The delivery of health care has proceeded for decades with a blind spot: Diagnostic errors—inaccurate or delayed diagnoses—persist throughout all settings of care and continue to harm an unacceptable number of patients. For example:
- A conservative estimate found that 5 percent of U.S. adults who seek outpatient care each year experience a diagnostic error.
- Postmortem examination research spanning decades has shown that diagnostic errors contribute to approximately 10 percent of patient deaths.
- Medical record reviews suggest that diagnostic errors account for 6 to 17 percent of hospital adverse events.
- Diagnostic errors are the leading type of paid medical malpractice claims, are almost twice as likely to have resulted in the patient’s death compared to other claims, and represent the highest proportion of total payments.
In reviewing the evidence, the committee concluded that most people will experience at least one diagnostic error in their lifetime, sometimes with devastating consequences. Despite the pervasiveness of diagnostic errors and the risk for serious patient harm, diagnostic errors have been largely unappreciated within the quality and patient safety movements in health care. Without a dedicated focus on improving diagnosis, these errors will likely worsen as the delivery of health care and the diagnostic process continue to increase in complexity.
Getting the right diagnosis is a key aspect of health care—it provides an explanation of a patient’s health problem and informs subsequent health care decisions. Diagnostic errors stem from a wide variety of causes, including: inadequate collaboration and communication among clinicians, patients, and their families;1 a health care work system that is not well designed to support the diagnostic process; limited feedback to clinicians about diagnostic performance; and a culture that discourages transparency and disclosure of diagnostic errors—impeding attempts to learn from these events and improve diagnosis. Diagnostic errors may result in different outcomes, and as evidence accrues, these outcomes will be better characterized. For example, if there is a diagnostic error, a patient may or may not experience harm. Errors can be harmful because they can prevent or delay appropriate treatment, lead to unnecessary or harmful treatment, or result in psychological or financial repercussions. Harm may not result, for example, if a patient’s symptoms resolve even with an incorrect diagnosis.
Improving the diagnostic process is not only possible, but also represents a moral, professional, and public health imperative. Achieving that goal will require a significant reenvisioning of the diagnostic process and a widespread commitment to change among health care professionals, health care organizations, patients and their families, researchers, and policy makers.
DEFINITION AND CONCEPTUAL MODEL
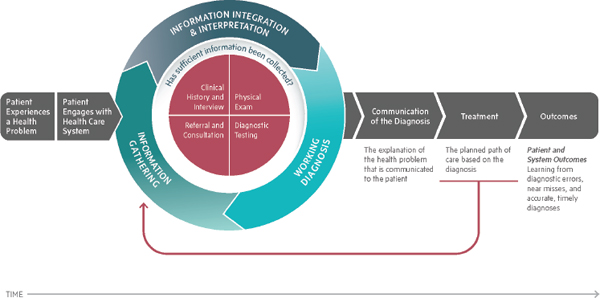
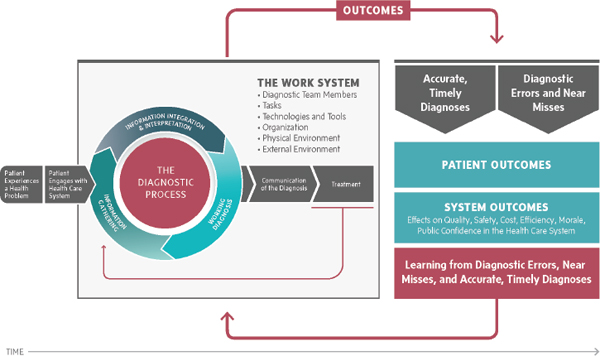
The committee concluded that a sole focus on diagnostic error reduction will not achieve the extensive change necessary; a broader focus on improving diagnosis is warranted. To provide a framework for this dual focus, the committee developed a conceptual model to articulate the diagnostic process (see Figure S-1), describe work system factors that influence this process (see Figure S-2), and identify opportunities to improve the diagnostic process and outcomes (see Figure S-3).
