The United States continues to experience an epidemic of overweight and obesity. This national health condition constitutes a startling setback to major improvements achieved in other areas of health during the past century. The substantial and long-term human and societal costs of obesity, the great difficulty of treating this problem once it has developed, and the relatively slow progress made thus far in turning the national obesity numbers around underline the urgent need to develop a plan for accelerating progress in obesity prevention.
The Institute of Medicine’s (IOM’s) Committee on Accelerating Progress in Obesity Prevention was formed to address this challenge. The committee’s overall charge was to develop a set of recommendations for accelerating progress toward obesity prevention over the next decade, as well as to recommend potential measures of progress toward this goal. Inherent in this charge was a recognition that, while a large number of promising individual programs and interventions currently are being supported, implemented, and evaluated, there is a growing need to identify a set of obesity prevention actions that, both individually and together, can accelerate meaningful change on a societal level.
Prior work by the nation’s researchers to illuminate various aspects of the obesity problem has helped inform obesity prevention efforts. For example, there is a broad consensus that changes are necessary in the environments in which people live and the settings they frequent. Another major revelation has been that there are no simple or single-pronged solutions. Earlier work has helped researchers and health professionals understand the need for a “meta-strategy” for obesity prevention that includes a range of recommendations. Any one potential strategy can contribute to obesity prevention, but alone cannot solve this complex problem.
![]()
1 This summary does not include references. Citations to support statements made herein are given in the body of the report.
THE CRITICAL IMPORTANCE OF OBESITY PREVENTION
Although the obesity epidemic in the United States has been instrumental in bringing worldwide attention to the problem, obesity also has become a problem worldwide. In the United States alone, one-third of adults are now obese, and the prevalence of obesity among children has risen from 5 to 17 percent in the past 30 years. Equally disturbing, these percentages generally are higher for ethnic minorities, for those who are low-income or less educated, and for rural populations. With obesity at these levels and with current trajectories suggesting the possibility of further increases, future health, social, and economic costs are likely to be devastating. Obesity is associated with major causes of death and disability, and its effect on predisposing individuals to the development of type 2 diabetes is so strong that the onset of this disease now is occurring in childhood.
In economic terms, the estimated annual cost of obesity-related illness based on data from the Medical Expenditure Panel Survey for 2000-2005 is $190.2 billion (in 2005 dollars), or nearly 21 percent of annual medical spending in the United States. Childhood obesity alone is responsible for $14.1 billion in direct medical costs. Many of these health-related obesity costs are absorbed by Medicare and Medicaid, important programs already under attack because of their national price tag. Moreover, obesity-related medical costs in general are expected to rise significantly, especially because today’s obese children are likely to become tomorrow’s obese adults. In fact, U.S. military leaders report that obesity has reduced their pool of potential recruits to the armed forces. As the U.S. economy struggles to stabilize and grow, obesity projections reveal that beyond the impact of growing medical costs attributable to obesity, the nation will incur higher costs for disability and unemployment benefits, and businesses will face the additional costs associated with obesity-related job absenteeism and lost productivity.
The causes of increased obesity in the United States—the influences that have led people to consume more calories (or energy) through food and beverages than they expend through physical activity—are multifactorial, ranging from cultural norms, to the availability of sidewalks and affordable foods, to what is seen on television. Many causes of obesity are the result of multiple changes in U.S. society that have affected various aspects of contemporary life, including physical activity and food consumption patterns. Exposure to these influences, both positive and negative, varies by subpopulation and can result in inequities in the prevalence of obesity. If a community has no safe places to walk or play, lacks food outlets offering affordable healthy foods, and is bombarded by advertisements for unhealthy foods and beverages, its residents will have less opportunity to engage
in physical activity and eating behaviors that allow them to achieve and maintain a healthy weight. Successful obesity prevention thus involves reducing negative and increasing positive influences on a societal level. There also are genetically or biologically mediated influences on obesity in individuals. Taking a population approach to obesity prevention is not to deny the importance of these genetic or biological factors, but to recognize the difficulty of maintaining energy balance when sedentary lives are the norm and high-calorie foods are ubiquitous.
Tremendous strides have been made in addressing the epidemic over the past decade, measured by the sheer amount of attention to the problem, and by the number and coherence of efforts to address the problem and bolster the scientific underpinnings and policy basis for taking action. Evidence of stabilization in obesity prevalence in at least some demographic groups suggests that these deliberate initiatives to address the problem are on track, perhaps in concert with other, spontaneous countering forces. Given the scope and scale of what is needed and the inevitability of a time lag before true progress can be estimated, however, the developments to date create a unique opportunity to restate goals and refine targets and approaches in order to accelerate progress.
