Fostering the Well-Prepared Stakeholder Culture
KEY SPEAKER POINTS
- Creating value is good, Peter Knox said, but the real goal should be to create value at speed.
- Two drivers of engagement, according to Peter Margolis, are (1) effective leadership, which builds shared responsibility for improving outcomes, making transparent measurements, and sharing data in a way that engages all participants in the system in collaboration to produce continuous learning, and (2) effective resources, such as tools, training, and financial support that enable all of the different constituencies to participate with reduced transactional barriers.
- Clinicians, Margolis said, have an intrinsic motivation of common purpose, a sense of mastery, a commitment to continuous improvement, and a sense of trust and solidarity, that can engage them in creating a culture of learning.
- When the clinical community fails to provide patients with the information they need, Bray Patrick-Lake said, patients go and create their own opportunities, particularly by using social media. “We need to figure out how to integrate people and help them get what they need out of the system,” he said.
- Patients need to be made aware of the benefits of belonging to a health care system that engages in research and that belongs to PCORnet, Patrick-Lake said.
The goal of this session was to discuss challenges and opportunities in the engagement of clinicians, patients, families, and the public in integrating care and research efforts. Integrating learning into the delivery of care is a cooperative activity involving the patients who receive care, the people who lead the systems in which research takes place, and the clinicians who provide care. It is an activity that is “not for the faint of heart and that takes ongoing, continuous work,” said session moderator Jean Slutsky, the director of the Communication and Dissemination Research Program at PCORI. In this session, Peter Knox, the executive vice president and chief learning and innovation officer at Bellin Health, spoke about his organization’s efforts to create a culture of learning that can also execute quickly on the basis of new knowledge. Peter Margolis, codirector of the Center for Health Care Quality at Cincinnati Children’s Hospital Medical Center, addressed the topic of physician engagement, and Bray Patrick-Lake, director of stakeholder engagement for the Clinical Trials Transformation Initiative and a member of the PCORnet Executive Leadership Committee, talked about the importance of patient engagement in a learning health system. A discussion moderated by Slutsky followed the three presentations.
CREATING A CULTURE OF LEARNING
Creating value is good, Peter Knox said, but the real goal should be to create value at speed. According to a recent evaluation, Knox said, his company, Bellin Health, was the best performing of the 32 pioneer accountable care organizations (ACOs) (L&M Policy Research et al., 2013). Based on the fact that Bellin Health had the lowest cost per member of the pioneer ACOs and also scored the highest on quality of care and patient experience, Knox argued that his organization created value for the government. Bellin accomplished this feat, Knox said, by learning how to overcome the odds that it, like most organizations regardless of what industry they are part of, would fail to execute its strategy successfully. What, he asked, does it require to succeed? “We believe an organization that can deliver value at speed requires intentionality, discipline, focus, and rhythm,” he said, explaining that the last factor, rhythm, is about managing energy, which is in limited supply in most organizations.
In 2000 Knox created a framework that has served as the template for his team’s efforts to produce value at speed at Bellin (see Figure 8-1). This framework holds that for an organization to execute effectively it must think about six dimensions. The first dimension is strategic position, which involves listening to and understanding the market, understanding the value proposition, and preparing the organization to focus on patients’ important priorities. The second dimension is the production system or organizational structure that delivers on the specifications developed according to the
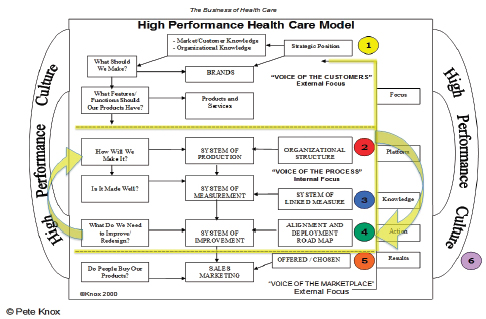
FIGURE 8-1 Bellin Health’s high-performance health care model.
SOURCE: Reprinted with permission from Peter Knox.
strategic position. The third dimension is a system of measurement that can be overlaid on the production system to provide insights into how the system is performing.
Once those first three dimensions are in place, only then is it time to create a system of improvement, which is the fourth dimension. “When I’m called in to work with health systems,” Knox said, “this is usually the problem that I see immediately—they’ve jumped in at dimension four. First you have to understand the market, understand how you’re producing your products and services, know where your gaps are, and be very focused on where you spend your time and energy. This is where I think we have to align research if it’s going to be relevant in the value equation.”