The diagnostic process is a complex and collaborative activity that unfolds over time and occurs within the context of a health care work system. The diagnostic process is iterative, and as information gathering continues, the goal is to reduce diagnostic uncertainty, narrow down the diagnostic possibilities, and develop a more precise and complete understanding of a patient’s health problem.
The committee sought to develop a definition of diagnostic error that reflects the iterative and complex nature of the diagnostic process, as
______________
1 The term “family” is used for simplicity, but the term is meant to encompass all individuals who provide support or informal caregiving to patients in the diagnostic process.
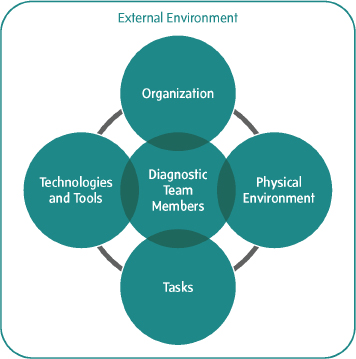
FIGURE S-2 The work system in which the diagnostic process takes place.
well as the need for a diagnosis to convey more than simply a label of a disease. The term “health problem” is used in the definition because it is a patient-centered and inclusive term to describe a patient’s overall health condition. The committee’s definition of diagnostic error is the failure to (a) establish an accurate and timely explanation of the patient’s health problem(s) or (b) communicate that explanation to the patient. The definition employs a patient-centered perspective because patients bear the ultimate risk of harm from diagnostic errors. A diagnosis is not accurate if it differs from the true condition a patient has (or does not have) or if it is imprecise and incomplete. Timeliness means that the diagnosis was not meaningfully delayed; however, timeliness is context-dependent. While some diagnoses may take days, weeks, or even months to establish, timely may mean quite quickly (minutes to hours) for other urgent diagnoses. The inclusion of communication is distinct from previous definitions, in recognition that communication is a key responsibility throughout the diagnostic process. From a patient’s perspective, an accurate and timely explanation of the health problem is meaningless unless this information
reaches the patient so that a patient and health care professionals can act on the explanation.2
In addition to defining and identifying diagnostic errors in clinical practice, the report places a broader emphasis on improving the diagnostic process. Analyzing failures in the diagnostic process can provide important opportunities for learning and continued improvement. Some failures in the diagnostic process will lead to diagnostic errors; however, other failures in the diagnostic process will not ultimately lead to a diagnostic error, because subsequent steps in the process compensate for the initial failure. In this report, the committee describes “failures in the diagnostic process that do not lead to diagnostic errors” as near misses.
A related but distinct concept to diagnostic error is overdiagnosis, defined as when a condition is diagnosed that is unlikely to affect the individual’s health and well-being. While overdiagnosis represents a true challenge to health care quality, it is not a diagnostic error. Overdiagnosis is only detectable in population-based analyses—it is virtually impossible to assess whether overdiagnosis has occurred for an individual patient. However, improving the diagnostic process—such as reducing unnecessary diagnostic testing—may help avert overdiagnosis.
RECOMMENDATIONS
The committee’s recommendations address eight goals to improve diagnosis and reduce diagnostic error (see Box S-1). These recommendations apply to all diagnostic team members and settings of care. Given the early state of the field, the evidence base for some of the recommendations stems from the broader patient safety and quality improvement literature. Patients and patient advocates have much to offer on how to implement the committee’s recommendations; leveraging the expertise, power, and influence of the patient community will help spur progress.
Facilitate More Effective Teamwork in the Diagnostic Process Among Health Care Professionals, Patients, and Their Families
The diagnostic process requires collaboration among health care professionals, patients, and their families. Patients and their families are critical partners in the diagnostic process; they contribute valuable input that facilitates the diagnostic process and ensures shared decision mak-
______________
2 Because not all patients will be able to participate in the communication process, in some instances communication would be between the health care professionals and a patient’s family or designated health care proxy.
