1
Assuring America’s Health
The Committee on Assuring the Health of the Public in the 21st Century was charged with the task of proposing an inclusive framework for action to assure the health of the public in the twenty-first century. To guide this process, the Committee embraced the vision set forth by Healthy People 2010 (DHHS, 2000)—healthy people in healthy communities—with its recognition of both individual and community dimensions. Healthy People 2010 calls for a national effort to improve overall population health and, where possible, to eliminate disparities in health in the United States. This vision has been endorsed as national policy at the highest levels of government and by most states, many localities, and a large coalition of business and nonprofit organizations. What is needed now is action at a broad societal level to achieve this vision. This report provides a framework for action, identifies those who must be involved, and outlines priority steps to be taken. In this chapter, the committee outlines our approach and the rationale for it. We
-
Review the nation’s health achievement in the past century, which is tempered by concerns about falling short in the present and being ill equipped to meet future challenges;
-
Explore the nature of health as a public good, the fundamental and statutory duty of government to assure the health of the public, and the need and rationale for multisectoral engagement in partnership with government;
-
Examine the reasons for the nation’s deficient health status;
-
Describe the system and actors who can work together to assure the nation’s health;
-
Propose action steps to help attain the vision; and
-
Discuss national and global trends that may affect America’s health in the coming decades.
ACHIEVEMENT AND DISAPPOINTMENT
The health of the American people at the beginning of the twenty-first century would astonish those living in 1900. By every measure, we are healthier, live longer, and enjoy lives that are less likely to be marked by injuries, ill health, or premature death. In the past century, infant mortality declined and life expectancy increased (DHHS, 2002). Vaccines and antibiotics made once life-threatening ailments preventable or less serious; and homes, workplaces, roads, and automobiles became safer. In addition to the many health achievements facilitated by public health1 efforts such as sanitation and immunization, unparalleled medical advances and national investment in health care also have contributed to improvements in health outcomes. Roughly 13 percent of our gross domestic product—about $1.3 trillion in 2000, which represents a higher percentage than that of any other major industrialized nation—goes toward health-related expenditures (DHHS, 2001; Levit et al., 2002).
Despite the nation’s wealth, expenditures for health care and research, and scientific and technical accomplishments, the United States is not fully meeting its potential in the area of population health (Kindig, 1997). For years, the life expectancies of both men and women in the United States have lagged behind those of their counterparts in most other industrialized nations (Starfield, 1998; Jee and Or, 1999). Life expectancy in the United States was slightly below the Organisation for Economic Cooperation and Development (OECD) median in 1999 (Reinhardt et al., 2002), and in 1998, the average life expectancy at birth for women was 79.5 years in the United States (73.9 for men), compared with 81.9 (76.9 for men) in Sweden and 84.0 (77.2 for men) in Japan (Anderson and Hussey, 2001). In 1998, the United States also ranked 28th in infant mortality among 39 industrialized nations (DHHS, 2002). In the area of chronic disease, reported inci
dence rates in 1990 for all cancers2 in males and females were highest in the United States among a group of 30 industrialized nations (Jee and Or, 1999). Some birth defects that appear to have links to environmental factors are increasing (Pew Environmental Health Commission, 1999). The prevalence of obesity and chronic diseases like diabetes are increasing, and infectious disease constitutes a growing concern because of newly recognized or newly imported agents like West Nile virus, the emergence of drug-resistant pathogens, and the all-too-real threat of bioterrorism (DHHS, 2002).
Moreover, a focus on national averages often masks serious and persistent disparities in health status between racial and ethnic groups, men and women, and populations with lower and higher levels of income and education. For example, in 1999, the infant mortality rate for blacks was 14.6, a level 2.5 times higher than that for whites (Hoyert et al., 2001). Life expectancy is consistently higher for women than for men, with a difference of 5.5 years in 1999 (Hoyert et al., 2001). Additionally, people with less than 12 years of education are twice as likely to die from chronic disease than those with more than 12 years of education (DHHS, 2000).
Although data on the relationship between investments in health and health outcomes are not fully adequate at this time (Anderson and Hussey, 2001), several trends are worth noting because they may help explain why the nation seems to fall short of its potential. The vast majority of health spending, as much as 95 percent by some estimates (McGinnis et al., 2002), is directed toward medical care and biomedical research. However, there is strong evidence that behavior and environment are responsible for more than 70 percent of avoidable mortality (McGinnis and Foege, 1993), and health care is just one of several determinants of health (McGinnis et al., 2002). It then follows that the nation’s heavy investment in the personal health care system3 is a limited future strategy for promoting health. Social and environmental factors create unnecessary health risks for individuals and entire communities. Frequently, those who are most likely to be at social and economic disadvantage live in communities that are at higher risk of environmental contamination, face greater exposure to intentional and unintentional injuries, and are least likely to have access to good medical care. Moreover, although the benefits of our current investments permit American medicine to prevent, treat, and cure diseases, these benefits are
inaccessible to many because of a lack of insurance or access to services; about 14.6 percent of the population, or 41 million people, lacked health insurance in 2001 (Mills, 2002).
HEALTH AS A SOCIAL AND POLITICAL UNDERTAKING
It is hardly necessary to argue that good health is fundamental to a good society (Beauchamp, 1988). Without a certain level of health, people may not be able to fully participate in many of the goods of life, including family and community life, gainful employment, and participation in the political process. Ethicists point to the special role that health plays in the enjoyment of an active life, a thriving community, and a productive nation (Daniels, 1985). This view is also grounded in international codes and agreements to which the United States is party, from the World Health Organization’s Constitution (WHO, 1946) to the United Nations’ Universal Declaration of Human Rights, which ascribe intrinsic value to health.
Theories of democracy demonstrate that the public’s health is an important collective good because public funds are expended to benefit all or most of the population (Walzer, 1983). The public’s health can be supported only through collective action, not through individual endeavor. Acting alone, persons of means may procure personal medical services and many of the necessities of living. Yet no single individual or group can assure the conditions needed for health. Meaningful protection and assurance of the population’s health require communal effort. The community as a whole has a stake in environmental protection, hygiene and sanitation, clean air, uncontaminated food and water, safe blood and pharmaceutical products, and the control of infectious diseases. These collective goods, and many more, are essential conditions for health, but these “public” goods can be secured only through organized action on behalf of the population (Gostin, 2000).
There are solid legal, theoretical, and practical grounds for government in its various forms to assume primary responsibility for the public’s health (Duffy, 1990; Novak, 1996). Although governmental actions and agencies constitute the backbone of all efforts to assure the health of the public, government cannot assure population health alone; other sectors and parties have an interest and a civic role to help create the conditions that make health possible.
