5
Role of Community and the Food Sector
RETAILERS’ INITIATIVES FOR MEETING THE DIETARY NEEDS OF OLDER ADULTS
Government programs play a vital role in meeting the nutrition needs of older adults. For-profit and nonprofit organizations also are critically important players. In the first of several presentations on the role of the for-profit sector, Annette Maggi spoke about the retail landscape. Maggi is President of Annette Maggi & Associates, Inc., a strategic nutrition marketing and communications consulting firm that specializes in the interface between food manufacturers and retail grocers.
Maggi outlined four objectives for her talk: (1) explain why retail is ideal for health promotion, (2) provide a landscape scan, (3) describe how health professionals are working at the retail level, and (4) show how retail presents a “total store message.”
Retail is ideal for health promotion, Maggi contended, because it is uniquely positioned to easily integrate a health and wellness program with its large consumer base. Consumers visit food or food/drug stores an average of 1.9 times per week. In addition, 92 percent of consumers live within 5 miles of a pharmacy (the average is 1.86 miles) (Nazaruk, 2009). Retail has a significant number of touchpoints with the health conscious consumer. In fact, Maggi asserted, this number is much higher than doctor visits.
In addition, the retailer typically carries 40,000 items and national, regional, and private label brands. Because of their brand neutrality, they are perceived differently than manufacturers and perhaps trusted in a different
way, said Maggi. Retailers are in a position to provide messages across the entire store to help consumers evaluate the differences between products.
Maggi emphasized that retailers are committed to health and wellness for a variety of reasons, including competitive advantage, opportunities to establish profit centers within the store, corporate responsibility, employee engagement, and reduced employee health insurance premiums. Maggi noted that Wegmans has what they call the “amplifier effect”—they believe they can increase the health and wellness education and knowledge of all of their employees and that, in turn, translates to the shoppers in their store.
Approaches to Leverage Health and Wellness
Maggi explained that retailers have used a variety of methods to sell products to shoppers to leverage health and wellness: store design, in-store displays, such as endcaps,1 in-store signage, couponing, advertising of “better-for-you” products, promotions, publications, and owned brands. Retailers are driving health and wellness through their own brands, which are popular with retailers, Maggi explained, because they provide a much better profit margin than national brands.
Maggi then noted that for health and wellness strategies to be effective in the retail space, senior leadership commitment is essential, as is the commitment of multiple corporate functions, including merchandising, marketing, communications, public relations, and operations. Retailers also are aware that consumers today have easy access to a variety of sources of health information, so providing a credentialed health professional to meet the shopper’s unique needs is a way for retailers to distinguish themselves from other stores. For example, although many retail chains have pharmacies in every store, nutrition education is outside the pharmacist’s scope of practice. Still, the pharmacist does play a potentially important role in disease management, medication adherence, guidance on supplements, and vaccinations, and retailers see that these are all elements of a total store health and wellness program, even though the “wellness shopper” may never visit the pharmacy nor look to the pharmacist for health and wellness guidance.
Store Dietitians Are a Key Resource
Maggi went on to explain that because of their background and training, dietitians play a key role in retail healthy living programs. Perhaps 600 to 700 dietitians are directly employed by retailers and many others are employed as consultants. Dietitians are versed in nutrition, but also
___________________
1 An endcap is a display of products placed at the end of an aisle in a grocery store.
healthy cooking techniques, behavior change education, food composition and science, food safety, and a host of other food and health topics. Maggi suggested that they are ideally suited to drive consumer education, partner throughout the store on “better-for-you” promotions, and build corporate policies on topics such as genetically modified organisms. The roles of retail dietitians tend to fall into three buckets: a corporate dietitian is at the corporate level, the regional dietitian tends to be focused on stores in a key market, and in-store dietitians tend to have the most direct contact with the shopper as they provide one-on-one education through store tours and cooking classes.
Maggi explained further that the industry is split on the reporting structure of retail dietitians. Those reporting through pharmacy may spend more time on disease management, including medical nutrition therapy and one-on-one consults. Those reporting through operations, merchandising, marketing, or communications tend to focus more on wellness and a total store approach to healthy living. Dietitians report, recounted Maggi, that they spend about 50 percent of their time on health and wellness and 50 percent on disease management, with much of the work being related to disease conditions and targeted at older adults. Immunization clinics, store tours, and cooking classes, Maggi said, are other opportunities for retail dietitians to engage older consumers in dialogue around health and wellness.
A Total Message on Health, Wellness, and Food
Maggi then moved on to the topic of the total store message. This emerging area of retail focuses on how to bring health, wellness, and food together to provide a comprehensive message to consumers. Partnerships between nutrition and pharmacy are potentially valuable and some stores, for example, have begun to promote and market the work of the dietitian combined with the pharmacist. Another example of this partnership is cross-promotion signage to promote vegetables and fruits displayed in the pharmacy and adding healthy nutrition messages to the prescription. For example, if a shopper is picking up a cholesterol medication, a dietitian can put tips about healthy eating to control cholesterol into the package.
Another link is with in-store clinics. Some retailers have medical clinics in their retail stores. The primary usage of these clinics is cold, cough, flu, and similar acute conditions, that occur more frequently in the winter months. To broaden their healthy living messages and to increase their return on investment, weight management and smoking cessation programs as well as school and sport physicals are being included as additional services in the clinics.
