___________
The scope of work for the study is to advise on a process to define and update the essential health benefits (EHB) package, which is a central element in the implementation of current health insurance reform efforts. The EHB will apply to a variety of private and public health insurance programs and will affect 68 million people or more. The content of the EHB will influence insurance product design, take-up rates by individuals and employers, and the comprehensiveness of insurance coverage. Balancing the comprehensiveness of coverage with affordability emerged as a key issue in the committee’s deliberation around essential benefits.
The Patient Protection and Affordable Care Act (herein known as the ACA)1 seeks to reduce the number of uninsured people in this country by providing access to affordable health insurance. As a result of implementation of the ACA, an estimated 30 million currently uninsured individuals are anticipated to obtain insurance through the private health insurance market or state expansion of Medicaid programs.2 Central to the development of private insurance packages under the ACA is the definition of what the law calls the essential health benefits. In the simplest terms, the EHB are a minimum standard set of benefits that insurers must offer, starting in 2014, in new plans for individual and small group purchasers. Insurers may offer and purchasers may buy plans with additional benefits.
The ACA requires the Secretary of the U.S. Department of Health and Human Services (HHS) to define the EHB. At the request of the Secretary, the Office of the Assistant Secretary for Planning and Evaluation (ASPE) contracted with the Institute of Medicine (IOM) to provide guidance on the methods and criteria by which HHS should establish and update the essential health benefits. This chapter starts with a review of the committee’s charge, an overview of key issues that emerged during the public input phase, a description of insurance coverage today and transitions under the ACA, the applicability of the EHB to various forms of public and private insurance, and choices in stakeholders’ decisions about participating in the new insurance landscape. Subsequent chapters of this report offer the committee’s conclusions and recommendations. The legislative foundation for the EHB is Section 1302 of the ACA, and that guidance is available in Appendix A.
1 Patient Protection and Affordable Care Act of 2010 as amended by the Health Care and Education Reconciliation Act of 2010. 111th Cong., 2d sess. (See http://docs.house.gov/energycommerce/ppacacon.pdf as amended through May 1, 2010; all references to the act reflect this version.)
2 The Congressional Budget Office estimates vary: 20 million by 2014, 31 million by 2016 (CBO, 2011b), and 30 million by 2016 and 32 million by 2019 (CBO, 2010). RAND projections note, “Relative to the status quo, the reform increases the number of nonelderly people with insurance by 35 million, or 16 percent” by 2016 (Eibner et al., 2010, p. 40).
Statement of Task
It is important to note that the IOM Committee on Defining and Revising an Essential Health Benefits Package for Qualified Health Plans was not formed to detail the specific services and items that should be included in the EHB package (see Statement of Task in Box 1-1). Instead, the committee was asked to provide guidance on policy foundations, criteria, and methods the Secretary should consider in determining and updating the EHB package for qualified health plans, particularly in light of the 10 required categories of care outlined in Section 1302(b)(1) and the requirement in Section 1302(b)(2)(A) for the EHB to be “equal to the scope of benefits provided under a typical employer plan.” State-based health insurance exchanges (HIEs) are being established to provide a competitive market through which individuals as well as employees of small businesses will be able to obtain private health insurance coverage. Purchasers are allowed but not obliged to buy their coverage through newly established HIEs; however, subsidies will be available through the exchanges on the basis of a sliding scale for individuals whose incomes are 139-400 percent of the federal poverty level (FPL).3
A qualified health plan is a plan that meets the requirements to be sold in an HIE, such as including the EHB, being offered by a licensed insurer that charges the same premium inside and outside the exchange, and other insurance reform elements.4 Discussions with HHS further indicated that the committee should also recognize the applicability of these benefits to plans beyond the qualified health plans (QHPs) (i.e., Medicaid benchmark, benchmark-equivalent, state basic insurance plans, and certain private plans sold outside the exchanges). The Secretary is expected to issue guidance on the EHB package during 2012 because Section 1321(c) of the ACA requires the Secretary to make an assessment by January 2013 that the states will have operational exchanges by January 1, 2014.5
BOX 1-1
Statement of Task for the Institute of Medicine Committee
The Patient Protection and Affordable Care Act (Affordable Care Act) established criteria for qualified health plans (QHPs) to participate in exchanges as defined in Section 1301 of the statute. An ad hoc IOM committee will make recommendations on the methods for determining and updating essential health benefits for QHPs based on examination of the subject matter below.