The actors selected by the committee to illustrate their potential individual power to promote health and the role they can play in an intersectoral public health system include the community, the health care delivery system, business, the media, and academic institutions. Some may question why the private sectors of society should act to produce “public” goods, such as the population’s health. To be sure, these groups do not have a
constitutional or statutory obligation to promote health, yet the private sector is affected by governmental actions. Government regulates private and nonprofit actors to ensure that they perform in ways that promote health (e.g., occupational health and safety rules, licenses, inspections, and nuisance abatements). Government provides economic incentives for engaging in health-promoting behavior (e.g., tax inducements to employers who provide health care benefits) and disincentives for engaging in risk behavior (e.g., taxes on cigarettes). Furthermore, the interest in and civic role for private- and nonprofit sector participation in health activities has been growing. For example, employers have recognized the benefits of making health and safety high priorities (WBGH, 2000). When businesses and voluntary organizations support the creation and maintenance of environments that are healthy and safe, they reap additional benefits from having healthy employees and satisfied consumers or clients and being good neighbors in communities (see Chapter 6).
This view of population health as an important social and political undertaking is justified by the importance of the natural (e.g., clean air and water), built (e.g., safe and livable cities), economic (e.g., reduced socioeconomic and racial disparities), and informational (e.g., accurate and accessible health information) environments in society (Gostin, 2002). “Healthy” public policy is an outcome of democratic and budgetary processes, and these political decisions should be informed by evidence, such as data showing the powerful influence of social and economic factors on the health of the population and the need to work with many partners to transform these factors. The collaboration of multiple actors in a public health system, broadly conceived, offers the best prospect for protecting and promoting the nation’s health for the future.
ISSUES THAT MAY SHAPE THE NATION’S HEALTH STATUS
Societal Norms and Influences
Faced with a mixture of satisfaction and concern about the status of population health in the United States, the committee sought possible answers. Although many factors may contribute to the nation’s less than stellar health, the committee believes some answers may be found in an examination of broad historical and cultural factors that have shaped health policy, planning and funding, and public perceptions and priorities about health.
Because health is the result of many interacting factors (see Chapter 2), it stands in the balance between economic, political, and social priorities and is caught in the middle of necessary and important tensions between rights and responsibilities—individual freedoms and community or social
needs, regulation, and free enterprise (Brandt and Gardner, 2000). These tensions pose complicated questions. How can the public’s health be maintained in the face of infectious disease threats without compromising individual privacy and confidentiality? Or how can a vibrant, prosperous economy be supported without sacrificing health to pollutants or to occupational hazards? How can society balance the individual desire to pursue the pleasures of life (e.g., food) with scientific evidence about health risk? Alternately, how are increased employment, better housing, health benefits, and an improved standard of living in a community achievable in the absence of economic development? In addition to securing the economic, environmental, and social elements that promote good health, how can more equitable access to them be ensured?
Moreover, health is part individual good served by medicine and part public good secured by public health activities. Instead of complementary and collaborating systems, the two disciplines, their institutional cultures, their agencies and organizations, and the public’s opinion of them have often been deeply divergent; and the individual focus of one and population focus of the other have become further reinforced and polarized. Often it has been harder to motivate and accomplish the long-term changes needed in the broad environments that influence health status because of the potential of immediate “silver bullet” solutions that can address poor personal health once it occurs. These attitudes and social influences may in part explain three interrelated characteristics of health-related investment, policy, and practice in this country:
-
the disproportionate preeminence given to the individual over the population health approach;
-
the greater emphasis on biomedical over prevention research and on medical care over preventive services; and
-
neglect of the evidence (and of the need for more empirical research) about the multiple factors that shape individual and population health, from the political to the environmental and from the social to the behavioral.
The personal health and health care agenda has dominated the nation’s health concerns and policy for quite some time. In fact, the majority of funding in the health care delivery system is public and there is a major public investment in biomedical research, yet the United States has failed to make the same level of commitment to population-based health promotion and disease prevention as it has to clinical care and research and biomedical technologies (Starfield, 2000). Medicine has thrived within the American economic system, and its remarkable advances in improving individual health have garnered understandable support from the public and from
policy makers (Lasker and the Committee on Medicine and Public Health, 1997). The public health approaches undertaken by governmental agencies in fulfillment of their statutory obligation and with some support from partners consistently have been underfunded and their importance in keeping populations healthy have been overlooked. With the decline of infectious disease in the twentieth century, public perception of the usefulness and necessity of governmental public health services diminished. However, with the resurgence of infectious diseases and the escalation of chronic diseases, as well as the newfound awareness of the multiple determinants of population health and the potential impact of macro-level and even global threats to health, the necessity of population-oriented approaches has become clearer. It has also been recognized that the infrastructure and capacity for such approaches must be permanent and sustained by resources equitably distributed between the governmental public health agencies and their partners and the biomedical and personal health care system.
Health (or the lack thereof) is associated with a complex, and not entirely understood, interplay among innate individual factors (e.g., a person’s sex, age, and genes), personal behavior, and a vast array of powerful environmental conditions4; investment and measures taken to address health needs do not give sufficient consideration to this issue. Because health is influenced by these complex interactions and because many threats to health (e.g., drug-resistant microbes or environmental contaminants) confront entire populations, protecting and assuring the population’s health requires an organized communal effort.
Health care services and biomedical technologies can generally address only the immediate causes of disease—for example, controlling high blood pressure to prevent heart attacks—and do so on an individual basis. The fact that excellent health care exists in this country means little to millions who lack access to it or to those who are more likely to experience poor health because of their race, ethnicity, or socioeconomic status (IOM, 2002). Preventive approaches that focus on populations are based on the evidence, presented in this report and elsewhere, on the multiple factors that influence health (DHHS, 2000; IOM, 2001; McGinnis et al., 2002). These factors or determinants of health affect entire populations, and their impacts may occur long before the onset of disease or disability. Preventive approaches to address them may include policies that support education, adequate housing, a living wage, and clean air or that attempt to deal with
some of the pervasive social and economic inequities that appear to be associated with profound disparities in health status, access, and outcomes.
Furthermore, the nation has experienced deepening income disparities over the past three decades; the incomes of the poorest fifth of the population have remained static in absolute terms (Weinberg, 1996; Deaton, 2002). Because many citizens face the possibility of experiencing social and economic deprivation at some point in their lives and these problems are associated with poorer health, society stands to benefit from the enactment of social and economic policies that are founded on the principles of reducing inequity (Mechanic, 2002). A national- or community-level commitment to enact socially equitable policies is more likely to result in more equitable opportunities over a lifetime for personal and societal advancement and will ultimately lead to improved population health.
The preceding discussion underscores the necessity of complementary and collaborative health care and population health orientations (Brandt and Gardner, 2000). Investing in population-based health promotion and disease prevention, in concert with the attention already given to personal health care, can be expected to positively affect the general health status and health outcomes of the American people (McGinnis et al., 2002).
