Summary
Legionnaires’ disease afflicts and kills more people in the United States than any other reportable waterborne disease. It is caused by bacteria of the Legionella genus, with the majority of diagnosed cases (from 80 to 90 percent) linked to Legionella pneumophila. Humans are primarily exposed to Legionella through inhalation of contaminated aerosols into the respiratory system. Patients infected with Legionella can develop pneumonia (classic Legionnaires’ disease) or a milder flu-like condition called Pontiac fever; both conditions are referred to as legionellosis. Legionnaires’ disease can be fatal, with between 3 and 33 percent of Legionella infections leading to death. Those at higher risk for developing Legionnaires’ disease include the elderly, males, smokers, and the immunosuppressed. In the United States, the reported incidence of Legionnaires’ disease increased more than six-fold from 2000 to 2018 (Figure S-1). Worldwide, the actual burden of Legionnaires’ disease is generally acknowledged to be underreported, by as much as eight- to ten-fold.
Legionella bacteria reside in many natural environments including rivers, lakes, and soils. They grow optimally inside protozoan hosts, such as free-living amoebae associated with microbial biofilms that coat wet surfaces. Hence, it is not surprising that these bacteria can be found in a variety of engineered systems that support biofilm growth, including drinking water distribution systems, building plumbing systems, faucets, showerheads, cooling towers, hot tubs, and fountains. These water systems are sometimes characterized by warm temperatures, stagnant water, excess nutrients due to pipe corrosion, and a lack of chemical disinfectants—conditions that promote the growth of biofilms, their associated protozoa, and consequently Legionella. When these built environments generate contaminated aerosols, humans in the vicinity can be exposed to Legionella via inhalation or aspiration. Most of our knowledge of Legionnaires’ disease comes from investigations of disease outbreaks, instances where two or more people are infected at the same time by the same source. However, the vast majority of Legionnaires’ disease cases (greater than 95 percent) are sporadic cases for which the primary exposure source is never identified.
In the 40 years since the discovery of L. pneumophila, much has been learned about its ecology, whereas less progress has been made in preventing Legionnaires’ disease or
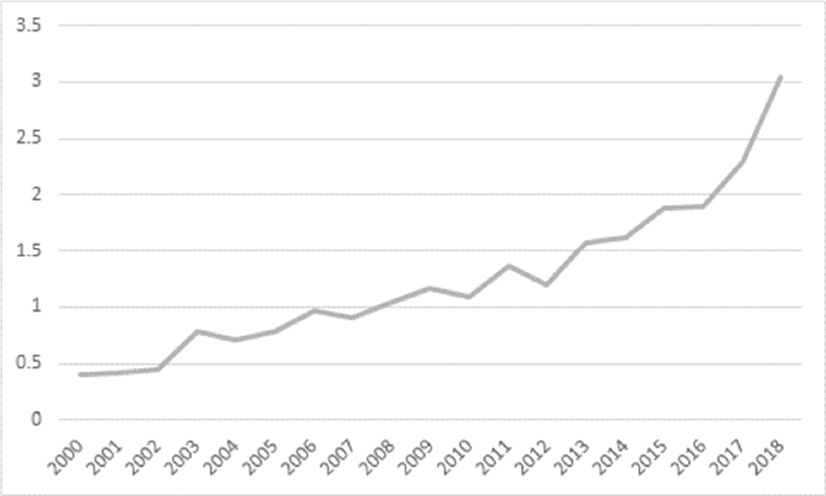
SOURCES: 2000-2002 data adapted from Shah et al. (2018); 2003-2013 data from Adams et al. (2015); 2014 data from Adams et al. (2016); 2015 data from Adams et al. (2017); 2016, 2017, and 2018 data from the National Notifiable Disease Surveillance System.
understanding the ecology of different species of pathogenic Legionella. Methods for monitoring both the disease incidence and L. pneumophila in water samples have evolved considerably, for both culture-based and molecular techniques. Yet, treatment of water systems to reduce colonization by Legionella continues to be complicated by the microbe’s complex ecology and the diversity of systems in which Legionella can thrive. Moreover, although the Safe Drinking Water Act has been effective in reducing disease rates of waterborne enteric organisms in the United States, it has had little impact on managing Legionella in water systems and buildings.