In so doing, the committee will identify the criteria and policy foundations for determination of the essential health benefits offered by QHPs taking into account benefits as described in Sections 1302(b)(1) and 1302(b)(2)(A), and the committee will assess the methods used by insurers currently to determine medical necessity and will provide guidance on the “required elements for consideration” taking into account those outlined in Section 1302(b)(4)(A-G), including ensuring appropriate balance among the categories of care covered by the essential health benefits, accounting for the health care needs of diverse segments of the population, and preventing discrimination against age, disability, or expected length of life. The committee will also take into account language in Section 1302 on periodic review of essential health benefits, and other sections of the Affordable Care Act: for example, coverage of preventive health services (Section 2713), utilization of uniform explanation of coverage documents and standardized definitions (Section 2715), and other relevant tasks found in the Affordable Care Act for the Secretary of the Department of Health and Human Services (HHS). The committee will provide an opportunity for public comment on the tasks of defining and revising the essential health benefits
3 Individuals whose incomes are at or below 133 percent of the FPL will be eligible for Medicaid, with an additional 5 percent income disregard, effectively raising the income eligibility level to 138 percent of FPL (§ 1902(e)(14) of the Social Security Act).
4 § 1301.
5 Personal communication with ASPE staff, October 26, 2010; updated by personal communication with Caroline Taplin, ASPE, June 14, 2011.
Public Comment
Per the last sentence in the statement of task, the public was afforded opportunities to provide advice directly to the committee and then to have that information shared with HHS. The committee began its work by gathering comments in response to a set of 10 online questions derived from its contract with ASPE, which were posted on the IOM project website (Appendix A). This involved a wider group of respondents than could be afforded an opportunity to speak in person with the committee, thus allowing their input to assist the committee in its deliberations and to identify varying perspectives related to the study topics. During the 6 months that the questions were posted, the committee received about 345 online responses from a variety of interested stakeholders, including provider groups, purchasers, insurers, consumer advocates, individual respondents, and government officials. These responses were analyzed and made available to the committee and provided to HHS as submitted. The responses have been open to public review at the IOM through its public access file, as have many other submissions received via e-mail and letters, whose contents were also reviewed by the IOM staff and committee.6
Fifty-nine speakers were invited to present at public sessions of the first and second committee meetings, held January 13-14, 2011, in Washington, DC, and March 2, 2011, in Costa Mesa, California. Because of widespread interest in the topic of the EHB, the first workshop was simultaneously audiocast, and audio files were posted on the project website. Initially, a single-day workshop was planned, but additional time was allotted on day 2 of the January meeting and the second workshop was held in March. A companion workshop report summarizes the presentations from the two workshops: Perspectives on Essential Health Benefits: Workshop Report.7 The workshop report is distinct from this consensus report in that it summarizes the individual perspectives of the speakers, rather than includes conclusions or recommendations from the committee. During its deliberations, the committee took into account all of the comments received, not just those received through the workshop venue, as it formulated its approach to identifying and addressing key issues.
Learning from the major themes raised in the workshops, other public comment, and additional research, the committee identified key issues surrounding the EHB that required its attention:
• Setting a balance between comprehensiveness and affordability. The basic tension was how comprehensive the EHB could be and still be affordable for consumers and payers and sustainable as a program over time (Gruber, 2011).
• Defining what “typical” should mean in typical employer. Section 1302 of the ACA requires the EHB to be equal to the scope of benefits provided under a typical employer plan. Congressional staff presented contrasting opinions regarding Congress’ intent during the committee’s first workshop. One perspective was that the EHB should be a minimum, basic plan affordable for small employers (Hayes, 2011; Spangler, 2011). An alternate perspective was that the EHB should be a more comprehensive plan, more like one that large employers offer, that would still be affordable to all participants in the exchange (Bowen, 2011; Schwartz, 2011). These opposing views were voiced by a variety of other stakeholders.
• Determining whether state mandates should be included. The ACA does not require the EHB to include the myriad existing benefits mandated by individual states.8 Proponents argued for inclusion of particular mandates based on the strength of evidence and/or consideration of popular support for mandates. Opponents noted their potential cumulative additive cost.
• Considering how specific EHB guidance should be and when variation from state to state might be allowable. The Secretary is required to define the national EHB package. Specificity in that benefit definition was variously viewed as bringing more uniformity to implementation across states, and more general guidance as promoting flexibility.
6 A request to view the public access file can be made at http://www8.nationalacademies.org/cp/ManageRequest.aspx?key=49299.
7 The workshop report is available at http://www.iom.edu/EHBperspectives.
8 § 1311(d)(3)(B).
• Developing criteria and methods that address calls for the best evidence, patient protection, opportunities for innovation, and fair processes. Submissions across stakeholder groups emphasized the need for using evidence to make decisions on covered benefits, to determine medical necessity, to set priorities, or to place limits on service. At the same time, there were calls to ensure there would be opportunities for innovation both in medical care and insurance design. The need for fair processes was viewed as applying not only to defining benefits, but also ensuring that patients are able to receive the coverage that is intended.
