4
Fostering Caregiver Well-Being Toward Healthy Child Development
INTRODUCTION
The focus of this chapter is on how to best foster children’s healthy psychosocial development, emotional adjustment, and physical health using what science has shown about risk and resilience among children and families in high-risk contexts. With the goal of systematically addressing inequities, the broad question to address is, “For those children who are at risk for negative outcomes, what can be done—guided by science-based evidence—to expediently and effectively move them toward positive developmental trajectories?” In other words, how can the playing field be leveled so that all children have the best possible opportunity to flourish and thrive in terms of their social-emotional, behavioral adjustment?
This chapter is structured in the following sections. At the outset is an overview of what developmental theory and research has demonstrated about “universals” in child development, beginning with a definition of core concepts in the phenomenon of resilience, followed by descriptions of risk and protective processes that are pervasive across diverse types of life adversities, with large and long-standing effects. Front and center among these universals are positive, supportive relationships and access to other basic and critical resources, such as good nutrition, health care, and early childhood education; these are all essential for developing children and for those charged with their care, and relevant theory and empirical evidence are provided on each. The primary focus is on fostering caregiver well-being and support, family cohesion, and social connections to promote healthy child development. This is reflected in the
most proximal level to the individual child’s development in the report conceptual model (see Figure 1-9). After discussions on these universals, the chapter continues with a consideration of some context-specific pathways to healthy child development: influences that are potent in and unique to particular subgroups of the population. As an example, issues of discrimination and segregation warrant attention for racial, ethnic, and sexual minorities. See Box 4-1 for an overview of this chapter.
The majority of this chapter is devoted to describing intervention programs that carry great promise in promoting positive outcomes among children in high-risk contexts. The focus is on interventions that are well grounded in developmental theory and research; have demonstrated significant improvements with replications; have moderate or substantial effect sizes with a meaningful impact for the population; and, importantly, can feasibly be taken to large scale. Methods used to deliver the interventions, to ensure fidelity (to intervention strategies), and to assess outcomes are described in detail to provide “blueprints” of science-based programs most likely to promote positive outcomes among young children and their caregivers who negotiate challenging life circumstances. For parameters and operational definitions used in this chapter, see Box 4-2.
Resilience
Under the definition of inequities (see Box 4-2) as unequal likelihood of thriving or attaining positive adjustment outcomes over time, the construct of resilience from developmental science is directly relevant to discussions here, as it implies correcting what otherwise might have been negative trajectories given major life stressors. Resilience can be defined as a dynamic process encompassing positive adaptation within the context of significant adversity (Cicchetti, 2010; Luthar et al., 2015; Masten, 2014). By this definition, there are two essential conditions that make up resilience: “a) exposure to significant threat, severe adversity, or trauma; and b) the achievement of positive adaptation despite major assaults on the developmental process” (Cicchetti, 2010, p. 145). With respect to a child’s health, resilience is evident when physical, behavioral, and emotional well-being and development tip toward positive outcomes, even when a heavy accumulation of negative influences or risk factors exists.
Reviewing the body of accumulated scientific literature on resilience and socio-emotional functioning, Luthar et al. (2015) summarize the following core findings:
- Resilience happens across risk and age groups; there will be a subset of individuals who show some positive adaptation.
- Resilience relies fundamentally on relationships, and this is true for children and adults.
- Children’s resilience is shaped by multiple transactional systems (i.e., proximal and distal processes and environments affect the child, and the developing child in turn affects each of these).
- Resilience is not fixed over time but is dynamic; periods of positive adaptation can be interrupted by times of struggles.
Resilience is not a unidimensional construct; among those at risk, successful adaptation in some areas (such as overt behaviors) can co-occur with difficulties in others (e.g., covert anxiety or depression). For information on physiological resilience and variability in susceptibility, see Chapter 2.
As noted above, there are important considerations for the context within which a child exists and how that environment affects resilience. As is true for all children—facing adversities or not—the developing child’s lived experience is shaped by the family, caregivers, community, and systems that the child interacts with on a daily basis. Reis et al. (2000) identify four propositions to describe this phenomenon: (1) from conception
forward, individuals exist within the context of their social relationships; (2) each relationship is nested in a social and physical environment system; (3) each relationship is embedded in larger societal and cultural systems; and (4) all of these systems are continuously changing and interacting with each other over time. For these reasons, taking a multilevel, transactional, and relationship-centered approach to understanding resilience and its determinants for children is important (Luthar et al., 2015; Reis et al., 2000).
Of particular salience and proximity are family-level influences of relationships on resilience in childhood, as will be described in detail within discussions that follow. While risk factors such as exposure to significant adversity often unfold within the context of the family, so too do the protective factors that have been shown to foster resilience, such as parental warmth, responsiveness, and sensitivity (Hamoudi et al., 2015). Therefore, the parent or primary caregiver is a major target for interventions to promote resilience in children.
Across socioeconomic strata and in most parts of the United States (and the world), the primary caregiver is generally the mother or a mother figure. It is certainly true that in general, it is better for children to have two parents in the home to share the responsibilities of child care and running the household. At the same time, even when there are two co-residing parents, one typically shoulders most of the child care, and this is generally the mother (e.g., see Ramey and Ramey, 2010). However, it should be clarified that in the discussions that follow, the term “mother” is used as a proxy for the primary caregiver who is a woman—whether that is the biological mother, grandmother, older sister, or other female relative. Considerations around men and fathers as primary caregivers are discussed separately later in this chapter, as the literature clearly indicates that there are distinct needs and issues that warrant specific, careful attention in interventions for men.
The critical importance of the parent–child relationship, specifically, is underscored in a 2017 special section published in Child Development, which highlights evidence-based interventions to maximize resilience in children and families. In their overview article, Luthar and Eisenberg (2017) outlined the key findings and recommendations that emerged from the collection of papers. Across these 11 papers, the single theme that most consistently recurred was the need to support the well-being of the primary caregiver—typically the mother. Contributing authors emphasized the importance of psychological and emotional support for mothers, particularly for single mothers (Taylor and Conger, 2017), those struggling with depression (Goodman and Garber, 2017), those at risk for maltreating their children (Valentino, 2017), and those living in poverty (Morris et al., 2017). A second important target for intervention identified from this set of articles was specific types of parenting behaviors that
most urgently warranted attention among at-risk families. It was particularly important to minimize harsh, rejecting, or neglectful parenting behaviors (e.g., Goodman and Garber, 2017; Harold et al., 2017; Reynolds et al., 2017), because the ill effects of maltreatment on children can be profound, pervasive across areas of adjustment, and long-standing, especially when it starts early in development and is prolonged. A third target area identified as beneficial for interventions was self-regulation and coping skills among adults—parents and teachers—as well as children (e.g., Domitrovich et al., 2017; Modecki et al., 2017; Morris et al., 2017; Smith et al., 2017). Promoting self-regulation and coping for both the parent and child is essential because parents are likely to adjust their parenting behavior based on their children’s behavior. Of course, for all parents living in challenging circumstances, there needs to be attention to not only their personal well-being and parenting but also the social and economic conditions that provoke the toxic stress response (discussed later in this chapter in the section on group difference).
HUMAN DEVELOPMENT IN THE CONTEXT OF RELATIONSHIPS
This chapter and the associated conclusions and recommendations are based on what is known from extant scientific literature about the major, critical building blocks to optimize the child’s development from pregnancy through puberty (approximately 8–10 years of age). Sections that follow begin with a synthesis of this literature providing the basis for what are considered the universal principles of human child development, that is, principles that are largely generalizable to most children and families in the United States. Following this is a discussion of instances where children and families in discrete subcultural groups have important, unique needs, given the presence of potent risk or protective processes in their particular contexts. The remainder of this chapter is focused on a review of interventions that have been proven to be effective to promote relational supports and well-being of caregivers toward maximizing resilient adaptation.
Universals of Human Development
Universals: The Interplay of Biology and Environment in Human Development
As described in Chapter 2, during prenatal development, genetic and environmental factors work together to build organ systems that promote the ability of the individual and species to thrive and survive (Center on the Developing Child at Harvard University, 2010; National Scientific Council on the Developing Child, 2010). It is an evolutionary conserved
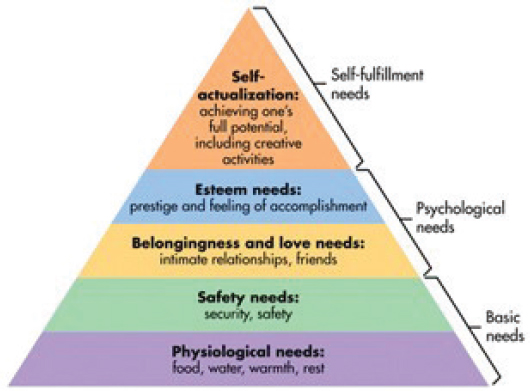
NOTE: Concepts from Maslow, 1943.
SOURCE: McLeod, 2018.
core principle that prenatal through early childhood development is both experience dependent and experience expectant.1 Thus, the adaptability of the organism to future challenges is influenced substantially by genetic and epigenetic factors that contribute to homeostatic boundaries within which the brain and other organ systems operate over the life course and the experiences that occur during development that the organism anticipates as the “future” contexts in which it will need to operate to survive and thrive. This core principle relates to both physical survival, which Maslow’s (1943) hierarchy of needs indicates is the most basic need for all humans (children and their caregivers), and relationships that contribute to physical and behavioral well-being. See Figure 4-1 for Maslow’s hierarchy pyramid.
All human circuits are built from the bottom up, with simple skills forming the foundation for the emergence of more complex skills (Center on the Developing Child at Harvard University, 2011). For sociability, the interaction between humans starts after birth, but the initial circuits
___________________
1 “Experience dependent” describes the aspects of development that depend on the quality of the environmental input (e.g., while babies are born with a capacity for language development, their ability to communicate verbally will depend on their exposure to language during early development). “Experience expectant” describes the normal, generalized development when the environment provides infants with the needed input to develop neural connections that enable function in certain domains (such as vision and hearing). If input during these critical periods of development is not received, these functions will be lost permanently (Gallagher and Nelson, 2003).
needed to direct interactions that are fundamental to early development, such as caregiver–infant attachment, are established prenatally. Infants are ready to use their senses to attend to environmental stimuli—what they hear, see, smell, feel, and taste—to receive the most important information that supports their immediate internal needs, such as hunger, thirst, and arousal (Hammock and Levitt, 2006). In essence, early experiences drive a process in which the motivation and attention circuits focus more and more on those stimuli that are most meaningful—a process known as contingent learning. Building these circuits occurs in a social context with the primary caregiver and others, providing key opportunities for the infant to associate stimuli with social meaning. Over time, as social context becomes more and more complex, the developing child engages cognitive and emotional regulatory processes to infer social meaning and ultimately, social responsiveness to cues—back and forth or “serve and return” interactions (National Scientific Council on the Developing Child, 2004). These skills develop over an extended period, through adolescence (Casey et al., 2016; Dahl, 2004).
There are extended discussions pertaining to the importance of all children having their basic needs met and the existing problems that place children and families at risk, including those related to access to adequate housing, good nutrition, and health care (along with the associated barriers, ranging from parents’ inability to take time off of work and lack of transportation to logistical problems deriving from the spread of critical services across physical locations and delivery systems). These issues are discussed extensively in Chapters 3 and 6.
Universals: Development in the Context of Proximal Family Relationships
The focus of this chapter is the next most basic need in Maslow’s (1943) hierarchy: belongingness and love. To set the foundation for the committee’s discussions on this topic, the following section outlines nine committee-generated, universal principles of human development that are derived from the scientific literature on child development in the context of relationships. To reiterate, these principles all pertain to the broad domain encompassing children’s psychological and behavioral adjustment. See Box 4-3 for a list of the nine universal principles of human development.
The first principle, deriving from more than eight decades of research on resilience, is the following, mentioned earlier: For all children, the single most important factor in promoting positive psychosocial, emotional, and behavioral well-being is having a strong, secure attachment to their primary caregivers; in most instances, this is their biological mother. This conclusion makes good sense intuitively, as it is the primary caregiver who is the most constant and proximal person who has everyday contact with the young child
and long-standing influence on the developing child from conception through late childhood. In most settings, this is typically the mother (relationships with fathers are also extremely important, and are discussed below). Even in families where they are employed outside the home, across socioeconomic contexts, it is typically mothers who have the earliest, most constant, and most prolonged everyday contact with the child. However, it should be noted that even when the primary caregiver is another adult, the universals that are described here would largely generalize to these other main caregivers (with a few exceptions that are discussed explicitly). See Box 4-4 for discussion of gender specificity.
Following this first universal—that a strong attachment to primary caregivers is critical for the child’s well-being—the second major universal is that this strong attachment presupposes effective parenting behaviors in everyday life, and “effective parenting” changes in nature and complexity and with development over time. In infancy, parenting is extremely demanding
on physical energy, and, of course, on sleep; at a psychological level, it calls for sensitivity to the child’s needs and appropriate responsiveness (e.g., soothing/comforting when the child is in discomfort or pain). Often, parents are physically exhausted and not sure about how to soothe a baby who might cry inconsolably for hours. As children grow into the toddler years, in addition to providing love and comfort, effective parenting calls for constant vigilance and appropriate limit setting. During the toddler years, children are physically very mobile, oblivious to physical dangers (e.g., sharp objects or electrical outlets), increasingly and energetically willing to explore the world around them, rarely responsive to a simple “no” from adults, and prone to tantrums. The use of language as a mediator of appropriate parent–child interactions becomes increasingly complex and important. In early childhood through the onset of kindergarten and formal schooling, in addition to the primary caregiver providing love and comfort and appropriate, consistent limit setting at home, a new developmental task for the child—and thus for that caregiver—is adjustment to external influences. This subsumes the transition to child care and then to kindergarten with separation from the primary caregiver and learning
to handle routines and a new set of socializing influences, including other adults plus children. During the elementary school years, failures and successes in various areas—academics, peer relations, sports, or other specialized arenas—need to be processed at the socio-emotional level. Peers and others adults can provide support to children and parents as they navigate increasingly diverse and demanding contexts.
The third universal is that effective parenting presupposes the caregivers’ own well-being. Being able to deal with the various tasks and demands of parenting is difficult at the best of times, and this becomes particularly challenging in the presence of high levels of life stress. Chronic exposure to poverty or prolonged periods of limited resources, as well as life events involving high levels of trauma, can lead to maternal depression, anxiety, and other mental health problems, which in turn can greatly compromise the quality of parenting. There are multiple studies showing that when mothers struggle with mental illness, this can significantly affect all of their parenting behaviors (Knitzer, 2000; Luthar and Sexton, 2007; Rahman et al., 2013). In particular, maternal depression and high stress have been linked consistently with tendencies to neglectful or harsh parenting, increasing the likelihood of the child’s exposure to adverse child experiences (ACEs) (Goodman and Garber, 2017; Plant et al., 2013; Toth et al., 2013; Valentino, 2017). Another important psychological element of effective parenting is parent agency or self-efficacy (i.e., the parent’s perceived ability to influence the development of the child) (Jones and Prinz, 2005). The report Parenting Matters: Supporting Parents of Children Ages 0–8 highlights parent self-efficacy as a contributing factor in shaping parenting competence and child self-regulation, social, and cognitive skills (NASEM, 2016). The report identifies one possible mechanism for this association as increased competence-promoting parenting practices (e.g., family routines or involvement with children in schools). As the current report’s conceptual model in Chapter 1 suggests (see Figure 1-9), caregivers and families live in the context of their social circumstances and living conditions; therefore, they need support in coping with related stressors or eliminating such sources of stress, in addition to efficacy-promoting supports.
The first three universals have been long cited in the developmental literature; the next has been more recently emphasized explicitly: from as early in a child’s life as possible, it is critical to ensure that mothers have the necessary supports for maintaining good mental health and psychological well-being. Resilience researchers have clearly articulated that in order to achieve positive mental health and functioning, the same principles that apply for children apply to their mothers. Just as children need ongoing unconditional love from their mothers, so do the mothers need ongoing love and support from other adults to function well across their life roles
(Luthar et al., 2015). In developmental science, for too many years, the tendency in studying families has been to discuss what parents should do and should not do, with little attention to what it is that allows parents themselves to function well and develop resilience at this daunting, decades-long task. In other words, what has been missing is mothers’ well-being as the dependent variable.
In the past few years, this has changed (see Balaji et al., 2007; Jolly et al., 2014; Luthar and Ciciolla, 2015; Taylor and Conger, 2017). There is now much more explicit emphasis on the need to understand what helps mothers do well over time, especially in highly stressful life circumstances. With accumulating evidence from both basic research and intervention trials, the answer is clear: the single most important need is dependable supports in their role as parents—emotional/intangible and tangible—from a dependable, reliable network of others in their lives (for a review on this topic, see Luthar and Eisenberg, 2017). The nature of these supports, furthermore, is both perceived (e.g., the expectation that comfort will be available when distressed or help will be forthcoming if needed for parenting/running the household) and instrumental (e.g., actual receipt of help with child care or aspects of running the home; see Balaji et al., 2007; Goodman and Garber, 2017, for more information). See Box 4-5 for more on supporting caregivers.
A fifth universal, and also one more recently emphasized specifically in the literature, is that if there is any concern about a parent “faltering,” the single most important dimension of parenting in which parents need to be helped is maltreatment (by parent figures or others).2 In general, psychologists have shown that “bad is stronger than good” (Baumeister et al., 2001); that is, the ill effects of harsh behaviors are much stronger than the positive effects of praise (see also Fredrickson and Losada, 2005; Sparks and Baumeister, 2008). Additionally, the accumulated literature on resilience has shown that early and chronic maltreatment is the one category of adversity in which it is rare to find children who “do well” over time, showing little to no trouble across major adjustment domains; in fact, this has many serious long-term effects across salient aspects of child development (see Bolger and Patterson, 2003; Cicchetti, 2013).
Therefore, as a society, prevention of maltreatment needs to be a top priority in promoting the well-being of children in high-risk contexts. This again implies attentiveness when primary caregivers are stretched too thin, because they are at the most risk for maltreatment. As noted earlier, living with chronically high stress or mental illnesses, such as untreated depression, can lead the most well-meaning and loving parent to become angry and slip into neglectful or harsh parenting behaviors. If caregivers are believed to be at risk for abusing or neglecting their children—or of not being able to protect them from maltreatment by other adults—the situation needs to be treated as urgent and the appropriate help identified. Most importantly, the best help would be providing supports and/or mental treatment for the primary caregiver to address the root cause of maltreatment or neglect (Cicchetti, 2013; Cicchetti et al., 2006; Lieberman et al., 2005; Luthar et al., 2007; Toth et al., 2013). In the most extreme cases, continued high risk for maltreatment or actual maltreatment could entail removing the child from the home; however, there is evidence that suggests that this is not always the best course of action for the child (Toth et al., 2016).