Marketing the product is the fifth dimension, and, again, this is a place where health systems often fail to execute. As an example, Knox recounted an advertisement he heard for a health system that bragged that its cancer survival rates were above average. Bellin’s approach was to use what its customers had said was most important to them—understanding their options when told they had cancer. Bellin worked with its physicians to improve its production system so that it could make a guarantee in the market that it would give individual patients diagnosis-to-treatment options within 3 days. The first five dimensions, Knox said, are all wrapped up in the final dimension, which is a high-performance culture that supports creating value at speed.
To strategically align their organization for success, Knox and his colleagues have defined three breakthrough initiatives: eliminating cost, waste, and variation; managing populations beyond its Medicare population covered by the pioneer ACO for triple aim outcomes; and new business development and growth. “These are the things we have to hit out of the park,” Knox said, and every quality improvement project that Bellin conducts has to fit within these three initiatives. As an example, Knox discussed Bellin’s new business development process. When looking at a possible improvement, if it is an incremental increase the organization sets a goal of defining, implementing, and disseminating the improvement across the organization within 60 days. New products, by contrast, are put into an incubator and nurtured so that they have a chance to succeed.
Knox explained that Bellin’s production system incorporates research at four levels. Population research is at the first level, and Knox said that the system is in the midst of a 10-year agreement with the Green Bay Packers to improve the health of their community. Second-level research is breakthrough research which, in particular, focuses on how to conduct research on best practices in primary care from around the world and implement those best practices in the Bellin system. Microsystem research, the third level, covers clinical trials aimed at improving care, and fourth-level research includes the studies that clinicians and researchers at Bellin are running to improve their ability to care for patients more efficiently and with better outcomes. As an example of this fourth level of research, Knox cited a study that aimed to understand why patients were missing appointments; the results of that study led to changes that caused no-show rates to drop from 12 percent to 4 percent.
Addressing the concept of managing energy, Knox said that the entire organization runs on a rhythm of 120-day cycles, with the leaders in the organization getting together every 120 days to redefine and recalibrate the organization’s priorities. In addition, a select group of executives, including the CEO, chief information officer, the chief medical officer, and the chief financial officer, get together weekly to talk about how they are managing organizational energy and the breakthrough and operational priorities as well as how to continuously foster the development of a culture to support the organization’s goals. Bellin has also built a competency model around the breakthrough initiatives that prepares the organization’s staff develop the competencies needed to operate in a world in which health care is being managed differently as it moves from a fee-for-service model to one that manages health.
Knox explained that Bellin has a delivery structure built around the patient and a project delivery structure designed to help the organization adopt breakthrough initiatives and operational priorities. The first structure integrates patients in nearly every aspect of quality improvement, and the
second integrates people from all over the organization. “These two distinct structures are designed to deliver service every day reliably and predictably to our customers, but also to achieve better and greater value each and every day,” Knox said in closing.
Engagement in a learning health system, according to Peter Margolis, means producing information, knowledge, and know-how to improve both personal health and the health care system. “This means participating in all phases of knowledge development and research, from forming questions, doing work, getting learning to happen, and applying the results,” he said. Based on lessons learned from scores of projects involving large numbers of clinicians and care teams, Margolis and his colleagues have identified several key drivers for engagement. These include effective leadership to build shared responsibility for improving outcomes and transparent measurements and data sharing that engages all participants in the system in collaboration to produce continuous learning. Also required are effective resources, such as tools, training, and financial support that enable all of the different constituencies to participate, and also tools that reduce transactional barriers.
As an example of a standardized process for engaging clinicians, Margolis discussed a project involving a network of about 75 endocrinology practices—50 pediatric and 25 adult—that focus on research for patients with Type 1 diabetes. Despite the widely accepted findings of a 1993 study (Diabetes Control and Complications Trial Research Group, 1993) showing that intensive therapy delays the onset and slows the progression of diabetic retinopathy, nephropathy, and neuropathy in patients with diabetes and that clinicians can help patients prevent the development of these complications by helping patients maintain glycemic control, the Type 1 Diabetes Exchange showed that there is a wide variation in the degree of glycemic control that patients are achieving today.
