Key Messages
• The Institute of Medicine’s (IOM’s) Committee on Accelerating Progress in Obesity Prevention was charged with charting pathways to a timely resolution of the obesity epidemic in the U.S. population.
• The committee’s vision is for a successful, sustainable society that supports obesity prevention and offers broad opportunities for everyone to lead a healthy, productive life.
• Taking a systems perspective will accelerate the realization of this vision.
• Achieving this vision will involve mobilizing the population through engagement and leadership at all levels—individuals, families, communities, and society—and in all sectors.
• Targeted actions are needed to reduce the inequitable distribution of health promotion resources and risk factors that contribute to health disparities in low-income, minority, and other disadvantaged populations.
The epidemic of obesity in the United States has major human and societal costs, both now and for future generations. Obesity affects the entire childhood experience, predisposes adolescents to obesity in adulthood, and increases the risk of chronic illness and reduced quality of life and success in adulthood. Currently, a majority of U.S. adults and a substantial proportion of children and adolescents have weight levels in the overweight or obese range (Flegal et al., 2010; Ogden et al., 2010a). The percentage of people who are already obese
translates to an estimated total of nearly 73 million adults and 12 million children and adolescents (Ogden et al., 2010b,c), and those overweight are likely to become obese if they gain weight over time. The United States is far from alone in facing the challenges of this epidemic. Many aspects of the epidemic and its causes reach across the globe. An estimated 1.5 billion adults worldwide are overweight or obese (Finucane et al., 2011), and the World Health Organization estimates that 35 million preschool children in developing countries and 43 million preschool children worldwide are overweight or obese (de Onis et al., 2010). However, the nature of the factors causing this epidemic is such that the search for effective solutions must focus on specific drivers as they exist and operate within countries, regions, and localities.
The purpose of this report, developed by the Institute of Medicine’s (IOM’s) Committee on Accelerating Progress in Obesity Prevention, is to chart the pathways to a timely resolution of the obesity epidemic in the U.S. population. The committee was tasked with formulating a coherent set of recommendations that, if implemented, would be likely to significantly accelerate progress toward preventing obesity over the next decade, taking advantage, where possible, of favorable emerging developments. The committee was tasked further with recommending tangible, practical indicators with which to measure progress toward this goal. Specifically, the committee’s charge was to review prior obesity-related recommendations; consider relevant information on progress toward their implementation; develop principles to guide the selection of recommendations fundamental to achieving progress in obesity prevention; and recommend potential indicators that can act as markers of progress and can be readily evaluated through the use of current databases and/or relatively simple measures or surveys. This report responds to the challenges of this charge. The audience for the report includes public policy makers at all levels; private-sector decision makers; leaders in other institutions, including foundations, the education system, and professional and community-based organizations and health agencies; and the public in general.
This chapter sets the stage by articulating the committee’s vision for success (Box 1-1) and introducing concepts of a systems perspective and of engagement and leadership as essential elements for achieving this vision. A clear vision is essential to guard against thinking about obesity prevention in isolation from the complex social and economic systems within which the determinants of obesity— physical activity and eating patterns—are embedded. The committee’s vision imagines what society would look like if obesity prevention were achieved effectively, equitably, and sustainably. It allows for the identification of socially desirable
BOX 1-1
A Vision for Success
The committee envisions a society of healthy children, healthy families, and healthy communities in which all people realize their full potential and develop the competencies required to interact successfully with their surrounding environments. There is an urgent need to employ large-scale transformative approaches focused on multilevel environmental and policy changes within interconnected systems to reduce the threat of obesity and sustain an enduring impact.
pathways for change and indicators for assessing whether initiatives undertaken are on the right track before their longer-term effects can be fully evaluated. Inherent in the committee’s vision is the belief that children and adults should be able to satisfy their needs, be productive, and lead high-quality lives. Another critical common value expressed in the committee’s development of this vision is the need for safeguards to ensure equity so that children and adults in communities affected by social and economic disparities have opportunities to achieve a healthy weight in the environments where they live, learn, work, and play.