Implicit within the above universals is that the well-being of the young child inherently involves the well-being of the primary caregiver; in fact, Seifer (2003) explicitly pointed out that it does not make sense to think about resilience of infants. Rather, we should consider the positive functioning of the mother–child dyad. Additionally, in many countries other than the United States, people think about the needs of the child through the needs of the caretaker: if the child is to be helped, that help is most effectively offered if it goes through the caretaker (e.g., see Hrdy, 1999).
___________________
2 The Centers for Disease Control and Prevention (CDC) defines child maltreatment as any type of abuse (e.g., physical, sexual, or emotional) and neglect of a child under 18 years of age by a parent, caregiver, or another person in a custodial role (CDC, 2014).
In many cultural contexts, pregnancy, childbirth, and motherhood are embedded in a system of multiple generations of women who provide support and troubleshooting to the younger generations in all aspects of caretaking. Extended family systems and/or fictive kin are available and ready to help with any problem that arises; they affect the development and well-being of the child and also the mother (see Barlow and Chapin, 2010; Kopp, 2013).
To reiterate the caveat noted earlier—that in many instances, it may not be the mother but another family member (or caretaker) who serves as the primary caregiver—the principles described above are still the same; that is, whomever is charged with primary (or salient) responsibility of taking care of the young child needs to receive regular replenishment and support. Child care providers and educators also need ongoing support, including teachers from preschool onward through the K–12 system. These are all jobs that are among the lowest paid and with high levels of burnout and turnover, especially for early childhood educators. Once again, research has shown that these care and education professionals can serve critical protective functions, stepping in to provide the nurturance and support that complement or supplement what mothers, fathers, or other primary caregivers are able to offer. Yet, solutions rarely consider what it is that can and should be done to help replenish these professionals who are the primary adults during significant portions of children’s daily lives. (For a more in-depth discussion of early care and education [ECE] professionals, see Chapter 7.)
Sixth, developmental research has clearly shown that relationships in the early childhood years are critical in shaping subsequent child development—but at the same time, there remains much room to change course and impact these trajectories in a positive fashion, with those starting out as negative changing to be more positive as well as the reverse. Without question, early attachments form the lens through which subsequent relationships are viewed (Lieberman et al., 2005; Sroufe et al., 2005; Yates et al., 2003; Zeanah and Zeanah, 1989), so that children with adverse early experiences are less likely to be open to or trusting of other nurturing people in their lives. Yet, there are certainly opportunities for reversals (e.g., at times of transition in life, including moves to new schools for children, and, later in life, marriage or employment changes). Many years ago, Rutter (1987) showed that women who were institutionalized as children were more likely to display positive parenting themselves if they married supportive spouses, and Sampson and Laub (2003) showed that for delinquent children followed over decades, both marriage and entry into the military conferred significant benefits to their well-being and adaptation. In short, even if subjected to early trauma, human beings are capable of recovering and healing.
The seventh universal principle is that the ill effects of toxic early environments (e.g., unhealthy relationships) can manifest in physical health problems in childhood and throughout life. Common health problems include asthma, headaches and backaches, and even elevated risk for heart disease and compromised immune functioning (e.g., Dong et al., 2004; Dube et al., 2009; Kalmakis and Chandler, 2015; Purewal et al., 2016; Wing et al., 2015). Therefore, once again, preventing exposure to such toxic experiences is of the essence, even if children appear to be adapting well behaviorally or psychologically to these adverse circumstances in their early years of childhood.
In a related vein is universal number eight: The ill effects of early childhood adversities (e.g., abuse or neglect by caregivers) can become most visibly apparent later in life (i.e., there can be latent or “sleeper” effects that are seen at later points in development). (See Chapter 2 for more information on sleeper effects.) For example, attachment insecurities developed in infancy could manifest in severe separation anxiety from the parent on starting kindergarten or significant difficulties in relating well with peers (Cicchetti and Toth, 2015, 2016). Other examples include behaviors that become relevant or salient closer to puberty or adolescence, such as delinquent behaviors or abuse of drugs and alcohol as a function of early relationship disturbances (Cicchetti and Toth, 2015, 2016). Perhaps the most obvious example is impaired parenting as adults; in general, there tends to be some intergenerational continuity of maltreatment (Adams et al., 2019; Cicchetti and Rizley, 1981; Kaufman and Ziegler, 1987; Pears and Capaldi, 2001; Rutter, 1987).
Universal nine—biology is not “destiny;” rather, while indicating relative risk rates, it sets “confidence limits” within which environmental influence can lead to relatively positive versus negative adaptation. Genetic factors, for example, can heighten children’s vulnerability to disorders (physical and psychological) that afflict their parents. At the same time, intergenerational transmission of disorders is far from inevitable. As noted earlier, the notion of resilience encompasses the phenomenon wherein children who are at risk for psychopathology—or mothers who are at risk for negative parenting behaviors—can show healthy outcomes if they have the appropriate corrective or buffering influences in their lives. In other words, biological factors affect children’s development, but they always operate in interaction with forces in the environment (Wise, 2009). The burgeoning field of epigenetics has shown that early life environments can lead to long-lasting changes in gene expression that “can leave indelible chemical marks on the brain and influence both physical and mental health later in life even when the initial trigger is long gone” (Murgatroyd and Spengler, 2011, p. 1; see also Dudley et al., 2011; Lerner and Overton, 2017; and Chapter 2 for more information).
To summarize, there are key take-home messages from the above discussion of universals to ensure positive psychological, behavioral, health, and social outcomes in early childhood. First, ensure the psychological well-being of the primary caregiver, as this will inevitably affect his or her parenting and the quality of attachment; this is best done by ensuring ongoing support for mothers in their everyday lives and communities (support during the child’s early infancy will not protect the mother for the child’s entire life). One population of particular importance for intervention is mothers under a high level of chronic stress and at risk for depression as this is strongly related to increased risk for neglect and maltreatment, which, of all parenting behaviors, are the ones that most urgently require prevention. Finally, in considering whether a child or parent has done well in spite of early adversities, it should be noted that ill effects of these adversities can become manifest later in life. At the same time, significant healing can happen, even well past childhood and adolescence, so that mothers who experience suboptimal care themselves as children can be effective caregivers if they receive appropriate support and help as they negotiate the challenges of motherhood.
Fathers
For the most part, this chapter has focused on mothers (or mother figures) because across cultures and socioeconomic settings, they are typically the primary caregivers of young children (e.g., Hrdy, 2011; Luthar and Eisenberg, 2017); however, there are many instances where fathers are primarily responsible for raising children. This section reviews the importance of fathers for children’s development. Following this, the extant evidence on interventions with fathers is reviewed and future needs are discussed.
While some research shows that fathers experience exclusion regarding parental involvement in child health and development (Plantin et al., 2011; Steen et al., 2012), there is empirical evidence that suggests they have an integral role in promoting the health and well-being of their children.
Some evidence points to a direct relationship between fathers and specific childhood outcomes. For example, research suggests that father education and supportiveness shapes language and cognitive development in children (Cabrera et al., 2007). Furthermore, varying levels of father involvement or connectedness with children are associated with differential self-regulation and aggression in children (Vogel et al., 2006). One study has even found that positive father–child relationships, as reported by fathers, are protective from pediatric injury (Schwebel and Brezausek, 2010). In terms of father well-being, paternal depression has been associated with increased odds of child neglect (Lee et al., 2012).
Other evidence suggests an indirect pathway by which fathers can influence their children’s well-being—through their mothers. Bloch et al. (2010) found that poor-quality relationships between fathers and mothers are associated with depressive symptoms, stress, substance use, and smoking among low-income mothers. Other research indicates that father involvement has a positive association with a mother’s health behaviors (e.g., seeking prenatal care in the first trimester, abstaining from drinking, drug use, and smoking) (Teitler, 2001). Finally, fathers can support maternal well-being and birth outcomes. For mothers, a supportive relationship with the father can have buffering effects on maternal depression and preterm birth (Giurgescu et al., 2018).
Involving Fathers in Preventive Interventions
As noted earlier in this chapter, developmental scientists have increasingly emphasized that it cannot be presumed that what helps fathers do well as parents is the same as what most benefits mothers (e.g., Grusec and Davidov, 2010). To illustrate, Lamb and his colleagues have shown that fathering can be more affected by the quality of the marital relationship (levels of satisfaction and support) than is mothering (see Lamb, 2004; Lewis and Lamb, 2003). Accordingly, it is important to attend to the gender-specific needs of parents in designing strategies to recruit and retain them in prevention programs related to their families and children (Pruett et al., 2017).
Cross-national interventions further attest to the critical importance of attention to gender-specific needs of parents. Randomized trials with families affected by HIV indicated that across countries (South Africa, Thailand, and the United States), men were more likely to respond to stress with flight-or-flight responses and women with tending and befriending (Rotheram-Borus et al., 2011). Accordingly, there have been efforts to design interventions to accommodate these gender differences in both delivery formats and activities. Community-based “mentor mothers,” for example, were most beneficial for mothers seeking help via interventions,
whereas men were more likely to be engaged via group activities, such as sports or vocational training. Similarly, Cabrera et al. (2015) note that fathers may be more willing to participate in a “game of basketball” than the “morning coffee” that many early childhood programs offer, and they recommend running support groups for “fathers” rather than just for “parents,” sending the message that the role of a father is valued and is supported, independent of support to mothers.
In their review of existing programs for fathers, Pruett and colleagues (2017) indicate that whereas it is generally more difficult to engage fathers than mothers in preventive intervention programs, there are some avenues that seem promising. These include efforts to recruit fathers along with mothers via couples’ work in early childhood (i.e., while the father is still involved with the mother and child before any possible estrangement, as it is much more difficult to engage fathers when strife has entered the inter-parent relationship). Pruett et al. (2017) also suggest focused efforts to make the facilities themselves more “father friendly” (e.g., by addressing implicit biases of staff that fathers will intrinsically be uninvolved and portraying pictures of fathers with babies in the program facilities). At the most basic level, other approaches would be to highlight in the media those men who are positive role models of fatherhood early in life and even bring such individuals to high schools to talk with young men on this topic, well before they become fathers.
Davison et al. (2019) examine strategies for and barriers to father engagement in early obesity prevention during the child’s first 1,000 days of life. The review finds that although obesity prevention programs have great potential to engage fathers, there are a number of micro- and macro-level barriers that hinder access and participation. Applying a policy, systems, and environmental perspective, the authors recommend the following strategies to enhance father engagement: integrate father-engagement standards into national practice guidelines (e.g., American Academy of Pediatrics, American College of Obstetricians and Gynecologists), develop educational and marketing materials (e.g., pamphlets) specific to fathers, and partner with local father advocacy organizations to identify new strategies to engage fathers. Other research has homed in on preconception (Kotelchuck and Lu, 2017) and pediatric care (Yogman and Garfield, 2016) as important platforms for engaging fathers.
What is clear is that speaking about promoting good parenting in gender-neutral terms will likely be a disservice to both fathers and mothers. The literature clearly delineates what mothers need most centrally to function well as mothers (again, aside from basic necessities for physical survival): authentic connections with and support from others in their everyday lives. Relationship-based strategies that are highly effective, such as those in home visiting programs for new mothers, will not
necessarily generalize to new fathers, paving the way to their enhanced mental health, positive fathering behaviors, and attachment to the child. For example, in low-income African American families, mothers responded well to the tend and befriend approach; however, the recruitment of biological fathers was more likely through opportunities for enhanced earnings to support their families (Jackson, 2015). Much more work is needed, therefore, on ascertaining how best to engage fathers and retain them in prevention and intervention programs.
It is important to note that the National Institutes of Health (NIH) changed their policies about gender inclusion around the 1990s, when there was a concerted move to include women in intervention trials. The NIH Office of Research on Women’s Health was formed in 1990
in response to congressional, scientific and advocacy concerns that a lack of systemic and consistent inclusion of women in NIH-supported clinical research could result in clinical decisions being made about health care for women based solely on findings from studies of men—without any evidence that they were applicable to women. (Mazure and Jones, 2015)
As researchers and practitioners think of how best to promote the wellbeing of young children via effective support for their primary caregivers, it would be prudent to avoid presuming that we can simply transfer program strategies and procedures from mothers to fathers. Although instances where a father is solely responsible for the child are not as common, this in no way obviates the need for understanding the most effective paths to reach and benefit these fathers. One evidence-based program that provides an avenue to reach fathers along with mothers is the Family Check-Up (FCU) program (see Box 4-6 for a description of FCU as a promising model).
Reviews of past national-level efforts targeting fathers further attest to the importance of further work in this area. As Lu and colleagues (2010) have noted, many fathers in the United States face substantial barriers to staying involved in their children’s lives, and this is especially the case for many low-income fathers and men of color. These barriers operate at multiple levels, including intrapersonal (e.g., poor knowledge, attitudes and behaviors toward parenting) and interpersonal (e.g., strained relationship with the mother or maternal grandmother), neighborhoods and communities (e.g., high unemployment and incarceration rates, which influence social norms), cultural or societal (e.g., popular cultural perceptions of black fathers as expendable and irresponsible, racial stratification and institutionalized racism), policy (e.g., the “marriage penalty” within Earned Income Tax Credit [EITC] and Temporary Assistance for Needy Families [TANF], child support enforcement), and even historic (slavery and forced family separation among African Americans
and forced removal of American Indians from their land) (Lu et al., 2010). Life course factors, such as ACEs or the absence of the father’s father growing up, can also influence father involvement. As discussed in the next section, institutionalized racism against men of color leads to higher rates of incarceration that precludes many fathers from being present in their children’s lives, establishing healthy relationships, and providing the necessary support to the mother.
In recognition of both the importance of fathers for child development, and the challenges fathers face, Congress has authorized and funded grants for fatherhood programs for more than a decade. Evaluation of
four federally funded Responsible Fatherhood programs from 2011 to 2018 has yielded mixed results (Avellar et al., 2019). All four programs consisted primarily of group-based workshops covering topics such as the meaning of fatherhood, child development, co-parenting, finding and retaining employment, and even personal development topics, such as coping with stress, responding to discrimination, problem solving, self-sufficiency, and goal planning. Participation in the programs resulted in improved parenting, specifically their self-reported nurturing behavior and engagement in age-appropriate activities with children, but not in-person contact, financial support, co-parenting, earnings, or socioemotional and mental well-being (Avellar et al., 2019).
One possible explanation for the mixed results is that most extant fatherhood programs still do too little, too late. Men’s capacity to support and nurture others needs to be cultivated over their entire life course, not only after they become fathers (Lu et al., 2010). This includes their capacity to form stable, positive relationships; as discussed throughout this report, this depends on the presence of a stable, nurturing relationship with a caregiver during their own early childhood. Thus, future research on father involvement needs to take a more integrative life course approach, studying how boys become men, men become fathers, and how we as a society can better nurture the development of fatherhood across the life course.
Future fatherhood programs also need to go beyond affecting individual knowledge, attitudes, and behaviors toward changing the family, neighborhood, social, and cultural contexts of fatherhood. Public policy changes to remove barriers—such as the “marriage penalty” within EITC and TANF, making child support more “father friendly” by calculating payment based on actual earnings, adjusting and forgiving arrearages, and allowing a greater amount of the child support payment to be passed through to the child—can go a long way toward strengthening father involvement. Micro- and macroeconomic policies to reduce poverty and strengthen fathers’ capacity to contribute financially to the family can also help. Most importantly, fatherhood initiatives, if they are going to succeed in advancing health equity, need to have a core objective that addresses institutionalized racism in employment, education, housing, health care,
criminal justice, and other systems that keep many low-income fathers and men of color from living out their true potentials in our society.
The Role of Culture as Context
Anthropological perspectives on the study of children’s development, pioneered by Margaret Mead, John and Beatrice Whiting, Robert A. Levine, and others, emphasize the importance of the cultural context that embeds children, families, and institutions that are important determinants of children’s development. Subsequent elaborations by Super and Harkness (1986) labeled these influences as the “developmental niche.” The developmental niche consists of “(1) the physical and social settings in which the child lives [micro systems in Bronfenbrenner’s (1979) work], (2) the culturally regulated practices of child care and child rearing [that exist in all microsystems, including family, education, and health care settings], and (3) the psychology of the caretakers” (p. 552). They expand as follows:
Regularities in the subsystems, as well as thematic continuities from one culturally defined developmental stage to the next, provide material from which the child abstracts the social, affective, and cognitive rules of the culture, much as the rules of grammar are abstracted from the regularities of the speech environment. The three components of the developmental niche form the cultural context of child development. (Bronfenbrenner, 1979, p. 552)
More recent formulations have refined these initial theoretical postulates to articulate more specifically how culture permeates the settings that children navigate and how they impinge on development. Rogoff (2003), Vygotski (1978), and Weisner (2002) describe culture as embedded in daily routines and interactions by which the child is enculturated into patterns of behavior, language/communication, and cognitions. A recent revision of Bronfenbrenner’s bio-ecological model emphasizes how settings or microsystems through social interactions, daily routines, space, and other resource allocations enact on a daily basis cultural belief systems that may or may not align on behalf of the children’s development (Vélez-Agosto et al., 2017). Service providers and caregivers need to be cognizant that practices that may be perceived or interpreted as harmful by other groups are embedded within a complex cultural system with its own deeply embedded logic. (See the section on Cultural Considerations for Subgroups for specific examples.) For that reason, cultural differences
need to be accepted, incorporated, or renegotiated as part of interventions and educational efforts. Traditional cultural practices, as unfamiliar as they might seem for some, might be sources of strengths and resilience.
Subgroup Differences
Although there are universal processes of development that point out the importance of the quality of intimate family relationships for early child development, there can also be powerful influences that are largely unique to particular contexts; these potent within-group processes can affect children in both positive and negative ways. Considering the former, for example, specific processes have been identified as strengths or natural coping mechanisms that foster resilience within particular racial or ethnic groups, such as familism and respect for family obligations among Latinos and other collective-oriented cultures and effective family racial/ethnic socialization. Familism and family obligations provide the bases for family members to be involved in crisis management and the daily needs of mothers and children. Racial socialization provides children of color with an age-appropriate understanding of how racism operates and instills strengths and coping mechanisms based on positive and strong ethnic pride and identity. At the same time, these family contexts can place unique demands on children and families and lead to obstacles if they are not understood or accepted or are undermined by the majority culture; unintentionally, they might contribute to the emergence of health disparities very early in life.