Systemic Issues
In addition to issues related to social norms and influences, there are a number of systemic problems that may provide additional explanations for the shortcomings of America’s health attainment. In 1988, the Institute of Medicine (IOM) found that the governmental component of the nation’s public health system was in disarray. The committee is seriously concerned that despite subsequent efforts for improvement, governmental public health agencies, the backbone of any public health system, still suffer from grave underfunding, political neglect, and continued exclusion from the very forums in which their expertise and leadership are most needed to assure an effective public health system (see Chapter 3). This calls for urgent action. The governmental public health infrastructure is built on a legal foundation replete with obsolete and inconsistent laws and regulations, and a great deal of public health law is not coordinated among states and territories. This state of affairs sometimes complicates rather than facilitates governmental contributions to the public health system. A similar fragmentation and lack of coordination is evident in the fact that responsibility for health issues is dispersed across several departments in the federal government and across federal, state, and local governments, with potentially dire consequences for the public’s health. Although significant funding for the governmental public health infrastructure recently has been made available specifically to address the threat of bioterrorism, there is reason to be
concerned about how it will be allocated, whether it is adequate to address the needs of the infrastructure, and whether it will be sustained in the long term, as funding decisions are often not based on evidence but, rather, on ideology or considerations of political expediency (Kinney, 2002). Additionally, the public health workforce is inadequate in terms of preparation for practice (CDC/ATSDR, 2001) as well as number, partly because of local budgetary restrictions (NACCHO, 2001).
Governmental public health agencies are plagued by deficiencies in the very tools and resources that are essential to assuring population health. Until recently, many agencies had limited or no access to the Internet and electronic mail (Fraser, 1999; Brewin, 2001) and had fragmented information systems that lacked optimal connectivity and technology. This has led to public health surveillance systems that provide little or no population-based data on chronic disease or health problems that may signal exposure to environmental toxins. Moreover, many state public health laboratories are unable to keep pace with the needs for the monitoring and tracking of known infectious agents and became overwhelmed in the wake of new health threats such as the anthrax attacks and the appearance of the West Nile virus. Governmental public health agencies constitute the backbone of the public health system and bear primary, legally mandated responsibility for assuring the delivery of essential public health services. Therefore, the role of government in assuring the nation’s health is one that must be continued and sustained. Threats to the health of the population may evolve over time; but the facilities, information networks, workforce, and policies that form the infrastructure that protects the public’s health must be supported by evidence and adequate resources. The resurgence of tuberculosis (TB) in the late 1980s offers a cautionary tale about what can happen when the public health infrastructure is not sustained (IOM, 2000). The success of TB prevention and treatment programs led to decreased funding and even dismantling of TB control as a routine public health activity. In the late 1980s, a resurgence of TB was beginning as a result of antimicrobial resistance, untreated immigrants, and the HIV/AIDS epidemic. The weakening of TB surveillance activities led to a massive spike in the prevalence of the disease and a renewed threat to the health of the public.
Efforts to assure the health of the public also face important challenges in the increasingly fragile health care sector, related, among other factors, to the high number of uninsured and underinsured people. The Medicare program, which provides health insurance for most adults aged 65 and older, provides little coverage for preventive services. People with mental health or substance abuse problems often remain untreated. Racial and ethnic minorities do not receive the same quality of care afforded to white Americans, even when socioeconomic differences and other factors affecting access to health care are considered (IOM, 2002). Furthermore, the
resources within the health care delivery system are too poorly distributed to be able to address the complex health care demands of an aging population, absorb normal spikes in demand for urgent care, or manage a large-scale emergency such as that posed by a terrorist attack.
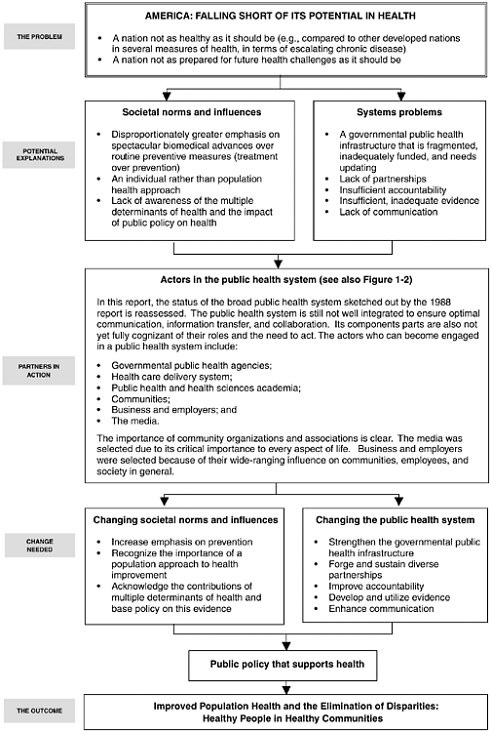
In Figure 1–1, the committee has outlined the logic framework for this report: from the problem statement and explanation, to the parties who are called to address the problem, and finally, to the strategies that should be employed to improve the current health status of the U.S. population and respond to the challenges and seize the opportunities that the future is expected to bring.
THE PUBLIC HEALTH SYSTEM AND ITS KEY ACTORS
In 1988, IOM, in its landmark report The Future of Public Health, defined public health as “what we as a society do collectively to assure the conditions in which people can be healthy” (IOM, 1988:1), a definition that this committee supports and reiterates in this report. The organizational mechanism for achieving the best population health—the public health system—was defined as encompassing “activities undertaken within the formal structure of government and the associated efforts of private and voluntary organizations and individuals” (IOM, 1988:42). While acknowledging the multiple participants in such an effort, the 1988 report focused specifically on ways to strengthen the performance of federal, state, and local governmental public health agencies—the governmental entities whose primary mission is to promote and protect the health of the public.
In the present report, the committee uses the term “public health system” in a manner that builds on the 1988 usage but that reflects present realities, including evidence about the determinants of health. The concept of a public health system describes a complex network of individuals and organizations that have the potential to play critical roles in creating the conditions for health. They can act for health individually, but when they work together toward a health goal, they act as a system—a public health system (see Figure 1–2). Furthermore, we must assure that our health and social policies facilitate their involvement in actions for health.