BOX S-1
Goals for Improving Diagnosis and Reducing Diagnostic Error
- Facilitate more effective teamwork in the diagnostic process among health care professionals, patients, and their families
- Enhance health care professional education and training in the diagnostic process
- Ensure that health information technologies support patients and health care professionals in the diagnostic process
- Develop and deploy approaches to identify, learn from, and reduce diagnostic errors and near misses in clinical practice
- Establish a work system and culture that supports the diagnostic process and improvements in diagnostic performance
- Develop a reporting environment and medical liability system that facilitates improved diagnosis by learning from diagnostic errors and near misses
- Design a payment and care delivery environment that supports the diagnostic process
- Provide dedicated funding for research on the diagnostic process and diagnostic errors
ing about the path of care. Health care professionals and organizations3 are responsible for creating environments in which patients and their families can learn about and engage in the diagnostic process and provide feedback about their experiences. One strategy is to promote the use of health information technology (health IT) tools that make a patient’s health information more accessible to patients. Involving patients and their families in efforts to improve diagnosis is also critical because they have unique insights into the diagnostic process and the occurrence of diagnostic errors.
The diagnostic process hinges on successful intra- and interprofessional collaboration among health care professionals, including primary care clinicians, physicians in various specialties, nurses, pharmacists, technologists, therapists, social workers, patient navigators, and many others. Thus, all health care professionals need to be well prepared and supported to engage in diagnostic teamwork. The roles of some health care professionals who participate in the diagnostic process have been insufficiently recognized. The fields of pathology and radiology are criti-
______________
3 The term “health care organization” is used for simplicity, but is meant to encompass all settings in which the diagnostic process takes place, including integrated care delivery settings, hospitals, clinician practices, retail clinics, and long-term care settings.
cal to diagnosis, but professionals in these fields are not always engaged as full members of the diagnostic team. Enhanced collaboration among pathologists, radiologists, other diagnosticians, and treating health care professionals4 has the potential to improve diagnostic testing.5 In addition, nurses are often not recognized as collaborators in the diagnostic process, despite their critical roles in ensuring communication, care coordination, and patient education; monitoring a patient’s condition; and identifying and preventing potential diagnostic errors.
Goal 1: Facilitate more effective teamwork in the diagnostic process among health care professionals, patients, and their families
Recommendation 1a: In recognition that the diagnostic process is a dynamic team-based activity, health care organizations should ensure that health care professionals have the appropriate knowledge, skills, resources, and support to engage in teamwork in the diagnostic process. To accomplish this, they should facilitate and support:
- Intra- and interprofessional teamwork in the diagnostic process.
- Collaboration among pathologists, radiologists, other diagnosticians, and treating health care professionals to improve diagnostic testing processes.
Recommendation 1b: Health care professionals and organizations should partner with patients and their families as diagnostic team members and facilitate patient and family engagement in the diagnostic process, aligned with their needs, values, and preferences. To accomplish this, they should:
- Provide patients with opportunities to learn about the diagnostic process.
- Create environments in which patients and their families are comfortable engaging in the diagnostic process and sharing feedback and concerns about diagnostic errors and near misses.
- Ensure patient access to electronic health records (EHRs), including clinical notes and diagnostic testing results, to facili-
______________
4 Treating health care professionals are clinicians who directly interact with patients.
5 The term “diagnostic testing” is broadly inclusive of all types of testing, including medical imaging, anatomic pathology and laboratory medicine, as well as other types of testing, such as mental health assessments, vision and hearing testing, and neurocognitive testing.
-
tate patient engagement in the diagnostic process and patient review of health records for accuracy.
- Identify opportunities to include patients and their families in efforts to improve the diagnostic process by learning from diagnostic errors and near misses.
Enhance Health Care Professional Education and Training in the Diagnostic Process
Getting the right diagnosis depends on all health care professionals involved in the diagnostic process receiving appropriate education and training. The learning sciences, which study how people learn, can be used to improve education and training. For example, feedback—or information about the accuracy of a clinician’s diagnosis—is essential for improved diagnostic performance. The authenticity of the learning environment can affect the acquisition of diagnostic skills; better alignment of training environments with clinical practice promotes development of diagnostic skills.
