4
The Community
The community stagnates without the impulse of the individual. The impulse dies away without the sympathy of the community.
William James
This chapter is at the heart of the Healthy People 2010 vision reiterated by the committee: “healthy people in healthy communities.” Communities are both the physical and cultural settings for and—through their residents and community-based organizations—participants in action to promote the public’s health. They are also points of convergence for the interests of employers, businesses, and academia; the messages of the media; and the services of governmental public health agencies and the health care delivery system.
This chapter examines the multiple dimensions of community and its critical importance to an effective public health system. This critical role has been a fundamental concept in the international literature on population health for many years. The Health For All initiative, begun by the World Health Organization in the 1970s, called for a strong primary care system to include basic health services, clean water and air, basic sanitation, adequate nutrition, and full engagement with the community served. In the United States, the sophistication of the health care delivery system and the emphasis on individual health have led to the focus of policy and resources on the high-technology and research ends of the health care delivery spectrum and an underestimation or overlooking of the role of the community in achieving health gains. This is changing.
DEFINING THE COMMUNITY
A community can be described as a group of people who share some or all of the following: geographic boundaries; a sense of membership; culture
and language; common norms, interests, or values; and common health risks or conditions (IOM, 1995; Jewkes and Murcott, 1996; Ruderman, 2000; Ricketts, 2001). Members of communities typically experience the shared reality of living or working in the same location or environment and so are in a position to influence and be influenced by the social, economic, and physical risk factors in that environment (Roussos and Fawcett, 2000; Kreuter et al., 2001). Although acknowledging the increasing influence of “communities of interaction” such as online groups, this chapter focuses mainly on activities based in geographic communities—neighborhoods, cities, counties, and in a few cases, states—that are critical to creating the conditions for a community to be as healthy as it can be.
Communities consist of individuals and families, as well as the various organizations and associations that make up a community’s “civil society”: nonprofit, nongovernmental, voluntary, or social entities, including ethnic and cultural groups; advocacy organizations; and the faith community (Salamon et al., 1999; Himmelman et al., 2001). Organizations exist between the level of the individual and that of the community or society. The United States has both a history of individualism and, as de Tocqueville observed in 1831, a rich civic tradition of individuals associating or organizing to accomplish common goals. The public sector at the community level encompasses local government officials and agencies traditionally seen as having health-related responsibilities, as well as many others that have important but sometimes less obvious roles in health but whose policies and objectives may have potential health consequences. The latter may include city councils, public schools, colleges and universities, police and fire departments, zoning boards, housing authorities, parks and recreation agencies, and agricultural development and cooperative extension services. Other members of the community may come from the private sector, including private schools, colleges, and universities; health care providers and payers; and small and large businesses.
A healthy community is a place where people provide leadership in assessing their own resources and needs, where public health and social infrastructure and policies support health, and where essential public health services, including quality health care, are available. In a healthy community, communication and collaboration among various sectors of the community and the contributions of ethnically, socially, and economically diverse community members are valued. In addition, the broad array of determinants of health is considered and addressed, and individuals make informed, positive choices in the context of health-protective and supportive environments, policies, and systems (Goodman et al., 1996; CDC, 1997; Norris and Pittman, 2000).
Health is a “fundamental resource to the individual, the community and to society” (Kickbusch, 1989:13). When people are healthy, they are
better able to work, learn, build a good life, and contribute to society. However, as noted in Chapter 2, the health of neither individuals nor populations occurs in a vacuum. Instead, it is shaped by a wide range of factors, such as income and education, social connectedness, employment, and access to quality health care. Inadequate and dangerous physical environments in homes, schools, neighborhoods, and workplaces and risk factors such as air and water pollution, unsafe food, social isolation, high rates of unemployment, violence, and crime constitute some of the problems experienced by communities. It may seem that these types of problems can be distanced from the concerns of the general population, as if these circumstances affect only certain groups (e.g., those with high blood pressure, smokers, or people who live in specific neighborhoods). In reality, the effects of health risks touch us all in many ways, and actions to address health at the population level benefit everyone in society (Rose, 1992). Moreover, the solutions for assuring population health are not owned by governmental public health agencies; they can be found in communities and in community organizations and partnerships (CDC, 1997; WHO, 1998; Bowles, 1999; Mitchell and Shortell, 2000). Today’s health challenges, ranging from jet-setting microbes and soaring obesity rates to emerging environmental risks and bioterrorism, highlight the interconnectedness of people and communities and the need for joint efforts to meet those challenges (McGinnis and Foege, 1993; Ruderman, 2000; Norton et al., 2002).
The linkages among people and communities and people are clearly evident in the processes set into motion by globalization. A local community in many areas of the United States may be a microcosm of the world community, with a complex mix of beliefs, traditions, and languages. Given the rich fabric of most American communities, it has become impossible to consider threats to health someone else’s problem. Disease and disability do not differentiate between cultures and ethnic backgrounds—microbes and environmental toxins move easily among and across nations and regions, and no person or community is completely safe unless all are safe.
COMMUNITY-BASED COLLABORATION
Growing Commitment to Collaboration
Although this report defines public health as “what we as a society do collectively to assure the conditions in which people can be healthy” (IOM, 1988:1), in practice, the community’s role in health programs has sometimes been that of passive recipient, beneficiary, or research subject, with active work in public health carried out by experts (e.g., governmental public health agencies) using approaches that are frequently unsuccessful in responding to the complex issues and needs of the community (Schwab and
Syme, 1997). A great deal has changed since the Committee for the Future of Public Health observed that health departments and public health professionals worked largely in isolation, with little in the way of “constituency building, citizen participation, or continuing (as opposed to crisis-driven) communications with elected officials or with the community at large” (IOM, 1988:5). Today, dialogue and collaboration between local health departments and the communities they serve have become more common in practice and more critical in concept. For example, a recent study of 10 local health departments from different states found that they were substantially involved with community and youth organizations, schools, and the media in the areas of tobacco use prevention, injury prevention, and physical activity promotion (McHugh et al., 2000).
Many communities, through individuals and organizations, have become partners with health departments in health improvement and have even become leaders in spearheading collaborative efforts (Fawcett et al., 1996; Mitchell and Shortell, 2000; Norton et al., 2002). The present committee found during its site visit to the Caring Community Network of the Twin Rivers, a Turning Point site in New Hampshire (see Appendix F), an example of an innovative way to create a local public health system that works effectively despite a limited governmental public health infrastructure. This community, a spread-out cluster of 12 towns, has no health department. Instead, each town has a more or less volunteer health officer, who in some cases is not a health professional. The work of assuring the public’s health is carried out through the collaborative efforts of committed individuals and groups, including the local public health officials, health care and mental health services providers, social service and community development organizations, educators, and the chamber of commerce (CCNTR, 2001).
In authentic community-based partnerships, the participation and contributions of various stakeholders are likely to produce benefits in the form of increased effectiveness and productivity by reducing duplication of effort and avoiding the imposition of solutions that are not congruent with the local culture and needs. Community partnerships are also likely to have the benefits of empowering the participants, strengthening social engagement, establishing trust, and ensuring accountability (Israel et al., 1998; Mitchell and Shortell, 2000; Robinson and Elliott, 2000; Steele, 2000; Butterfoss et al., 2001; Chaskin et al., 2001; Lasker et al., 2001; Williams and Yanoshik, 2001; Wolff, 2001a, 2001b).
A variety of vehicles can be used for community collaborations, including coalitions, partnerships, community advisory boards, consumers’ rights and advocacy groups, and nonprofit organizations. These groupings can bring together participants from many sectors of a community, including businesses, ethnic groups, faith-based organizations, and various public agencies. The Kansas LEAN (Leadership to Encourage Activity and Nutri-
tion) Coalition is an example of a statewide coalition that began at the local level in 1990. By 1997, it had expanded to include 60 organizations and 100 individuals. The coalition brought together governmental agencies such as the state and local public health departments and state and local extension offices, nonprofit community and professional organizations, and businesses such as supermarkets to prevent chronic disease through dietary change and exercise (Johnston et al., 1996).
Some opportunities for collaboration have less obvious but important health effects, as in the case of community redevelopment efforts. The economic condition of a community has clear implications for health. Higher employment levels, for example, tend to improve not only personal income and access to health insurance but also a community’s tax revenues and, thus, its ability to address health threats and to provide opportunities for health improvement. In some communities, local health departments have become partners in efforts to revitalize neighborhoods through the remediation of areas with industrial waste and environmental contamination (NACCHO, 2000a). Empowerment zones and enterprise communities are examples of public–private partnerships with significant government resources requiring collaboration at the local level to improve health in communities. A recent study found that 119 of the 144 national empowerment zones and enterprise communities initiatives had an interest in health issues (PHF, 2000).
Some collaborations come into existence through the independent initiative of communities or community groups, whereas others are created in response to an outside stimulus, such as when government agencies or foundations require the formation of broad partnerships as part of grant processes (Mitchell and Shortell, 2000). The committee is encouraged to see indications that governmental public health agencies, community health centers, hospitals, and health maintenance organizations recognize that community collaboration is a necessity in health improvement (CDC, 1997; Pronk and O’Connor, 1997; Omenn, 1999). Some of the major federal and foundation initiatives that require and support the creation of broad-based community coalitions include Healthy Start, a community-based infant mortality reduction program; Turning Point1 and Community Voices,2
|
1 |
Turning Point is a grant program of the W. K. Kellogg and Robert Wood Johnson Foundations that began in 1996 and ended in 2002. The goal of Turning Point has been to “transform and strengthen the public health infrastructure in the United States” by supporting states and local communities to “improve the performance of their public health functions through strategic development and implementation processes” (www.wkkf.org). |
|
2 |
Community Voices is a 5-year initiative launched by the W. K. Kellogg Foundation in 1998 in 13 U.S. communities. The goal of Community Voices is to improve health care for the uninsured and underinsured by strengthening and securing the safety net and community support services. |
privately funded community public health improvement grant programs; and Center for Substance Abuse Prevention programs, which support community-based substance abuse prevention “systems” that involve community coalitions and intersectoral collaboration (Lasker et al., 2001).
