4
Effects of Wildfires on Human Health
Wildfires have many acute and chronic effects on human health. They can cause respiratory and cardiovascular symptoms, burns, trauma, mental health effects, reproductive and immunological disorders, and a wide array of outcomes associated with social and financial disruption.
Six speakers at the workshop discussed these effects, including ways to minimize them.
THE HEALTH EFFECTS OF WILDFIRE SMOKE
Wildfires emit many air pollutants that have impacts on human health, including carbon monoxide, nitrogen dioxide, polycyclic aromatic hydrocarbons, volatile organic compounds (VOCs), particulate matter, and ozone. But most of the evidence in the epidemiological literature focuses on particulate matter, and specifically on fine particulate matter of less than 2.5 microns (PM2.5), observed Colleen Reid, assistant professor in the Department of Geography at the University of Colorado Boulder, in her review of the research literature on the health effects of wildfire smoke (Reid and Maestas, 2019; Reid et al., 2016). These particles are much smaller than the width of a human hair, which is typically 50 to 70 microns, or a particle of fine beach sand, which is about 90 microns wide. The concern is that these particles, which make up most of the plume of smoke from a wildfire, can get deep into the lungs and cause biological damage. Particles also can affect the cardiovascular system by causing pulmonary oxidative stress and inflammation, and the autonomic nervous system can be triggered. Some of the smallest particles can even cross into the bloodstream and travel throughout the body.
Almost every study that has investigated associations between smoke exposure and respiratory health outcomes has found significant associations with asthma exacerbation. Exacerbations of chronic obstructive pulmonary disease are also significantly associated with higher wildfire smoke in most studies, and evidence is growing of a link between wildfire smoke and respiratory infections, including pneumonia and bronchitis.
Many studies of cardiovascular disease and wildfire smoke have been null, but a few recent studies have found significant associations (Reid et al., 2016). Some of these newer studies have looked at particularly sensitive populations, including populations over age 65 or people who already have heart disease. Some have also looked at very specific endpoints, such as out-of-hospital cardiac arrests; and at exposure to multiple fires, which yields more statistical power to detect an effect. “We need to do more research to understand these differences and why we are seeing significant findings for cardiovascular disease in some studies but not in others.”
A few studies have found clear evidence of an impact between wildfire smoke and all-cause mortality, but no clear evidence yet exists for specific causes of mortality, such as respiratory or cardiovascular deaths. Again, said Reid, more research needs to be done into the mechanisms of biological damage and the possible causes of death.
A large and growing literature has assessed the effects of air pollution on birth outcomes, though much less has been done on wildfire smoke and
birth outcomes. In a study of wildfires that occurred in southern California in 2003, exposure to smoke was associated with a small but significant decline in birthweight, with more significant associations in the second and third trimesters (Holstius et al., 2012). “It is a very small effect, but it is over a very large population. We know that low birthweight can have an effect on long-term health outcomes, and therefore we need more research to look at other possible birth outcomes and at maternal health.”
In a paper published right before the workshop, Reid et al. (2019) found that ozone during the 2008 northern California wildfires was associated with an increased risk of respiratory hospitalizations. However, in multipollutant models, the effect went away for ozone but remained for PM2.5—likely because, in this specific fire, PM2.5 levels were about six times higher than normal, whereas ozone levels were not much higher than average during the fires and only exceeded the National Ambient Air Quality Standards (NAAQS) a few times. More research should be done to look at the background concentrations of ozone, the precursors of ozone, and a fire’s impact on ozone, she said, because the impacts of other fires on ozone concentrations, and thus health, could differ from what was found in this one study.
Most studies have found mental health impacts of wildfire smoke exposure, including posttraumatic stress disorder (PTSD) and depression. However, many of these studies were of populations that not only were exposed to smoke but also were evacuated or lost property or loved ones. Furthermore, these studies are susceptible to self-report bias, because they involve interviewing people and doing surveys after the fire, with people estimating both their exposure to smoke and their mental health impacts. “I still think that this is an important finding,” said Reid. In one qualitative study involving in-depth interviews of individuals in a few communities in the Northwest Territories in Canada, many of them First Nations communities, some of the quotations were particularly telling about the mental health impacts of a summer in which it was so smoky that people had to stay indoors (Dodd et al., 2018). As one respondent said,
It was like we didn’t have a summer, for me, because usually we get outside, we do things on the water. . . . We enjoy being in the North. We enjoy being outside. We enjoy the environment. We enjoy cooking. Everything that’s outside, we enjoy, and I feel like I lost that. . . . That impacts you emotionally and mentally.
Even in a place like California, said Reid, where the winters are not long and cold, being told to stay indoors in the summer could have mental health impacts.
Some subpopulations can be more impacted by wildfire smoke than the total population. A meta-analysis by Kondo et al. (2019) found that
only 10 studies in the literature on health and wildfire smoke had examined effect modification by different population characteristics, which limited the ability to look at differences by subgroups. A key finding was that lower levels of respiratory emergency department visits for youth occurred compared with adults and the elderly. Also, women were much more likely than men to go to the emergency department for respiratory health impacts, though that result was heavily influenced by the results of a single study. Too few studies have examined differences by socioeconomic status or race and ethnicity to draw conclusions. “We need to look at this more.”
Reid listed several pressing research questions:
- The long-term health impacts of repeated exposures to wildfires
- Other health endpoints related to wildfire smoke that have not been studied, including metabolic disorders, cognitive decline, child development, and maternal health
- Why findings differ across studies, particularly for cardiovascular disease
- Effects on vulnerable populations
- Impacts of other air pollutants in wildfire smoke, not just particulate matter
- The health impacts from ozone based on a wider variety of wildfires
- The effectiveness of public health interventions
CHALLENGES AND LIMITATIONS OF WILDFIRE SMOKE EXPOSURE RESEARCH
Reid also discussed some of the difficulties of ascertaining the effects of wildfire smoke on health. First, studying wildfires inevitably poses epidemiological challenges. Researchers do not know when a fire is going to happen, so they have to study health impacts after a fire has occurred and rely on health datasets that were collected earlier for comparison. Cascio (2017) pointed out that everyone exposed to wildfire smoke would be expected to have some subclinical effects for which they would feel no symptoms, such as an asymptomatic decrease in lung function or heart rate variability. But some more susceptible individuals would experience respiratory, cardiovascular, or other symptoms (for which it may be necessary to use or increase medications); emergency department visits, urgent care, physician office visits, and restricted activity days; and hospitalizations and death (see Figure 4-1). Epidemiologists tend to focus on hospitalization and death records or on records of emergency department visits, which are available and regularly collected. Only a few studies have looked at physician visits, medication refills, or symptoms. “In a way, we are only getting the tip of the iceberg in terms of the health impacts from smoke exposure,” said Reid.
