The Patient Protection and Affordable Care Act (ACA) authorized the largest expansion of health insurance coverage since the development of Medicare and Medicaid. As a result, by 2016, an estimated 30 million individuals, who would otherwise have been uninsured, are expected to obtain insurance through the private health insurance market or state expansion of Medicaid programs. To ensure a consistent level of benefits, the ACA calls for certain types of private and public insurance to incorporate a federally determined essential health benefits (EHB) package. The ACA gives the Secretary of the U.S. Department of Health and Human Services (HHS) sole authority to define the EHB.
HHS asked the Institute of Medicine (IOM) to recommend a process by which the Secretary could define and subsequently update the EHB. As part of its work, the committee sought the views of many experts and stakeholders. Presentations from the committee’s two public workshops are available as a separate publication, Perspectives on Essential Health Benefits: Workshop Report.1 Additionally, 10 questions were posted on the IOM website for 6 months to obtain wider public input. The committee developed its recommendations from this information, additional research, and its own deliberations.
WHO IS COVERED BY THE ESSENTIAL HEALTH BENEFITS?
Guidance by the Secretary on the definition of essential health benefits will determine the minimum benefit package that must be offered to individuals and small employers purchasing insurance, and by certain Medicaid expansion plans known as benchmark or benchmark-equivalent plans and state basic insurance plans. More than 68 million people are estimated to obtain insurance that must meet the EHB requirements (Eibner et al., 2010).
MULTIPLE POLICY FOUNDATIONS WERE INTEGRATED TO
FRAME THE PROCESS FOR DEVELOPING THE EHB
The Secretary of HHS asked the IOM committee to develop an explicit framework for developing the EHB package that would serve HHS now and in the future (Glied, 2011). Finding that no single policy foundation was
1 The workshop report can be accessed at http://www.iom.edu/EHBperspectives.
sufficient, the committee integrated perspectives from economics, ethics, evidence-based practice, and population health (Figure S-1) to create an overarching framework (Chapter 3).
EXPLICIT CRITERIA WERE DEVELOPED TO GUIDE THE OVERALL PACKAGE,
CHOICES OF COMPONENTS, AND THE METHODS FOR UPDATING
The committee used the integrated policy foundations to develop criteria that could guide decisions about the EHB, as the Secretary of HHS requested. As shown in Figure S-2, the committee developed criteria to guide the EHB content in the aggregate and on specific elements. The committee recognized that the process by which the EHB are initially defined and updated is critical to establishing trust in the results. The committee’s recommended criteria to guide the processes for establishing and updating the EHB are shown in Figure S-2.
A MULTI-STEP PROCESS IS RECOMMENDED FOR DEVELOPING THE INITIAL EHB
As background, the report reviews the relationships between the benefits that are eligible for coverage, the design of covered benefits, and how benefits are administered, and then discusses various approaches that have been taken by states and private insurers regarding each of these aspects of insurance (Chapter 2). The report also reviews how some of the conflicting or ambiguous issues in the ACA were interpreted by the committee to provide a common understanding from which to develop its recommendations (Chapter 4).
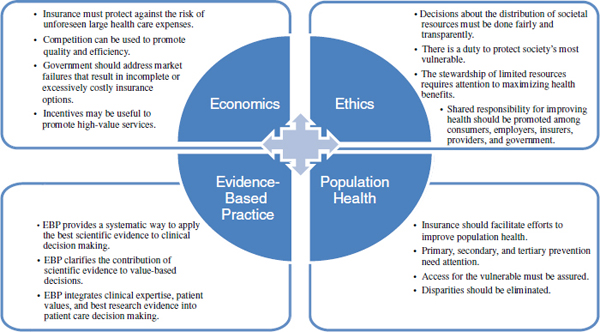
NOTE: EBP = evidence-based practice.
Criteria to Guide Content of the Aggregate EHB Package
In the aggregate, the EHB must:
• Be affordable for consumers, employers, and taxpayers.
• Maximize the number of people with insurance coverage.
• Protect the most vulnerable by addressing the particular needs of those patients and populations.
• Encourage better care practices by promoting the right care to the right patient in the right setting at the right time.
• Advance stewardship of resources by focusing on high value services and reducing use of low value services. Value is defined as outcomes relative to cost.
• Address the medical concerns of greatest importance to enrollees in EHB-related plans, as identified through a public deliberative process.