In late 2017, the National Academies of Sciences, Engineering, and Medicine convened an expert committee (the Committee on Management of Legionella in Water Systems) to review the state of the science with respect to Legionella contamination of water systems and issue a report that addresses the following:
- Ecology and Diagnosis: Describe the microbial ecology of water supplies (from the source to the tap and within built systems) as it relates to Legionella. What strains of L. pneumophila are of most concern and how can their diagnosis be improved (e.g., in terms of increased specificity, simplicity, and speed)?
- Transmission via Water Systems: What are the primary sources and routes of human exposure to Legionella? What features/characteristics of water systems make them more or less likely to support growth of Legionella?
- Quantification: Considering surveillance data, case studies of outbreaks, hospital data, other routine testing of water systems, what is known about the concentration of Legionella in water systems and the prevalence of Legionnaires’ disease over the past 20 years? How uncertain are these estimates and what can be done to reduce this uncertainty? How can quantitative risk assessment be improved?
- Prevention and Control: What are the most effective strategies for preventing and controlling Legionella amplification in water systems? What are the best methods to prevent exposure to Legionella, especially in at-risk populations? Is there a minimum level of contamination required to cause disease? What are the benefits, risks, gaps in implementation, and barriers to uptake of Legionella control programs?
- Policy and Training Issues: What policies, regulations, codes, or guidelines affect the incidence, control, quantification, and prevention of Legionnaires’ disease? How might they be built upon to better protect the public? How can Legionella control be best balanced with other water priorities?
ORGANIZATION OF THE REPORT
Chapter 2 discusses Legionnaires’ disease, the life history and complex ecology of Legionella in both natural and built water environments, and common exposure pathways. Chapter 3 focuses on the surveillance of Legionnaires’ disease in the United States, methods to detect Legionella, and the results of environmental Legionella monitoring in different built water systems. Chapter 4 considers the many strategies used to control Legionella, including the use of heat, biocides, flow control, plumbing materials, aerosol formation prevention, and distal devices, along with their application in several typical built environments. Finally, Chapter 5 takes on the array of laws, regulations, codes and standards, and guidance documents that relate to Legionella management, both in the United States and abroad. This final chapter makes suggestions for how these various policy tools can be strengthened to better protect the public from legionellosis. Each chapter ends with conclusions and recommendations that synthesize more technical and specific statements found within the body of each chapter. The most important conclusions and recommendations are repeated in this summary.
DIAGNOSIS, ECOLOGY, AND EXPOSURE PATHWAYS
Since its discovery in the 1970s, more than 61 species of Legionella have been described, half of which have been isolated from patients. In North America and Europe, L. pneumophila is the most dominant Legionella species isolated from patients. Other species can lead to disease, including L. micdadei, L. bozemanii, L. dumoffi, and L. longbeachae. In Oceania and parts of Asia, disease due to L. longbeachae approaches or exceeds that for L. pneumophila. The various species of Legionella differ in their virulence, infectivity, and preferred growth conditions (e.g., protozoan hosts and environmental factors). Yet what is known about legionellae ecology is almost exclusively based on studies with L. pneumophila. Similarly, a troublesome aspect of Legionnaires’ disease diagnosis is the overreliance on the urinary antigen test, which only detects L. pneumophila serogroup 1.
L. pneumophila can adapt to environmental change by differentiating into replicative, transmissive, filamentous, mature infectious, and viable-but-not-culturable-like (VBNC-like) cells—forms that differ in their infectivity and their response to water treatment technologies. Even more complicated is that as pathogenic legionellae grow to high concentrations in free-living protozoa, infectious bacteria may be released within aerosols in various forms: as free cells, cells within biofilm fragments, or cells associated with free-living protozoan trophozoites, cysts, or expelled vesicles. A deeper understanding of Legionella ecology and of the genetic traits that equip Legionella strains to colonize engineered water systems, to survive in aerosols, and to thrive in the human lung is required. The following conclusions and recommendations for research are found in Chapter 2.
