7
Recent Approaches to Assessing Nutritional Adequacy and Exploring Chronic Disease
The recommendations presented in the several editions of the Dietary Guidelines for Americans (DGA) Policy Report1 have traditionally been oriented toward the healthy U.S. population, ages 2 years and older, and have not been intended for the treatment or management of disease. Over the past several decades the landscape of the general population’s health status has shifted. Many Americans now live with one or more chronic disease (Ward et al., 2014). Furthermore, evidence is emerging that exposures to nutrition and other environmental factors in utero and in early life may play a role in “programming” the risk for chronic disease in later life (Hanson and Gluckman, 2015). This places an emphasis on optimizing nutrition and lifestyle in pregnancy and infancy, two population groups previously not included in the DGA. The Agricultural Act of 2014 mandated that dietary guidance for these populations be included in the 2020–2025 DGA (see Chapter 5 for details). Thus, understanding the relationship of diet to chronic disease prevention across the life span and developing relevant guidance in the DGA process is important.
This chapter explores how the 2005, 2010, and 2015 Dietary Guidelines Advisory Committees have approached assessing nutritional adequacy2 and the role of diet in health and chronic disease, noting similarities and
___________________
1 Refer to Chapter 1, Box 1-1, for an explanation of how the term DGA is used throughout this National Academies report.
2 This National Academies committee’s Statement of Task used the phrase “nutritional sufficiency.” However, to align with standard nomenclature used by the Dietary Reference Intakes, the phrases “nutritional adequacy” and “nutritional inadequacy” will be used in this report.
differences across the different cycles. Opportunities for improvements to the process are also identified.
ASSESSMENTS OF NUTRIENT INTAKE LEVELS OF THE U.S. POPULATION BY THE 2005, 2010, AND 2015 DGACs3
The health effects of dietary intake, particularly specific nutrients, are most pronounced at both ends of the spectrum of intake. Deficiencies of an essential nutrient, for example, can lead to nutrient-specific conditions (e.g., iron-deficiency anemia, scurvy, beriberi). Excessive nutrient intake can also lead to adverse effects (e.g., hypercalcemia, hypervitaminosis A). Nutritional adequacy without excessive intake, therefore, is one component for elucidating the relationship between diet and health.
Recent DGACs have evaluated current nutrient intake levels to determine the extent to which the U.S. population is meeting recommended intake goals, primarily as intake relates to the Dietary Reference Intakes (DRIs).4 The DRIs, defined in Box 7-1, describe nutrient intake requirements averaged over time in apparently healthy individuals. This concept of assessing usual intake is key, as “intake may vary substantially from day to day without ill effect in most cases” (IOM, 2000, p. 3). DRIs serve as benchmarks that can be used to assess inadequacy for a population and for an individual, and also to assess the potential for adverse effects caused by excess. DRIs are set for groups defined by life stage and gender. The framework used to set the current DRIs focuses on intakes that prevent deficiency as well as intakes that prevent adverse effects. Additionally, the existing DRI framework allows for the integration of data on safety, efficacy, and the reduction of chronic diseases, to the extent that specific evidence exists. However, owing to a lack of supporting evidence, few DRI values have been based on chronic disease data (see Appendix E). Efforts are currently under way to move toward using chronic disease end points to establish DRIs.5
___________________
3 The under- and overconsumption of food groups have also been evaluated by previous DGACs through food pattern modeling and descriptive data analyses. For additional information about such analyses, see Chapter 6.
4 For additional information about the DRIs, including their evolution and applications, see Appendix E.
5 A multidisciplinary working group sponsored by the Canadian and U.S. government DRI steering committees met from late 2014 through April 2016 to consider how to base DRI values on chronic disease end points. The working group produced a report that provided extensive discussion of the issues and ideas for paths forward (Yetley et al., 2017). An ad hoc consensus committee of the National Academies of Sciences, Engineering, and Medicine recently released a report in which the options presented by Yetley et al. (2017) are reviewed and recommends methods and guiding principles for including chronic disease end points in the DRI process (NASEM, 2017).
The 2005, 2010, and 2015 DGACs each used the current population intake levels to determine which nutrients are not being consumed at recommended levels. These identified “nutrients of concern” inform the DGACs’ food pattern modeling analyses, which ultimately play an integral role in the resulting DGA recommendations. The three most recent editions of the DGA Policy Report, for instance, have each included guidance on food groups to increase or limit in the diet to address under- and/or overconsumed nutrients (HHS/USDA, 2005a, 2015a; USDA/HHS, 2010a). This guidance ultimately underpins federal nutrition policy,
including regulations and nutrition education materials (see Box 1-2 for examples of how the government has applied the DGA), and has implications for changes in the food sector. Given this, identification of nutrients of concern appears to be a key step in the overall DGA process. The following sections describe how nutrients of concern have been identified and note how the methods and terminology have changed across the three most recent DGACs.