In conclusion, Maggi noted that although retail health and wellness programs are not specifically designated as programs for older adults,
they have considerable appeal for these audiences. Partnering with retail on health and wellness could have great impact because most food buying decisions are made at the point of purchase. It may be essential for interested partners to create win-win opportunities and understand the retail environment.
INSIGHTS FROM THE RETAIL SECTOR: THE LITTLE CLINIC AT KROGER
Eileen Myers is Vice President of Affiliations and Patient Centered Strategies for The Little Clinic at The Kroger Co. Kroger was founded in 1883 and headquartered in Cincinnati, Ohio. It is the nation’s largest traditional grocery retailer and also has 1,965 pharmacies throughout 32 states.
Characteristics of The Little Clinic
The Little Clinic is the health clinic inside of Kroger. Kroger now has 181 clinics in 9 states. The clinics are accredited by The Joint Commission and affiliated with local health systems, including Ohio State University, University of Colorado, University of Cincinnati, Virginia Commonwealth University, Vanderbilt Affiliated Network, Via Christi Health, and Covenant Medical Group. Kroger meets with these health systems and looks at gaps in care to determine how the clinics can help fill those gaps, such as through providing after-hours and same-day service, providing post-discharge follow-up, and serving as a portal for chronic disease management. Myers noted that this capability is especially useful for patients who are unwilling or unable to see a provider because of time or resource constraints. About half of its affiliations have an interface with electronic medical records, so health information from a Little Clinic visit can be shared with a primary care physician.
The clinics are operated by nurse practitioners and physician assistants, who focus on acute, episodic care and screenings for people ages 18 months and older. The clinics have seen growth in the number of visits by adults ages 50 and older; about 25 percent of the patients seen at The Little Clinic are older than age 50.
Myers noted that The Little Clinics have a number of strengths. They provide convenient and cost-effective access to a health care provider who can identify, diagnose, and treat. They are connected to well-established health systems and participate in Population Health Management2 and in
___________________
2 Population Health Management is the aggregation of patient data across multiple health information technology resources, the analysis of that data into one actionable patient record, and the actions through which care providers can improve both clinical and financial
clinical trials. They provide an avenue to build motivation for health behaviors and links to additional health and wellness, including healthy food in the store, pharmacists, and in-store dietitians.
At the same time, Myers admitted that The Little Clinics do face some barriers. These include legal challenges that prohibit the clinics from offering some services, depending on the state. Another barrier is that some payers will not reimburse for The Little Clinic services. Also, Myers mentioned, some health care practitioners, especially pediatricians, have difficulties accepting this new form of health care delivery.
In closing, Myers reiterated that the goal of The Little Clinic is to provide personal, relevant health care solutions that are easy and affordable. Kroger is now doing that in a small way, but Myers expressed confidence that this opportunity will grow in the years ahead.
PERSPECTIVES FROM A “HOME SERVICE” RETAILER
Beth Burrough, a Partner of Healthcare Alliances and Chief Marketing Officer for PurFoods LLC, turned the workshop participants’ attention to the practical realities of getting healthy and nutritious food to the aging and vulnerable. They market their product under the brand name of Mom’s Meals NourishCare. The company was founded in 1999 and is headquartered in Des Moines, Iowa. The company delivers more than 14 million meals per year through partnerships with state and local government agencies and health providers.
Mom’s Meals expertise is in rapid, direct-to-customer nationwide delivery of fresh prepared meals designed around the Dietary Reference Intakes (DRIs) and also nutritionals tailored for specific health conditions. Its mission is to be the leading expert on, and provider of, nutrition solutions that preserve health, help combat chronic disease, support recuperation, and nourish independence for higher- quality living at home.
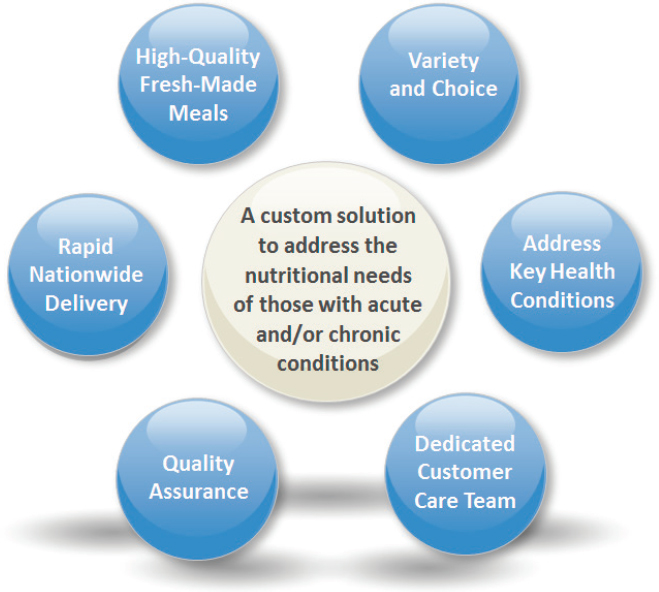
Burrough described how Mom’s Meals provides a unique solution created to address nutritional needs of older and disabled adults and patients (see Figure 5-1).
Burrough noted that providing a custom solution that is created and controlled by the customer is a critical point. The meals are designed to meet the needs of people with acute as well as chronic needs, including malnutrition and food insecurity. Burrough explained that the Mom’s Meals concept is an emerging health care area with considerable opportunity. The program appeals to Medicaid because it meets the goals of the Medicaid
___________________
outcomes. [NOTE: This definition is from http://www.wellcentive.com/what-is-population-health-management (accessed May 9, 2016).]