Broad positive societal changes that support and sustain individual and family behaviors will need to affect activity and eating environments for all ages. Prevention is critical to decreasing the prevalence of overweight and obesity among children, who are the focus of much of the prevention discussion. But obesity prevention in adults also is crucial to obesity prevention in children because adults are their role models, caregivers, and advocates. Moreover, prevention efforts can help reduce the gradual increase in weight that often occurs in adulthood and support the reduction of further excess weight gain among adults who are already overweight or obese.
STUDY APPROACH
In responding to its charge, the committee’s main goal was to provide direction on what recommendations, strategies, and actions should be implemented in the short term to accelerate progress in obesity prevention over the next 10 years. The committee identified close to 800 previously published recommendations and associated strategies and actions related to obesity prevention and assessed the potential of each to help achieve this goal. To guide this assessment, the committee formulated a set of principles, summarized in Box S-1. The committee identified recommendations and associated strategies and actions with the broadest reach and the greatest potential to impact the development of obesity and prioritized
BOX S-1
Guiding Principles
The Committee on Accelerating Progress on Obesity Prevention formulated the following principles to guide the scope of its work and its decisions:
1. Bold, widespread, and sustained action will be necessary to accelerate progress in obesity prevention.
2. Priority and targeted actions must drive cultural and societal changes to improve environments that influence physical activity and food intake options.
3. Cultural and societal changes are needed to address obesity, and a systems approach must be taken when formulating obesity prevention recommendations so as to address the problem from all possible dimensions.
4. Solutions to the obesity epidemic must come from multiple sources, involve multiple levels and sectors, and take into account the synergy of multiple strategies.
5. Obesity prevention recommendations should be based on the best available scientific evidence as outlined in the Locate Evidence, Evaluate Evidence, Assemble Evidence, Inform Decisions (L.E.A.D.) framework.
6. The cost, feasibility, and practicality of implementing prior and further recommendations must be considered.
7. Unintended consequences of obesity prevention efforts must be considered.
8. Obesity prevention recommendations should incorporate ongoing evaluation of progress toward achieving benchmarks and of the need for any course corrections.
9. Recommendations to accelerate progress in obesity prevention must include an assessment of the potential for high impact, the reach and scope of potential effects, the timeliness of effects, the ability to reduce disparities and promote equity, and clearly measureable outcomes.
them using the best available scientific evidence. The committee also took into consideration progress made to date in implementing these recommendations, strategies, and actions; their ability to be evaluated or measured to assess their progress or impact; the timeliness of their effects; any unintended consequences; their potential to reduce disparities in the risk of obesity; and the feasibility and practicality of their implementation.
At the same time, the committee identified relationships among the recommendations and strategies and actions that could inform and strengthen their individual and overall impacts. This way of thinking—called a systems approach—allowed the committee to visualize and understand how recommendations and strategies on their own can be important to accelerate progress, and when implemented together with others, can interact and reinforce and sometimes inhibit impact on preventing obesity. This systems approach also helped the committee identify potential unintended effects (both positive and negative) that might not be apparent in considering individual solutions alone. Throughout this assessment, the committee looked as well for gaps in recommendations published to date.
The result of this work was the emergence of five critical areas—or environments for change: (1) environments for physical activity, (2) food and beverage environments, (3) message environments, (4) health care and work environments, and (5) school environments. These environments serve as the basis for the committee’s recommendations and the respective strategies, actions, and outcome indicators.
TAKING A SYSTEMS PERSPECTIVE TO ACCELERATE PROGRESS
In this report, the committee presents five key interrelated recommendations whose implementation would have a substantial effect on accelerating obesity prevention over the next decade; an explanation of the kinds of engagement and leadership that can build capacity and mobilize action; and a call for monitoring progress in the implementation of the recommendations (see Figure S-1). While a Venn diagram such as that in Figure S-1 cannot illustrate the many and diverse interactions and feedback loops revealed by a systems map (as presented in Appendix B), it does reflect the critical areas of concern and their interrelationships. The committee’s recommendations can have a profound impact on people in the environments with which they interact on a regular basis, including schools, places of employment, doctors’ offices, child care settings, restaurants of all kinds, and everywhere food is sold. To implement these recommendations, the committee has identified strategies that individually have the greatest potential reach and
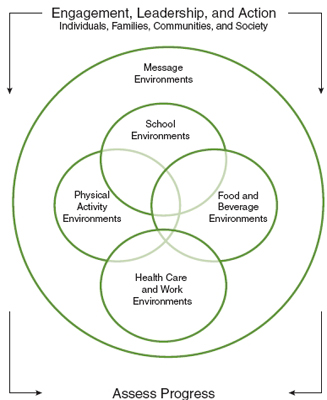
FIGURE S-1 Comprehensive approach of the Committee on Accelerating Progress in Obesity Prevention.
