
12 Polychlorinated Biphenyl (PCB) Toxicity
|
Environmental ALERT…
|
This monograph is one in a series of self-instructional publications designed to increase the primary care provider’s knowledge of hazardous substances in the environment and to aid in the evaluation of potentially exposed patients. The Agency for Toxic Substances and Disease Registry (ATSDR) and the Centers for Disease Control (CDC) designate this continuing medical education activity for 1 credit hour in Category 1 of the Physician’s Recognition Award of the American Medical Association and 0.1 continuing education units for other health professionals. See pages 17 to 19 for further information.
|
Guest Contributors: |
Roger Wabeke, CIH; Richard Weinstein, MD, MPH |
|
Guest Editor: |
Gideon Letz, MD |
|
Peer Reviewers: |
Charles Becker, MD; Jonathan Borak, MD; Joseph Cannella, MD; Bernard Goldstein, MD; Alan Hall, MD; Richard J.Jackson, MD, MPH; Jonathan Rodnick, MD; Robert Wheater, MS; Brian Wummer, MD |

U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES
Public Health Service
Agency for Toxic Substances and Disease Registry
Case Study
A 48-year-old handyman with progressive cystic acne and abnormal liver function
You have been treating a 48-year-old man conservatively for his facial acne vulgaris. He first sought treatment about 3 months ago, remarking that such blemishes are typical for a teenager but he never had them during adolescence. Therapy was initiated with benzoyl peroxide washes and topical antibiotics, in addition to instructions for skin hygiene. When no real improvement was noted, oral antibiotics were prescribed. Due to continued lack of efficacy, this regimen was later supplemented by Retin-A™* (tretinoin) cream.
The patient has returned for a follow-up visit and complains that the acne is worse. On examination, you agree, and tell the patient you would like to refer him to a dermatologist for Accutane™* (isotretinoin) therapy. A serum biochemical and hematologic profile are ordered to document baseline values before therapy begins.
To your surprise, the biochemical panel reveals the following abnormalities: total bilirubin 2.8 mg/dL (normal 0–1.5), direct bilirubin 0.4 mg/dL (normal 0–0.4), SGPT (ALT) 74 IU/L (normal 0–50), SGOT (AST) 88 IU/L (normal 0–50), GGPT (GGT) 190 IU/L (normal 15–85), LDH 230 IU/L (normal 50–225). Other testing, including complete blood count, alkaline phosphatase, BUN, creatinine, and urinalysis are within normal limits.
On questioning, the patient denies history of hepatitis, contact with hepatitis patients, other liver difficulties or blood transfusion. He informs you he has Gilbert’s syndrome and has had elevated bilirubin levels in the past. There is no family history of cardiovascular disease or cancer. The patient does not smoke; he drinks 2 to 3 bottles of beer each evening, and sometimes more on weekends. He is currently taking no medications other than those mentioned. Review of systems is otherwise unremarkable.
Social history reveals the patient is married with three teenaged children; his wife and children are in good health. They live in a high-rise apartment building where the patient has been handyman and part-time building manager for the last year. He spends much time in the basement area, which includes a workshop, recreation room with pool table, and laundry and heating facilities. An avid fisherman, he spends most weekends fishing in Lake Michigan with his two sons. Physical examination reveals mild, nontender hepatomegaly without jaundice. His acne, which is most prominent on the upper face lateral to the eyebrows, began about 8 months ago.
|
* |
Use of trade names is for identification only and does not imply endorsement by the Public Health Service or the U.S. Department of Health and Human Services. |
![]()
(a) What should be included in the patient’s problem list?
_________________________________________________________________
(b) What is a differential diagnosis for the patient’s altered liver enzymes?
_________________________________________________________________
(c) What tests would be useful in helping you arrive at a diagnosis?
_________________________________________________________________
Answers to the Pretest can be found on page 15.
Exposure Pathways
❑ PCBs persist in the environment, concentrating upward in the food chain.
❑ The primary nonoccupational source of PCB exposure is food, especially fish from contaminated water.