Ingredients for Successful Collaboration
Although collaborations to improve community health have become increasingly common, the committee recognizes that bringing together diverse agendas, institutional cultures and jargon, personalities, and expectations can be complicated, frustrating, and sometimes disappointing. One lesson that has been learned from such experiences, however, is that the community must be engaged before an agenda is set—the active participation of community leaders, members, and organizations is needed in the earliest stages of community-based public health action, if it is not already the force that drives such action (The Lewin Group, 2002). The initial communication and networking necessary to launch a community health improvement project entail frank examination and discussion of motivations, approaches, and goals by all stakeholders. At times, agencies and organizations may seek to implement their own unilateral agendas in communities, driven by scientific, political, economic, or professional interests, with token community involvement and often negative outcomes (Schwab and Syme, 1997; Fawcett, 1999; Norton et al., 2002). Many communities have been “coalitioned to death” without reaping any significant benefits (Himmelman et al., 2001). Such problems illustrate the need for thoughtful, broadly inclusive, well-planned, and realistic community health improvement approaches.
Clearly, community health initiatives involve complex social and relational dynamics, as well as efforts to produce change that require significant investments of time and resources (Wickizer et al., 1998; Kreuter et al., 2000; Sharpe et al., 2000; Shortell, 2000; Rhein et al., 2001). The importance of allotting adequate time to the process of collaborative planning was well illustrated during the committee’s site visit to Healthy New Orleans, a Turning Point project in Louisiana (see Appendix F). Healthy New Orleans worked over a period of 2 years to build a partnership of diverse stakeholders. After establishing and clarifying roles and relationships, the partnership was able to develop a plan for community health improvement that was truly a product of community knowledge and effort (Healthy New Orleans, 2001).
The HIV/AIDS movement provides another example of successful collaboration for community action (Stewart and Weinstein, 1997). AIDS volunteerism has uniquely demonstrated the effectiveness of turning people affected by AIDS into experts who both (1) mobilized community building
and (2) transformed community attitudes and norms to achieve behavioral change. Communities working on a range of health issues may have much to learn from the example set by the gay and lesbian communities’ collaborative action. Yet, although the HIV/AIDS movement has succeeded in mobilizing public opinion and action, more research is needed to show what has worked best in mobilizing action and changing community norms and thus warrants replication (Kegeles and Hart, 1998; Reger et al., 2000).
Research to assess the effectiveness of community collaborations has had somewhat mixed results because of the heterogeneity of communities, the long time lines involved in achieving community health improvement goals, and other complexities inherent in community-driven public health activities (Sharpe et al., 2000; Lasker et al., 2001). However, a growing base of empirical evidence from programs such as Turning Point and Community Voices provides a good road map for communities and their partners. Health improvement and other positive outcomes typically result from collaborations that are sustained over the long term, that institutionalize effective programs and processes, and that mobilize and utilize all available resources to deal with evolving challenges and population health issues (Fawcett et al., 2000b, 2000c).
Success is also more likely with strong community engagement, an awareness of the community’s social dynamics, and leadership that reflects the racial and ethnic diversity of the community (CDC, 1997). Other important ingredients include having a clear vision and goals to guide action planning; allotting adequate time and financial, technical, and other supportive resources to collaborations and their health improvement efforts; and recognizing the importance of data collection and dissemination (CDC, 1997; W. K. Kellogg Foundation, 1997; Fawcett et al., 2000c; Roussos and Fawcett, 2000). Success in specific health improvement activities can depend on the use of varied strategies and on their intensity, duration, and penetration into the community (Fawcett et al., 2000b; Wilcox and Knapp, 2000; Lasker et al., 2001; Paine-Andrews, 2002).
Problems arise around leadership, governance, and other management issues, such as planning and evaluation. Inadequate resources of various sorts— insufficient or inadequate funding or data, short time lines, or a lack of technical support—also contribute to problems, as does a lack of broad and authentic community engagement, which may be reflected in narrowly formed partnerships that do not include all the sectors of the community needed for efficient and effective action (Himmelman et al., 2001; Lasker et al., 2001).
Sharing Public Health Governance
Ultimate legal responsibility for safeguarding and promoting the health of the population rests with governmental public health agencies at the federal, state, and local levels (see Chapter 3), but those agencies cannot be
effective acting alone. They must be partners in a broader network of individuals and organizations with the potential to act within a public health system. At the local level, in particular, health departments can become the facilitators and supporters of strong local public health systems that are informed by community voices, responsive to community needs, and linked to community assets.
The committee supports a type of shared governance through which the agenda for population health is truly “owned” by the population it serves (Turning Point Community Health Governance Workgroup, 2001a and b; The Lewin Group, 2002). This entails providing opportunities for community input and leadership in planning and in funding decisions. It also requires educating the public about the concepts of public health, including the core functions and essential services (see Chapter 1), to help ensure that public health agencies are accountable to those they serve (Becnel, 2001). An approach used in some communities is governance of the health department by a local board of health, whose members come from various sectors of the community (see Chapter 3). The committee also encourages community involvement in the governance of other health-related activities. For example, a majority of the members of oversight boards for community health centers that receive federal funding (under Section 330 of the Public Health Law) must be community users of those facilities’ services.
The Turning Point initiative—which involves 41 communities across 14 states—exemplifies shared governance. The most successful of the Turning Point sites mobilized the community from the earliest stages of assessing needs and setting an agenda for public health system change. These partnerships made community engagement a permanent and ongoing element. In fact, the community’s role became institutionalized in the local public health system through formal policies, investments, and programs (The Lewin Group, 2002). This national experiment in transforming local governmental public health agencies (Turning Point Community Health Governance Workgroup, 2001b) suggests that making shared governance a reality requires tools that formalize the governance structure so that it can achieve legitimacy. Also necessary are optimal communication between the community and the governing group and systematic, efficient and flexible management of operations (Turning Point Community Health Governance Workgroup, 2001b). The National Public Health Performance Standards Program3 includes an evolving set of model standards for the role of a
governing body in a local public health system and an instrument for assessing the performance of that governing body (National Association of Local Boards of Health, 2002).
FRAMEWORK FOR COLLABORATIVE COMMUNITY ACTION ON HEALTH
Once the collaboration has been created, several frameworks are available for use by communities, health departments, and their partners. Some of these models include the Planned Approach to Community Health, Mobilizing for Action through Planning and Partnerships, and the Community Health Improvement Process (Kreuter, 1992; IOM, 1997). The models provide step-by-step guidance for various aspects of the health improvement process, including assessing the health status of the community and the capacity of the local governmental public health agency.
This chapter uses a simple framework provided by Fawcett and colleagues (2000b) to help describe the activities and processes involved in community action on health (CDC, 2002). This framework illustrates five key components of the activities and processes needed in community health action (Figure 4–1). Figure 4–1 illustrates a process that is often cyclical rather than linear, with work on one health improvement initiative leading to subsequent reassessments of a community’s health needs and priorities.
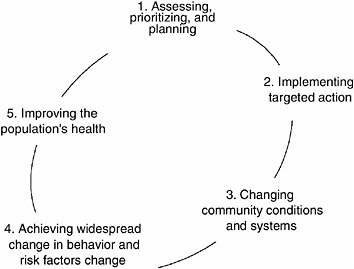
FIGURE 4–1 A framework for collaborative public health action by communities.
SOURCES: Fawcett et al. (2000b); CDC (2002).
Although the five components of this particular framework do not necessarily take place in the sequential fashion shown, the diagram reflects the progression of events that has been documented in successful community-based public health initiatives (Fawcett et al., 2000b; Foster-Fishman et al., 2001).
Each step of the framework for collaborative action will be discussed and illustrated with examples from the experience of community health improvement programs and initiatives.
Assessing, Prioritizing, and Planning
The processes of assessing, prioritizing, and planning will help community partnerships formulate a clear statement of goals to guide their work. These collaborative tasks are the first components of community action for health, but they also must be ongoing activities throughout a community’s health improvement efforts (IOM, 1996b, 1997; GHCF, 2001). By engaging in these activities, communities come to understand the context, causes, and solutions for various health problems. They include taking inventory of community assets and resources, identifying priorities for community action, and planning the actions to be taken. Community organizing and coalition building are necessary if these activities are to be collaborative.
The Health Action initiative in Monroe County, New York, provides a good example of community involvement in assessing, prioritizing, and planning for health improvement (Milbank Memorial Fund, 1998; Health Action, 2001). Founded in 1995, Health Action is a collaborative of health care providers, hospitals and clinics, the local health department, an urban health commission, a university, the chamber of commerce, a large employers’ organization, and a professional association. Between 1998 and 2001, report cards were developed and released for five areas: (1) the health of mothers and children, (2) the health of adolescents, (3) the health of adults, (4) the health of older adults, and (5) environmental health. Focused goals and action plans were developed for each area. For adults and older adults, Health Action selected two goals: to promote healthy behaviors that prevent or delay chronic disease and to promote the use of preventive health services. Health promotion objectives included increasing physical activity and providing nutrition education and weight management, with the aim of decreasing the chronic disease risks posed by overweight and obesity. In 2001, Health Action’s Adult/Older Adult coalition began work on a communications campaign supported by program activities (such as workplace fitness) to make Monroe County a more physically active community.
