5
Cross-Sector Workforce: National and Local Examples
Session moderator Gary Gunderson from the Wake Forest Baptist Medical Center, also representing Stakeholder Health, opened by providing a brief background on the session. It featured speakers from entities and organizations promoting population health by supporting other sectors in their efforts to incorporate a population health perspective into their missions, activities, and programs.
TRAIN LEARNING NETWORK AND COMPETENCIES FOR POPULATION HEALTH PROFESSIONALS1
Ron Bialek from the Public Health Foundation (PHF) outlined a two-part presentation. First, he gave an overview of the TrainingFinder Real-time Affiliate-Integrated Network (TRAIN) Learning Network, which has evolved from a narrow focus on governmental public health to one that is applicable to a broader range of health professionals, volunteers, and others.2 Bialek then discussed the recently developed competencies for population health professionals.
Bialek explained that the mission of PHF is to improve public health and population health practice to support healthier communities.3 He
___________________
1 This section summarizes information presented by Ron Bialek from PHF. The statements made are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
2 More information about the TRAIN Learning Network and its courses is available at https://www.train.org/main/welcome (accessed May 10, 2021).
3 More information about PHF is available at http://www.phf.org/Pages/default.aspx (accessed May 10, 2021).
added that workforce development is key to that mission. He described that one of the organization’s strategic goals was recently changed from “create opportunities for public health and health care alignment” to “create opportunities for cross-sector alignment,” reflecting that addressing population health and community health involves more than the public health and health care sectors.
Fifteen years ago, Bialek added, PHF created the TRAIN Learning Network in response to a need from state and local public health departments to find, access, and track training opportunities. The network has grown to more than 1.8 million users with 10 million courses completed. The network offers 4,300 free courses delivered by more than 3,000 providers. Current users include about half of the governmental public workforce (263,250 people in public health agencies), about 600,000 people in health care, and about 450,000 people in private industry, nonprofit organizations, and other industries. There are also users in other government agencies, including transportation and behavioral health, and other sectors, including construction companies, places of worship, renewable energy companies, and brokerage firms.
The top jobs of TRAIN’s users in public health and health care include nurses, emergency responders, public health and health care administrators, health officials, and frontline workers (see Figure 5-1).
Outside of public health and health care, the top TRAIN user roles are emergency responders, volunteers, management, and students. Students may receive non-degree-oriented training through the system that supplements their formal education (see Figure 5-2).
TRAIN addresses issues such as general public health, emergency preparedness, planning and policy, budgeting, and grants management. Bialek highlighted some examples of specific population health training topics, such as where to find and how to use data, healthy homes, food insecurity, principles of building construction, creating safe buildings, and
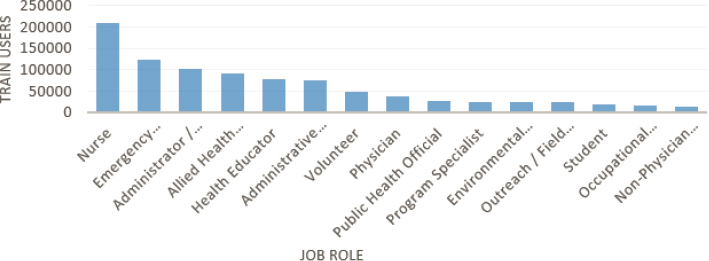
SOURCE: Bialek presentation, March 22, 2019.