The committee kept these issues in mind as it developed its recommendations on the criteria and methods for defining and updating the EHB package.
STATUS OF CURRENT HEALTH INSURANCE COVERAGE
Before embarking upon a more detailed discussion of the issues related to the EHB, it is useful to understand what health insurance is, who has and does not have health insurance now, and the transitions in insurance status under health reform. In 2014, each nonelderly individual in the country will be required to have health insurance or face a penalty (with a few exceptions such as experiencing financial hardship)—this is known as the individual mandate.9 Among the rationales for the individual mandate are that it would broaden the risk pool and seek to stop cost shifting for health care services from the uninsured to those who have insurance (Chandra et al., 2011; McGlynn et al., 2010).
Like other forms of insurance, health insurance is a mechanism for pooling risk—spreading health care costs over many individuals or families (IOM, 2001). Premiums, the dollar amount paid for the insurance package, are collected in advance, and those who get sick and obtain care will be covered from the collected premiums. Baicker and Chandra elaborate: “Uncertainty about when we may fall sick and need more health care is the reason we purchase insurance—not just because health care is expensive (which it is)” (Baicker and Chandra, 2008, p. w534). It is important to recognize that in addition to serving the typical functions of risk insurance, health insurance was developed as a mechanism for financing or pre-paying a variety of health care benefits, including routine preventive services or chronic disease care, whose use is neither rare nor unexpected (IOM, 2001; Mariner, 2010).
Population With and Without Insurance
Insurance coverage in this country for people under 65 years old is primarily employer-sponsored insurance (ESI)—approximately 60 percent of the nonelderly population had this type of coverage in 2010 (Fronstin, 2011b); employer-sponsored insurance figures contain employers in the private market and public sector employers, including those that self-insure rather than purchase insurance. Figure 1-1 shows the 2009 distribution of coverage by type of coverage or uninsurance. According to The Commonwealth Fund’s 2010 Biennial Health Insurance Survey, of the 26 million people who bought or tried to obtain private coverage in the individual market during the past 3 years, 19 million faced significant barriers—either they were refused coverage or charged a higher price because of a health problem (9 million), found it very difficult or impossible to find an affordable plan (16 million), or no plan was affordable for their needs (11 million) (Collins et al., 2011). A portion of the uninsured also reflects unemployment during the recent recession (Collins et al., 2011; DeNavas-Walt et al., 2011; Fronstin, 2011a).
Studies reveal that approximately 52 million individuals were uninsured in the United States for some period of time during 2010, up from 38 million in 2001 (Collins et al., 2011).10 Through a combination of individually purchased policies, employer-based coverage, Medicaid expansion, and federal subsidies, 30 million or more
9 Exemptions will be granted for financial hardship, religious objections, American Indians, those without coverage for less than 3 months, undocumented immigrants, incarcerated individuals, those for whom the lowest-cost plan option exceeds 8 percent of an individual’s income, and those with incomes below the tax filing threshold (in 2009 the threshold for taxpayers under age 65 was $9,350 for singles and $18,700 for couples) (§5000A(c)).
10 The U.S. Census Bureau reports 49.9 million without coverage in 2010; although this is a larger number than in 2009, the percentage of the population without insurance remains at 16.3 percent (DeNavas-Walt et al., 2011).
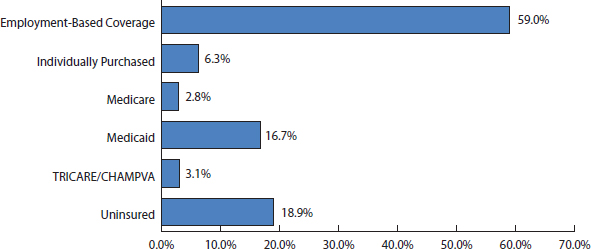
FIGURE 1-1 Nonelderly population with selected sources of health insurance coverage, 2009.
NOTE: Details do not add to 100 percent because individuals may receive coverage from more than one source; analyses are based on Current Population Survey data supplements. S-CHIP is the State Children’s Health Insurance Program; TRICARE is administered by the Department of Defense; CHAMPVA is the Civilian Health and Medical Program of the Department of Veterans Affairs.
SOURCE: Fronstin, 2010.
Americans are expected to have insurance than would have in the absence of the law (CBO, 2010, 2011b; Eibner et al., 2010).