This section describes subgroups in which there are specific, unique risk and protective factors that can affect the quality of parent–child relationships and the child’s development; these need to be taken into account as interventions are designed to address health disparities. It should be emphasized here that ensuing discussions of subgroups does not imply that “all are the same” within them. There is invariably great heterogeneity between individuals and families within each subgroup, and it is important to recognize this, particularly in the design and implementation of interventions. Furthermore, while there may be unique risk and protective factors ascribed to these groups, the existing intervention research does not provide one-size-fits-all approaches to guide programs and policies working to serve these subgroups. These subgroups can differ from mainstream groups due to a variety of reasons, including
- Differential access to critical health-promoting resources (e.g., families not having access to safe housing and neighborhoods, preventive care, appropriate educational opportunities);
- Cultural differences due to language (e.g., non-English speakers in a monolingual English environment), religious background (e.g., Muslims), or recent migration;
- Chronic stress (e.g., groups in poverty struggling to meet basic needs, such as shelter and health care, and those facing excessive pressures to achieve, usually in well-educated affluent communities); and
- Discrimination (e.g., racial or ethnic discrimination, homophobia, or discrimination against gender-atypical people [see Box 4-7 and the section on lesbian, gay, bisexual, transgender, queer [LGBTQ] youth and families]).
Children Living in Poverty: Meeting Basic Needs
As noted earlier, the most fundamental needs in Maslow’s hierarchy are related to physical survival; when parents struggle to have their basic human needs met—for shelter, food, and health care—all in the family are at risk. Parents who are preoccupied by fulfilling basic needs for themselves and their children inevitably find it challenging to attend to their children’s emotional, behavioral, and educational needs. Living in poverty is stressful on parents and can compromise the quality of their parenting behaviors, the evolving parent–child relationship, and the wellbeing of their developing children.
As discussed in Chapter 3, one of the most studied and documented factors that affects children adversely is living in poverty (Evans, 2004). Beyond physical survival, chronic poverty places children at risk because the physiological, safety, relational, self-esteem, and self-actualization needs—including those of the parents and the child—are all jeopardized; all of these need to be minimally fulfilled to prevent health disparities.
Low socioeconomic status (SES) and parental education are associated with limited access and use of critical health-promoting resources, and they contribute to psychological distress and physical health disparities. Research has consistently shown that poverty creates living conditions that negatively affect parenting and the mother–child relationship. The daily stresses associated with living in poverty lead to higher incidence of maternal depression, which, as noted earlier, is linked with a poorer quality of mother-infant interaction (Jackson, 2000; Taylor and Conger, 2017). Similarly, poverty has been linked to less capacity for parenting in a consistent and loving way, because it creates high levels of psychological distress that interfere with successful parenting (Conger and Conger, 2002; McLoyd, 1990). Families living in poverty with young children represent one of the most at-risk populations for health disparities, and programs and policies targeting them (see Chapter 6 for more on economic, food, and housing security) within a prevention and early intervention framework should be a priority for our nation.
Cultural Considerations for Subgroups
Other groups whose family relations might be at risk are those whose cultural background (i.e., lack of familiarity or congruency with the dominant North American culture and language) limits their access to critical health-promoting resources or can become an obstacle as they operate with daily practices and routines that are different from that dominant culture. For example, a limited grasp of the English language might impede a parent’s consideration of high-quality early intervention or preschool programs (Moss and Puma, 1995). They might also espouse different family constellations (e.g., where grandmothers are very involved in caretaking); these other adults might interfere with their family operations, as might external influences, such as educators or health care providers.
Differences in acculturation among family members can also be sources of risk and resilience for families of immigrant backgrounds or members of other nondominant cultures. It has been observed that as children acculturate more than their parents (i.e., become more familiar with dominant North American culture and language), there is more conflict between parents and children (Schwartz et al., 2012). In addition, children might assume parenting tasks, such as taking on adult roles, negotiating school systems, and communicating with other officials for services (e.g., driver’s licenses and bank accounts) for their parents.
The evidence on the effects of these added responsibilities on the children’s development, so-called family obligations or brokering, is mixed: in some contexts, they might be burdensome, while in others they seem
to be protective (Dorner et al., 2008; Fuligni and Pedersen, 2002). When taken to extremes and in developmentally inappropriate ways, however, taking on these roles is unhealthy for children. In recent years, the increased number of parental deportations and separation of parents and children at the southern U.S. border has led to an increasing number of children of immigrant background being traumatized and pushed into developmentally inappropriate parenting roles, which will lead to increasing relationship disturbances and subsequent health disparities (Bouza et al., 2018).
In other instances, traditional cultural practices that are appropriate in their original context clash with mainstream North American institutions, and these cultural practices inadvertently place children in at-risk pathways and contribute to problems in family relationships. As an example, many societies (i.e., Japanese, Korean) do not use direct verbal communications with infants and young children. Yamamoto and Li (2011) have shown that some preschools make Asian American students feel inadequate because their quietness, a desirable trait in their home culture, is considered a “problem” in the preschool environment. By contrast, acknowledging and fostering bicultural competencies in families, children, and service providers offers a good foundation for fostering early development in diverse populations (Ho, 2015; Padilla, 2008).
Finally, as presented in Chapter 3, discriminatory practices by systems, institutions, and the population at large can affect family relationships. Cultural mistrust from years of oppression from dominant groups, such as those experienced by African Americans, American Indians/Alaska Natives (AIs/ANs), and immigrants of various races and nationalities in this country, might interfere with family functioning. Cultural mistrust can be transmitted intergenerationally, as promoting mistrust has been identified as a particular type of ethnic racial socialization practice (Hughes et al., 2006). These attitudes permeate relationships with others, including with family members and health care providers (Moseley et al., 2007). Mothers and other main caregivers from other cultural backgrounds might not only have problems accessing supports from mainstream institutions but also experience family conflicts because the experiences of parents and children with mainstream institutions might differ. Although these factors can be listed individually, multiple factors are present in many individuals, families, neighborhoods, and regions (e.g., rural versus urban). This is why theoretical frameworks have emphasized the multiplicity of factors that are usually present in creating health disparities (García Coll et al., 1996). Moreover, new theories of intersectionality refer to those processes as differential access to power and as exclusion from benefits and assets and the existence of oppression and privilege at many societal levels (Bowleg, 2012; Brown et al., 2016;
Hankivsky and Christoffersen, 2008). Among the strongest factors associated with health disparities are gender, SES, and race (Becares and Priest, 2015; NASEM, 2017; Williams et al., 2010). In many instances, these factors are multiplicative, not additive, throughout childhood and adulthood.
At the same time, the protective factors that are unique for these populations need to be considered. The “immigrant paradox” refers to the findings that across physical and mental health and in educational and occupational outcomes, children and adults of immigrant backgrounds outperform native-born children, in spite of having been poorer and less acculturated to the dominant North American culture (García Coll and Marks, 2012). This phenomenon is poorly understood: it is unclear if motivational factors impel first and second generations to excel; if acculturation to poverty and its association with detrimental lifestyles and choices place subsequent generations at risk; or if discrimination and racism is more obvious to subsequent generations, and therefore its pernicious effects influence subsequent generations more.
Regardless, the traditional notion of rapid acculturation and complete assimilation as the successful model for incorporating immigrants has been questioned based on this evidence, and models of biculturalism and promotion of ethnic pride (Umaña-Taylor et al., 2014) are suggested as alternatives for successful incorporation. Finally, studies point out that state- and country-level policies that support families of immigrant background lead to fewer health disparities in youth (Filindra et al., 2011; Marks et al., 2018).
Children in Foster Care and Children with Incarcerated Parents
As discussed in the previous sections, a healthy (positive) relationship with main caregivers is one of the basic cornerstones of children’s development and is necessary to prevent many health disparities. There are populations that, for a variety of reasons, lack the stability and quality of parenting needed to promote their children’s development. Children in foster care and whose parents have been incarcerated often have multiple stressful life events before removal from parental care (Leve et al., 2012; Murray et al., 2012). The actual parental incarceration or loss of child custody is usually preceded by involvement with illegal activities and/or parental substance abuse, unstable housing, domestic violence, and/or child neglect or abuse. These children might be exposed to extreme stress, particularly during the prenatal period, when the in-utero child should be especially targeted at the first indication of any family relational difficulties.
Children in foster care Children in foster care are overrepresented as a group in terms of health disparities (Goemans et al., 2015, 2016;
Leloux-Opmeer et al., 2016; Leve et al., 2012). In most instances, these children’s parents have lost or given up their parental rights because they cannot provide their children with stable, healthy relationships and other critical health-promoting resources needed for their well-being. However, children from certain racial and ethnic populations are disproportionately represented in the child welfare system. For example, AI/AN families are twice as likely to be investigated as the national population of families, and cases are twice as likely to be substantiated, with AI/AN children three times as likely to be placed in foster care as the national population of children (Hill, 2007) (see Table 4-1 for data on this disproportionality).
TABLE 4-1 Disproportionate Foster Care of AI/AN Children: 15 States with the Highest Rates
| State | Disproportionality Ratea 2014 | Percent of Children Who Are AI/AN | Percent of Children in Foster Care Who Are AI/AN |
|---|---|---|---|
| Minnesota | 17.0 | 1.4% | 23.9% |
| Nebraska | 8.4 | 1.1% | 9.3% |
| Idaho | 5.2 | 1.2% | 6.0% |
| Iowa | 4.8 | 0.3% | 1.7% |
| Wisconsin | 4.8 | 1.1% | 5.1% |
| Washington | 4.3 | 1.5% | 6.3% |
| Oregon | 4.0 | 1.2% | 4.9% |
| Montana | 3.9 | 9.5% | 36.9% |
| North Dakota | 3.0 | 8.1% | 31.4% |
| South Dakota | 3.7 | 12.9% | 47.9% |
| Alaska | 2.6 | 17.8% | 46.6% |
| Utah | 2.5 | 0.9% | 2.3% |
| New Hampshire | 2.3 | 0.2% | 0.5% |
| California | 2.0 | 0.4% | 0.8% |
| North Carolina | 2.0 | 1.2% | 2.4% |
| Massachusetts | 1.2 | 0.2% | 0.2% |
| Maine | 1.1 | 0.8% | 0.9% |
a Data are sourced from Woods, S., and A. Summers. 2016. Technical assistance bulletin: Disproportionality rates for children of color in foster care (Fiscal Year 2014). Reno, NV: National Council of Juvenile and Family Court Judges.
SOURCE: NICWA, 2017.
Disruptions in attachment and other regulatory processes are consistently found in this population (Barone et al., 2017; Goemans et al., 2016; Leloux-Opmeer et al., 2016; Vasileva and Petermann, 2018). However, it has been found that foster care does not ameliorate these problems and actually might lead to more negative adaptive functioning after 1 year in such placement (Goemans et al., 2015).
Policies and practices of parental removal and replacement need to be carefully implemented. The stability of nurturing and supportive relationships, as described earlier in this chapter, is a crucial consideration for these populations (Jones Harden, 2004). If parents are unavailable or incapable of providing such conditions, placement with other family members, foster parents, or adoption is advisable, but only if these substitute parents can, in turn, provide stability and responsive parenting. That means that the quality and timing of care provided by family substitutes, including foster and/or kinship care and/or adoption or the reunification with the original biological family, has to be carefully planned and implemented to avoid re-traumatizing children through their interactions with these systems (Font et al., 2018).
In terms of supportive policies, the passage of the Family First Prevention Services Act in 2018 provides an opportunity to advance evidence-based child welfare policies through the investment of federal funds in children at risk for foster care, in foster family homes, or in qualified residential treatment programs or other special settings.3 Most notably, the legislation provides support for programs and practices to keep children with their families safely (e.g., allowing states to use Title IV-E funds to prevent children’s entry into foster care) (NCSL, 2019).
Children with incarcerated parents Incarceration is more prevalent in marginalized populations, adding to these populations’ multiple risks for poor health outcomes. Analysis of incarceration rates shows much higher rates in low-income, minority populations (Acker et al., 2019; Wildeman and Wang, 2017). It has been widely documented that discriminatory policies and practices in the definitions of crimes, arrests, sentencing, and incarceration practices lead to an overrepresentation of low-income and minority populations, which has resulted in widespread incarceration within these communities (Acker et al., 2019; NRC, 2014). These higher rates not only affect the developing mother–child relationship but also disrupt the networks of support for parents frequently found in other family or neighborhood members.
___________________
3 H.R.253—Family First Prevention Services Act of 2017.
Research clearly demonstrates the negative effects of parental incarceration on the child (Christian, 2009; Wildeman and Wang, 2017). Parental incarceration usually leads to family financial and housing instability and to more mental disorders and physical health problems in the partner (the parent who stays behind), which in turn is associated with higher incidence of child abuse and neglect (Acker et al., 2019). Various studies, including a meta-analysis, show that parental incarceration is associated with higher risks of children’s antisocial behaviors, learning disabilities, and behavioral problems (Murray et al., 2012; Turney, 2014). Long-term educational, occupational, and physical and mental health outcomes as well as criminal behaviors are all related to parental incarceration (Acker et al., 2019).
Given the importance of attachment to the primary caregiver, maternal incarceration is believed to be more detrimental for young children than paternal incarceration and is a serious risk factor for future psychopathology (Murray and Murray, 2010; Parke and Clarke-Stewart, 2001; Shlafer and Poehlmann, 2010). This is concerning, given that almost 80 percent of incarcerated women are mothers (McCambell, 2005). For that reason, policies and practices that ensure adequate access and visitation to the incarcerated parent and promote healthy attachments is seen as a fundamental need and right of the child(ren) left behind (UNM, 2011).
LGBTQ Parents and Children
The parents and children that do not conform to normative gender expression and sexual orientation schemas of society (the LGBTQ community) are also placed at risk by contextual circumstances. The current cultural, religious, and political climate in the United States is divided on the acceptance and approval of these behaviors. Although research indicates that same-sex parents have been found to raise children with similar developmental outcomes as those of opposite-sex parents (see Box 4-7), about one-third of the population still expects negative impacts on children (Drake, 2013).
From an equity perspective, the LGBTQ community has historically gained rights for families through legislation and court precedence, such as the Supreme Court decision to uphold same-sex marriage as a constitutional right in 2015.4 This landmark court case was instrumental in securing marital benefits (e.g., financial, social) for same-sex couples and their children. As of 2016, 20 states and Washington, DC, had enacted legislation that prohibits discrimination based on sexual orientation and gender identity or expression in employment, housing, and
___________________
4Obergefell v. Hodges, 576 U.S. (2015).
public accommodations—all of which are critical to promoting healthy development for children.
Even with such laws and policies, members of these populations are often subjected to discriminatory acts and microaggressions (IOM, 2011). Some have to “hide” their orientation and expressions from family, friends, and co-workers, which sometimes leads to the adoption of high-risk behaviors, such as unprotected sex, or internalizing disorders, such as depression, self-injurious behavior, and anxiety (IOM, 2011). Others may passively accept or actively repudiate discriminatory acts, exclusions, verbal and physical aggressions, and microaggressions as they express and adopt these less normative behaviors. These varied reactions to homophobia and discrimination can be associated with high levels of chronic stress and contribute to long-lasting health disparities (IOM, 2011).
While sexual orientation and gender identity may be more salient during adolescence, there is evidence to suggest that LGBTQ children demonstrate their inclinations to gender-atypical behaviors and same-sex orientation quite early (Rae et al., 2019). Many parents identify cross-dressing, toy preferences, and identification with heroes/heroines as displaying these preferences as early as the infancy and toddler years. As the typical puberty age has dropped, the issues that used to arise later in adolescence (i.e., identity, dating) are moving into childhood.
The LGBTQ population of children and youth is overrepresented in the adoption of risky behaviors and psychopathology. The 2011 Institute of Medicine report The Health of Lesbian, Gay, Bisexual, and Transgender People (IOM, 2011) identified the following key findings from the literature about LGBTQ youth during childhood and adolescence:
- LGBTQ youth are at increased risk for suicidal ideation and attempts and depression.
- Rates of smoking, alcohol consumption, and substance use may be higher among LGBTQ than heterosexual youth.
- The homeless youth population contains a disproportionate number of LGBTQ youth. Some research suggests that young transgender women are also at significant risk for homelessness.
- LGBTQ youth report experiencing elevated levels of violence, victimization, and harassment compared with heterosexual and non-gender-variant youth.
- Families and schools appear to be two possible focal points for intervention research.
These findings are corroborated by data from the Youth Risk Behavior Survey, which identify LGBTQ youth as being at risk for bullying, intimate partner violence (IPV), and sexual assault (CDC, 2017).
Children in High-Achieving Schools
As noted at the outset of this section, the standouts in groups of children and families exposed to high levels of chronic stress include those at both extremes of SES. Evidence of the challenges facing children and families in poverty, summarized here, have been reviewed extensively in the literature, with studies burgeoning around publication of the landmark Special Issue of Child Development on poverty more than 20 years ago (Brooks-Gunn and Duncan, 1997; Elder, 2018; Huston et al., 1994). By contrast, the evidence showing that youth in high-achieving contexts are an at-risk population is nascent, and the findings are counterintuitive for most. Extant evidence of adjustment difficulties among these children is presented here, followed by consideration of why this subgroup might merit attention in this particular report, which is focused on family-based prevention for children known to be at risk given life adversities.
With regard to the existing evidence on children of well-educated, relatively affluent parents, studies using varied samples and methods have converged in indicating relatively high levels of adjustment problems, likely linked with long-standing, ubiquitous pressures to excel at academics and extracurricular activities. Studies of students attending high-achieving schools (HASs) (public and independent; day and boarding; in different parts of the country) have consistently determined that they show rates of clinically significant problems, notably depression, anxiety, rule-breaking, and substance use, at rates that are (a) much higher than national norms and (b) sometimes higher than those in urban poverty (the latter is particularly true for substance misuse; see Luthar and Kumar, 2018; Luthar et al., 2013). Two large-scale analyses of national datasets in Norway and the United States (Coley et al., 2018; Lund et al., 2017) have confirmed a U-shaped association between community-level affluence and students’ adjustment problems; in fact, students at more affluent schools had the highest levels of substance use.
In a recent longitudinal study spanning 50 years, Gollner et al. (2018) showed that students at a HAS had poorer outcomes decades later than their counterparts at middle-achievement schools. The authors said that constant social comparisons among a population of largely talented students were likely implicated in this result, which led to lower educational expectations of the self. Similarly, a collection of three studies involving 5th- to 10th-graders in Germany (Pekrun et al., 2019) showed that in all three schools, being in a high-achieving context had negative links with self-concept and emotions, and conversely, being in less HASs was better for self-concept and emotion.
Over time, accumulating evidence on this population has led to global statements about the high levels of risk among these youth. Almost a decade ago, Koplewicz et al. (2009) referred to their problems
as “an epidemic.” A 2018 report on adolescent wellness, released by the Robert Wood Johnson Foundation, noted the following as the most critical “high-risk” environments: exposure to poverty, trauma, discrimination/racism, and high pressure to achieve, usually found in relatively affluent communities (Geisz and Nakashian, 2018).
Importantly, risks can be further exacerbated for vulnerable populations in HAS settings. Recent research has shown that African American boys in relatively high SES communities reported significantly higher depression and substance abuse, probably as a result of greater discrimination/racism in their communities—likely dominated by white families (Assari and Caldwell, 2018; Assari et al., 2018a,b; Lewis and Van Dyke, 2018). There is value, therefore, in considering issues of racial socialization for children of color who have the “double jeopardy” of having few children who look like them in their schools, neighborhoods, and communities.