Certain types of quantitative data, such as rates of disease, injury, and death, have usually been available to communities. Other data have become more readily available as more states and local communities, usually with the leadership or support of governmental public health agencies, have begun to
conduct systematic assessments of health status and the determinants of health. The availability of data for small areas (at the subcounty level) has been an issue in general for community health programs, and it highlights the need for high-quality, comprehensive assessments of community health to guide action. In 2000, the Health Resources and Services Administration’s Community Health Status Indicators (CHSI) Project produced a set of health assessment documents for each of the 3,082 counties in the United States and made them available online (www.communityhealth.hrsa.gov/). The CHSI documents, which used a set of indicators for which comparable data were available for nearly all counties, can serve as a useful starting point for selecting indicators of particular interest to a given community, for making comparisons with other communities throughout the country, or for planning an update of a community’s indicators.
A community-based approach to health improvement that considers the broad range of social and environmental determinants of health may call for the use of a variety of indicators, including ones that measure characteristics of the community rather than those of individuals (i.e., community-level indicators). Community report cards and other types of regular assessments should include not only measures directly related to health, such as infant mortality rates and the incidence of infectious diseases, but also measures related to various health determinants (IOM, 1997). Indicators could include local employment rates, housing stocks, and levels of income and education, along with less conventional indicators such as the density of liquor stores; the quality of air and water; the availability of parks and green spaces, housing, and public transportation; and other measures of livability. In addition, qualitative or anecdotal data (e.g., residents’ satisfaction with the community, feelings of community cohesion, or informal measures of social capital) may also be an important part of the assessment process.
The interest in community-level indicators is reflected in the work of a panel organized by the Centers for Disease Control and Prevention, which developed indicators for cardiovascular health in three risk areas: diet, physical inactivity, and tobacco use (Cheadle et al., 2000). The community-level indicators for physical inactivity, for example, included “miles of walking trails per capita” and “presence of local policy to include physical education in public K–12 curriculum” (Cheadle et al., 2000:112). Cross-cutting indicators included the number of media reports that dealt with smoking, nutrition, and physical activity and the number of assessments or screenings within the community for all cardiovascular risk factors. An added benefit of community-level indicators is the fact that they are sometimes easier and less expensive to measure than indicators based on the behaviors or characteristics of individuals, which may require costly household surveys.
The committee notes that new and evolving information and communications technologies are increasingly valuable resources for community-driven public health action (Fawcett et al., 2000a). The University of Kansas Community Tool Box, for example, is an online resource for community-based public health planning and action (http://ctb.lsi.ukans.edu/). The Internet has become instrumental in helping community groups and organizations obtain essential data and information, communicate with partners, and provide technical assistance and support to other collaborations and coalitions in their own community and elsewhere. In recent years, geographic information systems have also become a powerful tool for spatial analysis of diseases, environmental contamination, and social and demographic information (ATSDR, 2000). Some of the governmental jurisdictions (i.e., states) using this technology are able to share vital information with communities and their partners.
Implementing Targeted Action
The second component of community-driven health improvement efforts is implementing targeted action to address high-priority health issues (Fawcett et al., 2000b). As a result of some of the lessons learned in community collaborative action, observers commend the use of multiple strategies, such as education, various forms of communication, political or legal action, and environmental interventions (Fawcett, 1999). Some observers emphasize that community action should focus on changing the community conditions or individual behaviors that affect health risks rather than on only providing health care or other services to individuals (Johnston et al., 1996).
As a result of the sometimes long and often complicated chain of events between program implementation and desired health outcomes, communities are encouraged to focus on proven strategies and best practices to enhance their chances of success (IOM, 1997; Butterfoss et al., 2001). Resources such as The Guide to Community Preventive Services (Task Force on Community Preventive Services, 2000), which provides evidence-based evaluations of various interventions, can help communities select appropriate strategies. In some cases, however, coalitions may be justified in selecting interventions that are favored by the community, even if evidence for their effectiveness is weak, to build ownership in community action and to nurture meaningful participation (Himmelman, 2001; W. K. Kellogg Foundation, 2001). The challenge is to achieve a balance between the interrelated efforts to engage coalition involvement and sustain its well-being and to invest in strategies that increase the likelihood of meeting health goals.
The strategies and activities implemented by community partnerships may depend on the particular perspectives and resources brought to the
|
BOX 4–1 Community in Action to Address the Environment In New York State, the Monroe County Health Department and other public and private community partners formed the Water Education Collaborative to educate citizens about protecting water quality. The Industrial Management Council, the Monroe County Health Department, and the Rochester Institute of Technology are collaborating on a plan to provide environmental health training and technical assistance to small- and medium-size businesses. This will help local businesses develop environmental management systems (environmental monitoring, waste recycling). The Kodak and Xerox corporations, which are headquartered locally, already provide leadership in this area. SOURCE: Health Action (2001). |
table by participants. For example, groups that represent the interests of ethnic communities (e.g., National Council of La Raza, Congress of National Black Churches, and Association of Asian Pacific Community Health Organizations) or consumers’ rights and advocacy groups can help mobilize communities for action, provide public education, and advocate for policy change to safeguard population health. Businesses may change their practices and policies to address community health concerns and employee health needs (see Box 4–1). Depending on the nature of the business, such changes might include implementing policies to ban smoking in public places, providing health information to employees and customers, or improving compliance with environmental laws and regulations pertaining to air and water quality.
Religious congregations, which are among “the most pervasive voluntary organizations in our society,” and other faith-based entities can play a significant role in community health improvement (DHHS, 1999). For instance, the outreach workers of Oakland’s Asian Health Services reach Korean groups with information about health care access at church health fairs. Faith-based groups are often community institutions, deeply rooted in neighborhoods, and may play an important role in local public health systems and community-based health improvement initiatives (DHHS, 1999; Lundblad, 1999). This is especially true in many African-American communities. Additionally, faith communities can act as conveners and mobilizers of community residents and others affiliated with them around issues of health policy and interventions for health promotion and disease prevention (e.g., nutrition, fitness, and health screening services) (see Box 4–2).
|
BOX 4–2 A Project in the Faith Community Project Joy was conducted by university researchers in collaboration with a local faith community to promote cardiovascular health among church-going African-American women in Baltimore, Maryland (Yanek et al., 2001). Sixteen churches were randomly selected, and 529 female members of those churches received one of three behavioral interventions: an active intervention with a spiritual component, an active intervention without the spiritual component, and a self-help intervention as a control group. The active intervention consisted of weekly sessions on nutrition, including cooking demonstrations and taste tests, and 30 minutes of some moderate aerobic activity, conducted by project educators in collaboration with trained lay leaders from the churches. The spiritual component consisted of religious messages and prayer and gospel music for workout sessions. The control intervention provided only educational material and a hotline for health education consultation. By the end of the intervention, the two active groups were virtually indistinguishable, because the one without a preplanned spiritual component had created its own. Both of the groups with the active intervention experienced significant improvements, compared with the self-help group, in weight, waist circumference, blood pressure, dietary energy, and total fat and sodium intakes. The input and participation of the community in planning and implementation and a supportive social environment resulted in behavioral changes that led to improved health. Four years after the project began, eight of the nine churches with an active intervention, plus the church that hosted the pilot intervention, continue the weekly support and education sessions—an example of sustained, institutionalized change (Yanek et al., 2001). |
Communities can also contribute to the process of health improvement through the efforts of individuals who sometimes become part of the public health workforce. For example, in communities across the United States, health promoters,4 community health workers, or community outreach workers link community members to systems of care, help to mobilize communities to change the conditions for health, and conduct health education (Ramos et al., 2001). Community workers seem to be most effective when they are selected from among individuals who are respected and trusted by their communities, for example, informal community leaders. In addition to their knowledge of the community’s needs, their formal participation in the public health enterprise may also reassure community groups that are wary of gov-
ernment systems or health care providers for political, economic, or other reasons (University of Arizona, 1998; Ramos et al., 2001).
During site visits, the committee observed that community workers are used with apparent success by several projects around the country. In Orange County, California, Latino Health Access, a community-based organization, receives community input, works collaboratively with the local county health department, and manages paid promotores who provide education and link community members to services and resources, including those provided by the health department (Bracho, 2000). The Asian Health Services and La Clinica de La Raza in Oakland, California, use the services of staff members from several ethnic communities to conduct culturally and linguistically competent health promotion and health care outreach in those communities (see Appendix F).
Baltimore’s Vision for Health Consortium and Men’s Health Center (see Appendix F) have community advocates or outreach workers who perform a range of services, including linking uninsured community members to a “medical home,” following up with individuals who do not return for test results or treatment, and providing assistance with other referrals and linkages. Denver Health, in Denver, Colorado, also uses the services of community outreach workers to help community members who are uninsured gain access to health care services and to provide health promotion and health education services in the community (see Appendix F). Denver Health’s unique public–private public health infrastructure has developed a process for training community outreach workers and integrating them into the public health workforce. Classes and even a degree program are available through local community colleges. In Arizona, a similar promotora training program has been created by the Border Health Fronteriza project and is coordinated by the University of Arizona (HRSA, 2001).