Transitions in Insurance Status Under Health Reform
As millions become newly insured and others look for more affordable coverage, people will obtain insurance from new sources. For example, a Kaiser Family Foundation (KFF) study looks at where individual non-group enrollees will transition from, while a RAND microsimulation illustrates the complexity of movement across different forms of insurance or from a state of uninsurance. KFF estimates that the distribution of the Congressional Budget Office’s (CBO’s) projected 24 million enrolling as individuals in the exchanges in 2019 would be 16 million individuals otherwise uninsured, 3.5 million who lost their ESI, 1.5 million whose previous ESI took more than 9.5 percent of their total family income and are looking for more affordable coverage,11 2 million adults above 138 percent of the federal poverty level who lose Medicaid coverage, and 1 million who would have purchased individual coverage anyway (CBO, 2010; KFF, 2011a). Table 1-1 illustrates the outcomes of the RAND microsimulation using 2016 projections and shows movement of about 16 percent of employees into the exchanges from employer insurance, 78 percent of the individual non-group market taking advantage of the exchanges, and the currently uninsured participating in a variety of forms of insurance with the overall result of substantially reducing the number of individuals who would otherwise have been uninsured without health reform.
Accessing Subsidized Health Insurance
Exchanges, functioning as state-based government entities or a nonprofit organization, will be the major conduit for offering subsidized health insurance plans that contain the EHB. However, when a state opts not to open an exchange, the federal government will have the responsibility to operate an exchange directly or through a nonprofit organization. The ACA provides for two types of exchanges, one for individual purchasers (American Health Benefits Exchange) and one for small employers (Small Business Health Options Program [SHOP] Exchanges), but states may combine operations into one exchange (KFF, 2010). Furthermore, the ACA requires
11 Note: These are individuals who are eligible for premium tax credits, because the insurance they are offered by their employers exceeds this affordability threshold.
the federal Office of Personnel Management (OPM) to enter into contracts with health insurers to offer at least two multi-state qualified health plans through the exchanges;12 these are distinct from the Federal Employees Health Benefits Program (FEHBP), which OPM also administers.
| Post-Reform Insurance Status | ||||||
| Insurance in the Status Quo | ESI: Traditional(N) | ESI: Exchanges (N) | Individual Exchanges (N) | Medicaid(N) | Uninsured (N) | Other (N) |
| Employer (154) | 118 | 25 | 4 | 5 | 2 | 0 |
| Medicaid (37) | 1 | 2 | 0 | 34 | 0 | 0 |
| Non-group (18) | 1 | 3 | 14 | 0 | 0 | 0 |
| Other (16) | 0 | 0 | 0 | 0 | 0 | 16 |
| Uninsured (52) | 6 | 6 | 14 | 10 | 16 | 0 |
| Total (277) | 126 | 36 | 33 | 49 | 18 | 16 |
NOTE: Numbers may not total due to rounding. ESI means employer-sponsored insurance. The projections are for the nonelderly population in 2016. The 68 million estimate used in text is based on adding 35.6 million on ESI: Exchanges and 32.7 million in Individual Exchanges and then rounding.
SOURCE: Eibner et al., 2010.
IMPACT OF THE EHB ACROSS INSURANCE PROGRAMS
The reach of the EHB is extensive, both in terms of the type of insurance markets and the products it applies to, and ultimately in terms of the projected number of people who would obtain coverage that includes this defined benefit package.
EHB Requirement Applies to Some But Not All Insurance Products
The EHB will be incorporated into a variety of insurance program products—new private health insurance plans offered to individuals and to employers with 100 or fewer employees either inside or outside of the exchange, and certain public programs but not traditional Medicaid (Box 1-2). However, all private plans are not subject to the EHB, including plans offered by any small employer that self-insures, any “grandfathered” plan, and at this time, any plan sponsored by employers in the large group market.13 Exchanges do not open to larger employers until 2017, and even then it is at a state’s option to open the exchange to this segment of the market.14
Individual and employer plans in existence at the time of enactment of the ACA (March 23, 2010) qualify for the grandfathered status, whereby the EHB does not apply as long as no changes are made in the plan. For most of these plans, the grandfathered status will not endure; approximately 49-80 percent of small employer plans and 34-64 percent of large employer plans will relinquish grandfather status by the end of 2013 (U.S. Department of the Treasury et al., 2010). Other estimates include a Mercer study projection that 53 percent of firms would lose grandfathered status for one or more plans in 2011 and an additional 48 percent by 2014 (Mercer, 2010), while a Hewitt study estimated that 51 percent of self-insured and 46 percent of fully insured plans would lose grandfathered status in 2011(Hewitt Associates LLC, 2010). HHS estimates that even if a mid-range estimate of plans were to “relinquish” their grandfather status, perhaps as many as 66 percent of small employer plans would
12 § 1334 and § 10104(q).
