1
Introduction and Summary
An epidemic is both a medical and a social occurrence. Medically, it is the appearance of a serious, often fatal, disease in numbers far greater than normal. Socially, it is an event that disrupts the life of a community and causes uncertainty, fear, blame, and flight. The etymology of the word itself suggests the broader, social meaning: epi demos, in ancient Greek, means ''upon the people or the community."
The epidemic of acquired immune deficiency syndrome (AIDS)—which was recognized in the United States in 1981, continues today, and will continue into the foreseeable future—mirrors epidemics of the past. The medical meaning of the epidemic has been revealed in the sobering numbers reported in epidemiologic studies. During 1991, 45,506 new AIDS cases were reported to the Centers for Disease Control (CDC), which brought the cumulative total of cases in the United States to 206,392; 133,233 (65 percent) deaths have been tallied (Centers for Disease Control, 1992). It is estimated that 1 million people are currently infected with the human immunodeficiency virus (HIV), which causes AIDS (Centers for Disease Control, 1990), but this number is very uncertain (see Technical Note at the end of this chapter).
These numbers identify the first and most obvious impact of the HIV/AIDS epidemic on American society: the large population of infected, sick, and dying persons attacked by a previously unknown disease. Behind the epidemiologic reports and the statistical estimates lies the social disruption of the epidemic: the destroyed life for which each of the numbers stands
and the changed lives of many others touched by the disease. And behind the individual lives are the manifold ways in which a variety of institutions and practices have been affected by the epidemic.
In 1987 the National Research Council of the National Academy of Sciences established the Committee on AIDS Research in the Social, Behavioral, and Statistical Sciences. Two of the committee's reports, AIDS: Sexual Behavior and Intravenous Drug Use (Turner, Miller, and Moses, 1989) and AIDS: The Second Decade (Miller, Turner, and Moses, 1990), reviewed and evaluated a wide range of social and behavioral science research relevant to HIV/AIDS prevention, education, and intervention. In the course of preparing those reports, the committee noted that many of the social consequences of the epidemic were not being studied in any systematic way. It judged that systematic study would be beneficial in predicting the course of the epidemic's path through U.S. society and in formulating policies to deal with it. Thus, in 1989 the committee established the Panel on Monitoring the Social Impact of the AIDS Epidemic, with the general mandate to study the social impact of the epidemic and to recommend how it could be monitored in order to contribute to the formulation of policies that might effectively deal with it. In the course of its work, the panel, with the agreement of the parent committee and the several federal agencies that were sponsoring its work, modified this mandate and deleted the plan to recommend systems for monitoring.
This report is an unusual undertaking for the National Research Council. Its objective is to form a picture of the effects of the AIDS epidemic on selected social and cultural institutions in the United States and to describe how those institutions have responded to the impact of the epidemic. No attempt has been made to write a comprehensive history—there are not yet adequate studies of the epidemic upon which to base such an effort. Instead we have been selective in looking at those institutions for which sufficient information is available to describe impact and response. These descriptions cannot be considered complete and authoritative; but we do believe they suggest a pattern that should be of concern to the country and command the attention of policy makers attempting to deal with the epidemic over the next decade.
EPIDEMICS, IMPACTS, AND RESPONSES
The impact of AIDS has many dimensions, only a few of which are captured in official statistics or analysis by the research community. The numbers of AIDS cases and HIV infection count as an impact: cumulatively, they state the effect on the population of the United States and on particular subpopulations. Each case has many dimensions—personal, professional, and institutional—through the many social organizations that touch
the life of each infected person. Each set of interactions creates an impact, and the diverse impacts have generated equally diverse responses by individuals, groups, and communities.
The panel set out to study these impacts, and it immediately confronted the problem of defining the terms of reference. "Impact" is an overused word that in common parlance has become a synonym for "effect." In this sense, it indicates that one action or state of affairs is caused or influenced by some other action or state of affairs and is used to describe both major and minor effects. Reaching deeper into the language, however, impact has a more powerful meaning—collision. In this use of the word, an impact is an effect that radically changes the previous state of affairs or even destroys it.
After much discussion, the panel adopted a definition of impact that fits somewhere between these two meanings. "Impact" as used by the panel describes a concentrated force producing change, a compelling effect. We adopted this hybrid meaning not only because it more accurately describes the impact of AIDS on contemporary America—social institutions have not been destroyed—but because we quickly realized that social impact does not merely destroy; it evokes a reaction or a response. It is more organic than physical. Persons and societies do not merely feel the impact of an event; they remake their lives and institutions to accommodate, negate, or preserve its effects. In this report, we attempt to capture and describe the process of impact and response of selected social institutions to the HIV/AIDS epidemic.
The task of this panel was to go beyond, to the extent possible to limited human vision, the impression of the extraordinary impacts of AIDS on individual lives and on social institutions. We have tried to sort out those that will endure in such a way as to force, or to invite, Americans to take them into account in the next decade. This epidemic is not ordinary in one quite specific way: it can be determined many years in advance of the onset of actual illness in a patient that the illness will come. This epidemic is not, like many historical epidemics, an invasion of morbidity and mortality that rapidly sweeps through a population. It comes and will stay for years, not only in the population, but in the individual people infected, and its presence will often be known to them and to others long before they suffer the disabling, lethal effects. Similarly, rough estimates can be made of the numbers of people who will begin to experience those disabling, lethal effects years from now. Thus, Americans must think about this epidemic for many years into the future.
The institutions we studied appear to have absorbed the impact of AIDS and accommodated to it in a very limited way. However, even a response that is partial and apparently transitory may mark the beginning of more fundamental change. Several of the institutions we studied may follow this trajectory of limited initial response, followed some years later by very
significant changes. These longer term responses would be interesting to follow, and we hope that researchers will attempt to do so. However, the panel did not attempt to suggest a methodology for longer term monitoring: the data needs and methods of observation would be very different for the individual institutions studied.
