7
Potential Health Concerns
While the first day’s presentations and discussions focused on the physical science and engineering aspects of indoor PM, the second day’s presentations turned to what William Nazaroff called the “So what?” and “What now?” topics—the associated health risks of exposure to indoor PM and risk communication. In the first of the day’s two sessions, Ryan Allen of Simon Fraser University discussed the effect of indoor PM on cardiovascular health, David Rich from the University of Rochester Medical Center presented emerging evidence linking ambient PM and adverse birth outcomes, and Marc Weisskopf of the Harvard T.H. Chan School of Public Health addressed the role that PM may play in neurological and psychiatric disorders. An open discussion moderated by Howard Kipen of Rutgers University followed the three presentations.
INDOOR PM AND CARDIOVASCULAR HEALTH1
Ryan Allen began his presentation by noting that he was not going to cover household air pollution from solid fuel combustion, which, he indicated, is “arguably the most important environmental risk factor globally” but isn’t generally an issue in high-income countries. After reiterating that a significant percentage of indoor PM originates outdoors (Allen et al., 2012), he stated that, in his view, the line between indoor and outdoor PM
___________________
1 This section is based on the presentation by Ryan Allen, an associate professor on the faculty of health sciences at Simon Fraser University, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
is not as distinct as some might think. He said that while much of the early research on PM and health focused on respiratory health, there have been a growing number of studies over the past 15 years on the cardiovascular effects of PM exposure (Bai et al., 2007; Brook et al., 2010; Crouse et al., 2012; Koulova and Frishman, 2014; Kunzli and Tager, 2005; Simkhovich et al., 2008; Sun et al., 2010). An important conclusion from these studies, Allen said, is that exposure to PM has a causal effect on cardiovascular health, not just a statistical association. In 2010, he noted, the American Heart Association issued a statement declaring, “It is the opinion of the writing group that the overall evidence is consistent with a causal relationship between PM2.5 exposure and cardiovascular morbidity and mortality” (Brook et al., 2010, p. 2365). He noted that the evidence backing this statement came almost entirely from studies using outdoor measurements and models.
The accumulated evidence also supports the finding that adverse cardiovascular effects occur at the lowest levels that individuals encounter (Crouse et al., 2012), said Allen, noting that “The evidence seems to suggest the absence of a threshold or a safe exposure level.” In fact, he added, the data seem to suggest that the relationship between PM exposure and cardiovascular health outcomes is linear or even supralinear, where the dose–response curve is steepest at the low end of the exposure distribution. If this finding holds, the implication would be that there would be a health benefit from further reductions in PM exposures.
Taken together, Allen said, these data show that exposure to ambient PM is an important public health risk factor (see Figure 7-1) and that the public health impacts from PM are driven largely by its effects on cardiovascular and circulatory diseases. “We still tend to think of PM as a respiratory pollutant or toxicant, but in terms of its public health impacts it is the cardiovascular and circulatory effects of PM that are driving the public health burden,” he said.
Research suggests that there are three interrelated mechanisms linking PM exposure with cardiovascular health (see Figure 7-2). The first, Allen explained, involves an inflammatory response in the lungs to PM inhalation which leads to the release of cytokines and other biomolecules into the circulatory system. The second mechanism involves the activation of the autonomic nervous system, which in turn affects blood vessels, heart rhythm, heart variability, and other physiological systems. The third mechanism involves direct transport of the smaller particles into the bloodstream, where they interact with blood vessels and various blood cells.