13 Self-insured employers are not exempt from the ACA [42 U.S.C. 18054]; its provisions simply do not apply because the self-insured are not insurance companies (by operation of The Employee Retirement Income Security Act [ERISA] §514) and do not offer insurance policies on the exchange.
14 § 1312(f)(2)(B)(i).
be affected. Similarly, grandfathered individual plans would have a high rate of turnover (U.S. Department of the Treasury et al., 2010).
BOX 1-2
Which Programs Incorporate Essential Health Benefits (EHB)?
The EHB Apply to Multiple Insurance Programs, Starting in 2014
Individual Private Market
• Qualified health plans (QHPs) purchased through the exchanges (§ 1301(a)(1)(B) at any of the four actuarial defined “metal” levels [platinum, gold, silver, and bronze] (§ 1302(d)(1)(A)-(D));
• Catastrophic health plans for eligible persons (e.g., persons under age 30 before the beginning of the plan year or for financial hardship when premiums exceed 8 percent of income) purchased in the exchanges (§ 1302(e)(1)-(2));
• Individual and family policies or plans purchased outside the exchange in the individual market (§ 1201, amending § 2707(a) of the Public Health Service Act);
• Plans offered through Interstate Health Care Choice Compact (§ 1333(a)(3)(A));
• Multistate Plans, offered by the federal Office of Personnel Management (OPM) (§ 1334(c)(1)(A)); and
• QHPs offered by Consumer Operated and Oriented Plans (CO-OPs) (nonprofit, member-run health insurance) (§ 1322).
Small Group Private Market
• QHPs for purchase by small firms in the exchanges; a small firm or employer is defined as one with 100 or fewer employees (§ 1304(b)(2)); however, until 2016 states may opt to define small firms as those with 50 or fewer employees (§ 1304(b)(3)), and starting in 2017 exchanges can open to larger firms with 101 or more employees (§ 1312(f)(2)(B)).
• Small employer-sponsored insurance policies or plans purchased outside the exchange (§ 1201, amending § 2707(a) of the Public Health Service Act).
• QHP offered by CO-OPs (nonprofit, member-run health insurance) (§ 1322).
Public Programs Expansions
• Medicaid Benchmark and Benchmark-Equivalent programs, which states may use to provide newly eligible Medicaid beneficiaries with coverage (&3167; 1937(b) of the Social Security Act). States will also be given the authority to provide certain other groups of Medicaid beneficiaries with this coverage who qualify under existing rules (§ 1902 of the Social Security Act).
• State-Run Basic Health Plans, which provide coverage for persons with incomes between 133 and 200 percent of the federal poverty level (FPL) and for legal resident immigrants who are not eligible for Medicaid; premiums cannot exceed those in the exchanges (§ 1331(a)(1)).
Programs Not Subject to the EHB
• Self-insured employer-sponsored plans
• Grandfathered employer-sponsored plans
• Grandfathered plans in the small group market
• Grandfathered individual plans in the non-group market
• Existing Medicaid plans
Although not applying to the traditional Medicaid program, the EHB will apply to some public insurance expansion programs for individuals newly eligible for Medicaid. While states will still enroll “categorically” eligible individuals in traditional Medicaid, states may opt to enroll others who are now “financially” eligible in traditional Medicaid or benchmark/benchmark-equivalent programs (CMS, 2010; KFF, 2011b). The Deficit Reduction Act of 2005 permitted states to vary Medicaid benefits to designated populations, often designed to more closely resemble benefits in the private sector. The benefit plans do not need to follow all Medicaid rules and can be modeled on “benchmark” or “benchmark-equivalent” plans in the private sector such as a FEHBP standard plan.15,16 These programs will have to include the EHB starting in 2014. State basic health insurance programs are another optional vehicle for states to develop coverage for persons whose income falls between 133 and 200 percent FPL and for low-income legal resident immigrants who are not eligible to receive Medicaid.17 These expansions will be administered by a state agency but are not necessarily offered through the exchanges.
Millions Affected by the EHB
Estimates vary for the number of persons affected by the implementation of health reform, and thereby the number of persons whose policies incorporate the EHB in 2014 and in later years. By 2016, RAND estimates that 68 million will obtain insurance in the exchanges (35 million through ESI and 33 million purchasing as individuals) and when opened to larger firms with 100 or more employees, exchange participation could grow as high as 139 million (Eibner et al., 2010). In contrast, the CBO projects that 29 million will participate in exchanges in 2019 (24 million individuals and 5 million through employer-sponsored plans) (CBO, 2010). The actual number of affected plans and individuals additionally covered outside the exchange can be influenced by the percentage of plans that have status as grandfathered plans or employers that choose to self-insure.