SOURCE: Presented by Beth Burrough on October 29, 2015 (Mom’s Meals).
Waiver program3 by responding to the nutrition needs of a large number of individuals who qualify for, or would otherwise be going into, nursing homes. The program also has advantages for Medicare because it improves care transitions and chronic care management. The majority of states with which Mom’s Meals has contracts provide one or two meals per day, but many customers could use all three. Many customers are on a fixed income and are having to make decisions about whether to use that money to feed themselves, pay their rent, or buy their medications.
___________________
3 Medicaid’s home- and community-based service (HCBS) waiver program allows states to provide an array of home and community services, including home-delivered meals, nutrition counseling, and nutrition risk reduction to older adults. For more information, visit https://www.cms.gov/Outreach-and-Education/American-Indian-Alaska-Native/AIAN/LTSS-Roadmap/Resources/State-Federal-Relationships/National-Overview-of-1915c-HCBSWaivers.html (accessed May 9, 2016).
Characteristics of Mom’s Meals
Each Mom’s Meals provides one-third of the DRIs for a male ages 70 and older. Calories vary according to state requirements, though the default is the Dietary Guidelines for Americans recommendations. Vitamin levels also vary by state. Burrough noted that the company manages 17 different nutritional profiles conforming to the requirements for 31 states. Another challenge is that the DRIs were designed for healthy adults, yet 90 percent of the Mom’s Meals population is believed to have one or more chronic conditions based on CMS data. To address this reality and also meet the needs of the patients they serve, Mom’s Meals has developed health condition menus that meet scientific and health association guidelines for nine clinical conditions (i.e., heart friendly, diabetic friendly, renal friendly, cancer, pureed, lower sodium, general wellness, gluten free, vegetarian). The meals also must meet rigorous food quality and food safety requirements while being comfort foods. Mom’s Meals continually surveys its customers and their preferences always come back to these foods.
The Meal Delivery Process
The logistics of preparing and delivering meals is complex, involving six hundred staff people to carry out the approval, enrollment, order taking, and home delivery. This process, stated Burroughs, is taken very seriously because failure to deliver may mean someone does not eat. Mom’s Meals uses a combination of its own delivery trucks, UPS, and FedEx. The company is able to get to any area, including rural areas, within 1 to 3 days.
Mom’s Meals conducted a satisfaction survey with 152 customers, and the results demonstrated the impact the service has. Among respondents, 91 percent felt that their quality of life had improved, more than 75 percent felt they were actually eating better, and more than 40 percent reported that the meals help them remain in their own homes. Respondents also said that the service allows them to be self-sufficient and independent, and that is a significant quality-of-life issue.
Burrough closed her talk with some reflections on the need for scientific research. She stated that a fair amount of research on malnutrition and its prevalence and impact has been conducted, but very little research has been done on effective community-based interventions to address the impact of long-term nutritional interventions on quality of life, prevention of long-term institutionalization, rate and length of hospitalization, and overall medical costs. Mom’s Meals is collaborating with the University of Michigan and Columbia Presbyterian on an NIH-funded trial in post-discharge acute decompensated congestive heart failure patients. Mom’s Meals also
partners with Kaiser and hopes to gain more insight on how the meals affect their members’ health and quality of life.
Services like Mom’s Meals also provide an opportunity, noted Burrough, to rethink nutrition as more than a support service (which is how it has been characterized in the Medicaid Waiver Program), but as a critical health intervention for preventing nursing home care, aiding in post-discharge recovery, supporting chronic care management, and providing additional support to the Supplemental Nutrition Assistance Program (SNAP) participants. It also can be an avenue for refining DRI meal guidelines or adding therapeutic guidelines that are aligned with evidence-based nutrition specifications for health conditions.
FOOD PRODUCT DEVELOPMENT FOR OLDER ADULTS
John Ruff, former head of research and development for International and North American businesses at Kraft Foods and a past president of the Institute of Food Technology, opened his talk by explaining that he would consider the question of what the food industry is doing to address the needs and preferences of older adults. With a few exceptions, few successful food products have been specifically designed for older adults. On the other hand, the nutrient supplement business is incredibly successful, although recent research, said Ruff, places some doubt on whether some supplements, for instance calcium, have benefits for older adults (Tai et al., 2015).
Ruff set the stage by describing how the age 50 and older population segment is large and diverse. The key to making products for older adults, concluded Ruff, is not to make products specifically for them. Stereotyping this group will lead to products sitting on the shelves. Older American consumers are trying to eat more healthfully and the adoption of healthy food behaviors increases with age. For example, Ruff observed that 35 percent of younger Baby Boomers (those ages 50 to 68) eat whole grains on most days compared to 44 percent of seniors, and 21 percent of young Boomers consume omega-3 foods or supplements on a daily basis compared to 30 percent of older adults. That shift, Ruff pointed out, will make a difference and provide opportunities for overt development of products for the older population.
Impacts of the Baby Boomer Generation
Ruff then described the impact of the Baby Boomer generation. In 2014, Baby Boomers accounted for 23.6 percent of the total U.S. population. According to Ruff, they are by far the single largest and most influential demographic group in history, and they have the spending power to disrupt the entire food market. Citing a recent trend report (FONA Inter-
national, 2014), Ruff noted that in 3 years, nearly half of the U.S. population will be age 50 or older and they will control 70 percent of disposable income in the country. Boomers’ median household incomes and median expenditures exceed the average. They outspend other generations by $400 billion per year on consumer goods and services. Boomers’ annual spending has been estimated by some to be responsible for half of all consumer expenditures in the United States, to the tune of $2.3 trillion, annually (FONA International, 2014). They want an active lifestyle so that they can keep up with grandchildren and will spend what they need to in order to extend their ability to do those things. As a result, it is expected that the global market for functional foods, or super foods, is expected to reach $130 billion in 2015. In addition, they are taking a variety of actions to stay healthy, including consuming more protein and fruits and vegetables.