The underlying logic of the committee’s vision is illustrated in Figure 1-1. Favorable environments and behavioral settings positively influence individual, family, and population expectations, norms, and behaviors related to physical activity and healthy eating. Outcomes for individuals and society reflect decreased obesity rates with commensurate improvements in the health and societal outcomes highlighted in Chapter 2. Strategies and actions that drive overall environments in a health-promoting direction will be at the core of efforts to accelerate progress in preventing obesity. The cross-cutting factors listed at the bottom of the figure are a reminder that particular strategies and actions will affect individuals and populations differently depending on their circumstances, resources, and outlooks (IOM, 2007).
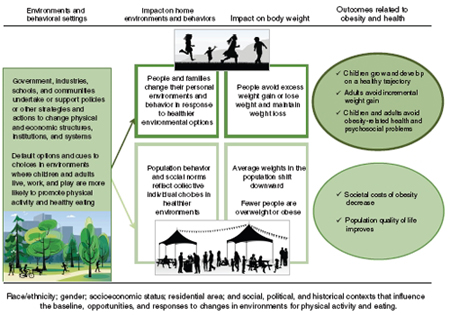
FIGURE 1-1 The logic of populationwide obesity prevention.
Several IOM reports and other prior analyses of potential solutions to the obesity epidemic, relevant both to the United States and globally, have established the inherent complexity of the problem (IOM, 2010). An impressive body of evidence confirms that the drivers of the epidemic involve interactions among several complex, ever-changing systems, including the food system, transportation systems, community infrastructure, school systems, health care systems, and the intricate behavioral and physiological systems that influence individual physical activity and eating behaviors and body weight. Reflecting this complexity, a prior IOM report calls for taking a systems approach to obesity prevention (IOM, 2010). Specifically, that report explains how a systems approach is an evolution of and expansion upon strategies already proposed or currently in use to prevent obesity. It is an approach that focuses on the whole picture and not just a single element, awareness of the wider context of any action, and an appreciation for interactions among different components of the problem. Further details on how the current committee took a systems approach can be found in Chapter 4 and Appendix B.
Building a society of healthy children, families, and communities will require coordinated change at multiple levels—from individuals, to families, to communities, to society as a whole. Pathways for change to curb and then reverse the epidemic of obesity involve core elements of the social fabric. The current environments in which eating and physical activity take place are the cumulative result of decisions that have been made over several decades, in numerous societal sectors. Many of those decisions have led—often inadvertently—to environments that run counter to the achievement or maintenance of healthy weight (Huang and Glass, 2008; Popkin et al., 2005). Americans have adjusted to these current ways of life and may strongly value many of the conveniences and pleasures they afford. Approaches that are inconsistent with fundamental values and principles will be undesirable and, ultimately, untenable.
Many initiatives needed for success in obesity prevention must occur through changes in societal sectors or institutions that influence health, including ones that are beyond the traditional health sector. Strategies must be carefully crafted to ensure that they will align with the goals and processes of these other sectors. Acceleration of obesity prevention will require reaching and engaging with multiple stakeholder groups. This need for action across a broad spectrum of society, together with the evolution of the problem over several decades, suggests that some time will be needed before solutions can be put in place and show effects.
The committee’s focus was on how the process of change that is needed—and is in many respects already under way—can be accelerated.
Two other elements are crucial for successful implementation of the committee’s recommendations to accelerate progress in obesity prevention utilizing a systems perspective: (1) the engagement of individuals, families, communities, and society and (2) the identification of leaders who can mobilize the changes needed while reducing disparities in the risk for obesity.
LEVELS OF ENGAGEMENT TO MOBILIZE CHANGE
The concept of “engagement” conveys the importance of collaborative approaches, “working with and through groups of people affiliated by geographic proximity, special interest, or similar situations” (CDC, 1997, p. 9)—that is, involving those affected by issues to address the issues that affect them. As described in this section, engagement is required at all levels of the population and across levels—individuals, families, communities, and the larger society—in order to build capacity, accelerate progress in obesity prevention, and reduce disparities in resources to ensure equity of impact in relation to the risk of obesity. The levels are interdependent, and all are necessary to achieve impact. Although its deliberations focused on strategies at the community and societal levels (see Chapter 3 for more detail), the committee recognizes the interdependence of these broader levels with the engagement of individuals and families. Every level of the population must play an active role in the system. Their engagement, as detailed below, could motivate a successful social movement for positive change.