Actors in the Public Health System
The governmental public health infrastructure (e.g., local and state health departments and laboratories), the health care delivery system, and the public health and health sciences segments of academia are most heavily engaged in and identified with health-related activities and are obvious actors in a public health system. There are other, less obvious actors who can shape population health by influencing and even generating the multiple
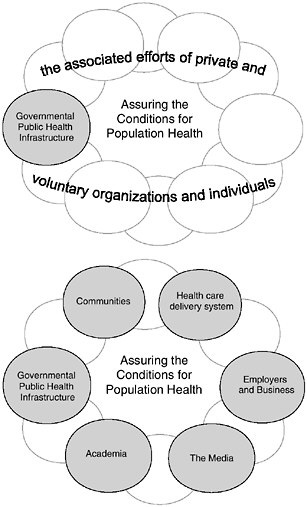
FIGURE 1–2 The intersectoral public health system. The 1988 IOM report described the public health system as the activities undertaken within the formal structure of government and the associated efforts of private and voluntary organizations and individuals” (IOM, 1988:42). The report’s primary focus was the governmental public health infrastructure. In the present report, the public–private nature of the public health system is further elucidated. Although the report examines the governmental public health infrastructure, some of its potential partners in an intersectoral public health system are also described. The committee has selected five actors who, together with the government public health agencies, are in a position to act powerfully for health. For the purpose of brevity, some sectors or potential partners have been subsumed under the category of community (e.g., schools, law enforcement). The shaded ovals represent actors who can work individually or together as part of a public health system to create the conditions necessary to assure the best possible health for the nation. The unshaded ovals signify other sectors and entities the committee did not single out for extensive discussion.
determinants of health (e.g., economic change, political will, knowledge, social connectedness, information, and language and cultural barriers).
A corporation may see itself solely as a manufacturer, for example, yet employers and businesses influence population health in many ways: through the provision of incomes to individuals and their influences on local economies, workplace conditions and health-related activities, the provision and type of employee health care benefits, environmental effects (industrial contaminants and other impacts), and the role they play in communities and neighborhoods. A television station may see itself as a source of news and entertainment, but the media may influence population health by shaping the relationships between individuals and the health care sector by conveying consumer information through broadcasts and online and between communities and governmental public health agencies by relaying breaking news and risk communication. The media also shapes public opinion, knowledge, and even behavior in the way in which it uses language and images and also through entertainment and advertising. Communities—schools, voluntary organizations, civic groups, local law enforcement and fire-fighting agencies, religious organizations, and others—play multiple roles in shaping health status, in terms of promoting a social connectedness that may support health instrumentally or psychologically, implementing organizational efforts and activism to attain policy change, and managing or engaging in population-level health interventions. By bringing communities, the media, and businesses and employers to the table, they can build the knowledge and capacity needed to channel some of their resources toward population health improvement. This benefits everyone. Businesses and employers will have healthier workforces and constructive relationships with the community, the media will better serve the public interest, and communities will be active participants and even leaders in their own health improvement process.
As these examples demonstrate, it is not just health departments that play a role in carrying out the 10 essential public health services (see Box 1–1). Other sectors of society can contribute by transforming their impacts on the public’s health so that they are no longer the result of random and unintentional actions but are the result of informed, strategic, and deliberate efforts to positively affect health.
Roles of Public Health System Actors in Carrying Out Essential Public Health Services
Achieving the vision and reaching the goals set forth by Healthy People 2010 will require the concerted and collaborative efforts of different components of society, whether it is the public sector, the private sector, state agencies, nongovernmental entities, learning institutions, or the community at large.
|
BOX 1–1 The Essential Public Health Services
SOURCE: Public Health Functions Steering Committee (1994). |
To attain the vision of healthy people in healthy communities, we must assure that all communities, no matter how small, have access to the essential public health services. All partners who can contribute to action as a public health system should be encouraged to assess their roles and responsibilities, consider changes, and devise ways to better collaborate with other partners. They can transform the way they “do business” to better act to achieve a healthy population on their own and position themselves to be part of an effective partnership in assuring the health of the population. Health policy should create incentives to make these partnerships easier.
Clearly, the health care delivery system already plays an important role in providing several of the Essential Public Health Services (ESs). For example, health care providers can contribute to public health surveillance and assessment of community health status (ESs 1 and 2), and they can employ their resources in health promotion and education activities (ES 3). The many entities that operate within communities can collaborate with other partners to monitor health and investigate health-related needs (ESs 1 and 2) and can play a dynamic role in education, empowerment, and mobilization for health improvement (ESs 3 and 4). Communities can also become involved in policy development (ES 5), either directly or indirectly through organizational efforts and advocacy. Academia informs, educates, and empowers people about health issues (ES 3) through partnerships with
communities that provide practical and service-oriented learning opportunities for students. Academia also assures workforce competence by providing high-quality education and training (ES 8), in addition to its substantial roles in evaluation and research (ESs 9 and 10). America’s businesses and employers have the opportunity to promote health and prevent disease and disability in their own workforces (ES 3). Employers are also a critical source of health care payment for personal health care services (ES 7). Furthermore, because businesses are closely involved with communities, they can collaborate in partnerships that monitor, identify, and address community health problems (ESs 1 and 4). Finally, the mass media can educate, inform, and thus empower (ES 3) communities with accurate and timely health communications.
PRESENT AND FUTURE CHANGES NEEDED FOR A HEALTHY NATION
The committee’s findings call attention to the fact that achieving the vision of healthy people in healthy communities is a difficult and complex task that cannot be accomplished through a single plan of action or by a single governmental agency or nongovernmental entity. Rather, broad societal action is required at every level; and such action needs to be better coordinated by all individuals, families and community members, businesses and workers, and health care providers and policy makers. Furthermore, responding to this vision requires a long-term public and political commitment to ensure that the policies, financial and organizational resources, and political and public wills are in place to assure the presence of the conditions necessary for all Americans to live longer, healthier lives. To support the creation of an effective intersectoral public health system, the committee identified six areas of action and change. These are reflected in the recommendations made to the potential public health system actors described in this report, but they are equally applicable to other components of the public health system not specifically addressed. Action and change are needed to:
-
Adopt a population health approach that builds on evidence of the multiple determinants of health;
-
Strengthen the governmental public health infrastructure—the backbone of any public health system;
-
Create a new generation of partnerships to build consensus on health priorities and support community and individual health actions;
-
Develop appropriate systems of accountability at all levels to ensure that population health goals are met;
-
Assure that action is based on evidence; and
-
Acknowledge communication as the key to forging partnerships, assuring accountability, and utilizing evidence for decision making and action.
The unique responsibility of government to assure action for health has been discussed and will be discussed further. The essence of the intersectoral public health system described in this report is partnerships linking those who contribute their expertise, resources, and perspectives to the process of assuring population health. Government agencies are subject to more formal systems of accountability through the political process, yet the success of specific activities for health depends on the setting of standards for program and workforce performance and in meeting the needs of the populations served. Emphasizing evidence as the basis for policies and programs acknowledges that information and data should form the basis for effective planning and decision making at all levels and among all partners within the public health system. There is strong and growing evidence that “healthy” public policy must include consideration of domains that are not traditionally associated with health but whose influences have health consequences (e.g., the education, business, housing, and transportation domains). Finally, improving communications is an essential component in the activities of all potential public health system actors. Improving communications capacity will involve, among other things, investment of resources, efficient adoption of cutting-edge technologies, training of workers, and even change in institutional cultures.