Questions and Data Sources Used to Determine Nutrient Intake Levels of the U.S. Population
In the current process to update the DGA, topics and questions reviewed in the scientific report are developed by the DGAC (see Chapter 5 for additional details). The 2005, 2010, and 2015 DGACs each included one or multiple questions related to the current nutrient intake status of the U.S. population. As outlined in Box 7-2, the questions have progressively expanded to include an evaluation of both under- and overconsumption of nutrients and consideration of sources of excesses.
Recent DGACs have relied on national survey data from the What We Eat in America component of the National Health and Nutrition Examination Survey (NHANES)6 to determine current nutrient intake levels. Both the 2005 and 2010 DGACs used a collection of existing published reports and data tables, which varied in terms of the time span the data reflected, the type of dietary intake represented (i.e., 1-day dietary intake, usual intake), and the analytical approach used. The nutrient intake analyses gathered and performed for the 2015 DGAC, in contrast, used consistent methodologies across a single dataset (2007–2010 NHANES) (HHS/USDA, 2015b).
Classification of Nutrient Intake Levels
Recent DGACs used the analyses of current intakes of the U.S. population to categorize nutrients and identify those that rise to the level “of (public health) concern.” Differences exist across the 2005, 2010, and 2015 DGACs with respect to terminology, thresholds used to classify nutrient intake levels, and the extent to which biochemical and health-related data have been incorporated into the process.
___________________
6 The 2005 DGAC used data from the Continuing Survey of Food Intakes by Individuals (CSFII). CSFII was integrated into the National Health and Nutrition Examination Survey (NHANES) in 2002 and is referred to as the “What We Eat in America” component of NHANES (USDA ARS, 2016).
Terminology Describing Nutrient Intake Levels
As presented in Table 7-1, the terminology used to describe nutrient intake levels has varied across the editions of the DGAC Scientific Report. The concept of a “shortfall nutrient” has remained relatively consistent across recent editions of the DGAC Scientific Report, describing a nutrient that is underconsumed across the population or in a specific group of the population, relative to DRI values (i.e., Estimated Average Requirement
TABLE 7-1 Terminology Used by the 2005, 2010, and 2015 DGACs to Classify Nutrient Intake Levels
| Terminology | Descriptions, as Presented in the DGAC Scientific Report | ||
|---|---|---|---|
| 2005 DGAC | 2010 DGAC | 2015 DGAC | |
| Shortfall nutrient |
|
|
|
| Nutrients that pose special challenges |
|
|
|
| Nutrients of concern |
|
|
|
| Nutrients of public health concern |
|
|
|
___________________
NOTE: AI = Adequate Intake; DGAC = Dietary Guidelines Advisory Committee; EAR = Estimated Average Requirement; N/A = not applicable—phrase not used in the corresponding DGAC Scientific Report.
a Nutrients of concern and nutrients of public health concern are defined here as they appear in the introduction of Part D, Chapter 1, of the 2015 DGAC Scientific Report (HHS/USDA, 2015b). However, later in the chapter, “nutrients of concern” are described as under- and overconsumed nutrients corroborated with biochemical markers of nutritional status, where available, and evidence for associations with health outcomes (HHS/USDA, 2015b).
b The 2010 DGAC also used the phrase “nutrients that are underconsumed by the general public and present a substantial public health concern” (USDA/HHS, 2010b).
[EAR] or Adequate Intake [AI]). In the two most recent editions of the DGAC Scientific Report, both under- and overconsumed nutrients were included in the classification of “nutrients of (public health) concern.” Also emerging in the 2010 and 2015 DGACs was the additional criterion of biochemical indices and/or direct relationship with health conditions as a requisite for a nutrient being classified as being “of (public health) concern.” The differentiation between “nutrients of concern” and “nutrients of public health concern,” however, has not been consistent across or within the two most recent editions of the DGAC Scientific Report.
Intake Level Thresholds Used to Classify Nutrients
The three most recent DGACs all used levels of inadequacy and/or adequacy as the criterion to identify underconsumed nutrients. None, however, explicitly stated a priori criteria or a rationale for the cutoffs used in determining shortfall nutrients. As previously described, the analyses used by the DGACs to assess current intake levels have been heterogeneous. These differences are reflected in the quantitative threshold intake levels of identified shortfall nutrients. Table 7-2 outlines the lowest levels of nutrient inadequacy and the highest levels of nutrient adequacy of the shortfall nutrients identified by the 2005, 2010, and 2015 DGACs.
In addition to assessing underconsumed nutrients, the 2010 and 2015 DGACs also explored overconsumed nutrients. In the 2010 DGAC Scientific Report, one nutrient was compared to its Tolerable Upper Intake Level (UL) (sodium),7 while two nutrients with no established ULs (saturated fat and cholesterol) were compared to quantitative intake goals estab-
___________________
7 Select nutrient intakes were compared to the UL in other sections of the 2010 DGAC report, with respect to total dietary intake (i.e., inclusive of dietary supplement intake).