Societal-Level Engagement
Prevention of obesity at the societal level requires supports for child health and development, including food, education, and family life. The health of the public is ultimately a collective responsibility, and the fear of engendering political opposition through bold and widespread action can stand in the way of positive change in the nation’s current physical activity, food, and other environments that influence individual behavior and choice. Awareness, will, and action on the part of the public and the business community/private sector, as well as government at all levels, must increase if the necessary changes are to occur.
Population behavior is influenced by several societal subsystems, including the economy, the political system, social institutions, and culture (de Silva-Sanigorski and Economos, 2010). To influence behavior on a broad societal level, multiple
subsystems must be targeted, and communities can be seen as important social forces in the process of change. As the broader society develops strategies to tackle the obesity epidemic, it will be able to draw on lessons learned from a range of successful social change efforts, such as those designed to increase breastfeeding rates, seat belt use, smoking cessation, and recycling (Economos et al., 2001). As described by de Silva-Sanigorski and Economos (2010, pp. 57-58) “key elements identified from these past successes include
• recognition that there was a crisis;
• major economic implications associated with the crisis;
• a science base including research, data, and evidence;
• sparkplugs, or leaders who can work for their cause through their knowledge, competence, talents, skills, and even charisma;
• coalitions to move the agenda forward and a strategic, integrated media advocacy campaign;
• involvement of the government at the state level to apply regulatory and fiscal authority, and at the local level to implement change;
• mass communication that includes consistent positive messages supported by scientific consensus and repeated in a variety of venues;
• policy and environmental changes that promote healthy lifestyle behaviors; and
• a plan that includes many components which work synergistically.”
Community-Level Engagement
Community engagement is a powerful vehicle for bringing about environmental and behavioral changes that will improve the health of the community and its members. It often involves partnerships and coalitions that help mobilize resources and influence systems, change relationships among partners, and serve as catalysts for changing policies, programs, and practices (CDC, 1997). As described later in this report, the recognition of social, cultural, and environmental factors influencing obesity has motivated a shift to community-level strategies for health promotion, with the understanding that change at this level will encourage and sustain individual-level behavior change. There is no consistent definition of a “community”; however, experience suggests that it may be defined as “a group of people sharing a common goal, interest, or identity—for example, culture, social, political, health, economic interests or a particular geographic association” (Bell et al., 2010, p. 233). Within the field of community health, this broad definition
gives way to two subclassifications of community: “communities of identity” (shared ethnicity, religion, illness) and “communities of location” (towns, cities, distinct neighborhoods) (Campbell and Murray, 2004; Israel et al., 2003).
Geographically defined communities hold diverse resources, ranging from the institutional (including worksites, places of worship, schools, and service and information providers), to the interpersonal (including peer networks, coalitions, and task forces), to community leaders and policy makers. Communities have their own history, social norms, traditions, and knowledge. These assets contribute points of leverage and resistance, intersections that spark strongly positive or negative reactions. Community-based interventions aim to apply community assets purposefully and efficiently to address an issue the community would like to resolve (Issel, 2009). Communities differ in their readiness or pre-existing capacity to address a given issue, such as obesity prevention, and those seeking to catalyze change in a community must employ different strategies for different readiness levels.
Community coalitions can be developed and supported to encourage the deep and meaningful engagement and organization of community members to realize systemic change at the local level (National Opinion Research Center, 2011). When people create or are involved in developing programs or policies, they value them more (Huang and Story, 2010). The formation of local, community-based coalitions can improve the reach and rate of information exchange nationally or at the societal level (Butterfoss et al., 1993).