The vision of healthy people in healthy communities can be achieved only if the governmental backbone of the public health system is strong; intersectoral partnerships create environments and conditions conducive to the best population health; accountability is valued and practiced by all stakeholders; evidence is effectively developed, shared, and translated into practice; and effective communication becomes a priority among all public health partners. In the next section, we describe a number of contextual changes and trends that will influence the kinds of health problems we will face as a society and the strategies we select to address them.
BROAD TRENDS INFLUENCING THE NATION’S HEALTH
This report examines some reasons for the nation’s current health status and proposes measures and actors that will help improve and continually assure the nation’s health in the future. As noted, there is a need to transform social norms and strengthen the potential for more effective partnerships within a public health system to ensure that they will promote and protect population health. A number of factors create both opportuni
ties and threats as we work to reach this goal. These include (1) population growth and demographic change (a population growing larger, older, and more racially and ethnically diverse, with a higher incidence of chronic disease); (2) unprecedented technological and scientific advances that create new channels for information and communication, as well as novel ways of preventing and treating disease; and (3) the geopolitical and economic challenge of globalization, including international terrorism (Brownson and Kreuter, 1997; Levy, 1998; Koplan and Fleming, 2000; McKinlay and Marceau, 2000). Some of these factors offer unprecedented opportunities for global and national health improvement, whereas others pose threats that make it more difficult to achieve the best conditions necessary for the nation’s health.
Population Growth and Demographic Change
The U.S. population will become much grayer in the twenty-first century, and strengthening community and individual capacities and resources to support good health at all ages will be essential. As the Baby Boom generation ages into retirement, the proportion of the U.S. population over age 65 is projected to reach 13.3 percent by 2010 and 18.5 percent by 2025 (Bureau of the Census, 1996; Campbell, 1997). In 21 states, the elderly population is expected to at least double between 1995 and 2025 (Campbell, 1997). The nation has also seen a doubling of the number of centenarians, from 30,000 to 60,000, over the past several years (Portnoi, 1999).
The graying of America doubtlessly will be accompanied by some changes in the population’s needs for health care, long-term care, and other services. This trend especially underscores the importance of services and social supports to promote healthy aging. Although care needs for the elderly have declined somewhat in recent years, there are concerns about society’s ability to respond effectively to the needs of this demographic group (Wolf, 2001). An aging population will require effective means of chronic disease prevention and management to help older people maintain the best possible levels of health and function. Although some health problems may be inevitable because of biologic and genetic factors, research is pointing to new opportunities for promoting health at older ages (Fried, 2000). For example, community-based interventions to support behavioral changes such as increases in physical activity and good nutrition may partially reverse some health damage and may help prevent the occurrence of additional problems (Andrews, 2001). Furthermore, earlier investments in health promotion and disease prevention could produce benefits at younger ages, before irreparable damage has occurred and before the chances for healthful, functional aging are reduced (Khaw, 1997; Andrews, 2001). Also, public policy could expand the social, economic, and lifestyle options avail-
able to aging populations (Jacobzone, 2000). Aging healthfully promises not only psychosocial benefits and the ability to remain functional and independent for as long as possible but may also result in medical cost savings (Reed et al., 1998).
The increasing number of elderly Americans will also draw increased attention to the need (shared by many others, including children and city dwellers) for adequate housing, safe and appropriate urban design, and for easily accessible transportation systems that allow for the continuation of both subsistence activities like grocery shopping and social interactions like participation in senior citizens’ groups (NRC, 2001). Moreover, it has already given rise to a well-defined political constituency (e.g., through organizations like the American Association of Retired Persons [AARP]) and can be expected to influence the medical and population-level health research agendas (NRC, 2001).
The United States is also becoming more racially and ethnically diverse through both immigration and natural growth (Day, 1996). The proportion of the population accounted for by Hispanics, African Americans, Asian Americans and Pacific Islanders, and Native Americans is expected to rise from 28 percent in 2000 to 32 percent by 2010 (IFTF, 2000). Although diversity enriches American culture and strengthens America’s democracy, it also challenges the systems that traditionally have provided for the health and welfare of American society. For example, minority groups are underrepresented among the population of health care professionals, and many health care workers are not sufficiently skilled in the delivery of culturally competent care. Additionally, the health system itself (as the broader sociocultural environment in which it is embedded) is characterized by complex undercurrents of pervasive inequities and institutional racism, which lead to stereotypes, biases, and uncertainties that result in unequal treatment of racial and ethnic minority patients (IOM, 2002). New immigrant groups also bring their own perceptions about the role of government, the meaning of community, and the definition of health and illness; and these must be considered in creating better ways to achieve a healthy nation.
Continuing disparities in health status and the outcomes of health care demonstrate the need for a greater effort to ensure equitable access to and services from the health care delivery system for people of different backgrounds (IOM, 2002). With an increasingly diverse population, the nation will need a more highly developed knowledge base concerning the social determinants of health and a continuing reassessment and improved understanding of the ways in which social, cultural, and ecological factors shape health behaviors and influence health status (IFTF, 2000).
Technological and Scientific Advances
In this age of technology, the acquisition of new scientific knowledge and capabilities is occurring at unprecedented speed. However, the new knowledge and capabilities in fields like biotechnology also carry ethical, social, and economic ramifications, and raise concerns about the risks of new technologies (Khoury et al., 2000). Some advances, like highly sophisticated medical instruments and better pharmaceuticals, seem most pertinent to the personal health care delivery system, but others are highly relevant for the protection of population health. Developments in genetics, for example, have shed new light on disease causation, thus providing new opportunities for intervention for disease prevention and health promotion (Khoury et al., 2000; Omenn, 2000).
Genomics is expected to transform the practice of medicine from disease screening and diagnostics to treatment. In fact, some health care may come to involve the detection of disease at the gene level, permitting preventive treatment before the disease even begins to unfold (PricewaterhouseCoopers, 1999). However, the promise of genetics is constrained by an incomplete understanding of interactions among genes and between genes and the environment (Austin et al., 2000). This not only poses research challenges but also raises other contentious issues concerning the causes of ill health, personal rights and responsibilities, and the possibility of achieving health equity. For example, can individual choices and behaviors be leveraged against genetic heritage and broader ecological factors in a way that is fair? Additionally, new genetic technologies may compromise efforts to improve overall population health if they lead to the stigmatization and exclusion of certain groups. Furthermore, genetic testing raises a complexity of issues regarding matters such as privacy, cost, employment, and insurability. Ultimately, the benefits of genetic research must be weighed against, and perhaps considered in conjunction with, interventions on behavioral and population-level factors in disease causation (Willett, 2002).
The technological advances in the medical and biological sciences are only rivaled by the recent decade’s rapid developments in information and communication technology. The increase in personal computer use and access to the ever-expanding offerings of the Internet present both opportunities and challenges to the goal of improving the health of the population. The Internet is a ready and popular medium for exchanging health information and news and for facilitating political and group mobilization to influence policy. Although the wider availability of health information may empower and inform consumers, erroneous or misleading information may also pose a danger to health.