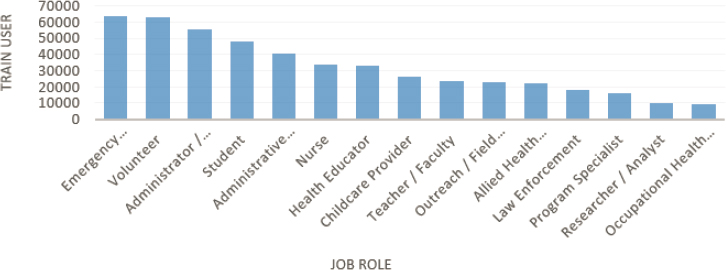
SOURCE: Bialek presentation, March 22, 2019.
skateboard parks. Leading topic areas for people outside of public health and health care include HIV/AIDS, preparedness and response, communications tools for health care professionals, and the Health Insurance Portability and Accountability Act (HIPAA). Leading topic areas for public health and health care professionals include preparedness and response, HIPAA, people with disabilities, and civil rights. Bialek noted that the data are available to researchers interested in doing further analysis.
Bialek next described work to provide guidance on the skills and competencies important for practicing population health. Population health competencies were intended to be cross-disciplinary and not address a specific role. In developing the competencies, PHF used a lengthy feedback process involving hospitals, the American Association of Medical Colleges, public health agencies, the Association of State and Territorial Health Officials, the National Association of County and City Health Officials, and broad public input. The process resulted in 57 competencies across 6 domains: community engagement, community health assessment, community health improvement planning and action, health equity and cultural awareness, systems thinking, and organizational planning and management.
As Bialek explained, PHF got involved in developing population health competencies after providing public health competencies to hospital professionals at the Association for Community Health Improvement annual meeting. The foundation also hosted a workshop with 40–45 hospital and health professionals to refine the public health competencies. These competencies were ultimately directed toward people working in community benefit for hospitals and health systems. The foundation held several public comment periods to gather input, learned that interest in the competencies extended beyond people working in community benefit,
and decided to revise them to make them broadly applicable to people working toward population health in all settings and disciplines.
Bialek next described some of the competencies in a few key domains. Community engagement competencies included describing the historical and current conditions affecting health in a community and collaborating with organizations to maximize use of community assets and resources. For example, Bialek noted that it is important to understand historical conditions with respect to adverse childhood experiences. Community health assessment competencies included describing factors affecting community health (e.g., inequity, income, education, environment, demographic trends, and legislation) and using informatics and information technology to access, collect, analyze, use, maintain, and disseminate data and information. Bialek explained that these data could include electronic health records and information on who is purchasing what, where. Health equity and cultural awareness competencies included communicating in writing and orally with linguistic and cultural proficiency and ensuring that the diversity of individuals and populations is addressed in policies, programs, and services that affect community health. Bialek noted that there are also competencies related to evaluating the extent to which this happens and considering unintended consequences. Within the category of systems thinking, one competency is explaining ways community development is funded to improve the health of populations at the local level. This involves describing activities of community development financial organizations and strategies for leveraging them as funding sources. The systems thinking competency describes the impact the organization is having on the health of the community.
As Bialek explained, PHF has developed training plans to support workers in developing the population health competencies. These plans are a compilation of some of the best trainings available through TRAIN and address specific topics, such as health equity and social determinants of health that cut across many competencies in various domains related to population health.
In closing, Bialek described next steps for PHF regarding TRAIN and the population health competencies. The foundation is exploring adding these competencies into TRAIN to allow people to search for trainings by competency. TRAIN already includes searchable competencies for public health professionals. The foundation is also exploring developing other training plans, similar to the social determinants of health training plan, for people who are not in public health or health care to help them identify what is most important for them to learn regarding population health. Bialek noted that the foundation is also working to disseminate the competencies through a range of partners and networks, using platforms such
as presentations, workshops, webinars, and interest groups. For example, the foundation is part of a social determinants innovation collaborative that involves 40–45 health systems and is working to help participating organizations understand and use the competencies.
Be a Change Leader, Build a Culture of Health4
Brian Smedley from the National Collaborative for Health Equity (NCHE) and the Robert Wood Johnson Foundation (RWJF) Culture of Health Leaders Program opened by explaining that his presentation would also describe a program focused on building a community of leaders who are well trained to work across sectors and within their own sector to build a culture of health.