impact on preventing obesity, based on research evidence and the current level of progress in each area. For each strategy, the report also suggests a set of actions that are likely to make a positive contribution to that strategy’s achievement based on research evidence or, where evidence is lacking or limited, have a logical connection with its achievement.
Each recommendation, strategy, and action has potential to accelerate obesity prevention. However, while the report necessarily presents the committee’s recommendations individually, in linear form, the committee suggests that they be viewed by key stakeholders and sectors as unfolding simultaneously and influencing each others’ success. This “systems perspective” helps to reveal, and create, the potential for combined impacts (or synergies) that can further accelerate progress in preventing obesity. This perspective also can assist in recognizing likely positive (i.e., supporting and accelerating success) and negative (i.e., acting as a barrier to success) interactions and feedback loops among the recommendations and strategies.
Engagement and Equity
It is essential to recognize that accelerating progress toward obesity prevention will need to occur at every level, from individual, to family, to community, to society as a whole. Acceleration will require engagement among all levels and all sectors in order to build capacity and achieve impact so that individuals and families can successfully manage and support healthy changes in lifestyle.
It is important to recognize as well that not all individuals, families, and communities are similarly situated. In many parts of the United States, low-income individuals and families live, learn, work, and play in neighborhoods that lack sufficient health-protective resources such as parks and open space, grocery stores, walkable streets, and high-quality schools. In any given community, the relative mix of community-level resources and risk factors is determined primarily through democratic local and regional decision-making processes; consequently, organized participation in these processes influences where these community resources and risks are located. Because of such factors as poverty, language barriers, and immigration status, low-income, minority, and other disadvantaged population groups often are underrepresented and their concerns marginalized in these decision-making processes. These groups are therefore less likely to benefit from access to health-protective resources. To change this situation, robust and long-term community engagement and civic participation among these disadvantaged populations become essential.
Leadership, Implementation, and Priorities
In presenting its recommendations throughout the report, the committee identifies leaders who are those individuals, agencies, organizations, or sectors traditionally seen as having the knowledge and control of and responsibility for
the particular environments, policies, and practices that must change. The committee also introduces new ways to think about leadership, including identifying and calling on a broader set of individuals, families, communities, and society at large. A major premise of the committee’s systems approach to leadership is that it is a shared responsibility across sectors and levels, and one that may not follow typical hierarchical or individual sector-based approaches. All individuals, organizations, agencies, and sectors that do or can influence physical activity and nutrition environments are called on to assess and begin to act on their potential roles as leaders in obesity prevention. Some traditional leaders may turn away from this responsibility, but many other less likely or unexpected leaders may step forward as willing actors.
Whether leaders are identified or self-identify, once awareness of the catastrophic nature of the obesity problem is understood and felt and the need for diverse and numerous leaders is recognized, all will share the moment of saying to themselves, “I can do something about this, and I want to play a role.” From that point on, viewing their roles with a systems lens will guide them in new directions. They will act with new foresight—seeing how what they plan to do can or will intersect and interact with other actions that may be or have already been taken in their sector, other sectors, or across sectors. Funding for implementation is likely to become available as the seriousness of the obesity threat is understood, and calls and support for resources to combat a potential disaster emerge. In addition, the diversity of leaders throughout the system can bring existing assets to bear for use or redeployment and make available new resources, often from unexpected sources, that previously were not apparent or available.
Implicit in the committee’s systems approach to leadership and implementation is the assumption that individual leaders will determine which recommendations, strategies, and potential actions are their priorities, or that those who choose to follow their lead will play a major role in determining these priorities. The committee did not give any recommended action or set of actions priority above any others, but rather saw leaders stepping up to implement different aspects of the five critical areas identified in Figure S-1. Leaders are called on to start from where they have the most influence and likelihood of success, a decision resulting from their unique assessment of a range of community-specific or local level factors.