TABLE 7-2 Lowest Levels of Nutrient Inadequacy and Highest Levels of Nutrient Adequacy of Shortfall Nutrients Identified by the 2005, 2010, and 2015 DGACs
| Nutrient Characteristic | Threshold Intake Levels of Identified Shortfall Nutrients | ||
|---|---|---|---|
| 2005 DGAC | 2010 DGAC | 2015 DGAC | |
| Nutrients with an EAR |
|
|
|
| Nutrients with an AI |
|
|
|
NOTES: The values presented in this table reflect the lowest level of inadequacy and highest level of adequacy presented as evidence for shortfall nutrients for the population group specified in the corresponding DGAC Scientific Report. The values do not reflect a threshold that was explicitly stated as an a priori decision or criterion in the editions of the DGAC Scientific Report. AI = Adequate Intake; DGAC = Dietary Guidelines Advisory Committee; EAR = Estimated Average Requirement.
a The 2010 DGAC used a U.S. Department of Agriculture Food and Nutrition Service report on intakes of school children as evidence of shortfall nutrients (USDA, 2008). The text indicates the classification was notably due to the intakes of adolescents (USDA/HHS, 2010b). As such, the values in this table reflect the levels of adequacy for children 14 to 18 years of age.
b The 2015 DGAC classified folate as an underconsumed nutrient for the U.S. population, ages 2 years and older. Both zinc and vitamin B6 had higher proportions of the total population with intakes below the EAR than for folate. Levels of intake of folate among adolescents and premenopausal women, however, were at similar levels as those presented in the above table for iron.
___________________
c In the 2010 DGAC Scientific Report, Figures D2.14 and D2.15 provided evidence of which 10 nutrient intakes qualified as tenuous among adult men and women (USDA/HHS, 2010b). Choline was noted as a shortfall nutrient for this population, but it was not included in either figure. As such, the values included in the table only reflect the levels presented in the two figures in the 2010 DGAC Scientific Report.
d The 2010 DGAC used a Food and Nutrition Service report on intakes of school children (USDA, 2008) as evidence of shortfall nutrients. The narrative text indicates the classification of calcium was notably due to the intakes of children 9 to 18 years of age, and the classification of potassium and fiber was based on the intakes of all children (USDA/HHS, 2010b). As such, the values in this table reflect the highest threshold across the noted population age groups.
e Based on an analysis by Bailey et al. (2010), which looked at dietary and total usual intakes of calcium and vitamin D. The 2010 DGAC indicated the analysis suggested calcium was a shortfall nutrient for children 4 to 8 years of age.
lished in preceding editions of the DGA Policy Report (< 10 percent total energy and < 300 milligrams per day, respectively) (USDA/HHS, 2010b). Although no explicit or a priori cutoff was stated in the 2010 DGAC Scientific Report, all three nutrients identified as being overconsumed had 50 percent or more of one or multiple population groups exceeding the UL or other standard of excessive intake. In the 2015 DGAC Scientific Report, an assessment was included of the percentage of the population above the UL for all nutrients evaluated with an established UL. This analysis showed that all but one nutrient (sodium) had 3 percent or less of the population exceeding the UL, suggesting relatively low risk of adverse effects in the general population due to excessive nutrient intake. The 2015 DGAC also used the same intake goals as used by the 2010 DGAC for saturated fat and cholesterol. Again, the assessment was descriptive and no quantitative threshold was explicitly stated for what level of intake in the population or specific group qualified as excessive.
Use of Biochemical and Health-Related Data to Support Classification of Nutrients
As reflected in the terminology used by recent DGACs to classify nutrient intake levels, a progressive shift occurred toward integrating data beyond just nutrient intake levels in the decision-making process for nutrient classification. For example, the primary focus of the 2005 DGAC’s assessment of nutrients of concern was on nutrient intake levels. For vitamin E, the 2005 DGAC identified intake levels suggesting widespread deficiency, but this was not accompanied by overt symptoms of deficiency in the U.S. population. Nevertheless, the 2005 DGAC still identified vitamin E as a nutrient of concern based on the dietary intake data alone.
In comparison to the 2005 DGAC’s approach, the use of biochemical indicators and other health-related data was more prominent in the 2010 DGAC’s categorization of nutrient intakes. Shortfall nutrients were not classified as nutrients of public health concern if a biochemical marker indicated approximately 7 percent or less of the population was inadequate8 or if the shortfall nutrient did not have nationally representative prevalence data on biochemical or functional deficiency. The 2010 DGAC used data from a variety of sources to justify the selected nutrients of (public health) concern, including biochemical indicator data, evidence presented in a corresponding DRI report supplemented with a literature search of recent publications, an Agency for Healthcare Research and Quality evidence report, and an American Dietetic Association position paper.9 For some of the nutrients, the evidence was directly linked to a specific question posed by the 2010 DGAC in another section of the scientific report (e.g., “What are the health benefits of dietary fiber?”). For two nutrients the 2010 DGAC identified as being overconsumed (saturated fat and cholesterol), the health-oriented justifications were supported by full Nutrition Evidence Library (NEL) evidence-based reviews conducted to answer specific questions posed by the DGAC elsewhere in the scientific report (i.e., “What is the effect of saturated fat intake on increased risk of cardiovascular disease or type 2 diabetes, including effects on intermediate markers such as serum lipid and lipoprotein levels?” and “What is the effect of dietary cholesterol intake on risk of cardiovascular disease, including effects on intermediate markers such as serum lipid and lipoprotein levels and inflammation?”). The other identified overconsumed nutrient (sodium) was justified by evidence presented in its corresponding DRI report, supplemented with literature published since the DRI report’s release.