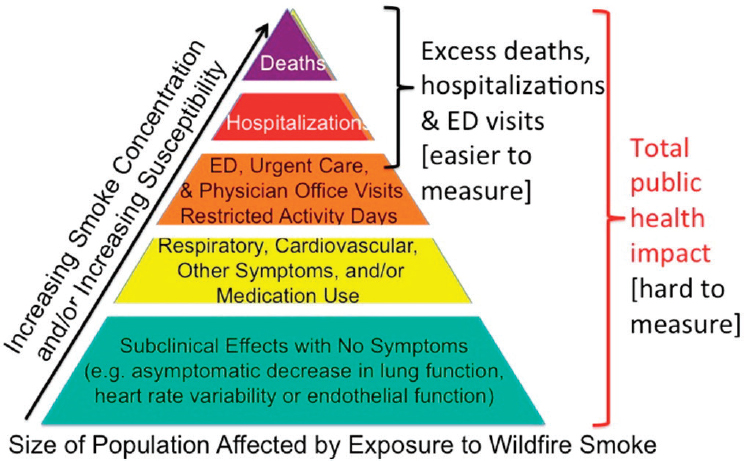
NOTE: ED = emergency department.
SOURCES: Presented by Colleen Reid. Cascio, 2017.
Assessing exposures is also difficult. When wildfire smoke moves through an area, it does not affect all portions of that area equally. Furthermore, even after a fire is contained, it can continue to smolder and release smoke.
Difficulties with measuring exposures make it hard to arrive at conclusions regarding the dose–response relationship. The health effects caused by an increased PM2.5 exposure cannot be calculated with certainty if the exposure is uncertain.
To quantify smoke exposure, “the first place to turn is monitoring data, and there’s a lot of this available,” said Reid. The U.S. Environmental Protection Agency (EPA) provides data on its website, as does the California Air Resources Board. However, monitors are not always in the location a researcher might prefer. For example, EPA’s monitors are often in urban areas, not in areas close to where a wildfire is burning. Also, smoke plumes are usually not well mixed. Under a plume, exposure can be very high, while nearby it is much lower.
Many EPA PM2.5 monitors only measure every third or sixth day, but wildfire smoke can change dramatically from day to day. “I’ve looked at satellite imagery of a smoke plume that’s captured every half hour, and you can see [it] meandering due to wind patterns,” Reid said. Even people
close to a monitor might get a different exposure than what the monitor detects.
Given the difficulties with monitors, researchers are increasingly turning to satellite data. Reid talked mostly about aerosol optical depth, which is a measure of the amount of light scattered by particles in the atmosphere. Benefits of this measure are that it provides full spatial coverage, except for cloud masking, and that it is an actual measurement of particle loading in the atmosphere. However, satellites measure the entire atmospheric column, not the particle concentration just at ground level. “If the smoke is aloft and very high, it will be picked up by the satellite, but it won’t actually be what people are breathing.”
Air-quality models can estimate particle concentrations at multiple elevations including at ground level. They can also allow researchers to assess the counterfactual—they can run the model with the wildfire emissions and run it without the wildfire emissions to calculate what the air quality would have been had the fires not happened. This can be informative in assessing the health impact of just the wildfire smoke. The disadvantage of such models is that their results can differ widely from the monitoring data because of the estimation of the emissions from the fire, how they are transported, and the chemical reactions of the air pollutants. One of the biggest uncertainties in models involves how much air pollution is being emitted from fires, which depends on the temperature of the fire and the height at which the smoke is being injected into the atmosphere.
To counter the uncertainties in satellite data, monitoring data, and air-quality models, exposure assessment researchers are increasingly using blended models that combine satellite data and monitoring data, and sometimes air-quality models and other data. For example, Gan et al. (2017) and Lassman et al. (2017) have used geographically weighted regressions to blend a variety of datasets to estimate PM2.5 exposures during wildfires, while Reid et al. (2015) and Yao et al. (2018) have used machine learning methods. The latter, for example, select from a long list of predictor variables and from a variety of statistical algorithms. Such an approach combines the strengths and weaknesses of different data sources to get better estimates of air quality that can be used for epidemiological purposes. Reid’s research group is putting together a dataset to do this kind of daily modeling for PM2.5 for an 11-year period across the western United States. To capture the wildfire component, it is using data on fire locations and the distance to the fire as important predictors. It hopes to make the output open data that everyone can use for studies of air pollution and health in the western United States.
However, blended models incorporate assumptions and include errors that can cause their performance to vary temporally and spatially, and these need to be understood, Reid said. To further improve models, Reid urged
that more comparisons be done among exposure models while possible errors are integrated into epidemiological models.
Finally, she briefly mentioned the use of social media, either on its own or in blended models, to estimate exposure. For example, Ford et al. (2017) found that Facebook posts do a better job than satellite data alone of estimating smoke exposure. Another option might be cheaper and more numerous sensors or personal monitoring.
Following Reid’s presentation, Colleen Ryan, a surgeon who represents the American Burn Association, pointed out that smoke inhalation increases mortality and the risk of infections in patients. She also asked whether some of the effects of exposure to fires might be due to emotional trauma rather than smoke inhalation. Reid acknowledged that trauma is a confounder, so that low birthweights in a population exposed to a wildfire could be due to stress and anxiety rather than or in addition to smoke exposure. “If they are highly correlated then it would be hard to disentangle that. I do not think any studies have tried to do so.”