Assessment
The changes recommended by the committee should begin now and, once implemented, continue for a sustained period. Much of this work has already begun in a number of sectors at the local, state, and national levels. It will be essential to monitor and track progress in the implementation of the committee’s recommendations, as well as to conduct sustained research on the magnitude and nature of their impact, both individually and in tandem. While the confluence of all the recommendations will likely have the most impact, each step toward acceleration of progress will be significant and cumulative in its impact.
The Vision
The committee’s recommendations, strategies, and actions can be seen as a system of large-scale transformative approaches that is urgently needed to accelerate progress in obesity prevention. This system comprises major reforms in access to and opportunities for physical activity; widespread reductions in the availability of unhealthy food and beverage options and increases in access to healthier options at affordable, competitive prices; an overhaul of messages that surround Americans (through marketing and education) with respect to physical activity and food consumption; expansion of the obesity prevention support structure provided by health care providers, insurers, and employers that interfaces with the U.S. population in every workplace and health care setting; and schools being made a major national focal point for obesity prevention. By viewing the committee’s recommendations from a systems perspective, one can see that as individual changes are achieved in each of these environments, these changes also have the potential to support and accelerate the progress of other recommended changes within each environment and in other environments as well.
To gain a better sense of the potentially transformational nature of this system of reforms, it is helpful to imagine a United States in which they have been fully implemented in ways that take into account the potential positive and negative aspects of their interaction. For example, physical activity would be an integral and routine part of most people’s lives, and adults and children would have access to places and opportunities for enjoyable movement everywhere they spend their time. Healthy foods would be the most visible, attractive, and easy to obtain options in all places that sell or serve food. Education about food would involve every child in hands-on skill-building experiences with making food choices in stores and restaurants and preparing foods at home, and children and their
parents would hear more from television and digital media about activity and healthy foods than about sedentary pursuits and unhealthy foods. Patients would leave every health care provider visit with more knowledge about obesity prevention that they could put into action, supported by their immediate environment, and workplaces would play a major role in increasing the physical activity and healthy foods available to their employees. And schools would be nutrition and wellness centers for children and their families in every community.
RECOMMENDATIONS AND STRATEGIES
The committee offers five recommendations, along with strategies for their implementation, under five respective overarching goals. Specific actions associated with each strategy, a detailed systems map illustrating the interactions among the recommendations and strategies, and indicators that can serve as measures of progress are presented in the body of the report. The committee firmly believes that implementing its recommendations is essential to improve and maintain the nation’s health. Without focused and sustained effort in these areas, the obesity epidemic will lead to more increases in the costs of being less well and less productive, including reduced ability for the nation and its citizens to compete in life and in the workplace. If these issues are important to each of the sectors with the potential to contribute to obesity prevention, it is their obligation to act promptly and in a sustained manner in the interests of the nation’s health and security.
Goal 1: Make physical activity an integral and routine part of life.
Recommendation 1: Communities, transportation officials, community planners, health professionals, and governments should make promotion of physical activity a priority by substantially increasing access to places and opportunities for such activity.2
Strategy 1-1: Enhance the physical and built environment. Communities, organizations, community planners, and public health professionals should encourage physical activity by enhancing the physical and built environment, rethinking community design, and ensuring access to places for such activity.
![]()
2 Note that physical education and opportunities for physical activity in schools are covered in Recommendation 5, on school environments.
Strategy 1-2: Provide and support community programs designed to increase physical activity. Communities and organizations should encourage physical activity by providing and supporting programs designed to increase such activity.
Strategy 1-3: Adopt physical activity requirements for licensed child care providers. State and local child care and early childhood education regulators should establish requirements for each program to improve its current physical activity standards.
Strategy 1-4: Provide support for the science and practice of physical activity. Federal, state, and local government agencies should make physical activity a national health priority through support for the translation of scientific evidence into best-practice applications.
Goal 2: Create food and beverage environments that ensure that healthy food and beverage options are the routine, easy choice.
Recommendation 2: Governments and decision makers in the business community/private sector3 should make a concerted effort to reduce unhealthy food and beverage options4 and substantially increase healthier food and beverage options at affordable, competitive prices.
Strategy 2-1: Adopt policies and implement practices to reduce overconsumption of sugar-sweetened beverages. Decision makers in the business community/private sector, in nongovernmental organizations, and at all levels of government should adopt comprehensive strategies to reduce overconsumption of sugar-sweetened beverages.5
![]()
3 The business community/private sector includes private employers and privately owned and/or operated locations frequented by the public, such as movie theaters, shopping centers, sporting and entertainment venues, bowling alleys, and other recreational/entertainment facilities.