Medicaid expansion might cover another 17 million persons by 2021 (CBO, 2011a). Because the development of new benchmark, benchmark-equivalent, and state basic health insurance programs—which all incorporate the EHB—is up to each state, it is unclear what the individual reach of those programs might eventually be.
Characteristics of New Individual Purchasers Under the ACA
Although the ACA provides for individual purchase, ESI, and Medicaid options for reducing the number of uninsured, the characteristics of the individual non-group market participants have been most closely studied.18 KFF expects many persons eligible to be individual (non-group) purchasers in the exchanges to have characteristics of uninsured populations, predicting new exchange enrollees to be “relatively older, less educated, lower income, and more racially diverse” and “in worse health but have fewer diagnosed chronic conditions” (KFF, 2011a, pp. 3-4). The Center for Studying Health System Change (HSC) similarly finds that 40 percent of the uninsured, who are eligible for premium subsidies, have chronic conditions or report fair or poor health status, and another 28 percent report they have experienced problems in accessing care or paying their medical expenses (Cunningham, 2010).
15 Benchmark plans are based on (1) the standard BlueCross BlueShield preferred provider option under the Federal Employee Health Benefit Plan, (2) the HMO (health maintenance organization) plan with the largest commercial, non-Medicaid enrollment in the state, (3) any generally available state employee plan (regardless of whether any state employees select the plan), and (4) any plan that the Secretary of HHS determines to be appropriate. Benchmark-equivalent plans must include inpatient and outpatient hospital services, physician services, laboratory and X-ray services, well-baby and child care (including immunizations), and “other appropriate preventive services” designated by the Secretary of HHS (Deficit Reduction Act of 2005 § 1937). Before the EHB provisions go into effect, CMS provided guidance on interim requirements (CMS, 2010).
16 Section 2001 of ACA describes the Medicaid expansion. Section 2001(c) stipulates that by January 1, 2014, any benchmark or benchmark-equivalent plan as outlined in Section 1937 of the Social Security Act must offer the EHB package. As of 2009, eight states offered these types of plans.
17 § 1331.
18 A study to examine the ESI population is under way by RAND for The Commonwealth Fund, but the results were not available for this report.
STAKEHOLDER DECISIONS WILL RESHAPE HEALTH INSURANCE MARKETS
The ACA lays out a broad set of 10 categories of care for the EHB package in an attempt to rectify deficiencies in some insurance instruments available today19 and to ensure a broad set of benefits, all while placing caps on premiums and cost sharing to make plans affordable for individual and small employers and eliminating financial barriers to many preventive care services. At present, because the EHB have yet to be defined and implementation does not start until 2014, less is known about what the full scope of covered services or exclusions will be, what premium would be required to obtain coverage of those services, who will choose to enroll in the exchanges, whether employers and insurers will participate or withdraw from the market, and how these and other decisions will determine the sustainability of the program for public funds. The definition of the EHB can ultimately influence each of these areas, particularly with respect to determining the affordability of the package for consumers, employers, and government as well as the adequacy of reimbursement for providers of care.
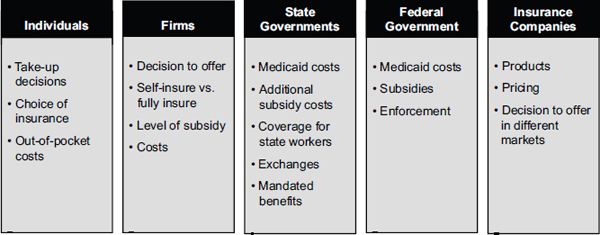
Figure 1-2 outlines different considerations various stakeholders will take into account for these decisions, and the effects of these decisions can be interactive. Each of these topics is explored in Appendix B, with identification of key financial triggers set in the ACA for eligibility to specific programs and decisions on participation. The cost of premiums, which will be influenced by the comprehensiveness of the EHB package among other benefit design features, compared with the penalty for not purchasing insurance is not strictly a financial one—having health insurance confers an advantage to the consumer whereas paying a penalty does not. Although the impact of some of the choices faced by the various stakeholders are informed by past experience and research simulations, the effect of initial EHB definition on stakeholder response will have to be monitored to inform updates to the EHB package.
The individual consumer is less likely steeped in the details of the ACA than other stakeholder groups and might wonder, “What do the EHB mean for me?”
• Will the ACA/EHB cover any service I want/need to get? The EHB will set a minimum set of standard benefits to include in health insurance plans offered initially to individuals and small businesses. Just as in current health insurance practice, plans developed with the EHB will not pay for anything the consumer wants, unless it is a covered benefit and it is medically appropriate for the particular patient. Plans may add additional benefits beyond those in the EHB package, and a consumer could choose to purchase a plan with additional benefits if that best suits his or her needs, although purchasing additional benefits could mean a higher premium.
