2
Background on the Pipeline to the Physician Workforce
Abstract: This chapter serves as background for this report’s assessment of graduate medical education (GME) financing and governance. It reviews trends in the characteristics of GME trainees and considers whether the GME system is producing the type of physicians that the nation requires. The focus is on specialty distribution, geographic location, the ability to care for diverse patient populations, and physicians’ overall readiness to practice medicine in settings where most Americans receive their health care. The committee finds that the recent expansion in physician education has occurred with little strategic direction. Several areas need the attention of policy makers to ensure the strategic investment of public funding for GME programs. These include learning how to motivate young physicians to train in specialties and locate in areas where they are most needed; identifying ways to improve the diversity of the physician trainees to better mirror the overall population; increasing GME training in community settings; and ensuring that newly trained physicians possess the skills essential for everyday practice.
Physician education has made significant progress since Flexner revealed the poor quality of medical schools in the early 20th century (Flexner, 1910). The nation has a robust and productive GME system with significant capacity to produce the nation’s physician workforce. Yet, there are also widespread concerns—and differences of opinion—about the size, competencies, and makeup of the physician workforce (Cassel and Reuben,
2011; COGME, 2013; Cronenwett and Dzau, 2010; Crosson et al., 2011; Detsky et al., 2012; Saha, 2014; Saha et al., 2008; Weiss et al., 2013).
The objective of this chapter is twofold: first, to briefly describe trends in the pipeline to graduate medical education (GME) programs (allopathic, osteopathic, and international medical school graduates)1 and second, to review what is known about the “output” of today’s GME system (newly trained physicians entering practice). The overarching question in this chapter is to what extent the GME system is producing an appropriately balanced physician workforce ready to provide high-quality, patient-centered, and affordable health care. The subsequent chapters examine the central focus of this study—the impact of GME financing and governance of GME on this question.
The sufficiency of the physician supply—and the public’s future role in financing the production of a larger physician supply—are among today’s most contentious health workforce issues (Iglehart, 2013a; Nicholson, 2009). Determining future workforce requirements is an inherently imprecise activity (Bipartisan Policy Center, 2011). As Figure 2-1 illustrates, understanding the dynamics of physician supply involves many variables and uncertainties. Health care reimbursement and the organization of health care services, for example, are far more important than GME in determining the makeup and productivity of the physician supply (Salsberg, 2009). Nevertheless, the capacity of the GME system is a limiting factor because states require at least 1 year of residency training in the United States before a physician can obtain an unrestricted license to practice medicine (FSMB, 2013).
Although the committee was not charged with projecting the future demand for physicians, it reviewed recent projections and analyses of the capacity of the physician workforce to meet the nation’s health needs (AAMC Center for Workforce Studies; 2012; Altschuler et al., 2012; Colwill et al., 2008; Green et al., 2013; Hofer et al., 2011; Ku et al., 2011; Petterson et al., 2012; Ricketts, 2011). Forecasts of the future physician supply are variable and contradictory in part because it is difficult to anticipate future directions in the health care system (Blumenthal, 2004; Iglehart, 2013b). In the 1970s, for example, concern about imminent shortages led to a significant push for expansion in the number of medical schools and students (Cooper, 2003). Title VII of the Public Health Service Act
________________
1 Allopathic medical schools confer the Doctor of Medicine (M.D.) degree and are accredited by the Liaison Committee of Medical Education. Osteopathic medical schools confer the Doctor of Osteopathy (D.O.) degrees and are accredited by the American Osteopathic Association.
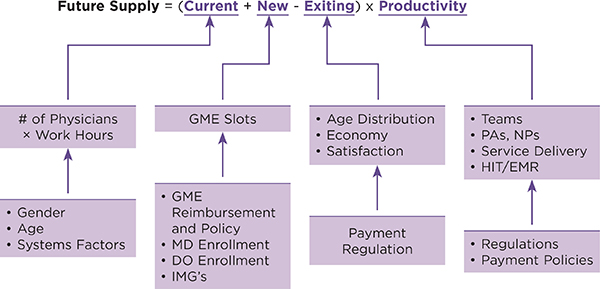
FIGURE 2-1 Physician supply: The complex reality.
NOTE: DO = doctor of osteopathy; EMR = electronic medical record; GME = graduate medical education; HIT = health information technology; IMG = international medical graduate; MD = medical doctor; NP = nurse practitioner; PA = physician assistant.
SOURCE: Salsberg, 2009 (AAMC State of the Physician Workforce Address).
provided significant funding for the expansion of medical schools (Phillips and Turner, 2012). From 1970 to 1984, the number of medical students increased by 66 percent and the number of residents by 25 percent. A decade later, the conventional wisdom was that the nation faced a significant oversupply of physicians because of the looming impact of managed care on demand for health care services (Fink et al., 2003; Pew Health Professions Commission, 1995).
More recently, projections of the physician supply suggest impending shortages that could prevent many people from getting needed health services. These analyses raise concerns that the rapid aging of the population and the expansion in health coverage in the Patient Protection and Affordable Care Act (ACA)2 will fuel demand for physician services far beyond current capacity (AAMC, 2012a; Grover and Niecko-Najjum, 2013; Kirch et al., 2012; Sheldon, 2010). However, the underlying methodologies and assumptions about the future in these studies are problematic. They often assume historic provider-patient ratios with limited relevance to either contemporary health care delivery or the pressing need for a more coordinated, affordable, and patient-centered health care system (Bipartisan Policy Center, 2011; Dower and O’Neill, 2011). Other analyses that con-
________________
2 Public Law 111-148.
sider the potential impact of changes in health care delivery draw opposite conclusions. These studies suggest that an expanded primary care role for physician assistants (PAs) and advanced practice registered nurses (APRNs), redesign of care delivery and other innovations in health care delivery, such as telehealth and electronic communication, may ultimately lessen the demand for physicians despite the aging of the population or coverage expansions (Auerbach et al., 2013a,b; Bodenheimer and Smith, 2013; Bodenheimer et al., 2009; Ghorob and Bodenheimer, 2012; Green et al., 2013; Reinhardt, 2013; Weiner et al., 2013).
In response to the forecasts of shortages, some stakeholders and policy makers are pushing for significant increases in Medicare GME funding. They argue that Medicare should raise the current cap on the number of Medicare-funded residency positions in order to ensure the production of more physicians (Grover and Niecko-Najjum, 2013; Jolly et al., 2013; Kirch et al., 2012). Yet, the available evidence suggests that increasing the production of physicians is not dependent on additional federal funding. A recent analysis of 20 years of residency data documents that, despite the implementation of Medicare caps on funded training slots in 1997, the number of first-year residency positions has grown steadily since 2003—at a rate of increase similar to the period before the caps (Chandra et al., 2014).
Some proponents of increased Medicare GME funding also claim that the number of medical school graduates will soon exceed the available GME training slots (Jolly et al., 2013). Recent evidence does not support this concern. According to the National Residency Matching Program (NRMP),3 about 3,500 new first-year Accreditation Council for Graduate Medical Education (ACGME)-accredited training slots have been created since 2010 (NRMP, 2014a,b). In the 2014 match, there were 7,000 more first-year residency slots than U.S. applicants: 22,300 U.S. allopathic and osteopathic medical school seniors applied for 1 of 29,666 first-year positions (Salsberg, 2014).
Simply increasing the numbers of physicians is unlikely to resolve workforce shortages in the regions of the country where shortages are most acute and is also unlikely to ensure a sufficient number of providers in all specialties and care settings. The evidence instead suggests that, although the capacity of the GME system has grown in recent years, it is not producing an increasing proportion of physicians who choose to practice primary care, to provide care to underserved populations, or to locate in rural
________________
3 The National Residency Matching Program (NRMP) is a private, non-profit corporation that matches applicants for ACGME-accredited training slots with ACGME-accredited training programs (NRMP, 2013). NRMP uses a computerized mathematical algorithm to match applicants’ preferences with the preferences of residency program directors at U.S. teaching hospitals.
or other underserved areas (Rabinowitz et al., 2012; Rosenblatt, 2010; Shipman et al., 2013; West and Dupras, 2012). Also, although the numbers of underrepresented minorities have increased, their proportion in medical school and physician populations does not reflect the increasing racial and ethnic diversity of the American population (AAMC, 2010, 2012a,b,c; Sullivan, 2010; Sullivan and Suez Mittman, 2010).