OCCUPATIONAL EXPOSURE TO WILDFIRE SMOKE AMONG AGRICULTURAL WORKERS
“You have the foundation of health effects in people,” said Heather Riden, manager of the Western Center for Agricultural Health and Safety at the University of California (UC), Davis. “Now I want to ground it in the day-to-day reality of workers.”
California produces two-thirds of the fruits and nuts grown in the United States and one-third of the vegetables. Most of the crops grown in California are labor intensive, requiring people to harvest crops by hand, as well as planting, irrigating, and weeding by hand. California has about 800,000 farmworkers (Martin et al., 2017). They are predominantly male and Spanish speaking, and 60 percent are unauthorized to work in the United States. Their annual average wage is under $20,000, which is relevant to housing, health care access, and other issues, said Riden.
Their health status is similar to that of the U.S. population as a whole, with high rates of obesity, diabetes, and pre-diabetes. They tend to live in crowded dwellings, experience a lack of health care access, and have concerns about the political climate and immigration. Agriculture is a hazardous industry where people face trips, falls, pesticide exposure, and heat illness. “This is the backdrop agricultural workers are experiencing when there is a fire event,” said Riden.
Riden’s study was designed to describe the perceived occupational health and safety impacts of extreme weather, including exposure to wildfire smoke, in the agricultural workplace, with the objective of developing safety awareness campaigns, best practices, and safety resources for the agricultural industry. She and her colleagues selected three geographic areas in California: the Central Valley, the Imperial Valley, and the Salinas Valley. A total of 9 focus groups were conducted with farmworkers in these 3 regions as well as 16 interviews with farmers. The focus groups were conducted in Spanish by a trained facilitator with 6 to 10 people in each group (Riden et al., 2020).
A farmworker who participated in a focus group noted, “We know that the fire season each year is stronger, or maybe sometimes less so. Maybe it’s not near here, but because the air travels it takes [air contaminants] everywhere.” However, wildfire smoke and air quality did not rank as high as heat illness as a health concern for farmworkers. Many also said that they would continue to work in unsafe conditions because, as one put it, “rent had to be paid” and “food has to be bought.” Riden said, “It is in that context that we need to be thinking about public policies and how to protect those people who have no choice but to work despite unsafe conditions.”
Farmworkers had varying knowledge of protective measures. Some were aware of respirators and how they could use masks to protect themselves. Others thought that the use of two bandanas over the mouth and nose would be sufficient. Barriers to using masks include supervisor indifference as well as heat. As one focus group member stated, “they [supervisors] just pointed at the masks and said, ‘Here are the masks, use them or don’t use them.’” At least masks were available, Riden observed: “The hope is that supervisors and employers can do more to give instruction on how to use them and why they are important.”
Not all workers wish to wear a mask. Anyone who has worn one for more than a few minutes knows that they are not comfortable, Riden pointed out. Farmworkers are laboring outside in the heat wearing a lot of clothing for many hours. That discomfort can create resistance to masks even if they are available.
Supervisors and employers play the largest role in the safety culture and in the farmworkers’ ability to implement safety precautions. “A supervisor or a crew leader who wants to make safety a priority can do that effectively, and the reverse is also true,” said Riden. Farmworkers see government as a resource and the potential for penalties as shaping how supervisors interact with workers. As one said, “The thing is that they [supervisors] take a lot of care for the crops, but they don’t take care of those who are harvesting them. But if there is no one to work the fields, what would happen then?” Added another: “And if one does not do it [work in the field during unsafe conditions], they fire us and then here comes another one.”
For their part, farmers were familiar with the precautions needed for heat, rain, and wind, but smoke was new for many of them. Said one: “We’ve never set up protocols for that [smoke], it’s not like rain that hits or doesn’t. You don’t see it [coming]. Sometimes you see it, but it’s more vague where you can measure it. We don’t have means for measuring air quality.” This is important in the context of the recently adopted emergency regulation in California for wildfire smoke, said Riden, because employers will need to be aware of air-quality conditions and be responsible for providing their workers with respirators as required.
Some employers put the responsibility on workers to protect themselves—“They know how to dress.” Others create policies to ensure that workers do not have to choose between their work and being safe. One farmer said, “We really put the crews first when we make decisions. If it’s uncomfortable for crews to do, we scrutinize whether we should be doing it. We make individual accommodations.”
At the time of the workshop, the California Occupational Safety and Health Standards Board was considering a petition for an emergency regulation on wildfire smoke exposure for outdoor workers. Employers would be required to provide respirators for workers to use on a voluntary basis when the Air Quality Index is 151 or greater. The request passed on July 18, 2019, and went into effect on July 29, 2019 (California Occupational Safety and Health Standards Board, 2019).
One finding from the focus groups with farmworkers and interviews with farm owners is the need for targeting outreach depending on the audience. Farmworkers need to know about their rights, said Riden, not only about wildfire smoke, but on other topics as well. “They need to know how to effectively use a respirator and not rely on their employer to give that instruction. Bandanas are not the same as an N95.”
Farmers need to know how to access air-quality information, she added. They also need to know best practices for protecting their workers, effective training for workers, and what their responsibilities are.
Occupational hazards from wildfire smoke affect not just farmworkers but construction workers, firefighters, utility workers, and many others, Riden observed, adding that “a policy does not work unless we acknowledge where people are and what information they need to be safe in the workplace. This includes the power dynamics that are at play in industries like agriculture.”
In response to a question from Winston Wong, Riden noted that California is dependent on the harvesting of produce when it is ripe and that farmworkers are a very vulnerable population. She also noted that during wildfires the general public is told to stay home, but “there is a double standard when we are then telling another population to keep working and protect yourself.” Given the power relationships in agricul-
ture, regulatory bodies will have a role in ensuring that all workers are safe, she said.
HEALTH EFFECTS FOR WILDLAND FIREFIGHTERS
Prior to the workshop, Kathleen Navarro, a forest planning specialist at the U.S. Forest Service, had been working on an interagency hot-shot crew focused on prescribed burns and wildfires.1 She described the kinds of exposures wildland firefighters face and the possible health effects of those exposures.
