not a substitute for a broad understanding of a system’s finances, she noted. Instead, the funding process must be connected to the broader process of innovation. Community collaboratives require an
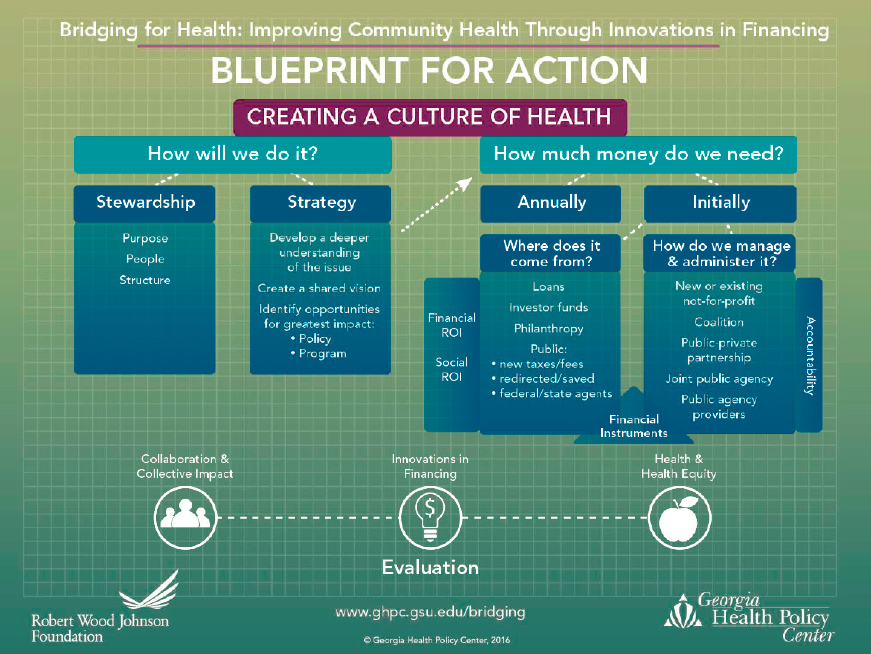
NOTE: ROI = return on investment.
SOURCES: Minyard presentation, June 25, 2020; www.ghpc.gsu.edu (accessed October 28, 2020).
evolutionary, not revolutionary, approach to financing population health, she added.
Minyard described a cycle of innovation that supported the development of the blueprint for action. The cycle begins with defining and agreeing on the terms and aims of a process, followed by a process of ideation and prototyping that can be used to develop innovations. These prototypes must then be tested and implemented with empathy and an appropriate mindset. The next step is to define and agree on terms for further iterations of the cycle. She shared that seven community collaboratives used this approach to develop a model of local wellness funds, which are vehicles for consolidating all locally available money. For communities to make progress in developing such pooled community wellness funds, questions about sources, uses, and structure need to be answered: (1) Where does the money come from? (2) What will the funds be used for? and (3) How will the funds be managed, administered, and stewarded? She added that maintaining a focus on the financing innovation—not program implementation—is critical but often challenging.
Spurring Innovations in Financing
Minyard remarked that a broader understanding of how money flows through systems requires both an appropriate mindset and open-mindedness. She said these are necessary to see beyond the obvious systemic and financial factors to identify the entire flow of funds. However, all levels of funding are to be seen together to develop innovative financing. She described those with a skill for seeing the flow of funds across a system as “money whisperers,” and she asserted that anyone could learn this skill with practice. Money whisperers might see money at the macro (system) level or micro (program) level. She offered two examples of this kind of insight. In one case, a rural banker realized that they could use their bank’s money to establish a loan and grant system to accomplish the community’s population health goals. In another community, a source of funding was identified within the local government. It had been earmarked to return to the general fund, but because they identified it they were able to divert it to a specific population health project.
Minyard closed by describing several steps to help cultivate the right mindset for innovations in financing. When focusing on population health, thinking should move upstream to look for approaches with the greatest leverage to improve health and well-being. Steps should be taken that also examine the flow of funds, taking care to look in the unlikely places where funds may be flowing. She also suggested building a culture of stewardship and shared collaboration among diverse stakeholder
groups. To explore financing vehicles, it is helpful to bear in mind that innovations in funding may include a combination of multiple vehicles to meet the needs of the local context. She suggested looking for intersections of health, money, and partners and encouraging collective investments in health and well-being. These steps should be repeated cyclically to ensure that the innovation cycle continues, Minyard added.
DISCUSSION
Equity in Rural Health
Smart opened the discussion by noting that there are 13 million people of color living in rural America, along with more than 2 million immigrants living in booming immigrant communities across the country. Many of those individuals are not well integrated into the traditional work of nonprofit organizations, institutions, and governments. He asked the panel how to ensure that all individuals in rural communities are incorporated in the works of rural health organizations.