With regard to why this subgroup of children and families might be relevant for this report on early childhood and equities in adaptation, two factors are relevant; one has to do with “sleeper effects” and the other with the need for early prevention. With regard to the first issue (as has been discussed earlier), the charge of this committee is not just to prevent problems that are manifested in early childhood—temper tantrums or bed-wetting—but, equally, those whose seeds are sown in early childhood and then “incubate” and become evident by early adolescence. It is clear that the prevention of problems among HAS youth (and other youth who suffer poor outcomes due to various types of adversity) cannot start when they are already teens; by then, a great deal of damage has already been done. Instead, what is needed is attention to these issues among parents when the children are still young. In fact, there are recent suggestions that the effects of high-achieving environments can be seen as early as preschool (Pekrun et al., 2019).
Second, there is a great deal of preventive potential in working with families in these settings toward raising awareness of the nature of risks and potential problems. Unlike low-income communities where an influx of resources is often needed for prevention, in this case, dissemination of accumulated evidence from science, with associated recommendations (Luthar et al., 2013), can be helpful. It is particularly important for parents to (a) understand the level and seriousness of adjustment problems that researchers have recurrently documented in HASs and (b) be vigilant in their own homes, starting from early childhood, against being overly invested in the child’s “resume-building” (Gollner et al., 2018; Luthar and Kumar, 2018; Pekrun et al., 2019).
It is also critical to note that just as children in high-achieving contexts can be vulnerable, so can their mothers (who are, again, as in most
contexts, their primary caregivers). Panel studies over time have shown that well-educated mothers have shown substantial increases in hours spent on activities related to their children, with increases greater than those among well-educated fathers and less well-educated mothers or fathers (Kalil et al., 2012; Ramey and Ramey, 2010). In terms of sheer hours, therefore, this group can be especially stretched thin and chronically stressed. Cross-disciplinary studies have established other factors that can challenge their well-being, including the “invisible labor” involved in being responsible for overseeing the schedules and activities of everyone in the household (see Ciciolla and Luthar, 2019; Lareau and Weininger, 2008; Yavorsky et al., 2015).
A 2019 study showing increases in depression over the past decade in the high-income groups, and among women in particular, provides additional testimony to the seriousness of these issues (Twenge et al., 2019). Changes over time were examined for four cohorts/generations and considering four groups of family incomes. The findings showed that cohort increases in serious psychological distress were the largest in the highest income group. Among adolescents, time period increases in rates of a major depressive episode were the largest in the highest income group and smallest in the lowest income group; among adults, the cohort increase in suicidal ideation was largest and smallest in the highest and lowest income groups, respectively. The authors concluded that “with the exception of adult MDE [major depressive episodes] and suicide attempts, the cohort increases were the largest and most consistently seen among those with the highest income” (Twenge et al., 2019, p. 10). Additionally, among adults, the increases in mood disorder indicators and all suicide related variables (suicidal thoughts, plans, and attempts) were consistently higher among women than men.
The evidence on youth and families in high-achieving contexts was reviewed above in some detail because this is a newly identified at-risk group, encompassing at least 20–25 percent of the U.S. population (e.g., Twenge et al., 2019). Additionally, despite the seriousness of the problems that are increasingly documented, there remains reluctance to afford attention to them in research and policy (Geisz and Nakashian, 2018).
In addition to HAS families, there are other such groups that are increasingly being identified as showing high vulnerability relative to norms, such as subgroups based on sexual identity and preference. Questions on both of these dimensions are now arising among children at younger and younger ages (often well before adolescence), creating stress and confusion for the child as well as the parents. Children who identify as neither male nor female but rather as “nonbinary” show elevated rates of anxiety, depression, and other psychological difficulties, as do children
who identify not as heterosexual but as lesbian, gay, bisexual, or questioning. Regarding transgender youth, considerations of gender reassignment are also now coming up in many families well before adolescence. All of these subgroups will need concerted attention in the years ahead in terms of understanding how best to help both children and parents effectively negotiate these issues at home and outside it, such as in the children’s peer groups.
Youth from Asian backgrounds are yet another illustration of a group that is potentially vulnerable but rarely included in discussions of children at risk. These children are often thought of as both privileged and “model minorities” (e.g., Lee et al., 2009; Ngo and Lee, 2007), but in fact, many U.S. families of Asian origin actually live in low-SES households. Furthermore, issues of discrimination arguably affect Asian youth just as they do other racial and ethnic minorities. At the same time, Asians are not considered as an ethnic minority group in discussions of discrimination, prejudice, and stereotype (Wong and Halgin, 2006) the way that youth from African American, Latino, or AI/AN backgrounds are. It is important to emphasize that this is not a zero-sum game; research and policy attention to the needs and challenges of Asian Americans by no means implies detracting from the very real and well-documented challenges faced by other ethnic minority groups in the United States.
In addition to including such neglected subgroups in discussions of those needing attention to prevention, more attention to risk processes that were not an issue at the time that From Neurons to Neighborhoods (NRC and IOM, 2000) was released is also warranted, and social media is critical in this regard. In discussions of why there continue to be increases in children’s depression since the early 2000s, social media is often noted as a major factor (Hoge et al., 2017). Yet, there remain several questions about which aspects of social media use are truly damaging to children’s mental health. Possibilities range from the amount of time spent on social media to spreading rumors about others, being the victim of bullying, “sexting” and accessing pornography, and constant social comparisons or feeling “less than” others. In Chapter 3, there is a section devoted to the problem of bullying even among young children; clearly, there is a lot of work that still remains to reduce this major risk process—and, now, to also disentangle and address the new challenges introduced by the widespread use of social media from young ages onward. As Weisz et al. (2019) note, the nature of childhood disorders may be changing faster than our treatments are:
Threats to youth mental health are becoming more diverse and multiform. . . . Current threats encompass pressures to excel as well as new pressures to excel in increasingly competitive academic and social
environments, images conveyed via advertising and social media that could make anyone feel inadequate, risks of harm via text messages and cyberbullying, and even fear of being gunned down at school. (Weisz et al., 2019, p. 233)
To summarize, as policy makers and prevention scientists think about groups of young children and caregivers whose life circumstances are likely to place them at high risk for adjustment problems, the needs of all families need to be taken into consideration. Low levels of maternal education, coexisting with poverty and often single motherhood, clearly spell risks for adjustment problems and parenting difficulties among mothers, as noted earlier. At the same time, there are other groups that are increasingly being identified as requiring attention in future prevention efforts, including children and parents in extremely fast-paced, stressful, competitive communities, and sexual minority youth. Similarly, there are new risk processes that have arisen in the past couple of decades that potentially have strong negative effects on children and merit concerted attention in future research and policy when considering what should and should not be prioritized in preventive interventions.
In conclusion, psychologists, educators, and other health professionals need to work with groups of families that are especially vulnerable due to exposure to high levels of stress or adversity, with efforts beginning from preconception onward. These efforts will involve harnessing protective processes, and minimizing risk factors, in interventions that have a sound basis in developmental theory, science, and cumulative research evidence; have shown promising results in prior prevention studies; and are pragmatic (i.e., can feasibly be taken to large scale in the real world).
In addition to addressing major goals relevant for children in general (e.g., fostering caregiver well-being and minimizing maltreatment), programs need to include components that specifically address unique, powerful risk and protective processes within these subgroups of children. As discussed above, it cannot be assumed that evidence-based interventions and promising models developed in specific populations will work in other contexts. The validity and adaptability of interventions need to be empirically tested in groups that differ greatly in the sources of chronic stress and cultural backgrounds.
INTERVENTIONS TO PROMOTE RELATIONAL SUPPORTS AND CAREGIVER WELL-BEING
As developmental scientists have emphasized the critical importance of relational supports for the well-being of mothers and thus, their parenting, intervention trials have shown strong benefits of relational interventions. Indeed, the core components of several effective interventions suggest that over and above learning particular skills, it is improvements in mothers’ overall well-being, within the context of supportive relationships, that are the most critical “engine” underlying the positive changes. To illustrate, the Incredible Years intervention by Webster-Stratton and colleagues (2001) targets children’s school readiness and parenting skills while helping parents to cope with personal problems; parents are able to form valuable support networks with “buddies” from parent groups (Borden et al., 2010). Ammerman and colleagues’ (2005) Every Child Succeeds program for depressed mothers provides in-home cognitive behavior therapy and a supportive home visiting component. A cardinal component in Dozier’s Attachment and Biobehavioral Catch-up (ABC) is consistent respect, warmth, and support displayed by project staff or therapists to participating mothers (Dozier et al., 2005).
This section focuses on interventions with the strongest evidence base to foster healthy child development through supporting caregivers. First, there is a discussion of the evidence on home visiting, a well-established model for providing services to children and families, and the following section describes a range of interventions that have shown promise. The committee presents these as opportunities to use the science to drive action on caregiver and child well-being; however, the presentation of these interventions does not indicate prioritization of one over another.
Different populations will require varying interventions based on their needs and context, in addition to specific tailoring to meet these unique needs depending on the population.
Home Visiting Programs
One of the earliest program models built around the notion of supporting caregivers is home visiting. Home visiting programs in the United States focus on promoting child health and development by providing parenting support and other child-centered services in the home (e.g., developmental screenings and referrals to services and treatment) to at-risk families from the prenatal stage through age 6 (HRSA, n.d.). One of the primary goals of home visiting is to improve child health and educational outcomes. Home visiting programs have provided services to families in the United States since the late 1800s (Minkovitz et al., 2016), but the 2010 federal Maternal, Infant, and Early Childhood Home Visiting (MIECHV) program led to the expansion and supported standardization of home visiting implementation and evaluation. In fiscal year 2018, the MIECHV program served approximately 150,000 parents and children in 76,000 families across all 50 states; Washington, DC; 5 territories; and 23 tribal and urban AI/AN communities, providing nearly 1 million home visits annually and 5.2 million home visits between 2012 and 2018 (HRSA, n.d.). By law, state and territory awardees have to spend the majority of their MIECHV program grants to implement evidence-based home visiting models, with up to 25 percent of funding available to implement promising approaches that will undergo rigorous evaluation.5 Tribal home visiting programs are encouraged to select evidence-based home visiting curricula, but as the research evidence is limited, this is not a program requirement. Most tribal home visiting programs chose to implement evidence-based curricula with cultural adaptations developed with intensive community input and engagement, which enhanced family engagement and retention (Pratt and Chapman, n.d.). Home visiting services may also receive support from many other federal, state, and local public and private sources.
This section summarizes the evidence on home visiting, highlighting a few exemplar programs. Given the multidisciplinary and cross-sector nature of this topic, the chapters later in the report will discuss home visiting with respect to specific levers in certain domains to enhance or support such programs. (See Chapters 5 and 7 for more on the role of the health system and of ECE, respectively.)
___________________
5 For more information see https://mchb.hrsa.gov/maternal-child-health-initiatives/ home-visiting-overview (accessed June 8, 2019).
Summary of the Evidence on Home Visiting Programs
A growing body of evidence suggests that home visiting by a nurse, a social worker, or an early educator during pregnancy and in the first years of a child’s life improves a whole host of child and family outcomes, including promotion of maternal and child health, prevention of child abuse and neglect, positive parenting, child development, and school readiness. The positive impact continues well into adolescence and early adulthood. For example, in a 19-year follow-up of a randomized controlled trial (RCT), Eckenrode et al. (2010) found that relative to the comparison group, girls in the pregnancy and infancy nurse-visited group were 58 percent less likely to have been arrested and 43 percent less likely to have been convicted. Nurse-visited girls born to unmarried and low-income mothers also had fewer children and less Medicaid use.
One meta-analysis examined the impact of 18 implementation factors (including staff selection, training, supervision, and fidelity monitoring) and four study characteristics (publication type, target population, study design, comparison group) in predicting program outcomes (Casillas et al., 2016). The greatest program effects were found to be on increased positive parenting and reduced likelihood of maltreatment; the former had the largest effects. The programs were significantly less effective for children’s health and behavior. Furthermore, provision of high-quality supervision and fidelity monitoring were key factors associated with beneficial outcomes. Programs serving families with one or more risk factors had significantly greater effect sizes compared to programs serving all families.
Avellar and Supplee (2013) reviewed the research on home visiting, and nearly 9 out of 12 programs (of the 32 reviewed) that met evidence-based criteria also showed favorable effects on children’s social-emotional development or behavioral problems. Five programs showed one or more favorable effects on cognitive development, and five showed improvements in reductions in some aspect of child maltreatment (only six of the programs assessed maltreatment).
Another meta-analysis examined the effect of home visiting on six outcomes: birth outcomes, parenting behavior and skills, maternal life course, child cognitive outcomes, child physical health, and child maltreatment (Filene et al., 2013). Mean effect sizes were significant and positive for three of the six outcome domains: maternal life course outcomes, child cognitive outcomes, and parent behaviors and skills (Filene et al., 2013). Effect sizes for birth outcomes were significantly larger for programs that used nonprofessional home visitors, matched clients and home visitors on race and/or ethnicity, or included problem solving.
Effect sizes were larger for parent behaviors and skills programs that addressed parental substance use and taught parents developmental
norms and appropriate expectations, discipline and behavior management techniques, and responsive and sensitive parenting practices. Improved child maltreatment outcomes were associated with problem solving and teaching parents how to select alternative caregivers for children. The effects on children’s cognition were better in programs that taught parents responsive and sensitive parenting practices or “required parents to role-play or practice skills during home visits. Using professional home visitors was a significant predictor of better child physical health outcomes, as was teaching discipline and behavior management techniques” (Filene et al., 2013, p. S104).
Following a review of the research literature in 2018 (Sama-Miller et al., 2018), the Home Visiting Evidence of Effectiveness project, established by the Administration for Children and Families (ACF) in the U.S. Department of Health and Human Services, identified 20 home visiting models as meeting criteria of effectiveness to recommend for state-based home visitation programs (OPRE, 2018). Based on the available high- or moderate-quality studies, the review showed that most of these programs have multiple favorable effects with sustained impact, with Healthy Families America and the Nurse-Family Partnership (NFP) showing favorable impact across the greatest breadth of outcomes. Most models had favorable impacts on primary measures of child development, school readiness, and positive parenting practices; none of the models, however, showed impacts on a primary measure of reductions in juvenile delinquency, family violence, and crime (Sama-Miller et al., 2018).
A national evaluation of the effectiveness of the MIECHV program from 2012 to 2017, based on random assignment of families, found statistically significant positive effects in 4 out of 12 confirmatory outcomes: the quality of the home environment, the frequency of psychological aggression toward the child, the number of Medicaid-paid child emergency department (ED) visits, and child behavior problems (Michalopoulos et al., 2019). Most estimated effects are similar to but somewhat smaller than the average found in past studies of individual home visiting models. Differences in effects among the evidence-based models are generally consistent with the models’ focuses. For example, Parents as Teachers produced the largest increase in parental supportiveness, and NFP produced the largest reduction in ED visits for children (Michalopoulos et al., 2019).
Potential to Reduce Disparities
The field of home visiting research continues to expand, with researchers identifying measurement frameworks (West et al., 2018) and factors contributing to implementation and replication (Paulsell et al., 2014). The state and tribal MIECHV recipients are required to implement rigorous
program evaluations, which also help inform best practices and identify model programs and approaches and support the development and implementation of cultural adaptations necessary to ensure program retention, engagement, and cultural fit (Denmark et al., 2018; Hiratsuka et al., 2018). While the evidence remains limited for significant improvements in the reduction of health disparities, some studies have demonstrated that home visiting resulted in improved outcomes and so offered savings in terms of a return on investment of $2–$4 for every dollar spent (Cannon et al., 2017).
Among nondepressed mothers or families without multiple Child Protective Services (CPS) reports prior to study enrollment, home visiting was associated with a significantly lower likelihood of CPS report recidivism. These results indicate potential for home visiting to prevent maltreatment recidivism but, importantly, suggest that home visiting approaches, with weekly in-home visits by a trained home visitor, is warranted for mothers exhibiting significant depressive symptoms or families with extensive CPS histories (Jonson-Reid et al., 2018). However, among 220 low-income home visiting enrollees in a regional setting, mothers who experienced maltreatment in childhood had a heightened risk for membership in the mild and moderate-severe depression subgroup trajectories (Teeters et al., 2016). Mothers reporting higher social support saw a significant reduction in the risk of experiencing either mild or moderate-severe depression subgroup trajectories, while mothers reporting an increased belief in having control over one’s life (i.e., locus of control) also saw a significantly reduced risk for assignment in either the mild or moderate-severe subgroups. Moreover, the depression score of mothers experiencing moderate to high depression was not significantly lower while enrolled in home visiting, though the depression scores for mothers at the minimal and mild levels of depression were significantly lower over time (Teeters et al., 2016). These results suggest that the effect of home visiting may also depend on maternal depression level, demonstrating that tailoring home visiting curricula to best fit maternal risk factors may be warranted.
Exemplar Programs and Promising Practices
The NFP home visiting curriculum has demonstrated multiple positive outcomes, including a reduction in domestic violence reports (Eckenrode et al., 2017). Mothers receiving visits from nurse home visitors had fewer health care encounters for injuries and higher ratings of the home environment and parent’s reports of caregiving (Kitzman et al., 1997; Macmillan et al., 2009; Olds et al., 1997; Zielinski et al., 2009). NFP is the only home visiting program to have statistically significant positive effects over time on substantiated cases of child maltreatment.
Healthy Families New York, a Healthy Families America–accredited home visiting program, has demonstrated positive effects for fathers’ participation. Families with father participation were more than four times as likely to be retained, and engaged fathers were more likely to live at home with the child and to remain emotionally involved at 6 months (McGinnis et al., 2018).
The Family Spirit home visiting intervention is the only program that has demonstrated efficacy in American Indian communities. To date, it has only been implemented in three rural, tribal communities in the Southwest. Nevertheless, Family Spirit has seen that high-risk mothers had significantly greater parenting knowledge (effect size = 0.42) and parental locus of control (effect size = 0.17), fewer depressive symptoms (effect size = 0.16) and externalizing problems (effect size = 0.14), and lower past-month use of marijuana (odds ratio [OR] = 0.65) and illegal drugs (OR = 0.67). Moreover, children in Family Spirit had fewer externalizing (effect size = 0.23), internalizing (effect size = 0.23), and dysregulation (effect size = 0.27) problems (Barlow et al., 2015).