Family/Household- and Individual-Level Engagement
The need for a major emphasis on change at the societal and community levels stems from the fact that many determinants of both voluntary and routine eating and physical activity behaviors are outside of the direct control of individuals and families. However, the ultimate success of changes at these levels depends on the extent to which the changes reach and are adopted and sustained by individuals and families. As described by Finegood (2011, p. 228), “given the heterogeneous nature of individuals and their environments, it is impossible to take individuals out of the solution equation.” This suggests it is important to consider the relationship between individuals/families and their environment to find effective solutions to obesity (Brownell et al., 2010). Engagement with individuals is foundational for achieving broad social action on obesity prevention in many ways. Children and adults, particularly caregivers, make decisions about their own physical activity and eating behaviors on a daily basis; they may also make decisions
that affect other people’s physical activity and food choices and environments, have responsibility for organizing the context in which people make such decisions (Finegood et al., 2010; Thaler and Sunstein, 2009), and take civic actions that influence policy makers. If individuals are engaged in the effort to accelerate obesity prevention, success is more likely to be achieved (Bar-Yam, 2004).
Building the awareness and will within households to influence the home environment and family dynamics positively with respect to physical activity and food choices is an essential part of changing the overall system. The reasons to foster will and action within households across the United States are especially clear in relation to prevention of obesity in children. Children learn to assimilate their parents’ health-related behaviors at a young age (Perryman, 2011). Furthermore, parents act as decision makers for their children in the areas of physical activity and nutrition. An estimated 66 percent of the caloric intake of children and adolescents occurs within the home (Poti and Popkin, 2011). Parents also serve as role models for their children, helping to shape physical activity values and behaviors, providing a sense of portion control and nutrient balance, and building related skills. For example, limiting children’s television time, using parental controls, and disallowing television in the bedroom can help reduce exposure to the marketing of unhealthy food products and reduce sedentary behavior.
Society benefits if all families have the social and material resources to raise their children to be healthy, educated, and productive members of their communities and nation. A healthy home environment can begin before conception with strong maternal nutrition, supported by other family members (IOM, 2005). It can prevent rapid early infant weight gain from ages 0 to 4 months, which has been shown to be a risk factor for childhood obesity (Birch and Davison, 2001; Stettler et al., 2003). And a healthy home environment can reach parents, grandparents, and extended family members, supporting a life-course perspective on obesity prevention.
The skill base for healthy living has eroded, however, and many people need support on parenting, cooking, and media use (Golan and Crow, 2004). Moreover, the resources available to parents to meet their children’s needs vary considerably. While the value of creating the optimal healthy environment for children is clear, society has largely left this responsibility to individual families, even though the financial or political resources to affect changes in major corporate interests, government programs, or policy generally are not available to individuals or individual families (Prilleltensky, 2010). For families to be able to raise healthy, well-educated children, communities and societal structures must assist in providing access to
opportunities for physical activity, healthy food, and adequate health care and other social services that support health (Scarr, 1996).
Reducing Disparities: Equity of Impact in Relation to Risk
Not all individuals, families, and communities are similarly situated with respect to environments that influence food and physical activity. A variety of characteristics historically linked to social exclusion or discrimination, such as race or ethnicity, religion, socioeconomic status, gender, age, mental health, disability, sexual orientation or gender identity, geographic location, and immigration status, are known to influence health status. In its 2011 Action Plan to Reduce Racial and Ethnic Health Disparities, the Department of Health and Human Services (HHS) highlights that health disparities “are closely linked with social, economic, and environmental disadvantage” and “are often driven by the social conditions in which individuals live, learn, work and play” (HHS, 2011, p. 1).
As described in Chapter 2, the burden of obesity is notably greater in racial/ethnic minority and low-income populations. A high level of community engagement and carefully targeted approaches will be particularly important to accelerate obesity prevention in such communities. In many parts of the United States, racial/ethnic minority and low-income individuals and families live, learn, work, and play in neighborhoods that lack sufficient health-protective resources, such as parks and open space, grocery stores, walkable streets, and high-quality schools (Adler et al., 2007; Iton et al., 2008). Additionally, community-level risk factors, including freeways, incinerators, ports, heavy industry, and other sources of noxious pollution, often are concentrated in these same places (Adler et al., 2007). This relative absence of health-promoting resources and disproportionate concentration of unhealthy risk factors contributes to increased levels of chronic stress among individuals experiencing these conditions (Iton et al., 2008), and this chronic stress is in turn associated with increased levels of sedentary activity and increased calorie consumption (Adler et al., 2007).