In 2018, at the height of fire season, more than 27,000 firefighters were deployed in the western United States to suppress wildfires. They work under arduous conditions, Navarro observed. A federal firefighter is generally limited to a 16-hour day. California firefighters generally do a 24-hour-on, 24-hour-off schedule. She explained that “if I am out on a fire, my typical day starts at 5 a.m. for a wake up, a 6 a.m. briefing, you are out on the line by 7 a.m., 8 a.m. at the latest, and then you are working until 7 or 8 p.m. You get back into camp. You eat dinner. You go to bed. Generally no showering.” Firefighters wear a hard hat and flame-resistant clothing. They carry a fire shelter, “which is essentially a sophisticated piece of aluminum foil that can protect during a burn-over or an entrapment.” They do not wear respiratory protection.
Firefighters are exposed to smoke both while they are working and while they are in fire camps, which are often located near fires. If they are on a hand crew, their job is to dig fire lines and put out fires with the hand tools that they have. Engine resources can carry up to 500 gallons of water and drive into areas that are accessible by roads. Aviation resources can drop water and fire retardant. Firefighters on the ground can then come in afterward to back up those resources.
To construct a fire line, firefighters come through with chainsaws and cut down all the vegetation, generally in a 10-foot-wide swath. Diggers then come in and dig down to the bare mineral soil. Once the fire line is in, firefighters hold that line (i.e., holding) to make sure the fire does not cross. They look into unburned areas to make sure no embers got there to start
___________________
1Prescribed fires or prescribed burns are fires that are intentionally ignited in accordance with applicable laws, policies, and regulations in order to support wildfire management actions.
a fire. This is one of the smokier tasks firefighters face, said Navarro. “On a prescribed burn this year, it was so bad I could not see in front of me.”
After a fire has come through, firefighters perform mop-ups where they put out any smoldering material that can be carried by the wind and reignite the fire. They might have an engine nearby to pump water through a hose. Otherwise they can carry a 45-pound backpack pump full of water and spray by hand or shovel cold dirt onto hot ash.
When firefighters conduct prescribed fires, they use a torch that burns a mixture of diesel and gasoline. Similarly, when they are performing a back burn, they are trying to burn any material between the fire line they have constructed and the oncoming main fire.
Navarro briefly reviewed previous studies of firefighters that have looked at exposure to different sizes of particulate matter and also carbon monoxide. Hejl et al. (2013) found an increase in inflammation markers, while Slaughter et al. (2004) and Gaughan et al. (2014) found decreases in lung function. In health assessments done before and after fire seasons, Liu et al. (1992) and Gaughan et al. (2008) found such effects as heightened airway responses, reduced lung function, increased inflammation, and increases in respiratory symptom scores. In a survey of firefighters with years of experience, Semmens et al. (2016) gathered self-reports of high blood pressure, heart arrythmia, and knee surgeries, the last of which Navarro found surprising “until I put a 30-pound pack on and went down a really steep hill.”
As part of her dissertation work, Navarro examined polycyclic aromatic hydrocarbon exposures for firefighters, including benzo(a)pyrene, a human carcinogen, and naphthalene, which is a suspected human carcinogen. Firefighters who were holding fire lines were most exposed on wildfires, and firefighters performing firing and holding were highly exposed on prescribed fires.2 Using exposure–response relationships and field measurements of PM4 and heart rates, Navarro et al. (2019) were able to estimate the lifetime risk of lung cancer and cardiovascular disease from exposure to particulate matter from smoke. They found that, for a 5-year career working shorter seasons, a firefighter has an excess risk of 8 percent for lung cancer and 16 percent for cardiovascular disease. For a 25-year career working longer seasons, the excess risk for lung cancer is 43 percent and the excess risk of cardiovascular disease is 30 percent. At the time of the workshop, the National Institute for Occupational Safety and Health was conducting a 3-year study focused on cardiovascular and respiratory health, asking such questions as whether firefighters are able to recover lung function between seasons.
___________________
2Firing is the process of intentionally setting fire to fuels between the main body of a fire and the fire control line. Holding is the process of monitoring and doing required fire suppression work so that the fire does not pass the fire control line.
Research on the health effects of firefighting faces several challenges, Navarro observed. Every day is different, so on some days exposures are high and on other days they are not. In fires that burn structures, firefighters are exposed not just to smoke, but to chemicals from burning buildings and infrastructure. Access to incidents and study subjects can be difficult, especially because firefighters tend to downplay the hazards. Often, the culture of firefighting is that, “This is what we have done. This is what we have always done. You need to suck it up.” For example, they tend not to wash their clothing—“it is a badge of honor to not take a shower for 14 days,” Navarro said—which results in dermal exposures.
Occupational exposure limits could be based on long-term risk, Navarro observed. For example, firefighters could be rotated in and out of heavy smoke areas, or they could be kept a certain distance from a fire. She also raised the issue of exposures to firefighters versus exposures to the public. “If we do not want to see smoke in our air and we are asking the firefighters to suppress that, how are we transferring that risk and what does that look like?”
This last point was reemphasized by David Eisenman, who raised the issue of prisoners working on fires. “We are talking about a vulnerable population that has probably little supervision about exposure to risk and little information.” Navarro said that she could not comment on equity issues involving prisoners but noted that prison firefighters “are exposed out on the line, just like any firefighter, and they are exposed in camp.”
Navarro also noted, in response to a question, that firefighters get little if any training on how to avoid smoke exposure. In the trainings that she conducts for firefighters, her focus is
making it simple and making it tangible and trying to get that message out that there are hazards in smoke and we need to start thinking about ways of reducing it. There is no easy answer, [which] is the hardest part of developing these trainings. There is not a magic respirator that anybody can put on. I do not want to wear a respirator when I am hiking at 9,000 feet carrying a 30-pound pack.
One approach, she said, is to get the topic into everyday conversation and then empower people to make good decisions.
As the moderator of this session of the workshop, Wayne Jonas, executive director of the Samueli Integrative Health Programs, said, leadership is crucial in changing the culture. “It is not just about individual risk. It is about the collective risk. You are putting your team at risk if you are risking your own ability to function or not function in those areas.” The military has training to demonstrate that, he added.