The methods for investigating the role of indoor PM on cardiovascular health include in vitro and epidemiologic studies. Epidemiologic studies, Allen said, have some important limitations, given the lack of good models for predicting indoor PM levels. “In most cases, we have to actually measure
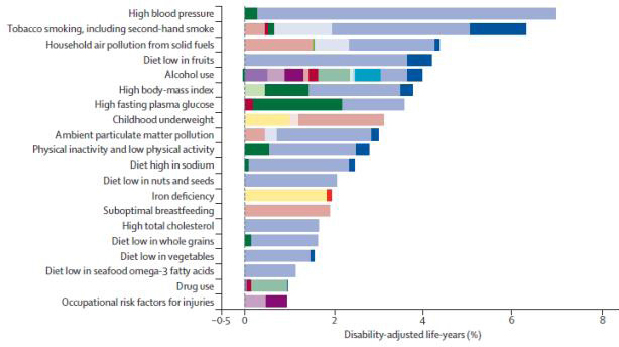
SOURCE: Allen slide 7, adapted from Lim et al. (2012) Figure 2C; reprinted with permission from Elsevier.
indoor PM,” he said, “and because these measurements are time-consuming and expensive, we end up studying relatively small populations that may be non-representative, creating challenges extrapolating our results to the broader general population.” The time and money constraints also lead to studies being restricted to examining short-term effects, on the order of days and weeks, rather than the years over which chronic disorders develop. The other main limitation of these studies is that they look at relatively subtle subclinical effects, such as changes in markers of inflammation and blood vessel function, rather than the clinically relevant outcomes of heart attack and stroke, among others.
As an illustration of the type of in vitro studies researchers perform, Allen described one study in which researchers collected PM samples inside and outside of homes in Boston, dosed rat lung macrophages with the particles, and then measured the release of cytokines from these immune system cells (Long et al., 2001). The results showed that there was a larger inflammatory response to indoor PM than to outdoor PM. Allen stressed that he did not want to overemphasize these data and that he was just using them as an example of the tools that investigators are bringing to bear on the challenge of understanding how indoor and outdoor PM affect inflammation and other relevant health indicators.
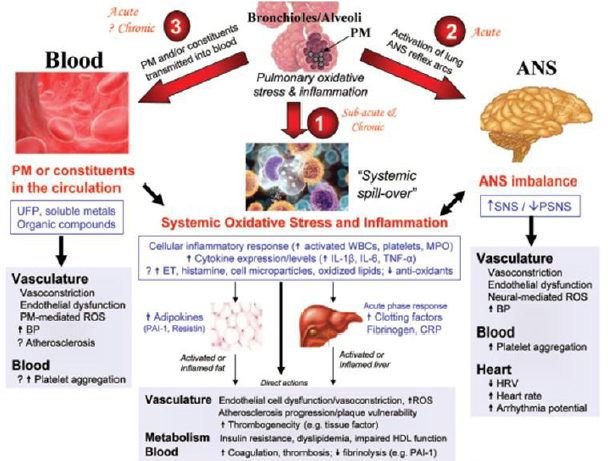
SOURCE: Allen slide 9, from Brook et al. (2010) Figure 3; reprinted with permission from Wolters Kluwer Health, Inc.
Allen then discussed some of the intervention studies that have been conducted. These studies use an air filter to reduce indoor PM levels, which, he explained, allows researchers to isolate the effects of PM from the polluting gases that may also be in the environment. In one study, Allen and his colleagues divided the residents of a wood smoke–affected community in the central part of British Columbia into two groups. Each participant was observed for two consecutive 7-day periods, during which time portable HEPA filters were operated in the participants’ living rooms and bedrooms. HEPA filters were operated normally during one 7-day period and without the internal filters in place (which was called “placebo filtration”) during the other period, thus blinding participants to the filters’ status. The order of filtration or non-filtration was random. Health measurements were made again after another week. The data showed that the use of portable HEPA filtration for 7 days, which reduced PM2.5 levels from 11 micro-
grams per cubic meter to 5 micrograms per cubic meter, was associated with improved blood vessel function and decreased systemic inflammation (Allen et al., 2011).
In a second study using the same design, Allen and his colleagues studied the differential effects of two different sources of PM: traffic emissions and residential wood combustion (Kajbafzadeh et al., 2015). Using previously developed spatial models, he and his colleagues were able to identify parts of Vancouver affected by traffic-related air pollution but not by wood smoke, and vice versa. The data from this study revealed an association between indoor PM2.5 and the blood levels of an inflammatory protein, but only in the group exposed to traffic-generated PM. “The take-home message,” Allen said, “is that indoor PM and its relation to health outcomes depends on where the PM2.5 is coming from, and this one small study suggests that particles produced by traffic may have some greater impacts than wood smoke particles on inflammation.”