Changing Community Conditions and Systems
Changing community conditions and systems is the third component of the framework for community action to improve health. It involves changing aspects of the physical, social, organizational, and even political environments to eliminate or reduce factors that contribute to health problems or to introduce new elements that promote better health. Such changes might include instituting new programs, policies, and practices; changing aspects of the physical or organizational infrastructure in the community; and changing community attitudes and beliefs or social norms (Fawcett et al., 2000b; Mitchell and Shortell, 2000) (see Box 4–3). Some policy changes, for example, are aimed directly at health-related concerns such as improving access to health care or preventing injury and disease through means such as regulation of alcohol and tobacco sales, the institution of require
|
BOX 4–3 Communities in Action to Address Mental Illness Communities can be catalysts for a change in societal attitudes toward depression and other mental illnesses—the first step in addressing the stigma attached to these conditions (Corrigan and Penn, 1999; Link et al., 1999; Corrigan et al., 2001). This change may encourage people dealing with mental illness to seek treatment. Through educational efforts, communities can reinforce the public health message that depression and other mental illnesses are real and disabling conditions that can be treated effectively (DHHS, 1999). Communities can also combat the stigma attached to mental illness through sponsorship of low-cost programs that constructively bring the public into contact with people with mental illness. |
ments for the use of seat belts or bicycle helmets, or the institution of rules and laws on the responsible disposal of hazardous industrial wastes. Various tools can be applied in efforts to achieve changes in community conditions and systems. These can include school and workplace-based educational programs, social marketing, and other social transformation activities. Community groups can also advocate for government bodies to take appropriate actions, such as regulating environmental pollutants. Informed and mobilized communities can help ensure that government agencies enforce such regulations.
The committee found many examples of community-based efforts to modify local conditions as part of a health improvement initiative. These are, in a very real sense, examples of a public health system in action to create conditions in communities for people to choose healthy behaviors. Holder and colleagues (2001), for example, reported on a multilevel intervention in a South Carolina community that was aimed at changing policies and practices through several proven components, including community coalition building and the development and enactment of policies on alcohol outlets. These interventions increased law enforcement as well as the perception in the community that drunk drivers would be caught. In addition, local businesses modified their policies for beverage service, and community groups became mobilized to change the zoning policies that governed the density of alcohol outlets. Following the intervention, rates of crashes related to drunk driving were significantly reduced and binge drinking declined. Holder and colleagues (2001) concluded that education and public awareness about a health problem had to be supplemented with environmental strategies that brought about community and system changes to achieve the health improvement goal of injury reduction.
Kansas LEAN, the state coalition mentioned previously, facilitated a
variety of community and system changes aimed at preventing chronic disease through dietary modifications and exercise. The system changes included modifying lunch menus in elementary schools, changing school curricula by adding nutrition education and enhanced exercise activities, supporting the adoption by several employers of a pilot-tested work-site program to lower the intake of dietary fat, working with supermarkets to implement price reductions and shelf prompts for lower-fat foods, and conducting events to promote lean eating in the African-American faith community and among state legislators (Fawcett et al., 1997).
The Healthy Neighborhoods Project (HNP) in western Contra Costa County, California, brought together community residents, the health department, community organizations, and sometimes other partners from the public, private, and civic sectors (Minkler, 2000). Using trained community organizers and neighborhood health advocates, the project conducted a qualitative assessment of the community’s health-related needs and capacities. Data on air quality led to changes in areas such as transportation (Minkler, 2000). Another part of the initiative reached recipients of food stamps with information about food and nutrition. HNP also worked with organizers of a local outdoor festival to ban smoking. The activities to change policies related to smoking built on a history of successes, including local collaboration among nonprofit organizations, the health department, and other groups to implement a strong clean-indoor-air policy as well as a tobacco-free youth policy. Today, the Contra Costa County health department provides a real and virtual (online) community gateway for getting involved with existing health-related coalitions, including HNP (Contra Costa Health Services, 2001).
Bias, prejudice, and stereotyping (IOM, 2002) and a sometimes overt lack of cultural competence (see Box 4–4) characterize many institutional and community health settings. Culturally competent public health services are essential for the success of efforts to improve health and eliminate disparities. Staff members present during the committee’s site visit to Oakland’s Community Voices project considered health care delivery services without cultural competence completely unacceptable, leading to health care encounters that lack basic communication and fail to empower or engage clients in addressing their own health needs (Bayne-Smith, 1996). However, altering discriminatory attitudes and norms, which are sometimes deceptively subtle, and overcoming cultural and linguistic barriers pose significant challenges and require institutional and individual commitments from all entities that are potential partners within the public health system.
Cultural diversity and the knowledge and resources often associated with it are valuable community assets, making communities and systems better equipped to interact appropriately with diverse populations. The
|
BOX 4–4 Working with Communities for Cultural Competence In 1994 the California Cultural Competency Taskforce defined cultural competence as “appropriate and effective communication which requires the willingness to listen to and learn from members of diverse cultures, and the provision of service and information in appropriate languages, at appropriate comprehension and literacy levels, and in the context of an individual’s cultural health beliefs and practices” (Chin, 2000:26). Cultural competence entails the provision of services, training, and promotional materials in the context of an individual’s or a community’s culture and social and historical circumstances and in a range of languages or through interpreters, to whom easy and rapid access is possible (Bayne-Smith, 1996; Chin, 2000). |
Office of Minority Health has developed standards for culturally and linguistically appropriate services in health care to provide guidance and tools for health care providers, policy makers, purchasers, patients and advocates, educators, and accreditation or credentialing entities (DHHS, 2001). Standard 12 recommends that health care organizations use a range of mechanisms to “develop participatory, collaborative partnerships with communities” to facilitate the community’s involvement in the processes that ensure cultural and linguistic competence (DHHS, 2001).
The process of changing community conditions and systems may also require modification of institutional cultures in terms of attitudes and beliefs about sharing power. This may include changes in attitudes about the role of an empowered citizenry vis-à-vis the role of experts, such as professionals who have traditionally occupied positions of authority (Schwab and Syme, 1997; Bowles, 1999). A participant in the committee’s site visit to Healthy New Orleans poignantly summarized an aspect of this tension by asking what it would take before communities could be heard without first having to get the “Ivory Tower Seal of Approval” (personal communication by coalition member to committee members, 2001). Dysfunctional organizational practices may indirectly shape public perceptions and action about health, for example, by discouraging community initiative or by dampening innovation through rigid categorical funding systems.
At the political level, the commitment of elected officials to communitywide health action can have an enormous influence on broadening the impact of a program and increasing the likelihood of sustainability of programs and outcomes. The American Health Decisions network of state organizations has been pioneering new methods of involving the public in community dialogues about health values and trade-off options. The
state of Oregon’s Health Decisions project in the 1980s may be the most visible example of such an effort. Led by the governor, it involved extensive public education and a long series of statewide public hearings, resulting in the Oregon Health Plan setting priorities for public and private health insurance coverage. The states of Georgia and California have initiated Health Decisions projects, and although mostly focused on health care reform, the model illustrates the power of political commitment in helping to mobilize community engagement on health issues (Kari et al., 1994).
Achieving Widespread Change in Behavior and Risk Factors
Changing individual behavior to avoid health-related risk factors is another stage on the road to health improvement. Behavioral change may sometimes be achieved through interventions, such as health education and counseling, that are aimed directly at individuals, although the evidence base shows that a broad array of interventions go beyond the individual and function at an ecological level (e.g., the neighborhood or the workplace). Efforts to change individual risk must consider the influence of community conditions and systems that affect the population in general (see Box 4–5).
The effective way to approach health improvement from a population health perspective has been to focus on a combination of individual and community factors. For example, Callahan (2000:164) observed that “people can and do stop smoking on their own, but it is easier for them if their family members and friends don’t smoke, if they can’t smoke in their workplace, and if the taxes on cigarettes make buying tobacco products exceedingly expensive.” Individual behavior and health risks can be shaped by conditions throughout the community, including the workplace, business practices, and neighborhood resources.
Many communities have been motivated to address tobacco-related issues, such as teen smoking, smoking cessation, and advertising for tobacco products, as exemplified by coalitions formed in Florida, Massachusetts, Minnesota, and Missouri to influence policy and public opinion (Heser and Begay, 1997; Fisher et al., 1998; Givel and Glantz, 2000; Johnson, 2000). In St. Louis, Missouri, Neighbors for a Smoke Free North Side took on smoking cessation (Fisher et al., 1998). The project was implemented in three neighborhoods, with four zip code areas in Kansas City, Missouri, serving as comparators. The interventions included media inputs (interviews and stories), billboards, community events, and other health promotion efforts. Unlike the COMMIT (Community Intervention Trial for Smoking Cessation) randomized controlled trials, which, although well designed, had just one modest and partial positive outcome (Susser, 1995), this project found a significant decline in the prevalence of self-reported smoking after the intervention. It also demonstrated an association between its success
|
BOX 4–5 Ideas for Communities in Action: Obesity Community-based programs are essential to combating the increasing rates of overweight and obesity in the United States (ACS, 2002). These programs should be culturally specific and relevant to the community being targeted because of cultural differences in foods and in perceptions and attitudes about weight and appearance. For example, in some cultures a heavy child may be viewed as being healthy, whereas a thin child may be considered weak or ill. The use of a range of strategies, such as social marketing, health education, and policy change, is essential. In addition to traditional methods that have some limited success—such as education about the value of eating well and being active—communities can engage in other activities that change the environments that enable sedentary lifestyles and poor eating choices. They can facilitate exercise by working with community development and planning agencies to make parks and playing fields safe and accessible. Schools can become sites for accessible and affordable community recreation centers. Communities might also develop relationships with farmers to make fresh fruits and vegetables more readily available and affordable through weekly markets. Recently, the Los Angeles Unified School District discontinued soda vending on all school premises in the district, thus removing an element that has been linked to childhood obesity (Wood, 2002). Community restaurants and grocery stores could offer and advertise healthy food choices. Communities could also engage the media and other partners. The recently launched Hearts N’ Parks program, sponsored by the National Heart, Lung, and Blood Institute and the National Recreation and Park Association, is getting communities interested and mobilized to become physically active by planning a variety of community and educational activities (NIH, 2001). |
and the profound involvement of community members in planning, implementation, and governance of the project (Fisher et al., 1998).