THE GME PIPELINE—MEDICAL SCHOOL ENROLLMENT
In the past decade, there has been a marked increase in the number of medical colleges (both allopathic and osteopathic) and the size of medical school classes. No one factor explains the expansion. Numerous studies in the 1990s predicting serious physician shortages probably had a role. It appears that much of the growth was spurred by local concerns—both public and private—about physician supply. For example, several states—including Arizona, Florida, Michigan, Pennsylvania, and Texas—invested in medical school expansion with the expectation that many graduates would remain to practice locally (Whitcomb, 2009, 2013).
In 2005, the Council on Graduate Medical Education (COGME) released an influential report predicting rapid increases in the demand for physician services with the aging of the baby boomer population, growing U.S. population, and expansions in health insurance coverage (COGME, 2005a). The following year, the Association of American Medical Colleges issued a call for a 30 percent increase in the physician supply (AAMC, 2006; Adler et al., 2013). Since then, the number of medical schools and school enrollments has grown substantially. As Table 2-1 indicates, in the decade ending in 2012, overall enrollment in U.S. undergraduate medical colleges rose by nearly 28 percent, increasing from 80,180 to 102,498 students (AAMC, 2013a). Both allopathic and osteopathic medicine have expanded class sizes at many schools and also built new medical schools. Fourteen allopathic medical schools increased class sizes by more than 10 percent in 2013 (AAMC, 2013b). The growth in osteopathic medical colleges has been even more dramatic. Enrollment in institutions that granted the Doctor of Osteopathy (D.O.) nearly doubled during the decade, increasing from 11,432 students to nearly 22,000 students.
In 2013 alone, four new allopathic and three osteopathic medical schools opened their doors (AAMC, 2013b). Additional growth is under way: As this report was prepared, five new allopathic medical schools have initiated applications for accreditation (LCME, 2013).
| 2002 | 2012 | 10-Year Change | ||
| Number | Percent | |||
| Number of medical colleges | 145 | 175 | 30 | 20.7 |
| Allopathic | 125 | 141 | 16 | 12.8 |
| Osteopathic | 20a | 34 | 14 | 70.0 |
| Students enrolled in U.S. medical colleges | 80,180 | 102,498 | 22,318 | 27.8 |
| Allopathic | 68,748 | 80,757 | 12,009 | 17.5 |
| Osteopathic | 11,432 | 21,741 | 10,309 | 90.2 |
| U.S. medical school graduate applicants to graduate medical education (GME) programs | 16,874b | 20,248c | 3,374 | 20.0 |
| International medical graduate (IMG) applicants to GME programs | 6,585 | 11,107 | 4,522 | 68.7 |
| U.S. citizen IMGs | 2,029 | 4,279 | 2,250 | 110.9 |
| Non–U.S. citizen IMG applicants | 4,556 | 6,828 | 2,272 | 49.9 |
| Total potential applicant pool for GME positions (U.S. plus IMGs) | 23,459 | 31,335 | 7,896 | 33.7 |
| Total potential applicant pool for GME positions (U.S. plus IMGs) | 23,459 | 31,335 | 7,896 | 33.7 |
aData from 2003-2004.
bClass of 2002-2003.
cIncludes seniors and previous graduates of U.S. allopathic medical schools, graduates of osteopathic medical schools, students and graduates of Canadian medical schools, and students and graduates of Fifth Pathway programs.
SOURCE: AACOM, 2012, 2013; AAMC, 2009, 2012b, 2013a; AOA, 2012; NRMP, 2002, 2012.
International Medical Graduates
In addition to the graduates of U.S. medical colleges, the GME pipeline also includes substantial numbers of graduates of international medical schools (referred to as IMGs), both U.S. citizens and foreign nationals. The IMG proportion of the GME applicant pool has been steadily increasing, as has the share of IMGs who are U.S. citizens. In 2012, fewer than two thirds of the GME applicant pool were graduates of U.S. medical schools (20,248, or 64.6 percent) (see Table 2-1) (NRMP, 2013). The remainder included
4,279 U.S. citizen graduates of international medical schools (13.6 percent), and 6,828 other international graduates (21.8 percent) (NRMP, 2013).
It is important to recognize the significant role of IMGs in U.S. health care; they make up a significant proportion of residents (27.0 percent) and practicing physicians (24.1 percent) (AAMC, 2013a). IMGs play a critical role in the health care of vulnerable populations because they are more likely to practice primary care and to locate in underserved regions of the country (Traverso and McMahon, 2012).
A concern, however, is that U.S. GME programs are contributing to a “brain drain” of physicians from low-income countries, as many of them do not return to their home country after residency training (Hagopian et al., 2004; Mullan, 2005).
Workforce planning involves gauging not only the numbers of needed personnel but also whether those with the right training are available “to deliver the right services to the right people at the right time” (Birch et al., 2009, p. S-56). Thus, to assess the output of the GME system, one should consider the capacity of the system to produce the types of physicians that will meet the health needs of a growing, aging, and diversifying population (Ricketts, 2011). This section provides a brief review of trends in the number and type of GME programs and the available evidence on key characteristics of the physician trainee population and recent GME graduates—by specialty and subspecialty, readiness to practice medicine in settings where most people seek health care, racial and ethnic diversity, and geographic location.
Numbers of GME Programs and Trainees
As noted earlier, the capacity of the GME system to train additional physicians has been growing. Both ACGME-accredited residency programs and residents have steadily increased in number over the last decade (see Table 2-2). Between academic years 2003-2004 and 2012-2013, the number of ACGME programs increased by 16.3 percent (from 7,968 to 9,265) and the number of residents by 17.5 percent (from 100,176 to 117,717). There were an additional 7,498 osteopathic physicians in 1,068 American Osteopathic Association (AOA)-accredited residencies in 2012-2013.4
________________
4 Osteopathic data were provided by personal communications from Konrad Miskowitz-Retz, Secretary, AOA, COCA, and Jim Swartwout, Executive Director, AOA, on March 17, 2014, and March 19, 2013, respectively.
TABLE 2-2 Growth in ACGME-Accredited Programs and Residents, Academic Years 2003–2004 to 2012–2013
| Academic Year | Increase | |||
| 2003–04 | 2012–13 | Number | Percent | |
| Number of ACGME-accredited programs | 7,968 | 9,265 | 1,297 | 16.3 |
| Initial residency period | 4,015 | 4,084 | 69 | 1.7 |
| Subspecialty programs | 3,953 | 5,181 | 1,228 | 31.1 |
| Number of residents in ACGME-accredited programs | 100,176 | 117,717 | 17,541 | 17.5 |
| Initial residency period | 85,513 | 97,155 | 11,642 | 13.6 |
| Subspecialty programs | 14,663 | 20,562 | 5,899 | 40.2 |
NOTE: ACGME = Accreditation Council for Graduate Medical Education.
SOURCE: Data drawn from ACGME, 2013.
Primary Care Training and Increasing Subspecialization in GME
The makeup of specialties and subspecialties5 in the American physician workforce has changed dramatically since the advent of Medicare and Medicaid GME funding. In the early 1960s, primary care doctors made up an estimated half of the physician workforce (COGME, 2010). In 2010, the percentage was roughly 33 percent (AHRQ, 2011).
In less than a generation—from 1999 to 2013—the number of specialty certificates issued by the American Board of Medical Specialties increased from 84 to 145 (see Table 2-3) (ABMS, 2013). Although some of the increase was due to the creation of new pipeline specialties (e.g., family medicine, emergency medicine), the greatest growth has been in subspecialty programs. As Table 2-2 indicates, the number of ACGME-accredited subspecialty programs rose by more than 30 percent from academic years 2003-2004 to 2012-2013. The number of fellows in subspecialty training grew by 40 percent.
The trend toward a highly specialized physician workforce is especially apparent in internal medicine (IM) (Cassel and Reuben, 2011). The proportion of IM residents interested in a primary care career has dropped precipitously. In 1998, 54 percent of third-year IM residents planned careers in general IM. By academic years 2009-2011, the percentage was only 21.5 percent (West and Dupras, 2012). After completing an IM
________________
5 Specialty terminology can be confusing. All physicians who successfully complete a residency program are considered specialists even if the specialty is a primary care specialty.
| Year | Number of Certificates |
| 1969 | 10 |
| 1979 | 20 |
| 1992 | 66 |
| 1996 | 74 |
| 1999 | 84 |
| 2013 | 145 |
SOURCE: ABMS, 2013.
residency, physicians can now pursue further training and certification in 22 subspecialties—5 of which are devoted just to heart disease (adult congenital heart disease, advanced heart failure and transplant cardiology, cardiovascular disease, clinical cardiology electrophysiology, and interventional cardiology) (see Table 2-4). The other IM subspecialties are adolescent medicine, critical care medicine, diabetes and metabolism, endocrinology, gastroenterology, geriatric medicine, hematology, hospice and palliative medicine, infectious disease, medical oncology, nephrology, pulmonary disease, rheumatology, sleep medicine, sports medicine, and transplant hepatology.