RESPONDING TO AND RECOVERING FROM WILDFIRE-CAUSED DRINKING-WATER SYSTEM CONTAMINATION
The changing climate and wildfire risk can trigger technological disasters, where a natural or humanmade fire hazard causes damage to infrastructure. Andrew Whelton, associate professor of civil engineering and environmental and ecological engineering at Purdue University, discussed a particular kind of technological disaster: damage to drinking-water systems. Wildfires affect both public water systems and private water systems, including private wells that provide water to 15 percent of the U.S. population. As he pointed out, drinking water is critical for community health, safety, and economic security. “If you do not have drinking water or a way to get water, it is going to be hard to have a sustainable community.”
In October 2017, the Tubbs Fire affected Sonoma and Napa Counties, where 5,656 structures burned; 2,500 parcels were affected in the city of Santa Rosa. Because of drinking-water system damage, Santa Rosa issued a boil water advisory. This is common when the possibility arises that bacteria could have been drawn into the water system through hydrants or broken pipes. About 1 month later and after the fire had been contained, the city received a drinking-water odor complaint. Chemical testing revealed VOC contamination of the drinking water. Benzene was at a level above both the California limit (1 part per billion) and the EPA limit (5 parts per billion), and other chemicals were also detected. “The water treatment plant was creating safe drinking water and providing it to the distribution system,” said Whelton. “But the chemical contamination originated from the distribution system pipes, meters, valves, and fittings.” In response, the city issued a “do not drink and do not boil” advisory, the latter because chemicals could volatilize if the water was heated by boiling or showering, and that would increase exposure.
The contamination was associated with only part of the area affected by the fire—about 350 parcels and just a few water mains, hydrants, and meters. In all, about 13 occupied homes and fewer than 20 people were affected in an area with 175,000 people on the public water system.
The response and recovery were overseen by the California State Water Resources Control Board and Region 9 of EPA. Initially, the idea was to remove and replace all of the affected systems, which would have cost
about $44 million. But by testing and replacing only the affected components, costs were reduced to about $8 million.
Repeated location sampling was necessary to find contamination, Whelton said. Water samples often needed to sit for more than 72 hours to allow chemicals to desorb from contaminated water. Chemicals in addition to benzene exceeded acute and chronic exposure limits, and estimates of benzene contamination could differ by as much as 77 percent from duplicate water samples for a single location. The city decided that if benzene was found at 0.5 parts per billion or more, an asset had to be replaced. This level is lower than the 1 part per billion limit that California sets for its drinking-water standards, but 0.5 was used as a decision limit because of a concern that infrastructure was actively leaching chemicals. Some parts of the system had very high levels of contamination, including one measurement in a service line of 40,000 parts per billion of benzene. All contaminated hydrants, water mains, air release valves, blow offs, and service lines were replaced, and long-term VOC monitoring was required.
The 2018 Camp Fire was on a different scale than the Tubbs Fire, with many more structures and water systems affected. Most of the town of Paradise was destroyed, along with parts of surrounding communities. The fire burned about 14,000 structures and caused at least 85 fatalities. Thirteen different water systems were affected by the fire, and more than 40,000 people received a boil water advisory. In addition, more than 2,400 private wells were affected by the Camp Fire, which also generated warnings about contaminated water.
Because of the heat of the fire, some plastic components in the water systems melted and decomposed before cooling. Some water meters did not survive, while others seemed to have no visual damage but were still contaminated. One possible primary source of contamination was the thermal decomposition of plastics, which is different than melting, Whelton said. Another possible source was contaminated air and materials being drawn into depressurized systems, after which chemicals partitioned in the water. Both plastic and forest biomass combustion can generate VOCs, and the source of the contamination still requires further research. Contaminated water from building plumbing can compromise the broader water system. In addition, chemicals entering a system can attach to the surface of an infrastructure material, such as a metal or plastic pipe, after which the chemicals would enter the water slowly over time. Plastics, however, are particularly susceptible to internally soaking up VOCs, requiring a much longer time than metals for decontamination. Whelton noted that it remains unclear what the source(s) of the contamination were, including the water infrastructure or contaminants being drawn into the system from elsewhere. “We do not know which of these is responsible or if it is a multitude of things that are causing the contamination,” Whelton said.
Benzene was a particular concern, though it was just one of many chemicals detected in water after the fire. The Paradise Irrigation District (PID) water system had more than 2,200 parts per billion of benzene in its water in January 2019, and the Del Oro Water Company had found benzene in two of its three systems. There are long-term exposure standards for benzene, Whelton noted, but acute exposures also can cause health problems. In April 2019 the California Office of Environmental Health Hazard Assessment showed that 26 to 1,000 parts per billion of benzene posed an acute risk to children. Some of those levels had been exceeded in the PID system as well as in the Del Oro Water Company systems.
How much exposure people get from boiling water and showering still remains unclear. “If you boil water with 40,000 parts per billion of benzene, what is that exposure, and is that exposure acceptable or not?” asked Whelton. Researchers need to look at what the potential exposures might be and what kinds of advisories are appropriate, he said.
More research is also needed on water distribution system decontamination, Whelton added. Numerical modeling done by EPA indicates that some assets would require 286 days of constant flushing at 2 gallons per minute for almost 1 year to be decontaminated. Work that Whelton’s team conducted previously has shown that plastic plumbing components require much longer than metal components to decontaminate. Some assets simply have to be removed because they are too costly to decontaminate.
Whelton and his colleagues at Purdue have helped the town of Paradise work out water testing plans for buildings, where they discovered methylene chloride above safe limits in the absence of benzene. The town also has been involved in discussions about what to do with the water that is chemically contaminated, due to regulatory requirements for the disposal of contaminated water. The greatest public health implications involve standing homes. “Some PID customers we know are not following the water use restrictions,” he said. “They are told not to take hot showers, but they are. They are told not to drink the water, but they are. We know this because they have called us and told us in the process of asking questions about their water safety.”