The RWJF Culture of Health Leaders Program is relatively young, recruiting its fourth cohort of leaders as of this workshop, although the first cohort has not yet completed it.5 Smedley pointed out that RWJF’s investment in leadership development has been the largest within the health sector, and the foundation has also recognized the need to reach and train leaders in other sectors. The program was developed a few years ago, when RWJF sunsetted some of its legacy leadership programs. RWJF has four new leadership programs:
- Health Policy Research Scholars, which supports graduate students committed to conducting research to address policy questions involving underserved populations that face inequities;
- Interdisciplinary Research Leaders, an innovative program that pairs researchers with community members to form more cohesive teams of collaboration across communities and campuses;
- Clinical Scholars, an innovative program connecting clinical professionals with community members to address problems; and
- Culture of Health Leaders Program (the topic of Smedley’s presentation).
Smedley explained that NCHE co-leads the Culture of Health Leaders Program with CommonHealth ACTION. Other innovative program partners include the Institute for Alternative Futures, the Center for Creative Leadership, the Leadership Learning Community, the American Planning
___________________
4 This section summarizes information presented by Brian Smedley from NCHE and the RWJF Culture of Health Leaders Program. The statements made are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
5 More information about the Culture of Health Leaders Program is available at https://cultureofhealth-leaders.org (accessed May 10, 2021).
Association (APA), and the Build Healthy Places Network, which connects public health with the community development sector.
The Culture of Health Leaders Program is a 3-year, intensive, advanced leadership development initiative that provides formal leadership training, professional coaching, and peer coaching. It challenges participants to conduct strategic, evidence-based work that changes conditions in organizations and communities. It is grounded in the principles of equity and social justice and focuses on addressing the root causes of inequity in systems and structures.
As Smedley described, the program has selected up to 40 leaders per year for the past 3 years from a range of disciplines and sectors, including arts, education, and policy. For example, one leader is a firefighter from Detroit. Current leaders are geographically diverse and represent nearly all 50 states and the District of Columbia; a future goal is to have leaders from all 50 states and the District of Columbia.
Smedley listed some of the characteristics of leadership program participants. They come to the program with well-developed leadership skills and tremendous expertise but are highly motivated, ready to learn, and planning to accelerate their leadership and engage more deeply with communities to realize the vision of healthy, equitable spaces. Participants embrace complexity and risk taking, strive to increase their influence and network more broadly, and intend to extend their work through these networks. Participants must commit 32–38 hours per month for 3 years.
The program model is based around developing four areas of mastery: environment, relationships, change, and the self. Mastery of environment is being able to understand historical and contemporary political and social challenges. Mastery of relationships is being able to bring out the best in others. Mastery of change is sustaining systemic changes. Mastery of self is having awareness and discipline to exert leadership. Smedley highlighted that the goal of the program is for leaders to be at the nexus of these four areas and able to influence others through their decisions, behaviors, and actions.
Smedley outlined the program progression; in year 1, the focus is on competencies related to self and relationships. Information is provided through in-person training, virtual learning, coursework, assessments, executive coaching, and peer coaching. In year 2, the focus is on mastery of environment and change. Activities include executive coaching, peer coaching, and ongoing assessments with the Center for Creative Leadership. In year 3, leaders begin to implement a strategic initiative in their communities focused on all four areas of mastery.