• Protect against the greatest financial risks due to catastrophic events or illnesses.
Criteria to Guide EHB Content on Specific Components
The individual service, device, or drug for the EHB must:
• Be safe—expected benefits should be greater than expected harms.
• Be medically effective and supported by a sufficient evidence base, or in the absence of evidence on effectiveness, a credible standard of care is used.
• Demonstrate meaningful improvement in outcomes over current effective services/treatments.
• Be a medical service, not serving primarily a social or educational function.
• Be cost effective, so that the health gain for individual and population health is sufficient to justify the additional cost to taxpayers and consumers.
Caveats:
Failure to meet any of the criteria should result in exclusion or significant limits on coverage.
Each component would still be subject to the criteria for assembling the aggregate EHB package.
Inclusion does not mean that it is appropriate for every person to receive every component.
Criteria to Guide Methods for Defining and Updating the EHB
Methods for defining, updating, and prioritizing must be:
• Transparent. The rationale for all decisions about benefits, benefit design, and changes is made publicly available.
• Participatory. Current and future enrollees have a role in helping define the priorities for coverage.
• Equitable and consistent. Enrollees should feel confident that benefits will be developed and administered fairly.
• Sensitive to value. To be accountable to taxpayers and plan members, the covered service must provide a meaningful health benefit.
• Responsive to new information. The EHB will change over time as new scientific information becomes available.
• Attentive to stewardship. For judicious use of pooled resources, budgetary constraints are necessary to keep the EHB affordable.
• Encouraging to innovation. The EHB should allow for innovation in covered services, service delivery, medical management, and new payment models to improve value.
• Data-driven. An evaluation of the care included in the EHB is based on objective clinical evidence and actuarial reviews.
Balancing Coverage and Cost
Congress provided guidance in the ACA to the Secretary about the contents of the EHB by listing 10 categories of care that must be included (Box S-1) and by indicating that coverage should be consistent with the typical employer plan. Given the ACA’s focus on providing access to health insurance for workers of small firms and individuals in the first years of the health insurance exchanges, the committee concluded that the EHB should be defined initially by what is typical in the small employer market. The committee noted that the insurance plans offered by small vs. large employers differ primarily in their benefit design and administration rather than in what benefits are covered. The committee also concluded that current state-mandated benefits should not receive any special treatment in the definition of the EHB and should be subject to the same evaluative method as all other parts of the EHB.
The committee’s vision for the EHB is that only medically necessary (or appropriate) services for individuals should be covered (Chapter 5). The committee believes that the concepts of individualizing care, ensuring value, and having medical necessity decisions strongly rooted in evidence should be reemphasized in any guidance on medical necessity. Inflexibility in the application of medical necessity, clinical policies, medical management, and limits without consideration of the circumstances of an individual case is undesirable and potentially discriminatory. The committee believes transparency in a rigorous appeals monitoring process is the primary approach to addressing the nondiscrimination provisions in benefit design and implementation, including medical necessity reviews.
Early in its deliberations the committee recognized that to achieve the ACA’s goal of improving access to health care services by maximizing the number of people with meaningful health insurance benefits, the cost of the package needs to be included in the definition of the EHB (Chapter 5). As the scope of benefits expands, individuals who are purchasing plans by themselves or through employers face higher premiums. A benefit package that is more expensive also places greater demand on the federal budget to provide subsidies for low-income purchasers and on state budgets to cover some newly eligible Medicaid enrollees.
The EHB can be viewed as a “market basket” of goods and services (i.e., benefit options) that enrollees who need those goods and services are eligible to have covered. The price for access to the services covered by that market basket is the premium. The committee considered two basic approaches the Secretary could take to establish the initial cost of the EHB: select the market basket of benefit options and then estimate what it would cost or set a cost target and determine what could be purchased within that constraint. The committee endorses the latter approach and recommends using as the cost target the estimated national average premium that would have been paid by small employers in 2014 for a silver level—equivalent plan if the ACA had not been enacted.2 This does not mean that the Secretary is setting a single premium for all silver plans purchased in the country but rather that the estimated average cost of the EHB would not exceed the national average premium for a silver plan. Premiums faced by consumers and employers will vary as they do today by region of the country, design and administration of the insurance plan, whether benefits beyond the EHB are included in the package, and other factors.