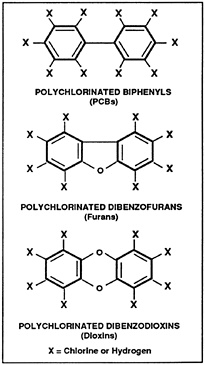
Polychlorinated biphenyls (PCBs) are a family of 209 chemicals with varying numbers of chlorine atoms attached in varying positions to two connected benzene rings (Figure 1). Commercial PCB products are always mixtures of PCBs and are usually contaminated with small amounts of polychlorinated dibenzofurans (furans) or polychlorinated dibenzodioxins (dioxins). Contamination by furans is a concern because their toxicity is generally much greater than that of PCBs.
Figure 1. Polychlorinated biphenyls and related compounds
Because of their insulating and nonflammable properties, PCBs have been used as heat exchange and dielectric fluids in transformers and capacitors, hydraulic and lubricating fluids, diffusion pump oils, plasticizers, extenders for pesticides, and as ingredients of caulking compounds, paints, adhesives, and flame retardants. PCBs have also been used in inks and carbonless paper. Trade names for PCBs include Aroclor, Askarel, Eucarel, Pyranol, Dykanol, Clorphen, Asbestol, Diaclor, Nepolin, and EEC-18.*
PCB mixtures are colorless to dark brown oils, viscous liquids, or sticky resinous semi-solids. They evaporate slowly at room temperature; however, their volatility increases dramatically with small increases in temperature. Overheated equipment that contains PCBs can vaporize significant quantities of these compounds, causing an inhalation hazard, especially in areas where ventilation is poor.
Today PCBs are found mainly in transformers and capacitors manufactured before the U.S. Environmental Protection Agency (EPA) banned the production of PCBs in 1977. Many of these old transformers and capacitors are still contained in industrial equipment (such as welding equipment), medical equipment (such as X-ray machines), and household appliances (such as refrigerators). Ballasts of fluorescent light fixtures may contain PCBs. During normal lighting operation, the PCBs are entirely enclosed; however, when the capacitor wears out, it may burn or break and leak PCBs.
PCBs can be released into the general environment from poorly maintained toxic waste sites; by illegal or improper dumping of PCB wastes, such as transformer fluids; through leaks or fugitive emissions from electrical transformers containing PCBs; and by disposal of PCB-containing consumer products in municipal landfills. PCBs have been found in at least 271 of 1177 hazardous waste sites on the EPA National Priorities List. Of the 1.25 billion pounds of PCBs produced in this country since 1929, about 450 million pounds have found their way into the environment. The chemical stability of these synthetic compounds accounts for their persistence in the environment. Another important reason for their persistence is their resistance to biodegradation.
Low levels of PCBs can be found throughout the world. PCBs in water or on soil surfaces evaporate and return to earth by rainfall or settling of dust particles. Because PCBs strongly adsorb to soil particles, significant leaching from soil and translocation to plants do not occur. Although PCBs are widespread in the
aquatic environment, their low water solubility helps to prevent high concentrations in drinking water supplies.
Food can be a major source of PCB exposure, usually from fish and animal fat. PCBs are lipophilic; they preferentially separate from water and adsorb to sediment. Bottom feeders and other aquatic organisms then ingest and accumulate PCBs, resulting in bioconcentration upward in the food chain. Composite analysis of commercial whole fish collected from Lake Ontario in 1980 found PCB levels of 0.11 to 4.90 parts per million (ppm).
The toxicity of PCBs was dramatically illustrated in 1968 when over 1600 people in Japan were poisoned by cooking oil contaminated with PCBs from a heat transfer unit. The contaminating oil likely contained furans and dioxins, compounds generally more toxic than PCBs themselves. The ensuing illnesses became known as “Yusho” (rice oil disease).
|
(1) Additional information for the case study: In response to your persistent, detailed questioning regarding his hobbies and possible contact with hepatotoxins, the patient reveals that while in the basement workshop he frequently wipes up a “dark, oily discharge” near a large electrical transformer in the work area. The discharge has also resulted in a gummy residue on tools and other surfaces. He mentions he sometimes feels dizzy and nauseated after working in the basement all day. Is there an association between the clinical findings and this additional information? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Who’s at Risk
❑ Certain workers can be exposed to PCBs during repair of equipment and accidents or spills.
❑ Fetuses and neonates may be more sensitive to PCBs than adults; nursing infants are at increased risk of exposure from PCB-exposed mothers.
❑ Persons with compromised hepatic function may metabolize PCBs less efficiently than healthy persons.