There is a need to better understand the mechanistic pathways for the development of Pontiac fever, and what roles the pathogen, endotoxins, Legionella-harboring amoebae, or other exposures play in disease pathogenesis. Because Pontiac fever is associated with less mortality, focused studies examining this clinical entity have been limited to date. There is a need to develop improved diagnostic tools for Pontiac fever (including molecular methods) that would enhance overall Legionella epidemiology and outbreak investigation.
Protocols should be developed to generate, identify, enumerate, and report distinct Legionella cell types. The capacity of L. pneumophila to resist detergents, heat, chemical disinfectants, and antibiotics, as well as predatory amoebae and white blood cells depends on its growth phase. The resilience and infection potential differ by orders of magnitude for replicative, stationary or transmissive phase, and the mature infectious form of L. pneumophila.
Whether L. pneumophila persistence within built water systems is promoted by the bacterium’s differentiation into an apparent viable-but-non-culturable state that is both resilient and reversible remains an urgent question with implications for public health. To date, studies of VBNC-like L. pneumophila are largely descriptive. Protocols to generate and isolate pure populations of VBNC-like cells for physiological, biochemical, genetic, molecular, and infection studies are needed.
Ecological studies have almost exclusively focused on the impact of environmental conditions on growth, survival, and inactivation of L. pneumophila. To clarify whether the ecological principles observed for L. pneumophila also apply to other pathogenic Legionella species, research on the ecology of L. longbeachae, L. micdadei, L. dumoffi, and other pathogenic Legionella species is warranted. The ecological conditions responsible for L. pneumophila growth in environments such as cooling towers, wastewater treatment plants, soils, and hot springs are largely unexplored compared to building water systems (i.e., premise plumbing).
Whether legionellae persist within free-living protozoa versus growing to high numbers appears to be influenced by many poorly understood factors, including temperature, species of bacterial prey available, presence of host symbionts, and host cell form. Direct observations and metagenomic studies of microbial diversity are required to identify the protozoa that control the growth of pathogenic Legionella in various environments. Microcosm studies could investigate how nutrients and biocides affect the life stages of the host protozoa (e.g., by triggering encystation), identify the key host species, and elucidate the role of other free-living protozoa that might feed on the primary hosts of legionellae.
QUANTIFICATION OF LEGIONELLA AND LEGIONNAIRES’ DISEASE
Chapter 3 addresses Legionnaires’ disease rates from surveillance systems and the occurrence of Legionella bacteria in various water systems including the methods used to detect Legionella in clinical and environmental samples. Monitoring of both Legionnaires’ disease and Legionella bacteria in the environment is fraught with difficulties, including which pneumonia patients are tested to diagnose the cause of their infection, where and when to sample in the environment, what detection methods to use, and how to interpret the data. More and improved environmental monitoring is needed to examine (1) the national occurrence of Legionnaires’ disease and Legionella concentrations in different built environments, (2) the environmental conditions and amplification niches for the bacteria, and (3) the sources of exposure for both sporadic and outbreak-associated Legionnaires’ disease.
Surveillance data show that Legionnaire’s disease rates have been rising in the United States and in Europe over the past 20 years. Current incidence rates are understood to be a substantial underestimate of the actual disease burden for many reasons, including the lack of adequate diagnostic testing among pneumonia patients in most U.S. hospitals and the virtual absence of diagnosis for outpatients. Using data from previous studies and current surveillance systems, the Committee estimates that the number of persons with Legionnaires’ disease ranges from 52,000 to 70,000 in the United States each year.