Up to the age of about 65, older adults are trying to lose weight, and after that they focus on maintaining weight. They are socially active and involved in the community. They travel more, Ruff stated. They pay attention to packaging designs and they own smartphones, but do not use them to their full potential. They are concerned about privacy, and advertising on social media is viewed as an invasion of privacy.
Those ages 50 and older believe that foods and beverages are important to improve health and help them stay young. Interestingly, continued Ruff, this generation is more concerned about nutritional value than the source of the ingredients. They have a tendency to accept fortification more in beverages than in food. They also tend to shop on the perimeter of the stores. Like many people, they look for value for money. One major challenge they face is declines in the senses of taste and smell, as well as increasing difficulties with chewing and swallowing, which affects the palatability of foods and the ability to eat and may increase the risk of malnutrition.
Product Development to Meet the Needs of Older Adults
Product development is complex, and especially so when dealing with the older population. A few examples of the complexities are the need for different portion sizes due to lowered appetite, the need for higher nutrient density and flavor enhancement, and better texture, compensatory strategies (to cope with reduced motor skills) and appropriate packaging (single portion or smaller pack sizes with readable fonts and easy-to-open packages).
Ruff mentioned food labeling and regulatory challenges that limit food product development. He also noted that, in contrast to the United States, Japan has developed the Food for Special Health Uses (FoSHU) concept with the backing of the government. This concept has led to innovation in foods using functional ingredients, with many of the products focusing on
health issues of an aging population. Foods that meet specific requirements for FoSHU are marketed under the FoSHU label and have an exclusive market protection, unlike similar products in the United States.
He ended with two additional points. The first was that the opportunities for the food industry to focus on older adults is going to get significantly greater as Baby Boomers age. The second one was that the best way to improve the health of the elderly is to improve the nutrition of younger adults.
THE ROLE OF COMMUNITY PROGRAMS: P.E.E.R., INC.
Sally Allocca, Senior Pastor of East Lake United Methodist Church in Birmingham, Alabama, explained that she would describe how a church kitchen can partner with a nonprofit organization to form a viable food system to support low-income community residents. To set the stage, she showed a video4 about the church and the nonprofit that was produced by two students from the University of Alabama for one of their classes.
South East Lake has undergone a dramatic demographic shift in the past 15 years. About 10 percent of the population is older than 65, and the community is predominately African American. About 28 percent of the population lives alone and the median income is $23,000. About one-third of the population receives SNAP benefits.
The East Lake United Methodist Church was founded more than 125 years ago with a commitment to be “in the neighborhood for good.” The mission of the church is radical hospitality, welcoming all as Jesus would welcome them, and this mission is lived out in diverse ministries. One such ministry is the “Downstairs Diner,” a commercially equipped kitchen onsite. This Health Department–licensed and –approved facility provides healthy and hearty meals to community members.
Reaching the Community Through P.E.E.R., Inc.
P.E.E.R. stands for Promoting Empowerment Enrichment Resources and it was started in 2005 to more effectively reach the community. Its flagship program is the East Lake farmers’ market, from May to October. Allocca noted that one of the market’s most popular programs is the Senior Market Basket Program. P.E.E.R. purchases foods in bulk from the farmers and delivers 150 boxes each week to low-income older adults in two neighboring communities. This program has been described in a paper published in the Journal of Hunger & Environmental Nutrition (Dover et al., 2013).
Other P.E.E.R. programs extend the purchasing power of money that
___________________
4 This video can be viewed at https://vimeo.com/94114446 (accessed May 9, 2016).
people spend at the market for vegetables and fruits. These efforts piggyback on programs that are already established so there are no additional application or eligibility process.
P.E.E.R. also has a mobile market bus that takes food to older adults. It was the mobile library for a nonprofit in town and they gave it to P.E.E.R. This bus goes to senior centers, facilities, and schools. P.E.E.R. also has a chef apprentice program where it trains unemployed or underemployed individuals in the neighborhood in culinary skills. This program gives people skills so that they can prepare the fresh food they get at the farmers’ market and it provides great training and opportunities for jobs in the food system. It also generates good cooks who can work in the Downstairs Diner.
The Importance of Community Partners
Allocca went on to discuss the importance of having good community partners and stable sources of support. The church was already known as a resource center, so many community groups were already associated with it. The church relies on the health department, the food bank, and many other nonprofits and they conduct many of their programs in cooperation with them. Funding comes from donations as well as from private and public funders. The church is being used by other groups for their own programs. For example, the University of Alabama acute care for elders unit partnered with the church to develop a home-delivered meals program to people who had just been released from the hospital or rehab to see if improved nutrition would reduce the risk of readmission. It worked well for both groups because the church did not have to do any of the research or program development and the university was able to use the church’s existing contacts with local farmers to obtain the food. Allocca encouraged researchers among the workshop participants to follow this example and look for local institutions to help them with their programs. East Lake also is preparing meals for other churches in the area, which are using them for their own older adult programs. This arrangement helps East Lake through the purchases of the meals, and helps the other churches by providing healthy meals for their older adults.