Opportunities to improve education and training in the diagnostic process include: greater emphasis on teamwork and communication with patients, their families, and other health care professionals; appropriate use of diagnostic testing and the application of test results to subsequent decision making; and the use of health IT. In addition, the lack of focus on developing clinical reasoning and understanding the cognitive contributions to decision making represents a major gap in education within all health care professions. Proposed strategies to improve clinical reasoning include instruction and practice on generating and refining a differential diagnosis, generating illness scripts, developing an appreciation of how diagnostic errors occur and strategies to mitigate them, and engaging in metacognition and debiasing strategies.
Oversight processes play a critical role in promoting competency in the diagnostic process. Many accreditation organizations already require skills important for diagnostic performance, but diagnostic competencies need to be a larger priority within these requirements. Organizations responsible for licensure and certification can also help ensure that health care professionals have achieved and maintain competency in the skills essential for the diagnostic process.
Goal 2: Enhance health care professional education and training in the diagnostic process
Recommendation 2a: Educators should ensure that curricula and training programs across the career trajectory:
- Address performance in the diagnostic process, including areas such as clinical reasoning; teamwork; communication with patients, their families, and other health care professionals; appropriate use of diagnostic tests and the application of these results on subsequent decision making; and use of health information technology.
- Employ educational approaches that are aligned with evidence from the learning sciences.
Recommendation 2b: Health care professional certification and accreditation organizations should ensure that health care professionals have and maintain the competencies needed for effective performance in the diagnostic process, including the areas listed above.
Ensure That Health Information Technologies Support Patients and Health Care Professionals in the Diagnostic Process
Health IT has the potential to improve diagnosis and reduce diagnostic errors by facilitating timely and easy access to information; communication among health care professionals, patients, and their families; clinical reasoning; and feedback and follow-up in the diagnostic process. However, many experts are concerned that health IT currently is not effectively facilitating the diagnostic process and may even be contributing to diagnostic errors. Challenges include problems with usability, poor integration into clinical workflow, difficulty sharing a patient’s health information, and a limited ability to support clinical reasoning and identification of diagnostic errors in clinical practice. Better alignment of health IT with the diagnostic process is warranted.
Because the diagnostic process occurs over time and can involve multiple health care professionals across different care settings, the free flow of information is critical. Improved interoperability across health care organizations and across laboratory and radiology information systems is needed to achieve this information flow.
Although there may be patient safety risks in the diagnostic process related to the use of health IT, it is difficult to determine the extent of the problem. Health IT vendors often limit the sharing of information about these risks. A previous IOM report recommended that the Department of Health and Human Services (HHS) ensure insofar as possible that health IT vendors support the free exchange of information about patient safety and not prohibit sharing of such information. The present committee endorses this recommendation and highlights the need for shared information about user experiences with health IT used in the diagnostic
process. Independent evaluations of health IT products could also identify potential adverse consequences that contribute to diagnostic errors.
Goal 3: Ensure that health information technologies support patients and health care professionals in the diagnostic process
Recommendation 3a: Health information technology (health IT) vendors and the Office of the National Coordinator for Health Information Technology (ONC) should work together with users to ensure that health IT used in the diagnostic process demonstrates usability, incorporates human factors knowledge, integrates measurement capability, fits well within clinical workflow, provides clinical decision support, and facilitates the timely flow of information among patients and health care professionals involved in the diagnostic process.
Recommendation 3b: ONC should require health IT vendors to meet standards for interoperability among different health IT systems to support effective, efficient, and structured flow of patient information across care settings to facilitate the diagnostic process by 2018.
Recommendation 3c: The Secretary of Health and Human Services should require health IT vendors to:
- Routinely submit their products for independent evaluation and notify users about potential adverse effects on the diagnostic process related to the use of their products.
- Permit and support the free exchange of information about real-time user experiences with health IT design and implementation that adversely affect the diagnostic process.
Develop and Deploy Approaches to Identify, Learn from, and Reduce Diagnostic Errors and Near Misses in Clinical Practice
Due to the difficulty in identifying diagnostic errors and competing demands from existing quality and safety improvement priorities, very few health care organizations have processes in place to identify diagnostic errors and near misses. Nonetheless, identifying these experiences, learning from them, and implementing changes will improve diagnosis and reduce diagnostic errors. Health care organizations can also ensure that systematic feedback on diagnostic performance reaches individuals, care teams, and organizational leadership.