By reviewing dozens of Legionella studies from various building types from around the world, the Committee found the available Legionella occurrence data are highly variable and sparse, making comparisons among studies difficult and detection of spatial and temporal trends almost impossible. Available data suggest that cooling towers, hot tubs, showers, and wastewater treatment plants can be hot spots for growth of Legionella and exposures. Several studies that recorded concentrations of culturable Legionella were compiled to determine if and when concentration could be indicative of outbreaks of Legionnaires’ disease. A Legionella concentration of 5 × 104 colony-forming units per liter (CFU/L) should be considered an “action level,” that is, a concentration high enough to warrant serious concern and trigger remediation. A lower action level may be necessary to protect those at higher risk for legionellosis, such as hospital patients, particularly those in intensive care, cancer, and solid-organ transplant units. Additional conclusions and recommendations about Legionnaires’ disease surveillance, environmental monitoring data, and quantitative microbial risk assessment are found below.
There is an urgent need to develop better clinical tools that will capture more cases of Legionnaires’ disease and identify pathogenic Legionella beyond L. pneumophila serogroup 1. Hospitals in both rural and urban areas should have access to on-site urinary antigen testing to facilitate more targeted antimicrobial therapy and to increase disease recognition. Efforts to develop standardized molecular methods for Legionella diagnoses (including non-pneumophila species and serogroups other than serogroup 1) should be prioritized by research laboratories and federal agencies. Finally, the U.S. Department of Health and Human Services should target research funding to multi-center prospective studies of clinical respiratory samples using these new assays to better understand prevalence and diversity of the Legionella species and serogroups causing disease.
An improved understanding of sporadic, community-acquired cases of Legionnaires’ disease is critical to reducing the rising rates observed over the past 20 years. Determining the most common sources of sporadic disease will require well-funded, population-based studies in multiple jurisdictions (e.g., cities, counties, states). Such studies would require the recruitment of multiple medical centers with an adequate number of Legionella cases each year, willingness and capacity to collect clinical samples for Legionella culture, personnel with knowledge of how to sample the most likely sources of exposure for legionellosis patients, and laboratory capacity to reliably grow Legionella from clinical and environmental samples.
Regional Centers of Excellence for prevention and control of legionellosis could serve as a backbone to strengthen the capacity of state health departments to detect and investigate cases of Legionnaires’ disease. Such centers could be modeled on the Integrated Food Safety Centers of Excellence and the Centers of Excellence for Vector Borne Diseases, with modifications to include the relevant disciplines needed for Legionella applied research and control. These centers could promulgate best practices for prevention and control measures and they could train and assist building managers as they create water management plans.
They could also help coordinate the in-depth, multiple-jurisdiction studies of environmental exposures recommended above.
A systematic study to compare culture methods for L. pneumophila (and other pathogenic legionellae) with quantitative polymerase chain reaction (qPCR), viability-qPCR, and reverse transcriptase qPCR is needed to determine comparability. qPCR and its variants offer a more rapid method to quantify Legionella in the environment, and could be used consistently to inform decisions on decontamination and restoration of affected systems, to investigate the bacteria’s ecology and exposure pathways, and as a quality control method. With side-by-side comparisons of methods in a broad range of settings, it may be that PCR-based or other simplified methods or test kits could be shown to be useful predictors of human health risk and adequacy of remediation.
There is a good framework to perform quantitative microbial risk assessment (QMRA) for various L. pneumophila exposures. QMRA can be used to determine Legionella concentrations in building water systems that correspond to certain Legionnaires’ disease risk levels; such information can be used, for example, to inform design and permitting decisions about pipe length, setback distances for large industrial cooling towers, and building-level hydraulic design to maintain acceptable microbial quality. To further advance QMRA, additional knowledge is needed about the impact of virulence and strain differences, phenotypic alterations in potency and aerosol survival, and generation rate of aerosols from various devices. Data on exposures, especially for cooling towers, are lacking.
STRATEGIES FOR LEGIONELLA CONTROL AND THEIR APPLICATION IN BUILDING WATER SYSTEMS
Chapter 4 focuses on strategies for Legionella control in building water systems. The controls considered are temperature control, disinfection, hydraulic management, nutrient limitation, choice of plumbing materials, distal devices, and prevention of aerosols. The chapter then discusses how specific controls are applied to building water systems, considering large engineered systems such as potable water supply, wastewater treatment, and reclaimed water systems, large institutional buildings and households, cooling towers and humidifiers, and hot tubs. The chapter also discusses several emerging issues, such as potential conflicts among strategies for green building design, water and energy conservation, and more prospective Legionella control strategies.