BOX S-1
Essential Benefits Categories in the Patient Protection and Affordable Health Care Act
Essential Health Benefits
• Ambulatory patient services
• Emergency services
• Hospitalization
• Maternity and newborn care
• Mental health and substance use disorder services, including behavioral health treatment
• Prescription drugs
• Rehabilitative and habilitative services and devices
• Laboratory services
• Preventive and wellness services and chronic disease management
• Pediatric services, including oral and vision care
SOURCE: §1302(b)(1)(A)-(J).
2 The ACA establishes four “metal” levels of plans to be offered on exchanges: platinum, gold, silver, and bronze. The plans all must include the EHB. The plans are distinguished by their actuarial value, that is, by the average proportion of eligible expenses that is paid by the plan. The actuarial values for the metal levels are 90 percent for platinum, 80 percent for gold, 70 percent for silver, and 60 percent for bronze. Premium subsidies are calculated based on the average cost of the second lowest premium for a silver plan in a market.
Public Input Should Be Obtained to Inform the Tradeoffs Between Covered Elements
The process recommended by the committee to define the EHB explicitly requires that tradeoffs be made between competing elements of the benefit package in order to meet the premium target. Setting priorities among benefit options necessitates integrating scientific evidence about effectiveness with value judgments about relative importance. Thus, the committee recommends that the Secretary undertake a public deliberative process to obtain input on the tradeoffs. The process that the committee supports is described in greater detail in Chapter 6.
Secretarial Guidance Should Be as Explicit as Possible
In examining coverage documents used by insurers today, the committee found that they frequently lacked specificity. The committee further observed that specificity increases the likelihood that consumers will be offered a uniform set of benefits no matter where or from whom they purchase insurance. The committee recommends that the Secretary be as explicit as possible to ensure that the ACA intent of a consistent package of benefits is achieved.
Recommendation 1: By May 1, 2012, the Secretary should establish an initial essential health benefits (EHB) package guided by a national average premium target.
A. The starting point in establishing the initial EHB package should be the scope of benefits and design provided under a typical small employer plan in today’s market. To specify the initial EHB package, this scope of benefits should then be modified to reflect
• The 10 general categories specified in Section 1302(b)(1) of the Affordable Care Act (ACA); and
• The criteria specified in this report for the content of specific elements and aggregate EHB package (see Figure S-2).
B. Once a preliminary EHB list is developed as described in (A), the package should be adjusted so that the expected national average premium for a silver plan with the EHB package is actuarially equivalent to the average premium that would have been paid by small employers in 2014 for a comparable population with a typical benefit design.
C. The Secretary should sponsor a public deliberative process to assist in determining how the adjustments to the EHB package should be made.
D. Initial guidance by the Secretary on the contents of the EHB package should list standard benefit inclusions and exclusions at a level of specificity at least comparable to current best practice in the private and public insurance market.
CREATING A FOUNDATION FOR UPDATING
THROUGH MONITORING AND RESEARCH
The committee expects that the EHB will change over time based on a variety of factors and stakeholder input. The Secretary should have a mechanism for learning how the priorities and tradeoffs made by the public are changing, what states are learning about the uptake of new insurance products in the exchanges and reductions in the number of people who are uninsured, what research suggests are the approaches to care delivery and benefit design that improve outcomes, and what innovations in insurance design promote high value care. To make certain that the Secretary can systematically learn from the implementation experience in the exchanges and the changing science base, a process for identifying data needs and developing a coordinated research agenda to support monitoring and updating the EHB should begin immediately (Chapter 7). The committee offers a two-part recommendation regarding a framework for data collection and coordinated research efforts.
A Framework Should Be Developed to Guide Data Collection
for Monitoring Implementation and Updating of the EHB
The state health insurance exchanges will determine which health plans are qualified to operate in the exchange, and can provide information about the progress of implementing the EHB. The ability of the states to provide consistent and usable information to the Secretary will be enhanced if a framework for collecting and analyzing data is developed in advance. The exchanges and other health care—related entities (insurers, providers) will be important sources of data for monitoring and updating the EHB. The committee recommends that the Secretary obtain guidance from expert groups on setting standards for uniform reporting of state-based data.