The persistence of concentrated health disparities in many American communities is strongly influenced by the relative paucity of community-based health improvement strategies focused on creating robust local participatory decision-making processes. In any given community, the relative mix of these community-level resources and risk factors is determined primarily through democratic local and regional land use decision-making processes; consequently, organized participation in these processes influences where these community resources and risks are located. Because of such factors as poverty, language barriers, and immigration
status, low-income, minority, and other disadvantaged population groups often are underrepresented and their concerns marginalized in these land use decision-making processes (Iton et al., 2008). These groups are therefore less likely to benefit from access to health-protective resources and more likely to live in proximity to noxious land uses. To change this inequitable resource and risk distribution, robust and long-term community engagement and civic participation among these disadvantaged populations must occur.
Responsibility for leading efforts to make the changes needed to prevent obesity potentially rests with everyone that can influence physical activity and food environments. There are obvious leaders that have traditionally been seen as having the responsibility for making environmental and policy changes to influence societal change, but the engagement of all individuals, families, communities, and society, as described in the previous section, may identify another set of willing and capable leaders whose actions will be necessary to achieve impact. Chapter 10 further details how taking a systems perspective helps define and identify leaders and how these leaders should approach implementing the necessary changes.
The committee’s vision, its decision to take a systems perspective, and its belief in the need for engagement and leadership at multiple levels and across multiple sectors help inform the issue of who is responsible for addressing the epidemic of obesity. Traditionally, obesity has been blamed on the failure of individuals to exercise personal responsibility (Brownell et al., 2010; Leichter, 2003). In addition, this view has been used as the basis for resisting government efforts—legislative and regulatory—to address the problem. Recently, the discourse has been reframed by Brownell and colleagues (2010) as a constructive approach to a controversial issue. They assert that “personal responsibility can be embraced as a value” (p. 378) by expanding its meaning to include such actions as improved school nutrition, menu labeling, changes in industry marketing practices, and even such controversial measures as taxes on foods and beverages that lead to the choice of healthier items. Such an approach could bridge the divide between views based on individual versus collective responsibility (Brownell et al., 2010). This train of thought argues for making obesity prevention a political priority that reestablishes the responsibility of the country—both the public and private sectors—to nurture
and protect children, and to support the health priorities of the adults and families who influence them and make the decisions that determine the overall physical activity and food environments.
The committee’s recommendations (outlined in Chapters 5-9) have the potential to accelerate progress in obesity prevention by identifying changes that are needed across all levels and sectors of society, but it is also important to view them as a whole—an interrelated system of critical areas in which changes are needed. The responsibility for implementing these changes is one that must be shared. Engagement and leadership across all levels and sectors of the population will be powerful vehicles for bringing about environmental and behavioral changes that can improve the health of the population.
The next two chapters provide background on and fundamentals of the problem of obesity, including an assessment of the current problem and how, in general, the problem is addressed at a population level. Chapter 2 describes the consequences of obesity; reviews current trends of overweight and obesity and societal trends that are drivers of excess weight gain at a population level; and outlines advances in and barriers to implementing environmental and policy changes that can help accelerate progress in obesity prevention. Chapter 3 describes the logic of obesity prevention, including goals and key pathways and targets for change, and explains the importance of taking a systems perspective on the problem. Chapters 2 and 3 are particularly geared toward audiences unfamiliar with the current situation regarding obesity and obesity prevention approaches from a societal perspective, but they also highlight several current issues that required the committee’s careful consideration in determining which strategies and actions to recommend. Chapter 4 then presents the methodology used by the committee in developing its recommendations. This chapter explains how the committee defined the concept of accelerating progress in obesity prevention in order to screen and evaluate the numerous interventions recommended in prior reports and to enhance or choose among these interventions, and highlights the importance of viewing the committee’s recommendations as an interrelated, synergistic system.