For any given building water system, multiple strategies can be successfully employed and should be used. The effectiveness of many of the controls are interdependent; for example, optimal hydraulics is required for effective delivery of thermal control and chemical disinfectant while reactivity of the plumbing materials and the water source chemistry could lead to disinfectant decay. Different strategies available for controlling Legionella in water systems are feasible at different stages of a building’s life cycle, with some being most important during initial construction (e.g., the choice of plumbing materials) while others are implemented during ongoing operation and maintenance (e.g., disinfection and flushing). The conclusions and recommendations below highlight key takeaways with respect to Legionella control strategies for various building and device types.
For all types of buildings, hot-water heater temperature should be maintained above 60°C (140°F), and the hot-water temperature to distal points should exceed 55°C (131°F). Maintaining temperature outside Legionella’s preferred growth range is the paramount
Legionella control strategy for all buildings that provide hot water and has been proven successful by numerous longitudinal field studies. Temperature control is most effective in large, complex hot-water systems that are hydraulically balanced, with dead-end pipes removed and faulty devices that compromise the distribution of hot water identified and replaced.
There is growing evidence that, compared to free chlorine, a monochloramine residual better controls Legionella risk from building water systems, although the reasons for the improved performance are not yet clear. It is possible that amoebae trophozoites are more sensitive to monochloramine, causing the amoebae to encyst and thus preventing the proliferation of Legionella within their host. Additional research is needed to examine the precise action of monochloramine on Legionella persistence and growth within pipe biofilms.
Research is needed to better understand the persistence of distribution system disinfectant residuals within building plumbing. Public water supplies that maintain a disinfectant residual and manage hydraulics to prevent stagnation are helping to reduce Legionella exposure from the distribution system. Nonetheless, it is unclear to what extent the disinfection residual can achieve Legionella control within premise plumbing, for both single-family homes and small buildings as well as larger buildings.
Guidance about Legionella is needed for homeowners, especially consumers from at-risk segments of the population. In particular, there is a need to identify plumbing configurations and devices that inadvertently increase risk of Legionella proliferation as well as accessible, practical control options such as flushing taps after periods of disuse. Residential water systems can benefit from most of the control strategies discussed in Chapter 4, yet they are almost never formally implemented because of a lack of understanding or awareness on the part of homeowners and occupants.
Low-flow fixtures should not be allowed in hospitals and long-term care facilities because of these buildings’ high-risk occupant populations. Low-flow fixtures have been promoted to conserve water and, in some cases, energy. Because of their lower flow, however, these fixtures, primarily low-flow faucets but also showers, increase water age and restrict disinfectant levels, including the disinfection provided by elevated water temperatures. As such, low-flow fixtures present a greater risk for Legionella development in the plumbing systems that feed them.
New designs are needed to help advance control of Legionella in cooling towers and humidifiers. Humidifier designs that produce water droplets within the temperature range conducive to Legionella growth should be avoided for use in new buildings, and existing units of these types should be replaced during building renovations. Strategies relying on disinfectants should consider using alternate types of biocides at regular intervals, since bacteria can regrow in cooling towers when biocide use is infrequent and irregular. Finally, cooling tower manufacturers should collectively design new systems that can operate at condenser water temperatures whereby the temperature going to the cooling tower will be greater than 60°C.
Green buildings have exacerbated many of the problems with Legionella by lengthening water residence times (which leads to loss of disinfectant residual) and lowering hot-water temperatures in premise plumbing. Criteria for certifying green buildings, energy-conserving features, and water-conserving features should be modified to take into account risk factors
for Legionella growth. Substantial water conservation can still be potentially achieved while protecting public health with more overt management of water age, for example, through routine flushing.