Culture is embedded across many important components of parenting, and it has only recently been actively integrated into home visiting services. However, few culturally specific home visiting curricula have sufficient evidence to be deemed evidence-based practices. Some are considered promising, with some positive quasi-experimental support for program, family, and child outcomes. For example, Kūlia I Ka Nu’u works with families with children 2.5–5 years old using a Montessori approach with Native Hawaiian culture to support parents in building their child’s school readiness and school success (Yoshimoto et al., 2014). Parent educators help families learn more about Native Hawaiian values and practices and incorporate these cultural values into the curriculum, which includes literacy, math, art, social studies, and science. Kūlia I Ka Nu’u is unique to the island of O’ahu. Pūlama I NāKeiki (PINK) provides services to Native Hawaiian families prenatally to 3 years of age. PINK supports families in identifying and learning more about cultural traditions and how strengthening cultural knowledge contributes to family life. Parent educators provide culturally based information about prenatal health, childbirth, child development, and child rearing (Yoshimoto et al., 2014).
Expanding the Impact of Home Visiting
To maximize the impact of effective home visiting programs, there is a need to expand their reach by scaling them to larger and different populations; currently, only 40 percent of U.S. counties provide home visiting services, with 13 states offering home visiting in 75 percent of counties and 10 states providing it in 10 or fewer counties (NHVRC, 2018). In 2017,
more than 300,000 families received home visiting services, though the National Home Visiting Resource Center estimates that about 18 million additional families could benefit but were not being reached (NHVRC, 2018). The MIECHV program was reauthorized in 2018 at a funding level of $400 million annually through 2022 (Sandstrom, 2019). To address remaining unmet needs, the federal program needs to be funded at a much higher level in the next reauthorization. States can further expand support for evidence-based home visiting services through state general funds, Medicaid financing, or braiding of different funding streams (Johnson, 2019). Presently, 20 states are using Medicaid to expand state capacity and reduce unmet needs for home visiting services, including universal home visiting, such as in Oregon and Washington State. Many states are using a Medicaid State Plan Amendment to support home visiting services under targeted case management benefit; other states, such as Maryland and South Carolina, had made home visiting demonstration or pilot projects part of a larger Medicaid 1115 or 1915(b) waiver. South Carolina is braiding approximately $17 million in philanthropic investments with $13 million in Medicaid funding through a 1115 waiver to finance a pay-for-success approach. Under this approach, private (and public) funders provide up-front capital to expand social services through a “social impact bond”; the government pays for all or part of the program only if it measurably improves the lives of participants (Johnson, 2019). South Carolina has committed an additional $7.5 million in payment if independent evaluators find positive results from expanded home visiting services (Johnson, 2019).
Scaling up requires more than simple replication of an effective home visiting model to reproduce positive effects. It entails the careful consideration and balance of fidelity, spread, and tailoring models for local adaptation. To support fidelity in the home visiting field, Paulsell et al. (2014) argue that two conditions need to be met: (1) research on efficacy, effectiveness, and dissemination need to document challenges that threaten fidelity; and (2) the field needs to standardize measurement and improve understanding of valid and reliable fidelity measures within and across models. While model fidelity is an important mediator of program success, home visiting implementation requires flexibility to tailor the program to the needs and/or assets of the community or population being served. This is especially critical when applying an equity approach, so that all children and families receive the services that they need. One strategy may be for the MIECHV program to work with model developers in identifying core program elements across models, while allowing state grantees to choose additional elements from various models to enhance and tailor the core program to the differential needs and vulnerabilities of individual families and communities. Additionally, others have proposed
proportionate universalism—a tiered approach where every new parent in a community receives at least one home visit, while the quantity and intensity of follow-up services are adjusted to the needs and assets of high-risk families, to improve program cost-effectiveness (Marmot et al., 2010). (See the section on Synthesizing the Evidence for Conclusion 4-5 on applying a tiered approach to services.) Most importantly, as the committee discusses in Chapter 5, home visiting must not become yet another siloed prenatal and early childhood service. Future evidence-based home visiting programs need to continue to partner with, coordinate, colocate with, and expand the reach and impact of other ECE programs and the future redesigned advanced medical home. Home visiting can thus serve as a linchpin between health care, social services, and early childhood education.
Lastly, the relatively modest impact of the MIECHV program demonstrated in the national evaluation has been observed in other early childhood programs that scaled up from RCTs to population-wide interventions (Center on the Developing Child at Harvard University, 2016). Studies that focus on average effects may mask wide variation in impacts if they do not or cannot account for the differential susceptibilities of individuals, families, or communities. Often, RCTs cannot easily be adjusted, adapted, or enhanced after randomization (see Chapter 1 for a discussion about the limitations of RCTs). Future home visiting and ECE research needs to move beyond searching for one-size-fits-all solutions to define more precisely which intervention works best for which patients or populations under what circumstances.
Researchers, program leaders, and policy makers should focus on expanding the concept of precision home visiting that advances which programs and activities are best for which family, in which communities, and for what outcomes.
State policy makers should further expand support for evidence-based home visiting services through general funds, Medicaid, and braiding of multiple funding streams. HRSA and ACF should continue to ensure program effectiveness and accountability of the expanded program. Expansion of home visiting programs should be done in conjunction with the expansion of other public investments and services.
Given the resources needed to provide high-quality home visiting, cost is an important consideration. Yarnoff et al. (2019) developed and piloted a tool to standardize the collection of home visiting data, in addition to assessing program costs for 45 local implementing agencies that participate in MIECHV. The study reported an average cost per family served of $12,556 for agencies serving less than 100 families, versus $7,117 for agencies serving more than 100 families.6Burwick et al. (2014) conducted a cost analysis for 25 implementing agencies and found that the average estimated annual cost to operate a home visiting program was $580,972.7 Costs varied drastically from program to program, ranging from $206,426 to $1,207,054. Estimating and comparing costs of home visiting programs—and by extension, of expanding them—can be difficult for a number of reasons. As noted above, program costs vary, and this could be attributable to the services offered, duration, transportation costs—particularly in rural and/or tribal communities—and family and agency characteristics (Burwick et al., 2014; Yarnoff et al., 2019). Further research is needed to understand how to expand home visiting programs cost effectively, and a tiered approach would provide tailored services based on family needs (see Conclusion 4-5 for more on a tiered approach). Finally, strengthening programmatic coordination and alignment across sectors, as indicated in the recommendation, could potentially reduce costs.
Other Evidence-Based Programs Focusing on Mothers
Outside of home visiting, perhaps the first program to explicitly target mothers’ well-being is Lieberman’s Infant Parent Psychotherapy (IPP), designed with the recognition that a critical prerequisite in working with mothers at high risk for maltreating their infants is attention to the women’s own psychological needs. The program has been expanded for
___________________
6 The study authors calculated cost of the program per family by dividing total program costs by the average monthly number of families served by the agency and then calculated weighted mean cost per family served as the sum of costs across all agencies divided by the sum of families served.
7 The cost analysis was conducted using “the ‘ingredient’ or resource cost method, which involved itemizing the types of resources (or ingredients) needed to provide services, gathering information on the types and value of resources used by each agency during the study period, and aggregating costs to estimate total program costs” (Burwick et al., 2014, p. xii).
work with mothers and toddlers (Toddler Parent Psychotherapy [TPP]), and therapeutic strategies combine cognitive behavioral, psychodynamic, and social learning theories. A cardinal ingredient, however, is high empathy and support for the mother, with recognition that “the most effective interventions are not spoken but rather enacted through the therapist’s empathic attitude and behavior toward the mother as well as the baby” (Lieberman and Zeanah, 1999, p. 556). A number of studies have now documented the benefits of IPP and TPP, implemented with mothers across diverse settings (see Lieberman et al., 2011).
Another program with a strong emphasis on respect, warmth, and support by intervention staff to participating mothers is Dozier’s ABC. In this program, goals are to target insecure early attachments by intervention services to foster caregivers’ positive qualities, including responsiveness, nurturance, and their own attachment states of mind (Dozier et al., 2002). The program has been refined and tested in RCTs for more than 20 years. Results show that those receiving the intervention showed significant gains compared to control groups, which included better quality of attachment between mothers and children and improved self-regulation in both (Bernard et al., 2015; Bick and Dozier, 2013; Dozier et al., 2002). See Box 4-8 for more on the ABC program as an example of a promising model.
Another program with focused attention on the well-being of mothers is the Relational Psychotherapy Mothers’ Group (RPMG) intervention (Luthar and Suchman, 2000), developed for mothers at risk for maltreating their children—specifically, low-income women with histories of substance abuse. As with IPP and ABC, core therapeutic components in RPMG include a strong emphasis on empathy, genuineness, and warmth and using insight-oriented approaches to improve parenting skills and efficacy. There were two major differences between RPMG and programs for mother–child dyads, both related to potential for scaling up. The first was the choice of a group format rather than individual sessions, thus potentially reaching more women for 1 hour of clinicians’ time. Second, RPMG was designed for mothers of children from birth through adolescence, with developmental issues addressed as part of the program, again allowing for inclusion of a wide range of women. Results of two clinical trials showed benefits of RPMG. Compared to treatment as usual in their methadone clinics, mothers who received the 24-week intervention showed lower risk for child maltreatment—by mothers’ and children’s reports—and better personal adjustment as well as both mothers’ and children’s reports of child maladjustment and on mothers’ drug use via urinalyses (Luthar and Suchman, 2000). At 6 months posttreatment, RPMG recipients continued to be at an advantage, although the magnitude of group differences was reduced. In the second trial, RPMG was compared to relapse prevention therapy (RPT). RPMG mothers again fared better
than RPT mothers at posttreatment per mothers’ self-reports, children’s reports, and urinalyses (Luthar et al., 2007). But again, at 6 months of follow-up, they lost many of their gains.
These findings collectively indicate that even after external interventions are completed, it is critical to ensure continuity in supports for mothers who are vulnerable to depression and other mental illness. Similar messages have emerged from Olds et al.’s (2007) widely used, efficacious program, NFP, which provides regular home visits for low-income, single mothers by a warm, supportive nurse. These home visits begin in the prenatal months and continue through the babies’ second birthdays. Yet, as Golden and colleagues (2011) underscore, mothers’ needs for help are not necessarily resolved when children reach 2 years old. In fact, mothers who have received this program report widespread, continuing depression in their communities, with many women desiring and needing support from others who can be reliable sources of caring over time.
In view of this accumulated work, therefore, one critical challenge for those working with vulnerable mothers is to ascertain how these mothers might continue to receive support even when time-limited supportive interventions cease, and in this regard, peer-based interventions are promising. Specifically, there is potential value in groups run by “graduates” of supportive programs who receive subsequent training and supervision in facilitating groups for peers (see Bryan and Arkowitz, 2015). Reportedly, this strategy has been used successfully with mothers who themselves had experienced perinatal depression, who regularly met with other women who were currently depressed. Bryan and Arkowitz (2015) conducted a meta-analytic review and found that peer-administered interventions (PAIs) produced substantial reductions in symptoms of depression. The magnitude of beneficial changes over time was significantly greater than those in no treatment conditions and was also comparable to non-peer-administered interventions. Interestingly, PAIs that were administered purely by peers were more effective than those that also involved a professional in the treatment, in a secondary role.
In future efforts to use such peer-based groups for mothers, some have suggested drawing on a type of model (not the intervention itself) that has been used extensively for decades and with minimal costs: the 12-step model (see Luthar et al., 2015). Community-based meetings in this program, specifically Alcoholics Anonymous, benefit more than 1.3 million Americans, and its benefits can be equal to or even greater than those of professional interventions (Kelly et al., 2012). A major “active ingredient” in this program, again, is ongoing access to dependable, authentic supports; members speak of unconditional acceptance with others sharing similar challenges and their ability to reach out to others when in distress. In the future, there could be value in using such community-based groups to promote resilience in at-risk
mothers. Sustaining the type of supportive connections that mothers came to depend on in the active phase of relational interventions might be possible with continued weekly meetings (Luthar, 2015).
This has been a recurrent theme in prevention and policy: scientists increasingly urge the use of networks that already exist in communities, bringing them to bear in interventions that become self-sustaining over time (Luthar, 2015). To illustrate, within affordable housing complexes, Antonucci and colleagues (2014) described programs that focused on creating mutually supportive networks among residents. Kazdin and Rabbitt (2013) described several low-cost, feasible, and effective interventions using lay people (rather than professional therapists), including hair stylists in beauty salons, trained to assess depression and to provide appropriate referrals. Hofmann and Hayes (2019) underscored the potential value of training paraprofessionals in the specific procedures that highly trained clinicians have identified as being most promising in engendering improved mental health.
An alternative approach is to deliberately foster women’s connections with reliable others in their everyday lives over the duration of a formal, relational intervention. This was the strategy used in an RCT of the Authentic Connections (AC) Groups program at the Mayo Clinic, tested with mothers who were health providers—a professional group at high risk for depression, burnout, and even suicide compared to norms. From the start of the 3-month program through the end, there was a focused, concerted effort to have women reach out to their “go-to committees” in their personal lives; thus, authentic connections were forged both within the groups and outside of them in the mothers’ everyday lives. In comparison with a control group (given 1 hour of freed time over 3 months to attend groups, as were intervention mothers), AC Groups women showed significantly greater gains across multiple adjustment indexes ranging from depression and self-compassion to lowered burnout at work and decreased levels of cortisol (Luthar et al., 2017). Moreover, effect sizes across outcomes were generally in the moderate range, and gains were still stronger 3 months after the intervention program was over (partial eta squares of 0.08–0.19; median, 0.16; according to Cohen [1988], partial eta squares correspond to the following effect sizes in the real world: 0.02 is small; 0.13 is medium; and 0.26 is large).
The success of these in-person AC Groups led to efforts to conduct them in a virtual format, via videoconferencing, to achieve potentially wider and easier dissemination (Luthar et al., in press). Results of this study indicated the successful completion of five different virtual groups (3–6 women each, for a total of 23), with the sample involving mostly mothers, most with advanced (graduate) degrees and almost all in high-pressure careers. As with the in-person version, the 3-month program
had zero dropouts. Participants’ mean ratings of the groups’ effectiveness were 9.6 of 10, and the “Net Promoter Score” (percent of promoters subtracting percent of detractors) fell in the exceptionally high range (Luthar et al., in press). Open-ended responses emphasized participants’ appreciation of access to robust, authentic connections with other caring women (which endured well after the program was completed). Given the low cost and ease of access—from mothers’ own workplaces, homes, or even while traveling—such virtual groups might be considered a useful model to be explored further in future work with mothers (indeed, the use of virtual connections have been increasingly emphasized; see Hofmann and Hayes, 2019; Weisz et al., 2019).
In concluding this section on interventions, the literature reviewed suggests the value of a tiered approach to psychological interventions for mothers at risk due to their life adversities, along with their children, and as early as possible—preferably prenatally. All approaches involve ensuring strong, dependable supports for the mother or other primary caregiver. At the broadest level of interventions, there is particular promise in those that bring together mothers in communities or virtually to provide such mutual, ongoing support. For women needing greater psychological help, time-limited, evidence-based group therapies emphasizing connections and mutual support and making maximal use of existing resources would be useful. The most intensive level would be one-on-one interventions, such as those involving home visiting or work with mother–child dyads to enhance strong attachment quality. Given the critical need to support caregiver well-being and to prevent child maltreatment (see Conclusions 4-1 and 4-2), in addition to the review of high-quality interventions that are offered in community settings for families, the committee offers the following recommendation to support the development and implementation of such interventions.
Measures to Be Used
In concluding this section, there is consideration of measures that should be included in evaluating results of large-scale preventive interventions targeting young children and their mothers. At a minimum, there
should be brief assessments of the mothers’ depressive symptoms, stress, feelings of rejection to the child, any involvement with CPS, and IPV, as well as the degree to which they have positive, buffering relationships in their lives. Possible measures include the 20-item Zung Self-Rating Depression Scale (Zung, 1965), 10-item Perceived Stress Scale-10 (Cohen et al., 1983), and 10-item subscale on parental undifferentiated rejection from the Parental Acceptance-Rejection Questionnaire (Rohner et al., 1980). For supportive relationships, potential measures might include the Satisfaction with Friends subscale (four items from the Inventory of Parent Experiences; Crnic, 1983) and two single items that have consistently shown significant, robust links with multiple aspects of mothers’ well-being: “Do you feel seen and loved for the person you are, at your inner core?” and “When you are deeply distressed, do you feel comforted in the ways you need?” (Ciciolla and Luthar, 2019; Luthar and Ciciolla, 2015). Finally, if any studies propose additional expensive assessments to inform future interventions (such as biomarkers as mediators, moderators, or outcomes), researchers need to explain how the findings from these will be applied not only in laboratory-based RCTs but also in large-scale interventions reaching vulnerable children and families in their own homes, schools, and community settings. Given the need to identify individuals at risk for early adversity and toxic stress, the committee offers the following recommendation to close a gap in the system. Furthermore, screening requires alignment with available services for children and families (see Chapters 5 and 8 for more on screening and alignment with services).
SYNTHESIZING THE EVIDENCE
To summarize, major conclusions deriving from this chapter include the following. Promoting resilience in childhood rests, first, on ensuring the well-being of children’s primary caregivers—usually, their mothers—and this requires the mothers’ ongoing access to strong, supportive relationships, beyond meeting basic needs for survival. Maltreatment is of utmost importance among the various parenting behaviors that should be targeted in preventive interventions; minimizing neglect and abuse by caregivers and others needs to be a top priority. Gender specificity is advised in interventions for parents, with separate delineation of how mothers and fathers each are most effectively recruited, retained, and
helped in interventions. When considering children who need preventive interventions, there are several subgroups whose unique challenges need to be considered. These include subgroups that have been extensively documented in past research to be at risk—such as children in chronic poverty, those separated from their parents, and recent immigrants—and those shown more recently as contending with high stress and distress, such as children and families in high-achieving communities and youth who are in the minority based on gender identification and sexual orientation.
As future interventions for mothers and children are taken to large scale, it will be useful to employ a tiered approach with the intensiveness of services increasing with the level of the mother’s distress. At a fundamental level, universal, supportive interventions for mothers from pregnancy onward are needed. This includes using existing resources for supportive group-based interventions (e.g., organized in their own communities, such as in preschools or schools) that are, where possible, led by peers and/or accessed virtually. Universal interventions also need to include at least one home visit after birth to ascertain if mother and child have the supports they need, and, if difficulties are found, to provide connections to local resources for the family.
To promote these first-level, universal programs, federal, state, and local agencies overseeing program implementation could develop and monitor community-based support groups for mothers within existing programs, such as the MIECHV program, Head Start, Early Head Start, and Special Supplemental Nutrition Program for Women, Infants, and Children. Care providers within these programs require appropriate referral sources for mothers and children who need intensive, one-on-one care (e.g., through home visiting). Enhanced coverage by major insurance providers for programs offering group-based care, support, and therapeutic interventions for mothers is also necessary (see Chapter 5 for more on health care needs for this population).
To identify mothers who might need more intensive services, a brief battery of questionnaires should be used as a screening tool. Specifically, measures of maternal stress and depression (described in this chapter) should be routinely administered at prenatal and pediatric
“well-baby” visits. Those mothers who manifest high distress will need referrals to programs that offer evidence-based therapeutic interventions.
