26 Taking an Exposure History
|
Environmental ALERT…
|
This monograph is one in a series of self-instructional publications designed to increase the primary care provider’s knowledge of hazardous substances in the environment and to aid in the evaluation of potentially exposed patients. See page 35 for more information about continuing medical education credits and continuing education units.
|
Guest Contributor: |
Arthur L.Frank, MD, PhD |
|
Guest Editor: |
Sophie J.Balk, MD |
|
Peer Reviewers: |
John Ambre, MD, PhD; Charles Becker, MD; Jonathan Borak, MD; Joseph Cannella, MD; Howard Kipen, MD, MPH; Richard J.Jackson, MD, MPH; Jonathan Rodnick, MD; Brian A.Wummer, MD |

U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES
Public Health Service
Agency for Toxic Substances and Disease Registry in conjunction with Centers for Disease Control and Prevention,
National Institute for Occupational Safety and Health
Case Study
On Tuesday afternoon, a 52-year-old man with previously diagnosed coronary artery disease controlled by nitroglycerin describes episodes of recurring headache for the past 3 weeks. Mild nausea often accompanies the headache; there is no vomiting. He describes a dull frontal ache that is not relieved by aspirin. The patient states that the headaches are sometimes severe; at other times they are a nagging annoyance. The durations range from half an hour to a full day. His visit was prompted also by a mild angina attack that he suffered this past weekend, shortly after awakening on Sunday morning. He has experienced no further cardiac symptoms since that episode.
History of previous illness indicates that the patient was diagnosed with angina pectoris 3 years ago and has been taking nitroglycerin 0.4 mg sublingually prophylactically before vigorous exercise. He also takes one aspirin every other day. He has been symptom-free for the past 2 1/2 years. Sublingual nitroglycerin relieved the pain of the Sunday morning angina attack within several minutes. The patient does not smoke and rarely drinks alcohol.
He is a trim man with a slightly ruddy complexion. At present, he is afebrile, and his vital signs are blood pressure 120/85, pulse 80, respirations 20. Physical examination including HEENT, heart, lungs, and neurologic exam is normal. The results of an EGG with a rhythm strip performed in your office are unremarkable. Subsequent laboratory testing reveals normal blood lipids, cardiac enzymes, CBC, sedimentation rate, glucose, creatinine, and thyroid function.
![]()
(a) What would you include in the patient’s problem list?
_________________________________________________________________
_________________________________________________________________
_________________________________________________________________
(b) What would you include in the differential diagnosis?
_________________________________________________________________
_________________________________________________________________
_________________________________________________________________
(c) What additional information would you seek to assist in the diagnosis?
_________________________________________________________________
_________________________________________________________________
_________________________________________________________________
Answers are on page 33.
Introduction
The preceding case study describes a patient with angina. He has new, nonspecific symptoms of headache and nausea. Suppose this patient lived near a hazardous waste site. Would your differential diagnosis change? If the patient refinished furniture as a hobby, would you consider this important? Is there a connection between his headaches and cardiac symptoms? How would you investigate the possible correlation? Could he be exposed to chemicals in his workplace? Each of these factors could play a role in the etiology of this patient’s illness; each exposure could cause disease.
The patient described in the case study—a 52-year-old male with angina—is portrayed in three different scenarios throughout this document. An exposure history form, completed by the patient in each scenario, provides clues that prompt the clinician to investigate the possibility of toxic exposure.
-
Scenario 1: This patient is an accountant who has had the same job and residence for many years.
-
Scenario 2: This patient owns a commercial cleaning service and uses cleaning products at various industrial and commercial sites.
-
Scenario 3: This patient is a retired advertising copywriter who lives in the vicinity of an aban doned industrial complex.
Most environmental and occupational diseases either manifest as common medical problems or have nonspecific symptoms. It is the etiology that distinguishes a disorder as an environmental illness. Unless an exposure history is pursued by the clinician, the etiologic diagnosis may be missed, treatment may be inappropriate, and exposure can continue.
Most people with illness caused or exacerbated by exposure to hazardous substances obtain their medical care from clinicians who are not specialists in either environmental or occupational medicine. Few clinicians, however, routinely elicit information about the home, workplace, or community environment as part of the demographic and social history. In a study of a primary care practice in an academic setting, only 24% of 625 charts had any mention of the patient’s occupation. Only 2% of the charts had information on exposures, duration of present employment, and past occupations. In addition, clinicians caring for adolescents seldom ask about their work exposure and history during routine health care visits or when evaluating symptoms.
Although many clinicians do recognize the importance of taking a work and exposure history for evaluating certain problems, most have had little training or practice in doing so. Extensive knowledge of toxicology is not needed to diagnose environmental and occupational disease. The same criteria are employed as those used in diagnosing other medical problems—history including onset and temporal pattern of symptoms, palliative and provocative factors, physical examination, and laboratory results. If necessary, consultation with industrial hygienists or environmental testing can be used. In addition to current exposures, the clinician must consider the long-term or latent effects of past exposures to agents such as asbestos, radiation, and chemical carcinogens.
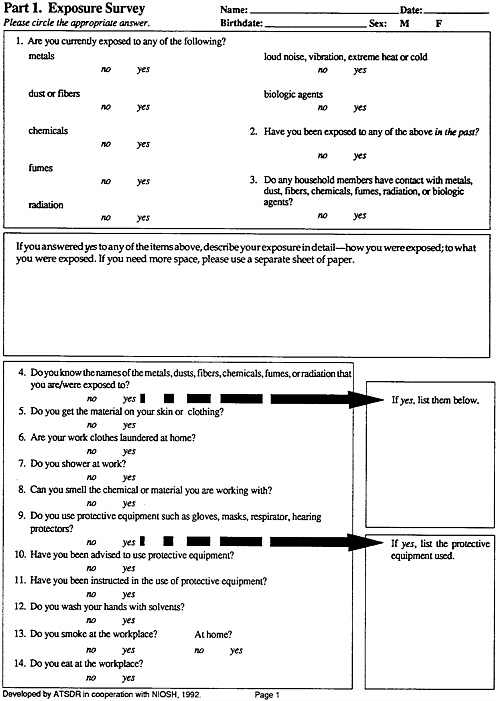
Investigating environmental and occupational illness is illustrated in this monograph. The aim is not to demonstrate all exposure possibilities but rather to illustrate the principles and the process of investigating this etiology. The exposure history form (pages 23–26), which can be completed by the clinician or by the patient (to save staff time), will guide the clinician through various aspects of this process. The form elicits many important points of an exposure history including job descriptions and categories associated with hazardous substances, physical and biologic agents, and temporal and activity patterns related to environmental and occupational disease. The form explores past and current exposures.
Taking an exposure history requires only a few minutes of the clinician’s time and can be abbreviated, expanded, or focused according to the patient’s signs and symptoms. The exposure history form is designed for quick scanning of important details and can be copied and used for a permanent database as well as for the investigation of current problems.
The diagnosis of environmental or occupational disease cannot always be made with certainty. Sound clinical judgment must be used, and common etiologies should be considered. The multifactorial nature of many conditions, particularly chronic diseases, must not be overlooked.
An exposure history should be taken on every patient. It is of particular importance if the patient’s illness occurs at an atypical age or is unresponsive to treatment. The clinician must also keep in mind that many organ systems are affected by toxic exposure (Table 1). The latency period from exposure to manifestation of disease can vary—ranging from immediate to delayed (hours or days) to prolonged (decades).
With practice using the exposure history form and a network of referrals, the primary care clinician can play an important role in detecting, treating, and preventing disease resulting from toxic exposures.
Organ Systems Affected by Toxic Exposure
The respiratory system is both a target organ and a portal of entry for toxicants. Adult-onset asthma and death from asthma are increasing. More than 100 toxicants are known to cause asthma, and many more can exacerbate it.
Irritant and allergic contact dermatitis account for 90% of occupational skin disorders. Other skin disorders with exposure etiologies include pigment alterations, chloracne, urticaria, and malignant neoplasms.
Alcohol abuse is a potential confounding factor in the evaluation of patients with suspected toxic exposure. However, a history of alcohol use does not necessarily exclude an environmental or occupational etiology. Symptoms of liver disease due to toxic exposure can mimic viral hepatitis.
About 4000 new cases of renal disease of unknown etiology are diagnosed annually. Organic solvents and heavy metals are two classes of toxicants known to adversely affect renal function.
Neurotoxins can cause peripheral neuropathy, ataxia, parkinsonism, seizures, coma, and death. Many chemicals cause mild central nervous system depression that may be misdiagnosed as personality disorders or that can progress to psychoses or dementia. Sensory impairment can also be caused by exposure to toxicants (e.g., visual disturbances caused by methanol) and physical agents (e.g., hearing impairment caused by loud noise).
About 200,000 infants are born annually with some form of birth defect. The causes of most of these defects are unknown.