A similar trend has occurred in surgery as surgical residents increasingly eschew general surgery for subspecialty practice in vascular surgery, pediatric surgery, surgical critical care, surgery of the hand, hospice and palliative medicine, complex general surgical oncology, or thoracic surgery. From 2001 to 2010, the number of new general surgery residents who expected to enter practice without specialized training declined by 33.3 percent (Jolly et al., 2013).
See Table 2-4 for a list of selected pipeline specialties with numerous pathways to subspecialization.
Influences on Specialty Career Choice
There is a considerable literature—based largely on surveys, questionnaires, and other personal reports—describing factors that influence physicians’ decision specialty choice. The evidence suggests that a complex interplay of many variables, including expected future income (and
TABLE 2-4 Selected Pipeline Specialties (Initial Residency Period) with Five or More Subspecialties
| Pipeline Specialty | Number of Subspecialties | Subspecialties |
| Anesthesiology | 5 | Critical Care Medicine, Hospice and Palliative Medicine, Pain Medicine, Pediatric Anesthesiology, Sleep Medicine |
| Emergency Medicine | 8 | Anesthesiology Critical Care, Emergency Medical Services, Hospice and Palliative Medicine, Internal Medicine-Critical Care Medicine, Medical Toxicology, Pediatric Emergency Medicine, Sports Medicine, Undersea and Hyperbaric Medicine |
| Internal Medicine | 22 | Adolescent Medicine, Adult Congenital Heart Disease, Advanced Heart Failure and Transplant Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, Critical Care Medicine, Diabetes and Metabolism, Endocrinology, Gastroenterology, Geriatric Medicine, Hematology, Hospice and Palliative Medicine, Infectious Disease, Interventional Cardiology, Medical Oncology, Nephrology, Pulmonary Disease, Rheumatology, Sleep Medicine, Sports Medicine, Transplant Hepatology |
| Neurology | 9 | Brain Injury Medicine, Clinical Neurophysiology, Epilepsy, Hospice and Palliative Medicine, Neurodevelopmental Disabilities, Neuromuscular Medicine, Pain Medicine, Sleep Medicine, Vascular Neurology |
| Pediatrics | 14 | Adolescent Medicine, Cardiology, Child Abuse Pediatrics, Critical Care Medicine, Developmental-Behavioral Pediatrics, Emergency Medicine, Endocrinology, Gastroenterology, Hematology-Oncology, Infectious Diseases, Neonatal-Perinatal Medicine, Nephrology, Pulmonology, Rheumatology |
| Psychiatry | 10 | Addiction Psychiatry, Brain Injury Medicine, Child and Adolescent Psychiatry, Clinical Neurophysiology, Forensic Psychiatry, Geriatric Psychiatry, Hospice and Palliative Medicine, Pain Medicine, Psychosomatic Medicine, Sleep Medicine |
| Surgery | 8 | General Surgery, Vascular Surgery, Pediatric Surgery, Surgical Critical Care, Surgery of the Hand, Hospice and Palliative Medicine, Complex General Surgical Oncology, Thoracic and General Surgery Joint Pathway |
NOTE: Neurology and Psychiatry are both governed by the American Board of Psychiatry and Neurology.
SOURCES: ABIM, 2014; ABR, 2014; American Board of Anesthesiology, 2013; American Board of Emergency Medicine, 2014; American Board of Pediatrics, 2014; American Board of Psychiatry and Neurology, 2013; American Board of Surgery, 2014.
physician payment rules that favor certain specialties and subspecialties), the prestige of the specialty (or lack of it for primary care), medical educators’ bias against primary care, design and location of residency programs, the personal desire for clearly defined responsibilities, lifestyle considerations, medical school debt, demographic factors, and practice location (Chen et al., 2013; Cordasco et al, 2009; Diehl et al., 2006; Dowdy, 2011; Garibaldi et al., 2005; Greysen et al., 2011; Hauer et al., 2008; Jeffe et al., 2010; Kussmaul, 2013; Phillips et al., 2009; Schwartz et al., 2011; Warm and Goetz, 2013; West et al., 2009).
The income differentials between various specialties and/or subspecialties are substantial (Bodenheimer et al., 2007; COGME, 2010; Vaughn et al., 2010) and a particularly strong influence on career choice (Ebell, 2008; Weida et al., 2010). For example, an analysis comparing the present value of career wealth (up to age 65) between a primary care physician and a cardiologist estimated a differential of more than $2.7 million (Vaughn et al., 2010). Other studies have documented annual income differentials ranging from about $100,000 to several hundred thousand depending on the subspecialty (Bodenheimer et al., 2007; COGME, 2010; Ebell, 2008).
Regardless, it is clear is that the GME system’s production of specialists and subspecialists has evolved without strategic direction in relation to the nation’s health needs. The overriding influences are the personal career choices of individual trainees and the decisions of teaching hospitals regarding what type of residencies to sponsor. As the next chapter will describe, Medicare GME funding is not linked in any way with local, regional, or national health care workforce priorities.
Primary Care Physicians
Many experts are concerned that the rapid transition to a highly specialized physician workforce has undermined the nation’s capacity to progress to a higher-quality and less costly health care system. The corresponding evidence, however, is inconclusive (Baicker and Chandra, 2004; Chang et al., 2011; Detsky et al., 2012). Regardless, the crucial issue is not necessarily the declining numbers of primary care physicians but effective organization, deployment of health personnel, and integration of primary care with other health care services. A growing body of literature demonstrates that the Patient-Centered Medical Home (PCMH) and other well-integrated delivery models provide higher-quality and more cost-effective care than the less coordinated systems of care typical of U.S. health care delivery (Gilfillan et al., 2010; IOM, 2012a; Liss et al., 2013; Maeng et al., 2012; Reid and Larson, 2012). There is also compelling evidence that integrating mental health and substance use services into primary care
improves outcomes, particularly for older adults with depression or at-risk drinking (IOM, 2012b).
Physicians make up approximately 74 percent of the primary care workforce; nurse practitioners, 19 percent; and PAs, 7 percent (Dower and O’Neill, 2011). No one ideal staffing mix for delivering effective primary care services has been determined. A variety of workforce models suggests that innovative mixes of primary care personnel—including greater use of APRNs, PAs, and team-based task delegation—may reduce the demand for primary care physicians in the future (Altschuler et al., 2012; Auerbach et al., 2013a,b; Bodenheimer and Pham, 2010; Bodenheimer and Smith, 2013; Bodenheimer et al., 2009; Ghorob and Bodenheimer, 2012). The PCMH model, for example, uses interprofessional teams of physicians, advanced practice nurses, physician assistants, pharmacists, nutritionists, social workers, health educators, and care coordinators to provide primary care. In nurse-managed health centers, nurse practitioners provide primary care services (Auerbach et al., 2013a). The role of the physician may vary from being central to a more consultative role (Patel et al., 2013).
Readiness to Practice
Many experts have observed that new physicians often lack sufficient training and experience in care coordination, team-based care, costs of care, cultural competence, and quality improvement (Center for Total Health, 2011). Various surveys indicate that recently trained physicians lack essential skills for office-based practice (Cordasco et al., 2009; Crosson et al., 2011a; MedPAC, 2009, 2010). A survey of the clinical department chiefs in IM, pediatrics, general surgery, and obstetrics/gynecology in Kaiser Permanente’s Northern California region, for example, found that new physicians had difficulties in managing routine conditions (e.g., care of minor depression and anxiety, minor chronic pain, certain acute musculoskeletal problems, basic dermatological conditions, and headaches) and performing simple procedures provided in outpatient settings (Crosson et al., 2011a).
In addition, although cultural competence is increasingly recognized as a core competency for all health providers (National Quality Forum, 2009; Wilson-Stronks et al., 2008), surveys of residents suggest that trainees feel ill prepared to provide culturally competent care to diverse populations (Betancourt et al., 2007; Weissman et al., 2005).
Other surveys have found little awareness of the costs of diagnostic procedures among residents and faculty (Patel et al., 2014; Sehgal and Gorman, 2011).