Although PCBs are no longer manufactured in the United States, the greatest potential for exposure to PCBs still occurs in the workplace. For example, workers may inhale or have dermal contact with PCBs during repair or maintenance of process equipment or electrical transformers and during accidents or spills involving PCBs. Exposure can also occur in disposal of PCB-containing materials at hazardous waste sites. Occupations entailing risk of PCB exposure include, but are not limited to, the following:
electric cable repair
electroplating
emergency response
firefighting
hazardous waste hauling/site operating
heat exchange equipment repair
maintenance cleaning
metal finishing
paving and roofing
pipefitting/plumbing
timber products manufacturing
transformer/capacitor repair
waste oil processing
Nonoccupational exposures have also occurred. The public has encountered PCBs through illegal roadside dumping of hazardous waste oils and through inhalation of smoke and soot from transformer or capacitor fires. Pyrolysis of PCBs can produce dioxins and furans, placing smoke-inhalation victims at increased risk of exposure to these toxic compounds.
Fetuses and neonates are potentially more sensitive to PCBs than adults because of transplacental distribution and physiologic differences. They lack the hepatic microsomal enzyme systems that facilitate metabolism and excretion of PCBs. Furthermore, PCBs accumulate in breast milk. Nursing infants are at additional risk because human milk contains a steroid that inhibits PCB glucuronidation and excretion.
Other populations potentially more sensitive to PCBs are persons with compromised hepatic functioning, including those with incompletely developed glucuronide conjugation mechanisms due to congenital disorders such as Gilbert’s syndrome, and persons with hepatic infections. Persons taking medications potentially toxic to the liver may also be at increased risk.
|
(2) Are other sources of PCB exposure likely for the patient described in the case study? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Biologic Fate
❑ PCBs are stored in lipid tissues.
❑ The liver is the primary site of PCB metabolism.
❑ The slow metabolism of PCBs leads to bioaccumulation.
PCBs are readily absorbed into the body but slowly metabolized and excreted. After absorption, PCBs partition between the aqueous and lipid compartments of the body in a biphasic pattern. During the first day after PCBs were administered to laboratory animals, they were distributed mainly to the liver and muscle tissue. In a second phase, PCBs were redistributed to the adipose tissue, skin and other fat-containing organs. More highly chlorinated PCBs redistribute to adipose tissue to a greater extent than do PCBs with a lower percentage of chlorine; the presence of more highly chlorinated PCBs appears to delay excretion of the lesser chlorinated compounds for reasons not clearly understood.
The liver is the primary site of PCB metabolism by hydroxylation and conjugation with glucuronic acid and sulfates. The rate of metabolism depends on the number and position of chlorine atoms, with lesser chlorinated isomers being more readily metabolized.
Excretion of PCBs is slow, so bioaccumulation occurs even at low exposure levels. As long as exposure continues, a true steady state is never achieved. PCBs metabolized with more difficulty are excreted almost exclusively by the biliary route; metabolites of PCBs with a smaller percentage of chlorination are eliminated through bile and urine. Urinary metabolites are in the form of conjugates, including glucuronides and sulfates.
There are essentially no pharmacokinetic data for humans. PCB half-lives in the rat range from 1 day to 460 days depending on the degree of chlorination.
Background levels in human sera are typically less than 20 parts per billion (ppb), and residues measured in human milk have ranged from 40 to 100 ppb. Reported levels in adipose tissue range from 1 to 2 ppm.
|
(3) Explain why patients with Gilbert’s syndrome may be at increased risk of adverse effects due to PCB exposure. _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Physiologic Effects
❑ PCBs have low potential to cause acute effects.
❑ EPA considers PCBs to be probable human carcinogens.
In humans, PCB toxicity affects the skin and liver, and may have developmental effects. Metabolic, reproductive, endocrine, and immunosuppressive effects have been noted in animals, but have not been adequately studied in humans. Although data from animal studies indicate that PCBs are definitely animal carcinogens, data from PCB-exposed human populations are inconsistent and inconclusive.
Dermatologic Effects
❑ PCB-induced chloracne can reflect systemic toxicity.
Chloracne is the only overt effect of PCB exposure in humans, but absence of chloracne does not rule out exposure. There is no reliable dose-response model for chloracne in exposed populations; the dose-response relationship may be dependent upon individual predisposition. Chloracne typically develops weeks or months after exposure. The lesions are often refractory to treatment and can last for years. One case persisted for more than 30 years.