The 2015 DGAC explicitly stated that it used the totality of evidence from a “three-pronged approach” to determine which under- and overconsumed nutrients posed a substantial public health concern. The three prongs included the dietary intake levels from 2007–2010 NHANES data, analyses from the Second National Report on Biochemical Indices of Diet and Nutrition in the U.S. Population (CDC, 2012), and prevalence statistics from the Centers for Disease Control and Prevention. Table 7-3 outlines the extent to which these types of evidence were available and used across the seven identified nutrients of public health concern. Only two of the seven nutrients of public health concern had biochemical indicator data available.
___________________
8 This criterion was not explicitly stated by the 2010 DGAC. It was determined by this National Academies committee’s review of the evidence presented in the 2010 DGAC Scientific Report.
9 The list presented here encompasses all sources used. Some of the listed sources were used for only one of the nutrients.
TABLE 7-3 Evidence Used by the 2015 DGAC to Justify Selection of Nutrients of Public Health Concern
| Nutrient | Dietary Intake | Biochemical Indicatora | Health Condition | Other Rationaleb |
|---|---|---|---|---|
| Calcium | % of population below EAR | No reliable biochemical marker exists | Associated with osteoporosis and other health outcomes | FDA’s designation as a nutrient of “public health significance”c |
| Fiber | % of population above the AId | No reliable biochemical marker exists | May play a role in coronary heart disease, colorectal cancer, type 2 diabetes, and obesity | None cited in narrative description |
| Irone | % of population below EAR | Serum ferritin indicating risk of iron deficiency anemia | Iron-deficiency anemia | FDA’s designation as a nutrient of “public health significance”c |
| Potassium | % of population above the AI | Not collectedf | Associated with hypertension and cardiovascular disease | FDA’s designation as a nutrient of “public health significance”c |
| Saturated fat | % of population consuming < 10% of energy from saturated fatg | No biochemical indicator data usedh | Cardiovascular disease | None cited in narrative description |
| Sodium | % of population above the UL | No biochemical indicator data usedi | Adverse health events, particularly hypertension | None cited in narrative description |
| Vitamin D | % of population below EAR | Low serum/plasma 25-hydroxyvitamin D concentrations | High prevalence of osteoporosis and low bone density, particularly in older women | FDA’s designation as a nutrient of “public health significance”c |
NOTE: AI = Adequate Intake; DGAC = Dietary Guidelines Advisory Committee; EAR = Estimated Average Requirement; FDA = U.S. Food and Drug Administration; UL = Tolerable Upper Intake Level.
a From the Centers for Disease Control and Prevention’s (CDC’s) Second Nutritional Report on Biochemical Indicators of Diet and Nutrition in the U.S. Population (2012), as part of the 2015 DGAC’s “three-pronged approach.”
___________________
b The information listed in this column was not part of the 2015 DGAC’s “three-pronged approach” for classifying nutrients of public health concern, but it was included in the narrative describing the rationale for selecting the nutrients.
c Used as evidence by the 2015 DGAC to support its classification.
d The AI is based on intake associated with greatest reduction in risk of coronary heart disease.
e Only a nutrient of public health concern for adolescent and premenopausal women.
f The 2015 DGAC noted that urinary potassium is the primary marker, but it was not collected in the CDC biomarker dataset.
g The 2015 DGAC noted that while median intake was not far from the recommended intake of < 10 percent of energy from saturated fat, the majority of the total population exceeded the 10 percent of energy from saturated fat.
h No biochemical indicator data from the CDC’s Second Nutritional Report on Biochemical Indicators of Diet and Nutrition in the U.S. Population (2012) were used to justify the selection of saturated fat as a nutrient of concern. The 2015 DGAC did, however, review existing reports on the relationship between saturated fat and cardiovascular disease in a different chapter of its scientific report (HHS/USDA, 2015b), which included assessing the effects of replacing saturated fatty acids with other types of fatty acids or carbohydrates on low-density lipoprotein (LDL-C), high-density lipoprotein (HDL-C), and triglycerides. The 2015 DGAC broadly pointed to this section of its scientific report to justify the selection of saturated fat as a nutrient of concern, but it did not mention the biochemical markers specifically.
i The CDC’s Second Nutritional Report on Biochemical Indicators of Diet and Nutrition in the U.S. Population (2012) did not include an indicator for sodium. The 2015 DGAC reviewed existing reports on the relationship between sodium and blood pressure in a different chapter of its scientific report (HHS/USDA, 2015b) and broadly pointed to it in its justification of sodium as a nutrient of concern.