Table 1. Organ systems often affected by toxic exposure
|
Organ/System |
Exposure Risks |
|
Respiratory |
|
|
Dermatologic |
dioxin,* nickel, arsenic,* mercury,* cement (chromium*), PCBs,* glues, rubber cement |
|
Liver |
|
|
Kidney |
cadmium,* lead,* mercury,* chlorinated hydrocarbon solvents* |
|
Cardiovascular |
carbon monoxide, noise, tobacco smoke, physical stress, carbon disulfide, nitrates,* methylene chloride* |
|
Reproductive |
|
|
Hematologic |
|
|
Neuropsychologic |
tetrachloroethylene,* mercury,* arsenic,* toluene,* lead,* methanol,* noise, vinyl chloride* |
|
*This substance is covered in Case Studies in Environmental Medicine, which is a series of self-instructional booklets on specific chemical hazards developed by the Agency for Toxic Substances and Disease Registry (ATSDR), Division of Health Education. A complete list of titles and information on how to obtain them is on page 38. |
|
The cardiovascular and hematologic systems are frequent targets of toxicants. Cardiovascular changes, as well as exacerbation of preexisting cardiovascular conditions, can result from exposure to noise and to chemicals such as carbon monoxide and tobacco smoke. Benzene can cause bone marrow changes leading to aplastic anemia, acute leukemia, and chronic myelogenous leukemia.
Toxicants in the Home/Environment
The clinician should consider the following sources, which are discussed below, when eliciting information on exposures in the home and environment:
-
Indoor air pollution
-
Common household products
-
Pesticides and lawn care products
-
Lead products and waste
-
Recreational hazards
-
Water supply
-
Soil contamination
Indoor Air Pollution
Tobacco Smoke
Does anyone in the household smoke? How many packs per day?
Environmental tobacco smoke is a mixture of more than 4700 compounds. Mainstream smoke is exhaled by the smoker, and sidestream smoke comes off the smoldering end of the cigarette and is inhaled by adjacent persons (passive smokers). Sidestream smoke contains more carcinogenic hydrocarbons and respirable particles than mainstream smoke. All smokers should be encouraged to stop smoking; if household members will not refrain from smoking, they should smoke only in well-ventilated or isolated areas.
Wood Stoves/Gas Ranges
Does the patient have a wood stove?
Is there a smoke smell indoors?
When was the last time the chimney and stove were cleaned?
Thirteen million wood stoves are in use in the United States, and 800,000 are sold annually. When not properly maintained and vented, wood stoves emit noxious gases including carbon monoxide, oxides of nitrogen, particulates, and hydrocarbons. Studies have shown that children living in homes heated with wood stoves have a significant increase in respiratory symptoms compared with children living in homes without wood stoves.
If the patient uses a gas range, is it in proper working order?
Does the patient use the gas range for heat?
Gas ranges, which may produce nitrogen oxide, a respiratory irritant, are used for cooking in more than half of U.S. homes. In low-income areas, gas stoves may be used not only for cooking but as a supplemental source of heat. Proper ventilation and routine inspection and maintenance are necessary in residences where wood or gas stoves are used.
Building Materials
Does the patient live in a mobile home?
Building materials, home improvement products, and textiles used in the home can pose health risks. For example, formaldehyde volatilizes
Was urea formaldehyde foam used for insulation?
Is cabinetry or furniture made of pressed wood?
from particle board, insulation materials, carpet adhesives, and other household products. This is a particular problem in the confined spaces of mobile homes. Formaldehyde exposure can cause rhinitis, nausea, dry skin or dermatitis, and upper respiratory and eye irritation. It has also been reported to precipitate bronchospasm in persons who have asthma.
Asbestos
Was asbestos insulation used on pipes or hot water tank?
Do walls and ceilings have sprayed-on or troweled-on material?
Is renovation work planned in any of the areas containing asbestos?
Are adults in the household exposed to asbestos on the job?
Asbestos was widely used from 1950 to the early 1970s in areas requiring sound proofing, thermal proofing, or durability (e.g., floor and ceiling coverings, heating and water pipe insulation). It was often applied as a spray-on material. Asbestos that is in good condition and not respirable is generally not a risk. However, when it becomes frayed or friable (i.e., easily crumbled), asbestos fibers can be released into the air. Exposure to these fibers has been associated with lung cancer, asbestosis, and mesothelioma. The occurrence of disease is influenced by type of asbestos mineral inhaled, concentration and dimension of the fibers, and exposure duration. In 1986, the Environmental Protection Agency (EPA) estimated that friable asbestos may be present in as many as 35,000 schools in the United States, potentially exposing 15 million schoolchildren and 1.4 million adults. Smoking cigarettes, in addition to asbestos exposure, increases the risk of cancer by an order of magnitude above smoking alone or asbestos exposure alone. Children may be at greater risk than adults because of their long life expectancy, high activity rates, high breathing rates, more time spent near the floor where fibers accumulate, and greater likelihood of contact (through curiosity or mischief). (For further information on the health hazards of asbestos exposure, consult Case Studies in Environmental Medicine: Asbestos Toxicity, ATSDR, June 1990.)
Radon
Has the patient’s home been tested for radon?
If yes, what were the results?
Are there high levels in homes in the area?
Do children spend a significant amount of time in the basement or on the first floor of the home, where radon might tend to be in higher concentrations?
Radon, a colorless, odorless gas, is a decay product of uranium found in significant concentrations in some areas. Radon itself does no harm, but its progeny attach to airborne particulates such as cigarette smoke and can be inhaled. During subsequent decay, the progeny emit high-energy alpha particles that may injure adjacent bronchial cells, thereby causing lung cancer. Five to ten percent of single-family homes in the United States have been estimated to exceed the EPA radon recommended guideline of 4 picocuries per liter of air. EPA estimates that approximately 14,000 lung cancer deaths per year are attributable to radon. (For further information about radon exposure and its health effects, see Case Studies in Environmental Medicine: Radon Toxicity, ATSDR, September 1992.)
Common Household Products
Does the patient use any of the following on a regular basis: cleaners for glass, oven, floors, drains, toilets, polishes, air fresheners and disinfectants, glues, solvents, paint strippers, sealants?
A 1987 EPA study found approximately 12 common organic pollutants in concentrations 2 to 5 times higher in air inside homes than in outdoor air from use of household products. Product warning labels are often inadequate and pertain to acute exposures only. Long-term or repeated use of some household chemicals, such as chlorinated hydrocarbons, can result in cancer. Commonly used compounds that
Where are these chemicals stored and disposed of?
can have serious adverse effects are methylene chloride (found in paint strippers and thinners, and adhesive removers), tetrachloroethylene (used in dry cleaning of clothes), and paradichlorobenzene (found in room air fresheners, toilet bowl deodorizers, and moth crystals). (See Case Studies in Environmental Medicine: Methylene Chloride Toxicity, ATSDR, June 1990, and Tetrachloroethylene Toxicity, ATSDR, June 1990.)
Pesticides and Lawn Care Products
Does the patient use pesticides on the garden and lawn?
Does the patient employ a professional lawn-care company?
Are children allowed to play in areas recently sprayed with pesticides or lawn-care products?
Does the patient use bug repellants?
Does the patient know what to do in case of accidental poisoning?
Pesticides and lawn care products are potentially hazardous, especially to children. Pesticide exposure can occur through dermal contact, inhalation, or ingestion. At least 1400 active ingredients can be found in more than 34,000 available preparations of insecticides, herbicides, fungicides, and other antibiologic preparations. These agents have different mechanisms of action and toxicity. Estimated annual use of these chemicals is 2.6 billion pounds.
Despite the ban on certain pesticides in the United States, exposure can still occur through improper use, storage, and disposal. Some banned pesticides are used in foreign countries and may return to this country on imported foods. Proper use and storage of household pesticides and proper cleaning of food, especially raw fruits and vegetables, can help protect consumers.
Lead Products and Waste
What year was the patient’s home built? Is indoor paint in poor repair?
Is the inside of the patient’s home being renovated?
Has the patient’s drinking water been tested for lead?
Does the patient use imported earthen-ware pottery?
Do any household members work with lead (e.g., in a lead refinery or smelter, battery factory, or power plant)? If yes, are work clothes brought home?
Do any household members work with arts and crafts products containing lead?
Does the patient live near a lead refinery or smelter, battery factory, or power plant?
Lead poisoning continues to be a significant health problem in the United States. Although lead was banned from paint for home use in 1972, millions of homes, particularly those built before 1950, still contain high amounts of lead in paint that is peeling and accessible for ingestion by children. Lead exposure also occurs through drinking water, especially in homes that have lead plumbing or lead-soldered pipes. Significant exposures have occurred in children who played in lead-contaminated soil. Acidic foods, such as juices, stored in imported pottery may leach lead from ceramic glazes. Some ceramic glazes used by hobbyists also may contain lead. Air can be contaminated with this metal through use of leaded gasoline. Parents can inadvertantly bring it home on their clothing and shoes, or in their cars if they work in jobs where they are exposed to lead dusts or lead-containing compounds.
More than a million U.S. workers are potentially exposed to lead daily in hundreds of occupations such as construction work, radiator repair, metals recycling, battery manufacturing, smelting, and pigments formulating. Good workplace and personal hygiene practices can prevent the majority of these “take-home” exposures.