Other intervention studies have shown that air filtration improves blood vessel function (Brauner et al., 2008; Karottki et al., 2013), reduces blood pressure (Padro-Martinez et al., 2015; Weichenthal et al., 2013), and reduces inflammatory and thrombogenic biomarkers (Chen et al., 2015). Allen also noted that one study in Massachusetts found results that were surprising and inconsistent in that filtration increased levels of a cytokine related to inflammation but also decreased blood pressure (Padro-Martinez et al., 2015). Allen said that the only cohort study of which he is aware, which looked at long-term exposure to indoor PM, found that long-term exposure to incense at home was associated with an increased risk of cardiovascular mortality (Pan et al., 2014).
In summary, Allen said, PM is an established cardiovascular risk factor, and the global public health burden of PM is primarily a result of its cardiovascular effects. Although the data are not entirely consistent, human studies have found links between indoor PM levels and increased systemic inflammation, blood vessel dysfunction, and increased blood pressure. The study of indoor PM, he said, presents an important epidemiologic research challenge, and more research is needed to better characterize the relative toxicity of PM generated indoors and outdoors, of PM from specific indoor and outdoor sources, and of PM2.5 versus UFP. Other knowledge gaps, he said in closing, concern the role that bioaerosols play in generating the cardiovascular effects of exposure to indoor PM and the relationship between long-term exposure and actual clinical outcomes such as heart attack and stroke.
AMBIENT PM AND ADVERSE BIRTH OUTCOMES2
The first indication that ambient PM levels might have an impact on adverse birth outcomes, David Rich said, came from a 1995 study in China. In this study (Xu et al., 1995), the investigators used the Beijing birth registry to identify all of the mothers living in one of two urban districts and data collected from ambient monitors in the city to calculate an estimated average pollutant concentration for the first, second, and third trimester and over the course of the entire pregnancy. These data showed that the mean pollutant concentration, as reflected by sulfur dioxide and total suspended particulate levels, in the 7 days before birth was correlated with a risk of preterm birth. The data from this study also revealed a significant increase in the risk of having a baby with low birth weight when average pollution levels rose during the third trimester (Wang et al., 1997). This type of study, using existing datasets of birth outcomes, birth registry data, and pollution levels, has been conducted in numerous locations around the world to evaluate whether air pollution exposure during pregnancy is associated with preterm birth, fetal growth restriction, and pregnancy complications, Rich said.
Another type of study, which Rich called a “natural experiment,” takes advantage of one-time events such as large sporting events, industrial facility closures, or government policies that drops ambient pollution levels for a defined time period and thus becomes a community-wide or region-wide intervention. One such study was conducted in the Utah Valley when a steel mill there closed for some 13 months, leading to a dramatic reduction levels of PM10 and other pollutants (Parker et al., 2008). The data from this study showed that the preterm birth rate in the Utah Valley dropped significantly during the period of the steel mill closure, whereas the preterm birth rate outside of the Utah Valley remained constant (see Figure 7-3). The finding that a drop in pollutant levels produced a beneficial health effect presents a powerful complement to studies showing an increase in pollutant levels produces a negative health effect, Rich said. “If this relationship is truly causal, we should see the effects in both directions,” he explained.