Allocca concluded by saying that the church works hard to raise money for its programs through as many avenues as possible, including fundraisers, selling value-added products made from fruits and vegetables purchased from farmers, and grant writing. It also depends heavily on its leadership and staff, and relies on the community to let them know that the church is meeting the needs that they have. The church works closely with area colleges, which supply volunteers and interns, and depends on its board to help with marketing and fundraising. It takes everyone working together to get the job done.
THE ROLE OF COMMUNITY PROGRAMS: CITY HARVEST
Leslie Gordon is the Senior Director of Program Strategy and Operations for City Harvest. City Harvest was founded in 1982 and it has been in the marketplace in New York City for more than 30 years. For 6 years, City Harvest has received a four-star rating from Charity Navigator, America’s largest independent charity evaluator. The organization has a staff of 160 people and more than 20,000 individuals volunteer throughout the year.
City Harvest is the world’s first, and New York City’s only, food rescue organization. It is dedicated to feeding New York’s hungry by collecting excess food that would otherwise go to waste and distributing it to those in need. The food comes from food manufacturers, wholesalers, corporate cafeterias, farms, and other sources. City Harvest, a member of Feeding America®, delivered its 500 millionth pound of food in 2014. In its first year, it delivered slightly more than 1 million pounds of food. Its 45,000 square foot warehouse facility opened in 2011 and it has given City Harvest the capability to move more food than ever before. It is on pace to deliver to hungry New Yorkers nearly 60 million pounds of good nutritious food in 2015. Even City Harvest’s food waste does not go to waste, as it has it worked with an organization called Build it Green. This organization gets any waste from City Harvest and produces compost from it that is used in city community gardens. City Harvest’s fleet of 22 refrigerated trucks, including two tractor-trailers, travel about 275,000 miles per year crisscrossing New York City, the equivalent of about eight times around the equator. City Harvest does all this for free, being the beneficiary of a highly diversified funding stream, with individuals as the largest base of donors.
Hunger in New York City
Hunger remains a serious problem in New York City and the problem has become increasingly complicated in recent years. About 1.4 million New Yorkers are food insecure and face hunger. Last year, the soup kitchens and pantries that City Harvest serves helped provide food to many of the 2.5 million city residents ages 50 and older. About 1.4 million New Yorkers are currently ages 60 and older; by 2030, that number will rise to about 1.8 million, making older adults roughly 20 percent of the New York City population. One out of every 10 older immigrants in the United States lives in New York City. Immigrants make up about 46 percent of the city’s older adult population (Gonzalez-Rivera, 2013). Older adult immigrants have lower incomes than their native counterparts, and typically much less in retirement savings. Gordon illustrated with a map of New York showing the convergence of hunger and diet-related disease in low-income neighborhoods (see Figure 5-2).
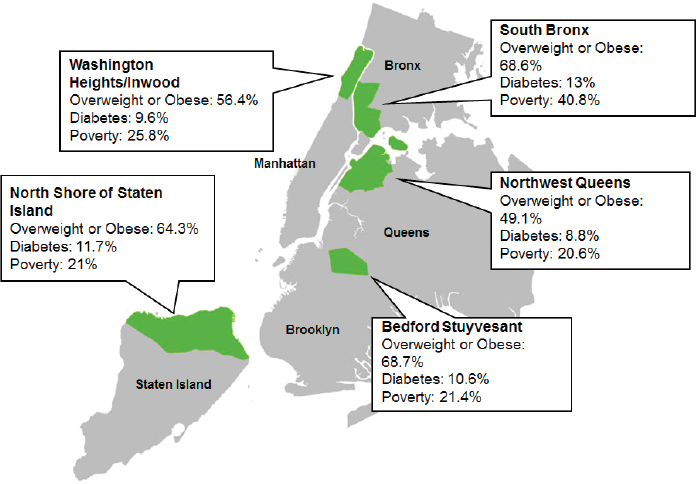
SOURCE: Presented by Leslie Gordon on October 29, 2015.
Across the country, Gordon stated, it is generally known that emergency food, originally intended to be used only in times of emergencies, is now needed on a regular basis. Older adults in New York, as in other places, struggle with hardships, such as low fixed income. They also must contend with extremely high housing costs. Higher rates of serious health conditions and low participation in SNAP contribute to long-term reliance on emergency foods. One in five older adults in New York lives below the federal poverty line. A similar number receive food from soup kitchens and food pantries, of which there are about 1,200 total across the five New York boroughs.
Communities where poverty is high also have high disease rates, noted Gordon. In addition, New York City Department of Health findings suggest that affordable healthy foods are hard to find, and farmers’ markets, supermarkets, and sources of fresh healthy foods are typically scarce. Sources of healthy food are vastly outnumbered by fast food restaurants and poorly stocked corner stores. New York has an abundance of heavily processed, cheap, convenient food that is highly caloric and low in nutritional value, stated Gordon, who added that this is the new normal in New York City.
SOURCE: Presented by Leslie Gordon on October 29, 2015 (City Harvest).
The Healthy Neighborhoods Program
This reality, stated Gordon, has required City Harvest to evolve how it conducts its program. Its new Healthy Neighborhoods Program has a vision in which healthy food is available, affordable, and in high demand. The program has several key goals, including relieving food insecurity, improving access to healthy and affordable food, increasing awareness of healthy habits and inspiring positive changes to dietary behaviors, and strengthening community capacity.