19 Deficiencies include, for example, specific disease and fixed-dollar indemnity policies.
• Will the ACA/EHB provide access to any provider I want to see? The ACA does not change current practice; which providers the consumer sees will depend on the health insurance purchased. Insurers now offer a variety of options for consumer choice of plans and provider networks. For example, if enrolled in a plan with a preferred provider network, the consumer can see those preferred providers and after paying the premium, only be responsible for the deductible and co-payment amounts. The consumer could see an out-of-network provider, but it would cost more than the deductible and usual co-payment share if there is a difference between the provider’s bill and the approved level of reimbursement for in-network providers.
• If the EHB is a standard set of benefits, does that mean that everyone will pay the same premium? The ACA encourages a variety of plans to be offered in the exchanges so that there will likely be a variety of choices of premiums, deductibles, and co-payment levels, just as there is now. Chapter 2 discusses the topic of benefit design.
This report is organized in the following way. This introductory chapter establishes the context for how the EHB, as a new legislative requirement, will significantly impact the health insurance system. Chapter 2 focuses on approaches to covered benefit definition and design, summarizing a sampling of different approaches that emphasize evidence, priority setting, and value-based insurance design. Chapter 3 provides a set of policy foundations and criteria that the committee used to guide its own deliberations and recommends to the Secretary for use in defining and updating benefits. Chapter 4 presents the committee’s conclusions about provisions in the ACA that provide possible conflicting direction for essential benefits, such as the meaning of typical, both in terms of employer size and benefit offerings, and the meaning of essential. These first four chapters provide the background foundation for the committee’s recommendations.
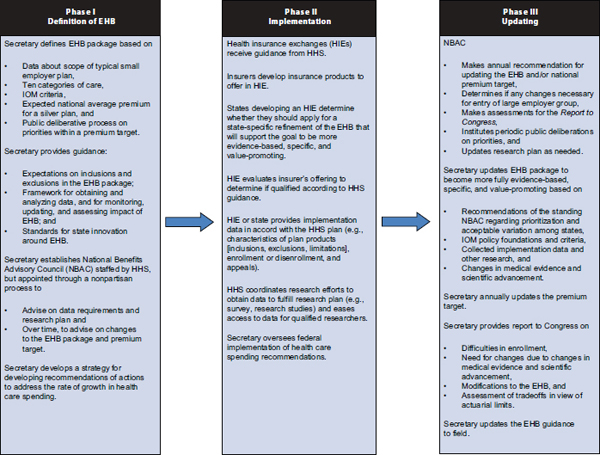
FIGURE 1-3 Learning cycle for defining and revising essential health benefits (EHB).
The committee organized its thinking about definition and updating as separate phases in a learning cycle, as outlined in Figure 1-3. Chapter 5 provides guidance for the definition of the EHB package and the nature of the Secretary’s guidance to insurers and exchanges. Chapter 6 explicates an approach to public deliberation for tradeoffs among benefits. Chapter 7 outlines the importance of not only learning from implementation in Phase II, but also planning in advance for that learning through thoughtful data collection and research with guidance from an appointed National Benefits Advisory Council. Chapter 8 allows for the possibility of alternative ways of defining essential health benefits through a state-initiated process. In Phase III, the learning culminates with updating the EHB. Chapter 9 outlines the updating process, accounting for medical inflation and other factors in the future cost of the EHB package, and a call for action on reducing the growth of health care spending across all payers.
Baicker, K. and A. Chandra. 2008. Myths and misconceptions about U.S. health insurance. Health Affairs 27(6):w534-543.
Bowen, D. 2011. Testimony to the IOM Committee on the Determination of Essential Health Benefits by David Bowen, Deputy Director for Global Health Policy and Advocacy, Gates Foundation, Washington, DC, January 13.
CBO (Congressional Budget Office). 2010. Letter to the Honorable Nancy Pelosi, Speaker, U.S. House of Representatives from Douglas W. Elmendorf, Director, Congressional Budget Office, March 20, 2010.
______. 2011a. CBO’s analysis of the major health care legislation enacted in March 2010. Statement by Director Douglas W. Elmendorf before the U.S. House of Representatives Subcommittee on Health Committee on Energy and Commerce, March 30, 2011. Washington, DC: Congressional Budget Office.
______. 2011b. Letter to the Honorable John Boehner, Speaker of the U.S. House of Representatives from Douglas W. Elmendorf, Director, Congressional Budget Office, February 18, 2011.