Most community partnerships mentioned in this chapter aimed to change behavior and risk factors for the community as a whole. The activities of Kansas LEAN, for example, focused on modifying the environment to encourage improved dietary choices, such as consumption of foods lower in fat. The coalitions associated with the Healthy New Orleans Turning Point project expressed an understanding of the relationship between health and built environments that are unsafe, unpleasant, or otherwise incompatible with living an active life. They described a vision of improving neighborhoods by adding green spaces to facilitate walking and other activities.
In Contra Costa County, California, observation and statistics indicated that African-American women were less likely to receive breast cancer screening for reasons related to the cost of care and a fear of diagnosis, leading to significantly higher rates of mortality from breast cancer in this
group (Ryan, 2001). Such barriers became an overwhelming factor in shaping the health behaviors of affected women. A collaborative health department–community initiative to improve access to breast cancer screening for African-American women helped promote behavioral change that ultimately closed the early diagnosis gap between African-American and white women.
Part of the difficulty of changing behaviors is related to the tension between historical, social, and cultural concepts of responsibilities and rights, such as the question of personal responsibility for poor health (e.g., in relation to lifestyle). The committee has found a growing recognition of and empirical support for the influence of population-level factors on the health risk and health status of individuals and populations. This is reflected in the determinants of health discussion in Chapter 2. Efforts to change health behavior and address risk factors cannot reach optimal effectiveness if they depend solely on one-on-one health education or health promotion interventions (Economos et al., 2001).
Improving the Population’s Health
Achieving improvement in the health of the public is the final step in the collaborative framework described in this chapter. Depending on the goals of community interventions, these improvements might take the form of lower rates of obesity, reductions in the number of injuries resulting from drunk driving, or fewer cases of sexually transmitted diseases. Sometimes, however, it can be difficult to directly link the desired health outcomes to a community’s health actions. The connecting pathways are frequently long and complex. For example, it takes 20 to 30 years to see lower rates of lung cancer after the percentage of the population that smokes has been reduced. Moreover, the effect of a community’s actions can be obscured by other societal (secular) trends that may either reinforce or counteract the desired change (Paine-Andrews et al., 2000a).
Despite the difficulties inherent in evaluating final outcomes, progress can be measured by monitoring changes in indicators that reflect intermediate outcomes of community actions, such as higher rates of screening for breast cancer (decreasing mortality) or an increase in the number of community recreation facilities (decreasing obesity). Although such indicators may not specifically measure health or health-related activities (Ricketts, 2001), intermediate measures of community and system changes can be associated with subsequent changes in health outcomes (Fawcett et al., 1997). For example, the activities of a coalition-driven substance abuse prevention project in Kansas led to changes in community policies, programs, and practices (e.g., enhanced law enforcement) that were ultimately linked to a decline in single-vehicle crashes at night and related reductions in injuries and deaths.
Observable and measurable changes within communities and the systems that provide services and assure health offer not only intermediate measures of progress and coalition performance but also vital feedback for community members. The Healthy People agendas (Healthy People 2000 and Healthy People 2010), which have been adopted to guide national health policy and which have been embraced by 47 states, play an important role in measuring the health status of the national “community.” An update of progress in meeting Healthy People 2000 goals indicates that of its 319 indicators (organized by 22 health objectives) 15 percent met the goals, 44 percent are making progress in the correct direction, 18 percent are moving away from the specified target, 9 percent have mixed results, and the progress for the remaining indicators cannot be measured at this time (NCHS, 1999).
EVALUATING AND RESEARCHING COMMUNITY HEALTH IMPROVEMENT
Communities interface with the research community in a variety of ways. Sometimes, community organizations collaborate with academic institutions to conduct needs assessments or monitor and evaluate program effectiveness. In other cases, academic researchers study communities to build an evidence base on the ways in which communities work and what works in communities. In more recent cases, community-based participatory research (see Chapter 8) has come to be a valued area of public health research, and partnerships among community groups and organizations and public health researchers and practitioners have become more common and fruitful (Israel et al., 1998).
The committee agrees with those who argue that communities and community members must, for both practical and ethical reasons, be partners in health improvement interventions and in the research that guides these interventions (Green and Kreuter, 1991; Kretzmann and McKnight, 1993; Blackwell and Colmenar, 2000; Potvin and Richard, 2001; Norton et al., 2002). On a practical level, engaging the community in public health research may help with complicated (and often sensitive) issues such as defining research priorities or interpreting results (Israel et al., 1998). Ethically, it is important to involve the community that is being studied— informed individual consent does not seem sufficient when interventions involve the needs, aspirations, and even the future of communities.
A significant amount of public health research has been conceived and conducted from its inception and at every stage of implementation without the involvement of the community or population most affected. This approach has contributed to community distrust of academic researchers and their projects. Additionally, research undertaken without the involvement
|
BOX 4–6 Community Perspectives on Research A qualitative study by public health researchers and community members in Seattle, Washington, uncovered mostly negative community perceptions of the research conducted in their communities. Respondents noted a power imbalance between researchers and community members and described researchers as focused solely on community needs and things to be fixed. They also expressed a lack of trust in their relationship with researchers and a perception that researchers did not respect the community and were impatient for results (Sullivan et al., 2001:137). There is “so much rhetoric around this whole issue of community-based [research], it takes an enormous amount of investment of time and energy and expertise and skill and patience in getting the foundation laid properly. . . . [Y]ou spend . . . three or four years, and a lot of funding institutions would probably go faint at that, but it really does take that kind of effort” (Sullivan et al., 2001:139). |
of those most affected not only may make it more difficult to develop and implement effective interventions for improvements in the health of the community but may also raise ethical questions (see Box 4–6). Furthermore, research has typically adhered to a scientific paradigm of objectivity and “universal” truth, whereas the issues, dynamics, and stories of communities are generally local, subjective, and unique (Schwab and Syme, 1997). This tension between the nature of the community and the nature of science may help explain why researching the effectiveness of community coalitions and community intervention has been a complicated endeavor and why investment in community-based research has been limited.
Community-based participatory research seeks to overcome some of the criticisms and distrust of academic research by emphasizing the participation and influence of nonacademic researchers in the process of creating knowledge (Israel et al., 1998). However, community members are frequently skeptical that proposed research efforts will be truly collaborative in nature. The promise of community-based participatory research brings with it the need to establish true partnerships with equal decision-making authority, mutual benefit, and shared responsibility. Major issues that must be confronted in such research include power and control, conflicts over funding, and who will be recognized as the community representative. Additionally, according to Israel and colleagues (1998), “emphasis needs to be placed on developing norms and ways of operating that promote understanding and demonstrate sensitivity and competence in working with diverse cultures.” All of these factors lead to the need for a well-developed review of ethical issues involved in community-based research and an ongo-
ing discussion of how to ensure that such research is conducted with the highest regard for those who participate. The committee believes that discussion and debate about the ethics of community-based research are necessary and that creating a forum for such dialogue is important.
Because the community is a complex and dynamic subject, the committee agrees with those who assert that entirely new paradigms of research and analysis must be developed, along with a “postmodern epidemiology” or a “participatory eco-epidemiology” that does not sacrifice rigor but that shares power and involves all local perspectives and opinions (Schwab and Syme, 1997). Collaborative public health research that engages the community at every possible level may mean that research will be applicable and useful to them (Israel et al., 1998; Sullivan et al., 2001). Furthermore, the expertise of local community members and groups would constitute a valuable addition to a research project’s assets (Omenn, 1999; Schwab and Syme, 1997).
A social marketing project to improve the health of agricultural workers in Florida provides an example of a fruitful partnership in community-based research (Flocks et al., 2001). Florida nursery and fernery workers, who are primarily Hispanic and Haitian, are exposed through their work to a large volume of pesticides known to be harmful to humans. In 1997, health researchers from the University of Florida entered into a partnership with a union, the Farmworker Association of Florida, and a social marketing firm for a project to help expand existing educational efforts and focus them into an effective, wide-scale intervention. Fernery employees participated at all stages of the research, contributing valuable cultural and occupational insights and information. The process has been lengthy and challenging because of the varied interests of the parties involved (workers, unions, health care providers, industry, academia, government agencies), but the initial work has begun to pay off. More funding has been secured, additional research has been launched, and work has begun on social marketing interventions to change employer practices and worker behaviors and on efforts to address barriers to adequate health care for this vulnerable population of workers exposed to environmental hazards (Flocks et al., 2001; L. Clarke, personal communication, April 9, 2002).
Additional discussion of issues in community-based research and the benefits of academic collaboration with communities appears in Chapter 8, which focuses on the role of academia in the public health system.
SUSTAINING COMMUNITY ACTION ON HEALTH
Assuring the health of communities requires continuous community participation and leadership in the context of a broader partnership with other potential actors in a public health system. Communities can work
with health departments, hospitals and other health care providers, and the corporate sector and employers. Communities can also develop the expertise and linkages needed to attract media attention to their efforts and messages.