The remainder of the report presents the committee’s recommendations for accelerating progress in obesity prevention. The committee identified five critical action arenas—environments for change—for making progress in obesity prevention. Chapters 5 through 9 present recommendations under five respective goals, together with specific strategies, actions, and outcome indicators, in relation to
these five environments: environments for physical activity (Chapter 5); food and beverage environments (Chapter 6); message environments with respect to physical activity and healthy eating (Chapter 7); health care and work environments (Chapter 8); and school environments (Chapter 9). Chapter 10 concludes the report by addressing leadership and implementation, prioritization, and assessment of the committee’s recommendations in the context of a systems perspective.
Adler, N. E., J. Stewart, S. Cohen, M. Cullen, A. Diez Roux, W. Dow, G. Evans, I. Kawachi, M. Marmot, K. Matthews, B. McEwen, J. Schwartz, T. Seeman, and D. Williams. 2007. Reaching for a healthier life: Facts on socioeconomic status and health in the US. San Francisco, CA: The John D. and Catherine T. MacArthur Foundation Research Network on Socioeconomic Status and Health.
Bar-Yam, Y. 2004. Making things work: Solving complex problems in a complex world, edited by C. Ramalingam, L. Burlingame, and C. Ogata. Cambridge, MA: NECSI-Knowledge Press.
Bell, C., E. Elliott, and A. Simmons. 2010. Community capacity building. In Preventing childhood obesity. Evidence policy and practice, edited by E. Waters, J. C. Seidell, B. A. Swinburn, and R. Uauy. Hoboken, NJ: Wiley-Blackwell. Pp. 232-242.
Birch, L. L., and K. K. Davison. 2001. Family environmental factors influencing the developing behavioral controls of food intake and childhood overweight. Pediatric Clinics of North America 48(4):893-907.
Brownell, K. D., R. Kersh, D. S. Ludwig, R. C. Post, R. M. Puhl, M. B. Schwartz, and W. C. Willett. 2010. Personal responsibility and obesity: A constructive approach to a controversial issue. Health Affairs 29(3):379-387.
Butterfoss, F. D., R. M. Goodman, and A. Wandersman. 1993. Community coalitions for prevention and health promotion. Health Education Research 8(3):315-330.
Campbell, C., and M. Murray. 2004. Community health psychology: Promoting analysis and action for social change. Journal of Health Psychology 9(2):187-195.
CDC (Centers for Disease Control and Prevention). 1997. Principles of community engagement. Atlanta, GA: CDC/ATSDR Committee on Community Engagement.
de Onis, M., M. Blossner, and E. Borghi. 2010. Global prevalence and trends of overweight and obesity among preschool children. American Journal of Clinical Nutrition 92(5):1257-1264.
de Silva-Sanigorski, A. M., and C. Economos. 2010. Evidence of multi-setting approaches for obesity prevention: Translation to best practice. In Preventing childhood obesity: Evidence, policy, and practice, edited by E. Waters, J. C. Seidell, B. A. Swinburn, and R. Uauy. Hoboken, NJ: Wiley-Blackwell. Pp. 57-63.
Economos, C. D., R. C. Brownson, M. A. DeAngelis, P. Novelli, S. B. Foerster, C. T. Foreman, J. Gregson, S. K. Kumanyika, and R. R. Pate. 2001. What lessons have been learned from other attempts to guide social change? Nutrition Reviews 59(3 Pt. 2):S40-S56; discussion S57-S65.
Finegood, D. T. 2011. The complex systems science of obesity. In The Oxford handbook of the social science of obesity, edited by J. H. Cawley. New York: Oxford University Press. Pp. 208-236.
Finegood, D. T., T. D. N. Merth, and H. Rutter. 2010. Implications of the foresight obesity system map for solutions to childhood obesity. Obesity 18(Suppl. 1):S13-S16.
Finucane, M. M., G. A. Stevens, M. J. Cowan, G. Danaei, J. K. Lin, C. J. Paciorek, G. M. Singh, H. R. Gutierrez, Y. Lu, A. N. Bahalim, F. Farzadfar, L. M. Riley, and M. Ezzati. 2011. National, regional, and global trends in body-mass index since 1980: Systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9.1 million participants. Lancet 377(9765):557-567.
Flegal, K. M., M. D. Carroll, C. L. Ogden, and L. R. Curtin. 2010. Prevalence and trends in obesity among US adults, 1999-2008. Journal of the American Medical Association 303(3):235-241.