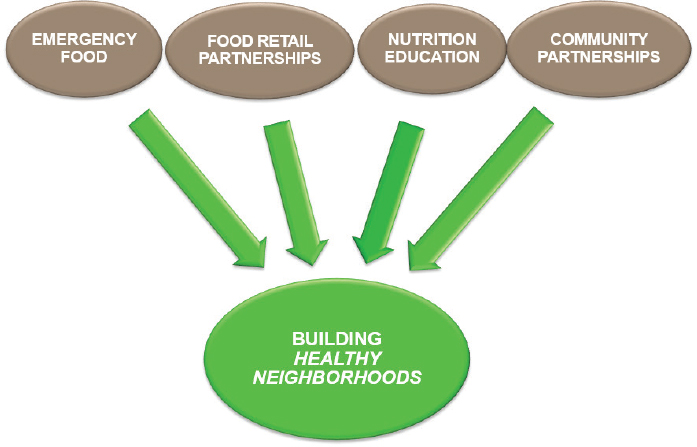
The program is built as an expansion of the work City Harvest started in the early 1980s: rescuing and delivering food. The program operates in low-income communities that have high rates of diet-related disease and challenges in finding healthy affordable food outlets. The program has four main elements that work together (see Figure 5-3):
- The program serves very low-income, low resource communities. The first step therefore is to ensure that the program brings emergency food into the neighborhood, focusing on fresh produce. This is done through City Harvest’s Mobile Markets and deliveries. City Harvest delivers food free of charge to soup kitchens and food pantries throughout New York City, including 74 of them in the
-
program’s Healthy Neighborhoods. City Harvest also has mobile markets, which are a free, fresh air, open distribution farmers’ markets that are done in conjunction with the New York City Housing Authority. These mobile markets are done 18 times per month and each event lasts about 3 hours. City Harvest brings up to 20,000 pounds of fresh produce in different varieties. The produce is distributed primarily to older adults. The markets provide an opportunity to talk with people about how to eat well, so the events also have cooking demonstrations and an “ask the doctor” table. City Harvest partners with hospitals that are often present at the mobile market. The markets provide a casual, comfortable way for health professionals to have conversation about disease management, asthma, diabetes, heart disease, and similar topics.
- City Harvest develops partnerships with food retailers because people do not need free food all of the time. When they are able, they want to purchase healthy food for themselves and their family, but they need a place to buy it. City Harvest is partnering with smaller independent supermarkets, corner stores, and bodegas to increase the variety of fresh produce they carry. It launched a program in 2012 to work with 64 retailers in the area by the end of 2017 to ensure their produce offerings are fresh and affordable and that their stores are in places where residents could and would like to spend their food budget. City Harvest works through local supermarkets to train store managers on how to successfully manage a produce section to increase sales of quality, affordable produce. City Harvest also works with area corner stores that are situated in areas that allow them to reach residents with fresh produce.
- City Harvest connects nutrition education with its emergency food and at food retail sites, including its mobile market, supermarkets, and corner stores. City Harvest believes that integrating nutrition education right where people are makes a big difference. Since 2000, City Harvest has been engaging residents in low-income communities—older adults included—in nutrition education programs that increase individual appreciation for and consumption of healthy, low-cost foods. Through hands-on cooking and nutrition courses, grocery store tours, and cooking demonstrations, community residents learn to shop for and prepare healthy, delicious dishes for themselves and their families while staying within their budget. City Harvest reaches older adults at senior centers, churches, and community centers. Its Well Seasoned course, developed by an in-house registered dietitian, addresses the specific needs of older adults. Over 8 weeks the course takes them through
-
food safety, budgeting, physical activity, nutrition, how to purchase healthy food on a limited budget, and reading food labels.
- City Harvest ties its work into the community. The success of the Healthy Neighborhoods Initiative depends on people and organizations that reside in communities where it works. Before entering a neighborhood with programming, City Harvest conducts a Community Food Assessment that helps it understand what a community wants, create a vision for how to go about doing it, and identify some barriers to success. It convenes Community Action Networks to provide a space for community organizations and residents to drive change in their neighborhoods. City Harvest plays a convening role.
Evaluation also is an important foundation for the program. City Harvest wants to know whether its programs are working, both at the individual and program level. At the individual level, it wants to know: Are people changing eating behaviors after participating in the nutrition programs? Are people shopping differently because of the program’s work in supermarkets? At the initiative level, it wants to know: Do residents feel they have improved access to healthy food in their neighborhoods? Do all programs result in people eating more produce?
Lessons Learned from the Healthy Neighborhoods Program
Gordon summarized some of the key lessons learned in the Healthy Neighborhoods program:
- Partnership-based programming requires time and patience.
- Each neighborhood is unique and dynamic.
- Community engagement is critical.
- Programming and messaging must be culturally sensitive.
- Anchor partners are key.
- Cross-sector collaborations are fruitful.
- A consistent presence builds credibility.
City Harvest is thinking about opportunities for additional programming in the future, including a potential retail program, pilot programs around using SNAP dollars to incentivize purchases for nutritious foods, ways to reach out to older adults with nutrition information and disease management information, and ways to use text messages to educate consumers. City Harvest also is thinking about how to engage consumers as change agents on the policy side and opportunities to change the built
environment in ways that can encourage healthy lifestyles and increased levels of fitness.
COMMUNITY PROGRAMS FOR CHRONIC DISEASE AND SENIORS
The final speaker for Session 5 was Hilary Seligman, the Senior Medical Advisor and Lead Scientist at Feeding America®. Seligman also is Associate Professor of Medicine and of Epidemiology and Biostatistics at the University of California, San Francisco.