Although specific programs may end once concrete objectives are achieved, communities and their populations are continually changing, as are their health status and the factors influencing their health. The cross-linkages that are created within communities from the pursuit of one health goal should be sustained and expanded or modified to respond to other persistent or emerging needs.
Under what circumstances are health improvement efforts most likely to continue? Institutional and community memories are replete with examples of community initiatives that came and left without much effect, projects that accomplished little, and great collective disappointments about squandered promises and resources (Mitchell and Shortell, 2000; Lasker et al., 2001). It is important to recognize that opposition and conflict are definite possibilities and to appreciate that small wins along the way in terms of program goals can be important in sustaining interest and commitment (Fawcett, 1999). Success appears to be the result of a synergistic blending of community capacity with the capacity of governmental public health agencies and other partners (NACCHO, 2000a; Becnel, 2001; Lasker et al., 2001; McHugh et al., 2001).
Capacity describes the mix of conditions (e.g., shared values, quality of programs and strategies, program congruence with community needs, and political support) and resources (e.g., knowledge, skills, money, time, and technical assistance) necessary for communities and community coalitions to accomplish and sustain change (Blackwell and Colmenar, 2000; Chaskin et al., 2001; Foster-Fishman et al., 2001; Norton et al., 2002). For example, a community can develop capacity by expanding its knowledge about best practices for organizing coalitions, planning programs, or conducting advocacy. Additionally, governmental public health agencies are increasingly aware of the need to build their own capacity by enhancing their ability to provide technical assistance, training, and support to build capable communities (Howat et al., 2001; Norton et al., 2002). Local health department staff generally possess the knowledge and resources needed in the community’s efforts to assess local health status, assets, and needs and to evaluate the outcomes of health initiatives. The fact that communities may rely on health departments to provide technical assistance underscores the need to enhance the skills and knowledge of the public health workforce (discussed in greater detail in the Chapter 8). The committee recommends that local governmental public health agencies support community-led efforts to inventory resources, assess needs, formulate collaborative responses, and evaluate outcomes for community health improvement and the elimi-
nation of health disparities. Governmental public health agencies should provide community organizations and coalitions with technical assistance and support in identifying and securing resources as needed and at all phases of the process.
The sustainability of health improvement efforts is reflected in the extent of community change and the degree to which initiatives remain in place after funding ends (Paine-Andrews et al., 2000b). A study of six community initiatives, three for teen pregnancy and three for substance abuse prevention, found that after the end of a 5-year grant period, at least a quarter of the activities initiated in each of the six projects were continuing. These activities included mentoring programs and an annual youth job fair, as well as alternative activities (Paine-Andrews et al., 2000b). Among the strategies for sustainability of initiatives identified by the study were grant writing, making a business plan, and integrating programs or individual program components into the regularly budgeted activities of a partner agency (Paine-Andrews et al., 2000b).
Governmental and private-sector funders can play an essential role in supporting the sustainability of changes in a community’s conditions for health. Funders can encourage communities to develop clear goals and to follow practices proven to be effective (W. K. Kellogg Foundation, 1997; Wickizer et al., 1998) (see Box 4–7).
For example, funders can require or support the adoption of specific program elements, such as the development of a business plan, and they can
|
BOX 4–7 Lessons from Turning Point A review of the Turning Point initiative identified five key lessons for public health policy:
SOURCE: Baxter (2001). |
encourage linkages with key local partners, including health departments (Fawcett et al., 2000c; NACCHO, 2000a; Paine-Andrews et al., 2000b; Brunner, 2001). Communicating or even partnering with local health departments may help prevent duplication of effort and may help coordinate activities with multiple participants. In addition, funders must realize that significant community change projects require long-term support and, often, active assistance in identifying continuing sources of financing when the initial grants expire. Because of the time lag between initiation of a community-level intervention and measurable health results, short-term “demonstration project” models are rarely effective and may increase community cynicism about outside partners. The committee recommends that governmental and private-sector funders of community health initiatives plan their investments with a focus on long-lasting change. Such a focus would include realistic time lines, an emphasis on ongoing community engagement and leadership, and a final goal of institutionalizing effective project components in the local community or public health system as appropriate.
Given the ever-changing nature of communities, health improvement efforts should be seen as a continuing journey rather than a specific destination.
CONCLUDING OBSERVATIONS
Communities and community organizations can be vital contributors to the resources and capacity of a public health system. A community’s right to self-determination, its knowledge of local needs and circumstances, and its human, social, and cultural assets, including the linkages among individuals, businesses, congregations, civic groups, schools, and innumerable others, are all important motivations for community health action. In cases in which community health promotion and protection activities are initiated by a health department or an organization, engaging the community is a primary responsibility. Realizing the vision of healthy people in healthy communities is possible only if the community, in its full cultural, social, and economic diversity, is an authentic partner in changing the conditions for health.
REFERENCES
ACS (American Cancer Society). 2002. American communities can change lifestyle habits to prevent cancer. Available online at http://www.cancer.org/docroot/nws/content/nws_1_1x_american_communities_can_change_lifestyle_habits_to_prevent_cancer.asp. Accessed March 6, 2003.
ATSDR (Agency for Toxic Substances and Disease Registry). 2000. Geographic information systems in public health: proceedings of the third national conference. Available online at www.atsdr.cdc.gov/gis/conference98/index.html. Accessed October 30, 2002.
Baxter RJ. 2001. What Turning Point tells us: implications for national policy. Prepared by The Lewin Group for the W. K. Kellogg Foundation on June 27, 2001. Available online at www.wkkf.org/pubs/Health/TurningPoint/Pub722.pdf. Accessed April 9, 2002.
Bayne-Smith M (Ed.). 1996. Race, Gender, and Health. Thousand Oaks, CA: Sage Publications.
Becnel B. 2001. Community-based public health: lessons on power, policy and grassroots leadership. Community-Based Public Health Policy & Practice, Issue No. 2. A policy brief of Partnership for the Public’s Health. Available online at http://www.partnershipph.org/documents/policy/pp1.pdf. Accessed December 18, 2001.
Blackwell AG, Colmenar R. 2000. Community-building: from local wisdom to public policy. Public Health Reports 115(2&3):161–166.
Bowles S. 1999. “Social capital” and community governance. Focus 20(3):6–10.
Bracho A. 2000. An institute of community participation. Adelaide, Australia: Dulwich Centre Publications. Available online at http://www.dulwichcentre.com.au/. Accessed May 2, 2002.
Brunner W. 2001. Community-based public health: a model for local success. Community-Based Public Health Policy and Practice, Issue No. 2. Available online at http://ccpublichealth.org/PDFs/PP1.PDF. Accessed October 31, 2002.
Butterfoss F, Cashman S, Foster-Fishman P, Kegler M, Berkowitz B. 2001. Roundtable discussion and final comments. American Journal of Community Psychology 29(2):229–239.
Callahan D (Ed.). 2000. Promoting Health Behavior: How Much Freedom? Whose Responsiblity? Washington, DC: Georgetown University Press.
CCNTR (Caring Community Network of the Twin Rivers). 2001. Caring Community Network of the Twin Rivers. Available online at www.ccntr.org. Accessed April 7, 2002.
CDC (Centers for Disease Control and Prevention). 1997. Principles of community engagement. CDC/ATSDR Committee on Community Engagement. Atlanta, GA: CDC.
CDC. 2001. National Public Health Performance Standards Program. Available online at www.phppo.cdc.gov/dphs/nphpsp. Accessed October 30, 2001.
CDC. 2002. Syndemics overview: what procedures are available for planning and evaluating initiatives to prevent syndemics? The National Center for Chronic Disease Prevention and Health Promotion Syndemics Prevention Network. Available online at www.cdc.gov/syndemics/overview-planeval.htm. Accessed April 7, 2002.
Chaskin RJ, Brown P, Venkatesh S, Vidal A. 2001. Building Community Capacity. New York: Aldine de Gruyter.
Cheadle A, Sterling TD, Schmid TL, Fawcett SB. 2000. Promising community-level indicators for evaluating cardiovascular health-promotion programs. Health Education Research 15(1):109–116.
Chin JL. 2000. Culturally competent health care. Public Health Reports 115(1):25–33.
Contra Costa Health Services. 2001. The Spectrum of Prevention. Available online at http://ccprevention.org/specrtum.html#top. Accessed April 2, 2002.
Corrigan PW, Penn DL. 1999. Lessons from social psychology on discrediting psychiatric stigma. American Psychologist 54(9):765–776.
Corrigan PW, Green A, Lundin R, Kubiak MA, Penn DL. 2001. Familiarity with and social distance from people who have serious mental illness. Psychiatric Services 52(7):953–958.
DHHS (Department of Health and Human Services). 1999. Engaging faith communities as partners in improving community health. Highlights from a forum sponsored by the CDC/ ATSDR and the Carter Center Interfaith Program. Available online at www.phppo.cdc.gov/documents/faithhealth.pdf. Accessed November 14, 2001.
DHHS. 2001. National standards for culturally and linguistically appropriate services in health care. Prepared for the Office of Minority Health. Available online at www.omhrc.gov/clas. Accessed February 25, 2002.
Economos CD, Brownson RC, DeAngelis MA, Foerster SB, Foreman CT, Tucker C, Gregson J, Kumanyika SK, Pate RR. 2001. What lessons have been learned from other attempts to guide social change? Nutrition Reviews 59(3):S40–S56.
Fawcett SB. 1999. Some lessons on community organization and change. In Rothman J (Ed.). Reflections on Community Organization: Enduring Themes and Critical Issues. Itasca, IL: F. E. Peacock Publishers.