4 Although there is no consensus on the definition of “unhealthy” foods/beverages, the term refers in this report to foods and beverages that are calorie-dense and low in naturally occurring nutrients. Such foods and beverages contribute little fiber and few essential nutrients and phytochemicals, but contain added fats, sweeteners, sodium, and other ingredients. Unhealthy foods and beverages displace the consumption of foods recommended in the Dietary Guidelines for Americans and may lead to the development of obesity.
5 Sugar-sweetened beverages are defined to include all beverages containing added caloric sweeteners, including, but not limited to, sugar- or otherwise calorically sweetened regular sodas, less than 100 percent fruit drinks, energy drinks, sports drinks, and ready-to-drink teas and coffees.
Strategy 2-2: Increase the availability of lower-calorie and healthier food and beverage options for children in restaurants. Chain and quick-service restaurants should substantially reduce the number of calories served to children and substantially expand the number of affordable and competitively priced healthier options available for parents to choose from in their facilities.
Strategy 2-3: Utilize strong nutritional standards for all foods and beverages sold or provided through the government, and ensure that these healthy options are available in all places frequented by the public. Government agencies (federal, state, local, and school district) should ensure that all foods and beverages sold or provided through the government are aligned with the age-specific recommendations in the current Dietary Guidelines for Americans. The business community and the private sector operating venues frequented by the public should ensure that a variety of foods and beverages, including those recommended by the Dietary Guidelines for Americans, are sold or served at all times.
Strategy 2-4: Introduce, modify, and utilize health-promoting food and beverage retailing and distribution policies. States and localities should utilize financial incentives such as flexible financing or tax credits, streamlined permitting processes, and zoning strategies, as well as cross-sectoral collaborations (e.g., among industry, philanthropic organizations, government, and the community) to enhance the quality of local food environments, particularly in low-income communities. These efforts should include encouraging or attracting retailers and distributors of healthy food (e.g., supermarkets) to locate in underserved areas and limiting the concentration of unhealthy food venues (e.g., fast-food restaurants, convenience stores). Incentives should be linked to public health goals in ways that give priority to stores that also commit to health-promoting retail strategies (e.g., through placement, promotion, and pricing).
Strategy 2-5: Broaden the examination and development of U.S. agriculture policy and research to include implications for the American diet. Congress, the Administration, and federal agencies should examine the implications of U.S. agriculture policy for obesity, and should ensure that such policy includes understanding and implementing, as appropriate, an optimal mix of crops and farming methods for meeting the Dietary Guidelines for Americans.
Goal 3: Transform messages about physical activity and nutrition.
Recommendation 3: Industry, educators, and governments should act quickly, aggressively, and in a sustained manner on many levels to transform the environment that surrounds Americans with messages about physical activity, food, and nutrition.6
Strategy 3-1: Develop and support a sustained, targeted physical activity and nutrition social marketing program. Congress, the Administration, other federal policy makers, and foundations should dedicate substantial funding and support to the development and implementation of a robust and sustained social marketing program on physical activity and nutrition. This program should encompass carefully targeted, culturally appropriate messages aimed at specific audiences (e.g., tweens, new parents, mothers); clear behavior-change goals (e.g., take a daily walk, reduce consumption of sugar-sweetened beverages among adolescents, introduce infants to vegetables, make use of the new front-of-package nutrition labels); and related environmental change goals (e.g., improve physical environments, offer better food choices in public places, increase the availability of healthy food retailing).
Strategy 3-2: Implement common standards for marketing foods and beverages to children and adolescents. The food, beverage, restaurant, and media industries should take broad, common, and urgent voluntary action to make substantial improvements in their marketing aimed directly at children and adolescents aged 2-17. All foods and beverages marketed to this age group should support a diet that accords with the Dietary Guidelines for Americans in order to prevent obesity and risk factors associated with chronic disease risk. Children and adolescents should be encouraged to avoid calories from foods that they generally overconsume (e.g., products high in sugar, fat, and sodium) and to replace them with foods they generally underconsume (e.g., fruits, vegetables, and whole grains). The standards set for foods and beverages marketed to children and adolescents should be widely publicized and easily available to parents and other consumers. They should cover foods and beverages marketed to children and adolescents aged 2-17 and should apply to a broad range of marketing and advertising practices, including digital marketing and the use of licensed characters and toy premiums. If such marketing standards have not been adopted within 2 years by a substantial
![]()
6 Note that instruction in food and nutrition for children and adolescents in schools is covered in Recommendation 5, on school environments.
majority of food, beverage, restaurant, and media companies that market foods and beverages to children and adolescents, policy makers at the local, state, and federal levels should consider setting mandatory nutritional standards for marketing to this age group to ensure that such standards are implemented.