Smedley pointed out that mastery of self includes self-management, self-regulation, self-insight, and self-development (see Figure 5-3). Mastery of relationships includes the ability to build collaborative relation-
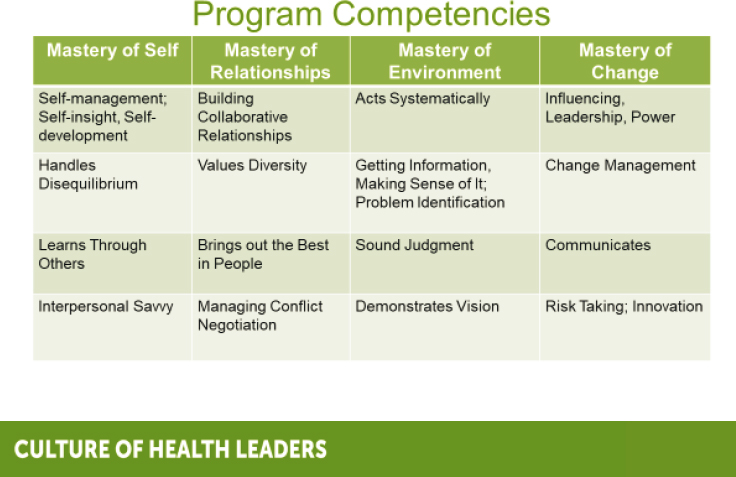

SOURCE: Smedley presentation, March 22, 2019.
ships and to bring out the best in people working across lines of difference. Mastery of the environment includes acting and thinking systemically, distilling complex information about complex problems that require sound judgment. Mastery of change includes being able to influence and lead others, communicate, and sustain meaningful change.
NONTRADITIONAL STUDENT TRAINING THROUGH THE BLOOMBERG AMERICAN HEALTH INITIATIVE6
Michelle Spencer from the Bloomberg American Health Initiative opened by explaining that her presentation would address training nontraditional students in public health through that initiative. Spencer began with some brief history on the initiative.7 As she explained, about 3 years ago, the Bloomberg Philanthropies provided a $300 million gift to the Johns Hopkins Bloomberg School of Public Health in honor of the school’s centennial. The funds were to address the recent decline in health expec-
___________________
6 This section summarizes information presented by Michelle Spencer from the Bloomberg American Health Initiative. The statements made are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
7 More information about the Bloomberg American Health Initiative is available at https://americanhealth.jhu.edu (accessed May 10, 2021).
tancy in the United States. The Bloomberg American Health Initiative aimed to use the tools of public health—education, research, policy, and action—to address health challenges in five focus areas: (1) addiction and overdose, (2) the environment, (3) obesity and the food system, (4) risks to adolescent health, and (5) violence. Cross-cutting themes included social, economic, and health equity; data and evidence; and policy levers, barriers, and needed changes.
This gift provided for 25 endowed professorships and a fellowship program offering up to 50 full tuition annual scholarships for M.P.H. degree students and 10 for Dr.P.H. degree students. As Spencer described, the fellowship program involved three areas of focus: education, research, and policy. The goal of the program is to have an impact and engage individuals in nontraditional spaces with responsibilities and actions that can inadvertently positively affect health outcomes.
As of the date of the workshop, 37 fellows representing 15 states, the District of Columbia, and 1 territory had initiated the program and 2 had completed it. Approximately 40 percent of the fellows represented local, state, and federal health agencies. Others came from nongovernmental organizations, and many had nontraditional backgrounds (outside of public health). Spencer provided examples of a few fellows’ experiences. Alison Miller worked for the North Carolina Office of the Chief Medical Examiner and had seen firsthand the growing number of young people who were dying of overdoses. She applied to the fellowship program wanting to understand what her office could do to support people and communities experiencing substance abuse. Amanda Capitummino worked with Sitkans Against Family Violence, a nonprofit organization in Alaska providing services to victims of domestic violence and sexual assault. She wanted to learn what could be done to address violence in her community. Jennifer Spiller in Grand Rapids worked with the Healthy Home Coalition of West Michigan, focusing on environmental challenges in the home. Spiller was interested in addressing what could be done to support healthy housing for individuals with asthma symptoms due to air quality issues. Ashley Hickson in Houston, Texas, worked with the American Heart Association to address food access in communities and implications for obesity, heart disease, and mortality. Veronica Helms from the Department of Housing and Urban Development (HUD) was focused on adolescent health and wanted to know how HUD’s health and housing initiatives intersect with adolescent health and what federal-level policies impacting health she could help to inform. The final example was Haven Wheelock in Portland, Oregon, who worked with a nonprofit organization called Outside In, which ran the first publicly funded needle/syringe exchange program.