Summary of DGAC Assessments of Nutrient Intake Levels of the U.S. Population
This National Academies of Sciences, Engineering, and Medicine (the National Academies) committee’s evaluation of the approaches taken to assess and categorize nutrient intake levels of the U.S. population highlights the evolution in the process that has taken place across the three most recent DGACs. The approach has evolved to consider both inadequate and excessive intakes, primarily as dietary intakes relate to the DRIs. The 2015 DGAC was able to apply consistent methodologies to a single dataset across the range of nutrients assessed. The DGACs have progressively shifted to considering evidence beyond just dietary intake data to identify nutrients of (public health) concern. Inconsistences exist in the availability of reliable biochemical data and the use of relationships to health outcomes. Standardization of the process by which nutrients of concern are identified is needed to enhance comparability of analyses across DGA cycles and to enhance transparency.
APPROACHES USED BY THE 2005, 2010, AND 2015 DGACs TO EXPLORE HEALTH AND CHRONIC DISEASES
Determining the relationship, effects, and significance of dietary intake on health and risk of chronic disease is more challenging than determining the health effects of inadequate or excessive intake of a single nutrient. Diets are multidimensional and vary by individuals and over time. Dietary intake includes interactions and interdependent relationships across nutrients and other food constituents, adding a layer of complexity to identifying the dietary factor(s) contributing to a given health effect. Chronic diseases are also complex, often exist with multiple morbidities, and develop and progress over long periods of time—even being rooted in exposures during the prenatal period and early infancy (see Chapter 5). The ability to characterize health status is dependent on the existence of a validated biomarker or other measure that represents a discrete state in the causal pathway to chronic disease. It is important to understand how and to what extent diet prevents or contributes to positive or negative health effects, especially in context of other contributing factors. The multifactorial nature of chronic diseases, the complex and dynamic nature of dietary intake, and the strengths and limitations of available evidence ultimately affect what can be explored through the review of the science.
The current DGAC process lacks an analytic framework to structure topic selection, synthesis, and interpretation of the evidence. Recent DGACs have used analytic frameworks to organize individual systematic reviews conducted by the NEL, but such frameworks have not been used
to consider the relationships between the questions posed or their purposes. The lack of an analytical framework guiding the overall structure of the evidence review makes it challenging to readily understand the overall approach and to identify gaps. This National Academies committee finds the lack of an analytic framework to be a major limitation of the current process, with respect to understanding the relationship between diet and chronic disease prevention. Recent DGACs have moved toward considering linkages between the specific research questions asked. The 2015 DGAC, for example, identified crosscutting topics that pertained to multiple concepts throughout the scientific report. As will be discussed later in this section, the 2015 DGAC also presented an organizing framework used to structure its scientific report. This framework, however, was largely theoretical.
In the absence of an analytical framework, this National Academies committee reviewed the questions posed by the 2005, 2010, and 2015 DGACs to evaluate what aspects of health and chronic disease status were addressed. The following sections review the DGACs’ research questions assessing the relationships between health outcomes and measures and the dietary and nondietary factors considered in questions related to health (e.g., a nutrient, dietary constituent, dietary pattern, behavior, or personal characteristic). Table C-2 in Appendix C provides a summary of the dietary and nondietary factors assessed by each of the three most recent editions of the DGAC Scientific Report. For a detailed assessment of the methodological approaches taken to answer the full range of questions posed by the 2015 DGAC, see Chapter 6.
Health Outcomes and Measures of Interest Explicitly Included in Questions
The three most recent editions of the DGAC Scientific Report used different types of outcomes and measures in the questions regarding health, which have varied in terms of specificity and scope (see Table C-2). The 2005 DGAC used the term health broadly in its research questions, appearing to have used such questions to explore the landscape of the literature and determine which health outcomes or measures have been assessed. The use of general terms was not limited to the 2005 DGAC. The 2010 DGAC measured a number of outcomes of interest, including health outcomes, health effects, and health benefits. However, the 2010 DGAC also narrowed the scope of its research questions by using the phrase selected health outcomes to describe a collection of chronic diseases and risk factors including, but not limited to, type 2 diabetes, cardiovascular disease, cancers, and body weight. The 2010 DGAC also posed a range of questions specific to cardiovascular disease and associated risk factors,
explicitly naming the health outcome or measure (e.g., inflammation, low-density lipoprotein [LDL] cholesterol levels, coronary heart disease). The 2015 DGAC continued the trend of posing more specific questions. While some questions used broad descriptors (e.g., health benefits, health outcomes, health), many questions explicitly stated the chronic disease or health measure of interest (e.g., breast cancer, cardiovascular disease, obesity). The specificity appears to reflect the guidance provided by the U.S. Department of Agriculture (USDA) and the U.S. Department of Health and Human Services (HHS). During the first meeting of the 2015 DGAC, USDA and HHS suggested that the DGAC explore topics that have the potential to affect food- and nutrition-related health outcomes of public concern, including “body weight status, cardiovascular disease, cancer, as well as type 2 diabetes, bone health, and the prevention of food-borne illness” (HHS/USDA, 2013).