Strategy 3-3: Ensure consistent nutrition labeling for the front of packages, retail store shelves, and menus and menu boards that encourages healthier food choices. The Food and Drug Administration (FDA) and the U.S. Department of Agriculture should implement a standard system of nutrition labeling for the front of packages and retail store shelves that is harmonious with the Nutrition Facts panel, and restaurants should provide calorie labeling on all menus and menu boards.
Strategy 3-4: Adopt consistent nutrition education policies for federal programs with nutrition education components. USDA should update the policies for Supplemental Nutrition Assistance Program Education and the policies for other federal programs with nutrition education components to explicitly encourage the provision of advice about types of foods to reduce in the diet, consistent with the Dietary Guidelines for Americans.
Goal 4: Expand the role of health care providers, insurers, and employers in obesity prevention.
Recommendation 4: Health care and health service providers, employers, and insurers should increase the support structure for achieving better population health and obesity prevention.
Strategy 4-1: Provide standardized care and advocate for healthy community environments. All health care providers should adopt standards of practice (evidence-based or consensus guidelines) for prevention, screening, diagnosis, and treatment of overweight and obesity to help children, adolescents, and adults achieve and maintain a healthy weight, avoid obesity-related complications, and reduce the psychosocial consequences of obesity. Health care providers also should advocate, on behalf of their patients, for improved physical activity and diet opportunities in their patients’ communities.
Strategy 4-2: Ensure coverage of, access to, and incentives for routine obesity prevention, screening, diagnosis, and treatment. Insurers (both public and private)
should ensure that health insurance coverage and access provisions address obesity prevention, screening, diagnosis, and treatment.
Strategy 4-3: Encourage active living and healthy eating at work. Worksites should create, or expand, healthy environments by establishing, implementing, and monitoring policy initiatives that support wellness.
Strategy 4-4: Encourage healthy weight gain during pregnancy and breastfeeding, and promote breastfeeding-friendly environments. Health service providers and employers should adopt, implement, and monitor policies that support healthy weight gain during pregnancy and the initiation and continuation of breastfeeding. Population disparities in breastfeeding should be specifically addressed at the federal, state, and local levels to remove barriers and promote targeted increases in breastfeeding initiation and continuation.
Goal 5: Make schools a national focal point for obesity prevention.
Recommendation 5: Federal, state, and local government and education authorities, with support from parents, teachers, and the business community and the private sector, should make schools a focal point for obesity prevention.
Strategy 5-1: Require quality physical education and opportunities for physical activity in schools. Through support from federal and state governments, state and local education agencies and local school districts should ensure that all students in grades K-12 have adequate opportunities to engage in 60 minutes of physical activity per school day. This 60-minute goal includes access to and participation in quality physical education.
Strategy 5-2: Ensure strong nutritional standards for all foods and beverages sold or provided through schools. All government agencies (federal, state, local, and school district) providing foods and beverages to children and adolescents have a responsibility to provide those in their care with foods and beverages that promote health and learning. The Dietary Guidelines for Americans provide specific science-based recommendations for optimizing dietary intake to prevent disease and promote health. Implementation of these guidelines would shift children’s and adolescents’ dietary intake to prevent obesity and risk factors associated with chronic disease risk by increasing the amounts of fruits, vegetables, and high-fiber
grains they consume; decreasing their consumption of sugar-sweetened beverages, dietary fat in general, solid fats, and added sugars; and ensuring age-appropriate portion sizes of meals and other foods and beverages. Federal, state, and local decision makers are responsible for ensuring that nutrition standards based on the Dietary Guidelines are adopted by schools; these decision makers, in partnership with regulatory agencies, parents, teachers, and food manufacturers, also are responsible for ensuring that these standards are implemented fully and that adherence is monitored so as to protect the health of the nation’s children and adolescents.
Strategy 5-3: Ensure food literacy, including skill development, in schools. Through leadership and guidance from federal and state governments, state and local education agencies should ensure the implementation and monitoring of sequential food literacy and nutrition science education, spanning grades K-12, based on the food and nutrition recommendations in the Dietary Guidelines for Americans.
