To help workshop participants understand the connections between food insecurity and chronic disease and why these community programs are so important, Seligman reminded them that 5.4 million seniors are food insecure and there is a very important difference between the concepts of hunger and the concepts of food insecurity (Ziliak and Gundersen, 2014). The official definition of hunger is that it is a physical sensation that everyone experiences no matter their financial access to food. In contrast, food insecurity is officially defined as an economic and social condition of limited or uncertain access to food. Seligman explained that she considers the differences between being hungry and being food insecure important because people who are food insecure engage in a never-ending sequence of coping strategies in order to avoid the physical sensation of hunger. These strategies occur in the context of preventing and managing chronic disease.
Food Insecurity and Coping Strategies
Coping strategies that food insecure adults use include shifting food choices toward low-cost foods. This tends to be fewer fruits and vegetables and more fats and carbohydrates because fruits and vegetables are more expensive calorie for calorie than are carbohydrates and fats. Seligman noted that food insecure adults also eat highly filling foods in the hope that they will be full for the rest of the day if they do not have access to a second or a third meal of the day. Other strategies include concentrating on a small variety of foods that are either comfort foods or that people are very confident will keep them full. A big effort to avoid any food waste and binging when adequate food is available to keep them healthier during anticipated times of food inadequacy of the future also occurs. Although people use many other coping strategies as well, Seligman said that she highlighted these because they are highly relevant to increased risk of obesity and other chronic diseases.
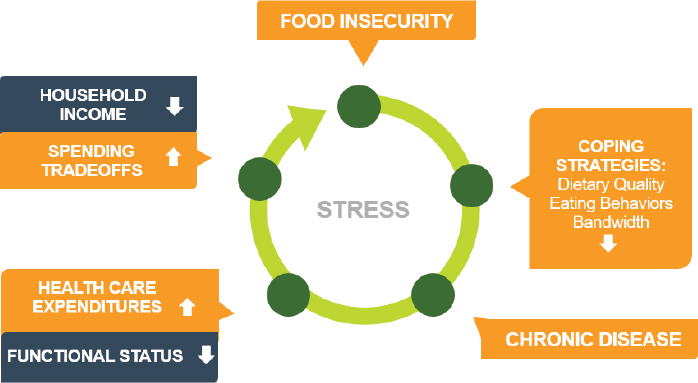
Seligman then elaborated, stating that these strategies start a cycle that is challenging for the food insecure adult to deal with. She provided a conceptual model to illustrate this cycle (see Figure 5-4).
Using this framework, Seligman explained that food insecure older
adults adopt a number of coping strategies that change the way they eat. These changes are accompanied by extreme stress that individuals live with when they do not have adequate money to afford food. The adoption of these coping strategies places individuals at higher risk of chronic disease. When chronic disease burden increases, health care expenditures go up and, particularly for older adults, functional status goes down. For younger older adults, employability also may decrease. As household income decreases, pressure on the household budget increases and spending trade-offs occur, leading to food insecurity. Seligman emphasized that because of the high costs associated with health care in the United States, once individuals enter this cycle of food insecurity and chronic disease, it is very challenging to get out of it. Stress and competing demands make it difficult to both manage food insecurity and a chronic disease. To illustrate, Seligman posed the example of an older adult with diabetes who has to make the choice of paying for test strips or having another meal to eat. She noted that for many food insecure people, the focus on finding the next meal crowds out other things. People have cognitive bandwidth for only a certain number of things, no matter what their age is. She showed several quotes from a study by Wolfe and colleagues (2003) that illustrate their experiences with food insecurity (see Box 5-1).
Because food insecure older adults are not always able to obtain the nutrient-rich food they need to enable their medications to work effectively
SOURCE: Presented by Hilary Seligman on October 29, 2015 (University of California, San Francisco).
and help keep themselves healthy, they face significant health challenges. Compared to their food-secure peers, food-insecure older adults are 60 percent more likely to experience depression, 53 percent more likely to report a heart attack, 52 percent more likely to report asthma, and 40 percent more likely to report congestive heart failure (Feeding America and NFESH, 2014). They also are more likely to have diabetes and a host of other diseases.
Key Intervention Points
Going back to the conceptual framework, Seligman pointed out two key intervention points—the point at which people experience food insecurity and the point at which they have developed chronic disease. To the extent that food insecurity can be resolved, said Seligman, clients and patients and older adults in our community can avoid the need for coping strategies that challenge the prevention and management of chronic disease. The goal, Seligman said, is to move interventions upstream, to the earliest point possible that is, moving interventions into the community. Food insecurity can be a very socially isolating experience, so community interventions that can
reduce food insecurity also have the bonus of reducing social isolation. The second is that food insecurity among older adults declines as people age.
Seligman then noted that older adults have a continuum of needs based on their mobility and ability to prepare meals, and this continuum influences the approach taken by Feeding America®. Different interventions are required to reach each of these groups. The three broad categories include older adults who are not homebound and can cook or access meals. Food pantries and meal sites are good interventions for this group. Because people are now using food pantries as a regular source of food not just for emergency food support, these sites provide an opportunity for other types of interventions, such as chronic disease management. Feeding America® currently has a project that provides diabetes self-management support in the food pantry. A person who comes to the food pantry every month can have his or her hemoglobin A-1c checked. The pantry can then not only make sure he gets the healthy food he needs but may even be able to connect him to appropriate disease management care.