The 1985 intervention level of 25 mg/dL has been revised downward to 10 mg/dL. Childhood lead exposure has been associated with lower class ranking and higher absenteeism in school, poor eye-hand coordination, slow reaction time, and lower vocabulary test scores. Consequences of childhood lead exposure have been shown to endure into adulthood. (See Case Studies in Environmental Medicine: Lead Toxicity, ATSDR, Revised September 1992.)
Recreational Hazards
Do the patient’s children play on wooden playground equipment that has been treated and sealed?
Do the children play in a sandbox that may contain tremolite (asbestos)?
Recreational areas and products can pose a hazard to health. Fishing and swimming in contaminated lakes and streams can expose participants to toxins contained in polluted waters. Wooden playground structures that have not been treated with protective sealants may allow children to have dermal contact with potentially hazardous wood preservatives; these include arsenic-containing compounds, pentachlorophenol, and creosote. Some play sands and clays have been reported to contain asbestos-like fibers. Other materials used in arts and crafts involve potentially hazardous silica, talc, solvents, and heavy metals such as lead and cadmium. Toxic materials may be encountered in making stained glass and jewelry, woodworking, model building, and oil and airbrush painting. One need not be directly involved in these activities to become exposed; merely being in the vicinity of a work area may cause exposure. Federal legislation (Labeling of Hazardous Materials Act) will require that all chronically hazardous materials be labeled as inappropriate for children’s use. (See ATSDR series Case Studies in Environmental Medicine: Arsenic Toxicity, June 1990; Pentachlorophenol Toxicity, December 1992; Cadmium Toxicity, June 1990; and Asbestos Toxicity, June 1990.)
Water Supply
What is the source of the patient’s water supply?
If the patient uses a private well, when was the last time the water was tested?
Both public water supplies and private wells can be a source of toxic exposure, especially for industrial solvents, heavy metals, pesticides, and fertilizers. For example, an EPA groundwater survey detected trichloroethylene in approximately 10% of the wells tested. It is estimated to be in 34% of the nation’s drinking water supplies. Up to 25% of the water supplies have detectable levels of tetrachloroethylene. Methylene chloride may remain in groundwater for years. Some solvents can volatilize from showers and during laundering of clothes, thereby creating risk of toxicity via inhalation. Nitrates, a common contaminant of rural shallow wells, pose a risk of methemoglobinemia, especially to infants. (See ATSDR series Case Studies in Environmental Medicine: Asbestos Toxicity, June 1990; Arsenic Toxicity, June 1990; Lead Toxicity, Revised September 1992; Nitrates/Nitrites Toxicity, October 1991; Trichloroethylene Toxicity, January 1992; Methylene Chloride Toxicity, June 1990; Tetrachloroethylene Toxicity, June 1990.)
Soil Contamination
Did the patient or previous owners use chlordane or other pesticides or termiticides in the home?
What is the history of the site on which the home was built?
Ingestion of contaminated soil poses a risk of toxicity, especially to children under the age of six because of natural mouthing behaviors. Lead is a common soil contaminant. Dioxin also adsorbs to soils. Certain pesticides such as chlordane can remain in the soil for years. (See ATSDR series Case Studies in Environmental Medicine: Arsenic Toxicity, June 1990; Lead Toxicity, Revised September 1992; Dioxin Toxicity, June 1990; Chlordane Toxicity, December 1992; Cadmium Toxicity, June 1990; Chromium Toxicity, June 1990.)
Using the Exposure History Form
A work and exposure history has three components: Exposure Survey, Work History, and Environmental History. The main aspects of an exposure history (summarized in Table 2) will be elicited through the exposure history form (pages 23–26). Although a positive response to any question on the form indicates the need for further inquiry, a negative response to all questions does not necessarily rule out a toxic exposure etiology or significant previous exposure.
All patients should complete exposure history forms, although the form need not be evaluated extensively in every clinical situation. As in all data-gathering activities, sound clinical judgment must be exercised.
Table 2. Components of an exposure history
|
Part 1. Exposure Survey A. Exposures Current and past exposure to metals, dust, fibers, fumes, chemicals, biologic hazards, radiation, noise, vibration Typical work day (job tasks, location, materials, agents used) Changes in routines or processes Other employees or household members similarly affected B. Health and Safety Practices at Worksite Ventilation Medical and industrial hygiene surveillance Employment exams Personal protective equipment (e.g., respirators, gloves, coveralls) Lockout devices, alarms, training, drills Personal habits (Smoke, eat in work area? Wash hands with solvents?) Part 2. Work History Description of all prior jobs including short-term, seasonal, part-time employment and military service Description of present job(s) Part 3. Environmental History Present and prior home locations Jobs of household members Home insulating, heating and cooling system Home cleaning agents Pesticide exposure Water supply Recent renovation/remodelling Air pollution, indoor and outdoor Hobbies: painting, sculpting, welding, woodworking, piloting, autos, firearms, stained glass, ceramics, gardening Hazardous wastes/spills exposure |
Part 1. Exposure Survey
Past and current exposures are recorded on pages 1 and 2 of the exposure history form, which is designed for easy completion by the patient and quick scanning for pertinent details by the clinician. The questions investigate the following: known exposure to metals, dust, fibers, fumes, chemicals, physical agents, and biologic hazards; details about known toxicant exposure; other persons affected; temporal patterns and activities, changes in routines and worksite characteristics, and protective equipment use.
If the patient answers yes to one or more questions on Part 1, the clinician must follow up by asking the patient progressively more detailed questions about the possible exposure. Special attention should be directed to the route, dose, duration, and frequency of any identified exposure.
Scenario 1 below illustrates the use of part 1 of the form with the patient described in the case study (page 1). The patient’s chart reveals that he has worked as an accountant in the same office for the past 12 years. On the completed form, he indicates that no other workers are experiencing similar or unusual symptoms, and he denies recent changes in his job routine. The patient answered yes to three questions: “Are family members experiencing the same or unusual symptoms?”; and “Do your symptoms get either worse or better at work? on weekends?” His explanations of these answers reveal a possible temporal relationship between his symptoms and home. The clue and the clinician/patient dialogue follow.
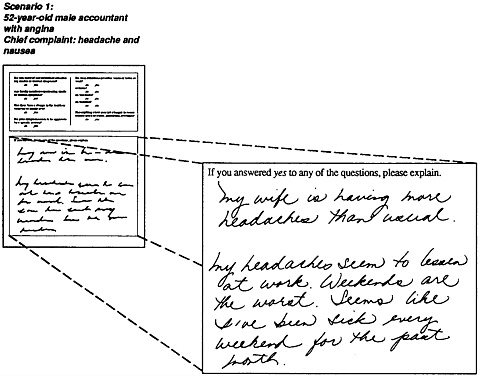
Clinician: I see that you noted that your wife is having headaches.
Patient: Yes. She has frequent headaches. In the last 3 or 4 weeks she has had more than usual. She usually has one every month or so; this past month she had three.
Clinician: You also state that your headaches are worse on weekends.
Patient: Yes, they seem to be. If I wake up on a Saturday or Sunday with a headache, it usually gets worse as the day progresses. In fact, that’s usually when I feel nauseated too.
Clinician: Do your symptoms seem to be aggravated by certain activities around the home? A hobby or task?
Patient: No, I usually wake up with the headache. I don’t think there’s a connection with anything I do.
Clinician: Do your symptoms change at all at work?
Patient: Now that you mention it, if I wake up with a headache, by the time I get to work-it takes about 25 minutes-the headache is usually gone.
Clinician: Your angina attack occurred on a Sunday morning. Describe your weekend leading up to the attack.
Patient: It was a fairly quiet weekend. We had dinner at home Friday evening and just relaxed. On Saturday I spent the day packing old books and storing them in the attic and chopping and stacking firewood. I took one nitroglycerin tablet before doing the heavy work, at about 2 PM. Saturday night we had friends over for dinner. We had a fire in the fireplace and visited until about 11 PM. I had one glass of wine with dinner. I was beginning to feel a little stiff and sore from the work I did that afternoon. Sunday morning I woke up with a headache again. A few minutes after awakening, while I was still in bed, I had the attack. It was mild, not the crushing pain I’ve had in the past. I had the headache all day.
The preceding dialogue reveals that the patient’s symptoms may be associated with the home environment and his cardiac symptoms, headache, and nausea may be related. His symptoms seem to be exacerbated at home and lessen at work. Further questioning is needed to pursue this lead.
Clinician: What does your wife do for a living?
Patient: She’s an attorney.
Clinician: Do either one of you have a hobby?
Patient: My hobby is photography. My wife is an avid gardener.
Clinician: Do you have your own darkroom?
Patient: No, I occasionally use a friend’s. For the past year I’ve had my film and prints processed commercially.
Clinician: Does your wife use any pesticides or chemicals in the garden?
Patient: No, she does strictly organic gardening and uses only natural means of pest control.
Clinician: Do you work on your car?
Patient: No.