Both allopathic and osteopathic medicine have undertaken ambitious initiatives to remodel the system for accrediting residency training
programs,6 in part, to better prepare physicians for practice in real world settings (Buser and Hahn, 2013; Nasca et al., 2010). The ACGME is currently implementing its “Next Accreditation System” (NAS) for all specialties. The new system was specifically developed to enhance the ability of the accreditation process to promote the training of physicians for practice in the 21st century. Assessments of educational outcomes and the clinical learning environment are key components of the NAS and are based on six core competencies—patient care, medical knowledge, practice-based learning and improvement, interpersonal and communication skills, professionalism, and systems-based practice (Nasca et al., 2010, 2014a,b).
In 2013, the AOA issued a “New Pathway of Medical Education,” a blueprint for training osteopathic primary care physicians ready to practice in contemporary health care settings (Buser and Hahn, 2013; Shannon et al., 2013). The Pathway builds on five core principles: (1) team-based, patient-centered care; (2) competency-based curriculum; (3) continuous, longitudinal education; (4) clinical experiences in a variety of settings; and (5) a focus on health care delivery science.
Training Site
Some of the problems related to readiness to practice may stem from the nature of the sites where physicians are trained. There is a striking contrast between the sites where residents train compared with the sites where they are likely to spend most of their careers (Sisson and Dalal, 2011). Nearly all GME training occurs in the hospital—even in primary care residencies. Wynn and colleagues (2013) analyzed the GME data that teaching hospitals submitted to Medicare in 2012. The researchers found that only 53 percent of primary care residents train in hospitals that provide training opportunities in non-hospital settings.
The Teaching Health Center (THC) program,7 established in the ACA, is one step toward expanding residency training in community settings. Unlike the Medicare program, which funnels GME funding through teaching hospitals to support residency training, the THCs receive GME funding for primary care residencies directly from the Health Services and Resources Administration (Chen et al., 2012). It is too soon to know if training in these sites will ameliorate some of the readiness issues, and evaluation of these outcomes is important. Unfortunately, however, the authorization for the program’s appropriations will expire in FY 2015 and its long-term prospects are uncertain. In academic year 2013, 333 residents in 45 residency
________________
6 See Chapter 4 for a discussion of GME governance including accreditation.
7 Chapter 3 provides more details on the funding of the THC program.
programs in 21 states were supported by THC awards (HRSA, 2013). Most of the funded programs are in family medicine.
Diversity of the Physician Trainee Pool
Producing a physician workforce that reflects the diversity of the American population has been a goal of medical schools, teaching hospitals, policy makers, and the health care professions for many years (AAMC and ASPH, 2012; COGME, 1998, 2005b; Grumbach and Mendoza, 2008; IOM, 2003a, 2004; Nivet and Berlin, 2013; Saha, 2014; Saha and Shipman, 2008). The importance of these efforts is underscored by strong evidence that racial, ethnic, and linguistic diversity among health care providers is correlated with better access to and quality of care for underserved populations (Grumbach and Mendoza, 2008). In addition, nearly two decades of research have documented that non-white physicians disproportionately care for underserved groups and racial and ethnic minority populations (IOM, 2003b; Komaromy et al., 1996; Marrast et al., 2013; Moy and Bartman, 1995). Recent studies also suggest that a more diverse student and faculty presence can enhance the learning environment of all students by providing formative multicultural experiences (Saha et al., 2008; Shaw, 2005).
The challenge in ensuring a diverse physician workforce is daunting. Real progress has been made; the numbers of underrepresented minorities in U.S. medical schools have increased. However, with the growing diversity of the overall U.S. population, the racial and ethnic differences between medical school graduates and the overall population is actually widening (as illustrated in Figure 2-2). In 2012, there were 5,630 African American and 7,225 Hispanic students in U.S. medical schools, representing 6.9 percent and 8.8 percent of total enrollment, respectively (AAMC, 2012c). The Census Bureau projects that, by 2015, 38 percent of the U.S. population will be persons who identify as a racial minority or of Hispanic background, and this proportion will rise to 51 percent by 2045 (U.S. Census Bureau, 2012). In some states and geographic regions, the contrast between the racial and ethnic makeup of the physician and overall population is especially striking. In California, for example, 36 percent of the population is Hispanic, compared with only 5 percent of the state’s physicians (UCLA International Medical Graduate Program, 2013).
Achieving greater income diversity in the GME pipeline is also a concern. More than 75 percent of medical students come from the two highest quintiles of family incomes, and only 5.5 percent have come from families in the lowest quintile of income ($19,178 or less in 2006) (AAMC, 2013b; Jolly, 2008).
There is promising evidence that GME programs can modify recruitment practices to attract competitive underrepresented minorities (Auseon
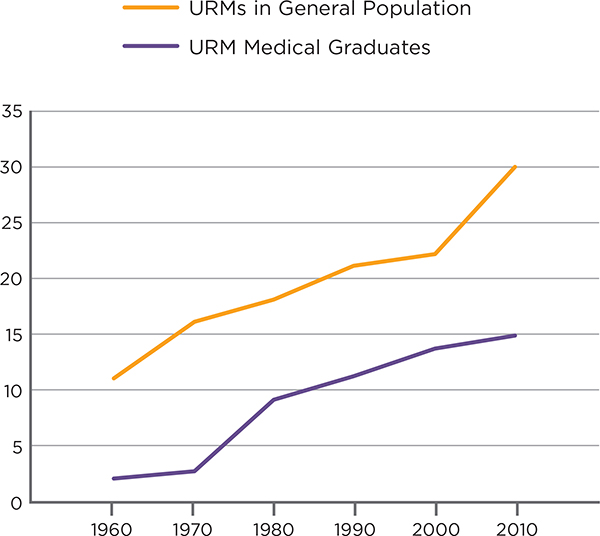
SOURCE: Sullivan, 2010 (AAMC).
et al., 2013). However, the GME system has limited leverage because the trainee population depends on the pipeline that begins with premedical education. Therefore, most diversity initiatives focus on interventions early in the physician education continuum—during application to medical school, college, or even earlier (Nivet and Berlin, 2013).
The lack of research on the effectiveness of diversity interventions is a major barrier to progress. Despite the decades of efforts to address the problem, little is actually known about what works.
Geographic Maldistribution
Physicians—whether primary care clinicians or subspecialists—live and practice primarily in suburban and metropolitan areas. Although about 19 percent of the U.S. population live in rural areas8 (U.S. Census Bureau,
________________
8 The U.S. Census Bureau defines rural as any population, housing, or territory outside urban areas.
2013), just 11 percent of physicians practice in these areas9 (Chen et al., 2010) and only 2.9 percent of medical students envision practicing in a rural or small-town environment (Fordyce et al., 2012; Rabinowitz et al., 2008; Rosenblatt et al., 2010). The proportion of medical students with rural backgrounds has declined in the past decade: In 1999-2001, 6.7 percent of medical students had rural backgrounds compared with 4.1 percent in 2009-2011 (Shipman et al., 2013).
The lack of sufficient numbers of all types of health care personnel in less populated areas has been a constant and seemingly unyielding problem in the United States (IOM, 1996; Rabinowitz et al., 2012; Ricketts, 2013). Indeed, it is a persistent and largely unsolved issue worldwide. It is unlikely that improving access to health care in American rural (or other underserved) areas can be achieved solely by expanding the overall pool of physicians. Recent experience demonstrates that simply producing more physicians has little impact on the problem. Most new physicians locate in cities and suburbs, including areas with a surplus of clinicians in their particular specialty.
The location of one’s medical school and GME training are predictive of practice location, and the longer the period of training is in a particular geographic area, the more likely the individual is to practice there, although it is not clear what factors actually drive this relationship (such as the relative influence of college, medical school, or residency training location). In 2012, states retained nearly half of the physicians (47.4 percent) graduating from the state’s residency programs and 66.6 percent of those who completed both undergraduate and graduate medical education in the state (AAMC, 2013a). Other influences on practice location in underserved geographic areas include exposure to rural or underserved populations during training, related curriculum and experience during training, growing up in a rural or underserved area, and closeness of a prospective practice location to one’s hometown (Barrett et al., 2011; Bazemore et al., 2009; Chen et al., 2010; Phillips et al., 2013; Quinn et al., 2011; Rabinowitz et al., 2005, 2008, 2012).