Seven months after the fire, contaminated water was still entering homes, which was a public health risk. Utilities are still trying to identify their contaminated assets, including service lines and hydrants. A concern, however, was that as they start fixing their systems, a loss of pressure in one part of their water system could draw water from contaminated areas into the clean side of the system, presenting a new health risk.
Many standing homes had received up to 6 months of contaminated water in their hot- and cold-water plumbing, which has left them with nonpotable water. The next step, said Whelton, is to determine what is necessary to make home plumbing safe again. He emphasized that differ-
ent plumbing designs and in-home treatment devices that people are using need to be factored into plumbing safety testing. Water system customers were paying for water testing results, but some of the results likely had little value, and commercial laboratories were misadvising them on how to collect water samples—such as telling them to flush the water from their plumbing for 10 minutes before taking a sample. This would purge water from their plumbing and instead they would then end up sampling water from the supply line or water main instead. Some irrigation systems were damaged, and some were contaminated. External water tank maintenance and microbial growth were emerging concerns.
Another issue is the economic capacity of the individuals who have been affected. If people have limited financial resources, they do not purchase bottled water or in-home treatment devices, even if the utility’s water testing data show that the water is contaminated. “These are the types of struggles that happen in affected communities. There really needs to be advocacy for these individuals.”
Insurance companies were also making decisions about in-home water treatment systems. People were being denied additional living expenses by insurance companies that were assuring them that in-home treatment makes water safe under any circumstance. But the devices being installed were tested for typical drinking water use, not for the use of heavily contaminated water, said Whelton.
Whelton and his colleagues identified six scientific challenges and opportunities associated with drinking water after wildfires:
- The sources and sinks of chemical contamination. Identifying where chemical contaminants come from would allow components of a water system to be altered so that contamination is less likely.
- Laboratory contamination, data reproducibility, and standard operating procedures. No standard operating procedures exist, for example, for how to take a water sample from a fire hydrant or building, even though such procedures would enable people to respond more quickly to a technological disaster.
- Evidence-based water use restrictions that protect public health. Understanding inhalation exposure, modeling of emissions, volatilization of chemicals, and other health-related factors would enable policies to be based on those results.
- Decision making for infrastructure testing, decontamination, and replacement. Past decisions have been made on the basis of the best judgment at the time, but these judgments were often based on little or no data.
- The environmental and human health impacts of disposing of chemically contaminated materials. For example, can people use
- Evidence-based private property chemical characterization and recovery steps. For example, what is the best way to test and decontaminate plumbing?
contaminated water on their vegetable gardens, or is it safe to walk past a hydrant that is misting?
In response to a question about how contaminated water is being treated or disposed, Whelton noted that some, such as water washed from hydrants, is being discharged to the ground. However, various organizations, including the PID and the Regional Water Quality Board, have been involved in testing water and making decisions about whether it can be discharged or first has to be treated. Similar decisions pertain to the contaminated infrastructure being removed from the area, such as burned and melted piping, some of which may have to be treated as hazardous waste.
Whelton also noted in response to a question that many lessons learned in the Tubbs Fire were not transmitted to the people involved in the Camp Fire response, despite the similarity of the large-scale contamination. “But we, as a nation, have to figure out how to respond to these incidents.” In particular, the transmission of knowledge across state agencies could enable government officials to start “several steps up the educational ladder instead of it having to be the first time for everybody,” he concluded.
TIME-SENSITIVE STUDIES OF WILDFIRE EFFECTS
In October 2017, fires broke out in the northern California counties of Napa, Lake, Sonoma, Mendocino, Solano, Nevada, Yuba, and Butte. More than 245,000 acres burned, close to 9,000 structures were destroyed, more than 100,000 people were evacuated, and 44 people died. Several people died in vehicles while trying to flee the area, and residents of Napa and Sonoma Counties were awakened in the middle of the night. The title of the documentary film shown at the workshop, Waking Up to Wildfires, has two meanings, said Irva Hertz-Picciotto, director of the UC Davis Environmental Health Sciences Center and a professor of public health sciences at the UC Davis School of Medicine. It reflects both the need to take wildfires seriously and the fact of waking up to life-threatening wildfires in the middle of the night.
The National Institute of Environmental Health Sciences of the National Institutes of Health has a mechanism for time-sensitive research, which Hertz-Picciotto and her colleagues used to do research on several
issues associated with the fires, including exposures, health impacts, and needs. Human health projects included an online survey, a study of a cohort of pregnant women and mothers and their children, and a door-to-door survey. Sample analyses were done of ash, air, and food. The combined projects had several goals:
- Describe the population’s experiences and needs
- Learn about exposures—smoke and contamination
- Address both physical and mental health consequences
- Establish cohorts to follow for long-term impacts on health
- Understand the role of community socioeconomic factors in predicting long-term health and recovery
- Collaborate and communicate with local organizations to enable improved future responses
Hertz-Picciotto directed her remarks largely to the online survey, which gathered the following information:
- Household—basic information, location, members of household
- When the fires broke out
- Evacuation details—respondent, other adults, and children in household
- Recovery period, including needs and concerns
- Handling debris from the fire
- Employment status
- Health status—respondent, other adults, and children in the household, before fires and since the fires broke out
- Demographic characteristics
- Contact information for follow-up studies
One issue Hertz-Picciotto and her colleagues wanted to pursue was the extent to which the underlying socioeconomic status of a community affects the long-term impacts. These wildfires were “equal opportunity” events, said Hertz-Picciotto, adding that “there were some very poor neighborhoods and also very wealthy neighborhoods that were hit very hard.” The result was a natural experiment in which different communities with equal exposures to fire impacts could be compared over time.
The survey sample was not representative, she cautioned, nor was it adjusted for having multiple people in the same households providing data. The survey was publicized through both social media and regular media. In the end, more than 2,000 households responded, representing more than 6,000 household members. About two-thirds were from Sonoma County; the mean age of the adults was 49 years, and the median age of the children
respondents was 9 years. Seventy-two percent of the respondents owned their own homes and 27 percent rented. Forty percent had been in the same house for 12 years or more. They were a highly educated group, with more than 60 percent having a bachelor’s, graduate, or professional degree as the highest degree completed.