Postmortem examinations are a critical source of information on the
epidemiology of diagnostic errors, but the number of postmortem examinations has declined precipitously. A greater emphasis on postmortem examination research—including more limited approaches to postmortem examinations—is warranted to better understand the incidence of diagnostic errors and the role of postmortem examinations in modern clinical practice.
Health care professional societies can be engaged to identify high-priority areas to improve diagnosis, similar to the Choosing Wisely initiative on avoiding unnecessary care. Early efforts could focus on identifying the most common diagnostic errors, “don’t miss” health conditions that may result in patient harm, or diagnostic errors that are relatively easy to address.
Goal 4: Develop and deploy approaches to identify, learn from, and reduce diagnostic errors and near misses in clinical practice
Recommendation 4a: Accreditation organizations and the Medicare conditions of participation should require that health care organizations have programs in place to monitor the diagnostic process and identify, learn from, and reduce diagnostic errors and near misses in a timely fashion. Proven approaches should be incorporated into updates of these requirements.
Recommendation 4b: Health care organizations should:
- Monitor the diagnostic process and identify, learn from, and reduce diagnostic errors and near misses as a component of their research, quality improvement, and patient safety programs.
- Implement procedures and practices to provide systematic feedback on diagnostic performance to individual health care professionals, care teams, and clinical and organizational leaders.
Recommendation 4c: The Department of Health and Human Services should provide funding for a designated subset of health care systems to conduct routine postmortem examinations on a representative sample of patient deaths.
Recommendation 4d: Health care professional societies should identify opportunities to improve accurate and timely diagnoses and reduce diagnostic errors in their specialties.
Establish a Work System and Culture That Supports the Diagnostic Process and Improvements in Diagnostic Performance
Health care organizations influence the work system in which diagnosis occurs and play a role in implementing change. The work systems of many health care organizations could better support the diagnostic process, for example, by integrating mechanisms to improve error recovery and resiliency in the diagnostic process.
The culture and leadership of health care organizations are key factors in ensuring continuous learning in the diagnostic process. Organizations need to promote a nonpunitive culture in which clinicians can identify and learn from diagnostic errors. Organizational leadership can facilitate this culture, provide resources, and set priorities for achieving progress in diagnostic performance and reducing diagnostic errors.
Health care organizations can also work to address diagnostic challenges related to fragmentation of the broader health care system. Although improved teamwork and interoperability will help with fragmentation in health care, organizations need to recognize that patients cross organizational boundaries and that this has the potential to contribute to diagnostic errors and failures to learn from them. Strengthening communication and reliable diagnostic test reporting is one area where this can be addressed.
Goal 5: Establish a work system and culture that supports the diagnostic process and improvements in diagnostic performance
Recommendation 5: Health care organizations should:
- Adopt policies and practices that promote a nonpunitive culture that values open discussion and feedback on diagnostic performance.
- Design the work system in which the diagnostic process occurs to support the work and activities of patients, their families, and health care professionals and to facilitate accurate and timely diagnoses.
- Develop and implement processes to ensure effective and timely communication between diagnostic testing health care professionals and treating health care professionals across all health care delivery settings.
Develop a Reporting Environment and Medical Liability System That Facilitates Improved Diagnosis by Learning from Diagnostic Errors and Near Misses
Reporting
Conducting analyses of diagnostic errors, near misses, and adverse events presents the best opportunity to learn from such experiences and implement changes to improve diagnosis. There is a need for safe environments, without the threat of legal discovery or disciplinary action, to analyze and learn from these events. Previously, the IOM recommended that Congress extend peer review protections to data that are collected for improving the safety and quality of care. Subsequent legislation established the Agency for Healthcare Research and Quality (AHRQ)-administered Patient Safety Organization (PSO) program which conferred privilege and confidentiality protections to patient safety information that is shared with PSOs.