As with the challenge of improving diversity, no interventions have been tested to identify effective ways of deploying physicians in rural health care settings. Conducting the necessary research will depend, in part, on modifying current Medicare GME payment rules because, under the current system, the geographic distribution of Medicare-funded GME training slots primarily is essentially frozen based on the location of residencies in 1996.10
________________
9 Chen et al. (2010) mapped zip codes to Rural-Urban Community Area codes to determine rural residence.
10 Chapter 3 describes Medicare payment rules that affect the geographic location of trainees.
The United States has a robust GME system, emulated by many other nations, with significant capacity to produce the nation’s physician workforce. GME programs are increasingly producing a highly specialized workforce. It is notable that growth in the number of specialties and subspecialties is occurring without any coordinated planning. This chapter’s examination of the makeup and output of the GME pipeline indicates that the trend toward greater specialization has occurred with little strategic direction—at least with respect to local, regional, and national needs for a balance of primary care practitioners and subspecialists. The number of physician trainees is increasing, but there is little evidence to suggest that the expansion in training capacity is in areas—either geographically or by specialty—where they are most needed.
The proportions of internal medicine residents pursuing careers in general internal medicine and of surgery residents pursuing careers in general surgery have markedly declined. Less than 3 percent of medical students expect to practice in a rural or small-town environment, where physician shortages are most acute.
The United States is rapidly becoming one of the most racially and ethnically diverse nations in the world, but the gap between the diversity among physician trainees compared with the overall population is actually widening. In addition, residents report that they feel ill-prepared to provide culturally competent care to diverse populations.
Much attention of late has focused on the possibility of future shortages in primary care and other specialties nationwide. But this concern is based on studies with unreliable methodologies that do not adequately relate the demand for physicians to the features of a high-performing system of care and that also ignore the regional variations in workforce supply. In contrast, too little focus has been given to how best to organize and deploy physicians through innovative approaches to care delivery. Much remains to be learned. But no interventions have been tested to identify what works to resolve persistent problems such as how to motivate young physicians to train in specialties and locate in areas where they are most needed or ways to reverse the widening gap between the diversity of the physician trainee population compared with the overall population.
Finally, and particularly concerning, is the evidence that recent GME graduates do not have some of the essential skills for office-based practice, where most of them will spend their careers. This is likely due, in part, to the overwhelming emphasis of current GME programs on training physicians in hospitals rather than in community settings.
In summary, there is a clear and compelling imperative for the nation to leverage its investment in GME toward producing a physician workforce
ready to provide high-quality, patient-centered, and affordable health care in all regions of the nation.
AACOM (American Association of Colleges of Osteopathic Medicine). 2012. Trends in osteopathic medical school applicants, enrollment and graduates. http://www.aacom.org/data/Documents/Trends-apps-enroll-grads.pdf (accessed December 27, 2013).
AACOM. 2013. Fast facts about osteopathic medical education preliminary enrollment report—Fall 2013. http://www.aacom.org/data/Documents/Prelim%20Enroll%20Report%202013%20fast%20facts.pdf (accessed October 24, 2013).
AAMC (Association of American Medical Colleges). 2006. AAMC calls for 30 percent increase in medical school enrollment. https://www.aamc.org/newsroom/newsreleases/2006/82904/060619.html (accessed April 26, 2013).
AAMC. 2009. Medical school enrollment plans through 2013: Analysis of the 2008 AAMC Survey. https://www.aamc.org/download/82788/data/enrollmentreport.pdf (accessed January 28, 2014).
AAMC. 2010. Diversity in the physician workforce. Facts and figures 2010. https://members.aamc.org/eweb/upload/Diversity%20in%20the%20Physician%20Workforce%20Facts%20and%20Figures%202010.pdf (accessed April 18, 2013).
AAMC. 2012a. Diversity resources and data snapshots. Washington, DC: AAMC.
AAMC. 2012b. Table 29: Total U.S. medical school graduates by race and ethnicity, permanent residency, and sex, 2003-2012. https://www.aamc.org/download/321536/data/2012factstable29.pdf (accessed January 29, 2014).
AAMC. 2012c. Table 31: Total enrollment by U.S. medical school and race and ethnicity, 2012. https://www.aamc.org/download/321540/data/2012factstable31.pdf (accessed February 9, 2014).
AAMC. 2013a. 2013 state physician workforce data book. Table 10. https://members.aamc.org/eweb/upload/State%20Physician%20Workforce%20Data%20Book%202013%20%28PDF%29.pdf (accessed November 26, 2013).
AAMC. 2013b. Physician education debt and the cost to attend medical school. Washington, DC: AAMC.
AAMC and ASPH (Association of Schools of Public Health). 2012. Cultural competence education for students in medicine and public health. Report of an expert panel. Washington, DC: AAMC and ASPH.
AAMC Center for Workforce Studies. 2012. Recent studies and reports on physician shortages in the United States. Washington, DC: AAMC.
ABIM (American Board of Internal Medicine). 2014. About ABIM. http://www.abim.org/about (accessed February 6, 2014).
ABMS (American Board of Medical Specialties). 2013. Expansion of specialties and growth of subspecialties. http://www.abms.org/About_ABMS/ABMS_History/Extended_History/Expansion.aspx (accessed December 21, 2013).
ABPN (American Board of Psychiatry and Neurology). 2013. American Board of Psychiatry and Neurology, Inc. http://www.abpn.com (accessed February 6, 2014).
ABR (American Board of Radiology). 2014. About the ABR. Radiology specialties and subspecialties. http://www.theabr.org/radiology-specialties-and-subspecialties (accessed February 6, 2014).
ACGME (Accreditation Council for Graduate Medical Education). 2013. Data resource book: Academic year 2012-2013. http://acgme.org/acgmeweb/Portals/0/PFAssets/PublicationsBooks/2012-2013_ACGME_DATABOOK_DOCUMENT_Final.pdf (accessed January 28, 2014).
Adler, B., W. S. Biggs, and A. W. Bazemore. 2013. State patterns in medical school expansion, 2000-2010: Variation, discord, and policy priorities. Academic Medicine 88(12): 1849-1854.
AHRQ (Agency for Healthcare Research and Quality). 2011. Primary care workforce facts and stats no. 1. The number of practicing primary care physicians in the United States. http://www.ahrq.gov/research/findings/factsheets/primary/pcwork1/pcwork1.pdf (accessed May 19, 2014).
Altschuler, J., D. Margolius, T. Bodenheimer, and K. Grumbach. 2012. Estimating a reasonable patient panel size for primary care physicians with team-based task delegation. Annals of Family Medicine 10(5):396-400.
American Board of Anesthesiology. 2013. The American Board of Anesthesiology. http://www.theaba.org/home/examinations_certifications (accessed February 6, 2014).
American Board of Emergency Medicine. 2014. Subspecialties at a glance, February 2014. http://www.abem.org/public/docs/default-source/default-document-library/subspecialtiesat-a-glance-february-2014.pdf (accessed February 6, 2014).
American Board of Pediatrics. 2014. Certifications and admission requirements. https://www.abp.org/ABPWebStatic/?anticache=0.8886296769657027#murl%3D%2FABPWebStatic%2Ftakeexamsub.html%26surl%3D%2Fabpwebsite%2Ftakeexam%2Fsubspecialtycertifyingexam%2Fadmissionrequirements.htm (accessed February 6, 2014).
American Board of Surgery. 2014. Latest ABS news. http://www.absurgery.org/default.jsp?index (accessed February 6, 2014).
AOA (American Osteopathic Association). 2012. 2012 osteopathic profession report. http://www.osteopathic.org/inside-aoa/about/aoa-annual-statistics/Documents/2012-OMPreport.pdf (accessed December 28, 2013).
Auerbach, D. I., P. G. Chen, M. W. Friedberg, R. Reid, C. Lau, P. I. Buerhaus, and A. Mehrotra. 2013a. Nurse-managed health centers and patient-centered medical homes could mitigate expected primary care physician shortage. Health Affairs 32(11):1933-1941.
Auerbach, D. I., P. G. Chen, M. W. Friedberg, R. O. Reid, C. Lau and A. Mehrotra. 2013b. New approaches for delivering primary care could reduce predicted physician shortage. Santa Monica, CA: RAND Health.
Auseon, A. J., A. J. Kolibash, and Q. Capers. 2013. Successful Efforts to Increase Diversity in a Cardiology Fellowship Training Program. Journal of Graduate Medical Education 5(3):481-485.
Baicker, K., and A. Chandra. 2004. The productivity of physician specialization: Evidence from the Medicare program. American Economic Review 94(2):357-361.