After extensive deliberation, the panel determined that it had sufficient information and understanding to describe social impact and response for six institutions (broadly defined):
-
the public health system
-
health care finance and delivery
-
clinical research and drug regulation
-
religion
-
voluntary organizations
-
the correctional system
These institutions were selected for several reasons: the panel members had the competence to study and evaluate them, we judged that sufficient empirical data and informed opinion existed to formulate our own assessment of impact and response, and they had not been treated in previous reports of the parent committee. The six institutions chosen are very different in structure, degree of centralization, and other dimensions. Such differences affect the level of generalization appropriate to each area.
In the course of our work we also began to see another kind of impact and response—on public policies not necessarily connected to institutions. The HIV/AIDS epidemic has clearly had an impact on policies related to families, and we thus decided to add to our study an examination of two policy areas: issues related to newborns and children and issues related to intimate nonmarital relationships.
Finally, in addition to examining institutional systems as a whole and selected family policies, the panel wanted to look at the impact of HIV/AIDS on communities, where several institutions converge and where the synergy resulting from that convergence is most clearly seen. Originally, three case studies were envisioned: New York, Miami, and Sacramento. We were able to complete only New York—a city that could never be described as typical, but one that does vividly illustrate the impact and response to AIDS among major social institutions.
It is common to find references to the impact of AIDS and HIV. It is also rather common to find such references expressed in quite strong terms. For example, Milbank Quarterly's two-volume study, A Disease of society: Cultural Responses to AIDS, opens with these words (Nelkin et al., 1991:1):
AIDS is no "ordinary" epidemic. More than a devastating disease, it is freighted with profound social and cultural meaning. More than a passing tragedy, it will have long-term, broad-ranging effects on personal relationships,
social institutions, and cultural configurations. AIDS is clearly affecting mortality—though in some communities more than others. It is also costly in terms of the resources—both people and money—required for research and medical care. But the effects of the epidemic extend far beyond their medical and economic costs to shape the very ways we organize our individual and collective lives.
It is not clear what an "ordinary" epidemic would be. No epidemic seems ordinary to those who experience it. The AIDS epidemic has invoked comparison with many epidemics of the past. Most commonly, the bubonic plague (the Black Death) that devastated Europe in the fourteenth century is recalled: between 1348 and 1350, some 20 million people, one-third of the population of Europe, died. (Additional tends of millions had died in Asia during the preceding decade [McNeil, 1976].) This epidemic had unquestionable impacts. Historians attribute to it, at least in part, the emergence of nation states, the rise of mercantile economies, and the religious movements that led to the Reformation (Campbell, 1931; McNeil 1976; Tuchman, 1978). As Anna Campbell (1931) noted, the Black Death "changed the minds of men" bringing new ways of understanding God, the meaning of death, the place of tradition, and the role of authority in religious and social life. Changes in the collective mind of a society might be the most profound of all impacts, for the new ideas generated by a major social tragedy can propel institutional change and outlast immediate changes to affect lives far in the future. Difficult though it might be to predict the future import of the present impact of the HIV/AIDS epidemic, one should not shrink from the task, especially when one must plan for that future.
AIDS has been compared with other epidemics, too: the resurgence of bubonic plague in England in the mid-seventeenth century, the cholera epidemics of the nineteenth century, the venereal disease epidemics of the sixteenth century and the early twentieth centuries, and the polio epidemics of the twentieth century (Brandt, 1988; Risse, 1988; Slack, 1988). AIDS has its analogies to each of these epidemics—number of deaths, methods of prevention, stigmatization of sufferers and presumed carriers, and responses of authorities—all can be compared in general or in detail. The comparisons are often illuminating, but sometimes misleading (Fee and Fox, 1988). It can be said with some assurance, however, that none of the historical epidemics was "ordinary." Each had impacts that struck its sufferers and subsequent commentators as "extraordinary."
The comparison with epidemics of the past invokes the features that are remembered about those plagues. They have, in this respect, had an impact on history or, as Campbell wrote (1931), "on the minds of men." They also left social institutions that sometimes affect present-day thinking about the AIDS epidemic: cholera, for example, left a public health approach to epidemic disease that stressed quarantine; venereal diseases gave rise to the
public health approach of contact tracing. These established public health practices have had to be reconsidered in the current epidemic. Many of the prominent, even dramatic impacts of past epidemics, however, have so melded into the social fabric that people are often astonished to hear of them today, and some, interesting though they be, seem of little relevance to the current problem. For example, to attribute the existence of Protestant Christianity to the effects of the Black Death on religious ideas and sentiments has little influence on the ways in which people today think about religion or about epidemics. Similarly, to attribute the existence of Canada as an independent nation to the fact that British troops had been vaccinated against smallpox before the Battle of Quebec, but American troops were decimated by the disease, is certainly to point to an effect of epidemic and, indeed, an impact. Yet that impact has been of little relevance to subsequent citizens and governments, except that "some Canadians to this day worship smallpox as the deliverer from United States citizenship" (Foege, 1988:332).
Many features of epidemics are no longer remembered and have left little imprint on the societies that they ravished for a time. Indeed, one of the greatest of epidemics, the influenza of 1918-1920, has been called by its historian "the forgotten epidemic" (Crosby, 1989). Worldwide, perhaps 30 million people died; in the United States, 675,000 people died, most of whom were not the usual victims of influenza (the very old, infants, and children), but men and women in their 20s and 30s. This terrible scourge might have had a great impact, but it passed and left almost no mark on the social institutions and practices of the time. Many people were mourned, but life quickly returned to normal. Even the absence of impact has a lesson for this study: it is possible that many of the effects currently taken as important and lasting will pass or be absorbed into the course of American life and culture. It is not entirely clear how confidently one should accept the words of Milbank editors Nelkin, Willis, and Parris (1991:1, 2):
More than a passing tragedy, it [AIDS] will have long-term, broad-ranging effects on personal relationships, social institutions, and cultural configurations … AIDS will reshape many aspects of society, its norms and values, its interpersonal relationships and its cultural representations … the future will be different from both the past and the present.
