Appendix B
Background Paper for a Workshop on Exploring a Business Case for High-Value Continuing Professional Development
Ronald Cervero, Uniformed Services University of the Health Sciences, and Holly Wise, American Council of Academic Physical Therapy
The purpose of this paper is to provide background and context for the upcoming workshop “Exploring a Business Case for High-Value Continuing Professional Development (CPD).” There are two main elements to this workshop. The first is to distinguish high-value CPD from CPD and continuing education (CE). The second is to understand what a business case is and how it can be used within the context of high-value CPD.
CONTINUING EDUCATION TO CONTINUING PROFESSIONAL DEVELOPMENT
Drawing from the 2010 Institute of Medicine (IOM) report Redesigning Continuing Education in the Health Professions, “CE often is associated with didactic learning methods, such as lectures and seminars, which take place in auditoriums and classrooms.” It is often viewed by health professionals as a path to maintaining licensure and certification through the accumulation of credits. Conversely, CPD embraces a wider array of learning formats and methods that are learner driven. Countries such as Canada, New Zealand, the United Kingdom, and those within the European Union have embraced CPD as a way of “maintaining, improving, and broadening knowledge and skill throughout one’s professional life.” It focuses on individual performance improvement that might drive quality and safety in a clinical environment and the health and well-being of populations in a public health setting.
CPD TO HIGH-VALUE CPD
High-value CPD is outcomes driven. Those outcomes—which may benefit the practitioner, individuals and patients, the team or collaboration, and populations—demonstrate value or the business case for improving health and health care in any or all of the identified stakeholders. Other stakeholders include funders, providers, governments, and regulators. For the purpose of this workshop, the value proposition for CPD is defined as an equation: Value = (Quality + Outcomes)/Cost. According to the 2010 IOM report, “Arriving at the value proposition for CPD will be essential to understanding the best ways to invest CPD resources.”
BUSINESS CASE FOR HIGH-VALUE CPD
Leatherman et al. (2003) define a business case for a health care improvement that was adapted to high-value CPD for this workshop. A business case for high-value CPD exists if
the entity that invests in the intervention realizes a financial return on its investment in a reasonable time frame, using a reasonable rate of discounting. This may be realized as “bankable dollars” (profit), a reduction in losses for a given program or population, or avoided costs. In addition, a business case may exist if the investing entity believes that a positive indirect effect on organizational function and sustainability will accrue within a reasonable time frame. (p. 18)
Most financial investors like to see a return on their investment within 1 to 2 years, although social investors and governments tend to be more willing to extend the timeline for demonstrating the intended outcomes. However, rarely do business cases extend beyond 5 years. Researching the value proposition is essential for making the business case that a CPD intervention will provide the intended return on investment within the defined period of performance. If the business case is approved, there will need to be financial and programmatic data collection and evaluation to demonstrate the positive return. This can be done using a variety of cost analysis tools that are described on page 85. Of note is that a business case may not demonstrate a financial return, but the value shown to its users may tip the balance so the decision is made to move forward with the business case despite the unlikely positive financial return. In addition, maintaining ethical standards of providers and financers of CPD is essential for guarding against potential conflicts of interest.
COST ANALYSIS TERMS
Cost–benefit analysis is the evaluation of alternatives according to their costs and benefits when each is measured in monetary terms (Walsh et al., 2013).
Cost/benefit ratio can be thought of as one stakeholder’s benefit is another stakeholder’s cost (Walsh et al., 2013).
Cost-effectiveness analysis refers to the evaluation of two or more alternative educational approaches or interventions according to their costs and their effects in producing a certain outcome (Walsh et al., 2013).
Cost-feasibility analysis involves simply measuring the cost of a proposed intervention in order to decide whether it is feasible, that is, whether it can or cannot be considered (Walsh et al., 2013).
Cost-utility analysis is the examination of two or more alternatives according to their cost and their utility. In this context, utility means the satisfaction among individuals as a result of one or more outcomes or the perceived value of the expected outcomes to a particular constituency. Data on user satisfaction can be derived in a number of ways, such as by analyzing the results of questionnaires or interviews. Cost-utility analysis is closely related to cost-effectiveness analysis (Walsh et al., 2013).
Fixed costs are expenses that must be paid by an organization regardless of any business activity (Walsh et al., 2013).
Net present value is the present value of money—a dollar today is worth more than a dollar will be in 2 years (Hooper, 2007).
Opportunity costs are the value of the best alternative that was not chosen in order to pursue the current endeavor, as in “What could have been accomplished with the resources expended in the undertaking?” It represents opportunities forgone (TRB, 2005).
Quality-adjusted life year (QALY) is a measure of the benefit of a medical intervention based on the number of years of life that would be added by the intervention. If the extra years would not be lived in full health, for example, if the patient would be blind, then the extra life-years are adjusted by a factor to account for this.
Return on investment (ROI) measures the amount of return on an investment relative to the investment’s cost. It is calculated as the following ratio (Investopedia, 2017):
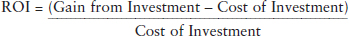
Value proposition: Value = (Outcomes + Quality)/Cost (Wehrwein, 2015).
Variable costs are costs that vary directly with the rate of output, such as labor, fuel, power, or cost of raw material. Also known as operating costs, prime costs, or direct costs (TRB, 2005).
REFERENCES
Hooper, P.K. 2007. FREP Handheld Business Case. https://www.for.gov.bc.ca/ftp/hfp/external/!publish/frep/ciworkshop/2007/tab10/Business-Case-FREP-Handheld.pdf (accessed November 6, 2017).
Investopedia. 2017. Return on investment-ROI. http://www.investopedia.com/terms/r/returnoninvestment.asp#ixzz4c9oxMQlq (accessed October 10, 2017).
IOM (Institute of Medicine). 2010. Redesigning continuing education in the health professions. Washington, DC: The National Academies Press.
Leatherman, S., D. Berwick, D. Iles, L. S. Lewin, F. Davidoff, T. Nolan, and M. Bisognano. 2003. The business case for quality: Case studies and an analysis. Health Affairs (Millwood) 22(2):17–30.
TRB (Transportation Research Board). 2005. Cost-benefit analysis of providing non-emergency medical transportation. Washington, DC: The National Academies Press.
Walsh, K., H. Levin, P. Jaye, and J. Gazzard. 2013. Cost analyses approaches in medical education: There are no simple solutions. Medical Education 47(10):962–968.
Wehrwein, Peter. 2015. The new equation of American health care. Managed Care 24(8):18–20.