Spencer explained that each fellowship program applicant was required to submit an application to the program along with their organization. The program could be completed either part time online or
full time in Baltimore. While the School of Public Health has clear academic requirements, courses were also informed by fellows’ organizations through bimonthly check-in calls. Organizations identified specific topics that would be useful, including health disparities, suicide prevention, and the opioid crisis, from a problem-solving perspective. Some of these topics were addressed through seminars. Participating organizations identified other training needs, including leadership development, advocacy, media and communications, and program implementation. Organizations providing fellows could also receive funding directly through the program for specific public health projects. For example, the Cherokee Nation was funded to conduct data assessments related to opioid use disorders, and ChangeLab Solutions, Indiana University, Child Justice, and the Fort Lauderdale Police Department wanted to conduct research with program faculty, connect with similar organizations around the country, and receive guidance related to policy change.
After completing the program, fellows were required to commit to going back to their organization and staying for at least 1 year. The intent of the program was for the fellows to educate those organizations about the tools of public health, the importance of achieving public health goals, and how public health can inform their processes.
As Spencer noted, nearly two-thirds (62 percent) of fellows were from nontraditional organizations, and 96 percent were women. The fellows represented diversity in terms of organizational and geographic area (see Figures 5-4 and 5-5). Spencer closed by stating that a goal is to have public health advocates in nontraditional public health spaces across the United States.
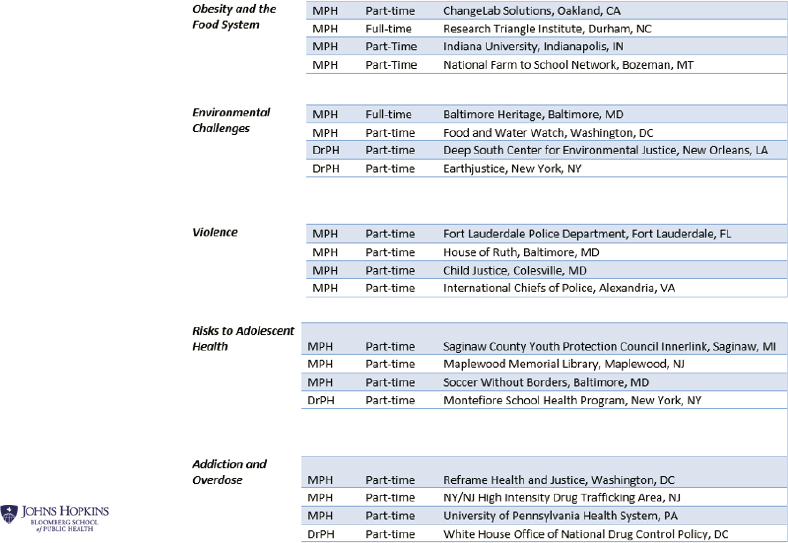
SOURCE: Spencer presentation, March 22, 2019.
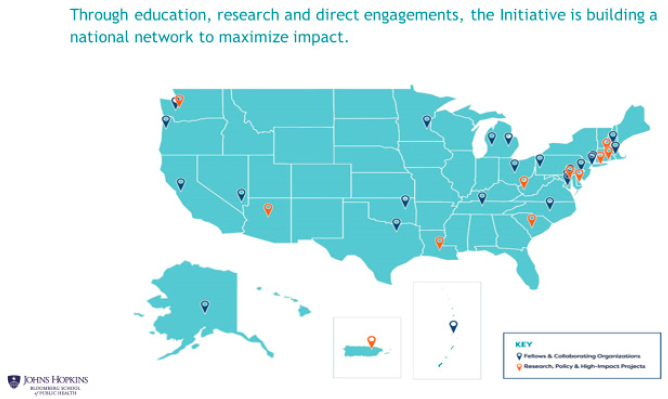
SOURCE: Spencer presentation, March 22, 2019.