Our report suggests that, in some respects, the AIDS epidemic may be more like the influenza of 1918 than the bubonic plague of 1348: many of its most striking features will be absorbed in the flow of American life, but, hidden beneath the surface, its worst effects will continue to devastate the lives and cultures of certain communities.
GENERAL FINDINGS AND CONCLUSIONS
Historically, certain epidemics have done great damage to social institutions: the Black Death in a 3-year sweep through Europe wiped out enough laborers to cause a major restructuring of the economy of the continent. The HIV/AIDS epidemic, although often compared to the Black Death, has not affected U.S. social institutions to any such extent. Although it had by the end of 1991 infected perhaps 1 million people, brought devastating sickness to 206,392, and death to 133,233, it had not significantly altered the structures or directions of the social institutions that we studied. Many of the responses have been ad hoc and may be reversed when pressures subside. Others may be more lasting, but only because they reinforced or accelerated changes already latent or budding within the institutions.
It is the panel's opinion that the limited responsiveness of institutions can in part be explained because the absolute numbers of the epidemic, relative to the U.S. population, are not overwhelming, and because U.S. social institutions are strong, complex, and resilient. However, we believe that another major reason for this limited response is the concentration of the epidemic in socially marginalized groups. The convergence of evidence shows that the HIV/AIDS epidemic is settling into spatially and socially isolated groups and possibly becoming endemic within them. Many observers have recently commented that, instead of spreading out to the broad American population, as was once feared, HIV is concentrating in pools of persons who are also caught in the "synergism of plagues" (see Wallace, 1988): poverty, poor health and lack of health care, inadequate education, joblessness, hopelessness, and social disintegration converge to ravage personal and social life. These coexisting conditions foster and aggravate HIV infection and AIDS. Our study of New York City (see Chapter 9) illustrates this dramatically for one epicenter of the epidemic. We believe that the patterns shown there are repeated throughout the country: many geographical areas and strata of the population are virtually untouched by the epidemic and probably never will be; certain confined areas and populations have been devastated and are likely to continue to be.
This epidemiological direction reveals the disconcerting implications of our major conclusion. The institutions that we studied are particularly weak at those points at which the epidemic is likely to be most destructive. For example, the health care system, which responded to the appearance of a new disease with some alacrity, is weakest organizationally and economically in those places where the affected populations are concentrated. The problems of caring for those who are infected are magnified by the particular configuration of the U.S. health care system, which emphasizes to a greater extent than other developed countries private insurance and ability-to-pay criteria. Providers, hospitals, and public health mechanisms can and
have responded to a flood of patients with AIDS, but those responses were most successful where health care was better organized and financed and where the populations to be served had sufficient knowledge to understand the disease and its modes of transmission and were capable of organizing themselves in ways that supported and supplemented the health care system.
Thus, our most general conclusion about the epidemic is that its impact has hit institutions hardest where they are weakest: serving the most disadvantaged people in U.S. society. Predictions of the imminent collapse of the health care system due to the epidemic, for example, now look shrill, but, conversely, hopes that the epidemic would force the country toward more rational and equitable reform of the system now also seem unrealistic. In the panel's judgment, the HIV/AIDS epidemic has effected many transient changes in the institutions that we studied and relatively few changes that we expect to be permanent. Among the more permanent, however, two are particularly noteworthy.
First, the institutions of public health, of health care delivery, and of scientific research have become more responsive to cooperation and collaboration with "outsiders." Policies and practices have been modified in these three institutions under pressure from and in collaboration with those who are affected by the epidemic and their advocates. Many of these changes are positive and will contribute to the efficiency and efficacy of the institutions. Similarly, volunteer organizations stimulated by the challenge of the epidemic have discovered ways not only of supplying help where extant institutions were lacking, they have also influenced the policies and practices of those institutions.
Second, even in institutions with very defined purposes and strong constraints—institutions as different as religious groups and correctional agencies—the response to the epidemic has reflected awareness of the scientific realities, as well as the social implications, of HIV/AIDS. Traditionally based doctrinal constraints in the case of religious groups and the stringent requirements of civil punishment in the case of correctional agencies are powerful forces that could and did dictate rigid and narrow response. Yet, powerful as those forces were, they did not negate more reflective responses that contributed to containment of the epidemic and respected the rights of individuals. We are concerned, however, that as the epidemic strikes with greater force in socially and economically deprived communities, the directions toward more communal involvement and respect for civil and personal liberties might be constricted and diverted.
The panel believes that a failure by scientists and policy makers to appreciate the interaction between social, economic, and cultural conditions and the propagation of HIV/AIDS disease has often led to public misunderstanding and policy mistakes about the epidemic. Although in the beginning of the epidemic, gay life and behavior were certainly at the center of
attention, even then they were noted primarily as "modes of transmission" and not as social contexts in which the disease had particular meanings around which strong forces for care, prevention, and political action could rally. Similarly, intravenous drug use was understood as a social behavior that could transmit infection, but its place in a matrix of social, cultural, and economic conditions was ignored.