Clinician: Have you gotten any new furniture or remodeled your home in the past few years?
Patient: No.
Clinician: What is your source of heating and cooking in the home?
Patient: We have a natural gas, forced-air heating system. We cook with gas and use the fireplace a lot in winter.
Clinician: How long have you lived in this home and how old is your furnace?
Patient: We’ve lived there for 23 years. The furnace was replaced about 12 years ago.
Clinician: I see that you recently insulated your home. What exactly did you do?
Patient: Yes. Last month I added extra insulation to the attic, insulated the crawl space, replaced all the windows with double-paned windows, and weatherized all doorways.
Clinician: Have you noticed that the headaches coincide with days you have used the fireplace?
Patient: There could be a connection. I definitely use the fireplace more on weekends. This past Saturday I had a fire blazing all day.
A temporal relationship between the headaches and being in the home has been revealed. Some sources of toxicants have been eliminated (formaldehyde and other volatile organic chemicals from new furniture and rugs; toxic chemicals used in hobbies or gardening). A correlation may exist between symptoms and use of the fireplace. The fireplace could increase negative pressure in the house, causing backdrafting of furnace gases. The furnace is old; it may be malfunctioning or producing excessive carbon monoxide. The patient’s symptoms, including his angina attack, would be consistent with carbon monoxide poisoning.
Although the patient’s symptoms could be associated with his preexisting disease, evidence is strong enough at this point to investigate the possibility of environmental exposure. Contacting the local gas company to request that they check the furnace and stove for malfunctions and leaks would be appropriate. The fireplace should be checked for proper drafting and for deposits of creosote in the chimney.
A carboxyhemoglobin (COHb) level on the patient may confirm carbon monoxide poisoning. The patient should be advised to ventilate the
house until the furnace is checked or to stay out of the house until the gas company deems it safe. Symptoms of headaches usually do not occur below 15% COHb, but the half-life of COHb is only several hours.
A COHb level performed on this patient is reported to be 6%, which is high for a nonsmoker. The gas company discovers a cracked heating element in the 12-year-old furnace, which resulted in carbon monoxide fumes circulating throughout the house. The use of the fireplace most likely increased the backdrafting of fumes. The furnace is replaced, the exposure ceases, and the patient’s symptoms abate. He experiences no further cardiac symptoms.
|
It is not necessary to understand the jargon of a particular trade; persistent questioning by the clinician can clarify the tasks involved and reveal possible exposures. |
The exposure history form may also alert the clinician to past exposures. Most often, neither the job title nor the patient’s initial description of job duties reveals clues of exposure. It is usually helpful to have a patient describe a routine work day, as well as unusual or overtime tasks. Patients tend to use jargon when describing their jobs. It is the clinician’s challenge to persistently question the patient to elucidate possible exposures; it is not necessary to have foreknowledge of a particular trade. Start with general questions and work toward the more specific.
Page 1 of the form reveals another clue—this patient was exposed to asbestos about 30 years ago. The questioning that the clinician conducts, despite having neither knowledge of the patient’s trade nor understanding of the jargon, follows.

Clinician: You state here that you were exposed to asbestos, fiberglass, and welders’ fumes way back in ’58.
Patient: Yes, during my days as a shipwright
Clinician: Did you actually handle the asbestos?
Patient: No, the pipe laggers were the tradesmen that handled the asbestos. Oh, you might be setting a bracket or plate next to a pipe and accidentally hit the pipe and dislodge some asbestos, but otherwise, shipwrights didn’t handle it You only had asbestos where there were steamlines from the boiler carrying high-pressure steam to other units like a winch or an auxiliary motor.
Clinician: What does a shipwright do? What was a routine day for you?
Patient: There was no routine day. The shipwrights were the cream of the journeymen crop; we did everything from outfitting, to establishing the cribbing on the launching gang, to shoring. I worked on the outfitting docks. We did ship reconversions. I did a lot of work on the forepeak and hawse pipes when I wasn’t working below decks.
Clinician: What exactly were your tasks below decks?
Patient: Most transporters were converted to passenger ships after the war; there was a lot of shifting of equipment and pipes. Basically, the ships were gutted. They would be completely revamped. The shipwrights would do all the woodworking, finish work, plates, and so on. Then, when everything was in place, it would be insulated and the pipes would be lagged.
Clinician: So you worked throughout the ship? And when you finished your tasks the laggers would come in?
Patient: No, no. There might be ten different tradesmen working in an afterpeak at one time. You’d be working next to welders, flangers, pipefitters, riveters, laggers; you name it. These conversions were done round-the-clock, 7 days a week; it could take a year and a half to complete a conversion. All the tasks were being done simultaneously.
Clinician: How long would the lagging take?
Patient: The lagging could take 6 to 10 months; sometimes longer. They were constantly cutting these sections of asbestos to fit the pipes. Then they would attach the sections with a paste and wrap it with asbestos wrapping.
Clinician: Could you see the asbestos in the air?
Patient: Oh yes. Sometimes it was so thick you couldn’t see 5 feet in front of you. It was white and hung in the welders’ fumes like smog.
Clinician: Did you use any protective equipment? Masks, respirators?
Patient: No. Nobody ever said it was dangerous. We were bothered more by the fiberglass and welders’ fumes than anything. We thought
fiberglass was more dangerous because it was itchy and caused a rash. The air was blue from the welding fumes; if you worked in that for a year, you knew it was affecting you. It inspired me to go back to school and get my accounting degree. But we were blue-collar workers; we were more concerned with welders’ flash, a boom breaking, or someone getting crushed between plates than we were with asbestos.
Clinician: You worked as a shipwright for 6 years?
Patient: Yes, about that. Five of those years as an outfitter on conversions.
The dialogue in which the clinician engaged the patient neither determines whether the patient’s asbestos exposure was significant, nor does it confirm that he suffered adverse effects from the exposure. It is merely a starting point for investigation. The questioning establishes that approximately 30 years ago this patient received a possibly severe exposure to asbestos fibers for a duration of 5 or 6 years. Because quantitative data on this patient’s exposure is impossible to obtain, a qualitative description (“Sometimes it was so thick you couldn’t see 5 feet in front of you”) can facilitate assessment of the exposure when consulting with an occupational medical specialist (see Appendix). In this scenario, the disclosure should prompt the clinician to monitor the patient closely for early detection of treatable health effects from asbestos exposure. A chest X ray would be advised and pulmonary function tests should be considered. Vaccination for influenza may be warranted, depending on the results of the chest X rays. Consulting an occupational medical specialist could help determine the best way to evaluate and treat this patient.
|
An exposure history may suggest the need for periodic monitoring by alerting the clinician to a past exposure. |
In this scenario, the clinician has successfully diagnosed an illness due to an environmental toxic exposure (carbon monoxide) and has noted a significant past exposure (asbestos), which needs follow-up. Had the clinician failed to pursue an exposure history, the patient’s current illness might have been misdiagnosed, treatment might have been inappropriate, or measures might not have been implemented to prevent further carbon monoxide exposure leading to a risk of continued progression of the angina, as well as coma and death involving other household occupants.
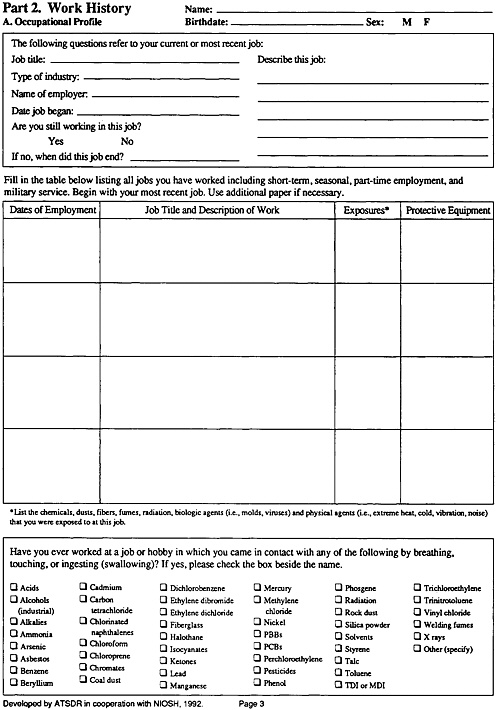
Part 2. Work History
Part 2 of the exposure history is a comprehensive inventory of the patient’s occupations, employers, and current and potential exposures in the workplace. No questions on allergies and principal symptoms have been included on the presumption that the clinician will provide more detail elsewhere in the medical record.
In evaluating Part 2 of the form, the clinician should note every job the patient had, regardless of duration. Information on part-time and temporary jobs could provide clues to toxic exposure. Details of jobs may reveal exposures unexpected from the job titles. Asking if any processes or routines have been changed recently can be helpful. Military service may have involved toxic exposure.