Intensive programs for mothers in distress can be for groups or individuals. Programs that are short term and involve groups of women, such as AC Groups or the Mental health Outreach for Mothers (MOMS) Partnership, can help to maximize both reach and cost-effectiveness. (See Box 4-9 for information on the MOMS Partnership as a promising model.)
Where necessary, mothers in serious distress need to be referred to more resource intensive, one-on-one programs, such as ABC and Infant/Toddler Parent Psychotherapy. Home visiting, with concurrent referrals to available supports as needed—formal and informal—should exist within the community. Ideally, all types of intensive services would be coordinated with the pediatricians’ offices in a team-based approach to providing care (see more on team-based approaches in the health care setting in Chapter 5).
It will be critical to allocate resources to monitoring the quality of interventions delivered. All intervention programs need to be culturally sensitive, be adapted to community needs, have clear procedures for the selection and training of clinicians, and have mechanisms in place to ensure fidelity and quality of services. Support is needed for programs across tier levels of delivery, universal and intensive. Furthermore, taking an ecological perspective on promoting caregiver well-being and attachment would require supportive policies that facilitate healthy social connections and family cohesion during these critical years of early life. For example, paid parental leave following the birth of a child is one policy that has evidence for shaping child and family outcomes (AEI-Brookings Working Group on Paid Family Leave, 2017). (See Chapter 6 for a full discussion and Recommendation 6-1 on implementing paid leave.)
Finally, in evaluating the effectiveness of programs for at-risk mothers and their children, measures need to focus on those maternal dimensions that are known to strongly affect the mother–child relationship and hence child well-being. This would include measures of maternal depression and stress, feelings of rejection or hostility to the child, available support for mothers, and any contact with CPS. These assessments should be a routine part of prenatal, postnatal, and pediatric visits, along with other physical health indexes that are assessed and recorded. Careful, balanced consideration of all of these aspects of intervention design, delivery, and measurement—with all of the investment of resources called for by each aspect—is critical to move toward meaningfully increasing equity in wellbeing, considering America’s most vulnerable children and families.
REFERENCES
ACF (Administration for Children and Families). 2018. Implementing Attachment and Biobehavioral Catch-up intervention. https://homvee.acf.hhs.gov/Implementation/3/Attachment-and-Biobehavioral-Catch-Up-ABC--Intervention-Model-Overview/51 (accessed January 11, 2019).
Acker, J., P. Braveman, E. Arkin, L. Leviton, J. Parsons, and G. Hobor. 2019. Mass incarceration threatens health equity in America. Princeton, NJ: Robert Wood Johnson Foundation.
Adams, T. R., E. D. Handley, J. T. Manly, D. Cicchetti, and S. L. Toth. 2019. Intimate partner violence as a mechanism underlying the intergenerational transmission of maltreatment among economically disadvantaged mothers and their adolescent daughters. Development & Psychopathology 31(1):83–93.
AEI-Brookings Working Group on Paid Family Leave. 2017. Paid family and medical leave: An issue whose time has come. Washington, DC: The Brookings Institution.
Ammerman, R. T., F. W. Putnam, J. Stevens, L. J. Holleb, A. L. Novak, and J. B. Van Ginkel. 2005. In-home cognitive behavior therapy for depression: An adapted treatment for first time mothers in home visitation. Best Practices in Mental Health 1:1–14.
Antonucci, T. C., K. J. Ajrouch, and K. S. Birditt. 2014. The convoy model: Explaining social relations from a multidisciplinary perspective. Gerontologist 54(1):82–92.
Assari, S., and C. H. Caldwell. 2018. High risk of depression in high-income African American boys. Journal of Racial and Ethnic Health Disparities 5(4):808–819.
Assari, S., F. X. Gibbons, and R. L. Simons. 2018a. Perceived discrimination among black youth: An 18-year longitudinal study. Behavioral Sciences 8(5).
Assari, S., B. Preiser, M. M. Lankarani, and C. H. Caldwell. 2018b. Subjective socioeconomic status moderates the association between discrimination and depression in African American youth. Brain Sciences 8(4).
ASU (Arizona State University) Reach Institute. 2018. Family check-up for providers. https://reachinstitute.asu.edu/family-check-up/agencies (accessed May 2, 2019).
Attachment Biobehavioral Catch-Up. 2017. The Attachment Biobehavioral Catch-up (ABC) program. http://www.abcintervention.org/about (accessed January 11, 2019).
Avellar, S. A., and L. H. Supplee. 2013. Effectiveness of home visiting in improving child health and reducing child maltreatment. Pediatrics 132:S90–S99.
Avellar, S., R. Covington, Q. Moore, A. Patnaik, and A. Wu. 2019. Effects of four responsible fatherhood programs for low income fathers: Evidence from the parents and children together evaluation. OPRE Report 2019-05. Washington, DC: Office of Planning, Research, and Evaluation, Administration for Children and Families, U.S. Department of Health and Human Services.
Balaji, A. B., A. H. Claussen, D. C. Smith, S. N. Visser, M. J. Morales, and R. Perou. 2007. Social support networks and maternal mental health and well-being. Journal of Women’s Health (Larchmt) 16(10):1386–1396.
Barlow, A., B. Mullany, N. Neault, N. Goklish, T. Billy, R. Hastings, S. Lorenzo, C. Kee, K. Lake, C. Redmond, A. Carter, and J. T. Walkup. 2015. Paraprofessional-delivered home-visiting intervention for American Indian teen mothers and children: 3-year outcomes from a randomized controlled trial. American Journal of Psychiatry 172(2):154–162.
Barlow, K., and B. L. Chapin. 2010. The practice of mothering: An introduction. Ethos 38(4):324–338.
Barone, L., F. Lionetti, and J. Green. 2017. A matter of attachment? How adoptive parents foster post-institutionalized children’s social and emotional adjustment. Attachment & Human Development 19(4):323–339.
Baumeister, R. F., E. Bratslavsky, C. Finkenauer, and K. D. Vohs. 2001. Bad is stronger than good. Review of General Psychology 5(4):323–370.
Becares, L., and N. Priest. 2015. Understanding the influence of race/ethnicity, gender, and class on inequalities in academic and non-academic outcomes among eighth-grade students: Findings from an intersectionality approach. PLoS ONE 10(10):e0141363.
Bernard, K., R. Simons, and M. Dozier. 2015. Effects of an attachment-based intervention on child protective services—referred mothers’ event-related potentials to children’s emotions. Child Development 86(6):1673–1684.
Bick, J., and M. Dozier. 2013. The effectiveness of an attachment-based intervention in promoting foster mothers’ sensitivity toward foster infants. Infant Mental Health Journal 34(2):95–103.
Bloch, J. R., D. A. Webb, L. Mathews, E. F. Dennis, I. M. Bennett, and J. F. Culhane. 2010. Beyond marital status: The quality of the mother-father relationship and its influence on reproductive health behaviors and outcomes among unmarried low income pregnant women. Maternal & Child Health Journal 14(5):726–734.
Bolger, K. E., and C. J. Patterson. 2003. Sequelae of child maltreatment: Vulnerability and resilience. In Resilience and vulnerability: Adaptation in the context of childhood adversities, edited by S. S. Luthar. New York: Cambridge University Press. Pp. 156–181.
Borden, L. A., T. R. Schultz, K. C. Herman, and C. M. Brooks. 2010. The Incredible Years parent training program: Promoting resilience through evidence-based prevention groups. Group Dynamics: Theory, Research, and Practice 14(3):230–241.
Bouza, J., D. E. Camacho-Thompson, G. Carlo, X. Franco, C. García Coll, L. C. Halgunseth, A. Marks, G. Livas Stein, C. Suarez-Orozco, and R. M. B. White. 2018. The science is clear: Separating families has long-term damaging psychological and health consequences for children, families, and communities. Washington, DC: Society for Research in Child Development.
Bowleg, L. 2012. The problem with the phrase women and minorities: Intersectionality—an important theoretical framework for public health. American Journal of Public Health 102(7):1267–1273.
Brennan, L. M., E. C. Shelleby, D. S. Shaw, F. Gardner, T. J. Dishion, and M. Wilson. 2013. Indirect effects of the Family Check-up on school-age academic achievement through improvements in parenting in early childhood. Journal of Educational Psychology 105(3):762.
Bronfenbrenner, U. 1979. The ecology of human development: Experiments by nature and design. London, UK: Harvard University Press.
Brooks-Gunn, J., and G. J. Duncan. 1997. The effects of poverty on children. The Future of Children 7(2):55–71.
Brown, T. H., L. J. Richardson, T. W. Hargrove, and C. S. Thomas. 2016. Using multiple-hierarchy stratification and life course approaches to understand health inequalities: The intersecting consequences of race, gender, SES, and age. Journal of Health and Social Behavior 57(2):200–222.
Bryan, A. E., and H. Arkowitz. 2015. Meta-analysis of the effects of peer-administered psychosocial interventions on symptoms of depression. American Journal of Community Psychology 55(3–4):455–471.
Burwick, A., H. Zaveri, L. Shang, K. Boller, D. Daro, and D. A. Strong. 2014. Costs of early childhood home visiting: An analysis of programs implemented in the supporting evidence-based home visiting to prevent child maltreatment initiative. Princeton, NJ: Mathematica Policy Research, Inc.
Cabrera, N. J., J. D. Shannon, and C. S. Tamis-LeMonda. 2007. Fathers’ influence on their children’s cognitive and emotional development: From toddlers to pre-K. Applied Developmental Science 11(4):208–213.
Cabrera, N. J., H. E. Fitzgerald, R. H. Bradley, and L. Roggman. 2014. The ecology of father-child relationships: An expanded model. Journal of Family Theory and Review 6:336–354.
Cabrera, N. J., L. Torres, R. Dion, and S. Baumgartner. 2015. H-pact: A descriptive study of responsible fatherhood programs serving hispanic men. OPRE report 2015-112. Washington, DC: Office of Planning, Research and Evaluation, Administration for Children and Families, U.S. Department of Health and Human Services.
Cannon, J. S., M. R. Kilburn, L. A. Karoly, T. Mattox, A. N. Muchow, and M. Buenaventura. 2017. Investing early: Taking stock of outcomes and economic returns from early childhood programs. Santa Monica, CA: RAND Corporation.
Casey, B. J., A. Galvan, and L. H. Somerville. 2016. Beyond simple models of adolescence to an integrated circuit-based account: A commentary. Developmental Cognitive Neuroscience 17:128–130.
Casillas, K. L., A. Fauchier, B. T. Derkash, and E. F. Garrido. 2016. Implementation of evidence-based home visiting programs aimed at reducing child maltreatment: A meta-analytic review. Child Abuse & Neglect 53:64–80.
CDC (Centers for Disease Control and Prevention). 2014. Understanding Child Maltreatment. https://www.cdc.gov/violenceprevention/pdf/cm-factsheet--2013.pdf (accessed April 2, 2019).
CDC. 2017. LGBT youth. https://www.cdc.gov/lgbthealth/youth.htm (accessed June 14, 2019).
Center on the Developing Child at Harvard University. 2010. The foundations of lifelong health are built in early childhood. Cambridge, MA: Harvard University.
Center on the Developing Child at Harvard University. 2011. Building the brain’s “air traffic control” system: How early experiences shape the development of executive function: Working paper no. 11. Cambridge, MA: Harvard University.
Center on the Developing Child at Harvard University. 2016. From best practices to breakthrough impacts: A science-based approach to building a more promising future for young children and families. Cambridge, MA: Harvard University.
Center on the Developing Child at Harvard University. 2019. MOMS partnership. https://developingchild.harvard.edu/innovation-application/innovation-in-action/moms (accessed June 10, 2019).
Christian, S. 2009. Children of incarcerated parents. Washington, DC: National Conference of State Legislatures.
Cicchetti, D. 2010. Resilience under conditions of extreme stress: A multilevel perspective. World Psychiatry 9(3):145–154.
Cicchetti, D. 2013. Annual research review: Resilient functioning in maltreated children—past, present, and future perspectives. Journal of Child Psychology and Psychiatry 54(4):402–422.
Cicchetti, D., and R. Rizley. 1981. Developmental perspectives on the etiology, intergenerational transmission, and sequelae of child maltreatment. New Directions for Child and Adolescent Development 11:31–55.
Cicchetti, D., and S. L. Toth. 2015. Child maltreatment. In Handbook of child psychology and developmental science: Socioemotional process, 7th ed. Vol. 3, edited by M. E. Lamb and R. M. Lerner. Hoboken, NJ: John Wiley & Sons.
Cicchetti, D., and S. L. Toth. 2016. Child maltreatment and developmental psychopathology: A multilevel perspective. In Developmental psychopathology: Maladaptation and psychopathology, 3rd ed. Vol. 3, edited by D. Cicchetti. Hoboken, NJ: John Wiley & Sons.
Cicchetti, D., F. A. Rogosch, and S. L. Toth. 2006. Fostering secure attachment in infants in maltreating families through preventive interventions. Development and Psychopathology 18(3):623–649.
Ciciolla, L., and S. S. Luthar. 2019. Invisible household labor and ramifications for adjustment: Mothers as captains of households. Sex Roles 1–20.
Clayton, A., L. Callinan, K. Klem, and M. Smith. 2018. Embracing 2-gen: Findings from the District of Columbia’s TANF survey. New Haven, CT: Yale School of Medicine.
Cohen, J. 1988. Statistical power analysis for the behavioral sciences, 2nd ed. New York: Academic Press.
Cohen, S., T. Kamarck, and R. Mermelstein. 1983. A global measure of perceived stress. Journal of Health and Social Behavior 24(4):385–396.
Coley, R. L., J. Sims, E. Dearing, and B. Spielvogel. 2018. Locating economic risks for adolescent mental and behavioral health: Poverty and affluence in families, neighborhoods, and schools. Child Development 89(2):360–369.
Conger, R. D., and K. J. Conger. 2002. Resilience in Midwestern families: Selected findings from the first decade of a prospective, longitudinal study. Journal of Marriage and Family 64:361–373.
Crnic, K. 1983. Inventory of parent experiences. University Park, PA: The Pennsylvania State University, Department of Psychology.
Crowl, A., A. Soyeon, and J. Baker. 2008. A meta-analysis of developmental outcomes for children of same-sex and heterosexual parents. Journal of GLBT Family Studies 4(3):385–407.
Dahl, R. E. 2004. Adolescent brain development: A period of vulnerabilities and opportunities. Keynote address. Annals of the New York Academy of Sciences 1021:1–22.
Davison, K. K., A. Gavarkovs, B. McBride, M. Kotelchuck, R. Levy, and E. M. Taveras. 2019. Engaging fathers in early obesity prevention during the first 1,000 days: Policy, systems, and environmental change strategies. Obesity (Silver Spring) 27(4):525–533.
Denmark, N., K. Peplinski, M. Sparr, J. Labiner-Wolfe, S. Zaid, P. Gupta, and K. M. Miller. 2018. Introduction to the special issue on taking home visiting to scale: Findings from the maternal, infant, and early childhood home visiting program state-led evaluations. Maternal and Child Health Journal 22(Suppl 1):1–2.
Dishion, T. J., and K. Kavanagh. 2003. Intervening in adolescent problem behavior: A family-centered approach. New York: Guilford Press.
Dishion, T. J., D. Shaw, A. Connell, F. Gardner, C. Weaver, and M. Wilson. 2008. The family check-up with high-risk indigent families: Preventing problem behavior by increasing parents’ positive behavior support in early childhood. Child Development 79(5):1395–1414.
Dishion, T. J., L. M. Brennan, D. S. Shaw, A. D. McEachern, M. N. Wilson, and B. Jo. 2014. Prevention of problem behavior through annual family check-ups in early childhood: Intervention effects from home to early elementary school. Journal of Abnormal Child Psychology 42(3):343–354.
Domitrovich, C. E., J. A. Durlak, K. C. Staley, and R. P. Weissberg. 2017. Social-emotional competence: An essential factor for promoting positive adjustment and reducing risk in school children. Child Development 88(2):408–416.
Dong, M., W. H. Giles, V. J. Felitti, S. R. Dube, J. E. Williams, D. P. Chapman, and R. F. Anda. 2004. Insights into causal pathways for ischemic heart disease: Adverse childhood experiences study. Circulation 110(13):1761–1766.
Dorner, L. M., M. F. Orellana, and R. Jiménez. 2008. “It’s one of those things that you do to help the family”: Language brokering and the development of immigrant adolescents. Journal of Adolescent Research 23(5):515–543.
Dozier, M., D. Dozier, and M. Manni. 2002. Recognizing the special needs of infants’ and toddlers’ foster parents: Development of a relational intervention. Zero to Three Bulletin 22:7–13.
Dozier, M., O. Lindhiem, and J. Ackerman. 2005. Attachment and Biobehavioral Catch-up: An intervention targeting empirically identified needs of foster infants. In Duke series in child development and public policy. Enhancing early attachments: Theory, research, intervention, and policy, edited by L. J. Berlin, Y. Ziv, L. Amaya-Jackson, and M. T. Greenberg. New York: Guilford Press.
Drake, B. 2013. Fewer Americans have negative views of more gays raising children. https://www.pewresearch.org/fact-tank/2013/06/25/fewer-americans-have-negative-views-of-more-gays-raising-children (accessed April 19, 2019).
Dube, S. R., D. Fairweather, W. S. Pearson, V. J. Felitti, R. F. Anda, and J. B. Croft. 2009. Cumulative childhood stress and autoimmune diseases in adults. Psychosomatic Medicine 71(2):243–250.
Dudley, K. J., X. Li, M. S. Kobor, T. E. Kippin, and T. W. Bredy. 2011. Epigenetic mechanisms mediating vulnerability and resilience to psychiatric disorders. Neuroscience and Biobehavioral Reviews 35(7):1544–1551.
Eckenrode, J., M. Campa, D. W. Luckey, C. R. Henderson, Jr., R. Cole, H. Kitzman, E. Anson, K. Sidora-Arcoleo, J. Powers, and D. Olds. 2010. Long-term effects of prenatal and infancy nurse home visitation on the life course of youths: 19-year follow-up of a randomized trial. Archives of Pediatric & Adolescent Medicine 164(1):9–15.
Eckenrode, J., M. I. Campa, P. A. Morris, C. R. Henderson, Jr., K. E. Bolger, H. Kitzman, and D. L. Olds. 2017. The prevention of child maltreatment through the Nurse Family Partnership program: Mediating effects in a long-term follow-up study. Child Maltreatment 22(2):92–99.
Elder, G. H. 2018. Children of the Great Depression. New York: Routledge.
Evans, G. W. 2004. The environment of childhood poverty. American Psychologist 59(2):77–92.