A constant theme of this report and of the AIDS literature is the stigma, discrimination, and inequalities of the AIDS epidemic. At its outset, HIV disease settled among socially disvalued groups, and as the epidemic has progressed, AIDS has increasingly been an affliction of people who have little economic, political, and social power. In this sense, AIDS is an undemocratic affliction. In "democratic epidemics" (Arras, 1988), communicable illnesses cut across class, racial, and ethnic lines and threatens the community at large. In traditional societies with limited medical knowledge and technology, epidemics fall on most, if not all, of the people. In the modern world, particularly in industrial societies, inequalities in morbidity and mortality are often more social than biological phenomena. With HIV/AIDS, the concentration of the epidemic from its beginnings was among those who were, for a variety of reasons, members of marginalized social groups. In this case, the biology of viral transmission matched existing social inequalities and resulted in an unequal concentration of HIV/AIDS in certain regions and among certain populations (see Grmek, 1990). This pattern has created tension between the social and geographical localization of the epidemic and the need to mobilize resources to deal with the epidemic from among individuals, groups, and institutions that are removed from the social groups that are at the epicenter of the epidemic. As the epidemic becomes endemic in already deprived and segregated populations, this tension will be intensified.
If the current pattern of the epidemic holds, U.S. society at large will have been able to wait out the primary impact of the epidemic even though the crisis period will have stretched out over 15 years. HIV/AIDS will "disappear," not because, like smallpox, it has been eliminated, but because those who continue to be affected by it are socially invisible, beyond the sight and attention of the majority population.
Specific Findings And Conclusions
Public Health
The public health systems of the country—federal, state and local—absorbed the first shock of the AIDS epidemic and have remained at the forefront of research and policy development. Because of the increasing concentration of the epidemic in low-income and minority communities, the
public health system at the local level has become the primary service provider for a large proportion of people with HIV disease or AIDS. Nowhere is this more apparent than in New York City.
HIV/AIDS challenged the public health community to set aside many of its traditional policies and practices for the containment of infectious disease. Quarantine, mass mandatory testing, and contact tracing all had notable disadvantages in dealing with a disease with a long latency period, that was spread chiefly through sexual activity or intravenous drug use, and that largely affected already stigmatized groups. Spokesmen for the affected groups, particularly the gay community, advanced other methods of containment that relied on community education and voluntary anonymous testing. This came to be know as an "exceptionalist" approach since it differed from responses to prior epidemics. However, mass education and other approaches to behavior modification were already emerging as the public health strategy of choice for substance abuse prevention, smoking, and behavioral disorders. Thus, HIV/AIDS accelerated the adoption of these approaches and invited their intensive application to an infectious disease. It also created a political environment that compelled the public health community to negotiate containment strategies with the population that was initially primarily infected—gay men.
As the second decade of the epidemic begins, some aspects of the exceptionalist approach are being reexamined and abandoned. More traditional public health methods are being reintroduced, although in forms modified by the experience of the first decade. The change is due in part to the availability of early treatment, which to infected individuals makes early identification more useful. It may also be the result of the steady shift of the epidemic itself into populations that are less politically potent than the gay community, primarily intravenous drug users and their sexual partners.
Overall, the impact of the epidemic on the public health system has been pervasive: it has prompted a critical examination of traditional responses to epidemics of infectious disease, challenged the public health community to devise more effective strategies for promoting behavioral change, and, because of the sheer size of the HIV/AIDS-related activities profoundly influenced the public's perception of the public health systems. HIV/AIDS has also increased the range of clinical responsibilities of public health agencies and further strained already burdened resources. In many cities, this has resulted in the neglect of traditional areas of public health activities such as sexually transmitted disease and tuberculosis.
The inextricable link between HIV disease and other diseases and conditions prevalent in poor populations (e.g., drug addiction, tuberculosis, and sexually transmitted diseases) means that public health providers will face even greater challenges as the HIV/AIDS epidemic unfolds in the 1990s. The newer views and practices of public health may revert into more traditional
ways as the epidemic settles in communities where the newer techniques are more difficult to implement. The epidemic thus presents an opportunity and a challenge for the revitalization of the practice of public health, both with regard to infectious conditions and the chronic disorders that represent so much of the task of public health in the United States today.
Health Care
The HIV/AIDS epidemic has sent more than 200,000 patients into that system over the last decade and may, in this decade, send up to 1 million more. A substantial proportion of these patients are drawn from the pool of the uninsured or patients who rapidly exhaust their insurance benefits due to job loss or benefit restrictions. The people who became HIV/AIDS patients challenged the provider community on a number of fronts: they were generally young and previously healthy people who engaged in life styles that affronted many in the provider community. Before the modes of transmission were well understood, many health care personnel feared contact with AIDS patients, and both hospitals and private physicians struggled with unfamiliar problems of how to provide sensitive and responsive care while preserving the privacy of AIDS patients and protecting staff and other patients from infection. These problems have been complicated by the fact that many AIDS patients cannot pay for care, and thus the subset of the health care delivery system that provides care to indigent patients has absorbed the brunt of the epidemic. In the handful of cities that are the focus of the epidemic, there is a serious strain on the provider community, particularly public and voluntary teaching hospitals; in other cities, the capacity of hospitals to absorb AIDS inpatients is not as pressing a concern as are the stigma and inadequate reimbursement associated with AIDS care.
The complexity of the disease remains another major challenge for the provision of services. HIV disease attacks virtually every organ system of the body. The diverse and uncoordinated nature of the U.S. health system—reinforced by the reimbursement practices of the multiple plans that pay for care—has been often criticized for its failure to provide comprehensive, coordinated primary care and for too great a reliance on specialists and subspecialists. And it is just such comprehensive, primary care that is necessary to cope with a disease that is chronic and disabling and not limited to any one organ system. The urgent need for coordinated community-based care for AIDS patients has pushed the development of improved case management approaches.
AIDS has influenced health care providers in both direct and subtle ways. The specialty of infectious disease has enjoyed a renaissance and is now viewed as one of the few shortage medical specialties. Concern is
growing, however, that the burden of the epidemic may further dissuade young physicians from entering specialties such as internal medicine or from practicing in a geographic location where the burden of caring for patients with HIV disease is perceived to be high. The care of AIDS patients in terminal stages of the disease falls very heavily on hospital-based nurses. Like the practice of oncology nursing, it is an emotionally as well as professionally demanding experience. It is impossible to assess the extent to which the HIV/AIDS epidemic has exacerbated staffing problems in hospitals and other institutional settings that care for AIDS patients; however, a shortage of nurses has been identified as a major obstacle to improved care of AIDS patients.