Scenario 2 below involves another instance of a 52-year-old male with angina as described in the case study (page 1); he suffered an angina attack and complains of recurring headaches and nausea. This patient is the owner of a commercial cleaning service. He performs some of the cleaning himself. Scanning pages 1 and 2 of the form, the clinician notes that, in his work, the patient is exposed to cleaning chemicals including detergents, ammonia, and cleansers. The patient does not notice any temporal relationship of symptoms to activity. Questioning the patient extensively about the cleaning products fails to yield any suspicious exposure possibilities. Perusal of Part 2. Work History, however, reveals another clue. The clinician’s investigation follows.
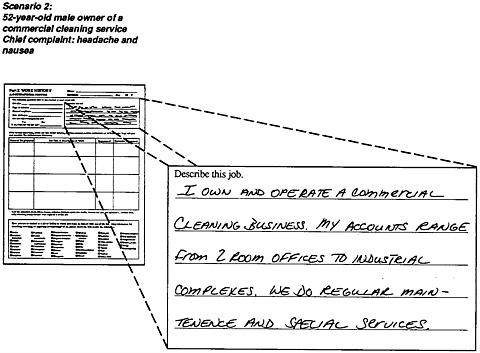
Clinician: You own a commercial cleaning service?
Patient: Yes, I’ve been in business for 10 years.
Clinician: Do you do the cleaning yourself?
Patient: I don’t do as much as I used to. I have a crew of about six full-time employees. I do more managing than cleaning but I have been known to roll up my sleeves and pitch in when need be.
Clinician: You clean residences and commercial businesses?
Patient: Yes, I have 20 residential accounts and 15 commercial accounts.
Clinician: What are the commercial accounts?
Patient: The downtown administrative offices of the school district, several realty offices downtown, and the business offices of the viscose rayon mill. I have six accounts in the Shaw Building downtown—small medical offices—and five retail stores in the Hilltop Mall.
Clinician: So your headaches have been occurring for about 3 weeks now? Have there been any changes in your routine-work or otherwise— in the last 3 weeks?
Patient: I’ve worked more hours than usual. I’ve been doing a special project for the rayon mill. They built new offices. We moved all the old offices into the new building. That has entailed cleaning and moving furniture, files, books, and exhibits. It’s been tedious. Fortunately, most of the staff has been either out on vacation or at an international conference in Europe; so the building has been empty. We’ve been able to set our own pace and come and go any day or time that suits us, so long as we clear it with security.
Clinician: Are any other workers having similar symptoms?
Patient: No, nobody else has complained about feeling sick.
Clinician: What exactly do they produce at that plant?
Patient: They make viscose-transparent paper. I used to work there during summers when I was in college. It was hot, hard work. And the whole place smelled like sulfur-rotten eggs. We used wood pulp cellulose, treated it with acids and other chemicals, and made cellulose filaments. I worked on the blending, ripening, and deaeration process.
Clinician: Can you smell the chemicals in the office building you’re working in?
Patient: Some days there’s a faint odor. Nothing like when I worked on the xanthating process. The business office building is on the northeast end of the complex. It’s pretty remote from the processing plant.
Clinician: So how many extra hours have you worked the past 3 weeks?
Patient: Only about 10 hours each week. This past weekend I put in an extra 7 hours. I had to finish setting up the exhibits. I didn’t trust the crew to handle the fragile exhibits, so I did the job myself.
Clinician: And on Sunday morning you had the angina attack. Tell me about your weekend leading up to the attack.
Patient: On Friday, I worked late setting up a huge model of the xanthating process. It was tedious work and I was sort of stressed by the time constraints to get the job done. I had broken a bottle from the exhibit when I disassembled the thing weeks ago. I was working especially carefully this time. On Saturday morning, I ran back to the plant to tie up all the loose ends and finish. In the afternoon, my wife and I spent several hours walking on the beach, despite an awful headache I had. We went to bed fairly early, about 10 PM. On Sunday morning, I had the attack. But the nitro helped almost immediately, and I had no other problems. It was pretty mild.
Clinician: What was in this bottle you broke?
Patient: I’m not sure, really. The bottle said carbon disulfide but the chemical did not smell like the carbon disulfide we used in the mill when I worked there. This stuff had a sweet odor. It was quite strong but it didn’t have the nauseating rotten-egg smell of the plant.
Clinician: How did you clean it up?
Patient: I just soaked it up with rags and threw them out. The carpet dried fairly quickly.
Clinician: Did you get any of the chemical on you?
Patient: When the bottle fell and shattered, it soaked my pant leg and the toes of my shoes. I probably got some on my hands, too, when I cleaned it up.Clinician: How much of the chemical was in the bottle? Did you report the accident to anyone at the plant?
Patient: The bottle was about a liter in size. It was full. No, I didn’t report the accident. Frankly, I’m embarrassed about it. I thought I would just talk with the manager when he returns from Europe later this week.
Clinician: What did you do with the bottle?
Patient: I put the broken pieces in a paper bag and tossed it into my truck.
Clinician: Can you get it so we can read the label?
Patient: Sure. I’ll call you as soon as possible.
The preceding conversation reveals a possible connection with the spill and this patient’s symptoms. It warrants further investigation. The results of the patient’s physical examination are normal.
The patient retrieves the broken bottle. The label on the bottle identifies the chemical—carbon disulfide—and the manufacturer. After obtaining permission from the patient, the clinician calls the manufacturer for information on carbon disulfide.
Clinician: My patient is a contract employee at a local textile company. In the process of his work he broke a bottle that was labeled carbon disulfide. He didn’t report the accident and just cleaned it up himself. I am concerned that he may be experiencing health effects from the exposure.
Manufacturer: It would not surprise me. Carbon disulfide is dangerous stuff. Strict industrial controls are in effect to prevent exposure.
Clinician: He says the chemical did not smell like the carbon disulfide he remembered working with in the plant years ago. He says it had a sweet odor.
Manufacturer: The odor of the commercial grade used in the plant is altogether different from pure carbon disulfide, which I suspect was what was in the bottle he broke. Pure-grade carbon disulfide has a sweet odor.
Clinician: Can you send me information on carbon disulfide?
Manufacturer: Certainly. I’ll send you a Material Safety Data Sheet on carbon disulfide today. I suggest that you report the accident to the safety manager at the textile plant.
The clinician receives a Material Safety Data Sheet on carbon disulfide (pages 29–30), reads the Health Hazard Data section, and discovers that this chemical can exacerbate cardiovascular disorders in persons receiving long-term exposure. Nausea and headache are among the acute effects of exposure, and primary routes of entry are inhalation and skin contact/absorption. Consultation with a toxicologist confirms that this patient’s symptoms could indeed be caused by exposure to carbon disulfide. The clinician orders a CBC, ECG, urinalysis, tests of liver and kidney function, and determinations of COHb and electrolyte levels on this patient.
Air sampling in the office in which the incident occurred reveals airborne concentrations of 0.8 parts of carbon disulfide per million parts of air (0.8 ppm). The permissible exposure limit for an 8-hour time-weighted average is 4 ppm. The concentrations were most likely higher at the time of the incident 3 weeks ago. This indicates that besides the acute exposure the patient incurred at the time of the accident, he has been chronically exposed to carbon disulfide for the previous 3 weeks, although for a limited number of hours each week while driving with the contaminated rags and bottle in his truck.
Results of the laboratory tests on this patient, including the COHb level, all are within normal limits. The patient’s exposure ceases, and he experiences no further symptoms. The clinician continues to monitor the patient’s angina, which remains stable. Other employees at risk of exposure from this spill are also examined; none incurred acute exposure or suffered ill effects. At the suggestion of the clinician, the safety manager at the mill instructs the employees in proper safety practices and no further incidents occur.
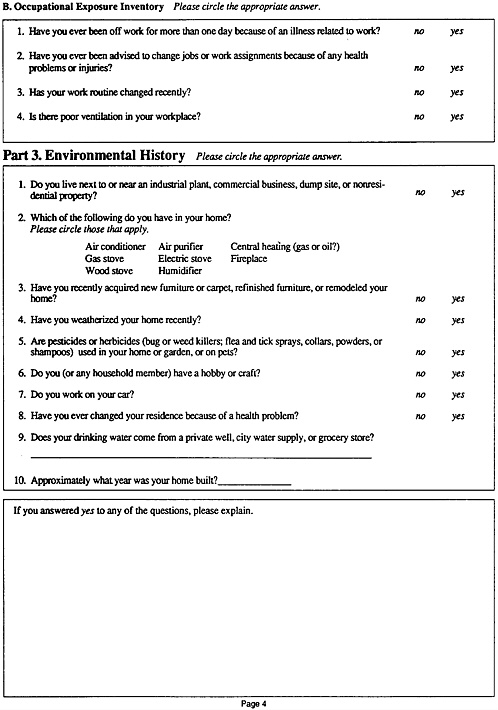
Part 3. Environmental History
Part 3 of the exposure history form contains questions regarding the home and surrounding environment of the patient. Dialogue with the patient should include queries about the location of the house, water supply, and changes in air quality.
Proximity to industrial complexes and hazardous waste sites could cause residents’ exposure to toxicants in the air, water, or soil. Community contamination is a growing public health concern; affected persons usually seek care first from their primary care providers. If a group of people with similar symptoms and exposures is identified, and an environmental exposure problem is suspected, the clinician should call the state health department or the federal Agency for Toxic Substances and Disease Registry at (404) 639–0615. (See Referral Resources, page 31, and the Appendix for more information.)