The acneform lesions arise from altered differentiation of acinar sebaceous base cells into keratinocytes. The chin, periorbital, and malar areas are affected most often, although lesions may
also appear on the chest, arms, thighs, genitalia, and buttocks-areas not commonly affected by acne vulgaris. The most distinctive lesions are cystic and measure from 1 to 10 millimeters (mm). Other prominent lesions are comedo. The cysts and comedones can become inflamed and secondarily infected. The papules and cysts may be surrounded by edema and erythema. Chloracne may result not only from dermal contact but also from ingestion and generally indicates systemic toxicity.
Besides chloracne, Yusho patients had hyperpigmentation of the skin, conjunctiva, gingiva, and nails. These pigmentation disturbances have also been noted in some PCB-exposed workers.
Hepatic Effects
❑ High-level PCB exposure may produce elevated levels of liver enzymes.
❑ Evidence suggests that PCBs cause hepatotoxicity in humans.
Epidemiologic studies and clinical surveys indicate that severe occupational exposure to PCBs can increase serum liver enzymes. The enzyme levels often show inconsistent patterns, however, and increases generally have not been associated with hepatic dysfunction, although approximately 10% of the Yusho patients experienced jaundice. Asymptomatic hepatomegaly has been reported in workers, many of whom had concomitant elevated serum PCB levels. Some researchers believe that aspartate aminotransferase (SGOT or AST) and gamma glutamyl transpeptidase (GGTP or GGT) are the most sensitive indicators of PCB exposure in humans, and that changes in these liver enzymes may occur at exposure levels below those at which chloracne appears. Liver damage, histologically documented, is the most consistent finding among laboratory animals tested with PCBs.
Increases in urinary porphyrin levels have been noted in a study of workers with low-level PCB exposure. Changes in porphyrin metabolism may be triggered by the induction of liver microsomal enzymes. PCBs are more potent enzyme inducers than phenobarbital, a drug that occasionally causes clinical problems due to its enzyme-inducing effects, and PCBs’ enzyme-inducing effects can persist long after cessation of exposure. The health implications for enzyme induction include the occurrence of disease secondary to increased metabolism of endogenous or exogenous substances, and interference in medical therapy due to increased metabolism of administered drugs.
Reproductive and Developmental Effects
❑ PCBs have a potential to cause developmental and fetotoxic effects in humans.
The Yusho incident documents PCBs’ potential to cause developmental and fetotoxic effects in humans. Two of the Yusho mothers had stillbirths; 10 of 13 infants had abnormal skin pigmentation, 9 of 13 had ocular discharge, and 12 of 13 were smaller than average. Two infants developed Yusho from breast feeding. In contrast, the authors of a study of nursing infants whose mothers were occupationally exposed to PCBs found no adverse health effects. Contaminants in the PCB oil cannot be ruled out as factors in Yusho disease. Follow-up of the Yusho infants revealed no persistent morphologic or behavioral abnormalities.
In laboratory animals, changes in estrous cycles, failure of ovum implantation, increased frequency of spontaneous abortions, and low birth weight of offspring have been reported after PCB exposure. No teratogenic effects have been reported in studies of humans or animals.
Carcinogenicity
❑ PCBs are considered potential human carcinogens on the basis of results from animal studies.
The epidemiologic evidence is insufficient to evaluate the potential of PCBs as human carcinogens. Although Yusho victims showed a slightly higher rate of deaths from neoplasms 15 years after the incident, the data were not adjusted for age or smoking and drinking patterns. Cancer data from other human populations are inconsistent and inconclusive.
Data from animal studies have shown that PCBs cause hepatocarcinomas, pituitary tumors, leukemia, lymphomas, and gastrointestinal tract tumors. On the basis of these data, EPA considers PCBs to be probable human carcinogens.
|
(4) Is there a need to be concerned about PCB exposure when the clinical effects of the patient in the case study seem so limited? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Clinical Evaluation
History and Physical Examination
A detailed history will facilitate the diagnosis of chronic PCB poisoning. Pertinent information includes occupational histories of all household members, medications, and diet, including ethanol intake. During the physical examination, physicians should pay particular attention to the skin and hepatic system. Encountering a patient with PCB toxicity should trigger consideration of whether this is a sentinel event, indicating the possibility of other similarly exposed persons such as coworkers or family members.
Signs and Symptoms
Acute Exposure
❑ Chloracne is the only known overt sign of PCB toxicity; however, absence of chloracne does not rule out exposure.