Consideration has also been given to biomarkers and surrogate end points (e.g., LDL cholesterol levels, blood pressure). Although not perfect replacements for clinical end points of chronic disease, validated biomarkers and surrogate end points have a number of strengths that could be leveraged to bolster the evidence base on the relationship between diet and chronic disease. While frameworks for evaluating biomarkers exist, the number of fully validated markers of diet and chronic disease is relatively limited (see Box 4-4 for a discussion of the use of biomarkers to measure dietary intakes) (IOM, 2010, 2016). Furthermore, use of validated biomarkers can lead to misinterpretation of risk if not evaluated in the context of other supporting data (FDA, 2016). Given that the science underlying biomarkers is still emerging, a clear understanding of the proper uses and limitations of such data is necessary for appropriate interpretation and application. Evidence that a systematic process was implemented to evaluate the validity of biomarkers prior to inclusion in a research question or the evidence base by recent DGACs was not immediately available.
The health outcomes of interest were relatively similar across the three most recent editions of the DGAC Scientific Report, with each having evaluated the science of dietary intake as it related to cardiovascular disease, cancers, type 2 diabetes, body weight, and blood pressure. DGACs have, however, expanded the set of chronic diseases considered. For example, the 2015 DGAC assessed the effect of dietary patterns on “neurological and psychological illness.” Whereas the 2010 DGAC limited its assessments of neurological and psychological illnesses to questions on the relationship between alcohol intake and cognitive decline with age and the effect of maternal intake on infant cognition, the 2015 DGAC placed neurological and psychological illness alongside other widely recognized leading chronic disease (e.g., obesity, cardiovascular disease,
type 2 diabetes). The 2015 DGAC Scientific Report provided the following rationale for inclusion of this health outcome: “[t]he rising numbers of U.S. older adults and the potential human and financial cost of age-related cognitive impairments, such as Alzheimer’s disease and other dementias, also have helped drive national interest in chronic mental disease” (HHS/USDA, 2015b). However, no explicit processes or criteria were described for identifying emerging or different health outcomes not included in previous editions of the DGAC Scientific Report.
Dietary and Nondietary Factors Included in Questions of Health Outcomes and Measures of Interest
A wide range of dietary and nondietary factors was assessed by the 2005, 2010, and 2015 DGACs in relation to health outcomes and measures of interest. Most of the questions focused on various aspects of dietary intake. All three DGACs, for example, asked questions about the relationship between the intake of a specific nutrient (e.g., sodium, folate, saturated fat) and one or more health outcomes of interest. Although there are similarities across scientific reports with respect to the nutrient-related questions (e.g., the relationship between sodium and blood pressure, health benefits of fiber), many are unique to a single DGAC. Assessments have not been limited to just nutrients. The 2015 DGAC posed questions regarding the relationship between constituents of dietary intake (e.g., caffeine, aspartame, low-calorie sweeteners) and one or more health outcomes or measures. The 2010 DGAC included health outcome–oriented questions about the intake of specific foods (i.e., chocolate, nuts), multivitamin/mineral supplements, and specific sources of nutrients (e.g., plant n-3 fatty acids). The 2010 DGAC also posed questions in which energy appeared to serve as an intermediate link between the dietary intake and health outcome of interest (e.g., “What is the impact of liquids versus solid foods on energy intake and body weight?”). Questions have also assessed broader groupings and descriptors of dietary intake. The 2005 and the 2010 DGACs explored the relationship between intakes of specific food groups (e.g., whole grains, vegetables and fruits) and health outcomes. Other health-oriented questions included measures or descriptors of dietary intake such as energy density, glycemic index and glycemic load, and macronutrient proportions. In a departure from the approaches used in 2005 and 2010, the 2015 DGAC expanded its assessment to include several questions about the relationship between dietary patterns and specific health outcomes.
Not all health-oriented questions posed by recent DGACs focused solely on relationships with measures of dietary intake. Questions exploring factors that have an interconnected relationship with diet and health
were included in the 2005, 2010, and 2015 editions of the DGAC Scientific Report. The 2005 DGAC, for example, asked questions related to body weight (“How much physical activity is needed to avoid weight regain in weight-reduced persons?”). The 2010 DGAC also asked questions about nondietary factors, such as the relationship between food environment and dietary behaviors on body weight and the relationship between pregnancy weight gain and maternal–child health. By contrast, the 2015 DGAC appears to have been encouraged by USDA and HHS to expand its exploration to topics that have the potential to affect food- and nutrition-related health outcomes of public concern, including “diet-related outcomes relevant to social, behavior[al], environmental topics; intakes of foods; food groups; dietary patterns; nutrients of public health concern; diet quality; and dietary behaviors” (HHS/USDA, 2013). For example, the 2015 DGAC reviewed reports of the relationship between physical activity and a health outcome of interest, as well as the effect of programs, policies, and approaches in various settings (e.g., schools, worksites) on weight status. Other factors explored by the 2015 DGAC included acculturation, household food insecurity, neighborhood and community access to food retail settings, use of diet and body weight self-monitoring strategies, eating out and/or take-away frequency, and frequency and regularity of family shared meals.
Frameworks and Conceptual Models Used by the 2010 and 2015 DGAC and Corresponding Editions of the DGA Policy Report
The movement to expand evaluations beyond the effect of dietary intake and health highlights the multifactorial and interconnected nature of diet, health, and a host of other nondietary factors. In its assessment of the low adherence with the DGA, the 2010 DGAC pointed to the range of factors that influence food intake and presented a socioecological framework. A modified version of this framework was presented in the 2010 DGA Policy Report, and was accompanied by a recognition that improvements in health require “comprehensive and coordinated systemwide approaches across [the nation]” (USDA/HHS, 2010a).