PLANNING AND PUBLIC HEALTH
Sagar Shah spoke on behalf of APA. He described the connection between planning and public health, how APA and the planning community have integrated public health and equity into their activities,8 and how planning and public health practitioners collaborate in theory and in practice.
Shah began by describing the intersection between planning and public health from a historical perspective. As he explained, until the end of the 19th century, planning and public health were synonymous. By the beginning of the 20th century, public health started moving away from engineering-based solutions to people-based approaches and initiatives, and planners began to focus on designing cities and communities. This changed in the 1980s and 1990s, when public health and planning united with the Healthy Cities movement, which emphasized the importance of addressing social determinants of health. According to Shah, since the beginning of the 21st century, public health and planning have worked together well, but there is still room for improvement.
Many aspects of public health are determined by factors beyond health care. Shah provided several examples of domains for planning healthy communities. One example is whether communities are walk-
___________________
8 This section summarizes information presented by Sagar Shah from APA. The statements made are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
able or car dependent, impacting people’s ability to be physically active. He noted that subdomains of active living include active transportation (going from one place to another with a purpose) and active recreation (activities such as going to parks and on walks and jogs). Another subdomain of active living is traffic safety. Planners also play an important role in influencing access to healthy foods through land use and zoning decisions and in creating inclusive public spaces that support social cohesion. An additional example was emergency preparedness and climate change. Planning can influence climate change by impacting carbon emissions from automobiles, which vary depending on whether development is sprawled or compact.
Shah next provided background on APA, including its organization and activities related to public health.9 APA is the largest membership organization for planners in the world, advocating excellence in planning and promoting education and citizen empowerment. Many of its members work in government at various levels. The organization has more than 45,000 members from all states and territories. There are 47 chapters, representing all 50 states, and 21 divisions focused on specific topics or groups of population, including sustainability, transportation, economic development, and women in planning. APA also has interest groups, which are established prior to formal divisions. One such interest group is the Healthy Communities Collaborative; it has more than 750 members, more than half of whom are public health professionals, and is focused on cross-sector collaboration between planning and public health.
APA also has a Planning and Community Health Center, managed by Shah. That center is one of the three flagship sponsored-research programs in APA’s research department. The center provides members with tools and training to integrate health and equity into planning at all levels of government. Shah provided some examples of its projects: creating healthy neighborhoods, the role of planners in health impact assessments, benefits of street-scale features, food systems and access to healthy foods, and access to physical activity locations. In recent years, APA’s Planning and Community Health Center has also worked to focus on emerging issues, such as the impact of climate change on health and the role of planners, how gentrification impacts health, and how planners can play a role in housing policy. The Center’s work falls into three broad categories: (1) applied research, including reviews of the academic and gray literature and development of reports and tools for members; (2) place-based work, including the flagship program PLAN4Health, which provided funding for 35 community coalitions involving public health and planning
___________________
9 More information about APA and its initiatives is available at https://www.planning.org (accessed May 10, 2021).
representatives and community-based organizations to address access to healthy foods or access to physical activity locations; and (3) training and education, including webinars, toolkits, and other resources for members. An example is a three-part webinar series on the role of planners in curbing the opioid epidemic.
Shah also provided examples of APA’s broader projects. One was a place-based project integrating health and equity into comprehensive plans in collaboration with The Pew Charitable Trusts and RWJF. The partnership has supported three communities in integrating health and equity into their city-level comprehensive plans. Another project involves creating educational models to help planners identify sites for Early Care and Education facilities in areas affected by disasters, accomplished in partnership with the National Environmental Health Association and the Centers for Disease Control and Prevention. Shah noted that partnerships—and particularly cross-sector partnerships—are an important component of APA’s strategy. Partners include national membership organizations, federal agencies, foundations, universities, and local organizations.