All health professionals are at risk of HIV infection through exposure by accidental cuts or punctures incurred while caring for HIV-infected patients. Procedures adopted to protect health care workers from accidental infection (universal precautions) are designed to avoid exposure to blood and body fluids regardless of whether patients or health care workers are believed to be infected. The techniques and behaviors in the health care setting that must be modified to reduce HIV transmission risks, however, may be as difficult to change as risky sexual behavior and drug-use habits. Health care procedures are learned behaviors and habits of years duration. The risk of transmission from patients to providers has been overshadowed in public attention by the extremely minor risk of transmission from providers to patients.
These and other considerations have made AIDS the most profound challenge to the care of patients that has faced the health care provider community in modern times. A substantial proportion of physicians avoid caring for patients with HIV disease or AIDS. This avoidance or outright refusal may result in a broad range of harm: in addition to leaving some patients without needed care, it stigmatizes patients and adds to the considerable psychological burdens of living with the disease. The avoidance or refusal also increases the risk for health care professionals who remain willing to treat patients and hence assume a disproportionate burden of the HIV/AIDS epidemic.
AIDS has challenged the economic arrangements of the health care system in many ways. Most visible, perhaps, has been the conflict over access to new drugs and a ''fair price" for new therapeutic agents. The introduction of universal precautions in hospitals has significantly increased the demand for barrier protection and hence the cost of hospitalization for all patients. The HIV/AIDS epidemic has also expanded fissures already present in the health insurance system: the expense of the disease has caused insurance firms to use all available markers to avoid enrolling AIDS patients; and group plans have in many cases been modified to exclude the cost of AIDS treatments. As providers struggle to cope with uninsured
patients, and patients struggle to pay for drugs and services they need, another voice has been added to the call for a comprehensive solution to the problem of health care financing.
Clinical Research and Drug Regulation
In perhaps no other area has the impact of the HIV/AIDS epidemic been more clear than in the identification, clinical testing, and regulation of new drugs and in the conduct of clinical research. The most profound change wrought by AIDS in drug development is simply the dramatic increase in public awareness of the nature, structure, and purpose of clinical trials. Debate about the ethics and scientific validity of clinical trials occurs not only among physicians, statisticians, and ethicists, but also among patients, activists, and politicians. AIDS has to a large degree publicized and politicized the aspects of clinical investigation that were heretofore largely within the private purview of the scientific community.
The modern history of clinical research and drug development shows that the interplay of politics, science, and ethics must be recognized as an ongoing dynamic during the twentieth century. The systems have been influenced by AIDS, but the effect has been more to accelerate change that was building in the system rather than to introduce fundamentally new concepts. The introduction of a parallel track model in clinical research and drug regulation in clinical trials is perhaps the most disquieting of the AIDS-related changes to the scientific community, since both the purposes and the procedures lack clarity or consensus. Pressure to expand clinical trials into community-based physicians' practices has similarly posed difficult questions of how to organize and support such trials, what results can realistically be expected from them, and how to distinguish between ad hoc extensions of experimental therapies into community practice and clinical research that produces replicable results. Although these questions were thrust on the research community by the HIV/AIDS epidemic, they will quickly become relevant to many other fields of research as increasing numbers of patients and their advocates seek access to the newest therapies.
HIV/AIDS has similarly challenged the traditional mode of scientific communication through peer-reviewed journals. That review process by scientific peers is time consuming, and the combination of review time and queuing for a place in the journals may result in long lag times between submission of a manuscript and publication. The cumbersome nature of the system has been accepted until now because of the safeguards it offers for objective assessment of the accuracy and relevance of research findings. AIDS, however, surfaced widespread objections to the delayed publication of research that appears to show a significant therapeutic benefit for serious diseases or that demonstrates a previously unknown toxicity of an accepted
therapy. HIV/AIDS studies have not been the only ones in which disclosure before publication has occurred, but the intervention of AIDS activists has thrust the dilemma more squarely into the spotlight. The scientific community is grappling with the difficult problems of how to implement a more pragmatic yet still responsible approach to traditional peer review.
Although it is impossible at this time in the epidemic to reach any definitive conclusions about the impact of AIDS on clinical research and the regulation of new drugs, it is apparent that patient activism and the exigencies of the AIDS epidemic have generated the most significant reevaluation of the research and regulation process to occur since World War II.
Voluntary and Community-Based Organizations
Government at all levels was slow to respond to the HIV/AIDS epidemic. The slow response was due partly to a general reduction in the growth of public spending on health care and social welfare and partly to a unique attribute of AIDS: its early association with two highly stigmatized minorities—gay men and intravenous drug users. When governments did respond, their flexibility and capacity to reach the groups in greatest need were limited, especially in regard to prevention education, for which there were constraints on how public monies could be used.
The vacuum was filled very early by an outpouring of volunteer activity. This was in part the result of the pulling together of the gay community in the belief that its members could best care for their own. The movement is also illustrative, however, of collective behavior in a period of social change and the forces that motivate individuals to volunteer their time. The response and mobilization of AIDS volunteers sheds light on the commitments individuals are willing to make to different kinds of social causes and it also points to new directions for understanding the meaning of volunteer work. In both San Francisco and New York, the AIDS crisis catalyzed volunteer movements that spanned both individual helping activities and strategic political campaigns. Particularly in San Francisco, the movement was innovative, effective, and enormously important in helping the gay community come to terms with the epidemic, as well as in shaping the response of the city's institutions to it.