Rich was involved in another natural experiment which looked at differences in birth weight associated with the 2008 Beijing Olympics, when the Chinese government mandated that, to improve air quality during the event, industries were shut down for 47 days, cars were only to be driven every other day, and several other pollution restrictions were put in place. This resulted in PM2.5 levels dropping 40 percent, though they remained markedly higher than U.S. levels. The study by Rich and his colleagues
___________________
2 This section is based on the presentation by David Rich, an associate professor of public health sciences at the University of Rochester Medical Center, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
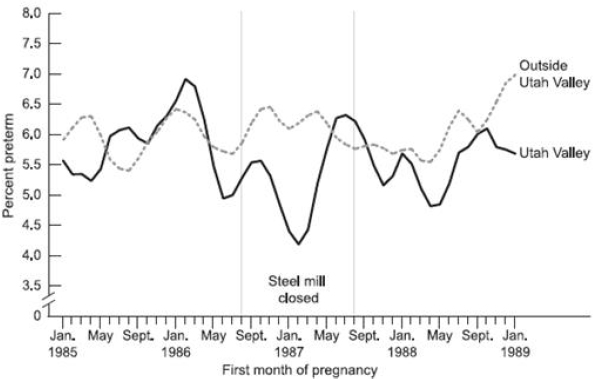
SOURCE: Rich slide 4, from Parker et al. (2008) Figure 1; reprinted with permission from Wolters Kluwer Health, Inc.
found an increase in birth weight for babies whose 8th month of gestation was during the Beijing Olympic Games period and its substantially lower air pollution levels (Rich et al., 2015). A separate analysis examining a longer study period and more pregnancies than just immediately before, during, and after the Beijing Olympic Games found that increases in 8th-month PM2.5, nitrogen dioxide, sulfur dioxide, and carbon monoxide levels were associated with decreased birth weight, which provided complementary evidence of a late-pregnancy air pollution effect on birth weight.
A review of 12 studies examining the connection between fetal growth and air pollution identified a number of methodological issues, Rich said (Woodruff et al., 2009). The authors of this review noted that the limitations to these studies included confounding by socioeconomic status and maternal characteristics, inconsistent reporting of when during a pregnancy the exposures occurred, and a limited examination of exposures and outcomes. The authors recommended increasing the use of natural experiments, accounting for the socioeconomic indicators in the regions being studied, using alternate outcome measures other than those in birth registries, and measuring alternate surrogates of exposure.
One outcome from this review was that an international group of investigators, including Rich, each ran the same analyses on their datasets and
found that the data, though not in total agreement, were consistent with the hypothesis that having a low-birthweight baby was associated with elevated exposures to PM10 during pregnancy (Parker et al., 2011). A more recent meta-analysis of these same studies’ data found that this relationship held for both PM2.5 and PM10 at a low but statistically significant level (Dadvand et al., 2013). “There is some evidence that air pollution causes or could cause fetal growth restriction, though the data are not consistent across the world and we do not yet fully understand mechanisms,” Rich said.
Rich then described a study in which researchers in Spain examined the relationship between nitrogen dioxide levels and markers of fetal development measured from ultrasound images. This analysis found that first-trimester exposure to nitrogen dioxide levels correlated with measures of fetal head size (Iñiguez et al., 2016). “The timing is not the same, but this study again suggests that exposure to elevated levels of air pollution during pregnancy can have an effect on fetal growth,” Rich said. One possible explanation for these findings could be that air pollution has an effect on the placenta that in turn affects fetal growth. To explore that possibility, a group of researchers looked at markers of placental growth and function and found that elevated levels of PM10 and nitrogen dioxide in the second trimester and during the entire pregnancy were associated with adverse changes in these markers (van den Hooven et al., 2012).
Pregnancy complications may also increase in frequency with elevated exposures to air pollutants. One study in southern California cited by Rich found an association between local traffic-generated air pollution—as measured by PM2.5 and nitrogen dioxide levels—and preeclampsia (Wu et al., 2009). Another study in New Jersey found that PM2.5, nitrogen dioxide, sulfur dioxide, and carbon monoxide levels were all correlated with an increased risk of stillbirth (Faiz et al., 2013).
Up to this point the studies that Rich discussed all dealt with ambient, or outdoor, PM, but he said that it should also be possible to study the effects of indoor PM exposure on birth outcomes. Pregnancy cohort studies, longitudinal panel studies that look at biomarkers throughout pregnancy, and intervention studies involving indoor air pollution could be used to study the effects of indoor PM on pregnancy outcomes, he suggested. Such studies would require identifying internal dose markers of individual exposures to indoor pollution and mechanistic biomarkers that could be measured throughout pregnancy. Rich suggested that researchers would need to determine when to make biomarker and pollutant measures, as well as whom to study and where such studies should be done.