Shah closed by sharing a joint call to action to promote healthy communities of eight national organizations working at the intersection of built environment and health, including APA, the American Institute of Architects, the American Public Health Association, the American Society of Civil Engineers, the American Society of Landscape Architects, the National Recreation and Park Association, the Urban Land Institute, and the Green Building Council.10 The goal is to have these organizations’ local members come together in their own communities to talk about health and cross-sector partnership.
HEALTH IN ALL POLICIES IN FAIRFAX COUNTY, VIRGINIA11
Anna Ricklin from the Fairfax County Health Department in Fairfax County, Virginia, described her role as a “health in all policies manager” and how it helps to promote health in all policies within the department. As Ricklin explained, she has training in public health with urban planning and transportation, having worked previously with APA and the Baltimore City Department of Transportation. Her position is in the Office of Innovation in the Fairfax County Health Department, the goal of which is to promote “Public Health 3.0” and create a culture of health. The
___________________
10 For more information, see https://www.planning.org/nationalcenters/health/calltoaction (accessed May 10, 2021).
11 This section summarizes information presented by Anna Ricklin from the Fairfax County Health Department in Fairfax County, Virginia. The statements made are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
Office of Innovation also includes a workforce strategist and a research analyst focused on special projects. One of these special projects involved developing a plan to address the opioid crisis within the county. Following delivery of that plan, the county executive hired an opioid director to implement it. The workforce strategist is focused on addressing workforce capacity within the health department, including how best to retain staff and provide career plans and opportunities for growth and development, which may include working with other agencies within Fairfax County and returning to the health department with new knowledge and cross-sector training and experience. Ricklin’s role is to serve as an ambassador for public health to agencies across the county, including those not typically considered to be public health actors. She has begun to build relationships with leaders in the departments of planning and zoning, transportation, housing, and neighborhood and community services. She highlighted that having someone from the health department embedded within other agencies has been key to advancing cross-sector collaboration and bringing health into new conversations.
Ricklin described the process to establish her position, noting that before she was even hired, there was an effort to build support for her position with other agencies. For example, during the interview process, Ricklin met with leaders of the county agencies overseeing health, transportation, urban planning, and land development. She noted that the director of the health department wanted these cross-sector leaders to have buy-in on who was hired to ensure that their staff in other departments would know their leadership supported working with the person in Ricklin’s position. She said there was initially pushback on hiring a city planner from the human resources department within the health department, because they had never done that before.
To facilitate interaction with staff within the county’s land development and zoning agencies, Ricklin’s physical office is located in the same building as the Departments of Planning and Zoning and Land Development Services, rather than the health department. Ricklin noted that a key component of her role is “gathering intelligence” through participating in meetings where the health department historically has not been represented, seeking to obtain information about other agencies’ plans and priorities and where there might be an opportunity for the health department to engage. For example, the health department could conduct a health impact assessment of a proposed development project. Ricklin completed a “desktop health impact assessment” of a large hospital development where there were concerns about community safety due to increased traffic and other impacts. She used a health equity and social determinants of health lens to assess factors extending beyond increased access to quality health care. Ricklin pointed out that her job is unique, with only “a hand-
ful” of health department staff across the country focused on health in all policies as their main job. As she stated, the position provides a new approach to cross-sector partnership and policy making.
Ricklin also described cross-sector training in the county. She noted that a 6-week course, called the Joint Training Academy, was developed out of an initiative called Fairfax First, which was designed to streamline land development. The course is open to all county staff and focuses on the land development process, including the comprehensive plan, zoning, permitting, and other complexities. There is also an ongoing lunch and learn series, for which she presented a session on health and all policies to land development staff. Another example was a healthy community design summit that the health department hosted a few years before with stakeholders from across the county, including leadership from land development, transportation, planning, zoning, and communities.