Recommendation 2a: By January 1, 2013, the Secretary should establish a framework for obtaining and analyzing data necessary for monitoring implementation and updating of the EHB. The framework should account for:
• Changes related to providers such as payment rates, contracting mechanisms, financial incentives, and scope and organization of practice;
• Changes related to patients and consumers such as demographics, health status, disease burden, and problems with access; and
• Changes related to health plans such as characteristics of plans (inclusions, exclusions, limitations), cost-sharing practices, patterns of enrollment and disenrollment, network configuration, medical management programs (including medical necessity determination processes), value-based insurance design, types of external appeals, risk selection, solvency, and impact of the ACA-mandated limits on deductibles, co-payments, and out-of-pocket spending on the ability of plans to offer acceptable products.
A Coordinated Research Agenda Will Enhance Assessments of the EHB
HHS’s component agencies, the Department of Labor, and other non-federal organizations routinely collect data that will be pertinent to assessing the EHB over time. In particular, the Secretary should examine how the scope of benefits contributes to expanded coverage and access to quality care, and how the EHB package can be updated to become more evidence-based and value-promoting. The committee recommends that, prior to implementation of the exchanges in 2014, HHS coordinates the development of a research plan to evaluate the implementation of the EHB and identify the data necessary to support this plan. Furthermore, the committee believes that, to the extent patient privacy can be assured, public access to these data for analysis should be enabled, just as HHS has sponsored access to other departmental data (e.g., http://www.health.data.gov).
Recommendation 2b: The Secretary should establish an appropriate infrastructure for implementing this framework that engages and coordinates the efforts of all of the appropriate HHS and other federal agencies
in producing and analyzing the necessary data in a timely manner. These data should be made easily accessible and affordable for public use.
ALLOWANCE FOR STATE-BASED INNOVATION
The committee acknowledges that some flexibility is necessary to encourage innovation. It is the committee’s intention that the initial design of the EHB continue to support innovation in the design of insurance products offered (Chapter 8). The ACA is clear that the Secretary of HHS has sole authority to define the EHB. The authority granted to HHS to define EHB does not, however, preclude the Secretary from using that authority to approve state-specific variations of the EHB definition. Those variations must be consistent with the requirements specified in the ACA, should produce a package that is of equivalent comprehensiveness and value, and should have undergone a systematic process for obtaining public input.
Recommendation 3: For states administering their own exchanges that wish to adopt a variant of the federal EHB package, the Secretary should use statutory authority to grant such requests, provided that the state-specific EHB definition is consistent with the requirements of Section 1302 of the ACA and the criteria specified in this report, that they produce a package that is actuarially equivalent to the national package established by the Secretary, and that the request is supported by a process that has included meaningful public input. To best achieve this, the Secretary should encourage a public deliberative process as described in this report and should provide technical assistance to the states for implementing that process.
UPDATING THE EHB
The Secretary asked the IOM to provide guidance on a process for updating the EHB over time. Congress also requires HHS to monitor whether the essential benefits package is being implemented appropriately for all eligible enrollees. As required in Section 1302, the Secretary must periodically update the EHB and provide a report to Congress and the public that addresses the following:
• whether enrollees are facing any difficulty accessing needed services for reasons of coverage or cost;
• whether the EHB needs to be modified or updated to account for changes in medical evidence or scientific advancement;
• how the EHB will be modified to address any such gaps in access or changes in the evidence base; and
• an assessment of the potential of additional or expanded benefits to increase costs and the interactions between the addition or expansion of benefits and reductions in existing benefits to meet actuarial limitations.3
The committee recommends that the Secretary undertake an approach to updating the EHB that incorporates the advances in medical science and insurance design within a cost target that is defined by the national average premium for a silver plan offered on the exchanges (Chapter 9). The committee offers a three-part recommendation for the updating process: first, set goals for the updated EHB package; second, propose a method for using costs to frame modifications to the EHB; third, call attention to the need to develop a strategy to address increases in health care spending that threaten the long term integrity of the EHB as a meaningful package.
Goals for Updating the EHB
The committee believes that over time the EHB package should become more explicitly based on evidence of effectiveness and should promote better outcomes for both individuals and the U.S. population relative to the
3 Patient Protection and Affordable Care Act of 2010, Public Law 111-148 as amended by the Health Care and Education Reconciliation Act of 2010. § 1302(b)(4)(H). 111th Cong., 2nd session.
cost of insurance coverage. The committee believes this will require more detailed specification of included and excluded services than will initially characterize the Secretary’s guidance. The report provides some examples available today of the desirable level of detail in future EHB definitions (Chapter 9).