Throughout the country, volunteer movements have carried a surprisingly large share of the burden of caring for AIDS patients, particularly outside hospitals. The cost of the epidemic for public agencies and private insurance has been significantly reduced by the extensive contributions of time and resources from volunteers. In addition, advocacy for appropriate social policies that would both contain the epidemic and protect the rights of affected individuals came from community-based organizations. At present, this powerful force has been weakened somewhat by financial constraints,
burnout, and bureaucratization. There is also doubt that the ethos of volunteering will provide the same benefits to the economically and socially deprived communities, in which the epidemic is increasingly centered, as it has to the gay communities in which it was first identified.
Religion and Religious Groups
Religion, manifested in personal belief and in organized denominations, is a large part of American life. The responses of major religious denominations and of religiously identified individuals to HIV/AIDS have been an important feature of the epidemic: from the beginning, HIV/AIDS has evoked a response from religious groups and from persons who identify themselves with the beliefs of those groups. Some adherents of Christianity linked early church traditions that saw plague as a divine punishment for sinfulness in general with the single sin of male homosexuality. Even though the roots of this association in early Christian doctrine have been forgotten by most modern Christians, this ancient association seems to echo in the collective memory of those who are ready to view AIDS as divine punishment visited on homosexuals. As it became evident that the infection touched others as well, that position became more difficult to maintain, but it has not been wholly abandoned.
From time immemorial, religious tradition and teaching have had a place for pestilential disease. This new pestilence, however, arrives at a time when religious and theological beliefs and practices are different in many ways from what they were in the past. They are more diverse, for religious traditions have separated into many branches. In addition, the relation between theological and scientific understanding is more complex; even those who believe that divine causality stands behind the events of the world do not always see that relationship in a direct, unambiguous way. Thus, today, religions have reacted to the HIV/AIDS epidemic in a complex way. They have almost inevitably done so with some reference to the powerful beliefs of the past, but also with the more subtle and nuanced interpretations of the present.
The religious response has generally involved censure of the behaviors, particularly the sexual behaviors, that were implicated in the spread of the disease and, to some extent, also criticized the degree of frankness that public health educators and activists have advocated in education. On these grounds, religion has been indicated as obstructionist about the epidemic. Yet many churches have engaged in extensive programs for the care and support of persons with AIDS and have, within their doctrinal limits, become active educators about the epidemic with regard to both discrimination and prevention. The response of religious groups to the epidemic is, of
course, defined by the doctrinal commitments of the various faiths, as well as by the attitudes of their congregations.
Because of the role of religious institutions in U.S. society, as well as the large number of people who identify with some religious group in the United States, it is important to elucidate the role that religious organizations have played in the epidemic and to understand the importance of taking their response into account in efforts to understand the impact of AIDS in American society. Overall, as the second decade of the epidemic begins, religious organizations have only begun to contribute to efforts to contain the epidemic or to deal with some of the social issues that surround it.
Correctional Systems
Approximately 1 million individuals are currently confined in prisons and local jails in the United States—426 out of every 100,000 residents. They are disproportionately black men, for whom the rate is 3,109 per 100,000. Since the beginning of the HIV/AIDS epidemic, the population in federal prisons and in prisons in the District of Columbia and 18 states has doubled. In California and New Jersey, two states hit particularly hard by the epidemic, the number of inmates tripled during the same period. The incarcerated population in the United States comprises in large part impoverished individuals from urban areas. Almost one-half of all prisoners are black. Not only are the majority of prisoners members of racial and ethnic minority groups, they are also overwhelmingly poor.
As the nation's prison population has burgeoned, so too has the population of inmates with HIV disease. The seroprevalence status of all inmates is not known, but it is certainly highly variable by region. In New York State prisons, approximately 17-20 percent of prisoners are HIV positive, which is probably the high end of the distribution. The question of whether to screen inmates for HIV antibodies has arisen with particular urgency in the prison setting, with no general resolution.
The question of whether to segregate HIV-positive inmates has been answered variously in different prison systems. In addition to concerns about transmission through forced or consensual sex, much attention has been paid to highly unlikely modes of transmission—casual contact or assaultive behaviors by HIV-positive inmates. Other potential mechanisms of disease spread are unique to prison culture and difficult to evaluate. At least 20 state prisons segregate all prisoners with AIDS, 8 segregate those with AIDS-related complex, and 6 segregate inmates who are HIV positive but not symptomatic. Segregation decisions have been justified on the grounds of inmate security, reducing the risk of transmission, or availability of specialized services. However, there is also widespread evidence that segregation is harmful, denying prisoners access to a range of services and exposing
them to additional stigma and likelihood of assault. Most prison systems have instituted HIV prevention education programs for inmates and staff.
Prisons have found it difficult to respond to the health care needs of inmates with AIDS. In most cases, funds for HIV care in prisons must come from corrections systems budgets that are already strained almost beyond the breaking point. In New York State, for example, two thirds of the correctional system's health care budget of approximately $100 million is earmarked for HIV/AIDS care. AIDS tests the limits of prison health care because treatments tend to be expensive and difficult to deliver. In some jurisdictions the impact of AIDS is causing prison officials to reconsider how prison health care is delivered and paid for and to look at new ways to attract and retain quality medical staff.
One of the most significant impacts of HIV disease in correctional facilities may be a sea change in the way epidemiological and clinical research involving prisoners is viewed. Regulations adopted to protect prisoners from exploitation at the hands of drug companies or clinical investigators are now being looked at in an entirely different light when they may block prisoners from receiving experimental treatments.
Public Policies on Children and Families
When the HIV/AIDS epidemic began, law and policy about families and intimate relationships were in transition, as they still are, and the epidemic has raised difficult questions. For example, because AIDS can be transmitted perinatally, public policies regarding the relationships between mothers and their fetuses and the care of sick children without maternal or family support had to be reconsidered. Because HIV/AIDS often affects people living in unconventional relationships, issues of health insurance, inheritance, and housing and health decisions—which are usually linked to conventional family structures—called for reexamination.