Fawcett SB, Paine-Andrews A, Francisco VT, Schultz JA, Richter KP, Lewis RK, Harris KJ, Williams EL, Berkley JY, Lopez CM, Fisher JL. 1996. Empowering community health initiatives through evaluation, pp. 161–187. In Fetterman DM, Kafterian SJ, Wandersman A (Eds.). Empowerment Evaluation: Knowledge and Tools for Self-Assessment and Accountability. Thousand Oaks, CA: Sage Publications.
Fawcett SB, Lewis RK, Paine-Andrews A, Francisco VT, Richter KP, Williams EL, Copple B. 1997. Evaluating community coalitions for prevention of substance abuse: the case of Project Freedom. Health Education & Behavior 24(6):812–828.
Fawcett SB, Francisco VT, Schultz JA, Berkowitz B, Wolff TJ, Nagy G. 2000a. The Community Tool Box: a web-based resource for building healthier communities. Public Health Reports 115(2&3):274–278.
Fawcett SB, Francisco VT, Hyra D, Paine-Andrews A, Schultz, Roussos S, Fisher JL, Evensen P. 2000b. Building healthy communities. In Tarlov AR, St. Peter RF (Eds.). The Society and Population Health Reader: A State and Community Perspective. New York: The New Press.
Fawcett SB, Francisco VT, Paine-Andrews A, Schultz JA. 2000c. A model memorandum of collaboration: a proposal. Public Health Reports 115(2&3):174–179.
Fisher EB, Auslander WF, Munro JF, Arfken CL, Brownson RC, Owens NW. 1998. Neighbors for a Smoke Free North Side: evaluation of a community organization approach to promoting smoking cessation among African Americans. American Journal of Public Health 88(11):1658–1663.
Flocks J, Clarke L, Albrecht S, Bryant C, Monaghan P, Baker H. 2001. Implementing a community-based special marketing project to improve agricultural worker health. Environmental Health Perspectives 109(Suppl. 3):461–468.
Foster-Fishman PG, Berkowitz SL, Lounsbury DW, Jacobson S, Allen NA. 2001. Building collaborative capacity in community coalitions: a review and integrative framework. American Journal of Community Psychology 29(2):241–261.
Givel MS, Glantz SA. 2000. Failure to defend a successful state tobacco control program: policy lessons from Florida. American Journal of Public Health 90(5):762–767.
Goodman RM, Wandersman A, Chinman M, Imm P, Morrisey E. 1996. An ecological assessment of community based interventions for prevention and health promotion: approaches to measuring community coalitions. American Journal of Community Psychology 24(11):33–61.
Green L, Daniel M, Novick L. 2001. Partnerships and coalitions for community-based research. Public Health Reports 116(Suppl. 1):20–31.
Green LW, Kreuter MM. 1991. Health Promotion Planning: An Educational and Environmental Approach, 2nd ed. Mountain View, CA: Mayfield Publishing Company.
Group Health Community Foundation (GHCF). 2001. Improving everyone’s quality of life: a primer on population health. Prepared for California Wellness Foundation’s Health Improvement Initiative. Seattle: Group Health Community Foundation.
Health Action. 2001. Health Action priorities for Monroe County. Available online at www.healthaction.org/. Accessed April 2, 2002.
Healthy New Orleans. 2001. Community Public Health System Improvement Plan. Prepared January 2001 as part of the implementation of a Turning Point grant. New Orleans, LA: Healthy New Orleans.
Heser PF, Begay ME. 1997. The campaign to raise the tobacco tax in Massachusetts. American Journal of Public Health 87(6):968–973.
Himmelman AT. 2001. On coalitions and the transformation of power relations: collaborative betterment and collaborative empowerment. American Journal of Community Psychology 29(2):277–284.
Himmelman AT, Johnson D, Kaye G, Salzman P, Wolff T. 2001. Roundtable discussion and final comments. American Journal of Community Psychology 29(2):205–211.
Holder HD, Grenewald PJ, Ponicki WR, Treno AJ, Grube JW, Saltz RF, Voas RB, Reynolds R, Davis J, Sanchez L, Gaumont G, Roeper P. 2001. Effect of community-based interventions on high-risk drinking and alcohol-related injuries. Journal of the American Medical Association 284(18):2341–2347.
Howat P, Cross D, Hall M, Iredell H, Stevenson M, Gibbs S, Officer J, Dillon J. 2001. Community participation in road safety: barriers and enablers. Journal of Community Health 26(4):257–270.
HRSA (Health Resources Services Administration). 2001. Fact sheet: HRSA’s Border Health Program. Available online at http://newsroom.hrsa.gov/factsheets/borderhealth2001.htm. Accessed April 5, 2002.
IOM (Institute of Medicine). 1988. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 1995. Assessing the Social and Behavioral Science Base for HIV/AIDS Prevention and Intervention: Workshop Summary and Background Papers . Washington, DC: National Academy Press.
IOM. 1996a. Healthy Communities: New Partnerships for the Future of Public Health. Washington, DC: National Academy Press.
IOM. 1996b. Using Performance Monitoring to Improve Community Health: Exploring the Issues. Washington, DC: National Academy Press.
IOM. 1997. Improving Health in the Community: A Role for Performance Monitoring. Washington, DC: National Academy Press.
IOM. 2001. Health and Behavior: The Interplay of Biological, Behavioral, and Societal Influences. Washington, DC: National Academy Press.
Israel BA, Schulz AJ, Parker EA, Becker AB. 1998. Review of community-based research: assessing partnership approaches to improve public health. Annual Review of Public Health 19:173–202.
Jewkes R, Murcott A. 1996. Meanings of community. Social Science and Medicine 43:555– 563.
Johnson DS. 2000. Minnesota Decides: a community blueprint for tobacco reduction. Tobacco Control 9(Suppl. 1):65–67.
Johnston JA, Marmet PF, Coen FS, Fawcett SB, Harris KJ. 1996. Kansas LEAN: an effective coalition for nutrition education and dietary change. Wichita, KS: Society for Nutrition Education.
Kari N, Boyte HC, Jennings B. 1994. Health as a civic question. Prepared for the American Civic Forum. Available online at www.cpn.org/sections/topics/health/. Accessed September 23, 2002.
Kegeles SM, Hart GJ. 1998. Recent HIV-prevention interventions for gay men: individual, small-group and community-based studies. AIDS 12(Suppl. A):S209–S215.
Kickbusch, I. 1989. Good planets are hard to find. WHO–EURO, Healthy Cities Papers, No. 5. Copenhagen: World Health Organization.
Kretzmann JP, McKnight JL. 1993. Building Communities from the Inside Out: A Path Toward Finding and Mobilizing a Community’s Assets. Evanston, IL: Institute for Policy Research.
Kreuter MW. 1992. PATCH: its origin, basic concepts, and links to contemporary public health policy. Journal of Health Education 23(3):135–139.
Kreuter MW, Sabol BJ, O’Donovan A, Donovan J, Klein L, Green LW, Vliet M, Bradley T, Campuzano MK, Tarlov AR. 2000. Commentaries from grantmakers on Fawcett et al.’s proposed memorandum of collaboration. Public Health Reports 115:180–190.
Kreuter MW, Lezin NA, Young L, Koplan AN. 2001. Social capital: evaluation implications for community health promotion. In Rootman I, Goodstadt M, Hyndman B, McQueen DV, Potvin L, Springett J, Ziglio E (Eds.). 2001. Evaluation in Health Promotion: Principles and Perspectives, WHO Regional Publications, European Series, No. 92. Copenhagen: World Health Organization.
Lasker RD, Weiss ES, Miller R. 2001. Partnership synergy: a practical framework for studying and strengthening the collaborative advantage. The Milbank Quarterly 79(2):179–205.
The Lewin Group. 2002. Community participation can improve America’s public health systems. Prepared for the W. K. Kellogg Foundation. Falls Church, VA: The Lewin Group.
Link BG, Phelan JC, Bresnahan M, Stueve A, Pescosolido BA. 1999. Public conceptions of mental illness: labels, causes, dangerousness, and social distance. American Journal of Public Health 89(9):1328–1333.
Lundblad JA. 1999. Finding our place at the table. Lutheran Partners. Available online at www.elca.org/lp/finding.html. Accessed September 12, 2002.
McGinnis JM, Foege WH. 1993. Actual causes of death in the United States. Journal of the American Medical Association 270(18):2207–2212.
McHugh M, Martinez RM, Kliman R, Roschwalb S. 2001. Health departments forge stronger partnerships. Mathematica Policy Research Inc., Issue Brief No. 5, page 1. Available online at http://www.mathematica-mpr.com/PDFs/PHIssueBr5.pdf. Accessed October 31, 2002.
Milbank Memorial Fund. 1998. Partners in community health: working together for a healthy New York 1998. Prepared by the Milbank Memorial Fund in collaboration with the New York State Community Health Partnership. Available online at www.milbank.org/nypartners/foreword.html. Accessed March 5, 2001.
Minkler M. 2000. Using participatory action research to build health communities. Public Health Reports 115(2&3):191–197.
Mitchell SM, Shortell SM. 2000. The governance and management of effective community health partnerships: a typology for research, policy, and practice. The Milbank Quarterly 78(2):241–289.
NACCHO (National Association of County and City Health Officials) and Centers for Disease Control and Prevention . 1995. 1992–1993 National profile of local health departments. Atlanta, GA: Centers for Disease Control and Prevention.
NACCHO. 2000a. Community revitalization and public health: issues, roles and relationships for local public health agencies. Supported through a cooperative agreement with the Agency for Toxic Substances and Disease Registry, U.S. Public Health Service. Washington, DC: NACCHO.