To illustrate how researchers are addressing these issues, Rich cited a study now under way in Mexico City that enrolled non-smoking women ages 18 and older who would agree to visit the hospital for testing every 4 weeks for assessment (O’Neill et al., 2013). The 800 women in this study
filled out extensive questionnaires that generated data on demographics, time, and activity in order to estimate pollution exposure, food intake, and GPS coordinates for home and work locations. Clinical data collected included ultrasound images, a glucose tolerance test at 22 weeks of pregnancy, and blood, urine, and other samples for biomarker measurements. At birth, the infant’s characteristics, gestational age, and the baby’s saliva were collected, along with a blood sample from the mother and the umbilical cord. Data collection is now complete, and analysis is under way to determine if exposure to certain pollutants at different time points during pregnancy is associated with the clinical outcome of preterm birth and with increases in levels of markers of inflammation, said Rich.
The final study Rich discussed was conducted by Ryan Allen and Enkhjargal Gombojav in Ulaanbaatar, Mongolia. It examined whether removing indoor PM using a portable HEPA filtration unit would prevent preterm birth. The researchers enrolled 465 women and collected data on preterm birth, birth weight, and maternal blood pressure. They also collected hair, whole blood, and blood spot samples for biomarker analysis. Data collection for this study was completed in December 2015, Rich said, and analysis is under way.
NEUROLOGICAL AND PSYCHIATRIC DISORDERS3
Researchers have begun studying the effects of air pollutants and PM on neurological and psychiatric disorders, Marc Weisskopf said, because of data showing that PM exposure has established consequences for cardiovascular diseases. “Frankly, there is a great deal of interaction between the vascular system and the brain, and many vascular risk factors are associated with cognition, dementia, and late-onset depression,” he said. He added that studies have shown that PM2.5 and UFPs can reach the brain, either via the nose and olfactory nerve (Oberdorster et al., 2004) or via the lungs and systemic circulation (Peters et al., 2006). The route through the olfactory system is perhaps the most relevant, Weisskopf said, because the olfactory nerve connects directly to important centers in the brain involved in emotional regulation and memory as well as to the limbic system. Crossing from the systemic circulation into the brain involves direct transport or damage to the blood–brain barrier (Calderón-Garcidueñas et al., 2008).
There is evidence that whichever route PM takes into the brain (see Figure 7-4), it alters neurotransmitter levels (Sirivelu et al., 2006) and trig-
___________________
3 This section is based on the presentation by Marc Weisskopf, an associate professor of environmental health and occupational epidemiology at the Harvard T.H. Chan School of Public Health, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
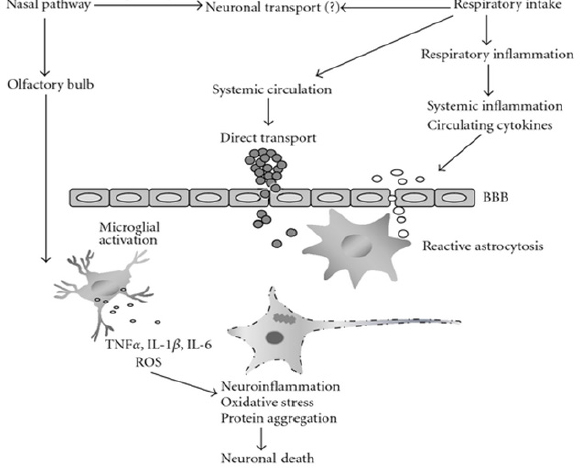
NOTE: BBB = blood-brain barrier; ROS = reactive oxygen species.