Social policy regarding family relationships is complex: specific law encodes certain features of policy, but much is embedded in practices formulated by public agencies, employers, and insurers—practices that sometimes lead to litigation. Convinced of the importance of examining the impact of the epidemic on policies regarding families and children, yet aware of their extreme complexity, the panel undertook two case studies of the interaction between the epidemic, law, and public policy. The first study examined issues of parental authority and foster parenting in Miami and New York. The second study examined how the legal definition of familial relationships evolved in two political and legislative controversies, in San Francisco and New York.
Proposals for the mandatory testing of all newborns or of all pregnant
women have raised long-standing disputes about public health needs and individual privacy and about the needs or rights of children as they may conflict with the rights of parents. Similarly, issues involved in caring for HIV-infected children or enrolling them in clinical trials of experimental therapies has starkly highlighted continuing arguments over the rights of biological parents versus the rights of foster parents or the state. In both cases, our study showed that there has as yet been no fundamental changes in broad policies, only changes in the clinical care and social services in certain communities. The rights of biological parents—regardless of their own degree of illness or ability to care for their children—have rarely been overridden in deciding on what will happen to their children.
There have been significant changes in the legal recognition of unmarried couples in some communities in recent years, but those changes were under way before the HIV/AIDS epidemic began, and it is impossible to determine exactly what role the epidemic played in bringing them about. In San Francisco, a domestic partnership ordinance was enacted in 1990, after failures in 1982 and 1989. It seems likely that the epidemic—and the increased organization among the gay and lesbian community in its wake—contributed to its passage. Similarly in New York, changes in the definition of "family" in relation to housing rights were, similarly, probably in part a result of effects of the HIV/AIDS epidemic.
In general, as the epidemic begins to center on economically and socially deprived communities, children will be increasingly affected. Born to infected mothers, they will be in need of special care and attention from their births. Some mothers die soon after their children's births, and many others are unable or unwilling, for financial and health reasons, to care for their children. In several cities where the problems are already noticeable, serious efforts have been made to meet those challenges. Still, those efforts reveal the basic tensions, inconsistencies, and anomalies in family policies that will need to be resolved as the epidemic becomes more endemic in those cities.
The epidemic first attacked the population of gay men. Such men have had to live outside the range of social policies that favored heterosexual couples joined in legal marriage and thus were often deprived of insurance, tax and inheritance benefits, and other legal rights and protections accorded to married couples. At the same time, gay men often are joined in enduring relationships and, in those relationships, often provide support and care to their ill partners. The effort to gain some social and legal recognition of those partnerships, already growing before the HIV/AIDS epidemic, was given some impetus by the epidemic. Questions about appropriate legal definitions of familial relationships will continue to be raised at least as long as the epidemic continues.
New York City
The panel examined the case of New York City—recognizing its atypicality—for the purpose of examining how the institutions we examined in the national context have been affected by and responded to the epidemic in a specific place. The objective was to improve understanding as well as call attention to the localized dimensions of the HIV/AIDS epidemic.
Much of the attention given to the epidemic has focused on national estimates and national needs. Ultimately, however, the epidemic and its impacts and the responses to it are experienced in specific locales, and responses are shaped by the resources, traditions, and leadership of the specific communities. The New York City study makes particularly clear the panel's major findings and conclusions in the context of specific local institutions and their management of issues presented by the epidemic. HIV disease in New York City occurs increasingly in the context of socioeconomic and ethnic deprivation, as well as among populations already suffering high levels of morbidity and mortality. The panel believes that this is a preview of the future of the epidemic in the country as a whole.
TECHNICAL NOTE
It is instructive to review briefly the procedures for estimating HIV incidence and prevalence to gain an understanding of the basis for the current uncertainty regarding the size of the epidemic and its prevalence among specific population groups. Given that there are no nationally representative seroprevalence surveys, the incidence and prevalence of HIV infection must be inferred from the reported cases of AIDS. New AIDS cases at time t result from infections acquired over a considerable period before that time. Suppose that the incubation distribution of duration from infection to AIDS is denoted by I(d) and that the number of new HIV infections at time t is denoted by H(t). Then the number of new AIDS cases at time t, A(t), is given by the equation
(1)
where ω is the maximum incubation period. Although this equation may appear complicated to those without training in mathematics, the concept underlying it is quite simple: the number of new AIDS cases in the current year, for example, is the sum of the number of new infections last year times the fraction of infections that are manifested in AIDS 1 year later, the number of new infections 2 years ago times the fraction of infections that are manifested in AIDS 2 years later, and so forth.
What one observes, of course, is only the time series A(t). One needs to
invert the equation to estimate H(t), the time series of new infections. It is well known that without knowledge of I(d)—the fraction of infections that progress to AIDS at each duration d since infection—there is no unique solution for H(t); in fact, there are infinitely many combinations of H(t) and I(t) that satisfy equation (1). Therefore, to make progress, one must obtain external knowledge of I(d). Estimates of the incubation distribution can be derived only from individuals whose date of infection is known. The most reliable data come from cohort studies of hemophiliacs and homosexual men (Brookmeyer, 1991). Note that these data provide information only on the waiting time from seroconversion to AIDS. The time from infection to seroconversion is assumed to be from 3 to 6 months, although seroconversion in some individuals is apparently much longer. The result is that if I(d) is taken from these studies, then the resulting estimates of H(t) pertain to seroconversions, not infections. In any event, one clear source of uncertainty in the estimates of H(t) is the degree to which the I(d) distribution obtained from either of these sources is applicable to the larger population of infected persons.