The partners in the public health system must ensure that emerging communication and information technologies are used effectively to pro-
mote the concepts and messages of public health. Public health partners must also become engaged in countering or critiquing media and social messages, products, and patterns that are potentially detrimental to health. Such a responsibility implies that health departments, health care delivery systems, and perhaps others engaged in population-oriented health efforts will be expected to construct and maintain a presence on the World Wide Web and use cyber methodologies to educate and inform consumers and communities. The public health system must gain greater skills to meet the challenge of using the mass media to promote health and to keep pace with the communication revolution. In this Information Age, high-quality web sites, e-newsletters, and Internet Q-and-A columns may become the primary means of delivering health messages, replacing the familiar brochures and posters.
U.S. technological expertise creates an important international dimension. The United States is a magnet for foreign graduate students in science, technology, and health, American specialists are a cornerstone of the international health community, and the nation is a world leader in high-technology exports. The National Research Council report The Pervasive Role of Science, Technology, and Health in Foreign Policy considers science, technology, and health developments as “such a pervasive force, they cannot be isolated from the fundamental concept of foreign policy” (NRC, 1999:2). The report calls on the leadership of the State Department to take a series of steps to increase the department’s capability to identify and act on science, technology, and health opportunities in countries of strategic importance and to coordinate these efforts within the department and with other cabinet agencies.
Globalization and Health
The increasing diversity of the average American community is an illustration of what has been occurring on the global scale as people with various backgrounds, nationalities, and ethnicities are migrating or working in places far from their native lands and diverse languages and cultures mix and mingle in cities, towns, and suburbs. Globalization is reflected in both positive and negative developments that include increased trade, travel, migration and demographic changes, food security issues, environmental degradation and unsustainable consumption patterns, the evolution and dissemination of technology and communications, and an increasingly global media (Navarro, 1998; Yach and Bettcher, 1998).
Globalization is a strong influence on population-level health both locally and internationally, and its ultimate impact will depend on society’s response (Beaglehole and Bonita, 1998; McMichael and Beaglehole, 2000). Global health issues include, for example, health risks arising from certain
infectious diseases, ozone depletion, and lifestyle changes, all of which transcend national borders. There are other factors that are (to various degrees) regulated at national borders, such as food and pharmaceutical quality and safety and the ability of health professionals to practice in countries other than those in which they were trained (Lee, 2001). In addition, socioeconomic determinants of health, such as income and employment status, are often influenced by the global economy. The liberalization of trade may benefit health status and outcomes by facilitating the diffusion of biomedical technologies and international food and agricultural safety standards (Bettcher et al., 2000). However, greater openness to trade may also have negative implications if the global economy engages in practices detrimental to health; examples include the export of tobacco products in developing world markets and the production and dumping of environmental toxins such as methylmercury (Keigher and Lowery, 1998; Sen and Bonita, 2000).
Information and communication technologies, especially those that use the Internet, are increasing at such a scope and rate that they are critical influences on populations through their transmission of knowledge. Their effects on health can range from making the most esoteric specialists available for consultation virtually anywhere in the world, to providing up-to-date scientific literature to isolated researchers and clinicians, to providing information directly to the public about health and illness. Barriers to realizing the health benefits of a global information society were identified in an expert survey reported for project G8-ENABLE, sponsored by the European Institute for Health and Medical Sciences in Surrey, United Kingdom. These barriers include the security of personal information, data standardization, intellectual property and reports, and network and messaging technologies, as well as education, culture, and cost (Rogers and Reardon, 1999). Aside from concerns about exacerbation of the knowledge gap between developed and developing countries, communication, especially popular culture reflected in the entertainment media, can create images and expose a population to behaviors that may introduce unhealthy practices (e.g., in diet and risk behavior) into cultures previously free of them.
With the increasing cross-border flows of people, pharmaceuticals, and food, countries cannot adequately protect their populations through unilateral domestic or foreign policy action; they must collaborate with other countries and within the frameworks of international agreements. The World Health Organization is a forum for setting standards and developing protocols on issues like international travel health standards, tobacco control (the Framework Convention on Tobacco Control), the quality of pharmaceuticals, and food quality and safety. Several issues may benefit from high levels of involvement from countries like the United States, with its
wealth and scientific expertise. These issues include a lack of funding for research on diseases and injuries that disproportionately affect the developing world (i.e., the “10/90 gap” [Davey, 2000]), the weakness in the research infrastructure in many developing countries, and the need to address issues of intellectual property involved in making basic drugs available to nations without their own production capacity.
Some have rightly urged that health should be included in America’s core foreign policy agenda (Kassalow, 2001) and that our nation must become engaged in matters of global health law (Fidler, 2002). In some instances like bioterrorism and infectious diseases it is a matter of national security, and in others it is a matter of national self-interest and positive identity (IOM, 1997). National-level assessments and policies regarding the health of the population must consider global factors, porous borders, and increasingly mobile people and germs. Historically overshadowed by trade and military issues, the health of the public has in recent years gained preeminence as an issue of national security. This turn of events has been precipitated by the global devastation wrought by HIV/AIDS, the emergence and reemergence of infectious disease, concerns about states that develop and accumulate biological weapons, and fear of bioterrorism (Fidler, 2002). Concern about global health issues led to an unprecedented session of the United Nations Security Council in 1999—the first ever on a health issue—on the global threat of HIV/AIDS. A public–private Global Fund to fight HIV/AIDS, malaria, and TB was established to provide resources to tackle these threats effectively; however, funding commitments to date have fallen far short of the goal. In fact, the current average overseas development aid funds are about 0.2 percent of the gross national product of industrialized countries, well below the 0.7 percent goal agreed upon internationally. U.S. spending is below the average (Kaul and Faust, 2001).
As world economies have become interconnected and interdependent, global health can no longer remain the domain of a few specialists because its repercussions are significant for our economy, our place in the world, and the cultural and human heritage that the populations of the world share. Microbes can weaken national security, impair economies, and destabilize societies. Surveillance efforts, public health research, the training of the workforce, the scope of laboratory activities, and local public health activities should all reflect the global community of which the United States is a part and the global threats and opportunities that the nation and the world confront.
Although this committee was convened to consider the best ways to assure the nation’s health in the new century, America is connected to the world through trade, travel, migration, and communication. In a sense, the recommendations put forth in this report have some relevance to considerations of global health. Intersectoral collaboration of the type described in
this report is necessary across nations to address common threats and to share information and technologies that will help to protect the health of all.
The future challenges just outlined are complex and far reaching. It is imperative that a strong public health system, with engaged partners, be in place to deal with these challenges if we are to promote and protect the nation’s health today and tomorrow.
