1
Introduction1
On August 11, 2020, the Global Forum on Innovation in Health Professional Education (the forum) held a virtual workshop titled Health Professions Faculty for the Future. The 3.5-hour workshop featured presentations from a variety of speakers and also used a chat box and live polling in order to encourage conversation among workshop participants.
The idea for the workshop, said Reamer Bushardt, senior associate dean in the School of Medicine and Health Sciences at The George Washington University and workshop committee member, originated from previous work of the forum. In November 2018, the forum jointly held a workshop with the National Center for Interprofessional Practice and Education called Strengthening the Connection Between Health Professions Education and Practice (NASEM, 2019). At that workshop, stakeholders from more than 15 different health professions came together from across the globe to present and discuss issues including education and training; patient-centered care; delivery and payment models; developing the workforce; and meeting the needs of populations, students, and educators. Workshop participants discussed the definition of a “health professions educator” and explored the knowledge, skills, and abilities that future health professions educators will need. A defining message of the workshop, said Bushardt, was that
___________________
1 The planning committee’s role was limited to planning the workshop, and this Proceedings of a Workshop was prepared by the rapporteurs as a factual account of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants and are not necessarily endorsed or verified by the National Academies of Sciences, Engineering, and Medicine. They should not be construed as reflecting any group consensus.
partnership and alignment between education and practice is critical for success and is built on relationships. He also recollected how the workshop participants brainstormed about the barriers and opportunities for bridging the gap between education and practice, and they discussed the role health professions faculty would play in preparing the future workforce. The outcome was a vision for future health professions educators, said Bushardt, which laid the foundation for this workshop.
WHERE DID THE IDEA FOR HEALTH PROFESSIONS FACULTY FOR THE FUTURE ORIGINATE?
Reamer Bushardt, The George Washington University, and Kathy Chappell, American Nurses Credentialing Center
In preparation for this virtual workshop, Bushardt described his work with Kathy Chappell, senior vice president at the American Nurses Credentialing Center, in creating a pictorial image of a five-step framework for faculty development. Bushardt and Chappell developed their framework based on discussions and ideas generated from the 2018 joint workshop described previously, and they shared their thoughts with others on the workshop planning committee. This framework—that aligns with the Statement of Task (see Box 1-1)—is a work in progress, said Bushardt. The workshop is an opportunity for participants to explore how this proposed framework might be tested, refined, and improved. It is hoped that the workshop’s discussions will contribute to a common framework that can facilitate ongoing innovation in the health professions education community, he said. The ultimate goal is to build a health professions faculty for “shaping a workforce that can navigate a dynamic health care landscape, lead person and family-centered care, seamlessly integrate technology to improve health, and advance health equity.”
Chappell emphasized the importance of thoughtful faculty development, noting that particularly in the era of coronavirus disease 2019 (COVID-19), faculty need the necessary knowledge and skills to be effective educators. She further remarked how there can sometimes be a tension between the role of clinician versus teacher, and that great clinicians who move into faculty positions are often not given the skills they need to be great teachers.
She then introduced the workshop participants to the framework that she and Bushardt developed (see Figure 1-1). There are other frameworks in the literature, noted Chappell, but after reviewing several of them, and realizing there are a fair number of overlapping elements, the two decided to tailor one that would be a better fit for this workshop.
The workshop emphasized diversity, equity, and inclusion—diversity of people and perspectives; equity in policy, practice, and position; and

SOURCE: Presented by Bushardt and Chappell, August 11, 2020.
inclusion via power, voice, and organizational culture—within the four key areas shown in Figure 1-1. For this workshop, diversity is being defined broadly to include race, ethnicity, gender, sexual orientation, and people with physical disabilities, as well as diversity across health professions and sectors. Also of note, was the view that learning extends from education into practice, so the term program development (see Figure 1-1), was meant to include the educational spectrum from faculty development (in education) to continuing professional development (in practice). However, given the time limitations for the workshop, Chappell explained the speakers’ primary focus was on faculty development.
Chappell encouraged workshop participants to give their feedback and input on the framework by using the chat box feature of the virtual meeting. She underscored the importance of participants’ involvement as a critical review, including comments on what steps are missing, which steps work well and which need improvement, what enabling factors and barriers are anticipated, and whether the language used resonates with different health professions fields and stakeholders. “Workshop participants’ input will be used to refine our framework,” she said.
The organization of the workshop followed the five steps of the framework spelled out under four key areas (see Figure 1-2). Steps 1 and 2, building the pipeline and broadening recruitment into health professions education, both fall within the area of “attracting talent.” Steps 3 through 5 work toward training faculty both formally and informally, and evaluating outcomes that are intricately linked to program design. However, Chappell
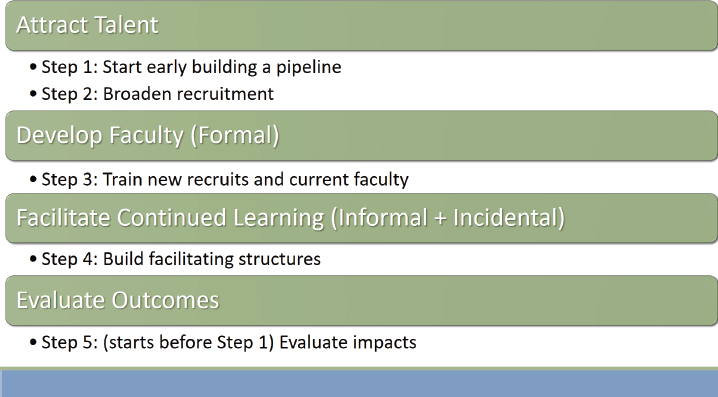
SOURCE: Presented by Bushardt and Chappell, August 11, 2020.
remarked, the workshop will “be starting with the end in mind,” beginning with step 5. By identifying the goals and desired outcomes of a faculty development program first, said Chappell, this becomes the “north star” that guides the program and measures progress.
SETTING THE STAGE: WHAT WE LEARNED FROM YOU!
Lawrence Sherman, Meducate Global, LLC, and Association for Medical Education in Europe
Before diving into the framework, Lawrence Sherman, principal at Meducate Global, LLC, and international development expert at the Association for Medical Education in Europe (AMEE), shared some background on the planning of the workshop that aimed to bring out the interests of the participants expressed through a survey linked to registration. This survey, he said, provided an assessment of the “needs” of the 329 people who registered for the workshop. There were three main results from the responses expressing what registrants hoped to get out of attending the workshop (see Figure 1-3). First, registrants wanted as much interaction and engagement as possible, despite the virtual nature of the experience. Second, they wanted to see technology used to its full capacity. Sherman said this would be accomplished through the use of polls, chat boxes, and other interactive tools. Third, registrants wanted the workshop to serve as a model of best practices for virtual learning (see Appendix D). Sherman

SOURCE: Presented by Sherman, August 11, 2020.
encouraged participants to give feedback in real time to be sure the workshop was meeting the needs and expectations of its attendees.
REFERENCE
NASEM (National Academies of Sciences, Engineering, and Medicine). 2019. Strengthening the connection between health professions education and practice: Proceedings of a joint workshop. Washington, DC: The National Academies Press. https://doi.org/10.17226/25407.