SOURCE: Weisskopf slide 4, adapted from Genc et al. (2012) Figure 1.
gers oxidative stress, inflammation, and other biochemical changes (Block and Calderón-Garcidueñas, 2009; Campbell et al., 2005; Kleinman et al., 2008), all of which can lead to neuronal degradation (Veronesi et al., 2005). All of these suggested negative consequences of particular exposure are evident in both human disorders and models of multiple neurodegenerative and psychiatric disorders, Weisskopf said. As an example, he cited one study in mice showing dramatic increases in the size of lateral ventricles—the space where cerebrospinal fluid circulates in the brain—with exposure to inhaled UFPs (Allen et al., 2015).
Experimental evidence suggesting involvement of the maternal inflammatory system in promoting autism-like behavior in mice (Choi et al., 2016), prompting researchers to look for a possible link between maternal PM exposure during pregnancy and autism. Using data from monitoring networks, meteorological readings, and a set of geographic information system–based predictors, Weisskopf and his colleagues created a time and space model of average predicted PM10 and PM2.5 levels from 1988 to 2007 (Yanosky et al., 2014). They then used this model to analyze data from the
Nurses’ Health Study II to estimate maternal exposure to PM10 and PM2.5 for 9 months before pregnancy, during pregnancy, and for 9 months after pregnancy and to identify those women who had children diagnosed with autism. Compared with a matched set of women who did not give birth to children who developed autism, there was an increased risk of autism in mothers who had higher PM2.5 exposure during any of those time periods, and particularly during the third trimester (Raz et al., 2015; Weisskopf et al., 2015). Weisskopf noted that several other groups have made similar observations (Becerra et al., 2013; Kalkbrenner et al., 2015; Talbott et al., 2015; Volk et al., 2013). “It’s becoming quite consistent to see this association between higher perinatal exposure to PM and increased risk of autism in many different settings,” Weiskopf said.
He and his colleagues have also been examining a potential link between PM exposure and anxiety. Data from the Nurses’ Health Study I showed that 15 percent of the nurses in this study had elevated anxiety symptoms. The researchers observed an association between elevated anxiety and PM2.5 exposure—but not PM10 exposure—within the month preceding the time at which the nurses filled out their questionnaires (Power et al., 2015). Weisskopf said that his team’s most recent analysis suggests that “very recent or maybe even daily exposure might affect anxiety levels.”
Other work from Weisskopf and his colleagues and other research teams in both the United States and Europe have revealed what Weisskopf called reasonably consistent results linking PM2.5 and UFP exposure to changes in cognitive function, including the development of dementia, Parkinson’s disease, and Alzheimer’s disease (Kioumourtzoglou et al., 2016; Power et al., 2011). He added that a group in Spain has started looking at the connection between PM and other pollutant levels near schools and cognitive function in children.
Finally, Weisskopf addressed some potential methodological issues that may confound the link between personal air pollutant exposure and neurological and behavioral disorders. One issue, which is common to epidemiologic studies, is that there may be others factor such as personal behavior that are related to both exposure and effect. That may be less of a concern with the aforementioned studies because the extensive work modeling ambient air pollution levels show that the inputs are largely independent of personal behaviors and many other factors that could also be related to disease. However, that independence is not likely to be true for indoor exposures to PM because personal behaviors are an important determinant of exposure. “That does not mean you cannot do these studies,” Weisskopf said, “but it raises concerns about bias issues that we have to pay attention to.” He suggested that one approach to dealing with this potential bias that could be applicable to studies of short-term cognitive function and perhaps anxiety would be to assess performance
on various cognitive tasks in a controlled office environment in which exposure levels could be adjusted.
DISCUSSION
To start the discussion, Howard Kipen commented that, in his opinion, the real challenge for the research community will be to identify which analyses will be useful to the regulating community in helping determine whether particular adverse health effects stem from indoor exposures or outdoor exposures. Rich said that the question becomes one of numbers with regard to how many people must be studied in order to have adequate statistical power to link outcomes with indoor PM exposure. He also said that an inexpensive validated marker of different indoor PM sources would be needed. Allen remarked that the epidemiologic studies that Weisskopf and Rich described are, in a sense, already addressing indoor PM given that people spend the majority of their time indoors. “So even when we see a signal from ambient PM, that has real relevance to what is happening inside people’s homes and in their workplaces,” he said.