Recommendation 4a: Beginning in 2015, for implementation in 2016 and annually thereafter, the Secretary should update the EHB package, with the goals that it becomes more fully evidence-based, specific, and value-promoting.
Incorporating Costs into Updates
The committee considered multiple methods of updating the initial national average premium in Recommendation 1. Based on the current secretarial authority and other factors, the committee recommends that any changes to the EHB result in a package that is no more expensive than the estimated subsequent year cost of the base-year package. This ensures that the EHB will not accelerate the increase in spending for those whose insurance is subject to the EHB. Further, it provides a mechanism for incorporating new categories or services within the cost target (premium), requiring tradeoffs be made explicitly between existing and new elements of coverage.
Recommendation 4b: The Secretary should explicitly incorporate costs into updates to the EHB package.
• The Secretary should obtain an actuarial estimate of the national average premium for a silver-level plan with the existing EHB package in the next year; the estimate will account for trends in medical prices, utilization, new technologies, and population characteristics.
• Any changes to the EHB package should not result in a package that exceeds the actuarially estimated cost of the current package in the next year. A public deliberative process should be used to inform choices about inclusions to or exclusions from the updated package, with specific attention to how inclusion of new benefits could affect the availability of existing covered benefits.
A Strategy Should Be Developed to Address Rising Costs
From the beginning of its deliberations, the Committee unanimously agreed that if the country does not address the problem of health care costs growing faster than the gross domestic product, it will undermine the ACA’s goal of substantially reducing the number of people without health insurance. In Recommendation 4b, the committee endorses allowing the cost of the EHB to increase with the rate of premium increases because that would enhance the likelihood of maintaining the initial level of comprehensiveness established by the Secretary. Unfortunately, this means that the cost of the EHB will likely continue to increase faster than wages and faster than the growth in the economy. In turn, the number of people who will be able to afford to purchase the EHB-defined insurance will decline. As the premiums increase, subsidies will take a larger share of the federal budget. As premiums rise, many more people will choose to enroll in Medicaid rather than a private plan on the exchange, increasing the strain on state budgets. All of these consequences violate one of the criteria established by the committee: the EHB should be affordable for consumers, employers, and taxpayers. The committee further envisioned that the pressure on federal and state budgets might lead to repeal of the EHB requirement. This threat to the long-term integrity of the EHB caused the committee to consider what could be done in order to mitigate these adverse consequences.
Achieving an appropriate balance between comprehensiveness and affordability of the EHB cannot be accomplished through actions taken only on behalf of EHB enrollees or only through the contents of the EHB. Effective efforts to change the rate of increase in health spending require a strategy that addresses all of the drivers of health care costs. The committee considered whether complementary Medicare-only or federal-only approaches to reducing rising health care costs would be sufficient and concluded they would not be. An all stakeholder strategy is required across the public and private sectors. Unless a strategy for containing costs throughout the health care system is adopted, the definition of an essential health benefits package will ultimately fail to achieve congressional intent to establish an appropriate basic package that is affordable.
Recommendation 4c: To ensure over time that EHB-defined packages are affordable and offer reasonable coverage, the Secretary of HHS, working in collaboration with others, should develop a strategy for controlling rates of growth in health care spending across all sectors in line with the rate of growth in the economy.
The committee believes desirable attributes of an approach to developing such a strategy are for it to be nonpartisan, include public and private sector collaboration, integrate activities across all sectors, and be able to ensure action on the recommendations. For example, the Secretary could co-convene a commission with a representative of the private sector experienced in purchasing health services to develop and implement meaningful actions to control costs. Because coordinated federal action would increase the likelihood of success in the public sector, the Secretary of HHS could coordinate federal participation in a commission and oversee federal implementation of such a commission’s recommendations. The committee considered whether an existing entity could take up this charge, specifically assessing the Independent Payment Advisory Board (IPAB), and decided it was less appropriate for the work envisioned by the committee as IPAB is currently constituted.
While it may appear that addressing the rate of growth in health care spending is beyond the scope of the EHB provisions, the committee views its Recommendations 4b and 4c as necessary complements. The committee’s Recommendation 4b is designed to preserve the scope of benefits over time and yet to ensure that the EHB package itself will not accelerate the increase in spending by keeping the package equivalent in content. But without making concerted progress in stemming rising health care costs (Recommendation 4c), it will cost more to purchase the same package of benefits each year, eroding the purchasing power of the estimated 68 million people who will depend on EHB coverage. Eventually, the EHB package will become a hollow promise of coverage. The committee’s charge was to develop a viable approach to defining the EHB that would work now and into the future, and this requires a two-pronged approach.