The PSO program is an important national lever to increase voluntary error reporting and analysis, but progress has been impeded by several challenges. For example, AHRQ developed Common Formats to encourage standardized event reporting, but the use of these formats is voluntary, and there is no Common Format specific to diagnostic error. Concern that the federal privilege protections do not protect organizations from state reporting requirements could also prevent voluntary submissions to PSOs and decrease the potential for improved learning. Given the PSO program’s potential to improve learning about diagnostic errors and near misses, it is important to evaluate the program.
Medical Liability
The core functions of medical liability are to compensate negligently injured patients and to promote quality by encouraging clinicians and organizations to avoid medical errors. The current approach for resolving medical liability claims sets up barriers to improvements in quality and patient safety. In addition, patients and their families are poorly served by the current system. While medical liability is broader than diagnosis, diagnostic errors are the leading type of paid medical malpractice claims.
Traditional medical liability reforms have not been effective in compensating negligently injured patients or deterring unsafe care. Alternative approaches are needed that enable patients and clinicians to become allies in making health care safer by encouraging transparency and disclosure of medical errors. These reforms can enable prompt and fair com-
pensation for avoidable injuries, while turning errors into opportunities for learning and improvement.
Communication and resolution programs (CRPs) provide a pragmatic approach for changing medical liability in that they are the most likely to be implemented. Safe harbors for adherence to evidence-based clinical practice guidelines could also help facilitate improvements in diagnostic accuracy by incentivizing the use of evidence-based diagnostic approaches; however, there are few clinical practice guidelines available for diagnosis, and implementation is complex. Administrative health courts offer a fundamental change that would promote a more open environment for identifying, studying, and learning from errors, but implementation is very challenging because of their operational complexity and resistance from stakeholders who are strongly committed to preserving the current tort-based system.
Risk Management
Professional liability insurance carriers and health care organizations that participate in captive or other self-insurance arrangements have an inherent interest and expertise in improving diagnosis. Improved collaboration between health professional liability insurance carriers and health care professionals and organizations could support education, training, and practice improvement strategies focused on improving diagnosis and minimizing diagnostic errors.
Goal 6: Develop a reporting environment and medical liability system that facilitates improved diagnosis by learning from diagnostic errors and near misses
Recommendation 6a: The Agency for Healthcare Research and Quality (AHRQ) or other appropriate agencies or independent entities should encourage and facilitate the voluntary reporting of diagnostic errors and near misses.
Recommendation 6b: AHRQ should evaluate the effectiveness of patient safety organizations (PSOs) as a major mechanism for voluntary reporting and learning from these events and modify the PSO Common Formats for reporting of patient safety events to include diagnostic errors and near misses.
Recommendation 6c: States, in collaboration with other stakeholders (health care organizations, professional liability insurance carriers, state and federal policy makers, patient advocacy groups,
and medical malpractice plaintiff and defense attorneys), should promote a legal environment that facilitates the timely identification, disclosure, and learning from diagnostic errors. Specifically, they should:
- Encourage the adoption of communication and resolution programs with legal protections for disclosures and apologies under state laws.
- Conduct demonstration projects of alternative approaches to the resolution of medical injuries, including administrative health courts and safe harbors for adherence to evidence-based clinical practice guidelines.
Recommendation 6d: Professional liability insurance carriers and captive insurers should collaborate with health care professionals on opportunities to improve diagnostic performance through education, training, and practice improvement approaches and increase participation in such programs.
Design a Payment and Care Delivery Environment That Supports the Diagnostic Process
Fee-for-service (FFS) payment has long been recognized for its inability to incentivize well-coordinated, high-quality, and efficient health care. There is limited information about the impact of payment and care delivery models on diagnosis, but it likely influences the diagnostic process and the occurrence of diagnostic errors. For example, FFS payment lacks financial incentives to coordinate care among clinicians involved in the diagnostic process, such as the communication among treating clinicians, pathologists, and radiologists about diagnostic test ordering, interpretation, and subsequent decision making.