Ferguson replied that a first step is to recognize and acknowledge the existence of racial inequities and other inequities of all kinds. Another step is to expand the understanding of leadership in the context of community-based strategies by bearing in mind that leaders come in all forms. For instance, a mother who is well connected to her community and knows more about the cultural needs and norms of her community might have better community leadership skills than a business executive or elected official. Ferguson added that various approaches can be used to engage the community, such as participatory democracy, to help ensure that decisions made duly reflect a community and its vision. For instance, organizers may choose to provide child care at meetings and choose not to hold meetings at times when only those paid to attend will be able to attend. Ferguson also noted the need to move away from expectations that people should fit within the dominant cultural context and to move toward more openness to different types of norms by adopting a more humble attitude, maintaining an open mind, and asking more questions to learn from the valuable experiences of others.
Barcus added that hospitals also need to maintain a community-centered perspective by meeting people where they are and potentially receiving uncomfortable feedback. She shared an example from a hospital that was conducting a CHNA. The hospital was dedicated to addressing breast cancer in their community, yet data from the community revealed a great burden of prostate cancer among African American men. The hospital’s administrators consulted with a local pastor of an African American
church, who told them that they should come to the church to encourage men to take action on prostate health, rather than expect those men to attend a seminar on prostate health at the hospital. Minyard commented that not everyone within rural communities holds the same views regarding race and racism, so it is important to be sensitive and responsive to differing viewpoints on complex situations.
Engaging Stakeholders, Changing the Narrative, and Securing Financing
Smart asked the panel to share more insights about garnering financial support for population health efforts, given that population health work is both expensive and lacking a standard funding mechanism. Bertsch suggested engaging with community-based extension offices, for example, and noted that some resources are more accessible through collaboration among providers to seek out different types of available funding. Collaboration can minimize individual responsibility among providers and reduce the financial resources that need to be expended. Ferguson pointed out that the costs of population health are not as expensive as the costs of caring for people who are sick. She suggested shifting the narrative to change policy and make financing available for population health, because most existing funding streams are designated for services rather than health care. Like other infrastructure improvements, financing should be channeled to the upfront costs of ensuring that the necessary population health coordination, strategies, and capacities are put in place to reduce costs in the long term.
Ferguson maintained that federal policy should be aligned with the aims of population health and recognize that population health spending is a long-term investment. Currently, sufficient funding is not available to rural communities to enable them to carry out the needed long-term investments in population health. Piecemeal funding may be available to these communities through various streams, amounting to as much as approximately $100 million, but that does not compare to the approximately $23 to $28 billion spent each year on economic infrastructure investment. She suggested that there is such limited investment in population health because of a misalignment of cultural values and the nature of budgetary systems. Sufficient emphasis has not been placed on the critical role of population health, and budgets are created with a short-term perspective that gives short shrift to the value of long-term investments. Thus, it is necessary to take control of the narrative around health spending and to emphasize the value of prevention in order to bring about real policy changes.
Ferguson suggested leveraging any and all available strategic and funding opportunities in order to make progress toward those immediate aims. Bertsch pointed out the complexities related to the incentives created by value-based approaches to health care. A focus on prevention can disincentivize the provision of services, but, going forward, value can be realized by the wise use of existing resources. Additionally, insurance providers, Medicare, and Medicaid offer payment for the provision of preventive services, said Bertsch.
Making the Case for Philanthropic Spending in Rural Population Health
Smart asked why philanthropists ought to invest in rural population health. Ferguson replied that the current model of rural health care is not workable. Indicators of health status and health outcomes are worsening, and rural hospitals are closing, so rural health warrants a radical systemwide transformation. This need creates an opportunity for philanthropic organizations to be impactful; impact is often a key criterion for philanthropic organizations seeking opportunities to invest. The rural health space is open to creative, risk-taking, and innovative approaches to realizing transformations. Ferguson remarked that philanthropists can help “blaze a trail” toward new models of population health, which governments and others may subsequently follow, because philanthropists are uniquely suited to take on the risk of investing in population health while also helping to drive change at the local level.
Panel Reflections
Smart invited the panel to give their final reflections on the session. Bertsch remarked on the importance of convening a diversity of expertise to address the challenges of population health. Diversity is a key aspect of community collaboration—including racial diversity and diversity in the provision of services—thus bringing more stakeholders to the table improves outcomes for all. Barcus emphasized the value of collaboration and engaging all stakeholders, such as art communities, theater and music communities, businesses, churches, and any other community groups that are concerned about health. Ferguson highlighted the need to bridge community economic development and health and the need to develop intellectual frameworks and language that enable individuals working on the ground to recognize that they are partners and allies in this work. Those working in health care, water infrastructure, and business development are all working to create more and better opportunities for better health outcomes for rural communities.
Ferguson suggested that by collaborating across geographies and industries, stakeholders can articulate a vision for the future of rural communities. Minyard underscored the importance of seeing how money flows through systems, leveraging the skills of “money whisperers” to serve as leaders in their communities or regions, and organizing funding streams in a way that supports population health. In closing, Smart remarked that the best rural philanthropic work often incorporates ideas raised by the panelists, including multidisciplinary community partnering. He suggested that rural settings should be considered as places first, rather than as the locus of a particular set of issues.
This page intentionally left blank.
