REGULATIONS AND GUIDELINES ON LEGIONELLA CONTROL IN WATER SYSTEMS
Unlike Australia, Canada, and many European countries, the management of Legionella in water systems in the United States occurs on an ad hoc basis, ranging from no requirements at all to regulations that require some buildings to have water management plans that include Legionella monitoring of water samples along with treatment. The federal Safe Drinking Water Act does not provide any substantial control of Legionella in water systems.
Regulations in the United States that affect Legionella management (by requiring water management plans or monitoring of water systems for Legionella) currently cover healthcare facilities in New York State, cooling towers in New York City and New York State, healthcare facilities within the Veterans Health Administration, and hospitals and healthcare facilities receiving Medicare or Medicaid funds. All other buildings and private residences are potentially protected from Legionella only through the application of building and plumbing codes. The following recommendations are made to develop a more comprehensive policy for Legionella management in the United States.
Expand the Centers for Medicare & Medicaid Services (CMS) Memorandum to Require Monitoring for Legionella in Environmental Water Samples. The CMS memo of 2017 requires that hospitals and long-term care facilities receiving CMS funding develop and implement water management plans. This memo has appropriately targeted buildings in which the mortality rates of Legionnaires’ disease are high because of the vulnerable patient population. Routine quantitative Legionella monitoring programs would enable these institutions to assess the effectiveness of their water management programs. Such enhanced data collection from within hospital systems could help refine the data thresholds needed for prevention. This emphasis on Legionella monitoring is supported by international regulations, by the Veterans Health Administration (VHA) directive and the New York State regulations, and by guidance from the American Industrial Hygiene Association (AIHA).
Register and Monitor Cooling Towers. Regulations and guidelines requiring the registration of cooling towers provide a demonstrable public health benefit with minimal regulatory burden to building owners and managers. Cooling tower registries enable a rapid public health response to community clusters of legionellosis cases, including timely remediation of possible sources of infection, and they can also be used to assess the contribution of cooling towers to overall disease incidence. In addition, regulations requiring ongoing Legionella monitoring of cooling towers have been shown to reduce cooling tower colonization rates in jurisdictions where they have been implemented (e.g., Quebec and Garland, Texas).
Require Water Management Plans in All Public Buildings Including Hotels, Businesses, Schools, Apartments, and Government Buildings. The standard of care specified for water management plans should be considered best management practice for all public buildings. The recommendation here is to codify what are currently voluntary standards for managing public buildings. ASHRAE 188, AIHA (2015), and other guidance documents are available to help create a water management plan that can meet this requirement. Ideally, this requirement would be codified by either local jurisdictions with authority (such as building
inspectors) or state authorities (such as departments of environmental protection or health). Once codified, the requirements could be supported by insurance companies; that is, without a water management plan, a building would not qualify for insurance.
Require a Temperature of 60°C (140°F) at Hot-Water Heaters and 55°C (131°F) to Distal Points. Optimal operating temperatures at critical points in the hot-water system are based on an international consensus that maintaining minimum temperatures across the different parts of a hot-water system is the first barrier to implement to restrict Legionella growth. Monitoring temperature at the distal points of hot-water systems would be necessary to verify that this requirement is being met. These temperature requirements could be codified by changing building and plumbing codes or by modifying the CMS memo. There is also the possibility of these requirements being incorporated into guidance documents as they undergo revision in the future.
***
The recommendations discussed above are not prioritized; accomplishing any one of them would lead to important legionellosis risk reduction, with a cumulative effect as more of them are accomplished. The recommendations differ substantially in their necessary implementation schedule, which entities would provide oversight, their cost, and what other capacities need to be in place to support them. In particular, the additional monitoring requirements will necessitate the development of guidelines to interpret monitoring data. QMRA could play an important role by, for example, being used to develop routine operational targets for different types of building water systems to determine that the risk of legionellosis is acceptably low. Finally, it will be important to expand training and education on legionellosis and on the prevention and control of Legionella amplification in water systems. Education and training are particularly needed for those designing water systems, those overseeing municipal water supplies, those developing and implementing plumbing codes, those responsible for maintenance of water operations and premise plumbing, and those in government who are responsible for the safety of buildings, cooling towers, and the potable water supply.