Hertz-Picciotto provided a broad overview of the survey results, pending publication. Respondents learned about the fires in a variety of ways, including from a friend or family member not in the house, from a neighbor, from the news, by seeing smoke, or by seeing flames. A majority of the households had to evacuate, and many of these evacuees had to relocate to three or more locations in the first 6 weeks.
Respondents reported a wide variety of needs both immediately and 1 week after the fire, including transitional housing, clothing, safe drinking water, medicine, cell phone service, electricity, heat, hot water, sleep, breathing masks, and transportation. Among the health-related concerns or questions they would like to see addressed by local officials were air quality, water contamination, the safety of locally grown produce, and what people can do to protect themselves and their families from long-term, fire-related exposures.
They reported a large variety of respiratory symptoms, including asthma attacks or bronchitis, wheezing or whistling in the chest, and coughs. Those with preexisting asthma were more likely to report either having an asthma attack, bronchitis, or wheezing or whistling in the chest compared to those without preexisting asthma, “so that is a vulnerable population to be aware of.”
The surveys were filled out between 4 and approximately 12 months after the fires, and many people were still reporting respiratory symptoms. This raises the question, Hertz-Picciotto noted, of the distinction between acute and chronic conditions when people are exposed to smoke repeatedly. Other questions, she observed, include “What about the ash? What about pollutants still in the soil and in the air? How deep do we need to clean homes? Can we keep the carpets? How long can it take to see illness that might be caused by the burning of the chemicals in homes?”
In neighborhoods with a lower socioeconomic status, the incidence of respiratory conditions was higher than in neighborhoods of higher socioeconomic status. In addition, women reported more symptoms than men.
Other associations were being studied at the time of the workshop, including effects on mental health, the persistence of respiratory symptoms, dose–response relationships, and effects on pregnant women.
On the issue of exposures, Hertz-Picciotto talked about exposure approaches they have been taking in their epidemiologic study. Though they collect address information, it is not required. For people who do not want to provide this information, such as undocumented individuals, there is an option of identifying an intersection near where they live.
Hertz-Picciotto’s team is interested in the combination of satellite measurements, which have good spatial coverage but do not necessarily have data from all time frames, with data from ground monitors, for which the opposite is the case. These data then could be linked to the address data. In addition, the team is considering the differences between people who evacuated and those who did not. Some of the people they have studied were just one to three blocks away from an active fire. “We were wondering about the mental health of some of those people, or their physical ability to actually get out [of the fire-threatened buildings],” Hertz-Picciotto explained. Some of their results do depend on evacuation status, particularly with respect to mental health.
The research team has also been gathering ash and air samples. For example, Hertz-Picciotto described an effort to outfit an electric car with air monitors so that it could get data in places without air monitors, though firefighters sometimes refused to let the cars enter fire areas. From ash samples taken from homes that had been destroyed, analysis has revealed the presence of hundreds or even thousands of chemicals, many of which are unique to built environments. Toxic chemicals can result from the combustion of building materials and interior furnishings, including solvents, glues, formaldehyde, metals, and halogenated compounds.
For the pregnancy study, researchers have been collecting biological specimens, including blood, urine, and hair. The latter is especially interesting, said Hertz-Picciotto, because a single hair can record differences from before, during, and after a fire. “You’re getting cross-sectional data, depending on the half-life of the chemicals.”
She also considered some of the advice given to individuals to limit their exposures, pointing out that “some of these things may be easier than others.” For example, if a fire goes on for weeks, keeping children inside that whole time can be very difficult. Clean air spaces or upgraded filter systems for schools or homes may partly solve the problem for some communities.
Finally, Hertz-Picciotto made the case for connecting wildfires and climate. In considering the health effects of wildfires, people need to think about the global warming that is contributing to those fires. As recent reports from the World Health Organization (WHO, 2018) and The Rockefeller Foundation–Lancet Commission on Planetary Health (2015) emphasize, climate and health are not yet linked in the public mind. “That’s a big task for all of us, to make that known and widely accepted and part of the culture.”
THE EFFECTS OF WILDFIRE SMOKE ON RHESUS MACAQUES
For the past 10 years, Lisa Miller, professor in the Department of Anatomy, Physiology, and Cell Biology at the UC Davis School of Veterinary Medicine, has been involved in a study of the effects of naturally occurring wildfire smoke on a cohort of rhesus macaque monkeys that live outdoors at the California National Primate Research Center. In June 2008, a dry low-pressure system produced approximately 25,000 lightning strikes, which ignited more than 2,000 forest fires across northern California in Humboldt and Trinity counties. The fires brought a significant amount of smoke into the Sacramento Valley and specifically to Yolo County, where the primate center is located. Miller was sitting in her office looking out the window at what seemed to be fog when a question occurred to her: Would this type of acute exposure event have a health outcome in the colony?
Rhesus macaque monkeys are unique in that they are seasonal breeders. In the springtime, the colony has anywhere from 500 to 700 infant monkeys outdoors, and in 2008 these monkeys were exposed to smoke from the Humboldt/Trinity wildfire. Fortunately, the California Air Resources Board has a number of monitoring stations throughout the state of California, and one is located on the UC Davis campus about 2.5 miles from the California National Primate Research Center, so good data on exposure levels were available. Peaks in PM2.5 concentrations occurred on June 24 and July 10 at more than two times the NAAQS (see Figure 4-2). “Clearly, the animals that were born in the year 2008 were exposed to a significant amount of PM2.5,” said Miller.
The California National Primate Research Center has about 4,500 rhesus macaque monkeys on site at any given time, with about half of them living outdoors on a 24/7 basis. With support from the California Air Resources Board, Miller and her colleagues studied the animals (who had been exposed to smoke shortly after they were born) 3 years later, when they were adolescents. Animals born in 2009, who were exposed to relatively clean air, served as a control. The tests were noninvasive so that the same approaches could be extended to human populations. To test the animals’ immune systems, the researchers collected peripheral blood and challenged it in the laboratory with components of bacterial cell walls to mimic a bacterial infection. The animals also underwent pulmonary mechanics testing, including a methacholine challenge, which measures for the development of asthma.