The county sponsors a Master of Public Administration (M.P.A.) degree at George Mason University for county employees. Students apply through the county, with their supervisor’s approval, and take courses in the evenings. The health department also recently finalized a new program for employees to receive a public health certificate at George Mason University that is also paid for by the county. As Ricklin explained, the certificate requires half the credits of an M.P.H. degree, providing an incentive for health department employees to continue their education toward an M.P.H. on their own. She noted that there is interest among health departments in other Northern Virginia cities and counties in offering a similar program to their employees.
DISCUSSION
Gunderson began the discussion portion of the session by encouraging the panelists to ask questions of each other. Ricklin began by asking Spencer how the Bloomberg American Health Initiative has changed the dialogue within the Johns Hopkins Bloomberg School of Public Health about what is public health. Spencer responded that one concrete impact of the initiative has been to demonstrate the need for more flexibility regarding the admission requirements of the School of Public Health. She noted that all fellowship program participants must first apply to the school, which used to recommend that all applicants have at least 2 years of health-related experience. However, lawyers or law enforcement officials who lack this experience would otherwise be good candidates for the program. The school has allowed flexibility in considering the other credentials and experience that these candidates bring and sometimes helped them take classes to qualify for acceptance. She also noted that the leadership of the school and department heads has also recognized the
importance of creating courses to meet partner organizations’ needs and doing things differently than they have in the past.
After Gunderson opened the discussion to the audience, Donna Grande from the American College of Preventive Medicine pointed out that there are more than 4,000 preventive medicine physicians and residents in medical colleges and schools of public health across the country, who could serve as allies and leaders in promoting community-based change. Grande clarified that preventive medicine physicians are doctors who typically also have an M.P.H. degree and additional training or experience in health departments. She pointed out that they hold about three-quarters of health officer positions. Grande asked Shah for any examples of situations in which APA worked with preventive medicine physicians within health departments or outside of government. While Shah did not have any specific examples to offer, he stated that the eight organizations that formed the call to action he described have been meeting regularly to discuss joint strategy and long-term goals. He noted that there has been discussion about including other organizations in the call to action, such as a transportation organization, and there could potentially be an opportunity to include preventive medicine physicians as well.
Both Gunderson and Kevin Barnett from the Public Health Institute and the California Health Workforce Alliance used the terms “disruptors” and “transformational” to describe the panelists. To achieve similar transformational, structural change in other organizations, Gunderson asked whether there is a need for more individual disruptors or if additional, broader changes must take place within organizations or government agencies. Bialek responded that, in collaboration with the Center for Creative Leadership and Leadership Learning Community, they are building “collaborative leadership,” which they define as leadership that understands the need for broader frames and ways of communicating across fields of understanding and deep engagement with communities. Bialek pointed out that common characteristics of many of RWJF’s leadership programs are that community linkages are critically important and community members have power. He stated that he believes public health is moving toward building collective efficacy and harnessing political power, clarifying that if the ultimate goal is to build collective power, collaborative leadership is essential.
Hanh Cao Yu from The California Endowment added that she appreciated Wiggins’s comment that CHW training often involves popular education. She noted that her organization is focused on power building involving those most affected, which resonates with the community rootedness and attention to well-being of the CHW role. Yu also highlighted an important question raised by Barnett of how to ensure that health care providers return to their communities following formal education and training.
Michael Rhein from the Institute for Public Health Innovation asked Ricklin whether she received pushback from other agencies that the health in all policies concept is too centered on public health and would be better if it were more broadly focused on equitable, prosperous communities. Ricklin responded that while the terminology “health in all policies” may not always resonate across agencies, the concepts do, and she often explains the concepts using examples. She noted that she is still working on developing the best messaging but generally recommends using other agencies’ language and terminology whenever possible. Ricklin added that the concept of equity has gained momentum in the county, such as the One Fairfax policy adopted in 2017 that requires using an equity lens with all policy-making projects across the county. Ricklin is part of a team led by the chief equity officer to operationalize that policy. Points made by the speakers in this section are highlighted below (see Box 5-1).
