Chandra, A., J. Gruber, and R. McKnight. 2011. The importance of the individual mandate—evidence from Massachusetts. New England Journal of Medicine 364(4):293-295.
CMS (Centers for Medicare & Medicaid Services). 2010. Re: Family planning services option and new benefit rules for benchmark plans. https://www.cms.gov/smdl/downloads/SMD10013.pdf (accessed November 14, 2011).
Collins, S. R., M. M. Doty, R. Robertson, and T. Garber. 2011. Help on the horizon: How the recession has left millions of workers without health insurance, and how health reform will bring relief. Findings from The Commonwealth Fund Biennial Health Insurance Survey of 2010. New York: The Commonwealth Fund.
Cunningham, P. J. 2010. Who are the uninsured eligible for premium subsidies in the health insurance exchanges? Washington, DC: Center for Studying Health System Change.
DeNavas-Walt, C., B. D. Proctor, and J. C. Smith. 2011. Income, poverty, and health insurance coverage in the United States: 2010. Washington, DC: U.S. Census Bureau.
Eibner, C., F. Girosi, C. C. Price, A. Cordova, P. S. Hussey, A. Beckman, and E. A. McGlynn. 2010. Establishing state health insurance exchanges: Implications for health insurance enrollment, spending, and small businesses. Santa Monica, CA: RAND Corporation.
Fronstin, P. 2010. Sources of health insurance and characteristics of the uninsured: Analysis of the March 2010 Current Population Survey. No. 347. Washington, DC: Employee Benefit Research Institute.
______. 2011a. The impact of the 2007-2009 recession on workers’ health coverage. No. 356. Washington, DC: Employee Benefit Research Institute.
______. 2011b. Sources of health insurance and characteristics of the uninsured: Analysis of the March 2011 Current Population Survey. Issue brief No. 362. http://www.ebri.org/pdf/briefspdf/EBRI_IB_09-2011_No362_Uninsured1.pdf (accessed November 14, 2011).
Gruber, J. 2011. Economic and political considerations in setting essential benefits. PowerPoint Presentation to the IOM Committee on the Determination of Essential Health Benefits by Jonathan Gruber, Professor of Economics, Massachusetts Institute of Technology, Washington, DC, January 13.
Hayes, M. 2011. Essential health benefits requirements under section 1302. PowerPoint Presentation by Mark Hayes, Health & FDA Practice Group, Greenberg Traurig, to the IOM Committee on the Determination of Essential Health Benefits, Washington, DC, January 13.
Hewitt Associates LLC. 2010. Employer reaction to health care reform: Grandfathered status survey. http://www.aon.com/attachments/02_ER_Reaction_HC_Grandfathered_Survey.pdf (accessed September 7, 2011).
IOM (Institute of Medicine). 2001. Coverage matters: Insurance and health care. Washington, DC: National Academy Press.
KFF (Kaiser Family Foundation). 2010. Explaining health care reform: Questions about health insurance exchanges. Washington, DC: Kaiser Family Foundation.
______. 2011a. A profile of health insurance exchange enrollees. Washington, DC: Kaiser Family Foundation.
______. 2011b. Medicaid policy options for meeting the needs of adults with mental illness under the Affordable Care Act. http://www.kff.org/healthreform/upload/8181.pdf (accessed November 14, 2011).
Mariner, W. K. 2010. Health reform: What’s insurance got to do with it? Recognizing health insurance as a separate species of insurance. American Journal of Law & Medicine 36(2/3):436-451.
McGlynn, E. A., A. Cordova, J. Wasserman, and F. Girosi. 2010. Could we have covered more people at less cost? Technically, yes; politically, probably not. Health Affairs 29(6):1142-1146.
Mercer. 2010. Even as reform pushes up benefit cost, employers will take steps to hold 2011 increase to 5.9%. http://www.mercer.com/press-releases/1391585 (accessed September 19, 2011).
Schwartz, D. 2011. Testimony to the IOM Committee on the Determination of Essential Health Benefits by David Schwartz, Senate Finance Committee Democratic Staff, U.S. Senate, Washington, DC, January 13.
Spangler, K. 2011. Testimony to the IOM Committee on the Determination of Essential Health Benefits by Katy Spangler, Senior Health Policy Advisor, Senate Health, Education, Labor and Pensions (HELP) Committee, U.S. Senate, Washington, DC, January 13.
U.S. Department of the Treasury, DOL (Department of Labor), and HHS (Department of Health and Human Services). 2010. Group health plans and health insurance coverage relating to status as a grandfathered health plan under the Patient Protection and Affordable Care Act; Interim final rule and proposed rule. Federal Register 75(116):34538-34570.