The second group is older adults who are homebound and can cook. Community-based programs, such as home-delivered groceries, are interventions that work well for this group. The third group is older adults who are homebound and cannot cook. Home-delivered meals are a valuable approach for this group.
Seligman explained that Feeding America®’s primary focus is on increasing access to food for older adults who are not homebound. It has chosen to primarily focus its strategy on this segment because of the alignment of serving this population with the core competencies of its nationwide network of 60,000 food pantries and meal programs. To meet the needs of other older adults across the spectrum, Feeding America® and its network take a supportive or a partnership role with other organizations. These two premises are the foundation on which Feeding America®’s senior hunger strategy is grounded.
QUESTION AND ANSWER SESSION
Following the Session 5 presentations the floor was opened for questions and general discussion. Presenters and workshop participants commented on a range of themes emerging from the presentations. These ideas included the growing awareness of food waste and how partnerships and programs can be formed to make more productive use of that food. Another theme was the need to intervene earlier to identify food insecurity. Determining food insecurity when a person has developed health conditions may be too late. A third idea was the power of community and that bringing their strengths to partnerships may be a key factor in their success. Some communities have strong efforts to help older adults, but in other commu-
nities, that help does not exist, and time and energy is needed to support those communities. Another theme was the importance of complete and wholesome nutrition for older adults and how it can be a challenge to get that wholesome food to many older adults and to provide the information they need for eating healthy and managing or preventing disease.
A participant asked each of the presenters about their thoughts about health and wellness in their area and, if there is a partnership that would help with that, what might that be? Maggi stated that it would be trans-formative in the supermarket to make it easier for people to buy, assemble, and obtain healthy food. Myers stated that a beneficial partnership in her mind would be efforts by store clinics to hire more dietitians in order to make healthy choices the easy choices. Burrough stated that it would be how nutrition will come into the medical equation at either care transitions or chronic care management. She feels that vulnerable older adults who are going home from the hospital are the next big priority group. They are not mobile and they do not have consistent caregiving. The Centers for Medicare & Medicaid Services (CMS), groups like AARP, and health plans will all need to be involved in addressing the needs of this group, Burrough suggested. Medical institutions and health plans also are becoming more involved in health and wellness initiatives.
Some presenters and workshop participants also noted the potential in emerging partnerships between food banks and food pantries and the health care system. The system of food pantries in the United States is extraordinary in scope. They are located in the neighborhoods of highest need. This creates an opportunity to reach people in their communities in a place that they are, in many cases, very comfortable going. They know the volunteers. Many pantries are open at a time that is worked into their schedule. Chronic disease management is very challenging from a health care perspective because it requires interaction frequently. Some presenters observed that it is hard to go to a doctor in an academic center once a month, and pay for parking or walk-in a full block from the bus stop. The food pantries are often right there and people are primed when they walk in to talk about health because food is understood so much in the context of health. Churches also can play a vital role in these partnerships because they are an established and trust part of the community.
A final comment from Leslie Gordon elaborated on the partnership idea. She noted that City Harvest is laying out the foundation for its healthy neighborhood programming over the next few years. One of the things it is acknowledging is that City Harvest is good at some things, but that others can provide necessary resources to address the needs of the whole person not just their food needs. One thing they will be thinking about, for example, is how to connect mental health providers and clinicians with the work they do and the emergency food network of food pantries and soup
kitchens. Currently, a smattering of the 1,200 emergency food programs in New York City distribute food and also address the care of the whole person, including conducting some mental health screening but, Gordon observed, it is not nearly enough.
REFERENCES
Dover, S. E., D. R. Buys, S. Allocca, and J. L. Locher. 2013. Farmers’ market produce delivery program for mitigating nutritional risk in older adults. Journal of Hunger & Environmental Nutrition 8(1):1-10.
Feeding America and NFESH (National Foundation to End Senior Hunger). 2014. Spotlight on senior health: Adverse health outcomes of food insecure older Americans. Chicago: Feeding America. http://www.feedingamerica.org/hunger-in-america/our-research/seniorhunger-research/or-spotlight-on-senior-health-executive-summary.pdf (accessed February 12, 2016).
FONA International. 2014. Baby Boomers: A boom to your business. Geneva, IL: FONA International.
Gonzalez-Rivera, C. 2013. The new face of New York’s seniors. New York: Center for an Urban Future.
Nazaruk, D. 2009. Retailing’s critical role in revolutionizing health care and revitalizing the economy: A blueprint for improving consumer health and wellness, transforming the health care industry, and energizing the U.S. economy through retail. Progressive Grocer. http://www.progressivegrocer.com/research-data/market-trends/role-retail-revolutionizing-health-care (accessed March 25, 2016).
Tai, V., W. Leung, A. Grey, I. R. Reid, and M. J. Bolland. 2015. Calcium intake and bone mineral density: Systematic review and meta-analysis. BMJ 351:h4183.
Wolfe, W. S., E. A. Frongillo, and P. Valois. 2003. Understanding the experience of food insecurity by elders suggests ways to improve its measurement. Journal of Nutrition 133(9):2762-2769.
Ziliak, J. P., and C. Gundersen. 2014. The state of senior hunger in America 2012: An annual report. Alexandria, VA: National Foundation to End Senior Hunger. http://www.nfesh.org/wp-content/uploads/2014/05/State-of-Senior-Hunger-in-America-2012.pdf (accessed February 12, 2016).






