Building on the work of the 2010 DGAC, the 2015 DGAC created a conceptual map10 of the interrelated nature of the influences and outcomes on diet and physical activity patterns and behaviors across the life span (see Figure 7-1). The map was described as providing structure to the
___________________
10 The phrase used by the 2015 DGAC for this visual was “conceptual model.” This National Academies committee, however, uses the phrase “conceptual map” instead to be congruous with terminology used throughout this report, which describe models as a computational technique.
2015 DGAC’s scientific review of a range of determinants of diet, physical activity behavior, and health and an array of nutrition, physical activity, and related health outcomes. The 2015 DGAC Scientific Report presented an outline of the factors encompassed by each of the components of the
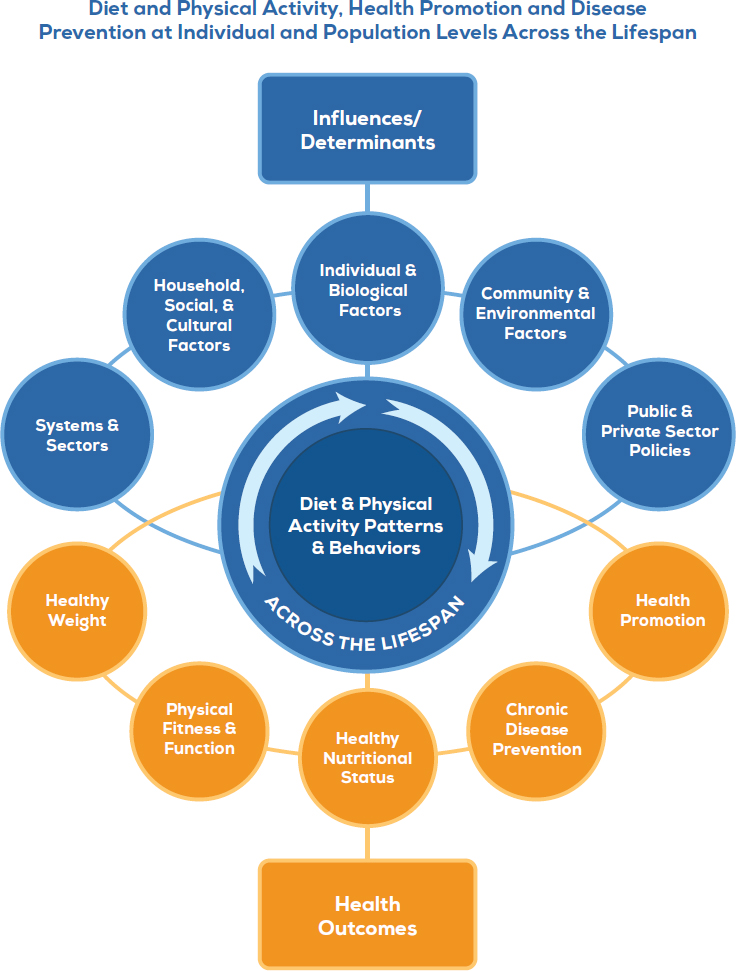
SOURCE: Adapted from HHS/USDA, 2015b.
framework and noted which factors were and were not addressed in the DGAC’s evidence review. Links, however, were not explicitly drawn between the questions posed by the 2015 DGAC and the conceptual map. The 2015–2020 DGA Policy Report also presented a social-ecological map for food and physical activity decisions, which differed from the model presented in the 2015 DGAC Scientific Report. Like its 2010 counterpart, the 2015–2020 DGA Policy Report map was used to explain and emphasize that multicomponent and multilevel strategies are needed to affect public health.
Summary of DGAC Approaches to Exploring Health and Chronic Diseases
Recent DGACs evaluated a wide range of health-related questions, varying in specificity and in scope. Although the chronic diseases included across the three most recent editions of the DGAC Scientific Report have been relatively similar, some expansion of health outcomes has taken place. Recent DGACs were more explicit about the health outcome of interest evaluated and have increasingly assessed the relationship between health and a broader range of nondietary factors. The DGACs’ approach to assessing the relationship between diet, health, and chronic disease currently lacks an analytic framework to structure the purpose, function, and relationship of the questions posed. Frameworks presented across the two most recent editions of the DGAC Scientific Report and DGA Policy Report begin to arrange how the different components and levels interface but remain conceptual in nature.