This challenge, Allen said, is largely an exposure assessment issue, and he said he wants data with which to develop a time-and-space model for indoor PM in the same way that such models have been developed for outdoor PM. His group has tried to do that using property tax records to see if there were variables such as the age of the home and location that would allow them to predict PM infiltration. “It showed some promise, but it was not good enough to use in an epidemiologic analysis,” he said. “Maybe we can explore other data sources that will help us understand residences, what is going on inside residences, and the infiltration of outdoor pollution indoors.”
Weisskopf agreed with Allen’s idea but said that he thought it would be difficult to find variables that will be good indoor predictors at the individual level. He added that he believes that intervention studies, where PM is removed from the indoor environment, could make possible the kind of analysis Kipen would like to see for short-term effects. For larger prospective cohort studies, he suggested doing smaller validation studies to see if there are simple questions that could be asked of study subjects that could probe the link between indoor activities and indoor air particulate levels. He mentioned the study on incense burning that Allen had described as an example. William Fisk thought it would be difficult to study a large enough population to get statistically meaningful data to link indoor PM exposures to long-term health issues. Barbara Turpin said there have been questionnaire-based studies in which 24- or 48-hour average PM levels were measured at the same time, but for the most part there is not a strong association between indoor PM levels and particular activities and sources in the
home. Finding such associations will require real-time PM measurements or a chronic exposure situation where an activity happens frequently every day.
Joseph Hughes from the IAQ Training Institute said that researchers at the Carnegie Mellon University Robotics Institute have developed an under-$200 device called Speck that measures and records PM2.5 levels in real time and uploads data to the Web. Rich mentioned that researchers at Clarkson University are trying to use some of these low-cost sensors to measure PM both indoors and outdoors. Weisskopf then asked if there is a filtration system that records how much PM is removed from circulated air and if such data could be used to calculate exposure levels. William Nazaroff replied that there are well-developed models for estimating indoor exposure in a mechanically ventilated building that could provide useful estimates for exposure at work, but this would still leave exposures at home to be determined. He added that he is optimistic that collaborations among members of the International Society of Environmental Epidemiology, the International Society of Exposure Science, and the International Society of Indoor Air Quality and Climate would provide a better mechanistic understanding of how to take outdoor PM levels and provide estimates of indoor exposures.
Arnold Schwartz from the Milken Institute of Public Health at the George Washington University asked Weisskopf if there were any correlations between pollution and olfactory nerve dysfunction. Weisskopf replied that there is evidence relevant to that question in occupational exposure settings and said that he and his research team are in the process of accumulating a large enough dataset to look at the effect of ambient air pollution exposures on olfactory nerve dysfunction. Schwartz then asked Rich if there is a correlation between inflammatory markers in placental tissue and in blood and if there are morphological changes within the placenta corresponding with those inflammatory markers. Rich replied that he is not aware of studies that have looked specifically at whether inflammation in the mother affects the placenta in a way that affects the fetus. He said he is optimistic that such studies would be performed soon. Weisskopf added that this is an important question for his work on autism because it points to something happening during the pregnancy period that is not tied to transport of particles to the fetal brain. “I think there is a maternal component we should be examining,” Weisskopf said. Schwartz also asked Allen if there are markers of indoor pollution that provide a linkage with atherosclerosis. Allen said he was unaware of any research explicitly looking at that link. He added, though, that inflammation is known to play an important role in the development of atherosclerosis, so it would make sense mechanistically that such a link might exist.
Paula Olsiewski from the Alfred P. Sloan Foundation asked if the panelists knew of anybody who is studying the effect of PM on the human
microbiome. Kipen said his group is conducting some pilot studies toward that end but not in the indoor air context. Rich said he has reviewed a few grants proposals in that area but has not yet seen any research in the literature.
Fisk said that there should be an explicit notice in the workshop summary that allergy and asthma were not addressed in this session on health concerns. Kipen, who was on the workshop planning committee, acknowledged the importance of allergy and asthma but said that the decision had been made to focus on lesser-known and emerging health concerns in the time available. Rich agreed that there is a large body of work on allergy and asthma and said that in his mind there are fewer questions about whether there is a relationship between those outcomes and PM exposure.