Golan, M., and S. Crow. 2004. Parents are key players in the prevention and treatment of weight-related problems. Nutrition Reviews 62(1):39-50.
HHS (U.S. Department of Health and Human Services). 2011. Action plan to reduce racial and ethnic health disparities. http://minorityhealth.hhs.gov/npa/files/Plans/HHS/HHS_Plan_complete.pdf (accessed October 25, 2011).
Huang, T. T., and T. A. Glass. 2008. Transforming research strategies for understanding and preventing obesity. Journal of the American Medical Association 300(15):1811-1813.
Huang, T. T. K., and M. T. Story. 2010. A journey just started: Renewing efforts to address childhood obesity. Obesity 18(Suppl. 1):S1-S3.
IOM (Institute of Medicine). 2005. Preventing childhood obesity: Health in the balance. Washington, DC: The National Academies Press.
IOM. 2007. Progress in preventing childhood obesity: How do we measure up? Washington, DC: The National Academies Press.
IOM. 2010. Bridging the evidence gap in obesity prevention: A framework to inform decision making. Washington, DC: The National Academies Press.
Israel, B. A., A. J. Schulz, E. A. Parker, A. B. Becker, A. J. I. Allen, and J. R. Guzman. 2003. Critical issues in developing and following community based participatory research principles. In Community-based participatory research for health, edited by M. Minkler and N. Wallerstein. San Francisco, CA: John Wiley & Sons. Pp. 53-76.
Issel, L. M. 2009. Health program planning and evaluation. A practical, systematic approach for community health. 2nd ed. Boston, MA: Jones and Bartlett Publishers.
Iton, T., S. Witt, and D. Kears. 2008. Life and death from unnatural causes. Health and social inequity in Alameda County. Oakland, CA: Alameda County Public Health Department.
Leichter, H. M. 2003. “Evil habits” and “personal choices”: Assigning responsibility for health in the 20th century. Milbank Quarterly 81(4):603-626.
National Opinion Research Center. 2011. Developing a conceptual framework to assess the sustainability of community coalitions post-federal funding. http://aspe.hhs.gov/health/reports/2010/sustainlit/report.shtml (accessed November 17, 2011).
Ogden, C. L., M. D. Carroll, L. R. Curtin, M. M. Lamb, and K. M. Flegal. 2010a. Prevalence of high body mass index in US children and adolescents, 2007-2008. Journal of the American Medical Association 303(3):242-249.
Ogden, C. L., M. M. Lamb, M. D. Carroll, and K. M. Flegal. 2010b. Obesity and socioeconomic status in children and adolescents: United States, 2005-2008. NCHS Data Brief (51):1-8.
Ogden, C. L., M. M. Lamb, M. D. Carroll, and K. M. Flegal. 2010c. Obesity and socioeconomic status in adults: United States, 2005-2008. NCHS Data Brief (50):1-8.
Perryman, M. L. 2011. Ethical family interventions for childhood obesity. Preventing Chronic Disease 8(5):A99.
Popkin, B. M., K. Duffey, and P. Gordon-Larsen. 2005. Environmental influences on food choice, physical activity and energy balance. Physiology and Behavior 86(5):603-613.
Poti, J. M., and B. M. Popkin. 2011. Trends in energy intake among US children by eating location and food source, 1977-2006. Journal of the American Dietetic Association 111(8):1156-1164.
Prilleltensky, I. 2010. Child wellness and social inclusion: Values for action. American Journal of Community Psychology 46(1-2):238-249.
Scarr, S. 1996. How people make their own environments: Implications for parents and policymakers. Psychology, Public Policy, and Law 2(2):204-228.
Stettler, N., S. K. Kumanyika, S. H. Katz, B. S. Zemel, and V.A. Stallings. 2003. Rapid weight gain during infancy and obesity in young adulthood in a cohort of African Americans. American Journal of Clinical Nutrition 77:1374-1378.
Thaler, R. H., and C. R. Sunstein. 2009. Nudge: Improving decisions about health, wealth and happiness. New York: Penguin Books.
