CONCLUSION
Opportunities exist to improve the process by which the DGAC approaches topics related to dietary intake and health. Using a clear set of terms, establishing one or multiple thresholds for nutrient inadequacy or adequacy that qualifies a nutrient as shortfall, and further integrating biochemical and health-related data in a systematic and consistent manner within and across the editions of the DGAC Scientific Report are improvements that may enhance the process by which nutrients of (public health) concern are classified. With respect to chronic disease, opportunities exist to create a process or mechanism by which the DGAC identifies new and emerging health outcomes for review. Related to this concept is the integration of biomarkers and surrogate end point data. While such evidence has the potential to strengthen the dietary recommendations for chronic disease prevention, an examination of the validity and appropriate applications of such data is warranted prior to inclusion into the
evidence base. Furthermore, this National Academies committee foresees the creation and use of analytic frameworks to guide topic selection and synthesis and interpretation of evidence as being a valuable addition to the DGAC process. Such an analytic framework would help clarify the purpose of each question, the relationship between questions, what questions are answerable, and what topics need evidence. Finally, this National Academies committee posits that further integrating systems thinking and methods into the DGA process would help to better elucidate mechanisms connecting dietary intake and health outcomes.
REFERENCES
Bailey, R. L., K. W. Dodd, J. A. Goldman, J. J. Gahche, J. T. Dwyer, A. J. Moshfegh, C. T. Sempos, and M. F. Picciano. 2010. Estimation of total usual calcium and vitamin D intakes in the United States. Journal of Nutrition 140(4):817-822.
CDC (Centers for Disease Control and Prevention). 2012. Second national report on biochemical indicators of diet and nutrition in the U.S. population. https://www.cdc.gov/nutritionreport/pdf/nutrition_book_complete508_final.pdf (accessed June 7, 2017).
FDA (U.S. Food and Drug Administration). 2016. FDA facts: Biomarkers and surrogate endpoints https://www.fda.gov/aboutfda/innovation/ucm512503.htm (accessed March 16, 2017).
Hanson, M. A., and P. D. Gluckman. 2015. Developmental origins of health and disease—global public health implications. Best Practice & Research Clinical Obstetrics & Gynaecology 29(1):24-31.
HHS/USDA (U.S. Department of Health and Human Services/U.S. Department of Agriculture). 2005a. Dietary Guidelines for Americans, 2005. Washington, DC: U.S. Government Printing Office. https://health.gov/dietaryguidelines/2005.asp (accessed May 31, 2017).
HHS/USDA. 2005b. The report of the Dietary Guidelines Advisory Committee on Dietary Guidelines for Americans, 2005. Washington, DC: Agricultural Research Service, USDA.
HHS/USDA. 2013. 2015 Dietary Guidelines Advisory Committee first meeting transcript. Bethesda, MD. https://health.gov/dietaryguidelines/2015-BINDER/meeting1/docs/Transcript-Day-2.pdf (accessed May 30, 2017).
HHS/USDA. 2015a. Dietary Guidelines for Americans 2015–2020: Eighth edition. https://health.gov/dietaryguidelines/2015/guidelines (accessed July 18, 2017).
HHS/USDA. 2015b. Scientific report of the 2015 Dietary Guidelines Advisory Committee. Washington, DC: USDA, Agricultural Research Service.
IOM (Institute of Medicine). 2000. Dietary Reference Intakes: Applications in dietary assessment. Washington, DC: National Academy Press.
IOM. 2003. Dietary Reference Intakes: Applications in dietary planning. Washington, DC: The National Academies Press.
IOM. 2005. Dietary Reference Intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids. Washington, DC: The National Academies Press.
IOM. 2010. Evaluation of biomarkers and surrogate endpoints in chronic disease. Washington, DC: The National Academies Press.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. Guiding principles for developing Dietary Reference Intakes based on chronic disease. Washington, DC: The National Academies Press.
USDA. 2008. Diet quality of American school-age children by school lunch participation status: Data from the National Health and Nutrition Examination Survey, 1999-2004. Alexandria, VA: Food and Nutrition Service.
USDA ARS (Agricultural Research Service). 2016. What We Eat in America/NHANES overview. https://www.ars.usda.gov/northeast-area/beltsville-md/beltsville-human-nutrition-research-center/food-surveys-research-group/docs/wweianhanes-overview (accessed July 3, 2017).
USDA/HHS. 2010a. Dietary Guidelines for Americans, 2010. 7th edition. Washington, DC. https://health.gov/dietaryguidelines/2010 (accessed May 15, 2017).
USDA/HHS. 2010b. Report of the Dietary Guidelines Advisory Committee on the Dietary Guidelines for Americans, 2010. Washington, DC: Agricultural Research Service, USDA.
Ward, B. W., J. S. Schiller, and R. A. Goodman. 2014. Multiple chronic conditions among US adults: A 2012 update. Preventing Chronic Disease 11:E62.
Yetley, E. A., A. J. MacFarlane, L. S. Greene-Finestone, C. Garza, J. D. Ard, S. A. Atkinson, D. M. Bier, A. L. Carriquiry, W. R. Harlan, D. Hattis, J. C. King, D. Krewski, D. L. O’Connor, R. L. Prentice, J. V. Rodricks, and G. A. Wells. 2017. Options for basing Dietary Reference Intakes (DRIs) on chronic disease endpoints: Report from a joint US-/Canadian-sponsored working group. American Journal of Clinical Nutrition 105(1):249S-285S.
This page intentionally left blank.






