CONCLUDING OBSERVATIONS
Health is shaped by both innate factors (e.g., genes, age, and sex) and other influences from the social, economic, natural, built, and political environments, ranging from the availability of shelter and food to questions of social connectedness and behavior. These multiple determinants of health, among others, constitute a reality that makes it impossible for one entity or one sector alone to bring about population health improvement. The broader efforts of many sectors and entities are needed within the context of a larger societal commitment to health. This commitment must be reflected in policies and programs at the national, state, and local levels that engage a broad spectrum of society—individual citizens and nongovernmental entities, health care providers, businesses, academic institutions, the media, and others—to work effectively together as a public health system and individually to create the conditions that allow people in the United States to be as healthy as they can be. Such a commitment will require political will that has yet to be mobilized.
Before exploring in more depth the potential role of each partner in the public health system, it is important to review the broad determinants of health that operate at the community and the societal levels to influence the health of individuals and populations.
REFERENCES
Acheson D. 1998. Independent Inquiry into Inequalities in Health. London: The Stationery Office.
Anderson G, Hussey PS. 2001. Comparing health system performance in OECD countries. Health Affairs 20(3):219–232.
Andrews GR. 2001. Promoting health and function in an aging population. British Medical Journal 322(7288):728–729.
ASPH (Association of Schools of Public Health). 1999. Demonstrating excellence in academic public health practice . Washington, DC: ASPH Council of Public Health Practice Coordinators. Available online at www.asph.org/uploads/demon.pdf. Accessed November 3, 2002.
Austin MA, Peyser PA, Khoury MJ. 2000. The interface of genetics and public health: research and educational challenges. Annual Review of Public Health 21:81–99.
Beaglehole R, Bonita R. 1998. Public health at the crossroads: which way forward? Lancet 351(9102):590–592.
Beaglehole R, Bonita R. 2000. Reinvigorating public health. Lancet 356(9232):786.
Beauchamp DE. 1988. The Health of the Republic: Epidemics, Medicine, and Moralism as Challenges to Democracy. Philadelphia: Temple University Press.
Bettcher DW, Yach D, Guidon GE. 2000. Global trade and health: key linkages and future challenges. Bulletin of the World Health Organization 78:521–534.
Brandt AM, Gardner M. 2000. Antagonism and accommodation: interpreting the relationship between public health and medicine in the United States during the 20th century. American Journal of Public Health 90(5):707–715.
Brewin B. 2001. Anthrax threat exposes IT ills. Computerworld, October 22.
Brownson RC, Kreuter MW. 1997. Future trends affecting public health: challenges and opportunities. Journal of Public Health Management 3(2):49–60.
Bureau of the Census. 1996. 65+ in the United States. Current Population Reports, Special Studies, P23–190. Washington, DC: Government Printing Office.
Campbell P. 1997. Population Projections: States, 1995–2025. U.S. Bureau of the Census, Current Population Reports, Population Projections, P25–1131. Washington, DC: U.S. Bureau of the Census.
CDC (Centers for Disease Control and Prevention) and ATSDR (Agency for Toxic Substances Disease Registry). 2001. A Global and National Implementation Plan for Public Health Workforce Development. Draft dated January 5, 2001. Atlanta, GA: CDC and ATSDR.
Daniels N. 1985. Just Health Care. New York: Oxford University Press.
Davey S. 2000. The 10/90 Report on Health Research 2000. Geneva: Global Forum for Health Research.
Day JC. 1996. Population projections of the United States by age, sex, race and Hispanic origin: 1995 to 2050. U.S. Bureau of the Census, Current Population Reports, P25– 1130. Washington, DC: Government Printing Office.
Deaton A. 2002. Policy implications of the gradient of health and wealth. Health Affairs 21(2):13–30.
DHHS (Department of Health and Human Services). 2000. Healthy People 2010, Vol. 1, p. 2–4 and p. 2–5. Available online at http://www.health.gov/healthypeople/document/tableofcontents.htm. Accessed October 5, 2001.
DHHS. 2001. Health, United States, 2001 with Urban and Rural Health Chartbook. Atlanta, GA: National Center for Health Statistics, Centers for Disease Control and Prevention, Department of Health and Human Services.
DHHS. 2002. Health, United States, 2002 with Chartbook on Trends in the Health of Americans. Atlanta, GA: National Center for Health Statistics, Centers for Disease Control and Prevention, Department of Health and Human Services.
Duffy J. 1990. The Sanitarians: A History of American Public Health. Urbana: University of Illinois Press.
Fidler D. 2002. A globalized theory of public health law. Journal of Law, Medicine, & Ethics 30:150–161.
Fraser MR. 1999. Information technology and local health departments. Presentation to the NACCHO Board Annual Meeting, Dearborn, Michigan, July 1999 . Available online at www.naccho.org/GENERAL156.cfm. Accessed October 25, 2002.
Fried LP. 2000. Epidemiology of aging. Epidemiologic Reviews 22(1):95–106.
Gostin LO. 2000. Public Health Law: Power, Duty, Restraint. Berkeley and New York: University of California Press and Milbank Memorial Fund.
Gostin LO. 2002. Public Health Law and Ethics: A Reader. Berkeley and New York: University of California Press and Milbank Memorial Fund.
The Hastings Center. 2000. Description of the project on civic health. Available online at www.thehastingscenter.org/OldSite/prog4_4.htm. Accessed October 25, 2002.
Hoyert DL, Arias E, Smith BL, Murphy SL, Kochanek KD. 2001Deaths: Final Data for 1999. National Vital Statistics Reports 49(8).
IFTF (Institute for the Future). 2000. Health & Health Care 2010: The Forecast, the Challenge. Prepared by the Institute for the Future with support from the Robert Wood Johnson Foundation. San Francisco, CA: Jossey-Bass Publishers.
IOM (Institute of Medicine). 1988. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 1997. America’s Vital Interest in Global Health: Protecting Our People, Enhancing Our Economy, and Advancing Our International Interests. Washington, DC: National Academy Press.
IOM. 1998. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 1999. The Pervasive Role of Science, Technology, and Health in Foreign Policy: Imperatives for the Department of State. Washington, DC: National Academy Press.
IOM. 2000. Ending Neglect: The Eliminations of Tuberculosis in the United States. Washington, DC: National Academy Press.
IOM. 2001. Health and Behavior. Washington, DC: National Academies Press.
IOM. 2002. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: National Academies Press.
Jacobzone S. 2000. Coping with aging: international challenges. Health Affairs 19(3):213– 224.
Jee M, Or Z. 1999. Health outcomes in OECD countries: a framework of health indicators for outcome oriented policy–making. OECD Labour Market and Social Policy Occasional Paper No. 36 (DEELSA/ELSA/WD(98)7). Available online at www1.oecd.org/els/social/docs.htm. Accessed October 5, 2001.
Kass NE. 2001. An ethics framework for public health. American Journal of Public Health 91(11):1776–1782.