PCBs have very low potential for producing acute toxic effects. The only overt sign of PCB exposure is chloracne, which is described on page 7. Acneform lesions do not appear in all severely exposed patients (only 82% of Yusho patients had chloracne); therefore, its absence does not rule out exposure. New cases of chloracne should be reported to the local or state health department.
Elevated liver enzymes are the most sensitive effect of PCB exposure in animals and have been detected in several human epidemiologic studies. Hepatomegaly has also been noted in some PCB-exposed workers.
Chronic Exposure
❑ Because of an EPA ban on PCB production in 1977, chronic exposure in the workplace is uncommon today.
Many people chronically exposed to PCBs have had no overt signs or symptoms of toxicity. In others, reported signs and symptoms of exposure with hepatic involvement have included weight loss, anorexia, nausea, vomiting, jaundice, and abdominal pain. The degree of liver injury was related to the degree of chlorination in the PCBs, dose and duration of exposure, and possible concurrent exposure to other hepatotoxins, infectious agents, or certain medications. Headache, dizziness, and edema have also been reported. Chronic PCB exposure in the workplace is unlikely to occur today.
Laboratory Tests
Direct Biologic Indicators
❑ Serum or adipose tissue PCB levels may indicate exposure, but they are difficult to interpret clinically.
Some researchers believe that PCB blood levels after long-term exposure correlate well with adipose tissue levels. However, PCB analysis of either blood or adipose tissue is expensive and time-consuming and is not recommended unless exposure has been massive. Breast milk analysis for PCBs should not be considered unless the exposure is severe. PCBs detected in breast milk are not necessarily an indication that breast-feeding should be stopped.
Indirect Biologic Indicators
❑ Elevated liver-enzyme levels are of limited value in diagnosing PCB exposure.
Liver function tests may be the most sensitive sign of PCB toxicity in the absence of chloracne; however, these measures are of questionable value because they are nonspecific. Also, normal liver enzyme values do not rule out significant exposure; body burden still may be elevated. PCB conjugates can often be detected in urine after exposure. Their analysis is expensive, unreliable, and not recommended.
|
(5) What confirmatory laboratory test can be ordered to establish the diagnosis of PCB exposure? _________________________________________________________________ (6) Additional information for the case study: The patient requests a serum PCB analysis. The laboratory reports a level of 125 ppb, with no normal range indicated. How will you interpret this report? _________________________________________________________________ _________________________________________________________________ |
Treatment and Management
Acute Exposure
❑ There is no antidote for PCB exposure; treatment is symptomatic.
In the event of PCB splashes in the eyes, irrigate with tepid water immediately for at least 15 minutes, and follow with ophthalmic evaluation. Remove contaminated clothing and discard properly. Gently wash affected skin with soap and warm water for at least 15 minutes.
In the rare event that PCB-containing substances are ingested, induce vomiting immediately if the patient is conscious. Gastric lavage may be subsequently administered at a medical facility until the gastric washings are clear. Activated charcoal has not been proven beneficial, but is not contraindicated. Exposed persons should have periodic follow-up examinations with particular attention to hepatic function and dermal lesions.
Chronic Exposure
❑ Removal from the source is the goal of treatment for PCB exposure.
There is no specific treatment for PCB toxicity. Diagnostic workup should be limited to liver function tests and dermatologic examination, with skin biopsy of lesions. Initial treatment of chloracne is based on cessation of exposure, good skin hygiene, and use of dermatologic measures commonly employed for acne vulgaris. If these measures are not efficacious, the patient should be referred to a dermatologist.
The carcinogenic potential of PCBs should be carefully reviewed with the patient, primarily to allay anxiety. Since there are no known methods of reducing reserves of PCBs in lipid tissues, attempts to purge the body of PCBs should not be undertaken. Saunas and nutritional therapies have no proven efficacy. Crash diets risk mobilizing PCBs stored in fat.
Since PCBs are hepatotoxins, history of exposure to other potentially hepatotoxic agents should be obtained and patients should be encouraged to avoid exposure to other hepatotoxins such as antibiotics or medications with known hepatotoxicity, alcohol, and chlorinated solvents.
|
(7) What steps should be recommended to patients when PCB-related health effects are suspected? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Standards and Regulations
Workplace
Air
❑ OSHA’s PEL is 1000 µg/m3for PCBs containing no more than 42% chlorine, and 500 µg/m3for compounds containing up to 54% chlorine.