Are chemicals used in a well-ventilated place?
Is protective equipment used?
Hobbies are potential sources of toxicant exposure. For instance, model building, pottery-making, silk screening, gardening, stained-glass making, and woodworking all have been associated with hazardous exposure. Ask the patient what his or her hobbies are. All members in a household may be exposed to the hazardous substances from one person’s hobby; small children may be especially susceptible.
Scenario 3 involves another patient described in the case study (page 1). In this scenario, the patient has been retired for 2 years; he took early retirement from a stressful job in advertising shortly after being diagnosed with angina. The patient’s answers to the questions on the Exposure Survey (part 1 of the form) were no: he denies exposure to metals, chemicals, fibers, dust, radiation, and physical and biologic agents; he is not aware of a connection between his symptoms and activity or time; and to his knowledge other persons are not experiencing similar symptoms.
A clue appears on Part 3 of this patient’s exposure history-the patient lives 2 miles from an abandoned industrial site and prevailing winds blow toward his house. In an effort to investigate this lead, the clinician initiates the dialogue that follows.
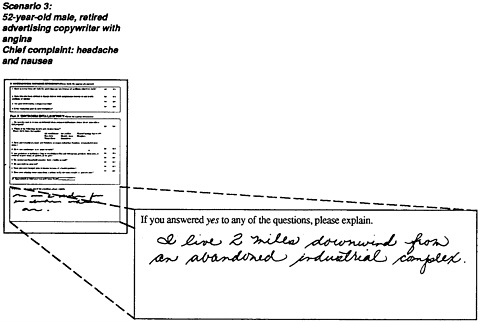
Clinician: You state that you live several miles downwind from an abandoned industrial site. Do you know what chemicals might have been used at the site or what type of industry it was?
Patient: There was a fire at the site several weeks ago. The newspaper said that they used methylene chloride to make some kind of plastics. The firefighters found drums of methylene chloride buried on the property.
Clinician: Do you ever smell chemicals in the air?
Patient: Yes, in the mornings when the wind blows from that direction, I sometimes smell a sweet odor. My neighbors have mentioned it too. In fact, they told me that the smell is really strong when they do laundry or dishes, and when they shower.
Clinician: Have you smelled it in your water?
Patient: No.
Clinician: What is the source of your water?
Patient: I have city water, but my neighbors have a private well.
Clinician: Do you know if any agency is testing your neighborhood for contamination?
Patient: Not as far as I know.
The preceding dialogue has uncovered a possibility that the patient was exposed to a toxicant. Furthermore, this patient may represent an index case; others may also be exposed. To follow up this lead, the clinician contacts the state health department. The health department confirms that the site contains buried drums of methylene chloride and that it is under investigation.
An industrial hygienist employed by the health department informs the clinician that the methylene chloride can indeed exacerbate signs and symptoms of angina. The odor threshold for the chemical is 100 to 300 parts per million (ppm). An 8-hour exposure to 250 ppm methylene chloride can cause a COHb level above 8%.
The laboratory reports that the patient’s COHb is 6%, indicating probable exposure to methylene chloride in this nonsmoker. The clinician calls the 24-hour consultation number ([404] 639–0615) of the Agency for Toxic Substances and Disease Registry (ATSDR), Emergency Response and Consultation Branch, for more information. The clinician is advised that COHb, which forms when methylene chloride metabolizes to carbon monoxide, can be detected in blood at levels of 4% to 9% when ambient air concentrations of methylene chloride are about 200 ppm. Many factors can influence body burden, including exposure level and duration, route of exposure, physical activity, and amount of body fat. A conference call with the emergency response coordinator, a toxicologist, an industrial hygienist, and a physician to
discuss the patient’s signs and symptoms ensues. The clinician is given the local Association of Occupational and Environmental Clinics (AOEC) contact, who recommends a specialist who will provide follow-up care for this patient.
Results of the health department’s tests of ambient air reveal no immediate crisis in the vicinity, although the levels are high; test results of water samples from private wells in the area are pending. ATSDR informs the regional office of the EPA of the situation. EPA provides immediate assistance to the affected area, clean-up is initiated, and threats to the surrounding population are mitigated.
Identifying Hazardous Agents
Identifying the toxicant, stopping the exposure, and arresting or reversing the progression of the patient’s illness are the goals of the exposure history. Often, patients do not know the chemicals to which they have been exposed although they may know the trade names or slang terms for the chemicals. Likewise, household products used by patients may have labeling that is inadequate for proper identification. A variety of printed reference sources are available to the clinician, including books, journals, and Material Safety Data Sheets (MSDSs). Other sources of information are described in the Appendix.
Material Safety Data Sheet
The Occupational Safety and Health Administration (OSHA) has developed a right-to-know regulation covering three basic areas: the generation and distribution of information about chemical hazards, requirements for the labeling of chemicals used in the workplace, and programs for training employees in the safe use of these chemicals. Many state and local right-to-know laws, however, are more comprehensive than the federal regulation.
The Material Safety Data Sheet (MSDS) is a component of the right-to-know law. Manufacturers and importers are required to provide an MSDS for each hazardous chemical in a shipment. Users of the chemicals must keep copies of MSDSs and make them available to workers, clinicians, or others. MSDSs contain information on the chemical properties of the substance, handling precautions, known health effects, and conditions that might worsen with exposure. The information on human health effects, however, can be vague and may have limited clinical value. The MSDS may not provide information on the synergistic effects of multiple chemical exposures. Clinical decisions should not be made solely from information obtained from MSDSs. (See MSDS, pages 29– 30.)
Additional Toxicologic Information
Books and journals provide the most accessible information on toxicologic issues. Some sources of information that the clinician can use to identify the chemicals, processes, and hazards of toxic substances are described below.
Hathaway G, Proctor NH, Hughes JP, Fischman, M, eds. Proctor and Hughes, Chemical hazards of the workplace. 3rd ed. New York: Van Nostrand Reinhold, 1991. A short text summarizing the most important occupational chemical hazards.
Sullivan JB Jr, Krieger GR, eds. Hazardous materials toxicology: clinical principles of environmental health. Baltimore: Williams & Wilkins, 1991. A complete reference including epidemiology, principles of management and evaluation of
toxic exposures, toxic hazards of specific industries and sites, and economic implications of medical and legal issues.
Gosselin RE, Smith RP, Hodge HC, eds. Clinical toxicology of commercial products. Baltimore: Williams & Wilkins, 1984. A classification of products and the chemicals they contain, including the adverse health effects produced by exposure.
Fay BA, Billings CE, eds. Index of signs and symptoms of industrial diseases. Atlanta: U.S. Dept. of Health and Human Services, Public Health Service, Centers for Disease Control, National Institute for Occupational Safety and Health, 1981. A guide to occupational and environmental diseases listed by associated clinical signs and symptoms.
Daugaard J. Symptoms and signs in occupational disease: a practical guide. Chicago: Year Book Medical Publishers, 1978. A classification of occupational and environmental diseases according to associated clinical signs and symptoms.
Rosenstock L, Cullen BR, eds. Clinical occupational medicine. Philadelphia: WB Saunders, 1986. Complete coverage of the clinical aspects of occupational medicine.
LaDou J. Occupational medicine. Norwalk, Connecticut: Appleton & Lange, 1990. Aids in the diagnosis, treatment, and remedial measures of occupational injuries and illnesses.
Last J, Wallace RB, eds. Maxcy-Rosenau-Last public health and preventive medicine. 13th ed. Norwalk, Connecticut: Appleton & Lange, 1992. Although communicable diseases continue to be the main focus of this book, increased emphasis has been placed on environmental and behavioral factors that can influence health.