When physicians are shown these data, Margolis said, their first response is to provide a variety of excuses, none having to do with the fact that some clinics have developed more effective processes for helping their diabetic patients achieve glycemic control. However, it turns out that within a short period of time after starting the discussion, clinicians start engaging in meaningful conversations about how to learn and apply lessons from the best performing clinics. “We talk about the things that motivate clinicians to make improvements,” Margolis said, “but the important intrinsic motivations that our model is meant to tap into are the common purpose, the sense of mastery, the commitment to continuous improvement in learn-
ing, and the sense of trust and friendship and solidarity that builds up in a network.”
Margolis said that when this process works—when clinicians get engaged in solving a problem—there are processes available that can help focus that engagement on outcomes and learning from data. What is important, he said, is engaging in a discussion that creates a sense of urgency and a culture of learning while at the same time reducing the fear and anxiety that any professional feels when his or her performance is not where it needs to be. When this works, it produces a culture where everyone is working together and where, as Margolis put it, “our networks steal and share shamelessly.”
In the session’s final presentation, Bray Patrick-Lake said that patients dream of a high-quality health care system that is patient-centered and efficient and that enables reliable and timely access to evidence-based prevention and treatment options that are responsive to individual patient needs. Moreover, she said, while the current health care system is not operating optimally for anyone, she believes that it is possible to create just such a system if everyone can come together to work on the issues that this workshop has identified: inefficient use of resources, siloed data that could be used to improve care on a daily basis, research that never filters back to patients, and lack of transparency when it comes to value and outcomes. She noted, too, the lack of any kind of useful information or data for many conditions and the fact that many guidelines are not based on evidence that patients might find to be reasonable.
Patrick-Lake said that the field needs to get smarter about the data it collects and how it explains those data to patients. “Can we identify elements that actually make a difference to patients and help physicians improve care?” she asked. “We have got to get smarter about making data work for us.” When the clinical community fails to provide patients with the information they need, patients go and create their own opportunities, particularly by using social media such as Facebook. “There are now 7,000 patient groups in this country, and I’m not sure we need any more,” she said. “But every time a patient steps forward and they don’t get what they need, they’re still going to try to get answers for themselves and for their children. And so we really need to figure out how we integrate people and help them get what they need out of the system, so we can stop going off and creating all of these different siloed activities.”
Another thing that is happening, she said, is that patients are getting more involved in the research endeavor and are experiencing many of the same frustrations that clinicians and researchers face in dealing with IRBs
and contracting offices. Patients, she continued, are becoming results-oriented, demanding more from the system, and in some cases taking control of the system. In her role with the Clinical Trials Transformation Initiative, an FDA-driven public–private partnership to improve the quality and speed of clinical trials, she harnesses the energy of patients to work with all of the stakeholders to produce systemic change.
Patrick-Lake noted that one way in which patients are driving this change is through the PPRNs that have been forming. These networks include people who have backgrounds in statistics and information technology and who are taking data and making it work for patients. These networks are creating benchmarks for patients so that they can see how they are doing compared to other patients. They are creating forums for real-world populations of patients to compare medication regimens and exchange other relevant information that they feel they are not getting from the clinical community. “Patients are coming together to create these user-designed systems that actually meet the triple aim and that have been shown to reduce spending,” Patrick-Lake said, adding that these networks need to think more about metrics and that she hoped that the PCORnet community would help with that task.
Her hope, she said, is that in another year or two all patients in the United States will know whether they are in a learning health care system and if the system they get their care from is part of PCORnet. Being part of PCORnet is a benefit, she said, and the community needs to communicate that to patients so that the patients realize that if they are not part of a research effort, research results will not be applicable to patients like them. “We need to be raising awareness every day,” she said. From her perspective as a patient with cardiac and vascular conditions, she said she hopes that nobody else has to go through what she has experienced and that others can benefit from the knowledge that her clinicians have gained in treating her.
One point that Patrick-Lake stressed is that PCORnet is a living laboratory that is working hard to engage patients and to develop new approaches for better engaging patients. But in the meantime, it is time for the community to start engaging patients in whatever way it can, using the many innovative methods that are available. “If you don’t know how to do it,” she said, “ask around because there are others that do, and hopefully we will have more evidence of what works in the future. Everything about patient engagement is not completely solved, but that doesn’t mean we shouldn’t do it now. We need to dig our feet in the ground and say that together we’re going to address these issues.”