Miller and her colleagues found that monkeys exposed to early-life wildfire smoke had immune systems that were suppressed in the ability to respond to a bacterial infection (Black et al., 2017). Also, the overall lung volume of animals that were exposed to wildfire smoke very early on in life was significantly reduced, and the animals exposed to wildfire smoke
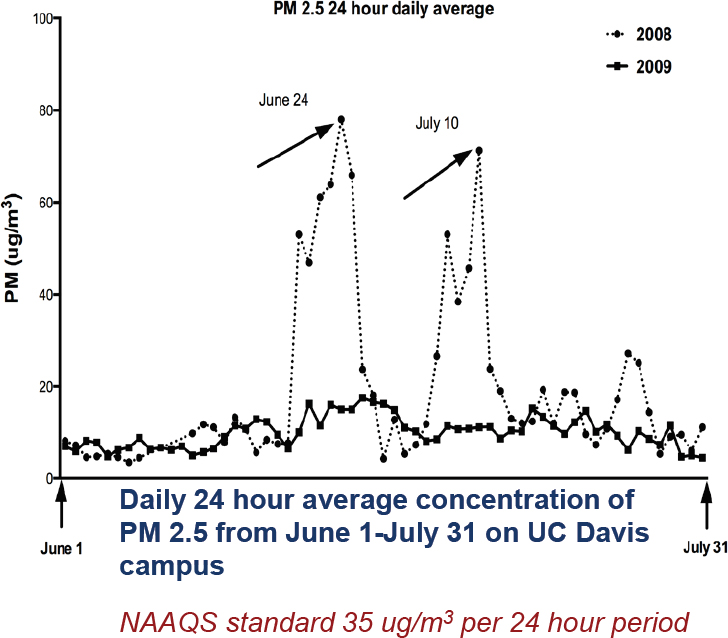
SOURCES: Presented by Lisa Miller. Black et al., 2017.
had reduced compliance in their lungs, which meant that their lungs were significantly stiffer than those of the control animals. The researchers did not find evidence of increased airway reactivity, which would signal the development of asthma, at 3 years of age.
When the animals were 8 years old, the females, which elicited the most significant response in lung function, still had dysregulated immune systems compared with the controls. They also had significantly reduced lung volume, which is consistent with what was observed in juveniles, and early-life wildfire smoke exposure was associated with increased airway radius and increased airway blood vessel density in adults.
“Something that takes place very early in life can have long-lasting and profound effects on the respiratory system as well as the immune system,” Miller concluded. Rhesus monkeys exposed to ambient wildfire smoke could serve as surrogates for health outcomes in susceptible populations with communities following a wildfire event, she suggested.
DISCUSSION
During the question-and-answer period, Jonas drew additional parallels with his experience in the military. For example, the military has a training program to prepare individuals to deliver first aid for anticipated trauma, and the educational component helps mitigate the fear of that trauma. These fear mitigation skills help people to not panic and to think more clearly about what they need to do. The training also includes simulations where people use these skills, preparing them for the real world.
Hertz-Picciotto pointed to major efforts to develop skills in people who are not mental health professionals for dealing with people who have mental health symptoms because of the traumas they have experienced in the counties affected by wildfires in California. For example, many of the people who evacuated were driving through flames on both sides of their cars and worrying that their tires were going to catch fire or melt.
There’s not a lot of roads going in and out of some of those towns in Napa and Sonoma, and they’re not very wide. Some people were on the road for hours hoping that they were not going to get trapped in their car. The degree of trauma was enormous.
To help people deal with emotional trauma, both public agencies and philanthropies have funded efforts such as a workshop for yoga teachers to help them work with people in their classes who are dealing with trauma.
On that point, Jonas remarked that some of the people who experience trauma are subsequently among the most resilient and the best at educating others. For example, the Department of Veterans Affairs uses peer-to-peer counselors, who themselves have experience with PTSD, to help others. Similarly, when Hurricane Katrina devastated New Orleans, people from the local community and from faith-based organizations came forward to help their neighbors and became a key part of the support for the community.
Commenting on another analogous circumstance, Colleen Ryan, a surgeon who represents the American Burn Association, pointed to the many opportunities to apply lessons from the burn community to wildfire preparations. For example, preparations to deal with wildfire smoke could also include information on bystander first aid. People still tend to treat burns by putting tomatoes or toothpaste on them rather than flushing them
for 20 minutes with cool water, which is the recommended treatment. She also mentioned the five stages of trauma preparedness: bystander care, pre-hospital care, hospital care, rehabilitation care, and recovery care. “There isn’t any reason why we can’t think about these things beforehand,” she said. For example, if a wildfire starts, a public service message would be tweeted out to both protect people and prepare them for dealing with trauma. Finally, she described the need to learn more about resiliency and people who are resilient. Resiliency “has been with humans forever,” she said. “There needs to be some way to study it.”
Hertz-Picciotto also pointed out, in response to a question, that not much is known about creating safe air spaces. “That’s an area ripe for research.” For example, how much time will people spend in clean air space? How often will they need to go outside or to school? Is the air indoors markedly better than the air outdoors? As another workshop participant pointed out, cooling centers and clean-air centers also raise issues of equity, because not everyone has access to them.
Reid noted that high-efficiency particulate air filters do decrease air pollution exposures indoors. Evacuations can exact a high physical and emotional toll, and sheltering in place could be a better option when a fire is not life threatening. However, the evidence does not indicate any threshold below which smoke exposure does not have a health impact. “Where to set that limit is more of a policy decision than a science decision.”
Finally, with regard to potential health effects, Michelle Bell, the Mary E. Pinchot Professor of Environmental Health from the Yale School of Forestry & Environmental Studies, pointed to the issues involved in assuming that the health impacts from wildfire smoke are the same as the impacts from, say, PM2.5 from traffic smoke. “That seems like a pretty bold assumption to me.” She also pointed out that acquiring the resources to deal with wildfire requires knowing the true economic and societal impacts of those fires. “To get the health impacts right, we need to have this research, so that’s why these research challenges are really important.”
