Assume that I(d) is known. A very simple model will illustrate both the principles and the problems involved in recovering H(t) through a procedure known as back-projection. Suppose it is known that of all HIV infections acquired in year t, 20 percent will progress to AIDS in year t + 2, 30 percent in year t + 3, and 50 percent in year t + 4. Suppose that 1980 is the first year in which AIDS cases appear. It follows that these can have resulted only from infections in 1978, since if there had been infections in 1977, there would have been AIDS cases in 1979. Suppose that one observes 100 AIDS cases in 1980, 400 in 1981, and 1,000 in 1982. One can then solve the following three equations for the three unknowns,
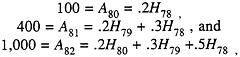
(2)
to obtain H78 = 500, H79 = 1,250, and H80 = 1,875. Thus, the prevalence of HIV infection in 1978 is 500, in 1979 is 1,750 (500 + 1,250) (minus any who have died of AIDS), and in 1980 is 3,625 (500 + 1,250 + 1,875) (minus any who have died of AIDS). Note that even at the end of 1982, one cannot obtain any estimate of the number of new infections in 1981 or 1982 since there is at least a 2-year delay between infection and AIDS. In order to get an estimate of H81 and H82 before the end of 1984, one must forecast A83 and A84 by extrapolating the prior time series of new AIDS cases or directly forecast H81 and H82 by extrapolating the estimated prior time series of new HIV infections.
This simple model can be used to identify three sources of uncertainty
in the estimates of HIV incidence and prevalence (Centers for Disease Control, 1990):
-
Estimates of new HIV infections for very recent periods are less likely to be accurate than estimates for the more distant past.
-
It is likely that the incubation distribution I(d) has changed over time as new therapies have been introduced for people who are HIV positive but are asymptomatic. In addition, changes over time in the stage of infection at which infected people are diagnosed would include changes in I(d). Furthermore, there is uncertainty about whether the I(d) distributions obtained from cohort studies of homosexual men or hemophiliacs accurately reflect the I(d) distribution for all infected people.
-
The time series of CDC counts of AIDS cases is not the time series of new AIDS cases, for two reasons. First, the case definition of AIDS has been expanded twice (in 1985 and 1987); consequently, the growth in AIDS cases is exaggerated. Second, there are delays from the time of diagnosis to the time a case is reported to the CDC. These delays would result in counts of diagnosed cases that are increasingly less complete as one moves from the past to the present. Some cases are never reported; these can be regarded as cases with infinite delays in reporting. The CDC estimates that its surveillance system identifies 70-90 percent of HIV-infection-related deaths and that it therefore provides a minimum estimate of HIV-infection-related mortality (Centers for Disease Control, 1991). Consequently, CDC counts must first be corrected for the changes in the case definition and for reporting delays before they can be used. Reporting delays may have changed over time, imparting further uncertainty into the corrected series, At (Harris, 1990).
REFERENCES
Arras, J.D. (1988) The fragile web of responsibility: AIDS and the duty to treat. Hastings Center Report 8(Suppl.):10-20.
Brandt, A.M. (1988) AIDS and metaphor: toward the social meaning of epidemic disease. Social Research 55:413-432.
Brookmeyer, R. (1991) Reconstruction and future trends of the AIDS epidemic in the United States. Science 253:37-42.
Campbell, A.M. (1931) The Black Death and Men of Learning. New York: Columbia University Press.
Centers for Disease Control (CDC) (1990) HIV prevalence and AIDS case projections for the United States: report based on a workshop. Morbidity and Mortality Weekly Report 39:(RR-16):1-31.
Centers for Disease Control (CDC) (1991) Mortality attributable to HIV infection/AIDS—United States, 1981-1990. Morbidity and Mortality Weekly Report 40:41-46.
Centers for Disease Control (CDC) (1992) HIV/AIDS Surveillance Report . Atlanta, Ga.: Centers for Disease Control.
Crosby, A.W. (1989) Epidemic and Peace, 1918: America's Forgotten Pandemic. New York: Cambridge University Press.
Fee, E., and D. Fox (1988) AIDS: The Burdens of History. Berkeley, Calif.: University of California Press.
Foege, W.H. (1988) Plagues: perceptions of risk and social responses. Social Research 55:331-342.
Grmek, M.D. (1990) The History of AIDS: Emergence and Origin of a Modern Pandemic. Princeton, N.J.: Princeton University Press.
Harris, J. (1990) Reporting delays and the incidence of AIDS. Journal of the American Statistical Association 85:915-924.
McNeil, W.H. (1976) Plagues and Peoples. New York: Doubleday.
Miller, H.G., C.F. Turner, and L.E. Moses, eds. (1990) AIDS: The Second Decade. Committee on AIDS Research and the Behavioral, Social, and Statistical Sciences, Commission on Behavior and Social Sciences and Education, National Research Council. Washington, D.C.: National Academy Press.
Nelkin, D., D.P. Willis, and S.V. Parris (1991) Introduction. In D. Nelkin, D.P. Willis, and S.V. Parris, eds., A Disease of Society: Cultural Responses to AIDS. New York: Cambridge University Press.
Risse, G.B. (1988) Epidemics and history: ecological perspectives and social responses. In E. Fee and D.M. Fox, eds., AIDS: The Burdens of History. Berkeley, Calif.: University of California Press.
Slack, P. (1988) Responses to plague in early modern Europe: the implications of public health. Social Research 55:433-453.
Tuchman, B. (1978) A Distant Mirror. The Calamitous 14th Century. New York: Knopf.
Turner, C.F., H.G. Miller, and L.E. Moses, eds. (1989) AIDS: Sexual Behavior and Intravenous Drug Use. Committee on AIDS Research and the Behavioral, Social, and Statistical Sciences, Commission on Behavioral and Social Sciences and Education, National Research Council. Washington, D.C.: National Academy Press.
Wallace, R. (1988) A synergism of plagues: ''planned shrinkage," contagious housing destruction and AIDS in the Bronx. Environmental Research 47:1-33.






