To start the discussion, session moderator Slutsky said that one of the take-home messages that she heard from these and other presentations is that if you are not part of a learning health system as a clinician, a health system, or a patient, you should be angry. She thought that all of the workshop attendees would agree that it should be an aspirational goal for everyone to be part of a learning health care system. She also noted that the situation with the health care system is somewhat analogous to what happened at General Motors with its ignition system problems: There was a simple fix, the data were available, yet because of an organizational failure, the problem was not corrected, and people died as a result. “The analogy with health care,” she said, “is that we often know about harms or have an inkling of a harm but as providers or a health care system we do not know how to change and fix the problem.” She added that a learning health care system represents the best way to address that sort of problem and to identify and fix problems before they become serious.
Jon White from AHRQ asked Knox to comment on the resources that a system needs to invest in, in an information system. Knox replied that he and his colleagues are building what they are calling a knowledge brain that has to operate at three levels: a strategic level that can look at populations, understand populations at a macro-level, and help devise strategies to improve population health; the mezzanine or registry level that operates outside of the boundaries of the Bellin Health system to help accomplish the triple aim; and a point-of-care level that helps clinicians when they are in front of patients. The base platform for this triple-level brain is an Epic EHR in which Bellin has invested about $30 million, and White said that he is working with a partner, Cryptic, to build out the strategic and mezzanine levels of the brain. He said that Bellin is investing in the development of the Cryptic system. “Our investment is significant for an organization of our size, but we’re very intentional about what we’re trying to build,” he said. “At every level we’ve defined clear specifications on what we need that level to do, and we’re working with partners to help us deliver on those specifications.” He added that each of the levels is imbedded in the Epic EHR so that information can move to and from the point-of-care level.
In a question posed to Patrick-Lake and Knox, James Rohack asked if they had ideas on how to balance the need to create an efficient organization with the need to invest in technology for competitive reasons. Patrick-Lake said that this is a challenge that has been amplified by patient distrust of the new ethos that less care is usually better care for the patient even though that is what the learning health care experience is finding to be true. Overcoming this distrust requires building strong relationships with the patient community that can help educate them about evidence-
based medicine. Knox added that it will be critical to work with partners to continue to develop evidence-based best practices and then put in the time and effort to prove to the patient community that this less-is-more approach to medicine creates value for more than just the health care system itself. He also noted that value is the key concept, and as an example he said that Bellin has invested heavily in robotic technology because it adds value, while at the same time it has been working with partners to provide access to technologies that would not provide value to Bellin alone. “For us, it keeps coming back to that value equation,” Knox said in summary.
Rachel Hess from the PaTH CDRN wondered how to balance the speed of implementation with the need to ensure that any new process will not harm patients. As an example, she cited the case of epogen, which initial data had suggested was beneficial to patients with breast cancer but which later data showed actually increased mortality. Patrick-Lake said that this is an issue that patients deal with every day as new information is published or appears in the media. One suggestion she made was to involve the relevant patient organizations and to ask them to review recommendations before disseminating them. Margolis added that one of the benefits of being in a learning health care system involving large groups of people engaged in standardized processes is that when there are competing views of what to do, it is possible to be intentional about mounting the studies needed to address conflicting data.
Patrick-Lake added that PCORnet offers the same opportunity on an even larger scale. “I think that’s the paradigm shift that we can see where we can partner and study things in a much broader capacity,” she said. This remark prompted Richard Platt of the Harvard Pilgrim Health Care Institute and director of the PCORnet Coordinating Center to note that he would be meeting with the various NIH institute directors to discuss how they might engage with PCORnet to take advantage of the opportunities created by working at the scale that PCORnet will create when it is fully implemented.
Jonathan Tobin said that another opportunity that PCORnet creates is to look at the organizational and clinician level measures that are embedded and interlinked with the delivery of services that may be important causal variables for understanding variation in outcomes, which are probably as much related or more related to those variables than they are to individual patient-level factors. “So if we think about the cascade of dissemination and implementation from the standpoint of understanding and explaining that variation,” he said, “one very prominent role that PCORnet can play is to monitor the downstream implementation of the innovations from clinical trials and to begin to understand the interaction of those patient and organizational and clinician level variables and understand how they can be
modified in a way to produce better results and at the same time advance the generalizable knowledge about dissemination and implementation.”
Physicians sometimes talk about empiric practice—using knowledge, instinct, and experience to treat a patient in the absence of hard evidence—and Harold Luft wondered if it might be possible to produce faster advances by returning to empiric practice but in a way that collects data for each patient to more quickly build an evidence base. Knox thought that such N-of-1 studies can provide a basis for an initial advance in knowledge that can then be tested on a larger scale. He noted that Bellin Health is working with its women’s services group to redesign the care experience for women and that it is testing some changes in as few as five patients, recording the results, adjusting the process, and then scaling from there.