Genium Publishing Corporation
1145 Catalyn Street
Schenectady, NY 12303–1836 USA
(518) 377–8854
Material Safety Data Sheets Collection:
Sheet No. 350
Carbon Disulfide
Issued 11/77 Revision: D, 3/92
|
Section 1. Material Identification Carbon Disulfide (CS2) Description: Prepared industrially by heating charcoal with vaporized sulfur or by reaction of natural petroleum fractions with sulfur. Used in manufacturing soil disinfectants, electronic vacuum tubes, viscose rayon, cellophane, flotation agents, ammonium salts and carbon tetrachloride; in insecticides, chemical analysis, electroplating, fumigation, oil extraction, dry cleaning and degreasing; and as a solvent for lipids, sulfur, rubber, oils, resin and waxes. Other Designations: CAS No. 75–15–0, carbon bisulfide, dithiocarbonic anhydride, sulphocarbonic anhydride, Weeviltox. Manufacturer: Contact your supplier or distributor. Consult latest Chemical Week Buyers’ Guide(73) for a suppliers list. Cautions: Carbon disulfide is a highly flammable, dangerous explosion hazard. It is irritating to eyes, skin, and mucous membranes, and toxic to the central nervous (CNS), peripheral nervous (PNS), and cardiovascular (CVS) systems. 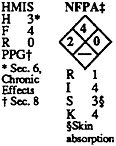 ‡The NFPA health rating of “2” is misleading due to the severity of this material’s toxicity to the CNS, CVS, and PNS and its chronic effects. A “3” is more appropriate. Section 2. Ingredients and Occupational Exposure Limits Carbon disulfide, ca 99% (major impurities are sulfur compounds) 1990 OSHA PELs (Skin) 8-hr TWA: 4 ppm (12 mg/m3) 15-min STEL: 12 ppm (36 mg/m3) 1990 NIOSH RELs TWA: 1 ppm (10 mg/m3) STEL: 10 ppm (30 mg/m3) 1990 IDLH Level 500 ppm 1991–92 ACGIH TLV (Skin) TWA: 10 ppm (31 mg/m3) 1990 DFG (Germany) MAKs TWA: 10 ppm (30 mg/m3) Peak Exposure Limit: 20 ppm/30 min /4 x/shift, momentary value Half-life: <2 hr 1985–86 Toxicity Data* Human, inhalation, TCLo: 40 mg/m3/91 weeks produced paternal effects (spermatogenesis) Human, inhalation, LCLo: 2000 ppm/5 min; no toxic effects noted Human, oral, LDLo: 14 mg/kg; toxic effects not yet reviewed Rat oral, LD50: 3188 mg/kg *See NIOSH, RTECS (FF6650000), for additional mutation, reproductive and toxicity data. Section 3. Physical Data Boiling Point: 115°F (46.5°C) Freezing Point: −168°F (−110.8°C) Vapor Pressure: 300 mm Hg at 68°F (20°C) Vapor Density (air=1): 2.64 Coefficient of Viscosity: 0.363 at 68°F (20°C) Molecular Weight: 76.13 Specific Gravity: 1.2632 at 68°F (20°C) Water Solubility: Slightly, 220 mg/100 cc water at 71.6°F (22°C) Other Solubilities: Soluble in alcohol, benzene and ether Refraction Index: 1.66232 at 77°F (25°C) Appearance and Odor: Clear, colorless to slightly yellow liquid with a sweet, chloroform-like odor when pure and a foul, rotten egg smell as the commercial product. The odor threshold is 0.1 to 0.2 ppm. Comments: From both health effect and fire/explosion perspectives, this liquid’s very high vapor pressure at room temperature indicates that airborne concentrations can build quickly to dangerous levels. Take precautions to ensure safety (Sec. 8). Section 4. Fire and Explosion Data
Extinguishing Media: Foams are more effective in carbon disulfide fires than previously believed, when water and dry chemical were the preferred extinguishing agents. Four foams tested are listed in order of increasing effectiveness: high-expansion, aqueous film-forming, fluoroprotein, and protein. If foam is unavailable, rely on carbon dioxide (CO2) or water spray. Do not scatter material with more water than necessary to put out fire. Unusual Fire or Explosion Hazards: Carbon disulfide’s burning rate is 2.7 mm/min. Vapor may travel to an ignition source and flash back. Container may explode in heat of fire. CS2 poses a vapor explosion hazard indoors, outdoors, and in sewers. Carbon disulfide can be ignited by friction, rusted or hot steam pipes, and may accumulate static electricity. Heat from an ordinary light bulb is enough to cause ignition. Special Fire-fighting Procedures: Since fire may produce toxic thermal decomposition products, wear a self-contained breathing apparatus (SCBA) with a full facepiece operated in pressure-demand or positive-pressure mode. Structural firefighters’ protective clothing is ineffective for fires involving carbon disulfide. Apply cooling water to sides of tanks until long after fire is extinguished. Stay away from ends of tanks. Immediately withdraw from area if you hear a rising sound from venting safety device or notice any tank discoloration due to fire. Be aware of runoff from fire control methods. Do not release to sewers or waterways. Section 5. Reactivity Data Stability/Polymerization: Carbon disulfide is stable at room temperature in closed containers under normal storage and handling conditions. Hazardous polymerization cannot occur. Chemical Incompatibilities: Carbon disulfide will decompose to its elements in contact with mercury fulminate. It is incompatible with alkali metals, chlorine and other halogens, nitrogen oxide, metal azides, oxidants, aluminum, ethylene diamine and zinc. Carbon disulfide reacts exothermically with phenyl copper-triphenylphosphine complexes. Conditions to Avoid: Exposure to ignition sources and contact with incompatibles. Hazardous Products of Decomposition: Thermal oxidative decomposition of carbon disulfide can produce carbon monoxide (CO), carbon dioxide (CO2), and toxic sulfur oxides (SOx) Section 6. Health Hazard Data Carcinogenicity: The IARC,(164) NTP,(142) and OSHA(164) do not list carbon disulfide as a carcinogen. Summary of Risks: CS2 enters the body primarily via the lungs (inhalation) but can be absorbed via skin. It is irritating to skin, eyes, and mucous membranes and can cause serious damage to CVS, CNS, and PNS. CS2 is cardiotoxic (toxic to heart), thrombotoxic (adversely affecting blood-clotting ability), and arrythmagenic (causing irregular heartbeat). A Parkinsonian-like effect is sometimesobserved. Exposure to 60 to 100 ppm for a short time can result in severe intoxication and death. Exposure to 5000 ppm is rapidly fatal. 70 to 90% of CS2 is metabolized, with lungs and kidney excreting the rest. Medical Conditions Aggravated by Long-Term Exposure: Coronary heart disease and CNS disorders. Target Organs: Skin, CNS, PNS, CVS, eyes, liver, kidney. |
No. 350 Carbon Disulfide 3/92
|
Section 6. Health Hazard Data, Primary Entry Routes: Inhalation and skin contact/absorption. Acute Effects: CS2 is irritating and corrosive to the eyes, skin, and mucous membranes. Introduction into eyes causes burning pain, red and swelling lids, and conjunctivitis. Skin contact with liquid may lead to burning and second- or third-degree burns. CS2 defats tissue and skin sensitization may occur. Skin absorption can result in peripheral nerve damage. Other symptoms from inhalation or skin absorption include headache, dizziness, euphoria, convulsions, nausea, vomiting, muscle weakness, and in severe cases may lead to death by respiratory failure. Chronic Effects: Chronic exposure to carbon disulfide may increase the risk of arteriosclerosis as well as cause delirium, psychosis, bad dreams leading to insomnia, CNS damage, peripheral neuropathies (abnormal and usually degenerative state of the nerves causing pain and unstimulated sensations), appetite loss, tremors, gastric disturbances, liver dysfunction, optical neuritis, and retinal hemorrhages. In women, chronic exposure to carbon disulfide can cause menstrual disorders. Spontaneous abortions and premature births are reported. FIRST AID Eyes: Gently lift eyelids and flush immediately and continuously with flooding amounts of water until transported to an emergency medical facility. Do not allow victim to rub or keep eyes tightly shut Consult a physician immediately. Skin: Quickly remove contaminated clothing. Rinse with flooding amounts of water for at least 15 min. Wash exposed area with soap and water. For reddened or blistered skin, consult a physician. Inhalation: Remove exposed person to fresh air and support breathing as needed. Ingestion: Never give anything by mouth to an unconscious or convulsing person. Contact a poison control center. Unless the poison control center advises otherwise, have that conscious and alert person drink 1 to 2 glasses of water, then induce vomiting with 1 to 2 tablespoons of Ipecac (adult dose). After patient vomits, give 2 tablespoons activated charcoal in 8 oz. of water to drink. After first aid, get appropriate in-plant, paramedic, or community medical support. Note to Physicians: Since effects may be delayed, keep victim under observation. The iodine-azide test is useful in detecting degree of exposure and hypersusceptibility of exposed workers. I.V. urea 0.5 to 1.5 g/kg is recommended to inactivate free carbon disulfide in the blood. Vitamin B6 in large doses is recommended. Obtain CBC, EKG, urinalysis, and electrolyte balance. Section 7. Spill, Leak, and Disposal Procedures Spill/Leak: Plan and design appropriate emergency-response procedures prior to carbon disulfide spills or leaks. Immediately notify safety personnel, isolate area, deny entry and stay upwind. Shut off all ignition sources. Cleanup personnel should wear fully encapsulating, vapor-protective clothing to protect against contamination. If possible, detoxify material before cleanup. For small spills, take up with earth, sand, vermiculite or other absorbent, noncombustible material and place in clean, dry containers with a secure lid for later disposal. For large spills, flush liquid to a special retention basin where it can collect under a layer of water (to prevent ignition or explosion) for disposal or reclamation. Perform all cleanup operations with nonsparking tools. Follow applicable OSHA regulations (29 CFR 1910.120). Environmental Transport: If released to water, carbon disulfide should volatilize with a half-life of 2.6 hr (according to model river plan) and should not bioconcentrate significantly in aquatic organisms. In the atmosphere, CS2 reacts