Barrett, F. A., M. S. Lipsky, and M. N. Lutfiyya. 2011. The impact of rural training experiences on medical students: A critical review. Academic Medicine 86(2):259-263.
Bazemore, A., K. Bennett, M. S. Dodoo, C. Legagneur, S. Petterson, J. Phillips, R. L. Phillips, J. A. Rudd, and I. Xierali. 2009. Specialty and geographic distribution of the physician workforce—what influences medical student and resident choices? Washington, DC: The Robert Graham Center.
Betancourt, J., J. S. Weissman, M. Kim, E. R. Park, and A. W. Maina. 2007. Resident physicians’ preparedness to provide cross-cultural care: Implications for clinical care and medical education policy. http://www.commonwealthfund.org/usr_doc/1026_Betancourt_resident_MDs_preparedness_provide_cross-cultural_care.pdf (accessed December 9, 2013).
Bipartisan Policy Center. 2011. The complexities of national health care workforce planning: A review of current data and methodologies and recommendations fopr future studies. Washington, DC: Deloitte Center for Health Solutions.
Birch, S., G. Kephart, G. T. Murphy, L. O’Brien-Pallas, R. Alder, and A. MacKenzie. 2009. Health human resources planning and the production of health: Development of an extended analytical framework for needs-based health human resources planning. Journal of Public Health Management and Practice 15(Nov (Suppl)):S56-S61.
Blumenthal, D. 2004. New steam from an old cauldron: The physician-supply debate. New England Journal of Medicine 350(17):1780-1787.
Bodenheimer, T., R. A. Berenson, and P. Rudolf. 2007. The primary care–specialty income gap: Why it matters. Annals of Internal Medicine 146:301-306. doi:10.7326/00034819-146-4-200702200-00011.
Bodenheimer, T. S., and H. H. Pham. 2010. Primary care: Current problems and proposed solutions. Health Affairs 29(5):799-805.
Bodenheimer, T. S., and M. D. Smith. 2013. Primary care: Proposed solutions to the physician shortage without training more physicians. Health Affairs 32(11):1881-1886.
Bodenheimer, T. S., E. Chen, and H. D. Bennett. 2009. Confronting the growing burden of chronic disease: Can the U.S. health care workforce do the job? Health Affairs 28(1):64-74.
Buser, B. R., and M. B. Hahn. 2013. Building the future: Educating the 21st century physician. http://mededsummit.net/uploads/BRC_Building_the_Future__Educating_the_21st_Century_Physician__Final_Report.pdf (accessed October 20, 2013).
Cassel, C. K., and D. B. Reuben. 2011. Specialization, subspecialization, and subsubspecialization in internal medicine. New England Journal of Medicine 364(12):1169-1173.
Center for Total Health. 2011. Synopsis of Roundtable on Physician Readiness for a Reformed Delivery System. Washington, DC: Center for Total Health.
Chandra, A., D. Khullar, and G. R. Wilensky. 2014. The economics of graduate medical education. New England Journal of Medicine 370:2357-2360.
Chang, C. H., T. A. Stukel, A. B. Flood, and D. C. Goodman. 2011. Primary care physician workforce and Medicare beneficiaries’ health outcomes. JAMA 306(2):162.
Chen, C., F. Chen, and F. Mullan. 2012. Teaching health centers: A new paradigm in graduate medical education. Academic Medicine 87(12):1752-1756.
Chen, C., I. Xierali, K. Piwnica-Worms, and R. Phillips. 2013. The redistribution of graduate medical education positions in 2005 failed to boost primary care or rural training. Health Affairs 32(1):102-110.
Chen, F., M. Fordyce, S. Andes, and L. G. Hart. 2010. Which medical schools produce rural physicians? A 15-year update. Academic Medicine 85(4):594-598.
COCA (Commission on Osteopathic College Accreditation). 2013. New and developing COMs and campuses. https://www.osteopathic.org/inside-aoa/accreditation/predoctoral%20accreditation/Documents/new-and-developing-colleges-of-osteopathic-medicine-andcampuses.pdf (accessed January 28, 2014).
COGME (Council of Graduate Medical Education). 1998. Twelfth report. Minorities in medicine. Rockville, MD: HRSA.
COGME. 2005a. Sixteenth report: Physician workforce policy guidelines for the United States. Rockville, MD: HRSA.
COGME. 2005b. Twelfth report: Minorities in medicine: An ethnic and cultural challenge for physician training: An update. Rockville, MD: HRSA.
COGME. 2010. Twentieth report: Advancing primary care. Rockville, MD: HRSA.
COGME. 2013. Twenty-first report: Improving value in graduate medical education. http://www.hrsa.gov/advisorycommittees/bhpradvisory/cogme/Reports/twentyfirstreport.pdf (accessed August 12, 2013).
Colwill, J. M., J. M. Cultice, and R. L. Kruse. 2008. Will generalist physician supply meet demands of an increasing and aging population? Health Affairs 27(3):w232-w241.
Cooper, R. A. 2003. Medical schools and their applicants: An analysis. Health Affairs 22(4):71-84.
Cordasco, K. M., M. Horta, N. Lurie, C. E. Bird, and B. O. Wynn. 2009. How are residency programs preparing our 21st century internists? A study conducted by staff from RAND Health for the Medicare Payment Advisory Commission. http://www.medpac.gov/documents/Jul09_ResidencyPrograms_CONTRACTOR_CB.pdf (accessed April 2, 2013).
Cronenwett, L., and V. J. Dzau, (Eds.). 2010. Who will provide primary care and how will they be trained? Proceedings of a conference sponsored by the Josiah Macy Jr. Foundation, Durham, NC, January 8-11.
Crosson, F. J., J. Leu, B. M. Roemer, and M. N. Ross. 2011. Gaps in residency training should be addressed to better prepare doctors for a twenty-first-century delivery system. Health Affairs 30(11):2142-2148.
Detsky, A., S. R. Gauthier, and V. R. Fuchs. 2012. Specialization in medicine: How much is appropriate? JAMA 307(5):463-464.
Diehl, A. K., V. Kumar, A. Gateley, J. L. Appleby, and M. E. O’Keefe. 2006. Predictors of final specialty choice by internal medicine residents. Journal of General Internal Medicine 21(10):1045-1049.
Dowdy, D. W. 2011. Trained to avoid primary care. Annals of Internal Medicine 154(11): 776-777.
Dower, K., and E. O’Neill. 2011. Primary care health workforce in the United States. http://www.rwjf.org/content/dam/farm/reports/issue_briefs/2011/rwjf402104/subassets/rwjf402104_1 (accessed November 1, 2012).
Ebell, M. H. 2008. Future salary and US residency fill rate revisited. JAMA 300(10):1131-1132.
Fink, K. S., R. L. Phillips, G. E. Fryer, and N. Koehn. 2003. International medical graduates and the primary care workforce for rural underserved areas. Health Affairs 22(2):255-262.
Flexner, A. 1910. Medical education in the United States and Canada: A report to the Carnegie Foundation for the Advancement of Teaching. New York: Carnegie Foundation for the Advancement of Teaching.
Fordyce, M. A., M. P. Doescher, F. M. Chen, and L. G. Hart. 2012. Osteopathic physicians and international medical graduates in the rural primary care physician workforce. Family Medicine 44(6):396-403.
FSMB (Federation of State Medical Boards). 2013. State-specific requirements for initial medical licensure. http://www.fsmb.org/usmle_eliinitial.html (accessed January 9, 2014).
Garibaldi, R. A., C. Popkave, and W. Bylsma. 2005. Career plans for trainees in internal medicine residency programs. Academic Medicine 80(5):507-512.
Ghorob, A., and T. Bodenheimer. 2012. Sharing the care to improve access to primary care. New England Journal of Medicine 366(21):1955-1957.
Gilfillan, R. J., J. Tomcavage, M. B. Rosenthal, D. E. Davis, J. Graham, J. A. Roy, S. B. Pierdon, F. J. Bloom, T. R. Graf, R. Goldman, K. M. Weikel, B. H. Hamory, R. A. Paulus, and G. D. Steele. 2010. Value and the medical home: Effects of transformed primary care. American Journal of Managed Care 16(8):607-614.
Green, L. V., S. Savin, and Y. Lu. 2013. Primary care physician shortages could be eliminated through use of teams, nonphysicians, and electronic communication. Health Affairs 32(1):11-19.