Filene, J. H., J. W. Kaminski, L. A. Valle, and P. Cachat. 2013. Components associated with home visiting program outcomes: A meta-analysis. Pediatrics 132(Suppl 2):S100–S109.
Filindra, A., D. Blanding, and C. G. Coll. 2011. The power of context: State-level policies and politics and the educational performance of the children of immigrants in the United States. Harvard Educational Review 81(3):407–438.
Font, S. A., K. Sattler, and E. Gershoff. 2018. Measurement and correlates of foster care placement moves. Child and Youth Services Review 91:248–258.
Fredrickson, B. L., and M. F. Losada. 2005. Positive affect and the complex dynamics of human flourishing. The American Psychologist 60(7):678–686.
Fuligni, A. J., and S. Pedersen. 2002. Family obligation and the transition to young adulthood. Developmental Psychology 38(5):856–868.
Gallagher, M., and R. J. Nelson. 2003. Handbook of psychology, biological psychology (Volume 3). Hoboken, NJ: John Wiley & Sons, Inc.
García Coll, C. T., and A. K. Marks. 2012. The immigrant paradox in children and adolescents: Is becoming American a developmental risk? Washington, DC: American Psychological Association.
García Coll, C., G. Lamberty, R. Jenkins, H. P. McAdoo, K. Crnic, B. H. Wasik, and H. Vazquez Garcia. 1996. An integrative model for the study of developmental competencies in minority children. Child Development 67(5):1891–1914.
Geisz, M. B., and M. Nakashian. 2018. Adolescent wellness: Current perspectives and future opportunities in research, policy, and practice. Princeton, NJ: Robert Wood Johnson Foundation.
Giurgescu, C., L. Fahmy, J. Slaughter-Acey, A. Nowak, C. Caldwell, and D. P. Misra. 2018. Can support from the father of the baby buffer the adverse effects of depressive symptoms on risk of preterm birth in black families? AIMS Public Health 5(1):89–98.
Goemans, A., M. van Geel, and P. Vedder. 2015. Over three decades of longitudinal research on the development of foster children: A meta-analysis. Child Abuse & Neglect 42:121–134.
Goemans, A., M. van Geel, M. van Beem, and P. Vedder. 2016. Developmental outcomes of foster children: A meta-analytic comparison with children from the general population and children at risk who remained at home. Child Maltreatment 21(3):198–217.
Golden, O., A. Hawkins, and W. Bearsdlee. 2011. Home visiting and maternal depression: Seizing the opportunities to help mothers and young children. Washington, DC: The Urban Institute.
Gollner, R., R. I. Damian, B. Nagengast, B. W. Roberts, and U. Trautwein. 2018. It’s not only who you are but who you are with: High school composition and individuals’ attainment over the life course. Psychological Science 29(11):1785–1796.
Goodman, S. H., and J. Garber. 2017. Evidence-based interventions for depressed mothers and their young children. Child Development 88(2):368–377.
Grusec, J. E., and M. Davidov. 2010. Integrating different perspectives on socialization theory and research: A domain-specific approach. Child Development 81(3):687–709.
Hammock, E. A. D., and P. Levitt. 2006. The discipline of neurobehavioral development: The emerging interface of processes that build circuits and skills. Human Development 49(5):294–309.
Hamoudi, A., D. W. Murray, L. Sorensen, and A. Fontaine. 2015. Self-regulation and toxic stress: A review of ecological, biological, and developmental studies of self-regulation and stress. OPRE report #2015-30. Washington, DC: U.S. Department of Health and Human Services, Administration for Children and Families, Office of Planning, Research and Evaluation.
Hankivsky, O., and A. Christoffersen. 2008. Intersectionality and the determinants of health: A Canadian perspective. Critical Public Health 18(3):271–283.
Harold, G. T., L. D. Leve, and R. Sellers. 2017. How can genetically informed research help inform the next generation of interparental and parenting interventions? Child Development 88(2):446–458.
Hill, R. B. 2007. An analysis of racial-ethnic disproportionality and disparity at the national state and county levels. Casey-CSSP Alliance for Racial Equity in Child Welfare.
Hiratsuka, V. Y., M. E. Parker, J. Sanchez, R. Riley, D. Heath, J. C. Chomo, M. Beltangady, and M. Sarche. 2018. Cultural adaptations of evidence-based home-visitation models in tribal communities. Infant Mental Health Journal 39(3):265–275.
Ho, J. 2015. Bicultural children: What parents and teachers should know. Childhood Education 91(1):35–40.
Hofmann, S. G., and S. C. Hayes. 2019. The future of intervention science: Process-based therapy. Clinical Psychological Science: A Journal of the Association for Psychological Science 7(1):37–50.
Hoge, E., D. Bickham, and J. Cantor. 2017. Digital media, anxiety, and depression in children. Pediatrics 140(S2):S76–S80.
Hrdy, S. B. 1999. Mother nature: A history of mothers, infants, and natural selection. New York: The Ballantine Publishing Group.
Hrdy, S. B. 2011. Mothers and others: The evolutionary origins of mutual understanding. Cambridge, MA: Harvard University Press.
HRSA (Health Resources and Services Administration). n.d. The maternal, infant, and early childhood home visiting program: Partnering with parents to help children succeed. https://mchb.hrsa.gov/sites/default/files/mchb/MaternalChildHealthInitiatives/HomeVisiting/pdf/programbrief.pdf (accessed August 13, 2018).
Hughes, D., J. Rodriguez, E. P. Smith, D. J. Johnson, H. C. Stevenson, and P. Spicer. 2006. Parents’ ethnic-racial socialization practices: A review of research and directions for future study. Developmental Psychology 42(5):747–770.
Huston, A. C., V. C. McLoyd, and C. García Coll. 1994. Children and poverty: Issues in contemporary research. Child Development 65(2):275–282.
IOM (Institute of Medicine). 2011. The health of lesbian, gay, bisexual, and transgender people: Building a foundation for better understanding. Washington, DC: The National Academies Press.
Jackson, A. 2015. Strategies for supporting low-income and welfare-dependent parents of young children. In Parenting Matters: Supporting Parents of Children Ages 0–8, Appendix A. Public Information-Gathering Session Agenda, meeting 2, panel: Addressing the Needs of Specific Populations. National Academies of Sciences, Engineering, and Medicine. Washington, DC: The National Academies Press. P. 397.
Jackson, A. P. 2000. Maternal self-efficacy and children’s influence on stress and parenting among single black mothers in poverty. Journal of Family Issues 21(1):3–16.
Johnson, K. 2019. Medicaid and home visiting: The state of states’ approaches. https://ccf.georgetown.edu/wp-content/uploads/2019/01/Medicaid-and-Home-Visiting.pdf (accessed March 20, 2019).
Jolly, S., K. A. Griffith, R. DeCastro, A. Stewart, P. Ubel, and R. Jagsi. 2014. Gender differences in time spent on parenting and domestic responsibilities by high-achieving young physician-researchers. Annals of Internal Medicine 160(5):344–353.
Jones, T. L., and R. J. Prinz. 2005. Potential roles of parental self-efficacy in parent and child adjustment: A review. Clinical Psychology Review 25(3):341–363.
Jones Harden, B. 2004. Safety and stability for foster children: A developmental perspective. The Future of Children 14(1):31–47.
Jonson-Reid, M., B. Drake, J. N. Constantino, M. Tandon, L. Pons, P. Kohl, S. Roesch, E. Wideman, A. Dunnigan, and W. Auslander. 2018. A randomized trial of home visitation for CPS-involved families: The moderating impact of maternal depression and CPS history. Child Maltreatment 23(3):281–293.
Kalil, A., R. Ryan, and M. Corey. 2012. Diverging destinies: Maternal education and the developmental gradient in time with children. Demography 49(4):1361–1383.
Kalmakis, K.A., and G. E. Chandler. 2015. Health consequences of adverse childhood experiences: A systematic review. Journal of the American Association of Nurse Practitioners 27(8):457–465.
Kaufman, J. S., and E. Ziegler. 1987. Do abused children become abusive parents? American Journal of Orthopsychiatry 57(2):186–192.
Kazdin, A. E., and S. M. Rabbitt. 2013. Novel models for delivering mental health services and reducing the burdens of mental illness. Clinical Psychological Science 1(2):170–191.
Kelly, J. F., B. Hoeppner, R. L. Stout, and M. Pagano. 2012. Determining the relative importance of the mechanisms of behavior change within Alcoholics Anonymous: A multiple mediator analysis. Addiction 107(2):289–299.
Kitzman, H., D. L. Olds, D. R. J. Henderson, C. A. Hanks, R. Cole, R. Tatelbaum, and K. Barnard. 1997. Effects of home visitation by nurses on pregnancy outcomes, childhood injuries, and repeated childbearing: A randomized controlled trial. JAMA 278(8):644–652.
Knitzer, J. 2000. Early childhood mental health services: A policy and systems development perspective. In Handbook of early childhood intervention, 2nd ed., edited by J. P. Shonkoff and S. J. Meisels. Cambridge, MA: Cambridge University Press. Pp. 416–438.
Koplewicz, H. S., A. Gurian, and K. Williams. 2009. The era of affluence and its discontents. Journal of the American Academy of Child and Adolescent Psychiatry 48(11):1053–1055.
Kopp, C. 2013. Becoming female: Perspectives on development. New York: Springer. Pp. 313–332.
Kotelchuck, M., and M. Lu. 2017. Father’s role in preconception health. Maternal and Child Health Journal 21(11):2025–2039.
Lamb, M. E. 2004. The role of the father in child development. New York: Wiley.
Lareau, A., and E. B. Weininger. 2008. Time, work, and family life: Reconceptualizing gendered time patterns through the case of children’s organized activities. Sociological Forum 23:419–454.
Lee, S., H. S. Juon, G. Martinez, C. E. Hsu, E. S. Robinson, J. Bawa, and G. X. Ma. 2009. Model minority at risk: Expressed needs of mental health by Asian American young adults. Journal of Community Health 34(2):144–152.
Lee, S. J., C. A. Taylor, and J. L. Bellamy. 2012. Paternal depression and risk for child neglect in father-involved families of young children. Child Abuse and Neglect 36(5):461–469.
Leloux-Opmeer, H., C. Kuiper, H. Swaab, and E. Scholte. 2016. Characteristics of children in foster care, family-style group care, and residential care: A scoping review. Journal of Child and Family Studies 25:2357–2371.
Lerner, R. M., and W. F. Overton. 2017. Reduction to absurdity: Why epigenetics invalidates all models involving genetic reduction. Human Development 60(2–3):107–123.
Leve, L. D., G. T. Harold, P. Chamberlain, J. A. Landsverk, P. A. Fisher, and P. Vostanis. 2012. Practitioner review: Children in foster care—vulnerabilities and evidence-based interventions that promote resilience processes. Journal of Child Psychology and Psychiatry 53(12):1197–1211.
Lewis, C., and M. E. Lamb. 2003. Fathers’ influences on children’s development: The evidence from two-parent families. European Journal of Psychology of Education 18(2):211–228.
Lewis, T. T., and M. E. Van Dyke. 2018. Discrimination and the health of African Americans: The potential importance of intersectionalities. Current Directions in Psychological Science 27(3):176–182.
Lieberman, A. F., and C. H. Zeanah. 1999. Contributions of attachment theory to infant-parent psychotherapy and other interventions with infants and young children. In Handbook of attachment, edited by J. Cassidy and P. R. Shaver. New York: Guilford Press. Pp. 555–574.
Lieberman, A. F., E. Padron, P. Van Horn, and W. W. Harris. 2005. Angels in the nursery: The intergenerational transmission of benevolent parental influences. Infant Mental Health Journal 26(6):504–520.
Lieberman, A. F., A. Chu, P. Van Horn, and W. W. Harris. 2011. Trauma in early childhood: Empirical evidence and clinical implications. Development and Psychopathology 23(2):397–410.
Lind, T., K. Bernard, E. Ross, and M. Dozier. 2014. Intervention effects on negative affect of CPS-referred children: Results of a randomized clinical trial. Child Abuse & Neglect 38(9):1459–1467.
Lino, M., K. Kuczynski, N. Rodriguez, and T. Schap. 2017. Expenditures on children by families, 2015. Miscellaneous publication no. 1528-2015. Alexandria, VA: U.S. Department of Agriculture, Center for Nutrition Policy & Promotion.
Lu, M. C., L. Jones, M. J. Bond, K. Wright, M. Pumpuang, M. Maidenberg, D. Jones, C. Garfield, and D. L. Rowley. 2010. Where is the F in MCH? Father involvement in African American Families. Ethnicity and Disease 20:S2–S49.
Lund, T. J., E. Dearing, and H. D. Zachrisson. 2017. Is affluence a risk for adolescents in Norway? Journal of Research on Adolescence 27(3):628–643.
Lunkenheimer, E. S., T. J. Dishion, D. S. Shaw, A. M. Connell, F. Gardner, M. N. Wilson, and E. M. Skuban. 2008. Collateral benefits of the Family Check-up on early childhood school readiness: Indirect effects of parents’ positive behavior support. Developmental Psychology 44(6):1737–1752.
Luthar, S. S. 2015. Mothering mothers. Research in Human Development 12(3–4):295–303.
Luthar, S. S., and L. Ciciolla. 2015. Who mothers mommy? Factors that contribute to mothers’ well-being. Developmental Psychology 51(12):1812–1823.
Luthar, S. S., and N. Eisenberg. 2017. Resilient adaptation among at-risk children: Harnessing science toward maximizing salutary environments. Child Development 88(2):337–349.
Luthar, S. S., and N. L. Kumar. 2018. Youth in high-achieving schools: Challenges to mental health and directions for evidence-based interventions. In Handbook of school-based mental health promotion, edited by A. W. Leschied, D. H. Saklofske, and G. L. Flett. Pp. 441–458.
Luthar, S. S., and C. C. Sexton. 2007. Maternal drug abuse versus maternal depression: Vulnerability and resilience among school-age and adolescent offspring. Development and Psychopathology 19(1):205–225.
Luthar, S. S., and N. E. Suchman. 2000. Relational psychotherapy mothers’ group: A developmentally informed intervention for at-risk mothers. Development and Psychopathology 12(2):235–253.
Luthar, S. S., N. E. Suchman, and M. Altomare. 2007. Relational psychotherapy mothers’ group: A randomized clinical trial for substance abusing mothers. Development and Psychopathology 19(1):243–261.
Luthar, S. S., S. H. Barkin, and E. J. Crossman. 2013. “I can, therefore I must”: Fragility in the upper-middle classes. Development and Psychopathology 25(4 Pt. 2):1529–1549.
Luthar, S., E. J. Crossman, and P. J. Small. 2015. Resilience and adversity. In Handbook of child psychology and developmental science, 7th ed., Vol. 3, edited by R. M. Lerner and M. E. Lamb. New York: Wiley. Pp. 247–286.
Luthar, S. S., A. Curlee, S. J. Tye, J. C. Engelman, and C. M. Stonnington. 2017. Fostering resilience among mothers under stress: “Authentic connections groups” for medical professionals. Women’s Health Issues 27(3):382–390.
Luthar, S. S., N. L. Kumar, and R. Benoit. In press. Authentic connections virtual groups: Fostering resilience among mothers in high-stress settings. Development and Psychopathology.
Macmillan, H. L., C. N. Wathen, J. Barlow, D. M. Fergusson, J. M. Leventhal, and H. N. Taussig. 2009. Interventions to prevent child maltreatment and associated impairment. The Lancet 373(9659):250–266.
Marks, A. K., J. L. McKenna, and C. García Coll. 2018. National immigration receiving contexts: A critical aspect of native-born, immigrant, and refugee youth well-being. European Psychologist 23(1):6–20.
Marmot, M., J. Allen, P. Goldblatt, T. Boyce, D. McNeish, and M. Grady. 2010. Fair society, healthy lives: Strategic review of health inequalities in England post-2010. The Marmot Review. http://www.instituteofhealthequity.org/resources-reports/fair-society-healthy-lives-the-marmot-review/fair-society-healthy-lives-full-report-pdf.pdf (accessed August 25, 2019).
Maslow, A. H. 1943. A theory of human motivation. Psychological Review 50(4):370–396.
Masten, A. S. 2014. Global perspectives on resilience in children and youth. Child Development 85(1):6–20.
Mazure, C. M., and D. P. Jones. 2015. Twenty years and still counting: Including women as participants and studying sex and gender in biomedical research. BMC Women’s Health 15:94.
McCambell, S. W. 2005. Gender-responsive strategies—for women offenders. Washington, DC: U.S. Department of Justice.
McEachern, A. D., G. M. Fosco, T. J. Dishion, D. S. Shaw, M. N. Wilson, and F. Gardner. 2013. Collateral benefits of the Family Check-up in early childhood: Primary caregivers’ social support and relationship satisfaction. Journal of Family Psychology 27(2):271–281.
McGinnis, S., E. Lee, K. Kirkland, C. Smith, C. Miranda-Julian, and R. Greene. 2018. Engaging at-risk fathers in home visiting services: Effects on program retention and father involvement. Child & Adolescent Social Work Journal 36(2):189–200.
McLeod, S. 2018. Maslow’s Hierarchy of Needs. https://www.simplypsychology.org/maslow.html (accessed January 24, 2019).
McLoyd, V. C. 1990. The impact of economic hardship on black families and children: Psychological distress, parenting, and socioemotional development. Child Development 61:311–346.
Michalopoulos, C., K. Faucetta, C. J. Hill, X. A. Portilla, L. Burrell, H. Lee, A. Dugggan, and V. Knox. 2019. Impacts on family outcomes of evidence-based early childhood home visiting-results from the Mother and Infant Home Visiting Program Evaluation. Washington, DC: U.S. Department of Health and Human Services, Administration for Children and Families, Office of Planning, Research and Evaluation.
Minkovitz, C. S., K. M. O’Neill, and A. K. Duggan. 2016. Home visiting: A service strategy to reduce poverty and mitigate its consequences. Academic Pediatrics 16(Suppl 3):S105–S111.
Modecki, K. L., M. J. Zimmer-Gembeck, and N. Guerra. 2017. Emotion regulation, coping, and decision making: Three linked skills for preventing externalizing problems in adolescence. Child Development 88(2):417–426.
MOMS (Mental health Outreach for Mothers) Partnership. n.d.-a. Impact. https://medicine.yale.edu/psychiatry/moms/impact (accessed June 10, 2019).
MOMS Partnership. n.d.-b. Where we’re going. https://medicine.yale.edu/psychiatry/moms/where/where.aspx (accessed June 10, 2019).
MOMS Partnership. n.d.-c. Who we are. https://medicine.yale.edu/psychiatry/moms/are/who.aspx (accessed January 28, 2019).
Morris, A. S., L. R. Robinson, J. Hays-Grudo, A. H. Claussen, S. A. Hartwig, and A. E. Treat. 2017. Targeting parenting in early childhood: A public health approach to improve outcomes for children living in poverty. Child Development 88(2):388–397.