NACCHO. 2000b. Mobilizing for Action through Planning and Partnerships (MAPP). Available online at http://mapp.naccho.org/lphsa/index.asp. Accessed February 25, 2002.
National Association of Local Boards of Health. 2002. Local Public Health Governance Performance Assessment Instrument. Final version OMB3.0. Bowling Green, OH: National Association of Local Boards of Health. Available online at http://www.nalboh.org/perfstds/perfstds.htm. Accessed June 14, 2002.
NCHS (National Center for Health Statistics). 1999. Healthy People 2000 Review, 1998– 1999. Hyatsville, MD: Public Health Service. Available online at www.cdc.gov/nchs/data/hp2000/hp2k99.pdf. Accessed October 30, 2002.
NIH (National Institutes of Health). 2001. Hearts N’Parks: Community Mobilization Guide. A project of the National Heart, Lung and Blood Institute and the National Recreation and Park Association. NIH Publication 01–1655. Rockville, MD: National Institutes of Health.
Norris T, Pittman M. 2000. The Healthy Communities movement and the Coalition for Healthier Cities and Communities. Public Health Reports 115(2&3):118–124.
Norton BL, Burdine JN, LeRoy KR, Felix MRJ, Dorsey AM. 2002. Community capacity: theoretical roots and conceptual challenges. In DiClemente R, Crosby R, Kegler M (Eds.). Emerging Theories in Health Promotion Practice and Research. Hoboken, New Jersey: Jossey-Bass Wiley Publishers.
Omenn GS. 1999. Caring for the community: the role of partnerships. Academic Medicine 74(7):782–789.
Paine-Andrews A, Fisher JL, Campuzano, Fawcett SB, Berkeley-Patton J. 2000a. Promoting sustainability of community health initiatives: an empirical case study. Health Promotion Practice 1(3):248–258.
Paine-Andrews A, Fisher JL, Harris KJ, Lewis RK, Williams EL, Vincent ML, Fawcett SB, Campuzano MK. 2000b. Some experiential lessons in supporting and evaluating community-based initiatives for preventing adolescent pregnancy. Health Promotion Practice 1(1):66–76.
Paine-Andrews A, Fisher JL, Patton JB, Fawcett SB, Williams EL, Lewis RK, Harris KJ. 2002. Analyzing the contribution of community change to population health outcomes in an adolescent pregnancy prevention initiative. Health Education and Behavior 29(2):183– 193.
PHF (Public Health Foundation). 2000. EZ/EC Health Planning Capacity Survey: Final Report. Washington, DC: Assistant Secretary for Planning and Evaluation, Department of Health and Human Services.
Potvin L, Richard L. 2001. Evaluating community health promotion programmes. In Rootman I, Goodstadt M, Hyndman B, McQueen DV, Potvin L, Springett J, Ziglio E (Eds.). Evaluation in Health Promotion: Principles and Perspectives. WHO Regional Publications, European Series, No. 92. Copenhagen: World Health Organization. Available online at www.who.dk/docpub/documents/hltprom.htm. Accessed October 5, 2001.
Pronk NP, O’Connor PJ. 1997. Systems approach to population health improvement. Journal of Ambulatory Care Management 20(4):24–31.
Ramos IN, May M, Ramos KS. 2001. Environmental health training of promotoras in colonias along the Texas-Mexico border. American Journal of Public Health 91(4):568–570.
Reger B, Wootan MG, Booth-Butterfield S. 2000. A comparison of different approaches to promote community-wide dietary change . American Journal of Preventive Medicine 18(4):271–275.
Rhein M, Lafronza V, Bhandari E, Hawes J, Hofrichter R, Burke N, Skinner I (Eds.). 2001. Advancing Community Public Health Systems in the 21st Century: Emerging Strategies and Innovations from the Turning Point Experience. Washington, DC: National Association of County and City Health Officials.
Ricketts TC. 2001. Community capacity to improve population health: defining community. Draft report. Princeton, NJ: Robert Wood Johnson Foundation.
Robinson K, Elliott SJ. 2000. The practice of community development approaches in heart health promotion. Health Education Research 15(2):219–231.
Rootman I, Goodstadt M, Hyndman B, McQueen DV, Potvin L, Springett J, Ziglio E (Eds.). 2001. Evaluation in Health Promotion: Principles and Perspectives. WHO Regional Publications, European Series, No. 92. Copenhagen: World Health Organization.
Rose G. 1992. The Strategy of Preventive Medicine. Oxford: Oxford University Press.
Rothman J (Ed.). 1999. Reflections on Community Organization: Enduring Themes and Critical Issues. Itasca, IL: F. E. Peacock Publishers.
Roussos ST, Fawcett SB. 2000. A review of collaborative partnerships as a strategy for improving community health. Annual Review of Public Health 21:369–402.
Ruderman M. 2000. Resource guide to concepts and methods for community-based and collaborative problem-solving. Women’s and Children’s Health Policy Center, Johns Hopkins University School of Public Health. Available online at www.med.jhu.edu/wchpc/pub/resrcgd.PDF. Accessed November 6, 2001.
Ryan J. 2001. The power of ordinary people. Community-Based Public Health Policy and Practice, Partnership for the Public’s Health, Issue No. 1. Available online at www.partnershipph.org/col4/policy/pp1.pdf. Accessed September 12, 2002.
Salamon LM, Anheier HK, List R, Toepler S, Wojciech Sokolowski S, and Associates. 1999. Global Civil Society: Dimensions of the Nonprofit Sector. Baltimore, MD: Johns Hopkins Comparative Nonprofit Sector Project.
Schwab M, Syme SL. 1997. On paradigms, community participation, and the future of public health. American Journal of Public Health 87(12):2049–2051.
Sharpe PA, Greaney ML, Lee PR, Royce SW. 2000. Assets-oriented community assessment. Public Health Reports 115(2&3):205–211.
Shortell SM. 2000. Community health improvement approaches: accounting for the relative lack of impact. Health Services Research 35(3):555–560.
Steele J. 2000. Leading the way with community health partnerships. Healthcare Executive, Sept. /Oct.:20–25.
Stewart E, Weinstein RS. 1997. Volunteer participation in context: motivations and political efficacy within three AIDS organizations. American Journal of Community Psychology 25(6):809–837.
Sullivan M, A Kone, KD Senturia, NJ Chrisman, SJ Ciske, JW Krieger. 2001. Researcher and researched-community perspectives: toward bridging the gap. Health Education and Behavior 28(2):130–149.
Susser M. 1995. The tribulations of trials–interventions in communities. American Journal of Public Health 85(2):156–158.
Task Force on Community Preventive Services. 2000. The guide to community preventive services. Available online at www.thecommunityguide.org/home_f.html. Accessed September 30, 2002.
Turning Point Community Health Governance Workgroup. 2001a. Strengthening and sustaining engagement in community health governance. Background paper prepared for the June 2001 Meeting of the Turning Point Community Health Governance Workgroup, Center for the Advancement of Collaborative Strategies in Health, New York Academy of Medicine. Available online at www.cacsh.org/pdf/EngagementTA.pdf. Accessed January 21, 2002.
Turning Point Community Health Governance Workgroup. 2001b. Using organizational formalization to achieve objectives of public health governance. Background paper prepared for the June 2001 Meeting of the Turning Point Community Health Governance Workgroup, Center for the Advancement of Collaborative Strategies in Health, New York Academy of Medicine. Available online at www.cacsh.org/pdf/orgta.pdf. Accessed January 21, 2002.
University of Arizona. 1998. The National Community Health Advisor Study: Weaving the Future. Final Report. Tucson, AZ: University of Arizona.
WHO (World Health Organization). 1998. Health for All in the 21st Century. Geneva: World Health Organization.
Wickizer TM, Wagner E, Cheadle A, Pearson D, Beery W, Maeser J, Psaty B, VonKorff M, Koepsell T, Diehr P, Perrin EB. 1998. Implementation of the Henry J. Kaiser Family Foundation’s Community Health Promotion Grant Program: a process evaluation. The Milbank Quarterly 76(1):121–147.
Wilcox R, Knapp A. 2000. Building communities that create health. Focus on Healthy Communities. Public Health Reports 115(2&3):139–143.
Williams RL, Yanoshik K. 2001. Can you do a community assessment without talking to the community? Journal of Community Health 26(4):233–247.
W. K. Kellogg Foundation. 1997. Sustaining community-based initiatives, Module 1: developing community capacity. An initiative of the W. K. Kellogg Foundation in partnership with the Healthcare Forum. Available online at www.wkkf.org/pubs/Health/Pub656.pdf. Accessed on February 15, 2001.
W. K. Kellogg Foundation. 2001. Community care network. Available online at www.wkkf.org. Accessed November 7, 2001.
Wolff T. 2001a. The future of community coalition building. American Journal of Community Psychology 29(2):263–268.
Wolff T. 2001b. Community coalition building—contemporary practice and research: introduction. American Journal of Community Psychology 29(2):165–172.
Wolkow KE, Ferguson HB. 2001. Community factors in the development of resiliency: considerations and future directions. Community Mental Health Journal 37(6):489–498.
Wood D. 2002. A farewell to fizz from LA lunchrooms. The Christian Science Monitor, August 30, 2002, p. 1.
Yanek LR, Becker DM, Moy TF, Gittelsohn J, Koffman DM. 2001. Project Joy: faith-based cardiovascular health promotion for African American women. Public Health Reports 116(Suppl. 1):68–81.


