Greysen, S. R., C. Chen, and F. Mullan. 2011. A history of medical student debt: Observations and implications for the future of medical education. Academic Medicine 86(7):840-845.
Grover, A., and L. M. Niecko-Najjum. 2013. Building a health care workforce for the future: More physicians, professional reforms, and technological advances. Health Affairs 32(11):1922-1927.
Grumbach, K., and R. Mendoza. 2008. Disparities in human resources: Addressing the lack of diversity in the health professions. Health Affairs 27(2):413-422.
Hagopian, A., M. J. Thompson, M. Fordyce, K. E. Johnson, and L. G. Hart. 2004. The migration of physicians from sub-Saharan Africa to the United States of America: Measures of the African brain drain. Human Resources for Health 2(17).
Hauer, K. E., S. J. Durning, W. N. Kernan, M. J. Fagan, M. Mintz, P. S. O’Sullivan, M. Battistone, T. DeFer, M. Elnicki, and H. Harrell. 2008. Factors associated with medical students’ career choices regarding internal medicine. JAMA 300(10):1154-1164.
Hofer, A., J. Abraham, and I. Moscovice. 2011. Expansion of coverage under the Patient Protection and Affordable Care Act and primary care utilization. Milbank Quarterly 89(1):69-89.
HRSA (Health Resources and Services Administration). 2013. Teaching Health Center GME payments: Aggregate payments through August 1, 2013. http://bhpr.hrsa.gov/grants/teachinghealthcenters/payments.html (accessed August 23, 2013).
Iglehart, J. K. 2013a. Expanding the role of advanced nurse practitioners—Risks and rewards. New England Journal of Medicine 368(20):1935-1941.
Iglehart, J. K. 2013b. The residency mismatch. New England Journal of Medicine 369(4): 297-299.
IOM (Institute of Medicine). 1996. Telemedicine. Washington, DC: National Academy Press.
IOM. 2003a. Health professions education: A bridge to quality (Quality Chasm Series). Washington, DC: The National Academies Press.
IOM. 2003b. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: The National Academies Press.
IOM. 2004. In the nation’s compelling interest. Ensuring diversity in the health care workforce. Washington, DC: The National Academies Press.
IOM. 2012a. Best care at lower cost: The path to continuously learning health care in America. Washington, DC: The National Academies Press.
IOM. 2012b. The mental health and substance use workforce for older adults: In whose hands? Washington, DC: The National Academies Press.
Jeffe, D. B., A. J. Whelan, and D. A. Andriole. 2010. Primary care specialty choices of United States medical graduates, 1997-2006. Academic Medicine 85(6):947-958.
Jolly, P. 2008. Diversity of U.S. medical students by parental income. Washington, DC: Association of American Medical Colleges.
Jolly, P., C. Erikson, and G. Garrison. 2013. U.S. graduate medical education and physician specialty choice. Academic Medicine 88(4):468-474.
Kirch, D. G., M. K. Henderson, and M. J. Dill. 2012. Physician workforce projections in an era of health care reform. Annual Review of Medicine 63:435-445.
Komaromy, M., K. Grumbach, M. Drake, K. Vranizan, N. Lurie, D. Keane, and S. B. Bindman. 1996. The role of black and Hispanic physicians in providing health care for underserved populations. New England Journal of Medicine 334(20):1305-1310.
Ku, L., K. Jones, P. Shin, B. Bruen, and K. Hayes. 2011. The states’ next challenge—securing primary care for expanded medicaid populations. New England Journal of Medicine 364(6):493-495.
Kussmaul, W. G. 2013. Too lazy for primary care? Annals of Internal Medicine 159(10): 711-712.
LCME (Liaison Committee on Medical Education). 2013. Medical school directory. http://www.lcme.org/directory.htm#pre-accredited-programs (accessed January 27, 2014).
Liss, D. T., P. A. Fishman, C. M. Rutter, D. Grembowski, T. R. Ross, E. A. Johnson, and R. J. Reid. 2013. Outcomes among chronically ill adults in a medical home prototype. American Journal of Managed Care 19(10):e348-e358.
Maeng, D. D., J. Graham, T. R. Graf, J. N. Liberman, N. B. Dermes, J. Tomcavage, D. E. Davis, F. J. Bloom, and G. D. Steele. 2012. Reducing long-term cost by transforming primary care: Evidence from Geisinger’s Medical Home Model. American Journal of Managed Care 18(3):149-155.
Marrast, L. M., L. Zallman, S. Woolhandler, D. H. Bor, and D. McCormick. 2013. Minority physicians’ role in the care of underserved patients: Diversifying the physician workforce may be key in addressing health disparities. JAMA Internal Medicine 174(2):289-291.
MedPAC (Medicare Payment Advisory Commission). 2009. Report to Congress: Improving incentives in the Medicare program. Washington, DC: MedPAC.
MedPAC. 2010. Graduate medical education financing: Focusing on educational priorities. In Report to Congress: Aligning incentives in Medicare. Washington, DC. Pp. 103-126. http://www.medpac.gov/chapters/jun10_ch04.pdf (accessed September 30, 2012).
Moy, E., and B. A. Bartman. 1995. Physician race and care of minority and medically indigent patients. JAMA 273(19):1515-1520.
Mullan, F. 2005. The metrics of the physician brain drain. New England Journal of Medicine 353:1810-1818.
Nasca, T. J., I. Philibert, T. Brigham, and T. C. Flynn. 2010. The next GME accreditation system—Rationale and benefits. New England Journal of Medicine 366:1051-1056.
Nasca, T., K. Weiss, J. Bagian, and T. Brigham. 2014a. The accreditation system after the “next accreditation system.” Academic Medicine 89(1):27-29.
Nasca, T. J., K. B. Weiss, and J. P. Bagian. 2014b. Improving clinical learning environments for tomorrow’s physicians. New England Journal of Medicine 370(11):991-993.
National Quality Forum. 2009. A comprehensive framework and preferred practices for measuring and reporting cultural competency: A consensus report. Washington, DC: National Quality Forum.
Nicholson, S. 2009. Will the United States have a shortage of physicians in 10 years? http://www.academyhealth.org/files/publications/HCFOReportDec09.pdf (accessed January 28, 2014).
Nivet, M. A., and A. C. Berlin. 2013. Diversity by design. Journal of Graduate Medical Education 5(3):526-527.
NRMP (National Resident Matching Program). 2002. Results and data: 2002 match. http://b83c73bcf0e7ca356c80-e8560f466940e4ec38ed51af32994bc6.r6.cf1.rackcdn.com/wp-content/uploads/2013/08/resultsanddata2002.pdf (accessed January 29, 2014).
NRMP. 2012. Results and data: Specialties matching service 2012 appointment year. Washington, DC: NRMP.
NRMP. 2013. Results and data: 2013 main residency match. Washington, DC: NRMP.
NRMP. 2014a. Advance data tables. 2014 main residency match. http://www.nrmp.org/wp-content/uploads/2014/03/2014-NRMP-Main-Residency-Match-Advance-Data-Tables-FINAL.pdf (accessed May 12, 2014).
NRMP. 2014b. U.S. medical students learn 2014 national resident matching program in main residency match day results in ceremonies today. http://www.nrmp.org/wp-content/uploads/2014/03/2014-National-Resident-Matching-Program-NRMP-Main-ResidencyMatch-Results-Press-Release.pdf (accessed May 12, 2014).
Patel, M. S., M. J. Arron, T. A. Sinsky, E. H. Green, D. W. Baker, J. L. Bowen, and S. Day. 2013. Estimating the staffing infrastructure for a patient-centered medical home. American Journal of Managed Care 19(6):509-516.
Patel, M. S., D. A. Reed, L. Loertscher, F. S. McDonald, and V. M. Arora. 2014. Teaching residents to provide cost-conscious care: A national survey of residency program directors. JAMA Internal Medicine 174(3):470-472.
Petterson, S., W. Liaw, Phillips, Jr., D. Rabin, D. Meyers, and A. Bazemore. 2012. Projecting U.S. primary care physician workforce needs: 2010-2025. Annals of Family Medicine 10(6):503-509.
Pew Health Professions Commission. 1995. Critical challenges: Revitalizing the health professions for the twenty-first century. http://futurehealth.ucsf.edu/Content/29/1995-12_Critical_Challenges_Revitalizing_the_Health_Professions_for_the_Twenty-First_Century.pdf (accessed January 2, 2014).
Phillips, R. L., Jr., and B. J. Turner. 2012. The next phase of Title VII funding for training primary care physicians for America’s health care needs. Annals of Family Medicine 10(2):163-168.