An online workshop participant asked if the neurological health effects of PM exposure are thought to be caused by the irritant effect or by the chemical composition of the particles, and Weisskopf replied that he would guess that the answer is both. The irritant effect could trigger the inflammatory cascade and activation of microglial cells that prune the connections between nerve cells, he said, and if there were metal ions in the particles, such as lead, they could certainly have direct adverse effects on nerve cells.
Lynn Hildemann said she is intrigued with idea of trying to identify which PM sources have more or less effect on human health, and she asked the panelists if studies of occupations could provide any relevant information. For example, she said, a study of cooks might provide a good first estimate of how important exposure to cooking emissions is in terms of impacts on human health. Rich said that would be a good approach for something such as birth outcomes where there is a defined event—birth—with a well-defined date. “I think that is the kind of innovative, novel idea to try to take first-pass stabs at whether or not these sources could have important impacts,” Rich said. Weisskopf noted that such studies are the foundation of classic occupational epidemiology. In fact, he said, he is doing just such a study in Denmark, where there are records tracking health outcomes and occupations for the entire population. What remains to be done, he said, is working with industrial hygienists and occupational epidemiologists to make measurements of indoor pollutant levels in various occupational settings.
Kipen asked if it should be possible to add a reasonable set of questions to the annual Nurses’ Health Study that could be used to provide a retrospective analysis of residential exposures. Rich responded that such an approach could be a relatively inexpensive way to get preliminary data to look at long-term exposures, but he said that it would not be very useful for acute effects. Weisskopf said that the Nurses’ Health Study III is in the process of recruitment and that it focuses specifically on younger women and includes questions on reproductive outcomes. “What we need to know,”
he said, is, “What are the questions to ask about the home environment? Which ones are the biggest drivers of changes in indoor particulate matter?” Developing those questions, he said, will require going into various types of homes, performing detailed assessments, analyzing the data to determine those factors that predict PM levels and account for the most variance, and then deciding if those factors can be captured in a reasonably simple question.
Allen added that it would be important to capture exposure variability. “If everybody is exposed to the same level, you cannot do an epidemiologic study,” he said. “You need the exposure contrast.” He also commented that questionnaires are only going to be able to capture information on the major sources of PM and said that there might not be sufficient variability in a specific population. “If everybody is cooking roughly the same amount in a week, it is going to be more difficult to see associations with health just because the exposure variability within the population will not be there,” he said.
Laura Kolb from EPA asked the panel to offers their views on the scope of indoor PM as a public health issue. Weisskopf replied that if there is a link between PM exposure and anxiety, then this is a significant public health problem. “I think environmental exposures have been under-appreciated in that realm, and the fact is, particulate matter is ubiquitous,” he said. “If it even has a subtle effect, across the population, I think, it could be quite large. If you are knocking down IQ (intelligence quotient) by even a few points or having a bad day in the office because of particulate matter, that is a big impact on productivity.” He noted, though, that there is the important question of how much exposure people are getting indoors over the course of the entire day.
Allen said he agreed completely with Weisskopf, both in terms of potential impact and the importance of determining indoor exposures, and he said that, at least for outdoor exposures, there does not appear to be a threshold in terms of dose–response level. “Any exposure seems to carry some health risk,” he said. In the context of cardiovascular disease, he said that because these are prevalent outcomes, increasing the risk by 5 or 10 percent adds a significant number of additional cases. The bottom line, he said, is, “We do not know, but the potential is there for this to be a significant public health issue.”
Rich agreed, adding that reproductive health outcomes were also a public health issue internationally. The issue with air pollutants such as PM is that everyone breathes, and so every pregnant woman is exposed to PM. “I think the absolute risk for some of these outcomes could be substantial simply because of the complete exposure everyone has,” Rich said.
This page intentionally left blank.
