At one point, the discussion turned to the issue of dissemination and scale, with several workshop attendees asking how it would be possible to take the lessons learned from exemplar systems and disseminate them nationally. Margolis said that one contributor to this problem is the unwillingness of systems to share their learnings, something that PCORnet is addressing directly. Knox added that there needs to be a nationwide assessment to identify gaps in knowledge transfer and to then apply a value equation in order to better understand and address those gaps. Patrick-Lake stressed that best practices cannot be considered proprietary.
Sally Okun recounted a project that she ran with the American Academy of Neurology that involved deploying its epilepsy care guidelines into the epilepsy patient population and surveying the patients to see if the care they were receiving met these guidelines. The results showed that care being delivered by neurologists varied significantly across the country, with the greatest departure from best practices seen in patients treated by neurologists who were not epilepsy specialists. There were two particularly disturbing findings: Neurologists did not discuss contraceptive control with patients on antiseizure drugs or the potential for surgical intervention. Okun wondered if patient education and activism could be a route to achieve better compliance with best practices at a scale extending beyond the exemplar learning health care systems.
Katherine Newton from GHRI said that one factor that slows the speed of dissemination is that many dissemination plans are based on prestige rather than patient needs. By that she was referring to the academic reward system that leads researchers to try to publish their research in top-tier journals that may not accept their papers, at which point they then submit to another journal, a process that can add months to the dissemination process. “Peer review can take a long time,” Newton said, “and even then, results are embargoed because we want the big press release, which again is about prestige. It seems to me that in this age there are some trials that are important enough that there will be a very fast dissemination plan that
will get out to our patients and practitioners as soon as they need it.” The problem, she said, is that such a process could negatively affect chances for promotion.
John Steiner said that one of the issues that underlie this problem is the need for control, explaining that the system that exists now is one in which researchers have perfected the art of controlling the agenda by limiting access to information until such time as they think it is ready to be released. “What this panel has done is point out that other groups have legitimate interests in that information far earlier in the process,” Steiner said. He added that this is a place where governance of research has to change in such a way that gets patients at the table early in the process. Referring to patient advocates such as Patrick-Lake, Steiner said, “I can’t imagine you standing for me saying I can’t release findings until I get to present it at a national meeting. Getting you at the table early, I think, creates the circumstances under which the traditional control of researchers is unlikely to endure, and that’s a really good thing.”
David Ballard from Baylor Scott & White Health wondered why more institutions are not using the entrepreneurial model that some health care delivery organizations have been using to get their best practice models to the market. As examples, he cited the Cleveland Clinic’s effort to market its cardiac surgery model to states and Geisinger’s partnering with XG Health Solutions, a venture capital firm in which it is a minority owner, to get its solutions to the market. Knox noted that Bellin is the fourth-largest vendor of retail clinics through its FastCare brand and that it is about to launch a franchise licensing model. Bellin has a dedicated group of people in its organization who actively seek out such opportunities and market voids that it could fill with its best practices. It then has a structured process for launching the appropriate solutions into those markets. “We’re trying to build a system that searches, identifies, and then launches,” Knox said.
Margolis said that Cincinnati Children’s Hospital Medical Center, as a not-for-profit organization, takes a different approach based on what is known as lead user innovation, which recognizes that in a community of people participating around a common purpose, some 15 to 30 percent will start product innovations that anticipate the needs of the rest of the community. Margolis said that the large network that he works with generates at least one new idea a week that someone thinks has the opportunity to produce value. Like Bellin Health, Cincinnati Children’s uses a formal design and prototyping process that takes advantage of the diversity that exists within its networks to test these ideas under a wide range of conditions. This process, he said, has the benefit of also producing champions in the system who, once the innovation is working, can advocate for its adoption once it gets distributed into the entire system. “We’re starting to be approached by industry and a variety of different disease-specific groups
that are interested in learning how to do this,” he said, “and it’s causing us to think a lot about how to scale that kind of system up and make it more widely available.” When asked by Ballard if this is being done in the context of a single 501(c)(3) organization, Margolis replied, “We do it in the context of a network that includes multiple medical centers and a 501(c)(3) working together, but with very complicated money flows.”