Moseley, K. L., G. L. Freed, C. M. Bullard, and S. D. Goold. 2007. Measuring African-American parent’s cultural mistrust while in a healthcare setting. Journal of the Medical Association 99(1):15–21.
Moss, M., and M. Puma. 1995. Prospects: The congressionally mandated study of educational growth and opportunity. First year report on language minority and limited English proficient students. Washington, DC: U.S. Department of Education, Office of Bilingual Education and Minority Languages Affairs.
Murgatroyd, C., and D. Spengler. 2011. Epigenetics of early child development. Frontiers in Psychiatry 2:16.
Murray, J., and L. Murray. 2010. Parental incarceration, attachment and child psychopathology. Attachment & Human Development 12(4):289–309.
Murray, J., D. P. Farrington, and I. Sekol. 2012. Children’s antisocial behavior, mental health, drug use, and educational performance after parental incarceration: A systematic review and meta-analysis. Psychological Bulletin 138(2):175–210.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Parenting matters: Supporting parents of children ages 0–8. Washington, DC: The National Academies Press.
NASEM. 2017. Communities in action: Pathways to health equity. Washington, DC: The National Academies Press.
National Partnership for Women & Families. 2018. Raising expectations: A state-by-state analysis of laws that help working family caregivers. Washington, DC: National Partnership for Women & Families.
National Scientific Council on the Developing Child. 2004. Young children develop in an environment of relationships (working paper 1). Cambridge, MA: Center on the Developing Child at Harvard University.
National Scientific Council on the Developing Child. 2010. Early experiences can alter gene expression and affect long-term development. Working paper no. 10. Cambridge, MA: Center on the Developing Child at Harvard University.
NCSL (National Conference of State Legislators). 2019. Family First Prevention Services Act. http://www.ncsl.org/research/human-services/family-first-prevention-services-actffpsa.aspx (accessed June 4, 2019).
Ngo, B., and S. J. Lee. 2007. Complicating the image of model minority success: A review of southeast Asian American education. Review of Educational Research 77(4):415–453.
NHVRC (National Home Visiting Resource Center). 2018. 2018 home visiting yearbook. https://www.nhvrc.org/wp-content/uploads/NHVRC_Yearbook_2018_FINAL.pdf (accessed March 20, 2019).
NICWA (National Indian Child Welfare Association). 2017. What is disproportionality in child welfare? https://www.nicwa.org/wp-content/uploads/2017/09/Disproportionality-Table.pdf (accessed June 4, 2019).
NRC (National Research Council). 2014. The growth of incarceration in the United States: Exploring causes and consequences. Washington, DC: The National Academies Press.
NRC and IOM. 2000. From neurons to neighborhoods: The science of early childhood development. Washington, DC: National Academy Press.
Olds, D. L., J. Eckenrode, C. R. Henderson, Jr., H. Kitzman, J. Powers, R. Cole, and D. Luckey. 1997. Long-term effects of home visitation on maternal life course and child abuse and neglect: 15-year follow-up of a randomized trial. JAMA 278(8):637–643.
Olds, D. L., H. Kitzman, C. Hanks, R. Cole, E. Anson, K. Sidora-Arcoleo, D. W. Luckey, C. R. Henderson, Jr., J. Holmberg, R. A. Tutt, A. J. Stevenson, and J. Bondy. 2007. Effects of nurse home visiting on maternal and child functioning: Age-9 follow-up of a randomized trial. Pediatrics 120(4):e832–e845.
OPRE (Office of Planning, Research and Evaluation). 2018. Home visiting models reviewing evidence of effectiveness. https://homvee.acf.hhs.gov/homevee_executive_summary_brief.pdf#Brief1 (accessed July 15, 2019).
Padilla, A. 2008. Developmental processes related to intergenerational transmission of culture. In Cultural transmission: Psychological, developmental, social, and methodological aspects, edited by U. E. Schonpflug. Cambridge, MA: Cambridge University Press. Pp. 185–211.
Parke, R. D., and K. A. Clarke-Stewart. 2001. Effects of parental incarceration on young children. Bethesda, MD: Office of the Assistant Secretary for Planning and Evaluation.
Paulsell, D., P. Del Grosso, and L. Supplee. 2014. Supporting replication and scale-up of evidence-based home visiting programs: Assessing the implementation knowledge base. American Journal of Public Health 104(9):1624–1632.
Pears, K. C., and D. M. Capaldi. 2001. Intergenerational transmission of abuse: A two-generational prospective study of an at-risk sample. ChildAbuse & Neglect 25(11):1439–1461.
Pekrun, R., K. Murayama, H. W. Marsh, T. Goetz, and A. C. Frenzel. 2019. Happy fish in little ponds: Testing a reference group model of achievement and emotion. Journal of Personality and Social Psychology 117(1):166–185.
Phares, V., E. Lopez, S. Fields, D. Kamboukos, and A. M. Duhig. 2005. Are fathers involved in pediatric psychology research and treatment? Journal of Pediatric Psychology 30(8):631–643.
Plant, D. T., E. D. Barker, C. S. Waters, S. Pawlby, and C. M. Pariante. 2013. Intergenerational transmission of maltreatment and psychopathology: The role of antenatal depression. Psychological Medicine 43(3):519–528.
Plantin, L., A. A. Olukoya, and P. Ny. 2011. Positive health outcomes of fathers’ involvement in pregnancy and childbirth paternal support: A scope study literature review. Fathering 9(1):87–102.
Pratt, J., and R. Chapman. n.d. Culture, collaboration, and innovation: How tribal home visiting programs are working to improve outcomes for children, families, and communities. https://www.acf.hhs.gov/sites/default/files/ecd/4478_thv_culture_collaboration_and_innovation_synthesis_report_final.pdf (accessed June 5, 2019).
Pruett, M. K., K. Pruett, C. P. Cowan, and P. A. Cowan. 2017. Enhancing father involvement in low-income families: A couples group approach to preventive intervention. Child Development 88(2):398–407.
Purewal, S. K., M. Bucci, L. G. Wang, K. Koita, S. S. Marques, D. Oh, and N. B. Harris. 2016. Screening for adverse childhood experiences (ACEs) in an integrated pediatric care model. Zero to Three 36(3):10–17.
Rae, J. R., S. Gulgoz, L. Durwood, M. DeMeules, R. Lowe, G. Lindquist, and K. R. Olson. 2019. Predicting early-childhood gender transitions. Psychological Science 30(5):669–681.
Rahman, A., P. J. Surkan, C. E. Cayetano, P. Rwagatare, and K. E. Dickson. 2013. Grand challenges: Integrating maternal mental health into maternal and child health programmes. PLoS Medicine 10(5):e1001442.
Ramey, G., and V. A. Ramey. 2010. The rug rat race. Brookings Papers on Economic Activity 41(1):129–199.
Reis, H. T., W. A. Collins, and E. Berscheid. 2000. The relationship context of human behavior and development. Psychological Bulletin 126(6):844–872.
Reynolds, A. J., S. R. Ou, C. F. Mondi, and M. Hayakawa. 2017. Processes of early childhood interventions to adult well-being. Child Development 88(2):378–387.
Rogoff, B. 2003. The cultural nature of human development. New York: Oxford University Press.
Rohner, E. C., R. P. Rohner, and S. Roll. 1980. Perceived parental acceptance-rejection and children’s reported behavioral dispositions: A comparative and intracultural study of American and Mexican children. Journal of Cross-Cultural Psychology 11(2):213–231.
Rotheram-Borus, M. J., J. A. Stein, and Y. Y. Lin. 2001. Impact of parent death and an intervention on the adjustment of adolescents whose parents have HIV/AIDS. Journal of Consulting and Clinical Psychology 69(5):763–773.
Rotheram-Borus, M. J., D. Swendeman, S. J. Lee, L. Li, B. Amani, and M. Nartey. 2011. Interventions for families affected by HIV. Translational Behavioral Medicine 1(2):313–326.
Rutter, M. 1987. Psychosocial resilience and protective mechanisms. The American Journal of Orthopsychiatry 57(3):316–331.
Sama-Miller, E., L. Akers, A. Mraz-Esposito, M. Zukiewicz, S. Avellar, D. Paulsell, and P. Del Grosso. 2018. Home visiting evidence of effectiveness review: Executive summary. OPRE Report #2017-58. Washington, DC: U.S. Department of Health and Human Services.
Sampson, R. J., and J. H. Laub. 2003. Desistance from crime over the life course. In Handbook of the life course. Boston, MA: Springer.
Sandstrom, H. 2019. Early childhood home visiting programs and health. Health Affairs Health Policy Brief, April 25, 2019.
Schwartz, S. J., J. B. Unger, S. E. Des Rosiers, S. Huang, L. Baezconde-Garbanati, E. I. Lorenzo-Blanco, J. A. Villamar, D. W. Soto, M. Pattarroyo, and J. Szapocznik. 2012. Substance use and sexual behavior among recent Hispanic immigrant adolescents: Effects of parent-adolescent differential acculturation and communication. Drug and Alcohol Dependence 125(Suppl 1):S26–S34.
Schwebel, D. C., and C. M. Brezausek. 2010. How do mothers and fathers influence pediatric injury risk in middle childhood? Journal of Pediatric Psychology 35(8):806–813.
Seifer, R. 2003. Young children with mentally ill parents: Resilient developmental systems. In Resilience and vulnerability: Adaptation in the context of childhood adversities, edited by S. S. Luthar. New York: Cambridge University Press. Pp. 29–49.
Shaw, D. S., T. J. Dishion, L. Supplee, F. Gardner, and K. Arnds. 2006. Randomized trial of a family-centered approach to the prevention of early conduct problems: 2–year effects of the Family Check-up in early childhood. Journal of Consulting and Clinical Psychology 74(1):1–9.
Shaw, D. S., A. Connell, T. J. Dishion, M. N. Wilson, and F. Gardner. 2009. Improvements in maternal depression as a mediator of intervention effects on early childhood problem behavior. Development and Psychopathology 21(2):417–439.
Shlafer, R. J., and J. Poehlmann. 2010. Attachment and caregiving relationships in families affected by parental incarceration. Attachment & Human Development 12(4):395–415.
Smith, J. D., S. M. St. George, and G. Prado. 2017. Family-centered positive behavior support interventions in early childhood to prevent obesity. Child Development 88(2):427–435.
Smith, M. 2018. PowerPoint presentation to the Committee on Applying Neurobiological and Socio-Behavioral Sciences from Prenatal Through Early Childhood Development: A Health Equity Approach. Washington, DC. August 6, 2018. http://nationalacademies.org/hmd/~/media/Files/Agendas/Activity%20Files/Children/Prenatal-Early%20Childhood%20Development/2018-AUG-06/2-4%20Smith%20-%20updated.pdf (accessed June 10, 2019).
Sparks, E. A., and R. F. Baumeister. 2008. If bad is stronger than good, why focus on human strength. Positive Psychology: Exploring the Best in People 1:55–79.
Sroufe, L. A., B. Egeland, E. A. Carlson, and W. A. Collins. 2005. The development of the person: The Minnesota study of risk and adaptation from birth to adulthood. New York: Guilford Press.
Steen, M., S. Downe, N. Bamford, and L. Edozien. 2012. Not-patient and not-visitor: A meta-synthesis fathers’ encounters with pregnancy, birth and maternity care. Midwifery 28(4):362–371.
Super, C. M., and S. Harkness. 1986. The developmental niche: A conceptualization at the interface of child and culture. International Journal of Behavioral Development 9:545–569.
Taylor, Z. E., and R. D. Conger. 2017. Promoting strengths and resilience in single-mother families. Child Development 88(2):350–358.
Teeters, A. R., R. T. Ammerman, C. E. Shenk, N. K. Goyal, A. T. Folger, F. W. Putnam, and J. B. Van Ginkel. 2016. Predictors of maternal depressive symptom trajectories over the first 18 months in home visiting. American Journal of Orthopsychiatry 86(4):415–424.
Teitler, J. O. 2001. Father involvement, child health, and maternal health behavior. Children and Youth Services Review 23(4/5):403–425.
The Center for Parents & Children. n.d. The family check-up. https://www.cpc.pitt.edu/intervention-models/the-family-check-up (accessed May 2, 2019).
Toth, S. L., J. A. Gravener-Davis, D. J. Guild, and D. Cicchetti. 2013. Relational interventions for child maltreatment: Past, present, and future perspectives. Development & Psychopathology 25:1601–1607.
Toth, S. L., C. L. M. Petrenko, J. A. Gravener-Davis, and E. D. Handley. 2016. Advances in prevention science: A developmental psychopathology perspective. In Developmental psychopathology, edited by D. Cicchetti. New York: Wiley.
Turney, K. 2014. Stress proliferation across generations? Examining the relationship between parental incarceration and childhood health. Journal of Health and Social Behavior 55(3):302–319.
Twenge, J. M., A. B. Cooper, T. E. Joiner, M. E. Duffy, and S. G. Binau. 2019. Age, period, and cohort trends in mood disorder indicators and suicide-related outcomes in a nationally representative dataset, 2005–2017. Journal of Abnormal Psychology 128(3):185–199.
Umaña-Taylor, A. J., S. M. Quintana, R. M. Lee, W. E. Cross, D. Rivas-Drake, S. Schwartz, M. Syed, T. Yip, E. Seaton, and ERI Study Group. 2014. Ethnic and racial identity during adolescence and into young adulthood: An integrated conceptualization. Child Development 85(1):21–39.
UNM (University of New Mexico). 2011. Connecting children with incarcerated parents. Child Protection Best Practices Bulletin. Pp. 1–6.
Valentino, K. 2017. Relational interventions for maltreated children. Child Development 88(2):359–367.
Vasileva, M., and F. Petermann. 2018. Attachment, development, and mental health in abused and neglected preschool children in foster care: A meta-analysis. Trauma, Violence, & Abuse 19(4):443–458.
Vélez-Agosto, N. M., J. G. Soto-Crespo, M. Vizcarrondo-Oppenheimer, S. Vega-Molina, and C. García Coll. 2017. Bronfenbrenner’s bioecological theory revision: Moving culture from the macro into the micro. Perspectives on Psychological Science 12(5):900–910.
Vogel, C. A., R. H. Bradley, H. H. Raikes, K. Boller, and J. K. Shears. 2006. Relation between father connectedness and child outcomes. Parenting: Science & Practice 6(2):189–209.
Vygotsky, L. S. 1978. Mind in society. Cambridge, MA: Harvard University Press.
Wainright, J. L., and C. J. Patterson. 2008. Peer relations among adolescents with female same-sex parents. Developmental Psychology 44(1):117–126.
Wainright, J. L., S. T. Russell, and C. J. Patterson. 2004. Psychosocial adjustment, school outcomes, and romantic relationships of adolescents with same-sex parents. Child Development 75(6):1886–1898.
Webster-Stratton, C., M. J. Reid, and M. Hammond. 2001. Preventing conduct problems, promoting social competence: A parent and teacher training partnership in Head Start. Journal of Clinical Child Psychology 30(3):283–302.
Weisner, T. S. 2002. Ecocultural understanding of children’s developmental pathways. Human Development 45(4):275–281.
Weisz, J. R., S. Kuppens, M. Y. Ng, R. A. Vaughn-Coaxum, A. M. Ugueto, D. Eckshtain, and K. A. Corteselli. 2019. Are psychotherapies for young people growing stronger? Tracking trends over time for youth anxiety, depression, attention-deficit/hyperactivity disorder, and conduct problems. Perspectives on Psychological Science 14(2):216–237.
West, A., A. K. Duggan, K. Gruss, and C. S. Minkovitz. 2018. Creating a measurement framework for service coordination in maternal and early childhood home visiting: An evidence-informed, expert process. Children and Youth Services Review 89:289–297.
White, R., A. Mosle, and M. Sims. 2018. States leading the way: Practical solutions that lift up children and families. Washington, DC: The Aspen Institute.
Wildeman, C., and E. A. Wang. 2017. Mass incarceration, public health, and widening inequality in the USA. The Lancet 389(10077):1464–1474.
Williams, D. R., S. A. Mohammed, J. Leavell, and C. Collins. 2010. Race, socioeconomic status, and health: Complexities, ongoing challenges, and research opportunities. Annals of the New York Academy of Sciences 1186:69–101.
Wing, R., A. Gjelsvik, M. Nocera, and E. L. McQuaid. 2015. Association between adverse childhood experiences in the home and pediatric asthma. Annals of Allergy, Asthma and Immunology 114(5):379–384.
Wise, P. H. 2009. Confronting social disparities in child health: A critical appraisal of life-course science and research. Pediatrics 124(Suppl 3):S203–S211.
Wong, F., and R. Halgin. 2006. The “model minority”: Bane or blessing for Asian Americans? Journal of Multicultural Counseling and Development 34(1):38–49.
Yamamoto, Y., and J. Li. 2011. Is being quiet a virtue or a problem? Implications of a study on Chinese immigrant children in the U.S. https://www.childresearch.net/papers/multi/2011_01.html (accessed May 2, 2019).
Yarnoff, B., O. Khavjou, C. Bradley, J. Leis, J. Filene, A. Honeycutt, R. Herzfeldt-Kamprath, and K. Peplinski. 2019. Standardized cost estimates for home visiting: Pilot study of the home visiting budget assistance tool (HV-BAT). Maternal and Child Health Journal 23(4):470–478.
Yates, T. M., B. Egeland, and A. Sroufe. 2003. Rethinking resilience. In Resilience and vulnerability: Adaptation in the context of childhood adversities, edited by S. S. Luthar. New York: Cambridge University Press.
Yavorsky, J. E., C. M. Dush, and S. J. Schoppe-Sullivan. 2015. The production of inequality: The gender division of labor across the transition to parenthood. Journal of Marriage and the Family 77(3):662–679.
Yogman, M., and C. F. Garfield. 2016. Fathers’ roles in the care and development of their children: The role of pediatricians. Pediatrics 138(1):e20161128.
Yoshimoto, D. K., N. T. Robertson, and D. K. Hayes. 2014. Insights in public health: The Hawai’i home visiting network: Evidence-based home visiting services in Hawai’i. Hawai’i Journal of Medicine & Public Health: A Journal of Asia Pacific Medicine & Public Health 73(5):155–160.
Zeanah, C. H., and P. D. Zeanah. 1989. Intergenerational transmission of maltreatment: Insights from attachment theory and research. Psychiatry 52(2):177–196.
Zielinski, D. S., J. Eckenrode, and D. L. Olds. 2009. Nurse home visitation and the prevention of child maltreatment: Impact on the timing of official reports. Development and Psychopathology 21(2):441–453.
Zung, W. W. 1965. A self-rating depression scale. Archives of General Psychiatry 12(1):63–70.




































