Phillips, R.L., Dodoo, M.S., Petterson, S., Xierali, I., Bazemore, A., 2009. Specialty and geographic distribution of the physician workforce: What influences medical student & resident choices? http://www.macyfoundation.org/docs/macy_pubs/pub_grahamcenterstudy.pdf (accessed April 7, 2013).
Phillips, R. L., S. Petterson, and A. Bazemore. 2013. Do residents who train in safety net settings return for practice? Academic Medicine 88(12):1934-1940.
Phillips, R., A. Bazemore, and L. Peterson. 2014. Effectiveness over efficiency: Underestimating the primary care physician shortage. Medical Care 52(2):97-98.
Quinn, K. J., K. Y. Kane, J. J. Stevermer, W. D. Webb, J. L. Porter, H. A. Williamson, Jr., and M. C. Hosokawa. 2011. Influencing residency choice and practice location through a longitudinal rural pipeline program. Academic Medicine 86(11):1397.
Rabinowitz, H. K., J. J. Diamond, F. W. Markham, and C. Rabinowitz. 2005. Long-term retention of graduates from a program to increase the supply of rural family physicians. Academic Medicine 80(8):728-732.
Rabinowitz, H. K., J. J. Diamond, F. W. Markham, and J. R. Wortman. 2008. Medical school programs to increase the rural physician supply: A systematic review and projected impact of widespread replication. Academic Medicine 83(3):235-243.
Rabinowitz, H. K., J. J. Diamond, F. W. Markham, and A. J. Santana. 2012. The relationship between entering medical students’ backgrounds and career plans and their rural practice outcomes three decades later. Academic Medicine 87(4):493-497.
Reid, R. J., and E. B. Larson. 2012. Financial implications of the patient-centered medical home. JAMA 308(1):83-84.
Reinhardt, U. 2013. Testimony before the U.S. Senate Committee on Health, Labor, Education & Pensions Subcommittee on Primary Health and Aging. Hearing on 30 million new patients and 11 months to go: Who will provide their primary care? http://www.help.senate.gov/imo/media/doc/Reinhardt.pdf (accessed November 26, 2013).
Ricketts, T. C. 2011. The health care workforce: Will it be ready as the boomers age? A review of how we can know (or not know) the answer. Annual Review of Public Health 32:417-430.
Ricketts, T. C. 2013. The migration of physicians and the local supply of practitioners: A five-year comparison. Academic Medicine 88(12):1913-1918.
Rosenblatt, 2010. Commentary: Do medical schools have a responsibility to train physicians to meet the needs of the public? The case of persistent rural physician shortages. Academic Medicine 85(4):572-574.
Saha, S. 2014. Taking diversity seriously: The merits of increasing minority representation in medicine. JAMA Internal Medicine 174(2):291-292.
Saha, S., and S. A. Shipman. 2008. Race-neutral versus race-conscious workforce policy to improve access to care. Health Affairs 27(1):234-245.
Saha, S., G. Guiton, P. F. Wimmers, and L. Wilkerson. 2008. Student body racial and ethnic composition and diversity-related outcomes in U.S. medical schools. JAMA 300(10): 1135-1145.
Salsberg, E. 2009. Annual State of the Physician Workforce address. AAMC. https://www.aamc.org/download/82844/data/annualaddress09.pdf (accessed January 28, 2013).
Salsberg, E. 2014. The 2014 GME residency match results: Is there really a “GME” squeeze? http://healthaffairs.org/blog/2014/04/24/the-2014-gme-residency-match-results-is-there-really-a-gme-squeeze (accessed April 28, 2014).
Schwartz, M. D., S. Durning, M. Linzer, and K. E. Hauer. 2011. Changes in medical students’ views of internal medicine careers from 1990 to 2007. Archives of Internal Medicine 171(8):744.
Sehgal, R. T., and P. Gorman. 2011. Internal medicine physicians’ knowledge of health care charges. Journal of Graduate Medical Education 3(2):182-187.
Shannon, S. C., B. R. Buser, M. B. Hahn, J. B. Crosby, T. Cymet, J. S. Mintz, and K. J. Nichols. 2013. A new pathway for medical education. Health Affairs 32(11):1899-1905.
Shaw, E. J. 2005. Researching the educational benefits of diversity. The College Board. Research Report number 2005-4. New York: The College Board.
Sheldon, G. F. 2010. Health care reform. Are we missing the important issues? Annals of Surgery 251(2):201-202.
Shipman, S. A., K. C. Jones, C. E. Erikson, and S. F. Sandberg. 2013. Exploring the workforce implications of a decade of medical school expansion: Variations in medical school growth and changes in student characteristics and career plans. Academic Medicine 88(12):1904-1912.
Sisson, S. D., and D. Dalal. 2011. Internal medicine residency training on topics in ambulatory care: A status report. American Journal of Medicine 124(1):86-90.
Sullivan, L. W. 2010. Increasing ethnic and racial diversity: A crucial measure for reducing health disparities. Presentation to the Roundtable on the Promotion of Health Equity and the Elimination of Health Disparities, Washington, DC, September 10.
Sullivan, L. W., and I. Suez Mittman. 2010. The state of diversity in the health professions a century after Flexner. Academic Medicine 85(2):246-253.
Traverso, G., and G. T. McMahon. 2012. Residency training and international medical graduates: Coming to America no more. JAMA 308(21):2193-2194.
UCLA International Medical Graduate (IMG) Program. 2013. https://giving.ucla.edu/Standard/NetDonate.aspx?SiteNum=256 (accessed January 28, 2014).
U.S. Census Bureau. 2012. Methodology and assumptions for the 2012 national projections. http://www.census.gov/population/projections/files/methodology/methodstatement12.pdf (accessed May 5, 2014).
U.S. Census Bureau. 2013. Frequently Asked Questions. How many people reside in urban or rural areas for the 2010 Census? What percentage of the U.S. population is urban or rural? https://ask.census.gov/faq.php?id=5000&faqId=5971 (accessed May 8, 2014).
Vaughn, B. T., S. R. DeVrieze, S. D. Reed, and K. A. Schulman. 2010. Can we close the income and wealth gap between specialists and primary care physicians? Health Affairs 29(5):933-940.
Warm, E. J., and C. Goetz. 2013. Too smart for primary care? Annals of Internal Medicine 159(10):709-710.
Weida, N. A., R. L. Phillips, Jr., and A. W. Bazemore. 2010. Does graduate medical education also follow green? Archives of Internal Medicine 170(4):389.
Weiner, J. P., S. Yeh, and D. Blumenthal. 2013. The impact of health information technology and e-health on the future demand for physician services. Health Affairs 32(11): 1998-2004.
Weiss, K. B., J. P. Bagian, and T. J. Nasca. 2013. The clinical learning environment: The foundation of graduate medical education. JAMA 309(16):1687-1688.
Weissman, J. S., J. Betancourt, E. G. Campbell, E. R. Park, M. Kim, B. Clarridge, D. Blumenthal, K. C. Lee, and A. W. Maina. 2005. Resident physicians’ preparedness to provide cross-cultural care. JAMA 294(9):1058-1067.
West, C. P., and D. M. Dupras. 2012. General medicine vs. subspecialty career plans among internal medicine residents. JAMA 308(21):2241-2247.
West, C. P., M. M. Drefahl, C. Popkave, and J. C. Kolars. 2009. Internal medicine resident self-report of factors associated with career decisions. Journal of General Internal Medicine 24(8):946-949.
Whitcomb, M. E. 2009. New and developing medical schools: Motivating factors, major challenges, planning strategies. New York: Josiah Macy Jr. Foundation.
Whitcomb, M. E. 2013. New and developing medical schools: Motivating factors, major challenges, planning strategies. Part 2. New York: Josiah Macy Jr. Foundation.
Wilson-Stronks, A., K. K. Lee, C. L. Cordero, A. L. Kopp, and E. Galvez. 2008. One size does not fit all: Meeting the health care needs of diverse populations. http://www.jointcommission.org/assets/1/6/HLCOneSizeFinal.pdf (accessed February 9, 2014).
Wynn, B.O., R. Smalley, and K. Cordasco. 2013. Does it cost more to train residents or to replace them? A look at the costs and benefits of operating graduate medical education programs. http://www.rand.org/pubs/research_reports/RR324. Santa Monica, CA: RAND Health.


