For all medical specialties, there are well-documented fee schedule distortions that result in more generous payments for procedures and diagnostic testing interpretations than for evaluation and management (E&M) services. E&M services reflect the cognitive expertise and skills that all clinicians use in the diagnostic process, and these distortions may be diverting attention and time from important tasks in the diagnostic process. Realigning relative value fees to better compensate clinicians for cognitive work in the diagnostic process has the potential to improve diagnosis while reducing incentives that drive inappropriate diagnostic testing utilization.
E&M documentation guidelines have been criticized as onerous, often irrelevant to patient care, and preventing clinical reasoning in the diagnostic process. Payment and liability concerns, facilitated by the growth
in EHRs, have resulted in extensive clinical documentation that obscures key information in patients’ medical records, results in inaccuracies in patients’ EHRs, and can contribute to diagnostic errors.
Due to the limitations in FFS payment, a number of alternative payment and care delivery models are under evaluation; for example, half of Medicare payments are expected to be based on alternative models by 2018. There is limited evidence concerning the impact of payment and care delivery models—including FFS—on the diagnostic process and the accuracy of diagnosis, and this represents a fundamental research need. Even when alternative approaches to FFS are employed, they are often influenced by FFS. Thus, the current challenges with FFS will need to be addressed, even with the implementation of alternative payment and care delivery models.
Goal 7: Design a payment and care delivery environment that supports the diagnostic process
Recommendation 7a: As long as fee schedules remain a predominant mechanism for determining clinician payment, the Centers for Medicare & Medicaid Services (CMS) and other payers should:
- Create current procedural terminology codes and provide coverage for additional evaluation and management activities not currently coded or covered, including time spent by pathologists, radiologists, and other clinicians in advising ordering clinicians on the selection, use, and interpretation of diagnostic testing for specific patients.
- Reorient relative value fees to more appropriately value the time spent with patients in evaluation and management activities.
- Modify documentation guidelines for evaluation and management services to improve the accuracy of information in the electronic health record and to support decision making in the diagnostic process.
Recommendation 7b: CMS and other payers should assess the impact of payment and care delivery models on the diagnostic process, the occurrence of diagnostic errors, and learning from these errors.
Provide Dedicated Funding for Research on the Diagnostic Process and Diagnostic Errors
The diagnostic process and diagnostic errors have been neglected areas within the national research agenda; federal resources devoted to
diagnostic research are overshadowed by those devoted to treatment. A major barrier to research is the organization and funding of the National Institutes of Health by disease or organ systems, which facilitates the study of these specific areas but impedes research efforts that seek to provide a more comprehensive understanding of diagnosis as a distinct research area. Given the potential for federal research on diagnosis and diagnostic error to fall between institutional missions, collaboration among agencies is needed to develop a national research agenda on these topics. Because overall federal investment in biomedical and health services research is declining, funding for diagnosis and diagnostic error will draw federal resources away from other priorities. However, given the consistent lack of resources for research on diagnosis, and the potential for diagnostic errors to contribute to patient harm and health care costs, funding for this research is necessary for broader improvements to the quality and safety of health care. In addition, improving diagnosis could potentially lead to cost savings by preventing diagnostic errors, inappropriate treatment, and related adverse events.
In addition to federal-level research, there is an important role for public–private collaboration and coordination among the federal government, foundations, industry, and other stakeholders. Collaborative funding efforts extend the existing financial resources and reduce duplications in research efforts. Parties can unite around areas of mutual interest and spearhead progress.
Goal 8: Provide dedicated funding for research on the diagnostic process and diagnostic errors
Recommendation 8a: Federal agencies, including the Department of Health and Human Services, the Department of Veterans Affairs, and the Department of Defense, should:
- Develop a coordinated research agenda on the diagnostic process and diagnostic errors by the end of 2016.
- Commit dedicated funding to implementing this research agenda.
Recommendation 8b: The federal government should pursue and encourage opportunities for public–private partnerships among a broad range of stakeholders, such as the Patient-Centered Outcomes Research Institute, foundations, the diagnostic testing and health information technology industries, health care organizations, and professional liability insurers to support research on the diagnostic process and diagnostic errors.