THE SECRETARY SHOULD OBTAIN ONGOING
EXTERNAL ADVICE ON UPDATING THE EHB
Having identified a set of recommendations for updating the EHB and addressing the sector-wide challenges with rising health care costs, the committee next considered whether the Secretary would benefit from forming a new advisory group focused on updates to the EHB. The committee refers to this advisory group as the National Benefits Advisory Council (NBAC).
The committee recommends that the NBAC advise the Secretary on (1) the research framework and scope of the data collection for monitoring implementation (Chapter 7), (2) updates to the overall benefit package and related benefit design issues, (3) changes to the cost target, and (4) appropriate mechanisms for evaluating new interventions. The IOM committee thought that while the NBAC might ideally have a role in defining the initial EHB, it would not be practical to get the NBAC appointed and operational in a timely enough fashion to be useful in this process. However, the public input obtained by the IOM committee and its own deliberations about defining the initial EHB is consistent with what the NBAC will be doing over time.
The NBAC should ensure that the EHB protect the most vulnerable members of society, encourage appropriate use of services, be evidence-based, and encourage cost-effective use of resources. Further, the NBAC is a mechanism to ensure that the process to define and apply decisions about updates to the EHB be fair and transparent.
The committee considered whether an existing entity could fulfill the functions envisioned for the NBAC and specifically considered the U.S. Preventive Services Task Force, the Medicare Evidence Development and Coverage Advisory Committee (MEDCAC), the Patient-Centered Outcomes Research Institute (PCORI), and the Consumer Operated and Oriented Plan (CO-OP) Program Advisory Board. The report describes the current functions of these groups and the extent to which they could undertake the NBAC mission. The committee concluded that none of these entities is designed to or could easily be modified to perform the necessary functions.
Recommendation 5: As soon as is feasible, the Secretary should establish a National Benefits Advisory Council (NBAC), staffed by HHS but appointed through a nonpartisan process, such as the Office of the Comptroller General of the United States. The NBAC should
• By January 1, 2013, advise the Secretary on a research plan and data requirements for updating the EHB package;
• Starting in 2015 for implementation in 2016, make recommendations annually to the Secretary regarding (1) any changes to the EHB package by applying the committee’s recommended criteria (see Figure S-2), (2) any changes to the premium target, and (3) any mechanisms that would enhance the evidence base of the EHB package and its potential for promoting value; and
• Advise the Secretary on conducting and using the results of a periodic national public deliberative process to inform its recommendations around updates to the EHB.
CONCLUSION
The ACA establishes an essential health benefits package and defines 10 general categories that must be included in that package. The ACA, however, left considerable discretion to the Secretary of HHS to design this package. The Secretary, in turn, asked the IOM to provide input on the process that might be undertaken to develop the EHB. In its deliberations, the most critical issue identified by the committee is the need to explicitly address the tradeoff between the cost of a benefit package and the comprehensiveness of coverage. If that tradeoff is not addressed, a number of consequences are possible:
• If the benefits are not affordable, fewer people will buy insurance.
• If the benefit design makes access too difficult, people will not get the care they need.
• If health care spending continues to rise faster than gross domestic product (GDP), the value of the EHB is likely to be eroded.
The committee concluded that the benefit package should be designed within the context of financial constraints, using a structured public process to establish priorities. The committee developed a set of criteria to guide the process for designing and updating the EHB. The EHB must be affordable, maximize the number of people with insurance, protect the most vulnerable individuals, protect against the greatest financial risks, promote better care, ensure stewardship of limited financial resources by focusing on high value services of proven effectiveness, promote shared responsibility for improving our health, and address the medical concerns of greatest importance to us all.
REFERENCES
Eibner, C., F. Girosi, C. C. Price, A. Cordova, P. S. Hussey, A. Beckman, and E. A. McGlynn. 2010. Establishing state health insurance exchanges: Implications for health insurance enrollment, spending, and small businesses. Santa Monica, CA: RAND Corporation.
Glied, S. 2011. Testimony to the IOM Committee on the Determination of Essential Health Benefits by Sherry Glied, Assistant Secretary for Planning and Evaluation, HHS, Washington, DC, January 13.