with atomic oxygen and photochemically produced hydroxyl radicals with a half-life of 9 days. Environmental Toxicity Values: Sunfish, LC100, 100 µg/L/hr; trout, LC100, 500 µg/L/0.1 hr. Soil Absorption/Mobility: Carbon disulfide is highly mobile and volatilizes or leaches into soil. Disposal: Large amounts of CS2 may be distilled for reclamation and packaged for reuse. Contact your supplier or a licensed contractor for detailed recommendations. Follow applicable Federal, state, and local regulations. EPA Designations Listed as a RCRA Hazardous Waste (40 CFR 261.33): No. P022 Listed as a CERCLA Hazardous Substance* (40 CFR 302.4): Reportable Quantity (RQ), 100 lb (45.4 kg) [* per RCRA, Sec. 3001 and CWA 311(b)(4)] Listed as a SARA Extremely Hazardous Substance (40 CFR 355) Listed as a SARA Toxic Chemical (40 CFR 372.65) OSHA Designations Listed as an Air Contaminant (29 CFR 1910.1000, Table Z-1-A) Section 8. Special Protection Data Goggles: Wear protective eyeglasses or chemical safety goggles, per OSHA eye- and face-protection regulations (29 CFR 1910.133). Because contact lens use in industry is controversial, establish your own policy. Respirator: Seek professional advice prior to respirator selection and use. Follow OSHA respirator regulations (29 CFR 1910.134) and, if necessary, wear a MSHA/NIOSH-approved respirator. Select respirator based on its suitability to provide adequate worker protection forgiven working conditions, level of airborne contamination, and presence of sufficient oxygen. For 10 ppm, use any chemical cartridge respirator with organic vapor cartridges. For 50 ppm, air-purifying respirator with organic vapor cartridges and a full facepiece. For emergency or nonroutine operations (cleaning spills, reactor vessels, or storage tanks), wear an SCBA. Warning! Air-purifying respirators do not protect workers in oxygen-deficient atmospheres. If respirators are used, OSHA requires a respiratory protection program that includes at least: training, fit-testing, periodic environmental monitoring, maintenance, inspection, cleaning, and convenient, sanitary storage areas. Other: Wear chemically protective gloves, boots, aprons, and gauntlets to prevent all skin contact. Suggested materials for protective clothing include polyvinyl alcohol (PVA) and polyethylene with breakthrough times of 8 and 4 hr, respectively. Ventilation: Provide general and local explosion-proof exhaust ventilation systems to maintain airborne concentrations below the OSHA PEL (Sec. 2). Local explosion-proof exhaust ventilation is preferred because it prevents contaminant dispersion into the work area by controlling it at its source.(103)Safety Stations: Make available in the work area emergency eyewash stations, safety/quick-drench showers, and washing facilities. Contaminated Equipment: Separate contaminated work clothes from street clothes. Launder contaminated work clothing before wearing. Remove this material from your shoes and clean personal protective equipment. Comments: Never eat, drink, or smoke in work areas. Practice good personal hygiene after using this material, especially before eating, drinking, smoking, using the toilet, or applying cosmetics. Section 9. Special Precautions and Comments Storage Requirements: Protect containers from physical damage. Store in iron, glass, porcelain or steel containers. Keep small quantities in cool, dry, well-ventilated area away from incompatibles (Sec. 5). Store large quantities in tanks; add water or inert gas (such as nitrogen) to fill emptying tanks. Submerge tanks in water or locate them above concrete basins large enough to hold the tanks’ contents. Equip storage facilities with automatic sprinklers and test regularly. Outside or detached storage is preferred. Engineering Controls: To reduce potential health hazards, use sufficient dilution or local exhaust ventilation to control airborne contaminants and to maintain concentrations at the lowest practical level. To prevent static sparks, electrically ground all system parts including piping, valves, and moveable containers. Prohibit electrical installations and heating facilities in or near storage areas. Never transfer carbon disulfide by means of air pressure; use pump, water, or inert gas. Use wooden sticks (no spark potential) to measure the contents of CS2 tanks and containers. Administrative Controls: Consider preplacement and periodic medical exams of exposed workers that emphasize eyes, skin, CNS, PNS, CVS, and reproductive system, and perform electrocardiograms. Transportation Data (49 CFR 172.101, .102) DOT Shipping Name: Carbon bisulfide or Carbon disulfide DOT Hazard Class: Flammable liquid ID No.: UN1131 DOT Label: Flammable liquid DOT Packaging Exceptions: None DOT Packaging Requirements: 173.121 IMO Shipping Name: Carbon disulphide IMO Hazard Class: 3.1 ID No.: UN1131 IMO Label: Flammable liquid, Poison IMDG Packaging Group: I MSDS Collection References: 26, 38, 73, 89, 100, 101, 103, 124, 126, 127, 132, 136, 140, 149, 153, 159, 162, 163, 164 Prepared by: M Gannon, BA; Industrial Hygiene Review: DJ Wilson, CIH, Medical Review: AC Darlington, MPH, MD; Edited by: JR Stuart, MS |
Summary and Follow-up
In each scenario, the clinician’s pursuit of the exposure history led to discovery of toxic exposure for each of the three patients. In each case, the diagnosis and treatment might have been inappropriate without an exposure history. The process required only a few minutes of the clinician’s time; each history was focused as indicated by the patient’s reported symptoms. Using the exposure history in managing the patients’ problems, as well as guiding the patients in appropriate preventive behaviors, is the practice of preventive medicine at its best.
Consultation
Industrial hygienists, who are often employed by state health departments or industry, are a source of information to the clinician investigating a possible toxic exposure. Industrial hygiene is the discipline devoted to the recognition, evaluation, and control of workplace-related factors or stresses that may cause illness, impaired health or well-being, or significant discomfort and inefficiency among workers or community members. Other medical specialists, such as clinicians specializing in occupational/environmental and general preventive medicine, can be helpful in assessing whether a significant exposure has occurred. Occupational health nurses, who often work at patients’ worksites, also have expertise and experience that may be valuable to the clinician.
Referral Resources
The clinician is encouraged to build a network of occupational and environmental medical specialists for information, consultation, and referral. The Association of Occupational and Environmental Clinics (AOEC) is a network of clinics that provide professional training, community education, exposure and risk assessment, clinical evaluations, and consultative services. Educational Resource Centers (ERCs) have been established in academic centers by the National Institute for Occupational Safety and Health (NIOSH) to educate professionals in occupational medicine topics. ERCs offer training courses in occupational and environmental medicine topics; continuing medical education credit is available. Other resources, including poison control centers and government agencies, are listed and described in the Appendix, pages 39–56.
Suggested Reading List
Bresnitz EA, Rest KM, Miller N. Clinical industrial toxicology: an approach to information retrieval. Ann Intern Med 1985;103(6 pt 1):967–72.
Coye MJ, Rosenstock L. The occupational health history in a family practice setting. Am Fam Physician 1983;28(5):229–34.
Environmental Protection Agency and Consumer Safety Commission. The inside story: a guide to indoor air quality. Washington, DC: Environmental Protection Agency, September 1988.
Goldman RH, Peters JM. The occupational and environmental health history. JAMA 1981;246:2831–6.
Levy BS, Wegman DH, eds. Occupational health: recognizing and preventing work-related disease. 2nd ed. Boston: Little, Brown & Company, 1988.
Mayer JL, Balk SJ. A pediatrician’s guide to environmental toxins. Contemporary Pediatrics 1988; Part 1:5(7):22– 40; Part 2:5(8):63–76.
National Research Council. Environmental tobacco smoke: measuring exposure and assessing health effects. Washington, DC: National Academy Press, 1986.
Rogan WJ. The sources and routes of childhood chemical exposures. J Pediatr 1980;97:861.
Rom WN, ed. Environmental and occupational medicine. 2nd ed. Boston: Little, Brown & Company, 1992.
The Western Journal of Medicine. December 1982. Entire issue devoted to occupational and environmental medicine.
Zenz C, ed. Developments in occupational medicine. Chicago: Mosby Year Book Medical Publishers, 1980.
Zenz C, ed. Occupational medicine: principles and practical applications. 2nd ed. Chicago: Mosby Year Book Medical Publishers, 1988. Third edition due for release in April 1993.
Sources of Information
More information on taking an exposure history can be obtained from ATSDR, your state and local health departments, and university medical centers. Case Studies in Environmental Medicine: Taking an Exposure History is one of a series. For other publications in this series, please use the order form on page 38. For clinical inquiries, contact ATSDR, Division of Health Education, Office of the Director, at (404) 639–6204.
Answers to Pretest
Pretest questions are on page 1.
-
The patient’s problem list includes recurrent headache and nausea, and unstable angina pectoris.
-
The patient’s differential diagnosis of chest pain includes myocardial infarction. The differential diagnosis of headache and nausea includes viral syndrome, tension headaches, migraine, brain tumor, tooth or sinus problems, psychogenic headache, medication reaction (nitroglycerin can cause headaches), and exposure to toxicants.
-
The additional information sought to make a diagnosis would include all aspects of a work and exposure history.








