The Occupational Safety and Health Administration’s (OSHA) permissible exposure limit (PEL) is a time-weighted average (TWA) airborne concentration of 1000 µg/m3 for PCBs containing 42% chlorine (average molecular formula of C12H7Cl3). PCBs with 54% chlorine and an average molecular formula of C12H5Cl5 have a PEL of 500 µg/m3. Both standards encompass all physical forms: aerosols, vapor, mist, sprays, and PCB-laden dust particles. OSHA considers that PCBs are absorbed through intact skin; therefore, dermal as well as inhalation exposure routes, should be evaluated by an industrial hygienist.
The National Institute for Occupational Safety and Health (NIOSH) recommends a ten-hour TWA of 1 µg/m3 based on the minimum reliable detectable concentration and potential carcinogenicity of PCBs. NIOSH also recommends that all workplace exposures be reduced to the lowest feasible level.
Environment
Water
❑ EPA does not have a standard for PCBs in drinking water.
EPA considers PCBs a probable human carcinogen and prohibits industrial discharges under the Clean Water Act Effluent Guidelines. Currently, there is no legal maximum contaminant level for PCBs in drinking water. However, EPA advises that the
level of PCBs in drinking water be limited to 0.5 µg/L on the basis of carcinogenicity at 10−4 to 10−6 risk levels.
Food
The Food and Drug Administration (FDA) mandates tolerances of 0.2 to 3.0 ppm PCBs for all foods, with a tolerance level in fish of 2 ppm. FDA also limits PCBs in plastic food-packaging materials to 10 ppm.
|
(8) What regulatory steps should be taken for the situation described in the case study? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Suggested Reading List
Clinical
Kimbrough RD. Human health effects of polychlorinated biphenyls (PCBs) and polybrominated biphenyls (PBBs). Annu Rev Pharmacol Toxicol 1987;27:87.
Letz G. The toxicology of PCBs—an overview for clinicians. West J Med 1983;138:534–40.
McKenna JP, Moskovitz M, Cox JL. Abnormal liver function tests in asymptomatic patients. Am Fam Physician 1989;39(3):117–26.
Epidemiology
Acquavella JF, Hanis NM, Nicolich MJ, Phillips SC. Assessment of clinical, metabolic, dietary, and occupational correlations with serum polychlorinated biphenyl levels among employees at an electrical capacitor manufacturing plant. J Occup Med 1986;28(11):1177–80.
Fischbein A, Wolff MS, Bernstein J, Selikoff IJ. Dermatological findings in capacitor manufacturing workers exposed to dielectric fluids containing polychlorinated biphenyls (PCBs). Arch Environ Health 1982;37(2):69–74.
Weaver G. PCB contamination in and around New Bedford, Mass. Environmental Science Technology 1983;18:22A–7A.
Toxicology
Fischbein L. Toxicology of chlorinated biphenyls. Annu Rev Pharmacol 1974. 14:139–56.
IARC (International Agency for Research on Cancer). IARC monographs on the evaluation of the carcinogenic risk of chemicals to humans. Lyon, France: World Health Organization, 1982.
Related Government Documents
Agency for Toxic Substances and Disease Registry. Toxicological profile for selected PCBs. Atlanta: US Department of Health and Human Services, Public Health Service, 1989. NTIS report no. PB/89/225403/ AS.
Environmental Protection Agency. Drinking water criteria document for polychlorinated biphenyls (PCBs). Washington, DC: US Environmental Protection Agency, 1988. EPA report no. ECAO-CIN-414.
Answers to Questions
Pretest
The pretest can be found on page 1.
-
The patient’s problem list includes acne vulgaris, which is atypical because of the location of the lesions and their late onset without history of outbreaks during adolescence. The mildly altered liver functions are nonspecific in their interpretation and clinically unexpected. Gilbert’s syndrome is a hereditary, relatively common, benign, unconjugated hyperbilirubinemia. It may contribute to the laboratory findings of elevated bilirubin (especially after a fast) but would not explain the clinical picture or elevated liver enzymes.