Kassalow JS. 2001. Why Health Is Important to US Foreign Policy. New York: Council on Foreign Relations and the Milbank Memorial Fund. Available online at www.milbank.org/Foreignpolicy.html. Accessed October 25, 2002.
Kaul I, Faust M. 2001. Global public goods: taking the agenda forward. International Journal of Public Health 79(9):869–874.
Keigher SM, Lowery CT. 1998. The sickening implications of globalization. Health and Social Work 23:153–158.
Khaw K. 1997. Healthy aging. British Medical Journal 315(7115):1090–1096.
Khoury MJ, Burke W, Thomson EJ. 2000. Genetic and public health: a framework for the integration of human genetics into public health practice. In Khoury MJ, Burke W, Thomson EJ (Eds.). Genetics and Public Health in the 21st Century: Using Genetic Information to Improve Health and Prevent Disease. New York: Oxford University Press.
Kindig DA. 1997. Purchasing Population Health: Paying for Results. Ann Arbor, MI: University of Michigan Press.
Kinney ED. 2002. Administrative law and the public’s health. Journal of Law, Medicine & Ethics 30:212–223.
Koplan JP, Fleming DW. 2000. Current and future public health challenges. Journal of the American Medical Association 284:1696–1698.
Lasker R, the Committee on Medicine and Public Health. 1997. Medicine and Public Health the Power of Collaboration. New York: The New York Academy of Medicine.
Last J. 1995. Dictionary of Epidemiology, 3rd ed. New York: Oxford University Press.
Lee K. 2001. Globalization: a new agenda for health, pp. 13–29. In McKee M, Garner P, Stott R (Eds.). International Cooperation in Health. Oxford: Oxford University Press.
Levit K, Smith C, Cowan C, Lazenby H, Martin A. 2002. Inflation spurs health spending in 2000. Health Affairs 21(1):172–181.
Levy BS. 1998. Creating the future of public health: values, vision, and leadership. American Journal of Public Health 88(2):188–192.
McGinnis GM, Foege WH. 1993. Actual causes of death in the United States. Journal of the American Medical Association 270(18):2207–2212.
McGinnis JM, Williams-Russo P, Knickman JR. 2002. The case for more active policy attention to health promotion. Health Affairs 21:78–93.
McKinlay J, Marceau L. 2000. US public health and the 21st century: diabetes mellitus. Lancet 356:757–761.
McMichael AJ, Beaglehole R. 2000. The changing global context of public health. Lancet 356:495–499.
Mechanic D. 2002. Disadvantage, inequality and social policy. Health Affairs 21(3):48–76.
Mills RJ. 2002. Health insurance coverage: 2001. U.S. Bureau of the Census, Current Population Reports, P60–220. Washington, DC: U.S. Bureau of the Census.
NACCHO (National Association of County and City Health Officials). 2001. Assessment of local bioterrorism and emergency preparedness. NACCHO Research Brief Number 5, October 2001. Available online at http://www.naccho.org/project48.cfmwww.naccho.org/project48.cfm. Accessed October 25, 2002.
Navarro V. 1998. Comment: whose globalization? American Journal of Public Health88:742– 743.
Novak WJ. 1996. The People’s Welfare: Law and Regulation in Nineteenth-Century America. Chapel Hill: University of North Carolina Press.
NRC (National Research Council). 1999. The Pervasive Role of Science, Technology, and Health in Foreign Policy: Imperatives for the Department of State. Washington, DC: National Academy Press.
NRC. 2001. Preparing for an Aging World: The Case for Cross-National Research. Washington, DC: National Academy Press.
OECD (Organisation for Economic Co-Operation and Development). 2001. Health data 2001, Table 1: life expectancy in years. Available online at www1.oecd.org/els/health/software/fad.htm. Accessed October 25, 2002.
O’Keohane R. Empathy and international regimes. 1990. In Mansbridge JJ (Ed.). Beyond Self-Interest. Chicago: University of Chicago Press.
Omenn GS. 2000. Public health genetics: an emerging interdisciplinary field for the post-genomic era. Annual Review of Public Health 21:1–13.
Parmet WE. 2002. After September 11: rethinking public health federalism. Journal of Law, Medicine & Ethics 30:201–211.
Petersen A, Lupton D. 1996. The New Public Health: Health and Self in the Age of Risk. London: Sage.
Pew Environmental Health Commission. 1999. Healthy from the start: why America needs a better system to track and understand birth defects and the environment. Pew Environmental Commission.
Portnoi VA. 1999. Progressing from disease prevention to health promotion. Journal of the American Medical Association 282(19):1812–1813.
PricewaterhouseCoopers. 1999. HealthCast 2010SM: smaller world, bigger expectations. Available online at www.pwchealth.com/healthcast2010.html. Accessed October 25, 2002.
Public Health Functions Steering Committee. 1994. The Public Health Workforce: An Agenda for the 21st Century. Full Report of the Public Health Functions Project, U.S. Department of Health and Human Services.
Reed DM, Foley DJ, White LR, Heimovitz H, Burchfiel CM, Masaki K. 1998. Predictors of healthy aging in men with high life expectancies. American Journal of Public Health 88(10):1463–1468.
Reinhardt UE, Hussey PS, Anderson GF. 2002. Trends: cross-national comparisons of health systems using OECD data, 1999. Health Affairs 21(3):168–191.
Rogers R, Reardon J. 1999. Recommendations for International Action: Barriers to a Global Information Society for Health. Report from the Project G8-ENABLE. Amsterdam: IOS Press.
Sen K, Bonita R. 2000. Global health status: two steps forward, one step back. Lancet 356:577–581.
Shain BA. 1996. The Myth of American Individualism: The Protestant Origins of American Political Thought. Princeton, NJ: Princeton University Press.
Starfield B. 1998. Primary Care: Balancing Health Needs, Services, and Technology. New York: Oxford University Press.
Starfield B. 2000. Is US health really the best in the world?Journal of the American Medical Association 284(4):483–485.
Turnock BJ. 2001. Public Health: What It Is and How It Works. Gaithersburg, MD: Aspen Publishers.
Walzer M. 1983. Spheres of Justice: A Defense of Pluralism and Equality. New York: Basic Books.
WBGH (Washington Business Group on Health). 2000. The business interest in a community’s health. Washington, DC: Washington Business Group on Health.
Weinberg DH. 1996. A brief look at postwar U.S. income inequality. U.S. Census Bureau Current Population Reports, P60–191.
WHO (World Health Organization). 1946. Constitution of the World Health Organization. New York: WHO Interim Commission.
Willett W. 2002. Balancing life-style and genomics research for disease prevention. Science 296:695–698.
Wolf DA. 2001. Population change: friend or foe of the chronic care system. Health Affairs 20(6):28–42.
Yach D, Bettcher, D. 1998. The globalization of public health, I. Threats and opportunities. American Journal of Public Health 88:735–738.




