-
The combination of asymptomatic hepatomegaly and mild nonspecific elevations of hepatic enzymes in this case is suggestive of a chronic inflammatory liver process or hepatitis. The causes of hepatitis can be classified as drug-induced, toxic, infectious, genetic, and connective tissue disease-associated. The major cause of liver disease in the United States is alcohol ingestion. Less common are environmental exposures, resulting in either acute or chronic toxic hepatitis. Infectious hepatitides include those due to the viruses such as A (infectious), B (serum), C (transfusion-associated) and other possible agents of non-A, non-B hepatitis. Some connective tissue diseases such as lupus erythematosus are associated with a specific type of hepatitis. Hepatitis may also occur with Epstein-Barr virus and cytomegalovirus infections.
Infiltrative diseases such as sarcoidosis or amyloidosis, and rare genetic diseases such as Wilson’s disease, primary hemochromatosis, and alpha1-antitrypsin deficiency must be excluded.
-
Viral serology and a heterophil antibody test should be considered. If there are suggestive signs or symptoms, a serum iron and total iron binding capacity, serum copper and ceruloplasmin, and antinuclear antibodies may be helpful. Assays for suspected hepatotoxins may also be of value. Further evaluation may include ultrasound and percutaneous liver biopsy.
Challenge
Challenge questions begin on page 4.
-
Older electrical transformers and capacitors can contain PCBs as a dielectric and heat transfer fluid. Leaks in the equipment could allow PCBs to volatilize under conditions of increased temperature, such as those in a basement. A person with chronic exposure to the residue could eventually receive a significant PCB dose through both dermal and inhalation routes.
-
Great Lakes fish, particularly from Lake Michigan, are known to be a potential source of PCBs. A correlation between consumption of PCB-contaminated fish and elevated serum PCB levels has been shown in a study of residents of New Bedford, Massachusetts. For the general population, however, a clinically significant human body burden of PCBs is unlikely to occur through fish consumption alone.
-
Persons with Gilbert’s syndrome have decreased UDP-glucuronyltransferase activity, resulting in impaired glucuronidation of bilirubin and, presumably, of PCBs also. Since a PCB elimination pathway is excretion of the glucuronide in urine, impaired capacity to conjugate PCBs with glucuronic acid can theoretically lead to accumulated PCBs and greater body burden. This hypothesis has never been tested, however.
-
Yes, it is important to be aware that potential carcinogenicity is the main reason PCB production was banned in the United States. Human evidence is still considered inadequate, but the animal evidence was strong enough for EPA, NIOSH, and IARC (the International Agency for Research on Cancer) to conclude that PCBs may have carcinogenic effects in humans.
-
Selected laboratories have the capability to perform PCB analyses on human tissue. The lipophilic nature of PCBs causes them to accumulate in fat; consequently, analysis of adipose tissue obtained by biopsy has been advocated as a measure of long-term exposure. Serum PCB analysis, which is less invasive than fat biopsy, can also be done. However, such tests are expensive and health risks often cannot be determined from the results. Testing human tissue for PCB content, therefore, remains principally a research tool.
-
A correlation between increasing levels of serum PCBs and dermatologic findings, including chloracne, has not been consistently found in human epidemiologic studies. However, one study involving 153 workers with occupational exposure to PCBs showed 22 subjects with dermal abnormalities and a mean plasma PCB level of 87 ppb, while 131 subjects without abnormalities had a mean serum level of 50 ppb. The difference was statistically significant. By comparison, plasma PCB levels in unexposed populations are less than 30 ppb. However, no serum PCB values are yet accepted as normal or toxic levels. Our patient’s PCB serum level of 125 ppb is nonetheless consistent with PCB exposure as an etiology for his unusual acne, and PCB exposure may be contributing to the hepatic effects noted.
-
The first response is clearly to stop the exposure. In this case, the patient should stay away from the basement until the transformer is repaired and the basement area cleaned. He should also refrain from eating Great Lakes fish until his PCB level normalizes and the fish are known to be uncontaminated. Avoiding exposure is especially important, as there is no specific treatment for PCB accumulation. The need to avoid other hepatotoxic substances including alcohol should be stressed. Currently, there are no data to support monitoring serum PCB levels.
-
Since cessation of exposure is of prime importance, the physician can be most helpful by specifically recommending proper abatement. In this case, the owner of the building should be notified of the potential health hazard. This may require the assistance of local, state, or federal agencies such as the department of public health and EPA. These agencies can work cooperatively with those involved to bring about remediation of the harmful exposure. It is important to prevent others from using the basement areas until cleanup is complete.

















